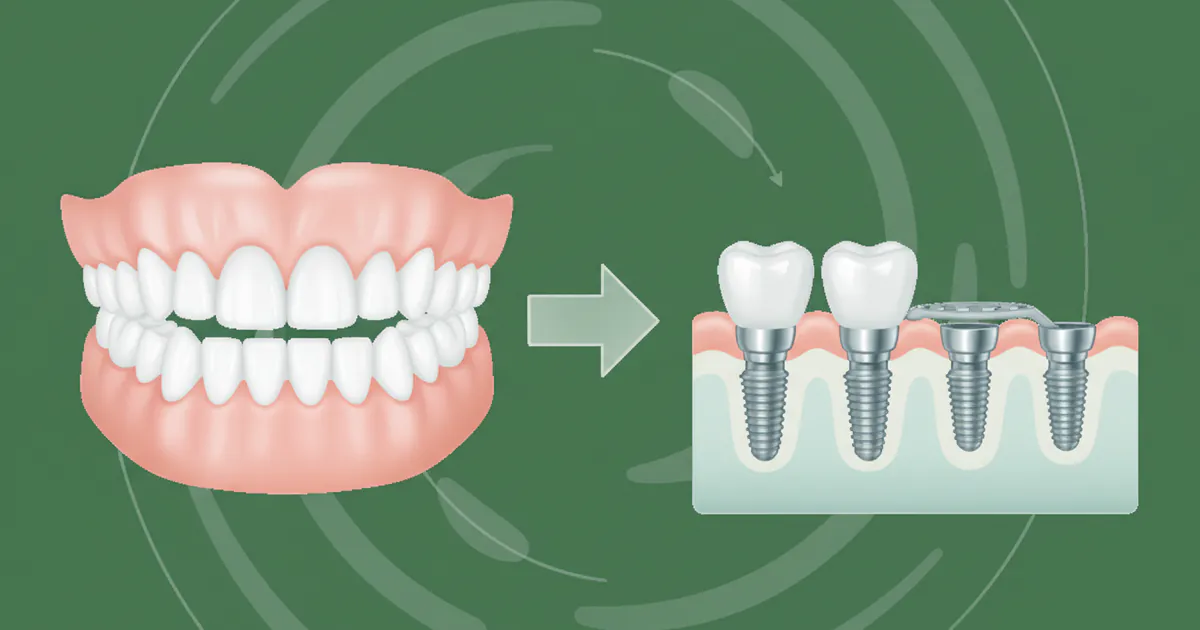
Can I Switch From Dentures to Implants?
Key Takeaways
- Are you among the millions of Americans who wear dentures but dream of a more stable, comfortable, and natural-feeling solution for missing teeth? If you've been wondering, "Can I switch from dentures to implants?", you're not alone. Many denture wearers experience a range of frustrations, from slip
Are you among the millions of Americans who wear dentures but dream of a more stable, comfortable, and natural-feeling solution for missing teeth? If you've been wondering, "Can I switch from dentures to implants?", you're not alone. Many denture wearers experience a range of frustrations, from slipping and discomfort to difficulty eating and speaking, which significantly impact their quality of life. The good news is that advancements in modern dentistry have made the transition from traditional dentures to dental implants not just possible, but a life-changing reality for many.
Dental implants offer a durable, long-term solution that mimics the function and appearance of natural teeth, addressing many of the limitations associated with conventional dentures. They provide unparalleled stability, restore chewing efficiency, preserve jawbone health, and can dramatically boost confidence. This comprehensive guide will walk you through everything you need to know about making the switch, exploring the types of implant solutions available, the step-by-step process, financial considerations including affordable dentures and implant options, recovery, and what to expect on your journey to a healthier, more confident smile.
Key Takeaways:
Key Takeaways:
- Yes, you can absolutely switch from dentures to implants. It's a common and highly successful transition for many individuals seeking improved stability, comfort, and oral health.
- Benefits are significant: Implants prevent bone loss, restore chewing function, eliminate slipping, improve speech, and enhance confidence, often leading to a higher quality of life than traditional dentures.
- Multiple implant options exist: From implant-retained overdentures (removable but stable) to fixed implant-supported bridges (like All-on-4® or All-on-X), solutions cater to varying needs and budgets.
- Bone density is key: Long-term denture wear can lead to jawbone atrophy. Bone grafting may be necessary before implant placement, adding to the treatment timeline and cost.
- Cost varies widely: A single dental implant can range from $3,000 to $6,000, while full-arch solutions like All-on-4® can cost $20,000 to $35,000 per arch. Insurance coverage is typically limited, but financing and payment plans are often available.
- The process involves several stages: This includes initial consultation, bone grafting (if needed), implant placement, a healing period (osseointegration), and finally, the attachment of your new teeth. The entire process can take 4 to 12 months, or even longer if extensive bone grafting is required.
- Long-term success is high: With proper care, dental implants boast a success rate of over 95%, offering a permanent solution that can last decades.
The Denture Dilemma: Why Consider a Switch?
For decades, traditional dentures have been the go-to solution for individuals missing most or all of their teeth. While they restore some level of chewing function and aesthetics, many denture wearers eventually find themselves dissatisfied. Understanding the inherent challenges of traditional dentures helps explain why so many people explore permanent alternatives like dental implants.
What Are Traditional Dentures?
Traditional dentures are removable prosthetic devices designed to replace missing teeth and surrounding tissues. They consist of artificial teeth set in a gum-colored acrylic base, custom-made to fit over your existing gums. Full dentures are used when all teeth in an arch are missing, while partial dentures replace only a few missing teeth.
Common Problems with Traditional Dentures
While affordable dentures and implant options exist, the initial lower cost of traditional dentures often comes with long-term drawbacks:
- Instability and Slipping: Dentures rely solely on suction and the underlying gum ridge for retention. This often leads to slipping, clicking, or even falling out, especially when eating, speaking, or laughing. Adhesives can help, but they don't solve the fundamental issue.
- Reduced Chewing Efficiency: Because they aren't anchored, dentures provide significantly less biting force than natural teeth. This limits food choices, making it difficult to eat crunchy, tough, or sticky foods, which can impact nutrition and overall health. Studies suggest denture wearers have only about 20-25% of the chewing power of those with natural teeth.
- Jawbone Atrophy (Bone Loss): This is perhaps the most significant long-term consequence. When natural teeth are lost, the jawbone no longer receives the stimulation it needs. Over time, the bone begins to resorb, or shrink. Traditional dentures do not stimulate the bone and can even accelerate this process. This leads to:
- Changes in facial structure, making a person look older.
- Loose-fitting dentures that require frequent relining or replacement.
- Difficulty wearing dentures at all as the ridge flattens.
- Sore Spots and Discomfort: The constant pressure of dentures on the gums can cause irritation, sores, and pain, especially as the jawbone changes shape.
- Speech Difficulties: Dentures can sometimes interfere with speech, causing lisping or mumbling, which can be a source of self-consciousness.
- Maintenance and Hygiene: Dentures require daily removal for cleaning, which can be inconvenient. Food particles can also get trapped underneath, leading to bad breath and gum irritation.
- Impact on Social Confidence: The fear of dentures slipping or causing embarrassing sounds can lead to social anxiety and reduced quality of life.
Signs and Symptoms Your Dentures Aren't Working for You
If you experience any of the following, it might be time to consider whether you can switch from dentures to implants:
- Your dentures frequently slip, click, or fall out.
- You find yourself avoiding certain foods because they are too difficult to chew.
- You experience persistent sore spots, gum irritation, or pain from your dentures.
- You notice changes in your facial appearance, such as sunken cheeks or a more prominent chin.
- You need to use excessive amounts of denture adhesive to keep them in place.
- Your dentures feel loose, even after recent adjustments.
- You have difficulty speaking clearly with your dentures.
- You feel self-conscious or anxious about your dentures in social situations.
Understanding Dental Implants: A Foundation for Change
Before delving into how you can switch from dentures to implants, it's crucial to understand what dental implants are and how do implants work.
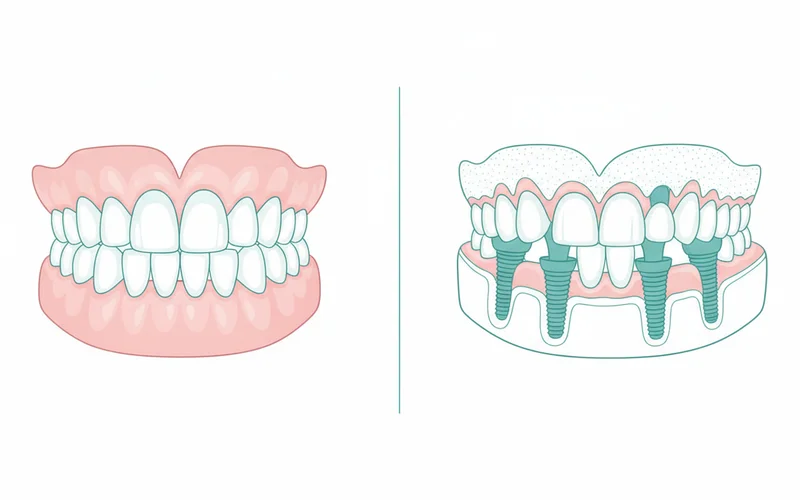
What Are Dental Implants?
A dental implant is a small, screw-shaped post, typically made of biocompatible titanium, that is surgically placed into the jawbone beneath the gum line. This post acts as an artificial tooth root, providing a stable foundation for a prosthetic tooth (a crown), a bridge, or a full set of teeth.
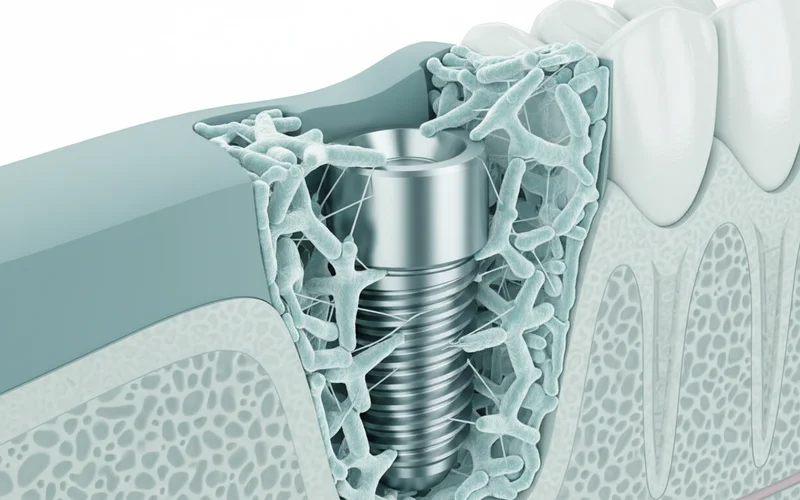
How Do Implants Work? The Power of Osseointegration
The remarkable success of dental implants lies in a biological process called osseointegration. This is where the titanium implant post fuses directly with the surrounding jawbone over several months. Think of it like a natural tooth root becoming firmly anchored in the bone.
Here's how do implants work in a simplified way:
- Placement: The titanium implant is surgically placed into the jawbone.
- Healing (Osseointegration): Over a period of 3 to 6 months (sometimes longer), the bone cells grow around and merge with the implant surface, creating a strong, stable anchor.
- Abutment Attachment: Once osseointegration is complete, a small connector post called an abutment is attached to the implant. This extends through the gum line.
- Prosthetic Attachment: Finally, a custom-made crown, bridge, or denture is securely fastened to the abutment, completing the restoration.
This osseointegration process is vital because it provides unparalleled stability, allowing implant-supported restorations to function much like natural teeth. Crucially, it also stimulates the jawbone, preventing the bone loss that is so common with traditional dentures.
Pro Tip: Titanium is used because it's highly biocompatible, meaning the body accepts it readily without rejection. This is key to successful osseointegration.
Types of Dental Implants for Denture Wearers
For individuals looking to switch from dentures to implants, there isn't a one-size-fits-all solution. Your dentist will recommend the best option based on your bone density, oral health, budget, and desired outcome. The primary goal is to provide greater stability and improve quality of life.
1. Implant-Retained Overdentures (Removable)
This is often considered a hybrid solution, offering a significant upgrade from traditional dentures without the full commitment or cost of a fixed prosthesis.
- What it is: A traditional full denture is modified or custom-made to snap onto a small number of dental implants (typically 2-4 in the lower jaw, 4-6 in the upper jaw).
- How it works: The implants are placed in the jawbone. Once healed, abutments are attached that have a ball, bar, or locator attachment. The denture has corresponding connectors that "snap" onto these attachments.
- Pros:
- Significantly improved stability compared to traditional dentures. No more slipping!
- Restores much more chewing ability.
- Still removable for easy cleaning.
- Often a more affordable dentures and implant option than fixed solutions.
- Can often be fabricated from an existing, well-fitting denture.
- Cons:
- Still removable, meaning daily removal for cleaning.
- May still cover the palate (upper denture), potentially affecting taste and sensation.
- Less biting force than fixed implant bridges.
- Requires periodic replacement of the locator attachments.
- Ideal for: Patients seeking enhanced stability and comfort, who may have limited bone volume, or are looking for a more budget-friendly implant solution.
2. Implant-Supported Fixed Bridges (Non-Removable)
These are the closest you can get to having your natural teeth back. They are permanently attached to the implants and cannot be removed by the patient.
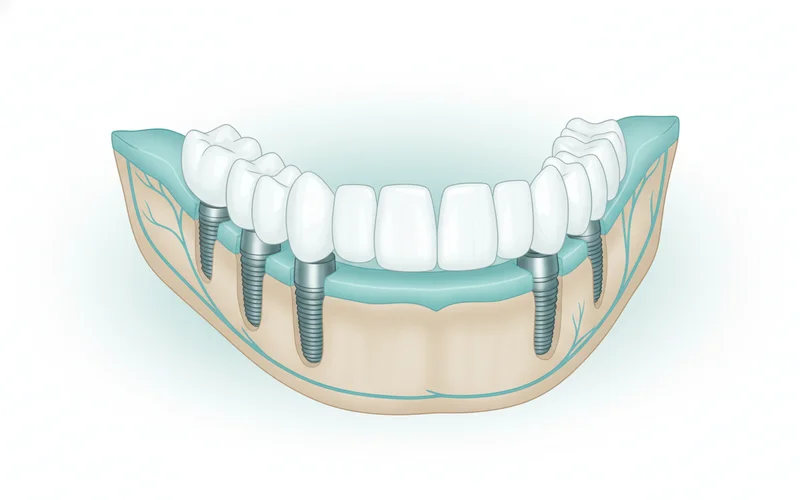
a. All-on-4® and All-on-X Systems
These are revolutionary full-arch solutions for patients missing all teeth in an arch or those with failing teeth requiring extraction.
- What it is: A full arch of prosthetic teeth (a bridge) is securely fastened to just four (All-on-4®) or sometimes six or eight (All-on-X) strategically placed dental implants. The implants are often tilted to maximize contact with available bone, avoiding the need for extensive bone grafting in some cases.
- How it works: After implant placement and healing, a custom-designed full bridge (made of acrylic, zirconia, or porcelain) is screwed onto the implants, becoming a permanent part of your mouth.
- Pros:
- Completely fixed and non-removable, feeling much like natural teeth.
- Restores nearly full chewing function (up to 90% of natural teeth).
- Eliminates all denture-related problems (slipping, adhesives, sore spots).
- Preserves jawbone and maintains facial structure.
- Upper arches leave the palate uncovered, enhancing taste and sensation.
- Often allows for "teeth-in-a-day" or "same-day smile" protocols, where a temporary bridge is attached immediately after implant placement.
- Cons:
- Higher initial cost than implant-retained overdentures.
- Requires good bone density for successful implant placement (though sometimes less bone grafting than traditional individual implants).
- More complex surgical procedure.
- Ideal for: Patients seeking the ultimate in stability, function, and aesthetics, and who are good candidates for implant surgery. It's an excellent solution for those who want to completely leave their denture days behind.
b. Conventional Multiple Implants with Bridges
In some cases, if a patient has more significant bone volume, a greater number of implants (e.g., 6-10 per arch) can be placed to support a fixed bridge. This offers even greater distribution of biting forces. This approach is less common for denture wearers converting from full dentures due to bone loss, but it's an option for those with good bone structure.
The Journey from Dentures to Implants: What to Expect
The process of switching from dentures to implants is a significant undertaking that requires careful planning and multiple stages. While the specific timeline and procedures can vary greatly depending on individual circumstances, here's a general step-by-step overview:
Step 1: Initial Consultation and Comprehensive Evaluation
This is the crucial first step. You'll meet with a qualified dental professional, typically an oral surgeon, periodontist, or prosthodontist, experienced in implant dentistry.
- Discussion: You'll discuss your goals, concerns, and dental history. This is where you openly ask, "Can I switch from dentures to implants?"
- Oral Examination: The dentist will meticulously examine your mouth, gums, and any remaining teeth.
- Diagnostic Imaging: This is critical. It involves:
- X-rays: Traditional 2D X-rays provide a general overview.
- 3D Cone Beam Computed Tomography (CBCT) Scan: This advanced imaging provides detailed cross-sectional views of your jawbone, showing bone density, quantity, and the location of vital structures like nerves and sinuses. This is essential for determining if you have enough bone for implants and for precise surgical planning.
- Health Review: A thorough review of your medical history, including medications, systemic conditions (e.g., diabetes, heart disease), and lifestyle habits (smoking), is essential as these can impact implant success.
- Treatment Plan Presentation: Based on the evaluation, the dentist will outline suitable implant options, discuss the procedure, potential timelines, and estimated costs.
Step 2: Pre-Surgical Procedures (If Needed)
Many long-term denture wearers experience significant jawbone loss. If the CBCT scan reveals insufficient bone, preparatory procedures will be necessary.
- Tooth Extractions: Any remaining compromised teeth will need to be extracted.
- Bone Grafting: This is a common procedure for denture wearers. It involves adding bone material (from your own body, a donor, or synthetic sources) to areas of the jawbone where volume or density is lacking. This creates a strong foundation for the implants.
- Types: Sinus lifts (for upper jaw, if sinuses are too low), ridge augmentation (to widen or heighten the bone), or socket preservation (after extraction).
- Healing Time: Bone grafting can add 3 to 9 months (or even longer) to your overall treatment timeline, as the graft material needs to integrate and mature before implant placement.
- Gum Grafting: Less common for full arches, but sometimes necessary to improve gum tissue quality around implant sites.
Step 3: Dental Implant Placement Surgery
Once your jawbone is ready, the implants can be placed.
- Anesthesia: Local anesthesia is typically used, often supplemented with sedation (oral, IV, or nitrous oxide) to ensure comfort and reduce anxiety.
- Incision: The gum tissue is gently incised and lifted to expose the jawbone.
- Pilot Hole: A small pilot hole is drilled into the bone at the precise, pre-planned location.
- Sequential Drilling: A series of progressively wider drills are used to create the exact size and shape for the implant.
- Implant Insertion: The titanium implant post is carefully screwed or tapped into the prepared bone.
- Closure: The gum tissue is then closed over the implant, or a healing abutment is placed that extends through the gum.
- Temporary Prosthesis: In some cases, especially with All-on-4®/All-on-X, a temporary set of teeth (denture or bridge) can be attached to the newly placed implants immediately, allowing you to leave with a functional smile. This is often referred to as "teeth-in-a-day." Otherwise, you will wear a temporary traditional denture during the healing phase.
Step 4: Osseointegration (Healing Period)
This is a critical phase where the magic of dental implants happens.
- Duration: The implant post fuses with the jawbone over 3 to 6 months. This period can be longer if bone grafting was performed or if the bone quality is less than ideal.
- Purpose: The bone cells grow around the titanium surface, creating a secure, rock-solid anchor for your future teeth.
- Monitoring: Your dentist will monitor your healing progress during this time.
Step 5: Abutment Placement (If Not Already Done)
After successful osseointegration, a second minor procedure may be performed if the implant was initially covered by gum tissue.
- Exposure: A small incision is made to uncover the top of the implant.
- Abutment Attachment: The abutment, a small connector post, is attached to the implant. This post will protrude through the gum, ready to support the final restoration.
- Healing: The gums around the abutment are given a few weeks to heal and mature.
Step 6: Fabrication and Attachment of Your New Teeth
This is the exciting final stage where your new, permanent smile takes shape.
- Impressions: Once the gums around the abutments are healed, precise digital or traditional impressions of your mouth are taken.
- Custom Design: These impressions are sent to a dental laboratory where skilled technicians custom-design and fabricate your new crown, bridge, or implant-supported overdenture. This ensures a perfect fit, natural appearance, and correct bite.
- Final Attachment: At your final appointment, your permanent restoration is securely attached to the abutments. For fixed bridges, they are screwed into place. For overdentures, they snap onto the attachments. Your dentist will ensure your bite is correct and make any necessary adjustments.
Pro Tip: Be patient with the healing process. Rushing osseointegration can lead to implant failure. Trust your dental team's timeline.
Financial Considerations: Cost, Insurance, and Affordability
When considering "Can I switch from dentures to implants?", cost is often a primary concern. Dental implants are a significant investment, but their long-term benefits and durability often outweigh the initial expense of constantly replacing or relining dentures. The cost can vary widely based on several factors:
- Type of Implant Solution: Individual implants, implant-retained overdentures, or fixed full-arch systems like All-on-4® have different price points.
- Number of Implants Needed: More implants generally mean higher costs.
- Need for Ancillary Procedures: Bone grafting, tooth extractions, or gum grafting will add to the total cost.
- Material of the Prosthesis: Acrylic, zirconia, or porcelain for the final teeth will affect the price.
- Geographic Location: Costs vary by region and even by practice within the United States. Major metropolitan areas tend to have higher prices.
- Dentist's Experience and Specialty: Highly experienced specialists may charge more.
Average US Cost Ranges (Approximate)
These are general ranges, and it's essential to get a detailed quote from your specific dental provider.
| Procedure | Average US Cost Range (per tooth/arch) |
|---|---|
| Single Dental Implant (post, abutment, crown) | $3,000 - $6,000 |
| Implant-Retained Overdenture (2 implants, lower) | $6,000 - $12,000 (for implants & denture) |
| Implant-Retained Overdenture (4 implants, upper) | $10,000 - $20,000 (for implants & denture) |
| All-on-4®/All-on-X (per arch, fixed bridge) | $20,000 - $35,000+ |
| Bone Grafting (per site) | $200 - $3,000+ (depending on extent) |
| Tooth Extraction | $75 - $450+ (per tooth, simple to surgical) |
Note on "affordable dentures and implant": While the upfront cost for implant-supported solutions is higher than traditional dentures, consider the long-term value. Implants can last decades, while traditional dentures often need replacement every 5-7 years, plus ongoing relines, adhesives, and repairs, which add up over time.
Insurance Coverage Details
Dental insurance typically offers limited coverage for dental implants.
- Medical vs. Dental: Because dental implants are considered both a dental and a medical procedure, sometimes parts of the treatment (like the bone graft or extraction) might be covered under medical insurance, while the implant placement and restoration fall under dental insurance.
- Percentage Coverage: Most dental insurance plans might cover 10% to 50% of the implant procedure, often up to your annual maximum, which usually ranges from $1,000 to $2,500. This means you will likely pay a significant portion out-of-pocket.
- Pre-Authorization: Always get a pre-authorization from your insurance company to understand exactly what will be covered before starting treatment.
- Medicare/Medicaid: Generally, Medicare does not cover routine dental care, including implants. Some Medicare Advantage plans might offer limited dental benefits. Medicaid coverage varies significantly by state but rarely includes implant procedures for adults.
Payment Plans and Financing Options
Because of the high cost and limited insurance coverage, most dental practices offer various payment solutions to make implants more accessible.
- In-Office Payment Plans: Many offices offer flexible payment schedules, allowing you to pay in installments over several months.
- Third-Party Financing: Companies like CareCredit®, LendingClub®, or Alphaeon Credit® specialize in healthcare financing. They offer various plans, including interest-free options for a certain period, or extended payment plans with fixed interest rates.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): These tax-advantaged accounts allow you to set aside pre-tax money for healthcare expenses, including dental implants.
Pro Tip: Don't let the upfront cost deter you. Discuss all financing options with your dental provider's administrative staff. They are often experts at helping patients navigate the financial aspects of treatment.
Recovery and Aftercare
The recovery period after switching from dentures to implants involves several stages, from immediate post-surgical healing to long-term maintenance.
Immediate Post-Surgical Recovery (First Few Days)
- Pain Management: You'll likely experience some discomfort, swelling, and bruising. Your dentist will prescribe pain medication or recommend over-the-counter options.
- Swelling: Apply ice packs to the outside of your face for 20 minutes on, 20 minutes off, for the first 24-48 hours to minimize swelling.
- Bleeding: Minor bleeding is normal. Your dentist will provide gauze pads and instructions on how to manage it.
- Diet: Stick to a soft diet for the first few days, avoiding crunchy, sticky, or hot foods. Drink plenty of fluids.
- Oral Hygiene: Follow your dentist's specific instructions. This often involves gentle rinsing with a prescribed antimicrobial mouthwash (like chlorhexidine) and avoiding brushing the surgical site directly for a few days.
- Activity: Avoid strenuous activity for several days to prevent increased bleeding or swelling.
- Smoking: Absolutely avoid smoking. It significantly hinders healing and can lead to implant failure.
Osseointegration Healing Period (3-6 Months)
- Temporary Prosthesis: If you have a temporary denture or bridge, avoid putting excessive biting force on it, as this can disturb the integrating implants. Stick to a softer diet as advised by your dentist.
- Regular Check-ups: Attend all scheduled follow-up appointments to monitor healing.
- Oral Hygiene: Maintain excellent oral hygiene, brushing and flossing regularly around your temporary prosthesis and remaining natural teeth.
Long-Term Care for Your New Implant-Supported Teeth
Once your permanent implants and prosthetic teeth are in place, they require diligent care to ensure their longevity.
- Excellent Oral Hygiene:
- Brushing: Brush your implant-supported teeth at least twice a day with a soft-bristled toothbrush and non-abrasive toothpaste.
- Flossing: Floss daily, paying special attention to the areas around the implants. Special floss designed for implants, interdental brushes, or water flossers can be particularly effective. Your dentist or hygienist will demonstrate proper techniques.
- Regular Dental Check-ups: Schedule professional cleanings and examinations every six months, or as recommended by your dentist. Dental hygienists use special instruments designed for cleaning implants to avoid scratching the titanium.
- Avoid Damaging Habits: Refrain from chewing on ice, biting hard candies, or using your teeth to open packages, as this can damage your restoration or implants. If you grind or clench your teeth (bruxism), your dentist may recommend a nightguard.
- Address Issues Promptly: If you notice any discomfort, looseness, redness, or swelling around your implants, contact your dentist immediately.
Pro Tip: Think of your dental implants as your new natural teeth. They require the same, if not more, meticulous care to prevent complications like peri-implantitis (gum disease around implants).
Potential Risks and How to Minimize Them
While dental implants have a very high success rate (over 95%), like any surgical procedure, there are potential risks and complications. Understanding these helps you make an informed decision when you ask, "Can I switch from dentures to implants?"
- Infection at the Implant Site: This is a risk with any surgery. It can be minimized with sterile surgical techniques, proper post-operative care, and antibiotics if prescribed.
- Damage to Surrounding Structures: Nerves, blood vessels, or adjacent teeth can be inadvertently damaged during placement. This risk is greatly reduced by thorough pre-surgical planning using 3D CBCT scans.
- Sinus Issues: For implants in the upper jaw, there's a risk of the implant protruding into the sinus cavity. A sinus lift procedure can prevent this.
- Implant Failure (Lack of Osseointegration): The implant may not fuse with the bone. This can be due to poor bone quality, infection, excessive force on the implant during healing, or certain medical conditions (e.g., uncontrolled diabetes, heavy smoking). If an implant fails, it may need to be removed, the site allowed to heal, and another implant placed.
- Peri-Implantitis: This is an inflammatory condition similar to gum disease that affects the tissues around the implant. It can lead to bone loss around the implant and, if left untreated, implant failure. It's often caused by poor oral hygiene.
- Mechanical Complications: The crown, bridge, or abutment can loosen, break, or chip. These are usually repairable or replaceable.
Minimizing Risks:
- Choose an Experienced Professional: Select a qualified and experienced implant dentist (oral surgeon, periodontist, or prosthodontist) with a proven track record. Ask about their training and success rates.
- Thorough Pre-Planning: Insist on 3D imaging (CBCT scan) for precise surgical planning.
- Disclose Medical History: Be completely honest about your medical history, medications, and lifestyle habits.
- Follow Post-Operative Instructions: Adhere strictly to all post-surgical care instructions.
- Maintain Excellent Oral Hygiene: This is paramount for long-term implant success.
- Regular Dental Check-ups: Attend all recall appointments for professional cleaning and monitoring.
- Quit Smoking: Smoking dramatically increases the risk of implant failure and peri-implantitis.
Preventing Further Bone Loss
One of the most compelling reasons to switch from dentures to implants is the preservation of jawbone health. Traditional dentures do nothing to stop bone loss and can even accelerate it. Dental implants, however, stimulate the bone, much like natural tooth roots do.
- The Role of Implants: When an implant is integrated into the jawbone, it transmits chewing forces directly to the bone. This stimulation signals the body to maintain the bone, preventing the resorption that occurs when teeth are missing.
- Early Intervention: If you are considering implants, doing so sooner rather than later can help preserve more of your existing bone, potentially reducing the need for extensive (and costly) bone grafting procedures.
- Good Oral Hygiene: Preventing gum disease (periodontitis) around natural teeth and peri-implantitis around implants is crucial, as these conditions are major causes of bone loss.
- Balanced Diet: A diet rich in calcium and Vitamin D supports overall bone health.
Comparison: Dentures vs. Implant-Supported Solutions
Let's look at a direct comparison to further illustrate why so many choose to switch from dentures to implants.
| Feature | Traditional Dentures | Implant-Retained Overdentures | Fixed Implant Bridges (All-on-4®/All-on-X) |
|---|---|---|---|
| Stability | Relies on suction, often slips/wobbles | Very stable, snaps onto implants | Extremely stable, fixed permanently |
| Chewing Efficiency | ~20-25% of natural teeth | ~50-70% of natural teeth | ~80-90% of natural teeth |
| Bone Preservation | Does NOT prevent bone loss, can accelerate it | Helps prevent bone loss at implant sites | Prevents bone loss throughout the arch |
| Comfort | Can cause sore spots, covers palate (upper) | Much more comfortable, less palate coverage | Highly comfortable, feels like natural teeth |
| Speech | Can affect speech, lisping | Generally improved | Natural speech |
| Appearance | Can look unnatural, changes facial structure over time | Natural-looking, preserves facial structure | Highly aesthetic, preserves facial structure |
| Maintenance | Daily removal for cleaning, adhesives, relines | Daily removal for cleaning, locator replacement | Brushing/flossing like natural teeth, professional cleanings |
| Lifespan | 5-7 years (needs relines, replacement) | 10-15 years (denture, implants last decades) | 15-25+ years (implants last decades) |
| Initial Cost | Low ($1,500 - $4,000 per arch) | Medium ($6,000 - $20,000 per arch) | High ($20,000 - $35,000+ per arch) |
| Impact on Quality of Life | Often leads to food restrictions, social anxiety | Significantly improved | Drastically improved |
Children / Pediatric Considerations
Dental implants are generally not recommended for children or adolescents. The jawbone needs to be fully developed before implants can be placed to ensure long-term success. Placing implants in a growing jaw can interfere with natural bone development and lead to complications as the child grows. Typically, dental implants are considered appropriate for individuals once their jaw development is complete, which is usually in their late teens or early twenties. For children missing teeth due to trauma or congenital conditions, temporary solutions like space maintainers or removable partial dentures are often used until they reach an age suitable for implants.
Frequently Asked Questions
What is the success rate of switching from dentures to implants?
Dental implants boast an impressive success rate of over 95%, making them one of the most reliable dental procedures. When following proper protocols and maintaining good oral hygiene, these high success rates are sustained, offering a predictable and long-lasting solution.
Is the implant procedure painful?
The implant placement procedure itself is typically performed under local anesthesia, so you shouldn't feel any pain during the surgery. Post-operative discomfort is manageable with prescribed pain medication and over-the-counter options. Most patients describe the sensation as less painful than a tooth extraction.
How long does the entire process take to switch from dentures to implants?
The full process can take anywhere from 4 to 12 months or even longer, especially if bone grafting is required. This timeline includes initial consultation, any necessary preparatory procedures like bone grafting (3-9 months healing), implant placement, osseointegration (3-6 months), and finally, the fabrication and attachment of your permanent prosthesis.
Can I get "teeth in a day" if I switch from dentures to implants?
Yes, "teeth-in-a-day" or "same-day smile" is an option for many patients, particularly with All-on-4® or All-on-X systems. This involves placing implants and attaching a temporary, functional set of teeth on the same day. While these temporary teeth are immediate, they are later replaced with a permanent, custom-fabricated restoration after the implants have fully integrated with the bone.
What if I don't have enough jawbone for implants?
If you have insufficient jawbone density due to long-term denture wear, bone grafting is often an option. Bone grafting adds volume and density to the jawbone, creating a stable foundation for implants. While it adds to the treatment time and cost, it makes implant treatment possible for many who would otherwise not be candidates.
How do I clean implant-supported dentures or bridges?
Fixed implant bridges are cleaned like natural teeth: brush twice daily with a soft toothbrush, floss daily (using special floss, interdental brushes, or water flossers around the implants), and attend regular professional cleanings. Removable implant-retained overdentures are removed daily for cleaning, just like traditional dentures, but the implant sites also need careful brushing.
Are there any alternatives to dental implants if I can't get them?
If implants aren't an option due to medical reasons, severe bone loss that can't be treated with grafting, or financial constraints, traditional dentures or removable partial dentures remain alternatives. However, it's important to understand these solutions do not offer the same stability, function, or bone preservation benefits as implants.
Will my new implant teeth look natural?
Absolutely. Modern dental implant restorations are custom-designed to match your facial features, gum line, and desired aesthetics. The materials used, like high-quality porcelain or zirconia, mimic the translucency and shade of natural teeth, resulting in a highly aesthetic and natural-looking smile.
How long do dental implants last?
With proper care and good oral hygiene, the dental implant posts themselves can last a lifetime. The prosthetic teeth (crowns, bridges, or dentures) attached to the implants are very durable but may require replacement after 15-25 years due to normal wear and tear.
Can I smoke with dental implants?
Smoking significantly jeopardizes the success of dental implants. It restricts blood flow, impairs healing, and drastically increases the risk of implant failure and peri-implantitis (gum disease around implants). Dentists strongly advise quitting smoking before and after implant surgery to ensure long-term success.
When to See a Dentist
If you are a denture wearer and have been experiencing any of the common problems listed in this article (slipping, discomfort, difficulty eating), or if you are simply tired of the limitations of your current dentures, it's an excellent time to see a dentist.
- Routine Consideration: If you're simply exploring options and want to understand if you can switch from dentures to implants, schedule a consultation with a general dentist, prosthodontist, oral surgeon, or periodontist. They can assess your oral health and provide personalized recommendations.
- Persistent Pain or Sores: If your current dentures are consistently causing pain, sore spots, or recurrent infections, it's a sign that they may no longer fit correctly or are causing irritation, and a professional evaluation is needed.
- Noticeable Changes in Facial Structure: If you observe changes in your jawline, a sunken appearance around your mouth, or your dentures feel increasingly loose, it indicates potential bone loss, which should be addressed promptly to determine if implants are still a viable option.
- Difficulty Eating a Varied Diet: If your ability to eat nutritious foods is compromised due to denture instability, it can impact your overall health and warrants a discussion about more stable solutions.
- Sudden Changes in Denture Fit: If your dentures suddenly become very loose or ill-fitting, or if you're using excessive adhesive, it's time for an assessment.
Don't wait for a crisis. Proactive consultation can help you understand your options, address potential issues early, and plan for a healthier, more confident smile with dental implants.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Implantologist: Complete Guide
Losing a tooth can be a significant setback, impacting not only your smile but also your ability to speak, chew, and maintain overall oral health. In fact, over 3 million Americans currently have dental implants, and that number is projected to grow significantly as more people seek a durable, n
March 8, 2026
Dentures Over Implants: Complete Guide
Missing multiple teeth or even an entire arch can profoundly impact your life, affecting everything from your ability to chew and speak to your self-confidence. For millions of Americans, traditional removable dentures have long been a solution, but they often come with compromises: slipping, discom
March 8, 2026
Implants Process: Complete Guide
Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the
March 8, 2026

Implants Dentaires: Complete Guide
Missing teeth can dramatically impact not just your smile, but your overall health, confidence, and quality of life. In the United States, an estimated 178 million adults are missing at least one tooth, while approximately 40 million are missing all their teeth. These statistics underscore a
March 8, 2026