Implants Process: Complete Guide
Key Takeaways
- Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the
Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the most effective and durable replacement options becomes crucial for your long-term oral health. This comprehensive guide will walk you through the entire implants process, from the initial consultation to the final restoration, providing you with all the essential information you need to make an informed decision about this life-changing dental solution. We'll delve into what a dental implant is, explore various types, discuss the step-by-step journey, break down costs, and explain what to expect during recovery and beyond, ensuring you have a complete picture of this advanced restorative treatment.
Key Takeaways:
- Dental implants are titanium posts surgically placed into the jawbone to support artificial teeth, offering a durable, long-lasting solution for tooth loss.
- The implants process typically spans 3 to 9 months, depending on individual healing and whether bone grafting is required.
- A single dental implant in the US can cost anywhere from $3,000 to $6,000 (implant post and abutment), with the crown adding an additional $1,000 to $3,000. Full mouth implant-supported restorations can range from $25,000 to $60,000+ per arch.
- Most dental insurance plans do not cover the implant post itself, but may cover parts of the restorative crown or preparatory procedures. Financing options are widely available.
- Proper oral hygiene and regular dental check-ups are vital for the long-term success of dental implants, which can last 20 years or even a lifetime with good care.
- Implants prevent bone loss in the jaw, maintain facial structure, and provide superior stability compared to traditional dentures or bridges.
- Individuals with sufficient bone density and good general health are typically ideal candidates, though bone grafting can often address bone deficiency.
What is a Dental Implant? An Overview
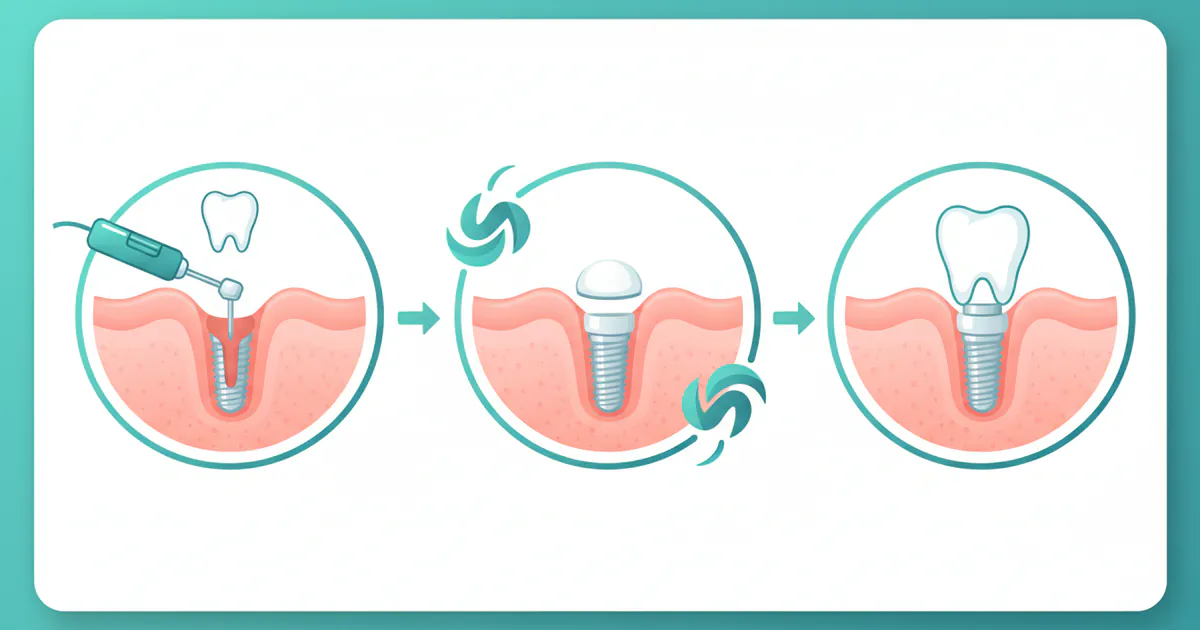
A dental implant is a sophisticated prosthetic device designed to replace missing tooth roots. It consists of a small, screw-shaped post, typically made of biocompatible titanium, which is surgically placed into the jawbone beneath the gum line. Over time, this titanium post fuses with the surrounding bone in a process called osseointegration, creating a strong, stable foundation for a replacement tooth or teeth.
Once integrated, an abutment (a small connector post) is attached to the implant, and then a custom-made crown, bridge, or denture is secured onto the abutment. The result is a restoration that looks, feels, and functions like a natural tooth. Dental implants are widely considered the gold standard for tooth replacement due to their durability, aesthetic appeal, and ability to preserve jawbone health. Unlike traditional bridges, they do not require altering adjacent healthy teeth, and unlike dentures, they offer superior stability and chewing efficiency.
Types and Variations of Dental Implants
The field of dental implants has evolved significantly, offering several types and approaches to suit diverse patient needs and clinical situations. Understanding these variations is key to determining the best implants process for you.
Endosteal Implants (In-Bone Implants)
These are the most common type of dental implant. Endosteal implants are typically shaped like small screws, cylinders, or tapered posts and are surgically placed directly into the jawbone. They are made from titanium, a material known for its biocompatibility and ability to fuse with bone. Once placed, they serve as the artificial tooth root, providing a sturdy anchor for prosthetic teeth.
Subperiosteal Implants (On-Bone Implants)
Less commonly used today, subperiosteal implants consist of a metal framework that fits on top of the jawbone, just under the gum tissue. This framework has posts that protrude through the gums to hold the prosthetic teeth. This type was historically used for patients who couldn't wear conventional dentures and had minimal bone height, but bone grafting techniques and advancements in endosteal implants have largely made them obsolete.
Mini Dental Implants (MDIs)
MDIs are significantly smaller in diameter than traditional endosteal implants, typically less than 3mm. They are primarily used to stabilize lower dentures or in situations where bone density is limited and traditional implants might not be feasible without extensive bone grafting. Their smaller size often allows for a less invasive placement procedure and quicker recovery, though they may not offer the same long-term stability as conventional implants for single tooth replacement in high-stress areas.
Implant-Supported Restorations
Dental implants can support various types of restorations, providing solutions for single missing teeth, multiple missing teeth, or even a full arch of missing teeth.
- Single Tooth Implants: A single implant post supports one custom-made crown, seamlessly blending with your natural teeth.
- Implant-Supported Bridges: For multiple adjacent missing teeth, two or more implants can support a bridge, eliminating the need to modify healthy adjacent teeth.
- Implant-Supported Dentures (Overdentures): This is a popular option, especially for patients in Houston and other metropolitan areas, seeking a more stable alternative to traditional removable dentures. Two to six implants are strategically placed in the jawbone to anchor a removable or fixed denture.
- Removable Overdentures: The denture snaps onto the implants, providing significantly more stability than conventional dentures but still allowing for easy removal for cleaning.
- Fixed Overdentures (All-on-4® or All-on-6®): A full arch of teeth is permanently attached to four to six implants. This offers maximum stability, chewing power, and a feeling very close to natural teeth, as it is not removable by the patient. This revolutionary approach often allows for the placement of implants and a temporary set of teeth in a single day.
Why Do People Need Dental Implants? (Causes of Tooth Loss)
While implants themselves don't have "causes" or "symptoms," the need for them arises from tooth loss, which can stem from various factors. Understanding these underlying causes highlights why dental implants are such a vital restorative option.
- Severe Tooth Decay: Untreated cavities can destroy a tooth's structure, leading to infection and eventual extraction if restorative treatments fail.
- Gum Disease (Periodontitis): Advanced gum disease is the leading cause of tooth loss in adults. It destroys the supporting bone and soft tissues around teeth, causing them to loosen and fall out.
- Trauma or Injury: Accidents, sports injuries, or falls can result in knocked-out or severely fractured teeth that require extraction.
- Congenital Conditions: Some individuals are born missing one or more permanent teeth (hypodontia).
- Failed Root Canals or Restorations: Sometimes, previous dental work fails, leading to the need for extraction and replacement.
- Erosion and Wear: Extensive wear from conditions like acid reflux, bruxism (teeth grinding), or abrasive habits can lead to tooth damage and loss over time.
- Age-Related Tooth Loss: While not a direct cause, the cumulative effect of wear, tear, and susceptibility to disease can contribute to tooth loss in older adults.
Signs You Might Need Dental Implants
If you experience any of the following, it might be an indication that dental implants could be a suitable solution for you:
- Missing Teeth: The most obvious sign. Whether it's a single tooth or multiple, a gap in your smile signals a need for replacement.
- Difficulty Chewing or Speaking: Gaps can make chewing certain foods challenging and can affect speech clarity.
- Shifting Teeth: When a tooth is lost, adjacent teeth can drift into the empty space, altering your bite and causing further problems.
- Deteriorating Jawbone: Tooth roots stimulate the jawbone. Without them, the bone can begin to resorb (shrink), leading to a sunken facial appearance.
- Unsatisfactory Dentures or Bridges: If your current dentures slip, cause sores, or your bridge compromises healthy adjacent teeth, implants offer a more stable and conservative alternative.
- Pain or Discomfort in Existing Teeth: If a tooth is severely damaged, infected, or failing, and extraction is the only option, implants can be the best follow-up.
Treatment Options: Implants vs. Alternatives
When you have missing teeth, dental implants are often presented as the gold standard, but it's important to understand the alternatives available, along with their respective pros and cons.
Dental Implants
- Pros:
- Durability and Longevity: Can last 20 years to a lifetime with proper care.
- Bone Preservation: Stimulates the jawbone, preventing bone loss and maintaining facial structure.
- Stability: Mimics natural teeth, providing excellent chewing power and no slippage.
- Aesthetics: Look and feel like natural teeth.
- Conservative: Does not require altering adjacent healthy teeth.
- Improved Speech and Comfort: No issues with clicking or shifting.
- Cons:
- Cost: Higher initial investment than other options.
- Treatment Time: The implants process can take several months due to osseointegration.
- Surgical Procedure: Requires minor surgery, with associated risks.
- Not for Everyone: Requires sufficient bone density and good overall health.
Fixed Dental Bridges
- Pros:
- Faster Treatment: Can be completed in a few weeks.
- Lower Initial Cost: Generally less expensive than implants.
- Non-Surgical: No surgery required.
- Cons:
- Requires Tooth Alteration: Adjacent healthy teeth must be ground down to support the bridge.
- Bone Loss: Does not stimulate the jawbone, so bone loss can still occur beneath the missing tooth.
- Shorter Lifespan: Typically lasts 5-15 years, requiring eventual replacement.
- Maintenance: More difficult to clean under the bridge, potentially leading to decay in supporting teeth.
Removable Partial or Complete Dentures
- Pros:
- Most Affordable: Lowest initial cost.
- Non-Invasive: No surgery or alteration of natural teeth.
- Quick Solution: Can be fabricated relatively quickly.
- Cons:
- Lack of Stability: Can slip, shift, or cause discomfort while eating and speaking.
- Bone Loss: Does not prevent jawbone deterioration.
- May Affect Taste: Upper dentures cover the palate, potentially impacting taste.
- Regular Adjustments/Relining: Dentures need to be adjusted or relined as the jawbone changes.
- Reduced Chewing Efficiency: Significantly less chewing power than natural teeth or implants.
Comparison Table: Tooth Replacement Options
| Feature | Dental Implants | Fixed Dental Bridge | Removable Denture (Partial/Complete) |
|---|---|---|---|
| Durability | Excellent (20+ years, often lifetime) | Good (5-15 years) | Fair (5-10 years) |
| Bone Health | Preserves bone, prevents resorption | Does not prevent bone loss | Does not prevent bone loss |
| Stability | Excellent (like natural teeth) | Good (fixed in place) | Fair (can slip, move) |
| Aesthetics | Excellent (natural look and feel) | Good (natural appearance) | Good (can look natural) |
| Adjacent Teeth | No alteration required | Requires altering adjacent teeth | No alteration required |
| Cost (Single Tooth) | $4,000 - $7,000+ | $2,000 - $5,000+ | $800 - $2,500+ |
| Treatment Time | Several months (due to osseointegration) | Weeks | Weeks |
| Invasiveness | Surgical procedure | Non-surgical (tooth preparation) | Non-invasive |
The Step-by-Step Implants Process
The dental implants process is a carefully planned and executed sequence of procedures, often spanning several months. While individual cases may vary, the general steps remain consistent.
Step 1: Initial Consultation and Planning
This crucial first step involves a comprehensive examination by a qualified dental professional, typically an oral surgeon, periodontist, or general dentist with extensive implant training.
- Medical History Review: The dentist will review your complete medical and dental history to identify any conditions (e.g., uncontrolled diabetes, certain autoimmune diseases) or medications (e.g., bisphosphonates) that might affect healing or implant success.
- Oral Examination: A thorough examination of your teeth, gums, and existing bone structure.
- Diagnostic Imaging:
- X-rays: Traditional 2D X-rays provide a basic view.
- 3D Cone Beam Computed Tomography (CBCT) Scan: This advanced imaging provides detailed 3D views of your jawbone, nerve pathways, and sinus cavities. It's essential for precisely planning implant placement, ensuring sufficient bone volume, and avoiding critical anatomical structures.
- Treatment Plan Development: Based on the assessment, a personalized treatment plan is created. This includes determining the number and type of implants, identifying any preparatory procedures (like bone grafting), estimating the timeline, and discussing costs.
- Discussion of Options: Your dentist will explain the proposed implants process, discuss alternatives, address your concerns, and answer all your questions.
Step 2: Preparatory Procedures (If Needed)
Some patients may require additional procedures to ensure a successful implant placement.
- Tooth Extraction: If a damaged or diseased tooth is still present in the implant site, it must be extracted first.
- Bone Grafting: This is often necessary if the jawbone lacks sufficient density or volume to support an implant. Bone graft material (from your own body, a donor, an animal, or synthetic) is placed to stimulate new bone growth. This can take 3 to 9 months to heal before implant placement can proceed.
- Sinus Lift (Sinus Augmentation): If implants are needed in the upper jaw (maxilla) near the molars, and the sinus cavity is too close to the bone, a sinus lift elevates the sinus floor and places bone graft material to create adequate bone height. This also requires a healing period.
Step 3: Dental Implant Placement Surgery
This is the surgical phase where the titanium implant post is inserted into the jawbone.
- Anesthesia: Local anesthesia is typically used to numb the area, but sedation options (oral, IV, or nitrous oxide) are also available for patient comfort and anxiety management.
- Incision: The dentist or surgeon makes a small incision in the gum tissue to expose the underlying jawbone.
- Drilling: A precise series of drills are used to create a pilot hole, then progressively widen it to the exact size and depth for the implant.
- Implant Insertion: The titanium implant post is carefully threaded or tapped into the prepared bone socket.
- Suturing: The gum tissue is closed over the implant with sutures. In some cases, a "healing abutment" (a small cap) is placed immediately, extending through the gum, to guide gum healing. In other cases, the implant is completely submerged and covered by the gum.
- Post-Operative Instructions: You'll receive detailed instructions for pain management, diet, oral hygiene, and follow-up care.
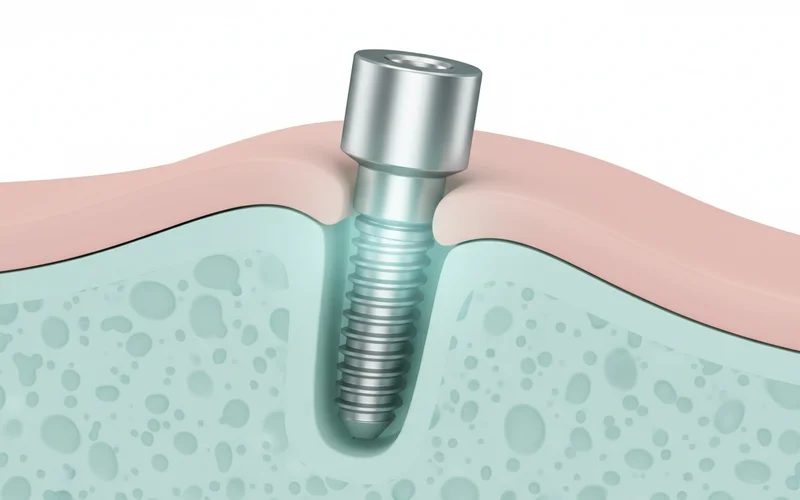
Step 4: Osseointegration (Healing Period)
This is perhaps the most critical part of the implants process. During osseointegration, the jawbone naturally grows around and fuses with the titanium implant surface.
- Duration: This healing period typically lasts 3 to 6 months, though it can vary based on individual healing capabilities, bone quality, and the number of implants.
- Temporary Solutions: During this time, you might wear a temporary denture or bridge to maintain aesthetics and function.
- Monitoring: The dentist will monitor your healing progress through periodic check-ups.
Step 5: Abutment Placement
Once osseointegration is complete, the abutment is attached to the implant.
- Exposure (if necessary): If the implant was completely covered by gum tissue, a minor surgical procedure is performed to expose the top of the implant.
- Abutment Attachment: A small connector piece (the abutment) is screwed onto the implant. This piece will eventually support the final crown, bridge, or denture.
- Gum Healing: The gum tissue is allowed to heal around the abutment for about 1-2 weeks, forming a cuff that will protect the implant.
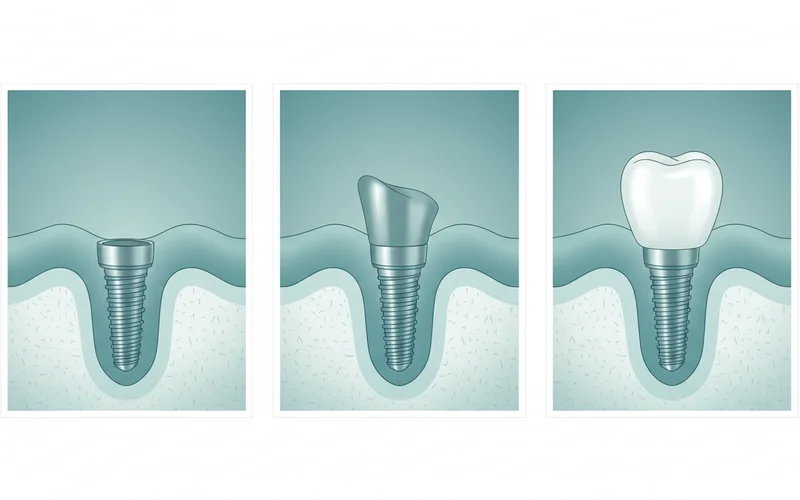
Step 6: Restoration (Crown, Bridge, or Denture Placement)
This is the final step where your new teeth are placed.
- Impressions: Once the gums have healed around the abutment, digital or traditional impressions (molds) of your mouth are taken.
- Custom Fabrication: These impressions are sent to a dental lab, where a custom-made crown, bridge, or denture is fabricated to match the color, shape, and size of your natural teeth.
- Final Placement: Once the restoration is ready, it is meticulously fitted onto the abutment and secured. Your dentist will ensure your bite is correct and comfortable.
Pro Tip: For patients undergoing the "All-on-4®" or "All-on-6®" procedure for full arch replacement, it's often possible to receive a temporary fixed bridge on the day of implant placement, allowing you to leave the office with a functional and aesthetic smile while the implants heal. A permanent, custom restoration will be placed after osseointegration.
Cost and Insurance for Dental Implants
The investment in dental implants reflects their complexity, the advanced materials used, and the long-term benefits they provide. Understanding the costs and insurance landscape is crucial for patients in the US.
Average US Cost Ranges (Per Implant)
The cost of a dental implant can vary significantly based on several factors, including:
- Geographic Location: Costs can be higher in major metropolitan areas like Houston, New York, or Los Angeles compared to rural areas.
- Number of Implants: A single implant is more expensive per unit than multiple implants placed in the same procedure (due to shared surgical fees).
- Type of Implant and Restoration: Mini implants, standard implants, and the type of crown/bridge/denture all affect the price.
- Preparatory Procedures: Bone grafting, sinus lifts, or extractions add to the overall cost.
- Dental Professional's Expertise: Highly experienced specialists may charge more.
- Materials Used: Zirconia implants or custom abutments can be pricier.
Here's a general breakdown of costs in the US:
- Single Dental Implant (Post Only): $1,500 - $3,000
- Abutment: $500 - $1,500
- Crown (Porcelain/Ceramic): $1,000 - $3,000
- Total for a Single Implant (Post, Abutment, Crown): $3,000 - $7,500+
For more extensive restorations:
- Implant-Supported Bridge (3-4 units on 2 implants): $6,000 - $15,000+
- Full Arch Implant-Supported Denture (All-on-4® or All-on-6®): $15,000 - $30,000+ per arch for a removable overdenture, and $25,000 - $60,000+ per arch for a fixed full-arch restoration (e.g., in Houston, these costs are often on the higher end due to specialized clinics).
- This includes the implants, abutments, and the final prosthetic arch.
Insurance Coverage
Dental insurance coverage for implants varies widely.
- Medical vs. Dental Insurance: While dental implants are a dental procedure, some parts of the treatment (especially those related to bone grafting or if tooth loss is due to an accident) might be partially covered by medical insurance if deemed medically necessary. Always check with both providers.
- "Missing Tooth Clause": Many dental insurance plans have a "missing tooth clause" that excludes coverage for teeth missing prior to enrollment in the plan.
- Limited Coverage: Typically, dental insurance does not cover the implant post itself, as it's often classified as a cosmetic procedure or a major procedure with limited benefits. However, they may cover:
- A percentage of the diagnostic procedures (X-rays, CT scans).
- A portion of the tooth extraction.
- A percentage of the crown or prosthetic appliance (which is similar to what they'd cover for a bridge or conventional crown).
- A portion of bone grafting if it's considered a necessary part of preparing the site for a covered procedure (like a crown).
Pro Tip: Before beginning the implants process, request a pre-determination of benefits from your dental insurance provider. This will give you a clear understanding of what your specific plan will cover and what your out-of-pocket expenses will be.
Recovery and Aftercare
Successful dental implant integration and longevity heavily depend on diligent recovery and aftercare.
Immediate Post-Operative Care (First 24-72 Hours)
- Bleeding Control: Bite down on gauze pads for 30-45 minutes. Replace as needed. Slight oozing is normal for 24-48 hours.
- Pain Management: Take prescribed pain medication as directed. Over-the-counter pain relievers (e.g., ibuprofen) can also help manage discomfort.
- Swelling: Apply ice packs to the outside of your face (15 minutes on, 15 minutes off) for the first 24-48 hours to minimize swelling.
- Diet: Stick to soft foods and liquids (e.g., soup, yogurt, mashed potatoes, smoothies) for the first few days. Avoid chewing directly on the implant site. Gradually reintroduce solid foods as comfort allows.
- Oral Hygiene:
- Do NOT rinse vigorously or spit for the first 24 hours, as this can dislodge the blood clot.
- After 24 hours, gently rinse your mouth with warm salt water (1/2 teaspoon salt in 8 ounces warm water) several times a day, especially after meals.
- Brush your other teeth carefully, avoiding the surgical site. Your dentist may prescribe an antimicrobial mouthwash.
- Activity: Avoid strenuous activity for several days to prevent increased bleeding and swelling.
- Smoking/Alcohol: Absolutely avoid smoking and alcohol, as they significantly impair healing and increase the risk of implant failure.
During Osseointegration (3-6 Months)
- Diet: Continue to eat a soft to moderate diet, especially avoiding hard, crunchy, or sticky foods on the implant site.
- Oral Hygiene: Maintain excellent oral hygiene, brushing and flossing regularly as instructed by your dentist.
- Avoid Pressure: Do not place any pressure on the implant site (e.g., by chewing or wearing a temporary denture that presses directly on it).
- Regular Check-ups: Attend all scheduled follow-up appointments with your dentist to monitor healing.
Long-Term Care (After Restoration)
- Excellent Oral Hygiene: Brush at least twice a day with a soft-bristled toothbrush and fluoride toothpaste. Floss daily, including around your implant crown(s). Specialized floss or interdental brushes may be recommended for cleaning around implants.
- Regular Dental Check-ups: Visit your dentist and hygienist every 6 months for professional cleanings and examinations. They will monitor the health of your implants, gums, and surrounding teeth.
- Avoid Hard/Sticky Foods: While implants are strong, excessive force on very hard foods (like ice, hard candies) can potentially damage the crown or even the implant over many years.
- Address Bruxism: If you grind or clench your teeth (bruxism), your dentist may recommend a nightguard to protect your implants and natural teeth.
- Quit Smoking: Smoking significantly increases the risk of peri-implantitis (gum disease around implants) and implant failure.
Prevention of Tooth Loss Leading to Implants
While dental implants are an excellent solution for missing teeth, preventing tooth loss in the first place is always the best approach.
- Maintain Excellent Oral Hygiene:
- Brush twice daily for two minutes each time with fluoride toothpaste.
- Floss daily to remove plaque and food particles from between teeth and under the gumline.
- Consider an antimicrobial mouthwash if recommended by your dentist.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months for professional cleanings and comprehensive examinations. This allows for early detection and treatment of cavities and gum disease.
- Balanced Diet: Limit sugary and acidic foods and drinks, which contribute to tooth decay.
- Protect Your Teeth:
- Wear a mouthguard during sports activities to prevent trauma.
- If you grind or clench your teeth (bruxism), use a nightguard to protect against excessive wear and fractures.
- Avoid Tobacco Products: Smoking and chewing tobacco are major risk factors for gum disease, tooth loss, and oral cancer.
- Address Dental Problems Promptly: Don't ignore tooth pain, sensitivity, or bleeding gums. Early intervention can save a tooth.
Risks and Complications of the Implants Process
While dental implants have a high success rate (typically 95% or higher), like any surgical procedure, there are potential risks and complications.
Surgical Risks (Short-Term)
- Infection: Though rare, bacterial infection at the implant site can occur. This is usually managed with antibiotics.
- Nerve Damage: In very rare cases, implant placement can damage nerves, leading to numbness, tingling, or pain in the lips, gums, tongue, or chin. Careful pre-surgical planning with CBCT scans minimizes this risk.
- Sinus Perforation: During upper jaw implant placement, the implant could penetrate the sinus cavity. This is usually managed immediately during surgery with a sinus lift or by selecting a shorter implant.
- Bleeding: Some bleeding is normal after surgery, but excessive or prolonged bleeding is a potential complication.
- Swelling and Bruising: Common and temporary, managed with ice packs and anti-inflammatory medication.
- Implant Failure (Early): The implant may not properly integrate with the bone. This can be due to poor bone quality, infection, smoking, or excessive force during the healing period.
Long-Term Complications
- Peri-implantitis: This is a serious inflammatory condition affecting the gum and bone tissues around a dental implant, similar to periodontitis around natural teeth. It can lead to bone loss and eventual implant failure if not treated. Smoking is a major risk factor.
- Mechanical Complications:
- Abutment/Screw Loosening or Fracture: The small screws holding the abutment or crown can loosen or, rarely, fracture.
- Crown/Prosthetic Damage: The prosthetic tooth itself can chip, crack, or break, similar to natural teeth or crowns.
- Implant Failure (Late): Even after successful osseointegration, an implant can fail years later due to peri-implantitis, trauma, or excessive biting forces.
- Esthetic Issues: In some cases, the gum line might recede, exposing a small part of the metal implant or abutment, which can be an aesthetic concern.
- Bruxism-Related Issues: Chronic teeth grinding can put excessive stress on implants, leading to complications.
Pro Tip: Choosing an experienced and highly qualified dental professional for your implants process significantly reduces the risk of complications. Always follow all post-operative instructions meticulously.
Children / Pediatric Considerations
Dental implants are generally not recommended for children or adolescents whose jaws are still developing. Placing an implant in a jaw that is still growing can lead to complications, as the implant will not move with the surrounding bone and teeth, potentially causing it to appear sunken or out of alignment as the child matures.
Typically, dentists advise waiting until jaw growth is complete, which is usually around 18-20 years of age for girls and 20-22 years for boys. For missing teeth in children, temporary solutions like space maintainers, removable partial dentures, or adhesive bridges are used until they reach an age suitable for implant placement.
Cost Breakdown: Detailed Overview and Financing
Beyond the general cost ranges, understanding the components of dental implant costs and available payment options is vital.
Average US Costs (Low, Mid, High) by Component
| Component | Low-End Estimate (US) | Mid-Range Estimate (US) | High-End Estimate (US) |
|---|---|---|---|
| Initial Consultation/X-rays | $50 | $150 | $300 |
| CBCT Scan | $200 | $400 | $700 |
| Tooth Extraction | $150 | $300 | $500 |
| Bone Grafting (per site) | $300 | $800 | $2,500 |
| Sinus Lift | $1,500 | $2,500 | $4,000 |
| Implant Post Surgery | $1,500 | $2,500 | $3,500 |
| Abutment | $500 | $1,000 | $1,500 |
| Crown (Porcelain/Ceramic) | $1,000 | $1,800 | $3,000 |
| Total for Single Implant | $3,800 (minimal prep) | $6,500 | $11,500+ |
| All-on-4® (per arch) | $15,000 | $25,000 | $40,000+ |
Note: These are average ranges. Exact costs will depend on your specific case, location (e.g., Houston often sees higher-end pricing), and chosen dental provider.
With vs. Without Insurance
As discussed, dental insurance coverage for implants is often limited.
- Without Insurance: You will be responsible for the full cost of the procedure. Many dentists offer cash discounts or payment plans for uninsured patients.
- With Insurance: Expect your insurance to cover only a portion of the total cost, typically for diagnostic X-rays, extractions, and potentially a percentage of the final crown. The implant post itself is rarely fully covered. Your out-of-pocket expenses will be the remaining balance after insurance contributions and any applicable deductibles or co-pays.
Payment Plans and Financing Options
Recognizing the significant investment, most dental practices offer or work with third-party financing solutions to make implants more accessible.
- In-Office Payment Plans: Some practices allow patients to make interest-free payments over a set period (e.g., 6-12 months).
- Third-Party Financing (e.g., CareCredit, LendingClub): These companies specialize in healthcare financing, offering various payment plans, including:
- Deferred Interest: No interest charged if the full amount is paid within a promotional period (e.g., 6, 12, 18, or 24 months). If not paid in full, interest is typically applied retroactively.
- Fixed Low-Interest Rates: Longer-term payment plans with consistent, manageable monthly payments.
- Personal Loans: You may consider a personal loan from a bank or credit union, though interest rates can vary.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have an HSA or FSA, you can use pre-tax dollars to pay for dental implant procedures, offering significant tax savings.
Pro Tip: Discuss all payment and financing options with your dental office's financial coordinator early in the implants process. They can help you navigate insurance benefits and find the best payment solution for your budget.
Frequently Asked Questions
### How painful is the dental implants process?
Most patients report that the implant placement surgery itself is less painful than expected, often comparable to a tooth extraction. Local anesthesia completely numbs the area during the procedure. Post-operative discomfort is manageable with prescribed pain medication and over-the-counter pain relievers, typically subsiding within a few days to a week.
### How long does the entire implants process take?
The full implants process, from initial consultation to final crown placement, typically takes 3 to 9 months. This timeline includes initial planning, any necessary preparatory procedures (like bone grafting, which can add several months), the surgical placement, and the crucial osseointegration period (3-6 months), followed by abutment placement and final restoration.
### Are dental implants permanent?
With proper care and maintenance, dental implants can last for 20 years or even a lifetime. The implant post itself is designed to be a permanent fixture in your jawbone. The crown or prosthetic attached to the implant may need to be replaced after 10-15 years due to normal wear and tear, similar to a natural crown or bridge.
### What are the alternatives to dental implants?
Alternatives to dental implants include traditional fixed dental bridges (which require support from adjacent teeth), removable partial dentures (for multiple missing teeth), and complete dentures (for a full arch of missing teeth). While these options are generally less expensive initially, they do not offer the same long-term benefits for bone preservation, stability, and natural feel as implants.
### Can I get dental implants if I have bone loss?
Yes, in many cases, you can still get dental implants even with some bone loss. Procedures like bone grafting or a sinus lift can augment the existing bone, creating sufficient volume and density to support an implant. Your dentist will determine the best course of action based on a detailed 3D CBCT scan.
### What is the success rate of dental implants?
Dental implants boast a very high success rate, generally around 95-98% when performed by experienced professionals and with proper patient selection and aftercare. Success rates can be slightly lower in specific situations, such as in smokers or individuals with certain uncontrolled systemic diseases.
### How do I clean my dental implants?
Cleaning dental implants is similar to cleaning natural teeth. You should brush them twice daily with a soft-bristled toothbrush and floss daily. Special interdental brushes or implant-specific floss may be recommended to clean around the implant crown and gum line effectively. Regular professional cleanings are also essential.
### Can dental implants fail? What happens then?
Yes, while rare, dental implants can fail. Failure can occur early if osseointegration doesn't happen, or later due to infection (peri-implantitis), excessive biting forces, or trauma. If an implant fails, it usually needs to be removed. After a healing period, and potentially another bone graft, a new implant can often be placed.
### Am I a good candidate for dental implants?
Most individuals in good general and oral health are candidates for dental implants. Key factors include sufficient jawbone density (or willingness to undergo grafting), healthy gum tissue, and a commitment to excellent oral hygiene. Conditions like uncontrolled diabetes, heavy smoking, or certain medical treatments might contraindicate implants, but a thorough evaluation by your dentist will determine your eligibility.
### What is "All-on-4" and how does it relate to implant-supported dentures in Houston?
"All-on-4" (or All-on-6) is a specific technique where a full arch of teeth (upper or lower) is supported by only four (or six) strategically placed dental implants. This method is popular for patients in Houston and elsewhere who need to replace all their teeth in an arch, as it often allows for a temporary fixed bridge to be placed on the same day as surgery, offering immediate aesthetic and functional benefits. The implants are typically angled to maximize contact with available bone, reducing the need for extensive bone grafting.
When to See a Dentist
It's crucial to know when to seek professional dental attention, both for the initial consideration of implants and for managing any concerns post-procedure.
Considering Dental Implants
- Missing one or more teeth: If you have gaps in your smile, difficulty chewing, or feel your speech is affected by missing teeth.
- Wearing ill-fitting or uncomfortable dentures: If your current dentures slip, cause sores, or impact your quality of life.
- Have failing teeth: If you have teeth that are severely decayed, fractured, or suffering from advanced gum disease, and extraction is imminent.
- Concerned about bone loss: If you've been told you have receding gums or a "sunken" facial appearance due to long-term tooth loss.
These are all valid reasons to schedule a consultation with a dentist, oral surgeon, or periodontist to discuss whether dental implants are a suitable option for you.
Warning Signs After Implant Surgery (Red Flags)
Contact your dental professional immediately if you experience any of the following after your implant surgery:
- Severe or worsening pain: Pain that doesn't subside with medication or worsens significantly after the initial 2-3 days.
- Excessive bleeding: Continuous heavy bleeding that saturates gauze pads quickly, even after applying pressure for a sustained period.
- Persistent swelling: Swelling that increases after 48-72 hours or extends to your neck or under your eye.
- Fever or chills: These could indicate an infection.
- Pus or foul discharge: Any sign of infection at the surgical site.
- Numbness: Prolonged or new onset of numbness in your lips, tongue, or chin beyond what was expected from the anesthesia.
- Loose implant: If you feel the implant post moving in the bone.
These symptoms warrant immediate attention to prevent serious complications and ensure the success of your implants process. Prompt communication with your dental team is essential for optimal outcomes.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Implantologist: Complete Guide
Losing a tooth can be a significant setback, impacting not only your smile but also your ability to speak, chew, and maintain overall oral health. In fact, over 3 million Americans currently have dental implants, and that number is projected to grow significantly as more people seek a durable, n
March 8, 2026
Dentures Over Implants: Complete Guide
Missing multiple teeth or even an entire arch can profoundly impact your life, affecting everything from your ability to chew and speak to your self-confidence. For millions of Americans, traditional removable dentures have long been a solution, but they often come with compromises: slipping, discom
March 8, 2026

Implants Dentaires: Complete Guide
Missing teeth can dramatically impact not just your smile, but your overall health, confidence, and quality of life. In the United States, an estimated 178 million adults are missing at least one tooth, while approximately 40 million are missing all their teeth. These statistics underscore a
March 8, 2026
Carolina Implant: Complete Guide
Dental implants represent a revolutionary advancement in restorative dentistry, offering a durable, aesthetically pleasing, and highly functional solution for missing teeth. For individuals seeking to restore their smile, chewing ability, and overall oral health, understanding the options available
March 8, 2026