Implantitis: Complete Guide
Key Takeaways
- Imagine investing in a solution to restore your smile and chewing function, only to face a new set of challenges later on. Dental implants boast a remarkable success rate, often cited as high as 95-98%, providing a durable and aesthetically pleasing replacement for missing teeth. However, like a
Implantitis: Complete Guide
Imagine investing in a solution to restore your smile and chewing function, only to face a new set of challenges later on. Dental implants boast a remarkable success rate, often cited as high as 95-98%, providing a durable and aesthetically pleasing replacement for missing teeth. However, like any medical procedure, they are not entirely immune to complications. One such complication, which can significantly impact the longevity and health of your implant, is implantitis. This inflammatory condition affecting the tissues surrounding a dental implant can jeopardize its stability and, if left untreated, lead to implant failure. Understanding implantitis is crucial for anyone with dental implants or considering them, as early detection and proper management are key to preserving your oral health and investment.
This comprehensive guide will delve deep into implantitis, exploring what it is, why it occurs, its tell-tale signs, and the various treatment options available. We'll also cover crucial aspects like prevention, costs, recovery, and what you can do to protect your smile. By the end of this article, you will have a clear understanding of implantitis, empowering you to take proactive steps for the long-term success of your dental implants.
Key Takeaways:
- Implantitis Defined: An inflammatory disease affecting the hard and soft tissues surrounding a dental implant, leading to progressive bone loss.
- Prevalence: Affects approximately 10-20% of dental implants, with severe forms being less common.
- Primary Cause: Bacterial infection, often exacerbated by poor oral hygiene, smoking, and certain systemic conditions like uncontrolled diabetes.
- Key Symptoms: Red, swollen, or bleeding gums around the implant, pus discharge, persistent discomfort, and visible implant threads due to bone loss.
- Treatment Costs: Non-surgical treatment can range from $300 to $1,500 per implant, while surgical interventions (e.g., debridement with bone grafting) can range from $1,500 to $5,000+ per implant, potentially reaching $8,000+ if implant removal and replacement are necessary.
- Prevention is Key: Meticulous oral hygiene, regular dental check-ups, smoking cessation, and managing systemic diseases are vital for preventing implantitis.
- Early Detection Matters: Prompt dental evaluation at the first sign of symptoms can significantly improve treatment outcomes and preserve your implant.
What It Is / Overview
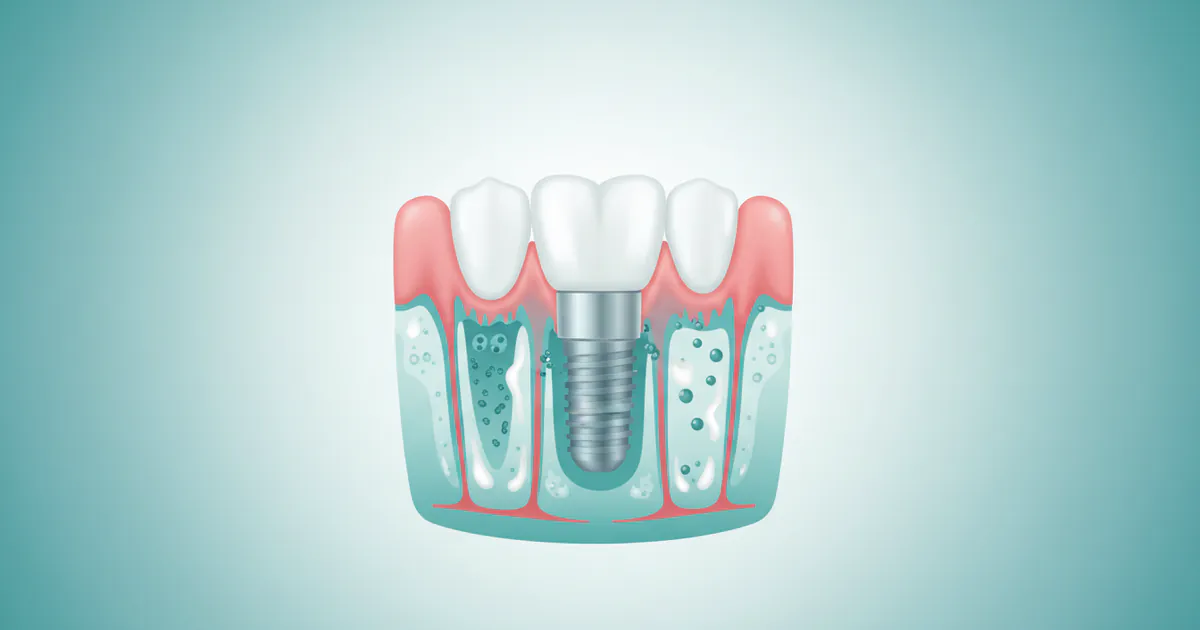
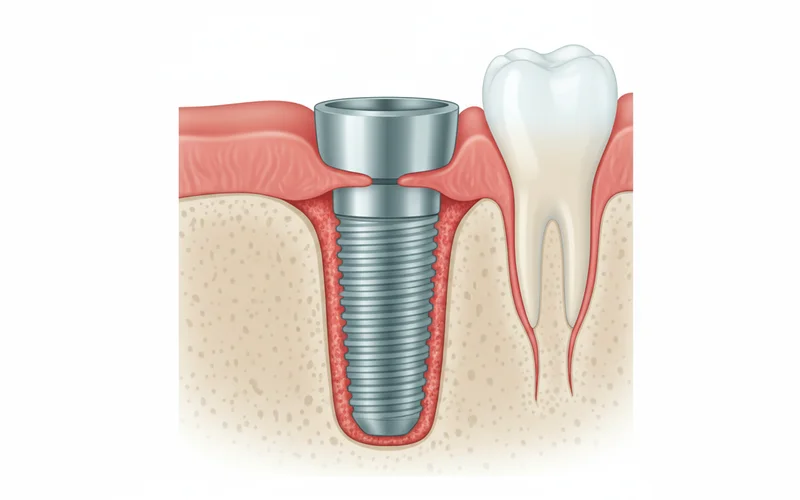
Implantitis is an inflammatory condition that affects the hard and soft tissues surrounding a functioning dental implant. It's essentially the dental implant equivalent of periodontitis (gum disease) that affects natural teeth. When a dental implant is placed, it integrates with your jawbone through a process called osseointegration, forming a strong, stable foundation for a prosthetic crown, bridge, or denture. Healthy peri-implant tissues—the gums and bone surrounding the implant—are crucial for its long-term success.
Implantitis begins when bacteria accumulate on the implant surface and the surrounding gum line, triggering an inflammatory response. This inflammation initially affects the soft tissues, similar to gingivitis around a natural tooth. If left unaddressed, it progresses to involve the supporting bone, leading to progressive bone loss around the implant. This bone loss weakens the implant's foundation, eventually causing it to become mobile and, in severe cases, necessitating its removal.
The condition is not rare. Research indicates that peri-implant mucositis (the precursor to implantitis, affecting only soft tissues) can affect up to 43% of implants, while implantitis itself affects approximately 10-20% of individuals with dental implants. While this still means the vast majority of implants remain healthy, the incidence is significant enough to warrant serious attention.
Types / Variations
Understanding implantitis involves recognizing its progression, often categorized into two main stages:
Peri-Implant Mucositis
This is the initial, milder form of inflammation that affects only the soft tissues (gums) around a dental implant. It is reversible if detected and treated early.
- Characteristics: Redness, swelling, and bleeding upon probing around the implant.
- Key Difference from Implantitis: No radiographic evidence of bone loss beyond the initial bone remodeling that occurs immediately after implant placement.
- Prognosis: Excellent with proper oral hygiene and professional cleaning.
Implantitis
This is the more advanced stage where the inflammation has progressed to involve the supporting bone, leading to irreversible bone loss around the implant.
- Characteristics: All symptoms of peri-implant mucositis (redness, swelling, bleeding, pus) plus radiographic evidence of progressive bone loss and, in severe cases, implant mobility.
- Progression: Can range from mild to severe, depending on the extent of bone loss and the presence of pus or mobility.
- Prognosis: More challenging to treat than mucositis and may require surgical intervention. Untreated implantitis can lead to implant failure.
It's also worth noting that implantitis can manifest differently depending on the location and specific characteristics of the implant and patient, but the underlying mechanism of bacterial infection and inflammatory bone destruction remains consistent.
Causes / Why It Happens
Implantitis is a multifactorial disease, meaning several factors can contribute to its development. The primary culprit, however, is bacterial infection. When bacteria accumulate around the implant, they form a biofilm (plaque) that triggers an inflammatory response in the surrounding tissues.
Here are the key contributing factors:
1. Poor Oral Hygiene
This is arguably the most significant risk factor. Just like natural teeth, dental implants require diligent brushing, flossing, and regular professional cleanings. Inadequate oral hygiene allows plaque and calculus (hardened plaque) to accumulate, providing a haven for pathogenic bacteria to thrive and initiate inflammation. ADA Guidelines: The American Dental Association consistently emphasizes the importance of good oral hygiene for maintaining overall oral health, which directly impacts implant longevity.
2. Smoking
Smoking significantly impairs the body's ability to heal and fight infection. It reduces blood flow to the gums, compromises immune function, and alters the bacterial environment in the mouth, making implant patients who smoke much more susceptible to implantitis. Smokers have a significantly higher risk of both implant failure and implantitis compared to non-smokers.
3. Systemic Diseases
Certain health conditions can increase the risk of implantitis:
- Uncontrolled Diabetes: High blood sugar levels impair immune function and wound healing, making individuals more prone to infections and inflammation around implants.
- Immunosuppression: Conditions or medications that suppress the immune system (e.g., organ transplant recipients, certain autoimmune diseases) can reduce the body's ability to combat bacterial challenges.
- Osteoporosis (especially with certain medications): While not a direct cause of infection, some medications used to treat osteoporosis (bisphosphonates) can, in rare cases, affect bone health and healing around implants, though this is distinct from typical implantitis.
4. History of Periodontitis
Patients who have a history of periodontitis (gum disease) around their natural teeth are at a higher risk of developing implantitis. The same bacteria that caused periodontitis can colonize the implant surfaces, and these individuals often have a genetic predisposition or behavioral patterns that make them susceptible to gum inflammation.
5. Occlusal Overload (Excessive Biting Forces)
While less of a direct cause of infection, excessive or improperly distributed biting forces on an implant can contribute to mechanical stress. This trauma, especially in conjunction with bacterial presence, might accelerate bone loss or create micro-gaps that facilitate bacterial invasion, particularly if the implant is poorly positioned or the prosthetic restoration is incorrectly designed.
6. Implant-Related Factors
- Rough Implant Surfaces: While many implants are designed with rough surfaces to enhance osseointegration, extremely rough surfaces can sometimes make them harder to decontaminate if bacteria colonize.
- Excess Cement: If too much dental cement is used to attach the crown to the implant abutment, excess cement can extrude into the surrounding gum tissue. This cement acts as a foreign body and a niche for bacterial accumulation, making cleaning difficult and provoking inflammation.
- Poor Implant Position/Design: Implants placed too close together, too shallow, or at an incorrect angle can create areas that are difficult to clean, leading to plaque accumulation. Similarly, poorly designed restorations that impinge on gum tissue can compromise oral hygiene.
- Surgical Trauma: While rare with experienced practitioners, surgical complications or contamination during implant placement can predispose to early inflammation.
7. Genetic Predisposition
Some individuals may be genetically more susceptible to inflammatory responses, which can exacerbate the progression of implantitis once it starts.
Pro Tip: If you have dental implants, be especially vigilant about your oral hygiene and lifestyle choices, particularly if any of these risk factors apply to you. Discuss your medical history and habits with your dentist or periodontist.
Signs and Symptoms
Recognizing the early signs of implantitis is critical for successful treatment. The symptoms can develop gradually and may not always be painful initially, making regular dental check-ups essential.
Early Warning Signs (Peri-Implant Mucositis Stage):
- Redness of the Gums: The gum tissue around the implant may appear redder than the surrounding healthy gum.
- Swelling: The gum tissue may be puffy or swollen around the implant.
- Bleeding on Probing: When you brush, floss, or during a professional dental cleaning, the gums around the implant may bleed easily. This is often the earliest and most common sign.
- Mild Tenderness or Discomfort: You might feel a subtle, dull ache or tenderness in the area.
Advanced Signs (Implantitis Stage):
- Persistent Bad Taste or Breath (Halitosis): Bacterial infection can lead to an unpleasant taste in your mouth or chronic bad breath.
- Pus Discharge: You may notice pus oozing from around the implant, especially when pressure is applied to the gum tissue. This is a clear indicator of active infection.
- Pain: While not always present in early stages, pain or throbbing around the implant can develop as the condition worsens, especially during chewing.
- Visible Implant Threads: As bone loss progresses, the metallic threads of the implant body may become visible above the gum line.
- Increased Probing Depth: Your dentist will measure the depth of the gum pocket around the implant. An increase in this depth indicates gum detachment and potential bone loss.
- Implant Mobility: This is a late and severe sign. If the implant feels loose when you touch it or chew, it indicates significant bone loss and compromised integration, often necessitating removal.
- Radiographic Bone Loss: This is the definitive diagnostic criterion for implantitis, visible on X-rays. Your dentist will compare current X-rays with baseline images taken after implant placement to detect progressive bone loss.
When to Seek Help: Do not wait for pain or mobility. Any sign of redness, swelling, or bleeding around your implant warrants an immediate visit to your dentist or periodontist. Early intervention can prevent the progression from reversible peri-implant mucositis to irreversible implantitis.
Treatment Options
The treatment for implantitis depends on the severity of the condition, specifically whether it's peri-implant mucositis or full-blown implantitis with bone loss, and the extent of that bone loss. The goal is always to eliminate the infection, decontaminate the implant surface, and regenerate lost tissue where possible.
A. Non-Surgical Treatment (Primarily for Peri-Implant Mucositis or Early Implantitis)
These methods focus on cleaning the implant surface and controlling the bacterial infection without surgical intervention.
-
Mechanical Debridement:
- What it is: Professional cleaning using specialized instruments (plastic or titanium curettes, ultrasonic scalers with plastic tips, air-abrasive devices with glycine powder) to remove plaque and calculus from the implant surface and surrounding tissues.
- Pros: Non-invasive, relatively inexpensive, often effective for mucositis.
- Cons: Limited access to deeply infected areas or roughened implant surfaces, may not fully remove bacterial biofilm.
- Cost: Typically ranges from $150-$400 per implant per session, often covered partially by dental insurance as a deep cleaning or specialized periodontal procedure.
-
Antimicrobial Therapy:
- What it is:
- Local Application: Placement of antibiotic gels, chips, or rinses (e.g., chlorhexidine) directly into the peri-implant pockets to target bacteria.
- Systemic Antibiotics: Oral antibiotics may be prescribed in conjunction with mechanical debridement, especially in cases of active infection with pus or significant inflammation.
- Pros: Directly combats bacterial infection.
- Cons: Risk of antibiotic resistance, potential side effects, local application might not reach all infected areas effectively.
- Cost: Varies, local antimicrobials can add $50-$200 per site. Oral antibiotics are typically $20-$100 for a course.
- What it is:
B. Surgical Treatment (For Established Implantitis with Bone Loss)
When non-surgical approaches are insufficient, or if there's significant bone loss, surgical intervention is necessary to access, clean, and potentially repair the damaged tissues.
-
Open Debridement and Surface Decontamination:
- What it is: The gum tissue is surgically flapped open to expose the entire implant surface and surrounding bone. The implant surface is meticulously cleaned and decontaminated using various methods (curettes, lasers, air-abrasion, chemical agents like citric acid or hydrogen peroxide).
- Pros: Allows for thorough cleaning and removal of granulation tissue (inflamed tissue).
- Cons: Invasive, requires healing time, may not regenerate lost bone.
- Cost: Ranges from $800 to $2,500 per implant, depending on complexity and region.
-
Reconstructive Surgery (Guided Bone Regeneration - GBR):
- What it is: After thorough cleaning and decontamination, bone graft materials (autogenous, allograft, xenograft, or alloplast) are placed in the bone defects around the implant. A barrier membrane is often used to protect the graft and encourage bone regeneration.
- Pros: Aims to regenerate lost bone, potentially improving implant stability and prognosis.
- Cons: More complex and costly, longer healing time, success is not guaranteed, especially if the bone defect is very large or implant surface is severely damaged.
- Cost: Can range from $2,000 to $5,000+ per implant, depending on the extent of grafting and materials used. This is often an add-on to the open debridement.
-
Implant Surface Modification/Ablation:
- What it is: Techniques like laser ablation or electrosurgery are used to remove or modify the contaminated surface of the exposed implant to make it less hospitable for bacteria.
- Pros: Can improve the effectiveness of decontamination.
- Cons: Can be technique-sensitive and potentially alter implant integrity.
- Cost: Often integrated into surgical debridement costs, may add a few hundred dollars.
-
Implant Removal (Explantation):
- What it is: In severe cases where there is extensive bone loss, uncontrollable infection, or significant implant mobility, the implant must be removed.
- Pros: Eliminates the source of infection, allows for healing of the site.
- Cons: Loss of the dental implant, requires further treatment (e.g., bone grafting and replacement implant, bridge, or partial denture) to restore the missing tooth.
- Cost: Implant removal can range from $300 to $1,000. If followed by bone grafting and a new implant placement, the total cost can easily exceed $5,000-$8,000.
Treatment Comparison Table:
| Treatment Type | Severity Addressed | Procedure Description | Pros | Cons | Average Cost (US) |
|---|---|---|---|---|---|
| Non-Surgical | Peri-Implant Mucositis, Early Implantitis | Professional cleaning, local/systemic antimicrobials | Less invasive, lower cost, good for early stages | Limited effectiveness for deep defects/bone loss | $300 - $1,500 |
| Surgical Debridement | Moderate to Advanced Implantitis | Gum flap, thorough cleaning of implant surface | Better access, thorough decontamination | Invasive, healing time required | $800 - $2,500 |
| Reconstructive (GBR) | Moderate to Advanced Implantitis (with bone defects) | Surgical debridement + bone grafting + membrane | Can regenerate lost bone, improve prognosis | More complex, higher cost, longer healing, success varies | $2,000 - $5,000+ |
| Implant Removal | Severe, Untreatable Implantitis | Surgical extraction of the failing implant | Eliminates infection source, allows healing | Loss of implant, need for further restoration | $300 - $1,000 |
Step-by-Step Process: What to Expect During Implantitis Treatment
The exact steps will vary based on the diagnosis and chosen treatment plan, but here's a general overview:
Step 1: Diagnosis and Assessment
- Initial Consultation: Your dentist or periodontist will evaluate your symptoms, medical history, and oral hygiene habits.
- Clinical Examination: This includes checking for redness, swelling, bleeding, and pus. They will use a periodontal probe to measure the depth of the gum pocket around the implant.
- Radiographic Examination: X-rays (periapical, panoramic, or 3D Cone Beam CT) will be taken to assess the extent of bone loss around the implant and compare it to previous images. This is crucial for distinguishing mucositis from implantitis.
- Treatment Plan Development: Based on the findings, a personalized treatment plan will be discussed with you, outlining the recommended procedures, their pros and cons, and expected outcomes.
Step 2: Non-Surgical Treatment (if indicated)
- Professional Cleaning: If it's peri-implant mucositis or early implantitis, your hygienist or dentist will perform a thorough cleaning of the implant and surrounding tissues, often using specialized non-metallic instruments to avoid scratching the implant surface.
- Antimicrobial Agents: You might be prescribed an antimicrobial mouth rinse (e.g., chlorhexidine) for home use or have a localized antibiotic applied to the gum pocket.
- Oral Hygiene Instruction: Detailed guidance on how to improve your daily brushing and flossing around the implant will be provided.
Step 3: Surgical Treatment (if non-surgical fails or implantitis is advanced)
- Anesthesia: Local anesthesia will be administered to numb the treatment area. Sedation options may also be available for comfort.
- Gum Flap: The gum tissue around the implant will be carefully lifted (a "flap" is created) to expose the infected implant surface and underlying bone.
- Debridement and Decontamination: All infected tissue (granulation tissue) will be removed. The exposed implant surface will be thoroughly cleaned using various techniques to remove bacteria and biofilm.
- Bone Grafting (if applicable): If there is significant bone loss that can be regenerated, bone graft material will be placed around the implant, often covered by a protective membrane.
- Repositioning and Suturing: The gum flap will be carefully repositioned and sutured back into place.
Step 4: Post-Treatment Care and Follow-up
- Medications: You may be prescribed pain relievers, anti-inflammatory drugs, or antibiotics.
- Home Care Instructions: Detailed instructions on how to care for the surgical site, including diet restrictions, oral hygiene modifications, and activity limitations, will be provided.
- Follow-up Appointments: Regular follow-up appointments will be scheduled to monitor healing, remove sutures (if non-resorbable), and assess the success of the treatment. This often involves taking new X-rays to check bone levels.
- Long-Term Maintenance: Regardless of the treatment, rigorous long-term maintenance, including excellent home care and regular professional cleanings, is paramount to prevent recurrence.
Cost and Insurance
The cost of implantitis treatment in the US can vary significantly based on the severity of the condition, the type of treatment chosen (non-surgical vs. surgical, with or without bone grafting), the location of the dental practice, and the expertise of the treating dentist or periodontist.
Average US Price Ranges:
-
Non-Surgical Debridement and Antimicrobial Therapy:
- Low: $300 - $600 per implant (e.g., thorough cleaning, local antiseptic rinse)
- Mid: $600 - $1,000 per implant (e.g., multiple deep cleaning sessions, local antibiotic placement)
- High: $1,000 - $1,500 per implant (e.g., more complex non-surgical protocols over extended visits)
-
Surgical Debridement (without bone graft):
- Low: $800 - $1,500 per implant
- Mid: $1,500 - $2,000 per implant
- High: $2,000 - $2,500 per implant
-
Surgical Debridement with Guided Bone Regeneration (GBR):
- Low: $2,000 - $3,500 per implant (for minor bone defects)
- Mid: $3,500 - $4,500 per implant (for moderate bone defects)
- High: $4,500 - $5,000+ per implant (for extensive bone defects requiring significant grafting)
-
Implant Removal (Explantation):
- Simple Extraction: $300 - $500
- Surgical Extraction (complex): $500 - $1,000
- If bone grafting is performed at the time of removal (to prepare for future implant placement), add $500 - $2,000 for the graft.
Total Cost for Complete Failure & Replacement: If an implant must be removed, and a new one is placed after healing (potentially with bone grafting), the total cost can quickly escalate. This could involve the cost of removal, bone grafting, a new implant, and a new crown, totaling $5,000 to $8,000+ per site. This highlights the importance of prevention and early treatment.
Insurance Coverage:
Dental insurance coverage for implantitis treatment can be complex and varies significantly between plans.
- Diagnostic Procedures: X-rays and examinations are usually covered under preventive or diagnostic benefits.
- Non-Surgical Treatment: Procedures like deep cleanings (code D4341/D4342 for periodontal scaling and root planing) or localized antimicrobial applications might be covered, similar to gum disease treatment for natural teeth.
- Surgical Treatment: Surgical procedures for implantitis might be classified as "major restorative" or "periodontal surgery" by your insurance. Coverage can range from 20% to 80%, but often with annual maximums (e.g., $1,000 - $2,000 per year). Some plans may not cover peri-implantitis surgery specifically, or they may apply strict limitations.
- Implant Removal/Replacement: If an implant needs to be removed and replaced, the new implant placement itself is often not covered or covered at a low percentage, as many plans still consider implants to be a "cosmetic" or "non-essential" procedure, especially older plans. However, coverage for the crown/restoration on the new implant might be available.
Pro Tip: Always contact your dental insurance provider before starting any treatment to understand your specific benefits, deductibles, co-pays, and annual maximums. Ask for pre-authorization if the estimated costs are high.
Recovery and Aftercare
Recovery from implantitis treatment depends heavily on the type and invasiveness of the procedure performed.
Non-Surgical Treatment:
- Immediate Aftercare: Minimal discomfort. You might experience some gum sensitivity, which typically resolves within a few days. You may be advised to use an antimicrobial mouth rinse.
- Healing Timeline: Gums usually feel better within a week.
- Long-term Aftercare: Critical. Maintain excellent daily oral hygiene (brushing, flossing, interdental brushes) as instructed. Adhere strictly to your dentist's recommended schedule for professional cleanings and follow-up examinations (often every 3-4 months initially).
Surgical Treatment (Debridement, GBR):
- Immediate Aftercare (First 24-72 hours):
- Pain: Expect some discomfort. Your dentist will prescribe pain medication or recommend over-the-counter options.
- Swelling: Swelling is common and can be managed with ice packs applied to the outside of your face.
- Bleeding: Minor oozing is normal; bite on gauze pads as instructed.
- Diet: Stick to soft, cool foods initially. Avoid hot foods, crunchy or sticky items, and using a straw (which can dislodge blood clots).
- Healing Timeline:
- Sutures: Dissolvable sutures will disappear in 1-2 weeks; non-dissolvable ones will be removed at a follow-up appointment.
- Soft Tissue Healing: Gums typically heal in 2-4 weeks.
- Bone Graft Healing (if performed): Bone regeneration takes much longer, often 4-6 months or more, before the new bone is mature.
- Long-term Aftercare:
- Oral Hygiene: Gently clean the area as directed, initially avoiding direct brushing on the surgical site. Once healed, resume meticulous hygiene.
- Follow-up Appointments: Crucial for monitoring healing, assessing bone levels with X-rays, and ensuring the implant's stability.
- Smoking Cessation: If you smoke, it's vital to quit or significantly reduce smoking to support healing and prevent recurrence.
- Regular Maintenance: Lifelong commitment to professional cleanings (e.g., every 3-4 months) and diligent home care is essential to protect your implant.
Prevention
Prevention is paramount when it comes to implantitis. Adopting good habits and managing risk factors can significantly reduce your chances of developing this condition.
-
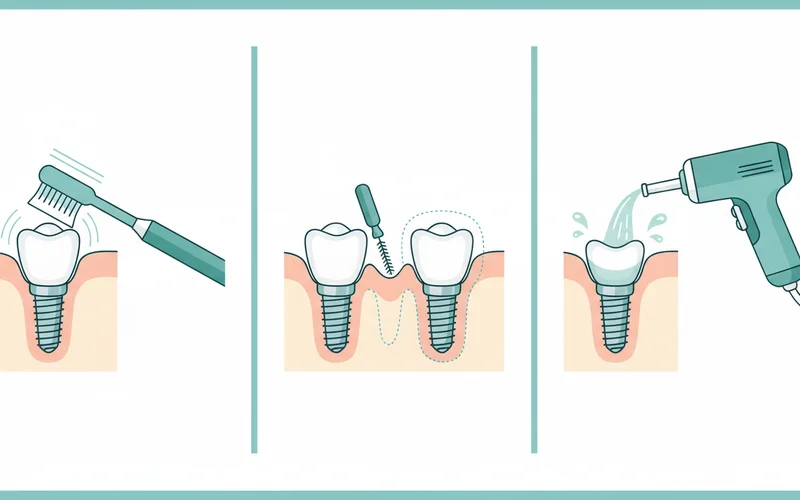
Meticulous Oral Hygiene:
- Brush Twice Daily: Use a soft-bristled toothbrush (manual or electric) and a non-abrasive toothpaste. Pay special attention to the areas around your implants, ensuring you clean the gum line thoroughly.
- Floss Daily: Use dental floss, interdental brushes, or specialized implant floss (e.g., super floss) to clean between implants and around the implant post.
- Water Flosser (Oral Irrigator): Many dentists recommend a water flosser for implant care, as it can effectively dislodge food particles and bacteria from around the implant and under the gum line, where traditional brushing and flossing might miss.
- Antimicrobial Mouthwash: Your dentist might recommend a non-alcohol antimicrobial mouthwash for daily use or specific periods.
-
Regular Dental Check-ups and Professional Cleanings:
- Schedule Regularly: Visit your dentist or periodontist every 3-6 months for professional cleanings and examinations. These appointments are crucial for removing plaque and calculus that home care can't reach and for early detection of any issues.
- Specialized Tools: Dental hygienists use specialized instruments designed for implants (e.g., plastic or titanium-tipped scalers) to prevent scratching the implant surface.
-
Quit Smoking: This is one of the most impactful preventive measures. Smoking dramatically increases the risk of implantitis and implant failure. Seek support to quit if you smoke.
-
Manage Systemic Diseases: If you have conditions like diabetes, ensure it is well-controlled. Work with your physician and dentist to manage any health issues that could compromise your oral health.
-
Address Occlusal Overload: If you grind or clench your teeth (bruxism), your dentist might recommend a nightguard to protect your implants and prevent excessive forces that could contribute to mechanical stress.
-
Avoid Excess Cement: When getting your implant crown, ensure your dentist uses proper techniques to prevent excess cement from seeping below the gum line. This is a common cause of inflammation.
-
Choose an Experienced Practitioner: While this isn't a direct preventive measure you take, selecting a highly skilled and experienced dental professional for implant placement and restoration can minimize surgical complications and ensure proper implant positioning and prosthetic design, which are foundational for long-term health.
Risks and Complications
While dental implants are highly successful, neglecting implantitis carries significant risks and complications:
- Implant Failure: The most severe complication. Untreated implantitis leads to irreversible and extensive bone loss, causing the implant to become loose and eventually fail, requiring removal.
- Loss of Surrounding Bone: Even if the implant doesn't completely fail, significant bone loss around it can compromise the stability of adjacent teeth or make future implant placement in that area more challenging.
- Pain and Discomfort: Chronic inflammation and infection can cause persistent pain, making chewing difficult and impacting your quality of life.
- Spread of Infection: In rare but serious cases, the infection can spread beyond the immediate implant site, potentially leading to cellulitis (skin infection), osteomyelitis (bone infection), or even systemic complications if left uncontrolled.
- Aesthetic Compromise: Bone and gum recession around an implant can expose the metallic implant or abutment, leading to an unsightly appearance, especially in the front of the mouth.
- Increased Treatment Complexity and Cost: Addressing advanced implantitis often requires complex surgical procedures, bone grafting, and potentially implant removal and replacement, which are far more expensive and time-consuming than early intervention.
- Impact on Overall Health: Chronic oral inflammation, including implantitis, has been linked to systemic health issues such as cardiovascular disease and worsened diabetes control.
Cost Breakdown: Implantitis Treatment in the US
As discussed, the costs associated with implantitis treatment can vary widely. Here's a further breakdown considering common scenarios and payment options.
Average US Costs (Low, Mid, High):
| Treatment Phase/Scenario | Low End ($) | Mid Range ($) | High End ($) | Notes |
|---|---|---|---|---|
| Initial Exam & X-rays | $100 | $250 | $400 | Often covered by insurance if for diagnostic purposes. |
| Peri-Implant Mucositis | ||||
| Non-Surgical Cleaning | $300 | $600 | $1,000 | Per implant. May require multiple sessions. |
| Local Antimicrobials | $50 | $150 | $250 | Per implant. Added to cleaning cost. |
| Early Implantitis | ||||
| Surgical Debridement | $800 | $1,500 | $2,500 | Per implant. Exposing and cleaning implant surface. |
| Advanced Implantitis | ||||
| Surgical Debridement + GBR | $2,000 | $3,500 | $5,000+ | Per implant. Includes bone graft material and membrane. |
| Implant Removal Only | $300 | $700 | $1,000 | If implant is failing and needs extraction. |
| Implant Removal + Site Prep | $1,000 | $2,500 | $4,000 | Removal + bone graft for future implant placement. |
| Full Failure & Replacement | ||||
| Total (Removal, Graft, New Implant, Crown) | $5,000 | $7,500 | $10,000+ | Per site. Represents the complete cost of starting over after failure. |
With vs. Without Insurance:
- Without Insurance: You will be responsible for 100% of the costs. This is why it's vital to discuss treatment plans and payment options upfront.
- With Insurance: As mentioned, coverage varies. Most plans will cover a percentage (e.g., 50-80%) of diagnostic and non-surgical treatments, subject to deductibles and annual maximums. Surgical procedures are often covered at a lower percentage (e.g., 20-50%) or may have specific exclusions for implant-related surgeries. If an implant needs to be replaced, the new implant body itself is frequently not covered. However, the crown or restoration on the new implant might be partially covered.
Payment Plans and Financing Options:
Many dental practices understand the financial burden of extensive dental work and offer solutions:
- In-Office Payment Plans: Some offices allow you to pay in installments directly.
- Third-Party Financing: Companies like CareCredit or LendingClub offer specialized healthcare credit cards with deferred interest or low-interest payment plans.
- Dental Discount Plans: These are not insurance but offer a percentage off services from participating dentists for an annual fee. They might be an option if you lack traditional insurance.
Cost-Saving Tips:
- Early Intervention: The single best cost-saving tip is to address implantitis at the earliest sign. Treating peri-implant mucositis is far less expensive and invasive than treating advanced implantitis or replacing a failed implant.
- Preventive Care: Diligent home care and regular check-ups prevent implantitis in the first place, saving you significant money in the long run.
- Shop Around (Carefully): While price shouldn't be the only factor, getting quotes from a few reputable periodontists or oral surgeons can help you compare costs for complex surgical procedures. Be wary of significantly "cheapest implants" offers, as compromised materials or less experienced practitioners could lead to future complications like implantitis, ultimately costing more.
- Maximize Insurance Benefits: Understand your plan's annual maximums and try to schedule treatment strategically across benefit years if possible.
- Discuss Options with Your Dentist: Your dentist can often present different treatment options with varying costs and help you prioritize.
Frequently Asked Questions
Is implantitis common?
While dental implants have a high success rate, implantitis is not uncommon. Studies show that peri-implant mucositis (the reversible precursor) affects up to 43% of implants, and implantitis itself (with bone loss) affects approximately 10-20% of implants or individuals with implants. The risk increases with certain factors like smoking and poor oral hygiene.
Can implantitis be cured?
Peri-implant mucositis is fully reversible with professional cleaning and improved oral hygiene. For implantitis, the goal is to arrest the progression of bone loss, eliminate infection, and stabilize the implant. While the lost bone may not always be fully regenerated, successful treatment can often save the implant and prevent further deterioration, effectively "curing" the active disease process.
How much does implantitis treatment cost?
Treatment costs vary widely depending on severity. Non-surgical treatment for peri-implant mucositis can range from $300 to $1,500 per implant. Surgical treatment for established implantitis, especially with bone grafting, can range from $1,500 to $5,000+ per implant. If the implant needs to be removed and replaced, the total cost can exceed $8,000.
What are the signs of implantitis?
Key signs include red, swollen, or bleeding gums around the implant, pus discharge, persistent bad taste, pain, and visible implant threads due to receding gums. In advanced stages, the implant may feel loose. Early detection is crucial, so any unusual symptoms warrant immediate dental attention.
Can implantitis spread?
Implantitis primarily affects the tissues immediately surrounding the dental implant. If left untreated, the infection and inflammation can spread further into the jawbone around that specific implant, leading to more extensive bone loss and potentially affecting adjacent teeth or implants. Rarely, severe, uncontrolled infections can lead to more widespread systemic issues, but this is uncommon.
Does ClearChoice prevent implantitis?
ClearChoice dental implants provide a full arch of teeth supported by multiple implants, often through an "All-on-4" or similar technique. While the quality of implants and surgical expertise at ClearChoice centers are generally high, they do not inherently prevent implantitis. Any dental implant, regardless of brand or provider, is susceptible to implantitis if proper oral hygiene is not maintained or if risk factors like smoking or uncontrolled diabetes are present. Long-term care and adherence to follow-up schedules are essential for preventing implantitis with any implant system.
Are there alternatives to dental implants if I'm worried about implantitis?
Yes, alternatives exist for replacing missing teeth. These include traditional dental bridges (which require altering adjacent natural teeth), removable partial dentures, or complete dentures. While these alternatives avoid the risk of implantitis, they come with their own considerations regarding stability, comfort, chewing efficiency, and bone preservation. It's best to discuss all options with your dentist to choose the best solution for your individual needs and budget, considering that the upfront cost of "cheapest implants" might not always be the lowest long-term cost if complications arise.
What's the recovery like after implantitis treatment?
Recovery depends on the treatment type. Non-surgical treatment has minimal downtime, usually just a few days of sensitivity. Surgical treatment involves more significant recovery, with a few days of discomfort, swelling, and dietary restrictions. Soft tissue healing typically takes 2-4 weeks, while bone grafting requires several months for full integration. Adhering to post-operative instructions is vital for successful healing.
How can I prevent implantitis?
Prevention relies on meticulous oral hygiene (brushing, flossing, interdental cleaners, water flosser), regular dental check-ups (every 3-6 months), quitting smoking, and effectively managing systemic health conditions like diabetes. Your dentist can provide specific guidance tailored to your needs.
What happens if implantitis is left untreated?
If implantitis is left untreated, the infection and inflammation will progressively destroy the bone supporting the implant. This will lead to increased implant mobility, persistent pain, pus discharge, and ultimately, the complete failure of the implant, necessitating its removal. Untreated implantitis can also compromise surrounding teeth and overall oral health.
When to See a Dentist
It's critical to be proactive when it comes to your dental implant health. Do not delay seeing a dentist if you experience any of the following:
Immediate Attention (Red Flags - See a dentist within 24-48 hours):
- Persistent Pain: Any pain or throbbing around your implant that doesn't subside within a day or two, especially during chewing.
- Pus Discharge: Seeing or tasting pus coming from around your implant is a clear sign of active infection and requires urgent evaluation.
- Implant Mobility: If your implant feels loose, wobbly, or you can visibly see it moving, this is a severe sign of advanced bone loss and requires immediate dental care to assess the situation and prevent further damage.
- Significant Swelling: Noticeable swelling around the implant that is painful, tender, or spreading.
Scheduled Appointment (Routine Care & Early Signs):
- Bleeding Gums: If your gums around the implant bleed easily when brushing, flossing, or during normal activity, it's an early sign of inflammation (peri-implant mucositis). While not an emergency, schedule an appointment soon.
- Red or Swollen Gums: Any persistent redness or puffiness of the gum tissue around the implant that lasts for more than a few days.
- Bad Taste or Breath: A persistent bad taste in your mouth or chronic bad breath originating from the implant area.
- Visible Implant Threads: If you start to see the metallic parts of your implant that were previously covered by gum tissue, it indicates gum and potentially bone recession.
- Any Discomfort or Changes: If something just "doesn't feel right" with your implant, even without severe symptoms, trust your instincts and get it checked.
Regular dental check-ups and cleanings, typically every 3-6 months, are your best defense against implantitis. Your dentist or periodontist can detect subtle changes before they become serious problems, often through clinical examination and routine X-rays. Don't wait for pain to be your guide – early intervention is always the most effective path to preserving your dental implants and your smile.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Implantologist: Complete Guide
Losing a tooth can be a significant setback, impacting not only your smile but also your ability to speak, chew, and maintain overall oral health. In fact, over 3 million Americans currently have dental implants, and that number is projected to grow significantly as more people seek a durable, n
March 8, 2026
Dentures Over Implants: Complete Guide
Missing multiple teeth or even an entire arch can profoundly impact your life, affecting everything from your ability to chew and speak to your self-confidence. For millions of Americans, traditional removable dentures have long been a solution, but they often come with compromises: slipping, discom
March 8, 2026
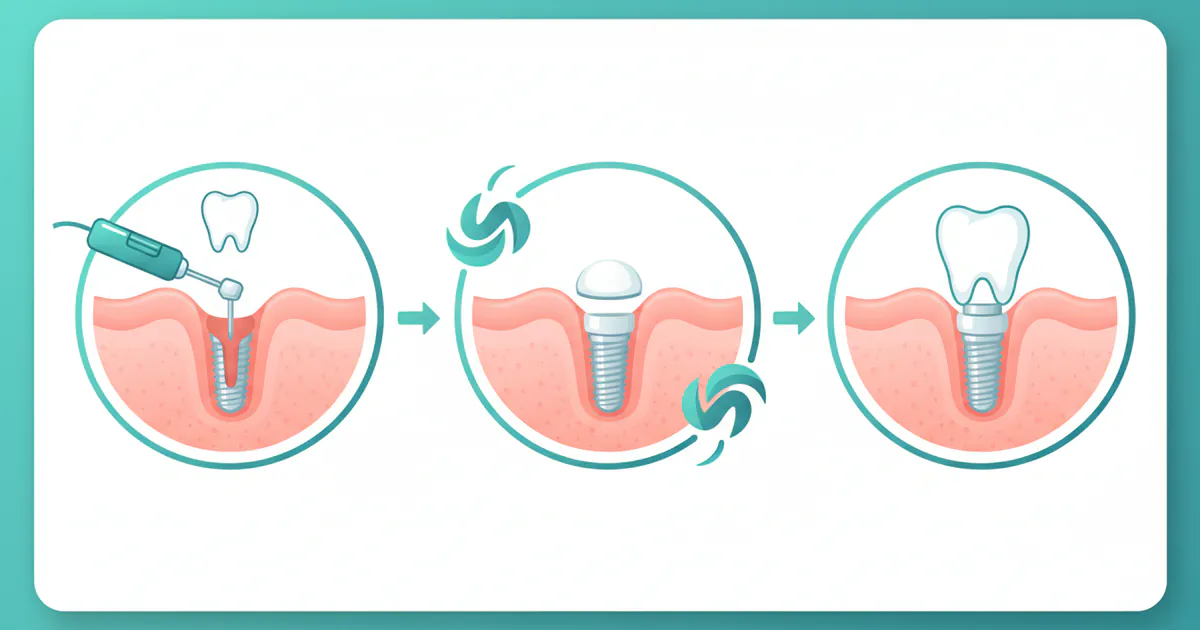
Implants Process: Complete Guide
Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the
March 8, 2026

Implants Dentaires: Complete Guide
Missing teeth can dramatically impact not just your smile, but your overall health, confidence, and quality of life. In the United States, an estimated 178 million adults are missing at least one tooth, while approximately 40 million are missing all their teeth. These statistics underscore a
March 8, 2026