Implantology: Complete Guide
Key Takeaways
- A missing tooth can significantly impact your daily life, affecting everything from your ability to chew and speak clearly to your confidence when you smile. In fact, an estimated 178 million Americans are missing at least one tooth, a number that underscores the widespread need for effective to
A missing tooth can significantly impact your daily life, affecting everything from your ability to chew and speak clearly to your confidence when you smile. In fact, an estimated 178 million Americans are missing at least one tooth, a number that underscores the widespread need for effective tooth replacement solutions. While traditional options like bridges and dentures have served many, the field of implantology has revolutionized restorative dentistry, offering a durable, natural-looking, and highly functional alternative. This comprehensive guide will explore the intricate world of mouth implants, detailing everything you need to know about these advanced dental solutions, from the initial consultation to long-term care. You'll gain a deep understanding of the various types of implants, the detailed implant procedure steps, associated costs, recovery expectations, and how dental implants can profoundly enhance your oral health and overall quality of life.
Key Takeaways:
- What they are: Dental implants are titanium posts surgically placed into the jawbone to replace tooth roots, supporting crowns, bridges, or dentures.
- Primary Benefit: Offer superior stability, aesthetics, and chewing function compared to traditional tooth replacements, closely mimicking natural teeth.
- Cost (US Averages): A single dental implant, crown, and abutment can range from $3,000 to $6,000+. Full-mouth solutions like All-on-4 can cost $20,000 to $50,000+ per arch.
- Timeline: The entire implant procedure, including healing (osseointegration), typically takes 3 to 9 months, though immediate load implants can reduce this.
- Success Rate: With proper care, dental implants boast a success rate of over 95%, lasting decades or even a lifetime.
- Insurance: Most dental insurance plans offer limited coverage for implants, often categorizing them as a major procedure, with many plans covering 0% to 50% of the cost after deductibles.
- Maintenance: Require diligent oral hygiene, including brushing, flossing, and regular dental check-ups, similar to natural teeth.
What It Is: An Overview of Dental Implantology
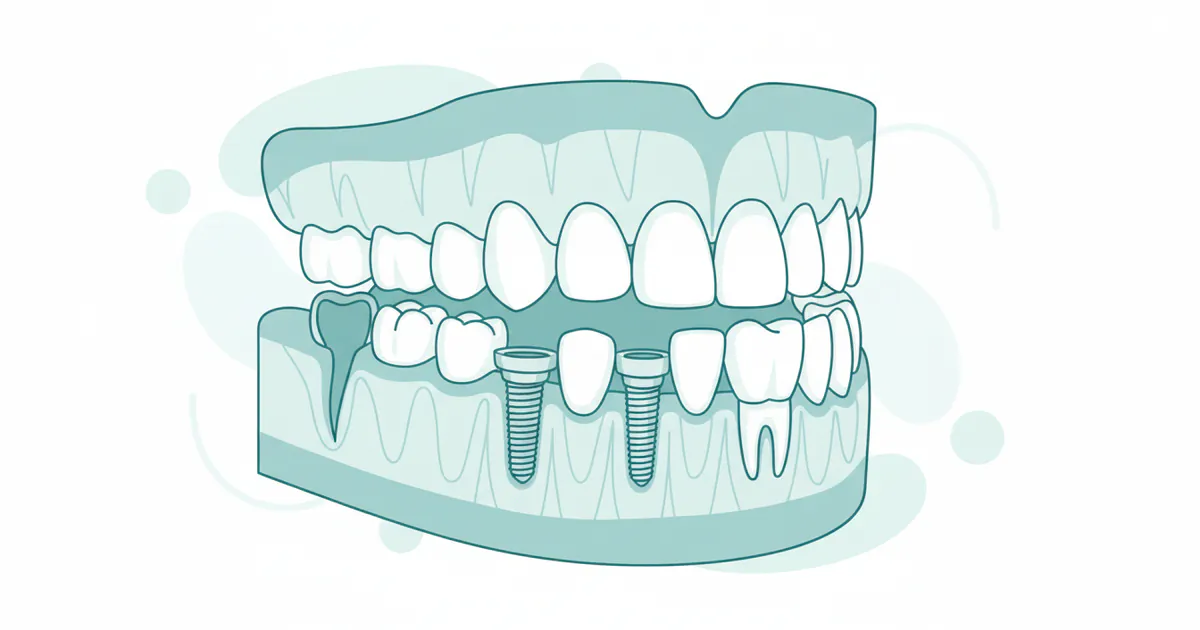
Dental implantology is the specialized branch of dentistry focused on surgically placing artificial tooth roots into the jawbone to support a dental prosthesis. These "mouth implants" provide a strong foundation for fixed (permanent) or removable replacement teeth that are designed to match your natural teeth. Unlike dentures that rest on the gums or bridges that rely on adjacent teeth for support, dental implants integrate directly with your bone, a process called osseointegration. This unique biological fusion creates an incredibly stable and durable base, preventing bone loss that often occurs when teeth are missing and preserving facial structure.
The core component of a dental implant is a small, screw-shaped post, most commonly made from titanium. Titanium is a biocompatible material, meaning it is well-tolerated by the human body and capable of fusing with bone without causing adverse reactions. The concept of using titanium for implants dates back to the 1950s when Swedish orthopedic surgeon Per-Ingvar Brånemark discovered titanium's ability to integrate with bone. Since then, the science and techniques of implantology have advanced dramatically, making dental implants the gold standard for tooth replacement.
When a tooth is lost, the underlying jawbone can begin to resorb or shrink due to lack of stimulation. This bone loss can lead to changes in facial appearance, difficulty chewing, and problems with speaking. Dental implants act as artificial tooth roots, stimulating the jawbone and helping to prevent this resorption, thereby preserving bone volume and maintaining facial integrity. They are a long-term solution designed to restore not just your smile, but also the full function and health of your oral cavity.
Types of Dental Implants and Variations
The field of implantology offers several types of dental implants and treatment approaches, each suited for different clinical situations and patient needs. Understanding these variations is crucial for making informed decisions with your dental professional.
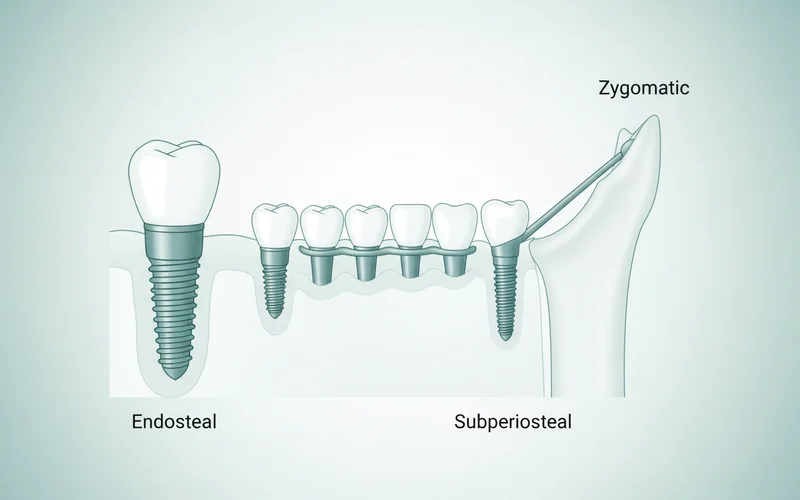
Endosteal Implants
Endosteal implants are the most common type of dental implant. They are typically made of titanium and are shaped like small screws, cylinders, or blades. "Endosteal" means "in the bone," referring to their placement directly into the jawbone. These are the implants most people envision when they hear the term "dental implant." They are suitable for most patients with healthy jawbone and are used for single tooth replacement, multiple teeth, or supporting full arches of teeth.
- Pros: High success rate, excellent long-term stability, versatile for various applications.
- Cons: Requires sufficient bone density, multi-stage procedure with healing time.
Subperiosteal Implants
Subperiosteal implants are less common today but may be an option for patients who cannot wear conventional dentures and have insufficient bone height for endosteal implants. These implants consist of a metal framework that is custom-made to fit on top of the jawbone, directly under the gum tissue. Posts attached to the framework protrude through the gums to support the prosthesis.
- Pros: May be suitable for patients with significant bone loss who cannot undergo bone grafting.
- Cons: Lower long-term success rate compared to endosteal implants, potential for gum irritation, less stable than endosteal.
Zygomatic Implants
Zygomatic implants are a specialized solution used for patients with severe bone loss in the upper jaw, where traditional implants or even extensive bone grafting are not feasible. These implants are much longer than conventional implants and are anchored into the zygoma (cheekbone) rather than the maxilla (upper jawbone). Due to the complexity, this procedure is typically performed by highly experienced oral surgeons.
- Pros: Provides a solution for extreme upper jaw bone loss, often avoids extensive bone grafting procedures.
- Cons: Highly specialized and complex surgery, longer healing time, higher cost.
Mini Dental Implants (MDIs)
Mini dental implants (MDIs) are similar to traditional endosteal implants but are much smaller in diameter (typically less than 3mm). They are primarily used to stabilize lower dentures, preventing them from shifting or rocking. In some cases, they can be used for small, single-tooth replacements, particularly in areas of limited space or for temporary solutions.
- Pros: Less invasive placement, often quicker procedure, lower cost, can be used when bone volume is limited, immediate loading sometimes possible.
- Cons: Less durable than traditional implants, not suitable for all situations, generally lower long-term success for permanent tooth replacement.
All-on-4® Dental Implants and Other Full-Arch Solutions
The All-on-4® technique is a popular and revolutionary solution for replacing a full arch of missing teeth (upper, lower, or both). Instead of placing an implant for every missing tooth, a full arch prosthesis is supported by just four strategically placed dental implants. Two implants are placed vertically in the anterior jaw, and two are tilted at an angle in the posterior jaw to maximize contact with available bone and avoid anatomical structures like the sinus cavities. Similar approaches exist, like All-on-6 or even All-on-X, which use more implants for increased stability, depending on the patient's bone density and desired outcome.
- Pros: Can provide a full set of fixed, non-removable teeth in a shorter timeframe (often with a temporary prosthesis placed the same day), reduces the need for bone grafting, restores chewing function and aesthetics dramatically.
- Cons: Significant initial investment, requires careful planning and surgical expertise, can be more complex than single implant placement.
Immediate Load Dental Implants ("Teeth in a Day")
In certain circumstances, a dental crown or prosthesis can be placed on the implant immediately after the implant surgery, often referred to as "Teeth in a Day." This is usually possible when there is sufficient bone density and stability for the implant to withstand initial chewing forces without compromising osseointegration. While appealing for its speed, not all patients are candidates for this technique.
- Pros: Immediate aesthetic and functional improvement, fewer appointments.
- Cons: Higher risk of implant failure if not properly selected and managed, requires ideal bone conditions.
Why Dental Implants Are Needed: Causes of Tooth Loss
Dental implants are a reconstructive treatment, meaning they are used to replace something that is missing—in this case, teeth. The reasons people lose teeth are varied, but typically fall into a few key categories:
Severe Tooth Decay
Uncontrolled dental caries (cavities) that progress deep into the tooth's pulp can lead to irreversible damage and infection. If the tooth structure is too compromised to be restored with a filling, crown, or root canal therapy, extraction becomes necessary. This is a common reason for single tooth loss.
Advanced Periodontal (Gum) Disease
Periodontal disease is a progressive infection of the gums and the bone supporting the teeth. If left untreated, the inflammation and infection can destroy the bone and ligaments that hold teeth in place, eventually leading to tooth mobility and loss. Periodontal disease is the leading cause of tooth loss in adults. Patients with a history of gum disease require careful management before and after implant placement to ensure the long-term success of their mouth implants.
Dental Trauma and Injuries
Accidents, falls, sports injuries, or other forms of trauma can cause teeth to be fractured beyond repair or completely knocked out (avulsed). In such cases, dental implants can often provide an excellent replacement, restoring both function and aesthetics.
Congenital Tooth Absence (Hypodontia/Anodontia)
Some individuals are born with missing teeth due to genetic factors (a condition known as hypodontia or anodontia). Dental implants can be a lifelong solution for these individuals once their jawbone development is complete.
Failed Root Canals or Previous Restorations
Even with modern dentistry, root canal treatments or other restorations can sometimes fail over time, leading to reinfection or structural compromise. If a previously treated tooth becomes unsalvageable, extraction and subsequent implant placement may be recommended.
Extensive Wear and Tear
Severe bruxism (teeth grinding) or prolonged acid erosion can wear down tooth structure significantly over many years, potentially to the point where teeth become too short, fractured, or painful to save, necessitating extraction.
When Dental Implants Are Indicated: Signs and Symptoms of Tooth Loss Impact
While "signs and symptoms" typically refer to illnesses, in the context of implantology, this section focuses on the issues that arise from missing teeth and signal that dental implants might be the right solution for you.
- Gaps in Your Smile: The most obvious sign is a visible gap where a tooth once was. Beyond aesthetics, these gaps can affect speech and cause adjacent teeth to shift.
- Difficulty Chewing: Missing teeth, especially molars, can severely impair your ability to chew food properly, leading to dietary limitations and digestive issues.
- Speech Impediments: Missing front teeth can affect the way you form certain sounds, leading to lisping or other speech difficulties.
- Shifting Teeth: When a tooth is lost, the neighboring teeth can drift into the empty space, altering your bite and potentially creating new gaps or crowding. The opposing tooth can also super-erupt (grow longer) into the empty space.
- Jawbone Deterioration (Resorption): This is a critical, often invisible, consequence of missing teeth. Without the stimulation from a tooth root, the jawbone in that area begins to shrink, which can change facial contours and make future tooth replacement more challenging.
- Facial Sagging or Sunken Appearance: Over time, extensive bone loss due to multiple missing teeth can lead to a sunken facial appearance, making you look older. This is particularly noticeable in individuals who have worn traditional dentures for many years.
- Discomfort or Instability with Dentures: If you currently wear removable dentures and experience pain, looseness, or difficulty eating certain foods, dental implants can offer a stable foundation for improved comfort and function.
- Chronic Headaches or TMJ Pain: A misaligned bite due to missing teeth can sometimes contribute to temporomandibular joint (TMJ) disorders, leading to headaches, jaw pain, and difficulty opening and closing your mouth.
If you experience any of these issues, it's crucial to consult with a dental professional to assess your oral health and determine if dental implants are a suitable treatment option for you.
Treatment Options for Missing Teeth: Implants vs. Alternatives
When faced with missing teeth, patients have several treatment pathways. Dental implants offer distinct advantages but also come with unique considerations. Here's a comparison of common tooth replacement options:
Dental Implants (Fixed, Permanent)
Description: Titanium posts surgically placed into the jawbone, acting as artificial tooth roots. They support individual crowns, multi-tooth bridges, or full-arch prostheses.
- Pros:
- Bone Preservation: Prevents jawbone loss, maintaining facial structure.
- Stability & Comfort: Feel and function like natural teeth; no slipping or clicking.
- Durability: Can last decades or a lifetime with proper care.
- Independent: Do not require altering adjacent healthy teeth.
- Aesthetics: Look highly natural.
- Cons:
- Cost: Highest initial investment among options.
- Time: Multi-stage procedure requiring healing time (several months).
- Surgery: Involves surgical procedures.
- Bone Requirement: Requires adequate jawbone density (though grafting can address deficiencies).
Fixed Dental Bridges (Fixed, Permanent)
Description: Consist of one or more artificial teeth (pontics) held in place by dental crowns cemented onto the natural teeth adjacent to the gap.
- Pros:
- Fixed Solution: Non-removable, feels relatively stable.
- Faster Treatment: Generally completed in a few weeks.
- Lower Cost: Less expensive than dental implants initially.
- Cons:
- Tooth Alteration: Requires shaping (grinding down) healthy adjacent teeth to support crowns.
- Bone Loss: Does not prevent jawbone deterioration under the missing tooth.
- Durability: Typically lasts 10-15 years; may need replacement.
- Hygiene Challenges: Can be difficult to clean effectively under the pontic.
Removable Partial or Complete Dentures (Removable)
Description: Artificial teeth set in a plastic base that mimics gum tissue. Partial dentures replace a few missing teeth, while complete dentures replace an entire arch. They are held in place by suction, clasps, or dental adhesives.
- Pros:
- Cost-Effective: Lowest initial cost.
- Non-Invasive: No surgery required.
- Quick Solution: Can be fabricated relatively quickly.
- Cons:
- Instability: Can slip, click, or cause sore spots.
- Chewing Limitations: Reduced chewing efficiency (typically 10-20% of natural teeth).
- Bone Loss: Accelerates jawbone resorption over time.
- Maintenance: Requires daily removal for cleaning, can be inconvenient.
- Speech & Comfort: Can affect speech and comfort, especially initially.
Pro Tip: While dentures and bridges offer quicker, less expensive initial solutions, dental implants are widely considered the superior long-term investment due to their ability to preserve bone, offer unparalleled stability, and provide the most natural feel and function. The American Dental Association (ADA) often recommends implants as the preferred option for suitable candidates due to their long-term health benefits.
Step-by-Step Implant Procedure
The journey to restoring your smile with dental implants involves several carefully planned stages. While the specific implant procedure steps can vary based on individual needs and the type of implant, the general process is as follows:
Step 1: Initial Consultation and Comprehensive Evaluation
This crucial first step involves a thorough examination by a qualified dental professional, typically an oral surgeon, periodontist, or general dentist with extensive implant training.
- Medical History Review: Discussion of your overall health, medications, and any pre-existing conditions (e.g., diabetes, heart disease) that might affect healing or surgery.
- Oral Examination: Assessment of your teeth, gums, and existing bone structure.
- Imaging: 3D Cone Beam Computed Tomography (CBCT) scans are often taken to provide detailed views of your jawbone, nerve pathways, sinus cavities, and surrounding anatomy. This allows for precise surgical planning and avoids potential complications.
- Treatment Planning: Based on the evaluation, your dentist will create a personalized treatment plan, discussing the number of implants needed, type of restoration, timeline, and associated costs. They will also address any need for pre-implant procedures like extractions or bone grafting.
Step 2: Pre-Implant Procedures (if necessary)
Some patients require preparatory procedures before implant placement to ensure the long-term success of the implant.
- Tooth Extraction: If the damaged tooth is still present, it will need to be surgically removed.
- Bone Grafting: If the jawbone is insufficient in quality or quantity (common after prolonged tooth loss), a bone graft may be necessary. This involves adding bone material (from your own body, a donor, or synthetic sources) to augment the jawbone. This typically requires several months of healing (3-9 months) before implant placement can proceed.
- Sinus Lift: If implants are needed in the upper jaw and the sinus cavity is too close to the jawbone due to bone loss, a sinus lift procedure may be performed. This involves gently lifting the sinus membrane and placing bone graft material to create sufficient bone height. This also requires a healing period.
Step 3: Dental Implant Placement Surgery
This is the surgical phase where the titanium implant post is placed into your jawbone.
- Anesthesia: Local anesthesia is typically used to numb the area, but sedation options (oral, IV, or nitrous oxide) are available for patient comfort.
- Incision: A small incision is made in the gum tissue to expose the underlying bone.
- Pilot Hole: A small pilot hole is carefully drilled into the jawbone using specialized instruments.
- Implant Insertion: The titanium implant screw is then gently threaded or tapped into the prepared bone socket.
- Sutures: The gum tissue is closed over the implant with sutures, or a healing cap may be placed to expose the top of the implant (depending on the chosen technique).
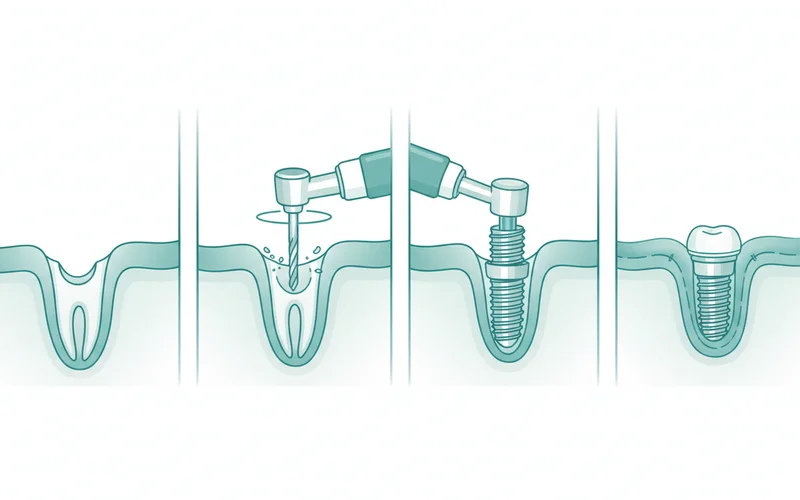
Step 4: Osseointegration (Healing Period)
This is perhaps the most critical phase, where the implant fuses with your jawbone.
- Duration: This process, called osseointegration, typically takes 3 to 6 months, though it can be longer in some cases, especially after bone grafting. During this time, the implant is not loaded with chewing forces.
- Temporary Solutions: Your dentist may provide a temporary crown, bridge, or denture to cover the gap during the healing period, ensuring aesthetics and some function without disturbing the implant.
- Monitoring: Regular follow-up appointments may be scheduled to monitor the healing progress.
Step 5: Abutment Placement
Once osseointegration is complete, and the implant is stable, an abutment is placed.
- Minor Surgery (if needed): If the implant was fully covered by gum tissue in Step 3, a small incision might be needed to expose the top of the implant.
- Abutment Attachment: The abutment, a small connector post, is attached to the implant. This post will protrude above the gum line and serve as the anchor for your new crown, bridge, or denture.
- Gum Healing: The gum tissue around the abutment is allowed to heal for a few weeks, creating a natural-looking collar around the final restoration.
Step 6: Fabrication and Placement of the Restoration
This is the final stage where your new artificial tooth or teeth are created and attached.
- Impressions: Digital scans or traditional impressions of your mouth, implants, and surrounding teeth are taken.
- Shade Matching: The shade of your natural teeth is carefully matched to ensure the new restoration blends seamlessly.
- Lab Fabrication: A dental laboratory uses these impressions to custom-fabricate your crown, bridge, or full-arch prosthesis.
- Final Placement: Once the restoration is ready, your dentist will attach it to the abutment, either cemented or screwed into place. The fit, bite, and aesthetics are meticulously checked and adjusted as needed.
Cost and Insurance for Dental Implants
Understanding the financial aspect of dental implants is crucial. The cost of mouth implants can vary significantly based on several factors, including the number of implants, the type of restoration, the need for preparatory procedures, the dental professional's fees, and geographic location within the US.
Average US Costs (Per Single Implant System)
A "single implant system" generally includes the implant post, the abutment (connector), and the crown.
- Implant Post (Surgery): Generally ranges from $1,500 to $3,000.
- Abutment: Typically costs $300 to $800.
- Crown (Prosthetic tooth): Can range from $1,000 to $2,500.
- Total for a single implant with crown: Averages $3,000 to $6,000 or more.
Additional Costs to Consider:
- Initial Consultation & Diagnostics: $100 - $500 (may include X-rays, CBCT scans).
- Tooth Extraction: $75 - $650 per tooth (depending on complexity).
- Bone Grafting: $200 - $3,000+ per site (depending on material and extent).
- Sinus Lift: $1,500 - $3,500+ per sinus.
- Temporary Restoration: $300 - $1,000+ (if needed during healing).
- Sedation: $200 - $1,000+ per procedure (depending on type and duration).
Full Arch Solutions (e.g., All-on-4)
These comprehensive solutions replace an entire arch of teeth.
- All-on-4 (per arch): Ranges from $15,000 to $30,000+ for a removable overdenture, and $20,000 to $50,000+ for a fixed hybrid prosthesis. These costs typically include extractions, implant placement, and the provisional and final prostheses.
Geographic Variations
Costs can differ significantly by region in the United States. Major metropolitan areas and coastal regions generally have higher fees than rural areas or states with lower costs of living. For instance, an implant in New York City or Los Angeles might be at the higher end of the range compared to one in a smaller city in the Midwest.
Dental Insurance Coverage
This is often a complex area for patients.
- Limited Coverage: Many dental insurance plans offer limited, if any, coverage for dental implants. Historically, implants were considered cosmetic or experimental, though this perception is changing.
- Major Procedure Category: If covered, implants are typically categorized as a "major procedure," meaning your plan might cover 0% to 50% of the cost after your annual deductible is met. Most plans have an annual maximum benefit, often ranging from $1,000 to $2,000, which may only cover a small portion of the total implant cost.
- Medical Insurance: In some specific cases, if tooth loss is due to a medical condition or accident, portions of the procedure (like initial exams, extractions, or bone grafting) might be covered by your medical insurance. It's essential to check with both your dental and medical insurance providers.
- Pre-Authorization: Always request a pre-authorization or pre-determination from your insurance company before starting treatment. This provides a clear estimate of what your plan will cover.
Payment Plans and Financing Options
Due to the significant investment, many dental practices offer or partner with third-party financing options.
- In-Office Payment Plans: Some practices allow patients to make payments over time.
- Healthcare Credit Cards: Services like CareCredit or LendingClub offer specialized credit lines for healthcare expenses, often with deferred interest or low-interest plans for qualified applicants.
- Personal Loans: Banks and credit unions offer personal loans that can be used for dental expenses.
- Dental Schools: University dental schools often provide services at a reduced cost, as procedures are performed by students under the close supervision of experienced faculty. This can be a more affordable option, though it may involve longer appointment times.
Pro Tip: Don't let the upfront cost deter you. Discuss all financing options with your dental office's financial coordinator. The long-term benefits of implants often outweigh the initial investment compared to recurring costs and compromises of alternative treatments.
Recovery and Aftercare for Dental Implants
Proper recovery and diligent aftercare are essential for the successful integration of your dental implants and their long-term health. Following your dentist's instructions carefully will minimize complications and ensure a smooth healing process.
Immediate Post-Operative Care (First 24-72 Hours)
- Bleeding: Some light bleeding or oozing is normal. Apply gentle pressure with a clean gauze pad for 30-60 minutes, changing as needed. Avoid vigorous rinsing or spitting.
- Swelling: Swelling is common. Apply an ice pack to the outside of your face, 20 minutes on, 20 minutes off, for the first 24-48 hours. Keep your head elevated, even when sleeping, to reduce swelling.
- Pain Management: Take prescribed pain medication as directed. Over-the-counter pain relievers (like ibuprofen or acetaminophen) can help with mild discomfort.
- Diet: Stick to soft foods for the first few days (e.g., yogurt, soup, mashed potatoes, scrambled eggs). Avoid hot liquids, spicy foods, crunchy items, and using a straw (which can dislodge blood clots).
- Oral Hygiene: Do not brush or rinse the surgical site for the first 24 hours. After 24 hours, gently rinse with a prescribed antiseptic mouthwash (like chlorhexidine) or warm salt water (1/2 teaspoon salt in 8 ounces warm water) 2-3 times a day. Brush other teeth carefully, avoiding the surgical area.
- Activity: Rest and avoid strenuous activity for 48-72 hours.
- Smoking: Absolutely avoid smoking as it significantly impairs healing and can lead to implant failure.
During the Osseointegration Period (3-6 Months)
- Diet: Gradually reintroduce harder foods, but avoid chewing directly on the implant site until your dentist clears it.
- Oral Hygiene: Maintain excellent oral hygiene. Brush twice a day with a soft-bristled toothbrush and floss daily. If you have a temporary restoration, clean around it meticulously.
- Follow-Up Appointments: Attend all scheduled follow-up appointments with your dentist to monitor the healing and osseointegration process.
- Avoid Pressure: Do not put any undue pressure on the implant site. If you have a removable temporary denture, your dentist might need to adjust it to ensure it doesn't press on the healing implant.
Long-Term Care and Maintenance (After Restoration Placement)
Once your permanent crown, bridge, or denture is placed, dental implants require maintenance similar to natural teeth, but with some specific considerations.
- Excellent Oral Hygiene:
- Brushing: Brush twice daily with a soft-bristled toothbrush. Consider an electric toothbrush for more effective cleaning.
- Flossing: Floss daily. Special implant-specific floss, interdental brushes, or water flossers (Waterpik) can be particularly effective for cleaning around implants and abutments.
- Mouthwash: Use an antimicrobial mouthwash as recommended by your dentist.
- Regular Dental Check-ups: Visit your dentist for professional cleanings and examinations at least twice a year, or more frequently if recommended. Your hygienist will use specialized tools designed for cleaning around implants to prevent damage.
- Avoid Harmful Habits:
- Smoking: Continues to be a major risk factor for peri-implantitis (gum disease around implants) and implant failure. Quitting is highly recommended.
- Bruxism (Teeth Grinding): If you grind or clench your teeth, your dentist may recommend a nightguard to protect your implants and natural teeth from excessive force.
- Hard Foods: While implants are strong, avoid chewing on extremely hard items like ice, hard candies, or non-food objects, which can damage the restoration or, in rare cases, the implant itself.
Pro Tip: Peri-implantitis, an inflammatory condition affecting the tissues around dental implants, is the most common long-term complication. It's similar to periodontal disease and can lead to bone loss around the implant. Early detection and treatment through regular dental visits and meticulous home care are key to prevention.
Prevention of Tooth Loss and Implant Complications
Prevention encompasses two aspects in implantology: preventing the tooth loss that necessitates implants in the first place, and preventing complications once implants are placed.
Preventing Tooth Loss
The best implant is the one you never need because you kept your natural tooth.
- Maintain Excellent Oral Hygiene: Brush your teeth at least twice a day for two minutes with fluoride toothpaste and floss daily. This is the cornerstone of preventing cavities and gum disease, the primary causes of tooth loss.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months for professional cleanings and examinations. Early detection of cavities, gum disease, or other issues allows for timely intervention before they become severe.
- Balanced Diet: Limit sugary and acidic foods and drinks, which contribute to tooth decay. Incorporate calcium-rich foods for strong bones, including your jawbone.
- Protect Your Teeth:
- Sports Guards: Wear a mouthguard during sports or any activity with a risk of facial impact.
- Nightguards: If you clench or grind your teeth (bruxism), wear a custom-fitted nightguard to protect your teeth from excessive wear and potential fractures.
- Avoid Tobacco Products: Smoking and smokeless tobacco significantly increase the risk of gum disease and oral cancers, both of which can lead to tooth loss.
- Address Dental Problems Promptly: Don't ignore tooth pain, sensitivity, or bleeding gums. Seek dental care immediately to prevent minor issues from escalating.
Preventing Implant Complications
Once you have received dental implants, specific measures can prevent issues.
- Adhere to Aftercare Instructions: Follow all post-operative instructions meticulously, especially regarding diet, oral hygiene, and activity restrictions during the initial healing phase.
- Commit to Lifelong Oral Hygiene: As detailed in the "Recovery and Aftercare" section, maintaining impeccable brushing, flossing, and potentially water flossing routines is critical for preventing peri-implantitis.
- Regular Dental Implant Maintenance: Schedule regular check-ups with a dentist or periodontist experienced in implant care. They can monitor the health of your implants, detect early signs of inflammation, and perform specialized cleanings.
- Avoid Smoking: Smoking is the most significant preventable risk factor for implant failure and peri-implantitis. Quitting dramatically improves the longevity of your implants.
- Manage Systemic Health Conditions: Conditions like uncontrolled diabetes can increase the risk of infection and impair healing, potentially affecting implant success. Work with your physician to manage any underlying health issues.
- Wear a Nightguard (if recommended): If you are a clencher or grinder, a custom nightguard protects your implants and restorations from excessive force, which could lead to complications like screw loosening or fracture.
Risks and Complications of Dental Implants
While dental implant procedures have a very high success rate (over 95%), like any surgical procedure, there are potential risks and complications. Being aware of these helps you make an informed decision and enables early detection if an issue arises.
General Surgical Risks
- Infection: Though uncommon due to sterile surgical techniques and antibiotics, infection at the implant site can occur. Symptoms include pain, swelling, redness, and pus.
- Bleeding: Some bleeding is normal, but excessive or prolonged bleeding can be a complication.
- Pain and Swelling: Expected post-surgery, but severe or persistent pain/swelling can indicate a problem.
- Bruising: Common around the surgical site.
- Numbness (Paresthesia): Rare, but nerve damage (e.g., to the inferior alveolar nerve in the lower jaw) can cause temporary or, in very rare cases, permanent numbness, tingling, or pain in the lip, chin, gums, or tongue. Careful pre-surgical planning with CBCT scans significantly reduces this risk.
Implant-Specific Complications
- Implant Failure (Lack of Osseointegration): The most significant complication is when the implant fails to fuse with the jawbone. This can happen due to poor bone quality, infection, excessive force on the implant during healing, or certain medical conditions.
- Symptoms: Implant mobility, persistent pain, swelling, and sometimes the implant simply doesn't integrate.
- Treatment: The failed implant usually needs to be removed, the site allowed to heal, and potentially re-grafted before another implant can be attempted.
- Peri-Implantitis: An inflammatory disease affecting the soft and hard tissues surrounding a dental implant, similar to periodontal disease around natural teeth. It's often caused by bacterial infection and can lead to progressive bone loss around the implant.
- Symptoms: Red, swollen, or bleeding gums around the implant, pus, pain, and eventually implant mobility.
- Treatment: Early stages can be managed with professional cleaning and antibiotics. Advanced cases may require surgical intervention to decontaminate the implant surface and regenerate bone. Untreated peri-implantitis can lead to implant failure.
- Sinus Perforation/Communication: During upper jaw implant placement, if the sinus membrane is very thin, it can be punctured, creating a communication between the mouth and the sinus cavity. A sinus lift procedure is often performed to prevent this.
- Symptoms: Nasal congestion, pain, or fluid leakage.
- Treatment: Small perforations often heal on their own; larger ones may require surgical repair.
- Damage to Adjacent Structures: Though rare with proper planning, implants can potentially damage nearby teeth, blood vessels, or bone.
- Prosthetic Complications: Issues related to the crown, bridge, or denture attached to the implant.
- Screw Loosening/Fracture: The small screws connecting the crown to the abutment or the abutment to the implant can loosen or, rarely, fracture.
- Crown/Abutment Fracture: The ceramic or porcelain material of the crown can chip or break.
- Poor Fit: A poorly fitting restoration can cause discomfort or lead to peri-implantitis.
Pro Tip: Choosing a highly qualified and experienced dental implant surgeon (e.g., an oral and maxillofacial surgeon or periodontist) who utilizes 3D imaging (CBCT) for precise planning is the most effective way to minimize these risks. Follow all post-operative instructions diligently and report any unusual symptoms to your dentist immediately.
Comparison Tables
Table 1: Comparison of Tooth Replacement Options
| Feature | Dental Implants | Fixed Dental Bridges | Removable Dentures |
|---|---|---|---|
| Anchoring | Surgically placed into jawbone | Anchored to adjacent natural teeth | Rests on gums, sometimes with clasps/adhesives |
| Bone Preservation | Yes, stimulates bone, prevents loss | No, bone loss continues under gap | No, accelerates bone loss |
| Stability | Excellent, feels like natural tooth | Good, but can put stress on anchor teeth | Variable (can slip, click) |
| Durability | Very Long-Term (Decades/Lifetime) | 10-15 years | 5-7 years (often needs relining/replacement) |
| Adjacent Teeth | Does not affect adjacent healthy teeth | Requires grinding down adjacent teeth | May put stress on adjacent teeth with clasps |
| Chewing Power | ~90% - 100% of natural teeth | ~60% - 70% of natural teeth | ~10% - 20% of natural teeth |
| Cost (Single) | $3,000 - $6,000+ (Implant, abutment, crown) | $2,000 - $5,000 (per bridge, 3 units) | $300 - $2,500 (partial); $1,000 - $3,000 (full) |
| Treatment Time | 3-9 months (including healing) | 2-4 weeks | 2-6 weeks |
| Maintenance | Regular brushing, flossing, dental check-ups | Careful cleaning under pontic, check-ups | Daily removal, cleaning, adhesives |
| Aesthetics | Excellent, very natural | Good, but can sometimes show margins | Variable, can look less natural |
Table 2: Estimated Cost Ranges for Common Implant Procedures in the US
| Procedure / System | Average Low-End Cost | Average High-End Cost | Notes |
|---|---|---|---|
| Single Implant (Post Only) | $1,500 | $3,000 | Does not include abutment or crown. |
| Single Implant (Full System) | $3,000 | $6,000+ | Includes post, abutment, and standard crown. |
| Mini Dental Implants (MDI) | $500 | $1,500 | Per implant, often used for denture stabilization (2-4 implants). |
| Bone Grafting (Minor) | $200 | $800 | Small site, simple material. |
| Bone Grafting (Major) | $1,000 | $3,000+ | Larger sites, more complex materials/techniques. |
| Sinus Lift (per sinus) | $1,500 | $3,500+ | Performed when upper jawbone is insufficient for implants. |
| All-on-4® (per arch, fixed) | $20,000 | $50,000+ | Includes 4 implants, extractions, temporary & final prosthesis. |
| All-on-4® (per arch, removable) | $15,000 | $30,000+ | Removable overdenture supported by 4 implants. |
| Full Mouth Implants (multiple single) | $30,000 | $80,000+ | Multiple individual implants supporting crowns/bridges. |
Note: These are average ranges and can vary based on location, dentist's experience, materials used, and specific patient needs.
Children / Pediatric Considerations for Dental Implants
Dental implants are generally not recommended for children or adolescents whose jawbones are still developing. The reason is that the jawbone undergoes significant growth and change during childhood and adolescence. Placing an implant in a growing jaw can lead to the implant becoming submerged or positioned incorrectly as the surrounding bone and teeth continue to develop. This can result in aesthetic issues, bite problems, and potential damage to the implant or surrounding structures.
When are Implants Considered for Younger Patients?
- Completion of Jaw Growth: The primary consideration is the cessation of jaw growth. This typically occurs around 16-18 years of age for females and 18-20 years of age for males, though it can vary for individuals. A dental professional will use X-rays and growth assessments to determine if the jaw has fully matured.
- Congenital Tooth Absence: For adolescents born with congenitally missing teeth (e.g., missing lateral incisors), implants may be considered after skeletal maturity.
- Traumatic Tooth Loss: In cases of severe trauma resulting in tooth loss, temporary tooth replacement options (like space maintainers or removable partial dentures) are used until the patient reaches an age where implants can be safely placed.
- Orthodontic Considerations: Sometimes, implants can be used as temporary anchors in orthodontics even in younger patients, but these are typically temporary mini-implants that are later removed, not permanent tooth replacements.
Alternatives for Children and Adolescents
Until a child's jaw is fully developed, other solutions for missing teeth include:
- Space Maintainers: To hold the space open for future tooth eruption or implant placement.
- Removable Partial Dentures ("Flippers"): A temporary, removable appliance that fills the gap and restores aesthetics.
- Orthodontic Treatment: To close spaces or prepare the jaw for future restorative options.
- Resin-Bonded Bridges: A less invasive bridge option that can be used temporarily without heavily preparing adjacent teeth.
Pro Tip: If your child loses a permanent tooth prematurely, consult with a pediatric dentist or orthodontist immediately. They can guide you on the best interim solutions to preserve space and prepare for definitive treatment once your child is older.
Cost Breakdown: Detailed US Averages and Financing
Delving deeper into the financial aspects, the investment in dental implants is significant but often provides unparalleled long-term value.
Average US Costs – A Closer Look
As discussed, costs vary, but here's a breakdown of what you might expect for common implant scenarios:
-
Single Tooth Implant:
- Low: $3,000 (e.g., general dentist, basic materials, no pre-procedures)
- Mid: $4,500 - $5,500 (e.g., experienced specialist, quality materials, minor preparatory work included)
- High: $6,000 - $8,000+ (e.g., complex case, extensive bone grafting, highly specialized surgeon, premium materials, high-cost-of-living area)
- What's included: Implant post, abutment, custom crown, surgical placement, follow-up visits.
-
Multiple Implants (e.g., 2-3 implants supporting a bridge):
- Costs will be per implant, plus the cost of the bridge. For example, two implants supporting a three-unit bridge might be in the range of $7,000 - $15,000+.
-
Full Arch (All-on-4 Fixed Hybrid):
- Low: $20,000 per arch (e.g., specific clinics offering package deals, potentially more basic materials)
- Mid: $30,000 - $40,000 per arch (e.g., experienced team, quality materials, comprehensive service)
- High: $45,000 - $50,000+ per arch (e.g., highly complex cases, custom milling, premium aesthetic results, advanced surgical techniques)
- What's included: Typically includes all extractions, 4-6 implants, provisional (temporary) prosthesis, final fixed hybrid prosthesis, and follow-up care for a period.
With vs. Without Insurance
- Without Insurance: You will be responsible for the full cost of the treatment. Many practices offer discounts for upfront payment or provide access to financing options.
- With Insurance: As noted, most dental insurance plans offer limited coverage.
- If your plan covers 50% of "major procedures" up to a $1,500 annual maximum, and a single implant costs $4,000:
- Your deductible (e.g., $50) would first apply.
- Then, 50% of the remaining cost (e.g., $1,975) would be covered, but only up to your annual maximum ($1,500).
- So, your insurance would pay $1,500, and you would owe $2,500 + deductible.
- It's important to understand your specific plan's limitations, deductibles, annual maximums, and waiting periods for major procedures.
- If your plan covers 50% of "major procedures" up to a $1,500 annual maximum, and a single implant costs $4,000:
Payment Plans and Financing Options
- Dental Practice Payment Plans: Many dental offices understand the financial commitment and offer flexible in-house payment options, allowing you to pay in installments.
- Third-Party Medical Financing: Companies like CareCredit, LendingClub Patient Solutions, and Alphaeon Credit specialize in healthcare financing. They offer various plans, including interest-free periods for qualified applicants (often 6-24 months) and extended payment plans with fixed interest rates.
- Personal Loans: Banks and credit unions offer unsecured personal loans that can be used for any purpose, including dental implants. Interest rates vary based on your credit score.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use pre-tax dollars to pay for dental implant procedures, offering a significant tax advantage.
- Credit Cards: Standard credit cards can be used, but be mindful of potentially high-interest rates if not paid off quickly.
- Dental Schools: As mentioned, dental schools across the US often provide high-quality care at significantly reduced prices, supervised by experienced faculty. This can be an excellent option for those on a tighter budget, though it may require more time and patience.
Cost-Saving Tips
- Compare Quotes: Get detailed quotes from a few different qualified dentists or specialists. Ensure the quotes are comprehensive and include all stages of treatment.
- Inquire About Package Deals: Some practices, especially those specializing in full-arch solutions like All-on-4, may offer package pricing that includes all steps.
- Max Out Insurance: Plan your treatment to maximize your annual insurance benefits, potentially splitting the procedure across two calendar years if your plan renews benefits annually.
- Use HSAs/FSAs: If available, contribute maximally to these accounts to use tax-free money for your implants.
- Consider Dental Tourism (with caution): While some individuals look to countries with lower healthcare costs for dental work, this carries significant risks regarding quality control, follow-up care, and legal recourse if complications arise. It's generally not recommended for complex procedures like implants.
Frequently Asked Questions
### How painful is the dental implant procedure?
Most patients report that the dental implant placement procedure itself is not painful due to local anesthesia and available sedation options. You might feel pressure, but not sharp pain. Post-surgery, some discomfort, swelling, and bruising are common, typically managed effectively with prescribed pain medication and over-the-counter pain relievers for a few days.
### How long do dental implants last?
With proper oral hygiene, regular dental check-ups, and a healthy lifestyle, dental implants can last for many decades, often a lifetime. The crown or bridge attached to the implant may need replacement after 10-15 years due to wear and tear, but the implant post itself is highly durable.
### Am I a good candidate for dental implants?
Good candidates generally have sufficient jawbone density to support the implant, healthy gum tissue, and good overall health. Chronic conditions like uncontrolled diabetes, heavy smoking, or certain medications can affect eligibility. A comprehensive dental exam, including 3D imaging, is necessary for your dentist to determine if you are a suitable candidate.
### What are the alternatives to dental implants?
The primary alternatives for replacing missing teeth are fixed dental bridges, which use adjacent teeth for support, and removable dentures (partial or complete). While generally less expensive upfront and quicker to complete, these options do not prevent jawbone loss and often offer less stability and comfort compared to implants.
### Can I get "teeth in a day" with dental implants?
Yes, in specific situations, immediate load dental implants (often called "teeth in a day") are possible. This technique allows a temporary crown or prosthesis to be placed on the implant immediately after surgery. However, it requires excellent bone quality and stability and is not suitable for all patients. Your dentist will determine if you are a candidate during the planning phase.
### Is the dental implant process long?
The complete dental implant process, from initial consultation to final restoration, typically takes 3 to 9 months. This timeline includes the healing period for osseointegration (3-6 months) after implant placement, where the implant fuses with your jawbone, plus time for any necessary preparatory procedures like bone grafting.
### Do dental implants feel like natural teeth?
One of the greatest advantages of dental implants is that they are designed to feel and function almost identically to natural teeth. Because they integrate with your jawbone, they provide a stable foundation, allowing you to chew, speak, and smile with confidence, without the slippage or discomfort associated with traditional dentures.
### What is peri-implantitis and how can I prevent it?
Peri-implantitis is an inflammatory condition affecting the tissues around a dental implant, similar to gum disease. It's often caused by bacterial infection and can lead to bone loss around the implant if untreated. Prevention is key: maintain excellent oral hygiene (brushing, flossing, mouthwash), avoid smoking, and attend regular dental check-ups for professional cleaning and monitoring.
### Will my insurance cover dental implants?
Most dental insurance plans offer limited coverage for dental implants, often classifying them as a "major procedure." Coverage typically ranges from 0% to 50% after your deductible, and plans usually have an annual maximum benefit (often $1,000-$2,000), which may cover only a portion of the total cost. Always get a pre-authorization from your insurer.
### Can dental implants fail?
While dental implants have a very high success rate (over 95%), they can fail. Common reasons include infection (peri-implantitis), lack of osseointegration (the implant doesn't fuse with the bone), smoking, uncontrolled systemic diseases (like diabetes), or excessive forces on the implant. Early detection and adherence to aftercare instructions are crucial for preventing failure.
When to See a Dentist
Knowing when to seek professional dental attention is key, both for general oral health and for specific concerns related to dental implants.
Red Flags Indicating Potential Implant Issues (See a Dentist Immediately)
If you have dental implants and experience any of the following, contact your dentist or oral surgeon without delay:
- Severe or persistent pain: While some discomfort is normal after surgery, severe or worsening pain after the initial recovery period (especially after 3-5 days) is a red flag.
- Implant mobility: If your dental implant (or the crown/abutment on it) feels loose or wobbly, this requires immediate attention, as it could indicate implant failure or a loose component.
- Significant swelling or pus: Swelling that is increasing or accompanied by pus around the implant site is a strong sign of infection.
- Bleeding that won't stop: While some initial bleeding is normal, persistent or heavy bleeding that doesn't subside after applying pressure needs urgent care.
- Numbness or tingling: If you experience new or persistent numbness or tingling in your lip, chin, or tongue, it could indicate nerve involvement and requires immediate assessment.
- Difficulty chewing or biting: If chewing becomes painful or the implant feels "off" when you bite down, it could signal an issue with the implant or restoration.
- Exposed implant threads: If you can see metal threads of the implant post through the gum tissue, it indicates gum recession or bone loss around the implant.
Routine Care and General Concerns (Schedule a Routine Appointment)
- Missing Teeth: If you have one or more missing teeth and are considering replacement options, schedule a consultation to discuss implantology.
- Unstable Dentures: If your current dentures are loose, uncomfortable, or limit your diet, explore implant-supported dentures.
- Loose or Damaged Crown/Bridge: If a crown or bridge on your implant feels loose, cracked, or is causing discomfort, schedule an appointment.
- Regular Check-ups: Adhere to your biannual (or more frequent, as recommended) dental check-ups and professional cleanings to maintain your oral health and monitor your implants.
- Concerns about oral hygiene: If you're unsure if you're cleaning your implants effectively, your dentist or hygienist can provide guidance and demonstrate proper techniques.
Pro Tip: Do not attempt to fix a problem with your dental implant yourself. Only a qualified dental professional can properly diagnose and treat issues related to dental implants. Ignoring symptoms can lead to more serious complications and potentially implant loss.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Implantologist: Complete Guide
Losing a tooth can be a significant setback, impacting not only your smile but also your ability to speak, chew, and maintain overall oral health. In fact, over 3 million Americans currently have dental implants, and that number is projected to grow significantly as more people seek a durable, n
March 8, 2026
Dentures Over Implants: Complete Guide
Missing multiple teeth or even an entire arch can profoundly impact your life, affecting everything from your ability to chew and speak to your self-confidence. For millions of Americans, traditional removable dentures have long been a solution, but they often come with compromises: slipping, discom
March 8, 2026
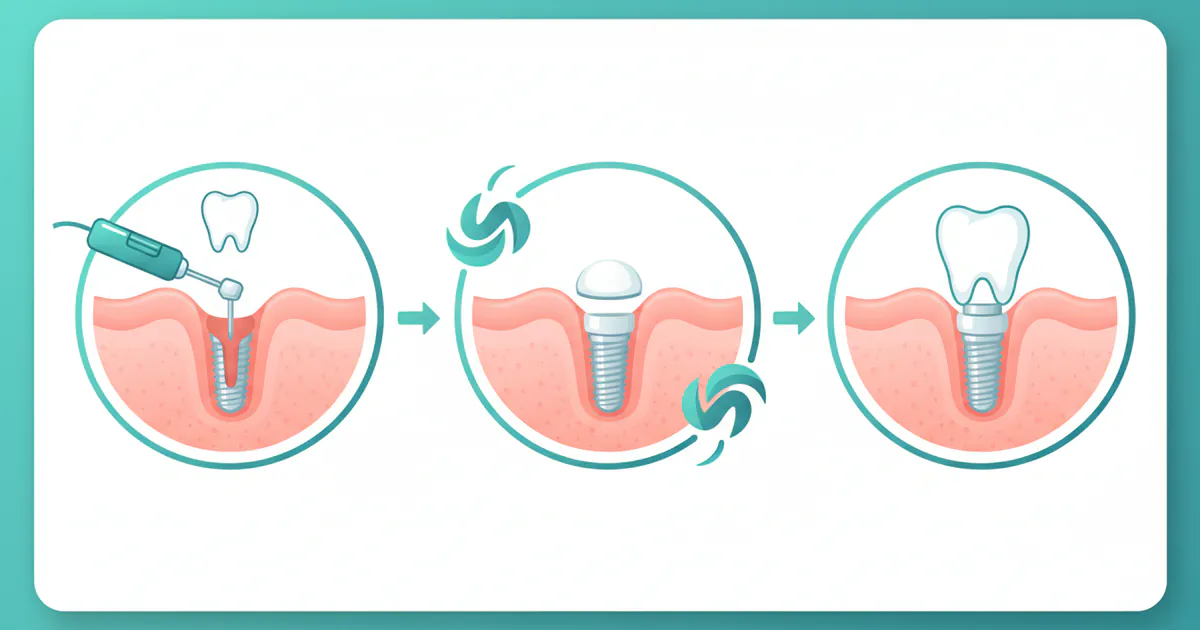
Implants Process: Complete Guide
Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the
March 8, 2026

Implants Dentaires: Complete Guide
Missing teeth can dramatically impact not just your smile, but your overall health, confidence, and quality of life. In the United States, an estimated 178 million adults are missing at least one tooth, while approximately 40 million are missing all their teeth. These statistics underscore a
March 8, 2026