Periimplantitis: Complete Guide
Key Takeaways
- A dental implant is a marvel of modern dentistry, offering a durable and aesthetically pleasing solution for missing teeth. However, like natural teeth, implants are susceptible to their own set of challenges, one of the most significant being periimplantitis. This inflammatory condition can jeo
A dental implant is a marvel of modern dentistry, offering a durable and aesthetically pleasing solution for missing teeth. However, like natural teeth, implants are susceptible to their own set of challenges, one of the most significant being periimplantitis. This inflammatory condition can jeopardize the stability and longevity of your dental implant, potentially leading to its loss if not addressed promptly. Are you experiencing discomfort around your implant, or perhaps noticing swelling or bleeding? Understanding periimplantitis is crucial for anyone with dental implants, as early detection and intervention can make all the difference in preserving your smile. This comprehensive guide will delve into what periimplantitis is, its causes, symptoms, treatment options, costs, and most importantly, how to prevent it, ensuring your dental implants remain a healthy, long-term solution.
Key Takeaways:
- Periimplantitis is an inflammatory disease affecting the tissues surrounding a dental implant, characterized by bone loss.
- Early Detection is Key: Look for signs like bleeding gums, swelling, pain, or pus around your implant. Regular dental check-ups are vital.
- Causes: Primarily bacterial plaque accumulation, but also influenced by poor oral hygiene, smoking, uncontrolled diabetes, and certain implant design factors.
- Treatment Options: Range from non-surgical debridement (cleaning) to surgical interventions (flap surgery, bone grafting, implant surface decontamination, or explantation).
- Cost Implications: Treatment can range from $500 to $4,000+ per implant, depending on severity and method. Explantation can add $200-$1,000, with replacement potentially costing $3,000-$6,000+.
- Prevention is Paramount: Excellent daily oral hygiene, regular professional cleanings, avoiding smoking, and managing systemic diseases are crucial for preventing periimplantitis.
- Long-Term Outlook: With timely and appropriate treatment, many cases can be managed, but severe cases may necessitate implant removal and potential replacement.
What It Is / Overview
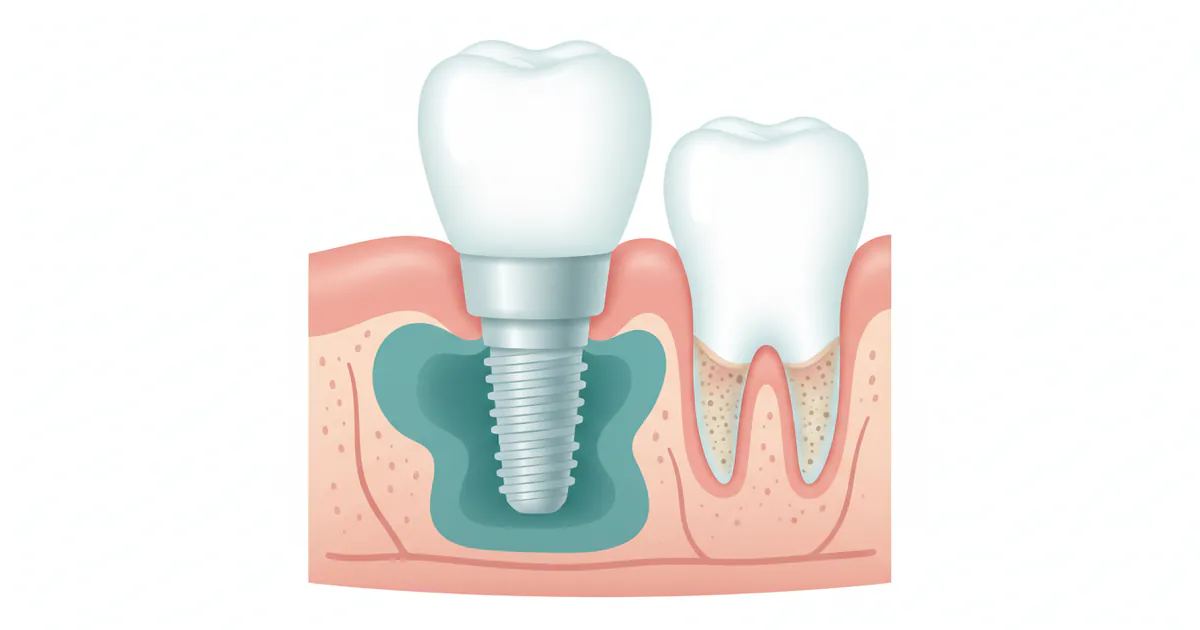
Periimplantitis is a chronic inflammatory disease that affects the soft tissues and bone supporting a dental implant. It's essentially the dental implant equivalent of periodontitis, which affects natural teeth. The condition is characterized by progressive destruction of the peri-implant bone, meaning the bone that has fused with and supports the implant begins to erode. If left untreated, this bone loss can lead to the loosening of the implant and ultimately, its failure or loss.
This condition typically develops after the implant has successfully integrated with the bone (osseointegration) and is already in function, meaning it's been supporting a crown, bridge, or denture. Studies suggest that periimplantitis affects approximately 10-20% of dental implants and up to 40% of patients with implants globally. In the US, with millions of dental implants placed annually, this translates to a significant number of individuals potentially facing this challenge. Understanding the mechanisms behind this disease is the first step toward effective management and prevention.
Types / Variations
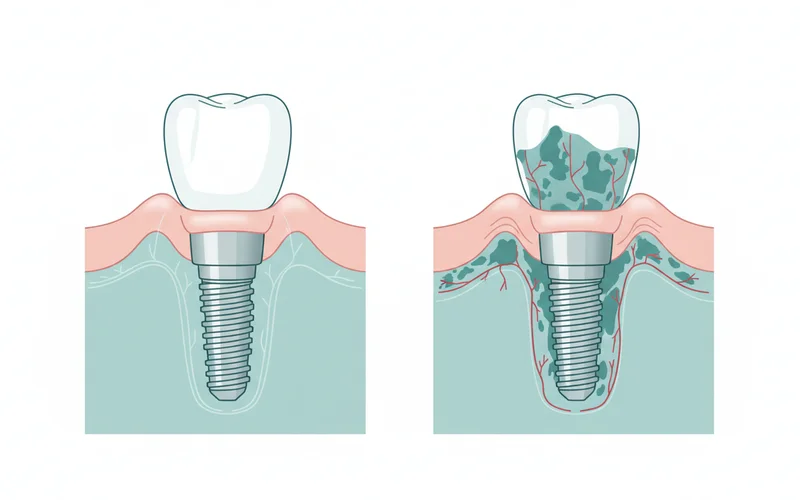
While periimplantitis refers specifically to bone loss around an implant, it's often preceded by a milder condition. Understanding the progression helps in early intervention:
Peri-Implant Mucositis
This is the precursor to periimplantitis, affecting only the soft tissues (gums) around the implant without any evidence of bone loss. It's similar to gingivitis around a natural tooth.
- Characteristics: Inflammation, redness, swelling, and bleeding upon probing around the implant.
- Reversibility: Often reversible with improved oral hygiene and professional cleaning, as no bone loss has occurred.
Periimplantitis
This is the more severe stage, where the inflammation has progressed beyond the soft tissues and has started to cause destruction of the supporting alveolar bone.
- Characteristics: Inflammation, redness, swelling, bleeding upon probing, pus formation, and most importantly, radiographic evidence of progressive bone loss around the implant, accompanied by an increase in probing depth.
- Reversibility: Not easily reversible, requiring more intensive treatment to halt progression and ideally regenerate lost bone.
Classification by Severity
Dentists often classify periimplantitis by its severity, which guides treatment decisions:
- Mild Periimplantitis: Initial signs of bone loss beyond the normal physiological remodeling, often less than 2mm from the implant shoulder, with soft tissue inflammation.
- Moderate Periimplantitis: More significant bone loss (2-4mm), often accompanied by deeper probing depths and potentially visible pus.
- Severe Periimplantitis: Extensive bone loss (over 4mm), significant probing depths, mobility of the implant, and severe inflammation, often requiring explantation.
Causes / Why It Happens
The development of periimplantitis is multifactorial, meaning several factors can contribute to its onset and progression. The primary driver, however, is bacterial infection, specifically the accumulation of plaque biofilm around the implant.
Primary Cause: Bacterial Plaque Accumulation
Just like natural teeth, dental implants can accumulate plaque, a sticky film of bacteria. If not removed regularly through diligent oral hygiene, this plaque hardens into calculus (tartar) and the bacteria within it release toxins. These toxins trigger an inflammatory response in the surrounding tissues. The unique surface characteristics of dental implants, which are often rough to promote bone integration, can also inadvertently harbor bacteria more easily than the smooth enamel of natural teeth if not cleaned properly.
Contributing Factors:
Several factors can increase a patient's susceptibility to developing periimplantitis:
- Poor Oral Hygiene: This is perhaps the most significant modifiable risk factor. Inadequate brushing and flossing around implants allow plaque to accumulate unchecked.
- Smoking: Smokers have a significantly higher risk of periimplantitis. Smoking impairs the immune response, reduces blood flow to the gums, and hinders tissue healing, making them more vulnerable to infection and less able to recover.
- History of Periodontitis: Patients who have previously suffered from periodontitis (gum disease) are at a much higher risk for periimplantitis. The same bacteria that caused gum disease around their natural teeth can colonize their implants.
- Uncontrolled Diabetes: Poorly controlled diabetes compromises the body's immune system and healing capacity, increasing the risk of infections, including periimplantitis.
- Excess Cement: During the placement of the dental crown on the implant, excess dental cement can sometimes be left beneath the gum line. This cement acts as a foreign body and a plaque trap, irritating the tissues and initiating inflammation.
- Implant Position and Design:
- Suboptimal Implant Placement: If an implant is placed too deep, too close to another tooth or implant, or at an incorrect angle, it can create areas that are difficult to clean, leading to plaque accumulation.
- Rough Implant Surfaces: While beneficial for osseointegration, rough implant surfaces exposed to the oral environment due to bone loss can become difficult to decontaminate, favoring bacterial adhesion.
- Prosthetic Design: Overcontoured crowns or poorly fitting prosthetic components can create ledges and niches where food debris and bacteria can accumulate, making cleaning challenging.
- Lack of Regular Dental Check-ups: Skipping routine cleanings and examinations means that early signs of peri-implant mucositis or periimplantitis might be missed, allowing the condition to progress silently.
- Genetic Predisposition: Some individuals may be genetically more susceptible to inflammatory responses.
- Occlusal Overload: Excessive biting forces on an implant (e.g., from teeth grinding/bruxism or an improperly aligned bite) might contribute to bone loss around the implant, though its role as a primary cause of periimplantitis is debated.
Pro Tip: If you have risk factors like a history of gum disease or smoking, discuss these with your dentist before getting implants. They can provide tailored advice and a more intensive follow-up schedule.
Signs and Symptoms
Recognizing the signs and symptoms of periimplantitis early is critical for successful treatment and preventing further damage. Unlike natural teeth, implants lack the nerve endings that signal pain from dental caries, so inflammation often progresses silently until it's more advanced.
Look out for these indicators around your dental implant:
- Bleeding Gums: One of the earliest and most common signs. If your gums bleed when you brush, floss, or even when gently probed by your dentist, it's a red flag.
- Redness and Swelling: The gum tissue around the implant may appear redder than usual and swollen or puffy.
- Tenderness or Pain: While implants themselves don't have nerves, the surrounding inflamed tissues can become tender to the touch or painful, especially when chewing or brushing. This pain might be mild at first and worsen over time.
- Pus Formation (Suppuration): A more advanced sign, indicating an active infection. You might notice a discharge of pus from around the gum line of the implant, often when pressure is applied.
- Bad Breath (Halitosis) or Bad Taste: Persistent bad breath or an unpleasant taste in your mouth can be a sign of bacterial infection.
- Increased Probing Depths: Your dentist will measure the depth of the gum pocket around the implant. An increase in these measurements compared to previous appointments indicates soft tissue inflammation and potentially bone loss.
- Visible Threading of the Implant: As bone loss progresses, the metallic threads of the implant, normally hidden beneath the gum line, may become visible.
- Loosening of the Implant or Prosthesis: This is a late-stage sign. If your implant feels wobbly, or the crown attached to it becomes loose, it indicates significant bone loss and compromised stability.
- Receding Gums: The gum tissue around the implant may pull away, exposing more of the implant or its abutment.
It's important to note that some of these symptoms, particularly mild redness or bleeding, can also indicate peri-implant mucositis. However, any persistent symptom warrants a visit to your dentist for a thorough evaluation, including X-rays, to differentiate between mucositis and periimplantitis.
Treatment Options
The treatment of periimplantitis aims to eliminate the bacterial infection, reduce inflammation, decontaminate the implant surface, and, if possible, regenerate lost bone. The approach depends on the severity of the condition, the amount of bone loss, and specific patient factors.
1. Non-Surgical Treatment (for early-stage periimplantitis or mucositis)
This is typically the first line of defense, especially for peri-implant mucositis or mild periimplantitis.
- Mechanical Debridement:
- Process: The dentist uses specialized instruments (plastic or titanium curettes, ultrasonic scalers with non-metallic tips, or air-abrasive devices) to remove plaque and calculus from the implant surface and the surrounding pocket.
- Pros: Less invasive, lower cost, quick recovery.
- Cons: Limited effectiveness in deeper pockets or when the implant surface is significantly contaminated/roughened, as it can't access all affected areas.
- Antimicrobial Rinses:
- Process: Prescribed mouthwashes containing chlorhexidine gluconate are used to reduce bacterial load.
- Pros: Supports mechanical cleaning, reduces inflammation.
- Cons: Not a standalone treatment; can cause temporary staining or altered taste.
- Local or Systemic Antibiotics:
- Process: Antibiotics may be placed directly into the peri-implant pocket (local) or prescribed as oral medication (systemic) to target specific bacteria.
- Pros: Can effectively reduce bacterial populations.
- Cons: Risk of antibiotic resistance, potential side effects, often used as an adjunct to mechanical debridement.
2. Surgical Treatment (for moderate to severe periimplantitis)
When non-surgical approaches are insufficient, or if there's significant bone loss, surgical intervention is necessary.
- Open Flap Debridement with Implant Surface Decontamination:
- Process: The gum tissue is surgically lifted (a "flap") to expose the implant and underlying bone. This allows for thorough cleaning of the implant surface and removal of all calculus and diseased tissue. Various methods are used to decontaminate the exposed implant surface, including curettes, air-abrasion (using biocompatible powders like glycine), laser therapy (e.g., Nd:YAG, Er:YAG), or chemical agents (e.g., citric acid, hydrogen peroxide).
- Pros: Provides direct visibility and access for complete debridement and decontamination.
- Cons: More invasive, longer recovery, higher cost.
- Osseous Resective Surgery (Apical Repositioned Flap):
- Process: If the bone defect around the implant is shallow and broad, and the implant is well-positioned, the goal might be to eliminate the peri-implant pocket by reshaping the bone and repositioning the gum tissue apically (towards the root). This creates a shallow, easily maintainable pocket.
- Pros: Creates a maintainable environment; effective in specific situations.
- Cons: Sacrifices some healthy gum tissue, can expose implant threads, might not be aesthetically ideal.
- Regenerative Procedures (Guided Bone Regeneration - GBR):
- Process: After thorough cleaning and decontamination, bone grafting materials (autogenous, allograft, xenograft, or alloplast) are placed in the bone defect around the implant. A barrier membrane may be used to protect the graft and guide bone growth, preventing soft tissue from growing into the defect.
- Pros: Aims to rebuild lost bone, potentially restoring implant support and aesthetics.
- Cons: Unpredictable success rates, especially in complex defects; higher cost, longer healing time; requires careful case selection.
- Implant Explantation (Removal):
- Process: If the periimplantitis is severe, the implant is mobile, or other treatments have failed, removal of the implant (explantation) may be the only option. This can be done with specialized trephine burs or reverse torque instruments.
- Pros: Eliminates the source of infection, stops further bone loss.
- Cons: Loss of the dental implant, requires further treatment for tooth replacement (e.g., new implant, bridge, removable denture), potentially higher overall cost in the long run.
- Pro Tip: If explantation is necessary, discuss future tooth replacement options like a new implant placement, a dental bridge, or a partial denture with your dentist. Factors like the amount of remaining bone and the cause of the initial failure will influence the best choice. For patients considering another implant, this might lead to questions like "root canal or implant?" for other failing teeth, or "clear choice implants cost" for potential replacement.
Comparison of Treatment Approaches for Periimplantitis
| Feature | Non-Surgical Treatment | Surgical Treatment (Debridement) | Regenerative Surgery | Explantation |
|---|---|---|---|---|
| Severity | Mild periimplantitis, peri-implant mucositis | Moderate to severe periimplantitis | Moderate to severe periimplantitis with reconstructible defects | Severe, untreatable periimplantitis, mobile implant |
| Goal | Reduce inflammation, decontaminate, halt progression | Eliminate infection, decontaminate, facilitate tissue health | Rebuild lost bone, stabilize implant | Remove failed implant, resolve infection |
| Procedure | Scaling, root planing (implant), antibiotics, rinses | Flap surgery, mechanical/laser/chemical decontamination | Flap surgery, bone graft, membrane placement, decontamination | Surgical removal of implant |
| Cost Range (US) | $500 - $1,500 | $1,500 - $3,500 | $2,500 - $4,500+ | $200 - $1,000 (for removal only) |
| Healing Time | Days to weeks | 2-4 weeks for initial healing, months for full recovery | 6-9 months for bone maturation, longer for full recovery | 1-2 weeks for soft tissue, several months for bone regeneration if replanted |
| Success Rate | High for mucositis, moderate for mild periimplantitis | Moderate to high, depending on severity and technique | Variable, challenging, depends on defect morphology | 100% for removal of infection source |
| Pros | Less invasive, quicker recovery | Direct access, thorough cleaning | Potential for implant salvage and bone regrowth | Definitive solution for failed implant, resolves infection |
| Cons | Limited efficacy in advanced cases | More invasive, potential for gum recession | Unpredictable, higher cost, longer recovery, complex | Loss of implant, requires future tooth replacement |
Step-by-Step Process: What to Expect During Treatment
The journey through periimplantitis treatment typically follows a structured approach, starting with diagnosis and escalating if necessary.
1. Diagnosis and Assessment
- Initial Exam: Your dentist will perform a visual examination, checking for signs like redness, swelling, and pus. They will use a specialized probe to measure pocket depths around the implant.
- Radiographic Evaluation (X-rays): Dental X-rays (periapical, panoramic, or 3D CBCT scans) are crucial to assess the extent of bone loss around the implant. This helps determine the severity of periimplantitis and guides treatment planning.
- Patient History: Discussion of your medical history, oral hygiene habits, and risk factors (e.g., smoking, diabetes).
2. Non-Surgical Treatment Phase (if applicable)
- Professional Cleaning: The dentist or hygienist will perform thorough scaling and debridement around the implant, removing plaque and calculus. This might involve using specialized instruments that won't scratch the implant surface.
- Antimicrobial Therapy: You may be prescribed an antimicrobial mouth rinse (e.g., chlorhexidine) and/or local or systemic antibiotics, depending on the infection's severity.
- Oral Hygiene Instruction: Crucial step where your dental professional will re-educate you on proper brushing techniques for implants, interdental cleaning aids, and other home care practices.
- Follow-up: A follow-up appointment is scheduled to reassess the inflammation and determine if further treatment is needed.
3. Surgical Treatment Phase (if non-surgical fails or initial diagnosis is severe)
- Anesthesia: Local anesthesia will be administered to numb the treatment area. Sedation options may also be available for patient comfort.
- Flap Surgery: The gum tissue around the implant is carefully incised and lifted to create a "flap," exposing the implant surface and the underlying bone defect.
- Debridement and Decontamination: The exposed implant surface is meticulously cleaned to remove bacteria and calculus. Various techniques may be used, including mechanical scaling, air-abrasion, laser, or chemical agents.
- Defect Management:
- If bone regeneration is planned, bone graft material and a barrier membrane will be placed into the bone defect.
- If resective surgery is performed, minor bone reshaping might occur to eliminate deep pockets.
- Suturing: The gum flap is repositioned and sutured back into place.
- Post-operative Instructions: You'll receive detailed instructions on medication, diet, pain management, and oral hygiene during the healing period.
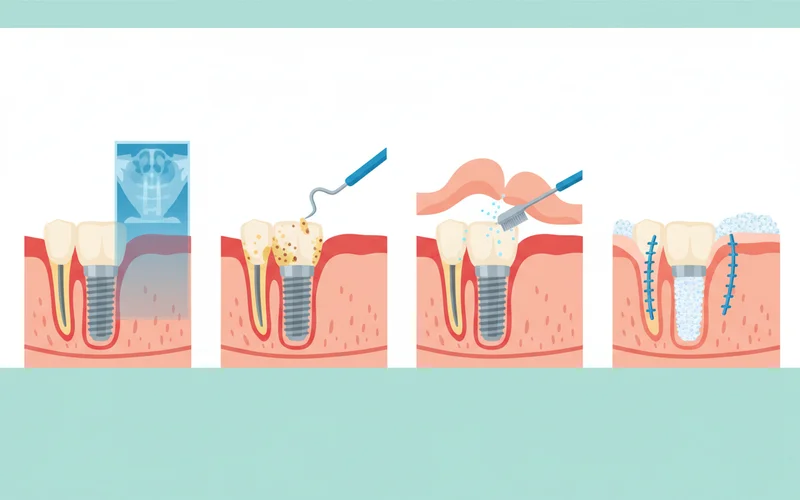
4. Explantation (If necessary)
- Anesthesia: Local anesthesia is administered.
- Surgical Removal: The failing implant is carefully removed using specialized instruments to minimize trauma to surrounding bone.
- Site Management: The extraction site may be cleaned, and bone grafting might be performed immediately or in a subsequent procedure to prepare the area for a potential future implant or another restorative option.
- Post-operative Instructions: Similar to other surgical procedures, focusing on pain management and healing.
5. Maintenance and Long-Term Care
Regardless of the treatment path, a rigorous maintenance schedule is crucial. This typically involves more frequent recall appointments (every 3-4 months) for professional cleanings, monitoring of implant health, and reinforcement of oral hygiene practices.
Cost and Insurance
The cost of periimplantitis treatment in the US can vary significantly based on the severity of the condition, the type of treatment needed, the dental professional's fees, geographic location (e.g., urban vs. rural, high cost of living areas), and whether specialists are involved.
Average US Cost Ranges:
- Initial Diagnosis & X-rays: $100 - $300 (often covered by routine dental check-up benefits).
- Non-Surgical Treatment (Per implant):
- Scaling and debridement: $500 - $1,500. This often involves multiple appointments and specific instruments.
- Local antimicrobial delivery: Additional $100 - $300 per site.
- Surgical Treatment (Per implant):
- Flap surgery with decontamination (without bone graft): $1,500 - $3,500.
- Flap surgery with decontamination and bone grafting/membrane (regenerative): $2,500 - $4,500+. This includes the cost of graft materials and membrane.
- Resective surgery: $1,500 - $3,000.
- Implant Explantation (Removal): $200 - $1,000 per implant. This cost is for removal only and does not include replacement.
Pro Tip: For patients with Clear Choice implants, the cost structure for initial implant placement is often bundled. However, periimplantitis treatment would typically be billed separately as a medical or dental procedure, similar to any other implant. Don't assume that the initial Clear Choice cost covers future complications; always clarify with your provider.
Insurance Coverage:
Dental insurance coverage for periimplantitis treatment can be complex and varies widely by plan.
- Diagnostic Procedures: Routine exams and X-rays are usually covered, often at 80-100%.
- Non-Surgical Treatment: Some plans may cover non-surgical debridement under "periodontal maintenance" or "major restorative" categories, often at 50-80%.
- Surgical Treatment: Coverage for surgical procedures is less common or may be limited. Many plans classify these as "major procedures" and might cover 0-50%, often after a deductible is met. Regenerative procedures (bone grafts) may have separate or no coverage.
- Implant Explantation: Removal may be covered under surgical extraction codes, often at 50-80%.
- Replacement Implants: If an implant needs to be removed and replaced, the new implant and crown will incur significant costs (typically $3,000-$6,000+ per implant) and may have limitations on coverage or a waiting period. Some plans may not cover implants at all.
It's crucial to contact your insurance provider directly and get a pre-determination of benefits (PDB) for any planned treatment. Your dental office can assist you with this by providing treatment codes and necessary documentation.
Recovery and Aftercare
Recovery from periimplantitis treatment, especially surgical intervention, requires diligence and patience. Proper aftercare is crucial for successful healing and preventing recurrence.
Immediate Post-Treatment (First few days):
- Pain Management: You may experience mild to moderate pain. Your dentist will prescribe pain medication or recommend over-the-counter options like ibuprofen.
- Swelling: Swelling is common, especially after surgery. Apply an ice pack to your cheek intermittently for the first 24-48 hours.
- Bleeding: Minor bleeding or oozing from the treated area is normal. Avoid rinsing vigorously.
- Diet: Stick to soft, cool foods for the first few days to avoid irritating the surgical site. Avoid hot, spicy, or crunchy foods.
- Oral Hygiene:
- Avoid the Treated Area: Do not brush or floss directly on the treated area for a specified period (usually 1-2 weeks), as advised by your dentist.
- Mouth Rinses: You'll likely be prescribed an antiseptic mouth rinse (e.g., chlorhexidine) to use gently, starting 24 hours after surgery. Avoid alcohol-based rinses.
- Gentle Cleaning: Clean other areas of your mouth normally but very gently.
- Activity: Avoid strenuous physical activity for a few days to minimize swelling and bleeding.
- Smoking: Absolutely avoid smoking, as it severely impairs healing and increases the risk of complications.
Long-Term Aftercare:
- Exceptional Oral Hygiene: This is the cornerstone of preventing periimplantitis recurrence.
- Brush Twice Daily: Use a soft-bristled toothbrush or an electric toothbrush, paying close attention to the area around your implant.
- Interdental Cleaning: Utilize interdental brushes, water flossers (like Waterpik), or specialized implant floss to clean around and beneath your implant crown. Your dentist can demonstrate the best techniques and tools for your specific implant.
- Regular Dental Check-ups and Cleanings: These are more critical than ever. Your dentist will likely recommend more frequent recall appointments (e.g., every 3-4 months) for professional cleaning and monitoring.
- Avoid Smoking: If you smoke, quitting is the single most impactful step you can take to protect your dental implants.
- Manage Systemic Conditions: If you have conditions like diabetes, ensure they are well-controlled, as they directly impact your immune response and healing capabilities.
- Nightguard: If you grind or clench your teeth (bruxism), a custom-made nightguard can protect your implants from excessive forces that could contribute to bone loss.
Pro Tip: Consider investing in a high-quality electric toothbrush and a water flosser specifically designed for implant care. These tools can significantly enhance your home oral hygiene routine around implants.
Prevention
Prevention is always better than cure, especially when it comes to periimplantitis. Implementing stringent preventive measures can significantly reduce your risk and ensure the long-term success of your dental implants.
1. Meticulous Oral Hygiene:
This is the most crucial aspect.
- Brushing: Brush at least twice daily using a soft-bristled toothbrush or an electric toothbrush. Focus on gently cleaning around the gum line of your implant.
- Interdental Cleaning: Use interdental brushes, special implant floss, or a water flosser daily. These tools are designed to access the unique contours around implants and effectively remove plaque from hard-to-reach areas.
- Antiseptic Mouthwash: Your dentist may recommend a therapeutic mouthwash, especially if you have a history of gum disease.
2. Regular Dental Check-ups and Professional Cleanings:
- Frequency: Don't skip your routine dental appointments. Most implant patients are advised to have professional cleanings and check-ups every 3-6 months.
- Specialized Care: Your hygienist will use special instruments (plastic or titanium-tipped scalers) to clean around your implants, preventing damage to their surfaces.
- Early Detection: Regular visits allow your dentist to detect early signs of peri-implant mucositis or periimplantitis through probing and X-rays, enabling timely intervention before severe bone loss occurs.
3. Lifestyle Modifications:
- Quit Smoking: Smoking is a major risk factor for implant failure and periimplantitis. Quitting or significantly reducing smoking drastically improves your implant prognosis.
- Manage Systemic Diseases: If you have diabetes, heart disease, or other systemic conditions, work closely with your physician to keep them well-controlled.
- Balanced Diet: A healthy diet supports overall oral and systemic health.
4. Address Parafunctional Habits:
- Bruxism (Teeth Grinding/Clenching): If you grind or clench your teeth, especially at night, your dentist may recommend a custom nightguard. Excessive forces can traumatize the bone around the implant, potentially contributing to bone loss.
5. Proper Implant Placement and Prosthetic Design:
While these are the responsibility of your dental professional, ensure you choose an experienced and qualified implant dentist.
- Optimal Positioning: Implants should be placed in optimal positions to allow for easy cleaning and proper load distribution.
- Well-Fitting Restorations: Crowns or bridges on implants should fit precisely, without excess cement or overhanging margins that can trap plaque.
6. Post-Surgical Follow-up:
After implant placement, adhere strictly to all post-operative instructions and follow-up appointments. This ensures proper healing and early identification of any issues.
By adopting these preventive strategies, you empower yourself to protect your investment in dental implants and enjoy a healthy, functional smile for many years to come.
Risks and Complications
While dental implants boast a high success rate, the development of periimplantitis introduces several risks and potential complications, both during and after treatment.
During Treatment:
- Pain and Discomfort: While managed with anesthesia, post-operative pain and discomfort are common.
- Swelling and Bruising: Expected after surgical procedures, but can be more pronounced in some individuals.
- Bleeding: Minor bleeding is normal, but excessive or prolonged bleeding is a complication.
- Infection: Despite decontamination efforts, there's always a risk of persistent or new infection, especially if oral hygiene is compromised.
- Nerve Damage: Though rare, surgical procedures carry a slight risk of temporary or permanent nerve damage, leading to numbness or altered sensation.
- Damage to Adjacent Structures: Accidental damage to adjacent teeth, implants, or anatomical structures (like the maxillary sinus) is a rare but possible complication.
After Treatment / Long-Term Complications:
- Recurrence of Periimplantitis: Without diligent aftercare and lifestyle changes, periimplantitis can recur, leading to further bone loss and potentially requiring more aggressive treatment.
- Treatment Failure: Not all periimplantitis treatments are successful, especially in advanced cases or for patients with uncontrolled risk factors. The implant may continue to lose bone or remain inflamed.
- Implant Loss/Failure: This is the ultimate complication. If periimplantitis cannot be controlled, the implant will eventually loosen and need to be removed. This means losing your dental implant and potentially needing further procedures (bone grafting) before a new tooth replacement can be considered.
- Aesthetic Compromise: Bone loss and gum recession around the implant can lead to an undesirable aesthetic outcome, especially in the front of the mouth. This can expose the implant threads or metal collar.
- Difficulty with Future Replacement: If an implant is lost due to severe periimplantitis, the remaining bone may be insufficient for immediate replacement with another implant. Extensive bone grafting might be required, delaying the process and adding to the cost.
- Spread of Infection: In rare, severe cases, an uncontrolled infection could spread to other areas, though this is highly uncommon with regular dental care.
Understanding these risks underscores the importance of prompt treatment, meticulous follow-up, and strict adherence to your dentist's post-treatment and preventive care instructions.
Children / Pediatric Considerations
Dental implants, and consequently periimplantitis, are not typically a concern for children or adolescents. The primary reason for this is that dental implants require a fully developed and mature jawbone for successful and stable integration. In children and teenagers, the jawbones are still growing and developing. Placing an implant before growth is complete could interfere with normal jaw development, lead to improper positioning of the implant, or cause the implant to become submerged as the surrounding bone continues to grow.
Generally, dental implants are only considered after skeletal maturity, which typically occurs around 16-18 years for females and 18-20 years for males. Therefore, periimplantitis, a condition affecting already-placed implants, is almost exclusively an adult health concern.
For children who lose permanent teeth, other restorative options like space maintainers, removable partial dentures, or adhesive bridges are usually considered until they reach skeletal maturity and implants become a viable, long-term solution.
Cost Breakdown
A more detailed look at the financial aspects of periimplantitis treatment, beyond the general ranges provided earlier, will help you prepare. Remember, these are averages and can fluctuate.
Average US Costs (Low, Mid, High by procedure):
| Procedure Type | Low-Range (US$) | Mid-Range (US$) | High-Range (US$) | Notes |
|---|---|---|---|---|
| Initial Consultation & X-rays | $100 | $200 | $350 | Periapical, panoramic, or CBCT scan. Often covered by insurance. |
| Non-Surgical Debridement | $500 | $800 | $1,500 | Per implant, often multiple sessions. Includes specialized scaling. |
| Local Antibiotic Delivery | $100 | $200 | $300 | Per site, often an adjunct to debridement. |
| Surgical Flap Debridement | $1,500 | $2,500 | $3,500 | Per implant, includes surgical access and cleaning. |
| Bone Grafting (Regenerative) | $1,000 | $2,000 | $3,000+ | Additional cost to surgical debridement; includes material and membrane. |
| Implant Explantation | $200 | $500 | $1,000 | Per implant, removal only. Does not include new implant or replacement. |
| New Implant Placement | $3,000 | $4,500 | $6,000+ | If explanted implant needs replacement. Cost for implant body, abutment, crown. |
| Follow-up & Maintenance | $150/visit | $250/visit | $350/visit | Typically 3-4 months initially, then every 6 months, after initial treatment. |
Note: Costs can vary significantly between general dentists and specialists (periodontists, oral surgeons), and geographically.
With vs. Without Insurance:
- With Insurance: If your dental insurance covers periimplantitis treatment, you might expect to pay 20-80% of the total cost out-of-pocket, depending on your plan's specifics (deductibles, annual maximums, percentage of coverage for "major procedures," waiting periods). For example, if a surgical treatment costs $2,500 and your insurance covers 50% after a $500 deductible, you would pay $1,750 ($500 deductible + $1,250 co-pay). Many plans have an annual maximum (e.g., $1,000-$2,000), which can quickly be reached with surgical periimplantitis treatment or new implant placement.
- Without Insurance: You will be responsible for 100% of the costs. This is where payment plans and financing options become particularly important.
Payment Plans and Financing Options:
- In-Office Payment Plans: Many dental offices offer interest-free payment plans for a portion of the treatment cost, allowing you to pay in installments over a few months.
- Third-Party Medical Financing: Companies like CareCredit are widely accepted in dental offices. They offer various financing options, including interest-free periods (typically 6-24 months) if the balance is paid in full within that time, or longer-term plans with interest.
- Personal Loans: Banks and credit unions offer personal loans that can be used for medical expenses.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use pre-tax dollars to pay for dental treatments, effectively saving you money.
Cost-Saving Tips:
- Early Detection: The most significant cost-saving measure is preventing periimplantitis or catching it early. Non-surgical treatments are substantially less expensive than surgical or explantation procedures.
- Preventive Care: Adhering to excellent oral hygiene and regular check-ups can prevent the disease from starting or progressing.
- Shop Around (Carefully): While not advisable to choose a dentist solely on price, obtaining a second opinion and comparing treatment plans and costs from different reputable providers can be beneficial.
- Maximize Insurance Benefits: Understand your insurance plan thoroughly. Schedule treatments strategically if you have an annual maximum to utilize benefits across two calendar years.
- Ask About Discounts: Some dental offices offer discounts for upfront payment in full.
- Consider Dental Schools: If there's a reputable dental school nearby, they often offer services at a reduced cost, as procedures are performed by students under the close supervision of experienced faculty.
For those curious about "clear choice implants cost" in the context of periimplantitis, it's important to differentiate. Clear Choice is a brand that typically offers full-arch implant solutions. While their initial costs are bundled, any subsequent periimplantitis treatment on those implants would fall under the general cost structures outlined above, and may or may not be covered by their initial warranty or by your personal dental insurance. Always clarify this directly with your provider.
Frequently Asked Questions
Is periimplantitis common?
Yes, periimplantitis is relatively common. Studies estimate that it affects about 10-20% of individual dental implants and up to 40% of patients with implants. Its prevalence increases with time after implant placement.
Can periimplantitis be cured?
Periimplantitis can be managed and controlled, but a complete "cure" in the sense of reversing all bone loss and restoring the implant to its initial healthy state is challenging, especially in advanced cases. The goal of treatment is to halt the disease progression, eliminate inflammation, decontaminate the implant surface, and ideally achieve some level of bone regeneration.
How painful is periimplantitis treatment?
The pain level depends on the type of treatment. Non-surgical cleaning might cause mild discomfort, managed with local anesthetic. Surgical treatments will involve local anesthesia, so you won't feel pain during the procedure, but you'll experience soreness, swelling, and moderate pain during recovery, managed with prescribed medication.
How long does periimplantitis treatment take?
Non-surgical treatment might involve one or a few appointments over a few weeks. Surgical treatment involves one main procedure, but the healing phase can last several weeks for soft tissue and several months for bone regeneration. Long-term maintenance and follow-up will be ongoing.
What happens if periimplantitis is left untreated?
If periimplantitis is left untreated, the inflammation and bone loss will progressively worsen. This can lead to significant destruction of the bone supporting the implant, resulting in implant mobility, persistent infection, pain, and eventually, the loss of the dental implant.
What are the alternatives if my implant needs to be removed?
If an implant needs to be removed due to severe periimplantitis, alternatives for tooth replacement include a traditional dental bridge (if adjacent teeth are suitable), a removable partial denture, or, if sufficient bone can be regenerated, another dental implant placed after a healing period.
Can I get another implant after explantation?
Yes, in many cases, you can get another implant after the failing one has been removed (explantation). However, you will likely need a period of healing, and bone grafting might be required to rebuild the lost bone before a new implant can be placed successfully.
What is the difference between peri-implant mucositis and periimplantitis?
Peri-implant mucositis is inflammation of the soft tissues (gums) around an implant without bone loss, similar to gingivitis. It's reversible. Periimplantitis is a more severe condition involving inflammation and progressive bone loss around the implant, similar to periodontitis, and is not easily reversible.
What is the role of "root canal or implant" in this context?
While directly related to natural teeth, the question "root canal or implant" sometimes arises if a patient has a failing natural tooth adjacent to an implant affected by periimplantitis, or if the initial implant was placed because a root canal failed. It speaks to the broader decision-making process for tooth replacement and preservation, emphasizing the importance of comprehensive dental health and considering all options when facing dental issues.
Are Clear Choice implants more susceptible to periimplantitis?
Clear Choice implants, like any other dental implant system, are susceptible to periimplantitis. The brand itself doesn't inherently make them more or less prone to the condition. The risk factors (oral hygiene, smoking, systemic health, etc.) and the quality of implant placement and maintenance are the primary determinants. "Clear Choice implants cost" typically reflects a full-arch solution, and future periimplantitis treatment would be a separate consideration.
When to See a Dentist
Given the silent progression of periimplantitis, knowing when to seek professional help is vital. Don't wait until you experience severe pain or your implant feels loose.
You should see your dentist immediately if you notice any of the following warning signs around your dental implant:
- Bleeding gums: Especially if it happens regularly when brushing, flossing, or spontaneously. This is often an early sign of inflammation.
- Redness or swelling: If the gum tissue around your implant appears red, puffy, or swollen.
- Tenderness or discomfort: Any persistent or increasing tenderness or pain around the implant, even if it's mild.
- Pus: If you see or taste any yellowish discharge (pus) coming from around the implant.
- Bad breath or bad taste: Persistent bad breath or an unpleasant taste that cannot be resolved with routine brushing.
- Visible implant threads: If you notice that more of the metallic part of the implant, which should be covered by gum and bone, is becoming visible.
- Loose implant or crown: This is a late-stage sign requiring urgent attention. If your implant or the crown attached to it feels wobbly, see your dentist immediately.
Regular, scheduled appointments (every 3-6 months for most implant patients, as recommended by your dentist) are crucial for detecting early signs of peri-implant mucositis or periimplantitis before they become severe. These routine check-ups, even without noticeable symptoms, are your best defense against the progression of this condition.
Don't hesitate to contact your dentist if you have any concerns about your dental implant's health. Early intervention significantly improves the prognosis for treating periimplantitis and preserving your dental implant.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Implantologist: Complete Guide
Losing a tooth can be a significant setback, impacting not only your smile but also your ability to speak, chew, and maintain overall oral health. In fact, over 3 million Americans currently have dental implants, and that number is projected to grow significantly as more people seek a durable, n
March 8, 2026
Dentures Over Implants: Complete Guide
Missing multiple teeth or even an entire arch can profoundly impact your life, affecting everything from your ability to chew and speak to your self-confidence. For millions of Americans, traditional removable dentures have long been a solution, but they often come with compromises: slipping, discom
March 8, 2026
Implants Process: Complete Guide
Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the
March 8, 2026

Implants Dentaires: Complete Guide
Missing teeth can dramatically impact not just your smile, but your overall health, confidence, and quality of life. In the United States, an estimated 178 million adults are missing at least one tooth, while approximately 40 million are missing all their teeth. These statistics underscore a
March 8, 2026