Permanent Dentures vs Implants: Complete Comparison Guide
Key Takeaways
- Deciding how to replace missing teeth is a critical health decision, impacting not just your smile but your overall well-being. Over 178 million Americans are missing at least one tooth, and roughly 40 million are edentulous (missing all teeth). When faced with tooth loss, the choice often comes
Deciding how to replace missing teeth is a critical health decision, impacting not just your smile but your overall well-being. Over 178 million Americans are missing at least one tooth, and roughly 40 million are edentulous (missing all teeth). When faced with tooth loss, the choice often comes down to advanced restorative options that offer stability and longevity. This guide provides a comprehensive comparison between permanent dentures vs implants, offering the in-depth information you need to make an informed decision about restoring your smile and oral function. We'll explore everything from what these treatments entail and their costs, to the step-by-step process and recovery.
Key Takeaways:
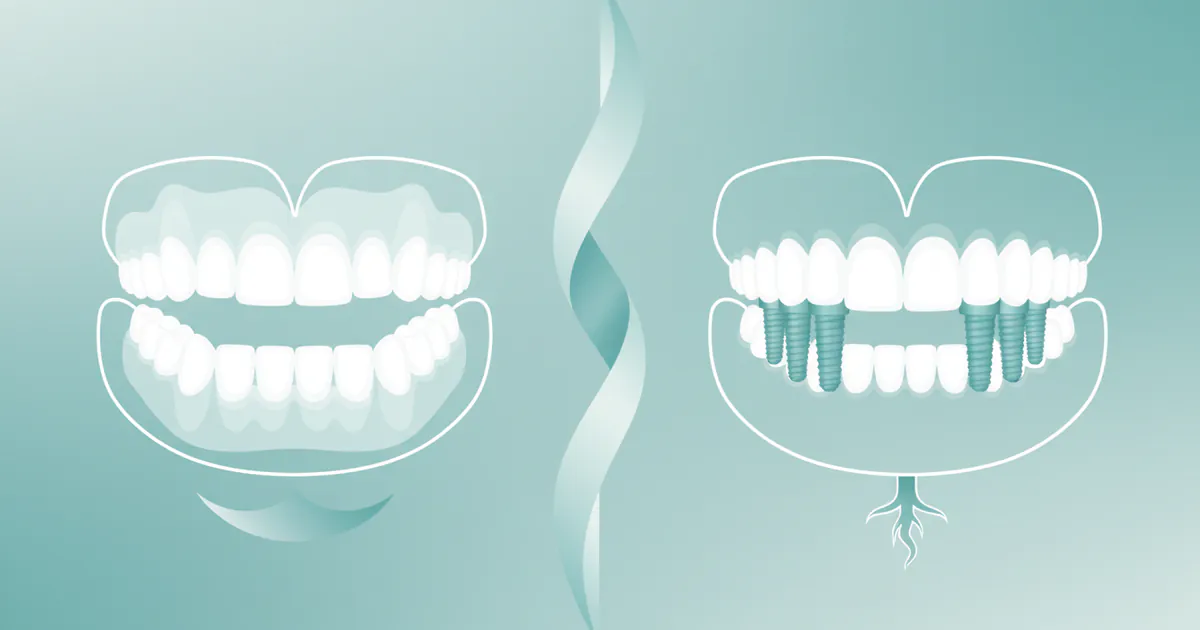
- Dental Implants are surgically placed artificial tooth roots, offering the highest stability, bone preservation, and a feel closest to natural teeth. They are a long-term investment, often lasting a lifetime.
- Permanent Dentures typically refer to implant-supported dentures (either removable snap-in or fixed screw-retained), which provide significantly more stability and comfort than traditional dentures.
- Cost Variance: A single dental implant can range from $3,000 to $6,000 (excluding bone grafts/extractions), while a full arch of implant-supported fixed dentures (e.g., All-on-4) can cost $20,000 to $40,000 per arch. Traditional full dentures are significantly less, typically $1,000 to $3,000 per arch.
- Treatment Timeline: A single implant can take 4-9 months from extraction to final crown, especially if bone grafting is needed. Full arch implant-supported dentures can also follow a similar timeline, though immediate load options can provide teeth sooner.
- Bone Health is Key: Dental implants require adequate bone density. If bone loss has occurred, bone grafting procedures will be necessary, adding to cost and treatment time.
- Insurance Coverage: Many dental insurance plans offer some coverage for dental implants or implant-supported dentures, often covering a percentage of the surgical component or the restorative prosthetic, but rarely 100%. Maximize benefits by understanding your annual limits and waiting periods.
- Longevity: Dental implants boast a 95-98% success rate and can last 25 years to a lifetime with proper care. Implant-supported dentures can last 10-20 years, with the implants themselves lasting longer.
What It Is / Overview
Understanding the fundamental difference between "permanent dentures" and dental implants is the first step toward choosing the right solution for your oral health needs. While both aim to replace missing teeth and restore function, their design, stability, and interaction with your jawbone are distinct.
Dental Implants: The Gold Standard for Tooth Replacement
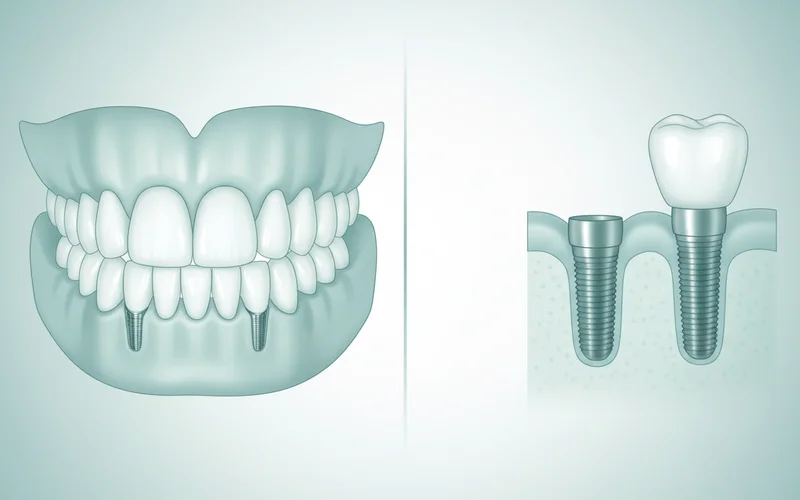
A dental implant is a sophisticated prosthetic device designed to replace the root of a missing tooth. It consists of a small, screw-shaped post, typically made of biocompatible titanium, which is surgically placed into the jawbone beneath the gum line. Over a period of several months, the implant fuses directly with the jawbone in a process called osseointegration. Once integrated, it provides a stable foundation for an abutment (a connector) and a custom-made crown, bridge, or even a full denture.
The key characteristic of dental implants is their independent nature; they don't rely on neighboring teeth for support and they actively stimulate the jawbone, preventing the bone loss that typically occurs after tooth extraction. This makes them the closest functional and aesthetic replica of natural teeth.
Permanent Dentures: Stability Through Implants
The term "permanent dentures" can be somewhat ambiguous, as traditional removable dentures are not truly permanent. However, in modern dentistry, "permanent dentures" almost always refers to implant-supported dentures. These are full or partial dental prostheses that are securely anchored to a series of dental implants rather than resting on the gums alone.
There are two primary types of implant-supported permanent dentures:
- Removable, Implant-Supported Overdentures (Snap-In Dentures): These dentures "snap" onto a few strategically placed implants (typically 2-4 in the lower jaw, 4-6 in the upper). While they offer significantly greater stability and retention than conventional dentures, they can still be removed by the patient for cleaning and daily care.
- Fixed, Implant-Supported Dentures (Screw-Retained or Hybrid Dentures): These prostheses are permanently attached to a greater number of implants (typically 4-6 or more per arch, often referred to as "All-on-4" or "All-on-6" systems) and can only be removed by a dentist. They provide the highest level of stability and chewing efficiency among denture options, closely mimicking the feel of natural teeth.
The defining feature of permanent dentures, therefore, is their reliance on dental implants for their stability and "permanent" attachment, preventing the slipping, discomfort, and bone loss associated with traditional dentures.
Types / Variations
The field of restorative dentistry offers several specialized variations for both dental implants and permanent dentures, tailored to individual needs, bone quality, and budget.
Dental Implants: Precision and Versatility
The core concept of a dental implant is consistent, but its application varies:
- Single Tooth Implant: This is the most common application, replacing a single missing tooth without affecting adjacent healthy teeth. It involves one implant, one abutment, and one custom crown.
- Multiple Tooth Implants (Implant-Supported Bridge): When several adjacent teeth are missing, two or more implants can support a dental bridge. This avoids the need to grind down healthy teeth, as is done with traditional bridges.
- Full Arch Implants (All-on-4, All-on-6, Zygomatic Implants): These systems are designed to replace an entire arch of missing teeth using a minimal number of implants (typically 4-6) to support a fixed, full-arch bridge or denture.
- All-on-4/6: This technique strategically places four or six implants in the jawbone, often at an angle in the posterior, to maximize bone contact and stability, even in cases of moderate bone loss. It often allows for immediate placement of a temporary prosthesis.
- Zygomatic Implants: For patients with severe upper jawbone loss, where traditional implants are not feasible, zygomatic implants are longer implants anchored into the dense zygoma bone (cheekbone). This avoids the need for extensive bone grafting.
- Mini Dental Implants (MDIs): These are smaller in diameter than conventional implants and are often used for stabilizing traditional dentures, particularly in the lower jaw, or for temporary orthodontic anchorage. They are generally less expensive and involve a less invasive placement procedure but may not offer the same long-term stability as standard implants for all applications.
Permanent Dentures: Enhanced Stability
As discussed, "permanent dentures" primarily refer to implant-supported solutions:
- Removable Overdentures (Snap-In): These utilize 2 to 4 implants per arch, fitted with ball or bar attachments that correspond to receivers on the underside of the denture. The denture snaps into place, offering significant improvement in retention over conventional dentures. They are removed daily for cleaning.
- Fixed Hybrid Dentures (Screw-Retained): These are permanently secured to 4 to 6 or more implants per arch. The denture is fabricated with a metal bar framework that is then directly screwed onto the implants, making it non-removable by the patient. This offers the highest level of stability and chewing power, virtually indistinguishable from natural teeth in function. These are often used in "All-on-4" or "All-on-6" protocols.
- Implant-Supported Partial Dentures: In cases where several teeth are missing but some natural teeth remain, implants can be used to support a partial denture, providing greater stability and reducing the strain on remaining natural teeth.
Causes / Why It Happens
The need for tooth replacement, whether with dental implants or permanent dentures, stems from a variety of factors leading to tooth loss. Understanding these root causes can emphasize the importance of prevention and timely intervention.
- Severe Tooth Decay (Cavities): Untreated cavities can progress deep into the tooth, infecting the pulp (nerve tissue) and leading to structural compromise that makes the tooth unrestorable.
- Advanced Gum Disease (Periodontitis): This is the leading cause of tooth loss in adults. Periodontitis is a chronic inflammatory disease that destroys the soft tissues and bone supporting the teeth, causing them to loosen and eventually fall out.
- Trauma or Injury: Accidents, sports injuries, or falls can result in knocked-out teeth (avulsion) or fractures that are too severe to repair.
- Failed Root Canal Treatment: While root canals aim to save infected teeth, some treatments may fail, leading to reinfection or structural weakness that necessitates extraction.
- Congenital Conditions: Some individuals are born with missing teeth (hypodontia or anodontia), requiring prosthetic solutions from a young age (though implants are typically delayed until jawbone maturity).
- Aging and Wear and Tear: Over time, teeth can become worn down, cracked, or simply become too fragile to maintain, especially without proper dental care.
- Systemic Diseases: Certain systemic conditions, such as diabetes, osteoporosis, or autoimmune disorders, can increase the risk of gum disease and tooth loss.
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque and tartar buildup, leading to decay and gum disease, which are primary drivers of tooth loss.
When one or more teeth are lost, the surrounding bone begins to resorb or shrink due to lack of stimulation. This bone loss can affect facial aesthetics and the stability of any future tooth replacements, underscoring the benefits of bone-preserving solutions like dental implants.
Treatment Options: Pros and Cons
Both dental implants and permanent dentures (implant-supported) offer significant advantages over traditional removable dentures, but they also come with their own set of considerations.
Dental Implants (Single or Multiple)
Pros:
- Natural Feel and Function: Closest to natural teeth in comfort, chewing power, and aesthetics.
- Bone Preservation: Stimulates the jawbone, preventing bone loss and maintaining facial structure.
- Independent: Does not require altering adjacent healthy teeth.
- High Success Rate: Over 95-98% success rate with proper care.
- Longevity: Can last 25 years to a lifetime with good oral hygiene.
- Improved Speech: No slipping or clicking, allowing for clear speech.
- Enhanced Confidence: Stable, secure, and aesthetically pleasing.
Cons:
- Higher Initial Cost: Generally the most expensive tooth replacement option.
- Surgical Procedure: Requires minor surgery, which comes with standard surgical risks.
- Longer Treatment Time: Osseointegration takes 3-6 months; total treatment can be 4-9 months or longer if bone grafting is needed.
- Bone Requirements: Requires sufficient jawbone density; bone grafting may be necessary if bone loss has occurred.
- Not for Everyone: Contraindications include uncontrolled diabetes, heavy smoking, certain medical conditions, and very young patients whose jawbones are still developing.
Permanent Dentures (Implant-Supported Overdentures - Removable Snap-In)
Pros:
- Improved Stability: Far more stable and comfortable than traditional dentures, reducing slipping and sore spots.
- Better Chewing Efficiency: Allows for consumption of a wider variety of foods.
- Enhanced Speech: Less likely to slip, leading to clearer pronunciation.
- Bone Preservation (Partial): Implants help to reduce jawbone resorption compared to traditional dentures.
- Easier to Clean: Can be removed for thorough cleaning.
- Often More Affordable: Generally less expensive than fixed implant bridges, requiring fewer implants.
Cons:
- Still Removable: Though stable, they are not permanently fixed and require daily removal for cleaning.
- Less Chewing Power: While improved, still not as strong as fixed implants or natural teeth.
- Bulkier: The denture base can feel bulkier than natural teeth or fixed bridges.
- Maintenance: Attachments (e.g., O-rings) may need periodic replacement.
- Surgical Procedure: Requires implant placement surgery.
Permanent Dentures (Fixed Hybrid Dentures - Screw-Retained All-on-4/6)
Pros:
- Excellent Stability and Chewing Power: Very close to natural teeth, allowing for a full diet.
- Non-Removable: Permanently fixed, offering maximum confidence and convenience.
- Bone Preservation: Implants stimulate the jawbone, minimizing resorption.
- Streamlined Design: Often less bulky than removable overdentures, improving comfort.
- Rapid Rehabilitation (Often): In many cases, a temporary fixed prosthesis can be placed on the same day as implant surgery.
- High Esthetics: Custom-designed to look natural.
Cons:
- Higher Cost: More expensive than removable overdentures, comparable to or slightly less than individual implants for a full arch.
- Surgical Procedure: Requires significant surgical intervention for multiple implants.
- Bone Requirements: While All-on-4/6 systems are designed for moderate bone loss, severe cases may still require grafting.
- Cleaning Challenges: While not removable by the patient, special hygiene tools (e.g., water flossers, interproximal brushes) are needed to clean under the bridge.
- Potential for Complications: Though rare, complications like implant failure or prosthetic fracture can occur.
Step-by-Step Process
The journey to a restored smile with dental implants or implant-supported permanent dentures involves several stages. While specific timelines can vary, the general process follows a predictable sequence.
Dental Implant Process (Single Tooth Example)
- Initial Consultation and Planning:
- The dentist or oral surgeon performs a thorough examination, including X-rays, 3D cone-beam computed tomography (CBCT) scans, and digital impressions.
- This determines jawbone quality and quantity, identifies vital structures (nerves, sinuses), and plans the precise implant placement.
- Medical history is reviewed to ensure you are a suitable candidate.
- Tooth Extraction (If Necessary):
- If the tooth is still present and needs removal, it will be extracted.
- Pro Tip: In some cases, immediate implant placement after extraction is possible, reducing overall treatment time.
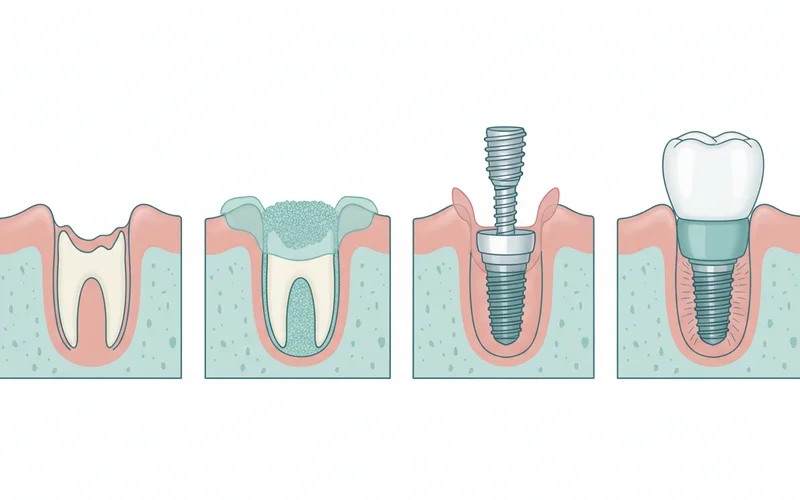
- Bone Grafting (If Necessary):
- If there's insufficient bone, a bone grafting procedure is performed to augment the site. This could be a minor graft for a single tooth or a sinus lift for the upper jaw.
- Healing time for bone grafts typically ranges from 3 to 9 months.
- Implant Placement Surgery:
- Under local anesthesia (sometimes with sedation), an incision is made in the gum to expose the jawbone.
- A small pilot hole is drilled, and the titanium implant post is carefully threaded into the bone.
- The gum tissue is then sutured over the implant, or a healing abutment is placed to allow the gum to heal around it.
- This is typically performed by an oral surgeon, like specialists at a Bakersfield Oral Surgery and Implant Center.
- Osseointegration (Healing Phase):
- The implant integrates with the jawbone over 3 to 6 months. This crucial period allows the bone cells to grow around and bond with the implant surface, ensuring a stable foundation.
- Abutment Placement:
- Once osseointegration is complete, a small connector piece called an abutment is attached to the implant. This piece will protrude through the gum line and serve as the anchor for the final crown. Sometimes, this is placed during the initial surgery.
- Restoration (Crown Placement):
- Impressions of your mouth are taken to custom-fabricate your permanent crown (or bridge).
- The crown is color-matched to your existing teeth and cemented or screwed onto the abutment.
Implant-Supported Denture Process (Full Arch Example - All-on-4)
The initial consultation, planning, extraction, and bone grafting steps are similar to single implants.
- Initial Consultation and Planning: Comprehensive evaluation, 3D imaging, and treatment planning, often involving collaboration between an oral surgeon and a restorative dentist.
- Implant Placement Surgery:
- Typically 4-6 implants are strategically placed in the jawbone, often at an angle in the posterior to utilize available bone and avoid vital structures.
- This procedure is designed to maximize stability, often allowing for "immediate loading."
- Immediate Load (Optional, but Common):
- In many All-on-4/6 cases, a temporary, fixed prosthesis is attached to the newly placed implants on the same day as surgery. This allows you to leave with a functional set of teeth, though a soft diet is required.
- Osseointegration and Healing:
- The implants heal and integrate with the bone over 3 to 6 months, while you wear the temporary prosthesis.
- Final Prosthesis Fabrication:
- Once healing is complete, new impressions are taken, and your custom-designed, permanent fixed denture is fabricated. This will be made from stronger, more durable materials like zirconia or acrylic reinforced with a titanium bar.
- Final Prosthesis Placement:
- The temporary denture is removed, and the permanent fixed denture is securely screwed onto the implants. Only a dental professional can remove this.
Cost and Insurance
Understanding the financial investment required for permanent dentures vs implants is crucial. Costs can vary significantly based on the type of procedure, the number of implants, materials used, the complexity of the case, and geographic location.
Average US Cost Ranges (Without Insurance)
These are general ranges and can vary widely:
-
Single Dental Implant:
- Implant Fixture: $1,500 - $3,000
- Abutment: $500 - $1,500
- Crown: $1,000 - $2,500
- Total for a single implant (fixture, abutment, crown): $3,000 - $7,000
- Additional costs:
- Tooth Extraction: $75 - $300 (simple), $200 - $600 (surgical)
- Bone Grafting: $250 - $1,500 (minor), $2,000 - $4,000+ (major, e.g., sinus lift)
- CT Scans/Imaging: $250 - $500
-
Implant-Supported Removable Overdenture (Full Arch):
- 2-4 Implants (lower jaw): $6,000 - $15,000
- 4-6 Implants (upper jaw): $10,000 - $25,000
- Denture Fabrication: $2,000 - $5,000 per arch
- Total for a full arch removable overdenture: $8,000 - $30,000 per arch
-
Implant-Supported Fixed Hybrid Denture (Full Arch - All-on-4/6):
- 4-6 Implants: $10,000 - $20,000
- Prosthesis Fabrication (High-Strength Materials): $10,000 - $20,000+ per arch
- Total for a full arch fixed hybrid denture: $20,000 - $40,000+ per arch
Regional Variation: Costs can fluctuate based on the cost of living in an area. For instance, procedures at a Bakersfield Oral Surgery and Implant Center might have different average pricing compared to a metropolitan area like Los Angeles or New York. It's always best to get a detailed quote from your local dental professional.
Insurance Coverage: How much does a tooth implant cost with insurance?
Dental insurance coverage for implants and implant-supported dentures is improving but still varies significantly.
- Medical vs. Dental Insurance: Sometimes, if tooth loss is due to an accident or a medical condition, some portions of the treatment (like bone grafting or extractions) might be covered by your medical insurance, especially if performed by an oral surgeon in a hospital setting.
- Dental Insurance Coverage:
- Many dental insurance plans will cover a portion of the cost, typically 10-50% after deductibles are met.
- Coverage often categorizes the implant into different components: the surgical placement of the implant, the abutment, and the crown/prosthetic. They may cover different percentages for each.
- Some plans may categorize implants as "major restorative care."
- Annual Maximums: Most dental plans have annual maximums (e.g., $1,000 - $2,500). For extensive implant work, you will likely exceed this maximum, requiring out-of-pocket payment.
- Waiting Periods: Be aware of waiting periods, which can be 6-12 months for major procedures like implants.
- Missing Tooth Clause: Some older or less comprehensive plans have a "missing tooth clause" which may exclude coverage for a tooth that was missing before you enrolled in the plan.
- Maximizing Benefits:
- Pre-authorization: Always request a pre-authorization or pre-determination from your insurance company to understand exactly what will be covered before starting treatment.
- Stagger Treatment: If your treatment spans multiple years, you might be able to utilize two annual maximums by performing some steps (e.g., implant placement) in one year and the final restoration (e.g., crown) in the next.
- HSA/FSA: Use Health Savings Accounts (HSAs) or Flexible Spending Accounts (FSAs) to pay for dental implant costs with pre-tax dollars.
Payment Plans and Financing Options
- In-Office Payment Plans: Many dental offices offer their own payment plans, allowing you to pay in installments.
- Third-Party Financing: Options like CareCredit, LendingClub, or Alphaeon Credit offer specialized healthcare financing with various interest rates and payment terms, including interest-free periods for qualified applicants.
- Personal Loans: Banks and credit unions offer personal loans that can be used for dental expenses.
Pro Tip: Don't let the initial cost deter you. Discuss all financial options with your dental provider. Investing in quality tooth replacement can prevent more expensive problems down the road and significantly improve your quality of life.
Recovery and Aftercare
Proper recovery and diligent aftercare are essential for the success and longevity of both dental implants and implant-supported dentures.
Initial Recovery (First 7-14 Days Post-Surgery)
- Pain Management: Expect some discomfort, swelling, and bruising. Over-the-counter pain relievers (ibuprofen, acetaminophen) or prescribed pain medication will help manage pain.
- Swelling Reduction: Apply ice packs to the outside of your face for 20 minutes on, 20 minutes off, for the first 24-48 hours.
- Bleeding: Minor bleeding is normal for the first day. Bite gently on gauze pads and replace as needed. Avoid vigorous rinsing.
- Diet: Stick to soft foods and liquids initially (soups, yogurt, smoothies, mashed potatoes). Gradually reintroduce firmer foods as comfort allows. Avoid hot liquids, alcohol, and spicy foods.
- Oral Hygiene:
- Avoid brushing the surgical site directly for the first few days.
- Rinse gently with a prescribed antimicrobial mouthwash (e.g., chlorhexidine) or warm salt water (1/2 tsp salt in 8 oz warm water) after 24 hours.
- Brush other areas normally.
- Activity: Rest and avoid strenuous activity for the first few days. Elevate your head when sleeping.
- Smoking/Alcohol: Absolutely avoid smoking and alcohol, as they significantly impair healing and increase the risk of implant failure.
- Follow-up: Attend all post-operative appointments as scheduled to ensure proper healing.
Long-Term Aftercare (For Implants and Permanent Dentures)
- Excellent Oral Hygiene: This is paramount for the long-term success of implants.
- Brushing: Brush at least twice a day with a soft-bristled brush, paying attention to the gum line around the implants/prosthesis.
- Flossing: Use implant-specific floss, water flossers (like a Waterpik), interdental brushes, or specialized floss threaders to clean around and under the implant crowns or fixed denture bridges. Your dentist or hygienist will recommend the best tools.
- Mouthwash: Use an antimicrobial or therapeutic mouthwash as recommended.
- Regular Dental Check-ups: Visit your dentist and dental hygienist every 6 months (or more frequently if advised) for professional cleanings and examinations. They will check the health of your gums, implants, and prosthesis, and remove any calculus buildup.
- Avoid Hard/Sticky Foods: While implants allow for a wide diet, extremely hard candies, ice, or very sticky foods can still damage the restoration or, in rare cases, the implant.
- Protect Against Bruxism: If you grind or clench your teeth (bruxism), your dentist may recommend a nightguard to protect your implants and restorations from excessive force.
- Address Issues Promptly: If you notice any pain, swelling, loosening of a crown/denture, or difficulty cleaning, contact your dentist immediately.
Pro Tip: Treat your dental implants and permanent dentures like natural teeth. Consistent, meticulous home care combined with professional dental visits is the formula for lifelong success. The ADA emphasizes the importance of regular professional cleanings and examinations for maintaining implant health.
Prevention
While dental implants and permanent dentures are excellent solutions for tooth loss, preventing the need for them in the first place is always the best approach. Prevention also extends to preventing complications once these restorations are in place.
Preventing Tooth Loss
- Maintain Excellent Oral Hygiene:
- Brush twice a day for two minutes with fluoride toothpaste.
- Floss daily to remove plaque and food particles from between teeth and under the gum line.
- Use an antimicrobial mouthwash if recommended by your dentist.
- Regular Dental Check-ups and Cleanings:
- Visit your dentist every six months for comprehensive examinations and professional cleanings. This allows for early detection and treatment of cavities and gum disease.
- Healthy Diet: Limit sugary and acidic foods and drinks, which contribute to tooth decay.
- Avoid Tobacco Products: Smoking and chewing tobacco are major risk factors for gum disease and oral cancer, both of which can lead to tooth loss.
- Limit Alcohol Consumption: Excessive alcohol intake can contribute to dry mouth, increasing the risk of decay and gum disease.
- Wear a Mouthguard for Sports: Protect your teeth from trauma during contact sports.
- Address Bruxism (Teeth Grinding): If you grind or clench your teeth, wear a nightguard to prevent excessive wear and potential tooth fractures.
- Manage Systemic Diseases: Conditions like diabetes can impact oral health. Work with your physician to manage these conditions effectively.
Preventing Complications After Implant/Denture Placement
- Diligent Home Care: As detailed in the "Recovery and Aftercare" section, maintaining superb oral hygiene is crucial to prevent peri-implantitis (gum disease around implants).
- Avoid Traumatic Forces: While durable, avoid using your implants or permanent dentures to open packages, bite on ice, or chew extremely hard objects.
- Regular Professional Maintenance: Routine check-ups allow your dentist to monitor implant health, check the integrity of the restoration, and perform specialized cleanings to prevent issues.
- Immediate Reporting of Issues: Any pain, swelling, bleeding, or noticeable changes should be reported to your dentist immediately.
Risks and Complications
While dental implants and implant-supported dentures boast high success rates, no surgical procedure is entirely without risk. Understanding potential complications helps in preparation and prompt action if issues arise.
Risks Associated with Implant Surgery
- Infection: As with any surgery, there's a risk of bacterial infection at the implant site. This is usually managed with antibiotics.
- Nerve Damage: Rarely, implant placement can injure nerves, leading to numbness, tingling, or pain in the lips, gums, tongue, or chin. This is often temporary but can be permanent in rare cases. Proper 3D imaging significantly reduces this risk.
- Sinus Perforation: For upper jaw implants, there's a small risk of the implant penetrating the sinus cavity. This is usually managed during surgery or with a sinus lift procedure.
- Implant Failure (Lack of Osseointegration): The implant may not fuse properly with the bone. Causes can include infection, insufficient bone, uncontrolled systemic diseases (like diabetes), or excessive early force on the implant. If failure occurs, the implant may need to be removed, the site allowed to heal, and a new implant placed later.
- Peri-implantitis: This is an inflammatory condition affecting the tissues surrounding a dental implant, leading to progressive bone loss around the implant. It's similar to gum disease in natural teeth and is often caused by poor oral hygiene or certain systemic conditions. It can lead to implant failure if untreated.
Risks Associated with the Prosthetic (Crowns, Bridges, Dentures)
- Screw Loosening or Fracture: The screws holding the crown or fixed denture to the abutment or implant can occasionally loosen or, rarely, fracture.
- Prosthetic Fracture or Chipping: The crown or denture material can chip, crack, or fracture, especially if subjected to excessive biting forces or trauma.
- Wear and Tear: Over time, the materials (especially acrylic for dentures) can wear down and may require repair or replacement.
- Denture Sore Spots (Removable Overdentures): While less common than with traditional dentures, ill-fitting or poorly maintained removable overdentures can still cause pressure points or irritation.
- Esthetic Issues: In rare cases, the final restoration might not perfectly match the shade or shape of surrounding teeth, or there might be minor gum recession exposing the implant collar.
Factors Increasing Risk
- Smoking: Significantly increases the risk of implant failure and peri-implantitis.
- Uncontrolled Diabetes: Impairs healing and increases infection risk.
- Certain Medications: Some medications (e.g., bisphosphonates for osteoporosis) can affect bone healing.
- Poor Oral Hygiene: A primary cause of peri-implantitis.
- Bruxism (Teeth Grinding): Can place excessive stress on implants and prosthetics.
Your dental professional will thoroughly assess your medical history and lifestyle factors to discuss these risks with you before proceeding with treatment.
Comparison Tables
To summarize the key differences and help you visualize the choices, here are two comparison tables:
Table 1: General Comparison - Permanent Dentures vs Implants
| Feature | Individual Dental Implants | Implant-Supported Removable Overdentures ("Snap-In") | Implant-Supported Fixed Dentures (e.g., All-on-4/6) |
|---|---|---|---|
| What it Replaces | Single or multiple missing teeth, individually | Full arch of missing teeth (removable) | Full arch of missing teeth (fixed) |
| Attachment | Individual crown/bridge cemented/screwed to abutment | Denture snaps onto ball/bar attachments on implants | Denture/bridge permanently screwed onto implants |
| Stability | Excellent, feels like natural tooth | Very Good, much better than traditional dentures | Excellent, very close to natural teeth |
| Bone Preservation | Excellent, prevents bone loss at implant site | Good, significantly reduces bone loss compared to traditional | Excellent, prevents bone loss at implant sites |
| Chewing Power | Excellent, nearly identical to natural teeth | Good, allows for broader diet than traditional dentures | Excellent, highly efficient chewing |
| Maintenance | Regular brushing, flossing (like natural teeth) | Daily removal and cleaning, periodic attachment replacement | Regular brushing, specialized cleaning under bridge (water flosser) |
| Removability | Non-removable (by patient) | Removable by patient daily | Non-removable (only by dentist) |
| Esthetics | Excellent, custom-matched to natural teeth | Good to Very Good, can be bulkier | Excellent, natural appearance and feel |
| Speech | No impact, no slipping | Improved over traditional, minimal impact | No impact, no slipping |
| Impact on Adjacent Teeth | None, completely independent | None | None |
| Complexity | Moderate to High | Moderate | High |
| Longevity | Implants: 25+ years to lifetime; Crowns: 10-20 years | Implants: 25+ years to lifetime; Denture: 10-20 years | Implants: 25+ years to lifetime; Denture: 10-20 years |
Table 2: Cost and Timeline Comparison
| Feature | Individual Dental Implants (per tooth) | Implant-Supported Removable Overdentures (per arch) | Implant-Supported Fixed Dentures (All-on-4/6, per arch) |
|---|---|---|---|
| Average Cost (US, without insurance) | $3,000 - $7,000 (crown included) | $8,000 - $30,000 | $20,000 - $40,000+ |
| Additional Costs (Typical) | Extractions: $75-$600; Bone Graft: $250-$4,000+ | Extractions & Grafting: may be included or extra ($500-$5,000+) | Extractions & Grafting: often included in overall package, but complex cases extra ($1,000-$7,000+) |
| Total Treatment Time | 4-9 months (longer with grafts) | 4-9 months (initial healing, then denture fabrication) | 4-9 months (often with immediate temporary fixed teeth) |
| Number of Implants | 1 implant per tooth | 2-4 implants (lower); 4-6 implants (upper) | 4-6+ implants |
| Insurance Coverage | Often 10-50% for components, subject to annual maximums ($1k-$2.5k) | Often 10-50% for components, subject to annual maximums | Often 10-50% for components, subject to annual maximums |
| Payment Options | Financing, payment plans, HSA/FSA | Financing, payment plans, HSA/FSA | Financing, payment plans, HSA/FSA |
Children / Pediatric Considerations
Dental implants and permanent dentures (implant-supported) are not suitable for children or adolescents whose jawbones are still developing. The jawbone needs to reach full maturity before implants can be placed. Placing implants in a growing jaw can interfere with natural bone development and lead to the implant appearing sunken or misaligned as the surrounding jaw continues to grow.
- Minimum Age: Generally, dental implants are recommended for individuals aged 18 or older, though some oral surgeons may wait until the early 20s for females and mid-20s for males to ensure complete jaw development.
- Adolescent Tooth Loss: If a child or teenager loses a permanent tooth, temporary solutions like space maintainers, removable partial dentures (flippers), or adhesive bridges are used until the jawbone is fully developed and implants can be considered.
- Orthodontic Treatment: Sometimes, orthodontic treatment is initiated to create optimal spacing for future implant placement once maturity is reached.
Parents of children with missing permanent teeth should consult with a pediatric dentist or orthodontist to discuss the best interim solutions and future treatment planning.
Frequently Asked Questions
How long do dental implants and permanent dentures last?
Dental implants themselves have an excellent long-term prognosis, often lasting 25 years to a lifetime with proper care, boasting a 95-98% success rate. The prosthetic restorations on top of implants (crowns, bridges, or dentures) typically last 10-20 years before potentially needing repair or replacement due to wear and tear.
Is the dental implant procedure painful?
The dental implant placement procedure is performed under local anesthesia, so you should feel no pain during the surgery. Many patients also opt for various forms of sedation (oral, IV, or nitrous oxide) to enhance comfort and reduce anxiety. Post-surgery, some discomfort, swelling, and bruising are common, but these are typically managed effectively with prescribed pain medication and over-the-counter pain relievers.
How much does a full set of teeth implants cost?
A full set of teeth implants, typically referring to a full arch of fixed implant-supported dentures (like All-on-4 or All-on-6), can cost anywhere from $20,000 to $40,000+ per arch without insurance. This comprehensive fee usually includes the implants, the abutments, and the custom-fabricated, permanent prosthesis. Costs can fluctuate based on materials, the number of implants, and the complexity of the case.
Can I get permanent dentures if I have bone loss?
Yes, often. While significant bone loss can complicate treatment, various techniques can make permanent dentures (implant-supported) possible. This includes bone grafting procedures (sinus lifts, ridge augmentation) to rebuild bone, or specialized implant techniques like All-on-4/6 which strategically place implants in areas of denser bone, or zygomatic implants for severe upper jawbone deficiency. Your oral surgeon will assess your bone quality with 3D imaging.
How long does it take to get permanent dentures or implants?
The overall treatment timeline for both individual implants and implant-supported dentures typically ranges from 4 to 9 months, and sometimes longer if significant bone grafting is required. This includes the initial healing period for implant osseointegration (3-6 months), abutment placement, and the fabrication and placement of the final restoration. Some procedures, like All-on-4, can offer immediate temporary teeth on the day of surgery.
Are permanent dentures comfortable?
Implant-supported permanent dentures (both removable overdentures and fixed hybrid dentures) are significantly more comfortable than traditional removable dentures. They eliminate the slipping, rubbing, and sore spots associated with conventional dentures, as they are securely anchored. Fixed hybrid dentures are generally considered the most comfortable, feeling very much like natural teeth.
What are the alternatives to permanent dentures and implants?
The primary alternative to dental implants and implant-supported permanent dentures is traditional removable dentures (full or partial). While more affordable and non-invasive, they lack the stability, chewing efficiency, and bone-preserving benefits of implant-supported options. Another alternative for single or a few missing teeth is a traditional dental bridge, which uses adjacent natural teeth for support and requires grinding down healthy tooth structure.
Do dental implants require special care?
Dental implants require meticulous oral hygiene similar to natural teeth. This includes brushing twice daily, flossing (often with specialized floss or a water flosser), and using interdental brushes to clean around the implant and under prosthetics. Regular dental check-ups and professional cleanings (every 6 months or as recommended) are also crucial for monitoring implant health and preventing peri-implantitis.
What is the success rate for dental implants?
Dental implants have an impressive success rate, generally reported to be 95-98% over 10 years when performed by experienced professionals and maintained with proper oral hygiene. Success rates can be slightly lower in specific situations, such as in heavy smokers or individuals with uncontrolled systemic diseases.
Can I eat normally with permanent dentures and implants?
With dental implants and fixed implant-supported dentures, you can typically eat a wide variety of foods with confidence, very much like natural teeth. Removable implant-supported overdentures also offer significantly improved chewing ability compared to traditional dentures, allowing for a much broader diet. However, extremely hard or sticky foods should still be approached with caution to prevent damage to the restorations.
When to See a Dentist
Knowing when to seek professional dental advice is crucial for maintaining your oral health, especially when considering or undergoing complex restorative treatments like dental implants or permanent dentures.
Immediate Attention (Red Flags - See a Dentist ASAP):
- Severe Pain or Swelling: If you experience intense, throbbing pain, or significant, persistent swelling around an implant site (newly placed or long-term), this could indicate infection or a complication.
- Excessive Bleeding: While some light bleeding is normal after surgery, heavy or prolonged bleeding that doesn't subside after a few hours warrants immediate contact with your dentist or oral surgeon.
- Fever or Chills: These are signs of a systemic infection and require urgent medical and dental evaluation.
- Numbness or Tingling: If you experience persistent numbness, tingling, or altered sensation in your lips, tongue, or jaw that doesn't improve after a few days post-surgery, it could indicate nerve involvement.
- Loosening of an Implant or Prosthesis: If an implant feels wobbly, or if your crown, bridge, or fixed denture becomes noticeably loose, contact your dentist immediately. This is not normal and needs prompt assessment.
- Signs of Allergic Reaction: Hives, rash, difficulty breathing, or severe itching after a dental procedure require emergency medical attention.
Scheduled Appointments (Routine Care and Consultations):
- Missing Teeth: If you are missing one or more teeth and are considering replacement options, schedule a consultation to discuss whether permanent dentures vs implants are right for you.
- Loose or Ill-Fitting Traditional Dentures: If your current dentures are uncomfortable, causing sore spots, or making it difficult to eat or speak, it's a good time to explore implant-supported alternatives.
- Prior to Tooth Extraction: If you know you need a tooth extracted, discuss immediate tooth replacement options like implants with your dentist before the extraction, as this can sometimes streamline the process.
- Regular Check-ups: Maintain your routine dental check-ups and professional cleanings (typically every six months) even after you have received implants or permanent dentures. These visits are vital for monitoring the health of your implants, gums, and overall oral health.
- Changes in Oral Health: Any new or persistent oral health concerns, such as bleeding gums, chronic bad breath, or changes in how your teeth fit together, should prompt a visit to your dentist.
Your dental professional is your best resource for personalized advice and care. Don't hesitate to reach out with any questions or concerns regarding your oral health and treatment options.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Implantologist: Complete Guide
Losing a tooth can be a significant setback, impacting not only your smile but also your ability to speak, chew, and maintain overall oral health. In fact, over 3 million Americans currently have dental implants, and that number is projected to grow significantly as more people seek a durable, n
March 8, 2026
Dentures Over Implants: Complete Guide
Missing multiple teeth or even an entire arch can profoundly impact your life, affecting everything from your ability to chew and speak to your self-confidence. For millions of Americans, traditional removable dentures have long been a solution, but they often come with compromises: slipping, discom
March 8, 2026
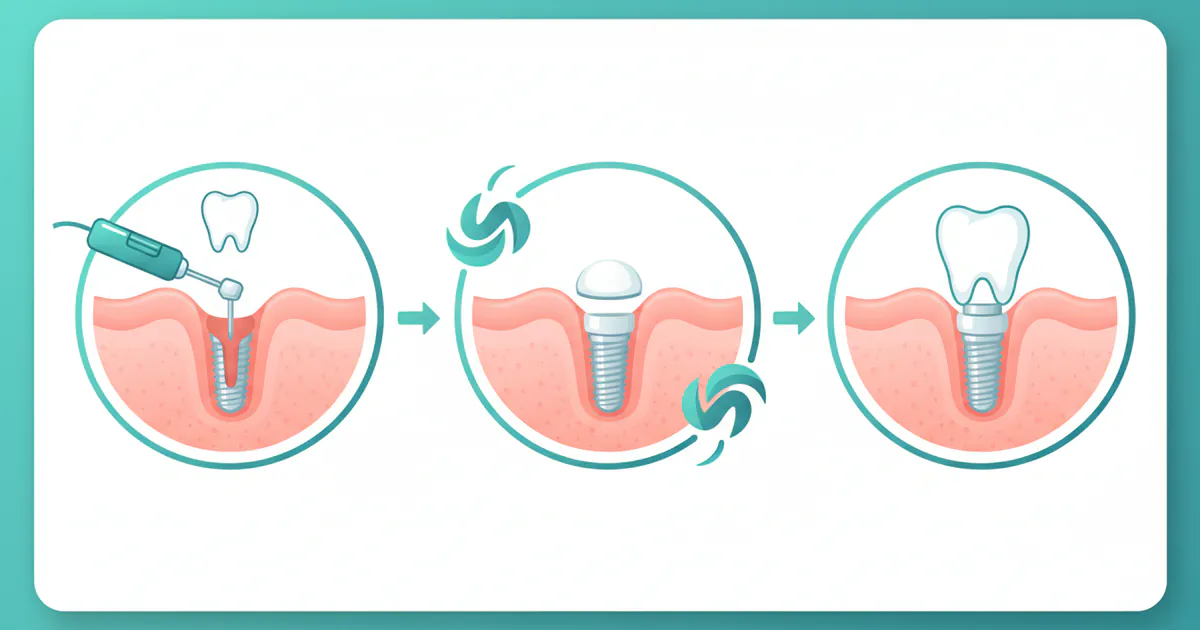
Implants Process: Complete Guide
Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the
March 8, 2026

Implants Dentaires: Complete Guide
Missing teeth can dramatically impact not just your smile, but your overall health, confidence, and quality of life. In the United States, an estimated 178 million adults are missing at least one tooth, while approximately 40 million are missing all their teeth. These statistics underscore a
March 8, 2026