Tooth Implant Recovery: Complete Guide
Key Takeaways
- When facing the prospect of tooth loss, dental implants stand out as a revolutionary solution, offering unparalleled stability, function, and aesthetics. But while the thought of a complete smile restoration is exciting, understanding the journey to get there – particularly *tooth implant recovery
When facing the prospect of tooth loss, dental implants stand out as a revolutionary solution, offering unparalleled stability, function, and aesthetics. But while the thought of a complete smile restoration is exciting, understanding the journey to get there – particularly tooth implant recovery – is crucial for a successful outcome. It's not just about the procedure itself; it's about the detailed, often multi-stage healing process that follows, ensuring your new implant integrates perfectly with your jawbone. For anyone considering or preparing for dental implant surgery, knowing what to expect during recovery can alleviate anxiety, empower you with vital aftercare knowledge, and significantly contribute to the long-term success of your implant. This comprehensive guide will walk you through every aspect of tooth implant recovery, from the initial healing phase to long-term care, helping you achieve a healthy, lasting smile.
Key Takeaways:
- Recovery Timeline: Initial healing takes 1-2 weeks, soft tissue integration 2-4 months, and complete osseointegration (bone fusion) 3-6 months, sometimes longer with bone grafts.
- Pain Management: Expect mild to moderate discomfort managed with prescribed or OTC pain relievers, typically subsiding within a few days.
- Cost: A single tooth implant (including abutment and crown) can range from $3,000 to $6,500 per tooth in the US, while full-arch solutions like All-on-4 can cost $15,000 to $30,000 per arch.
- Diet: Stick to soft foods for the first week, gradually reintroducing solid foods as comfort allows. Avoid sticky, hard, or crunchy items.
- Oral Hygiene: Gentle brushing around the surgical site after 24 hours, saline rinses, and avoiding harsh mouthwashes are critical.
- Complications: While rare, watch for persistent severe pain, swelling, fever, pus, or implant mobility, and contact your dentist immediately.
- Long-Term Success: With proper care, dental implants boast a 95-98% success rate and can last a lifetime, far surpassing the longevity of many traditional alternatives.
What Are Dental Implants? An Overview
A dental implant is a sophisticated dental prosthetic designed to replace missing teeth. Unlike traditional bridges or dentures, which rest on existing teeth or gums, an implant functions like an artificial tooth root, providing a stable foundation for a replacement tooth (a crown), bridge, or even full dentures.
The core component of a dental implant is a small, screw-shaped post, typically made from biocompatible titanium. This post is surgically placed into your jawbone beneath the gum line. Over a period of several months, a remarkable biological process called osseointegration occurs, where the titanium post fuses directly with the surrounding bone tissue. This fusion creates an incredibly strong and durable anchor, mirroring the natural strength of a tooth root. Once osseointegration is complete, a small connector piece called an abutment is attached to the implant, and then a custom-made crown (or other prosthetic) is secured to the abutment, completing the restoration.
Dental implants are widely considered the gold standard for tooth replacement due to their numerous benefits, including improved chewing ability, preserved jawbone health, prevention of adjacent tooth shifting, and a natural appearance that blends seamlessly with your existing teeth.
Types of Dental Implants and Their Recovery Implications
While the basic principle of osseointegration remains the same, dental implants come in various forms, each suited for different clinical situations and influencing the overall recovery timeline and experience.
Single Tooth Implants
As the name suggests, a single tooth implant replaces one missing tooth. This is the most common type of implant and involves placing one titanium post, topped with an abutment and a custom crown.
- Recovery Implications: Recovery for a single tooth implant is typically straightforward. The focus is on healing the single surgical site and allowing the one implant to integrate with the bone. Pain and swelling are usually localized and manageable.
Multiple Tooth Implants (Implant-Supported Bridges)
When several adjacent teeth are missing, an implant-supported bridge can be an excellent solution. Instead of relying on natural teeth for support (as with traditional bridges), this prosthetic is anchored by two or more dental implants. For instance, two implants might support a bridge of three or four crowns.
- Recovery Implications: Recovery might be slightly more extensive than a single implant due to multiple surgical sites, but the principles are similar. You might experience a bit more widespread tenderness or swelling, but overall aftercare remains consistent.
Full-Arch Implants (All-on-4, All-on-6)
For individuals missing an entire arch of teeth (upper, lower, or both), full-arch implant solutions like All-on-4 or All-on-6 provide a fixed, permanent alternative to traditional dentures. These systems involve placing four to six strategically angled implants in the jawbone to support a full set of prosthetic teeth.
- Recovery Implications: This procedure is more extensive than single or multiple implants, often involving extractions if remaining teeth are present. Consequently, the initial recovery can be more intense, with greater swelling and discomfort. However, patients often receive a temporary set of teeth on the same day as implant placement (immediate load), which, while not meant for heavy chewing, allows for immediate aesthetic and some functional improvement. The long-term osseointegration phase is critical before the final, permanent prosthesis is placed.
Zygomatic Implants
In cases of severe jawbone atrophy, especially in the upper jaw, where conventional implants aren't feasible without extensive bone grafting, zygomatic implants are an option. These longer implants anchor into the cheekbone (zygoma) rather than the jawbone.
- Recovery Implications: Zygomatic implant surgery is more complex and invasive. Recovery will typically be longer and involve more significant swelling and discomfort compared to conventional implants. This is usually a specialized procedure performed by an oral and maxillofacial surgeon.
Why Dental Implants Are Needed: Causes of Tooth Loss
Understanding why someone might need a dental implant sheds light on the overall patient profile and the context of their recovery journey. Tooth loss, which dental implants address, can occur for various reasons:
- Severe Tooth Decay: Untreated cavities can progress to infect the tooth's pulp, leading to irreversible damage, severe pain, and eventually, the need for extraction.
- Periodontal Disease (Gum Disease): Advanced gum disease, known as periodontitis, destroys the bone supporting the teeth. As bone loss progresses, teeth become loose and eventually fall out or require extraction. This is a leading cause of tooth loss in adults.
- Trauma or Injury: Accidents, sports injuries, or falls can lead to fractured teeth beyond repair or complete avulsion (knocked-out teeth).
- Congenital Conditions: Some individuals are born with congenitally missing teeth (hypodontia), where certain teeth never develop.
- Failed Root Canal Treatment: While root canals save teeth, some can fail over time, leading to infection or fracture that necessitates extraction.
- Excessive Wear and Tear: Over many years, severe grinding (bruxism) or acidic erosion can wear down teeth to a point where they are unsalvageable.
Regardless of the cause, replacing missing teeth with dental implants not only restores aesthetics and function but also prevents common issues associated with tooth loss, such as jawbone atrophy and the shifting of adjacent teeth.
The Step-by-Step Implant Placement Process
Understanding the stages of dental implant placement helps demystify the process and sets realistic expectations for recovery at each phase.
Phase 1: Initial Consultation and Treatment Planning
Your journey begins with a thorough examination by your dentist or oral surgeon. This involves:
- Comprehensive Oral Exam: Assessment of your remaining teeth, gums, and oral health.
- X-rays and 3D Cone Beam CT Scans: These imaging techniques provide detailed views of your jawbone density, nerve pathways, and sinus locations, crucial for precise implant placement.
- Medical History Review: To ensure you are a suitable candidate and identify any potential risks (e.g., uncontrolled diabetes, certain medications).
- Treatment Plan Development: Your dental professional will outline the recommended implant type, number of implants, and the overall timeline, including any necessary preliminary procedures.
Phase 2: Preliminary Procedures (If Needed)
Some patients may require preparatory procedures before implant placement to ensure a strong foundation. These can significantly impact the overall recovery timeline.
- Tooth Extraction: If damaged teeth are still present, they will be removed. Recovery for extraction typically takes 1-2 weeks for initial healing.
- Bone Grafting: If your jawbone lacks sufficient density or volume, a bone graft may be performed. This involves adding bone material (from your own body, a donor, or synthetic sources) to the implant site.
- Recovery Implications: Bone grafting requires a significant healing period, often 3-9 months, before implant placement can proceed. Initial recovery for the graft site itself is usually 2-4 weeks.
- Sinus Lift: If implants are needed in the upper jaw and the sinus cavity is too close to the implant site, a sinus lift procedure raises the sinus floor to create more bone height.
- Recovery Implications: Similar to bone grafting, a sinus lift adds several months (typically 4-9 months) to the overall timeline before implant placement.
Phase 3: Dental Implant Placement Surgery
This is the surgical phase where the titanium implant post is inserted into your jawbone.
- Anesthesia: Local anesthesia is typically used to numb the area, but sedation options (oral, IV) are often available for patient comfort.
- Incision: The dentist makes a small incision in your gum tissue to expose the jawbone.
- Drilling: A series of small holes are precisely drilled into the bone at the planned implant site.
- Implant Insertion: The titanium implant post is carefully screwed into the prepared bone.
- Suturing: The gum tissue is then closed over the implant with stitches, either completely covering it or leaving a small part exposed, depending on the chosen technique (one-stage vs. two-stage).
- Recovery Implications: This is the beginning of your immediate tooth implant recovery. You'll experience some pain, swelling, and bruising, primarily in the first 3-7 days.
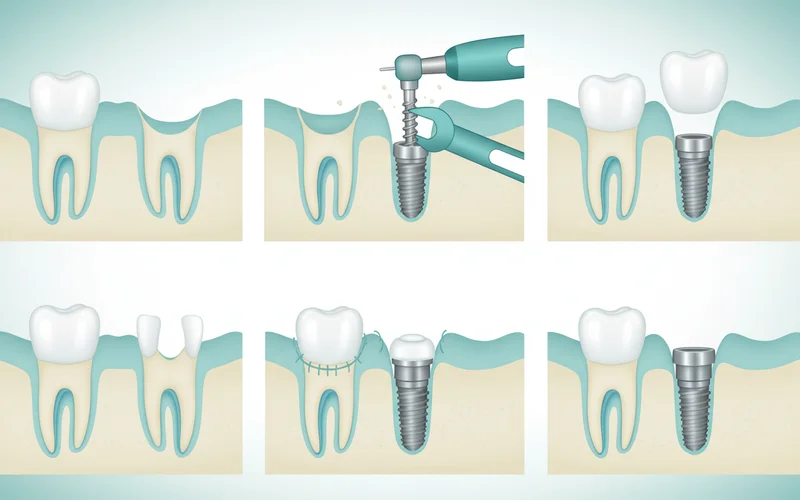
Phase 4: Osseointegration (Healing Period)
After implant placement, the crucial process of osseointegration begins. This is where your jawbone grows around and fuses with the titanium implant surface.
- Duration: This healing period typically lasts 3 to 6 months, but can vary depending on individual healing capabilities, bone quality, and whether bone grafting was performed.
- Recovery Implications: During this phase, there is usually no pain, but you'll need to be mindful of your diet to avoid putting excessive stress on the healing implant. You may wear a temporary crown or bridge that doesn't put pressure on the implant, or a temporary removable denture. This period is vital for the implant's long-term success.
Phase 5: Abutment Placement (If Two-Stage Surgery)
If the implant was fully covered by gum tissue during initial placement (two-stage surgery), a minor secondary procedure is needed to expose the implant and attach the abutment.
- Procedure: A small incision is made to uncover the top of the implant, and a healing cap or the abutment itself is attached. The gum tissue is then closed around it.
- Recovery Implications: This is a much less invasive procedure than the initial implant placement. Recovery is usually minimal, involving only mild soreness for a few days.
Phase 6: Provisional and Final Restoration Placement
Once osseointegration is complete and the abutment is securely in place, your final prosthetic tooth (crown, bridge, or denture) can be fabricated and attached.
- Impression Taking: Digital scans or traditional impressions are taken of your mouth and the abutment to design your custom restoration.
- Provisional Restoration: Sometimes a provisional (temporary) crown or bridge is placed first to allow the gums to shape naturally around it before the final restoration.
- Final Placement: Your custom-made crown, precisely matched in color, shape, and size to your natural teeth, is permanently cemented or screwed onto the abutment.
- Recovery Implications: This phase involves no surgery. You simply adjust to your new tooth. Any discomfort is usually related to the fit, which your dentist can adjust.
Pro Tip: Be patient throughout the entire implant process, especially during osseointegration. Rushing the healing can compromise the implant's long-term stability.
Tooth Implant Recovery and Aftercare: Your Detailed Guide
The success of your dental implant largely depends on meticulous recovery and aftercare. Following your dentist's instructions precisely is paramount.
Immediate Post-Surgery (First 24-72 Hours)
This is the most critical period for managing discomfort and preventing complications.
- Bleeding: Some light bleeding or oozing is normal for the first 24-48 hours. Bite gently on gauze pads placed over the surgical site, changing them every 30-45 minutes until bleeding subsides. Avoid vigorous rinsing or spitting, as this can dislodge the blood clot.
- Pain Management:
- Prescription Medication: Your dentist may prescribe pain relievers (e.g., ibuprofen 800mg, narcotics for severe cases). Take them as directed, before the local anesthesia wears off if possible.
- Over-the-Counter (OTC) Medication: For milder pain, ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) can be effective. Avoid aspirin or other blood thinners unless specifically advised by your dentist or physician, as they can increase bleeding.
- Swelling: Swelling is common and can peak around 48-72 hours.
- Ice Packs: Apply ice packs to the outside of your face near the surgical site for 15-20 minutes on, 15-20 minutes off, during the first 24-48 hours. This helps reduce swelling and bruising.
- Head Elevation: Keep your head elevated, even while sleeping, to minimize swelling.
- Diet:
- Liquid/Soft Diet: For the first 24-48 hours, stick to liquids and very soft, cool foods. Examples include smoothies, yogurt, applesauce, mashed potatoes, lukewarm soup (avoiding hot temperatures that can increase bleeding).
- Avoid: Hot foods/drinks, spicy foods, crunchy or hard foods (nuts, chips, popcorn), sticky foods, and anything requiring significant chewing.
- Straws: Do NOT use straws, as the sucking motion can dislodge blood clots and lead to a painful dry socket (though less common with implant surgery than extractions, it's still a risk).
- Oral Hygiene:
- No Rinsing for 24 hours: Avoid rinsing your mouth for the first 24 hours to protect the blood clot.
- Gentle Rinsing (after 24 hours): After 24 hours, gently rinse with a warm salt water solution (1/2 teaspoon salt in 8 ounces of warm water) 3-4 times a day, especially after meals. Do not spit vigorously; let the water gently fall out of your mouth.
- Brushing: Avoid brushing directly on the surgical site for the first few days. You can gently brush other teeth, being careful not to disturb the healing area.
- Activity:
- Rest: Rest is crucial. Avoid strenuous physical activity, heavy lifting, or bending over for at least 48-72 hours, as these can increase blood pressure and bleeding.
- Smoking/Alcohol: Absolutely avoid smoking and alcohol for at least the first week, ideally longer. Smoking significantly impairs healing and increases the risk of implant failure. Alcohol can thin your blood and interfere with medications.
Short-Term Recovery (Weeks 1-2)
As initial discomfort subsides, the focus shifts to protecting the healing site.
- Diet Progression: Gradually reintroduce softer solid foods, ensuring you chew away from the surgical site. Continue to avoid hard, sticky, or chewy foods.
- Oral Hygiene:
- Continue warm salt water rinses.
- You can start gently brushing the surgical site with a soft-bristled toothbrush, being very careful not to disturb stitches or the implant.
- Your dentist might prescribe an antimicrobial mouthwash (like chlorhexidine) for a limited period. Use as directed.
- Stitches: If non-dissolving stitches were used, they will be removed by your dentist usually around 7-14 days post-surgery. Dissolvable stitches will disappear on their own.
- Follow-up Appointments: Attend all scheduled follow-up appointments. Your dentist will monitor healing, remove stitches if needed, and provide further instructions.
Long-Term Recovery (Months 1-6 and Beyond)
The bulk of implant healing, osseointegration, occurs during this period.
- Osseointegration: This phase is critical. While you won't feel it happening, your jawbone is actively fusing with the implant. It's vital not to disrupt this process. Continue to follow any dietary restrictions given by your dentist, especially if you have a temporary restoration that isn't fully load-bearing.
- Oral Hygiene: Maintain excellent oral hygiene with regular brushing (twice daily) and flossing. Once your final crown is placed, treat it like a natural tooth. Special brushes or flossers may be recommended for cleaning around implants.
- Regular Dental Check-ups: Continue with routine dental cleanings and check-ups (typically every 6 months). Your dentist will monitor the implant's health and the surrounding gum tissue.
- Protection: If you grind or clench your teeth (bruxism), your dentist may recommend a nightguard to protect your implant and natural teeth from excessive forces.
Pro Tip: Your commitment to excellent oral hygiene and adherence to dietary restrictions are the most impactful factors in ensuring successful osseointegration and the longevity of your implant.

Risks and Complications During Recovery
While dental implant procedures have a high success rate (often 95-98%), it's important to be aware of potential risks and complications, especially during the recovery phase.
Common, Minor Complications
- Pain and Swelling: Expected after surgery, usually manageable with medication and ice.
- Bruising: Common, especially in the first few days, typically resolves within a week.
- Numbness: Temporary numbness due to local anesthesia is normal. Persistent numbness can indicate nerve involvement (see below).
- Minor Bleeding: Oozing is normal; heavy, persistent bleeding is not.
More Serious (But Rare) Complications
- Infection: Bacteria can enter the surgical site, leading to pain, swelling, pus, and fever. This requires immediate antibiotic treatment and potentially surgical intervention.
- Nerve Damage: Though rare, especially with careful planning, implants can sometimes be placed too close to a nerve, leading to permanent numbness, tingling, or pain in the lips, chin, or tongue.
- Sinus Problems: If an implant is placed in the upper jaw, it can sometimes protrude into the sinus cavity, leading to pain, pressure, or chronic sinusitis. This may require further surgery to correct.
- Implant Failure (Lack of Osseointegration): This is when the implant fails to fuse with the jawbone. It can be due to:
- Insufficient Bone Quality/Quantity: If the bone isn't strong enough.
- Infection: At the surgical site.
- Excessive Early Pressure: Putting too much force on the implant during healing.
- Smoking: A major risk factor.
- Certain Medical Conditions: Uncontrolled diabetes, autoimmune diseases.
- Poor Oral Hygiene: Leading to peri-implantitis.
- Peri-Implantitis: This is a serious inflammatory condition affecting the gum and bone tissues surrounding a dental implant, similar to periodontal disease. It's usually caused by bacterial infection and can lead to bone loss and eventual implant failure if not treated. Signs include redness, swelling, bleeding, and pus around the implant.
- Fracture of the Implant or Restoration: While durable, implants or their crowns can fracture under extreme biting forces, trauma, or material fatigue over many years.
Pro Tip: Your active participation in monitoring your recovery and immediately reporting any unusual symptoms to your dental professional is your best defense against serious complications.
Cost of Dental Implants and Insurance Coverage in the US
Dental implants are a significant investment in your oral health and quality of life. Understanding the cost breakdown and insurance landscape is vital for planning.
Average US Cost Ranges for Dental Implants
The cost of dental implants varies widely based on several factors: the number of implants, the type of implant system, the need for preparatory procedures (e.g., bone grafts, extractions), the geographic location of the dental practice, and the experience of the dental professional.
| Implant Type & Components | Average US Cost Range (Per Tooth/Arch) | What's Included |
|---|---|---|
| Single Tooth Implant | $3,000 - $6,500 | Includes implant post, abutment, and custom crown. Does NOT include preliminary procedures like extraction or bone graft. |
| Implant-Supported Bridge | $6,000 - $15,000+ | For 2-4 missing teeth supported by 2 implants. Cost varies significantly based on number of implants and bridge units. |
| Full Arch (All-on-4/6) | $15,000 - $30,000+ per arch | Includes 4-6 implants and a full arch of prosthetic teeth (temporary and permanent). This is a complex procedure often requiring significant upfront cost. |
| Bone Grafting | $200 - $3,000+ | Per site. Varies by material (synthetic vs. patient's own bone) and complexity of the graft. |
| Tooth Extraction | $75 - $400+ | Per tooth. Varies by complexity (simple vs. surgical). |
| Sinus Lift | $1,500 - $2,500+ per side | Varies by technique (internal vs. external) and grafting material. |
Regional Variations:
- Urban vs. Rural: Costs tend to be higher in major metropolitan areas (e.g., New York, Los Angeles) compared to rural regions.
- Practice Overhead: Location, rent, technology, and staff salaries all influence pricing.
Dental Insurance and Implants
This is a complex area, as many standard dental insurance plans have historically considered dental implants a "cosmetic" procedure and excluded them from coverage. However, this is slowly changing as implants become more recognized for their health benefits.
- Coverage Limitations: Many plans still do not cover the implant post itself. However, they might cover related procedures:
- Extraction: Often covered at 50-80%.
- Bone Grafting/Sinus Lift: Sometimes covered, especially if deemed medically necessary for jaw function.
- The Crown/Bridge: The prosthetic part (crown, bridge) might be covered under major restorative benefits (e.g., 50%).
- Diagnostic Procedures: X-rays and consultations are usually covered at a higher percentage.
- Medical Insurance: If the tooth loss is due to a medical condition (e.g., trauma, tumor removal) rather than routine decay, your medical insurance might cover a portion of the implant procedure. It's crucial to consult with both your dental and medical insurance providers.
- Annual Maximums: Most dental insurance plans have annual maximums (e.g., $1,000-$2,000 per year). Since implant treatment often exceeds this, you might need to spread treatment over two calendar years to maximize benefits.
- Affordable Dentures and Implants Reviews: When researching affordability, look for practices that openly discuss financing options and clearly break down costs. Many dental practices offer in-house payment plans or work with third-party financing companies (e.g., CareCredit) that provide low or no-interest payment options. Some dental schools also offer implant services at a reduced cost.
Pro Tip: Always get a detailed, written treatment plan from your dentist that clearly outlines all costs. Then, submit this plan to your dental insurance provider before starting treatment to understand your exact out-of-pocket expenses.
Prevention of Implant Complications and Maintaining Longevity
Prevention isn't just about preventing tooth loss; it's also about preventing complications after implant placement and ensuring your implants last a lifetime.
- Rigorous Oral Hygiene: This is the cornerstone of implant longevity.
- Brushing: Brush twice daily for at least two minutes with a soft-bristled toothbrush. Consider an electric toothbrush for superior plaque removal.
- Flossing: Floss daily, ensuring you clean thoroughly around the implant and under the crown. Special implant flosses, water flossers (Waterpik), or interdental brushes can be very effective in reaching tight spaces.
- Mouthwash: Use an ADA-approved antimicrobial mouthwash if recommended by your dentist, but avoid alcohol-based rinses which can dry out tissues.
- Regular Dental Check-ups and Cleanings:
- Visit your dentist every 6 months (or more frequently if advised) for professional cleanings and examinations.
- Your dental hygienist will use specialized tools designed for implants to avoid scratching the implant surface.
- Your dentist will check the health of your implant, gums, and surrounding bone, looking for early signs of peri-implantitis or other issues.
- Avoid Harmful Habits:
- Smoking: As mentioned, smoking is a major risk factor for implant failure and peri-implantitis. Quitting is crucial for implant success.
- Excessive Alcohol Consumption: Can impair healing and overall oral health.
- Bruxism (Teeth Grinding/Clenching): If you grind or clench your teeth, especially at night, discuss a custom nightguard with your dentist. The excessive forces can damage implants and crowns over time.
- Chewing Hard Objects: Avoid chewing on ice, pens, fingernails, or using your teeth as tools. This can chip or fracture your implant crown or even damage the implant itself.
- Manage Underlying Health Conditions: If you have conditions like diabetes, it's vital to keep them well-controlled, as they can impact your body's ability to heal and fight infection around implants.
- Healthy Diet: A balanced diet supports overall health, including strong bones and healthy gums, which are crucial for implant stability.
Children / Pediatric Considerations for Dental Implants
Dental implants are generally not recommended for children or adolescents whose jaws are still developing. Here's why:
- Jawbone Growth: Children's jawbones are continually growing and changing. Placing an implant in a growing jaw would interfere with normal development and could lead to the implant being out of alignment as the surrounding bone matures.
- Permanent Tooth Eruption: Implants are placed after all permanent teeth have erupted and the jaw has reached its adult size, typically in the late teens or early twenties (around 18-20 for girls, and 20-22 for boys, but individual variations exist).
- Alternatives for Children: If a child loses a permanent tooth due to trauma or other reasons, temporary solutions like space maintainers, removable partial dentures, or adhesive bridges (Maryland bridges) are used until they are old enough for an implant. These maintain space, prevent adjacent teeth from shifting, and restore aesthetics.
- Exceptions: In extremely rare cases, such as severe trauma or congenital defects where other options are not viable, an implant might be considered with extensive planning and consultation among a team of specialists, but this is highly unusual.
Pro Tip: If your child has lost a permanent tooth, consult with a pediatric dentist or orthodontist to discuss appropriate temporary solutions and long-term treatment planning.
Frequently Asked Questions
H3: How painful is dental implant recovery?
Initial discomfort after dental implant surgery is normal and typically comparable to a tooth extraction. Most patients describe it as mild to moderate pain, manageable with prescribed or over-the-counter pain relievers. The most intense pain usually subsides within 3-7 days, with residual soreness for a week or two.
H3: How long does the entire dental implant process take from start to finish?
The entire process, from initial consultation to the placement of the final crown, can take anywhere from 3 to 9 months, and sometimes up to a year or more if extensive bone grafting or preliminary procedures are required. The longest phase is the osseointegration period, where the implant fuses with your jawbone.
H3: Can I get a temporary tooth while waiting for my implant to heal?
Yes, in many cases, a temporary restoration can be provided. This might be a temporary crown, a removable partial denture (flipper), or even an immediate load temporary bridge for full-arch cases. These temporary solutions help maintain aesthetics and some function while the implant integrates, but usually cannot withstand heavy chewing forces.
H3: What is the success rate of dental implants?
Dental implants boast a very high success rate, generally ranging from 95% to 98% when performed by experienced professionals and maintained with good oral hygiene. Factors like bone quality, overall health, and adherence to aftercare instructions significantly influence success.
H3: Are there any alternatives to dental implants?
Yes, common alternatives include traditional dental bridges (which require altering adjacent healthy teeth) and removable partial or full dentures. While often more affordable upfront, these alternatives do not offer the same stability, bone preservation benefits, or long-term durability as dental implants.
H3: What foods should I strictly avoid during recovery?
For the first few days, strictly avoid hot, spicy, hard, crunchy, sticky, or chewy foods. This includes nuts, popcorn, chips, tough meats, raw vegetables, and sticky candies. Gradually introduce softer solids as comfort allows, always chewing away from the surgical site.
H3: Can I smoke or drink alcohol after getting a dental implant?
It is strongly advised to avoid smoking and alcohol for at least the first week, and ideally for the entire healing period. Smoking significantly impairs blood flow and healing, dramatically increasing the risk of implant failure and complications like peri-implantitis. Alcohol can thin your blood and interfere with medications.
H3: What is osseointegration and why is it important?
Osseointegration is the biological process where your jawbone directly fuses with the titanium surface of the dental implant. It's crucial because this fusion creates the incredibly strong, stable, and permanent anchor that allows the implant to function like a natural tooth root. Without successful osseointegration, the implant will not be stable.
H3: Will my dental implant feel like a natural tooth?
Once the final crown is placed, most patients report that their dental implant feels very much like a natural tooth. It functions normally for chewing, speaking, and smiling. Unlike dentures, implants don't slip or click, providing a sense of confidence and comfort similar to your original teeth.
H3: What if my implant fails? Can it be replaced?
In the rare event of implant failure (e.g., due to lack of osseointegration or infection), the implant may need to be removed. In many cases, after a period of healing and potentially further bone grafting, another implant can be placed successfully in the same site.
When to See a Dentist During Recovery
While some discomfort and swelling are normal during tooth implant recovery, certain signs indicate a potential complication that requires immediate attention from your dental professional.
Emergency Situations (Call Your Dentist Immediately):
- Excessive or Persistent Bleeding: If bleeding is heavy, continuous, and doesn't subside after applying pressure with gauze for 30-45 minutes, or if it suddenly worsens after the first 24 hours.
- Severe, Uncontrolled Pain: If pain is intense, throbbing, and not relieved by prescribed pain medication, or if it suddenly escalates several days after surgery.
- Significant Swelling Beyond 3-4 Days: While swelling is normal, if it continues to worsen after 72 hours, extends to your neck, or makes swallowing difficult, it could indicate an infection.
- Fever or Chills: These are classic signs of a systemic infection.
- Pus or Discharge: Any yellow, green, or foul-smelling discharge from the surgical site.
- Numbness that Doesn't Subside: While temporary numbness from anesthesia is expected, if numbness persists for several days in your lips, chin, or tongue, it could indicate nerve involvement.
- Wiggling or Movement of the Implant: If you feel the implant itself moving (not just the temporary crown or healing cap), this is a serious sign of potential implant failure.
Routine Concerns (Contact Dentist for Advice):
- Loose or Lost Stitches: If your stitches come out prematurely, especially within the first few days.
- Difficulty Opening Your Mouth: Mild stiffness is common, but significant trismus (inability to open your mouth wide) could be concerning.
- Minor Soreness or Bruising: If it's manageable but you have questions about its duration or intensity.
- Questions about Diet or Medication: Any uncertainty regarding your post-operative instructions.
Always err on the side of caution. If something feels "not right" or you have any concerns about your recovery, don't hesitate to contact your dental professional. They are your best resource for guidance and support throughout your tooth implant journey.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Implantologist: Complete Guide
Losing a tooth can be a significant setback, impacting not only your smile but also your ability to speak, chew, and maintain overall oral health. In fact, over 3 million Americans currently have dental implants, and that number is projected to grow significantly as more people seek a durable, n
March 8, 2026
Dentures Over Implants: Complete Guide
Missing multiple teeth or even an entire arch can profoundly impact your life, affecting everything from your ability to chew and speak to your self-confidence. For millions of Americans, traditional removable dentures have long been a solution, but they often come with compromises: slipping, discom
March 8, 2026
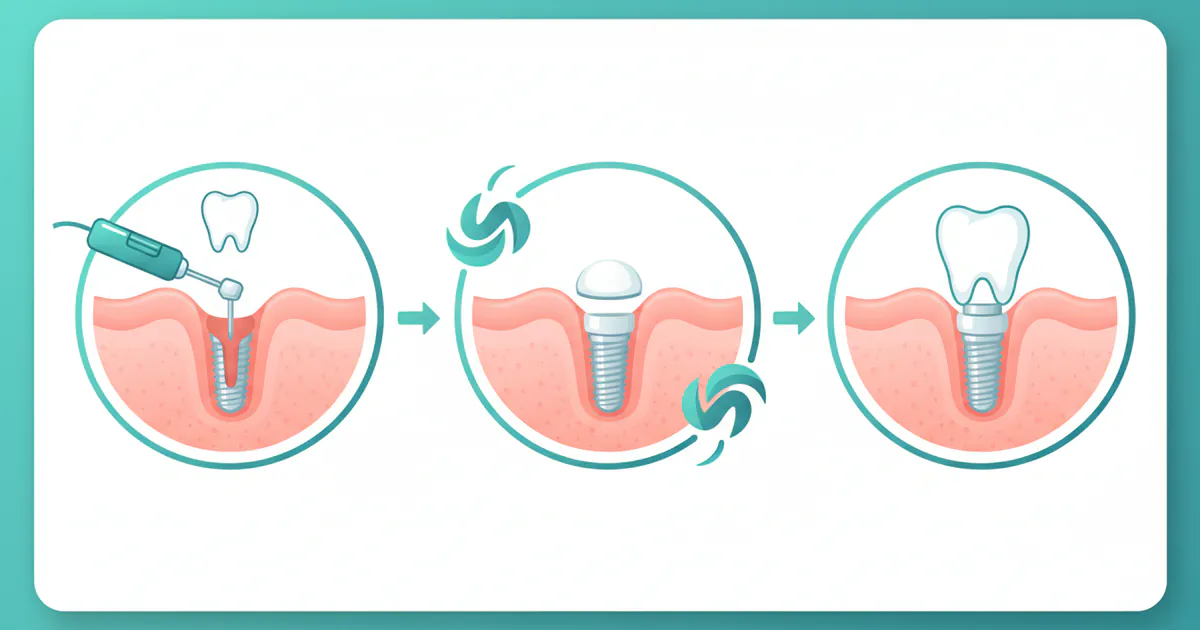
Implants Process: Complete Guide
Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the
March 8, 2026

Implants Dentaires: Complete Guide
Missing teeth can dramatically impact not just your smile, but your overall health, confidence, and quality of life. In the United States, an estimated 178 million adults are missing at least one tooth, while approximately 40 million are missing all their teeth. These statistics underscore a
March 8, 2026