How to Fix Receding Gums
Key Takeaways
- Receding gums, a common dental concern affecting millions of Americans, can be more than just a cosmetic issue; it's often a significant indicator of underlying oral health problems that require attention. **Understanding how to fix receding gums is crucial for maintaining your oral health, preventi
Receding gums, a common dental concern affecting millions of Americans, can be more than just a cosmetic issue; it's often a significant indicator of underlying oral health problems that require attention. Understanding how to fix receding gums is crucial for maintaining your oral health, preventing tooth loss, and preserving your overall well-being. This condition occurs when the gum tissue surrounding the teeth pulls back or wears away, exposing more of the tooth's root. The exposed root can lead to increased sensitivity, aesthetic concerns, and, if left untreated, can even compromise the stability of your teeth. The American Dental Association (ADA) estimates that gum recession affects a substantial portion of the adult population, particularly as they age, with mild to moderate forms present in over 50% of adults aged 30 and older.
This comprehensive guide from SmilePedia.net will delve deep into the causes, signs, and, most importantly, the effective treatment options available to address receding gums. We'll explore everything from lifestyle changes and non-surgical interventions to advanced surgical procedures, providing clear insights into what to expect during treatment, recovery, costs, and crucial prevention strategies. By understanding this condition thoroughly, you can make informed decisions to protect your smile and ensure a lifetime of optimal dental health.
Key Takeaways:
- Early Detection is Key: Look for increased tooth sensitivity, visibly longer teeth, bleeding gums, and changes in gum color or texture as early signs.
- Causes Vary: Recession can stem from aggressive brushing, genetics, poor oral hygiene leading to gum disease (periodontitis), tobacco use, or orthodontic issues.
- Non-Surgical Options First: For mild recession, deep cleaning (scaling and root planing), antibiotics, and correcting oral hygiene habits are often the initial steps, costing $150-$400 per quadrant.
- Surgical Interventions: Gum grafting (connective tissue, free gingival, pedicle grafts) and the Pinhole Surgical Technique are effective for moderate to severe recession, with costs ranging from $600-$3,000 per tooth.
- Recovery & Aftercare: Post-surgical recovery typically takes 1-2 weeks for initial healing, with full healing taking several months. Strict adherence to aftercare instructions is vital.
- Prevention is Paramount: Gentle brushing with a soft-bristled toothbrush, daily flossing, regular dental check-ups, and addressing contributing factors like smoking are essential.
- Insurance Coverage: While often considered cosmetic, many treatments for medically necessary recession (e.g., due to periodontitis) are partially covered by dental insurance.
``
What It Is / Overview
Gum recession refers to the process in which the margin of the gum tissue surrounding the teeth pulls back, or retracts, exposing more of the tooth, or the tooth's root. When the root surface becomes exposed, it can lead to a host of problems. Unlike the enamel-covered crown of the tooth, the root surface is covered by cementum, a softer tissue that is more vulnerable to decay and abrasion. This exposure can make your teeth appear longer, create gaps between them, and result in heightened sensitivity to hot, cold, or sweet foods and drinks. Beyond the cosmetic implications, receding gums can indicate underlying gum disease, specifically periodontitis, which is an infection of the tissues that hold your teeth in place. If left unaddressed, gum recession can weaken the tooth's support structure, leading to loose teeth and eventually tooth loss. It's a progressive condition that often develops gradually, making it easy to overlook until it becomes more advanced.

Types / Variations
Gum recession isn't a single condition but rather a symptom that can manifest in different ways and be classified according to severity and cause. Understanding these variations helps dental professionals determine the most appropriate periodontitis treatment and intervention.
The most common classification system for gum recession is the Miller Classification, though newer systems like the Cairo Classification are also used.
Miller Classification of Gingival Recession
- Class I: Recession that does not extend to the mucogingival junction (the line where the firm, attached gum tissue meets the looser, movable lining mucosa). There is no loss of interdental papilla (gum tissue between teeth) or bone. This type is generally easier to treat successfully.
- Class II: Recession extends to or beyond the mucogingival junction. Similar to Class I, there is no loss of interdental papilla or bone.
- Class III: Recession extends to or beyond the mucogingival junction, with some loss of interdental papilla or bone in the interdental areas. This means some of the gum tissue between your teeth has also receded or been lost.
- Class IV: Recession extends to or beyond the mucogingival junction, with severe loss of interdental papilla and bone. This is the most severe form, often making complete root coverage difficult or impossible.
Other Categorizations
- Localized Recession: Affects only one or a few teeth.
- Generalized Recession: Affects multiple teeth throughout the mouth.
- Marginal Recession: Refers specifically to the loss of gum tissue at the gum line.
- Interproximal Recession: Loss of gum tissue between the teeth, often associated with bone loss.
The specific type and severity of your gum recession will significantly influence the recommended approach for how to fix receding gums, ranging from simple adjustments to oral hygiene to complex surgical procedures.
Causes / Why It Happens
Receding gums can be attributed to a variety of factors, often a combination of several. Identifying the root cause is essential for effective treatment and preventing further progression.
1. Periodontal Disease (Gum Disease)
This is by far the most common cause of gum recession. Periodontal disease, particularly its advanced stage known as periodontitis, is a bacterial infection of the gum tissue and bone that support your teeth. The bacteria in plaque and tartar irritate the gums, leading to inflammation, swelling, and eventually the destruction of the soft tissue and bone that hold your teeth in place. As the gums become inflamed and detach from the teeth, they pull back, exposing the root. Poor oral hygiene is a primary driver of periodontitis.
2. Aggressive Tooth Brushing
Brushing your teeth too hard, using a hard-bristled toothbrush, or incorrect brushing techniques can physically wear away gum tissue and tooth enamel over time. This mechanical trauma can push the gums down, leading to recession. Many people mistakenly believe that harder brushing leads to cleaner teeth.
3. Insufficient Oral Hygiene
While aggressive brushing is detrimental, neglecting oral hygiene is equally harmful. Inadequate brushing and flossing allow plaque to accumulate and harden into tartar (calculus). Tartar buildup creates a rough surface that harbors bacteria, leading to gingivitis (the mildest form of gum disease) and eventually periodontitis. The presence of tartar near the gum line can also physically push the gums away from the teeth.
4. Genetics
Some individuals are simply predisposed to gum recession due to genetic factors. If one or both of your parents experienced gum recession, you might have a higher risk, regardless of how well you care for your teeth. This includes naturally thinner or more fragile gum tissue.
5. Tobacco Use
Smoking and other forms of tobacco use significantly increase the risk of developing gum disease and recession. Tobacco impairs blood flow to the gums, making them more susceptible to infection and hindering their ability to heal. Smokers are far more likely to have gum recession than non-smokers.
6. Hormonal Changes
Fluctuations in hormone levels, particularly in women during puberty, pregnancy, and menopause, can make gums more sensitive and vulnerable to gum disease and recession. Increased estrogen and progesterone levels can lead to increased blood flow to the gums, making them more prone to inflammation.
7. Teeth Grinding and Clenching (Bruxism)
Chronic grinding or clenching of teeth can put excessive force on the teeth and the surrounding gum tissue and bone. Over time, this stress can contribute to the detachment of gum tissue and lead to recession. This is especially true if there's an existing predisposition to gum issues.
8. Misaligned Teeth or Malocclusion
Teeth that are crooked, crowded, or misaligned can create areas where plaque and tartar are difficult to remove, increasing the risk of gum disease. Additionally, teeth that are not properly aligned can place uneven pressure on the gums and bone, leading to recession on certain teeth.
9. Oral Piercings
Piercings in the lip or tongue can irritate the gum tissue, especially if they constantly rub against the gums. This chronic irritation can lead to the wearing away of gum tissue over time.

10. Trauma or Injury
A sudden injury to the mouth, such as a sports injury or an accident, can cause localized gum recession. Dental procedures that are not performed meticulously can also sometimes contribute to localized trauma.
Understanding these varied causes is the first step in creating an effective treatment plan and establishing preventive measures to ensure the long-term health of your gums and teeth.
Signs and Symptoms
Recognizing the signs of gum disease and recession early is critical for timely intervention and preventing more serious complications. Since gum recession often progresses slowly, many people may not notice it until it becomes significant.
Here's what to look for:
1. Increased Tooth Sensitivity
This is one of the most common early indicators. When gum tissue recedes, the softer dentin of the tooth root, which contains tiny tubules leading to the nerve, becomes exposed. This exposure makes teeth highly sensitive to hot, cold, sweet, or acidic foods and drinks, and even to touch or cold air.
2. Visibly Longer Teeth
As gums pull back, more of the tooth surface, including the root, becomes visible. This gives the appearance that your teeth are "growing longer" than they used to be. You might notice a noticeable difference in length between affected teeth and unaffected ones.
3. Change in Gum Color or Texture
Healthy gums are typically firm, pink, and stippled (like an orange peel). Gums affected by recession or gum disease may appear red, swollen, or purple. The texture might become puffy or tender. The gum margin itself might appear ragged or uneven.
4. Bleeding Gums
Gums that bleed easily during brushing, flossing, or even when eating hard foods are a significant sign of gum disease, often gingivitis or early periodontitis, which can lead to recession. Healthy gums should not bleed.
5. Swollen or Tender Gums
Inflamed gums, a hallmark of gum disease, can appear swollen, puffy, and be tender to the touch. This inflammation is a precursor to the gum tissue detaching and receding.
6. Bad Breath (Halitosis)
Persistent bad breath, even after brushing, can be an indicator of bacterial accumulation beneath the gum line, a common feature of gum disease that contributes to recession.
7. Gaps Between Teeth
As gums recede, the small triangles of gum tissue (papillae) between your teeth can also shrink, creating visible spaces or "black triangles" where there were none before. Food can easily get trapped in these new spaces.
8. Loose or Shifting Teeth
In advanced stages of gum recession, especially when accompanied by significant bone loss due to periodontitis, the teeth may start to feel loose or shift in position. This occurs because the supporting structures are compromised.
9. Pain at the Gum Line
While often painless initially, some people might experience a dull ache or discomfort at the gum line, especially during brushing or after consuming certain foods.
If you notice any of these signs, particularly persistent sensitivity or visible changes in your gum line, it's crucial to schedule an appointment with your dentist or a periodontist promptly. Early diagnosis can prevent the condition from worsening and allow for less invasive treatment options.
Treatment Options
The approach to how to fix receding gums depends heavily on the severity of the recession, its underlying causes, and the overall oral health of the patient. Treatments range from non-surgical interventions for mild cases to advanced surgical procedures for more significant recession.
A. Non-Surgical Treatments
These methods are typically employed for mild recession, when the primary cause is gum inflammation or aggressive brushing, or as an initial step before surgical intervention.

1. Scaling and Root Planing (Deep Cleaning)
- What it is: This is a non-surgical procedure performed by a dentist or dental hygienist. Scaling involves removing plaque and tartar (calculus) from above and below the gum line. Root planing smooths the root surfaces, making it harder for bacteria to reattach and promoting gum reattachment.
- Pros: Highly effective for treating gum disease (periodontitis treatment), relatively non-invasive, can halt progression of recession, improves gum health.
- Cons: Not suitable for advanced recession where significant tissue is lost, may cause temporary sensitivity.
- Cost (US): Typically $150-$400 per quadrant (a quarter of your mouth), depending on the severity and region.
2. Antibiotics
- What it is: After deep cleaning, oral or topical antibiotics (mouth rinses or gels containing antimicrobials) may be prescribed to control bacterial infection, especially if pockets between the gums and teeth are present.
- Pros: Reduces bacterial load, aids healing.
- Cons: Can have side effects (e.g., digestive upset with oral antibiotics), temporary solution if not combined with good oral hygiene.
- Cost (US): Varies based on prescription, but generally $10-$50 for a course of oral antibiotics or an antimicrobial rinse.
3. Correcting Oral Hygiene Practices
- What it is: Guidance from your dentist on proper brushing techniques (soft-bristled toothbrush, gentle circular motions), daily flossing, and using an antiseptic mouthwash.
- Pros: Prevents further recession, cost-effective, empowers the patient.
- Cons: Requires consistent patient adherence, cannot reverse existing recession.
- Cost (US): Minimal, primarily the cost of a new soft toothbrush (around $5-$15) and floss.
4. Desensitizing Agents/Varnishes
- What it is: For mild sensitivity caused by exposed roots, dentists can apply desensitizing agents, fluoride varnishes, or prescribe special toothpastes.
- Pros: Provides temporary relief from sensitivity.
- Cons: Does not address the underlying recession, needs reapplication.
- Cost (US): $30-$70 per application, desensitizing toothpaste $5-$15.
B. Surgical Treatments
When recession is moderate to severe, or non-surgical methods are insufficient, surgical intervention by a periodontist is often necessary to restore gum tissue.
1. Gum Grafting Surgery
This is the most common surgical approach for how to fix receding gums. The goal is to cover the exposed tooth root with new gum tissue, reducing sensitivity and preventing further recession and bone loss. There are several types:
-
a. Connective Tissue Graft:
- What it is: The most common type. A small piece of tissue is removed from the roof of your mouth (palate) from underneath a flap of skin (subepithelial connective tissue) and then stitched to the gum tissue around the exposed root.
- Pros: Excellent aesthetic results, good blood supply from the underlying tissue, provides a natural look.
- Cons: Requires two surgical sites (palate and recipient site), can cause temporary discomfort at the palate donor site.
- Cost (US): $800-$3,000 per tooth, depending on complexity and region.
-
b. Free Gingival Graft:
- What it is: Similar to a connective tissue graft, but a small piece of tissue is taken directly from the surface of the roof of your mouth and attached to the exposed area.
- Pros: Can provide a thicker band of gum tissue, good for areas needing more robust tissue.
- Cons: Palate donor site can be more uncomfortable, results might not be as aesthetically pleasing as connective tissue grafts due to a potential color mismatch.
- Cost (US): $700-$2,500 per tooth.
-
c. Pedicle Graft (Lateral or Coronal Repositioned Flap):
- What it is: This procedure uses gum tissue from adjacent to the receded tooth. A flap of gum tissue is partially cut, leaving one edge attached (the pedicle) to maintain its blood supply, and then stretched over the exposed root and stitched into place.
- Pros: Uses tissue from the patient's own mouth (same color), only one surgical site, good blood supply promotes healing.
- Cons: Only possible if there is enough healthy gum tissue adjacent to the receded area; cannot be used if generalized recession is present.
- Cost (US): $600-$2,000 per tooth.
2. Pinhole Surgical Technique (PST) / Chao Pinhole Surgical Technique™
- What it is: A minimally invasive procedure. Instead of cutting tissue, a small hole is made in the gum above the affected tooth. Specialized instruments are used to loosen the gum tissue and gently slide it down to cover the exposed root. Collagen strips are then inserted to help stabilize the gum.
- Pros: No cutting or stitches, less pain and swelling, faster recovery than traditional grafting, multiple teeth can be treated in one session.
- Cons: Requires specific training and certification for the periodontist, not suitable for all types of recession (e.g., severe bone loss), long-term efficacy studies are still ongoing compared to traditional grafting.
- Cost (US): Often $2,000-$4,000 per tooth due to its specialized nature.
3. Guided Tissue Regeneration (GTR)
- What it is: When recession is accompanied by bone loss, GTR can be performed to regenerate lost bone and tissue. A small piece of mesh-like material (membrane) is inserted between the gum tissue and the bone. This membrane creates space for bone and tissue cells to grow, preventing the gum tissue from growing into the area where bone should be.
- Pros: Regenerates lost bone and attachment, addresses both soft tissue and bone defects.
- Cons: More complex surgical procedure, longer healing time, higher risk of complications.
- Cost (US): Can range from $1,500-$4,000 per tooth, often combined with a graft.
Pro Tip: Always seek consultation from a board-certified periodontist to determine the most appropriate treatment option for your specific case. They specialize in gum health and can offer the best assessment and care.
Comparison Table of Common Recession Treatments
| Treatment Type | Best For | Procedure Description | Pros | Cons | Typical Cost (US, per tooth/quadrant) | Recovery Time |
|---|---|---|---|---|---|---|
| Scaling & Root Planing | Mild recession due to gum disease | Deep cleaning above and below gum line, smoothing roots. | Non-invasive, addresses infection, prevents progression. | Not for significant tissue loss, temporary sensitivity. | $150-$400 per quadrant | 1-2 days |
| Connective Tissue Graft | Moderate to severe recession (aesthetic) | Tissue taken from under palatal flap, stitched to exposed root. | Excellent aesthetics, natural look, durable. | Two surgical sites, palate discomfort. | $800-$3,000 | 1-2 weeks |
| Free Gingival Graft | Moderate recession (needs thicker tissue) | Tissue taken directly from palatal surface, stitched to exposed root. | Creates thick, robust gum tissue. | Palate discomfort, potential color mismatch. | $700-$2,500 | 1-2 weeks |
| Pedicle Graft | Localized recession with adjacent healthy gum | Flap of adjacent gum tissue rotated over exposed root. | Single surgical site, good blood supply, natural color. | Requires sufficient adjacent tissue, limited applicability. | $600-$2,000 | 1-2 weeks |
| Pinhole Surgical Technique (PST) | Generalized mild to moderate recession | Minimally invasive, gums loosened through a small hole, repositioned over roots. | No cutting/stitches, less pain, faster recovery. | Specialized training needed, not for all cases, newer. | $2,000-$4,000 | 1-2 days |
Step-by-Step Process: What to Expect During Gum Grafting Surgery
Let's detail the process for a common surgical treatment, such as a connective tissue graft, as an example for how to fix receding gums surgically.
1. Initial Consultation and Diagnosis
- Your periodontist will conduct a thorough examination, including measuring pocket depths, assessing the amount of recession, and taking X-rays. They will discuss your medical history, oral hygiene habits, and lifestyle factors.
- A detailed treatment plan will be presented, explaining the chosen grafting technique, expected outcomes, potential risks, and cost. This is your opportunity to ask questions.
2. Pre-Operative Preparation
- You may be prescribed antibiotics to take before the surgery to prevent infection.
- Instructions will be given regarding eating and drinking before the procedure, especially if sedation is used.
- Arrange for transportation if you will be sedated.
3. The Surgical Procedure (Typically 1-2 hours per site)
- Anesthesia: Local anesthesia will be administered to numb the surgical site (both the recipient site and the donor site, if applicable). Sedation options (oral, nitrous oxide, IV sedation) may also be offered to help you relax.
- Recipient Site Preparation: The periodontist will gently clean the exposed root surface and prepare the area where the new gum tissue will be placed. This often involves creating a small flap or pocket to receive the graft.
- Donor Tissue Harvest (for Connective or Free Gingival Grafts): For a connective tissue graft, a small incision is made on the roof of your mouth, and a thin piece of tissue from underneath the outer layer is carefully removed. For a free gingival graft, the tissue is taken directly from the surface. The donor site is then typically closed with a few stitches, or a protective dressing may be applied.
- Graft Placement: The harvested tissue is meticulously placed over the exposed root surface at the recipient site.
- Suturing: The graft is secured in place with very fine sutures. A periodontal dressing may be applied over the surgical area to protect it during the initial healing phase.
``
4. Post-Operative Instructions
- Detailed instructions for aftercare, including pain management, diet, oral hygiene, and activity restrictions, will be provided before you leave.
- You'll schedule follow-up appointments to monitor healing and remove sutures.
Cost and Insurance
Understanding the financial aspects of how to fix receding gums is a significant concern for many patients. Costs can vary widely based on the type of procedure, the number of teeth involved, the complexity of the case, the periodontist's fees, and your geographic location within the US.
Average US Price Ranges (Per Tooth/Quadrant)
- Scaling and Root Planing: $150-$400 per quadrant
- Connective Tissue Graft: $800-$3,000 per tooth
- Free Gingival Graft: $700-$2,500 per tooth
- Pedicle Graft: $600-$2,000 per tooth
- Pinhole Surgical Technique (PST): $2,000-$4,000 per tooth
- Guided Tissue Regeneration (GTR): $1,500-$4,000 per tooth (often in addition to a graft)
These ranges can fluctuate. For example, procedures in major metropolitan areas like New York City or Los Angeles might be on the higher end, while those in rural areas might be lower.
Insurance Coverage Details
Dental insurance often provides some coverage for procedures deemed medically necessary to treat gum disease or prevent further damage.
- Diagnostic Procedures: X-rays, exams, and periodontal charting are usually covered at a high percentage (e.g., 80-100%).
- Non-Surgical Treatments: Scaling and root planing (often coded as D4341 or D4342) are typically covered by most dental insurance plans, usually at 50-80% after your deductible.
- Surgical Treatments: Gum grafts (various codes depending on the type) are often covered, especially if they are necessary to prevent tooth loss, address severe sensitivity, or treat periodontal disease. Coverage can range from 20-70% depending on your plan's major restorative or periodontal benefits.
- Cosmetic Exclusion: If the primary reason for the graft is purely aesthetic, insurance may deny coverage. Your periodontist will typically phrase the necessity in terms of health benefits (e.g., preventing further bone loss, reducing sensitivity, protecting root surfaces) to maximize coverage.
- Pinhole Surgical Technique (PST): Since PST is a newer technique, some insurance companies may consider it experimental or may not have specific codes for it, which could affect coverage. It's crucial to verify with your provider.
- Deductibles and Annual Maximums: Be aware of your plan's deductible (the amount you pay before insurance starts covering) and annual maximum (the total amount your insurance will pay in a year). Periodontal procedures can quickly use up your annual maximum.
Pro Tip: Always get a pre-authorization or pre-determination from your insurance company before undergoing significant treatment. This will give you a clear understanding of what will be covered and what your out-of-pocket expenses will be. Your periodontist's office staff can usually assist with this process.
Recovery and Aftercare
Proper recovery and diligent aftercare are paramount to the success of any gum recession treatment, especially surgical procedures. Following your periodontist's instructions precisely will minimize complications and optimize healing.
Immediate Post-Procedure (First 24-48 Hours)
- Pain Management: Expect some discomfort. Your periodontist will prescribe pain medication or recommend over-the-counter options like ibuprofen. Take them as directed.
- Swelling: Apply an ice pack to the outside of your face for 20 minutes on, 20 minutes off, during the first 24 hours to reduce swelling.
- Bleeding: Minor bleeding is normal. Avoid rinsing vigorously or spitting, as this can dislodge blood clots. If bleeding is heavy, apply gentle pressure with a clean gauze pad.
- Diet: Stick to soft, cool foods. Avoid hot, spicy, crunchy, or acidic foods that can irritate the surgical site. Examples include yogurt, smoothies, mashed potatoes, and soups.
- Rest: Limit physical activity and get plenty of rest to aid healing. Avoid strenuous exercise for at least 24-48 hours, or longer if advised.
First Week
- Oral Hygiene:
- Avoid Brushing/Flossing Directly on the Surgical Site: Your periodontist will likely instruct you to avoid brushing or flossing the treated area for a specific period (usually 1-2 weeks).
- Gentle Rinsing: You may be prescribed an antiseptic mouthwash (e.g., chlorhexidine) to gently rinse your mouth, especially after meals. Do not use over-the-counter mouthwashes containing alcohol.
- Brush Other Areas: Continue to gently brush and floss the rest of your mouth to maintain overall hygiene.
- Diet: Continue with soft foods, gradually reintroducing firmer textures as comfort allows. Avoid chewing directly on the grafted area.
- Medications: Continue antibiotics if prescribed, and take pain medication as needed.
- Avoid Irritants: Refrain from smoking, drinking alcohol, and using straws (the sucking motion can dislodge the graft) for at least a week, preferably longer.
- Sutures: Some sutures are dissolvable and will disappear on their own. Non-dissolvable sutures will be removed at a follow-up appointment, typically within 7-14 days.

Weeks 2-4 and Beyond
- Gradual Return to Normal Hygiene: Your periodontist will guide you on when and how to resume gentle brushing and flossing near the treated area, often recommending an extra-soft toothbrush.
- Avoid Aggressive Brushing: Permanently adopt a gentle brushing technique to prevent future recession.
- Diet: Most patients can return to a normal diet within 2-4 weeks, but continue to be cautious with very hard or sticky foods.
- Follow-up Appointments: Regular check-ups are essential to monitor healing and assess the long-term success of the graft.
- Full Healing: While initial healing of the soft tissue takes 1-2 weeks, complete maturation and integration of the gum tissue can take several months (3-6 months). The treated area may look slightly different in color or texture during this period.
Adhering to these aftercare guidelines is crucial for the successful integration of the gum graft and achieving the desired outcome of covering your exposed tooth roots.
Prevention
Preventing receding gums is far more desirable than treating them, and many of the preventive measures align with general excellent oral hygiene. Consistent effort can significantly reduce your risk.
1. Master Proper Oral Hygiene
- Brush Gently: Use a soft-bristled toothbrush. Hold it at a 45-degree angle to your gum line and use gentle, circular strokes. Avoid scrubbing vigorously back and forth. The goal is to clean, not scour.
- Floss Daily: Floss at least once a day to remove plaque and food particles from between your teeth and under the gum line, where your toothbrush can't reach.
- Antiseptic Mouthwash: Consider using an antimicrobial mouthwash recommended by your dentist to reduce bacteria, especially if you have a history of gum disease.
- Replace Your Toothbrush: Change your toothbrush every 3-4 months, or sooner if the bristles are frayed. Frayed bristles are less effective and can be abrasive.
2. Regular Dental Check-ups and Cleanings
- Schedule Bi-Annual Visits: Visit your dentist or dental hygienist every six months for professional cleanings and check-ups. These visits allow for the removal of stubborn plaque and tartar that home brushing cannot eliminate, and early detection of signs of gum disease.
- Periodontal Evaluations: If you have risk factors for gum disease, your dentist may recommend more frequent periodontal evaluations.
3. Address Underlying Causes
- Quit Tobacco: If you smoke or use other tobacco products, quitting is one of the most impactful steps you can take for your gum health and overall health.
- Manage Bruxism: If you grind or clench your teeth, your dentist can recommend a custom night guard to protect your teeth and gums from excessive force.
- Correct Misaligned Bites: Orthodontic treatment can correct crooked teeth and bite issues, making them easier to clean and distributing biting forces more evenly.
- Monitor Oral Piercings: If you have an oral piercing, ensure it's not irritating your gums. Consider removing it if it's causing trauma.
4. Healthy Lifestyle Choices
- Balanced Diet: A diet rich in fruits, vegetables, and whole grains supports overall health, including gum health. Limit sugary foods and drinks that promote bacterial growth.
- Stay Hydrated: Drinking plenty of water helps wash away food particles and maintains saliva flow, which neutralizes acids and helps protect teeth and gums.
- Manage Stress: Chronic stress can negatively impact your immune system, potentially making you more susceptible to gum disease.
5. Be Mindful of Medications
Certain medications can cause dry mouth, which reduces saliva's protective effects and increases the risk of gum disease. Discuss any medications you are taking with your dentist.
By adopting these preventive strategies, you can significantly reduce your risk of developing gum recession and maintain a healthy, beautiful smile for years to come.
Risks and Complications
While treatments for receding gums are generally safe and highly effective, it's important to be aware of the potential risks and complications, both from the recession itself and from its treatment.
Risks and Complications of Untreated Receding Gums
- Increased Tooth Sensitivity: Exposed tooth roots are highly sensitive to temperature changes and touch, leading to chronic discomfort.
- Root Decay: The root surface (cementum) is softer than enamel and more susceptible to cavities and decay, which can progress rapidly.
- Tooth Loss: As recession advances, especially with associated bone loss due to periodontitis, the supporting structure of the tooth weakens, leading to mobility and potentially tooth extraction.
- Aesthetic Concerns: Visibly longer teeth and "black triangles" between teeth can significantly impact a person's smile and self-confidence.
- Difficulty Cleaning: Irregular gum lines and exposed root surfaces can make proper oral hygiene more challenging, exacerbating plaque buildup and the risk of further recession and decay.
- Gum Disease Progression: Untreated recession is often a symptom of underlying periodontitis, which can continue to worsen, leading to deeper pockets, more bone loss, and infection.
Risks and Complications of Gum Recession Treatment (e.g., Grafting)
While uncommon, surgical procedures carry some inherent risks:
- Pain and Discomfort: Post-operative pain, swelling, and bruising are common, particularly at the donor site (if tissue is taken from the palate).
- Infection: Though rare with proper antibiotic use and sterile techniques, infection can occur at either the donor or recipient site.
- Bleeding: Excessive or prolonged bleeding, while uncommon, is a potential complication.
- Graft Failure: The graft may not "take" successfully, especially if there's poor blood supply, infection, or if post-operative instructions aren't followed. This means the tissue does not integrate or survive.
- Nerve Damage: In rare cases, nerve damage at the donor site on the palate can lead to temporary or, very rarely, permanent numbness or altered sensation.
- Root Sensitivity: While grafting aims to reduce sensitivity, some patients may experience temporary or, less commonly, persistent sensitivity in the treated tooth.
- Aesthetic Mismatch: With free gingival grafts, there can sometimes be a color or texture mismatch between the grafted tissue and the surrounding gums, though periodontists strive for the best aesthetic outcome.
- Relapse: Despite successful treatment, if the underlying causes (e.g., aggressive brushing, unmanaged gum disease) are not addressed, recession can reoccur.
Your periodontist will discuss all potential risks and benefits specific to your recommended treatment plan. Choosing an experienced and board-certified periodontist significantly minimizes these risks.
Children / Pediatric Considerations
Receding gums are far less common in children than in adults, but they can occur. When recession is observed in a child, it often warrants careful investigation by a pediatric dentist or a periodontist to identify the underlying cause.
Common reasons for gum recession in children can include:
- Aggressive Tooth Brushing: Children, especially those still learning proper brushing techniques, can sometimes brush too hard, leading to physical trauma to the gums.
- Orthodontic Treatment: Braces can sometimes cause temporary or localized recession if brackets or wires irritate the gum tissue, or if teeth are moved too rapidly or into an unfavorable position.
- High Frenum Attachment: A frenum is a fold of tissue that connects the lip or cheek to the gum. If a frenum is attached too high or too close to the gum line, it can pull on the gum tissue, causing recession.
- Trauma: Injuries to the mouth or teeth can damage gum tissue.
- Eruption Issues: Sometimes, teeth erupt in an abnormal position, leading to thin or receded gum tissue over the root.
- Early-Onset Periodontitis: Though rare, aggressive forms of gum disease can affect children and adolescents, leading to significant gum recession and bone loss.
Treatment for children often focuses on addressing the cause: modifying brushing habits, monitoring orthodontic treatment, or in some cases, a minor surgical procedure called a frenectomy to reposition a high frenum. Gum grafting might be considered in specific cases, but often after permanent teeth have fully erupted and growth is stable. Parents should seek prompt dental evaluation if they notice any signs of gum recession in their child.
Cost Breakdown
A more granular look at the cost of how to fix receding gums provides a better understanding of potential expenses. Prices fluctuate by region, the expertise of the dental professional, and the complexity of the case.
| Service/Procedure | Average Low (US) | Average Mid (US) | Average High (US) | Notes |
|---|---|---|---|---|
| Initial Consultation/Exam (Periodontist) | $100 | $250 | $400 | Often includes X-rays and charting. May be partially covered by insurance. |
| Scaling & Root Planing (per quadrant) | $150 | $250 | $400 | For addressing gum disease, often covered 50-80% by insurance. |
| Connective Tissue Graft (per tooth) | $800 | $1,500 | $3,000 | The most common graft, good aesthetic outcome. Varies based on location and periodontist experience. |
| Free Gingival Graft (per tooth) | $700 | $1,300 | $2,500 | For areas needing more robust tissue. |
| Pedicle Graft (per tooth) | $600 | $1,100 | $2,000 | Only if sufficient adjacent tissue is available. |
| Pinhole Surgical Technique (PST) (per tooth) | $2,000 | $3,000 | $4,000 | Specialized procedure, often priced higher due to required training. Check insurance coverage. |
| Guided Tissue Regeneration (GTR) (per tooth) | $1,500 | $2,500 | $4,000 | For bone regeneration, often an add-on or combined procedure. |
| Follow-up Visits (post-surgery) | $50 | $150 | $300 | Typically included in the overall surgical fee for a certain period, but confirm with your periodontist. |
| Pain Medication (prescription) | $10 | $30 | $70 | Cost of actual medication. |
| Antiseptic Mouthwash (prescription) | $15 | $25 | $40 | Often prescribed post-surgery. |
With vs. Without Insurance
- With Insurance: If your procedure is deemed medically necessary (e.g., due to periodontitis treatment or to prevent root decay), dental insurance may cover a portion. For surgical procedures, this often means 20-70% coverage after your deductible is met, up to your annual maximum. For a $1,500 gum graft, you might pay $450-$1,200 out of pocket, assuming a 50-70% coverage and factoring in deductibles.
- Without Insurance: You will be responsible for the full cost. Many periodontists offer discounts for upfront cash payments.

Payment Plans and Financing Options
- In-Office Payment Plans: Some dental offices offer their own interest-free payment plans, allowing you to pay in installments.
- Third-Party Financing: Options like CareCredit or LendingClub provide specialized healthcare credit cards with low or no-interest promotional periods for qualifying applicants.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): These tax-advantaged accounts allow you to set aside pre-tax money for healthcare expenses, including dental procedures.
Cost-Saving Tips
- Preventive Care: The best cost-saving tip is to prevent recession in the first place through excellent oral hygiene and regular check-ups.
- Early Intervention: Addressing recession in its early stages often requires less invasive and less expensive treatments.
- Shop Around (Carefully): While expertise is paramount, comparing prices from a few reputable periodontists in your area might reveal differences.
- Negotiate: For uninsured patients, politely inquire if there's a cash discount available.
- Maximize Insurance Benefits: Plan procedures around your deductible and annual maximums. If you have extensive work, you might spread it across two calendar years to utilize two annual maximums.
Frequently Asked Questions
What happens if receding gums are left untreated?
If left untreated, receding gums can lead to increased tooth sensitivity, higher risk of root decay, bacterial infection (periodontitis), eventual loosening of teeth, and potentially tooth loss. The aesthetic appearance of your smile can also be significantly impacted.
Is fixing receding gums painful?
Modern dental techniques and anesthesia make procedures like gum grafting surprisingly manageable. You will receive local anesthesia, and sedation options are available. Post-procedure, discomfort is common but usually well-controlled with prescribed pain medication, typically lasting a few days to a week.
How long does it take for gums to heal after treatment?
Initial healing of the soft tissue after gum grafting typically takes 1-2 weeks. During this time, sutures are removed, and significant discomfort subsides. However, complete integration and maturation of the grafted tissue, leading to full strength and stability, can take several months, usually 3 to 6 months.
Are there any natural remedies to fix receding gums?
No, there are no scientifically proven "natural remedies" that can reverse or fix receding gums. While good oral hygiene practices (like gentle brushing and flossing) are crucial for prevention and maintaining gum health, once gum tissue has receded, it cannot grow back on its own. Professional dental intervention is required.
Can receding gums grow back on their own?
Unfortunately, gum tissue cannot regenerate once it has receded. The only way to restore lost gum tissue is through professional treatments like gum grafting surgery or techniques like the Pinhole Surgical Technique, which effectively reposition existing gum tissue.
What is the success rate of gum grafting?
Gum grafting procedures generally have a high success rate, often exceeding 90% for root coverage, especially for Class I and II recession types. Success depends on factors like the patient's overall health, adherence to post-operative instructions, and the expertise of the periodontist.
Does dental insurance cover gum grafting?
Yes, dental insurance often covers a portion of gum grafting procedures if they are deemed medically necessary to treat gum disease, prevent root decay, or reduce sensitivity. However, coverage varies widely by plan, with typical coverage ranging from 20-70% after deductibles, up to annual maximums. Purely cosmetic procedures might not be covered.
Can orthodontics cause or worsen receding gums?
Orthodontic treatment can sometimes contribute to gum recession, particularly if teeth are moved too quickly, moved into an unfavorable position (e.g., too far outside the bone), or if there's aggressive force application. However, carefully planned orthodontics can also improve gum health by aligning teeth, making them easier to clean and distributing biting forces more evenly. A thorough evaluation by an orthodontist and periodontist is recommended.
When to See a Dentist
Recognizing when to seek professional dental care for receding gums is paramount to preventing irreversible damage and maintaining your oral health.
Clear Warning Signs That Need Immediate Attention:
- Significant or Rapid Recession: If you notice a sudden or dramatic pulling back of your gum tissue on one or more teeth.
- New or Worsening Tooth Sensitivity: Persistent or increasing sensitivity to hot, cold, or sweets, indicating exposed root surfaces.
- Visible Tooth Roots: If you can clearly see the yellow or darker root portion of your teeth above the gum line.
- Loose or Shifting Teeth: This is a serious sign of advanced gum disease and significant bone loss, requiring urgent attention.
- Pain or Discomfort at the Gum Line: Any persistent ache, tenderness, or throbbing sensation originating from your gums.
- Abscess or Swelling: A painful, pus-filled swelling in your gums can indicate an active infection that needs immediate treatment.
- Bleeding Gums with Pain: While some bleeding during brushing can be gingivitis, bleeding accompanied by significant pain or pus suggests a more severe issue.
Red Flags vs. Routine Care Guidance:
- Red Flags (See a dentist immediately): Sudden severe pain, rapid recession, extreme sensitivity preventing eating/drinking, signs of infection (pus, fever), or noticeably loose teeth. These could indicate an emergency or rapidly progressing disease.
- Routine Care (Schedule an appointment soon): Gradual recession, mild or intermittent sensitivity, mild bleeding during brushing that persists, or if you simply suspect your gums are receding. These situations warrant a scheduled appointment to assess the condition and develop a preventive or treatment plan.
The American Dental Association recommends regular check-ups every six months. If you notice any of the above signs or have concerns about your gum health, don't wait for your next routine appointment. Contact your dentist or a periodontist promptly. Early detection and intervention are key to successfully addressing receding gums and preserving your smile.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
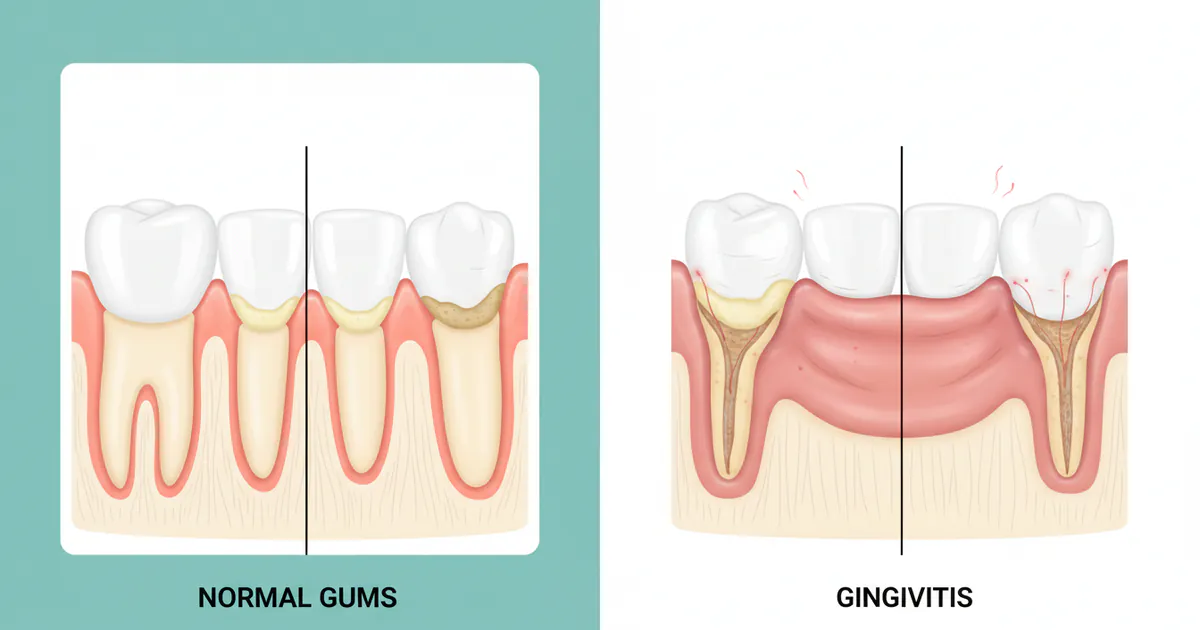
Normal Gums vs Gingivitis: Complete Comparison Guide
Did you know that nearly half of American adults over 30 show signs of gum disease, a condition that can range from mild inflammation to severe infection leading to tooth loss? Understanding the difference between healthy gums and those affected by early gum disease, known as gingivitis, is cruc
February 22, 2026
Can You Get Rid of Gingivitis
More than 50% of American adults aged 30 or older suffer from some form of gum disease, with gingivitis being the earliest and most common stage. This often silent condition, marked by inflammation of the gums, can seem daunting, leading many to wonder: can you get rid of gingivitis? The good ne
February 22, 2026
What Causes Receding Gums
Receding gums, a condition where the gum tissue surrounding the teeth pulls back or wears away, exposing more of the tooth or the tooth's root, affects a significant portion of the adult population in the United States. In fact, estimates suggest that **up to 88% of people over the age of 65 have on
February 22, 2026
Signs of Gingivitis: Complete Guide
Did you know that nearly half of American adults aged 30 and older suffer from some form of gum disease? While that statistic might sound alarming, the good news is that the earliest and most common stage, gingivitis, is entirely reversible. Recognizing the signs of gingivitis early is your
February 22, 2026