Normal Gums vs Gingivitis: Complete Comparison Guide
Key Takeaways
- Did you know that nearly half of American adults over 30 show signs of gum disease, a condition that can range from mild inflammation to severe infection leading to tooth loss? Understanding the difference between healthy gums and those affected by early gum disease, known as gingivitis, is cruc
Normal Gums vs Gingivitis: Complete Comparison Guide
Did you know that nearly half of American adults over 30 show signs of gum disease, a condition that can range from mild inflammation to severe infection leading to tooth loss? Understanding the difference between healthy gums and those affected by early gum disease, known as gingivitis, is crucial for maintaining your oral health and preventing more serious complications. This comprehensive guide will illuminate the distinct characteristics of normal gums vs gingivitis, explore the underlying causes of gum issues including what causes gum recession, detail effective periodontal treatment options, and equip you with the knowledge to safeguard your smile. We'll delve into the signs, symptoms, costs, and prevention strategies, ensuring you have a complete roadmap to healthier gums.
Key Takeaways:
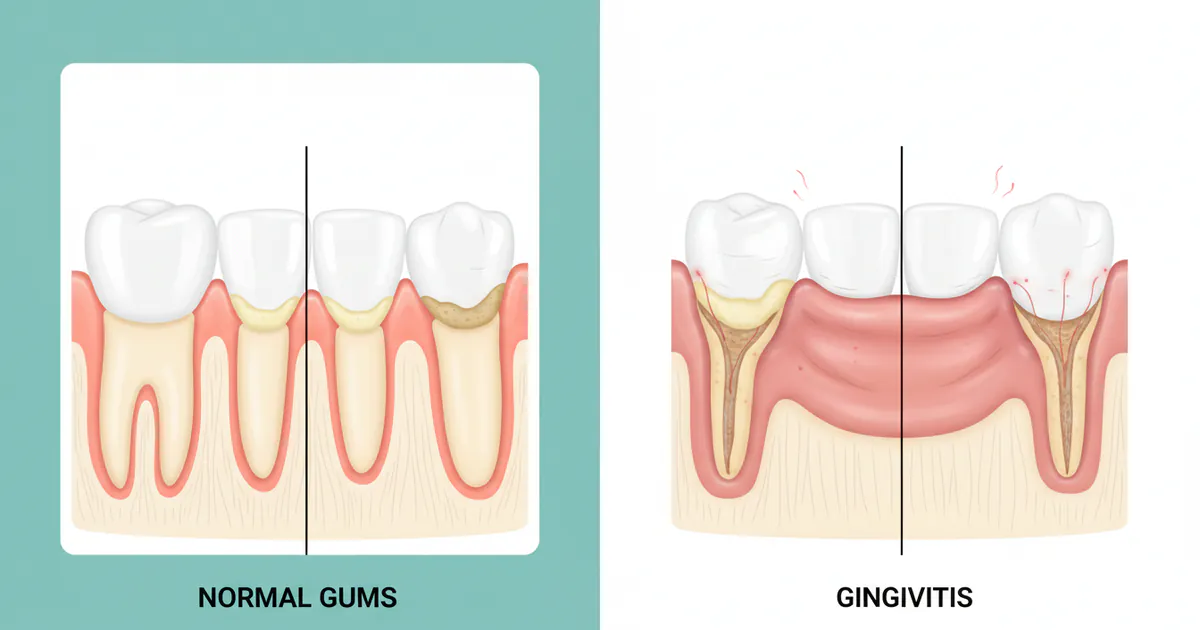
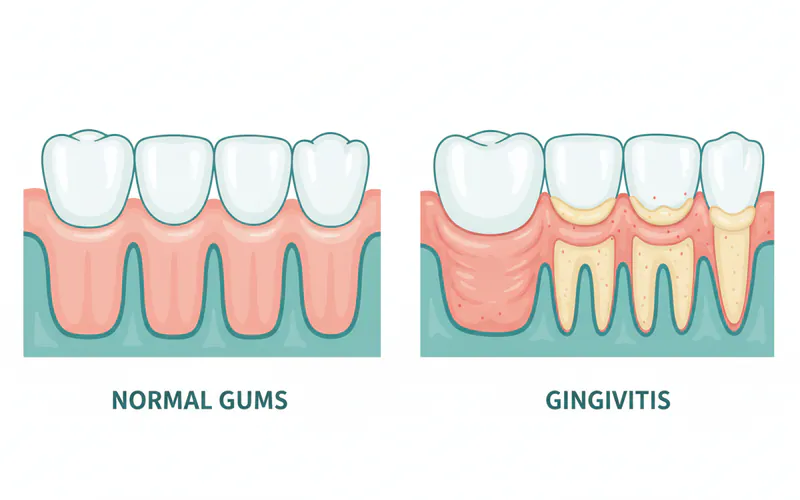
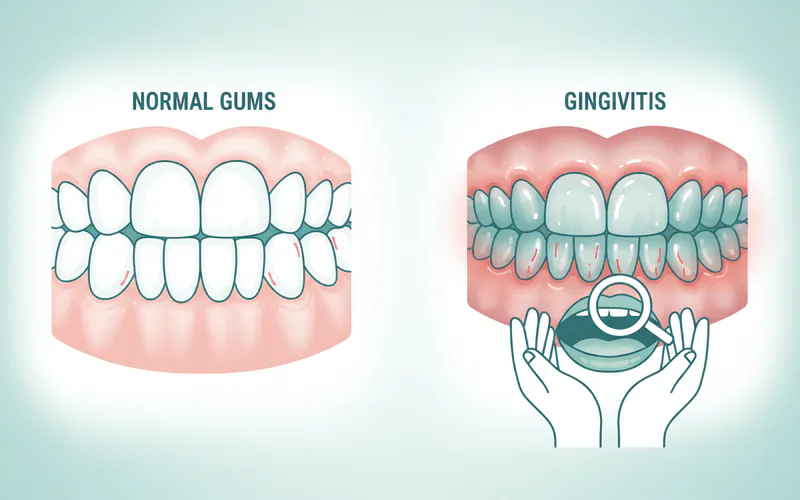
- Normal Gums: Appear pale pink, firm, stippled, and do not bleed when brushed or flossed.
- Gingivitis: Characterized by red, swollen, tender gums that bleed easily; it is the mildest and reversible form of gum disease.
- Primary Cause: Inadequate oral hygiene leading to plaque buildup is the leading cause of gingivitis.
- Reversibility: Gingivitis is fully reversible with professional cleaning (prophylaxis) and improved home care, typically within 1-2 weeks.
- Progression Risk: If left untreated, gingivitis can advance to periodontitis, an irreversible condition that leads to bone loss and potential tooth loss.
- Treatment Costs: A professional dental cleaning (prophylaxis) for gingivitis generally ranges from $75 to $200 without insurance, while deep cleaning (scaling and root planing) for early periodontitis can cost $200 to $400 per quadrant.
- Prevention is Key: Consistent daily brushing, flossing, and regular dental check-ups (every 6 months) are vital for preventing both gingivitis and its progression.
Understanding Normal Gums: The Foundation of Oral Health
Healthy gums are the unsung heroes of your mouth, providing a protective seal around your teeth and safeguarding the underlying bone. Recognizing the signs of normal, healthy gums is the first step in identifying when something might be amiss.
What Are Normal Gums?
Normal gums, scientifically known as gingiva, are the soft tissues that surround the bases of your teeth and cover the alveolar bone. They play a critical role in supporting your teeth and protecting them from bacteria and trauma. When your gums are healthy, they create a strong, resilient barrier.
Characteristics of Healthy Gum Tissue
- Color: Healthy gums are typically a shade of pale or coral pink. In individuals with darker skin tones, healthy gums can naturally appear darker, sometimes with melanin pigmentation appearing as brownish or purplish spots. The key is uniformity in color.
- Texture: Healthy gums have a firm, resilient texture. They are not puffy or swollen. Many people's healthy gums exhibit a slight "stippling" — a texture resembling an orange peel. This stippling indicates good collagen fiber content and tissue health.
- Contour: The gum tissue around each tooth should have a "knife-edge" margin, meaning it's thin and tightly hugs the tooth, forming a shallow, V-shaped groove (sulcus) that is typically 1-3 millimeters deep. There should be no signs of recession, where the gum line pulls back from the tooth surface.
- Bleeding: Healthy gums do not bleed during routine brushing, flossing, or dental examinations. Any bleeding is a significant indicator of inflammation.
- Pain/Sensitivity: Healthy gums are typically pain-free and not sensitive to touch or temperature changes.
- Attachment: Gums should be firmly attached to the teeth and underlying bone, preventing food particles and bacteria from accumulating in deep pockets.
``
Maintaining these characteristics is paramount, as they signify a robust defense against oral bacteria and the various issues that can compromise dental health.
Demystifying Gingivitis: The First Stage of Gum Disease
Gingivitis represents the initial and mildest stage of gum disease. It is an inflammatory condition that, while not immediately damaging to the supporting structures of your teeth, serves as a crucial warning sign that your oral health is at risk.
What is Gingivitis?
Gingivitis is defined as inflammation of the gingiva (gum tissue) caused primarily by the accumulation of bacterial plaque at the gum line. This inflammation can cause noticeable changes in the gums' appearance, but crucially, it does not yet involve the destruction of the bone or connective tissue that hold the teeth in place. This distinction makes gingivitis a reversible condition, unlike the more advanced stage, periodontitis.
Causes of Gingivitis
The primary culprit behind gingivitis is dental plaque, a sticky, colorless film of bacteria that constantly forms on your teeth. If plaque is not removed daily through proper brushing and flossing, the bacteria in it produce toxins that irritate the gum tissue, leading to inflammation. Over time, plaque can harden into calculus (tartar), which is much more difficult to remove and provides a rough surface for further plaque accumulation.
Beyond poor oral hygiene, several other factors can contribute to or exacerbate gingivitis:
- Poor Oral Hygiene: Infrequent or ineffective brushing and flossing allow plaque to build up.
- Smoking or Chewing Tobacco: Tobacco use significantly impairs the immune system and the body's ability to fight off bacterial infections, making smokers more susceptible to gingivitis and hindering healing.
- Systemic Diseases: Conditions like diabetes, especially when poorly controlled, can weaken the immune system and increase susceptibility to infections, including gum disease. Other conditions, such as Crohn's disease or certain autoimmune disorders, can also affect gum health.
- Hormonal Changes: Fluctuations during pregnancy, puberty, menstruation, or menopause can make gums more sensitive and prone to inflammation, often referred to as "pregnancy gingivitis."
- Medications: Some drugs can cause dry mouth (xerostomia), reducing saliva flow which naturally helps wash away food particles and neutralize acids. Others, like certain anti-seizure medications or calcium channel blockers, can cause gingival enlargement (overgrowth of gum tissue), making cleaning more difficult.
- Poor Nutrition: A diet lacking essential vitamins and minerals, particularly Vitamin C, can compromise gum health.
- Ill-fitting Dental Restorations: Crowns, bridges, or fillings that don't fit properly can create areas where plaque accumulates easily and is difficult to remove.
- Compromised Immunity: Conditions like HIV/AIDS or treatments that suppress the immune system can increase vulnerability.
- Genetics: Some individuals may be genetically predisposed to developing gum disease.
Signs and Symptoms of Gingivitis
Recognizing the early signs of gingivitis is key to prompt treatment and reversal. Look out for these indicators:
- Red or Purplish Gums: Instead of a healthy pale pink, affected gums often appear reddened or even purplish due to increased blood flow from inflammation.
- Swollen or Puffy Gums: The gum tissue may look enlarged, puffy, or tender, losing its firm, tight contour around the teeth.
- Bleeding Gums: This is one of the most common and telling signs. Gums that bleed during brushing, flossing, or even when eating hard foods are a strong indicator of gingivitis. Healthy gums should not bleed.
- Tender Gums: Gums may be sensitive or sore to the touch, or when chewing.
- Receding Gums: While more characteristic of advanced gum disease (what causes gum recession is chronic inflammation leading to bone loss and subsequent gum shrinkage), gingivitis can sometimes be accompanied by slight recession as the inflammatory process begins to break down gum tissue attachment.
- Persistent Bad Breath (Halitosis): The accumulation of bacteria in plaque and inflamed tissues can release foul-smelling gases.
- Shiny Gums: The loss of stippling and the presence of inflammation can make gums appear glossy or shiny.
Pro Tip: Don't ignore bleeding gums, even if it's minimal or infrequent. Many people mistakenly believe it's normal to have some bleeding after flossing, but it's a clear sign your gums need attention.
Normal Gums vs. Gingivitis: A Detailed Side-by-Side Comparison
Understanding the subtle yet significant differences between healthy gums and those suffering from gingivitis is critical for self-assessment and knowing when to seek professional help.
| Feature | Normal Gums | Gingivitis |
|---|---|---|
| Color | Pale pink (may vary with natural pigmentation) | Red, dark red, purplish-red |
| Texture/Consistency | Firm, resilient, often stippled (orange peel-like) | Swollen, puffy, soft, spongy, loss of stippling |
| Contour | Knife-edge margin, tightly adapted to teeth | Rolled, blunted, enlarged, moves away from teeth |
| Bleeding | None with brushing, flossing, or probing | Commonly bleeds with brushing, flossing, or probing |
| Pain/Sensitivity | Generally pain-free | May be tender, sensitive, or sore |
| Bad Breath | Not typically associated | Often present (halitosis) |
| Reversibility | Always healthy | Fully reversible with treatment and good hygiene |
| Bone Loss | None | None (bone intact) |
Color Differences
The most striking visual difference often lies in the color. Healthy gums are consistently pale pink, a sign of good vascularization without excessive inflammation. Gums affected by gingivitis, however, will appear distinctly redder, often a bright red, dusky red, or even purplish-red. This change in color is due to increased blood flow to the area as the body attempts to fight off the bacterial infection.
Texture and Consistency
When you gently touch healthy gums, they feel firm and resilient. The surface might even have a subtle stippled appearance, much like the skin of an orange, which is indicative of strong connective tissue. In contrast, gingivitis causes the gums to become swollen, soft, and puffy. They may lose their stippled texture and instead feel spongy or boggy to the touch due to fluid accumulation from inflammation.
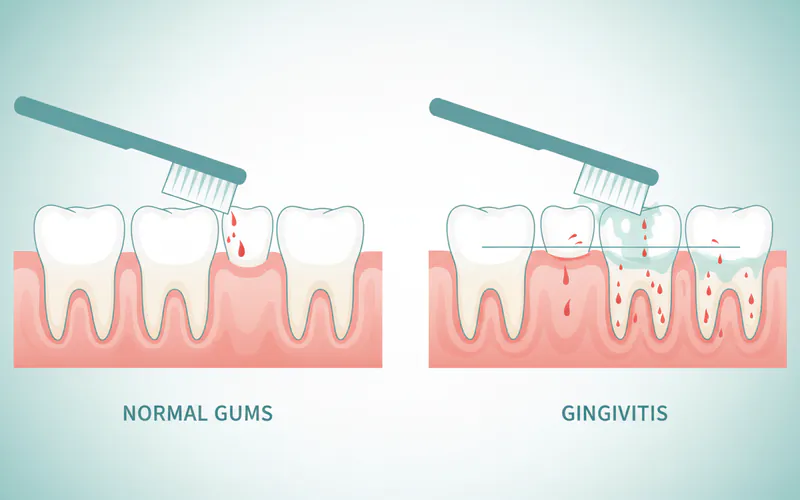
Bleeding Upon Brushing/Flossing
Perhaps the most common and alarming symptom of gingivitis is bleeding. Healthy gums simply do not bleed during normal oral hygiene practices. If your gums consistently bleed when you brush your teeth, especially along the gum line, or when you floss, it is a definitive sign of inflammation and gingivitis. This bleeding indicates fragile blood vessels within the inflamed tissue that rupture easily.
Gum Margins and Attachment
The margin of a healthy gum should be thin and tightly adapted around the tooth, resembling a "knife-edge." This tight seal prevents food particles and bacteria from invading the deeper structures. With gingivitis, the gum margins become swollen and blunted, losing this crisp appearance. They may pull away slightly from the tooth, creating a slightly deeper sulcus (the pocket between the tooth and gum) where plaque can accumulate more readily.
Bad Breath (Halitosis) Implications
While bad breath can have many causes, persistent halitosis that doesn't resolve with brushing can be a symptom of gingivitis. The bacteria thriving in the plaque and calculus, combined with the inflammatory processes in the gums, produce volatile sulfur compounds that lead to an unpleasant odor. Addressing the gingivitis often significantly improves or eliminates this type of bad breath.
``
The Path to Periodontitis: When Gingivitis Progresses
If gingivitis is left untreated, it can pave the way for a more serious and irreversible condition known as periodontitis. This progression is why early detection and intervention are so critical.
Understanding Gum Recession
One of the significant concerns associated with chronic gum inflammation and subsequent periodontitis is gum recession. What causes gum recession? While aggressive brushing can cause it, the primary cause of widespread gum recession in the context of gum disease is the ongoing inflammatory process. When gingivitis progresses to periodontitis, the chronic inflammation causes the inner layer of the gum and bone to pull away from the teeth. This forms "pockets" between the teeth and gums that collect food debris and bacteria. As the infection deepens, the body's immune response, combined with bacterial toxins, starts to break down the bone and connective tissue that hold the teeth in place. As this supporting structure is lost, the gums literally recede, exposing more of the tooth root. Exposed roots are often sensitive and more susceptible to decay.
From Gingivitis to Periodontitis
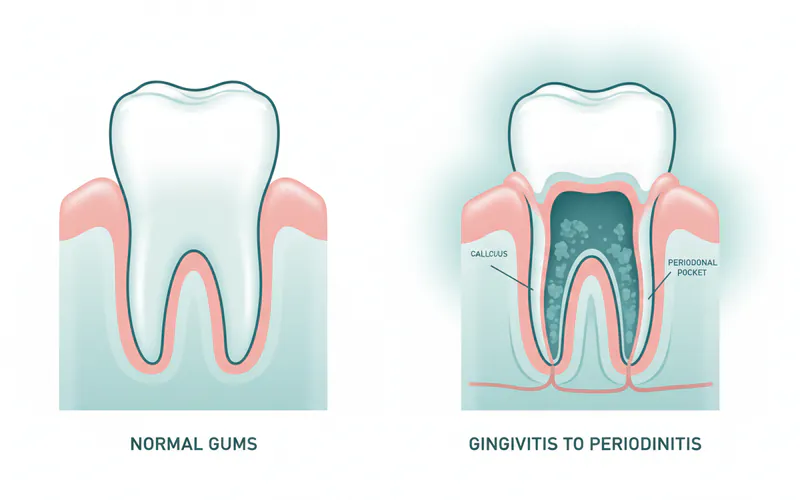
The transition from gingivitis to periodontitis marks a critical turning point. In periodontitis, the inflammation moves beyond the gum tissue to affect the deeper supporting structures of the teeth.
- Pocket Formation: As the bone and connective tissue deteriorate, the shallow gum sulcus deepens, forming periodontal pockets. These pockets act as traps for bacteria, creating an environment where they can thrive, multiply, and become increasingly aggressive, leading to further destruction.
- Irreversible Bone Loss: Unlike gingivitis, periodontitis involves the irreversible loss of the alveolar bone that anchors the teeth. This bone loss cannot typically be regained naturally.
- Tooth Mobility: As bone support diminishes, teeth may become loose or shift positions. In advanced stages, teeth can become so mobile that they need to be extracted.
- Abscesses and Pus: Pockets can become infected, leading to painful gum abscesses filled with pus.
- Systemic Health Impacts: Periodontitis is not just an oral health issue. The chronic inflammation and bacterial load in the mouth can impact overall health, contributing to conditions like heart disease, stroke, diabetes complications, respiratory disease, and adverse pregnancy outcomes.
Diagnosis of Gingivitis and Periodontal Health
A thorough dental examination is essential for accurately diagnosing gingivitis and assessing overall periodontal health. Early diagnosis allows for timely intervention and prevents the progression to more severe forms of gum disease.
Professional Dental Exam
Your dentist or dental hygienist will perform a comprehensive evaluation during your regular check-up:
- Visual Inspection: They will visually examine your gums for signs of inflammation, such as redness, swelling, and changes in contour or texture. They will also look for visible plaque and calculus buildup.
- Periodontal Probing: A small, thin instrument called a periodontal probe is used to gently measure the depth of the sulcus (the space between your tooth and gum). Healthy sulcus depths are typically 1-3 millimeters. Depths greater than 3 mm, especially with bleeding upon probing, indicate gingivitis or periodontitis. This measurement helps identify the presence of periodontal pockets.
- X-rays: Dental X-rays may be taken to assess the condition of the underlying bone. While gingivitis itself doesn't cause bone loss, X-rays are crucial for detecting bone loss if periodontitis is suspected. They also help identify calculus buildup and any tooth decay.
- Plaque and Bleeding Indices: Dental professionals might use indices to quantify the amount of plaque present and the extent of gum bleeding, providing a baseline for tracking progress.
Importance of Early Detection
Detecting gingivitis early is paramount because it is the only stage of gum disease that is fully reversible. Catching it before it progresses to periodontitis means you can restore your gums to full health, avoid irreversible bone damage, and prevent the need for more complex and costly treatments. Regular dental check-ups, ideally every six months, are your best defense.
Treatment Options for Gingivitis and Early Periodontal Disease
The good news is that gingivitis is highly treatable. The goals of periodontal treatment at this stage are to remove the source of inflammation (plaque and calculus) and establish conditions that allow the gums to heal.
Professional Dental Cleaning (Prophylaxis)
For gingivitis, the primary treatment is a professional dental cleaning, also known as prophylaxis.
- Process: A dental hygienist or dentist uses specialized instruments (scalers and ultrasonic devices) to meticulously remove plaque and calculus from above and just below the gum line. The teeth are then polished to remove surface stains and smooth the tooth surfaces, making it harder for plaque to adhere.
- Benefits: This procedure removes the bacterial irritants, allowing the gum tissue to heal, reduce inflammation, stop bleeding, and return to a healthy state.
- Frequency: Most individuals with gingivitis will benefit from regular cleanings every six months, though some might require more frequent visits (e.g., every 3-4 months) initially until their gum health improves.
Scaling and Root Planing (Deep Cleaning)
If gingivitis has progressed to early or moderate periodontitis, where periodontal pockets have formed and bone loss has begun, a more intensive procedure called scaling and root planing (SRP) is necessary. This is often referred to as a "deep cleaning."
- Process: SRP involves thoroughly cleaning the root surfaces of the teeth below the gum line to remove plaque, calculus, and bacterial toxins from within the periodontal pockets. The root surfaces are then "planed" (smoothed) to remove bacterial toxins and prevent future plaque buildup, facilitating reattachment of the gum tissue to the tooth.
- Local Anesthesia: Due to the depth of cleaning, local anesthesia is usually administered to numb the gums and ensure patient comfort.
- Multiple Appointments: SRP is typically performed over two to four appointments, focusing on one quadrant of the mouth at a time, to minimize discomfort and ensure thoroughness.
- Benefits: Reduces pocket depths, eliminates infection, helps prevent further bone loss, and can halt the progression of periodontitis.
Antimicrobial Rinses and Local Antibiotics
In some cases, your dentist may recommend adjunctive therapies:
- Antimicrobial Mouthrinses: Prescription mouthwashes containing chlorhexidine gluconate may be prescribed for short-term use after SRP to further reduce bacteria. Over-the-counter therapeutic mouthrinses (containing essential oils or cetylpyridinium chloride) can also be recommended for daily use as part of a comprehensive oral hygiene routine.
- Local Antibiotics: For persistent or isolated deep pockets, antibiotics may be placed directly into the periodontal pockets in the form of gels, chips, or microspheres. These release medication slowly over time to target bacteria at the site of infection.
Oral Hygiene Instruction
A critical component of any periodontal treatment is personalized oral hygiene instruction. Your dental professional will demonstrate proper brushing techniques (e.g., Bass method), effective flossing methods, and the correct use of interdental cleaners (e.g., interdental brushes, water flossers). This education empowers you to maintain your oral health at home, which is essential for preventing recurrence.
Pro Tip: Consistency is key! Even the best professional cleaning won't prevent gingivitis from returning if you don't commit to a meticulous daily oral hygiene routine. Make brushing twice a day and flossing once a day non-negotiable habits.
``
Cost and Insurance for Gum Care in the US
Understanding the financial aspects of dental care, especially for gum disease, is crucial. Costs can vary significantly based on location, the severity of the condition, and whether you have dental insurance.
Typical Costs for Cleanings and Deep Cleanings
Here's an overview of average costs in the US without insurance:
- Professional Dental Cleaning (Prophylaxis): For gingivitis, this routine cleaning typically ranges from $75 to $200. The cost can be higher in urban areas or specialized clinics.
- Scaling and Root Planing (SRP): This "deep cleaning" is priced per quadrant (one-quarter of the mouth). A single quadrant can cost anywhere from $200 to $400. Therefore, a full-mouth SRP (four quadrants) could range from $800 to $1,600 or more.
- Full Mouth Debridement: If there's extensive calculus buildup that obstructs the dentist's view and prevents a comprehensive exam, a preliminary procedure called full mouth debridement might be performed, costing around $100 to $250.
- Antimicrobial Rinses: Prescription mouthrinses like chlorhexidine can cost $20 to $50 per bottle.
- Local Antibiotic Placement: If applied, this can add $50 to $100 per site.
Insurance Coverage Details
Most dental insurance plans in the US offer coverage for preventive and basic restorative procedures.
- Preventive Care: Routine cleanings (prophylaxis) are usually covered at 80-100% by most dental insurance plans, often without a deductible, if performed twice a year.
- Basic Restorative Care: Scaling and root planing is typically categorized as a "basic restorative" procedure. Insurance coverage usually ranges from 50-80% after your deductible has been met.
- Waiting Periods: Many insurance plans have waiting periods (e.g., 3-6 months) before they will cover major or sometimes even basic procedures like SRP. It's essential to check your specific policy details.
- Annual Maximums: Most dental insurance plans have an annual maximum benefit, typically ranging from $1,000 to $2,000. Once this limit is reached, you are responsible for 100% of additional costs.
- PPO vs. HMO:
- PPO (Preferred Provider Organization): Offers more flexibility in choosing dentists, but typically has higher out-of-pocket costs for out-of-network providers.
- HMO (Health Maintenance Organization): Requires you to choose a primary dentist within their network and typically offers lower monthly premiums and co-pays.
Comparison Table: Cost of Common Gum-Related Procedures (US Averages, without insurance)
| Procedure | Average Cost Range (Without Insurance) | Typical Insurance Coverage |
|---|---|---|
| Professional Cleaning | $75 - $200 | 80-100% (often no deductible) |
| Scaling & Root Planing (per quadrant) | $200 - $400 | 50-80% (after deductible) |
| Full Mouth Debridement | $100 - $250 | 50-80% |
| Antimicrobial Mouthrinse (prescription) | $20 - $50 | Varies, often not covered |
| Local Antibiotic Placement (per site) | $50 - $100 | Varies, sometimes 50% |
Payment Plans and Financing Options
If you don't have insurance or face significant out-of-pocket costs, several options can help:
- CareCredit and Other Medical Credit Cards: These offer special financing options, often with deferred interest for a set period.
- In-Office Payment Plans: Many dental offices offer their own payment plans, allowing you to pay in installments. Don't hesitate to ask your dental office about their options.
- Dental Schools: University dental schools often provide services at a reduced cost, as treatment is performed by students under the supervision of experienced faculty.
- Community Dental Clinics: Look for local community health centers or public dental clinics that may offer sliding scale fees based on income.
Recovery and Aftercare Post-Treatment
After receiving periodontal treatment for gingivitis or early periodontitis, proper recovery and diligent aftercare are essential for long-term success.
What to Expect After a Cleaning/SRP
- Mild Discomfort/Soreness: It's normal to experience some gum soreness or tenderness for a few days, especially after a deep cleaning (SRP). Over-the-counter pain relievers like ibuprofen or acetaminophen can help manage this.
- Sensitivity: Your teeth, particularly the roots if they were exposed, might be sensitive to hot, cold, or sweet stimuli for a week or two. This is because the procedures expose previously covered tooth surfaces. Your dentist might recommend sensitivity toothpastes or fluoride rinses.
- Slight Bleeding: Minor bleeding may occur for a day or two, but it should subside quickly.
- Swelling Reduction: You should notice a significant reduction in gum swelling and redness within a few days to a week. The gums will start to look firmer and healthier.
Essential Home Care
Your commitment to home oral hygiene is the most crucial factor in preventing gingivitis from returning.
- Brushing: Brush your teeth twice a day for two minutes each time, using a soft-bristled toothbrush. Pay close attention to the gum line, using a gentle, circular motion or a specific technique like the Bass method (brushing at a 45-degree angle towards the gum line). Consider an electric toothbrush for enhanced plaque removal.
- Flossing: Floss at least once a day to remove plaque and food particles from between your teeth and under the gum line, areas your toothbrush can't reach. Use a gentle C-shape motion against each tooth.
- Interdental Cleaners: For some, interdental brushes, dental picks, or a water flosser can be excellent adjuncts to traditional flossing, especially if you have larger spaces between teeth or struggle with string floss.
- Mouthwash: Therapeutic mouthrinses (antiseptic or fluoride-containing) can be recommended by your dentist to help control plaque and strengthen enamel, but they should never replace brushing and flossing.
- Diet: Maintain a balanced diet and limit sugary snacks and drinks, which contribute to plaque formation.
Follow-Up Appointments
Your dentist or hygienist will schedule follow-up appointments, often called "periodontal maintenance" cleanings, to monitor your gum health. For individuals recovering from gingivitis or periodontitis, these are often recommended every 3-4 months instead of the standard 6 months, to ensure bacteria levels are controlled and to catch any signs of recurrence early.
Preventing Gum Disease: Your Best Defense
Prevention is always better than cure, especially when it comes to gum disease. By adhering to a few simple practices, you can largely protect your gums from inflammation and disease.
Optimal Oral Hygiene Routine
This is the cornerstone of prevention:
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes each time, covering all surfaces of your teeth and gently along the gum line. Replace your toothbrush every 3-4 months, or sooner if the bristles are frayed.
- Floss Daily: Floss at least once a day to remove food particles and plaque from between your teeth and under the gum line. This step is non-negotiable for gum health.
- Consider Additional Tools: Incorporate mouthwash, interdental brushes, or a water flosser as recommended by your dental professional, especially if you have braces, bridges, or difficulty with traditional flossing.
Regular Dental Check-ups and Cleanings
Professional care is crucial:
- Schedule Every 6 Months: Visit your dentist for check-ups and professional cleanings at least twice a year. These appointments allow your dental team to remove stubborn plaque and calculus that home care can't tackle and to detect any early signs of gingivitis or other issues.
- Periodontal Maintenance: If you have a history of gum disease, your dentist might recommend more frequent periodontal maintenance appointments (e.g., every 3-4 months) to keep your gums healthy and prevent recurrence.
Lifestyle Factors
Your overall health and habits significantly impact your gum health:
- Quit Smoking: Smoking is one of the most significant risk factors for developing severe gum disease. Quitting is the single best thing you can do for your gum health.
- Balanced Diet: Eat a diet rich in fruits, vegetables, and whole grains. Limit sugary and starchy foods that feed plaque bacteria.
- Manage Systemic Conditions: If you have conditions like diabetes, ensure they are well-managed. Poorly controlled diabetes dramatically increases your risk of gum disease.
- Stress Management: Chronic stress can weaken your immune system, making you more susceptible to infections, including gum disease.
- Avoid Teeth Grinding/Clenching: Chronic grinding (bruxism) can put excessive force on your teeth and supporting tissues, potentially exacerbating gum issues. Your dentist can recommend a nightguard.
By integrating these preventive measures into your daily routine, you can significantly reduce your risk of developing gingivitis and maintain a healthy, vibrant smile.
Risks and Complications of Untreated Gum Disease
Ignoring gingivitis or failing to manage it effectively carries substantial risks, potentially leading to severe oral health problems and impacting your overall well-being.
Progression to Periodontitis
The most immediate and concerning risk of untreated gingivitis is its progression to periodontitis. As detailed earlier, this means the inflammation extends beyond the gums to destroy the bone and connective tissues supporting your teeth. This destruction is irreversible and leads to:
- Deepening Periodontal Pockets: These pockets become breeding grounds for more aggressive bacteria.
- Further Bone Loss: Continued loss of the jawbone, eventually making teeth unstable.
- Tooth Mobility and Loss: Teeth can become loose, shift out of alignment, and ultimately fall out or require extraction.
- Gum Recession: Significant pulling back of the gum tissue, exposing sensitive tooth roots.
- Abscesses: Painful infections within the gum tissue or bone.
Systemic Health Links
The impact of untreated gum disease extends far beyond your mouth. The chronic inflammation and bacteria from your gums can enter your bloodstream and affect other parts of your body, increasing the risk or worsening various systemic conditions. The American Dental Association (ADA) and other health organizations emphasize these critical connections:
- Heart Disease and Stroke: Research suggests a link between periodontitis and an increased risk of heart attack and stroke. Bacteria from the mouth can enter the bloodstream, potentially contributing to arterial plaque formation (atherosclerosis) or blood clot formation.
- Diabetes: There's a bidirectional relationship between diabetes and gum disease. Uncontrolled diabetes makes individuals more susceptible to severe periodontitis, and severe periodontitis can make blood sugar control more difficult for diabetics.
- Respiratory Disease: Oral bacteria can be aspirated into the lungs, potentially leading to respiratory infections such as pneumonia, especially in individuals with compromised immune systems or chronic lung conditions.
- Adverse Pregnancy Outcomes: Pregnant women with periodontitis may have an increased risk of premature birth and low birth weight babies.
- Other Conditions: Links have also been suggested with rheumatoid arthritis, certain cancers, and even cognitive decline.
``
Given these potential complications, treating gingivitis promptly and maintaining excellent oral hygiene are not just about saving your teeth; they are about protecting your overall health.
Children and Gum Health: Pediatric Considerations
While gingivitis is more prevalent in adults, children and adolescents are not immune. Understanding the unique aspects of gum health in younger individuals is important for parents.
Gingivitis in Children
Gingivitis can occur in children, though it is often milder than in adults. It's frequently linked to:
- Poor Oral Hygiene: Children may not brush or floss effectively, allowing plaque to accumulate.
- Orthodontic Appliances: Braces can make it more challenging to clean teeth thoroughly, leading to plaque buildup around brackets and wires.
- Eruption Gingivitis: As permanent teeth erupt, the surrounding gum tissue can become temporarily inflamed.
- Hormonal Changes: Puberty can cause hormonal shifts that make gums more susceptible to inflammation, similar to pregnancy gingivitis in adults.
- Mouth Breathing: Chronic mouth breathing can dry out the gums, especially in the front of the mouth, making them more prone to inflammation.
- Systemic Conditions: Certain medical conditions or medications can also increase a child's risk of gingivitis.
Signs of gingivitis in children are similar to adults: red, swollen gums that bleed easily when brushed or flossed.
Parental Role in Oral Hygiene
Parents play a critical role in establishing good oral hygiene habits from an early age:
- Start Early: Begin cleaning your infant's gums with a soft cloth even before teeth erupt. Once teeth appear, brush them twice a day with a small, soft-bristled toothbrush and a tiny smear of fluoride toothpaste (rice grain size for under 3, pea-size for 3-6 years old).
- Supervise Brushing: Supervise children's brushing until they are about 7 or 8 years old to ensure they are doing a thorough job.
- Teach Flossing: Introduce flossing once teeth begin to touch each other, typically around age 2-3. You may need to help them floss until they develop the necessary dexterity.
- Lead by Example: Children often mimic their parents, so demonstrating good oral hygiene habits yourself is powerful.
- Regular Dental Visits: Take your child to the dentist for their first check-up by age one, and then for regular check-ups every six months. Pediatric dentists are specially trained to address children's unique dental needs.
Signs to Watch For
Parents should be vigilant for any signs of gingivitis in their children, particularly bleeding gums. If you notice persistent redness, swelling, or bleeding, schedule an appointment with your pediatric dentist. Early intervention is key to reversing gingivitis and preventing it from becoming a more serious problem.
Frequently Asked Questions
Is gingivitis reversible?
Yes, absolutely. Gingivitis is the only stage of gum disease that is fully reversible. With professional dental cleaning (prophylaxis) to remove plaque and calculus, combined with diligent daily home oral hygiene, gum inflammation can resolve, and the gums can return to a healthy state, typically within 1-2 weeks.
How long does it take to treat gingivitis?
The active treatment for gingivitis usually involves a single professional cleaning appointment. However, the healing process and the full reversal of symptoms, such as redness and bleeding, can take several days to a couple of weeks, provided you maintain excellent oral hygiene at home. Consistent long-term care prevents recurrence.
What is the average cost of scaling and root planing?
Scaling and root planing (deep cleaning) typically costs between $200 and $400 per quadrant (one-quarter of the mouth) without insurance. For a full mouth (four quadrants), the total cost could range from $800 to $1,600 or more, depending on the severity and location. Dental insurance usually covers a portion of these costs.
Can gingivitis cause bad breath?
Yes, persistent bad breath, also known as halitosis, is a common symptom of gingivitis. The bacteria in the accumulated plaque and calculus, along with the inflammatory process in the gums, produce foul-smelling volatile sulfur compounds that lead to an unpleasant odor. Addressing the gingivitis often resolves the bad breath.
Is gum bleeding normal?
No, healthy gums do not bleed. Any bleeding from your gums, whether during brushing, flossing, or eating, is a sign of inflammation and is usually an indicator of gingivitis. It should always be brought to the attention of your dentist.
What's the difference between a regular cleaning and a deep cleaning?
A regular cleaning (prophylaxis) removes plaque and calculus from above the gum line and slightly below it, typically for healthy gums or mild gingivitis. A deep cleaning (scaling and root planing) is a more intensive procedure that cleans thoroughly below the gum line, removing plaque, calculus, and bacterial toxins from within periodontal pockets and smoothing root surfaces, used for periodontitis.
Does flossing make gingivitis worse initially?
When you first start flossing regularly, especially if you haven't done so consistently, your inflamed gums might bleed more or feel tender. This is a temporary reaction as the gums begin to heal and the plaque is removed. It does not mean flossing is making it worse; it means you're addressing the underlying inflammation. Consistent flossing will lead to healthier, non-bleeding gums.
Can natural remedies cure gingivitis?
While some natural remedies like salt water rinses or certain essential oils may offer temporary relief from symptoms or help reduce some bacteria, they cannot "cure" gingivitis. Professional dental cleaning is necessary to remove the hardened plaque and calculus (tartar) that cause the inflammation. Natural remedies should only be used as an adjunct to, not a replacement for, professional dental care and diligent home hygiene.
How often should I see a dentist if I have gingivitis?
If you have been diagnosed with gingivitis, your dentist will typically recommend a professional cleaning and then suggest follow-up visits every 3-4 months initially, rather than the standard six months. This increased frequency helps ensure the inflammation has fully resolved and allows your dental team to monitor your progress and reinforce good oral hygiene habits.
What are the signs that gingivitis has progressed to periodontitis?
Signs that gingivitis has advanced to periodontitis include persistent bad breath or a bad taste, noticeable gum recession (gums pulling away from teeth), the formation of deep pockets between teeth and gums, pus between teeth and gums, changes in how your teeth fit together when you bite, and increasingly loose or shifting teeth. Unlike gingivitis, periodontitis involves irreversible bone loss.
When to See a Dentist
Knowing when to seek professional dental care is crucial for preventing minor issues from escalating into major problems.
You should schedule a routine dental check-up and cleaning at least every six months, even if you don't notice any specific symptoms. These regular visits are essential for preventive care, early detection of issues like gingivitis, and professional plaque and calculus removal that your home routine can't achieve.
However, certain warning signs indicate you need to see a dentist sooner rather than later:
- Persistent Bleeding Gums: If your gums consistently bleed during brushing or flossing, or even spontaneously, it's a clear sign of inflammation that needs attention.
- Red, Swollen, or Tender Gums: Gums that appear visibly red, puffy, or are painful to the touch are indicative of gingivitis or a more serious infection.
- Receding Gums: If you notice your gum line pulling back from your teeth, making your teeth appear longer, this is a sign of gum recession, which can indicate periodontitis.
- Persistent Bad Breath or Bad Taste: If halitosis doesn't resolve with good oral hygiene, it could be a symptom of bacterial overgrowth in your gums.
- Loose or Shifting Teeth: This is a serious sign of advanced periodontal disease and requires immediate dental intervention to try and save the affected teeth.
- Pus Around Teeth and Gums: The presence of pus indicates an active infection (abscess) that needs urgent treatment.
- Changes in Bite or Denture Fit: If your teeth suddenly feel different when you bite down, or if your partial dentures no longer fit properly, it could be a sign of bone loss or shifting teeth due to gum disease.
- Increased Sensitivity: While general tooth sensitivity can have various causes, new or worsening sensitivity, especially at the gum line, can be due to receding gums exposing tooth roots.
If you experience any of these red flags, do not delay. Prompt attention from a dental professional can often prevent irreversible damage, save your teeth, and protect your overall health. For severe pain, significant swelling, or a rapidly spreading infection, consider it a dental emergency and seek immediate care.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Can You Get Rid of Gingivitis
More than 50% of American adults aged 30 or older suffer from some form of gum disease, with gingivitis being the earliest and most common stage. This often silent condition, marked by inflammation of the gums, can seem daunting, leading many to wonder: can you get rid of gingivitis? The good ne
February 22, 2026
What Causes Receding Gums
Receding gums, a condition where the gum tissue surrounding the teeth pulls back or wears away, exposing more of the tooth or the tooth's root, affects a significant portion of the adult population in the United States. In fact, estimates suggest that **up to 88% of people over the age of 65 have on
February 22, 2026
Signs of Gingivitis: Complete Guide
Did you know that nearly half of American adults aged 30 and older suffer from some form of gum disease? While that statistic might sound alarming, the good news is that the earliest and most common stage, gingivitis, is entirely reversible. Recognizing the signs of gingivitis early is your
February 22, 2026
Gum Disease Medical Procedure: Complete Guide
Gum Disease Medical Procedure: Complete Guide
February 22, 2026