Xerostomia: Complete Dental Guide
Key Takeaways
- Xerostomia, more commonly known as chronic dry mouth, is a condition characterized by a reduced flow of saliva, leading to a persistently dry oral cavity. Far more than just an uncomfortable sensation, xerostomia is a serious dental health concern that can significantly impact an individual's qualit
Xerostomia: Understanding Chronic Dry Mouth and Its Impact on Dental Health
Introduction
Xerostomia, more commonly known as chronic dry mouth, is a condition characterized by a reduced flow of saliva, leading to a persistently dry oral cavity. Far more than just an uncomfortable sensation, xerostomia is a serious dental health concern that can significantly impact an individual's quality of life. Saliva plays a crucial role in maintaining oral health: it helps neutralize acids, wash away food particles, remineralize tooth enamel, aid in digestion, and provide antimicrobial protection. When saliva production diminishes, the mouth's natural defense mechanisms are compromised, paving the way for a cascade of oral health problems.
This condition affects a substantial portion of the population. While often associated with aging, it is not an inevitable part of the aging process itself, but rather a side effect of medications commonly taken by older adults or systemic health issues. Estimates suggest that xerostomia affects approximately 10% of the general population, with prevalence rising significantly in specific groups, reaching up to 20% in older adults and as high as 40% in individuals taking multiple medications. Understanding what is xerostomia and its profound xerostomia dental implications is the first step toward effective management and preserving long-term oral health.
Key Takeaways:
- Xerostomia is chronic dry mouth caused by insufficient saliva production, not just temporary thirst.
- Saliva is vital for oral health, protecting against decay, infections, and aiding digestion.
- Common causes include medications, systemic diseases (like Sjogren's syndrome, diabetes), and radiation therapy.
- Untreated xerostomia significantly increases the risk of severe dental problems, including rampant Caries (tooth decay), gum disease, and persistent Halitosis.
- Diagnosis involves a dental examination and often saliva flow measurements.
- Management focuses on alleviating symptoms, preventing complications, and addressing the underlying cause where possible.
Detailed Explanation
Types and Classifications of Xerostomia
Xerostomia can be broadly categorized based on its nature and perception:
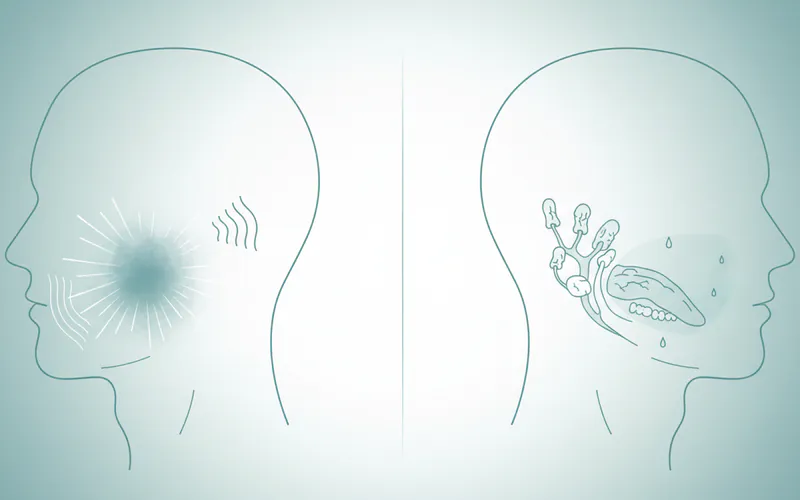
- Subjective Xerostomia: This refers to the feeling of dry mouth, even if measurable saliva flow is within normal limits. It's often related to changes in saliva composition or neurological perception.
- Objective Xerostomia (Hypofunctioning Salivary Glands): This is when there is a measurable reduction in saliva production, confirmed by diagnostic tests. This is the more severe form with clearer dental health consequences.
- Transient vs. Chronic: Some dry mouth episodes can be temporary (e.g., due to acute dehydration or anxiety), while chronic xerostomia persists over a long period, indicating an underlying issue.
Causes and Risk Factors
The causes of xerostomia are multifaceted, ranging from common medications to serious systemic diseases. Understanding these factors is crucial for both diagnosis and effective management.
-
Medications: This is by far the most common cause. Over 500 prescription and over-the-counter drugs can cause dry mouth as a side effect. These include:
- Antihistamines (for allergies)
- Decongestants
- Antidepressants and anxiolytics
- Antihypertensives (for high blood pressure)
- Diuretics
- Pain relievers (especially opioids)
- Muscle relaxants
- Certain chemotherapy drugs
-
Systemic Diseases and Conditions:
- Sjögren's Syndrome: An autoimmune disease where the body's immune system attacks moisture-producing glands, including the salivary glands. It's a leading cause of severe xerostomia.
- Diabetes: Poorly controlled blood sugar levels can damage nerves affecting salivary glands and increase fluid loss.
- Rheumatoid Arthritis and Lupus: Other autoimmune conditions that can impact salivary gland function.
- HIV/AIDS: The virus itself or medications used to treat it can cause dry mouth.
- Parkinson's Disease: Can affect the nervous system's control over saliva production.
- Alzheimer's Disease: Patients may have difficulty communicating their symptoms or maintaining hydration.
- Thyroid Disorders: Can sometimes contribute to dry mouth.
-
Medical Treatments:
- Radiation Therapy to the Head and Neck: Radiation can permanently damage salivary glands, leading to severe and often irreversible xerostomia. The severity depends on the dose and area treated.
- Chemotherapy: While often temporary, some chemotherapy drugs can cause a transient reduction in saliva flow.
- Stem Cell Transplants: Can lead to graft-versus-host disease, which may affect salivary glands.
-
Nerve Damage: Injury or surgery that affects the nerves controlling the salivary glands can impair function.
-
Lifestyle Factors:
- Dehydration: Insufficient fluid intake.
- Smoking and Tobacco Use: Irritates oral tissues and reduces saliva flow.
- Alcohol Consumption: Alcohol acts as a diuretic and dries out oral tissues.
- Excessive Caffeine Intake: Similar to alcohol, caffeine can contribute to dehydration.
- Mouth Breathing: Often due to nasal congestion or sleep apnea, leads to evaporation of saliva.
- Stress and Anxiety: Can temporarily reduce saliva production.
-
Aging: While aging itself doesn't cause xerostomia, older adults are more likely to take multiple medications and have systemic diseases that contribute to the condition.
Signs and Symptoms to Watch For
Recognizing the signs of xerostomia is critical for early intervention. Patients often experience the following:
- Sticky, dry feeling in the mouth: The most common complaint.
- Frequent thirst: A constant need to drink water, especially at night.
- Sore throat or hoarseness: Due to lack of lubrication.
- Difficulty speaking, chewing, and swallowing: Food feels dry and hard to manipulate without saliva.
- A burning or tingling sensation in the mouth: Often on the tongue.
- Changes in taste: Food may taste different or bland.
- Rough, dry tongue: May appear fissured or red.
- Cracked lips and corners of the mouth (angular cheilitis): Often due to fungal infections thriving in a dry environment.
- Increased incidence of Caries (tooth decay): Especially around the gumline and on the tips of teeth, as saliva's protective buffering capacity is lost. Studies show a 3- to 5-fold increase in caries risk for xerostomia patients.
- Gum inflammation (gingivitis) and gum disease (periodontitis): Lack of saliva allows bacteria to proliferate more easily.
- Persistent Halitosis (bad breath): Bacteria thrive and produce volatile sulfur compounds without the cleansing action of saliva.
- Difficulty wearing dentures: They may slip, rub, and cause irritation.
- Oral infections: Increased susceptibility to fungal infections like oral thrush (candidiasis).
Diagnosis Process — What Your Dentist Does
Diagnosing xerostomia dental is a multi-step process that typically involves a thorough dental examination and a review of your medical history.
- Medical and Dental History: Your dentist will ask about your medications (both prescription and over-the-counter), any existing medical conditions, and your lifestyle habits. This is crucial as medications are a primary cause.
- Clinical Examination: The dentist will look for visual signs of dry mouth, such as:
- Dry, sticky oral mucosa (lining of the mouth)
- Lack of pooling saliva in the floor of the mouth
- Fissured tongue or redness
- Evidence of increased Caries, especially cervical caries (near the gumline)
- Signs of oral candidiasis or angular cheilitis
- Saliva Flow Measurement (Sialometry): This objective test measures the rate of saliva production. It can be stimulated (e.g., by chewing on paraffin wax) or unstimulated.
- Unstimulated Sialometry: Normal flow is typically >0.3-0.4 mL/min. A flow rate <0.1 mL/min is indicative of severe salivary gland hypofunction.
- Stimulated Sialometry: Normal flow is typically >1.0 mL/min. A flow rate <0.7 mL/min suggests hypofunction.
- Imaging (Rarely): In some cases, if salivary gland blockages or tumors are suspected, imaging techniques like sialography (X-rays of salivary glands), CT scans, or MRI might be used.
- Biopsy (Rarely): If Sjögren's syndrome or other autoimmune conditions are suspected, a minor salivary gland biopsy (usually from the lip) might be performed to examine glandular tissue.
- Blood Tests: To check for markers of autoimmune diseases (e.g., anti-Ro/SSA, anti-La/SSB antibodies for Sjögren's syndrome) or other systemic conditions like diabetes.
Treatment Options with Pros, Cons, and Costs
Treatment for xerostomia focuses on three main areas: addressing the underlying cause, symptomatic relief, and preventing complications.
-
Addressing the Underlying Cause:
- Medication Review: If medications are the culprit, your dentist or physician may suggest:
- Adjusting the dosage.
- Switching to an alternative drug with fewer xerostomic side effects.
- Scheduling medication intake to minimize dry mouth during key periods (e.g., before sleep).
- Pros: Can resolve the issue directly if successful.
- Cons: Not always possible, requires physician collaboration, and may affect treatment for other conditions.
- Cost: Generally no direct cost, but medication changes may incur different prescription costs.
- Management of Systemic Diseases: Treating conditions like diabetes or Sjögren's syndrome can sometimes improve salivary flow.
- Pros: Improves overall health.
- Cons: May not fully restore salivary function; often requires ongoing medical management.
- Cost: Varies widely depending on the disease and treatment; typically covered by medical insurance.
- Medication Review: If medications are the culprit, your dentist or physician may suggest:
-
Symptomatic Relief (Saliva Substitutes and Oral Moisturizers):
- Products: Gels, sprays, rinses, lozenges, and toothpastes specifically designed to moisturize the mouth and mimic natural saliva. Common brands include Biotene, Oasis, Xerodent, and ACT Dry Mouth. Many contain xylitol, carboxymethylcellulose, or hydroxyethylcellulose.
- Pros: Provide immediate, temporary relief; over-the-counter and easily accessible; non-pharmacological.
- Cons: Short-acting, requires frequent reapplication; doesn't address the underlying cause or stimulate natural saliva production.
- Cost: $5 - $25 per product, typically lasting 1-4 weeks depending on frequency of use. Not usually covered by dental or medical insurance, but some FSA/HSA plans may cover them.
-
Salivary Stimulants (Sialogogues):
- Prescription Medications:
- Pilocarpine (Salagen): A cholinergic agonist that stimulates muscarinic receptors on salivary glands. Taken orally, typically 5 mg, 3-4 times daily.
- Cevimeline (Evoxac): Also a cholinergic agonist, with a longer duration of action. Taken orally, typically 30 mg, 3 times daily.
- Pros: Stimulates the body's natural saliva production (if functional glandular tissue remains); more effective for moderate to severe xerostomia.
- Cons: Requires a prescription; potential side effects include sweating, nausea, dizziness, increased urination, and blurred vision; contraindications for certain conditions (e.g., uncontrolled asthma, narrow-angle glaucoma); not effective if salivary glands are severely damaged (e.g., post-radiation).
- Cost: Pilocarpine: $30 - $150 per month (generic usually cheaper). Cevimeline: $100 - $300 per month. Often covered by medical insurance with a co-pay.
- Over-the-Counter (OTC) Stimulants: Sugar-free gum, lozenges, or candies containing xylitol.
- Pros: Readily available, can help stimulate saliva, and xylitol has Caries-preventive benefits.
- Cons: Less effective for severe dry mouth, high consumption can cause gastrointestinal upset.
- Cost: $2 - $10 per pack/bag.
- Prescription Medications:
-
Fluoride Therapy and Caries Prevention:
- Importance: With reduced saliva, the risk of Caries (tooth decay) skyrockets. Aggressive Fluoride therapy is paramount.
- Methods:
- Prescription-strength fluoride toothpaste (e.g., 5000 ppm): Used daily.
- Fluoride rinses (e.g., 0.05% sodium fluoride): Used daily.
- Topical fluoride varnish applications: Applied by the dentist during regular check-ups (every 3-6 months).
- Pros: Essential for preventing rampant Caries and can help remineralize early lesions.
- Cons: Requires consistent adherence; prescription fluoride can be an added cost.
- Cost: Prescription fluoride toothpaste: $15 - $30 per tube. Fluoride rinses: $8 - $20 per bottle. Professional fluoride application: $30 - $70 per visit, often covered by dental insurance.
-
Managing Halitosis (Bad Breath):
- Approaches: Since dry mouth exacerbates Halitosis, treatment involves:
- Maintaining excellent oral hygiene (brushing, flossing).
- Using tongue scrapers.
- Incorporating antimicrobial mouthwashes (alcohol-free).
- Treating any underlying oral infections.
- Addressing the dry mouth itself.
- Pros: Improves social confidence and overall oral hygiene.
- Cons: Requires diligence; some mouthwashes can further dry the mouth if they contain alcohol.
- Cost: Regular oral hygiene products $10-$30 per month. Alcohol-free mouthwash $5-$15 per bottle.
- Approaches: Since dry mouth exacerbates Halitosis, treatment involves:
Step-by-Step: What to Expect During Treatment
- Initial Assessment & Diagnosis: Your dentist will conduct a thorough exam, review your history, and perform sialometry.
- Discussion of Causes: Based on the diagnosis, your dentist will identify potential causes (e.g., specific medications, underlying conditions).
- Treatment Plan Development: A personalized plan will be created, often involving a combination of strategies. This may include:
- Consulting your physician to discuss medication changes.
- Prescribing salivary stimulants.
- Recommending specific over-the-counter products (saliva substitutes, fluoride rinses).
- Providing detailed instructions on oral hygiene and diet.
- Scheduling regular fluoride applications and follow-up appointments.
- Implementation: You'll start using prescribed medications and recommended products, and adjust your daily habits.
- Monitoring & Adjustment: Regular follow-up appointments (often every 3-6 months initially) are crucial to monitor your symptoms, check your oral health, and adjust the treatment plan as needed. The dentist will look for improvements in moisture levels, reduction in Caries, and overall oral comfort.
Recovery Timeline and Aftercare
There isn't a "cure" for many causes of chronic xerostomia, especially those due to irreversible salivary gland damage (like severe radiation therapy). Therefore, recovery is often about managing the condition effectively and preventing complications.
- Symptomatic Relief: You may feel relief from saliva substitutes or stimulants within days to weeks, but consistent use is key.
- Dental Health Improvement: Reducing Caries and gum disease risk is a long-term goal. With diligent Fluoride therapy and oral hygiene, you can see a significant reduction in new decay within 6-12 months.
- Aftercare is ongoing: Xerostomia often requires lifelong management.
- Strict Oral Hygiene: Brush twice daily with fluoridated toothpaste, floss daily.
- Consistent Hydration: Sip water frequently throughout the day.
- Avoid Irritants: Limit caffeine, alcohol, tobacco, and sugary/acidic foods.
- Regular Dental Visits: At least every 3-6 months for check-ups, cleanings, and professional fluoride applications.
- Medication Adherence: Take prescribed salivary stimulants as directed.
- Dietary Modifications: Opt for moist, soft foods, use sauces and gravies.
Prevention Strategies
While some causes of xerostomia are unavoidable (e.g., radiation therapy), several strategies can help prevent or mitigate the condition:
- Review Medications Regularly: Discuss all medications with your physician and dentist to identify potential xerostomic side effects and explore alternatives if possible.
- Stay Hydrated: Drink plenty of water throughout the day. Keep a water bottle handy.
- Practice Excellent Oral Hygiene: This won't prevent dry mouth, but it will significantly reduce the risk of Caries and Halitosis if xerostomia develops. Use fluoridated products.
- Avoid Tobacco and Limit Alcohol/Caffeine: These substances dry out the mouth and irritate tissues.
- Breathe Through Your Nose: Address any conditions (allergies, nasal polyps) that lead to chronic mouth breathing, especially during sleep.
- Use a Humidifier: Especially in your bedroom at night to keep the air moist.
- Chew Sugar-Free Gum or Suck on Sugar-Free Candies: Those containing xylitol can stimulate saliva and help prevent Caries.
Cost Ranges in the US (with/without insurance)
The overall cost of managing xerostomia can vary significantly based on the severity of the condition, the chosen treatment options, and insurance coverage.
- Initial Dental Visit & Diagnosis:
- Exam & X-rays: $100 - $300
- Sialometry (Saliva Flow Test): $50 - $150 (may be included in exam or billed separately)
- With Dental Insurance: Typically covered at 80-100% after deductible for routine exams.
- Prescription Medications (Salivary Stimulants):
- Pilocarpine (generic): $30 - $150 per month
- Cevimeline (generic): $100 - $300 per month
- With Medical Insurance: Varies widely by plan and formulary. Co-pays can range from $10 - $70 per month. Without insurance, these costs are out-of-pocket.
- Over-the-Counter Products (Saliva Substitutes, Fluoride Rinses):
- Gels, Sprays, Rinses: $5 - $25 per product, lasting 1-4 weeks.
- Prescription Strength Fluoride Toothpaste: $15 - $30 per tube.
- Insurance: Generally not covered by dental or medical insurance.
- Professional Dental Care (for Caries Prevention & Management):
- Routine Cleanings & Exams: $80 - $200 per visit (typically 2-4 times a year).
- Professional Fluoride Applications: $30 - $70 per application (often done 2-4 times a year).
- Fillings (for Caries): $100 - $300+ per filling, depending on size and material.
- With Dental Insurance: Routine care often covered at 80-100%; fillings covered at 50-80% after deductible.
- Specialist Consultations (e.g., Rheumatologist for Sjögren's):
- Initial Consult: $200 - $500+
- With Medical Insurance: Covered by medical insurance, usually with a specialist co-pay ($30 - $70+).
Total Estimated Annual Cost (without insurance, moderate xerostomia):
- Medications: $360 - $3600 (depending on stimulant choice and generic vs. brand)
- OTC products: $120 - $600
- Dental Visits (4x/year, fluoride): $440 - $1080
- Total: Approximately $920 - $5280 annually, excluding any costs for new Caries treatment or specialist medical care.
Treatment Options Comparison Table
| Treatment Type | Mechanism of Action | Pros | Cons | Typical Cost (US, per month) |
|---|---|---|---|---|
| Saliva Substitutes | Mimic natural saliva, moisturize | Immediate relief, OTC, few side effects | Temporary, frequent reapplication, doesn't stimulate glands | $5 - $25 per product |
| OTC Saliva Stimulants | Mechanical stimulation (gum), xylitol | Natural feel, pleasant, xylitol is anti-Caries | Less effective for severe cases, high consumption can cause GI upset | $2 - $10 per pack |
| Pilocarpine (Rx) | Stimulates muscarinic receptors on glands | Effective if glands are functional, natural saliva | Requires Rx, side effects (sweating), not for damaged glands | $30 - $150 (generic) |
| Cevimeline (Rx) | Similar to pilocarpine, longer action | Effective if glands functional, natural saliva | Requires Rx, side effects (sweating), not for damaged glands | $100 - $300 (generic) |
| Fluoride Therapy | Strengthens enamel, prevents demineralization | Crucial for Caries prevention, remineralizes | Requires consistent use, can be an added cost | $15 - $30 (toothpaste) + $30 - $70 (per professional application) |
| Addressing Underlying Cause | Modifies medication, treats systemic disease | Can resolve the issue directly | Not always possible, requires physician collaboration | Varies (med changes, disease treatment) |
For Parents / Pediatric Considerations
Xerostomia is less common in children than in adults but can occur and has significant implications. Pediatric dry mouth can be particularly concerning due to children's developing dentition and their potential difficulty articulating symptoms.
- Causes in Children:
- Medications: Antihistamines, decongestants, and certain asthma medications can cause dry mouth.
- Systemic Conditions: Autoimmune diseases (like juvenile Sjögren's), diabetes, cystic fibrosis, and certain neurological conditions.
- Radiation Therapy: Children undergoing radiation for head and neck cancers can experience severe, permanent xerostomia.
- Mouth Breathing: Often due to chronic allergies, enlarged tonsils/adenoids, or orthodontic issues.
- Dehydration: Children may not always recognize or communicate thirst effectively.
- Signs to Watch For: Similar to adults, but also look for increased thirst, frequent fluid intake during meals, refusal of dry foods, difficulty speaking, and noticeably increased Caries, especially "rampant caries" affecting many teeth rapidly.
- Dental Implications: Childhood Caries can progress rapidly in a dry mouth environment, potentially leading to pain, infection, and premature tooth loss, which can affect speech, chewing, and proper jaw development.
- Management:
- Identify and address the underlying cause (e.g., change medications with physician, treat allergies).
- Encourage frequent sips of water.
- Use child-friendly, alcohol-free saliva substitutes or fluoride rinses.
- Stress excellent oral hygiene with fluoridated toothpaste.
- Regular dental check-ups (every 3-4 months) with professional fluoride applications.
- Avoid sugary drinks and snacks, especially between meals.
- Consider humidifier in the child's room.
Frequently Asked Questions
Q1: What happens if xerostomia is left untreated?
A: Untreated xerostomia significantly increases the risk of severe dental problems. Without saliva's protective effects, you are much more susceptible to rampant Caries (tooth decay), advanced gum disease (periodontitis), frequent oral infections (like oral thrush), persistent Halitosis (bad breath), difficulty speaking and swallowing, and poor nutrition due to inability to eat certain foods. The quality of life can drastically decline.
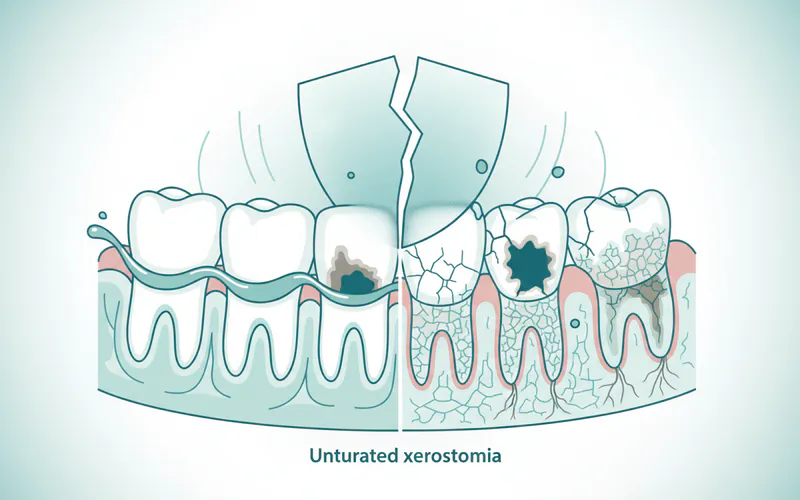
Q2: Is xerostomia painful?
A: While xerostomia itself isn't inherently painful, the lack of moisture can lead to uncomfortable sensations like a burning tongue, cracked lips, and mouth sores. More importantly, the complications of dry mouth, such as extensive Caries or severe oral infections, can cause significant pain and discomfort.
Q3: How long does treatment for xerostomia last?
A: For many individuals, xerostomia is a chronic condition that requires ongoing management. While symptomatic relief can be immediate, addressing the root cause and preventing complications often requires long-term commitment. If the cause is reversible (e.g., a temporary medication), the condition may resolve. However, for causes like Sjögren's syndrome or post-radiation damage, treatment is typically lifelong.
Q4: Are there natural or alternative treatments for xerostomia?
A: While not scientifically proven to cure xerostomia, some natural approaches can help manage symptoms. These include sipping water frequently, chewing sugar-free gum with xylitol, sucking on sugar-free candies, using a humidifier, avoiding dehydrating foods/drinks (caffeine, alcohol), and consuming moist foods. Some people report relief with herbal remedies like aloe vera juice or ginger, but these should be discussed with your dentist or doctor, especially if you're taking other medications. Always prioritize evidence-based treatments.
Q5: Will my dental or medical insurance cover xerostomia treatments?
A: Coverage varies significantly.
- Dental Insurance: Often covers routine exams, cleanings, X-rays, and professional Fluoride applications (often 80-100%). Fillings for Caries are typically covered at 50-80%.
- Medical Insurance: Usually covers prescription medications like pilocarpine or cevimeline (often with a co-pay). Medical tests (blood work, biopsies, specialist consultations) for underlying systemic diseases are also typically covered.
- Over-the-counter products: Saliva substitutes, special toothpastes, and rinses are generally not covered by either dental or medical insurance. You may be able to use a Flexible Spending Account (FSA) or Health Savings Account (HSA) for these. It's crucial to check with your specific insurance providers about coverage details.
Q6: Can xerostomia be cured?
A: Whether xerostomia can be "cured" depends entirely on its underlying cause. If the dry mouth is a side effect of a medication that can be safely discontinued or switched, or if it's due to treatable dehydration, then it can often resolve completely. However, if the cause is irreversible damage to the salivary glands (e.g., from radiation therapy) or a chronic autoimmune disease (like Sjögren's syndrome), the condition cannot be cured and requires ongoing management to alleviate symptoms and prevent complications.
Q7: Does alcohol-free mouthwash help with xerostomia?
A: Yes, using an alcohol-free mouthwash is highly recommended for individuals with xerostomia. Alcohol-based mouthwashes can further dry and irritate the delicate oral tissues, exacerbating dry mouth symptoms. Many specific dry mouth rinses contain moisturizing agents and Fluoride for added protection against Caries, providing both relief and therapeutic benefits without the drying effects of alcohol.
When to See a Dentist
It's important to differentiate between temporary dry mouth (e.g., after a vigorous workout) and chronic xerostomia.
See your dentist routinely (at least annually, preferably every 3-6 months if you experience dry mouth) if you notice:
- A persistent dry, sticky feeling in your mouth that doesn't go away with water.
- Difficulty chewing, swallowing, or speaking.
- Increased thirst or a need to drink water frequently, especially at night.
- Changes in your sense of taste.
- Any of the symptoms described in the "Signs and Symptoms" section, particularly increased Caries, Halitosis, or mouth sores.
- You've started a new medication and noticed dry mouth as a side effect.
See your dentist immediately or seek emergency care if you experience:
- Severe oral pain, swelling, or signs of a serious infection (fever, pus).
- Rapidly worsening Caries that causes severe sensitivity or pain.
- Difficulty breathing or swallowing that is suddenly severe and persistent.
Your dental professional is your primary partner in diagnosing and managing xerostomia. Early intervention can make a significant difference in preserving your oral health and overall well-being.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Zirconia: Complete Dental Guide
In the ever-evolving landscape of modern dentistry, zirconia stands out as a groundbreaking material that has transformed how dental professionals restore smiles. At its core, zirconia is a robust, tooth-colored ceramic material, chemically known as zirconium dioxide (ZrO2). It's not a metal
February 22, 2026
X-Ray (Dental): Complete Dental Guide
Short Definition: Diagnostic imaging that uses low-dose radiation to capture images of teeth, bones, and surrounding tissues, revealing problems not visible during a clinical examination.
February 22, 2026
Wisdom Tooth: Complete Dental Guide
Welcome to SmilePedia.net, your definitive resource for understanding all aspects of dental health. In this comprehensive article, we delve deep into the topic of wisdom teeth, often a source of curiosity, concern, and sometimes, discomfort for many adults.
February 22, 2026
Veneer: Complete Dental Guide
A radiant, confident smile can be one of your most valuable assets, impacting everything from personal interactions to professional opportunities. For many, achieving that ideal smile involves addressing aesthetic concerns like discoloration, chips, gaps, or misaligned teeth. This is where dental **
February 22, 2026