Complete Guide to Soft Tissue & Oral Conditions: Everything You Need to Know
Key Takeaways
- Did you know that estimates suggest nearly half of all Americans will experience at least one oral health issue beyond tooth decay and gum disease in their lifetime? From the annoying pain of a canker sore to the often misunderstood discomfort of tonsil stones, our mouths are complex eco
Complete Guide to Soft Tissue & Oral Conditions: Everything You Need to Know
Did you know that estimates suggest nearly half of all Americans will experience at least one oral health issue beyond tooth decay-conditions-diseases-everything-you-need-to-know "Complete Guide to Dental Conditions & Diseases: Everything You Need to Know") and gum disease in their lifetime? From the annoying pain of a canker sore to the often misunderstood discomfort of tonsil stones, our mouths are complex ecosystems susceptible to a variety of conditions affecting the soft tissues. These conditions, while often benign, can significantly impact your comfort, ability to eat and speak, and overall quality of life. Understanding the nuances of common soft tissue and oral conditions, such as hand foot and mouth disease, cold sore outbreaks, oral thrush, angular cheilitis, and even the intriguing patterns of geographic tongue, is crucial for maintaining optimal oral and systemic health.
This comprehensive guide from SmilePedia.net aims to empower you with medically accurate, detailed information on these frequently encountered issues. We will delve into what these conditions are, their underlying causes, how to recognize their signs and symptoms, and the most effective treatment and prevention strategies available today. Whether you're seeking relief for a persistent hand foot and mouth infection or simply curious about unusual tongue patterns, this article will equip you with everything you need to know to better manage your oral health and understand when it’s time to consult a dental professional.
Key Takeaways:
- Tonsil Stones (Tonsilloliths) are calcified deposits often asymptomatic, but can cause bad breath, sore throat, or difficulty swallowing. Removal can range from $0 (home) to $200-$500 (dental/ENT), typically not covered by basic dental insurance unless part of a medical procedure.
- Canker Sores (Aphthous Ulcers) are painful, non-contagious mouth sores lasting 1-2 weeks. Treatment focuses on pain relief (OTC gels: $5-$20) and can involve prescription rinses (up to $50-$100) or laser therapy ($100-$300 per sore).
- Cold Sores (Herpes Labialis) are contagious, virus-induced blisters, typically lasting 7-10 days. OTC creams are $10-$30, while prescription antivirals (e.g., Acyclovir) can cost $20-$60 for a course.
- Hand, Foot, and Mouth Disease (HFMD) is a common viral infection, especially in children, causing rash and sores. It usually resolves in 7-10 days without specific treatment beyond symptom management. Doctor visits can range from $100-$300 (uninsured).
- Oral Thrush (Candidiasis) is a fungal infection presenting as white patches. It's treatable with antifungal medications (mouth rinses, lozenges, or systemic drugs, costing $15-$150) within 1-2 weeks.
- Angular Cheilitis manifests as cracked, inflamed corners of the mouth. Treatment involves antifungal/antibiotic creams (typically $10-$40) and lifestyle changes, often resolving in few days to 2 weeks.
- Geographic Tongue is a harmless, benign inflammatory condition causing map-like patterns on the tongue. It requires no specific treatment, and symptoms are managed with OTC pain relievers if discomfort arises.
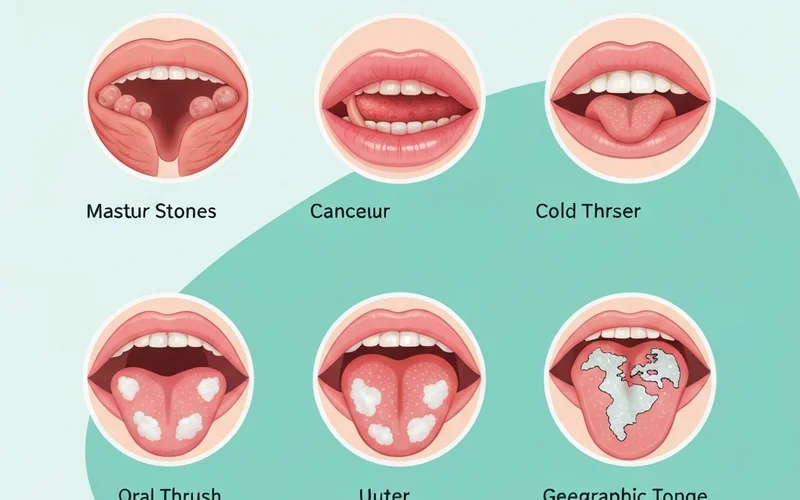
!A vibrant infographic showing different oral conditions with small, clear illustrations: tonsil stones on tonsils, a canker sore inside the lip, a cold sore on the outer lip, white patches of oral thrush on the tongue, and the characteristic map-like pattern of geographic tongue.
Understanding Common Soft Tissue and Oral Conditions
The soft tissues of your mouth — your tongue, cheeks, gums, lips, and throat — are vital for speaking, eating, and acting as a protective barrier. When these tissues are compromised, it can lead to discomfort, pain, and sometimes, more serious health issues. Here, we explore some of the most common soft tissue and oral conditions.
Tonsil Stones (Tonsilloliths)
a. What It Is / Overview Tonsil stones, also known as tonsilloliths, are calcified deposits that form in the crypts (small pockets) of the tonsils. They are composed of bacteria, food debris, mucus, and dead cells that accumulate and harden over time. While often small and asymptomatic, they can grow large enough to cause noticeable symptoms. These stones are surprisingly common, particularly in adults who have had chronic tonsillitis.
b. Causes / Why It Happens The primary cause of tonsil stones is the accumulation of debris in the tonsillar crypts, combined with poor oral hygiene and bacterial activity. Factors contributing to their formation include:
- Deep Tonsillar Crypts: Individuals with deeper, more numerous crevices in their tonsils are more prone to debris accumulation.
- Chronic Tonsillitis: Frequent inflammation of the tonsils can lead to more debris trapping.
- Poor Oral Hygiene: Inadequate brushing and flossing can leave food particles in the mouth that migrate to the tonsils.
- Mucus Production: Excess mucus from allergies or post-nasal drip can contribute to the debris.
- Certain Medications: Some medications that cause dry mouth can also indirectly contribute by reducing saliva's cleansing action.
c. Signs and Symptoms Many small tonsil stones go unnoticed. However, larger or symptomatic stones can cause:
- Bad Breath-everything-you-need-to-know "Complete Guide to Bad Breath (Halitosis): Everything You Need to Know") (Halitosis): This is one of the most common and often the first noticeable symptom, due to the putrefying bacteria within the stones.
- Sore Throat: A feeling of irritation or discomfort in the back of the throat.
- Difficulty Swallowing (Dysphagia): Especially if the stones are large.
- Tonsil Swelling: One or both tonsils may appear enlarged.
- White or Yellow Debris: Visible small white or yellowish lumps on the tonsils.
- Ear Pain: Referred pain can sometimes be felt in the ear.
- Persistent Cough: An irritating sensation in the throat can trigger a cough.
d. Treatment Options Treatment for tonsil stones varies based on size and symptoms:
- Home Remedies:
- Vigorous Gargling: With salt water or non-alcoholic mouthwash can dislodge small stones.
- Manual Removal: Using a cotton swab or a clean finger to gently dislodge visible stones (use caution to avoid injury or gag reflex).
- Oral Irrigators: Water flossers can be effective for flushing crypts gently.
- Professional Removal:
- Dental/ENT Removal: A dentist or ENT specialist can manually remove larger or stubborn stones using specialized tools.
- Laser Cryptolysis: A laser is used to reshape or reduce the size of the tonsillar crypts, making them less prone to trapping debris. This is a more invasive option.
- Coblation Cryptolysis: Similar to laser cryptolysis but uses radiofrequency energy at a lower temperature.
- Tonsillectomy: Surgical removal of the tonsils is a permanent solution for recurrent, problematic tonsil stones, usually reserved for severe cases.
e. Prevention
- Maintain excellent oral hygiene: Brush twice daily, floss daily, and use an ADA-approved mouthwash.
- Gargle regularly: With salt water after meals.
- Stay hydrated: Drink plenty of water to prevent dry mouth.
- Manage allergies: Address post-nasal drip if it contributes to mucus buildup.
f. Risks and Complications While generally harmless, complications can include chronic bad breath, persistent sore throat, difficulty swallowing, and, in rare cases, tonsil abscesses if infections occur around large stones.
g. Cost and Insurance (US)
- Home Remedies: $0-$20 (for salt, mouthwash, or a water flosser).
- Manual Removal (Dentist/ENT): $50-$200 per visit, typically not covered by dental insurance unless deemed medically necessary and coded as a medical procedure.
- Laser/Coblation Cryptolysis: $500-$1,500 per session. Often considered elective and may not be covered by insurance.
- Tonsillectomy: $3,000-$6,000 or more (including anesthesia and facility fees). Often covered by medical insurance if deemed medically necessary due to recurrent tonsillitis or severe tonsil stones.
Pro Tip: For chronic tonsil stones, consult with an Ear, Nose, and Throat (ENT) specialist to discuss permanent solutions like cryptolysis or tonsillectomy, which may offer long-term relief.
Canker Sore (Aphthous Ulcer)
a. What It Is / Overview A canker sore, or aphthous ulcer, is a small, painful, shallow lesion that develops on the soft tissues inside your mouth or at the base of your gums. Unlike cold sores, canker sores are not contagious and do not appear on the surface of the lips. They are one of the most common oral lesions, affecting a significant portion of the population.
b. Types / Variations Canker sores are categorized into three main types:
- Minor Canker Sores: The most common type, usually small (less than 1 centimeter), oval-shaped with a red border, and heal within 1-2 weeks without scarring.
- Major Canker Sores: Larger and deeper, often irregularly shaped, extremely painful, and can take up to six weeks to heal, often leaving scars. Less common than minor canker sores.
- Herpetiform Canker Sores: Despite the name, these are not caused by the herpes virus. They appear as clusters of tiny ulcers (10-100 at a time) that sometimes merge into a large ulcer. They are common in older adults and heal in 1-2 weeks.
c. Causes / Why It Happens The exact cause of canker sores is unknown, but a combination of factors is believed to contribute:
- Minor Mouth Injury: Biting your cheek, aggressive brushing, sports injuries, or dental work.
- Acidic/Spicy Foods: Sensitivity to acidic fruits (citrus, pineapples), chocolate, coffee, nuts.
- Nutritional Deficiencies: Lack of vitamin B12, zinc, folate, or iron.
- Hormonal Shifts: Often seen in women during menstrual cycles.
- Emotional Stress: A known trigger for many people.
- Certain Toothpastes/Mouthwashes: Those containing sodium lauryl sulfate (SLS).
- Immune System Issues: A weakened immune system or certain autoimmune diseases.
- Bacterial/Viral Infections: Though not directly caused by herpes, secondary infections can occur.
- Underlying Medical Conditions: Crohn's disease, celiac disease, Behçet's disease.
d. Signs and Symptoms
- Painful Sore(s): Typically round or oval, white or yellow center, with a red border.
- Tingling/Burning Sensation: Often precedes the visible sore by a day or two.
- Difficulty Eating/Speaking: Due to the pain.
- Fever/Malaise: In severe cases, especially with major or herpetiform sores.
e. Treatment Options Treatment focuses on pain relief, speeding healing, and preventing infection:
- Over-the-Counter (OTC) Remedies:
- Topical Anesthetics: Benzocaine (Orajel), lidocaine, or various numbing gels/sprays.
- Protective Pastes: Oral bandages or patches that cover the sore, providing relief and promoting healing.
- Antiseptic Rinses: Diluted hydrogen peroxide or chlorhexidine rinses can help prevent secondary infection.
- Prescription Medications:
- Corticosteroid Gels/Rinses: Fluocinonide, dexamethasone, or clobetasol to reduce inflammation and pain.
- Antimicrobial Rinses: Chlorhexidine gluconate.
- Oral Medications: For severe, recurrent canker sores, systemic corticosteroids or immunosuppressants may be prescribed.
- Laser Treatment: Low-level laser therapy (LLLT) can significantly reduce pain and accelerate healing time for individual sores.
f. Recovery and Aftercare Most minor canker sores heal naturally within 1-2 weeks. During this time:
- Avoid irritating foods (spicy, acidic, hot).
- Use a soft-bristled toothbrush.
- Maintain good oral hygiene to prevent secondary infection.
- Stay hydrated.
g. Prevention
- Identify and avoid trigger foods.
- Use an SLS-free toothpaste.
- Manage stress.
- Address any nutritional deficiencies with your doctor.
- Be gentle when brushing and flossing.
h. Cost and Insurance (US)
- OTC Gels/Rinses: $5-$25.
- Prescription Rinses/Gels: $20-$100 (cost depends on medication and insurance coverage).
- Laser Treatment: $100-$300 per sore, often not covered by dental insurance as it's considered an elective or palliative treatment.
- Doctor/Dentist Visit: $75-$250 without insurance. Insurance may cover a portion if it's considered a diagnostic or medical visit.
Cold Sore (Herpes Labialis)
a. What It Is / Overview A cold sore, also known as a fever blister or herpes labialis, is a common viral infection caused by the herpes simplex virus type 1 (HSV-1). It manifests as small, fluid-filled blisters on or around the lips, though they can sometimes appear on the nose or chin. Cold sores are highly contagious and can be transmitted through direct contact. Once infected, the virus remains dormant in nerve cells and can reactivate periodically, leading to recurrent outbreaks.
b. Causes / Why It Happens Cold sores are caused exclusively by the HSV-1 virus. Initial exposure usually occurs in childhood through close contact with an infected person (e.g., kissing, sharing utensils). Triggers for reactivation include:
- Stress: Emotional or physical stress.
- Sunlight/Wind Exposure: UV radiation can trigger an outbreak.
- Fever/Illness: Hence the name "fever blister."
- Hormonal Changes: Menstruation or pregnancy.
- Immune Suppression: Weakened immune system due to illness or medications.
- Dental Procedures/Trauma: Manipulating the lips or mouth area.
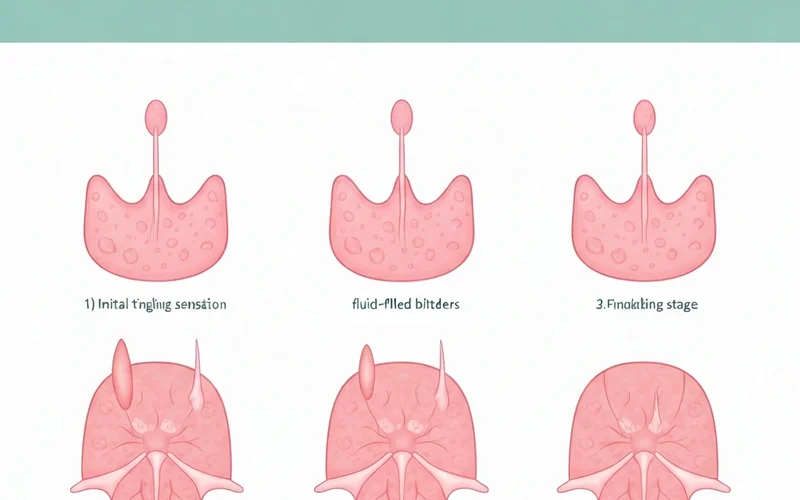
c. Signs and Symptoms Cold sores typically progress through several stages:
- Tingling, Itching, or Burning: Often the first sign, felt a day or two before the blisters appear.
- Blisters: Small, fluid-filled blisters erupt, usually along the border of the lips.
- Oozing and Crusting: The blisters burst, forming shallow, open sores that then dry out and crust over with a yellow or brownish scab.
- Healing: The scab falls off, and the sore heals, usually without scarring.
The entire process typically takes 7-10 days.
d. Treatment Options While there's no cure for HSV-1, treatments can speed healing and reduce discomfort:
- Over-the-Counter (OTC) Creams:
- Docosanol (Abreva): Can shorten healing time if applied at the first sign.
- Pain Relievers: Benzocaine or lidocaine creams for discomfort.
- Petroleum Jelly: To keep the area moist and prevent cracking.
- Prescription Antiviral Medications:
- Topical Creams: Acyclovir, penciclovir (Denavir).
- Oral Antivirals: Acyclovir (Zovirax), valacyclovir (Valtrex), famciclovir (Famvir). These are most effective when started at the very first sign of an outbreak (tingling stage) and can significantly shorten the duration and severity of the sore.
e. Step-by-Step Process (for an Outbreak)
- Prodromal Stage: At the first tingle, itch, or burn, immediately apply an OTC antiviral cream like Abreva or take prescribed oral antivirals.
- Blister Stage: Keep the area clean and moist (e.g., with petroleum jelly). Avoid picking or popping the blisters, as this can spread the virus and lead to secondary infection.
- Oozing and Crusting: Continue keeping the area clean. Use a mild antiseptic if recommended by your dentist/doctor.
- Healing: The sore will gradually heal. Avoid touching it unnecessarily.
f. Prevention
- Avoid Triggers: Identify and try to minimize exposure to personal triggers (sunscreen on lips, stress management).
- Protect from Sun: Use lip balm with SPF 30 or higher.
- Hygiene: Avoid sharing utensils, lip balm, or towels with others, especially during an active outbreak.
- Antiviral Medication: For very frequent outbreaks, a doctor might prescribe daily suppressive antiviral therapy.
g. Risks and Complications
- Spread to other body parts: Herpetic whitlow (fingers), ocular herpes (eyes, potentially leading to blindness).
- Spread to others: Highly contagious.
- Secondary bacterial infection: If the sore becomes infected.
- Immunocompromised individuals: More severe and prolonged outbreaks.
h. Cost and Insurance (US)
- OTC Creams (Abreva, pain relievers): $10-$30.
- Prescription Topical Antivirals: $20-$70 (generic) or $100-$200+ (brand name) without insurance, often covered by prescription plans.
- Prescription Oral Antivirals: A course of generic acyclovir can be $20-$60. Valacyclovir or Famciclovir can range from $50-$150 for a short course, depending on insurance.
!A series of illustrations depicting the stages of a cold sore outbreak: 1) initial tingling sensation, 2) appearance of fluid-filled blisters, 3) blisters rupturing and crusting over, and 4) the final healing stage.
Hand, Foot, and Mouth Disease (HFMD)
a. What It Is / Overview Hand, Foot, and Mouth Disease (HFMD) is a common, contagious viral infection that primarily affects infants and young children, though adults can contract it. It is most commonly caused by coxsackievirus A16, but other enteroviruses can also be responsible. HFMD is characterized by sores in the mouth and a rash on the hands and feet. It is distinct from foot-and-mouth disease (hoof-and-mouth disease) which affects livestock.
b. Causes / Why It Happens HFMD is spread through person-to-person contact with respiratory droplets (coughing, sneezing), fluid from blisters, or stool of an infected person. It is highly contagious, especially in settings like daycare centers and schools.
c. Signs and Symptoms Symptoms typically appear 3-7 days after exposure:
- Fever: Often the first symptom, usually low-grade.
- Sore Throat: Followed by mouth sores.
- Malaise: General feeling of being unwell.
- Painful Mouth Sores: Flat, red spots that blister and often appear on the tongue, gums, and inside of the cheeks. These can make eating and drinking very painful.
- Rash: Red spots, sometimes with blisters, on the palms of the hands, soles of the feet, and sometimes the buttocks. The rash is typically non-itchy.
- Loss of Appetite: Due to painful mouth sores.
d. Treatment Options There is no specific antiviral treatment for HFMD. Treatment focuses on symptom relief while the body fights off the infection:
- Pain Relief:
- OTC Pain Relievers: Acetaminophen (Tylenol) or ibuprofen (Advil, Motrin) for fever and pain.
- Topical Oral Anesthetics: Gels or rinses (e.g., those containing lidocaine or benzocaine, or "magic mouthwash" concoctions prescribed by a doctor) can help numb mouth sores.
- Hydration: Crucial to prevent dehydration, especially in children who may refuse to drink due to painful sores. Offer cool liquids, water, diluted juices, or popsicles.
- Soft Foods: Serve soft, bland foods that are easy to swallow. Avoid acidic, spicy, or hot foods.
e. Step-by-Step Process (Managing HFMD)
- Monitor Symptoms: Watch for fever, sore throat, and the appearance of mouth sores and rash.
- Hydrate: Encourage fluid intake consistently.
- Pain Management: Administer age-appropriate OTC pain relievers as directed.
- Oral Comfort: Use gentle mouth rinses or prescribed topical anesthetics for mouth sores.
- Isolate: Keep the infected individual home from school/daycare to prevent spread, typically until fever is gone and mouth sores have healed.
- Hand Hygiene: Emphasize frequent hand washing for all household members.
f. Prevention
- Frequent Hand Washing: With soap and water for at least 20 seconds, especially after changing diapers or using the toilet.
- Disinfection: Regularly disinfect frequently touched surfaces and shared toys.
- Avoid Close Contact: Do not kiss, hug, or share eating utensils or drinks with infected individuals.
- Stay Home When Sick: Keep children home from school or daycare until they are fever-free and feeling better.
g. Risks and Complications Dehydration is the most common complication due to painful mouth sores preventing adequate fluid intake. Rarely, more severe complications like viral meningitis or encephalitis can occur, requiring urgent medical attention.
h. Children / Pediatric Considerations HFMD is most common in children under 5. Parents should be particularly vigilant about hydration and pain management. Always consult a pediatrician for diagnosis and specific guidance. The use of "magic mouthwash" (often a mix of lidocaine, antacids, and diphenhydramine) should be discussed with a doctor, especially for young children, due to potential side effects.
i. Cost and Insurance (US)
- OTC Pain Relievers: $5-$15.
- Doctor/Pediatrician Visit: $100-$300 without insurance, often covered by medical insurance plans.
- Prescription Oral Rinses: $20-$70, depending on formulation and insurance.
Oral Thrush (Oral Candidiasis)
a. What It Is / Overview Oral thrush, also known as oral candidiasis, is a fungal infection of the mouth and throat caused by an overgrowth of Candida albicans, a yeast that is naturally present in small amounts in the mouth. When the immune system is compromised or the balance of microorganisms in the mouth is disrupted, Candida can multiply unchecked, leading to symptoms.
b. Causes / Why It Happens Several factors can lead to an overgrowth of Candida:
- Weakened Immune System: Infants, the elderly, and individuals with conditions like HIV/AIDS, cancer, or organ transplants are at higher risk.
- Antibiotic Use: Broad-spectrum antibiotics can kill beneficial bacteria, allowing Candida to thrive.
- Corticosteroid Use: Inhaled corticosteroids for asthma (without rinsing afterward) or oral corticosteroids.
- Diabetes: Uncontrolled blood sugar levels create a favorable environment for yeast growth.
- Dry Mouth (Xerostomia): Reduced saliva flow can impair the mouth's natural cleansing mechanisms.
- Denture Use: Ill-fitting or improperly cleaned dentures can trap Candida.
- Smoking: Can alter the oral environment.
c. Signs and Symptoms
- White, Creamy Lesions: Typically on the tongue, inner cheeks, roof of the mouth, gums, and tonsils. These patches may resemble cottage cheese.
- Redness or Soreness: Beneath the white patches, the tissue may be red and inflamed.
- Mild Bleeding: If the lesions are scraped or rubbed.
- Cracking at Mouth Corners (Angular Cheilitis): Often accompanies oral thrush.
- Loss of Taste: Or an unpleasant taste in the mouth.
- Pain while Eating or Swallowing: If the infection spreads to the throat.
d. Treatment Options Treatment involves antifungal medications:
- Topical Antifungals:
- Nystatin (Mycostatin): An antifungal rinse or lozenge that dissolves in the mouth.
- Clotrimazole (Mycelex): An antifungal lozenge.
- Systemic Antifungals:
- Fluconazole (Diflucan): An oral antifungal pill, usually prescribed for more severe cases or when topical treatments are ineffective.
e. Step-by-Step Process (for treatment)
- Diagnosis: A dentist or doctor will usually diagnose thrush visually or by gently scraping a lesion for microscopic examination.
- Prescription: An antifungal medication (rinse, lozenge, or pill) will be prescribed.
- Administration: Follow dosage and duration instructions carefully. For rinses, swish for several minutes before swallowing or spitting. For lozenges, allow them to dissolve slowly.
- Denture Care: If you wear dentures, they must be thoroughly cleaned and disinfected daily. Soaking them overnight in an antiseptic solution (e.g., chlorhexidine or dilute bleach solution) may be recommended.
- Oral Hygiene: Continue regular brushing and flossing gently.
f. Prevention
- Good Oral Hygiene: Brush twice daily, floss daily.
- Rinse After Inhaled Steroids: If using an inhaled corticosteroid, rinse your mouth with water and spit after each use.
- Denture Care: Clean dentures thoroughly every day and remove them at night.
- Diabetes Control: Manage blood sugar levels effectively.
- Address Dry Mouth: Use saliva substitutes if experiencing xerostomia.
g. Risks and Complications In individuals with severely compromised immune systems, oral thrush can spread beyond the mouth to the esophagus, lungs, or other parts of the body, leading to systemic infections.
h. Children / Pediatric Considerations Oral thrush is very common in infants, especially newborns. It often presents as white patches in the mouth and can cause discomfort during feeding. It can be passed between mother and baby during breastfeeding. Treatment involves antifungal drops or gel for the infant and sometimes for the mother's nipples.
i. Cost and Insurance (US)
- Topical Antifungals (Nystatin, Clotrimazole): $15-$70 for a course, often covered by prescription insurance.
- Oral Antifungals (Fluconazole): $10-$50 for a short course, highly dependent on generic vs. brand and insurance.
- Dentist/Doctor Visit: $75-$250 without insurance.
Angular Cheilitis (Perleche)
a. What It Is / Overview Angular cheilitis, also known as perleche or angular stomatitis, is an inflammatory condition affecting the corners of the mouth. It typically presents as redness, cracking, soreness, and sometimes crusting or bleeding at one or both labial commissures (the angles of the mouth). It's not usually contagious through casual contact but can be a sign of underlying issues.
b. Causes / Why It Happens Angular cheilitis is often multifactorial, usually involving a combination of moisture, irritation, and opportunistic infection:
- Moisture Trapping: Saliva accumulates at the corners of the mouth, creating a warm, moist environment conducive to microbial growth. This is common in people who frequently lick their lips, have ill-fitting dentures, or experience excessive drooling.
- Fungal Infection: Most commonly Candida albicans (yeast), similar to oral thrush.
- Bacterial Infection: Staphylococcus aureus or Streptococcus species can also cause or complicate the condition.
- Nutritional Deficiencies: Iron, zinc, or B vitamin (especially B2/riboflavin, B9/folate, B12) deficiencies.
- Ill-fitting Dentures: Can reduce the vertical dimension of the face, leading to deeper folds at the mouth corners where saliva pools.
- Immunosuppression: Weakened immune system.
- Chronic Dry Mouth: Can lead to lip licking, exacerbating the problem.
- Smoking: Irritates the oral tissues.
- Medical Conditions: Diabetes, inflammatory bowel disease.
c. Signs and Symptoms
- Redness and Inflammation: At the corners of the mouth.
- Cracking and Fissures: Painful splits in the skin.
- Scaling and Crusting: Dry, flaky skin, sometimes with scabs.
- Pain and Discomfort: Especially when opening the mouth wide, eating, or speaking.
- Bleeding: If the fissures are deep.
- Burning or Itching Sensation.
d. Treatment Options Treatment targets the underlying cause and involves:
- Topical Antifungal Cream: If Candida is suspected (e.g., nystatin, clotrimazole, miconazole).
- Topical Antibiotic Cream: If bacterial infection is present (e.g., fusidic acid, mupirocin).
- Combination Creams: Some creams contain both antifungal and mild corticosteroid components to reduce inflammation.
- Moisturizing Agents: Petroleum jelly or thick emollients to keep the corners of the mouth protected and prevent further cracking.
- Nutritional Supplements: If a deficiency is identified (iron, zinc, B vitamins).
- Denture Adjustment/Replacement: If ill-fitting dentures are a contributing factor.
e. Recovery and Aftercare With appropriate treatment, angular cheilitis usually resolves within a few days to two weeks.
- Avoid licking the affected area.
- Keep the corners of the mouth clean and dry.
- Apply prescribed creams as directed.
- Ensure dentures are clean and fit properly.
f. Prevention
- Maintain good oral hygiene.
- Address any underlying nutritional deficiencies.
- Ensure dentures fit well and are cleaned regularly.
- Avoid excessive lip licking.
- Keep lips moisturized to prevent dryness.
g. Risks and Complications Untreated angular cheilitis can become chronic, lead to secondary bacterial infections, or cause significant discomfort.
h. Cost and Insurance (US)
- OTC Lip Balms/Emollients: $5-$15.
- Prescription Topical Creams (antifungal/antibiotic): $10-$40 for a tube, typically covered by prescription insurance.
- Nutritional Supplements: $10-$30 per month.
- Dentist/Doctor Visit: $75-$250 without insurance.
Geographic Tongue (Benign Migratory Glossitis)
a. What It Is / Overview Geographic tongue, medically known as benign migratory glossitis, is a harmless inflammatory condition affecting the surface of the tongue. It gets its name from its characteristic map-like appearance: irregular, red, smooth patches (where papillae are missing) surrounded by raised, whitish or yellowish borders. These patterns can change location, size, and shape over hours or days, making it "migratory." It is not contagious and is not a sign of infection or cancer.
b. Causes / Why It Happens The exact cause of geographic tongue is unknown, but it's believed to be an inflammatory process. It often runs in families, suggesting a genetic predisposition. While typically harmless, it has been linked to:
- Psoriasis: A skin condition, though the link is not fully understood.
- Allergies: Some individuals report triggers related to specific foods or environmental allergens.
- Stress: Emotional stress can sometimes exacerbate symptoms.
- Hormonal Fluctuations: In some women, it may coincide with menstrual cycles.
- Nutritional Deficiencies: Rarely, iron or B vitamin deficiencies are implicated.
- Fissured Tongue: Often occurs concurrently with geographic tongue.
c. Signs and Symptoms
- Irregular Red Patches: Smooth, red areas on the top or sides of the tongue where tiny, mushroom-shaped projections (filiform papillae) are absent.
- Raised White/Yellow Borders: Surrounding the red patches.
- Changing Patterns: The patches can appear, disappear, and migrate to different areas of the tongue within a short period.
- Mild Discomfort/Sensitivity: Some individuals experience sensitivity to hot, spicy, acidic, or salty foods, or a mild burning or stinging sensation. Many people experience no symptoms at all.
d. Treatment Options Geographic tongue is a benign condition that typically requires no treatment. If discomfort or sensitivity is present, management focuses on symptom relief:
- Avoid Irritants: Steer clear of very hot, spicy, acidic, or salty foods and alcoholic beverages that may exacerbate sensitivity.
- OTC Pain Relievers: Acetaminophen or ibuprofen can help with mild discomfort.
- Topical Anesthetics: Numbing gels (e.g., benzocaine) can provide temporary relief.
- Antihistamines/Corticosteroids: In rare cases of significant discomfort, a dentist or doctor may prescribe a topical corticosteroid mouth rinse or antihistamine rinse to reduce inflammation and sensitivity.
e. Prevention Since the cause is unknown, specific prevention is not possible. However, avoiding known irritants can help manage symptoms.
f. Risks and Complications Geographic tongue is harmless and does not lead to cancer or other serious health problems. The main "complication" is the psychological distress some individuals experience due to the unusual appearance of their tongue.
g. Cost and Insurance (US)
- OTC Pain Relievers/Numbing Gels: $5-$25.
- Prescription Rinses (if needed): $20-$100, depending on medication and insurance.
- Dentist/Doctor Visit: $75-$250 without insurance, primarily for diagnosis and reassurance.
Comparison of Common Oral Conditions
To help distinguish between some of these conditions, especially those with similar-looking symptoms or causes, here's a comparison table:
| Feature | Tonsil Stones | Canker Sore (Aphthous Ulcer) | Cold Sore (Herpes Labialis) | Oral Thrush (Candidiasis) |
|---|---|---|---|---|
| Location | Tonsils | Inside cheeks, lips, tongue, gums | Outside lips, near nose/chin | Tongue, inner cheeks, roof of mouth |
| Appearance | White/yellow calcified lumps | White/yellow center, red border, round/oval | Fluid-filled blisters, then crusts | Creamy white patches, can be scraped off |
| Contagious? | No | No | Yes, highly contagious | No (but can spread yeast) |
| Cause | Debris, bacteria, calcification | Unknown (trauma, stress, deficiencies) | Herpes Simplex Virus Type 1 (HSV-1) | Candida albicans overgrowth |
| Pain Level | Mild to moderate (sore throat, swallowing issues) | Moderate to severe | Moderate to severe (tingling, burning) | Mild to moderate (soreness, discomfort) |
| Duration | Chronic, or dislodged in days | 1-2 weeks (minor), up to 6 weeks (major) | 7-10 days (outbreak) | 1-2 weeks (with treatment) |
| Treatment | Gargling, manual removal, surgery | OTC gels, prescription rinses, laser therapy | Antiviral creams/pills | Antifungal rinses/pills |
| Prevention | Oral hygiene, hydration | Avoid triggers, SLS-free toothpaste | Avoid triggers, sunscreen, antivirals | Good hygiene, manage underlying conditions |
Estimated Treatment Cost Comparison (US Dollars, Uninsured)
| Condition | Initial Consultation | OTC Treatments | Prescription Medications (short course) | Advanced/Specialty Treatment | Total Estimated Cost Range (Typical) |
|---|---|---|---|---|---|
| Tonsil Stones | $75 - $250 | $5 - $20 | N/A | $500 - $6,000 (cryptolysis/tonsillectomy) | $0 - $6,000+ |
| Canker Sore | $75 - $250 | $5 - $25 | $20 - $100 | $100 - $300 (laser per sore) | $5 - $500 |
| Cold Sore | $75 - $250 | $10 - $30 | $20 - $150 | N/A | $10 - $300 |
| HFMD | $100 - $300 (Pediatrician) | $5 - $15 (pain relief) | $20 - $70 (oral rinses) | N/A | $5 - $370 |
| Oral Thrush | $75 - $250 | N/A | $15 - $150 | N/A | $15 - $400 |
| Angular Cheilitis | $75 - $250 | $5 - $15 | $10 - $40 | N/A | $5 - $300 |
| Geographic Tongue | $75 - $250 | $5 - $25 | $20 - $100 | N/A | $5 - $375 |

Note: These are estimated ranges for uninsured individuals in the US and can vary widely based on location, provider, and specific treatment plan. Insurance coverage will significantly reduce out-of-pocket costs for many items.
Children / Pediatric Considerations
Many soft tissue and oral conditions are particularly common or present unique challenges in children. Understanding these age-specific considerations is vital for parents and caregivers:
- Hand, Foot, and Mouth Disease (HFMD): As discussed, HFMD predominantly affects young children. Parents must focus on hydration to prevent dehydration due to painful mouth sores. Lukewarm or cool liquids, popsicles, and soft, bland foods are best. Monitor for signs of severe dehydration (decreased urination, lethargy) and seek medical attention if concerned.
- Oral Thrush: Infants, especially newborns, frequently develop oral thrush because their immune systems are still maturing, and the balance of oral flora is easily disrupted. It appears as white patches that don't wipe away easily. Treatment usually involves prescription antifungal drops or gels for the baby and, if breastfeeding, potentially for the mother's nipples to prevent reinfection.
- Canker Sores: While less common in very young children, older children and teenagers can get canker sores, often triggered by stress, minor trauma (like biting their cheek), or certain foods. Pain relief with OTC numbing gels and avoiding irritants are key.
- Cold Sores: Children can contract HSV-1, usually through close contact with an infected adult. The first outbreak can sometimes be severe (herpetic gingivostomatitis) with widespread mouth sores and fever. Subsequent outbreaks are typically limited to a single cold sore. Education on not sharing utensils or drinks and avoiding direct contact during an outbreak is important to prevent spread.
- Angular Cheilitis: While less common than in adults, children can develop angular cheilitis, often linked to thumb-sucking, pacifier use, or excessive drooling that keeps the mouth corners moist. Addressing these habits and treating any fungal/bacterial infection is crucial.
For any persistent or concerning oral condition in a child, a consultation with a pediatrician or pediatric dentist is recommended. They can provide accurate diagnosis and age-appropriate treatment plans, adhering to guidelines from the American Academy of Pediatric Dentistry (AAPD).
Cost Breakdown
The financial aspect of managing soft tissue and oral conditions can vary significantly. Understanding potential costs and insurance coverage is important.
Average US Costs (Low, Mid, High, without insurance):
- Routine Dental/Medical Visit: $75 - $250
- Basic Over-the-Counter (OTC) Treatments: $5 - $30
- Prescription Oral Medications/Rinses: $15 - $150 per course
- Minor In-Office Procedures (e.g., manual tonsil stone removal, laser for canker sore): $50 - $300
- Major Surgical Procedures (e.g., tonsillectomy for severe tonsil stones): $3,000 - $6,000+
With vs. Without Insurance:
- Dental Insurance: Generally focuses on restorative and preventive care. While some plans might cover diagnostic exams for oral lesions, they typically do not cover medications or procedures specifically for conditions like cold sores, canker sores, or HFMD, as these are often considered medical rather than dental issues.
- Medical Insurance: Most prescription medications (antivirals, antifungals, antibiotics, strong topical steroids) for these conditions are covered by medical prescription plans, often with a co-pay (e.g., $5-$50). Doctor/ER visits are also typically covered, subject to deductibles and co-pays (e.g., $20-$100). Surgical procedures like tonsillectomy, when medically necessary, are usually covered by medical insurance.
- No Insurance: Without insurance, you are responsible for the full cost of consultations, prescriptions, and any procedures. This is where costs can quickly add up, especially for conditions requiring specialists or multiple visits.
Payment Plans and Financing Options:
- Dental/Medical Offices: Many offices offer in-house payment plans for larger procedures, allowing you to pay over several months.
- Healthcare Credit Cards: Options like CareCredit offer special financing for health-related expenses, often with interest-free periods if paid in full within a certain timeframe.
- Flexible Spending Accounts (FSAs) and Health Savings Accounts (HSAs): If you have an FSA or HSA through your employer or health plan, you can use pre-tax dollars to cover eligible medical and dental expenses, including prescriptions and treatments for these conditions.
Cost-Saving Tips:
- Communicate with your provider: Ask about generic medication options, which are significantly cheaper than brand names.
- Shop around for prescriptions: Use apps or websites (e.g., GoodRx) to compare prices at different pharmacies.
- Preventive Care: Good oral hygiene and managing underlying health conditions can reduce the frequency and severity of many oral problems, saving future treatment costs.
- Telehealth: For initial consultations or follow-ups for non-emergency conditions, telehealth appointments can sometimes be a more affordable option than in-person visits.
- Community Clinics: Look for local health centers or dental schools that may offer services at reduced rates.
Frequently Asked Questions
What causes recurrent canker sores, and how can I prevent them?
Recurrent canker sores are often triggered by a combination of factors including minor trauma, stress, acidic foods, nutritional deficiencies (like B12, iron, folate), or certain toothpastes containing sodium lauryl sulfate (SLS). Prevention strategies include identifying and avoiding personal triggers, using an SLS-free toothpaste, managing stress, and ensuring a balanced diet. If they are very frequent, your dentist or doctor may investigate underlying systemic conditions.
Are tonsil stones harmful, and do they always need to be removed?
Tonsil stones are generally not harmful, though they can cause symptoms like bad breath, sore throat, or difficulty swallowing. Small, asymptomatic stones usually do not require professional removal and can often be managed with vigorous gargling. Removal is typically recommended if they cause significant discomfort, chronic bad breath, or recurrent infections. In severe cases, surgical options might be considered.

How can I tell the difference between a cold sore and a canker sore?
The key differences lie in their location and contagiousness. Cold sores appear on the outside of the lips or around the mouth, are caused by the highly contagious HSV-1 virus, and start as blisters that crust over. Canker sores form inside the mouth (cheeks, gums, tongue), are not contagious, and present as painful, open ulcers with a white or yellow center and a red border.
Is Hand, Foot, and Mouth Disease dangerous for adults?
While HFMD is usually a mild illness that resolves in 7-10 days, adults can contract it and may experience more severe symptoms than children, including higher fever, more intense body aches, and a more pronounced rash. Serious complications like viral meningitis are rare but can occur in both children and adults. Pregnant women should be especially cautious, as infection near delivery could pass to the newborn.
Can oral thrush be a sign of a more serious health problem?
Yes, oral thrush can sometimes indicate an underlying health issue, particularly a weakened immune system. While common in infants and individuals on certain medications (like antibiotics or corticosteroids), persistent or recurrent thrush in otherwise healthy adults should prompt a medical evaluation to rule out conditions such as diabetes, HIV, or other immune-compromising disorders.
How long does it take for angular cheilitis to heal?
With appropriate treatment, angular cheilitis typically starts to improve within a few days and fully resolves within one to two weeks. The duration depends on the underlying cause (fungal, bacterial, or nutritional deficiency) and how consistently the prescribed topical creams are applied and contributing factors (like lip licking or ill-fitting dentures) are addressed.
Do I need to treat geographic tongue, even if it doesn't hurt?
No, if geographic tongue is asymptomatic and causes no discomfort, no specific treatment is necessary. It is a benign condition that does not lead to serious health problems. The primary goal of treatment, if symptoms arise, is to manage any sensitivity or burning sensations. Reassurance from a dental professional about its harmless nature is often the most important "treatment."

Can stress cause oral conditions like canker sores or cold sores?
Absolutely. Stress is a well-known trigger for both canker sores and cold sores. Emotional and physical stress can suppress the immune system, making the body more susceptible to flare-ups of conditions like cold sores (reactivating the dormant HSV-1 virus) or triggering the onset of canker sores in susceptible individuals. Managing stress through relaxation techniques, exercise, and adequate sleep can help reduce outbreaks.
Are there any dietary changes that can help prevent these conditions?
For some conditions, yes. A balanced diet rich in vitamins and minerals (especially B vitamins, iron, and zinc) can help prevent canker sores and angular cheilitis linked to nutritional deficiencies. Avoiding very acidic, spicy, or crunchy foods can reduce irritation that might trigger canker sores or exacerbate geographic tongue symptoms. For oral thrush, reducing sugar intake may help, as yeast thrives on sugar.
Should I see a dentist or a doctor for soft tissue conditions?
For most soft tissue conditions in the mouth, your dentist is often the first and best point of contact. Dentists are experts in oral health and can diagnose and often treat many conditions. However, for systemic conditions like Hand, Foot, and Mouth Disease, or if you suspect an underlying medical cause (e.g., weakened immune system, severe nutrient deficiencies), consulting your primary care physician is appropriate. For recurrent or complex cases, your dentist may refer you to an oral surgeon, periodontist, or an Ear, Nose, and Throat (ENT) specialist.
When to See a Dentist
While many soft tissue and oral conditions are minor and resolve on their own, there are clear warning signs that necessitate a visit to your dentist or, in some cases, an emergency medical professional. Don't hesitate to seek professional advice if you experience any of the following:
- Persistent Sores: Any mouth sore that does not heal within two weeks should be evaluated by a dentist. This is especially critical for any lesion that appears white, red, or mixed red and white, as it could be a sign of oral cancer.
- Severe Pain: If an oral lesion causes severe, debilitating pain that interferes with eating, speaking, or sleeping, a dentist can provide diagnosis and pain management solutions.
- Difficulty Swallowing or Breathing: These are medical emergencies. If you experience sudden difficulty swallowing (dysphagia), shortness of breath, or a feeling of a lump in your throat, seek immediate medical attention. This could indicate a severe infection, allergic reaction, or airway compromise.
- Fever and Malaise: If an oral condition is accompanied by a high fever, swollen lymph nodes, or a general feeling of illness, it could indicate a more widespread infection that requires medical assessment.
- Rapidly Spreading Rash/Sores: For conditions like Hand, Foot, and Mouth Disease, while generally mild, a rapidly spreading or unusually severe rash, or signs of dehydration (especially in children), warrants a doctor's visit.
- Bleeding: Unexplained or persistent bleeding from an oral lesion or your gums should always be checked by a dentist.
- Recurrent Issues: If you frequently experience cold sores, canker sores, or oral thrush, a dental professional can help identify triggers, prescribe preventive medications, or investigate potential underlying health issues.
- White Patches That Won't Scrape Off: While oral thrush can often be scraped off, other white lesions like leukoplakia (a precancerous condition) cannot. Any persistent white patch should be examined.
Regular dental check-ups are crucial for early detection and management of all oral conditions, even those you might not notice yourself. Your dentist is an invaluable partner in maintaining not just your teeth, but your entire oral and often systemic health.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

Oral Candidiasis Symptoms: Complete Guide
Oral candidiasis, commonly known as oral thrush, is a fungal infection of the mouth caused by an overgrowth of Candida yeast, most often Candida albicans. While Candida is a normal inhabitant of the human mouth in small amounts, an imbalance can lead to uncomfortable and sometimes painful symptoms
February 23, 2026
Are Cold Sores Contagious
In the United States, an estimated 67% of the population under age 50 carries the herpes simplex virus type 1 (HSV-1), the primary cause of cold sores. This means millions of Americans are susceptible to these often painful and highly visible oral lesions. Beyond the discomfort and cosmetic conc
February 23, 2026
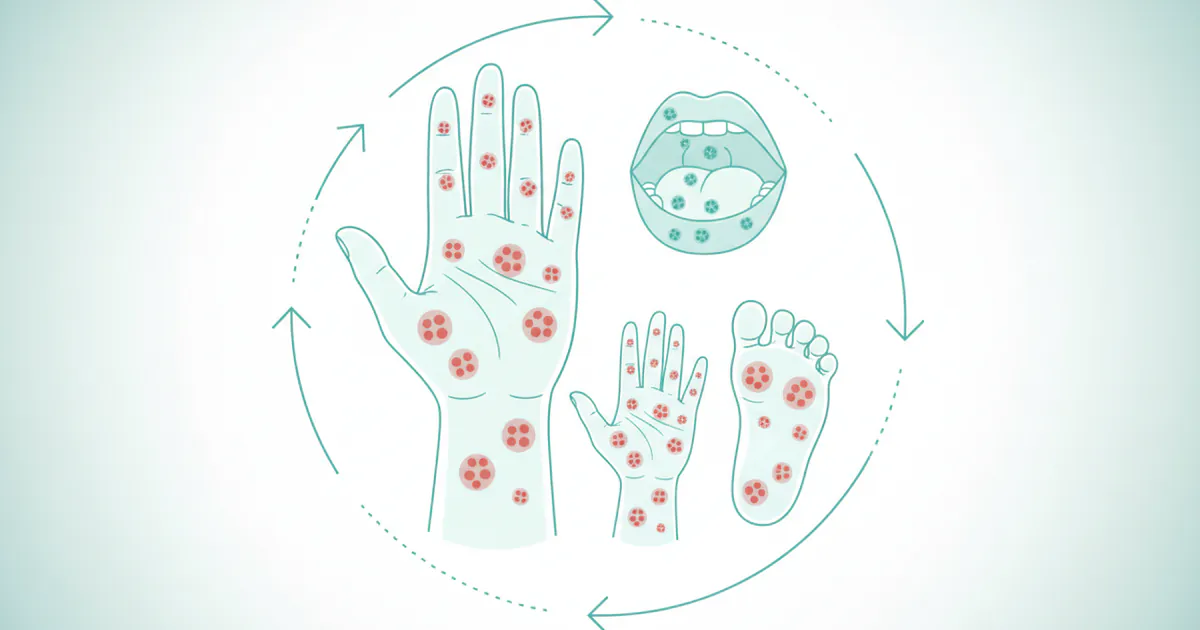
How Long Does Hand Foot and Mouth Last
Hand, Foot, and Mouth Disease (HFMD) is a common, often uncomfortable, viral illness that can affect anyone but is particularly prevalent among young children. If you or a loved one has ever experienced the tell-tale rash or painful mouth sores, you've likely wondered: **how long does Hand Foot and
February 23, 2026
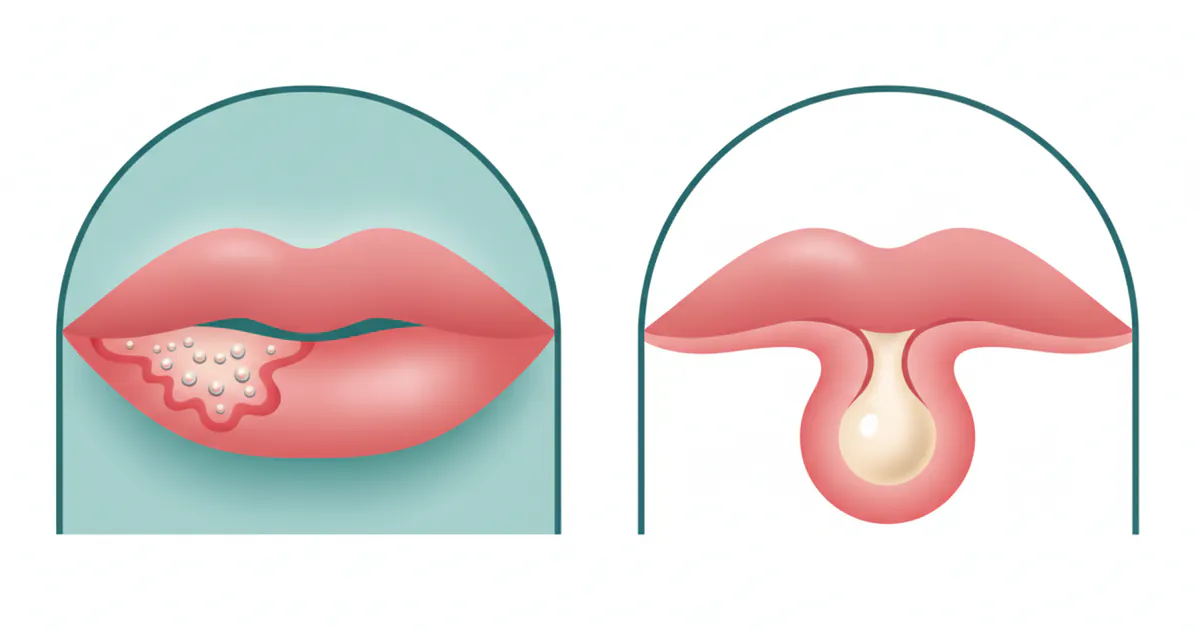
Cold Sore vs Pimple on Lip: Complete Comparison Guide
When you notice an unexpected bump or lesion on your lip, your mind might immediately jump to questions of what it is, how long it will last, and most importantly, if it's contagious. The confusion between a cold sore vs pimple on lip is incredibly common, yet the distinction is crucial for prop
February 23, 2026