Are Cold Sores Contagious
Key Takeaways
- In the United States, an estimated 67% of the population under age 50 carries the herpes simplex virus type 1 (HSV-1), the primary cause of cold sores. This means millions of Americans are susceptible to these often painful and highly visible oral lesions. Beyond the discomfort and cosmetic conc
In the United States, an estimated 67% of the population under age 50 carries the herpes simplex virus type 1 (HSV-1), the primary cause of cold sores. This means millions of Americans are susceptible to these often painful and highly visible oral lesions. Beyond the discomfort and cosmetic concerns, a critical question arises for anyone who experiences these recurrent blisters: are cold sores contagious? Understanding the contagious nature of cold sores is not just about personal hygiene; it's about protecting loved ones, preventing spread, and managing outbreaks effectively.
Cold sores, also known as fever blisters or oral herpes, are a common viral infection that manifests as small, fluid-filled lesions on or around the lips. While they typically resolve on their own within one to two weeks, their highly contagious nature means that vigilance and proper care are essential. This comprehensive guide from SmilePedia.net will delve deep into everything you need to know about cold sores, from their causes and symptoms to the full spectrum of treatment options, prevention strategies, and crucial insights into their contagiousness. We will explore how these lesions spread, when they are most infectious, and practical steps you can take to minimize the risk to yourself and others.
Key Takeaways:
- Cold sores are highly contagious from the moment you feel a tingling sensation until the sore has completely healed and the scab has fallen off.
- The primary cause of cold sores is the Herpes Simplex Virus Type 1 (HSV-1), which is permanent in the body once acquired, leading to recurrent outbreaks.
- Transmission occurs through direct contact with an infected area, such as kissing, sharing utensils, or towels, even when no visible sore is present (though less likely).
- Antiviral medications can shorten the duration of an outbreak by 1-2 days and reduce symptoms if taken at the first sign of a cold sore.
- Over-the-counter treatments typically cost $10-$30, while prescription antiviral medications can range from $30-$150 per course without insurance, though often covered.
- Preventative measures include avoiding triggers like sun exposure, stress, and certain foods, along with strict hygiene during outbreaks.
- Cold sores are not the same as angular cheilitis, which is a non-contagious inflammatory condition at the corners of the mouth with different causes and treatments.
What It Is / Overview: Understanding Cold Sores
Cold sores, medically known as herpes labialis or oral herpes, are a common viral infection caused almost exclusively by the Herpes Simplex Virus Type 1 (HSV-1). Less commonly, HSV-2 (typically associated with genital herpes) can also cause oral cold sores. Once an individual contracts HSV-1, the virus remains dormant within the nerve cells of the body for life. This means that while outbreaks may come and go, the virus itself is a permanent resident.
When the virus reactivates, it travels along the nerve pathways to the skin's surface, resulting in the characteristic lesions. These typically appear as small, fluid-filled blisters that form in clusters, most often on the lips or around the mouth, but can also occur on the nose, chin, or cheeks. These blisters eventually break open, ooze, and then crust over before healing. The entire process usually takes about 7 to 14 days.
It's crucial to understand that cold sores are not simply cosmetic annoyances; they are manifestations of a viral infection that can be spread to others. The discomfort can range from mild tingling to significant pain, itching, and burning sensations, impacting daily activities like eating, speaking, and smiling. Beyond the physical symptoms, cold sores can also carry a social stigma due to their visible nature and association with herpes, often causing emotional distress for sufferers.
The term "fever blister" is often used interchangeably with cold sore because outbreaks can sometimes be triggered by a fever or illness, though many other factors can also lead to reactivation. While some people experience only one primary infection and never have another outbreak, others may suffer from recurrent cold sores multiple times a year.
Types / Variations: Primary vs. Recurrent Infection
When discussing cold sores, it's important to distinguish between the initial, or primary, infection and subsequent recurrent outbreaks.
Primary Herpes Simplex Infection (Gingivostomatitis)
The first time an individual is infected with HSV-1, the symptoms can be much more severe than typical cold sore outbreaks, especially in children. This primary infection is often referred to as herpetic gingivostomatitis. While adults can experience this, it's more common in young children (ages 6 months to 5 years). Symptoms may include:
- Multiple painful blisters inside the mouth (on gums, tongue, cheeks, and throat), not just on the lips.
- Swollen, red, and bleeding gums.
- Fever, body aches, and general malaise.
- Difficulty eating and drinking due to pain, potentially leading to dehydration.
- Swollen lymph nodes.
This initial infection typically lasts 10 to 14 days and requires careful management of symptoms, including pain relief and ensuring adequate hydration. It's during this phase that the virus establishes latency in the nerve ganglia, setting the stage for potential future reactivations.
Recurrent Herpes Labialis (Cold Sores)
After the primary infection, the HSV-1 virus retreats to the trigeminal ganglion, a bundle of nerves near the ear, where it remains inactive, or "dormant." Recurrent outbreaks, or cold sores, occur when the dormant virus reactivates and travels back down the nerve pathway to the skin's surface, typically manifesting in the same area as previous outbreaks. These are the more commonly recognized cold sores on or around the lips.
The frequency and severity of recurrent outbreaks vary greatly among individuals. Some people may have only one or two outbreaks in their lifetime, while others may experience several per year. Over time, the body's immune response often strengthens, potentially leading to less frequent or less severe outbreaks.
Differentiating Cold Sores from Angular Cheilitis
It's critical to clarify a common confusion: cold sores are NOT angular cheilitis. While both conditions affect the mouth area, they are entirely different in their cause, contagiousness, and treatment.
- Cold Sores: Caused by the HSV-1 virus. They are highly contagious, appearing as blisters that ooze and crust, typically on the lips. They are viral.
- Angular Cheilitis: This is an inflammatory condition affecting one or both corners of the mouth, causing redness, cracking, and scaling. It is not contagious. Its causes are usually multifactorial, including:
While a cold sore can technically occur at the corner of the mouth, its appearance would be blister-like, consistent with herpes, rather than the cracked, scaling inflammation typical of angular cheilitis. Therefore, angular cheilitis treatment is completely different from cold sore treatment, focusing on antifungal/antibacterial creams, barrier ointments, and addressing underlying causes.
Causes / Why It Happens: The HSV-1 Reactivation
As established, cold sores are caused by the Herpes Simplex Virus Type 1 (HSV-1). The initial infection, often acquired in childhood through contact with an infected individual (e.g., a kiss from an adult with an active cold sore), is often asymptomatic or presents as gingivostomatitis. Once inside the body, the virus travels along nerve pathways and settles in nerve ganglia, where it remains dormant.
The key to understanding recurrent cold sores lies in the triggers that can reactivate this dormant virus. These triggers can vary widely from person to person but commonly include:
- Stress: Physical or emotional stress is a major trigger. The body's stress response can suppress the immune system, allowing the virus to reactivate.
- Sun Exposure/UV Light: Excessive exposure to sunlight or tanning beds can often trigger an outbreak. UV radiation weakens the skin's local immune defenses.
- Fever or Illness: Any illness that causes a fever (e.g., a common cold, flu, pneumonia) can stress the immune system, leading to an outbreak. This is why they are often called "fever blisters."
- Hormonal Changes: Fluctuations in hormones, particularly during menstruation, pregnancy, or menopause, can trigger outbreaks in some women.
- Fatigue: Lack of sleep or chronic tiredness can weaken the immune system.
- Injury to the Mouth/Lips: Trauma, dental work (like injections or extensive procedures), or even chapped lips can sometimes provoke an outbreak.
- Compromised Immune System: Individuals with weakened immune systems due to conditions like HIV/AIDS, organ transplantation, or chemotherapy are at higher risk of frequent and severe outbreaks.
- Certain Foods or Medications: While less common, some individuals report specific foods or medications can act as triggers.
Understanding your personal triggers is a powerful tool in prevention and managing outbreaks. Keeping a diary of when outbreaks occur and what might have preceded them can help you identify and avoid these factors.
Signs and Symptoms: What to Look For
Cold sores progress through several distinct stages, each with its own set of signs and symptoms. Recognizing these stages, especially the earliest ones, is crucial for timely intervention and potentially shortening the duration of the outbreak.
Stage 1: Tingling, Itching, or Burning (Prodromal Stage)
This is often the first and most crucial stage, occurring 12 to 24 hours before any visible blister appears. You might feel an itching, burning, tingling, or numbing sensation around the lips or wherever the sore is about to emerge. This "prodromal" stage is your body's warning sign and the best time to start antiviral treatment.
Stage 2: Blister Formation
Within a day or two of the prodromal symptoms, small, fluid-filled blisters begin to appear. These typically form in clusters on a red, swollen base, most commonly on the outer edge of the lips, though they can also appear on the nose, chin, or cheeks. These blisters are painful and tender to the touch.
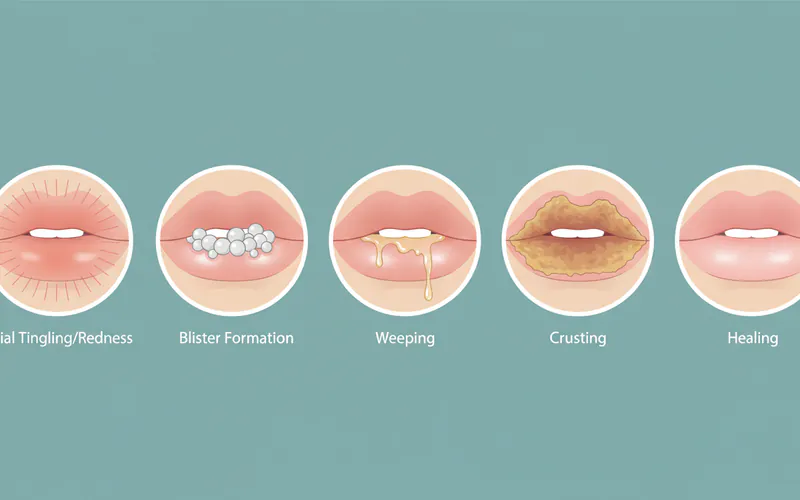
Stage 3: Weeping and Oozing (Open Sore Stage)
After a few days, the blisters rupture, leaving behind shallow, open sores. These sores are often moist and may ooze clear fluid, which is highly contagious and contains a high concentration of the active virus. This stage is usually the most painful and the most contagious period of the entire outbreak.
Stage 4: Crusting and Scabbing
As the sores begin to dry out, a yellowish or brownish crust (scab) forms over them. This scab protects the healing skin underneath. The area may still feel tight, itchy, or painful, and the scab might crack, causing some bleeding. It's important not to pick at the scab, as this can delay healing and increase the risk of secondary bacterial infection.
Stage 5: Healing
The scab eventually falls off, revealing new, healthy skin underneath. There may be some residual redness or slight discoloration, but this typically fades over time. The healing process is complete when the scab is gone, and the skin has fully regenerated.
Pro Tip: Pay close attention to the tingling, itching, or burning sensation. Starting treatment with a prescription antiviral medication during this prodromal stage can significantly reduce the severity and duration of the cold sore.
Are Cold Sores Contagious? A Definitive Answer
Yes, cold sores are unequivocally contagious, and understanding when and how they spread is paramount for preventing transmission. The contagiousness of a cold sore directly relates to the presence of the active virus.
When Are Cold Sores Most Contagious?
Cold sores are most contagious during the weeping and oozing stage (Stage 3), when the blisters have ruptured and are leaking fluid. This fluid is teeming with active HSV-1 particles. However, it's crucial to understand that the contagiousness actually begins even before the blisters appear:
- Prodromal Stage (Tingling/Itching): Even before a visible sore erupts, the virus is replicating and traveling to the skin's surface. While less contagious than the open sore stage, transmission is possible.
- Blister Stage: The fluid inside the blisters is highly infectious.
- Open Sore/Weeping Stage: This is the peak contagiousness period. Direct contact with the fluid makes transmission highly likely.
- Crusting/Scabbing Stage: As the sore dries and a scab forms, the amount of active virus decreases, but the sore can still be contagious until it has completely healed and the scab has fallen off.
- Healing Stage: Once the scab has fallen off and new skin is visible, the sore is generally no longer considered contagious.
Can Cold Sores Spread When No Sore Is Visible? (Asymptomatic Shedding)
Yes, this is an important and often overlooked aspect of HSV-1. The virus can shed from the oral area even when no visible cold sore or symptoms are present. This phenomenon is called asymptomatic shedding. While the risk of transmission during asymptomatic shedding is significantly lower than during an active outbreak, it is still possible. This explains why some people contract HSV-1 without ever recalling direct contact with a visible cold sore.
How Do Cold Sores Spread?
Transmission primarily occurs through direct skin-to-skin contact with an infected area. Common methods of transmission include:
- Kissing: The most common way oral herpes is spread.
- Sharing Eating Utensils: Cups, straws, forks, spoons, etc.
- Sharing Personal Items: Razors, towels, lip balms, toothbrushes.
- Direct Contact with Lesions: Touching a cold sore and then touching another person or another part of your own body.
Protecting Yourself and Others:
- Avoid Contact: Do not kiss anyone or engage in intimate contact when you have an active cold sore.
- Do Not Share: Refrain from sharing food, drinks, utensils, towels, or personal care items.
- Hand Hygiene: Wash your hands thoroughly with soap and water after touching your cold sore, especially before touching your eyes or other people.
- Avoid Touching: Try not to touch the cold sore unnecessarily. If you must, wash your hands immediately afterward.
It's important to remember that most people acquire HSV-1 in childhood or adolescence, often unknowingly. While the virus is permanent, managing outbreaks and understanding its contagious nature helps minimize spread and discomfort.
Treatment Options: Managing Outbreaks
While there is no cure for HSV-1, various treatments can help manage cold sore outbreaks, reduce pain, shorten healing time, and decrease the frequency of recurrence.
1. Antiviral Medications (Prescription)
These are the most effective treatments, especially when started at the very first sign of an outbreak (the tingling stage). They work by inhibiting the virus's ability to replicate.
-
Oral Antivirals:
- Acyclovir (Zovirax®): Typically taken 2-5 times a day for 5-10 days.
- Valacyclovir (Valtrex®): A prodrug of acyclovir, often taken once or twice a day for 1-5 days, making it more convenient.
- Famciclovir (Famvir®): Usually taken in a single dose or twice daily for 1 day.
- Pros: Can significantly shorten healing time (by 1-2 days), reduce severity, and help prevent an outbreak if taken early. For frequent outbreaks, daily suppressive therapy can reduce recurrence by 70-80%.
- Cons: Require a prescription, can have side effects (nausea, headache), and are most effective when started at the very first symptom.
-
Topical Antivirals:
- Penciclovir (Denavir®): A cream applied every 2 hours while awake for 4 days.
- Acyclovir (Zovirax® Cream): Applied 5 times a day for 4 days.
- Pros: Can shorten healing time and reduce pain, directly target the lesion.
- Cons: Often less effective than oral antivirals, require frequent application, and may not prevent an outbreak if applied too late.
2. Over-the-Counter (OTC) Topical Treatments
These medications typically focus on relieving symptoms and accelerating healing, but do not target the virus itself.
- Docosanol (Abreva®): The only FDA-approved non-prescription cream that has antiviral properties. It helps block the virus from entering healthy cells and shortens healing time. Applied 5 times a day until the sore is healed (up to 10 days).
- Pros: Readily available, can reduce healing time.
- Cons: Must be applied early and frequently, less potent than prescription antivirals.
- Pain Relief/Numbing Creams: Benzocaine or lidocaine-containing gels and creams can temporarily numb the area, providing relief from pain and itching.
- Drying Agents: Products containing alcohol or acetone can help dry out the blisters.
- Skin Protectants: Ointments like petroleum jelly or zinc oxide can keep the sore moist, prevent cracking, and protect it from secondary infection, aiding healing.
- Pros: Symptom relief, easily accessible.
- Cons: Do not treat the viral cause, mainly palliative.
3. Home Remedies and Supportive Care
While not substitutes for medical treatment, these can complement therapy and provide comfort.
- Cold Compress: Applying a cold, damp cloth or ice pack can reduce pain, swelling, and redness.
- Aloe Vera Gel: Known for its soothing properties, can be applied to the sore.
- Lysine Supplements: Some individuals report that daily lysine supplementation (an amino acid) can help prevent outbreaks or reduce their severity. Research on this is mixed, but anecdotal evidence is strong for some.
- Avoiding Irritants: Steer clear of acidic foods, salty snacks, and spicy dishes that can irritate the sore.
- Hydration: Drink plenty of fluids, especially if eating is painful.
- Stress Management: Techniques like meditation, yoga, or deep breathing can help reduce stress, a common trigger.
Pro Tip: Always consult your dentist or physician to determine the most appropriate treatment plan for your specific needs, especially if you experience frequent, severe, or unusually painful cold sore outbreaks. They can assess if prescription antivirals are right for you.
Step-by-Step Process: What to Expect During an Outbreak
Understanding the typical progression of a cold sore can help you manage it more effectively.
- Prodromal Stage (Day 1): You'll feel a tingling, itching, burning, or throbbing sensation in the area where the cold sore will appear. This is the ideal time to start antiviral medication (oral or topical).
- Blister Stage (Day 2-3): Small, red bumps develop, quickly turning into fluid-filled blisters. These clusters of blisters are typically painful and appear swollen.
- Action: Continue antiviral treatment. Keep the area clean and avoid touching. Apply OTC numbing creams for pain relief if needed.
- Weeping/Oozing Stage (Day 4-5): The blisters burst open, releasing clear fluid. This stage is the most painful and most contagious.
- Action: Gently clean the area. Continue medication. Strictly avoid contact with others and practice rigorous hand hygiene. You can apply petroleum jelly to keep the area moist and prevent cracking, but avoid heavy creams that might trap bacteria.
- Crusting/Scabbing Stage (Day 6-9): The sores dry out and form a yellowish-brown crust or scab. This scab may crack, leading to slight bleeding.
- Action: Continue keeping the area clean. Avoid picking or scratching the scab, as this can delay healing and introduce bacteria. Maintain hydration and general wellness.
- Healing Stage (Day 10-14): The scab shrinks, peels off, and new skin forms underneath. The cold sore is generally no longer contagious once the scab is gone.
- Action: Continue protecting the new skin, especially from sun exposure. Maintain good oral hygiene.
The entire process, from first tingle to complete healing, usually takes about 10-14 days without treatment. With effective antiviral treatment started early, this can be shortened to 7-10 days.
Cost and Insurance: US Price Ranges
The cost of cold sore treatment can vary significantly depending on whether you opt for over-the-counter remedies or prescription medications, as well as your insurance coverage.
Over-the-Counter (OTC) Treatments
These are generally the most affordable options.
- Docosanol (Abreva®) Cream: Approximately $15-$30 for a 2-gram tube.
- Pain-relieving/Numbing Gels (e.g., Benzocaine): Around $5-$15 per tube.
- Lip Balms/Protectants (e.g., Vaseline, zinc oxide): Typically $3-$10.
- L-Lysine Supplements: A bottle of capsules can range from $10-$25.
Prescription Antiviral Medications
These costs can vary widely based on the specific drug, dosage, duration of treatment, and whether generic versions are available.
- Acyclovir (Generic Zovirax®):
- Oral tablets: A typical 5-day course (e.g., 200mg, 5x/day) can range from $30-$70 for generic, or $100-$200+ for brand name.
- Topical cream: A 5g tube can be $50-$150 for generic, much higher for brand.
- Valacyclovir (Generic Valtrex®):
- Oral tablets: A single-day treatment for an outbreak (e.g., 2g once) can be $40-$80 for generic. A multi-day course or daily suppressive therapy will be proportionally higher, potentially $80-$150+ per month for daily use.
- Brand name Valtrex can be $300-$500+ for a single course.
- Famciclovir (Generic Famvir®): A single-dose treatment can be $50-$100 for generic.
Insurance Coverage
Most medical insurance plans (including employer-sponsored plans, Medicare, and Medicaid) typically cover prescription antiviral medications for cold sores, especially when a generic option is available.
- Co-pays: If you have insurance, you will likely pay a co-pay ranging from $10-$50 for a prescription, depending on your plan and whether it's a generic or brand-name drug.
- Deductibles: If you haven't met your annual deductible, you might pay the full cash price until your deductible is met.
- HSA/FSA: Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs) can be used to pay for both OTC and prescription cold sore treatments.
Pro Tip: Always check with your insurance provider about your specific coverage details for prescription medications. Utilizing discount cards (like GoodRx) can also significantly reduce the cost of generics if you don't have insurance or have a high deductible.
Comparison of Cold Sore Treatment Options
| Treatment Type | Examples | Average US Cost (Without Insurance) | Duration of Treatment | Effectiveness | Key Benefits |
|---|---|---|---|---|---|
| Oral Antivirals | Valacyclovir, Acyclovir, Famciclovir | $30-$150 (generic) / $300+ (brand) | 1-10 days | High (reduces duration by 1-2 days, can prevent if taken early) | Shortens healing, reduces severity, can prevent outbreaks, suppressive option. |
| Topical Antivirals | Penciclovir (Denavir), Acyclovir Cream | $50-$150 (generic) / $200+ (brand) | 4-10 days | Moderate (reduces duration slightly, localized effect) | Localized treatment, reduces pain and healing time. |
| OTC Antiviral Cream | Docosanol (Abreva) | $15-$30 | 7-10 days | Moderate (reduces duration by ~0.5-1 day) | No prescription needed, readily available, helps block viral entry. |
| OTC Symptom Relief | Benzocaine creams, Petroleum jelly, Zinc oxide | $5-$15 | As needed | Low (does not treat virus, only symptoms) | Pain relief, prevents cracking, protects skin. |
| L-Lysine Supplements | Oral capsules | $10-$25 | Daily/As needed | Variable (anecdotal evidence for prevention/reduction, research is mixed) | Natural option, potential for prevention. |
Recovery and Aftercare: Post-Treatment Care
Even after a cold sore begins to heal, proper aftercare is essential to ensure smooth recovery, prevent secondary infections, and minimize the risk of scarring.
- Continue Hygiene: Maintain excellent hand hygiene. Even if the cold sore is scabbing, avoid touching it unnecessarily and wash your hands after any contact.
- Avoid Picking the Scab: It's tempting to pick at a healing scab, but this can rip off the new, delicate skin underneath, delay healing, potentially cause bleeding, and increase the risk of scarring or introducing bacteria.
- Moisturize: Once the scab has fallen off, the new skin may be dry and sensitive. Apply a gentle, fragrance-free moisturizer or lip balm to keep the area hydrated.
- Sun Protection: The new skin is particularly vulnerable to sun damage, which can also trigger future outbreaks. Use a lip balm with SPF 30 or higher, even on cloudy days, and wear a wide-brimmed hat when outdoors. The American Dental Association (ADA) emphasizes the importance of sun protection for oral health, including preventing cold sore triggers.
- Monitor for Secondary Infection: Watch for signs of a secondary bacterial infection, such as increased redness, swelling, pus, or persistent pain after the cold sore should be healing. If these occur, consult a healthcare professional.
- Discard Contaminated Items: Once an outbreak is completely healed, consider replacing your toothbrush, lip balm, and any other items that came into direct contact with the sore to prevent re-infection or spreading the virus.
- Manage Triggers: Reflect on potential triggers that may have caused the outbreak (stress, sun, illness) and take steps to mitigate them for future prevention.
Prevention: How to Avoid Cold Sore Outbreaks and Transmission
Preventing cold sores involves a two-pronged approach: avoiding initial infection (if you don't have HSV-1) and preventing recurrent outbreaks and transmission (if you do).
Preventing Initial Infection (If You Are HSV-1 Negative)
- Avoid Direct Contact: Do not kiss someone who has an active cold sore.
- Do Not Share Items: Avoid sharing eating utensils, drinks, straws, lip balms, razors, or towels with anyone, especially those with visible cold sores.
Preventing Recurrent Outbreaks (If You Are HSV-1 Positive)
- Identify and Avoid Triggers: This is perhaps the most effective strategy. Keep a diary to pinpoint what causes your outbreaks and try to avoid those triggers.
- Sun Protection: Use lip balms with SPF 30 or higher before sun exposure. Wear hats.
- Stress Management: Practice relaxation techniques like meditation, yoga, or deep breathing. Ensure adequate sleep.
- Immune Support: Maintain a healthy lifestyle with a balanced diet, regular exercise, and sufficient sleep to support your immune system.
- Manage Illnesses: Treat fevers and colds promptly to reduce immune system stress.
- Daily Antiviral Therapy: For individuals who experience very frequent or severe outbreaks (e.g., more than 6 times a year), a healthcare provider may prescribe daily oral antiviral medication (e.g., valacyclovir) to suppress the virus and significantly reduce the frequency of outbreaks. This can reduce recurrence rates by 70-80%.
- Dental Care: Be mindful during dental procedures. While most procedures don't trigger cold sores, extensive work or local anesthetic injections can sometimes be a trigger. If you're prone to cold sores and anticipate extensive dental work, discuss it with your dentist; sometimes, a prophylactic dose of antiviral medication can be prescribed.
Preventing Transmission During an Outbreak (If You Have an Active Cold Sore)
- Avoid Kissing: Refrain from kissing anyone, especially infants, young children, and immunocompromised individuals.
- Do Not Share Personal Items: Absolutely do not share eating utensils, cups, towels, razors, toothbrushes, or lip products.
- Hand Hygiene: Wash your hands thoroughly and frequently with soap and water, especially after touching your cold sore.
- Avoid Touching Your Eyes: HSV-1 can cause a serious eye infection called ocular herpes (herpes keratitis) if transferred from your cold sore to your eye.
- Avoid Other Body Parts: Be cautious not to transfer the virus to other parts of your own body or to others. This includes avoiding oral sex during an outbreak.
Risks and Complications: What Can Go Wrong
While cold sores are typically a benign condition that resolves on its own, certain risks and complications can arise, especially in vulnerable populations or if the virus spreads to other areas.
- Ocular Herpes (Herpes Keratitis): This is one of the most serious complications. If HSV-1 is transferred from a cold sore to the eye (e.g., by touching the sore and then rubbing the eye), it can cause an infection of the cornea. Symptoms include eye pain, redness, blurred vision, and sensitivity to light. If left untreated, ocular herpes can lead to corneal scarring, vision loss, or even blindness. Seek immediate medical attention if you suspect eye involvement.
- Herpetic Whitlow: This occurs when HSV-1 infects a finger, causing painful blisters. It's common in children who suck their thumb or fingers during an outbreak, or in healthcare workers who come into contact with cold sores without proper protection.
- Eczema Herpeticum: Individuals with eczema or other skin conditions that compromise the skin barrier are at risk of a widespread, severe HSV infection called eczema herpeticum. This involves numerous blisters covering large areas of the skin, often accompanied by fever and malaise, and requires urgent medical treatment.
- Spread to Other Body Parts: While less common, HSV-1 can spread to other areas of the body, causing lesions.
- Immunocompromised Individuals: People with weakened immune systems (e.g., HIV/AIDS, cancer patients, organ transplant recipients) are at higher risk of severe, prolonged, or atypical cold sore outbreaks. They may experience lesions that spread to internal organs, are more painful, and take longer to heal. These individuals often require more aggressive antiviral therapy.
- Psychological Impact: Beyond the physical discomfort, the visible nature of cold sores can cause significant emotional distress, self-consciousness, and social anxiety.
Children / Pediatric Considerations
Cold sores are incredibly common in children. Many children acquire HSV-1 in their early years, often through a casual kiss from an adult or contact with an infected object.
- Primary Infection (Gingivostomatitis): As mentioned, the first exposure to HSV-1 in children often manifests as herpetic gingivostomatitis, which can be quite severe.
- Symptoms: High fever, multiple painful sores inside the mouth (gums, tongue, cheeks), swollen and bleeding gums, difficulty eating and drinking, swollen lymph nodes.
- Parental Guidance: Ensure adequate hydration (offer small, frequent sips of water, diluted juice, or popsicles). Pain relief (acetaminophen or ibuprofen, as directed by a pediatrician) is crucial. Avoid acidic foods. If a child cannot drink due to pain or shows signs of dehydration, seek immediate medical attention. A pediatrician may prescribe oral antivirals for severe cases.
- Recurrent Cold Sores in Children: Subsequent cold sores usually resemble those in adults, appearing as blisters on the lips.
- Contagion: Children can be less diligent with hygiene, making transmission to playmates, siblings, or other family members more likely. Teach children about hand washing and avoiding sharing items.
- Prevention: Help children identify their triggers (e.g., sun, stress from school). Use child-safe lip balms with SPF.
- Treatment: Topical OTC creams (like Abreva) can be used for older children, following product instructions. Oral antivirals are generally reserved for more severe or frequent cases and must be prescribed by a pediatrician.
- Dental Visits: Inform your child's pediatric dentist if your child has an active cold sore. The dentist may reschedule routine appointments to avoid irritating the sore, causing discomfort, or spreading the virus in the dental office.
Frequently Asked Questions
Is a cold sore always herpes?
Yes, by definition, a cold sore is always caused by the Herpes Simplex Virus, predominantly HSV-1. The terms "cold sore" and "oral herpes" are synonymous. If it's a blister on or around the lips caused by the virus, it's herpes. Other conditions might cause lip lesions, but they are not true "cold sores."
Can I get a cold sore if I don't kiss someone?
Yes, while kissing is a common transmission method, the virus can also spread through sharing objects like eating utensils, cups, straws, lip balms, or towels. It can also spread via asymptomatic shedding, where the virus is present on the skin without a visible sore.
How long does a cold sore typically last?
Without treatment, a cold sore typically lasts 10 to 14 days, progressing through the stages of tingling, blistering, weeping, crusting, and healing. With early intervention using antiviral medications, the duration can often be shortened to 7 to 10 days.
What is the fastest way to get rid of a cold sore?
The fastest way to treat a cold sore is to start a prescription oral antiviral medication (like valacyclovir or acyclovir) at the very first sign of tingling or itching. These medications can significantly reduce the duration and severity of the outbreak if taken early enough. Over-the-counter antiviral creams like docosanol (Abreva) can also help speed up healing.
Does insurance cover cold sore treatment?
Most medical insurance plans in the US typically cover prescription antiviral medications for cold sores, especially generic versions. You will likely be responsible for a co-pay, and costs may apply towards your deductible. Over-the-counter treatments are usually not covered but can often be purchased with FSA/HSA funds.
Is a cold sore an emergency?
Typically, no. Most cold sores resolve on their own and can be managed at home or with a visit to a primary care provider. However, if the cold sore spreads to your eye, causes widespread skin rashes (especially with eczema), occurs in an infant, or in someone with a severely compromised immune system, it is an emergency and requires immediate medical attention.
Can stress cause cold sores?
Yes, stress is a very common trigger for cold sore outbreaks. Both physical and emotional stress can suppress the immune system, allowing the dormant HSV-1 virus to reactivate and cause a cold sore. Managing stress through relaxation techniques can be a preventative measure.
What is the difference between a cold sore and a canker sore?
Cold sores are caused by the highly contagious HSV-1 virus, appear as blisters on the outside of the mouth (lips, nose, chin), and are contagious. Canker sores (aphthous ulcers) are non-contagious, usually appear as painful open sores inside the mouth (on cheeks, tongue, gums), and are thought to be caused by factors like stress, injury, nutritional deficiencies, or certain foods, not a virus.
Why do some people get cold sores and others don't?
Everyone who gets cold sores has been infected with HSV-1. Many people carry the virus but never experience an outbreak, or only rarely. Those who get recurrent cold sores tend to have a virus that reactivates more easily due to specific triggers or individual immune responses. Some people are never exposed to the virus at all.
Can dental work trigger a cold sore?
Yes, dental procedures, especially those involving injections around the mouth or trauma to the lips/gums, can sometimes act as a trigger for a cold sore outbreak in individuals who carry the HSV-1 virus. If you are prone to cold sores, inform your dentist, who may recommend a prophylactic dose of antiviral medication before extensive procedures.
When to See a Dentist or Doctor
While most cold sores resolve on their own, there are specific situations where seeking professional medical advice is crucial:
- Prolonged or Severe Outbreaks: If a cold sore is unusually large, extremely painful, doesn't start healing within two weeks, or keeps recurring very frequently (e.g., more than 6 times a year).
- Spread to Other Body Parts: If you suspect the infection has spread beyond your lips, particularly to your eyes (redness, pain, discharge in the eye – seek immediate medical attention for ocular herpes), or to your fingers (herpetic whitlow).
- Compromised Immune System: If you have a weakened immune system due to conditions like HIV/AIDS, cancer treatment (chemotherapy/radiation), or organ transplant, cold sores can be more severe and lead to serious complications.
- Signs of Secondary Bacterial Infection: Increased redness, swelling, pus, or fever accompanying the cold sore can indicate a secondary bacterial infection requiring antibiotics.
- In infants or young children: If an infant (especially under 6 months) develops cold sores or severe gingivostomatitis, or if a child cannot eat or drink due to pain, contact a pediatrician immediately to prevent dehydration and manage symptoms.
- Undiagnosed Lesions: If you have a lesion on or around your lips that you're unsure about, especially if it doesn't fit the typical cold sore pattern or doesn't heal, it's always best to have it examined by a dentist or doctor to rule out other conditions.
For routine cold sore management, your family physician can often prescribe antiviral medications. However, your dentist is also a valuable resource for oral health and can provide guidance, especially regarding the impact of cold sores on dental procedures or if you need help differentiating them from other oral lesions. The American Dental Association (ADA) recommends consulting a dentist for any concerning oral lesions.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

Oral Candidiasis Symptoms: Complete Guide
Oral candidiasis, commonly known as oral thrush, is a fungal infection of the mouth caused by an overgrowth of Candida yeast, most often Candida albicans. While Candida is a normal inhabitant of the human mouth in small amounts, an imbalance can lead to uncomfortable and sometimes painful symptoms
February 23, 2026
How Long Does Hand Foot and Mouth Last
Hand, Foot, and Mouth Disease (HFMD) is a common, often uncomfortable, viral illness that can affect anyone but is particularly prevalent among young children. If you or a loved one has ever experienced the tell-tale rash or painful mouth sores, you've likely wondered: **how long does Hand Foot and
February 23, 2026
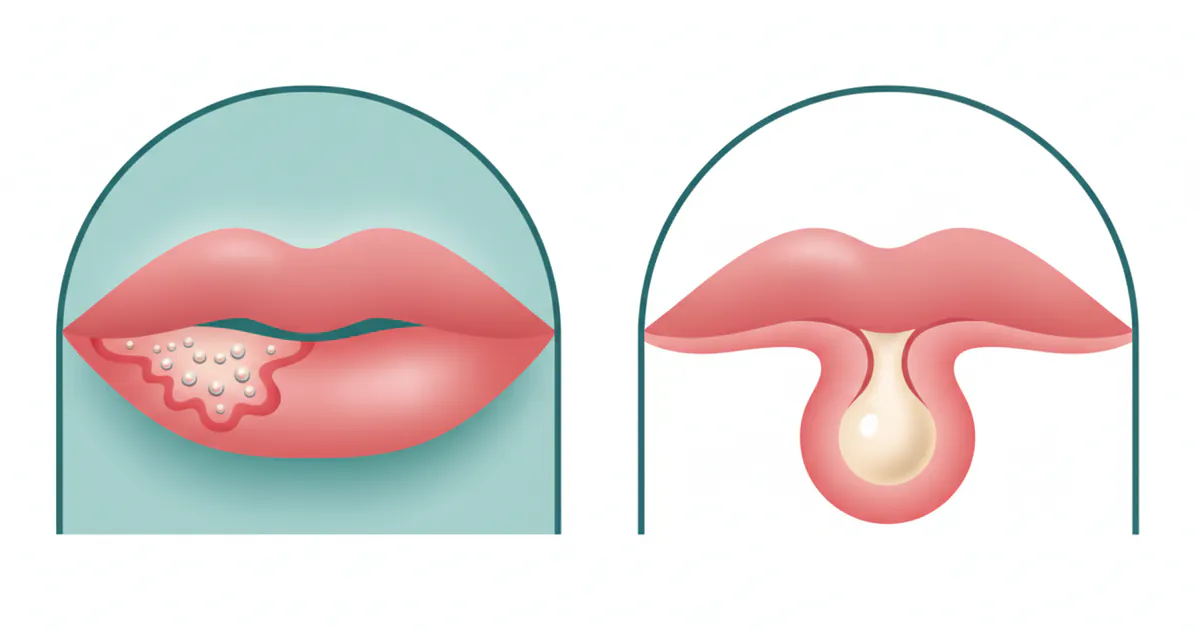
Cold Sore vs Pimple on Lip: Complete Comparison Guide
When you notice an unexpected bump or lesion on your lip, your mind might immediately jump to questions of what it is, how long it will last, and most importantly, if it's contagious. The confusion between a cold sore vs pimple on lip is incredibly common, yet the distinction is crucial for prop
February 23, 2026
Hand Foot and Mouth Symptoms: Complete Guide
Imagine your child wakes up with a fever, feels a little off, and then you spot painful sores appearing in their mouth, followed by a tell-tale rash on their hands and feet. This scenario, unfortunately common, is often the first encounter with Hand Foot and Mouth Disease (HFMD). Affecting millions
February 23, 2026