Cold Sore vs Pimple on Lip: Complete Comparison Guide
Key Takeaways
- When you notice an unexpected bump or lesion on your lip, your mind might immediately jump to questions of what it is, how long it will last, and most importantly, if it's contagious. The confusion between a cold sore vs pimple on lip is incredibly common, yet the distinction is crucial for prop
When you notice an unexpected bump or lesion on your lip, your mind might immediately jump to questions of what it is, how long it will last, and most importantly, if it's contagious. The confusion between a cold sore vs pimple on lip is incredibly common, yet the distinction is crucial for proper treatment and prevention. Did you know that an estimated 67% of the world population under 50 is infected with herpes simplex virus type 1 (HSV-1), the virus responsible for cold sores? This statistic underscores just how prevalent these lesions are, making accurate identification vital for your health and the health of those around you.
Understanding the differences between these two seemingly similar conditions can prevent unnecessary anxiety, guide effective self-care, and indicate when professional medical or dental attention is needed. While a pimple is typically a benign skin condition, a cold sore is a viral infection that requires specific management to reduce its duration, discomfort, and risk of transmission. This comprehensive guide from SmilePedia.net will delve into the causes, symptoms, treatment options, and preventative measures for both cold sores and pimples on the lip. We will equip you with the knowledge to confidently identify your lip lesion, understand its implications, and explore various solutions, including cost considerations and when to consult a healthcare professional.
Key Takeaways:
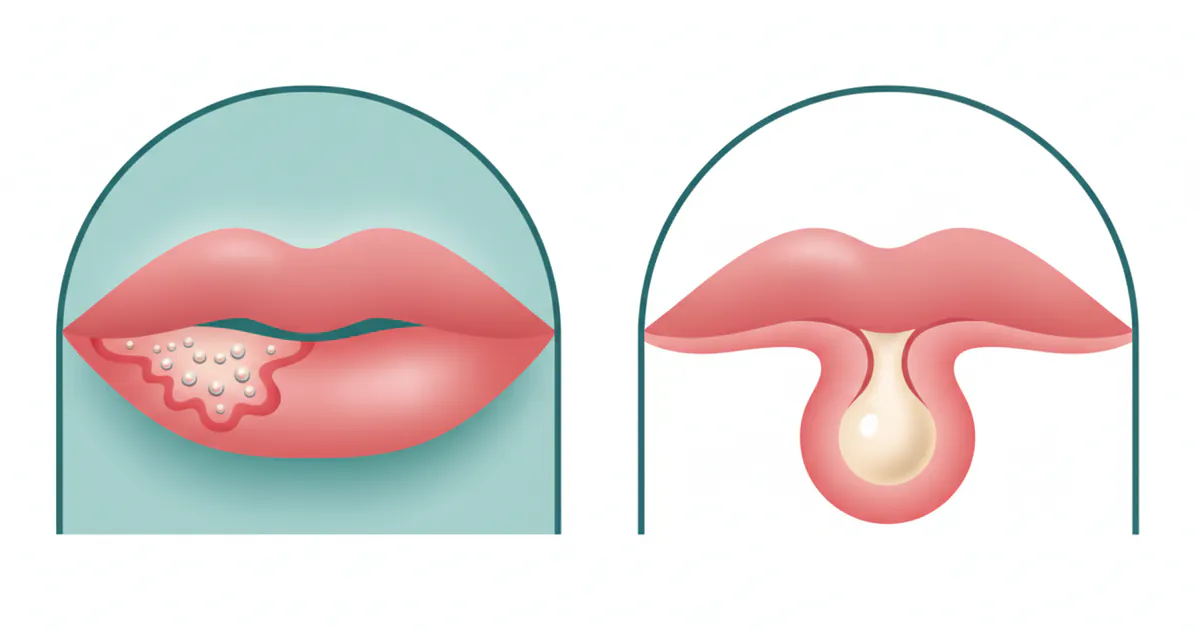
- Cold sores are caused by the highly contagious Herpes Simplex Virus type 1 (HSV-1), appearing as clusters of fluid-filled blisters, often preceded by tingling.
- Pimples on the lip are non-contagious bacterial infections of hair follicles or sebaceous glands, typically appearing as a single red bump with a whitehead.
- Duration: Cold sores usually last 7-14 days with a full healing cycle; pimples typically resolve within 3-7 days.
- Treatment Costs: Over-the-counter (OTC) cold sore treatments range from $10-$30, while prescription antivirals can cost $50-$200+ per course. Pimple treatments (OTC) are generally $5-$40.
- Prevention: Stress reduction, sun protection, and antiviral prophylaxis can prevent cold sores. Good hygiene and non-comedogenic products prevent pimples.
- Contagion: Cold sores are highly contagious from the tingling stage until completely crusted over; pimples are not contagious.
- When to See a Dentist/Doctor: Seek professional help if a lesion is persistent, unusually painful, spreading, accompanied by fever, or if you suspect it might be
herpes inside mouthor a more serious condition.
Cold Sore vs Pimple on Lip: The Fundamental Differences
Distinguishing between a cold sore and a pimple on your lip is the first step toward effective management. While both can cause discomfort and appear as red bumps, their underlying causes, appearances, and prognoses are fundamentally different.

What is a Cold Sore?
A cold sore, also known as a fever blister, is a common viral infection caused primarily by the Herpes Simplex Virus type 1 (HSV-1). Once you contract HSV-1, the virus remains dormant in your nerve cells for life, often reactivating periodically to cause new outbreaks. These outbreaks typically manifest as small, fluid-filled blisters that form in clusters, most commonly on or around the lips, but can also occur inside the mouth, on the gums, or on the roof of the mouth. This is why sometimes individuals may experience herpes inside mouth, which can be particularly uncomfortable. Cold sores are highly contagious and are easily spread through direct contact, such as kissing or sharing utensils, particularly during the active blister phase.
Key characteristics of cold sores:
- Viral Origin: Caused by HSV-1.
- Appearance: Start as small, red, fluid-filled blisters that often cluster together. These blisters eventually rupture, forming a crust or scab.
- Location: Predominantly on the lip line, but can extend to the skin around the mouth or sometimes inside the mouth.
- Contagiousness: Highly contagious from the tingling stage until fully healed.
- Recurrence: Tend to recur in the same area due to viral reactivation.
What is a Pimple on the Lip?
A pimple, or acne lesion, on the lip is a common skin condition that occurs when hair follicles or sebaceous (oil) glands become clogged with oil (sebum), dead skin cells, and bacteria. Unlike cold sores, pimples are not caused by a virus and are not contagious. They can appear anywhere on the skin, including around the lips, where hair follicles are present. Pimples on the lip are typically isolated occurrences, though they can sometimes appear in groups if there's widespread inflammation or an acne breakout.
Key characteristics of pimples on the lip:
- Bacterial/Follicular Origin: Caused by clogged pores and bacterial overgrowth (often Propionibacterium acnes).
- Appearance: Typically a single, red, tender bump that may or may not have a whitehead (pus-filled center). It's usually a solid bump, not a cluster of fluid-filled blisters.
- Location: Can occur on the lip line, around the mouth where hair follicles are present, or sometimes directly on the vermillion border (the red part of the lip).
- Contagiousness: Not contagious.
- Recurrence: Can recur due to skin type, hygiene, or hormonal factors, but not in the same "dormant virus" way as cold sores.
Key Distinguishing Features
The most reliable way to differentiate between a cold sore and a pimple is by carefully observing their appearance, accompanying sensations, and progression.
-
Appearance:
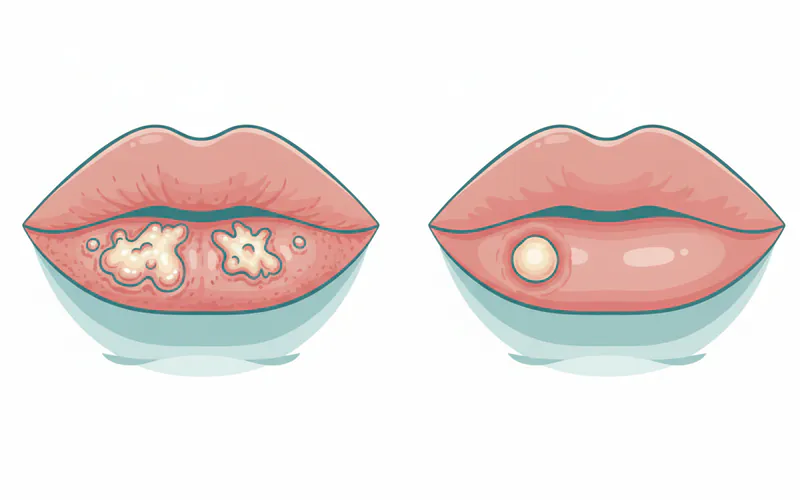
- Cold Sore: Typically begins as a patch of small, clustered, clear or yellowish fluid-filled blisters on a red base. These blisters are often grouped like a bunch of grapes. As they progress, they burst and weep, then crust over with a yellowish or brownish scab.
- Pimple: Usually appears as a single, red, solid bump. It may develop a white center (pus) or a blackhead. It doesn't typically form fluid-filled blisters that burst and weep.
-
Sensation:
- Cold Sore: Often preceded by a distinct tingling, itching, burning, or throbbing sensation in the area where the lesion will appear, sometimes a day or two before any visible signs. This is known as the prodromal stage.
- Pimple: Usually feels tender or painful to the touch from the outset, without the preceding tingling or itching.
-
Progression:
- Cold Sore: Follows a predictable cycle: tingling -> redness/swelling -> blister formation -> weeping -> crusting -> healing. This entire process can take 7-14 days.
- Pimple: Develops as a red bump, potentially forms a whitehead, and then gradually subsides. The healing process is typically quicker, lasting 3-7 days.
-
Contagion:
- Cold Sore: Highly contagious, especially when blisters are present and weeping. The virus can spread through direct contact (kissing, sharing utensils, towels).
- Pimple: Not contagious.
-
Recurrence Pattern:
- Cold Sore: Tends to reappear in roughly the same spot due to the dormant HSV-1 virus reactivating. Triggers include stress, sunlight, fever, hormonal changes, and injury.
- Pimple: Can recur anywhere on the face due to clogged pores, but doesn't have a specific "dormant virus" recurrence pattern.
Causes and Risk Factors
Understanding the root causes of cold sores and pimples helps in both prevention and treatment.
Causes of Cold Sores
Cold sores are caused by the Herpes Simplex Virus type 1 (HSV-1). Initial infection usually occurs in childhood, often without noticeable symptoms (asymptomatic) or presenting as a severe gingivostomatitis (inflammation of gums and mouth lining). Once infected, the virus travels along nerve pathways and lies dormant in nerve cells. Various triggers can reactivate the dormant virus, leading to an outbreak:
- Stress: Emotional or physical stress weakens the immune system, allowing the virus to reactivate.
- Sunlight Exposure: UV radiation can trigger outbreaks.
- Fever or Illness: Any condition that compromises the immune system, such as a cold, flu, or fever, can trigger a cold sore.
- Hormonal Changes: Menstrual periods, pregnancy, or hormone fluctuations can induce outbreaks.
- Physical Trauma: Injury to the lip or dental procedures can sometimes trigger an outbreak in the affected area.
- Weakened Immune System: Conditions like HIV/AIDS, chemotherapy, or organ transplant medications can lead to more frequent or severe outbreaks.
Causes of Pimples on the Lip
Pimples on the lip are primarily caused by the same factors that lead to acne elsewhere on the face:
- Excess Sebum Production: Overactive sebaceous glands produce too much oil, which can clog pores.
- Dead Skin Cells: When dead skin cells don't shed properly, they mix with sebum and clog follicles.
- Bacteria: Propionibacterium acnes (P. acnes), a common skin bacterium, thrives in clogged follicles and causes inflammation.
- Hormonal Fluctuations: Androgens (male hormones present in both sexes) can increase sebum production, explaining why acne is common during puberty, menstruation, and pregnancy.
- Cosmetics and Lip Products: Certain oil-based or comedogenic (pore-clogging) lip balms, lipsticks, or moisturizers can block pores around the lips.
- Diet: While direct links are debated, some studies suggest high glycemic index foods or dairy products may contribute to acne in some individuals.
- Poor Hygiene: Not regularly cleansing the face can lead to a buildup of oil and dead skin cells.
- Touching or Picking: Frequently touching your lips or face can transfer bacteria and oil, irritating the skin and leading to breakouts.
Signs and Symptoms: What to Look For
Recognizing the specific signs and symptoms is key to proper identification and timely intervention.
Cold Sore Symptoms
A cold sore outbreak typically progresses through several stages:
- Prodromal Stage (Day 1): Often characterized by a tingling, itching, burning, or throbbing sensation around the lips, usually 12-24 hours before any visible lesion appears. Some people experience a localized soreness or numbness. This is the most contagious stage, even without visible blisters.
- Blister Stage (Day 2-3): Small, red, fluid-filled blisters (vesicles) develop, often in a cluster along the lip line. These blisters are painful and tender to the touch. In severe primary infections, widespread
herpes inside mouthcan occur, leading to painful sores on the gums, tongue, or inner cheeks. - Weeping/Ulceration Stage (Day 4): The blisters burst open, releasing clear fluid and leaving behind shallow, open sores. This stage is highly contagious due to the exposed virus. The sores may look raw and red.
- Crusting Stage (Day 5-8): The open sores begin to dry out and form a yellowish or brownish crust/scab. This scab may crack, bleed, and cause discomfort.
- Healing Stage (Day 9-14): The scab gradually shrinks and flakes off, revealing new skin underneath. The area may remain red for a few days, but typically heals without scarring.
Other symptoms, especially during a primary infection (the first time someone gets HSV-1), can include fever, swollen lymph nodes in the neck, muscle aches, and sore throat. Recurrent outbreaks are usually milder and localized.
Pimple Symptoms
Pimples on the lip present differently:
- Red Bump: Starts as a single, red, inflamed bump that is often tender or painful to the touch.
- Pus-filled Center: As it develops, a whitehead (a pus-filled center) may become visible.
- Swelling: The area around the pimple may be slightly swollen.
- Lack of Prodromal Symptoms: No preceding tingling, itching, or burning sensation.
- No Clustering: Usually appears as a solitary lesion, not a cluster of small blisters.
- Location: Can occur directly on the lip, in the corner of the mouth, or on the skin directly above or below the lip.
Diagnosis: How Your Dentist or Doctor Determines the Issue
Most cases of cold sores and pimples are diagnosed based on a visual examination and patient history.
- Clinical Examination: A dentist or medical doctor can usually differentiate between a cold sore and a pimple simply by looking at the lesion, its location, and assessing its progression. They will ask about your symptoms, when the lesion appeared, and if you've experienced similar lesions before.
- Patient History: For cold sores, a history of recurrent lesions in the same spot, especially preceded by tingling, is a strong indicator. For pimples, questions about skin care, cosmetics, and hormonal factors might be relevant.
- Laboratory Tests (Less Common for typical cases): In ambiguous or severe cases, especially if there's suspicion of a primary HSV infection or an atypical presentation (like persistent
herpes inside mouth), a viral culture or polymerase chain reaction (PCR) test can be performed to confirm the presence of HSV. For pimples, laboratory tests are almost never necessary unless a secondary bacterial infection is suspected and resistant strains are an concern.
Treatment Options for Cold Sores and Pimples
Effective treatment depends entirely on accurate diagnosis. Treating a cold sore like a pimple, or vice-versa, will be ineffective and could worsen the condition.
Treating Cold Sores
The goal of cold sore treatment is to reduce pain, shorten healing time, and prevent viral spread. Early intervention, ideally during the prodromal (tingling) stage, is most effective.
- Antiviral Medications: These are the cornerstone of cold sore treatment.
- Oral Antivirals (Prescription):
- Acyclovir (Zovirax®), Valacyclovir (Valtrex®), Famciclovir (Famvir®): These medications inhibit the replication of the HSV-1 virus. They are most effective when taken at the very first sign of an outbreak (tingling). They can significantly shorten healing time, reduce severity, and even prevent an outbreak if taken early enough. A typical course is 1-5 days.
- Pros: Highly effective, can prevent or significantly reduce outbreak duration and severity.
- Cons: Require a prescription, can be costly without insurance, may cause mild side effects like headache or nausea.
- Topical Antivirals (Prescription/OTC):
- Penciclovir cream (Denavir® - Prescription): Applied directly to the lesion multiple times a day. Can reduce healing time by about half a day.
- Docosanol cream (Abreva® - OTC): Available without a prescription, applied 5 times daily at the first sign of an outbreak. Works by inhibiting the virus from entering cells, shortening healing time.
- Pros: Direct application, may be convenient for some.
- Cons: Less potent than oral antivirals, frequent application needed, may not prevent full outbreak.
- Oral Antivirals (Prescription):
- Pain Relief:
- OTC Pain Relievers: Ibuprofen (Advil®, Motrin®) or acetaminophen (Tylenol®) can help manage pain and discomfort.
- Topical Anesthetics: Creams or gels containing lidocaine or benzocaine (e.g., Orajel®) can temporarily numb the area.
- Home Remedies and Supportive Care:
- Cold Compress: Applying a cool, damp cloth can reduce redness, swelling, and discomfort.
- Aloe Vera: Known for its soothing properties, can be applied to the lesion.
- Petroleum Jelly: Keeps the scab moist, preventing cracking and promoting healing.
- Lysine Supplements: Some individuals find that taking L-lysine supplements can reduce the frequency or severity of outbreaks, though scientific evidence is mixed.
- Avoid Irritants: Steer clear of acidic or spicy foods that can irritate the lesion.

Treating Pimples on the Lip
Treatment for pimples focuses on unclogging pores, reducing inflammation, and killing bacteria.
- Topical Treatments (OTC and Prescription):
- Salicylic Acid: Exfoliates the skin, helping to unclog pores. Available in cleansers, pads, and spot treatments.
- Benzoyl Peroxide: Kills acne-causing bacteria and helps shed dead skin cells. Available in various strengths.
- Retinoids (e.g., Adapalene - Differin® OTC; Tretinoin - Prescription): Vitamin A derivatives that promote cell turnover and prevent clogged pores.
- Topical Antibiotics (Prescription): Clindamycin or erythromycin applied to reduce bacteria and inflammation.
- Pros: Directly target the affected area, generally well-tolerated.
- Cons: Can cause dryness, redness, or irritation; may take time to show results.
- Warm Compress: Applying a warm, moist compress can help to bring pus to the surface, making the pimple resolve faster, or gently facilitate drainage if it's a whitehead. Do not pick or squeeze forcefully.
- Avoid Picking: Never pick, squeeze, or pop a pimple on your lip. This can push bacteria deeper, cause scarring, lead to infection, and prolong healing.
- Professional Drainage (Rare): For very large, painful cystic pimples, a dermatologist may perform a sterile incision and drainage to relieve pressure and speed healing. This is rarely needed for a typical lip pimple.
- Corticosteroid Injections (Rare): For severe, inflamed cysts, a dermatologist might inject a diluted corticosteroid to rapidly reduce inflammation.
Comparison Table: Cold Sore vs Pimple Treatment Options
| Feature | Cold Sore Treatment | Pimple on Lip Treatment |
|---|---|---|
| Primary Goal | Inhibit viral replication, reduce duration/pain | Unclog pores, reduce inflammation, kill bacteria |
| Medication Type | Antivirals (oral: acyclovir, valacyclovir; topical: penciclovir, docosanol) | Topicals (salicylic acid, benzoyl peroxide, retinoids, antibiotics) |
| Availability | OTC (docosanol), Prescription (oral antivirals, penciclovir) | OTC (salicylic acid, benzoyl peroxide, adapalene), Prescription (stronger retinoids, oral/topical antibiotics) |
| Application | Oral pills, topical creams/ointments | Topical creams, gels, washes; sometimes oral antibiotics for severe acne |
| Best Time to Use | At first sign (tingling) for antivirals | Regularly for prevention, or as spot treatment |
| Contagion Risk | Focus on reducing transmission | No contagion risk |
| Average Duration Reduction | 1-3 days shorter healing with antivirals | Pimple typically resolves in 3-7 days; treatment can speed up or prevent. |
Step-by-Step Management and What to Expect
Knowing how to react when you discover a lip lesion can significantly impact its duration and your comfort.
Managing a Cold Sore Outbreak
- Recognize the Prodrome (Day 0-1): At the first sign of tingling, itching, or burning, immediately begin treatment. This is your best chance to minimize the outbreak.
- Apply Antiviral Cream or Take Oral Medication: If you have a prescription for oral antivirals, take it as directed. Apply an OTC antiviral cream like docosanol or a prescription cream like penciclovir several times a day.
- Manage Pain: Use OTC pain relievers (ibuprofen, acetaminophen) or topical anesthetics if needed.
- Practice Good Hygiene (Day 1-14):
- Wash your hands thoroughly with soap and water after touching your cold sore.
- Avoid touching your eyes or other parts of your body.
- Do not share utensils, cups, towels, or razors.
- Avoid kissing or close contact with others, especially infants, young children, and immunocompromised individuals, until the cold sore is fully healed and crusted over.
- Keep Lesion Moist (Day 4-14): Once the blisters burst and crust, apply petroleum jelly or a lip balm to keep the scab soft and prevent cracking, which can be painful and delay healing.
- Monitor Healing: The cold sore should progress through the weeping and crusting stages and heal within 7-14 days. If it persists longer, worsens, or causes severe pain, consult your dentist or doctor.
Managing a Lip Pimple
- Cleanse Gently: Wash the area gently with a mild cleanser twice a day. Avoid harsh scrubbing, which can irritate the skin.
- Apply Targeted Treatment: Apply an OTC spot treatment containing salicylic acid or benzoyl peroxide directly to the pimple. Follow product instructions.
- Apply a Warm Compress: A warm, moist compress for 5-10 minutes several times a day can help reduce inflammation and bring the pimple to a head, facilitating natural drainage.
- DO NOT Pick or Squeeze: This is crucial. Picking at a pimple can introduce more bacteria, lead to infection, cause scarring, and prolong the healing process.
- Keep Area Clean: Avoid using oil-based lip products or heavy makeup directly on the pimple.
- Monitor Healing: A typical pimple should resolve within 3-7 days. If it's persistent, very painful, or shows signs of infection (spreading redness, increased pain, pus), consult a dermatologist or doctor.
Cost and Insurance Coverage
Understanding the financial aspect of treating lip lesions is important for planning your care. Costs can vary significantly based on location, type of treatment, and insurance coverage.
Cold Sore Treatment Costs
- Over-the-Counter (OTC) Treatments:
- Docosanol (Abreva®): Approximately $15-$25 per tube.
- Topical Anesthetics (e.g., Orajel®): Approximately $8-$15 per tube.
- L-Lysine Supplements: Approximately $10-$20 per bottle, depending on brand and quantity.
- Prescription Antivirals:
- Oral Acyclovir, Valacyclovir, Famciclovir: A typical course can range from $50-$200+ without insurance, depending on the dosage and quantity. Generic versions are less expensive.
- Topical Penciclovir (Denavir®): Can be quite expensive, ranging from $70-$150+ per small tube without insurance.
- Doctor's Visit: A general practitioner or dentist visit for diagnosis and prescription can cost $100-$300 without insurance, or a co-pay of $20-$75 with insurance.
Insurance Coverage: Most health insurance plans, and some dental plans, will cover prescription antiviral medications for cold sores, often with a co-pay. OTC treatments are generally not covered. It's best to check with your specific insurance provider for details. The American Dental Association (ADA) encourages regular dental check-ups, which can be a good time to discuss any oral lesions with your dentist.
Pimple Treatment Costs
- Over-the-Counter (OTC) Treatments:
- Salicylic Acid/Benzoyl Peroxide Spot Treatments: Approximately $5-$20 per tube/bottle.
- Adapalene Gel (Differin® OTC): Approximately $15-$30 per tube.
- Prescription Topicals:
- Topical Retinoids (e.g., Tretinoin): Can range from $30-$150+ per tube without insurance, depending on the brand and strength. Generic versions are more affordable.
- Topical Antibiotics (e.g., Clindamycin): Approximately $20-$60 per bottle without insurance.
- Dermatologist Visit: A visit to a dermatologist for severe or persistent acne can cost $150-$400 without insurance, or a co-pay of $30-$100 with insurance. Procedures like professional drainage or corticosteroid injections would be additional costs, typically $50-$200 per procedure.
Insurance Coverage: Medical insurance typically covers prescription acne medications and dermatologist visits, subject to deductibles and co-pays. OTC products are usually not covered.
Table: Estimated Costs for Cold Sore and Pimple Treatments (US)
| Treatment Item | Without Insurance (Low-High) | With Insurance (Co-pay/Estimated) |
|---|---|---|
| Cold Sore Treatments | ||
| OTC Docosanol (Abreva®) | $15 - $25 | Not typically covered |
| Prescription Oral Antivirals (Generic Course) | $50 - $150 | $10 - $60 |
| Prescription Topical Penciclovir | $70 - $150 | $20 - $75 |
| Doctor/Dentist Visit | $100 - $300 | $20 - $75 |
| Pimple Treatments | ||
| OTC Spot Treatment (Salicylic Acid/BP) | $5 - $20 | Not typically covered |
| OTC Adapalene Gel (Differin®) | $15 - $30 | Not typically covered |
| Prescription Topical Retinoid (Generic) | $30 - $100 | $15 - $50 |
| Dermatologist Visit | $150 - $400 | $30 - $100 |
| Pimple Drainage/Injection | $50 - $200 | $20 - $75 |
Pro Tip: Always inquire about generic versions of prescription medications, as they are significantly more affordable and equally effective. Many pharmacies also offer discount programs or coupons for common prescriptions.
Recovery and Aftercare
Proper aftercare is crucial for both rapid healing and preventing complications or future outbreaks.
Cold Sore Recovery
Once the cold sore begins to scab and flake, it's in its final stages of healing.
- Moisturize the Scab: Continue to apply petroleum jelly, unmedicated lip balm, or a gentle moisturizer to the healing scab. This prevents the scab from drying out, cracking, and becoming painful or bleeding, which could potentially introduce secondary bacterial infection.
- Avoid Picking the Scab: Let the scab fall off naturally. Picking it prematurely can lead to scarring and prolong healing.
- Sun Protection: New skin under the scab is sensitive. Use a lip balm with SPF 30 or higher, even after healing, to help prevent future sun-triggered outbreaks.
- Maintain Hygiene: Continue good hand hygiene until the lesion is completely gone to avoid spreading the virus.
- Discard Contaminated Items: Consider replacing your toothbrush or lip balm after an outbreak to prevent re-infection or spreading the virus.
Pimple Aftercare
- Gentle Cleansing: Continue a gentle cleansing routine to keep the area clean and prevent further breakouts.
- Moisturize: Use a non-comedogenic (non-pore-clogging) moisturizer to keep the skin hydrated, especially if using drying acne treatments.
- Sun Protection: Sun exposure can worsen post-inflammatory hyperpigmentation (dark spots) that sometimes remain after a pimple heals. Use a broad-spectrum sunscreen.
- Scar Prevention: If you have a tendency to scar, discuss options with a dermatologist. Early treatment and avoiding picking are the best ways to prevent scarring.
- Address Post-Inflammatory Hyperpigmentation: Dark spots left after a pimple can fade over time. Products containing niacinamide, vitamin C, or alpha hydroxy acids (AHAs) can help speed up the process.

Prevention Strategies
Preventing cold sores and pimples requires different, but equally important, approaches.
Preventing Cold Sore Outbreaks
Since HSV-1 is a lifelong virus, prevention focuses on avoiding triggers and managing the virus.
- Identify and Avoid Triggers: Pay attention to what causes your outbreaks (stress, sun, illness, certain foods). Once identified, try to avoid or mitigate these triggers.
- Sun Protection: Use lip balm with an SPF of 30 or higher daily, especially before sun exposure. Wear a wide-brimmed hat.
- Stress Management: Practice stress-reducing techniques such as meditation, yoga, regular exercise, or adequate sleep.
- Boost Immune System: Maintain a healthy lifestyle with a balanced diet, regular exercise, and sufficient sleep to keep your immune system strong.
- Antiviral Prophylaxis: For individuals with very frequent or severe outbreaks, a doctor may prescribe daily oral antiviral medication (e.g., valacyclovir) to suppress the virus and reduce the frequency of outbreaks.
- Avoid Close Contact During Outbreaks: Do not kiss, share drinks, food, or personal items (lip balm, razors) with others while you have an active cold sore.

Preventing Lip Pimples
Prevention here centers on good skincare and lifestyle habits.
- Good Oral and Facial Hygiene:
- Wash your face twice daily with a mild cleanser, especially around the mouth after eating or using lip products.
- Gently brush your teeth twice a day and floss daily, as bacteria from the mouth can sometimes contribute to lip-adjacent breakouts.
- Use Non-Comedogenic Products: Choose lip balms, lipsticks, and moisturizers labeled "non-comedogenic" or "oil-free" to prevent pore clogging.
- Avoid Touching Your Face/Lips: Hands can transfer dirt, oil, and bacteria to your lips, leading to breakouts.
- Clean Phone Screens: Your phone screen can harbor bacteria and oil, which can transfer to your face during calls. Clean it regularly.
- Diet Considerations: While not a direct cause, if you notice certain foods (like sugary snacks or excessive dairy) seem to trigger your breakouts, consider reducing them.
- Shower After Sweating: If you exercise or sweat heavily, shower promptly to remove sweat and bacteria from your skin.
Risks and Complications
While usually benign, both cold sores and pimples can lead to complications if not managed properly.
Cold Sore Complications
- Spread to Other Areas (Autoinoculation): The virus can be spread to other parts of your own body if you touch the cold sore and then touch another area before washing your hands.
- Ocular Herpes: Touching the eye can lead to a serious eye infection that can cause vision loss.
- Herpetic Whitlow: Infection of the fingers.
- Genital Herpes: Spread to the genital area.
- Widespread Infection: In individuals with weakened immune systems (e.g., HIV/AIDS, chemotherapy patients), cold sores can spread widely and cause more severe, persistent lesions, or even internal organ involvement, though this is rare.
- Eczema Herpeticum: A severe and widespread HSV infection in individuals with eczema, which can be life-threatening.
- Secondary Bacterial Infection: Open cold sores can become infected with bacteria, leading to pus, increased pain, and delayed healing.
- Scarring: While cold sores usually heal without scars, severe or repeatedly picked lesions can sometimes leave a mark.
- Herpes Inside Mouth: While typical cold sores are on the outside of the lip, HSV-1 can cause lesions inside the mouth, particularly during a primary infection (herpetic gingivostomatitis). These can be extremely painful and make eating and drinking difficult.
Pimple Complications
- Scarring: Severe or deeply inflamed pimples, especially if picked or squeezed, can lead to permanent scarring, including ice pick scars, boxcar scars, or rolling scars.
- Post-Inflammatory Hyperpigmentation (PIH): Dark spots or patches that remain after a pimple heals, particularly common in individuals with darker skin tones. These are not scars but can take months to fade.
- Secondary Bacterial Infection: Picking at a pimple can introduce more bacteria, leading to a more severe infection, cellulitis (a spreading bacterial skin infection), or abscess formation.
- Pain and Discomfort: Large, inflamed pimples can be quite painful and affect eating, speaking, or smiling.
Children / Pediatric Considerations
Both cold sores and pimples can affect children, though their presentation and management might have specific considerations.
Cold Sores in Children
- Primary Infection (Herpetic Gingivostomatitis): A child's first exposure to HSV-1 can be more severe than recurrent outbreaks. It often presents as painful blisters throughout the mouth (
herpes inside mouth), on the gums, tongue, and lips. Symptoms can include high fever, swollen and bleeding gums, difficulty eating and drinking, swollen lymph nodes, and general malaise. Dehydration is a significant concern in young children due to painful eating and drinking. - Recurrent Cold Sores: After primary infection, cold sores in children typically resemble those in adults, appearing on the lips. They are usually triggered by fever, sun exposure, or stress.
- Parental Guidance: Parents should avoid kissing children if they have an active cold sore. Teach children not to touch their cold sores and to wash their hands frequently to prevent spread to eyes or other children.
- Treatment: Antiviral medications can be prescribed for children, especially for severe primary infections. Pain relief and ensuring adequate fluid intake are crucial. Consult a pediatrician or pediatric dentist for diagnosis and treatment.
Pimples in Children
- Infant Acne: Newborns can develop "baby acne" due to maternal hormones, which typically resolves on its own without treatment.
- Childhood Acne: Before puberty, pimples are less common. If a young child develops persistent or severe acne, it might warrant investigation for underlying hormonal issues, and a dermatologist should be consulted.
- Teenage Acne: Acne is very common during puberty due to hormonal changes. Pimples on the lip in teenagers are managed similarly to adults, with good hygiene and OTC treatments. Encourage teens not to pick at their pimples.
Pro Tip: For any persistent or concerning lesion on a child's lip or in their mouth, always seek professional medical or dental advice. Self-diagnosing in children can lead to misdiagnosis and delayed appropriate care.
Frequently Asked Questions
Is a cold sore always herpes?
Yes, a cold sore is always caused by the Herpes Simplex Virus type 1 (HSV-1). Once you have a cold sore, it means you have been infected with HSV-1, and the virus remains dormant in your body for life, potentially causing future outbreaks.
Can you get herpes inside mouth and confuse it with a canker sore or other lesion?
Yes, HSV-1 can cause lesions inside the mouth, especially during a primary infection (herpetic gingivostomatitis), presenting as widespread sores on the gums, tongue, and inner cheeks. This can sometimes be confused with canker sores (aphthous ulcers), which are not viral and typically appear as single, round, white/yellow ulcers with a red border, usually on the soft tissues inside the mouth (cheeks, tongue, floor of mouth), not usually on the outside of the lips or hard palate/gums like herpes. Other oral lesions can also cause confusion, highlighting the importance of professional diagnosis.
How long does a cold sore last? How long does a pimple last?
A cold sore typically lasts for 7 to 14 days from the initial tingling sensation to complete healing. A pimple on the lip usually resolves much faster, within 3 to 7 days, depending on its size and inflammation.
Is it okay to pop a cold sore? What about a pimple?
No, you should never pop a cold sore. Popping it can spread the highly contagious virus to other areas of your body or to other people, increase the risk of secondary bacterial infection, and potentially lead to scarring. Similarly, it's generally advised not to pop a pimple, especially one on the lip, as this can push bacteria deeper, cause more inflammation, increase the risk of infection, and lead to scarring.
What are some natural remedies for cold sores or pimples?
For cold sores, some people find relief with home remedies like applying a cold compress, aloe vera, or taking L-lysine supplements (though scientific evidence is mixed). For pimples, a warm compress can help. However, for both, these are typically supportive measures and not replacements for medically proven treatments, especially for cold sores where antiviral medications are most effective.
Can lip balm cause pimples?
Yes, certain lip balms, particularly those that are heavy, greasy, or contain comedogenic ingredients (ingredients known to clog pores), can contribute to pimples around the lip line. Look for lip balms labeled "non-comedogenic" or "oil-free" if you are prone to lip pimples.
Can stress cause both cold sores and pimples?
Yes, stress is a known trigger for both conditions. Emotional or physical stress can weaken the immune system, making it easier for the dormant HSV-1 virus to reactivate and cause a cold sore. Stress can also increase inflammation and hormonal fluctuations, which can exacerbate acne and lead to pimples.
How common are cold sores?
Cold sores are extremely common. The World Health Organization estimates that 67% of the global population under 50 is infected with HSV-1. While not everyone infected experiences outbreaks, it highlights the widespread nature of the virus.
What's the difference between a cold sore and a canker sore?
Cold sores (herpes simplex labialis) are caused by the HSV-1 virus, are contagious, and typically appear as blisters on the outside of the lips or mouth, or sometimes on the gums/hard palate (herpes inside mouth). Canker sores (aphthous ulcers) are not viral, not contagious, and appear as single, painful, round, white/yellow ulcers with a red border, exclusively on the soft tissues inside the mouth (cheeks, tongue, floor of mouth, soft palate).
Could a sore or bump on the lip actually be a symptom of something more serious?
While most lip bumps are either cold sores or pimples, any persistent, non-healing sore, white patch, or red patch on the lip or inside the mouth that lasts for more than two weeks should be evaluated by a dentist or oral surgeon. These could potentially be early signs of more serious conditions like oral cancer, or other oral lesions. For general oral health, conditions like how to get tonsil stones out are related to different parts of the mouth (tonsils) but highlight the importance of paying attention to all oral symptoms.
When to See a Dentist or Doctor
While many lip lesions can be managed at home, there are clear instances when professional medical or dental attention is necessary.
See a dentist or doctor if:
- Uncertainty of Diagnosis: If you are unsure whether the lesion is a cold sore or a pimple, or if it doesn't fit the typical description of either.
- Persistent Lesion: The lesion doesn't heal within 14 days, or it gets worse despite home care or OTC treatments.
- Severe Pain or Discomfort: The lesion is unusually painful, making it difficult to eat, drink, or speak.
- Signs of Secondary Infection: The area around the lesion becomes increasingly red, swollen, warm, or develops pus, indicating a possible bacterial infection.
- Systemic Symptoms: You develop a fever, swollen lymph nodes, or general malaise along with the lip lesion, especially if it's your first cold sore outbreak.
- Compromised Immune System: If you have a weakened immune system (due to illness, medication, or medical conditions), any cold sore or oral lesion warrants a doctor's visit immediately, as complications can be more severe.
- Lesions Spreading: The blisters or sores are spreading rapidly to other parts of your face, eyes, or body. This is particularly critical for cold sores, as spread to the eyes can lead to vision problems.
- Frequent Recurrence: You experience very frequent cold sore outbreaks (e.g., more than 6 times a year) that significantly impact your quality of life. Your doctor might consider antiviral suppressive therapy.
- Large or Cystic Pimples: A pimple on the lip is unusually large, deeply inflamed, or cystic and doesn't respond to OTC treatments. A dermatologist might need to drain it or provide stronger prescription medication.
Emergency vs. Scheduled Appointment:
- Emergency Care (Seek immediate attention):
- Any lesion accompanied by a high fever, severe headache, confusion, or difficulty breathing (rare, but indicates severe infection or systemic involvement).
- Cold sore spreading to the eyes (pain, redness, vision changes).
- Signs of widespread infection in an immunocompromised individual.
- Scheduled Appointment:
- Typical persistent lesions as described above.
- Frequent recurrences.
- Uncertainty about the lesion's nature.
- Concerns about scarring or long-term management.
Your dental professional, adhering to American Dental Association (ADA) guidelines, is often the first healthcare provider to spot unusual oral lesions and can guide you on the next steps, including referral to a specialist if needed. Don't hesitate to reach out for professional advice.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

Oral Candidiasis Symptoms: Complete Guide
Oral candidiasis, commonly known as oral thrush, is a fungal infection of the mouth caused by an overgrowth of Candida yeast, most often Candida albicans. While Candida is a normal inhabitant of the human mouth in small amounts, an imbalance can lead to uncomfortable and sometimes painful symptoms
February 23, 2026
Are Cold Sores Contagious
In the United States, an estimated 67% of the population under age 50 carries the herpes simplex virus type 1 (HSV-1), the primary cause of cold sores. This means millions of Americans are susceptible to these often painful and highly visible oral lesions. Beyond the discomfort and cosmetic conc
February 23, 2026
How Long Does Hand Foot and Mouth Last
Hand, Foot, and Mouth Disease (HFMD) is a common, often uncomfortable, viral illness that can affect anyone but is particularly prevalent among young children. If you or a loved one has ever experienced the tell-tale rash or painful mouth sores, you've likely wondered: **how long does Hand Foot and
February 23, 2026
Hand Foot and Mouth Symptoms: Complete Guide
Imagine your child wakes up with a fever, feels a little off, and then you spot painful sores appearing in their mouth, followed by a tell-tale rash on their hands and feet. This scenario, unfortunately common, is often the first encounter with Hand Foot and Mouth Disease (HFMD). Affecting millions
February 23, 2026