Complete Guide to Dental Conditions & Diseases: Everything You Need to Know
Key Takeaways
- Did you know that over 90% of adults aged 20-64 have had at least one cavity? Dental conditions and diseases are remarkably common, affecting millions of Americans every year. Far from being mere inconveniences, these issues can significantly impact your overall health, leading to chronic pain, diff
Complete Guide to Dental Conditions & Diseases: Everything You Need to Know
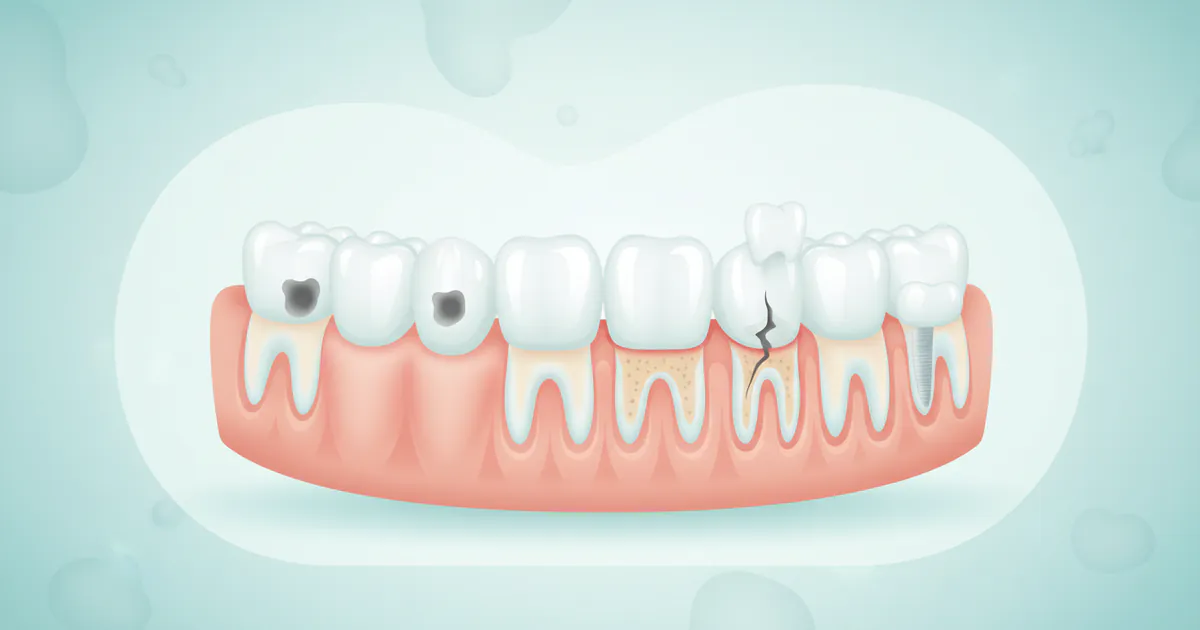
Did you know that over 90% of adults aged 20-64 have had at least one cavity? Dental conditions and diseases are remarkably common, affecting millions of Americans every year. Far from being mere inconveniences, these issues can significantly impact your overall health, leading to chronic pain, difficulty eating, and even systemic problems if left untreated. Understanding the most common dental conditions – from persistent toothaches and the early signs of a cavity to the urgent need to address a painful abscess tooth – is your first line of defense in maintaining a healthy smile and a healthy body.
This comprehensive guide from SmilePedia.net will equip you with essential knowledge about various dental conditions, their causes, symptoms, and the effective treatments available. We’ll delve into everything from the early stages of tooth decay to the critical steps needed to manage a severe tooth abscess, ensuring you know what does a cavity look like and when to seek immediate professional help. By the end of this article, you'll be empowered with the information to protect your oral health proactively, understand your treatment options, and make informed decisions about your dental care.
Key Takeaways:
- Cavities (tooth decay) are among the most common chronic diseases, preventable with good oral hygiene, fluoride, and regular dental check-ups. Untreated cavities can lead to severe pain and infection.
- A dental abscess is a serious bacterial infection that can develop rapidly, often causing intense toothache, swelling, and fever. It requires immediate professional treatment (drainage, antibiotics, root canal, or extraction) and can cost $300-$2,500+ depending on complexity.
- Recognizing early symptoms like persistent sensitivity, visible changes in tooth color, or bleeding gums can prevent minor issues from escalating into complex, painful, and costly conditions.
- Professional dental treatments for common issues range widely: Fillings for cavities typically cost $50-$250 per tooth (amalgam) or $100-$450 (composite). A root canal can range from $700-$2,000 for front teeth and $900-$2,500 for molars, often followed by a crown costing $800-$3,000.
- Ignoring dental pain, especially a severe toothache, is dangerous. Home remedies offer temporary relief at best; professional diagnosis and treatment are essential to prevent serious complications like widespread infection.
- Regular preventive care – including brushing twice daily, flossing daily, and bi-annual dental check-ups – is the most effective and cost-efficient strategy for avoiding most dental conditions.
Understanding Dental Conditions: The Basics
Your mouth is a complex ecosystem, and while it's incredibly resilient, it's also susceptible to various conditions and diseases. These can range from minor irritations to severe infections that impact your overall systemic health. Most dental problems stem from bacteria naturally present in your mouth, which, when allowed to accumulate, form plaque. This sticky film can harden into tartar and lead to a cascade of issues if not regularly removed.
Understanding the common pathways of dental disease is crucial for prevention. For example, acids produced by plaque bacteria erode tooth enamel, leading to cavities. Similarly, persistent plaque buildup along the gumline can inflame the gums, initiating gum disease. When these conditions progress, they can lead to infections, chronic pain, and even tooth loss.
Tooth Decay (Cavities): The Silent Threat
Tooth decay, commonly known as a cavity, is one of the most widespread chronic diseases in the world, affecting people of all ages. It's an irreversible process that involves the destruction of your tooth's outer surface (enamel) and deeper layers.
What It Is / Overview
A cavity is a hole that forms in a tooth due to the erosion of its hard structure. This erosion is caused by acids produced by bacteria in plaque. When you consume sugary or starchy foods and drinks, these bacteria feed on the carbohydrates, converting them into acids. These acids then attack your tooth enamel, demineralizing it over time. If not treated, this process continues, creating a visible hole and potentially reaching the sensitive inner pulp of the tooth.
Types / Variations of Tooth Decay
Tooth decay can manifest in different ways and locations:
- Coronal Cavities: These are the most common type, occurring on the chewing surfaces or between teeth.
- Root Cavities: As gums recede with age, the tooth roots become exposed. These areas are softer than enamel and more susceptible to decay.
- Recurrent Decay (Secondary Decay): Decay can form around existing fillings and crowns. This happens when the filling material becomes compromised, allowing bacteria to seep underneath.
Causes / Why It Happens
The primary cause of tooth decay is the interaction between bacteria, sugar, and tooth enamel. Key contributing factors include:
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque to build up.
- Frequent Snacking/Sipping: Constant exposure to sugars and starches doesn't give your saliva enough time to neutralize acids and remineralize enamel.
- Sugary and Acidic Foods/Drinks: Sodas, fruit juices, candies, and processed carbohydrates all contribute.
- Dry Mouth (Xerostomia): Saliva helps wash away food particles and neutralize acids. A lack of saliva (due to medications, medical conditions, or radiation therapy) increases decay risk.
- Lack of Fluoride: Fluoride strengthens enamel and helps prevent decay.
- Age: Older adults may experience gum recession, exposing roots to decay, and may have reduced salivary flow.
Signs and Symptoms
In its early stages, a cavity may not cause any noticeable symptoms. As it progresses, however, you might experience:
- Toothache: Ranging from mild sensitivity to sharp, sudden pain, especially when biting down. This is a common indicator of a developing cavity or deeper tooth decay.
- Sensitivity: Pain or discomfort when consuming hot, cold, sweet, or acidic foods and drinks.
- Visible Holes or Pits: These are clear signs of advanced tooth decay.
- Brown, Black, or White Staining: Discoloration on the surface of a tooth can indicate areas of demineralization or active decay. What does a cavity look like? Early cavities can appear as white spots (enamel demineralization). As decay progresses, these spots may turn light brown, then darker brown or black. A visible hole or pit confirms the presence of a cavity.
- Pain When Chewing: Pressure from chewing can exacerbate pain in a decayed tooth.
``
Treatment Options
Treatment for tooth decay depends on its severity:
- Fluoride Treatments: For very early decay (demineralization without a hole), professional fluoride applications can help remineralize enamel.
- Pros: Non-invasive, prevents progression.
- Cons: Only effective for earliest stages.
- Fillings: The most common treatment for a formed cavity. The decayed part of the tooth is removed, and the hole is filled with a material like amalgam (silver), composite resin (tooth-colored), or sometimes gold or porcelain.
- Pros: Restores tooth function and aesthetics, durable.
- Cons: Requires drilling, can cause temporary sensitivity.
- Crowns: If the decay is extensive but the tooth's root is healthy, a crown (a cap placed over the entire tooth) may be needed after the decayed material is removed.
- Pros: Protects a weakened tooth, restores shape and function.
- Cons: More invasive than a filling, higher cost.
- Root Canal Treatment (Endodontic Therapy): If the decay reaches the pulp (nerve) of the tooth, causing infection or significant inflammation, a root canal is necessary. The infected pulp is removed, the canals are cleaned and disinfected, and then filled and sealed. A crown usually follows. This is crucial for severe toothache caused by deep decay.
- Pros: Saves the natural tooth, relieves severe pain.
- Cons: More complex procedure, often requires a crown afterward.
- Tooth Extraction: If the tooth is too severely damaged by decay to be restored, it may need to be extracted. This is a last resort to prevent the spread of infection, especially when a tooth abscess has formed.
- Pros: Eliminates source of infection and pain.
- Cons: Loss of natural tooth, potential for shifting teeth or need for replacement (implant, bridge).
Step-by-Step Process: Dental Filling
- Diagnosis: Your dentist uses X-rays and visual examination to identify the cavity.
- Anesthesia: A local anesthetic is administered to numb the area around the affected tooth.
- Removal of Decay: The dentist uses a high-speed drill to remove the decayed tooth structure.
- Preparation: The tooth is shaped to prepare it for the filling material. For composite fillings, an etching gel is applied to create a strong bond.
- Filling Application: The chosen filling material is applied to the prepared cavity. Composite resin is cured with a special light.
- Shaping and Polishing: The dentist shapes the filling to match your natural bite and polishes it for a smooth finish.
Cost and Insurance (US)
The cost of cavity treatment varies based on the size of the cavity, the material used, and your geographic location.
| Treatment Type | Average Cost Range (Without Insurance) | Insurance Coverage |
|---|---|---|
| Fluoride Treatment | $30 - $70 | Often 100% |
| Amalgam Filling | $50 - $250 | 50-80% |
| Composite Filling | $100 - $450 | 50-80% |
| Crown | $800 - $3,000+ | 50% |
| Root Canal | $700 - $2,500+ | 50-80% |
| Extraction | $75 - $300 (simple) / $200 - $600+ (surgical) | 50-80% |
- Most dental insurance plans cover a significant portion of preventive care (like fluoride) and basic restorative care (fillings). Major procedures like crowns and root canals typically have 50% coverage, often subject to deductibles and annual maximums.
Recovery and Aftercare
After a filling, you might experience temporary sensitivity to hot or cold for a few days to weeks. Avoid chewing hard or sticky foods on the treated tooth immediately after. For root canals or extractions, follow specific post-operative instructions provided by your dentist, which may include pain medication and soft food diets.
Prevention
Preventing tooth decay is straightforward:
- Brush Twice Daily: Use a fluoride toothpaste and brush for two minutes each time.
- Floss Daily: Remove plaque and food particles from between teeth and under the gumline.
- Limit Sugary & Acidic Foods/Drinks: Reduce frequency of consumption.
- Regular Dental Check-ups & Cleanings: At least every six months. Your dentist can spot early signs of tooth decay and apply preventive treatments like sealants or fluoride.
- Dental Sealants: Thin, protective coatings applied to the chewing surfaces of back teeth to prevent food and bacteria from getting into the grooves.
- Use Fluoridated Water/Products: Drink tap water if it's fluoridated, and use fluoride mouthwash if recommended by your dentist.
Risks and Complications
Untreated tooth decay can lead to:
- Intensifying toothache.
- Infection of the pulp, requiring a root canal.
- Formation of a dental abscess (a localized collection of pus).
- Tooth loss.
- Spread of infection to other parts of the body in severe cases.
Gum Disease: Beyond Bleeding Gums
Gum disease, also known as periodontal disease, is an inflammatory condition affecting the tissues surrounding and supporting your teeth. It ranges from simple gum inflammation (gingivitis) to a serious condition that can result in significant damage to the soft tissue and bone that support your teeth (periodontitis).
What It Is / Overview
Gum disease begins when plaque bacteria build up on teeth, especially along the gum line. The toxins produced by these bacteria irritate the gum tissue, leading to inflammation.
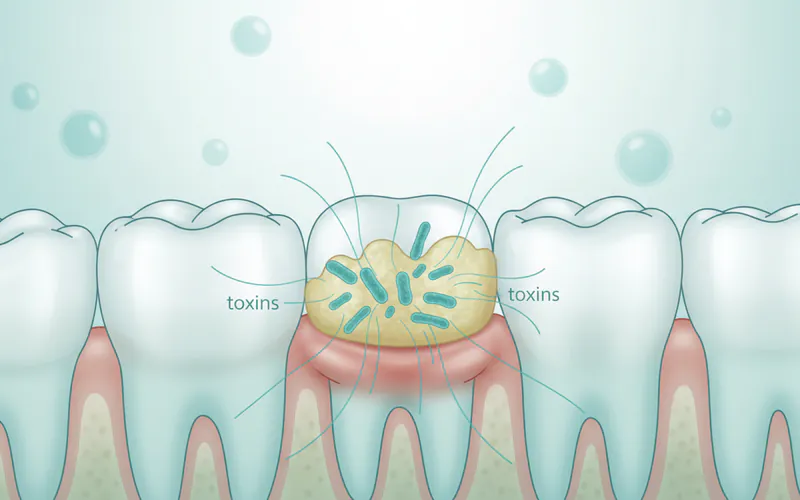
- Gingivitis: The mildest form. Gums become red, swollen, and bleed easily. At this stage, the bone and connective tissue supporting the teeth are not yet affected, and the condition is reversible with professional treatment and good home care.
- Periodontitis: If gingivitis is left untreated, it can advance to periodontitis. This chronic inflammatory condition causes the gums to pull away from the teeth, forming "pockets" that become infected. As the body tries to fight the infection, it starts to break down the bone and connective tissue that hold teeth in place. This can lead to loose teeth, persistent toothache from gum inflammation, and eventually tooth loss.
Types / Variations
Beyond chronic periodontitis, which is the most common form, other types include:
- Aggressive Periodontitis: Characterized by rapid destruction of gum tissue and bone.
- Necrotizing Periodontal Disease: A severe form seen in individuals with compromised immune systems, causing tissue death.
- Periodontitis as a Manifestation of Systemic Diseases: Conditions like diabetes, heart disease, or respiratory diseases can influence the progression of gum disease.
Causes / Why It Happens
The primary cause is bacterial plaque buildup. Other factors that increase the risk include:
- Poor Oral Hygiene: Inadequate brushing and flossing.
- Smoking/Vaping: Significantly increases the risk and severity of gum disease.
- Hormonal Changes: During pregnancy, puberty, menopause, which can make gums more sensitive.
- Genetics: Some people are more prone to gum disease.
- Certain Medications: Some drugs can cause dry mouth or affect gum health.
- Systemic Diseases: Diabetes, autoimmune diseases, and certain cancers.
- Poor Nutrition: A diet lacking essential nutrients can impair immune function.
Signs and Symptoms
Recognizing the signs early is key:
- Swollen, Red, or Tender Gums.
- Bleeding Gums: Especially when brushing or flossing.
- Persistent Bad Breath (Halitosis): Caused by bacteria in the mouth.
- Receding Gums: Gums pulling away from the teeth, making teeth appear longer.
- Pus Between Teeth and Gums.
- Loose or Shifting Teeth.
- Changes in Bite: How your teeth fit together when you bite.
- New Spaces Between Teeth.
- Dull Toothache: Caused by inflamed gums or exposed roots.
Treatment Options
Treatment aims to remove plaque and tartar, reduce inflammation, and prevent disease progression.
- Professional Dental Cleaning (Prophylaxis): For gingivitis, removal of plaque and tartar above the gum line.
- Pros: Non-invasive, reversible stage.
- Cons: Requires consistent home care to maintain.
- Scaling and Root Planing (Deep Cleaning): For periodontitis, involves meticulously cleaning below the gum line to remove plaque, tartar, and bacterial toxins from the root surfaces.
- Pros: Non-surgical, highly effective for early-to-moderate periodontitis.
- Cons: Can cause temporary sensitivity, may require multiple appointments.
- Medications: Oral antibiotics, antibiotic gels/chips placed in gum pockets, antiseptic mouthwashes.
- Pros: Helps control bacterial infection.
- Cons: Not a standalone treatment; often an adjunct.
- Surgical Treatments: For advanced periodontitis.
- Flap Surgery (Pocket Reduction Surgery): Gums are lifted back, tartar is removed, and irregular bone surfaces are smoothed.
- Bone Grafts: Uses fragments of your own bone, synthetic bone, or donated bone to rebuild bone destroyed by periodontitis.
- Soft Tissue Grafts: Uses tissue from other areas of your mouth to cover exposed roots or reinforce thin gums.
- Pros: Can save teeth, reduce pocket depth.
- Cons: More invasive, higher cost, longer recovery.
``
Step-by-Step Process: Scaling and Root Planing
- Anesthesia: Local anesthetic is applied to numb the gums and root surfaces.
- Scaling: Specialized instruments (ultrasonic scalers, hand curettes) are used to remove plaque and tartar deposits from above and below the gum line.
- Root Planing: The root surfaces are smoothed to remove bacterial toxins and prevent future plaque buildup, allowing the gums to reattach.
- Irrigation (Optional): An antimicrobial rinse may be used to further disinfect the pockets.
- Follow-up: Multiple appointments may be needed, followed by regular periodontal maintenance cleanings.
Cost and Insurance (US)
Costs for gum disease treatment vary:
| Treatment Type | Average Cost Range (Without Insurance) | Insurance Coverage |
|---|---|---|
| Routine Cleaning (Prophylaxis) | $75 - $200 | Often 100% |
| Scaling & Root Planing (per quadrant) | $150 - $450 | 50-80% |
| Oral Antibiotics (prescription) | $10 - $50 | Medical insurance often covers |
| Antibiotic Chip/Gel (per site) | $50 - $150 | 50-80% |
| Flap Surgery (per quadrant) | $500 - $1,500+ | 50% |
| Bone Graft (per site) | $400 - $1,200+ | 50% (often limited) |
| Soft Tissue Graft (per site) | $600 - $1,500+ | 50% (often limited) |
- Many dental insurance plans cover routine cleanings at 100%. Scaling and root planing often receive 50-80% coverage, while surgical procedures are typically covered at 50% after deductibles.
Recovery and Aftercare
After scaling and root planing, you might experience temporary gum tenderness, sensitivity, and minor bleeding for a few days. Follow your dentist's instructions, which typically include using an antimicrobial mouthwash and maintaining meticulous home oral hygiene. Surgical recovery involves more significant discomfort and requires strict adherence to post-operative instructions.
Prevention
- Brush and Floss Daily: Crucial for removing plaque.
- Regular Dental Check-ups: Allows for early detection and professional cleanings.
- Avoid Tobacco Products: Smoking is a major risk factor.
- Healthy Diet: Limit sugary and processed foods.
- Manage Systemic Conditions: Keep diabetes and other health issues under control.
Risks and Complications
Untreated gum disease can lead to:
- Tooth loss.
- Persistent toothache from exposed roots or inflammation.
- Increased risk of heart disease, stroke, diabetes complications, and respiratory problems (as recognized by the ADA).
- Pregnancy complications, including premature birth and low birth weight.
Dental Abscesses: A Painful Emergency
A dental abscess is a localized collection of pus caused by a bacterial infection. It can be incredibly painful and, if left untreated, can lead to serious, even life-threatening, complications. Understanding the signs of an abscess tooth and seeking immediate care is critical.
What It Is / Overview
There are two main types of dental abscesses:
- Periapical Abscess (Tooth Abscess): This forms at the tip of the tooth root. It usually results from an untreated cavity or tooth fracture that allows bacteria to invade the tooth's pulp (nerve chamber). The infection then spreads out of the root into the surrounding bone. This type is a common cause of severe toothache.
- Periodontal Abscess: This forms in the gum tissue next to the root of a tooth. It typically results from advanced gum disease where bacteria accumulate in deep periodontal pockets, causing infection in the supporting structures around the tooth.
Causes / Why It Happens
- Untreated Tooth Decay (Cavities): The most common cause of a periapical abscess tooth. A deep cavity allows bacteria to reach the pulp.
- Trauma to the Tooth: A chipped or broken tooth can expose the pulp to bacteria.
- Cracked Tooth: Even a microscopic crack can provide an entry point for bacteria.
- Advanced Gum Disease (Periodontitis): Leads to periodontal abscesses.
- Failed Root Canal: Rarely, an existing root canal can become reinfected.
Signs and Symptoms
The symptoms of a dental abscess are usually acute and noticeable:
- Severe, Persistent, Throbbing Toothache: This is the hallmark symptom, often radiating to the ear, jaw, or neck. It can be intense and interfere with sleep, and is the primary reason people search for ways to "kill tooth pain nerve in 3 seconds permanently" (which is not possible without professional help and is dangerous to attempt at home).
- Sensitivity to Hot and Cold Temperatures.
- Pain When Chewing or Biting.
- Swelling in the Face or Cheek: Often on the side of the affected tooth.
- Tender, Swollen Gums: Redness around the affected tooth.
- Pimple-Like Bump on the Gums: A "fistula" that may intermittently release pus, relieving pressure and temporarily reducing pain.
- Fever: Indicates a spreading infection.
- Swollen, Tender Lymph Nodes: In the neck or under the jaw.
- Foul Taste in the Mouth: From pus drainage.
Treatment Options
A dental abscess is a serious condition requiring immediate professional treatment. The goal is to eliminate the infection, preserve the tooth if possible, and prevent complications.
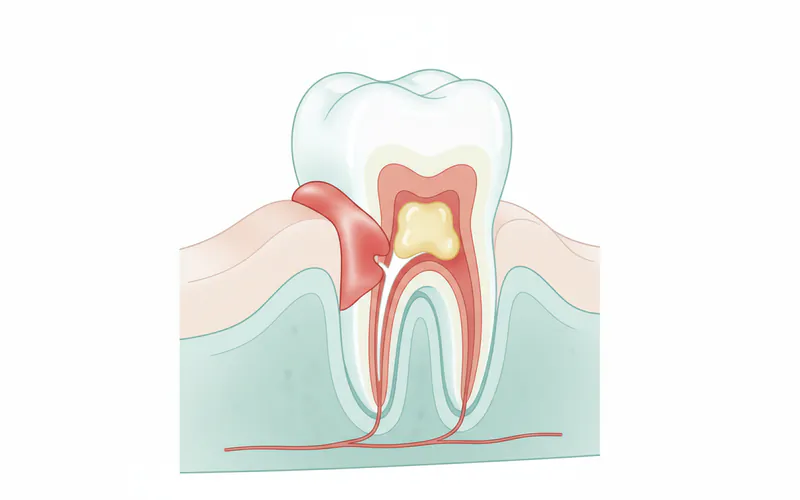
- Drainage of the Abscess: The dentist makes a small incision in the swollen area to drain the pus. This provides immediate relief from pressure and pain.
- Pros: Quick pain relief, essential first step for significant swelling.
- Cons: Does not treat the underlying cause.
- Root Canal Treatment: If the abscess tooth is caused by a periapical infection, a root canal is often the preferred treatment to save the tooth. The infected pulp is removed, the canals are cleaned, disinfected, and then filled.
- Pros: Saves the natural tooth, effectively eliminates the source of infection.
- Cons: Requires a crown afterwards, multiple visits potentially.
- Tooth Extraction: If the tooth is too extensively damaged by the abscess to be saved, or if a root canal is not feasible, extraction may be necessary.
- Pros: Removes the source of infection permanently.
- Cons: Loss of natural tooth, requires considering replacement options.
- Antibiotics: Prescribed to kill the bacteria causing the infection, especially if the infection has spread to other areas of the face or jaw, or if the patient has a weakened immune system. Antibiotics alone cannot cure an abscess; the source of infection (the tooth or gum pocket) must be treated.
- Pros: Controls spreading infection, reduces swelling.
- Cons: Not a definitive cure; must be combined with drainage or removal of the infected tissue.
Pro Tip: For patients searching for "kill tooth pain nerve in 3 seconds permanently," it's crucial to understand that severe toothache from an abscess indicates a live, infected nerve. There is no safe, permanent 3-second at-home fix. Attempting to "kill the nerve" yourself is extremely dangerous, can cause further infection, and will not address the root cause of the abscess. Immediate dental attention is the only way to safely and effectively relieve the pain and treat the infection.
Step-by-Step Process: Root Canal for an Abscessed Tooth
- Diagnosis: X-rays are taken to confirm the abscess and assess the extent of the infection.
- Anesthesia: Local anesthetic is administered to numb the tooth and surrounding area.
- Access Opening: A small opening is made through the crown of the tooth to access the pulp chamber.
- Pulp Removal & Cleaning: The infected or inflamed pulp is carefully removed from the pulp chamber and root canals. The canals are then cleaned and shaped using small files.
- Disinfection: The canals are irrigated with an antiseptic solution to kill bacteria.
- Filling the Canals: The cleaned canals are filled with a biocompatible material (gutta-percha) and sealed.
- Temporary Filling: A temporary filling is placed in the crown opening.
- Restoration: A permanent crown or filling is placed in a subsequent appointment to protect the tooth.
Cost and Insurance (US)
Costs for treating a dental abscess vary significantly based on the chosen treatment:
| Treatment Type | Average Cost Range (Without Insurance) | Insurance Coverage |
|---|---|---|
| Abscess Drainage | $100 - $300 | 50-80% |
| Antibiotics (prescription) | $10 - $50 | Medical insurance often covers |
| Root Canal (Front Tooth) | $700 - $1,500 | 50-80% |
| Root Canal (Premolar) | $800 - $1,800 | 50-80% |
| Root Canal (Molar) | $900 - $2,500 | 50-80% |
| Tooth Extraction (Simple) | $75 - $300 | 50-80% |
| Tooth Extraction (Surgical) | $200 - $600+ | 50-80% |
| Crown (after root canal) | $800 - $3,000+ | 50% |
- Emergency visits for an abscess tooth may incur additional fees. Dental insurance typically covers 50-80% of treatments like root canals and extractions after deductibles.
Recovery and Aftercare
After an abscess is treated, it's normal to experience some tenderness and discomfort. Follow all post-operative instructions:
- Pain Management: Take prescribed pain relievers or over-the-counter options.
- Antibiotics: Finish the entire course of antibiotics as prescribed, even if you feel better.
- Soft Diet: Eat soft foods for a few days to avoid irritating the area.
- Oral Hygiene: Continue gentle brushing and flossing, avoiding the immediate treatment site initially.
- Follow-up: Attend all follow-up appointments to ensure the infection has cleared and for final restoration.
Prevention
Preventing an abscess tooth centers on good oral hygiene and addressing dental problems promptly:
- Prompt Cavity Treatment: Don't delay treating a cavity.
- Good Oral Hygiene: Brush twice daily, floss daily.
- Regular Dental Check-ups: Detect and treat issues before they become severe.
- Mouthguards: Wear a mouthguard during sports to prevent trauma.
- Address Gum Disease: Treat gingivitis and periodontitis early to prevent periodontal abscesses.
Risks and Complications
An untreated dental abscess is extremely dangerous:
- Spread of Infection: Bacteria can spread to the jaw, neck, head, and even the brain, leading to life-threatening conditions like sepsis, cellulitis, or Ludwig's angina (a severe infection in the floor of the mouth and neck).
- Bone Loss: The infection can destroy surrounding bone.
- Systemic Health Issues: Increased risk of endocarditis (heart infection) in susceptible individuals.
- Increased Pain: A persistent and worsening toothache.
Other Common Dental Conditions
While cavities, gum disease, and abscesses are the most critical, several other conditions commonly affect dental health.
Tooth Sensitivity
What It Is: A sharp, temporary pain when teeth are exposed to hot, cold, sweet, or acidic stimuli. Causes: Worn enamel, exposed tooth roots (due to gum recession), cavities, cracked teeth, aggressive brushing. Treatment: Desensitizing toothpaste, fluoride treatments, bonding agents, gum grafts for root exposure. Prevention: Proper brushing technique, soft-bristle toothbrush, fluoride toothpaste, avoiding highly acidic foods.
Bruxism (Teeth Grinding/Clenching)
What It Is: Involuntary grinding or clenching of teeth, often during sleep. Causes: Stress, anxiety, sleep disorders, misaligned bite. Signs & Symptoms: Headaches, jaw pain, worn-down teeth, cracked teeth, muscle soreness in the face. Treatment: Nightguards, stress management, orthodontic correction, Botox injections for severe cases. Prevention: Awareness, relaxation techniques, custom-fitted nightguard.
Impacted Wisdom Teeth
What It Is: Third molars that don't have enough space to erupt properly and remain partially or fully trapped beneath the gum line or bone. Causes: Lack of space in the jaw. Signs & Symptoms: Pain, swelling, infection (pericoronitis), damage to adjacent teeth, cyst formation, difficulty opening mouth. Treatment: Extraction is often recommended to prevent complications. Prevention: Early dental evaluation and potential prophylactic removal.
Children / Pediatric Considerations
Children's dental health is crucial for their overall development and lifelong oral well-being. The most prevalent dental condition in children is tooth decay.
- Early Childhood Caries (ECC): Often called "baby bottle decay," this is severe cavity formation in infants and toddlers, primarily caused by prolonged exposure to sugary liquids (milk, juice) in bottles, especially at night.
- Prevention is Key:
- Start Early: Clean gums with a soft cloth even before teeth erupt.
- First Dental Visit: By age one or within six months of the first tooth erupting.
- Brush Twice Daily: With fluoride toothpaste (a smear for under 3, pea-sized for 3-6 years).
- Limit Sugary Drinks: Avoid bottles at bedtime with anything other than water.
- Dental Sealants: Applied to molars as they erupt (around age 6 and 12) to prevent cavities in deep grooves.
- Fluoride Varnish: Applied by dentists to strengthen enamel.
- Recognizing Cavities in Children: Look for white or brown spots on teeth. What does a cavity look like in a child? Often starts as a white spot near the gum line, progressing to brown and then black holes. Children may not complain of toothache until the cavity is advanced.
- Abscesses in Children: Can occur from untreated cavities. An abscess tooth in a child needs immediate attention, as infection can spread rapidly.
- Trauma: Children are prone to dental injuries. Always seek dental advice for chipped, broken, or knocked-out teeth.
Cost Breakdown
Understanding the financial aspect of dental care is vital. While costs can vary significantly, here's a general overview of US averages:
Average US Costs (Low, Mid, High)
- Preventive Care (e.g., Exam, X-rays, Cleaning): $150 - $400
- Basic Restorative (e.g., Fillings): $50 - $450 per tooth
- Major Restorative (e.g., Crowns, Root Canals): $700 - $3,000+ per tooth
- Oral Surgery (e.g., Extractions, Wisdom Teeth): $75 - $600+ per tooth
With vs. Without Insurance
- Without Insurance: You pay 100% of the listed costs. This can make extensive treatment very expensive.
- With Insurance:
- Preventive: Often 80-100% covered.
- Basic: Typically 50-80% covered.
- Major: Usually 50% covered.
- Note: Most plans have deductibles (amount you pay before coverage starts, usually $50-$150) and annual maximums (the most the insurance company will pay in a year, typically $1,000-$2,000).
Payment Plans and Financing Options
Many dental offices offer:
- In-house Payment Plans: Installment plans directly with the practice.
- Third-Party Financing: Companies like CareCredit or LendingClub offer specialized healthcare credit cards with low or no-interest payment options.
- Dental Savings Plans: Not insurance, but a membership that provides discounts on dental services from participating providers.
- Flexible Spending Accounts (FSAs) / Health Savings Accounts (HSAs): Pre-tax dollars set aside for healthcare expenses.
Cost-Saving Tips
- Prioritize Prevention: Regular cleanings and check-ups are far cheaper than treating advanced cavities or gum disease.
- Don't Delay Treatment: A small cavity is cheaper to fill than a large one requiring a root canal.
- Ask About Options: Discuss different material choices (e.g., amalgam vs. composite fillings) with your dentist.
- Get Multiple Opinions: For complex or expensive procedures, getting a second opinion can be helpful.
- Utilize Dental Schools: Dental schools often offer lower-cost treatment performed by supervised students.
Frequently Asked Questions
What does a cavity look like when it first starts?
When a cavity first starts, it often appears as a small white spot on the tooth surface. This indicates early demineralization of the enamel. As it progresses, it may turn light brown, then darker brown or black, eventually forming a visible pit or hole. Early detection is key for less invasive treatment.
How can I kill tooth pain nerve in 3 seconds permanently?
There is no safe, permanent way to "kill tooth pain nerve in 3 seconds permanently" at home. Severe toothache, especially from an abscess tooth, indicates a serious underlying issue requiring professional dental care. Attempting to self-treat can lead to further infection, damage, and potentially life-threatening complications. Over-the-counter pain relievers or cold compresses can offer temporary relief, but you must see a dentist immediately for proper diagnosis and treatment.
Is a tooth abscess an emergency?
Yes, a dental abscess is a dental emergency. It indicates a severe bacterial infection that can spread rapidly to other parts of your body, including your jaw, neck, and brain, potentially leading to life-threatening conditions like sepsis. If you suspect an abscess tooth (severe toothache, swelling, fever), seek immediate dental attention.
What causes a toothache that comes and goes?
A toothache that comes and goes can be a sign of various issues, including early tooth decay (a developing cavity), tooth sensitivity, a cracked tooth, or even early-stage gum disease. It suggests intermittent nerve irritation or inflammation. While less urgent than a constant, severe toothache, it still warrants a dental visit to determine the cause and prevent progression.
Can a cavity heal itself?
No, a true cavity (a hole in the tooth) cannot heal itself. While early enamel demineralization (white spots) can sometimes be remineralized with fluoride, once the enamel is breached and a physical hole forms due to tooth decay, it requires professional dental intervention (a filling, crown, or root canal) to restore the tooth's structure and prevent further decay.
How much does it cost to treat a tooth abscess in the US?
The cost to treat a tooth abscess in the US varies widely, typically ranging from $300 to $2,500+ without insurance. This depends on the specific treatment needed: drainage ($100-$300), antibiotics ($10-$50), root canal ($700-$2,500), or extraction ($75-$600+). A crown after a root canal adds another $800-$3,000. Dental insurance usually covers 50-80% of these costs after deductibles.
What happens if a tooth abscess is left untreated?
If a tooth abscess is left untreated, the infection can spread. This can lead to cellulitis (a serious infection of the soft tissues of the face and neck), Ludwig's angina (a life-threatening infection of the floor of the mouth), sepsis (a whole-body inflammatory response to infection), or even brain abscesses. It can also cause severe bone loss around the tooth and eventually tooth loss.
What are alternatives to a root canal for a deep cavity?
For a deep cavity that has reached the pulp, a root canal is often the best option to save the tooth. The main alternative is tooth extraction. If the tooth is extracted, you would then need to consider options for tooth replacement, such as a dental implant, bridge, or partial denture, to prevent shifting of surrounding teeth and maintain proper chewing function.
How long does a dental filling last?
The lifespan of a dental filling depends on the material, its size, your oral hygiene, and chewing habits. Amalgam (silver) fillings typically last 10-15 years or more. Composite (tooth-colored) fillings usually last 5-10 years. Gold and porcelain fillings can last 15-20 years or longer. Regular dental check-ups help monitor the condition of your fillings.
Can gum disease be cured?
Gingivitis, the mildest form of gum disease, is curable with professional dental cleanings and diligent home oral hygiene. Periodontitis, the more advanced form, cannot be fully "cured" in the sense of reversing all tissue and bone loss. However, it can be effectively managed and controlled with deep cleanings (scaling and root planing), medications, and sometimes surgery, preventing further progression and preserving your teeth.
When to See a Dentist
Knowing when to seek dental care can prevent minor issues from becoming major emergencies.
Seek Immediate Dental Attention (Emergency):
- Severe, persistent toothache: Especially if accompanied by swelling in the face or jaw, fever, or difficulty swallowing. These are signs of a potential abscess tooth or other serious infection.
- Swelling: Any unexplained swelling in your mouth, face, or neck.
- Trauma: A knocked-out tooth, severe tooth fracture, or any injury to your mouth.
- Pus Drainage: A foul taste or visible pus from your gums or around a tooth.
- Sudden looseness of a tooth.
Schedule an Appointment Promptly (Within a few days):
- Toothache that comes and goes: Even if mild, it indicates an underlying problem like a developing cavity or a cracked tooth.
- Sensitivity: New or worsening sensitivity to hot, cold, or sweets.
- Bleeding gums: Especially if it's new or persistent when brushing or flossing.
- Visible changes: You notice what does a cavity look like on your tooth (a dark spot, hole, or discoloration).
- Loose filling or crown.
- Persistent bad breath.
- Clicking or pain in your jaw.
Routine Care (Regularly Scheduled):
- Bi-annual check-ups and cleanings: Essential for preventing tooth decay and gum disease, and for early detection of issues.
- Fluoride treatments or sealants: For children, or adults at high risk for cavities.
Maintaining optimal oral health is an ongoing commitment. By understanding the common dental conditions, recognizing their symptoms, and knowing when to seek professional help, you empower yourself to keep your smile healthy and vibrant for years to come.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Is an Abscess
Imagine a throbbing pain deep within your jaw, a persistent ache that keeps you awake at night and makes even the softest foods unbearable. This isn't just a bad toothache; it could be a sign of something much more serious: a dental abscess. Affecting millions of Americans annually, an abscess is an
February 22, 2026
Cracked Tooth Syndrome: Complete Guide
Cracked Tooth Syndrome: Complete Guide Category: Dental Conditions & Diseases
February 22, 2026
Dentinogenesis Imperfecta: Complete Guide
Imagine a world where your teeth, fundamental to chewing, speaking, and even smiling confidently, are inherently fragile, discolored, and prone to rapid wear from the moment they emerge. For individuals affected by dentinogenesis imperfecta (DI), this is a reality. While relatively rare, affecti
February 22, 2026
Stage 1 Early Cavity: Complete Guide
Did you know that dental cavities are one of the most common chronic diseases globally, affecting both children and adults? In the United States, over 90% of adults have had a cavity, and a significant portion of these begin as a stage 1 early cavity. Often invisible and painless in its nasc
February 22, 2026