Stage 1 Early Cavity: Complete Guide
Key Takeaways
- Did you know that dental cavities are one of the most common chronic diseases globally, affecting both children and adults? In the United States, over 90% of adults have had a cavity, and a significant portion of these begin as a stage 1 early cavity. Often invisible and painless in its nasc
Stage 1 Early Cavity: Complete Guide
Did you know that dental cavities are one of the most common chronic diseases globally, affecting both children and adults? In the United States, over 90% of adults have had a cavity, and a significant portion of these begin as a stage 1 early cavity. Often invisible and painless in its nascent stages, an early cavity, also known as incipient caries or enamel demineralization, represents the crucial tipping point where your tooth enamel starts to weaken but before a full-blown hole forms. Understanding this initial stage is paramount, as early detection and intervention can completely reverse the damage, preventing the need for fillings or more invasive procedures down the line.
This comprehensive guide from SmilePedia.net will demystify the stage 1 early cavity, explaining what it is, why it happens, how to identify the subtle signs, and the array of effective, minimally invasive treatments available. We'll delve into prevention strategies, discuss typical costs and insurance considerations in the US, and provide practical advice for maintaining optimal oral health. By understanding the earliest indicators and proactive steps, you can safeguard your smile and avoid the progression to more severe dental problems, including the later tooth abscess stages that can result from untreated decay.
Key Takeaways:
- A stage 1 early cavity (incipient caries) is the first sign of tooth decay, characterized by enamel demineralization, often appearing as a white spot. It has not yet broken through the enamel surface.
- At this stage, cavities are often reversible through remineralization treatments like fluoride varnish, prescription toothpastes, or dental sealants.
- Early detection is crucial; these lesions are typically painless and require a dental professional for diagnosis, usually during routine check-ups.
- Costs for early cavity treatment are significantly lower than for advanced decay, ranging from $30-$70 for fluoride varnish to $40-$80 per tooth for sealants, or $150-$400 for a small composite filling if a cavitated lesion forms.
- Most dental insurance plans in the US cover preventive treatments like fluoride and sealants, and often a portion of small fillings.
- Prevention through good oral hygiene, a balanced diet, and regular dental visits is the most effective strategy to avoid stage 1 cavities and their progression.
- While searching for "glenoid cavity" might bring up anatomical information, it refers to a part of the shoulder joint and is entirely unrelated to dental health. Focus on "dental cavity" for oral health information.
What It Is / Overview
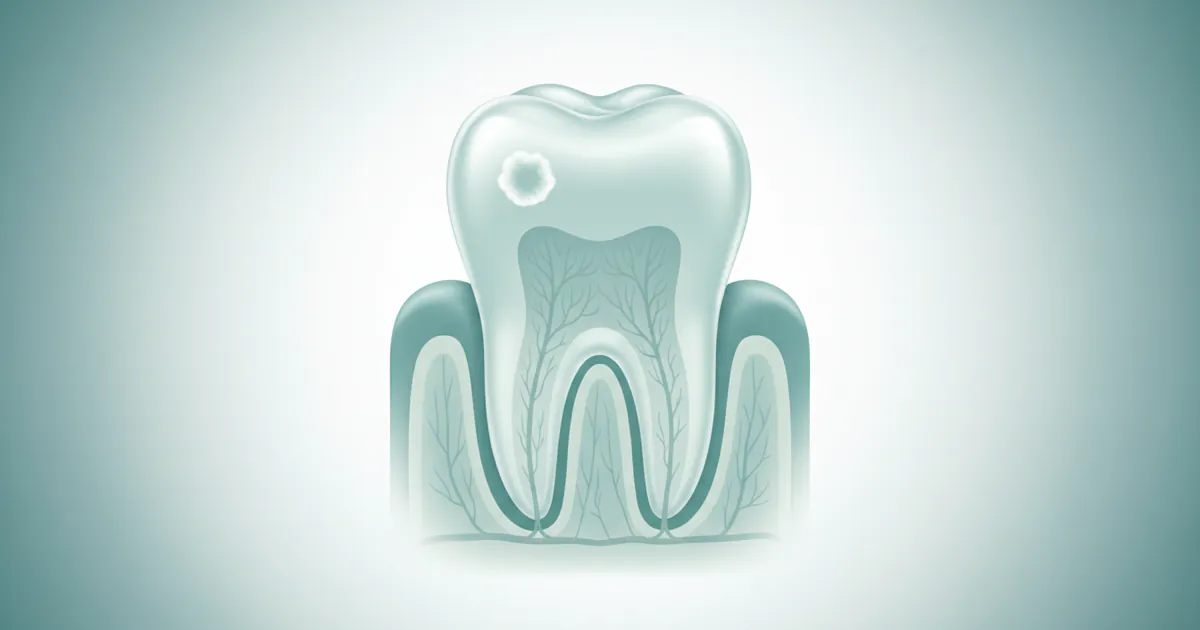
A stage 1 early cavity signifies the very beginning of tooth decay, a process often referred to as incipient caries or initial enamel lesion. At this stage, the outer protective layer of your tooth, the enamel, begins to lose its vital mineral content due to acid attacks. This process is called demineralization.
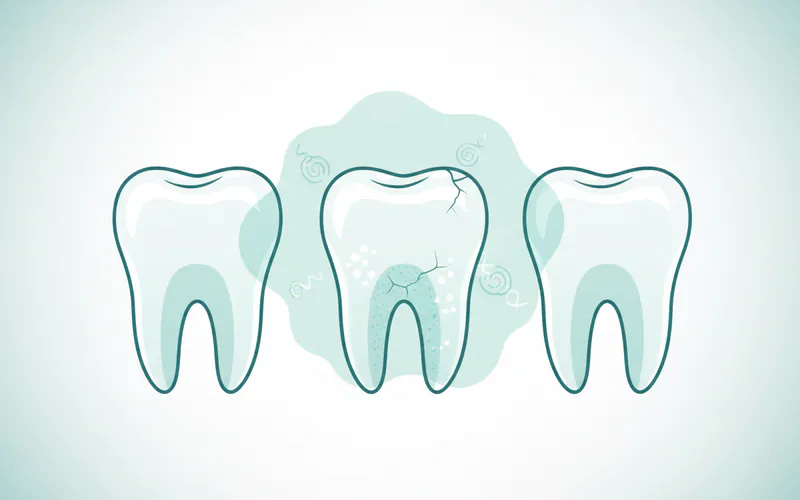
Imagine your tooth enamel as a tightly woven fabric made of mineral crystals, primarily hydroxyapatite. When acids, produced by bacteria consuming sugars in your mouth, come into contact with this enamel, they begin to dissolve these minerals. Initially, this demineralization doesn't create a visible hole or "cavity" in the traditional sense. Instead, it manifests as a tiny, often chalky-white or slightly yellowish spot on the tooth surface. This is known as a white spot lesion.
Crucially, at stage 1, the demineralization is limited to the outer half of the enamel layer. The surface enamel might still be intact, meaning no physical breakdown or hole has occurred. This makes it a non-cavitated lesion. This stage is particularly significant because it's reversible. Given the right conditions and interventions, your tooth can naturally repair itself through a process called remineralization, where minerals (like calcium, phosphate, and fluoride) are redeposited into the enamel, strengthening it again.
If left untreated, however, the demineralization process continues. The white spot lesion can eventually progress to a deeper brown or black spot, and eventually, the weakened enamel surface will collapse, forming a visible hole (cavitation). This marks the transition from a stage 1 early cavity to a more advanced stage, requiring a dental filling.
Understanding the difference between demineralization and cavitation is key. A stage 1 early cavity is essentially a warning sign, a "pre-cavity" where the enamel is under attack but still salvageable without drilling. This is why regular dental check-ups are so vital; dentists can identify these lesions long before they cause pain or require invasive treatment.
Types / Variations
While the core process of enamel demineralization is consistent, stage 1 early cavities can vary based on their location on the tooth and how they present:
1. Smooth Surface Caries
These are the most common type of early cavities and occur on the flat, smooth surfaces of the teeth, typically along the gum line (gingival third), between teeth (interproximal surfaces), or on the cheek/tongue-facing surfaces. Smooth surface caries are often easily detectable by dentists during an exam, sometimes with X-rays for interproximal areas. They usually appear as white spot lesions.
2. Pit and Fissure Caries
These occur in the grooves and depressions on the chewing surfaces of the back teeth (molars and premolars). These pits and fissures are naturally harder to clean, making them prime targets for food particles and bacteria accumulation. Early lesions here can be more challenging to detect visually as the demineralization can start deep within the grooves. Dental sealants are particularly effective at preventing this type of early cavity.
3. Root Surface Caries
Though less common for early stage 1 lesions, root surface caries can occur if the gums recede, exposing the softer root surface (dentin and cementum). These surfaces are more susceptible to decay than enamel and can demineralize more rapidly. While often more advanced when first noticed, the initial stages would still involve demineralization of the cementum.
4. Incipient vs. Arrested Lesions
- Incipient Lesions: These are active demineralization sites, where the decay process is ongoing and progressing. They often appear chalky, opaque white, and rough when probed.
- Arrested Lesions: These are early cavities that have stopped progressing. They typically appear shiny, hard, and may be stained brown or black, but the surface is intact and stable. An arrested lesion no longer requires active intervention beyond continued monitoring and good oral hygiene.
5. Non-Cavitated Lesions
This is the overarching term for stage 1 early cavities where the surface enamel is still physically intact, even if it's demineralized. The key here is that there's no actual hole (cavitation) yet. These are the lesions that are most amenable to non-invasive remineralization treatments.
Causes / Why It Happens
The development of a stage 1 early cavity is a complex interplay of several factors over time. It's not usually caused by a single event but rather a sustained imbalance in the oral environment. Here’s a breakdown of the primary causes:
1. Acid-Producing Bacteria
Your mouth is home to hundreds of types of bacteria, some of which are beneficial, while others contribute to decay. Specifically, bacteria like Streptococcus mutans and Lactobacillus are notorious for metabolizing sugars and carbohydrates from your diet. When these bacteria consume sugars, they produce acids as a byproduct. These acids are the primary culprits in initiating enamel demineralization.
2. Dietary Sugars and Carbohydrates
Frequent consumption of sugary foods and drinks (sodas, juices, candies, pastries) provides a constant fuel source for acid-producing bacteria. Even starchy foods like bread, pasta, and potato chips can break down into simple sugars in the mouth, contributing to the acid attack. The longer these sugars remain in contact with your teeth, the more acid is produced, and the greater the risk of demineralization. Snacking frequently throughout the day, without allowing time for saliva to neutralize acids, significantly increases this risk.
3. Inadequate Oral Hygiene
Poor brushing and flossing habits allow plaque to accumulate. Plaque is a sticky, colorless film of bacteria, food particles, and saliva that constantly forms on your teeth. If plaque isn't effectively removed through daily brushing and flossing, it harbors the acid-producing bacteria close to the enamel surface, leading to prolonged acid exposure and demineralization.
4. Dry Mouth (Xerostomia)
Saliva plays a critical role in preventing cavities. It helps wash away food particles, neutralizes acids, and contains minerals like calcium and phosphate that aid in the natural remineralization process. Conditions that reduce saliva flow, such as certain medications (antihistamines, antidepressants), systemic diseases (Sjögren's syndrome), radiation therapy, or even dehydration, significantly increase the risk of developing cavities, including stage 1 lesions.
5. Lack of Fluoride Exposure
Fluoride is a natural mineral that strengthens tooth enamel, making it more resistant to acid attacks. It also aids in the remineralization process. Insufficient exposure to fluoride – whether from fluoridated tap water, fluoride toothpaste, or professional fluoride treatments – leaves teeth more vulnerable to decay. The ADA (American Dental Association) strongly endorses the use of fluoride for caries prevention.
6. Genetics and Tooth Anatomy
While less controllable, genetics can play a role in your susceptibility to cavities. Some individuals may naturally have softer enamel or tooth structures with deeper pits and fissures that are harder to clean. Misaligned teeth can also create areas where food and plaque can accumulate more easily.
7. Acid Reflux or Eating Disorders
Frequent exposure to stomach acids due to conditions like GERD (Gastroesophageal Reflux Disease) or eating disorders (e.g., bulimia, which involves frequent vomiting) can directly erode tooth enamel, making it more susceptible to demineralization by oral bacteria.
Pro Tip: It's not just what you eat, but how often you eat that impacts cavity risk. Frequent snacking keeps your mouth in an acidic state, reducing the time your saliva has to neutralize acids and remineralize your enamel.
Signs and Symptoms
One of the most challenging aspects of a stage 1 early cavity is that it's often asymptomatic. This means you might not experience any pain, sensitivity, or noticeable discomfort, which is why regular dental check-ups are so vital. However, there are subtle signs that your dentist, and occasionally you, might identify:
What to Look For (Dentist's Perspective):
- White Spot Lesions: This is the hallmark of a stage 1 early cavity. The demineralized enamel appears as an opaque, chalky white spot on the tooth surface. It might be duller than the surrounding healthy enamel and can be more visible when the tooth is dry. These are most commonly seen on smooth surfaces or near the gum line.
- Rough Texture: When a dentist runs an explorer tool over a demineralized area, it might feel slightly rough or "sticky" compared to the smooth surface of healthy enamel.
- Radiographic Changes (Early Interproximal Caries): For early cavities between teeth (interproximal), dentists rely on bite-wing X-rays. While visible cavitation isn't present, the X-ray might show a subtle radiolucency (darker shadow) in the outer half of the enamel, indicating mineral loss.
- Staining (Later Stage 1): Over time, a white spot lesion can absorb stains from food and drinks, turning light brown or yellowish. At this point, it still might be a non-cavitated lesion, but the color change indicates ongoing or arrested demineralization.
What You Might Notice (Less Common for Stage 1):
- Subtle Sensitivity: In very rare cases, especially if the demineralization is progressing deeper into the enamel or is on a sensitive area like the gum line, you might experience a fleeting, mild sensitivity to cold, sweet foods, or when brushing. However, significant pain or persistent sensitivity usually indicates a more advanced cavity that has penetrated beyond the enamel.
- Visible Dull Spot: While often hard for the untrained eye, you might notice a small, dull, non-shiny spot on your tooth that doesn't brush away. It's usually not a hole, but an area where the enamel looks different.
Pro Tip: If you notice any unusual spots, changes in tooth texture, or experience even minor, transient sensitivity, it's always best to consult your dentist. Early detection of a stage 1 cavity is your best defense against more invasive treatments.
Treatment Options
The excellent news about a stage 1 early cavity is that it is often reversible and treatable with minimally invasive or non-invasive methods. The goal of treatment is to promote remineralization, arrest the decay process, or protect the vulnerable enamel.
1. Remineralization Therapies (Non-Invasive)
These treatments aim to replenish lost minerals in the enamel, strengthening it and reversing the early demineralization.
- Fluoride Varnish/Gel:
- Description: Professional application of a concentrated fluoride solution directly onto the tooth surface. Fluoride integrates into the enamel, making it more resistant to acid and promoting remineralization.
- Pros: Highly effective, quick application (minutes), painless, non-invasive, safe. Recommended by the ADA for caries prevention and early lesion management.
- Cons: Requires professional application, may leave a temporary sticky feeling or yellowish tint.
- Prescription High-Fluoride Toothpaste/Rinses:
- Description: Your dentist may prescribe toothpaste with a higher concentration of fluoride (e.g., 5000 ppm) than over-the-counter options, or a fluoride mouthrinse, for daily at-home use.
- Pros: Convenient for daily use, effectively boosts remineralization, can be used long-term.
- Cons: Requires consistent use, can be more expensive than regular toothpaste, not suitable for children who might swallow it.
- Calcium and Phosphate Pastes (e.g., MI Paste):
- Description: These pastes contain bioavailable calcium and phosphate ions that can help rebuild enamel structure. Often used in conjunction with fluoride.
- Pros: Provides building blocks for remineralization, can reduce sensitivity, pleasant taste.
- Cons: Not a substitute for fluoride, often requires prescription or dental office purchase.
2. Dental Sealants (Preventive/Arrestive)
- Description: A thin, plastic coating painted onto the chewing surfaces of molars and premolars. The sealant flows into the pits and fissures, creating a smooth surface that blocks food particles and bacteria from accumulating.
- Pros: Highly effective in preventing pit and fissure decay, can arrest very early, non-cavitated lesions by sealing off bacteria, painless application, long-lasting (up to 10 years).
- Cons: Primarily for chewing surfaces, can sometimes chip or wear down over time requiring reapplication.
3. Silver Diamine Fluoride (SDF)
- Description: A liquid solution painted onto the tooth, SDF works by stopping cavity progression and remineralizing the tooth structure. It contains silver for antimicrobial action and fluoride for remineralization.
- Pros: Non-invasive, quick application, highly effective at arresting decay, can be beneficial for very young children or those with special needs who might struggle with traditional fillings.
- Cons: Permanently stains the treated area black, which can be an aesthetic concern, especially on front teeth.
4. Resin Infiltration (e.g., Icon)
- Description: A micro-invasive technique where a highly fluid resin is infiltrated into the demineralized enamel lesion. This resin fills the microscopic pores, strengthening the enamel and preventing further acid penetration. It can also improve the appearance of white spot lesions.
- Pros: Preserves tooth structure, non-drilling approach, can improve aesthetics of white spots, quick procedure.
- Cons: Best for specific types of non-cavitated lesions (e.g., interproximal or smooth surface), requires meticulous application, can be more expensive than fluoride.
5. Minor Filling (If Cavitation Occurs)
- Description: If the stage 1 lesion has progressed and the enamel surface has broken down, forming a small hole (cavitation), then a minimal intervention filling may be required. The dentist removes only the decayed portion and fills it with a tooth-colored composite resin.
- Pros: Restores tooth structure, prevents further decay, durable, aesthetically pleasing.
- Cons: Invasive (requires drilling), more expensive than non-invasive options, may cause temporary sensitivity.
Pro Tip: Your dentist will assess the specific characteristics of your early cavity (location, activity, depth) to recommend the most appropriate treatment. The goal is always the least invasive option first.
Step-by-Step Process (Example: Fluoride Varnish Application)
When addressing a stage 1 early cavity with a non-invasive treatment like fluoride varnish, the process is quick, painless, and straightforward. Here’s what you can expect:
1. Examination and Diagnosis
Your dental hygienist or dentist will first perform a thorough oral examination. They might use a small mirror, a dental explorer, and good lighting to visually inspect your teeth for any white spot lesions or rough areas. If an early cavity is suspected between teeth, recent X-rays will be reviewed. They will confirm that the lesion is non-cavitated, meaning there is no actual hole.
2. Tooth Preparation
The specific teeth to be treated will be isolated. The dental professional will gently clean and dry the tooth surface(s) to ensure the fluoride varnish adheres properly. This might involve a quick wipe with gauze or a gentle air-dry. No drilling or needles are involved.
3. Fluoride Varnish Application
Using a small brush or applicator, the dentist or hygienist will paint a thin layer of fluoride varnish directly onto the identified early cavity and surrounding tooth surface. The varnish has a sticky consistency and often a pleasant taste (e.g., mint, caramel). It takes only a few seconds per tooth.
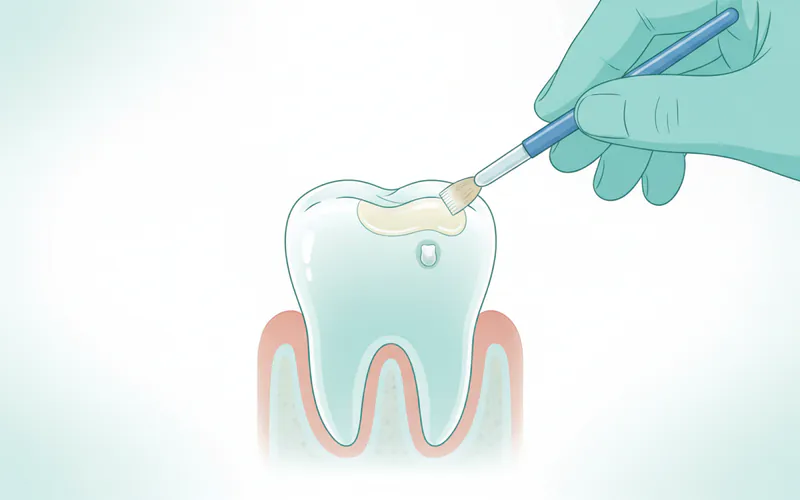
4. Drying and Setting
The varnish quickly dries upon contact with saliva, forming a protective, sticky film over the tooth. You will be instructed on post-treatment care, which typically includes: * Avoiding brushing or flossing the treated teeth for at least 4-6 hours (sometimes longer, as instructed). * Avoiding hard, crunchy, or sticky foods immediately after. * Sticking to soft foods and cool liquids for the rest of the day. * Avoiding hot beverages or alcohol for several hours.
5. Follow-up and Maintenance
You will be advised to resume your normal oral hygiene routine after the specified waiting period. Depending on your individual risk factors and the nature of the early cavity, your dentist may recommend subsequent fluoride varnish applications at regular intervals (e.g., every 3-6 months) or prescribe a high-fluoride toothpaste for at-home use. Regular dental check-ups remain essential to monitor the lesion and ensure remineralization is occurring.
Cost and Insurance
Understanding the costs associated with treating a stage 1 early cavity in the US can help you plan and budget. Fortunately, early intervention is significantly less expensive than treating advanced decay. Prices can vary widely based on your geographic location (urban vs. rural), the dental practice, and the specific treatment required.
Average US Price Ranges (Without Insurance):
| Treatment Option | Low Range | Mid Range | High Range | Notes |
|---|---|---|---|---|
| Fluoride Varnish Application | $30 - $50 | $50 - $70 | $70 - $100 | Per application, usually covered by insurance. |
| Prescription High-Fluoride TP | $15 - $30 | $30 - $45 | $45 - $60+ | Per tube, often not covered or partial coverage. |
| Dental Sealants | $40 - $60 | $60 - $80 | $80 - $100+ | Per tooth, very common for children, often covered. |
| Silver Diamine Fluoride (SDF) | $50 - $80 | $80 - $120 | $120 - $150+ | Per tooth, varies by number of surfaces. |
| Resin Infiltration (Icon) | $200 - $350 | $350 - $500 | $500 - $700+ | Per tooth, less commonly covered by insurance. |
| Small Composite Filling | $150 - $250 | $250 - $400 | $400 - $600+ | Per tooth (1-2 surfaces), if cavitation occurs. |
Insurance Coverage Details:
Most dental insurance plans in the US recognize the importance of preventive care and typically offer good coverage for stage 1 early cavity treatments:
- Fluoride Varnish/Treatments: Often covered at 80-100%, especially for children, as part of routine preventive benefits. Some plans may limit the frequency (e.g., twice a year).
- Dental Sealants: Commonly covered at 80-100% for children and adolescents (up to age 14 or 18, depending on the plan), primarily on permanent molars. Coverage for adults is less common but increasing.
- Prescription High-Fluoride Toothpaste: Coverage varies significantly. Some plans may cover a portion if prescribed for a specific condition, but many consider it an over-the-counter item.
- Silver Diamine Fluoride (SDF): Coverage is increasing as SDF gains wider acceptance, but it can still be variable. Some plans may cover it under "preventive" or "restorative" benefits, potentially at 50-80%.
- Resin Infiltration (Icon): This is a newer, more specialized treatment. Coverage can be inconsistent. It may be covered at a lower percentage (e.g., 20-50%) or not at all, depending on your plan's specific policy regarding "cosmetic" or "alternative restorative" procedures.
- Small Composite Filling: If the early cavity progresses to require a filling, it falls under basic restorative care. Most plans cover fillings at 50-80% after you've met your deductible.
Pro Tip: Always contact your dental insurance provider directly before treatment to understand your specific benefits, coverage percentages, deductibles, and annual maximums. Ask for a pre-treatment estimate from your dental office if you're unsure.
Payment Plans and Financing Options:
If you don't have insurance or face high out-of-pocket costs, several options can help manage expenses:
- Dental Savings Plans: These are not insurance but membership programs where you pay an annual fee and get discounted rates on dental services.
- Payment Plans: Many dental offices offer in-house payment plans, allowing you to pay in installments.
- Third-Party Financing: Companies like CareCredit offer special financing options for healthcare expenses, often with interest-free periods if paid in full within a certain timeframe.
- Community Dental Clinics: Often provide services at reduced rates based on income.
- Dental Schools: May offer lower-cost treatment performed by students under faculty supervision.
Recovery and Aftercare
Recovery from treatment for a stage 1 early cavity is typically very minimal, especially with non-invasive remineralization therapies. The focus shifts to long-term aftercare and prevention to ensure the lesion is arrested or reversed and to prevent new ones from forming.
Immediate Aftercare (Post-Treatment Specifics):
- After Fluoride Varnish/SDF:
- Avoid brushing or flossing for at least 4-6 hours (or as instructed by your dentist) to allow the fluoride to fully absorb and harden.
- Avoid hard, crunchy, sticky, or very hot foods and drinks for the rest of the day. Stick to soft foods and cool liquids.
- You may notice a temporary yellowish or brownish tint on your teeth (from varnish) or a black stain on the treated area (from SDF). The varnish stain will disappear after you resume brushing.
- After Dental Sealants:
- Avoid chewing on hard foods, ice, or sticky candies for the first 24 hours to allow the sealant to fully cure and bond.
- You might notice a slightly different texture or height on your chewing surface initially, but this should feel normal within a day or two. If it feels too high and affects your bite, contact your dentist.
- After Resin Infiltration:
- Similar to sealants, avoid extremely hard foods for the first day. The treated tooth may feel slightly different to your tongue initially.
- You might be advised to avoid highly staining foods/drinks for a short period to allow full stabilization of the resin.
- After a Small Composite Filling (if needed):
- If local anesthetic was used, be cautious not to bite your cheek, tongue, or lip until the numbness wears off completely (usually a few hours).
- Avoid chewing directly on the filled tooth for the first 24 hours, especially if it was a larger filling, to allow the material to fully set and prevent premature wear.
- Mild sensitivity to hot, cold, or pressure is common for a few days up to a couple of weeks. This should subside. If it persists or worsens, contact your dentist.
Long-Term Aftercare and Maintenance:
Regardless of the specific treatment, consistent home care and professional follow-up are critical for long-term success:
- Maintain Excellent Oral Hygiene:
- Brush twice daily for two minutes with a fluoride toothpaste.
- Floss daily to clean between teeth and under the gum line.
- Consider an antimicrobial or fluoride mouthrinse if recommended by your dentist.
- Dietary Modifications:
- Limit frequent snacking and reduce consumption of sugary and acidic foods and drinks.
- Choose water over sugary beverages.
- If you consume acidic foods/drinks, rinse your mouth with water immediately afterward.
- Regular Dental Check-ups and Cleanings:
- Visit your dentist every six months, or more frequently if you have a high risk of cavities. These appointments allow for early detection of new lesions and professional cleanings to remove stubborn plaque.
- Professional Fluoride Treatments: Your dentist may recommend periodic professional fluoride applications, especially if you have a history of early cavities or are at high risk.
- Monitor for Changes: Pay attention to your teeth. If you notice new white spots, sensitivity, or any discomfort, don't wait for your next appointment; contact your dental office.
Pro Tip: Your dentist will likely want to monitor the treated early cavity during subsequent check-ups to confirm that it has remineralized or remained arrested. This ongoing vigilance is key to preventing progression.
Prevention
Preventing a stage 1 early cavity is far easier and less expensive than treating one. The good news is that most preventive measures are simple, effective, and beneficial for your overall oral and systemic health. Adhering to these guidelines, many supported by the ADA, can significantly reduce your risk.
1. Excellent Oral Hygiene Routine:
- Brush Twice Daily with Fluoride Toothpaste: Use a soft-bristled toothbrush and brush thoroughly for at least two minutes, covering all tooth surfaces. Fluoride toothpaste strengthens enamel and aids remineralization.
- Floss Daily: Flossing removes plaque and food particles from between teeth and along the gum line, areas where toothbrushes can't reach and where smooth surface and interproximal cavities often begin.
- Consider Mouthwash: An antiseptic mouthwash can help reduce bacteria, while a fluoride mouthwash can provide an extra layer of enamel protection, especially if you have a high cavity risk.
2. Smart Dietary Choices:
- Limit Sugary and Acidic Foods/Drinks: Reduce your intake of soda, fruit juices, candies, cookies, and other high-sugar items. These feed acid-producing bacteria.
- Minimize Frequent Snacking: Each time you eat, your mouth becomes acidic. Giving your mouth a break between meals allows saliva to neutralize acids and initiate remineralization.
- Choose Water: Water helps rinse away food particles and acids. Tap water in many areas is fluoridated, offering an added benefit.
- Eat Enamel-Friendly Foods: Dairy products (cheese, milk, yogurt), leafy greens, and crunchy vegetables can help stimulate saliva flow and provide beneficial minerals.
3. Regular Dental Check-ups and Professional Cleanings:
- Visit Your Dentist Every Six Months: These routine visits are crucial for early detection of stage 1 cavities (often before you even notice them), professional cleanings to remove plaque and tartar, and personalized risk assessment.
- Professional Fluoride Treatments: Your dentist may recommend in-office fluoride applications, particularly if you're at high risk for cavities, to strengthen your enamel.
4. Dental Sealants:
- Protect Chewing Surfaces: Dental sealants are thin, plastic coatings applied to the chewing surfaces of molars and premolars. They create a smooth barrier over the natural pits and fissures, preventing food and bacteria from getting trapped and causing decay. They are highly recommended for children and adolescents but can also benefit adults.
5. Adequate Fluoride Exposure:
- Fluoridated Water: If available in your community, drinking fluoridated tap water is an easy and effective way to get systemic and topical fluoride benefits.
- Fluoride Toothpaste: Always use a fluoride toothpaste.
- Prescription Fluoride Products: If you have a high risk of cavities, your dentist may prescribe a higher-strength fluoride toothpaste or rinse.
6. Address Dry Mouth:
- If you suffer from dry mouth, discuss it with your dentist and physician. Strategies include drinking more water, using saliva substitutes, chewing sugar-free gum, and adjusting medications if possible.
| Prevention Strategy | How It Works | Benefits for Stage 1 Cavities | Who Benefits Most |
|---|---|---|---|
| Daily Brushing/Flossing | Removes plaque and food particles, reducing acid-producing bacteria. | Prevents initial demineralization, especially on smooth surfaces. | Everyone, essential foundation. |
| Fluoride Use | Strengthens enamel, makes it acid-resistant, promotes remineralization. | Prevents and reverses early demineralization. | Everyone, especially those at higher risk. |
| Dietary Modifications | Reduces sugar availability for bacteria, limits acid attacks. | Decreases frequency and intensity of demineralization. | Individuals with high sugar intake, frequent snackers. |
| Dental Sealants | Physical barrier in pits/fissures, blocking bacteria and food. | Highly effective for preventing pit & fissure caries. | Children, adolescents, adults with deep grooves. |
| Regular Dental Visits | Professional cleaning, early detection, risk assessment, topical fluoride. | Identifies early lesions before they become symptomatic. | Everyone, crucial for ongoing monitoring. |
Risks and Complications
While a stage 1 early cavity is the least severe form of tooth decay, leaving it untreated carries significant risks and can lead to a cascade of more serious dental problems. The primary complication is its progression to more advanced stages.
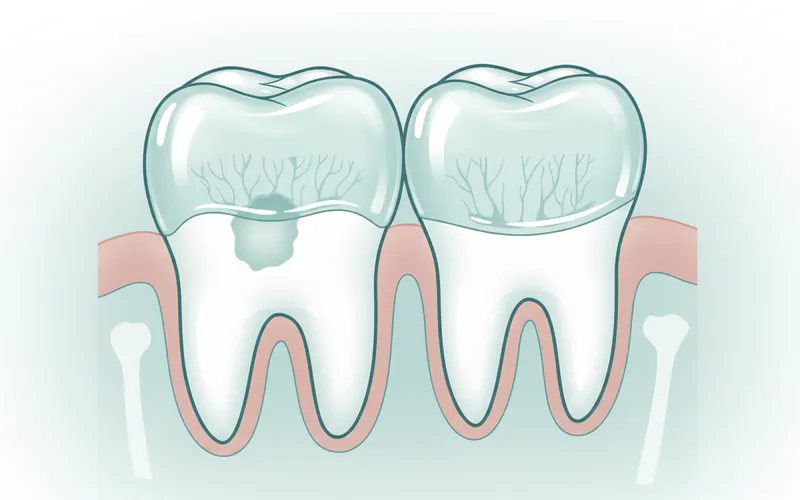
1. Progression to Deeper Cavities (Cavitation)
The most immediate risk is that the demineralized enamel will eventually break down, forming a visible hole (cavitation). Once a hole forms, the cavity is no longer considered "early" and cannot be reversed by remineralization alone. It will require a dental filling to restore the tooth structure. This means drilling, which is more invasive and costly than early interventions.
2. Increased Sensitivity and Pain
As the cavity progresses beyond the enamel and into the softer, more porous dentin layer beneath, you will likely start to experience more noticeable symptoms. This can include: * Increased sensitivity to hot, cold, or sweet foods and drinks. * Lingering pain or discomfort, especially when chewing. * Pain that doesn't go away quickly after the stimulus is removed.
3. Pulp Infection (Pulpitis)
If the decay continues unchecked, it will eventually reach the innermost part of the tooth, the dental pulp, which contains nerves and blood vessels. This can lead to a painful infection called pulpitis. Symptoms include severe, throbbing pain, sensitivity to pressure, and sometimes swelling. Pulpitis can be reversible if caught early, but often requires more extensive treatment.
4. Dental Abscess
An untreated pulp infection can spread beyond the tooth's root tip and into the surrounding bone, forming a painful pocket of pus called a dental abscess. This is a serious condition that can cause: * Intense, persistent pain. * Swelling in the face or jaw. * Fever. * A pimple-like bump on the gums. * Difficulty opening the mouth or swallowing. A dental abscess requires immediate treatment, which may include a root canal, drainage of the infection, and antibiotics. If left untreated, the infection can spread to other parts of the body, potentially leading to life-threatening complications like sepsis. This is the advanced stage often associated with tooth abscess stages mentioned in search queries.
5. Tooth Loss
In the most severe cases of extensive decay and infection, the tooth may become so compromised that it cannot be saved and must be extracted. This leads to further complications like shifting teeth, difficulty chewing, and the need for costly tooth replacement options like implants or bridges.
6. Systemic Health Issues
Chronic oral infections, including those stemming from untreated cavities and abscesses, have been linked to broader systemic health problems. Research suggests connections between poor oral health and conditions such as heart disease, stroke, diabetes complications, and adverse pregnancy outcomes.
Pro Tip: Never ignore even mild or intermittent tooth sensitivity or discomfort. While a stage 1 cavity might be silent, its progression is often marked by increasing symptoms that signal deeper trouble. Early intervention is always the best course of action.
Children / Pediatric Considerations
A stage 1 early cavity in children's primary (baby) teeth warrants particular attention. While baby teeth are temporary, they play crucial roles in chewing, speech development, and holding space for permanent teeth. An early cavity in a child can quickly escalate due to the thinner enamel of primary teeth.
Why Early Cavities Are a Concern in Children:
- Thinner Enamel: Children's primary teeth have a thinner enamel layer compared to adult permanent teeth. This means that demineralization can progress to a full-blown cavity (cavitation) much faster.
- Rapid Progression: What might be a slowly progressing white spot lesion in an adult can become a deep cavity in a child in a relatively short period.
- Pain and Infection Risk: Even small cavities can cause pain, affecting a child's eating, sleeping, and school performance. Untreated cavities can lead to infections and abscesses, which can impact the developing permanent teeth beneath.
- Space Maintenance: If a primary tooth is lost prematurely due to extensive decay or extraction, it can lead to space loss, causing permanent teeth to erupt incorrectly or become crowded.
- Habit Formation: Early childhood caries can establish a pattern of poor oral health that continues into adulthood.
Pediatric Treatment and Prevention Strategies:
- First Dental Visit by Age One: The ADA recommends a child's first dental visit by their first birthday or when their first tooth erupts. This establishes a "dental home" and allows for early risk assessment and parental education.
- Fluoride Varnish: Highly recommended for children starting from when their first tooth erupts. Regular professional fluoride applications are a cornerstone of pediatric cavity prevention and treatment of early lesions.
- Dental Sealants: Crucial for protecting the chewing surfaces of permanent molars as soon as they erupt (typically around ages 6 and 12). Sealants can also be placed on primary molars if deep grooves are present.
- Silver Diamine Fluoride (SDF): An excellent option for arresting early cavities in young children, especially those who are uncooperative with traditional drilling. While it stains the tooth black, it's a non-invasive way to stop decay progression.
- Parental Involvement: Parents play the primary role in establishing good oral hygiene habits.
- Brush your child's teeth twice a day with a smear (rice grain size for under 3) or pea-sized amount (for 3-6) of fluoride toothpaste.
- Floss your child's teeth daily once teeth are touching.
- Avoid "baby bottle decay" by not letting children sleep with bottles containing milk, juice, or formula.
- Limit sugary snacks and drinks.
- Dietary Counseling: Pediatric dentists will often provide guidance on healthy eating habits and how to minimize sugar exposure.
Pro Tip for Parents: If you notice any white spots, discoloration, or roughness on your child's teeth, or if they complain of any sensitivity, schedule an appointment with their pediatric dentist promptly. Early action can save their teeth and prevent a visit that requires a drill.
Frequently Asked Questions
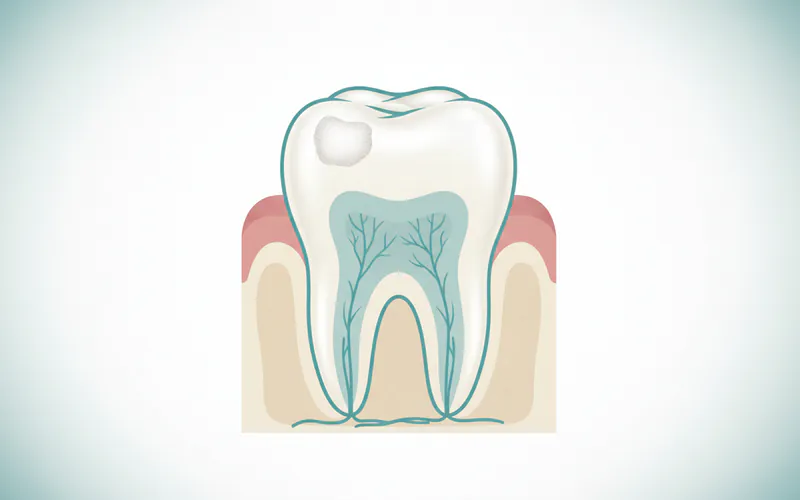
What does a stage 1 early cavity look like?
A stage 1 early cavity typically appears as a chalky white or dull spot on the tooth surface, often visible when the tooth is dry. This "white spot lesion" indicates demineralization of the enamel. It usually doesn't have a visible hole or breakdown of the tooth surface yet.
Is a stage 1 early cavity reversible?
Yes, absolutely. One of the most significant advantages of catching a cavity at stage 1 is that it is often reversible through remineralization. Treatments like professional fluoride applications, prescription fluoride toothpaste, and improved oral hygiene can help the enamel regain its lost minerals and strengthen itself.
How long does it take for a stage 1 cavity to progress?
The progression rate varies greatly depending on factors like diet, oral hygiene, saliva flow, and individual susceptibility. Some early cavities can remain stable for years, while others can progress to deeper cavitation within months, especially in children with thinner enamel or individuals with poor oral hygiene.
Is a stage 1 early cavity painful?
Generally, no. Stage 1 early cavities are typically painless because the demineralization is confined to the outermost layer of enamel, which has no nerve endings. Pain or sensitivity usually indicates that the decay has progressed deeper into the tooth, often into the dentin.
Does a stage 1 early cavity require a filling?
Not usually. The primary goal for a stage 1 early cavity is to remineralize the enamel and arrest the decay process using non-invasive methods like fluoride varnish, sealants, or prescription fluoride products. A filling is typically only required if the lesion has progressed and formed a visible hole (cavitation) that cannot be reversed.
How can I tell if I have an early cavity at home?
It can be very difficult to identify a stage 1 early cavity at home, as they are often subtle and painless. You might notice a dull white spot or a slightly rough area on your tooth. However, regular dental check-ups are crucial because dentists are trained to spot these early signs, sometimes with the aid of X-rays, long before they become apparent to you.
What is the difference between a cavity and a "glenoid cavity"?
A dental cavity (or dental caries) refers to a hole or breakdown in a tooth caused by decay. In contrast, the "glenoid cavity" is an anatomical term that refers to the shallow socket on the shoulder blade (scapula) where the head of the humerus (upper arm bone) articulates. It is entirely unrelated to dental health and teeth.
What happens if a stage 1 cavity is left untreated?
If left untreated, a stage 1 early cavity will likely progress. The demineralization will continue, eventually leading to the breakdown of the enamel and the formation of a deeper cavity that requires a filling. Further progression can lead to tooth sensitivity, pain, infection of the tooth pulp, a dental abscess, and potentially tooth loss.
Can diet alone reverse a stage 1 cavity?
While diet plays a crucial role in preventing cavities and supporting remineralization, it's unlikely to fully reverse an active stage 1 lesion on its own. Reducing sugary and acidic foods is vital, but professional interventions like fluoride treatments are often necessary to effectively halt and reverse the demineralization process.
Are there natural remedies for a stage 1 early cavity?
While some natural approaches like oil pulling or specific herbal rinses are sometimes promoted, there is limited scientific evidence to support their effectiveness in reversing or treating existing stage 1 early cavities. The most scientifically proven methods for remineralization involve fluoride and other mineral-rich dental products, alongside excellent oral hygiene and a healthy diet. Always consult your dentist before relying on unproven remedies.
When to See a Dentist
Given that a stage 1 early cavity is often asymptomatic, knowing when to see a dentist is crucial for early detection and intervention. Regular dental check-ups are your best defense, but there are also specific warning signs that warrant an earlier visit.
Routine Care Guidance (Crucial for Early Cavities):
- Schedule Regular Check-ups (Every 6 Months): This is the most important recommendation. During these visits, your dentist and hygienist can thoroughly examine your teeth, take X-rays (when needed), and identify stage 1 early cavities long before they cause any symptoms or progress. This allows for non-invasive, preventive treatments.
- Professional Cleanings: These appointments also include professional cleanings, which remove plaque and tartar that contribute to decay.
Red Flags That Need Attention (Don't Wait):
While a stage 1 cavity itself might not cause these, their presence could indicate progression or other issues, and warrant an immediate check:
- Persistent Sensitivity: If you experience new or lingering sensitivity to hot, cold, or sweet foods/drinks that doesn't quickly disappear.
- Toothache or Pain: Any persistent toothache, throbbing pain, or discomfort, especially when biting down.
- Visible Spots or Discoloration: If you notice any new white, brown, or black spots on your teeth, or areas that look dull and different from the surrounding enamel.
- Roughness or "Catching" on Your Toothbrush/Floss: If your toothbrush or floss consistently snags on a particular spot, it could indicate a developing cavity.
- Swelling or Redness Around a Tooth: This can be a sign of infection or a developing tooth abscess, which requires urgent attention.
- Unpleasant Taste or Bad Breath: While common, persistent bad breath or an unpleasant taste in your mouth could signal underlying decay or infection.
Emergency vs. Scheduled Appointment Guidance:
- Emergency: Seek immediate dental care if you experience severe, throbbing pain, significant swelling in your face or jaw, a fever accompanying dental pain, or difficulty swallowing. These could be signs of a serious infection or abscess.
- Scheduled Appointment: For less urgent concerns like mild, transient sensitivity, new discolorations, or a general feeling that "something isn't right" with a tooth, schedule an appointment with your dentist as soon as possible. While not an emergency, addressing these promptly can prevent the progression of a stage 1 early cavity into a more severe problem.
Remember, early detection and proactive management of a stage 1 early cavity are key to maintaining long-term oral health and avoiding more invasive, painful, and costly dental procedures.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Is an Abscess
Imagine a throbbing pain deep within your jaw, a persistent ache that keeps you awake at night and makes even the softest foods unbearable. This isn't just a bad toothache; it could be a sign of something much more serious: a dental abscess. Affecting millions of Americans annually, an abscess is an
February 22, 2026
Cracked Tooth Syndrome: Complete Guide
Cracked Tooth Syndrome: Complete Guide Category: Dental Conditions & Diseases
February 22, 2026
Dentinogenesis Imperfecta: Complete Guide
Imagine a world where your teeth, fundamental to chewing, speaking, and even smiling confidently, are inherently fragile, discolored, and prone to rapid wear from the moment they emerge. For individuals affected by dentinogenesis imperfecta (DI), this is a reality. While relatively rare, affecti
February 22, 2026
Clove Oil for Toothache: Complete Guide
Few experiences are as acutely distressing as a throbbing toothache, often striking at the most inconvenient times, like the middle of the night. It's a pain that can disrupt sleep, concentration, and overall well-being. While modern dentistry offers definitive solutions, many individuals seek immed
February 22, 2026