Dry Mouth Causes: Complete Guide
Key Takeaways
- Do you frequently experience a parched throat, a sticky sensation in your mouth, or difficulty speaking and swallowing? If so, you're not alone. Dry mouth, medically known as xerostomia, is a common condition affecting millions of Americans, with estimates suggesting it impacts up to **25% of adults
Do you frequently experience a parched throat, a sticky sensation in your mouth, or difficulty speaking and swallowing? If so, you're not alone. Dry mouth, medically known as xerostomia, is a common condition affecting millions of Americans, with estimates suggesting it impacts up to 25% of adults and even higher percentages among the elderly. Beyond the discomfort, understanding the root dry mouth causes is crucial because saliva plays a vital role in maintaining your overall oral and systemic health. It helps neutralize acids, wash away food particles, remineralize tooth enamel, and prevent infections. A persistent lack of saliva can lead to serious dental complications and significantly impact your quality of life.
This comprehensive guide from SmilePedia.net will delve deep into the many reasons why your mouth might be feeling dry. We'll explore the various types of dry mouth, identify common signs and symptoms, and provide an exhaustive list of contributing factors, from medications and medical conditions to lifestyle choices. Furthermore, we'll equip you with knowledge about effective treatment options, prevention strategies, and when it’s essential to consult a dental professional. By the end of this article, you will have a clear understanding of dry mouth and how to manage it for a healthier, more comfortable smile.
Key Takeaways:
- Prevalence: Dry mouth (xerostomia) affects approximately 25% of the general adult population in the US, with higher rates among seniors due to polypharmacy.
- Primary Causes: Medications (over 500 drugs can cause dry mouth), certain medical conditions (e.g., Sjögren's Syndrome, diabetes), and cancer therapies (radiation to the head/neck) are the most common culprits.
- Symptoms: Look for persistent thirst, difficulty chewing/swallowing/speaking, bad breath, altered taste, cracked lips, and increased susceptibility to cavities or oral infections.
- Diagnosis: A dentist can diagnose dry mouth through a comprehensive oral exam and sometimes a salivary flow test (sialometry), typically costing $50-$150 without insurance.
- Treatment Avenues: Solutions range from over-the-counter (OTC) saliva substitutes ($5-$30/month) and lifestyle modifications to prescription medications like pilocarpine or cevimeline ($30-$200+/month).
- Complications: Untreated dry mouth significantly increases the risk of severe tooth decay, gum disease, and oral candidiasis (thrush).
- Prevention: Staying hydrated, avoiding dehydrating substances (caffeine, alcohol, tobacco), and regular dental check-ups are key preventive measures.
What It Is / Overview
Dry mouth, scientifically known as xerostomia, is not a disease in itself but rather a symptom defined by the subjective sensation of oral dryness. While it’s the feeling that brings patients to the dentist, the underlying issue is often hyposalivation, which is an objective decrease in saliva production by the salivary glands.

Saliva, often underestimated, is a complex fluid crucial for maintaining oral health and initiating digestion. Produced by three major pairs of salivary glands (parotid, submandibular, and sublingual) and numerous minor glands, saliva performs several vital functions:
- Lubrication: It moistens food, making chewing and swallowing easier, and lubricates the mouth tissues, preventing friction and irritation.
- Digestion: Saliva contains enzymes (like amylase) that begin the breakdown of carbohydrates in food.
- Protection: It continuously washes away food debris and bacteria, reducing the risk of plaque formation and subsequent cavities and gum disease.
- Buffering: Saliva neutralizes acids produced by bacteria and from acidic foods, protecting tooth enamel.
- Remineralization: It carries essential minerals like calcium and phosphate, which help repair and strengthen tooth enamel, counteracting early signs of decay.
- Antimicrobial Action: Saliva contains antibodies and enzymes (e.g., lysozyme, lactoferrin) that fight bacteria, fungi, and viruses, preventing oral infections like candidiasis (thrush).
- Taste: It helps dissolve taste molecules, allowing taste buds to detect flavors.
When saliva flow is significantly reduced, these protective functions are compromised, leading to a cascade of oral and systemic health problems. This makes understanding the dry mouth causes and addressing them paramount for overall well-being.
Types / Variations
Dry mouth can manifest in several ways, often categorized by its duration or the clarity of its underlying cause:
Transient vs. Chronic Dry Mouth
- Transient Dry Mouth: This type is temporary and often resolves once the immediate cause is removed. Examples include dryness experienced during acute dehydration, short-term medication use, or temporary anxiety.
- Chronic Dry Mouth: This form is persistent and often indicates an ongoing underlying issue, such as a chronic medical condition, long-term medication use, or permanent damage to salivary glands. This is the more concerning type requiring sustained management.
Objective (Hyposalivation) vs. Subjective (Xerostomia)
It's important to distinguish between the feeling of dry mouth and the actual reduction in saliva:
- Xerostomia (Subjective Dry Mouth): This refers to the patient's perception of dryness. Interestingly, some individuals may feel their mouth is dry even when their salivary flow is normal, perhaps due to changes in saliva composition or nerve sensitivity. Conversely, some individuals may have reduced flow but not report dryness.
- Hyposalivation (Objective Dry Mouth): This is the measurable reduction in salivary flow rate. A healthy unstimulated salivary flow rate is typically 0.3-0.4 mL/minute. A rate below 0.1-0.2 mL/minute is generally considered hyposalivation and objectively confirms dry mouth. This objective measure is often assessed by a dentist or oral medicine specialist using a test called sialometry.
Specific Causes-Related Variations
While not distinct "types," dry mouth can also be categorized by its primary etiology, such as:
- Medication-Induced Dry Mouth: The most common form, directly linked to pharmaceutical side effects.
- Radiation-Induced Dry Mouth: Occurs in cancer patients receiving radiation therapy to the head and neck, often leading to permanent salivary gland damage.
- Systemic Disease-Related Dry Mouth: A symptom of underlying autoimmune diseases (e.g., Sjögren's Syndrome) or other chronic illnesses.
Understanding these distinctions helps dental and medical professionals accurately diagnose and manage the condition, focusing on the specific dry mouth causes at play.
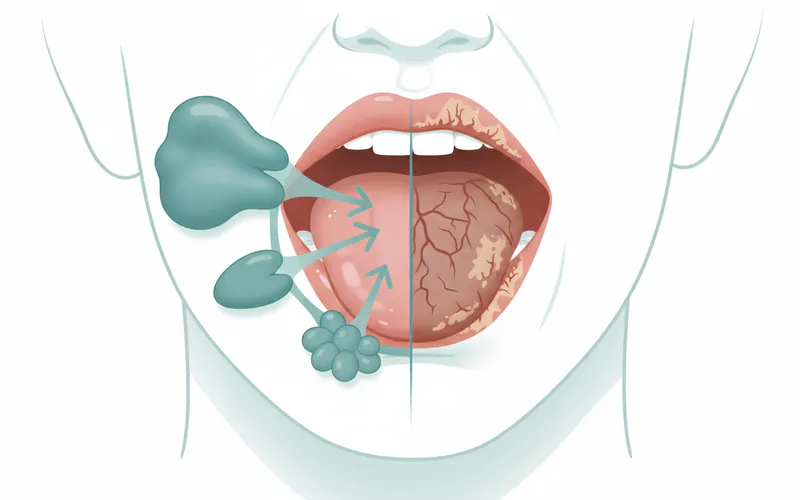
Causes / Why It Happens
The causes of dry mouth are diverse, ranging from simple lifestyle factors to complex medical conditions and treatments. Identifying the specific dry mouth causes is the first critical step toward effective management.
Medications
This is by far the most common cause of dry mouth. Over 500 prescription and over-the-counter (OTC) medications list dry mouth as a potential side effect. Many drugs affect the autonomic nervous system, which controls saliva production, often leading to reduced flow.
Common classes of medications that can cause dry mouth include:
- Antihistamines: Used for allergies (e.g., diphenhydramine, loratadine).
- Decongestants: Used for colds and flu (e.g., pseudoephedrine).
- Antidepressants: Especially tricyclic antidepressants (TCAs) and selective serotonin reuptake inhibitors (SSRIs) (e.g., amitriptyline, fluoxetine).
- Anti-anxiety medications: Benzodiazepines (e.g., lorazepam, alprazolam).
- Antihypertensives (Blood Pressure Medications): Diuretics (e.g., hydrochlorothiazide), beta-blockers, ACE inhibitors.
- Muscle Relaxants: (e.g., cyclobenzaprine).
- Pain Medications: Opioids (e.g., oxycodone, morphine).
- Antiemetics: Used for nausea (e.g., ondansetron).
- Antispasmodics: Used for irritable bowel syndrome (e.g., dicyclomine).
- Bronchodilators: Used for asthma and COPD (e.g., ipratropium).
- Parkinson's Disease Medications: (e.g., levodopa).
- Bladder Control Medications: Anticholinergics (e.g., oxybutynin).
Pro Tip: If you suspect a medication is causing your dry mouth, do not stop taking it without consulting your physician. They may be able to adjust the dosage or switch you to an alternative medication with fewer oral side effects. Always bring a current list of all your medications (prescription and OTC) to your dental appointments.
Medical Conditions
Numerous systemic diseases can directly or indirectly lead to dry mouth:
- Autoimmune Diseases:
- Sjögren's Syndrome: A chronic autoimmune disorder that primarily targets moisture-producing glands, including the salivary and tear glands, leading to severe dry mouth and dry eyes. It affects an estimated 0.5-1% of the US population, predominantly women.
- Rheumatoid Arthritis and Lupus: Other autoimmune conditions that can sometimes affect salivary glands.
- Diabetes: Poorly controlled blood sugar levels can lead to dehydration and affect nerve function, impacting salivary glands. Diabetic neuropathy can also contribute.
- Parkinson's Disease: While some Parkinson's medications cause dry mouth, the disease itself can affect the autonomic nervous system, impacting salivary function.
- Alzheimer's Disease: Patients may have difficulty communicating their symptoms, and cognitive impairment can lead to reduced fluid intake and reliance on medications.
- HIV/AIDS: The virus itself or the medications used to treat it can cause dry mouth.
- Stroke: Can result in nerve damage affecting salivary gland function or muscle weakness that impacts swallowing.
- Anxiety and Depression: Psychological stress can activate the sympathetic nervous system, reducing salivary flow. Medications for these conditions also frequently cause dry mouth.
- Thyroid Disorders: Both hypo- and hyperthyroidism can sometimes be associated with salivary gland dysfunction.
Cancer Therapy
- Radiation Therapy: Particularly when directed at the head and neck region for cancers like oral, throat, or thyroid cancer, radiation can cause irreversible damage to the salivary glands. The severity and permanence depend on the radiation dose and the area treated. This is a very common and often long-term cause of severe dry mouth.
- Chemotherapy: While generally less damaging to salivary glands than radiation, some chemotherapy drugs can cause temporary dry mouth as a side effect.
Lifestyle Factors
Certain habits and choices can contribute to or worsen dry mouth:
- Dehydration: Insufficient fluid intake is a direct cause. This can result from not drinking enough water, excessive sweating, or illness with fever, vomiting, or diarrhea.
- Smoking and Tobacco Use: Tobacco in any form (cigarettes, cigars, chewing tobacco) reduces salivary flow and irritates oral tissues.
- Alcohol Consumption: Alcohol is a diuretic and can lead to dehydration, thereby reducing saliva production.
- Excessive Caffeine Intake: Similar to alcohol, caffeine has diuretic properties.
- Mouth Breathing: Chronic mouth breathing, often due to nasal congestion, allergies, or sleep apnea, allows saliva to evaporate rapidly, leading to dryness, especially at night.
- Recreational Drugs: Methamphetamine and marijuana use are well-known to cause severe dry mouth ("meth mouth" is a severe consequence).
Nerve Damage
Injury or surgery that damages the nerves supplying the salivary glands can impair their function, leading to reduced saliva production.
Aging
While aging itself is not a direct cause of dry mouth, older adults are more susceptible. This is often due to:
- Polypharmacy: Taking multiple medications, increasing the likelihood of dry mouth as a side effect.
- Increased Prevalence of Systemic Diseases: Conditions like diabetes or autoimmune disorders become more common with age.
- Reduced Fluid Intake: Older adults may naturally drink less water due to decreased thirst perception or mobility issues.
Understanding these multifaceted dry mouth causes is essential for you and your healthcare providers to form an effective management strategy.
Signs and Symptoms
Recognizing the signs and symptoms of dry mouth is key to seeking timely intervention. The symptoms can range from mild annoyance to severe discomfort and can significantly impact daily life and oral health.
Common signs and symptoms include:
- A Sticky, Dry Feeling in Your Mouth: The most characteristic symptom, often described as a feeling like cotton in the mouth.
- Frequent Thirst: A constant need to drink water to relieve dryness.
- Sores in the Mouth: Mouth ulcers or canker sores that appear more frequently and heal slowly.
- Cracked Lips and Split Skin at the Corners of Your Mouth: The lack of moisture causes the delicate skin to dry out and crack.
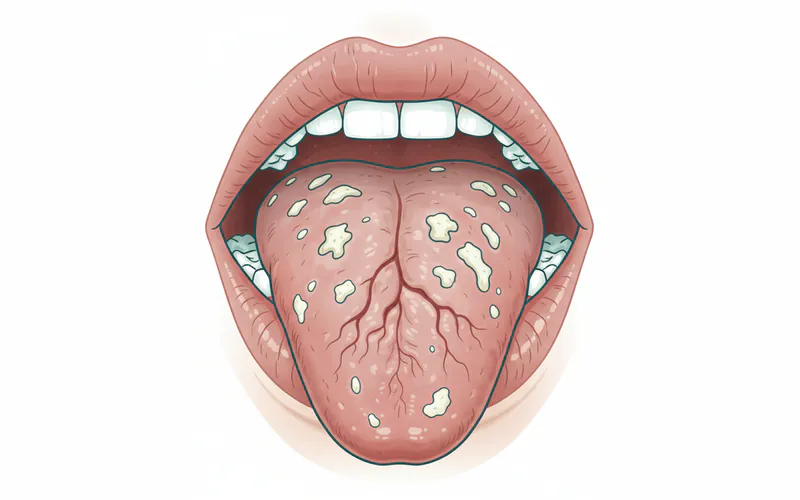
- A Dry or Grooved Tongue: The tongue may appear red, parched, and lose its normal bumpy texture, sometimes looking shriveled or deeply furrowed.
- Difficulty Speaking, Chewing, or Swallowing: Lack of lubrication makes these basic functions challenging and uncomfortable. You might notice food getting stuck or needing water to help chew.
- Persistent Bad Breath (Halitosis): Saliva helps wash away odor-causing bacteria. Without it, bacteria can accumulate, leading to chronic bad breath.
- Altered Sense of Taste: Foods may taste different, or a metallic, bitter, or salty taste may persist.
- Sore Throat or Hoarseness: The throat can become dry and irritated.
- Increased Tooth Decay (Cavities): This is a serious long-term consequence, as saliva's protective buffering and remineralizing properties are lost, making teeth highly vulnerable to acid attacks.
- Gum Inflammation (Gingivitis) and Periodontal Disease: Reduced saliva can exacerbate gum issues.
- Oral Yeast Infections (Candidiasis or Thrush): The antifungal properties of saliva are diminished, allowing yeast to overgrow, appearing as white patches on the tongue and oral tissues.
- Difficulty Wearing Dentures: Dentures may slip, rub, and cause sores due to lack of lubrication and adhesion.
If you experience several of these symptoms persistently, it's a strong indication of dry mouth, and you should consult your dentist or physician to identify the underlying dry mouth causes and discuss treatment options.
Treatment Options
Effective treatment for dry mouth usually involves a multi-pronged approach: addressing the underlying cause, increasing saliva production, and managing symptoms and complications.
A. Addressing the Root Cause (When Possible)
The most effective "treatment" is to eliminate or mitigate the dry mouth causes:
- Medication Review: Consult your physician about your medications. They might be able to:
- Adjust the dosage.
- Change the timing of medication intake.
- Substitute the medication with an alternative that has fewer dry mouth side effects.
- Managing Medical Conditions: If an underlying condition like Sjögren's Syndrome or diabetes is the cause, optimizing its management can sometimes improve salivary flow.
- Lifestyle Modifications:
- Quit Smoking and Tobacco Use: This is one of the most impactful changes.
- Reduce Alcohol and Caffeine Intake: These dehydrating substances should be limited.
- Stay Hydrated: Consistently drink water throughout the day.
- Address Mouth Breathing: If chronic mouth breathing is an issue, consult an ENT (ear, nose, and throat) specialist to treat nasal obstructions or discuss sleep apnea management.
B. Saliva Substitutes and Stimulants
These aim to either replace lost moisture or encourage the body to produce more saliva.
Over-the-Counter (OTC) Solutions:
- Saliva Substitutes: These products are designed to mimic natural saliva and coat the mouth, providing temporary relief. They come in various forms:
- Sprays: Easy to apply throughout the day (e.g., Biotene Dry Mouth Oral Rinse, ACT Total Care Dry Mouth Mouthwash).
- Gels: Provide longer-lasting lubrication, often preferred for nighttime use (e.g., Biotene OralBalance Gel, Oasis Mouth Moisturizing Gel).
- Rinses: Used like regular mouthwashes, but formulated to moisturize (e.g., TheraBreath Dry Mouth Rinse).
- Saliva Stimulants (Sugar-Free): These products encourage your salivary glands to produce more saliva through mechanical or chemical means.
- Xylitol-containing Gums and Mints: Chewing sugar-free gum with xylitol can stimulate saliva flow. Xylitol also helps prevent cavities.
- Sucking on Ice Chips: Provides moisture and stimulates flow.
Prescription Medications:
For more severe cases, a dentist or physician may prescribe medications to stimulate saliva production:
- Pilocarpine (Salagen®): This drug enhances the activity of nerves that stimulate salivary glands. It is taken orally, typically 3-4 times a day.
- Pros: Highly effective for many patients, especially those with Sjögren's syndrome or radiation-induced dry mouth.
- Cons: Can have side effects such as sweating, nausea, diarrhea, increased urination, and blurred vision. Not suitable for everyone, especially those with certain heart or lung conditions.
- Cevimeline (Evoxac®): Similar to pilocarpine, cevimeline is also a cholinergic agonist that stimulates saliva. It is typically taken 3 times a day.
- Pros: May have fewer side effects than pilocarpine for some individuals; effective for Sjögren's syndrome.
- Cons: Similar side effect profile to pilocarpine, including sweating and gastrointestinal issues.
C. Oral Hygiene and Complication Management
Since dry mouth significantly increases the risk of dental problems, aggressive oral hygiene is paramount.
- Fluoride Products:
- High-Fluoride Toothpaste: Your dentist may prescribe a toothpaste with a higher concentration of fluoride than OTC options (e.g., 5000 ppm fluoride).
- Fluoride Rinses: Daily use of a fluoride mouth rinse can help remineralize enamel and prevent cavities.
- Fluoride Varnish or Gel: Applied professionally by your dentist during check-ups.
- Regular Dental Check-ups: More frequent visits (e.g., every 3-4 months instead of 6) are often recommended to monitor for cavities, gum disease, and oral infections.
- Treatment of Oral Infections: If oral candidiasis (thrush) occurs, antifungal medications (topical or systemic) will be prescribed.

Step-by-Step Process: Diagnosing and Managing Dry Mouth
When you seek help for dry mouth, here's generally what you can expect during the diagnostic and initial treatment process:
-
Initial Dental/Medical Consultation:
- Comprehensive History: Your dentist or physician will ask detailed questions about your symptoms (when they started, severity, what makes them better/worse), your medical history, and critically, a complete list of all medications you are currently taking (prescription, OTC, supplements). This is a primary step in identifying dry mouth causes.
- Oral Examination: The dentist will visually inspect your mouth for signs of dryness, such as a dry, fissured tongue, lack of saliva pooling, inflamed gums, cracked lips, and signs of increased tooth decay or oral infections. They might also palpate your salivary glands to check for swelling or tenderness.
-
Salivary Flow Test (Sialometry):
- If dry mouth is suspected, a simple test to measure your salivary flow rate may be performed. You might be asked to spit all your saliva into a measuring cup for a certain period (e.g., 5 or 10 minutes) without stimulation, and then with stimulation (e.g., chewing on paraffin wax or a sugar-free gum).
- A normal unstimulated flow rate is generally 0.3-0.4 mL/minute, while a stimulated rate is 1-2 mL/minute. A rate below 0.1 mL/minute (unstimulated) or 0.7 mL/minute (stimulated) indicates hyposalivation.
-
Further Diagnostic Tests (If Needed):
- If an underlying medical condition like Sjögren's Syndrome is suspected, your physician may order blood tests (e.g., for autoantibodies like ANA, anti-Ro/SSA, anti-La/SSB).
- In rare cases, imaging of the salivary glands (sialography, MRI) or a minor salivary gland biopsy (lip biopsy) may be performed, usually by an oral surgeon or rheumatologist.
-
Identification of Dry Mouth Causes:
- Based on the collected information, the dental or medical professional will identify the most probable dry mouth causes. This might involve linking it to specific medications, diagnosing an underlying medical condition, or attributing it to lifestyle factors.
-
Treatment Planning and Recommendations:
- Medication Adjustment: If medications are the culprit, your physician will discuss options for dosage changes or alternatives.
- Lifestyle Counseling: You'll receive advice on hydration, avoiding dehydrating substances, and proper oral hygiene.
- OTC Product Recommendations: Guidance on effective saliva substitutes, moisturizing rinses, and xylitol products.
- Prescription Medications: For severe cases, a prescription for pilocarpine or cevimeline may be considered.
- Aggressive Fluoride Therapy: Prescription fluoride toothpaste or rinses to prevent cavities.
- Management of Complications: If you have cavities, gum disease, or oral infections, specific treatments for these will be initiated.
-
Follow-up:
- Regular follow-up appointments with your dentist are crucial, often every 3-4 months, to monitor your symptoms, assess the effectiveness of treatments, and check for new complications. Your physician will also monitor any underlying medical conditions.
Cost and Insurance
The costs associated with diagnosing and treating dry mouth can vary depending on the specific dry mouth causes, the severity of the condition, and the chosen treatment methods.
A. Diagnostic Costs:
- Dental Visit/Consultation:
- Without insurance: $50 - $200 (initial exam, not including X-rays or extensive procedures).
- With insurance: Typically covered, with a co-pay of $0 - $50.
- Salivary Flow Test (Sialometry):
- Without insurance: $50 - $150.
- With medical insurance: May be partially covered if considered medically necessary to diagnose an underlying condition. Dental insurance typically does not cover this.
- Blood Tests/Specialist Consults (e.g., Rheumatologist for Sjögren's):
- Without insurance: Varies widely, from $100s to $1000s depending on specific tests and specialist fees.
- With medical insurance: Often covered under medical benefits, subject to deductibles and co-insurance.
B. Treatment and Product Costs:
| Product/Service | Average Cost (Without Insurance, US) | Insurance Coverage | Notes |
|---|---|---|---|
| OTC Saliva Substitutes (Sprays, Gels, Rinses) | $5 - $30 per product/month | None | Can add up over time; try different brands to find what works best. |
| Xylitol Gums/Mints | $5 - $15 per pack/month | None | Also offers cavity prevention benefits. |
| Prescription Pilocarpine / Cevimeline | $30 - $200+ per month | Medical Insurance | Coverage depends on plan; generics are significantly cheaper. |
| High-Fluoride Toothpaste (Prescription) | $15 - $40 per tube | Dental Insurance | May require a prescription, partially covered by some dental plans. |
| Professional Fluoride Varnish/Gel | $25 - $75 per application | Dental Insurance | Usually covered during routine hygiene visits (1-2 times per year). |
| Frequent Dental Cleanings (e.g., 3-4x/year) | $100 - $250 per cleaning | Dental Insurance | Many plans cover 2 cleanings/year; additional ones may be out-of-pocket. |
| Treatment for Complications (Cavities, Gum Disease, Thrush) | Varies widely: $100s - $1000s | Dental/Medical | Fillings ($100-$300), deep cleanings ($200-$500), antifungals ($20-$100). |
| Humidifier | $30 - $150 (one-time) | None | Improves ambient moisture, especially at night. |
C. Insurance Coverage Details:
- Dental Insurance: Primarily covers preventative care (cleanings, fluoride treatments) and restorative procedures (fillings, crowns) if complications like cavities arise. It typically does not cover OTC dry mouth products or prescription medications for salivary stimulation.
- Medical Insurance: Usually covers prescription medications like pilocarpine and cevimeline (especially if a diagnosis like Sjögren's is made), blood tests for underlying conditions, and specialist consultations. Coverage will depend on your plan's formulary, deductible, and co-insurance.
D. Payment Plans and Financing Options:
For more extensive treatments for complications, many dental offices offer:
- In-house payment plans: Spreading the cost over several months.
- Third-party financing: Such as CareCredit, which offers interest-free periods or low monthly payments.
- Dental discount plans: Not insurance, but provides reduced fees for dental services for an annual membership fee.
Pro Tip: Always clarify coverage with your dental and medical insurance providers before starting any expensive treatments or purchasing prescription medications. Ask your dentist for procedure codes (CDT codes) and provide them to your insurer.
Recovery and Aftercare
Managing dry mouth is often an ongoing process, especially if the dry mouth causes are chronic (e.g., medication side effects, autoimmune disease, radiation damage). Consistent aftercare and adherence to recommended strategies are crucial for maintaining oral health and quality of life.
-
Maintain Consistent Oral Hygiene:
- Brush at least twice a day with a fluoride toothpaste, ideally a prescription-strength one if recommended.
- Floss daily to remove plaque and food debris between teeth.
- Use an alcohol-free mouthwash that is specifically formulated for dry mouth or contains fluoride. Avoid regular mouthwashes with alcohol, as they can further dry and irritate the mouth.
- Pro Tip: Consider using an electric toothbrush for more effective plaque removal, which is even more critical with reduced saliva.
-
Regular Dental Check-ups and Cleanings:
- Due to the increased risk of cavities and gum disease, your dentist may recommend more frequent visits, perhaps every 3-4 months, instead of the standard six. These visits allow for early detection and intervention for any developing complications.
- Professional fluoride applications (varnishes or gels) at these appointments can provide extra protection.
-
Stay Hydrated Throughout the Day:
- Sip water frequently, even small sips, to keep your mouth moist. Keep a water bottle handy.
- Consider drinking water with meals to aid in chewing and swallowing.
-
Continue Using Saliva Substitutes/Stimulants:
- If OTC products or prescription medications are providing relief, continue using them as directed. It may take some experimentation to find the specific products and routines that work best for you.
-
Dietary Modifications:
- Avoid or limit dry, crunchy, sugary, acidic, and spicy foods, as these can exacerbate symptoms or contribute to tooth decay.
- Choose soft, moist foods.
- Chew sugar-free gum or suck on sugar-free candies (preferably with xylitol) to stimulate saliva.
-
Avoid Dehydrating Substances:
- Minimize or eliminate alcohol, caffeine, and tobacco products.
- If using mouthwashes, ensure they are alcohol-free.
-
Use a Room Humidifier:
- Especially at night, a humidifier in your bedroom can add moisture to the air, preventing your mouth from drying out further while you sleep.
-
Monitor for Complications:
- Be vigilant for signs of new cavities, gum inflammation, or oral candidiasis (white patches, soreness). Report these to your dentist immediately.
-
Communicate with Your Healthcare Team:
- Keep both your dentist and physician informed about your dry mouth symptoms, especially if there are changes in your medications or medical conditions. They are partners in managing your oral and overall health.
Prevention
While not all dry mouth causes are preventable (e.g., certain medical conditions or cancer therapy), many instances of dry mouth, or its severity, can be reduced or prevented through proactive measures.
-
Stay Adequately Hydrated:
- The simplest and most fundamental step. Drink water regularly throughout the day, even if you don't feel thirsty. Aim for at least 8 glasses (64 ounces) daily, more if you are physically active or in a hot climate.
- Pro Tip: Carry a reusable water bottle as a constant reminder to sip throughout the day.
-
Review Medications with Your Doctor:
- If you are starting a new medication or experiencing dry mouth, discuss it with your physician. They may be able to prescribe an alternative, adjust the dosage, or suggest strategies to mitigate the side effect. This is particularly important for polypharmacy (taking multiple medications).
-
Avoid Dehydrating Substances:
- Tobacco: Smoking and using smokeless tobacco products significantly reduce salivary flow and should be avoided entirely.
- Alcohol: Limit alcohol consumption, as it has a diuretic effect and can dehydrate you.
- Caffeine: While a morning cup of coffee is generally fine, excessive caffeine intake can contribute to dehydration.
- Alcohol-based Mouthwashes: Choose alcohol-free mouth rinses to prevent further drying and irritation of oral tissues.
-
Breathe Through Your Nose:
- Chronic mouth breathing, especially during sleep, causes saliva to evaporate quickly. If you frequently breathe through your mouth due to allergies, nasal congestion, or sleep apnea, consult an ENT specialist to address the underlying issue. Using nasal strips can sometimes help.
-
Practice Excellent Oral Hygiene:
- Regular and thorough brushing and flossing are essential to protect your teeth and gums from the increased risk of decay and gum disease that accompanies reduced saliva. Use fluoride toothpaste.
-
Regular Dental Check-ups:
- Consistent visits to your dentist (at least twice a year, or more frequently if recommended) allow for early detection of dry mouth or its complications. Your dentist can provide preventive fluoride treatments and advice.
-
Humidify Your Environment:
- Using a humidifier, especially in your bedroom at night, can help keep the air moist, reducing evaporation of oral moisture while you sleep.
-
Chew Sugar-Free Gum or Suck on Sugar-Free Candies with Xylitol:
- These mechanically stimulate saliva flow and the xylitol helps prevent cavities.
By taking these proactive steps, you can often prevent the onset or reduce the severity of dry mouth, thereby safeguarding your oral health.
Risks and Complications
The implications of persistent dry mouth extend far beyond discomfort. The absence of adequate saliva significantly compromises the mouth's natural defenses, leading to a range of serious oral and sometimes systemic complications. Understanding these risks underscores the importance of addressing the dry mouth causes promptly.
-
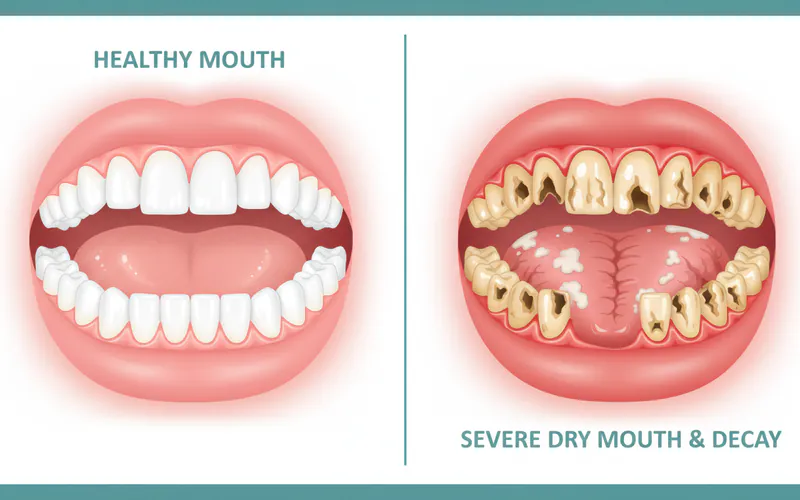
Rampant Tooth Decay (Dental Caries): This is perhaps the most significant and common complication. Saliva's buffering, cleansing, and remineralizing actions are crucial for protecting enamel. Without them:
- Acids from food and bacteria remain in contact with teeth longer.
- Food debris and plaque build up more quickly.
- The enamel loses its ability to repair itself.
- This often results in widespread, rapid decay, particularly at the gumline and on root surfaces if exposed.
-
Periodontal (Gum) Disease: Reduced saliva can exacerbate plaque accumulation, leading to gingivitis (gum inflammation) and, if untreated, progressing to periodontitis, which involves bone loss around the teeth.
-
Oral Infections:
- Oral Candidiasis (Thrush): The antifungal properties of saliva are diminished, allowing the Candida albicans fungus to overgrow. This appears as white, creamy patches on the tongue and inner cheeks, often accompanied by soreness and altered taste.
- Bacterial Infections: The mouth becomes a less hospitable environment, but opportunistic bacteria can still thrive without the cleansing action of saliva.
-
Difficulty Eating, Speaking, and Swallowing (Dysphagia):
- Chewing and swallowing become painful and challenging without lubrication, potentially leading to choking or aspiration.
- Speaking can become difficult, with the tongue sticking to the palate, resulting in slurred speech or hoarseness.
- This can significantly impact social interactions and quality of life.
-
Malnutrition:
- Difficulty chewing and swallowing may lead individuals to avoid certain foods (e.g., dry, fibrous meats, fresh fruits and vegetables), potentially leading to an unbalanced diet and nutritional deficiencies.
-
Denture Problems:
- For denture wearers, dry mouth causes dentures to lose their suction, leading to slippage, irritation, and the development of sores or ulcers under the dentures.
-
Persistent Bad Breath (Halitosis):
- Lack of saliva means bacteria and food particles are not adequately washed away, leading to a constant foul odor.
-
Compromised Quality of Life:
- The constant discomfort, pain, and challenges with daily activities like eating and speaking can lead to emotional distress, anxiety, and social isolation.
Addressing dry mouth isn't just about comfort; it's a vital step in preventing these severe and often irreversible complications.
Comparison Tables
Here are two comparison tables to help illustrate key aspects of dry mouth management and its common causes.
Table 1: Common Dry Mouth Remedies: OTC vs. Prescription
| Feature | OTC Saliva Substitutes/Stimulants (e.g., Gels, Sprays, Xylitol Gums) | Prescription Saliva Stimulants (e.g., Pilocarpine, Cevimeline) |
|---|---|---|
| Mechanism | Physically moisten mouth; mechanically or chemically stimulate residual salivary glands. | Systemically stimulate salivary glands via neurotransmitter pathways. |
| Effectiveness | Temporary relief for mild-to-moderate dry mouth; requires frequent reapplication. | More profound and sustained increase in saliva flow for moderate-to-severe cases. |
| Availability | Widely available without a prescription at pharmacies and supermarkets. | Requires a prescription from a dentist or physician. |
| Cost (Monthly, US) | $5 - $30 (can vary based on brand/type). | $30 - $200+ (generics cheaper; medical insurance may cover). |
| Pros | No systemic side effects; convenient; some (xylitol) prevent cavities. | Can significantly improve salivary flow; effective for chronic, severe dry mouth. |
| Cons | Temporary relief; can be costly over time; doesn't address underlying cause. | Potential for systemic side effects (sweating, nausea, etc.); not suitable for all patients. |
| Best For | Mild dryness, temporary relief, adjunct to other treatments. | Chronic, moderate-to-severe dry mouth, especially due to Sjögren's or radiation. |
Table 2: Major Categories of Dry Mouth Causes
| Cause Category | Typical Impact on Saliva | Examples of Specific Causes | Management Approach |
|---|---|---|---|
| Medication Side Effects | Mild to Severe | Antihistamines, Antidepressants, Diuretics, Opioids | Physician consultation for dosage adjustment or alternative. |
| Medical Conditions | Moderate to Severe, often Chronic | Sjögren's Syndrome, Diabetes, Parkinson's, HIV/AIDS | Medical management of the underlying disease; specialist care. |
| Cancer Therapy | Often Severe and Permanent | Radiation to head/neck, certain Chemotherapy agents | Symptomatic relief, aggressive preventive dental care. |
| Lifestyle Factors | Mild to Moderate | Dehydration, Smoking, Alcohol, Mouth Breathing, Caffeine | Behavioral changes, hydration, oral care. |
| Nerve Damage | Localized or Generalised | Trauma, surgery affecting salivary gland nerves | Symptomatic relief; may require long-term management. |
Children / Pediatric Considerations
Dry mouth in children is less common than in adults, but it can occur and should not be overlooked, as its consequences can be severe for developing dentition. Identifying dry mouth causes in children requires careful attention.
Causes in Children:
- Medications: Children on certain medications, particularly antihistamines, decongestants, some antidepressants, or ADHD medications, can experience dry mouth.
- Medical Conditions:
- Diabetes: Poorly controlled diabetes can lead to dehydration and dry mouth in children.
- Cystic Fibrosis: While primarily affecting the lungs and digestive system, it can impact salivary gland function.
- Sjögren's Syndrome: Although rare in children, juvenile Sjögren's can occur.
- Other Autoimmune Diseases: Lupus or juvenile rheumatoid arthritis.
- Mouth Breathing: Chronic mouth breathing due to enlarged tonsils/adenoids, allergies, or nasal obstruction can lead to dry mouth, especially at night. This also often contributes to orthodontic issues.
- Dehydration: Children, especially infants and toddlers, are more susceptible to dehydration during illness (fever, vomiting, diarrhea) or intense physical activity.
- Salivary Gland Disorders: Rare congenital conditions or infections (like mumps) affecting salivary glands.
Signs and Symptoms in Children: Detecting dry mouth in children can be challenging, as they may not articulate their discomfort clearly. Look for:
- Frequent thirst or asking for water often.
- Difficulty eating dry foods (crackers, cereals).
- Reluctance to eat due to discomfort.
- A dry, red, or fissured tongue.
- Cracked lips or sores around the mouth.
- Frequent bad breath.
- Unexplained increase in cavities, especially smooth surface cavities or those near the gumline.
- Oral candidiasis (thrush).
Pediatric Management:
- Pediatric Dentist Consultation: Essential for diagnosis and management. A pediatric dentist is experienced in identifying and treating dry mouth in young patients.
- Identify and Address Cause: The first step is to work with the child's pediatrician to identify and address the underlying dry mouth causes, such as adjusting medications or treating medical conditions.
- Hydration: Encourage frequent sips of water throughout the day.
- Oral Hygiene: Emphasize meticulous brushing and flossing. A pediatric dentist may recommend prescription-strength fluoride toothpaste or fluoride varnish applications.
- Xylitol: Sugar-free xylitol gums or lollipops (age-appropriate) can help stimulate saliva and prevent cavities.
- Humidifier: Use a humidifier in the child's bedroom at night.
- Avoid Sugary/Acidic Foods: Limit sugary snacks and drinks, as they drastically increase cavity risk with dry mouth.
- Saliva Substitutes: OTC saliva substitute sprays or gels can be used, but ensure they are age-appropriate and palatable for children. Discuss with the pediatric dentist.
Early intervention is critical in children to prevent extensive and rapid tooth decay, which can severely impact their oral health and development.
Frequently Asked Questions
What are the main dry mouth causes?
The primary dry mouth causes include side effects from over 500 medications (such as antihistamines, antidepressants, and blood pressure drugs), various medical conditions like Sjögren's Syndrome and diabetes, and cancer therapies, particularly radiation to the head and neck. Lifestyle factors like dehydration, smoking, and mouth breathing also contribute significantly.
Can dry mouth be cured permanently?
Whether dry mouth can be cured depends entirely on its underlying cause. If it's due to temporary dehydration or a reversible medication side effect, it can resolve. However, if the cause is a chronic medical condition (like Sjögren's Syndrome) or permanent damage from radiation, the dry mouth itself may not be "cured" but can be effectively managed with ongoing treatment and lifestyle adjustments.
What are the best home remedies for dry mouth relief?
Effective home remedies include sipping water frequently throughout the day, chewing sugar-free gum or sucking on sugar-free candies (especially those with xylitol) to stimulate saliva, using a humidifier in your bedroom at night, and avoiding dehydrating substances like caffeine, alcohol, and tobacco. Over-the-counter saliva substitutes (sprays, gels, rinses) can also provide temporary relief.
How long does it take for dry mouth to go away?
The duration of dry mouth varies widely. If it's an acute issue (e.g., temporary dehydration or a short-term medication), relief can be immediate or within a few days of addressing the cause. For chronic conditions, dry mouth may persist indefinitely, requiring continuous management to mitigate symptoms and prevent complications.
Is dry mouth a serious condition?
Yes, persistent dry mouth is a serious condition beyond just discomfort. It significantly increases the risk of rampant tooth decay, gum disease, and oral infections like candidiasis. It can also cause difficulty eating, speaking, and swallowing, leading to nutritional deficiencies and a reduced quality of life. Prompt diagnosis and management are crucial to prevent these complications.
What over-the-counter products are recommended for dry mouth?
Several OTC products can help. Look for saliva substitutes in spray, gel, or rinse form (e.g., Biotene, Oasis, ACT Dry Mouth). Sugar-free chewing gum and lozenges, particularly those containing xylitol, are also highly recommended for stimulating saliva and preventing cavities. Ensure all products are alcohol-free.
Does anxiety cause dry mouth?
Yes, anxiety can cause dry mouth. When you're anxious, your body activates the "fight or flight" response, which redirects blood flow away from non-essential functions like saliva production. Additionally, many anti-anxiety medications list dry mouth as a common side effect, creating a dual impact.
Can certain foods cause dry mouth?
While foods don't directly "cause" dry mouth in the way medications or diseases do, certain foods can exacerbate the feeling or contribute to dehydration. Very dry, salty, spicy, or acidic foods can irritate an already dry mouth. High-sugar foods, when combined with reduced saliva, drastically increase the risk of tooth decay.
How does dry mouth affect dental health?
Dry mouth severely compromises dental health by eliminating saliva's protective functions. This leads to a rapid increase in cavities (especially at the gumline), progression of gum disease, and higher susceptibility to oral infections like thrush. It also makes chewing, swallowing, and speaking difficult, impacting overall oral function and comfort.
Is there a link between dry mouth and other oral conditions like cold sores?
While dry mouth doesn't directly cause cold sores, it can indirectly contribute to their frequency or severity. A constantly dry oral environment is a sign of compromised oral health and immune function in the mouth. When the oral environment is stressed or imbalanced, it can make an individual more susceptible to various oral infections, including flare-ups of conditions like cold sores (herpes labialis) if the virus is already present. However, dry mouth is not a primary cause of cold sores; it's more about creating a less resilient oral tissue environment. (Regarding the keyword "what kills cold sores instantly," it's important to note that no product "instantly kills" cold sores, but antiviral medications can shorten their duration and severity).
When to See a Dentist
Recognizing when dry mouth is more than just a temporary nuisance and requires professional attention is crucial for your oral and overall health. Don't delay seeking help if you experience the following:
- Persistent Dryness: If your dry mouth symptoms last for more than a few days or weeks, despite trying home remedies like drinking more water, it's time to see a dentist.
- Difficulty with Daily Activities: If dry mouth significantly impacts your ability to chew, swallow, speak, or wear dentures comfortably.
- New or Worsening Symptoms: Any significant change in the severity of your dry mouth, or the appearance of new symptoms like a burning sensation, altered taste, or persistent bad breath.
- Signs of Oral Complications: This is a red flag. If you notice an unusual increase in cavities, bleeding gums, recurrent mouth sores, or white patches on your tongue or inside your cheeks (which could indicate oral candidiasis/thrush), seek immediate dental attention.
- Medication-Related Concerns: If you believe your dry mouth is a side effect of a medication, consult your physician (who may also advise you to see a dentist for symptom management). Never stop taking prescribed medication without your doctor's guidance.
- Unexplained Dry Mouth: If you cannot identify an obvious cause for your dry mouth, a dentist can help diagnose the underlying issue and rule out more serious medical conditions.
Your dentist can accurately diagnose the specific dry mouth causes, assess its impact on your oral health, and develop a comprehensive treatment plan to alleviate your symptoms and prevent serious complications. Regular dental check-ups are always your first line of defense against oral health issues.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles

Oral Candidiasis Symptoms: Complete Guide
Oral candidiasis, commonly known as oral thrush, is a fungal infection of the mouth caused by an overgrowth of Candida yeast, most often Candida albicans. While Candida is a normal inhabitant of the human mouth in small amounts, an imbalance can lead to uncomfortable and sometimes painful symptoms
February 23, 2026
Are Cold Sores Contagious
In the United States, an estimated 67% of the population under age 50 carries the herpes simplex virus type 1 (HSV-1), the primary cause of cold sores. This means millions of Americans are susceptible to these often painful and highly visible oral lesions. Beyond the discomfort and cosmetic conc
February 23, 2026
How Long Does Hand Foot and Mouth Last
Hand, Foot, and Mouth Disease (HFMD) is a common, often uncomfortable, viral illness that can affect anyone but is particularly prevalent among young children. If you or a loved one has ever experienced the tell-tale rash or painful mouth sores, you've likely wondered: **how long does Hand Foot and
February 23, 2026
Cold Sore vs Pimple on Lip: Complete Comparison Guide
When you notice an unexpected bump or lesion on your lip, your mind might immediately jump to questions of what it is, how long it will last, and most importantly, if it's contagious. The confusion between a cold sore vs pimple on lip is incredibly common, yet the distinction is crucial for prop
February 23, 2026