Halitosis Treatments: Complete Guide

Key Takeaways
- Halitosis Treatments: Complete Guide
Halitosis Treatments: Complete Guide
Bad breath, medically known as halitosis, is more than just a momentary embarrassment; it's a common condition affecting an estimated 25-50% of adults globally, with a significant portion experiencing chronic bad breath. In the United States alone, millions seek solutions for this persistent issue, making halitosis treatments a crucial topic for dental health. While often perceived as merely a social stigma, chronic bad breath can signal underlying oral or systemic health problems that require professional attention. Ignoring halitosis can impact your self-confidence, personal relationships, and overall well-being. This comprehensive guide will explore the various causes, effective treatments, preventative strategies, and financial considerations for managing and eliminating bad breath, helping you understand why this topic matters to your health and how you can achieve lasting fresh breath. We’ll delve into everything from daily hygiene improvements to advanced dental interventions, ensuring you have all the information needed to tackle halitosis head-on.
Key Takeaways:
- Primary Cause: Approximately 90% of halitosis cases originate in the mouth, primarily due to volatile sulfur compounds (VSCs) produced by bacteria.
- Initial Treatment: The first line of defense often involves optimizing oral hygiene, including thorough brushing, daily flossing, and tongue scraping, which can improve breath by up to 80-90% for many.
- Professional Care Costs: A dental check-up and professional cleaning typically range from $75 to $200 without insurance, while deep cleaning (scaling and root planing) can cost $200-$500 per quadrant.
- Duration of Treatment: Addressing oral causes usually shows improvement within 1-4 weeks of consistent hygiene and professional intervention. Systemic causes may require longer, ongoing medical management.
- Early Intervention: Persistent bad breath warrants a dental visit, as it can be a sign of underlying issues like gum disease, tooth decay, or even systemic health conditions.
- Comprehensive Approach: Effective treatment often combines meticulous home care, professional dental treatments, and, if necessary, medical assessment for non-oral causes.
- Prevention is Key: Regular dental check-ups (every 6 months) and a robust daily oral hygiene routine are your best tools for long-term halitosis prevention.
What Halitosis Is: An Overview
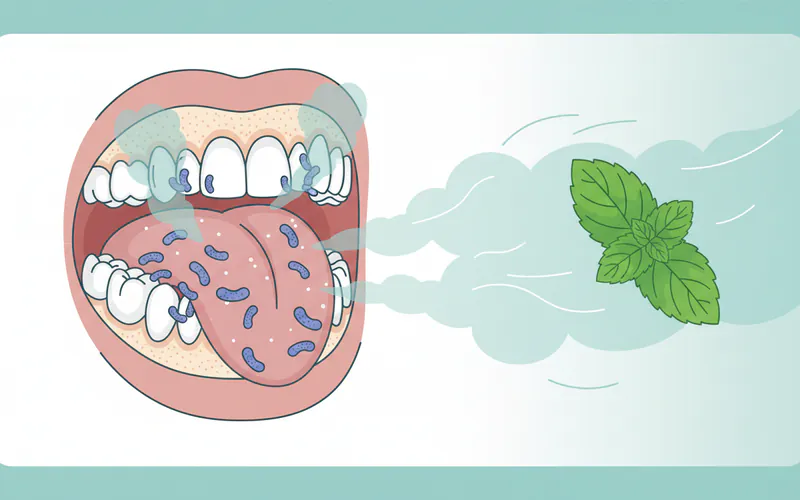
Halitosis, commonly known as bad breath, is the term used to describe an unpleasant odor emanating from the mouth. While transient bad breath can occur after consuming certain foods like garlic or onions, chronic halitosis is a persistent problem that does not resolve with routine brushing or mouthwash. It's not just a social concern; it's a medical condition that often indicates an underlying oral health issue or, less commonly, a systemic health problem.

The primary culprit behind most cases of halitosis is the production of volatile sulfur compounds (VSCs) by anaerobic bacteria residing in the mouth, particularly on the back of the tongue, between teeth, and in periodontal pockets. These VSCs, such as hydrogen sulfide, methyl mercaptan, and dimethyl sulfide, are responsible for the characteristic unpleasant odor associated with bad breath. Understanding the nature of halitosis is the first step toward effective halitosis treatments.
Types of Halitosis
Halitosis can be categorized based on its origin and persistence:
Oral (Intra-oral) Halitosis
This is the most common type, accounting for approximately 90% of all cases. It originates directly from the mouth due to bacteria breaking down food particles, dead cells, and other debris.
- Physiological Halitosis: Often referred to as "morning breath," this type is temporary and caused by reduced salivary flow during sleep, allowing bacteria to multiply and produce VSCs. It usually resolves after eating and oral hygiene.
- Pathological Halitosis: This indicates an underlying oral health problem.
- Oral Conditions: This includes periodontal (gum) disease, extensive tooth decay (caries), oral infections (abscesses), dry mouth (xerostomia), oral candidiasis (thrush), and impacted food particles around fillings or wisdom teeth.
- Tongue Coating: A significant bacterial reservoir, especially on the posterior dorsum of the tongue, contributes heavily to VSC production.
- Tonsil Stones (Tonsilloliths): Small, calcified deposits that form in the crypts of the tonsils, trapping bacteria and debris, releasing foul odors.
Extra-oral (Systemic) Halitosis
Less common, this type originates from outside the mouth, indicating an underlying medical condition.
- Blood-borne Halitosis: Occurs when odorous compounds are carried by the bloodstream to the lungs and exhaled.
- Respiratory Tract Infections: Sinusitis, bronchitis, pneumonia, post-nasal drip.
- Gastrointestinal Issues: Gastroesophageal reflux disease (GERD), hiatal hernia, H. pylori infection.
- Metabolic Conditions: Diabetes (ketoacidosis produces a fruity odor), liver failure (fishy odor), kidney failure (ammonia-like odor).
- Other Conditions: Certain cancers, autoimmune disorders like Sjögren's syndrome (causing dry mouth).
Halitophobia (Pseudohalitosis and Delusional Halitosis)
This is a psychological condition where an individual believes they have bad breath, even when objective clinical examination and tests reveal no such odor. It can stem from past experiences or heightened self-consciousness. In cases of delusional halitosis, the belief is firmly held despite strong evidence to the contrary, often requiring psychological intervention.
Halitosis Causes: Why It Happens
Understanding the root causes of bad breath is paramount to effective halitosis treatments. As mentioned, most cases originate in the mouth.
Primary Oral Causes (Approximately 90% of cases)
- Bacterial Activity on the Tongue: The rough surface of the back of the tongue provides an ideal environment for anaerobic bacteria to thrive, especially when saliva flow is reduced. These bacteria break down proteins from food debris, dead cells, and post-nasal drip, releasing foul-smelling VSCs. This is often the single biggest contributor to chronic bad breath.
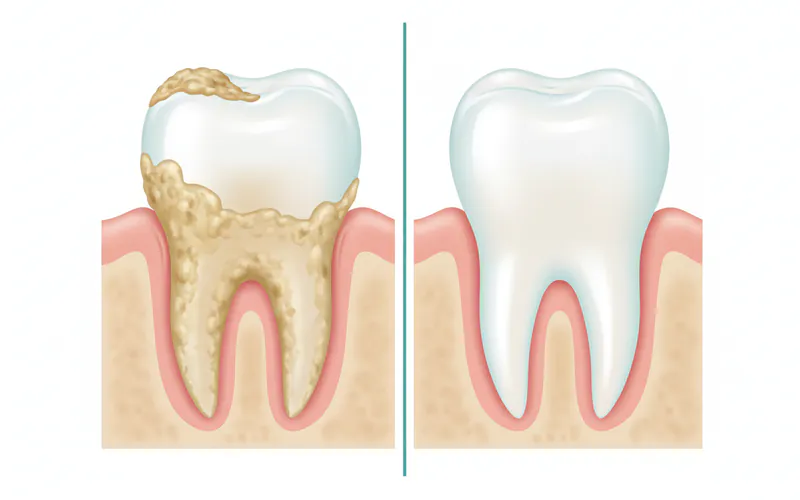
- Periodontal Disease (Gum Disease): Gingivitis (inflammation of the gums) and periodontitis (a more severe infection affecting the bone supporting the teeth) create deep pockets around the teeth where anaerobic bacteria can accumulate and proliferate. These bacteria release VSCs and other compounds that cause persistent bad breath, often accompanied by bleeding gums. The American Dental Association (ADA) emphasizes that healthy gums are essential for overall oral health and fresh breath.
- Dental Caries (Tooth Decay) and Oral Infections: Cavities provide protected spaces for bacteria to multiply, trapping food particles and dead cells. Abscesses, tooth infections, or even poorly fitting dental restorations can also harbor bacteria and contribute to odor.
- Dry Mouth (Xerostomia): Saliva plays a crucial role in cleansing the mouth, washing away food particles and bacteria. Reduced saliva flow (xerostomia) allows bacteria to accumulate, leading to increased VSC production. Causes of dry mouth include:
- Medications: Over 400 common medications, including antihistamines, decongestants, antidepressants, and diuretics, can cause dry mouth as a side effect.
- Systemic Diseases: Sjögren's syndrome, diabetes, and certain autoimmune conditions.
- Lifestyle Factors: Mouth breathing, smoking, and alcohol consumption.
- Radiation Therapy: Particularly for head and neck cancers.
- Food and Drink: Certain foods and beverages, such as garlic, onions, strong spices, coffee, and alcohol, contain volatile compounds that are absorbed into the bloodstream and exhaled through the lungs, creating temporary bad breath. While temporary, chronic consumption can contribute to a persistent issue.
- Tobacco Products: Smoking and chewing tobacco cause a distinct, unpleasant odor. They also contribute to dry mouth, increase the risk of gum disease, and stain teeth, all of which worsen halitosis.
- Tonsil Stones (Tonsilloliths): These are small, whitish-yellow formations that can develop in the crevices of the tonsils. They are composed of calcified bacteria, food debris, and dead cells. As they grow, they can release extremely foul-smelling odors.
- Poor Oral Hygiene: Infrequent or ineffective brushing and flossing allow food particles to remain in the mouth, feeding bacteria and leading to plaque buildup. This is a foundational cause that often compounds other oral issues.
Secondary Extra-oral (Systemic) Causes (Approximately 10% of cases)
- Respiratory Tract Conditions:
- Sinusitis and Post-Nasal Drip: Mucus from the nasal passages can drip down the back of the throat, providing a food source for bacteria, leading to a foul odor.
- Bronchitis, Pneumonia, Lung Abscesses: Infections in the lower respiratory tract can produce odorous compounds that are exhaled.
- Gastrointestinal (GI) Conditions:
- Gastroesophageal Reflux Disease (GERD): Stomach acids and undigested food can reflux into the esophagus and mouth, causing a sour taste and unpleasant breath.
- Helicobacter pylori (H. pylori) Infection: This bacterium, known to cause stomach ulcers, has also been linked to halitosis in some individuals.
- Hiatal Hernia: Can contribute to acid reflux.
- Metabolic Diseases:
- Diabetes (Diabetic Ketoacidosis): Uncontrolled diabetes can lead to ketoacidosis, producing ketones that give the breath a distinctive sweet, fruity, or acetone-like smell.
- Liver Disease: Severe liver failure can result in "fetor hepaticus," a distinct musty, fishy, or sweet odor.
- Kidney Disease: Chronic kidney failure can cause an ammonia-like or urine-like smell on the breath due to the buildup of waste products.
- Certain Medications: Beyond causing dry mouth, some medications, when broken down by the body, can release chemicals that are exhaled. Examples include nitrates, chemotherapy drugs, and tranquilizers.
- Dietary Factors (Systemic): Low-carbohydrate or ketogenic diets, during which the body burns fat for fuel, can produce ketones that result in "keto breath," a distinctive fruity or metallic odor. Fasting can also produce similar effects.
Understanding these diverse causes is crucial for dentists and medical professionals to accurately diagnose and recommend the most effective halitosis treatments.
Signs and Symptoms of Halitosis
While the most obvious symptom is an unpleasant mouth odor, other signs can accompany halitosis, signaling a need for attention:
- Bad Taste in the Mouth: A persistent sour, metallic, or generally unpleasant taste, even after brushing.
- Dry Mouth: A feeling of stickiness or dryness, often due to reduced saliva flow.
- White Coating on the Tongue: Particularly noticeable on the back of the tongue. This coating is often a prime habitat for odor-producing bacteria.
- Red, Swollen, or Bleeding Gums: Signs of gingivitis or periodontitis, a common source of bad breath.
- Loose Teeth or Pus Around Gums: Advanced signs of periodontal disease.
- Difficulty Swallowing: Can be related to tonsil stones or other throat issues.
- Throat Soreness or Post-Nasal Drip: Often linked to sinus issues or respiratory infections contributing to bad breath.
- Self-Consciousness: Many individuals become highly aware of their breath and may constantly chew gum, use mints, or cover their mouth when speaking.
How to Check Your Own Breath: You can often detect your own bad breath by licking your wrist, letting it dry for a few seconds, and then smelling it. Another method is to gently scrape the back of your tongue with a clean spoon, let the residue dry, and then smell it. While helpful, these methods aren't always definitive, as smell perception can be subjective. A trusted friend or family member can offer a more objective assessment. For a definitive diagnosis, a dental professional uses specific tests.
Halitosis Treatments: All Available Options
Effective halitosis treatments are multifaceted and tailored to the underlying cause. A comprehensive approach typically begins with identifying the source of the odor.
1. Oral Hygiene Improvements (First Line of Defense)
For the vast majority of cases stemming from oral causes, meticulous oral hygiene is the cornerstone of treatment.
- Brushing: Brush your teeth at least twice a day for two minutes, using a fluoride toothpaste. Pay attention to all tooth surfaces, including the gum line. An electric toothbrush can often be more effective at plaque removal.
- Pros: Inexpensive, easily accessible, foundational to oral health.
- Cons: Can miss areas if not thorough, doesn't address all causes.
- Flossing: Floss daily to remove food particles and plaque from between teeth and under the gum line, where toothbrushes can't reach. This is critical for preventing gum disease and removing odor-causing bacteria.
- Pros: Essential for interdental cleaning, prevents gum disease.
- Cons: Can be challenging for some, requires consistency.
- Tongue Scraping/Brushing: This is perhaps one of the most effective immediate solutions for tongue-related halitosis. Use a tongue scraper or the back of your toothbrush to gently scrape the white coating from your tongue from back to front.
- Pros: Highly effective at removing VSC-producing bacteria from the tongue, provides immediate improvement.
- Cons: Can trigger gag reflex for some, needs to be done daily. Pro Tip: Incorporate tongue scraping into your daily routine; studies show it can reduce VSCs by up to 75%.
- Antimicrobial Mouthwashes:
- Chlorine Dioxide Mouthwashes: Neutralize VSCs rather than just masking the odor. They contain oxygenating agents that help eliminate anaerobic bacteria.
- Pros: Directly addresses VSCs, non-staining.
- Cons: Some brands might have a specific taste.
- Zinc-based Mouthwashes: Zinc ions bind with sulfur compounds, converting them into non-volatile, odorless salts.
- Pros: Effective at neutralizing VSCs, helps prevent their formation.
- Cons: Can sometimes leave a metallic taste.
- Cetylpyridinium Chloride (CPC) Mouthwashes: Antiseptic agents that kill bacteria, often found in over-the-counter mouthwashes.
- Pros: Reduces bacterial load.
- Cons: Less effective on established VSCs, can be drying for some.
- Essential Oil Mouthwashes (e.g., Listerine): Contain ingredients like eucalyptol, menthol, and thymol, which have antiseptic properties.
- Pros: Kills bacteria, provides fresh feeling.
- Cons: Can contain alcohol, which can be drying and worsen dry mouth in the long run. The ADA recommends alcohol-free mouthwashes for daily use.
- Pros: Can provide temporary relief and reduce bacterial load.
- Cons: Many only mask odor; alcohol-based varieties can cause dry mouth, which exacerbates halitosis. Choose alcohol-free, ADA-accepted therapeutic mouthwashes.
- Chlorine Dioxide Mouthwashes: Neutralize VSCs rather than just masking the odor. They contain oxygenating agents that help eliminate anaerobic bacteria.
2. Professional Dental Treatments
If home care is insufficient, a visit to the dentist is crucial.
- Professional Dental Cleanings: Regular cleanings (prophylaxis) remove plaque and tartar buildup, especially below the gum line, which can harbor odor-causing bacteria.
- Pros: Essential for removing hardened plaque (calculus) that brushing can't remove, prevents gum disease.
- Cons: Not a one-time fix, requires regular appointments.
- Treatment of Periodontal Disease: For gingivitis or periodontitis, treatments include:
- Scaling and Root Planing (Deep Cleaning): A non-surgical procedure to remove plaque and tartar from below the gum line and smooth the tooth roots, helping gums reattach to teeth.
- Antibiotics: Oral or topical antibiotics may be prescribed to control bacterial infection.
- Laser Therapy: Can be used in conjunction with scaling and root planing to remove infected tissue and reduce bacteria.
- Periodontal Surgery: In advanced cases, surgery may be needed to reduce pocket depths and regenerate lost tissue.
- Pros: Addresses the root cause of gum-related halitosis, prevents tooth loss.
- Cons: Can be invasive, involves recovery time, costs more.
- Restorative Dentistry:
- Filling Cavities: Removing decay and filling cavities eliminates bacterial havens.
- Replacing Faulty Restorations: Old, cracked, or ill-fitting fillings and crowns can trap food and bacteria.
- Treating Abscesses: Draining infections and root canal therapy if needed.
- Pros: Eliminates sources of infection and bacterial accumulation.
- Cons: Varies by procedure, can be costly.
- Tonsil Stone Removal: Dentists can manually remove visible tonsil stones. For recurrent stones, a referral to an ENT specialist for potential laser cryptolysis or tonsillectomy might be considered.
- Pros: Immediate relief from associated odor.
- Cons: May recur, surgical options are more invasive.
3. Addressing Dry Mouth (Xerostomia)
- Saliva Substitutes/Stimulants: Over-the-counter gels, sprays, and lozenges can help moisten the mouth. Prescription medications like pilocarpine or cevimeline can stimulate saliva production for chronic dry mouth.
- Pros: Provides relief, reduces bacterial growth.
- Cons: Temporary, requires consistent use, prescription options have side effects.
- Hydration: Drinking plenty of water throughout the day is crucial.
- Avoid Irritants: Reduce or eliminate caffeine, alcohol, and tobacco.
- Humidifiers: Using a humidifier at night can help, especially for mouth breathers.
4. Dietary and Lifestyle Modifications
- Limit Odor-Causing Foods: Reduce consumption of garlic, onions, and strong spices.
- Balanced Diet: A diet rich in fruits and vegetables, and low in processed sugars, supports overall oral health.
- Stay Hydrated: Water helps wash away food particles and bacteria.
- Quit Smoking: Smoking is a major contributor to bad breath and gum disease.
5. Medical Consultation for Systemic Causes
If a thorough dental examination reveals no oral source for halitosis, your dentist will likely refer you to a medical doctor.
- Diagnosis and Treatment of Underlying Conditions: This could involve:
- ENT Specialist: For chronic sinusitis, tonsillitis, or other respiratory issues.
- Gastroenterologist: For GERD, H. pylori infection, or other digestive problems.
- Endocrinologist: For diabetes management.
- Nephrologist/Hepatologist: For kidney or liver disease.
- Psychologist/Psychiatrist: For halitophobia.
- Pros: Addresses the root medical cause, improves overall health.
- Cons: Can be complex, require ongoing treatment, potentially involve multiple specialists.
Step-by-Step Process for Halitosis Treatment
Addressing chronic bad breath typically follows a systematic approach:
- Initial Dental Consultation (Assessment & Diagnosis):
- Medical and Dental History: Your dentist will ask about your oral hygiene routine, diet, medications, lifestyle (smoking, alcohol), and any general health conditions.
- Oral Examination: A thorough check for gum disease, cavities, infections, ill-fitting restorations, and a visual inspection of your tongue and tonsils.
- Odor Assessment: The dentist may conduct an organoleptic assessment (smelling your breath) or use specialized devices like a halimeter (measures VSCs) or gas chromatography (identifies specific VSCs).
- Differentiation: The goal is to determine if the halitosis is oral or extra-oral in origin.
- Developing a Treatment Plan:
- If Oral Origin: The dentist will outline specific oral hygiene improvements, recommend professional cleanings, and treat any underlying dental issues (fillings, gum disease treatment).
- If Suspected Extra-oral Origin: If no oral cause is found, your dentist will refer you to your primary care physician or a relevant medical specialist for further investigation.
- Implementing Oral Treatments:
- First Phase (Home Care): You'll be instructed on proper brushing, flossing, and tongue scraping techniques. You might be recommended specific ADA-accepted mouthwashes.
- Second Phase (Professional Dental Procedures): This includes professional cleanings, deep cleanings, cavity fillings, or other necessary restorative work.
- Follow-up and Monitoring:
- Regular check-ups will monitor the effectiveness of the treatments and make any necessary adjustments. This helps ensure long-term fresh breath and address any new issues promptly.
- Pro Tip: Be open and honest with your dentist about your habits and concerns. The more information they have, the better they can tailor your halitosis treatments.
Cost and Insurance for Halitosis Treatments
The cost of halitosis treatments in the US varies widely depending on the underlying cause, the type of treatment needed, and your geographic location. Dental insurance can significantly offset these costs, but coverage varies by plan.
Typical Costs (Without Insurance)
- Initial Dental Check-up & Consultation: $50 - $200 (for assessment of oral causes).
- Professional Dental Cleaning (Prophylaxis): $75 - $200. Usually covered by insurance (often 100% for two cleanings/year).
- Deep Cleaning (Scaling and Root Planing):
- Per Quadrant: $200 - $500. A full mouth deep cleaning (4 quadrants) could range from $800 - $2,000.
- Generally covered by insurance, often at 50-80% after deductible.
- Cavity Fillings:
- Amalgam (silver): $50 - $150 per filling.
- Composite (tooth-colored): $100 - $250 per filling.
- Typically covered by insurance at 50-80%.
- Periodontal Treatments (Beyond Deep Cleaning):
- Antibiotic therapy (localized gel/chip): $50 - $150 per application.
- Periodontal surgery: Can range from $500 - $3,000+ per quadrant, depending on complexity. Often covered by insurance at 50% or less.
- Tonsil Stone Removal:
- Manual removal by dentist: Often included in check-up fee or small additional fee ($50 - $150).
- Tonsillectomy (by ENT for recurrent issues): $3,000 - $6,000+. Medical insurance usually covers this if medically necessary.
- Saliva Stimulants/Substitutes:
- Over-the-counter products: $10 - $30 per item (monthly cost).
- Prescription medications (e.g., pilocarpine): $30 - $100+ per month.
- Not always covered by dental or medical insurance.
- Over-the-Counter Oral Hygiene Products:
- Toothbrushes (manual/electric heads): $5 - $15 per brush/pack.
- Tongue scrapers: $5 - $15.
- Fluoride toothpaste: $3 - $10.
- Floss: $3 - $8.
- Therapeutic mouthwash: $8 - $20 per bottle.
- These are out-of-pocket expenses.
Insurance Coverage
- Dental Insurance: Most standard dental insurance plans focus on preventative care (check-ups, cleanings, X-rays) with 100% coverage. Basic restorative procedures (fillings) are typically covered at 50-80%. Major procedures (deep cleanings, gum surgery) might be covered at 20-50%. It's crucial to check your specific plan's details regarding deductibles, annual maximums, and waiting periods for major procedures.
- Medical Insurance: If halitosis is determined to be caused by an underlying systemic medical condition (e.g., GERD, diabetes, kidney disease), the diagnosis and treatment of that condition would fall under your medical insurance plan. This includes specialist visits (ENT, gastroenterologist, endocrinologist), diagnostic tests, and prescribed medications.
Payment Plans and Financing Options
Many dental offices offer payment plans or work with third-party financing companies (e.g., CareCredit) to help patients manage costs, especially for more extensive treatments. These plans often allow you to pay for treatment over several months, sometimes interest-free.

Recovery and Aftercare
Successful halitosis treatments require consistent commitment to recovery and aftercare. The goal is to maintain fresh breath and prevent recurrence.
- Maintain Exemplary Oral Hygiene: This is non-negotiable. Continue brushing twice daily, flossing daily, and incorporating tongue scraping into your routine. This becomes your daily defense against odor-causing bacteria.
- Follow Dentist's Recommendations: Adhere to any specific instructions regarding mouthwashes, prescription medications, or special cleaning techniques.
- Regular Dental Check-ups: Schedule and attend your routine dental cleanings and examinations, typically every six months, or more frequently if recommended for gum disease management. These visits allow your dentist to monitor your oral health and address any emerging issues before they become problematic.
- Hydration: Continuously drink water throughout the day to keep your mouth moist and help wash away bacteria and food debris.
- Dietary Awareness: Be mindful of foods that can temporarily cause bad breath and manage their consumption. A balanced diet rich in fiber and low in sugar also promotes good oral health.
- Address Dry Mouth: If you suffer from xerostomia, continue using saliva substitutes, humidifiers, and avoiding dehydrating substances.
- Manage Underlying Medical Conditions: If your halitosis was linked to a systemic issue, diligent management of that condition (e.g., diabetes, GERD) under a medical doctor's care is vital.
- Avoid Tobacco and Limit Alcohol: These habits are detrimental to both oral health and fresh breath. Quitting tobacco is one of the most impactful steps you can take.
- Self-Monitoring: Periodically check your breath (as described earlier) and be attuned to any changes in taste or smell in your mouth. Early detection allows for quicker intervention.
Prevention of Halitosis
Preventing bad breath is largely about maintaining consistent, excellent oral hygiene and a healthy lifestyle.
- Brush and Floss Religiously: Brush your teeth for two minutes, twice a day, and floss once a day. This is the foundation of preventing plaque buildup and bacterial growth. The ADA recommends soft-bristled brushes and fluoride toothpaste.
- Clean Your Tongue Daily: Use a tongue scraper or toothbrush to remove bacteria from the surface of your tongue.
- Stay Hydrated: Drink plenty of water throughout the day. Water not only helps rinse your mouth but also stimulates saliva flow.
- Chew Sugar-Free Gum: Chewing sugar-free gum after meals can stimulate saliva production, which helps neutralize acids and wash away food particles and bacteria. Look for gums containing xylitol.
- Regular Dental Check-ups and Cleanings: Visit your dentist every six months for professional cleanings and examinations. This allows for early detection and treatment of issues like cavities, gum disease, and dry mouth before they contribute to chronic bad breath.
- Avoid Tobacco Products: Quitting smoking or chewing tobacco will dramatically improve your breath and overall oral health.
- Limit Alcohol and Coffee: These can dry out your mouth and contribute to bad breath. If consumed, follow with water.
- Mind Your Diet: Reduce intake of strong-smelling foods like garlic and onions. Eat a balanced diet rich in fruits and vegetables.
- Treat Underlying Health Conditions: If you have conditions like chronic sinusitis, GERD, or diabetes, work with your medical doctor to manage them effectively.
Risks and Complications of Untreated Halitosis
While often seen as a social inconvenience, untreated chronic halitosis can lead to several complications:
- Social and Psychological Impact: Persistent bad breath can cause significant social anxiety, self-consciousness, embarrassment, and can negatively affect personal relationships, career opportunities, and overall quality of life. It can lead to social isolation and even depression in severe cases.
- Progression of Oral Diseases: Since halitosis is often a symptom of underlying oral health issues, ignoring it means allowing these conditions to worsen.
- Periodontal Disease: Untreated gingivitis can progress to severe periodontitis, leading to bone loss, receding gums, and eventually tooth loss.
- Dental Decay: Untreated cavities will expand, potentially leading to pain, infection, and tooth extraction.
- Oral Infections: Untreated infections can spread to other parts of the body, causing more severe health problems.
- Masking Serious Systemic Conditions: If the halitosis is a symptom of a non-oral health issue (e.g., diabetes, liver disease, kidney failure, respiratory infection), ignoring the bad breath means delaying the diagnosis and treatment of a potentially serious or life-threatening medical condition.
- Nutritional Deficiencies: In some cases, severe oral pain or discomfort associated with the causes of halitosis (e.g., advanced gum disease, multiple painful cavities) can make eating difficult, potentially leading to poor nutrition.
Comparison of Common Halitosis Treatments
To help you visualize the various halitosis treatments, here are a couple of comparison tables highlighting key aspects.
Table 1: Comparison of Oral Hygiene Techniques for Halitosis
| Treatment Method | Primary Action | Effectiveness for Halitosis | Cost Range (USD) | Pros | Cons |
|---|---|---|---|---|---|
| Brushing (2x daily) | Removes plaque, food debris from tooth surfaces | High | $3 - $15 (brush) | Foundational, prevents cavities & gum disease | Misses interdental/tongue areas, requires proper technique |
| Flossing (1x daily) | Removes interdental plaque, food particles | High | $3 - $8 (floss) | Crucial for gum health, removes hidden odor sources | Can be tricky, requires consistency |
| Tongue Scraping | Removes bacteria/debris from tongue dorsum | Very High | $5 - $15 (scraper) | Direct removal of primary VSC source, immediate relief | Can trigger gag reflex for some |
| Antimicrobial Mouthwash | Kills bacteria, neutralizes VSCs | Moderate to High | $8 - $20 (bottle) | Provides temporary freshness, reduces bacterial load | Many only mask odor; alcohol-based can dry mouth |
| Professional Cleaning | Removes hardened plaque (calculus) & tartar | Very High | $75 - $200 | Cleans areas impossible to reach at home | Requires dental visit, not a daily solution |

Table 2: Comparison of Professional Treatments for Chronic Halitosis (Beyond Basic Cleaning)
| Treatment Method | Primary Action | Average Cost (USD, without insurance) | Typical Duration/Frequency | Pros | Cons |
|---|---|---|---|---|---|
| Deep Cleaning (SRP) | Removes plaque/tartar below gum line, smooths roots | $200 - $500 per quadrant | 1-4 appointments, then regular maintenance | Treats gum disease, major source of halitosis | Can be uncomfortable, requires local anesthesia |
| Cavity Fillings | Removes decay, seals tooth | $50 - $250 per filling | 1 appointment per filling | Eliminates bacterial traps, prevents further decay | Cost depends on material/size |
| Tonsil Stone Removal (Dentist) | Manual removal of stones | $50 - $150 (often part of exam) | As needed | Immediate relief from stone-related odor | Stones may recur, may require ENT referral |
| Saliva Stimulants (Rx) | Increases natural saliva production | $30 - $100+ per month | Daily ongoing use | Addresses dry mouth, improves natural cleansing | Prescription needed, potential side effects, ongoing cost |
| Referral to Medical Specialist | Diagnoses & treats systemic causes | Varies greatly (specialist fees, tests) | Ongoing as needed | Addresses underlying health issue, comprehensive care | Can be complex, involves multiple appointments & tests |
Children / Pediatric Considerations
Halitosis in children is less common than in adults but can occur. Addressing it requires a slightly different approach, often focusing on simpler causes first.
Common Causes of Bad Breath in Children:
- Poor Oral Hygiene: This is the most frequent cause. Children may not brush or floss effectively, leading to plaque buildup, food debris, and tongue coating.
- Dry Mouth: Can be caused by mouth breathing (due to allergies, enlarged tonsils/adenoids), certain medications, or insufficient hydration.
- Oral Infections: Untreated cavities, gum inflammation (gingivitis), or oral thrush can cause odor.
- Tonsillitis/Adenoiditis: Enlarged or infected tonsils/adenoids can harbor bacteria or form tonsil stones, leading to a foul odor. Post-nasal drip from allergies or colds can also contribute.
- Foreign Objects in the Nose: Young children sometimes insert small objects into their nostrils, which can lead to infection and a very strong, unilateral (one-sided) bad odor.
- Gastroesophageal Reflux: In infants and young children, reflux can cause bad breath.
- Systemic Diseases: Although rare, conditions like diabetes can manifest with a distinctive breath odor.
Halitosis Treatments for Children:
- Improve Oral Hygiene:
- Supervision: Parents should supervise and assist young children with brushing and flossing until they develop adequate dexterity (around age 7-8).
- Tongue Cleaning: Gently encourage children to brush or scrape their tongue.
- Positive Reinforcement: Make oral hygiene fun and consistent.
- Address Dry Mouth:
- Ensure adequate water intake.
- Consult a pediatrician or ENT for chronic mouth breathing (due to allergies or enlarged tonsils/adenoids).
- Dental Check-ups: Regular visits to a pediatric dentist are crucial to detect and treat cavities, gingivitis, or other oral infections early.
- Pediatrician Consultation: If oral causes are ruled out, a pediatrician can investigate other possibilities, such as chronic sinusitis, tonsillitis, GERD, or a foreign object in the nasal passage.
- Dietary Guidance: Limit sugary snacks and drinks, which contribute to cavities and bacterial growth. Encourage a balanced diet.
Pro Tip for Parents: If your child has persistent bad breath, start by reviewing their brushing and flossing habits and ensuring they are drinking enough water. If the problem persists after a week of diligent home care, schedule an appointment with your pediatric dentist.
Cost Breakdown
A dedicated look at the cost implications for halitosis treatments, summarizing and elaborating on earlier points.
Average US Costs (Without Insurance)
- Low End (Basic Care):
- Dental Exam: $50
- Basic Cleaning: $75
- Over-the-counter hygiene products: $20 - $50 (initial purchase of scraper, good toothbrush, specific mouthwash).
- Total Initial: ~$145 - $175 (recurring monthly product cost: $10-$20)
- Mid-Range (Addressing Mild-Moderate Issues):
- Dental Exam & X-rays: $150 - $250
- Deep Cleaning (1-2 quadrants): $400 - $1000
- 1-2 Composite Fillings: $200 - $500
- Ongoing specialized mouthwash/saliva substitutes: $20 - $50/month
- Total Initial: ~$750 - $1,750 (can vary widely based on number of quadrants for deep cleaning and fillings).
- High End (Complex Cases, Systemic Issues, or Multiple Oral Problems):
- Comprehensive Periodontal Therapy (full mouth deep cleaning + surgery/antibiotics): $2,000 - $5,000+
- Multiple Fillings/Crowns/Root Canals: $1,000 - $5,000+
- Referral to Medical Specialist (e.g., ENT consult, diagnostic tests, medications for GERD/sinusitis): $300 - $2,000+ (can be covered by medical insurance).
- Total Initial: $3,300 - $12,000+ (highly variable depending on specific procedures and medical conditions).
With vs. Without Insurance
- Preventative Care (Exams, Cleanings): Most dental insurance plans cover 80-100% of these costs, often allowing for two cleanings per year with no or low co-pay.
- Basic Restorative Care (Fillings): Insurance typically covers 50-80%.
- Major Restorative/Periodontal Care (Deep Cleanings, Surgery, Crowns): Coverage can range from 20-50%, often with deductibles and annual maximums (e.g., $1,000-$2,000 per year). Once you hit your annual maximum, you pay 100% out-of-pocket for the remainder of the year.
- Medical Insurance: For halitosis caused by systemic issues, medical insurance will cover specialist visits, diagnostic tests (e.g., blood tests, endoscopy), and prescription medications according to your plan's terms (co-pays, deductibles, coinsurance).
Payment Plans and Financing Options
Many dental offices understand the financial burden of extensive treatments and offer:
- In-house Payment Plans: Allows you to pay in installments directly to the dental office, often with no interest if paid within a certain timeframe.
- Third-Party Financing: Companies like CareCredit or LendingClub Patient Solutions offer specialized healthcare credit cards or loans. These can provide low-interest or interest-free financing for a set period, allowing you to manage large treatment costs over time.
- Dental Schools: University dental schools often provide treatments at a reduced cost, as procedures are performed by students under the supervision of experienced faculty.
Cost-Saving Tips
- Preventative Care: The single best way to save money is to prevent dental problems. Regular brushing, flossing, and dental check-ups can prevent costly issues like gum disease and large cavities.
- Dental Insurance: Invest in a good dental insurance plan, especially if you anticipate needing more than just basic cleanings. Understand your plan's benefits and limitations.
- Health Savings Account (HSA) or Flexible Spending Account (FSA): If you have access to an HSA or FSA through your employer, you can use pre-tax dollars to pay for qualified medical and dental expenses, including halitosis treatments.
- Negotiate Cash Discounts: If you don't have insurance, ask your dental office if they offer a discount for upfront payment in cash.
- Comparison Shop: For extensive treatments, it's acceptable to get a second opinion and compare treatment plans and costs from different providers.
Frequently Asked Questions
What is the main cause of chronic bad breath?
The primary cause of chronic bad breath, in about 90% of cases, originates in the mouth. It's usually due to the accumulation of odor-producing bacteria, particularly on the back of the tongue and between teeth, which break down food particles and dead cells, releasing volatile sulfur compounds (VSCs).
Can chronic bad breath be a sign of a serious illness?
Yes, while most cases are oral in origin, chronic bad breath can sometimes be a symptom of underlying systemic health conditions such as uncontrolled diabetes, kidney failure, liver disease, chronic sinus infections, or gastroesophageal reflux disease (GERD). If no oral cause is found, your dentist will recommend a medical evaluation.
How quickly can halitosis treatments show results?
Many oral halitosis treatments, such as improved brushing, flossing, and tongue scraping, can show noticeable improvement within a few days to a week. Professional dental cleanings can offer significant improvement immediately. Treating underlying dental diseases like gum disease may take several weeks or months for full resolution.
Are mouthwashes effective for halitosis?
Mouthwashes can be effective, but their efficacy varies. Therapeutic mouthwashes containing ingredients like chlorine dioxide, zinc, or cetylpyridinium chloride can kill bacteria and neutralize odor-causing compounds. However, many cosmetic mouthwashes only temporarily mask the odor. The ADA recommends alcohol-free, therapeutic mouthwashes.
Is halitosis curable, or will I always have to manage it?
For most people, halitosis is curable, especially when the cause is oral. By identifying and treating the underlying dental issue, combined with meticulous daily oral hygiene, lasting fresh breath can be achieved. However, if the cause is a chronic systemic condition, ongoing management of that condition will be necessary to control the breath odor.
What is the role of tongue scraping in halitosis treatment?
Tongue scraping is a highly effective component of halitosis treatment. It mechanically removes the thick bacterial film, food debris, and dead cells from the surface of the tongue, which are major sources of volatile sulfur compounds (VSCs). Regular daily scraping significantly reduces the bacterial load and improves breath freshness.
Can diet affect bad breath?
Yes, diet plays a significant role. Strong-smelling foods like garlic and onions can cause temporary bad breath. Additionally, high-sugar diets can fuel oral bacteria, while low-carbohydrate diets can lead to "keto breath." A balanced diet, adequate hydration, and limiting processed sugars support better oral health and breath.
How much does it cost to get halitosis treated?
The cost varies widely. Basic dental check-ups and cleanings might range from $75 to $200. If underlying issues like gum disease (requiring deep cleaning at $200-$500 per quadrant) or cavities (fillings at $50-$250 each) are found, the costs increase. Extensive treatments or medical referrals can be thousands of dollars, though insurance often covers a portion.
Is treatment for halitosis painful?
Treatments for halitosis are generally not painful. Basic oral hygiene adjustments are painless. Professional dental cleanings might cause minor sensitivity, which can be managed. Procedures like deep cleaning (scaling and root planing) are often performed with local anesthesia to ensure your comfort. If a medical condition is the cause, its treatment will determine any discomfort.
What if my dentist can't find a cause for my bad breath?
If your dentist thoroughly examines your mouth and finds no oral cause, they will likely refer you to a medical doctor or specialist. This step is crucial because, in about 10% of cases, halitosis stems from underlying systemic conditions, and a medical professional can diagnose and treat these non-oral causes.
When to See a Dentist
It's important to differentiate between temporary bad breath and a persistent problem that warrants professional attention.
Clear Warning Signs That Need Immediate Attention:
- Persistent Bad Breath Despite Excellent Oral Hygiene: If you're consistently brushing, flossing, and cleaning your tongue well, and your bad breath doesn't improve after a week or two, it's a strong indicator of an underlying issue.
- Accompanying Symptoms: If bad breath is accompanied by:
- Bleeding, swollen, or tender gums.
- Pus around teeth or gums.
- Loose teeth.
- Chronic dry mouth.
- A persistent bad taste in your mouth.
- Pain in your teeth or jaw.
- Difficulty swallowing or a sore throat.
- Distinctive Odors: If your breath has a noticeably fruity, ammonia-like, or unusually sweet smell, it could signal a serious medical condition like diabetes, kidney, or liver disease, requiring immediate medical evaluation.
Red Flags vs. Routine Care Guidance:
- Routine Care: If your bad breath is primarily "morning breath" or linked to specific foods and resolves with brushing and flossing, it's likely physiological and managed with routine care. Regular dental check-ups (every 6 months) are still essential for prevention.
- Red Flags: Any persistent, unexplained bad breath, or breath accompanied by the symptoms listed above, is a red flag. Do not dismiss it as merely a cosmetic issue.
Emergency vs. Scheduled Appointment Guidance:
- Scheduled Appointment: For chronic bad breath that doesn't resolve with home care, or if you suspect an underlying oral issue like gum disease or cavities, schedule a regular dental appointment. Your dentist can perform a thorough examination and recommend appropriate halitosis treatments.
- Emergency Appointment: If bad breath is accompanied by severe pain, swelling, fever, difficulty breathing, or sudden significant changes in overall health, seek immediate medical or dental attention. These could be signs of acute infection or a critical systemic condition.
Ignoring chronic bad breath is not an option for your oral and general health. A timely visit to your dentist is the most effective step toward diagnosing the cause and initiating the most appropriate halitosis treatments for a healthier, fresher you.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Cause Bad Breath
For many, a quick mint or a swig of mouthwash is the go-to solution for an unpleasant taste or odor in the mouth. But what if that bad breath, medically known as halitosis, is a persistent problem that no amount of peppermint can conquer? It’s a far more common issue than you might think, affecting
February 23, 2026

Dogs Bad Breath: Complete Guide
One whiff is all it takes: that distinctly unpleasant odor emanating from your beloved canine companion. If you've ever wondered, "Why does my dog's breath smell so bad?" you're not alone. It's a common concern among pet owners, with over 80% of dogs showing signs of oral disease by age three. W
February 23, 2026

Sudden Bad Breath in Toddlers: Complete Guide
When your toddler, who usually smells sweet and innocent, suddenly develops an unpleasant odor in their breath, it can be an alarming experience for any parent. Sudden bad breath in toddlers, also known as halitosis, is more common than you might think, affecting a significant number of young ch
February 23, 2026

Mouth Wash for Bad Breath: Complete Guide
Bad breath, medically known as halitosis, is an incredibly common and often embarrassing condition that affects a significant portion of the global population. In the United States alone, more than 80 million people suffer from chronic bad breath, impacting social interactions, professional conf
February 23, 2026