What Is Gingivitis
Key Takeaways
- Around 47% of adults aged 30 and older in the United States suffer from some form of gum disease, with gingivitis being the earliest and most common stage. This often silent condition, if left unaddressed, can escalate into more severe problems that threaten not only your oral health but your ov
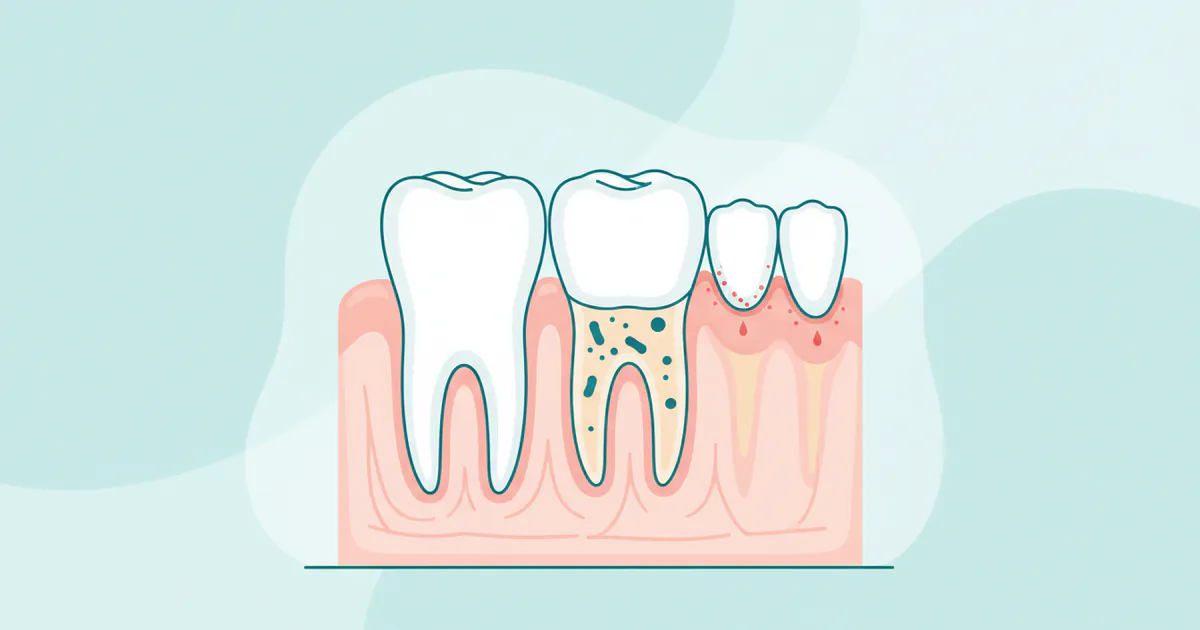
Around 47% of adults aged 30 and older in the United States suffer from some form of gum disease, with gingivitis being the earliest and most common stage. This often silent condition, if left unaddressed, can escalate into more severe problems that threaten not only your oral health but your overall well-being. So, what is gingivitis? It's an inflammation of the gums, typically caused by plaque buildup along the gumline. While it might start subtly with a little bleeding when you brush, understanding its causes, recognizing its signs, and knowing your treatment and prevention options are crucial steps toward maintaining a healthy smile. This comprehensive guide from SmilePedia.net will delve deep into gingivitis, exploring its origins, detailing effective treatments, outlining the costs involved, and providing actionable steps to keep your gums healthy and strong, preventing the progression to more serious periodontal disease.
Key Takeaways:
- What It Is: Gingivitis is the earliest and mildest form of gum disease, characterized by inflamed, red, swollen, and often bleeding gums. It is caused primarily by plaque buildup.
- Reversible: Unlike more advanced periodontal disease, gingivitis is fully reversible with proper treatment and improved oral hygiene.
- Primary Treatment: Professional dental cleaning (prophylaxis) to remove plaque and tartar, combined with diligent daily brushing and flossing, is the cornerstone of gingivitis treatment.
- Cost: A standard dental cleaning (prophylaxis) in the US typically ranges from $75 to $200 without insurance. Insurance often covers 80-100% of preventive care, including two cleanings per year.
- Timeline for Improvement: Symptoms like bleeding and inflammation usually improve within 1-2 weeks of professional cleaning and consistent home care. Complete resolution can take several weeks.
- Prevention is Key: Regular brushing twice a day, flossing daily, and routine dental check-ups (every 6 months) are essential to prevent gingivitis.
- Risk of Progression: If left untreated, gingivitis can progress to periodontitis, a severe and irreversible form of gum disease that can lead to tooth loss and impact overall systemic health.
What It Is / Overview
Gingivitis (pronounced jin-juh-VYE-tis) is the initial stage of periodontal disease, a common inflammatory condition affecting the tissues surrounding your teeth. The term itself literally means "inflammation of the gums" ("gingiva" refers to gums, and "-itis" means inflammation). It occurs when plaque, a sticky, colorless film of bacteria, constantly forms on your teeth. If plaque isn't removed through regular brushing and flossing, it can harden into tartar (calculus), which irritates the gum tissue. This irritation leads to inflammation, causing your gums to become red, swollen, and prone to bleeding.

Crucially, gingivitis is a non-destructive form of periodontal disease. This means that at this stage, the bone and ligaments that hold your teeth in place are not yet affected. The inflammation is confined to the gum tissue. This distinction is vital because, unlike advanced gum disease (periodontitis), gingivitis is completely reversible with good oral hygiene and professional dental care. Ignoring gingivitis, however, allows the bacterial infection to spread deeper, potentially leading to the destruction of the supporting bone and tissue, which is the hallmark of periodontitis.
The primary culprit behind gingivitis is dental plaque. This biofilm, composed of bacteria, food particles, and saliva, adheres to tooth surfaces. The bacteria in plaque produce toxins that irritate the gingival tissues, triggering an inflammatory response. Over time, if plaque isn't adequately removed, it mineralizes and forms tartar. Tartar is rough and porous, providing an even more favorable surface for plaque accumulation and making it much harder to remove with just brushing and flossing. Only a dental professional can effectively remove tartar.
Types / Variations
While the most common form of gingivitis is directly linked to plaque, the American Dental Association (ADA) and the American Academy of Periodontology (AAP) recognize different classifications. Understanding these can help in diagnosis and treatment.
Plaque-Induced Gingivitis
This is by far the most prevalent type of gingivitis, affecting the vast majority of individuals who experience gum inflammation. It is directly associated with the accumulation of dental plaque on the tooth surfaces.
- Characteristics: Inflammation, redness, swelling, and bleeding gums. The severity often correlates with the amount of plaque present and the individual's immune response.
- Reversibility: Fully reversible with effective plaque removal through professional cleaning and improved daily oral hygiene.
- Contributing Factors: Poor oral hygiene, crowded teeth, ill-fitting dental restorations (fillings, crowns) that trap plaque, certain medications, smoking, and systemic conditions like diabetes.
Non-Plaque Induced Gingival Lesions
These forms of gingivitis are less common and are not directly caused by plaque buildup, although plaque can exacerbate them. They are often manifestations of systemic conditions, genetic factors, infections, or allergic reactions.
- Genetic/Developmental Disorders: Conditions like hereditary gingival fibromatosis, which causes excessive gum tissue growth.
- Specific Infections:
- Bacterial: Can be caused by specific bacterial pathogens other than those typically found in plaque, such as Neisseria gonorrhoeae or Treponema pallidum (syphilis).
- Viral: Herpesvirus lesions (e.g., primary herpetic gingivostomatitis, recurrent oral herpes).
- Fungal: Candidiasis (thrush) affecting the gums.
- Inflammatory and Immune Conditions:
- Autoimmune Diseases: Pemphigoid, lichen planus, lupus erythematosus, affecting gum tissues.
- Allergic Reactions: To dental materials (nickel, mercury, acrylics), food products, or toothpaste ingredients.
- Traumatic Lesions: Physical or chemical injury to the gums, such as from aggressive brushing, burns, or chemical exposure.
- Systemic Conditions:
- Mucocutaneous Disorders: Conditions affecting skin and mucous membranes, like erythema multiforme.
- Endocrine Conditions: Hormonal changes, particularly during puberty, pregnancy, or with diabetes, can alter the gum's response to plaque, making them more susceptible to inflammation (e.g., pregnancy gingivitis).
- Nutritional Deficiencies: Scurvy (Vitamin C deficiency) can lead to severe gingival inflammation and bleeding.
- Blood Dyscrasias: Leukemias or other blood disorders can present with severe gingival manifestations.
- Medication-Induced: Certain medications can cause gingival overgrowth (hyperplasia), making plaque removal difficult and leading to inflammation. Examples include:
- Anticonvulsants: Phenytoin (Dilantin)
- Immunosuppressants: Cyclosporine
- Calcium Channel Blockers: Nifedipine, verapamil
While these non-plaque induced gingivitis types require different diagnostic approaches and often involve treating the underlying systemic cause, good oral hygiene remains crucial to manage any plaque-related inflammation that may coexist or complicate the condition.
Causes / Why It Happens
The primary cause of gingivitis is the accumulation of bacterial plaque on your teeth and around the gum line. However, several other factors can significantly contribute to its development or worsen existing gingivitis.
The Primary Cause: Dental Plaque
- Bacterial Biofilm: Plaque is a sticky, colorless-to-pale yellow film that constantly forms on your teeth. It consists of bacteria, their byproducts, food particles, and saliva.
- Toxin Production: The bacteria in plaque feed on sugars and starches in your diet and produce acids and toxins. These toxins irritate the delicate gum tissue, leading to an inflammatory response.
- Tartar (Calculus) Formation: If plaque isn't thoroughly removed through daily brushing and flossing, it hardens into tartar. Tartar is a calcified deposit that strongly adheres to the tooth surface, often above and below the gum line. Its rough surface provides an ideal breeding ground for more plaque bacteria, further irritating the gums. Once tartar forms, it cannot be removed by brushing and flossing; only a professional dental cleaning can remove it.
Contributing Factors and Risk Factors
Even with plaque present, certain factors can increase your susceptibility to gingivitis or exacerbate its severity.
- Poor Oral Hygiene: This is the most direct contributing factor. Inconsistent or ineffective brushing and flossing allow plaque to accumulate unchecked.
- Smoking and Tobacco Use: Tobacco is a significant risk factor for all forms of gum disease. Smoking impairs the immune system, making it harder for gum tissue to heal, reduces blood flow to the gums, and can mask the classic signs of gingivitis (like bleeding) because nicotine constricts blood vessels. Smokers are far more likely to develop gingivitis and periodontitis.
- Hormonal Changes: Fluctuations in hormones can make gums more sensitive and reactive to plaque.
- Pregnancy: "Pregnancy gingivitis" is common due to increased progesterone and estrogen levels, which can exaggerate the inflammatory response to plaque.
- Puberty, Menstruation, Menopause: Similar hormonal shifts can lead to increased gum sensitivity.
- Certain Medications:
- Dry Mouth (Xerostomia): Many medications (antihistamines, antidepressants, diuretics, high blood pressure meds) reduce saliva flow. Saliva helps wash away food particles and neutralize acids, so reduced saliva increases plaque buildup.
- Gingival Enlargement: Some drugs, like phenytoin (for seizures), cyclosporine (immunosuppressant), and calcium channel blockers (for heart conditions), can cause gums to overgrow, making them harder to clean and more prone to inflammation.
- Systemic Diseases:
- Diabetes: People with poorly controlled diabetes are more susceptible to infections, including gum disease. High blood sugar levels impair the immune response and the ability to heal.
- Compromised Immunity: Conditions like HIV/AIDS or treatments like chemotherapy can weaken the immune system, making individuals more vulnerable to gum infections.
- Nutritional Deficiencies:
- Vitamin C Deficiency (Scurvy): While rare in developed countries, severe vitamin C deficiency can lead to fragile, bleeding gums.
- Genetics: Some people are genetically predisposed to developing gum disease, meaning they may be more susceptible even with good oral hygiene.
- Age: The risk of gum disease tends to increase with age.
- Stress: Chronic stress can weaken the immune system, potentially making you more vulnerable to infections, including gum disease.
- Poorly Fitting Dental Restorations: Crowns, fillings, or bridges that have rough or ill-fitting margins can create areas where plaque easily accumulates and is difficult to remove.
- Crowded or Misaligned Teeth: Teeth that are crowded, crooked, or rotated create more challenging surfaces for effective brushing and flossing, allowing plaque to accumulate.
Understanding these causes and risk factors is the first step toward effective prevention and treatment of gingivitis. Addressing underlying conditions and modifying lifestyle habits can significantly improve gum health.
Signs and Symptoms
Recognizing the signs and symptoms of gingivitis early is crucial for successful treatment and preventing its progression. Healthy gums are typically firm, pink, and do not bleed when brushed or flossed. If you notice any deviations from this, you may be experiencing gingivitis.
Here's what to look for:
- Red or Purplish Gums: One of the earliest and most noticeable signs. Healthy gums are a coral pink. Inflamed gums appear redder or even purplish due to increased blood flow from inflammation.
- Swollen or Puffy Gums: The gum tissue may appear enlarged, puffy, or tender to the touch. The normal scalloped appearance around the teeth can become blunted or rounded.
- Bleeding Gums: This is a hallmark symptom of gingivitis. Gums may bleed easily when you brush your teeth, floss, or even when you eat hard foods. Many people mistakenly believe that bleeding gums are normal or a sign of brushing too hard, but it's almost always an indicator of inflammation.
- Tenderness or Pain: While gingivitis is often painless in its early stages, some individuals may experience mild discomfort or tenderness, especially when touching or brushing their gums.
- Receding Gums: In some cases, the gum tissue may start to pull away from the tooth surface, making the teeth appear longer. This creates pockets where more plaque can accumulate.
- Bad Breath (Halitosis): The accumulation of bacteria and decaying food particles in the inflamed gum areas can release unpleasant odors, leading to persistent bad breath.
- Shiny Gums: Inflamed gums can sometimes have a shiny appearance due to swelling.
- Soft Gums: Healthy gums are firm. With gingivitis, the gums may feel softer and more spongy.
It's important to note that gingivitis can be subtle and painless in its early stages, which is why regular dental check-ups are so important. A dental professional can spot the signs even before you notice them.
``
Table: Healthy Gums vs. Gingivitis Symptoms
To help you distinguish between healthy and inflamed gums, here's a comparison table:
| Feature | Healthy Gums | Gums with Gingivitis |
|---|---|---|
| Color | Coral pink | Red, dark red, or purplish |
| Appearance | Firm, tight around teeth, stippled (orange peel texture), knife-edged margin | Swollen, puffy, rounded or blunted margins, shiny appearance |
| Bleeding | No bleeding during brushing or flossing | Bleeds easily during brushing, flossing, or probing |
| Tenderness | No tenderness | May be tender or sore to the touch |
| Bad Breath | Generally fresh breath | Persistent bad breath (halitosis) |
| Recession | No significant gum recession | May show signs of early recession |
| Pain | No pain | Usually painless, but can be mildly uncomfortable |
Pro Tip: If you notice blood in the sink after brushing or on your floss, do not ignore it. This is a primary indicator of gingivitis and signals that it's time to see your dentist.
Treatment Options
The good news is that gingivitis is completely reversible with proper treatment. The primary goal of treatment is to remove the source of inflammation – the bacterial plaque and tartar – and to establish an environment where gums can heal.
1. Professional Dental Cleaning (Prophylaxis)
This is the cornerstone of gingivitis treatment.
- What it Involves: A dental hygienist or dentist uses specialized instruments to remove plaque and tartar from above and slightly below the gum line. This process is often referred to as scaling.
- Benefits:
- Removes hardened plaque (tartar) that cannot be removed by home care.
- Removes bacterial biofilm, allowing gums to heal.
- Polishes tooth surfaces to make them smoother and less hospitable for new plaque accumulation.
- Provides an opportunity for the dental professional to assess your oral health and provide personalized oral hygiene instructions.
- Pros: Highly effective, relatively quick, usually covered by dental insurance.
- Cons: Some mild discomfort or sensitivity during/after, especially if significant tartar buildup.
- Frequency: Typically recommended every 6 months, but your dentist might suggest more frequent cleanings (e.g., every 3-4 months) in initial stages of treatment or for those prone to plaque buildup.
2. Improved Home Oral Hygiene
Once professional cleaning removes existing plaque and tartar, consistent and effective daily home care is paramount to prevent recurrence.
- Brushing: Brush at least twice a day for two minutes each time, using a soft-bristled toothbrush and fluoride toothpaste. Angle the brush at 45 degrees to the gum line, gently sweeping away plaque. Electric toothbrushes are often more effective for plaque removal.
- Flossing: Floss daily to remove plaque and food particles from between teeth and under the gum line, where a toothbrush cannot reach. Dental picks or interdental brushes can also be used.
- Mouthwash: Therapeutic (antiseptic) mouthwashes can help reduce bacteria. Over-the-counter options often contain ingredients like cetylpyridinium chloride (CPC) or essential oils. Your dentist might prescribe a stronger chlorhexidine gluconate (CHX) rinse for short-term use in more severe cases of gingivitis.
- Pros: Enhances plaque control, freshens breath.
- Cons: Some over-the-counter rinses can contain alcohol, which can be drying; prescription rinses like CHX can cause temporary staining or alter taste.
- Pros: Empowerment of self-care, cost-effective long-term prevention.
- Cons: Requires discipline and proper technique.
3. Addressing Contributing Factors
- Ill-fitting Restorations: If rough or poorly contoured fillings or crowns contribute to plaque accumulation, your dentist may recommend replacing or repairing them.
- Malocclusion/Crowding: Orthodontic treatment (braces, aligners) can straighten teeth, making them easier to clean and reducing areas where plaque can hide.
- Smoking Cessation: Quitting smoking is one of the most impactful steps you can take for your gum health and overall health. Your dentist can offer resources or referrals to help.
- Managing Systemic Diseases: For individuals with diabetes, maintaining good blood sugar control is vital for gum health. Regular communication between your dentist and physician is important.
- Medication Review: If a medication is causing gingival enlargement or dry mouth, your dentist may consult with your physician to explore alternative medications or strategies to manage side effects.

4. Advanced Treatments (Rarely for pure Gingivitis)
While generally not needed for simple gingivitis, in cases where inflammation is severe or if there's a risk of progression, these might be considered:
- Antibiotics: Systemic antibiotics (pills) or topical antibiotic gels/chips are generally reserved for more advanced periodontal disease. They are rarely used for gingivitis unless there's an aggressive or unusual bacterial component, or in immunocompromised patients.
- Laser Therapy: Sometimes used as an adjunct to traditional scaling, laser therapy can help reduce bacteria and promote healing. Its role in treating pure gingivitis is still evolving, and it's more commonly associated with periodontitis treatment.
The vast majority of gingivitis cases are effectively treated and reversed through professional dental cleaning combined with a reinforced commitment to excellent daily oral hygiene.
``
Step-by-Step Process
Understanding what to expect when seeking treatment for gingivitis can help alleviate anxiety and prepare you for a healthier smile. The process typically involves a diagnostic phase, professional cleaning, and ongoing maintenance.
Step 1: Initial Dental Examination and Diagnosis
- Comprehensive Oral Exam: Your dentist or dental hygienist will conduct a thorough examination of your mouth, teeth, and gums. They will look for signs of inflammation, redness, swelling, and bleeding.
- Probing: A small measuring tool (periodontal probe) will be gently inserted into the sulcus (the shallow space between the tooth and the gum) around each tooth. Healthy sulcus depths are typically 1-3 millimeters. Deeper pockets can indicate more advanced disease, but even in gingivitis, the gum tissue might be slightly swollen, making the sulcus appear a bit deeper.
- Plaque and Tartar Assessment: The dental professional will identify areas of plaque accumulation and assess the presence and extent of tartar buildup, especially along the gum line.
- X-rays (if necessary): While gingivitis primarily affects soft tissues, X-rays might be taken to rule out underlying bone loss (which would indicate periodontitis) or other dental issues contributing to plaque retention, such as cavities or ill-fitting restorations.
- Discussion and Diagnosis: Based on the findings, your dentist will explain your condition, confirm the diagnosis of gingivitis, and discuss the recommended treatment plan.
Step 2: Professional Dental Cleaning (Prophylaxis)
- Scaling: This is the process of removing plaque and tartar (calculus) from the tooth surfaces, both above and slightly below the gum line. The hygienist will use manual scaling instruments (curettes and sickles) and/or an ultrasonic scaler. Ultrasonic scalers use high-frequency vibrations and water spray to break down and flush away deposits.
- Polishing: After scaling, your teeth will be polished using a rotary brush and abrasive paste. This removes any remaining surface stains and smooths the tooth surfaces, making it harder for plaque to adhere.
- Flossing: A final flossing session may be performed to ensure all interdental areas are clean.
- Fluoride Treatment (Optional): A fluoride application might be offered to help strengthen tooth enamel and reduce sensitivity, though it's not a direct treatment for gingivitis itself.
Step 3: Oral Hygiene Instruction
- Personalized Guidance: This is a critical part of the treatment. Your hygienist will demonstrate proper brushing techniques (e.g., Bass method, using a soft-bristled brush, angling at 45 degrees to the gum line) and flossing techniques. They might recommend specific tools like interdental brushes, water flossers, or an electric toothbrush.
- Product Recommendations: You may receive advice on specific toothpastes (e.g., fluoride-containing), mouthwashes (e.g., antiseptic rinses), or other oral care products that can aid in plaque control.
- Dietary Advice: Advice on reducing sugary or acidic foods and drinks that contribute to plaque formation may be provided.
Step 4: Recovery and Follow-up
- Initial Healing: Your gums may be slightly sensitive or tender for a day or two after a thorough cleaning, especially if there was significant inflammation. This is normal.
- Ongoing Home Care: Diligent and consistent home care (brushing twice daily, flossing daily) is essential to allow the gums to heal completely and prevent the return of gingivitis.
- Follow-up Appointment: Your dentist will typically recommend a follow-up appointment, usually within 6 months, for your next routine cleaning and to re-evaluate your gum health. If your gingivitis was more severe, they might suggest an earlier follow-up. In most cases, with good home care, the signs of gingivitis resolve completely within 1-2 weeks.
By following these steps, you can effectively treat gingivitis and restore your gums to a healthy state.
Cost and Insurance
Understanding the financial aspects of gingivitis treatment is important for planning your dental care. In the United States, costs can vary significantly based on geographic location, the specific dental practice, and the severity of the condition.
Average US Costs for Gingivitis Treatment
The primary treatment for gingivitis is a professional dental cleaning, also known as prophylaxis.
-
Standard Dental Cleaning (Prophylaxis):
- Without Insurance: Typically ranges from $75 to $200. In some high-cost urban areas, it might reach up to $250. This fee usually covers the examination by the dentist, scaling (removal of plaque and tartar), polishing, and sometimes fluoride application.
- With Insurance: Most dental insurance plans categorize standard cleanings as preventive care. This means they often cover 80-100% of the cost, usually for two cleanings per year. You might only be responsible for a small co-pay or nothing at all, depending on your plan.
-
Scaling and Root Planing (Deep Cleaning):
- While not typically for pure gingivitis, if the inflammation is borderline periodontitis or if there is significant subgingival (below the gum line) tartar and early pocketing, your dentist might recommend a "deep cleaning." This procedure involves more extensive scaling and root planing, which smooths the root surfaces to deter bacterial reattachment.
- Without Insurance: This is a more involved procedure, usually done over multiple appointments (e.g., one quadrant at a time). The cost can range from $250 to $600 per quadrant, or $1,000 to $2,400 for the full mouth.
- With Insurance: Deep cleanings are usually considered a "basic" or "major" procedure. Insurance typically covers 50-80% of the cost, after a deductible. You will likely have a higher out-of-pocket expense compared to a standard cleaning.
-
Other Related Costs (if applicable):
- Initial Exam/Consultation: $50-$150 (often included with a cleaning, or partially covered by insurance).
- Dental X-rays: $25-$150 (depending on type and number, usually covered under preventive care).
- Antiseptic Mouthwash (Prescription): $15-$40 per bottle (chlorhexidine, not always covered by dental insurance, may be covered by medical insurance if prescribed).
Insurance Coverage Details
- Preventive Care: Most dental insurance plans emphasize preventive care, covering regular check-ups, cleanings, and X-rays at a high percentage (80-100%). This is because preventing problems is far less costly than treating them.
- Basic vs. Major Services: If gingivitis has progressed to require a deep cleaning (scaling and root planing), it moves into the "basic" or sometimes "major" services category. This means your insurance might cover a lower percentage (e.g., 50-80%) and you'll likely have to pay a deductible and a co-insurance amount.
- Waiting Periods: Some dental insurance plans have waiting periods (e.g., 3-6 months) before they will cover basic or major services. Preventive care is usually covered immediately.
- Annual Maximums: Most dental insurance plans have an annual maximum benefit (e.g., $1,000-$2,000). Once you reach this limit, you are responsible for 100% of any further dental costs for that year.
- HSA/FSA: If you have a Health Savings Account (HSA) or Flexible Spending Account (FSA), you can use these tax-advantaged accounts to pay for dental treatments, including gingivitis care, examinations, and cleanings.
Cost-Saving Tips
- Preventive Care: The best way to save money is to prevent gingivitis altogether through excellent home care and regular check-ups. Catching it early means simpler, less expensive treatment.
- Understand Your Plan: Familiarize yourself with your dental insurance policy's coverage details, deductibles, co-pays, and annual maximums.
- Ask for an Estimate: Before any treatment, ask your dental office for a detailed estimate of costs and how much your insurance is expected to cover.
- Dental Savings Plans: If you don't have insurance, consider a dental savings plan. These are subscription services that offer discounts (typically 10-60%) on dental procedures at participating dentists.
- Payment Plans: Many dental offices offer in-house payment plans or work with third-party financing companies (like CareCredit) to help you manage costs over time, often with low or no interest options.
- Dental Schools: Dental schools often offer treatments at a reduced cost, as procedures are performed by students under the supervision of experienced faculty.
By being proactive about your oral health and understanding your financial options, you can ensure that gingivitis is treated effectively and affordably.
Recovery and Aftercare
The journey to healthy gums doesn't end after your professional dental cleaning. The recovery phase is relatively quick for gingivitis, but sustained aftercare is paramount to prevent recurrence.
Immediate Post-Cleaning
- Mild Sensitivity: It's common to experience some mild gum tenderness, sensitivity to hot or cold, or slight bleeding for a day or two after a thorough professional cleaning, especially if there was significant tartar buildup and inflammation. This is a normal part of the healing process as your gums recover.
- Over-the-Counter Pain Relief: If you experience discomfort, over-the-counter pain relievers like ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) can help.
- Soft Diet: For the first 24 hours, you might prefer to stick to softer foods to avoid irritating sensitive gums.
- Avoid Irritants: Steer clear of extremely hot, cold, spicy, or acidic foods and beverages for a day or two. Also, avoid tobacco products and alcohol, as they can hinder healing.

Ongoing Aftercare: The Key to Long-Term Gum Health
The most critical aspect of aftercare for gingivitis is a consistent and effective daily oral hygiene routine.
-
Brush Twice Daily:
- Use a soft-bristled toothbrush (manual or electric) and a fluoride toothpaste.
- Brush for at least two minutes each time, covering all tooth surfaces and the gum line.
- Angle the brush at 45 degrees to the gum line, gently sweeping away plaque. Avoid aggressive scrubbing, which can damage gums.
- Replace your toothbrush every 3-4 months, or sooner if the bristles are frayed.
-
Floss Daily:
- Flossing is essential to remove plaque and food particles from between your teeth and beneath the gum line, areas your toothbrush can't reach.
- Use an 18-inch piece of floss, winding most of it around your middle fingers.
- Gently guide the floss between your teeth, making a "C" shape around each tooth, and gently slide it up and down against the tooth surface, going slightly below the gum line. Use a clean section of floss for each tooth.
- If traditional floss is difficult, consider interdental brushes, dental picks, or a water flosser as alternatives.
-
Use an Antiseptic Mouthwash (Optional but Recommended):
- Your dentist might recommend an over-the-counter antiseptic rinse (containing ingredients like cetylpyridinium chloride or essential oils) to help reduce bacterial plaque.
- If gingivitis was more severe, a prescription chlorhexidine gluconate (CHX) rinse might be prescribed for short-term use. Follow your dentist's instructions carefully, as CHX can cause temporary staining with prolonged use.
-
Maintain a Healthy Diet:
- Limit sugary snacks and drinks, as sugar feeds the bacteria that form plaque.
- Eat a balanced diet rich in fruits, vegetables, and lean proteins to support overall health, including gum tissue.
-
Avoid Tobacco Products:
- Smoking and other tobacco use significantly increase the risk of gum disease and hinder healing. Quitting is one of the most beneficial steps for your oral and general health.
Follow-up Dental Appointments
- Regular Check-ups: Continue to visit your dentist for routine check-ups and professional cleanings typically every six months. These appointments are crucial for monitoring your gum health, removing any new plaque or tartar buildup, and reinforcing good oral hygiene habits.
- Adjustments: Your dentist can adjust your oral hygiene routine or recommend additional tools if needed based on your progress.
Pro Tip: Look at your gums regularly in the mirror. They should be pink, firm, and not bleed when you brush. If you notice any redness, swelling, or bleeding returning, don't wait for your next scheduled appointment – contact your dentist promptly. Early intervention is key.
Prevention
Preventing gingivitis is largely straightforward and involves consistent, effective oral hygiene practices combined with regular professional dental care. It's much easier and less costly to prevent gingivitis than to treat it once it develops.
1. Excellent Oral Hygiene Practices
This is the cornerstone of gingivitis prevention.
- Brush Twice Daily: Use a soft-bristled toothbrush (manual or electric) and fluoride toothpaste. Brush for at least two minutes each time, covering all surfaces of your teeth and gently along the gum line. Angle the bristles at a 45-degree angle to the gumline to sweep away plaque. The ADA recommends soft bristles to prevent gum damage.
- Floss Daily: Flossing is crucial for removing plaque and food particles from between your teeth and under the gum line, areas a toothbrush cannot reach. Make sure to use a fresh section of floss for each tooth and form a "C" shape around the tooth, gently sliding it up and down.
- Use Antiseptic Mouthwash: Consider using an antimicrobial mouthwash (e.g., containing cetylpyridinium chloride or essential oils) as an adjunct to brushing and flossing. It can help reduce bacteria that cause plaque and gingivitis.
- Tongue Cleaning: Brushing or scraping your tongue can remove bacteria that contribute to bad breath and oral biofilm.
2. Regular Dental Check-ups and Professional Cleanings
- Semi-Annual Visits: Schedule professional dental cleanings and check-ups at least every six months, or more frequently if recommended by your dentist due to specific risk factors.
- Plaque and Tartar Removal: Dental hygienists remove hardened plaque (tartar) that cannot be removed by brushing and flossing alone. They also polish your teeth, making it harder for plaque to adhere.
- Early Detection: Your dentist can spot early signs of gingivitis or other oral health issues before they become serious, allowing for timely intervention.
3. Healthy Lifestyle Choices
- Balanced Diet: Limit sugary and starchy foods and drinks. These provide fuel for plaque-forming bacteria. Instead, choose a diet rich in fruits, vegetables, and whole grains, which support overall health and a strong immune system.
- Avoid Tobacco Products: Smoking and other forms of tobacco use are major risk factors for gingivitis and periodontal disease. Quitting tobacco significantly reduces your risk.
- Manage Stress: Chronic stress can compromise your immune system, potentially making you more susceptible to infections, including gum disease.
- Stay Hydrated: Drinking plenty of water helps wash away food particles and bacteria, and promotes saliva flow, which neutralizes acids.
4. Address Contributing Factors
- Control Systemic Diseases: If you have conditions like diabetes, work closely with your physician to manage it effectively. Good blood sugar control is vital for gum health.
- Review Medications: Discuss any medications you are taking with your dentist, especially if they cause dry mouth or gingival overgrowth. They may suggest strategies to mitigate these side effects.
- Correct Dental Problems: Address crowded teeth, crooked teeth, or ill-fitting dental restorations with your dentist. These conditions can create areas that trap plaque and make effective cleaning difficult. Orthodontic treatment or restorative work can help.
By diligently following these preventive measures, you can significantly reduce your risk of developing gingivitis and maintain a healthy, beautiful smile for years to come.
Risks and Complications
While gingivitis is the mildest form of gum disease and fully reversible, ignoring it carries significant risks, potentially leading to more severe and irreversible oral health problems, and even impacting systemic health.
1. Progression to Periodontitis
This is the most serious and common complication of untreated gingivitis.
- Destruction of Supporting Structures: If the inflammation from gingivitis is left unchecked, the bacterial infection can spread deeper beneath the gum line. It begins to break down the bone and connective tissues that hold your teeth in place.
- Pocket Formation: The gums pull away from the teeth, forming "periodontal pockets" where more plaque, tartar, and bacteria can accumulate, deepening the infection.
- Irreversible Damage: Unlike gingivitis, the bone loss and tissue damage associated with periodontitis are irreversible. While treatment can halt progression, the lost bone and tissue generally cannot be fully regenerated naturally.
- Tooth Loosening and Loss: As periodontitis advances, the supporting bone and ligaments are severely weakened, causing teeth to become loose, shift, and eventually fall out or require extraction.
2. Abscess Formation
- In severe cases, deep pockets filled with bacteria and debris can become infected, leading to the formation of a painful gum abscess (a localized collection of pus). This requires immediate dental attention, often involving drainage and antibiotics.
3. Increased Risk of Other Oral Issues
- Increased Decay: Inflamed gums can recede, exposing the root surfaces of teeth. Root surfaces are softer than enamel and more susceptible to cavities.
- Halitosis (Severe Bad Breath): Chronic inflammation and bacterial accumulation significantly contribute to persistent and often severe bad breath.
4. Systemic Health Implications
The link between oral health and overall systemic health is well-established. Untreated gum disease, particularly periodontitis, has been associated with:

- Cardiovascular Disease: The inflammation and bacteria from infected gums can enter the bloodstream, potentially contributing to the development of atherosclerosis (hardening of the arteries), increasing the risk of heart attack and stroke.
- Diabetes: There's a bidirectional relationship between gum disease and diabetes. People with diabetes are more susceptible to gum disease, and severe gum disease can make it harder to control blood sugar levels.
- Respiratory Diseases: Oral bacteria can be aspirated into the lungs, potentially leading to respiratory infections like pneumonia, especially in older adults or those with weakened immune systems.
- Adverse Pregnancy Outcomes: Pregnant women with periodontitis may have an increased risk of preterm birth and low birth weight babies.
- Other Conditions: Emerging research suggests potential links between periodontal disease and other systemic conditions such as rheumatoid arthritis, kidney disease, certain cancers, and even Alzheimer's disease.
The financial and emotional toll of treating advanced periodontal disease, including potential tooth loss and the need for complex restorative procedures like implants, is far greater than the effort and cost of preventing and treating gingivitis. This underscores why early detection and consistent care are so vital.
``
Children / Pediatric Considerations
Gingivitis is not exclusive to adults; it can affect children and adolescents as well. While often milder, it's crucial for parents to be aware of the signs and encourage good oral hygiene from an early age to prevent more serious issues.
Prevalence in Children
Studies indicate that gingivitis is quite common in children, with prevalence rates varying but often starting in the preschool years and increasing during puberty. The main cause, similar to adults, is the accumulation of bacterial plaque.
Causes and Contributing Factors Unique to Children
- Ineffective Brushing/Flossing: Children may lack the dexterity or motivation to brush and floss thoroughly. They often miss areas, especially around the gum line and posterior teeth.
- Poor Diet: Diets high in sugary snacks and drinks contribute significantly to plaque formation.
- Orthodontic Appliances: Braces, retainers, and other orthodontic devices create additional surfaces where plaque can accumulate, making cleaning more challenging. "Orthodontic gingivitis" is a common concern.
- Hormonal Changes During Puberty: Similar to pregnancy gingivitis, the hormonal surges during puberty can make a teenager's gums more reactive to plaque, leading to increased inflammation even with moderate plaque levels.
- Mouth Breathing: Children who habitually breathe through their mouth (e.g., due to allergies, enlarged tonsils/adenoids) can experience dry gums, particularly in the upper front teeth area, which can contribute to inflammation.
- Eruption Gingivitis: As permanent teeth erupt, the surrounding gum tissue can become temporarily inflamed, making it more susceptible to plaque buildup.
Signs and Symptoms in Children
The signs are similar to adults:
- Red, swollen, or puffy gums.
- Gums that bleed easily during brushing or flossing.
- Bad breath (halitosis).
- Gums that appear shiny or tender.
Parents might notice their child avoiding brushing certain areas due to discomfort, or complaining of a bad taste in their mouth.
Treatment for Children
Treatment for gingivitis in children mirrors that for adults, focusing on plaque removal and improved hygiene.
- Professional Dental Cleaning: Regular dental check-ups and cleanings (every 6 months) are vital. The dental hygienist can effectively remove plaque and tartar and provide tailored advice.
- Parental Involvement and Supervision:
- Toddlers and Young Children: Parents should brush their child's teeth (or assist them) until they develop sufficient dexterity, usually around 6-8 years old.
- Older Children and Teens: Supervise their brushing and flossing to ensure they are using proper technique and doing it thoroughly.
- Oral Hygiene Education: Educate children about the importance of good oral hygiene in an age-appropriate manner. Make it fun!
- Dietary Modifications: Limit sugary and processed foods. Encourage water consumption.
- Orthodontic Care: For children with braces, extra attention to cleaning around brackets and wires is essential. Your orthodontist or general dentist can recommend specialized tools like interdental brushes or water flossers.
- Addressing Underlying Issues: If mouth breathing is a factor, consult with a pediatrician or ENT specialist.
Pro Tip for Parents: Make brushing and flossing a routine, fun activity. Use disclosing tablets occasionally to show children where they're missing plaque. Lead by example and brush and floss with your child! Early habits are critical for lifelong oral health.
Cost Breakdown
A detailed look at the typical costs associated with gingivitis care in the US helps in financial planning. These are average ranges, and actual costs can vary significantly based on location, dentist's fees, and individual patient needs.
Average US Costs for Common Gingivitis-Related Procedures
| Procedure | Description | Average Cost (Without Insurance) | Average Cost (With Insurance - Patient Portion) |
|---|---|---|---|
| D0120: Periodic Oral Evaluation | Routine check-up, oral exam by dentist. | $50 - $100 | $0 - $20 (often 100% covered) |
| D0150: Comprehensive Oral Evaluation | Initial extensive exam for new patients or complex cases. | $75 - $150 | $0 - $30 (often 100% covered) |
| D0210: Full Mouth X-rays | Set of X-rays to see all teeth and surrounding bone. | $100 - $200 | $0 - $40 (often 100% covered, once every 3-5 years) |
| D0274: Bitewing X-rays (4 films) | Standard set of X-rays to check for cavities between teeth. | $50 - $100 | $0 - $20 (often 100% covered, annually) |
| D1110: Prophylaxis (Adult Cleaning) | Routine dental cleaning to remove plaque and tartar above the gum line. | $75 - $200 | $0 - $40 (often 80-100% covered, twice annually) |
| D1120: Prophylaxis (Child Cleaning) | Routine dental cleaning for children. | $60 - $150 | $0 - $30 (often 80-100% covered, twice annually) |
| D4346: Scaling in Presence of GINGIVAL INFLAMMATION | Code specifically for patients with moderate to severe gingival inflammation but no bone loss. More extensive than prophylaxis. | $100 - $300 | $30 - $100 (variable, may be considered basic) |
| D4341: Periodontal Scaling and Root Planing (per quadrant) | "Deep Cleaning" for early to moderate periodontitis. More extensive than gingivitis treatment. | $250 - $600 per quadrant | $50 - $200 per quadrant (50-80% covered, after deductible) |
| Prescription Mouthwash (e.g., Chlorhexidine) | If prescribed for specific bacterial control. | $15 - $40 | Varies (often not covered by dental, may be by medical) |
Note: The codes (e.g., D0120) are ADA procedure codes often used for insurance claims.
With vs. Without Insurance
- Without Insurance: You will pay the full cost out-of-pocket for each service. This can add up quickly, especially if multiple visits or procedures are needed.
- With Insurance: Dental insurance typically covers a significant portion of preventive services (exams, cleanings, routine X-rays) – often 80-100%. For basic services (like more extensive cleanings for moderate gingivitis or early periodontitis), coverage might be 50-80% after you meet your deductible. Always verify your specific plan benefits before treatment.
Payment Plans and Financing Options
Many dental practices understand the financial burden of dental care and offer solutions:
- In-house Payment Plans: Some offices allow patients to pay for services over several months, often without interest, directly through the practice.
- Third-Party Financing: Companies like CareCredit are popular options. They offer special financing options, including interest-free periods if the balance is paid within a set timeframe (e.g., 6, 12, or 18 months). Interest rates can be high if the balance isn't paid off within the promotional period.
- Dental Savings Plans: These are not insurance but membership programs where you pay an annual fee and receive discounted rates on dental services from participating providers. Discounts can range from 10% to 60%. This can be a good option for those without traditional dental insurance.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have access to these through your employer, you can use pre-tax dollars to pay for qualified dental expenses, including exams, cleanings, and gingivitis treatments.
Cost-Saving Tips
- Prioritize Prevention: The most cost-effective approach is preventing gingivitis. Regular brushing, flossing, and semi-annual cleanings prevent the need for more expensive treatments.
- Max Out Preventive Benefits: If you have insurance, make sure to utilize your two covered cleanings and annual X-rays each year.
- Ask About Bundled Services: Sometimes, an initial exam and X-rays are included or discounted when bundled with a cleaning for new patients.
- Compare Prices: Don't hesitate to call a few dental offices in your area to inquire about their fees for a basic cleaning and exam, especially if you're paying out-of-pocket.
- Dental Schools: As mentioned, dental schools often offer high-quality care at significantly reduced prices, though appointments may take longer.
By being informed and proactive, you can manage the costs associated with gingivitis treatment and maintain your oral health effectively.
Frequently Asked Questions
What is the main cause of gingivitis?
The primary cause of gingivitis is the accumulation of bacterial plaque on your teeth and around the gum line. If this sticky film of bacteria isn't removed through regular brushing and flossing, it can harden into tartar, further irritating the gums and leading to inflammation.

Is gingivitis contagious?
No, gingivitis is not contagious. It is caused by an overgrowth of bacteria naturally present in your mouth and your body's inflammatory response to that bacteria and its byproducts, not by a specific infectious agent that can be spread from person to person.
How long does it take to get rid of gingivitis?
With professional dental cleaning and consistent, improved home oral hygiene, the signs of gingivitis (like bleeding and inflammation) typically begin to resolve within 1-2 weeks. Complete resolution and restoration of gum health usually occur within several weeks to a month.
Is gingivitis painful?
Gingivitis is often painless, especially in its early stages. This lack of pain is one reason many people don't realize they have it. However, as it progresses, gums can become tender, swollen, and mildly uncomfortable, particularly when brushing or eating.
Can gingivitis be completely reversed?
Yes, absolutely. Gingivitis is the only stage of gum disease that is fully reversible. With proper treatment, which includes professional cleaning and diligent daily oral hygiene, the gums can return to a completely healthy state without any lasting damage.
What happens if gingivitis is left untreated?
If left untreated, gingivitis can progress to periodontitis, a more severe form of gum disease. Periodontitis leads to the irreversible destruction of the bone and tissues supporting your teeth, forming pockets, causing teeth to loosen, and potentially leading to tooth loss. It can also impact overall systemic health.
Can I treat gingivitis at home without seeing a dentist?
While excellent home oral hygiene (brushing and flossing twice daily) is crucial for managing and preventing gingivitis, it's difficult to reverse existing gingivitis without professional help. A dentist or hygienist needs to remove hardened tartar (calculus) that home care cannot, which is often a major contributor to inflammation.
How much does it cost to treat gingivitis?
The primary treatment for gingivitis is a professional dental cleaning (prophylaxis). Without insurance, this typically costs between $75 and $200. Most dental insurance plans cover 80-100% of preventive care like cleanings, making the out-of-pocket cost minimal or zero.
Does pregnancy cause gingivitis?
Pregnancy itself doesn't cause gingivitis, but hormonal changes during pregnancy (increased progesterone and estrogen) can make a pregnant woman's gums more sensitive and reactive to the plaque bacteria, leading to a condition known as "pregnancy gingivitis." Good oral hygiene remains critical.
What's the difference between gingivitis and periodontitis?
Gingivitis is the early, mildest, and reversible stage of gum disease, involving only inflammation of the gum tissue without bone loss. Periodontitis is a more advanced, irreversible stage where the inflammation has spread, leading to the destruction of the bone and ligaments that support the teeth, resulting in pocket formation and potential tooth loss.
When to See a Dentist
Knowing when to seek professional dental care is crucial for managing gingivitis and preventing its progression. While routine check-ups are always recommended, certain signs warrant prompt attention.
Red Flags: See a Dentist Soon
You should make an appointment to see your dentist without delay if you experience any of the following:
- Persistent Bleeding Gums: If your gums bleed consistently when you brush, floss, or even spontaneously, this is the most common and clear indicator of gingivitis. Don't dismiss it as normal.
- Red, Swollen, or Puffy Gums: If your gums appear noticeably redder, swollen, or feel puffy and tender compared to their usual firm, pink state.
- Chronic Bad Breath (Halitosis): If you have persistent bad breath that doesn't improve with brushing and mouthwash, it could be a sign of bacterial accumulation and gum inflammation.
- Receding Gums: If you notice your gums pulling away from your teeth, making your teeth appear longer. This can be a sign of more advanced gum disease, but can also start with gingivitis.
- Loose Teeth or Changes in Bite: While typically a sign of periodontitis, any feeling of loose teeth or changes in how your teeth fit together (malocclusion) is a serious red flag requiring immediate evaluation.
- Pus Around Teeth or Gums: The presence of pus indicates an active infection (abscess) and requires urgent dental care.
- Pain or Tenderness in Gums: Although gingivitis is often painless, any increasing discomfort, tenderness, or pain in your gums should be checked.
Routine Care Guidance
Even if you don't experience the above red flags, regular dental visits are paramount for prevention and early detection:
- Every Six Months for Check-ups and Cleanings: The American Dental Association (ADA) recommends professional dental check-ups and cleanings at least twice a year. These routine visits allow your dentist and hygienist to:
- Monitor your overall oral health.
- Identify and remove plaque and tartar buildup that you can't manage at home.
- Catch early signs of gingivitis or other dental problems before they become severe and more difficult (and expensive) to treat.
- Provide personalized oral hygiene instruction and product recommendations.
Emergency vs. Scheduled Appointment
- Emergency: Any severe, acute pain, signs of abscess (pus, severe swelling, fever), or rapidly worsening symptoms (like sudden tooth mobility) warrant calling your dentist for an emergency appointment or seeking urgent care.
- Scheduled Appointment: For general bleeding, redness, or swelling of the gums without severe pain or signs of acute infection, a scheduled appointment within a few days to a week is usually appropriate. However, don't postpone it indefinitely. The sooner gingivitis is addressed, the easier and more effective the treatment will be.
Remember, your gums are the foundation of your smile and crucial for your overall health. Being proactive about their care and knowing when to consult a dental professional is the best way to maintain a healthy, vibrant smile.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
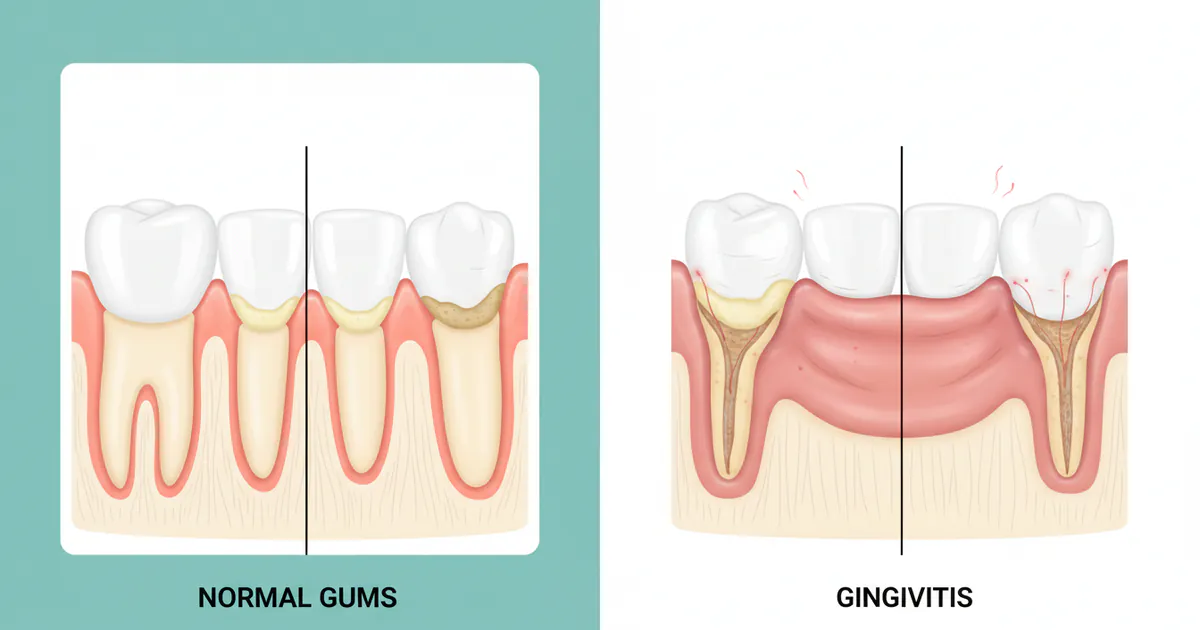
Normal Gums vs Gingivitis: Complete Comparison Guide
Did you know that nearly half of American adults over 30 show signs of gum disease, a condition that can range from mild inflammation to severe infection leading to tooth loss? Understanding the difference between healthy gums and those affected by early gum disease, known as gingivitis, is cruc
February 22, 2026
Can You Get Rid of Gingivitis
More than 50% of American adults aged 30 or older suffer from some form of gum disease, with gingivitis being the earliest and most common stage. This often silent condition, marked by inflammation of the gums, can seem daunting, leading many to wonder: can you get rid of gingivitis? The good ne
February 22, 2026
What Causes Receding Gums
Receding gums, a condition where the gum tissue surrounding the teeth pulls back or wears away, exposing more of the tooth or the tooth's root, affects a significant portion of the adult population in the United States. In fact, estimates suggest that **up to 88% of people over the age of 65 have on
February 22, 2026
Signs of Gingivitis: Complete Guide
Did you know that nearly half of American adults aged 30 and older suffer from some form of gum disease? While that statistic might sound alarming, the good news is that the earliest and most common stage, gingivitis, is entirely reversible. Recognizing the signs of gingivitis early is your
February 22, 2026