Complete Guide to Oral-Systemic Health: Everything You Need to Know

Key Takeaways
- Did you know that 90% of all systemic diseases have oral manifestations? Your mouth is often the first place to show signs of trouble elsewhere in your body, and conversely, the health of your mouth can profoundly impact your overall well-being. This interconnected relationship, known as oral-sy
Complete Guide to Oral-Systemic Health: Everything You Need to Know
Did you know that 90% of all systemic diseases have oral manifestations? Your mouth is often the first place to show signs of trouble elsewhere in your body, and conversely, the health of your mouth can profoundly impact your overall well-being. This interconnected relationship, known as oral-systemic health, is far more significant than many realize. It's not just about brushing and flossing to prevent cavities; it’s about understanding how conditions like diabetes, heart disease, pregnancy, and even osteoporosis are intimately linked with your oral cavity-conditions-diseases-everything-you-need-to-know "Complete Guide to Dental Conditions & Diseases: Everything You Need to Know"). Ignoring this connection can lead to serious health consequences, from worsening chronic conditions to increasing your risk for new ones.

At SmilePedia.net, we believe that empowering you with knowledge is key to a healthier life. This comprehensive guide will delve deep into the fascinating and crucial world of oral-systemic health. We'll explore what it means, uncover the intricate pathways that connect your mouth to the rest of your body, discuss specific conditions like diabetes and teeth health, highlight the pervasive impact of inflammation of the gums and mouth inflammation, and provide actionable advice on how to protect both your smile and your health. Get ready to transform your understanding of what true health really means.
Key Takeaways:
- Oral-systemic health describes the bidirectional link between your oral health and your overall bodily health. Conditions like diabetes, heart disease, and pregnancy significantly impact your mouth, and oral infections can affect systemic health.
- Inflammation is the primary bridge: Chronic oral inflammation, especially periodontitis (gum disease), can release bacteria and inflammatory mediators into your bloodstream, exacerbating or initiating systemic conditions.
- Diabetes and teeth are deeply connected: Individuals with diabetes are 3-4 times more likely to develop severe gum disease, and gum disease can make it harder to control blood sugar levels. They also commonly experience diabetes and dry mouth.
- Prevention is paramount and cost-effective: Regular brushing, flossing, and dental check-ups (typically every 6 months) are crucial. A routine cleaning usually costs $75-$200 without insurance, significantly less than advanced treatments.
- Common oral issues with systemic links: Inflammation of the gums (gingivitis), inflammation of the mouth (stomatitis), and inflammation of tooth pulp (pulpitis) are warning signs. Untreated, these can lead to more serious systemic complications.
- Treatment costs vary: A non-surgical deep cleaning (scaling and root planing) for moderate gum disease can range from $250-$800 per quadrant. Root canal therapy for inflammation of tooth pulp costs $700-$2,000 for front teeth and $1,000-$2,500 for molars, often taking 1-2 appointments.
- Timelines for recovery: Gingivitis often resolves within 1-2 weeks with improved hygiene. Periodontitis treatment can take several months of active therapy and ongoing maintenance appointments.
Understanding Oral-Systemic Health: The Bidirectional Link
The concept of oral-systemic health recognizes that your mouth is not an isolated entity but an integral part of your body. What happens in your mouth can affect your entire system, and conversely, your overall health can manifest in your oral cavity. This bidirectional relationship means that neglecting your oral health can have far-reaching consequences for your general well-being, and managing systemic conditions is crucial for maintaining a healthy mouth.
What is Oral-Systemic Health?
Simply put, oral-systemic health is the medical understanding that the health of your mouth, teeth, and gums is intrinsically linked to the health of your entire body. It’s a holistic view that challenges the historical separation of dental and medical care, emphasizing that oral health is a vital component of overall health. This connection is primarily mediated by bacteria, inflammation, and immune responses.
Why Does Your Mouth Matter So Much?
Your mouth is a gateway to your body, teeming with bacteria – both beneficial and harmful. When oral hygiene is neglected, harmful bacteria can proliferate, leading to infections and inflammation. This is where the profound impact on systemic health begins:
- Inflammation as a Bridge: Chronic inflammation, particularly from gum disease (periodontitis), is a key driver in the oral-systemic link. When your gums are inflamed, the body's immune response triggers inflammatory mediators (cytokines, C-reactive protein) that can travel through the bloodstream. These systemic inflammatory responses can contribute to conditions like atherosclerosis (hardening of the arteries) and increase insulin resistance.
- Bacterial Pathways: Oral bacteria from infections like periodontitis can enter the bloodstream, especially during chewing, brushing, or dental procedures. Once in the bloodstream, these bacteria can travel to distant organs, potentially contributing to infections in the heart (infective endocarditis), lungs, or even prosthetic joints.
- Shared Risk Factors: Many lifestyle factors contribute to both poor oral health and systemic diseases. Smoking, unhealthy diets high in sugar, stress, and lack of exercise are common culprits that weaken the immune system and foster both oral and systemic health problems.
- Genetic Predispositions: Certain genetic factors can make individuals more susceptible to both periodontal disease and systemic conditions, highlighting an underlying biological link.
``
Key Systemic Conditions and Their Oral Manifestations
Numerous systemic conditions have a direct and often profound impact on oral health, and vice versa. Understanding these specific connections is vital for comprehensive health management.
Diabetes and Oral Health
The link between diabetes and teeth health is one of the most well-established oral-systemic connections. Diabetes, a chronic metabolic disease characterized by high blood sugar levels, significantly increases the risk and severity of several oral health problems.
- Periodontal Disease: Individuals with diabetes are three to four times more likely to develop periodontitis (severe gum disease), and it tends to be more aggressive. High blood sugar levels impair the body's ability to fight infection and heal, making diabetic patients more susceptible to bacterial overgrowth and chronic inflammation of the gums. Periodontitis, in turn, can make blood sugar control more difficult, creating a vicious cycle. The chronic inflammation from gum disease can increase systemic insulin resistance, making it harder for the body to utilize insulin effectively.
- Diabetes and Dry Mouth (Xerostomia): High blood sugar levels can lead to nerve damage and affect salivary glands, resulting in reduced saliva flow. Diabetes and dry mouth is a very common complaint. Saliva is crucial for washing away food particles, neutralizing acids, and fighting bacteria. A lack of saliva increases the risk of tooth decay (cavities), gum disease, and oral thrush (candidiasis).
- Increased Risk of Infection: Diabetics have a compromised immune system, making them more prone to oral infections like candidiasis (oral thrush), which presents as white patches on the tongue and inner cheeks.
- Delayed Healing: After dental procedures like extractions or oral surgery, wound healing can be significantly slower in individuals with uncontrolled diabetes, increasing the risk of post-operative complications.
- Burning Mouth Syndrome: Some diabetic patients experience a persistent burning sensation in the mouth, tongue, or lips.
Cardiovascular Disease and Oral Health
The connection between gum disease and heart disease has been extensively researched. While a direct causal link is still debated, the correlation is strong, and the underlying mechanisms involve systemic inflammation.
- Systemic Inflammation: The chronic inflammation of the gums associated with periodontitis releases inflammatory chemicals into the bloodstream. These chemicals can contribute to the formation of plaque in the arteries (atherosclerosis), a key risk factor for heart attacks and strokes.
- Bacterial Invasion: Oral bacteria from infected gums can enter the bloodstream and attach to fatty plaques in the arteries, potentially contributing to clot formation and further inflammation. Studies have found oral bacteria DNA in arterial plaques.
- Infective Endocarditis: For individuals with certain heart conditions (e.g., artificial heart valves), oral bacteria entering the bloodstream can cause infective endocarditis, a serious infection of the heart's inner lining.
Pregnancy and Oral Health
Pregnancy and teeth health require special attention. Hormonal changes during pregnancy make expectant mothers more susceptible to certain oral health issues, which can, in turn, affect pregnancy outcomes.
- Pregnancy Gingivitis: This is the most common oral condition during pregnancy, affecting 60-75% of pregnant women. Increased progesterone levels lead to exaggerated responses to plaque bacteria, causing swollen, tender, and bleeding gums (inflammation of the gums).
- Periodontitis: Untreated pregnancy gingivitis can progress to periodontitis. Some research suggests a link between severe periodontitis in pregnant women and adverse outcomes such as preterm birth and low birth weight, though more research is needed to establish causality.
- Morning Sickness and Erosion: Frequent vomiting associated with morning sickness exposes teeth to stomach acid, which can erode tooth enamel.
- Cavity Risk: Dietary changes and cravings, coupled with potential neglect of oral hygiene due to nausea or fatigue, can increase the risk of cavities.
Pro Tip: If you're pregnant or planning a pregnancy, inform your dentist. Regular check-ups and cleanings are safe and highly recommended during pregnancy to prevent and manage these issues.
Osteoporosis and Oral Health
Does osteoporosis affect your teeth? The answer is yes, indirectly but significantly. Osteoporosis, a condition characterized by progressive bone density loss, primarily affects skeletal bones but can also impact the bones supporting your teeth.
- Jawbone Loss: Osteoporosis can lead to a reduction in the density of the alveolar bone, which anchors your teeth. This bone loss can result in tooth loosening and increased risk of tooth loss.
- Denture Instability: For those with dentures, reduced jawbone density can lead to ill-fitting and uncomfortable dentures, making eating and speaking difficult.
- Medication-Related Osteonecrosis of the Jaw (MRONJ): A serious but rare complication, especially for patients taking bisphosphonates (medications for osteoporosis) who undergo oral surgery (like tooth extraction). This condition involves the death of jawbone tissue.
Respiratory Diseases and Oral Health
Oral bacteria can play a role in the development or exacerbation of respiratory conditions.
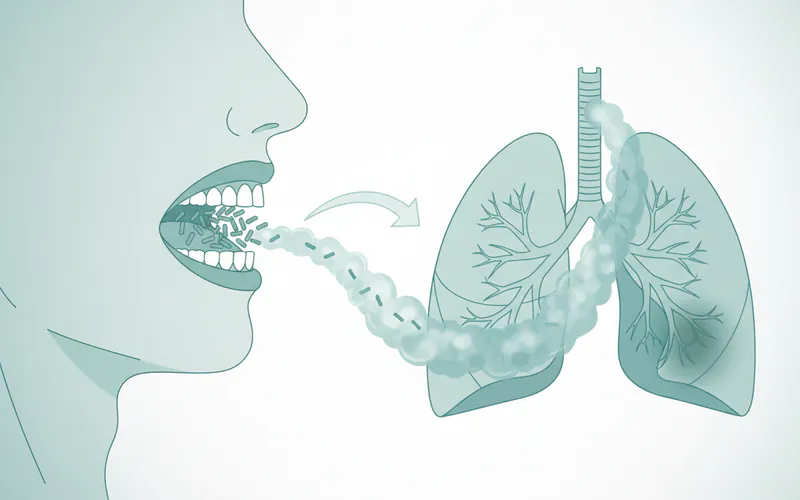
- Aspiration Pneumonia: For individuals with compromised immune systems, reduced salivary flow, or difficulty swallowing, bacteria from the mouth can be aspirated (inhaled) into the lungs, leading to aspiration pneumonia, particularly in hospital settings or among the elderly.
- Exacerbation of COPD: Chronic obstructive pulmonary disease (COPD) can be worsened by oral infections.
Autoimmune Diseases and Oral Health
Many autoimmune conditions manifest in the mouth, often causing significant discomfort and increasing the risk of dental problems.
- Sjögren's Syndrome: This autoimmune disorder primarily affects moisture-producing glands, leading to severe diabetes and dry mouth (xerostomia) and dry eyes. This drastically increases the risk of cavities and oral infections.
- Lupus, Crohn's Disease, Pemphigus, Pemphigoid: These conditions can cause oral lesions, ulcers, or burning sensations, contributing to overall mouth inflammation.
Cancer Treatment and Oral Health
Treatments for cancer, particularly chemotherapy and radiation to the head and neck, can have severe oral side effects.
- Oral Mucositis: This painful inflammation of the mouth lining is a common side effect, causing ulcers and making eating, swallowing, and speaking difficult.
- Xerostomia: Chemotherapy and radiation can damage salivary glands, leading to chronic dry mouth, increasing the risk of cavities and infections.
- Osteoradionecrosis: A severe complication of radiation to the jaw, where bone tissue dies, often triggered by tooth extraction.
- Taste Changes: Dysgeusia (altered taste) is common during and after cancer treatment.
The Pervasive Threat of Inflammation
Inflammation is the body's natural response to injury or infection. While acute inflammation is protective, chronic inflammation, especially in the mouth, can become a destructive force, driving many of the oral-systemic connections.
Inflammation of the Gums (Gingivitis)
Gingivitis is the earliest and mildest form of periodontal disease, characterized by inflammation of the gums.
- Causes: Primarily caused by plaque buildup – a sticky film of bacteria that constantly forms on your teeth. Poor oral hygiene allows plaque to accumulate and calcify into tartar (calculus), which irritates the gums.
- Signs and Symptoms: Red, swollen, tender gums that bleed easily, especially during brushing or flossing. You may also notice persistent bad breath (halitosis). There is typically no bone loss at this stage.
- Treatment: Gingivitis is reversible with professional dental cleaning (prophylaxis) to remove plaque and tartar, followed by consistent daily brushing and flossing.
Periodontitis: Advanced Gum Inflammation
Untreated gingivitis can progress to periodontitis, a more severe form of gum disease where the inflammation of the gums extends below the gumline, affecting the bone and tissues supporting the teeth.
- Causes: Chronic bacterial infection and the body's inflammatory response lead to the breakdown of gum tissue and the bone supporting the teeth. Risk factors include genetics, smoking, diabetes, poor nutrition, and certain medications.
- Progression: As the disease progresses, pockets form between the teeth and gums, filling with bacteria, plaque, and tartar. These pockets deepen, leading to further bone loss and eventual tooth loosening or loss. This chronic bacterial presence contributes to systemic mouth inflammation.
- Signs and Symptoms: Swollen, bright red or purplish gums; tender or bleeding gums; persistent bad breath; pus between teeth and gums; loose teeth; painful chewing; changes in bite; receding gums, making teeth appear longer.
- Treatment: Requires more intensive treatment than gingivitis, often involving deep cleaning procedures like scaling and root planing, antibiotics, and in advanced cases, surgical interventions.
Inflammation of Tooth Pulp (Pulpitis)
The innermost part of your tooth, the pulp, contains nerves, blood vessels, and connective tissue. Inflammation of tooth pulp, or pulpitis, is a common cause of toothache.
- Causes: Primarily caused by deep tooth decay (cavities) that reaches the pulp, trauma to the tooth (a crack or fracture), or repeated dental procedures on the same tooth.
- Types:
- Reversible Pulpitis: Mild inflammation where the pulp can recover if the irritant (e.g., shallow cavity) is removed. Symptoms include sharp, short-lived pain to cold or sweet stimuli.
- Irreversible Pulpitis: Severe inflammation where the pulp cannot heal and eventually dies. Pain is often severe, prolonged, spontaneous, and may radiate. It can be triggered by heat or persist after cold stimulus is removed.
- Signs and Symptoms: Tooth sensitivity to hot, cold, or sweet; spontaneous throbbing pain; pain that wakes you up at night; pain when chewing; facial swelling; a small pimple-like bump on the gum near the affected tooth (indicating an abscess).
- Treatment: For reversible pulpitis, removing the irritant (filling a cavity) is usually sufficient. For irreversible pulpitis, root canal therapy or tooth extraction is necessary to relieve pain and prevent the spread of infection. If left untreated, the infection can spread to the jawbone, causing a dental abscess, which can further contribute to systemic inflammation of the mouth.
General Mouth Inflammation (Stomatitis)
Mouth inflammation, or stomatitis, is a broader term referring to the general inflammation of the oral mucous membranes. It can be caused by various factors, not just plaque.
- Causes:
- Infections: Viral (herpes simplex, hand, foot, and mouth disease), fungal (oral thrush), bacterial.
- Allergic Reactions: To foods, dental materials, or oral hygiene products.
- Irritants: Alcohol, tobacco, hot foods/drinks, ill-fitting dentures.
- Nutritional Deficiencies: Iron, B vitamins.
- Systemic Diseases: Autoimmune conditions (Lupus, Crohn's), cancer treatments (mucositis), medications.
- Signs and Symptoms: Redness, swelling, pain, burning sensation, ulcers, blisters, difficulty eating or speaking.
- Treatment: Depends on the underlying cause. It may involve antiviral/antifungal medications, corticosteroids, pain relievers, or addressing systemic conditions.
Recognizing the Signs: Symptoms of Oral-Systemic Issues
Paying attention to both your oral and general health symptoms is crucial for early detection and intervention.
General Oral Symptoms that could indicate Systemic Issues:
- Persistent Bad Breath (Halitosis): Can signal gum disease, dry mouth, or underlying systemic conditions like diabetes or kidney disease.
- Bleeding Gums: A primary sign of gingivitis or periodontitis, which are linked to systemic inflammation.
- Dry Mouth (Xerostomia): Often a side effect of medications, but can also be a symptom of diabetes, Sjögren's syndrome, or other autoimmune diseases.
- Loose Teeth or Changes in Bite: Indicative of advanced periodontitis or jawbone loss (potentially related to osteoporosis).
- Oral Lesions, Ulcers, or White Patches: Can be signs of autoimmune diseases, viral/fungal infections, or even oral cancer.
- Frequent Cavities: May be exacerbated by dry mouth, high sugar intake, or compromised immunity due to systemic conditions.
- Burning Sensation in the Mouth: Can be associated with diabetes, nutritional deficiencies, or certain neurological conditions.
Specific Systemic Symptoms that might Signal Oral Issues:
- Unexplained Weight Loss or Difficulty Eating: Could be due to painful oral conditions like advanced periodontitis, mucositis, or ill-fitting dentures.
- Difficulty Controlling Blood Sugar (for Diabetics): Periodontal disease can make diabetes management significantly harder.
- Chest Pain or Other Heart Symptoms: While not directly caused by oral issues, chronic inflammation from gum disease is a risk factor for cardiovascular events.
- Frequent Respiratory Infections: Can be linked to aspiration of oral bacteria in vulnerable individuals.
Diagnosis: How Your Dentist Connects the Dots
A thorough dental examination is essential for diagnosing oral-systemic health issues. Your dentist is often the first healthcare provider to identify signs of systemic disease in your mouth.
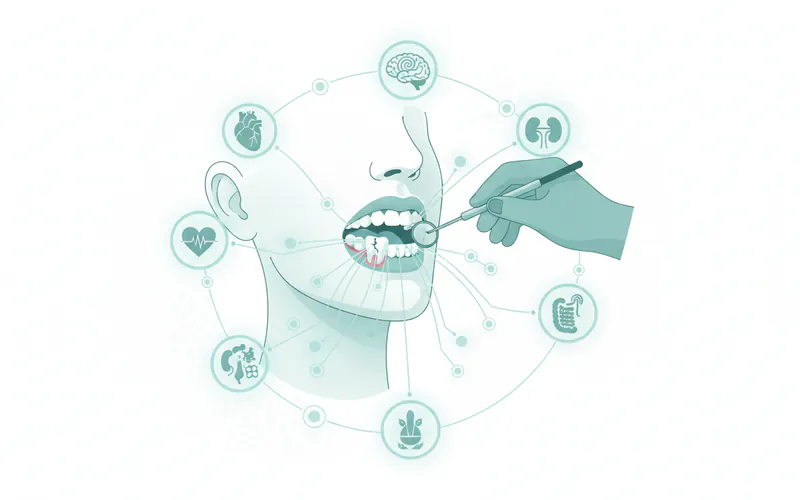
- Comprehensive Medical History: Your dentist will ask about your overall health, existing medical conditions (like diabetes, heart disease, osteoporosis), medications you are taking, and any allergies. Be honest and complete, as this information is critical.
- Oral Examination: A visual inspection of your teeth, gums, tongue, cheeks, palate, and throat. The dentist looks for signs of decay, gum inflammation, lesions, dry mouth, and other abnormalities.
- Periodontal Probing: A small probe is used to measure the depth of the pockets around your teeth. Deeper pockets (typically 4mm or more) indicate gum attachment loss and potential bone loss, key indicators of periodontitis. Bleeding upon probing is also noted.
- Dental X-rays: Periapical and bitewing X-rays show the extent of bone loss around teeth, detect cavities, and identify abscesses or other underlying bone issues. A panoramic X-ray provides a broader view of the entire jaw.
- Salivary Flow Assessment: If dry mouth is suspected, your dentist may assess your salivary flow rate.
- Screening for Oral Cancer: Your dentist will perform a visual and tactile examination of your mouth and neck to check for any suspicious lumps, lesions, or changes in tissue texture.
- Discussion and Referral: If your dentist identifies oral manifestations of a systemic disease or suspects an underlying medical condition, they will discuss their findings with you and may recommend a consultation with your physician or a specialist.
Comprehensive Treatment Options
Treating oral-systemic health issues often requires a collaborative approach between your dentist and your medical doctor. The goal is to address both the oral symptoms and the underlying systemic condition.
Addressing Periodontal Disease
Treatment for inflammation of the gums (gingivitis) and periodontitis aims to remove bacteria, reduce inflammation, and prevent further damage.
- Scaling and Root Planing (Deep Cleaning): This non-surgical procedure involves meticulously removing plaque and tartar from above and below the gumline (scaling) and smoothing the root surfaces (root planing) to eliminate bacterial toxins. This often requires local anesthesia and is performed over one to four appointments, depending on the severity.
- Antibiotics: Oral antibiotics or topical antibiotic gels/chips placed directly into periodontal pockets may be used to control bacterial infection, especially in conjunction with scaling and root planing.
- Laser Therapy: Some dentists use lasers to remove inflamed tissue and kill bacteria during periodontal treatment.
- Periodontal Surgery: For advanced periodontitis with significant bone loss, surgical interventions may be necessary:
- Flap Surgery (Pocket Reduction Surgery): Gums are lifted back, tartar is removed, and irregular bone surfaces are smoothed to reduce pocket depth.
- Bone Grafts: To regenerate bone lost to periodontitis, using fragments of your own bone, synthetic bone, or donated bone.
- Soft Tissue Grafts: To cover exposed roots due to gum recession, often taking tissue from the roof of your mouth.
Managing Dry Mouth (Xerostomia)
Addressing diabetes and dry mouth or dry mouth from other causes is crucial to prevent further dental problems.
- Over-the-Counter Solutions: Artificial saliva substitutes (sprays, gels), oral moisturizers, and lozenges can provide temporary relief.
- Prescription Medications: Pilocarpine (Salagen®) or cevimeline (Evoxac®) can stimulate saliva production in some cases.
- Lifestyle Adjustments: Sip water frequently, chew sugar-free gum (with xylitol), avoid caffeine, alcohol, and sugary drinks, use a humidifier at night.
- Fluoride Therapy: To protect teeth from increased cavity risk.
Treating Dental Caries (Cavities)
- Fillings: For small to moderate cavities, the decayed portion of the tooth is removed, and the tooth is restored with a filling material (amalgam, composite resin, gold, porcelain).
- Crowns: For larger cavities or weakened teeth, a crown (cap) covers the entire tooth surface, restoring its shape, strength, and appearance.
Treating Pulpitis
- Reversible Pulpitis: Treating the underlying cause, typically filling a cavity, often resolves the inflammation.
- Irreversible Pulpitis:
- Root Canal Therapy (Endodontic Treatment): The inflamed or infected pulp is removed, the inside of the tooth is cleaned and disinfected, and then filled and sealed. A crown is usually placed afterward to protect the tooth. This directly addresses inflammation of tooth pulp.
- Tooth Extraction: If the tooth is too damaged to be saved with a root canal, extraction may be necessary.
Collaborative Care: Dentist and Physician
For chronic conditions like diabetes or cardiovascular disease, your dentist will work closely with your physician to manage your overall health. This might involve sharing dental findings with your doctor, adjusting medications that affect oral health, or coordinating treatment plans.
A Step-by-Step Look at Periodontal Treatment (Scaling and Root Planing)
Scaling and root planing (SRP) is the most common non-surgical treatment for periodontitis. Here’s what you can expect:
- Initial Consultation and Diagnosis: Your dentist or periodontist (a gum specialist) will evaluate your gum health, measure pocket depths, take X-rays, and discuss your medical history. This helps determine if SRP is the appropriate treatment and rule out other causes of inflammation of the gums.
- Local Anesthesia: Before starting, your dental professional will administer a local anesthetic to numb the area of your mouth being treated. This ensures you remain comfortable throughout the procedure. Depending on the extent of your gum disease, the procedure may be done in one appointment or divided into two or four quadrants over separate visits.
- Scaling: Using specialized instruments (ultrasonic scalers and hand scalers), the hygienist or dentist will meticulously remove plaque and tartar (calculus) from above and below the gumline. This step cleans the visible surfaces and the areas within the periodontal pockets.
- Root Planing: After scaling, the root surfaces of your teeth are smoothed. This removes bacterial toxins, makes it harder for plaque to reattach, and helps the gum tissue reattach to the clean, smooth root surface.
- Rinsing and Post-Procedure Instructions: Once the cleaning is complete, you'll rinse your mouth. Your dental professional will provide aftercare instructions, which may include using an antiseptic mouthwash, managing sensitivity, and advice on oral hygiene.
- Follow-up Appointments: Several weeks after your SRP, you'll have a follow-up appointment to assess gum healing, re-measure pocket depths, and check for any remaining mouth inflammation. You will likely need more frequent "periodontal maintenance" cleanings (typically every 3-4 months) to prevent recurrence of the disease.
``
Preventing Oral-Systemic Health Problems
Prevention is always better (and less costly) than treatment. A robust preventive strategy involves excellent oral hygiene, regular dental visits, and proactive management of your overall health.
-
Daily Oral Hygiene:
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes, covering all surfaces of your teeth and gently brushing your tongue.
- Floss Daily: Flossing removes food particles and plaque from between your teeth and under the gumline, areas your toothbrush can't reach, significantly reducing inflammation of the gums.
- Use Mouthwash: An antiseptic mouthwash can help reduce bacteria, but it's not a substitute for brushing and flossing. Pro Tip: Consider an electric toothbrush. Studies show electric toothbrushes are more effective at removing plaque than manual ones, leading to healthier gums and less mouth inflammation.
-
Regular Dental Check-ups and Cleanings:
- Visit your dentist at least twice a year for professional cleanings and examinations. These appointments allow your dental team to remove stubborn plaque and tartar, identify issues like inflammation of tooth pulp or early gum disease, and monitor your overall oral health.
- Inform your dentist about any changes in your medical history or medications.
-
Healthy Diet:
- Limit sugary foods and drinks, which fuel bacteria that cause cavities and gum disease.
- Eat a balanced diet rich in fruits, vegetables, and whole grains. Vitamin C is essential for gum health, and calcium and Vitamin D support bone health, which is critical if you're concerned about does osteoporosis affect your teeth.
-
Manage Systemic Conditions:
- If you have diabetes, work with your physician to keep your blood sugar levels well-controlled. This is the single most important step to mitigate diabetes and teeth issues and diabetes and dry mouth.
- Follow your doctor's advice for managing heart disease, osteoporosis, and other chronic conditions.
-
Avoid Tobacco and Excessive Alcohol:
- Smoking is a major risk factor for severe gum disease, oral cancer, and delayed healing. It also contributes to mouth inflammation.
- Excessive alcohol consumption can increase the risk of oral cancer and contribute to dry mouth.
Risks and Complications of Unmanaged Oral-Systemic Health
Ignoring the signs of oral health problems and their systemic connections can lead to a cascade of serious consequences, impacting both your quality of life and longevity.
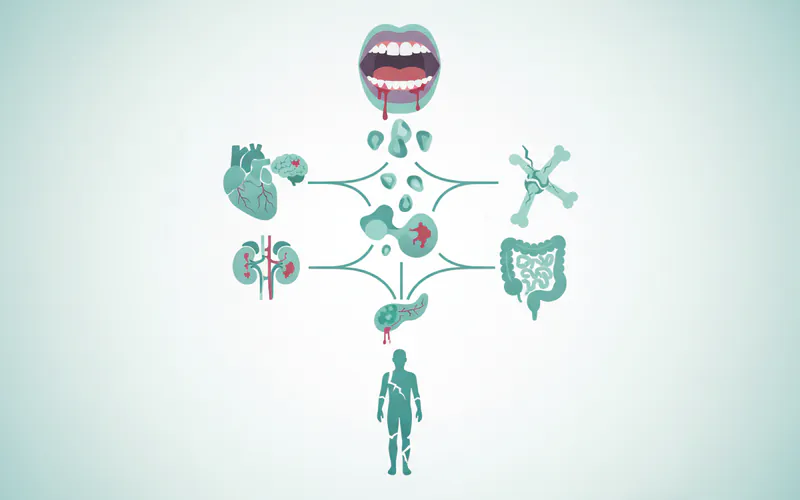
- Worsening Systemic Conditions: Uncontrolled periodontal disease can make blood sugar management significantly harder for diabetics, increase the risk of cardiovascular events, and potentially contribute to adverse pregnancy outcomes.
- Tooth Loss: Chronic gum disease and untreated cavities/pulpitis are leading causes of tooth loss, affecting your ability to eat, speak, and your self-confidence.
- Increased Treatment Difficulty and Cost: What might start as reversible gingivitis or a small cavity, if left untreated, can progress to severe periodontitis requiring extensive surgery, or irreversible inflammation of tooth pulp needing a root canal, all of which are significantly more expensive and invasive.
- Spread of Infection: Untreated oral infections, such as a dental abscess resulting from inflammation of tooth pulp, can spread to other parts of the body, potentially leading to serious conditions like cellulitis, sinusitis, or even life-threatening sepsis, especially in immunocompromised individuals.
- Impact on Quality of Life: Chronic pain, difficulty chewing, bad breath, and aesthetic concerns can severely affect your quality of life, leading to nutritional deficiencies, social anxiety, and reduced overall well-being.
- Medication Complications: For example, osteonecrosis of the jaw in patients taking bisphosphonates if dental extractions are performed without proper precautions.
Comparative Overview of Oral Health Management Strategies
| Strategy | Description | Primary Goal | Typical Cost (USD) | Timeline | Effectiveness |
|---|---|---|---|---|---|
| Prevention | Daily brushing, flossing, regular dental check-ups & cleanings | Maintain health, prevent disease | $75-$200 (cleaning) | Ongoing | Highly Effective |
| Early Intervention | Treating gingivitis, small cavities, initial dry mouth | Reverse disease, stop progression | $100-$300 (filling) | Days to Weeks | Very Effective |
| Moderate Treatment | Scaling & root planing (deep cleaning), multiple fillings, crowns, dry mouth meds | Manage periodontitis, restore damaged teeth | $250-$800 (per quadrant SRP), $800-$3,000 (crown) | Weeks to Months | Effective |
| Advanced Treatment | Periodontal surgery, root canal therapy, extractions, implants | Salvage teeth, replace missing teeth, manage severe infection | $700-$2,500 (root canal), $1,000-$4,000+ (surgery) | Months to Years | Variable (Often Last Resort) |
Children / Pediatric Considerations
Oral-systemic health is just as important in children, if not more so, as their bodies are still developing.
- Early Detection: Systemic conditions often present unique oral signs in children. For instance, children with diabetes are also at increased risk for gum inflammation and candidiasis. Genetic conditions or nutritional deficiencies can manifest as delayed tooth eruption, enamel defects, or increased susceptibility to decay.
- Impact on Growth and Development: Poor oral health, such as severe early childhood caries (ECC) or uncontrolled oral infections, can affect a child's nutrition, growth, sleep, and school performance.
- Special Needs Children: Children with certain systemic health issues (e.g., heart conditions, immunodeficiencies, developmental disabilities) may require specialized dental care due to increased risk of oral complications, difficulty with hygiene, or interactions with medications.
- Parental Guidance: Parents should ensure children maintain excellent oral hygiene, have regular dental check-ups starting by age one, and are educated about the importance of a healthy diet. Informing the pediatric dentist about any underlying medical conditions or medications is crucial for comprehensive care.
Cost Breakdown
Understanding the costs associated with dental care, especially when managing oral-systemic issues, is vital for budgeting and planning. Prices vary significantly by region, dentist, and your insurance plan.
Average US Dental Costs (Without Insurance)
| Procedure | Low Range | Mid Range | High Range |
|---|---|---|---|
| Routine Cleaning & Exam | $75 | $150 | $250 |
| Composite (White) Filling (1 surface) | $100 | $250 | $450 |
| Amalgam (Silver) Filling (1 surface) | $80 | $180 | $350 |
| Scaling & Root Planing (per quadrant) | $250 | $500 | $800 |
| Simple Tooth Extraction | $100 | $250 | $400 |
| Surgical Tooth Extraction | $250 | $500 | $800 |
| Root Canal (Front Tooth) | $700 | $1,000 | $1,500 |
| Root Canal (Molar) | $1,000 | $1,500 | $2,500 |
| Dental Crown (Porcelain) | $800 | $1,500 | $3,000 |
With vs. Without Insurance
- With Insurance: Most dental insurance plans follow a "100-80-50" structure:
- 100% coverage for preventive care (cleanings, exams, X-rays).
- 80% coverage for basic procedures (fillings, simple extractions, root canal on front teeth).
- 50% coverage for major procedures (crowns, bridges, dentures, periodontal surgery, root canal on molars).
- Plans typically have an annual maximum (e.g., $1,000-$2,000) and may have a deductible (e.g., $50-$100).
- Without Insurance: You are responsible for 100% of the cost. Many dentists offer a discount for cash payments or in-house membership plans.
``
Payment Plans and Financing Options
- In-House Payment Plans: Many dental offices offer flexible payment arrangements, allowing you to pay for treatment over several months.
- Third-Party Financing: Companies like CareCredit or LendingClub offer specialized healthcare credit cards with deferred interest options if paid within a promotional period.
- Dental Schools: University dental schools often provide services at a reduced cost, as students gain experience under supervision of experienced faculty.
- Community Health Centers: Federally Qualified Health Centers (FQHCs) and other community clinics often offer sliding scale fees based on income.
- Medicaid/CHIP: State-run programs for low-income individuals and children provide varying levels of dental benefits.
Cost-Saving Tips
- Prioritize Prevention: Regular cleanings and good home care are the most cost-effective ways to avoid expensive treatments for inflammation of the gums or inflammation of tooth pulp.
- Address Issues Early: Don't delay treatment. A small cavity can become a root canal if left too long, increasing costs exponentially.
- Get Multiple Quotes: For major procedures, it can be helpful to get treatment plans and cost estimates from a few different dentists.
- Discuss All Options: Ask your dentist about the pros and cons of different treatment materials and approaches, which can have cost implications.
- Max Out Insurance: If you have an annual maximum, try to utilize your benefits before they reset at the end of the year.
Frequently Asked Questions
Is oral-systemic health a real concern, or just a new health trend?
Oral-systemic health is a scientifically well-established concept, supported by extensive research over decades. It's not a trend but a fundamental shift in understanding how different parts of the body interact, emphasizing that the mouth is not separate from the rest of the body. Leading medical and dental organizations, including the ADA, recognize its profound importance.
Can gum disease truly cause heart disease?
While the exact causal pathway is still under investigation, strong correlational evidence suggests that severe gum disease (periodontitis) is a risk factor for cardiovascular disease. The chronic inflammation of the gums releases inflammatory mediators and bacteria into the bloodstream, which can contribute to plaque formation in arteries and exacerbate existing heart conditions.
How often should I visit the dentist if I have diabetes?
If you have diabetes, it is generally recommended to visit your dentist for check-ups and cleanings at least every three to six months, rather than the standard twice a year. This allows for closer monitoring of your gum health, early detection of issues like diabetes and dry mouth or infections, and proactive management of any oral manifestations of your diabetes.
What are the common signs of mouth inflammation?
Common signs of mouth inflammation (stomatitis) include redness, swelling, tenderness, or a burning sensation in the soft tissues of your mouth (gums, tongue, cheeks, lips). You might also notice ulcers, sores, or white patches. These symptoms can make eating, speaking, and swallowing uncomfortable.
Can pregnancy permanently affect my teeth?
While hormonal changes during pregnancy (e.g., pregnancy gingivitis) can make your gums more susceptible to inflammation of the gums, these changes are usually temporary and reversible with good oral hygiene after childbirth. However, untreated gum disease or increased cavity risk from morning sickness or dietary changes during pregnancy can lead to lasting damage if not addressed promptly.
Does dental work help or hurt osteoporosis?
Dental work, when properly managed, generally helps maintain oral health in individuals with osteoporosis. Regular dental care is crucial to prevent tooth loss due to reduced jawbone density (does osteoporosis affect your teeth). It's vital to inform your dentist if you are taking bisphosphonates for osteoporosis, as certain dental procedures like extractions may require special precautions to prevent Medication-Related Osteonecrosis of the Jaw (MRONJ).
What's the average cost of a deep cleaning (scaling and root planing)?
The average cost for a deep cleaning (scaling and root planing) in the US typically ranges from $250 to $800 per quadrant without insurance. Most full-mouth treatments require cleaning all four quadrants. This cost can vary significantly based on your location, the severity of your gum disease, and whether additional treatments like antibiotics are included.
How long does it take to treat gum disease?
Treating gum disease depends on its severity. Mild gingivitis can resolve within 1-2 weeks with professional cleaning and improved home care. Moderate periodontitis requiring scaling and root planing might involve 2-4 appointments over a few weeks, followed by ongoing periodontal maintenance cleanings every 3-4 months indefinitely to manage the condition. Advanced cases with surgery will take longer for recovery and follow-up.
Are there alternatives to antibiotics for gum infection?
For gum infections, antibiotics are often used in conjunction with mechanical cleaning (scaling and root planing). Alternatives or complementary treatments might include antiseptic mouthwashes (like chlorhexidine), topical antimicrobial agents placed in periodontal pockets, or in some cases, laser therapy for bacterial reduction. However, antibiotics are often crucial for controlling active infections and their systemic spread.
Can I get financing for expensive dental treatments?
Yes, many dental practices offer various financing options for expensive treatments. These can include in-house payment plans directly with the dental office, third-party medical financing companies like CareCredit, or even personal loans. It's always best to discuss payment options and potential plans with your dental office's financial coordinator before beginning extensive treatment.
When to See a Dentist
Knowing when to seek dental care is crucial for preventing minor issues from escalating and for managing your oral-systemic health proactively.
Routine Care (Scheduled Appointments):
- Every 6 Months: For regular check-ups and professional cleanings, even if you don't have any pain or obvious problems. This is essential for preventing inflammation of the gums, detecting cavities early, and screening for other oral health issues.
- Before or During Pregnancy: To address any potential pregnancy and teeth issues and ensure optimal oral health for both mother and baby.
- If You Have a Chronic Systemic Condition: Such as diabetes, heart disease, or osteoporosis. Your dentist can help manage specific oral risks like diabetes and dry mouth or assess if does osteoporosis affect your teeth is becoming an issue. Inform your dentist about any new medical diagnoses or medications.
Red Flags / Urgent Care (Seek prompt attention):
- Persistent Toothache: Especially if it's severe, throbbing, spontaneous, or keeps you awake at night. This could indicate inflammation of tooth pulp (pulpitis) or an infection.
- Swelling in Your Gums, Face, or Neck: This is a serious sign of infection that needs immediate attention, potentially indicating an abscess or a spreading infection.
- Bleeding Gums That Don't Stop: While some bleeding during brushing can be gingivitis, persistent, excessive, or spontaneous bleeding could indicate advanced gum disease or other systemic issues.
- Sores, Lumps, or Red/White Patches in Your Mouth: Especially if they don't heal within two weeks. These could be signs of oral cancer or other serious mouth inflammation.
- Sudden Sensitivity to Hot or Cold: Could indicate a new cavity, a cracked tooth, or receding gums.
- Loose Teeth or a Change in Your Bite: These are signs of advanced periodontal disease or other underlying issues with jawbone support.
- Difficulty Swallowing or Opening Your Mouth: Can indicate a severe infection or other serious conditions.
- Persistent Dry Mouth: Especially if accompanied by increased cavities, could be a sign of a systemic condition like diabetes or Sjögren's syndrome, or a medication side effect that needs management.
Remember, your oral health is a window to your overall health. Don't wait for pain to be your only indicator. Regular preventive care and prompt attention to any alarming symptoms are your best defense in maintaining a healthy smile and a healthy body.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Does Oil Pulling Help Gut Health
The intricate connection between our oral health and overall well-being is a topic of growing fascination and scientific inquiry. Often, when we think of health, we focus on specific organs or systems, overlooking the crucial role of the mouth as a gateway to the rest of the body. One ancient practi
February 23, 2026
Does Oil Pulling Help With Inflammation
It's a question many health-conscious individuals ask as they explore natural remedies: does oil pulling help with inflammation? In an era where holistic approaches to wellness are gaining traction, the ancient practice of oil pulling has resurfaced, promising benefits that extend beyond oral hy
February 23, 2026
Oil Pulling for Kidney Disease: Complete Guide
Chronic kidney disease (CKD) affects an estimated 37 million adults in the United States, often progressing silently until advanced stages. What many may not realize is the profound connection between the health of their mouth and the health of their kidneys. As a bridge between traditional wisd
February 23, 2026
Oil Pulling Oral Microbiome: Complete Guide
Have you ever considered the bustling universe thriving within your mouth? This intricate community, known as the oral microbiome, consists of billions of microorganisms – some beneficial, some harmful – all playing a critical role in your oral and overall systemic health. Maintaining a balanced
February 23, 2026