Oral Inflammation: Complete Guide
Key Takeaways
- Oral inflammation is a silent epidemic affecting millions of Americans, often overlooked until it escalates into more serious systemic health issues. While commonly associated with gum disease, oral inflammation encompasses a broader spectrum of conditions, from mild irritation to severe infecti
Oral inflammation is a silent epidemic affecting millions of Americans, often overlooked until it escalates into more serious systemic health issues. While commonly associated with gum disease, oral inflammation encompasses a broader spectrum of conditions, from mild irritation to severe infections, and its implications extend far beyond the mouth. Did you know that an estimated 47.2% of adults aged 30 years and older have some form of periodontal disease, a major inflammatory condition of the gums and bone? This pervasive issue can not only lead to discomfort, tooth loss, and bad breath but also significantly impact your overall well-being, influencing conditions like heart disease, diabetes, and even digestive health. Understanding oral inflammation is the first step toward safeguarding your smile and your health. This comprehensive guide will explore what oral inflammation is, its various forms, underlying causes—including the surprising connection between gut health and bad breath—effective treatment options, and crucial prevention strategies to empower you with the knowledge to maintain optimal oral and systemic health.
Key Takeaways:
- Prevalence: Nearly half of all adults over 30 experience some form of periodontal disease, a leading cause of oral inflammation.
- Systemic Link: Oral inflammation is strongly linked to chronic conditions like heart disease, diabetes, and even contributes to issues like gut health bad breath.
- Early Detection: Symptoms like persistent red, swollen, or bleeding gums, chronic bad breath, and sensitivity warrant immediate dental attention.
- Treatment Costs: Non-surgical periodontal treatments (e.g., scaling and root planing) can range from $200 to $600 per quadrant, while advanced surgical options may cost $500 to $4,000 per tooth/site, with most dental insurance plans covering a portion (typically 50-80%).
- Prevention is Key: Daily brushing, flossing, regular dental check-ups (typically every 6 months, costing $100-$300 without insurance), and a balanced diet are crucial for preventing oral inflammation.
- Gut-Oral Axis: A disrupted gut microbiome can exacerbate oral inflammation and contribute to halitosis, reinforcing the question: does bad gut health cause bad breath?
- Treatment Timeline: Initial non-surgical treatments usually require 1-2 appointments, with recovery times of a few days. Surgical interventions may involve longer recovery, typically 1-2 weeks.
What It Is / Overview
Oral inflammation is the body's natural response to irritation, infection, or injury within the oral cavity. It's a complex biological process involving immune cells, blood vessels, and molecular mediators, all working to eliminate harmful stimuli and initiate tissue repair. While acute inflammation is a necessary and protective mechanism, chronic oral inflammation can become destructive, leading to tissue damage and contributing to systemic diseases. Essentially, when bacteria, trauma, or other irritants trigger the immune system in the mouth, the affected tissues (gums, tongue, cheeks, palate) become red, swollen, painful, and sometimes warm. This response is designed to localize the problem, but if the irritant persists, this protective mechanism can turn detrimental, leading to ongoing tissue destruction.

The Underlying Mechanisms of Oral Inflammation
At a cellular level, oral inflammation begins when immune cells, such as neutrophils and macrophages, detect pathogens (like bacteria in plaque) or damaged cells. They release pro-inflammatory cytokines, chemokines, and prostaglandins, which signal other immune cells to migrate to the site of injury. This influx of immune cells and increased blood flow causes the classic signs of inflammation: redness (erythema), swelling (edema), heat, pain, and loss of function.
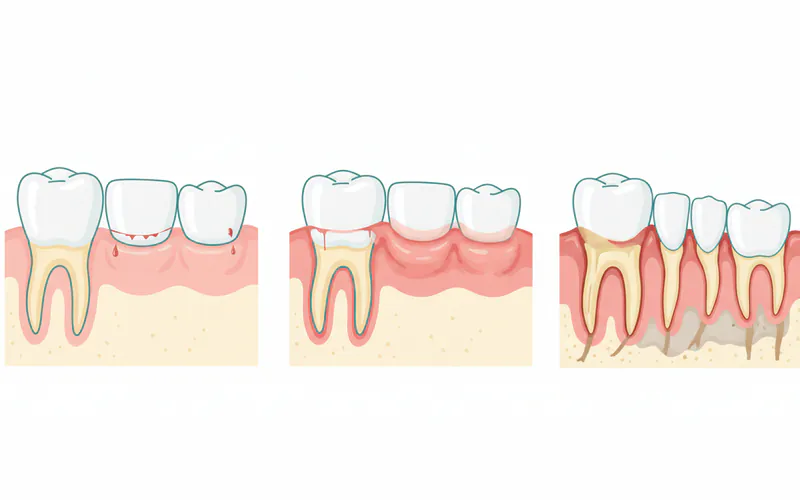
For instance, in the case of gum disease, bacteria colonize the tooth surfaces, forming a sticky film called plaque. If plaque is not removed, the bacteria produce toxins that irritate the gum tissue. The body's immune response to these toxins leads to gingivitis, characterized by inflamed, bleeding gums. If left untreated, this can progress to periodontitis, where the inflammation extends to the bone supporting the teeth, causing irreversible damage and potentially tooth loss.
Understanding these mechanisms highlights why timely intervention is crucial. Chronic low-grade inflammation in the mouth can constantly flood the bloodstream with inflammatory mediators and bacteria, creating a systemic inflammatory burden that impacts organs far from the oral cavity.
Types / Variations
Oral inflammation manifests in various forms, each with distinct characteristics and potential causes. Recognizing the specific type is key to effective diagnosis and treatment.
1. Gingivitis
This is the mildest and most common form of periodontal disease, affecting the gums. It's characterized by inflammation of the gingiva (gum tissue) without affecting the underlying bone.
- Characteristics: Red, swollen, tender gums that bleed easily, especially during brushing or flossing.
- Cause: Primarily caused by plaque buildup due to inadequate oral hygiene.
- Prognosis: Reversible with proper oral hygiene and professional cleaning.
2. Periodontitis
An advanced form of gingivitis, periodontitis involves inflammation and infection that spreads below the gum line, affecting the ligaments and bone supporting the teeth. It's the leading cause of tooth loss in adults.
- Characteristics: Deep gum pockets, receding gums, persistent bad breath (halitosis), loose teeth, changes in bite, pus between teeth and gums.
- Cause: Untreated gingivitis, bacterial infection, genetics, systemic diseases (e.g., diabetes), smoking.
- Prognosis: Irreversible bone loss, but progression can be halted with treatment.
3. Stomatitis
A general term for inflammation of the mucous membranes of the mouth. It can affect the cheeks, gums, tongue, lips, and palate.
- Characteristics: Redness, swelling, pain, difficulty eating/speaking, sometimes ulcers or sores.
- Types include:
- Aphthous Stomatitis (Canker Sores): Small, painful ulcers with a white or yellow center and a red border. Causes are often unknown but can be linked to stress, trauma, nutritional deficiencies, or certain foods.
- Herpetic Stomatitis (Cold Sores): Caused by the Herpes Simplex Virus, presenting as painful blisters that burst and form ulcers, often on the lips or around the mouth.
- Denture Stomatitis: Inflammation under dentures, often caused by fungal infection (Candida albicans) or ill-fitting dentures.
- Allergic Stomatitis: Reaction to allergens like certain foods, dental materials, or oral hygiene products.
4. Cheilitis
Inflammation of the lips, often affecting the corners (angular cheilitis) or the entire lip surface.
- Characteristics: Dry, cracked, red, and sometimes painful lips, with fissures at the corners of the mouth.
- Causes: Fungal infection (Candida), bacterial infection, vitamin deficiencies (B vitamins, iron), excessive drooling, ill-fitting dentures, sun exposure.
5. Oral Mucositis
A common and painful side effect of cancer treatments like chemotherapy and radiation therapy to the head and neck.
- Characteristics: Redness, swelling, ulceration, and pain throughout the mouth and throat, making eating, swallowing, and speaking extremely difficult.
- Cause: Damage to rapidly dividing cells in the oral mucosa by cancer treatments.
6. Peri-implantitis
Inflammation affecting the soft tissues and bone surrounding a dental implant.
- Characteristics: Redness, swelling, bleeding around the implant, pus, and eventually bone loss, potentially leading to implant failure.
- Cause: Bacterial infection, often due to poor oral hygiene, smoking, or systemic diseases.
Causes / Why It Happens
Oral inflammation doesn't just appear; it's a response to various triggers, ranging from local irritants to systemic health conditions. Understanding these causes is fundamental to prevention and effective treatment.
1. Poor Oral Hygiene and Plaque Buildup
This is the most common culprit. When you don't brush and floss regularly, bacteria in your mouth multiply and form plaque—a sticky, colorless film on your teeth. If plaque isn't removed, it hardens into tartar (calculus), which is even more difficult to remove and provides a rough surface for more plaque to adhere to. The bacteria in plaque and tartar release toxins that irritate gum tissues, initiating gingivitis and potentially progressing to periodontitis.
2. Bacterial, Viral, and Fungal Infections
- Bacteria: Beyond plaque, specific bacteria can cause infections leading to stomatitis or abscesses.
- Viruses: Herpes Simplex Virus causes cold sores (herpetic stomatitis). Other viral infections can also manifest orally.
- Fungi: Candida albicans is a yeast that causes oral thrush (candidiasis), particularly in infants, the elderly, denture wearers, and those with weakened immune systems.
3. Traumatic Injury
Physical trauma to the mouth can cause inflammation. This includes:
- Accidental biting of the cheek or tongue.
- Burns from hot food or drinks.
- Irritation from ill-fitting dentures or sharp edges of broken teeth/fillings.
- Aggressive brushing or flossing techniques.
4. Systemic Diseases and Conditions
Many diseases that affect the entire body can manifest as oral inflammation:
- Diabetes: Individuals with diabetes are more susceptible to infections and have impaired healing, making them more prone to severe gum disease.
- Autoimmune Diseases: Conditions like Crohn's disease, lupus, and Sjögren's syndrome can cause oral lesions and dry mouth, increasing susceptibility to inflammation.
- Immunosuppression: Conditions like HIV/AIDS or medications that suppress the immune system make individuals more vulnerable to oral infections and inflammation.
- Inflammatory Bowel Disease (IBD): Both Crohn's disease and ulcerative colitis can cause oral manifestations, including painful ulcers and swelling, directly linking digestive health to oral inflammation.
5. Nutritional Deficiencies
Lack of essential vitamins and minerals can compromise oral tissue health and immune response.
- Vitamin C: Deficiency (scurvy) can lead to bleeding gums and poor wound healing.
- B Vitamins (e.g., Folate, B12): Deficiencies can cause angular cheilitis, glossitis (inflamed tongue), and recurrent aphthous ulcers.
- Iron: Iron deficiency anemia can contribute to angular cheilitis and atrophic glossitis.
6. Medications
Certain medications can contribute to oral inflammation or dryness (xerostomia), which then increases the risk of inflammation:
- Antihypertensives, antidepressants, antihistamines: Can cause dry mouth, reducing saliva's protective effects.
- Phenytoin (anti-seizure medication), Cyclosporine (immunosuppressant), Nifedipine (calcium channel blocker): Can cause gingival overgrowth, making gums harder to clean and more prone to inflammation.
- Bisphosphonates: Can lead to osteonecrosis of the jaw (ONJ) in rare cases, a severe inflammatory bone condition.
7. Smoking and Tobacco Use
Tobacco products, in all forms, are major risk factors. Smoking impairs the immune system's ability to fight off bacterial infections, reduces blood flow to the gums, and hinders healing. This significantly increases the risk and severity of periodontitis and oral cancers.
8. Stress
Chronic stress can suppress the immune system, making the body more vulnerable to infections, including those in the mouth. Stress can also lead to habits like teeth grinding (bruxism) or clenching, which can put undue pressure on teeth and gums, contributing to inflammation.
9. Hormonal Changes
Fluctuations in hormones, such as during pregnancy, puberty, menstruation, or menopause, can make gums more sensitive and reactive to plaque bacteria, leading to gingivitis.
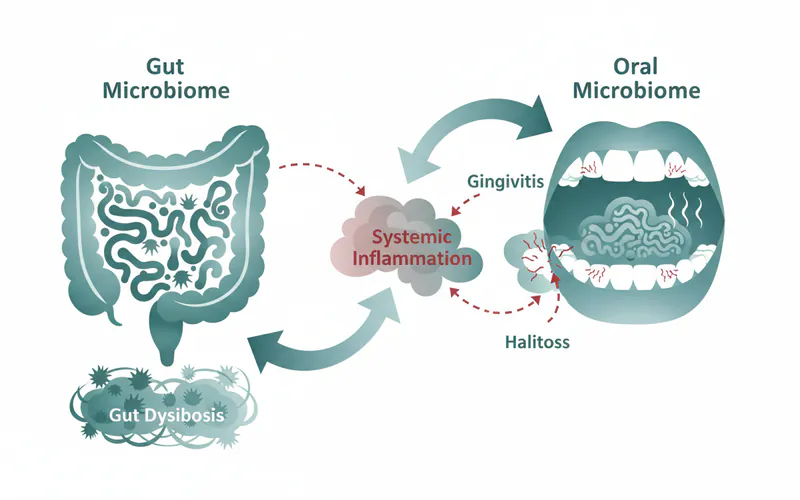
The Gut-Oral Axis: Connecting Gut Health and Bad Breath
This is a critical area often overlooked in discussions of oral inflammation. The concept of the "gut-oral axis" highlights the bidirectional relationship between the microbiomes of your mouth and your gut. Both are complex ecosystems of bacteria, fungi, and viruses, and imbalances in one can affect the other.
Does bad gut health cause bad breath? The answer is often yes, indirectly and sometimes directly.
- Indirectly: A disrupted gut microbiome (dysbiosis) can impair overall immune function and nutrient absorption. This can weaken the body's ability to combat oral infections, making you more susceptible to conditions like periodontitis, which is a major source of chronic halitosis. Furthermore, systemic inflammation originating in the gut can contribute to generalized inflammation throughout the body, including the mouth.
- Directly: While most cases of halitosis originate in the mouth (due to volatile sulfur compounds produced by oral bacteria), certain gut issues can produce distinctive odors that can be perceived as bad breath. Conditions like gastroesophageal reflux disease (GERD), Helicobacter pylori infection in the stomach, or severe malabsorption issues can release gases that travel up the esophagus and into the mouth, contributing to an unpleasant odor. Additionally, if you have a significant overgrowth of certain bacteria or yeasts in your gut, the metabolites they produce might be absorbed into your bloodstream and then exhaled through your lungs, although this is less common than oral causes.
Gut health bad breath can also arise from an imbalanced gut leading to systemic issues that reduce salivary flow or alter its composition, creating a more favorable environment for odor-producing oral bacteria. Maintaining a healthy gut microbiome through diet (prebiotics, probiotics) and lifestyle can therefore indirectly support a healthier oral microbiome and fresher breath.
Signs and Symptoms
Recognizing the early signs of oral inflammation is vital for timely intervention. While some symptoms are obvious, others can be subtle.
- Red or Swollen Gums: Healthy gums are typically firm and pink. Inflamed gums appear puffy, tender, and reddish or purplish.
- Bleeding Gums: Gums that bleed easily during brushing, flossing, or even spontaneous bleeding are a hallmark sign of gingivitis.
- Persistent Bad Breath (Halitosis): While often attributed to food, chronic bad breath can be a significant indicator of bacterial overgrowth and infection, especially in gum disease. This is where the gut health bad breath connection can also play a role, making it crucial to consider both oral and systemic causes.
- Gum Recession: Gums pulling away from the teeth, making teeth appear longer. This exposes sensitive tooth roots.
- Loose Teeth or Changes in Bite: A sign of advanced periodontitis, where the bone supporting the teeth is being destroyed.
- Pus Between Teeth and Gums: Indicates an active infection.
- Pain or Tenderness: Localized pain when chewing or general discomfort in the mouth.
- Increased Tooth Sensitivity: Especially to hot or cold temperatures, often due to exposed tooth roots from gum recession.
- Sores, Ulcers, or Blisters: These can appear on the gums, tongue, cheeks, or lips, varying in appearance depending on the type of stomatitis or cheilitis.
- Difficulty Eating, Swallowing, or Speaking: Severe inflammation or ulceration can make these basic functions painful.
- Dry Mouth (Xerostomia): Reduced salivary flow removes the mouth's natural cleansing action, increasing the risk of inflammation and infection.
Treatment Options
Treating oral inflammation depends heavily on its underlying cause and severity. A comprehensive approach often combines professional dental care with improved home care.
1. Professional Dental Cleanings (Prophylaxis)
- Description: For gingivitis, a standard dental cleaning removes plaque and tartar above and just below the gum line.
- Pros: Non-invasive, quick, effective for mild inflammation, crucial for prevention.
- Cons: Not sufficient for advanced gum disease.
- Cost: Typically $75 - $200 for an uninsured adult in the US, often covered by insurance.

2. Scaling and Root Planing (Deep Cleaning)
- Description: This non-surgical procedure is the gold standard for treating mild to moderate periodontitis. It involves meticulously scraping away plaque and tartar from above and below the gum line (scaling) and then smoothing the tooth roots (planing) to remove bacterial toxins and prevent further plaque buildup. Often performed under local anesthesia.
- Pros: Highly effective for stopping the progression of periodontitis, reduces gum pocket depth, relatively non-invasive compared to surgery.
- Cons: Can cause temporary sensitivity, may require multiple appointments, not a permanent cure if oral hygiene isn't maintained.
- Cost: Ranges from $200 - $600 per quadrant (a fourth of your mouth) or $800 - $2,400 for a full mouth deep cleaning without insurance. Most dental insurance plans cover 50-80% of the cost after deductibles.
3. Antibiotics
- Description: Can be used in conjunction with deep cleaning to target bacterial infections. Options include oral antibiotic pills, antibiotic mouth rinses, or antibiotic gels/microspheres placed directly into gum pockets.
- Pros: Effectively reduces bacterial load, can help heal infections.
- Cons: Oral antibiotics can have systemic side effects, contribute to antibiotic resistance, may not be necessary for all cases.
- Cost: Oral antibiotics typically $10 - $50 for a prescription. Localized antibiotic gels can add $50 - $150 per site to treatment costs.
4. Anti-inflammatory Medications
- Description: Over-the-counter NSAIDs (like ibuprofen) can manage pain and reduce inflammation. Prescription anti-inflammatory medications may be used in specific cases.
- Pros: Provides symptomatic relief, reduces discomfort.
- Cons: Long-term use of NSAIDs can have side effects (stomach issues, kidney problems).
5. Periodontal Surgery
- Description: For advanced periodontitis, surgical options may be necessary to reduce pocket depths, regenerate lost bone and tissue, or graft new tissue.
- Pocket Reduction Surgery (Flap Surgery): Gums are folded back, tartar removed, and irregular bone surfaces smoothed before the gum tissue is sutured back, reducing pocket depth.
- Bone Grafts: Uses fragments of your own bone, synthetic bone, or donated bone to rebuild bone destroyed by periodontitis.
- Soft Tissue Grafts: Uses tissue from another part of your mouth or a donor source to cover exposed roots or enhance gum tissue.
- Guided Tissue Regeneration: Uses a barrier membrane to prevent soft tissue from growing into the area where bone should be, allowing bone and connective tissue to regenerate.
- Pros: Can halt severe disease progression, save teeth, regenerate lost tissue/bone.
- Cons: More invasive, longer recovery, higher cost, potential for post-operative pain and swelling.
- Cost: Highly variable. Pocket reduction surgery can range from $500 - $2,000 per quadrant. Bone grafts or soft tissue grafts can cost $600 - $4,000 per tooth/site, depending on complexity and material used.
6. Laser Therapy
- Description: Lasers can be used as an adjunct to traditional scaling and root planing or as a standalone procedure (e.g., LANAP protocol) to remove inflamed tissue and kill bacteria.
- Pros: Minimally invasive, less bleeding, potentially faster healing, less post-operative discomfort.
- Cons: Higher cost, not universally covered by insurance, long-term efficacy comparable to traditional surgery is still debated in some contexts.
- Cost: Typically $1,000 - $4,000 for a full mouth laser treatment, often not covered as comprehensively as traditional treatments.
Step-by-Step Process (Example: Scaling and Root Planing)
If you're diagnosed with moderate periodontitis, your dentist or periodontist will likely recommend scaling and root planing. Here's what you can expect:
- Initial Assessment & Diagnosis: Your dentist will examine your gums, measure pocket depths around your teeth using a periodontal probe, and take X-rays to assess bone loss.
- Anesthesia: To ensure comfort, the dental hygienist or dentist will administer local anesthesia to numb the specific quadrant(s) of your mouth being treated. This allows for thorough cleaning without discomfort.
- Scaling: Using specialized instruments (ultrasonic scalers and manual curettes), the hygienist or dentist will meticulously remove all plaque and tartar (calculus) from the tooth surfaces, both above and below the gum line, extending into the periodontal pockets.
- Root Planing: After scaling, the root surfaces of your teeth will be smoothed. This process removes any remaining bacterial toxins and rough spots on the root that could attract new plaque, making it harder for bacteria to reattach and easier for gums to reattach to the clean surface.
- Irrigation (Optional): Some practitioners may flush the gum pockets with an antimicrobial solution after scaling and root planing to further reduce bacteria.
- Localized Antibiotic Placement (Optional): In some cases, a sustained-release antibiotic gel or chip may be placed directly into deep pockets to continue fighting bacteria for several days or weeks.
- Post-Treatment Instructions: You'll receive specific instructions on how to care for your mouth after the procedure, including dietary advice, pain management, and oral hygiene adjustments.
- Follow-up Appointment: A follow-up visit, typically 4-6 weeks later, is essential to re-evaluate gum health, measure pocket depths again, and ensure proper healing. Maintenance cleanings (periodontal maintenance) will then be recommended more frequently than standard cleanings, usually every 3-4 months.
Pro Tip: Do not skip your follow-up appointments after a deep cleaning. These are crucial for assessing the success of the treatment and planning ongoing maintenance to prevent recurrence of periodontitis.
Cost and Insurance
The cost of oral inflammation treatments in the US can vary significantly based on the type of treatment, the severity of the condition, the dental professional's fees, and your geographic location.
Average US Costs (Without Insurance):
| Procedure Type | Average Cost Range (Per Quadrant/Site) | Average Cost Range (Full Mouth/Major) |
|---|---|---|
| Standard Cleaning (Prophylaxis) | N/A | $75 - $200 |
| Scaling & Root Planing (SRP) | $200 - $600 | $800 - $2,400 |
| Localized Antibiotic Placement | $50 - $150 (per site) | N/A |
| Pocket Reduction Surgery | $500 - $2,000 | $2,000 - $8,000+ |
| Bone Grafts (Minor) | $600 - $1,200 (per site) | N/A |
| Soft Tissue Grafts (Minor) | $700 - $1,500 (per site) | N/A |
| Laser Periodontal Therapy (LANAP) | N/A | $1,000 - $4,000 |
- Geographic Variation: Costs tend to be higher in major metropolitan areas (e.g., New York, Los Angeles) compared to rural regions or smaller cities.
- Specialist Fees: A periodontist (gum specialist) may charge more than a general dentist for advanced periodontal procedures.
Insurance Coverage Details:
Most dental insurance plans (PPO, HMO, DMO) offer some level of coverage for oral inflammation treatments:
- Preventive Care (e.g., standard cleanings, X-rays): Typically covered at 80-100%.
- Basic Procedures (e.g., scaling and root planing): Often covered at 50-80% after your deductible is met. Many plans classify SRP as a "basic" or "major" procedure depending on the severity.
- Major Procedures (e.g., periodontal surgery, grafts): Usually covered at 20-50% after your deductible, and often subject to annual maximums (e.g., $1,000 - $2,000 per year).
- Medicaid/Medicare:
- Medicaid: Varies significantly by state. Some states offer comprehensive dental benefits for adults, including basic and major periodontal care, while others may only cover emergency extractions. Children on Medicaid usually have more extensive coverage.
- Medicare: Original Medicare does NOT cover routine dental care, including most oral inflammation treatments. Medicare Advantage plans (Part C) often include some dental benefits, but coverage levels can vary widely.
Pro Tip: Always contact your dental insurance provider directly or consult your plan's benefits summary before starting treatment to understand your specific coverage, deductibles, co-pays, and annual maximums.
Recovery and Aftercare
Proper recovery and diligent aftercare are essential for the success of any oral inflammation treatment and for preventing recurrence.
After Non-Surgical Treatment (e.g., Scaling and Root Planing):
- Pain and Sensitivity: You may experience mild to moderate pain and sensitivity for a few days. Over-the-counter pain relievers (like ibuprofen or acetaminophen) are usually sufficient.
- Gum Soreness: Gums may be sore, swollen, or slightly sensitive to touch.
- Diet: Stick to soft foods for 24-48 hours. Avoid very hot, cold, spicy, or crunchy foods.
- Oral Hygiene: Resume gentle brushing and flossing within 24 hours unless otherwise instructed. Your dentist may recommend a prescription antimicrobial mouth rinse (e.g., chlorhexidine) for a short period.
- Avoid Smoking: Refrain from smoking or using tobacco products, as they can significantly impede healing.
- Follow-up: Attend all scheduled follow-up appointments and maintain a rigorous periodontal maintenance schedule (typically every 3-4 months).
After Surgical Treatment (e.g., Flap Surgery, Grafts):
- Pain and Swelling: More significant pain and swelling are common. Prescription pain medication may be provided. Apply ice packs to the outside of your face for the first 24-48 hours.
- Bleeding: Some light bleeding or oozing is normal for the first day. Bite gently on a gauze pad if needed.
- Sutures: If sutures were placed, you'll likely return in 7-10 days to have them removed, or they may dissolve on their own.
- Diet: Strictly adhere to a soft, bland diet for at least 1-2 weeks, avoiding chewing on the treated side.
- Oral Hygiene: You'll be given specific instructions on how to clean the surgical site gently. Avoid brushing or flossing directly on the treated area initially. Rinse with a prescribed antimicrobial mouthwash.
- Physical Activity: Avoid strenuous exercise for several days post-surgery.
- Smoking: Absolutely no smoking or tobacco use, as it can severely compromise healing and lead to complications.
- Expectations: Full healing can take several weeks to months, especially with bone or soft tissue grafts. Follow your periodontist's instructions meticulously.
ADA Guideline: The American Dental Association emphasizes the importance of consistent professional maintenance and excellent home care to control periodontal disease and prevent its recurrence after treatment.
Prevention
Preventing oral inflammation is far easier and less costly than treating it. A proactive approach is key.
1. Excellent Oral Hygiene
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste to brush for at least two minutes, twice a day. Pay attention to the gum line.
- Floss Daily: Flossing removes plaque and food particles from between your teeth and under the gum line where a toothbrush can't reach. This is crucial for preventing interdental inflammation.
- Use Mouthwash (Optional): An antimicrobial or fluoride mouthwash can supplement brushing and flossing but should not replace them.
2. Regular Dental Check-ups and Cleanings
- Every Six Months: Schedule routine dental check-ups and professional cleanings every six months, or more frequently if you are prone to gum disease. These appointments allow your dentist to identify and address issues early.
- Early Detection: Your dentist can spot early signs of gingivitis or other inflammation before they become severe.
3. Balanced Diet
- Nutrient-Rich Foods: Consume a diet rich in fruits, vegetables, lean proteins, and whole grains. These provide essential vitamins (especially C and B vitamins) and minerals that support gum health and immune function.
- Limit Sugary and Acidic Foods/Drinks: Sugars feed bacteria that produce plaque, and acids erode enamel, making teeth more susceptible to decay and inflammation.
- Stay Hydrated: Drink plenty of water to maintain saliva flow, which naturally cleanses the mouth.
4. Avoid Tobacco Products
- Quit Smoking/Chewing: Tobacco use is one of the most significant risk factors for severe gum disease and oral cancers. Quitting is the single most impactful step you can take to improve your oral and overall health.
5. Manage Systemic Health Conditions
- Diabetes Control: If you have diabetes, strict blood sugar control is crucial for reducing your risk of periodontal disease.
- Treat Underlying Conditions: Work with your doctor to manage autoimmune diseases, inflammatory bowel disease, and other systemic conditions that can impact oral health.
- Address Gut Health: Pay attention to your digestive health. A balanced gut microbiome can support overall immune function and reduce systemic inflammation, indirectly benefiting your oral health and potentially reducing gut health bad breath.
6. Address Dry Mouth
- Identify Cause: If you experience chronic dry mouth, discuss it with your dentist or doctor. It might be a side effect of medication or an underlying condition.
- Solutions: Use saliva substitutes, drink water frequently, chew sugar-free gum, and avoid caffeine and alcohol.
7. Stress Management
- Reduce Stress: Chronic stress can weaken the immune system. Incorporate stress-reduction techniques like meditation, yoga, or regular exercise into your routine.
Risks and Complications
Untreated oral inflammation can lead to a cascade of problems, both locally in the mouth and throughout the body.
Local Complications:
- Tooth Loss: This is the most severe local complication of periodontitis. As the bone and supporting tissues are destroyed, teeth become loose and eventually fall out or need extraction.
- Dental Abscesses: Pockets of pus can form in the gums or around the roots of teeth, causing severe pain and swelling.
- Bone Loss: Irreversible destruction of the jawbone, affecting facial structure and future restorative options like dental implants.
- Receding Gums: Exposing tooth roots, leading to sensitivity and increased risk of root decay.
- Increased Risk of Decay: Exposed roots are softer than enamel and more prone to cavities.
- Impact on Nutrition: Pain, sensitivity, and tooth loss can make eating difficult, potentially leading to nutritional deficiencies.

Systemic Complications (Oral-Systemic Link):
The chronic inflammation and bacterial load from the mouth can enter the bloodstream, contributing to systemic health issues.
- Cardiovascular Disease: Studies show a strong link between periodontitis and an increased risk of heart attack, stroke, and other cardiovascular problems. Oral bacteria can enter the bloodstream, contributing to plaque buildup in arteries.
- Diabetes Complications: Oral inflammation can make it harder for individuals with diabetes to control their blood sugar levels, creating a vicious cycle where uncontrolled diabetes worsens gum disease, and severe gum disease worsens blood sugar control.
- Respiratory Diseases: Oral bacteria can be aspirated into the lungs, potentially leading to pneumonia, bronchitis, and other respiratory infections, especially in the elderly or immunocompromised.
- Adverse Pregnancy Outcomes: Pregnant women with periodontitis have a higher risk of preterm birth and low birth weight babies.
- Rheumatoid Arthritis: Some research suggests a link between oral bacteria (e.g., P. gingivalis) and the onset or exacerbation of rheumatoid arthritis.
- Kidney Disease: Chronic inflammation, including that from oral sources, has been implicated in the progression of chronic kidney disease.
- Alzheimer's Disease: Emerging research is exploring a potential link between periodontitis and an increased risk or acceleration of Alzheimer's disease, with oral bacteria found in the brains of affected individuals.
This robust evidence underscores why addressing oral inflammation isn't just about your teeth and gums; it's about safeguarding your entire body.
Children / Pediatric Considerations
Oral inflammation is not exclusive to adults; it can affect children too, albeit often presenting differently. Parents need to be aware of the signs and encourage good oral hygiene from an early age.
Common Types in Children:
- Gingivitis: The most common form of oral inflammation in children, often caused by inadequate brushing and flossing. It presents as red, swollen, and easily bleeding gums. It's usually mild and reversible.
- Herpetic Gingivostomatitis: A primary infection with the Herpes Simplex Virus, common in infants and young children. It causes widespread inflammation of the gums and oral mucosa, along with painful blisters, fever, and malaise.
- Aphthous Ulcers (Canker Sores): Recurrent painful sores inside the mouth, similar to those in adults, can be triggered by stress, trauma, or certain foods.
- Oral Thrush (Candidiasis): A fungal infection (Candida albicans) common in infants, presenting as white patches on the tongue and inner cheeks. It can also occur in children on antibiotics or with weakened immune systems.
- Traumatic Injuries: Children are prone to falls and accidents, which can cause cuts, bruises, or burns in the mouth, leading to localized inflammation.
- Eruption Gingivitis: Mild inflammation around erupting teeth, especially molars, as they break through the gum tissue.
Age-Specific Guidance for Parents:
- Infants (0-12 months):
- Wipe gums gently with a soft, damp cloth or infant toothbrush after feedings.
- Monitor for signs of thrush (white patches).
- Address teething discomfort (which is a form of inflammation) with teething rings or gentle gum massage.
- Toddlers (1-3 years):
- Start brushing with a tiny smear (rice-grain size) of fluoride toothpaste twice a day.
- Schedule the first dental visit by age one or when the first tooth appears.
- Supervise brushing closely.
- Preschoolers and School-Aged Children (3+ years):
- Use a pea-sized amount of fluoride toothpaste.
- Encourage independent brushing but continue to supervise and assist as needed, especially with flossing.
- Teach them the importance of regular brushing, flossing, and healthy eating.
- Limit sugary snacks and drinks.
- Ensure they wear mouthguards during sports activities to prevent oral trauma.
- Adolescents:
- Monitor for gingivitis, especially if they have braces, as oral hygiene can be more challenging.
- Discuss the dangers of smoking, vaping, and oral piercings, which can significantly contribute to oral inflammation and other complications.
- Reinforce the importance of consistent oral hygiene, even with busy schedules.
Pro Tip for Parents: Make oral hygiene a fun routine rather than a chore. Use engaging toothbrushes, timers, or apps to encourage consistent and thorough brushing and flossing.
Cost Breakdown
A more detailed look at the financial aspects of managing oral inflammation can help you plan and budget for necessary care.
Average US Costs (Low, Mid, High)
These are general ranges and can fluctuate based on location, practitioner, and specific case complexity.
| Procedure | Low Range (e.g., rural/general dentist) | Mid Range (e.g., suburban/general dentist) | High Range (e.g., metro/specialist) |
|---|---|---|---|
| Initial Exam & X-rays | $50 - $150 | $100 - $250 | $150 - $400 |
| Standard Cleaning | $75 - $125 | $100 - $175 | $150 - $200+ |
| Scaling & Root Planing (per quadrant) | $200 - $350 | $300 - $450 | $400 - $600+ |
| Periodontal Maintenance (per visit) | $100 - $175 | $150 - $250 | $200 - $350+ |
| Gingivectomy (minor gum reshaping) | $300 - $600 (per quadrant) | $500 - $1,000 | $800 - $1,500+ |
| Bone Graft (per site) | $600 - $1,500 | $1,000 - $2,500 | $2,000 - $4,000+ |
| Soft Tissue Graft (per site) | $700 - $1,600 | $1,200 - $2,800 | $2,500 - $4,500+ |
With vs. Without Insurance:
- Without Insurance: You will be responsible for the full sticker price of all procedures. This is why many uninsured individuals delay care, leading to more expensive problems down the line.
- With Insurance:
- Your annual deductible (e.g., $50 - $150) must be met before your plan starts paying.
- Co-pays are fixed amounts you pay at the time of service (e.g., $10 - $50 for a cleaning).
- Coinsurance is a percentage of the cost you pay after your deductible (e.g., 20-50%).
- Annual maximums (typically $1,000 - $2,000) limit how much the insurance company will pay in a year. Once reached, you pay 100% of subsequent costs.
Payment Plans and Financing Options:
- In-Office Payment Plans: Many dental offices offer their own payment plans, allowing you to pay in installments. These are usually interest-free for a short period.
- Third-Party Financing (e.g., CareCredit, LendingClub): These are healthcare credit cards or loans specifically designed for medical and dental expenses. They often offer deferred interest options for 6-24 months if paid in full, or low-interest financing for longer terms.
- Dental Discount Plans: These are not insurance but offer a reduced fee for dental services from participating providers (e.g., 10-60% off). You pay an annual membership fee.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have these, you can use pre-tax dollars to pay for dental care, including oral inflammation treatments.
Cost-Saving Tips:
- Preventive Care: The best cost-saving tip is prevention. Regular cleanings and good home care minimize the need for expensive treatments.
- Shop Around: Fees can vary between dentists and specialists. Get a few quotes for major procedures.
- Ask for Cash Discounts: Many offices offer a discount (e.g., 5-10%) for patients paying in full at the time of service without using insurance.
- Utilize Dental Schools: Dental schools often provide high-quality care at reduced costs, as procedures are performed by students under the supervision of experienced faculty.
- Community Health Clinics: Some community clinics offer sliding scale fees based on income for those without insurance.
Frequently Asked Questions
What is the primary cause of oral inflammation?
The most common cause of oral inflammation, particularly in the gums, is plaque buildup due to insufficient oral hygiene. Bacteria in plaque release toxins that irritate the gum tissue, leading to an inflammatory response.
Can oral inflammation affect my overall health?
Absolutely. Chronic oral inflammation, especially periodontitis, has been linked to an increased risk or exacerbation of various systemic conditions, including heart disease, diabetes, respiratory issues, adverse pregnancy outcomes, and even potentially Alzheimer's disease.
Does bad gut health cause bad breath?
Yes, bad gut health can contribute to bad breath. While most bad breath originates in the mouth, an imbalanced gut microbiome can lead to systemic inflammation or the release of odorous gases that travel up the esophagus, thus contributing to halitosis. It also weakens the body's ability to fight oral infections.
Is oral inflammation painful?
The level of pain varies. Mild gingivitis might cause only slight tenderness or no pain at all. However, severe periodontitis, stomatitis, or abscesses can cause significant pain, discomfort, and difficulty with eating and speaking.
How long does it take to treat oral inflammation?
Mild inflammation like gingivitis can resolve in a few days to a couple of weeks with improved oral hygiene and professional cleaning. More severe conditions like periodontitis require ongoing treatment, with initial procedures like deep cleaning spanning 1-2 appointments and surgical recovery taking weeks to months.
What is the cost of treating severe oral inflammation?
Treating severe oral inflammation (periodontitis) can range from several hundred dollars for non-surgical deep cleanings (e.g., $800-$2,400 for a full mouth) to several thousands for surgical interventions and grafts (e.g., $2,000-$10,000+), depending on complexity and the number of affected sites.
Can oral inflammation be completely cured?
Gingivitis is fully reversible. Periodontitis, however, involves irreversible bone loss, so it cannot be "cured" in the sense of regenerating all lost tissue. However, its progression can be halted and managed effectively with consistent professional treatment and diligent home care.
Are there home remedies for oral inflammation?
While home remedies like saltwater rinses can provide temporary relief and aid healing, they are not a substitute for professional dental treatment. For persistent or severe inflammation, a dentist must be consulted to address the underlying cause.
What is periodontal maintenance?
Periodontal maintenance is a specialized cleaning performed more frequently (typically every 3-4 months) for individuals who have undergone treatment for periodontitis. It's crucial for controlling bacteria, preventing recurrence, and maintaining gum health long-term.
Can my diet influence oral inflammation?
Absolutely. A diet rich in inflammatory foods (sugars, processed foods) can exacerbate inflammation systemically, including in the mouth. Conversely, a diet rich in anti-inflammatory foods (fruits, vegetables, omega-3s) supports oral and overall health.
When to See a Dentist
Knowing when to seek professional dental care is critical for managing oral inflammation effectively and preventing its progression.
Routine Care vs. Warning Signs:
- Routine Care: You should schedule a dental check-up and professional cleaning at least once every six months, even if you don't have any noticeable symptoms. Regular preventive care is the best defense against oral inflammation.
- Warning Signs for a Scheduled Appointment (within a few days/week):
- Gums that consistently bleed when you brush or floss.
- Persistent red, swollen, or tender gums.
- Chronic bad breath that doesn't improve with brushing.
- Gums that appear to be pulling away from your teeth (recession).
- Mild tooth sensitivity to hot or cold.
- A persistent sore or lesion in your mouth that hasn't healed within 1-2 weeks.
Red Flags Needing Prompt Attention (within 24-48 hours):
- Severe and Constant Pain: Intense, throbbing pain in your gums, teeth, or jaw that disrupts sleep or daily activities.
- Swelling of Face or Jaw: Swelling that extends beyond the gum line to your face or jaw, which could indicate a spreading infection or abscess.
- Pus Drainage: Visible pus oozing from around a tooth or gum.
- Loose or Shifting Teeth: If a tooth suddenly feels very loose or your bite changes, it could be a sign of advanced bone loss requiring immediate assessment.
- Difficulty Swallowing or Breathing: If oral inflammation is severe enough to cause difficulty swallowing or breathing, this is an emergency that needs immediate medical or dental attention.
- Fever with Oral Symptoms: A fever accompanied by oral pain, swelling, or general malaise can indicate a serious infection.
Emergency vs. Scheduled Appointment:
- Emergency: Any severe pain, uncontrolled bleeding, facial swelling, or difficulty breathing/swallowing requires immediate attention. Contact your dentist's emergency line or go to an urgent care facility or emergency room.
- Scheduled: Most other symptoms of oral inflammation, while serious, can typically wait for a scheduled appointment with your dentist or periodontist within a reasonable timeframe (e.g., a few days to a week). Do not delay addressing warning signs, as early intervention often prevents more severe and costly problems.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Does Oil Pulling Help Gut Health
The intricate connection between our oral health and overall well-being is a topic of growing fascination and scientific inquiry. Often, when we think of health, we focus on specific organs or systems, overlooking the crucial role of the mouth as a gateway to the rest of the body. One ancient practi
February 23, 2026
Does Oil Pulling Help With Inflammation
It's a question many health-conscious individuals ask as they explore natural remedies: does oil pulling help with inflammation? In an era where holistic approaches to wellness are gaining traction, the ancient practice of oil pulling has resurfaced, promising benefits that extend beyond oral hy
February 23, 2026
Oil Pulling for Kidney Disease: Complete Guide
Chronic kidney disease (CKD) affects an estimated 37 million adults in the United States, often progressing silently until advanced stages. What many may not realize is the profound connection between the health of their mouth and the health of their kidneys. As a bridge between traditional wisd
February 23, 2026
Oil Pulling Oral Microbiome: Complete Guide
Have you ever considered the bustling universe thriving within your mouth? This intricate community, known as the oral microbiome, consists of billions of microorganisms – some beneficial, some harmful – all playing a critical role in your oral and overall systemic health. Maintaining a balanced
February 23, 2026