Diabetes and Bad Breath: Complete Guide
Key Takeaways
- Diabetes and Bad Breath: Complete Guide
Diabetes and Bad Breath: Complete Guide
Living with diabetes presents a unique set of challenges, many of which extend beyond blood sugar management to impact various aspects of your health, including your oral cavity. For the estimated 37.3 million Americans living with diabetes, and the 96 million adults with prediabetes, understanding the intricate link between systemic health and oral health is paramount. One particularly common and often distressing symptom that can signal underlying issues is persistent bad breath, medically known as halitosis. If you're wondering, "Is my diabetes and bad breath connected?" the answer is a resounding yes. This comprehensive guide will delve deep into the multifaceted relationship between diabetes and oral malodor, exploring the causes, symptoms, available treatments, and crucially, how you can prevent this often-embarrassing condition to safeguard your overall health. We'll also touch upon the broader implications for oral health, including the connection between gut health and bad breath, and potential severe outcomes like those associated with osteoporosis teeth symptoms.
Bad breath, while sometimes attributed to simple dietary choices, can be a critical indicator of uncontrolled blood sugar levels or other diabetes-related complications. Far from just a cosmetic concern, it signals an imbalance that requires attention from both your medical doctor and your dental professional. Throughout this article, we will explore the different ways diabetes impacts your oral environment, from dry mouth and gum disease to more severe conditions. You'll learn about effective strategies for managing halitosis, the importance of regular dental care, what treatments entail, and how much they might cost. Our goal is to empower you with the knowledge to maintain optimal oral health and overall well-being despite living with diabetes.
Key Takeaways:
- Direct Link: Uncontrolled diabetes significantly increases the risk and severity of persistent bad breath (halitosis) due to elevated blood sugar, dry mouth, increased susceptibility to infections, and diabetic ketoacidosis.
- Professional Dental Care: Regular dental check-ups (at least twice a year) and professional cleanings are crucial. A standard dental exam with cleaning in the US costs between $100-$300 without insurance, while deep cleaning (scaling and root planing) can range from $200-$500 per quadrant.
- Blood Sugar Control is Key: Maintaining optimal blood glucose levels (A1C below 7%) is the single most effective way to prevent and manage diabetes-related oral health issues, including bad breath.
- Oral Hygiene is Essential: Brush twice daily for two minutes with fluoride toothpaste, floss daily, and use an ADA-approved antimicrobial mouthwash. Consider a tongue scraper.
- Addressing Dry Mouth: Diabetes often causes xerostomia. Strategies include drinking plenty of water, chewing sugar-free gum, and using saliva substitutes which can cost $10-$30 per bottle/tube monthly.
- Gut-Oral Axis: Imbalances in gut microbiome, common in diabetes, can contribute to volatile sulfur compounds and bad breath. Probiotics and dietary changes may help support gut health and bad breath improvement.
- Early Intervention: Don't ignore persistent bad breath, especially if you have diabetes. It could be a sign of worsening gum disease, oral infections, or even diabetic ketoacidosis, requiring immediate medical attention.
What Is Bad Breath (Halitosis) and Its Connection to Diabetes?
Bad breath, or halitosis, is a common condition characterized by an unpleasant odor emanating from the mouth. While it can often stem from poor oral hygiene, certain foods, or smoking, persistent halitosis, particularly in individuals with diabetes, often points to more significant underlying health issues.

For someone living with diabetes, the body's inability to effectively manage blood sugar levels creates a cascade of effects that directly impact oral health. High blood glucose levels not only foster an environment where harmful bacteria thrive but also impair the body's natural defense mechanisms. This systemic connection means that if your diabetes is not well-controlled, your risk for various oral complications, including halitosis, significantly increases.
The Diabetic Oral Environment
The mouth is a complex ecosystem teeming with bacteria, both beneficial and harmful. In a healthy individual, saliva plays a crucial role in washing away food particles, neutralizing acids, and providing antimicrobial properties. However, diabetes can disrupt this delicate balance in several ways:
- Elevated Glucose Levels in Saliva: When blood glucose levels are high, some of this excess sugar can appear in the saliva. This creates a sugary feast for bacteria in the mouth, leading to increased bacterial growth and the production of volatile sulfur compounds (VSCs), which are the primary culprits behind bad breath.
- Reduced Saliva Production (Xerostomia): Diabetes, particularly when poorly managed, often leads to dry mouth. High blood sugar can damage the small blood vessels that supply the salivary glands, reducing their ability to produce saliva. Without adequate saliva, food particles and bacteria are not properly cleared, leading to a build-up of plaque, increased risk of cavities, and, inevitably, bad breath.
- Impaired Immune Response: Diabetes can weaken the immune system, making individuals more susceptible to infections. This includes oral infections like gum disease (periodontitis) and oral thrush, both of which are significant contributors to halitosis.
Understanding these foundational connections is the first step toward effectively managing and preventing diabetes and bad breath.
Causes: Why Diabetes Leads to Bad Breath
The causes of bad breath in people with diabetes are multifactorial, stemming from both direct metabolic effects and secondary complications. It's not just one factor but often a combination that creates a challenging oral environment.
1. Diabetic Ketoacidosis (DKA)
One of the most distinctive and serious causes of bad breath in individuals with diabetes, particularly Type 1, is Diabetic Ketoacidosis (DKA). This life-threatening complication occurs when the body, lacking enough insulin, starts breaking down fat for fuel. This process produces ketones, which are acidic chemicals that build up in the blood. The body tries to excrete these ketones through urine and breath.
- Distinctive Odor: The breath of someone experiencing DKA often has a very characteristic sweet, fruity, or acetone-like smell. It's often compared to nail polish remover.
- Severity: DKA is a medical emergency requiring immediate attention. If you or someone you know with diabetes exhibits this type of breath along with other symptoms like extreme thirst, frequent urination, nausea, vomiting, abdominal pain, weakness, confusion, or rapid breathing, seek emergency medical care.
2. Periodontal Disease (Gum Disease)
Periodontal disease is significantly more prevalent and severe in people with diabetes, especially those with poorly controlled blood sugar. It's a progressive inflammatory condition affecting the gums and the bone supporting the teeth.
- Bidirectional Relationship: Diabetes can worsen gum disease, and severe gum disease can, in turn, make diabetes harder to control by increasing systemic inflammation and insulin resistance.
- Bacterial Overgrowth: The pockets that form between infected gums and teeth become breeding grounds for anaerobic bacteria. These bacteria release VSCs and other foul-smelling compounds, causing persistent bad breath.
- Symptoms: Beyond halitosis, symptoms include red, swollen, tender, or bleeding gums, receding gums, pus between teeth and gums, and eventually, loose teeth. This bone loss around teeth, often a concern in patients with osteoporosis, can be a severe complication of uncontrolled diabetes and gum disease, leading to symptoms like loose teeth. This is why individuals with diabetes should be particularly vigilant about any signs of bone loss around their teeth, as it can mimic or exacerbate osteoporosis teeth symptoms.
3. Dry Mouth (Xerostomia)
As mentioned, dry mouth is a very common complication of diabetes, affecting up to 50% of individuals with the condition.
- Reduced Saliva Flow: High blood glucose levels can impair nerve function (neuropathy) that controls salivary glands or directly affect salivary gland function, leading to decreased saliva production. Certain diabetes medications can also contribute to dry mouth.
- Bacterial Accumulation: Saliva's natural cleansing and buffering actions are diminished. This allows food particles and bacteria to accumulate more easily, particularly on the tongue and around the teeth, leading to increased VSC production and bad breath.
- Increased Risk of Infections: Dry mouth also increases the risk of other oral infections, further exacerbating bad breath.
4. Oral Thrush (Candidiasis)
Oral thrush is a fungal infection caused by an overgrowth of Candida albicans yeast in the mouth. People with diabetes are more prone to thrush for several reasons:
- High Glucose in Saliva: The sugar-rich environment provides an ideal breeding ground for yeast.
- Weakened Immune System: Compromised immunity makes it harder for the body to fight off fungal overgrowth.
- Dry Mouth: Reduced saliva can allow yeast to proliferate more easily.
- Antibiotic Use: Frequent antibiotic use, common in diabetics managing various infections, can disrupt the natural oral microbiome, allowing Candida to take over.
- Symptoms: Oral thrush presents as creamy white lesions on the tongue, inner cheeks, roof of the mouth, or tonsils. These lesions can be painful and contribute to a stale, unpleasant odor.
5. Other Contributing Factors
- Poor Oral Hygiene: While not unique to diabetes, poor brushing and flossing habits significantly exacerbate the issues caused by diabetes, allowing plaque and bacteria to accumulate.
- Smoking: Smoking further impairs blood flow to the gums, weakens the immune system, and directly contributes to bad breath, making it a particularly dangerous habit for diabetics.
- Gastric Issues and Gut Health: Diabetics are more prone to gastrointestinal issues like gastroparesis (delayed stomach emptying) and gastroesophageal reflux disease (GERD). These conditions can cause food to ferment in the stomach or stomach acids to back up into the esophagus and mouth, leading to unpleasant breath. Furthermore, imbalances in the gut microbiome, often observed in diabetic individuals, have been linked to systemic inflammation and the production of malodorous compounds that can enter the bloodstream and be exhaled, influencing gut health and bad breath.
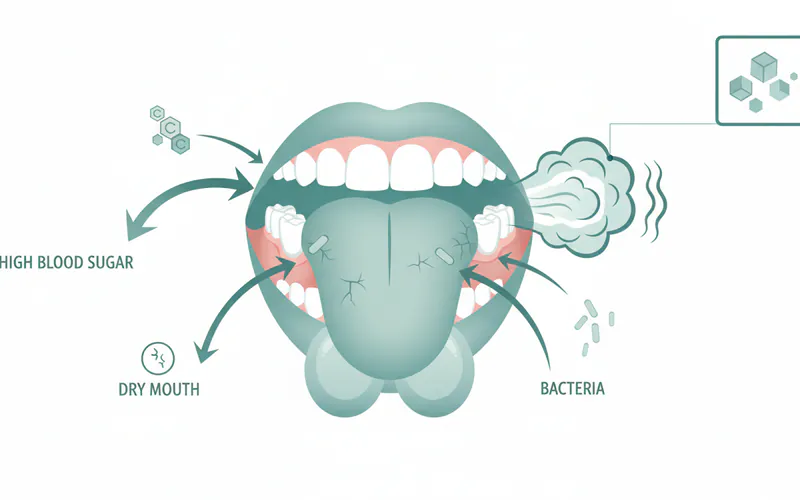
Signs and Symptoms Beyond Bad Breath
While bad breath is the primary focus, it's often accompanied by other oral symptoms in individuals with diabetes. Recognizing these signs can help you identify the underlying problem and seek timely intervention.
- Persistent Dry Mouth (Xerostomia): A constant feeling of dryness, difficulty swallowing, or speaking, and frequent thirst.
- Red, Swollen, or Bleeding Gums: Gums that are tender to the touch, bleed easily during brushing or flossing, or appear puffy. These are classic signs of gingivitis, the early stage of gum disease.
- Receding Gums: Gums pulling away from the teeth, making teeth appear longer.
- Loose or Shifting Teeth: A sign of advanced periodontal disease where bone loss is occurring, which can lead to tooth mobility and potential tooth loss. This can be especially concerning for individuals already at risk for bone density issues, mirroring some osteoporosis teeth symptoms.
- Sores that Don't Heal: Mouth sores, cuts, or infections that take longer than usual to heal. Diabetes impairs the body's healing process.
- White Patches in the Mouth (Thrush): Creamy white lesions on the tongue, inner cheeks, or roof of the mouth, which may be painful or bleed slightly when scraped.
- Foul Taste in the Mouth: A persistent bitter, metallic, or generally unpleasant taste, even after brushing.
- Frequent Oral Infections: Repeated occurrences of gum infections, abscesses, or thrush.
If you experience any of these symptoms in conjunction with persistent bad breath, it's crucial to consult your dentist and physician to ensure comprehensive management of your diabetes and oral health.
Treatment Options for Diabetes-Related Bad Breath
Effectively treating diabetes-related bad breath requires a two-pronged approach: rigorous diabetes management and targeted oral health interventions. Addressing only one aspect will likely yield limited results.
1. Optimal Diabetes Management (The Foundation)
This is the most critical step. Without consistent control of blood glucose levels, other treatments for bad breath will be less effective.
- Medication Adherence: Take all prescribed diabetes medications (insulin, oral hypoglycemics) exactly as directed by your physician.
- Dietary Management: Follow a balanced, low-sugar diet recommended by your doctor or a registered dietitian.
- Regular Exercise: Physical activity helps improve insulin sensitivity and glucose control.
- Blood Glucose Monitoring: Regularly check your blood sugar levels to ensure they stay within your target range. Aim for an A1C below 7% as recommended by the American Diabetes Association (ADA).
2. Enhanced Oral Hygiene Practices
Even with well-controlled diabetes, excellent oral hygiene is non-negotiable.
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush gently for at least two minutes, covering all tooth surfaces and the gum line. Consider an electric toothbrush for enhanced plaque removal.
- Floss Daily: Floss thoroughly between all teeth and just below the gum line to remove plaque and food particles that brushing can't reach.
- Tongue Scraper: A significant source of bad breath bacteria resides on the tongue. Use a tongue scraper daily to remove this bacterial film.
- Antimicrobial Mouthwash: Use an ADA-approved therapeutic mouthwash, preferably alcohol-free, to reduce bacteria. Rinse for 30-60 seconds daily.
- Pros: Reduces bacterial load, freshens breath temporarily, can help with gingivitis.
- Cons: Can mask underlying issues, some alcohol-containing rinses can further dry the mouth.
- Hydration: Drink plenty of water throughout the day to help wash away food particles and bacteria, especially if experiencing dry mouth.
3. Professional Dental Care
Regular visits to your dentist are vital for preventing and treating diabetes-related oral complications.
- Routine Check-ups and Cleanings: Schedule professional cleanings at least twice a year, or more frequently if recommended by your dentist (e.g., every 3-4 months for those with active gum disease). These cleanings remove plaque and tartar build-up that cannot be removed by brushing alone.
- Periodontal Treatment: If you have gum disease, your dentist or periodontist may recommend:
- Scaling and Root Planing (Deep Cleaning): This procedure involves thoroughly cleaning the root surfaces below the gum line to remove plaque and tartar and smoothing the root to remove bacterial toxins.
- Pros: Highly effective for early to moderate gum disease, can halt progression.
- Cons: Can cause temporary sensitivity, may require local anesthetic, typically performed in multiple appointments.
- Antibiotics: Oral or topical antibiotics may be prescribed to control bacterial infection.
- Laser Therapy or Surgery: For advanced cases, surgical procedures may be needed to reduce pocket depth or regenerate lost bone and tissue.
- Scaling and Root Planing (Deep Cleaning): This procedure involves thoroughly cleaning the root surfaces below the gum line to remove plaque and tartar and smoothing the root to remove bacterial toxins.
- Management of Dry Mouth: Your dentist can recommend various solutions:
- Over-the-counter (OTC) Saliva Substitutes: Sprays, gels, and lozenges (e.g., Biotene, Oasis) provide temporary relief and lubrication.
- Pros: Accessible, easy to use, provide immediate comfort.
- Cons: Temporary effects, not a cure, can be costly over time.
- Prescription Medications: Pilocarpine (Salagen) or cevimeline (Evoxac) can stimulate saliva production, but come with potential side effects.
- Pros: More sustained relief, can significantly improve quality of life.
- Cons: Prescription required, potential side effects (e.g., sweating, nausea).
- Over-the-counter (OTC) Saliva Substitutes: Sprays, gels, and lozenges (e.g., Biotene, Oasis) provide temporary relief and lubrication.
- Treatment for Oral Thrush:
- Antifungal Medications: Typically prescribed as lozenges, rinses, or systemic pills (e.g., Nystatin, Fluconazole).
- Pros: Effective at clearing fungal infections.
- Cons: Requires prescription, potential side effects, may interact with other medications.
- Antifungal Medications: Typically prescribed as lozenges, rinses, or systemic pills (e.g., Nystatin, Fluconazole).
Pro Tip: Always inform your dentist about your diabetes diagnosis, medications, and recent A1C levels. This information is crucial for tailoring your dental care and recognizing potential complications.
Step-by-Step Process: What to Expect During Treatment
Addressing diabetes and bad breath involves a systematic approach, often coordinated between your medical doctor and your dental team.
Step 1: Initial Assessment (Medical and Dental)
- Medical Assessment: Your physician will evaluate your diabetes control, including reviewing your A1C, blood glucose logs, medications, and overall health status. They will rule out conditions like DKA.
- Dental Exam: Your dentist will conduct a thorough oral examination.
- Visual Inspection: Looking for signs of gum inflammation, plaque, tartar, cavities, oral thrush, or other lesions.
- Periodontal Probing: Measuring the depth of gum pockets around each tooth to assess for gum disease.
- Saliva Flow Measurement: Checking for dry mouth.
- Breath Test: Some dentists use specific devices to measure VSCs, which cause bad breath.
- Medical History Review: Providing your dentist with a complete medical history, including your diabetes diagnosis, medications, and any other health conditions, is crucial.
Step 2: Diagnosis and Treatment Planning
Based on the assessments, your dentist will diagnose the specific cause(s) of your bad breath and formulate a personalized treatment plan. This plan will integrate with your diabetes management.

- For DKA: Immediate medical emergency care is required.
- For Periodontal Disease: A plan for professional cleanings (e.g., scaling and root planing) and potentially adjunctive antibiotics will be outlined.
- For Dry Mouth: Recommendations for saliva substitutes, lifestyle changes, or prescription medications.
- For Oral Thrush: Prescription for antifungal medication.
- For General Halitosis: Emphasis on improved oral hygiene and possibly specific mouthwashes.
Step 3: Treatment Implementation
This phase involves carrying out the prescribed treatments.
- Dental Procedures: Undergo professional cleanings, deep cleanings (if needed), and any other recommended dental procedures. These are typically done over one or more appointments.
- Medication: Start taking any prescribed antifungal medications or saliva stimulants.
- Oral Hygiene Education: Your dental hygienist will provide detailed instructions on proper brushing, flossing, and tongue scraping techniques.
- Lifestyle Modifications: Implement recommended changes such as increased water intake, dietary adjustments, and smoking cessation.
Step 4: Follow-up and Maintenance
Regular follow-up is critical for long-term success.
- Dental Recall: Attend scheduled follow-up appointments with your dentist (e.g., every 3-6 months) for maintenance cleanings and monitoring of your oral health.
- Medical Follow-up: Continue to manage your diabetes closely with your physician, ensuring your blood glucose levels remain stable.
- Self-Monitoring: Continuously monitor your own oral hygiene habits and any changes in your breath or oral health, reporting concerns promptly to your dental or medical team.
Pro Tip: Consistency is paramount. Even with the best treatments, if you revert to poor oral hygiene or neglect your diabetes management, bad breath and other oral complications will likely return.
Cost and Insurance: Understanding US Price Ranges
The cost of dental care in the US can vary significantly based on your location, the dentist's fees, the complexity of the treatment, and your insurance coverage. Here's a general breakdown for procedures relevant to diabetes and bad breath:
Common Procedures and Average US Costs (Without Insurance)
| Procedure | Low Range (USD) | Mid Range (USD) | High Range (USD) | Description |
|---|---|---|---|---|
| Dental Exam (New Patient) | $50 | $100 | $200 | Comprehensive oral evaluation, typically includes X-rays. |
| Routine Cleaning (Prophylaxis) | $75 | $125 | $200 | Standard cleaning for healthy gums, removes plaque and tartar above the gum line. Often covered twice yearly by insurance. |
| Scaling & Root Planing (per quadrant) | $200 | $350 | $500 | Deep cleaning for gum disease, removes plaque and tartar from below the gum line. 4 quadrants total. |
| Antifungal Medication (Oral Thrush) | $10 | $50 | $100 | Cost for a typical course of Nystatin or Fluconazole, varies by type and duration. |
| Saliva Substitutes (OTC) | $10/month | $20/month | $30/month | Sprays, gels, lozenges for dry mouth relief. |
| Prescription Saliva Stimulants | $50/month | $150/month | $300/month | Pilocarpine, Cevimeline (may be partially covered by medical insurance). |
| Periodontal Maintenance (after deep cleaning) | $100 | $175 | $250 | Special cleanings for patients with a history of gum disease, usually every 3-4 months. |
Note: These are average ranges. Urban areas and specialist fees tend to be higher. Always ask for a detailed estimate before starting treatment.
Insurance Coverage
- Dental Insurance (PPO/HMO):
- Routine Cleanings & Exams: Most dental insurance plans (PPO, HMO) cover 100% of preventive care (two exams and cleanings per year) after any deductible is met.
- Basic Procedures (Fillings, Scaling & Root Planing): Typically covered at 50-80%. Scaling and root planing is usually considered a basic or major procedure, depending on the plan.
- Major Procedures (Surgery, Crowns): Often covered at 50% or less, with higher deductibles.
- Annual Maximums: Most dental plans have an annual maximum benefit, typically ranging from $1,000 to $2,000. Once you reach this limit, you pay out-of-pocket.
- Medical Insurance (for diabetes management and some related oral issues):
- Diabetes Medications: Covered by most medical plans, though co-pays and deductibles apply.
- Prescription Saliva Stimulants: May be covered by your medical insurance, as they are often prescribed for a systemic condition (dry mouth).
- Oral Thrush Medications: Often covered by medical insurance if prescribed by a physician or dentist.
- Medicare/Medicaid:
- Medicare: Original Medicare generally does NOT cover routine dental care. Some Medicare Advantage (Part C) plans may include limited dental benefits.
- Medicaid: Varies significantly by state. Many state Medicaid programs offer some dental benefits for adults, which may include exams, cleanings, and basic restorative care.
Pro Tip: Always call your insurance provider directly to confirm coverage for specific procedures before your appointment. Ask about deductibles, co-pays, percentages covered, and annual maximums.
Recovery and Aftercare
Recovery from dental treatments aimed at resolving bad breath linked to diabetes is generally straightforward, but it requires consistent effort and adherence to aftercare instructions.
Immediate Aftercare (Post-Dental Procedures)
- Scaling and Root Planing: You might experience temporary gum sensitivity, soreness, or minor bleeding for a few days. Over-the-counter pain relievers (like ibuprofen) can help. Your dentist may recommend a special antimicrobial rinse for a short period.
- Tooth Sensitivity: If you experience sensitivity after deep cleaning, use a desensitizing toothpaste.
- Diet: Stick to soft foods for the first day or two after deep cleaning to avoid irritating sensitive gums.
Long-Term Aftercare
The cornerstone of long-term success is unwavering commitment to both your diabetes management and your oral hygiene.
- Strict Blood Glucose Control: This cannot be overstressed. Maintaining stable blood sugar levels is the single most effective way to prevent the recurrence of diabetes-related bad breath and other oral complications. Regular monitoring, medication adherence, and a healthy lifestyle are essential.
- Excellent Home Oral Hygiene:
- Brush twice daily with fluoride toothpaste for two minutes.
- Floss daily.
- Use a tongue scraper daily.
- Use an ADA-approved antimicrobial mouthwash as recommended.
- Regular Dental Visits: Continue with your prescribed recall schedule (often every 3-4 months for those with a history of gum disease, or every 6 months for general maintenance). These visits allow your dental team to monitor your oral health, remove any new plaque and tartar, and address issues before they become severe.
- Hydration and Saliva Management: If you suffer from dry mouth, continue to:
- Drink plenty of water.
- Chew sugar-free gum or suck on sugar-free candies to stimulate saliva.
- Use saliva substitutes (sprays, gels) as needed.
- Healthy Lifestyle Choices:
- Quit Smoking: Smoking significantly worsens gum disease and dry mouth, making bad breath more severe and harder to treat.
- Balanced Diet: Limit sugary and acidic foods and drinks that can contribute to bacterial growth and dry mouth. Include fibrous vegetables and fruits.
- Manage Stress: Stress can impact blood sugar levels and overall health.
Prevention: Stopping Diabetes-Related Bad Breath Before It Starts
Prevention is always better than cure, especially when it comes to diabetes and bad breath. Proactive measures can significantly reduce your risk.
- Aggressive Diabetes Management:
- Maintain Target A1C: Work with your doctor to keep your A1C below 7% and your daily blood glucose readings within target ranges. This is the primary defense against most diabetes-related complications, including oral issues.
- Medication Adherence: Take all prescribed diabetes medications consistently.
- Healthy Diet: Prioritize whole, unprocessed foods, control carbohydrate intake, and avoid excessive sugars.
- Regular Physical Activity: Incorporate exercise into your daily routine.
- Impeccable Oral Hygiene:
- Brush and Floss Daily: This is foundational. Mechanical removal of plaque and food particles prevents bacterial build-up.
- Use a Tongue Scraper: This significantly reduces bacteria on the tongue, a major source of VSCs.
- Antimicrobial Mouthwash: Use as an adjunct to brushing and flossing.
- Routine Dental Check-ups:
- Don't Skip Appointments: Schedule professional cleanings and exams at least twice a year. Your dentist can detect early signs of gum disease or other problems before they escalate.
- Inform Your Dentist: Always remind your dental team of your diabetes diagnosis, even if it's well-controlled.
- Stay Hydrated: Drink water regularly throughout the day to combat dry mouth, especially if you take medications that cause dryness.
- Avoid Tobacco Products: Smoking severely compromises oral health and worsens diabetes complications. Quitting is one of the most impactful steps you can take.
- Healthy Gut, Healthy Breath: Consider incorporating probiotics through diet (fermented foods) or supplements to support a balanced gut microbiome. A healthy gut contributes to overall systemic health and can indirectly influence gut health and bad breath.
- Manage Other Health Conditions: Address any co-existing conditions like GERD or allergies that can contribute to bad breath.
Risks and Complications of Untreated Diabetes-Related Bad Breath
Ignoring persistent bad breath when you have diabetes is not just a social inconvenience; it can lead to severe health consequences.
- Worsening Periodontal Disease: Untreated halitosis often indicates active gum disease. This can progress from gingivitis to severe periodontitis, leading to:
- Gum Recession: Gums pulling away from teeth.
- Bone Loss: Destruction of the bone supporting teeth, mimicking or exacerbating osteoporosis teeth symptoms.
- Tooth Mobility and Loss: Eventually, teeth can become loose and fall out or require extraction.
- Difficulty Controlling Blood Sugar: The chronic inflammation associated with advanced gum disease can increase insulin resistance, making it much harder to manage your diabetes and keep blood glucose levels in target range. This creates a vicious cycle where poor diabetes control worsens gum disease, and vice versa.
- Increased Risk of Systemic Complications: Periodontal disease is linked to an increased risk of heart disease, stroke, kidney disease, and other serious health problems, particularly in individuals with diabetes, due to the spread of inflammation and bacteria throughout the body.
- Oral Infections: Untreated dry mouth and high sugar levels can lead to recurrent oral thrush and other bacterial or fungal infections, causing discomfort and potentially spreading.
- Nutritional Deficiencies: Pain from gum disease, tooth loss, or oral infections can make it difficult to chew and eat a healthy diet, leading to nutritional deficiencies.
- Impact on Quality of Life: Persistent bad breath can significantly affect self-confidence, social interactions, and overall mental well-being, leading to anxiety and social isolation.
- Missed Diagnosis of DKA: If the distinctive fruity breath of DKA is dismissed as "just bad breath," it can delay crucial emergency medical treatment, putting your life at risk.
Comparison Tables
Comparison of Diabetic Bad Breath Types
| Type of Bad Breath | Primary Cause | Odor Description | Associated Symptoms | Urgency for Medical Attention |
|---|---|---|---|---|
| Diabetic Ketoacidosis (DKA) | High ketones due to severe insulin deficiency | Sweet, fruity, acetone-like (like nail polish remover) | Extreme thirst, frequent urination, nausea, vomiting, abdominal pain, confusion, rapid breathing, fatigue. | Emergency |
| Periodontal Disease | Anaerobic bacteria in gum pockets | Rotten eggs, sulfurous, stale, generally unpleasant | Red/swollen/bleeding gums, receding gums, pus, loose teeth, foul taste. | High (dental/medical) |
| Dry Mouth (Xerostomia) | Reduced saliva flow | Stale, general bad breath, persistent dryness | Sticky mouth, difficulty swallowing/speaking, frequent thirst, increased cavities, burning sensation in mouth. | Moderate (dental/medical) |
| Oral Thrush | Candida yeast overgrowth | Mildly unpleasant, sometimes yeasty, stale | Creamy white patches, soreness, burning, difficulty tasting. | Moderate (dental) |
| Gastric Issues (GERD/Gut) | Acid reflux, fermentation in gut/stomach | Sour, regurgitated, onion/garlic-like (if consumed) | Heartburn, indigestion, burping, stomach discomfort. (Links to gut health and bad breath due to systemic impact of gut imbalances). | Moderate (medical) |
Comparison of Oral Hygiene Products for Bad Breath
| Product Type | Pros | Cons | Average Monthly Cost (USD) |
|---|---|---|---|
| Fluoride Toothpaste | Essential for cavity prevention, helps remove plaque. | Does not directly treat systemic bad breath causes. | $3 - $10 |
| Soft-Bristle Toothbrush | Gentle on gums, effective plaque removal. | Manual brushing requires proper technique; electric brushes are more effective. | $5 - $20 (manual) / $50-$200 (electric initial, $5-$15 replacement heads) |
| Dental Floss/Interdental Brushes | Crucial for removing interdental plaque and food. | Can be difficult to use for some, requires consistent daily effort. | $3 - $10 |
| Tongue Scraper | Very effective at removing bacteria from tongue surface. | Must be used correctly to be effective. | $5 - $15 |
| Antimicrobial Mouthwash (Alcohol-Free) | Kills bacteria, freshens breath, helps with gingivitis. | Temporary effect, can mask underlying issues, some active ingredients may stain teeth over long term. | $5 - $15 |
| Saliva Substitutes (OTC) | Provides temporary relief for dry mouth, lubricates. | Temporary, does not address root cause of dry mouth. | $10 - $30 |
Children / Pediatric Considerations
Diabetes, particularly Type 1, affects millions of children and adolescents in the US. The link between diabetes and bad breath is just as relevant, if not more critical, for this younger population. Parents of children with diabetes need to be especially vigilant about their child's oral health.
- Type 1 Diabetes Prevalence: The Centers for Disease Control and Prevention (CDC) estimates that over 210,000 children and adolescents under 20 years old in the U.S. have been diagnosed with type 1 diabetes.
- Early Onset of Oral Issues: Children with poorly controlled diabetes are at an increased risk for:
- Early Childhood Caries (Cavities): High sugar levels in saliva accelerate tooth decay.
- Gingivitis and Early Periodontal Disease: Inflammation of the gums can start at a young age.
- Oral Thrush: Common in infants and young children with diabetes.
- Bad Breath: Can be an early sign of poor blood sugar control or emerging oral infections.
- Diabetic Ketoacidosis (DKA) in Children: DKA is a serious concern for children with Type 1 diabetes. Parents must be aware of the fruity breath odor as a key sign of DKA and seek emergency care immediately.
- Parental Role in Oral Hygiene: Parents play a crucial role in establishing good oral hygiene habits from an early age:
- Supervised Brushing and Flossing: Help younger children brush twice daily with fluoride toothpaste and floss daily.
- Dietary Guidance: Limit sugary snacks and drinks. Encourage water consumption.
- Regular Pediatric Dental Visits: Schedule dental check-ups every six months, informing the pediatric dentist about the child's diabetes status. The ADA recommends children see a dentist by their first birthday.
- Open Communication: Encourage children and teens to talk about any discomfort or changes in their mouth, including persistent bad breath. Open communication between parents, the child, the pediatrician, and the pediatric dentist is key to holistic diabetes and oral health management.
Pro Tip: Make oral hygiene a fun, consistent routine. Use colorful toothbrushes, flavored toothpaste (sugar-free), and lead by example. Empowering children to take ownership of their oral health early can have lifelong benefits.
Cost Breakdown (Consolidated)
While individual costs vary, here's a consolidated look at what you might expect to pay for the management of diabetes and bad breath in the US:

- Preventive Care (Routine Exam + Cleaning):
- Without Insurance: $100 - $300 (per visit, usually twice a year)
- With Insurance: Often 100% covered after deductible, or a low co-pay ($0-$50)
- Deep Cleaning (Scaling & Root Planing):
- Without Insurance: $800 - $2,000 (for all four quadrants)
- With Insurance: Typically 50-80% covered, leaving you with $160 - $1000 out-of-pocket (depending on coverage and annual max).
- Periodontal Maintenance (after deep cleaning):
- Without Insurance: $100 - $250 (per visit, often 3-4 times a year)
- With Insurance: Often 50-80% covered, similar to regular cleaning.
- Medications (Antifungals, Saliva Stimulants):
- Antifungal Course (e.g., Nystatin): $10 - $100 (often covered by medical insurance with co-pay).
- Prescription Saliva Stimulants: $50 - $300 per month (co-pays apply with medical insurance).
- Over-the-Counter Products:
- Toothpaste, mouthwash, floss, tongue scraper, saliva substitutes: $20 - $70 per month.
Payment Plans and Financing Options
- In-Office Payment Plans: Many dental offices offer interest-free payment plans for larger treatments, allowing you to spread the cost over several months.
- Dental Discount Plans: These are not insurance but offer reduced fees at participating dentists for an annual membership fee (e.g., Aetna Dental Access, Cigna Dental Savings).
- Healthcare Credit Cards: Services like CareCredit offer special financing options for health expenses, often with interest-free periods if paid in full within a certain timeframe.
- Flexible Spending Accounts (FSAs) / Health Savings Accounts (HSAs): If you have an FSA or HSA through your employer, you can use pre-tax dollars to pay for qualified medical and dental expenses.
Cost-Saving Tips
- Preventive Care: The best way to save money is to prevent major problems. Regular exams and cleanings are far less expensive than treating advanced gum disease or tooth loss.
- Shop Around: Get quotes from a few different dental offices for major procedures.
- Ask About Bundled Services: Some dentists may offer a discount if you commit to a comprehensive treatment plan.
- Negotiate: Don't be afraid to discuss payment options or potential discounts, especially if you're paying out-of-pocket.
- Good Insurance Coverage: Invest in a dental insurance plan that adequately covers your anticipated needs, especially if you have chronic conditions like diabetes.
Frequently Asked Questions
### What causes the fruity smell in diabetic breath?
The fruity smell, often compared to nail polish remover, is caused by the presence of ketones in the breath. This occurs during Diabetic Ketoacidosis (DKA), a severe complication where the body burns fat for fuel due to insufficient insulin, producing acidic ketones as a byproduct that are then exhaled.
### Can bad breath from diabetes go away completely?
Yes, in many cases, bad breath related to diabetes can significantly improve or go away, especially with optimal blood sugar control. Addressing underlying causes like gum disease, dry mouth, or oral thrush through targeted dental and medical treatments, combined with rigorous oral hygiene, is crucial for resolution.
### Is diabetes-related bad breath a serious health concern?
Absolutely. Persistent bad breath in diabetics is often a warning sign of uncontrolled blood sugar, developing gum disease, or even a medical emergency like DKA. Ignoring it can lead to severe oral complications like tooth loss, worsening diabetes control, and increased risk of systemic health issues.
### What if my blood sugar is well-controlled, but I still have bad breath?
Even with well-controlled blood sugar, other factors can contribute. These include specific medications that cause dry mouth, the presence of untreated gum disease from a previous period, or other oral infections like thrush. Your dentist and physician should investigate these possibilities.
### Are there specific home remedies for diabetes-related bad breath?
While not a substitute for professional care, home remedies can help manage symptoms. These include drinking plenty of water, chewing sugar-free gum, using an ADA-approved antimicrobial mouthwash, and daily tongue scraping. However, these only address symptoms and not the underlying diabetic cause.
### Do certain foods worsen bad breath for diabetics?
Yes, foods high in sugar can exacerbate the issue by feeding oral bacteria. Foods with strong odors like garlic and onions can also contribute temporarily. For diabetics, maintaining a balanced diet with controlled carbohydrates is vital to prevent blood sugar spikes that fuel oral bacteria.
### Can dental procedures for bad breath be painful?
Routine cleanings are generally not painful. Procedures like scaling and root planing (deep cleaning) may cause some discomfort, but local anesthetic is typically used to ensure comfort. Any post-procedure soreness is usually manageable with over-the-counter pain relievers.
### How long does it take to get rid of diabetes-related bad breath?
The timeline varies depending on the cause and severity. If due to DKA, breath will normalize once blood sugar is stabilized. For gum disease, improvement in breath can be noticed within weeks of deep cleaning and improved hygiene, but full resolution takes ongoing commitment. Dry mouth relief can be immediate with substitutes but requires continuous management.
### Is it possible to have "osteoporosis teeth symptoms" from diabetes?
While diabetes doesn't directly cause osteoporosis, severe, long-standing periodontal disease, which is more common and aggressive in diabetics, can lead to significant bone loss around the teeth. This bone destruction can cause loose teeth, a symptom often associated with osteoporosis teeth symptoms, and weaken the structural support for your teeth.
### What dental alternatives are there if I can't afford extensive treatment?
Discuss your financial situation with your dentist. They might offer payment plans, suggest breaking treatment into smaller, more manageable phases, or refer you to dental schools or community clinics that offer reduced-cost care. Prioritizing essential treatments like deep cleanings and extractions over elective procedures can also be a strategy.
When to See a Dentist
Given the significant link between diabetes and oral health, knowing when to seek professional dental attention is crucial.
Schedule a routine dental check-up if you have diabetes and:
- It's been six months or more since your last dental visit.
- You notice any persistent bad breath, even if you brush and floss regularly.
- You have minor gum bleeding during brushing or flossing.
- You experience occasional dry mouth.
Seek prompt dental attention (within a few days) if you notice:
- Persistent bad breath that doesn't improve with regular oral hygiene.
- Gums that are consistently red, swollen, tender, or bleed easily.
- Receding gums.
- Persistent dry mouth that makes it difficult to eat, swallow, or speak.
- Any unexplained sores or white patches in your mouth.
- A persistent foul taste in your mouth.
Seek immediate medical or emergency dental attention if you experience:
- A distinctly sweet, fruity, or acetone-like breath odor, especially if accompanied by extreme thirst, frequent urination, nausea, vomiting, abdominal pain, or confusion. This could indicate Diabetic Ketoacidosis (DKA), a medical emergency.
- Severe tooth pain or swelling around a tooth or your jaw.
- Noticeably loose or shifting teeth.
- Pus coming from your gums or around a tooth.
- Any rapidly progressing oral infection or swelling.
Remember, your dental team is an integral part of your diabetes care team. Open communication and regular visits are your best defense against oral complications and can help safeguard your overall health.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Does Oil Pulling Help Gut Health
The intricate connection between our oral health and overall well-being is a topic of growing fascination and scientific inquiry. Often, when we think of health, we focus on specific organs or systems, overlooking the crucial role of the mouth as a gateway to the rest of the body. One ancient practi
February 23, 2026
Does Oil Pulling Help With Inflammation
It's a question many health-conscious individuals ask as they explore natural remedies: does oil pulling help with inflammation? In an era where holistic approaches to wellness are gaining traction, the ancient practice of oil pulling has resurfaced, promising benefits that extend beyond oral hy
February 23, 2026
Oil Pulling for Kidney Disease: Complete Guide
Chronic kidney disease (CKD) affects an estimated 37 million adults in the United States, often progressing silently until advanced stages. What many may not realize is the profound connection between the health of their mouth and the health of their kidneys. As a bridge between traditional wisd
February 23, 2026
Oil Pulling Oral Microbiome: Complete Guide
Have you ever considered the bustling universe thriving within your mouth? This intricate community, known as the oral microbiome, consists of billions of microorganisms – some beneficial, some harmful – all playing a critical role in your oral and overall systemic health. Maintaining a balanced
February 23, 2026