Inflammation of Gums: Complete Guide
Key Takeaways
- Few health issues are as common, yet as commonly underestimated, as the inflammation of gums. Studies show that nearly half of American adults aged 30 and older suffer from some form of gum disease, the primary cause of inflamed gums. Far from being a minor inconvenience, inflamed gums are a cri
Inflammation of Gums: Complete Guide
Few health issues are as common, yet as commonly underestimated, as the inflammation of gums. Studies show that nearly half of American adults aged 30 and older suffer from some form of gum disease, the primary cause of inflamed gums. Far from being a minor inconvenience, inflamed gums are a critical indicator of your oral health, and increasingly, a signal for your overall well-being. This condition, medically known as gingivitis or, in its advanced stages, periodontitis, can lead to tooth loss and has been definitively linked to serious systemic health problems, including cardiovascular disease, diabetes, and even conditions affecting bone density like osteoporosis and teeth.
Understanding why your gums become inflamed, what it means for your health, and crucially, what you can do about it, is not just about preserving your smile – it’s about protecting your entire body. This comprehensive guide will walk you through everything you need to know, from the initial signs and symptoms to the latest treatment options, cost considerations, and essential preventive measures, empowering you to take control of your gum health.
Key Takeaways:
- Gingivitis is reversible: Mild gum inflammation (gingivitis) can often be resolved within 1-2 weeks with professional cleaning and improved home oral care.
- Periodontitis requires intervention: Advanced gum disease (periodontitis) is not curable but manageable, often requiring deep cleanings (scaling and root planing) costing $200-$600 per quadrant and potentially surgical interventions ranging from $500 to $10,000+.
- Oral-systemic link is real: Chronic gum inflammation is linked to heart disease, diabetes complications, stroke, and can exacerbate conditions like osteoporosis, affecting jawbone density and thus the stability of your teeth.
- Prevention is key: Daily brushing (twice a day for 2 minutes), flossing, and regular dental check-ups (every 6 months) are the most effective ways to prevent gum inflammation.
- Early detection saves teeth and money: Ignoring inflamed gums can lead to tooth loss, requiring expensive replacements like dental implants (up to $6,000 per tooth).
- Insurance varies: Dental insurance typically covers a portion of preventive and basic restorative services (like deep cleanings), but coverage for advanced surgical procedures can be limited, often requiring patients to pay 20-50% out-of-pocket.
What It Is: Understanding Gum Inflammation
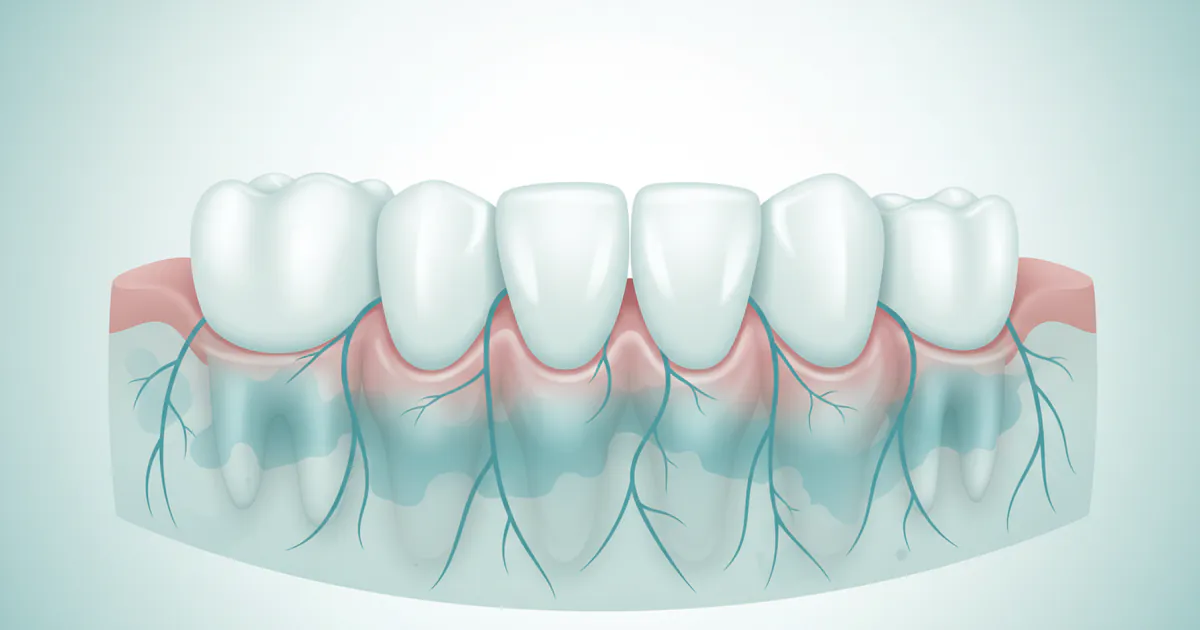
Gum inflammation is your body's immune response to harmful bacteria accumulating along the gumline. This accumulation, primarily in the form of plaque and tartar, irritates the delicate gum tissue, leading to a cascade of protective mechanisms that manifest as the classic signs of inflammation: redness, swelling, and sometimes pain or bleeding.
At its core, gum inflammation begins with plaque, a sticky, colorless film of bacteria that constantly forms on your teeth. If plaque isn't removed daily through brushing and flossing, it hardens into tartar (calculus), which is much rougher and more porous, providing an ideal breeding ground for bacteria and further irritating the gums. Tartar can only be removed by a dental professional.
When the gums are inflamed, the body sends more blood to the area to deliver immune cells, which causes the redness and swelling. This increased blood flow also makes the gums more fragile and prone to bleeding, especially during brushing or flossing.
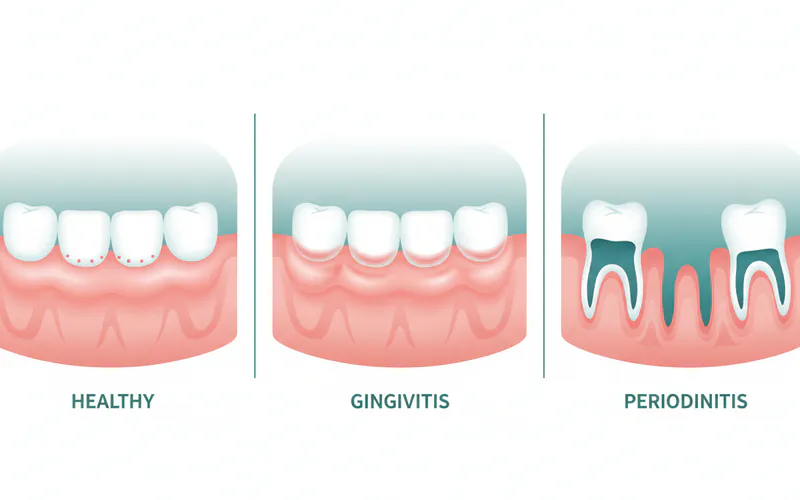
Types of Gum Inflammation: From Mild to Severe
Gum inflammation isn't a single condition; it progresses through distinct stages, each with increasing severity and potential for damage.
Gingivitis: The Reversible Stage
Gingivitis is the mildest form of gum disease and refers specifically to the inflammation of the gum tissue (gingiva) surrounding the teeth. It's characterized by:
- Red, swollen gums: The normally pale pink gums become noticeably redder and puffier.
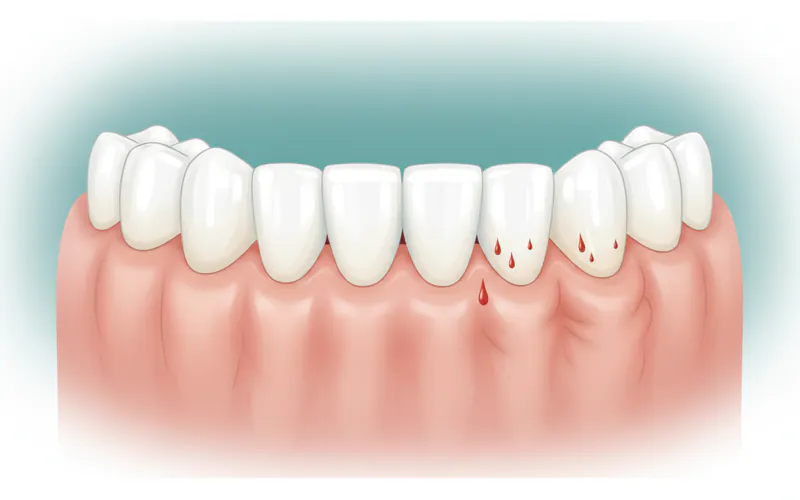
- Bleeding gums: Often the first noticeable sign, gums may bleed easily during brushing, flossing, or even spontaneous instances.
- Tenderness or discomfort: While often painless, some individuals may experience mild soreness.
- Bad breath (halitosis): Caused by the accumulation of bacteria.
Pro Tip: If you notice blood when you brush or floss, don't stop! This is a sign you need to be more diligent with your oral hygiene, not less. Gentle, thorough cleaning can often reverse gingivitis.
Gingivitis is highly prevalent, affecting a significant portion of the adult population. The good news is that it is typically reversible with professional dental cleaning (scaling) and a consistent, effective home oral hygiene routine.
Periodontitis: The Destructive Stage
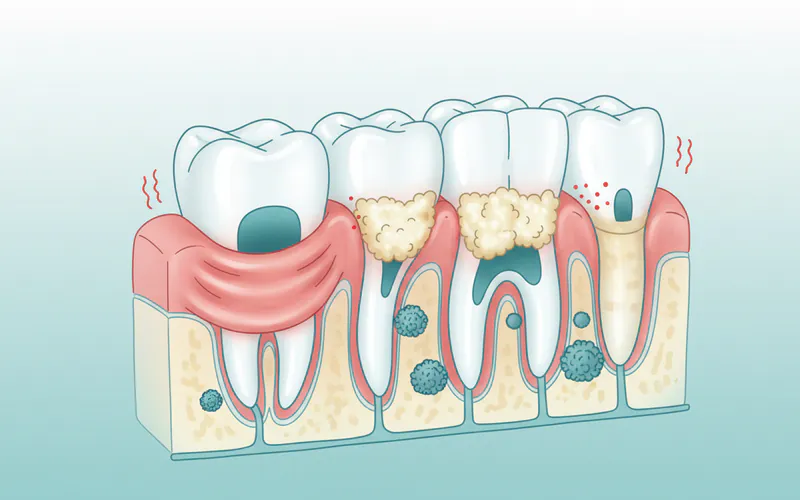
If gingivitis is left untreated, it can advance to periodontitis, a more severe and destructive form of gum disease. Periodontitis involves the breakdown of the tissues and bone that support your teeth, leading to irreversible damage. There are several forms of periodontitis:
- Chronic Periodontitis: The most common form, characterized by slow progression and often seen in adults. It involves inflammation within the supporting tissues of the teeth, progressive attachment loss, and bone loss. Pockets form between the gums and teeth, allowing plaque and bacteria to accumulate below the gumline.
- Aggressive Periodontitis: A less common but rapidly progressing form of periodontitis, often seen in younger individuals. It involves rapid attachment loss and bone destruction.
- Necrotizing Periodontal Diseases: These are severe infections characterized by the death of gum tissue, ligaments, and bone. They are more common in individuals with compromised immune systems, such as those with HIV/AIDS, malnutrition, or heavy smokers. Examples include Necrotizing Ulcerative Gingivitis (NUG) and Necrotizing Ulcerative Periodontitis (NUP).
- Periodontitis as a Manifestation of Systemic Diseases: Some systemic conditions can significantly influence the onset and progression of periodontal disease, such as diabetes, certain blood disorders, and genetic syndromes.
Unlike gingivitis, periodontitis is not curable, but it is manageable. Early diagnosis and aggressive treatment are crucial to halt its progression and preserve your teeth.
Causes: Why Gums Become Inflamed
While plaque and tartar are the immediate culprits, various factors contribute to and exacerbate gum inflammation.
Primary Cause: Poor Oral Hygiene
The most significant cause of gum inflammation is the inadequate removal of dental plaque. When plaque isn't consistently brushed and flossed away, the bacteria within it produce toxins that irritate the gum tissue, initiating the inflammatory response. Over time, plaque mineralizes into tartar, which further irritates the gums and provides a rough surface for more plaque to adhere to, creating a vicious cycle.
Contributing Factors and Risk Enhancers:
- Smoking and Tobacco Use: Tobacco users are at a significantly higher risk for developing severe gum disease. Smoking impairs the immune system's ability to fight off gum infections and also restricts blood flow to the gums, masking the typical signs of inflammation (like bleeding), making diagnosis more challenging.
- Hormonal Changes: Fluctuations in hormones, such as those occurring during pregnancy, puberty, menstruation, or menopause, can make gums more sensitive and prone to inflammation. "Pregnancy gingivitis" is a common condition.
- Certain Medications: Some drugs can cause dry mouth (xerostomia), reducing saliva's protective effects, or cause gum tissue overgrowth (gingival hyperplasia), making cleaning difficult and increasing inflammation. Examples include anticonvulsants, immunosuppressants, and some calcium channel blockers.
- Systemic Diseases:
- Diabetes: People with diabetes are more susceptible to infections, including gum disease. Uncontrolled blood sugar levels impair the body's ability to heal and fight off bacteria, leading to more severe and rapidly progressing periodontitis.
- Immune-Compromising Conditions: Diseases like HIV/AIDS weaken the immune system, making individuals more vulnerable to severe gum infections.
- Cardiovascular Disease: The link between gum disease and heart conditions is well-established, with chronic inflammation thought to play a role in hardening arteries.
- Osteoporosis and Teeth: This is a crucial connection. Osteoporosis, a condition causing bones to become brittle and weak, particularly affects bone density throughout the body, including the jawbone (alveolar bone) that supports your teeth. When this supportive bone is compromised due to osteoporosis, it can significantly worsen the progression of periodontitis. The reduced bone density means that the inflammation has an easier time destroying the underlying support structure, leading to faster attachment loss, deeper periodontal pockets, and an increased risk of tooth mobility and loss. This explains why phrases like "osteoporosis teeth" are becoming more common in dental discussions – it highlights the critical impact of systemic bone health on oral health, particularly the stability and longevity of your dentition.
- Genetic Predisposition: Some individuals are genetically more prone to developing gum disease, even with good oral hygiene.
- Poor Nutrition: A diet lacking essential nutrients, especially Vitamin C, can compromise the immune system and gum health.
- Stress: Chronic stress can weaken the immune system, making the body more susceptible to infections, including gum disease.
- Ill-fitting Dental Restorations: Crowns, bridges, or fillings that don't fit properly can create areas where plaque accumulates and is difficult to remove, contributing to inflammation.
- Teeth Grinding (Bruxism) or Clenching: While not a direct cause of gingivitis, excessive force on teeth can accelerate bone loss in individuals already suffering from periodontitis.
Signs and Symptoms: What to Look For
Recognizing the early signs of gum inflammation is vital for timely intervention. Don't wait for pain to prompt a visit to your dentist.
Early Warning Signs (Gingivitis):
- Red, Swollen, or Tender Gums: Healthy gums are typically pink and firm. Inflamed gums appear darker red, puffy, and may be tender to the touch.
- Bleeding Gums: The most common early symptom. Gums bleed easily when brushing, flossing, or sometimes even spontaneously.
- Bad Breath (Halitosis): Persistent bad breath that doesn't improve with brushing.
- Receding Gums: Gums appear to pull away from the teeth, making teeth look longer. This can expose sensitive root surfaces.
- Changes in Gum Texture: Gums may lose their stippled (orange peel-like) appearance and become smooth and shiny.
Advanced Signs (Periodontitis):
As gum disease progresses, the symptoms become more severe and indicative of structural damage:
- Persistent Bad Breath or Bad Taste: More pronounced than in gingivitis, often due to deeper bacterial pockets.
- Pus Between Teeth and Gums: A sign of active infection.
- Deep Pockets Between Teeth and Gums: This is a hallmark of periodontitis. As the gum tissue detaches from the tooth root, it forms pockets that harbor bacteria.
- Loose or Shifting Teeth: As bone support is lost, teeth may become mobile or change position, creating gaps.
- Changes in Bite: The way your upper and lower teeth fit together may change.
- Dull Aches or Sensitivity: Particularly when chewing or when teeth are exposed to hot or cold temperatures due to root exposure.
- Visible Tartar Buildup: Hardened plaque visible near the gumline.
Treatment Options: Restoring Gum Health
The treatment approach for gum inflammation depends entirely on its severity and type. The goal is always to eliminate the infection, reduce inflammation, and prevent further damage.
For Gingivitis (Mild Gum Inflammation):
- Professional Dental Cleaning (Prophylaxis): A routine cleaning performed by a dentist or dental hygienist removes plaque and tartar from above and slightly below the gumline. This is usually sufficient to reverse gingivitis.
- Pros: Non-invasive, quick, highly effective for mild cases.
- Cons: Requires patient commitment to improved home care.
- Cost: Typically $75 - $200 in the US, often fully covered by dental insurance.
- Improved Home Oral Hygiene: This is critical. Daily brushing twice a day with a fluoride toothpaste, flossing once a day, and using an antimicrobial mouthwash (if recommended) are essential.
For Periodontitis (Moderate to Severe Gum Disease):
Treatment for periodontitis aims to control the infection and prevent further bone and tissue loss. It often involves a combination of non-surgical and surgical approaches.
Non-Surgical Treatments:
- Scaling and Root Planing (Deep Cleaning): This is the cornerstone of non-surgical periodontal therapy.
- What it is: A thorough cleaning procedure where plaque and tartar are meticulously scraped away from both above and below the gumline (scaling). Then, the rough spots on the tooth roots are smoothed out (root planing) to remove bacterial toxins and prevent future plaque adhesion. This often requires local anesthesia and is typically done over 2-4 appointments, treating one quadrant of the mouth at a time.
- Pros: Highly effective for moderate periodontitis, less invasive than surgery, can significantly reduce pocket depths and inflammation.
- Cons: Can cause temporary sensitivity; requires commitment to follow-up maintenance appointments.
- Cost: Ranges from $200 - $600 per quadrant, so a full mouth deep cleaning could be $800 - $2,400. Insurance typically covers 50-80% after deductible.
- Antibiotics:
- Oral Antibiotics: Systemic antibiotics (e.g., amoxicillin, doxycycline) may be prescribed to control bacterial infection, especially for aggressive or rapidly progressing periodontitis.
- Topical Antibiotics: Antibiotic gels, chips, or microspheres can be placed directly into periodontal pockets after scaling and root planing to release medication slowly and target bacteria locally.
- Pros: Effective against specific bacteria, can aid in healing.
- Cons: Oral antibiotics can have side effects (upset stomach, yeast infections), risk of antibiotic resistance, topical forms are not a standalone solution.
- Cost: Oral antibiotics typically $10 - $50 (with insurance); topical applications can add $50 - $200 per pocket.
- Laser Therapy (Adjunctive): While not a primary treatment, lasers can be used as an adjunct to scaling and root planing to remove inflamed tissue and kill bacteria in pockets.
- Pros: Minimally invasive, potentially less bleeding and discomfort than traditional surgery.
- Cons: Efficacy compared to traditional methods is still under extensive research; can be more expensive.
- Cost: Adds $200 - $1,000+ to scaling and root planing costs, depending on the extent.
Surgical Treatments (for advanced periodontitis):
When non-surgical treatments are insufficient, or if significant bone loss has occurred, surgical intervention may be necessary.
- Flap Surgery (Pocket Reduction Surgery):
- What it is: The gums are lifted back to allow the periodontist direct access to thoroughly clean the roots and remove infected tissue and irregular bone surfaces. The gums are then sutured back into place, often snugly around the teeth, reducing pocket depth.
- Pros: Highly effective for reducing deep pockets, allows for thorough cleaning and recontouring of bone.
- Cons: More invasive, requires healing time, potential for post-operative discomfort and gum recession.
- Cost: $500 - $3,000 per quadrant, or $2,000 - $12,000 for a full mouth.
- Bone Grafting:
- What it is: Used to regenerate bone destroyed by periodontitis. Small fragments of your own bone, synthetic bone, or donated bone are placed where bone has been lost.
- Pros: Can help restore lost bone structure, stabilize loose teeth, and prepare for dental implants.
- Cons: Invasive, requires significant healing time, success varies, potential for graft rejection.
- Cost: $400 - $1,200 per tooth or site, depending on material and complexity.
- Soft Tissue Grafts:
- What it is: Used to treat gum recession, where gum tissue has pulled away from the teeth, exposing roots. Tissue is usually taken from the roof of your mouth (palate) or a donor source and attached to the receding gum area.
- Pros: Covers exposed roots, reduces sensitivity, improves aesthetics, helps prevent further recession and bone loss.
- Cons: Invasive, can be uncomfortable at the donor site, requires healing time.
- Cost: $600 - $2,000 per tooth or site.
- Guided Tissue Regeneration (GTR):
- What it is: A regenerative procedure where a small, mesh-like membrane is placed between the bone and gum tissue. This membrane prevents the gum tissue from growing into the area where bone and connective tissue should be, allowing these slower-growing cells to regenerate.
- Pros: Can regenerate lost bone and ligament, preserving teeth.
- Cons: Invasive, complex procedure, high cost, variable success rates.
- Cost: $1,000 - $4,000 per site, often combined with bone grafting.
Comparison of Periodontal Treatments
To help you understand your options, here's a comparison table for common periodontal treatments:
| Treatment Type | Purpose | Invasiveness | Typical Cost Range (US) | Recovery Time |
|---|---|---|---|---|
| Professional Cleaning (Prophylaxis) | Remove plaque/tartar, reverse gingivitis | Minimal | $75 - $200 | Immediate |
| Scaling & Root Planing (SRP) | Deep clean roots, remove bacteria/toxins | Moderate | $200 - $600 per quadrant | 1-3 days mild soreness |
| Local Antibiotic Placement | Target bacteria in pockets (adjunctive to SRP) | Minimal | $50 - $200 per pocket | None |
| Flap Surgery | Reduce deep pockets, access root surfaces | Moderate/High | $500 - $3,000 per quadrant | 1-2 weeks |
| Bone Grafting | Regenerate lost bone | High | $400 - $1,200 per site | Weeks to Months |
| Soft Tissue Grafting | Cover exposed roots, increase gum volume | High | $600 - $2,000 per site | 1-3 weeks |
| Guided Tissue Regeneration (GTR) | Regenerate bone/ligament | High | $1,000 - $4,000 per site | Weeks to Months |
Step-by-Step Process: What to Expect During Treatment
Let's detail the typical process for a common periodontitis treatment: Scaling and Root Planing (SRP).
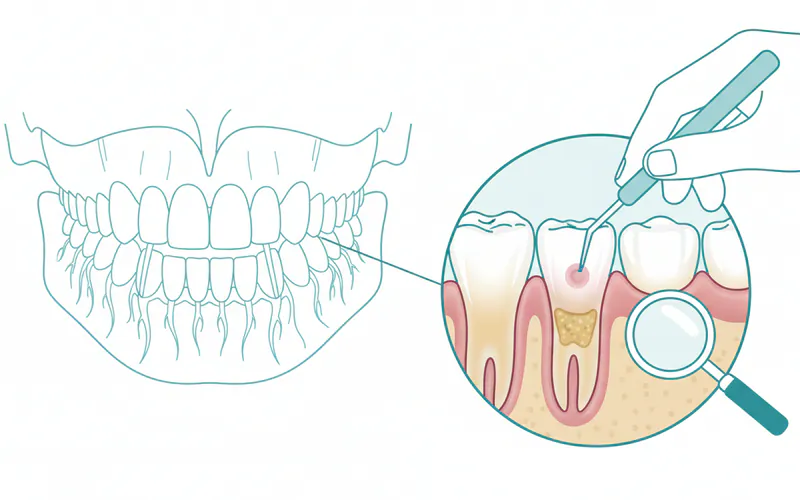
- Initial Examination and Diagnosis: Your dentist or periodontist will perform a comprehensive oral exam, including measuring pocket depths around your teeth with a periodontal probe and taking X-rays to assess bone loss. They'll review your medical history, especially noting conditions like diabetes or osteoporosis and teeth, which can influence treatment and prognosis.
- Treatment Planning: Based on the diagnosis, a customized treatment plan will be developed, outlining the number of appointments, procedures, and estimated costs.
- Local Anesthesia: Before starting, the dental professional will numb the area of your mouth being treated with local anesthesia to ensure your comfort. You will be awake but won't feel pain.
- Scaling: Using specialized instruments (ultrasonic scalers and hand scalers), the hygienist or periodontist will meticulously remove plaque and tartar from the tooth surfaces, both above and below the gumline, down into the periodontal pockets.
- Root Planing: After scaling, the root surfaces are smoothed. This removes bacterial toxins and makes it harder for plaque to reattach, promoting gum reattachment to the clean root surface.
- Irrigation and Rinsing: The pockets may be flushed with an antimicrobial solution to further reduce bacteria.
- Medication Placement (Optional): In some cases, a localized antibiotic (e.g., Arestin) may be placed directly into deep pockets to continue fighting bacteria for several days or weeks.
- Post-Procedure Instructions: You'll receive detailed instructions on post-treatment care, including managing any discomfort, maintaining oral hygiene, and dietary recommendations.
- Follow-up and Maintenance: You'll typically be scheduled for a follow-up visit (often a periodontal maintenance appointment) 4-6 weeks after SRP to assess healing and ensure the pockets are reducing. Regular periodontal maintenance cleanings (every 3-4 months, instead of 6) will be crucial to prevent recurrence.
Cost and Insurance: Understanding the Financial Aspect
The cost of treating gum inflammation varies widely based on the severity of the condition, the type of treatment required, the region of the US, and whether you have dental insurance.
Average US Price Ranges:
- Routine Cleaning (Prophylaxis): $75 - $200.
- Scaling and Root Planing (per quadrant): $200 - $600. A full mouth deep cleaning (4 quadrants) could be $800 - $2,400.
- Perio-Maintenance (after SRP): $100 - $250 per visit (more frequent than routine cleanings).
- Antibiotic Gels/Chips (per pocket): $50 - $200.
- Flap Surgery (per quadrant): $500 - $3,000.
- Bone Graft (per site/tooth): $400 - $1,200.
- Soft Tissue Graft (per site/tooth): $600 - $2,000.
- Guided Tissue Regeneration (per site): $1,000 - $4,000.
- Consultation with a Periodontist: $75 - $250 (may be applied to treatment cost if performed on the same day).
Geographic Variation: Costs tend to be higher in major metropolitan areas (e.g., New York, Los Angeles) compared to rural areas or the Midwest. For example, a quadrant of SRP might be $400 in Iowa but $650 in California.
Dental Insurance Coverage:
- Preventive Care (Routine Cleanings, X-rays): Most dental insurance plans (PPO, DPO, HMO) cover 80-100% of preventive services, often with no deductible.
- Basic Restorative Care (Scaling and Root Planing): Typically covered at 50-80% after you meet your deductible. For SRP, you might pay $40 - $120 per quadrant out-of-pocket with good insurance.
- Major Restorative Care (Surgical Procedures): Coverage is usually 0-50%, meaning you could be responsible for a significant portion of the cost. Many plans have an annual maximum benefit (e.g., $1,000 - $2,500), which can be quickly exhausted by surgical periodontal treatments.
- HMO/DMO Plans: These often have lower premiums but restrict you to a specific network of dentists and may have fixed co-payments for services, rather than percentages.
Pro Tip: Always contact your dental insurance provider directly or have your dental office submit a pre-treatment estimate ("pre-auth") to understand your exact coverage and out-of-pocket costs before proceeding with major treatments.
Recovery and Aftercare: Maintaining Your Results
Effective recovery and diligent aftercare are paramount to the long-term success of any gum inflammation treatment.
After Non-Surgical Treatments (e.g., Scaling and Root Planing):
- Discomfort: Expect some mild soreness, tenderness, and sensitivity for a few days. Over-the-counter pain relievers (e.g., ibuprofen, acetaminophen) can help.
- Sensitivity: Teeth may be more sensitive to hot, cold, or sweet foods/drinks for a few days or weeks. Using a desensitizing toothpaste can help.
- Bleeding: Minor bleeding may occur for a day or two.
- Oral Hygiene: Resume gentle brushing and flossing within 24 hours, or as advised by your dentist. Use a soft-bristled brush.
- Rinsing: Rinse with warm salt water several times a day to aid healing and reduce swelling. An antimicrobial mouthwash may also be prescribed.
- Diet: Stick to soft foods for the first 24-48 hours. Avoid very hot, cold, spicy, or crunchy foods.
- Avoid Smoking: Smoking significantly hinders healing and can undermine treatment success.
After Surgical Treatments (e.g., Flap Surgery, Grafts):
Recovery is more involved and requires stricter adherence to post-operative instructions.
- Pain and Swelling: More pronounced than non-surgical treatments. Prescription pain medication may be necessary. Apply ice packs to the outside of your face to reduce swelling.
- Bleeding: Some oozing or bleeding is normal for the first 24-48 hours.
- Dressing/Stitches: A periodontal dressing may be placed over the surgical site. Stitches (sutures) will typically dissolve or be removed within 1-2 weeks.
- Diet: A soft diet is crucial for several days to weeks. Avoid chewing near the surgical site.
- Oral Hygiene: Avoid brushing or flossing the surgical site directly for a specified period (e.g., 1-2 weeks). Your dentist will provide specific instructions, which may include gentle rinsing with prescribed mouthwash.
- Activity: Limit strenuous activity for a few days to a week to prevent increased bleeding and swelling.
- Follow-up Appointments: Essential for monitoring healing, removing sutures if needed, and ensuring proper recovery.
Long-Term Maintenance: Regardless of the treatment received, ongoing periodontal maintenance appointments (typically every 3-4 months) are critical. These specialized cleanings target deeper pockets and monitor your gum health, preventing the recurrence of disease. Your home oral hygiene routine must also remain exemplary.
Prevention: The Best Defense Against Gum Inflammation
Preventing gum inflammation is far easier, less painful, and less expensive than treating it. Adhering to these guidelines is your best defense:
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes, covering all surfaces of your teeth and gently along the gumline. Electric toothbrushes are often more effective at plaque removal.
- Floss Daily: Flossing removes plaque and food particles from between teeth and under the gumline where a toothbrush can't reach. This is non-negotiable for preventing interdental inflammation.
- Regular Dental Check-ups and Cleanings: Visit your dentist or hygienist every six months for a professional cleaning and examination. These appointments allow for early detection and removal of plaque and tartar that you might have missed.
- Use an Antimicrobial Mouthwash: While not a substitute for brushing and flossing, an ADA-approved antimicrobial mouthwash can help reduce plaque and gingivitis. Ask your dentist for a recommendation.
- Eat a Balanced Diet: Limit sugary foods and drinks that promote bacterial growth. Consume a diet rich in fruits, vegetables, and whole grains, which provide essential nutrients for gum health and a strong immune system.
- Avoid Tobacco Products: Quitting smoking or using smokeless tobacco is one of the single most impactful actions you can take to improve your gum health and overall health.
- Manage Systemic Conditions: If you have diabetes, osteoporosis, or other systemic diseases, work closely with your medical doctor to manage them effectively. Well-controlled systemic conditions significantly reduce your risk and severity of gum disease. For those concerned about osteoporosis and teeth, maintaining bone density through diet, exercise, and appropriate medication is crucial for preserving the integrity of the jawbone.
- Address Stress: Chronic stress can compromise your immune system, making you more susceptible to infections. Practice stress-reduction techniques.
- Stay Hydrated: Drinking plenty of water helps wash away food particles and bacteria, and promotes saliva production, which is a natural protector against gum disease.
Risks and Complications: When Inflammation Goes Unchecked
Ignoring gum inflammation carries significant risks, not only for your oral health but for your entire body.
Oral Complications:
- Tooth Loss: The most severe direct consequence. As periodontitis destroys the bone and connective tissue supporting your teeth, they can loosen and eventually fall out or require extraction.
- Dental Abscesses: Pockets of pus can form in the gums or jawbone, causing severe pain, swelling, and systemic infection.
- Increased Tooth Sensitivity: Exposed tooth roots due to gum recession are highly sensitive to hot, cold, and sweets.
- Changes in Bite: Shifting teeth can alter your bite, leading to problems with chewing and jaw joint (TMJ) issues.
- Need for Complex and Costly Treatments: Untreated gum disease often necessitates extensive and expensive interventions like dental implants or dentures, bone grafts, and gum surgery.
Systemic Health Complications (Oral-Systemic Link):
The mouth is a gateway to the body. Chronic inflammation in the gums can release bacteria and inflammatory mediators into the bloodstream, impacting distant organs and systems. This is a rapidly evolving area of medical research, supported by the American Dental Association (ADA) and other health organizations.
- Cardiovascular Disease: Studies show a strong link between severe gum disease and an increased risk of heart attack, stroke, and other cardiovascular problems. Chronic inflammation from the gums may contribute to the hardening of arteries (atherosclerosis).
- Diabetes: There's a bidirectional relationship. Diabetes makes individuals more susceptible to gum disease, and severe gum disease can make it harder to control blood sugar levels. This makes managing both conditions together critical.
- Respiratory Diseases: Oral bacteria from infected gums can be aspirated into the lungs, potentially leading to respiratory infections like pneumonia, especially in older adults or those with weakened immune systems.
- Adverse Pregnancy Outcomes: Pregnant women with periodontitis may have an increased risk of preterm birth and low birth weight babies.
- Rheumatoid Arthritis: Some research suggests a link between gum disease and rheumatoid arthritis, another inflammatory condition.
- Osteoporosis: As mentioned, osteoporosis and teeth have a crucial connection. While osteoporosis doesn't cause periodontitis, the systemic bone loss associated with osteoporosis can accelerate the destruction of the jawbone when periodontitis is present. This makes individuals with osteoporosis more prone to advanced bone loss around their teeth, leading to increased risk of tooth mobility and loss. Maintaining good oral health is therefore doubly important for individuals with osteoporosis to preserve their remaining osteoporosis teeth and jawbone density.
- Certain Cancers: Emerging research suggests possible associations between periodontal disease and certain cancers, though more studies are needed to establish definitive causal links.
| Disease Progression | Key Characteristics | Treatment Strategy | Potential Complications (if untreated) |
|---|---|---|---|
| Gingivitis | Red, swollen, bleeding gums; no bone loss | Professional cleaning, improved home oral hygiene | Progression to Periodontitis |
| Early Periodontitis | Minor bone loss, shallow pockets (3-4mm), early gum recession | Scaling & Root Planing (SRP), consistent home care | Moderate periodontitis, increased sensitivity, early tooth mobility |
| Moderate Periodontitis | Moderate bone loss, deeper pockets (4-6mm), noticeable gum recession | SRP, potentially local antibiotics, close monitoring | Severe periodontitis, significant tooth mobility, early tooth loss |
| Severe Periodontitis | Extensive bone loss, deep pockets (6mm+), significant tooth mobility, pus | Surgical interventions (flap surgery, grafts), antibiotics | Tooth loss, severe pain, dental abscesses, systemic health issues (heart disease, diabetes complications, aggravated bone loss with osteoporosis) |
Children / Pediatric Considerations
While often associated with adults, gum inflammation, specifically gingivitis, can affect children and adolescents. It's often milder than in adults but still requires attention.
Causes in Children:
- Poor Oral Hygiene: Inadequate brushing and flossing are the most common culprits. Children may not have the dexterity or discipline to clean effectively.
- Eruption Gingivitis: As permanent teeth erupt, the gum tissue around them can become temporarily inflamed.
- Hormonal Changes: Puberty can lead to increased gum sensitivity and inflammation, similar to pregnancy gingivitis in adults.
- Orthodontic Appliances: Braces can make cleaning more challenging, trapping food and plaque and leading to localized inflammation.
- Mouth Breathing: Can dry out gum tissue, making it more susceptible to inflammation.
- Systemic Conditions: Less common, but conditions like diabetes or certain genetic syndromes can increase a child's risk.
Signs and Symptoms in Children:
Similar to adults, but often more subtle:
- Red, swollen gums
- Bleeding during brushing
- Bad breath
Treatment and Prevention in Children:
- Parental Guidance: Parents play a crucial role in establishing good oral hygiene habits. Supervise brushing until around age 7-8 and assist with flossing.
- Education: Teach children the importance of brushing for two minutes, twice a day, and flossing once a day. Make it fun!
- Regular Dental Check-ups: Children should see a dentist every six months for cleanings and examinations.
- Address Orthodontic Challenges: If your child has braces, ensure they receive specific instructions and tools (e.g., floss threaders, interdental brushes) for effective cleaning.
- Balanced Diet: Limit sugary snacks and drinks.
Pro Tip for Parents: If your child's gums bleed, don't assume it's normal. It's a sign of inflammation and warrants a visit to the pediatric dentist. Early intervention prevents progression.
Cost Breakdown: Navigating Treatment Expenses
The comprehensive nature of periodontal treatment means costs can range significantly. Beyond the per-procedure estimates, it's important to consider the overall financial picture.
Average US Costs (Low, Mid, High Estimates):
- Mild Gingivitis Treatment:
- Low: $75 (Routine cleaning, good insurance coverage)
- Mid: $150 (Routine cleaning, some out-of-pocket)
- High: $200 (Routine cleaning, minimal insurance)
- Moderate Periodontitis Treatment (Full Mouth SRP):
- Low: $400 (Excellent insurance, 80% coverage on $2000 treatment)
- Mid: $1,200 (Standard insurance, 50% coverage on $2400 treatment)
- High: $2,400 (No insurance for $2400 treatment)
- Severe Periodontitis Treatment (SRP + 2 Quadrants Flap Surgery + 2 Grafts):
- Low: $2,000 (Very good insurance, high annual max, covering 50% of $4000)
- Mid: $6,000 (Average insurance, high out-of-pocket for $12,000 treatment)
- High: $12,000+ (No insurance for extensive surgical procedures)
With vs. Without Insurance:
- With Insurance: Generally reduces out-of-pocket costs by 50-100% for preventive care and 20-50% for basic and major procedures, up to an annual maximum. It's crucial to understand your plan's annual maximum and how much you've already utilized.
- Without Insurance: You will be responsible for the full sticker price of all treatments. Many dental offices offer discounts for cash payments or payment plans for uninsured patients.
Payment Plans and Financing Options:
- In-Office Payment Plans: Many dental practices offer interest-free payment plans for larger treatment costs, allowing you to pay in installments over a few months.
- Third-Party Financing (e.g., CareCredit, LendingClub): These companies specialize in healthcare financing, offering short-term, interest-free plans or longer-term plans with competitive interest rates.
- Dental Schools: University dental schools often provide treatment at a reduced cost because procedures are performed by students under the close supervision of experienced faculty. This can be a significant cost-saving option for complex treatments.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use these pre-tax dollars to pay for dental treatments, effectively saving you money.
Cost-Saving Tips:
- Prioritize Prevention: The best way to save money is to prevent gum disease in the first place through diligent home care and regular check-ups.
- Seek Early Treatment: Addressing gingivitis is far less expensive than treating advanced periodontitis.
- Compare Costs: Don't hesitate to get a second opinion and compare treatment plans and costs from different periodontists, especially for major surgical procedures.
- Negotiate: Some dental offices may be willing to offer a discount for upfront cash payments if you don't have insurance.
- Dental Discount Plans: These are not insurance but offer a percentage discount on services from participating dentists for an annual membership fee.
Frequently Asked Questions
### Q1: Is inflammation of gums always a sign of serious disease?
A1: Not always. Mild inflammation, known as gingivitis, is common and often reversible. It becomes serious if left untreated, as it can progress to periodontitis, which involves irreversible damage to the bone and tissues supporting your teeth. Regular dental check-ups are key to distinguishing between mild and severe cases.
### Q2: How long does it take for inflamed gums to heal?
A2: For gingivitis, significant improvement can be seen within 1-2 weeks of professional cleaning and diligent home care. For periodontitis, healing after deep cleaning (scaling and root planing) takes several weeks for gum tissue to reattach, with full tissue maturation taking months. Surgical recovery also varies from weeks to months.
### Q3: Can home remedies cure gum inflammation?
A3: While some home remedies like saltwater rinses can help reduce symptoms and promote healing, they cannot cure gum inflammation or remove plaque and tartar. Professional dental cleaning is essential to remove hardened deposits and address the root cause of the inflammation. Home remedies should only be used as an adjunct to professional treatment.
### Q4: Is treatment for inflamed gums painful?
A4: Most non-surgical treatments like scaling and root planing are performed under local anesthesia, so you won't feel pain during the procedure. You may experience some mild soreness or sensitivity for a few days afterward, which can typically be managed with over-the-counter pain relievers. Surgical procedures involve more discomfort, but pain management protocols are in place.
### Q5: What is the typical cost of treating severe gum inflammation without insurance?
A5: Treating severe periodontitis without insurance can be very expensive, potentially ranging from several thousand dollars to over $10,000 or more, depending on the number of teeth involved and the extent of surgical procedures required (e.g., flap surgery, bone grafts). This emphasizes the importance of early detection and prevention.
### Q6: Can inflamed gums affect my overall health?
A6: Absolutely. Chronic inflammation of the gums is directly linked to systemic health issues, including an increased risk of heart disease, stroke, diabetes complications, and respiratory problems. It can also exacerbate conditions like osteoporosis and teeth stability by accelerating jawbone loss, highlighting the critical oral-systemic connection.
### Q7: Are electric toothbrushes better for inflamed gums?
A7: Many dental professionals recommend electric toothbrushes, especially those with oscillating-rotating or sonic technology, for their superior plaque removal capabilities. Their built-in timers and pressure sensors can also help ensure you brush effectively without damaging inflamed gum tissue.
### Q8: What if my gums continue to bleed after brushing and flossing?
A8: Persistent bleeding gums, despite diligent daily oral hygiene, are a strong indicator of unresolved inflammation or underlying gum disease. You should schedule an appointment with your dentist or a periodontist promptly. This is a crucial sign that professional intervention is needed.
### Q9: Can gum inflammation lead to loose teeth?
A9: Yes, if left untreated, gum inflammation can advance to periodontitis, where the bacterial infection destroys the ligaments and bone that support your teeth. As this support structure weakens, teeth can become loose, shift, and eventually may even fall out or require extraction.
### Q10: How does osteoporosis relate to gum inflammation and teeth?
A10: While osteoporosis doesn't cause gum inflammation directly, it significantly impacts the outcome if you have periodontitis. The reduced bone density throughout the body, including the jawbone, means that when gum disease sets in, the bone supporting your teeth is more vulnerable to destruction. This accelerates bone loss, increases the risk of tooth loss, and highlights why managing both conditions, especially concerning osteoporosis teeth, is crucial for maintaining dental stability.
When to See a Dentist
Recognizing the signs that warrant a dental visit is crucial for preventing the progression of gum inflammation and protecting your overall health.
Schedule a routine check-up if you notice:
- Gums that are red, swollen, or tender.
- Occasional bleeding when brushing or flossing.
- Persistent bad breath.
- Mild gum recession.
Schedule an urgent appointment if you experience any of these red flags:
- Frequent or heavy gum bleeding when brushing, flossing, or spontaneously.
- Severe pain or tenderness in your gums or when chewing.
- Visible pus coming from between your teeth and gums.
- Noticeably loose or shifting teeth.
- Significant gum recession where teeth appear much longer.
- Any changes in how your teeth fit together when you bite.
- Swelling in your face or jaw accompanied by gum pain, which could indicate an abscess.
If you have a chronic systemic condition such as diabetes or osteoporosis, and you notice any signs of gum inflammation, it is especially important to consult your dentist promptly. These conditions can accelerate the progression of gum disease, and early intervention is vital. Don't wait for pain to be your guide; many forms of gum disease progress silently until significant damage has occurred. Regular dental care is your most powerful tool for maintaining healthy gums and a healthy body.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Does Oil Pulling Help Gut Health
The intricate connection between our oral health and overall well-being is a topic of growing fascination and scientific inquiry. Often, when we think of health, we focus on specific organs or systems, overlooking the crucial role of the mouth as a gateway to the rest of the body. One ancient practi
February 23, 2026
Does Oil Pulling Help With Inflammation
It's a question many health-conscious individuals ask as they explore natural remedies: does oil pulling help with inflammation? In an era where holistic approaches to wellness are gaining traction, the ancient practice of oil pulling has resurfaced, promising benefits that extend beyond oral hy
February 23, 2026
Oil Pulling for Kidney Disease: Complete Guide
Chronic kidney disease (CKD) affects an estimated 37 million adults in the United States, often progressing silently until advanced stages. What many may not realize is the profound connection between the health of their mouth and the health of their kidneys. As a bridge between traditional wisd
February 23, 2026
Oil Pulling Oral Microbiome: Complete Guide
Have you ever considered the bustling universe thriving within your mouth? This intricate community, known as the oral microbiome, consists of billions of microorganisms – some beneficial, some harmful – all playing a critical role in your oral and overall systemic health. Maintaining a balanced
February 23, 2026