Gum Infection: Complete Guide
Key Takeaways
- An estimated 47.2% of American adults aged 30 and older have some form of periodontal disease, the more advanced stage of gum infection. This staggering statistic, provided by the Centers for Disease Control and Prevention (CDC), highlights just how pervasive this condition is. A gum infection i
An estimated 47.2% of American adults aged 30 and older have some form of periodontal disease, the more advanced stage of gum infection. This staggering statistic, provided by the Centers for Disease Control and Prevention (CDC), highlights just how pervasive this condition is. A gum infection isn't merely an inconvenience; it's a serious health concern that can range from mild inflammation (gingivitis) to severe tissue and bone destruction (periodontitis), ultimately leading to tooth loss and impacting your overall systemic health. Understanding the causes, recognizing the gingivitis symptoms, and knowing your treatment options are crucial steps toward protecting your smile and your well-being. This comprehensive guide from SmilePedia.net will equip you with everything you need to know about gum infections, from prevention to advanced treatments, ensuring you have the knowledge to maintain optimal oral health. We'll delve into the different types of gum disease, the tell-tale signs like swollen gums, the latest treatment approaches, costs, and essential prevention strategies.
Key Takeaways:
- Gum infection (periodontal disease) affects nearly half of US adults over 30, with severity ranging from mild gingivitis to advanced periodontitis.
- Gingivitis, the mildest form, is reversible with professional cleaning and improved oral hygiene, often costing $75-$200 for a routine cleaning.
- Periodontitis involves irreversible bone and tissue damage; early intervention with non-surgical treatments like scaling and root planing (deep cleaning) is critical, typically costing $200-$600 per quadrant without insurance.
- Signs like swollen gums, bleeding when brushing, persistent bad breath, and receding gums are key indicators that warrant immediate dental attention.
- Advanced periodontitis may require surgical interventions (flap surgery, grafts), with costs ranging from $500-$1,500 per tooth or quadrant for individual procedures.
- Prevention is paramount: daily brushing, flossing, regular dental check-ups (every 6 months), and avoiding tobacco products significantly reduce your risk.
- Untreated gum infections can lead to tooth loss and are linked to systemic health issues like heart disease, diabetes, and stroke.
What Is a Gum Infection? An Overview
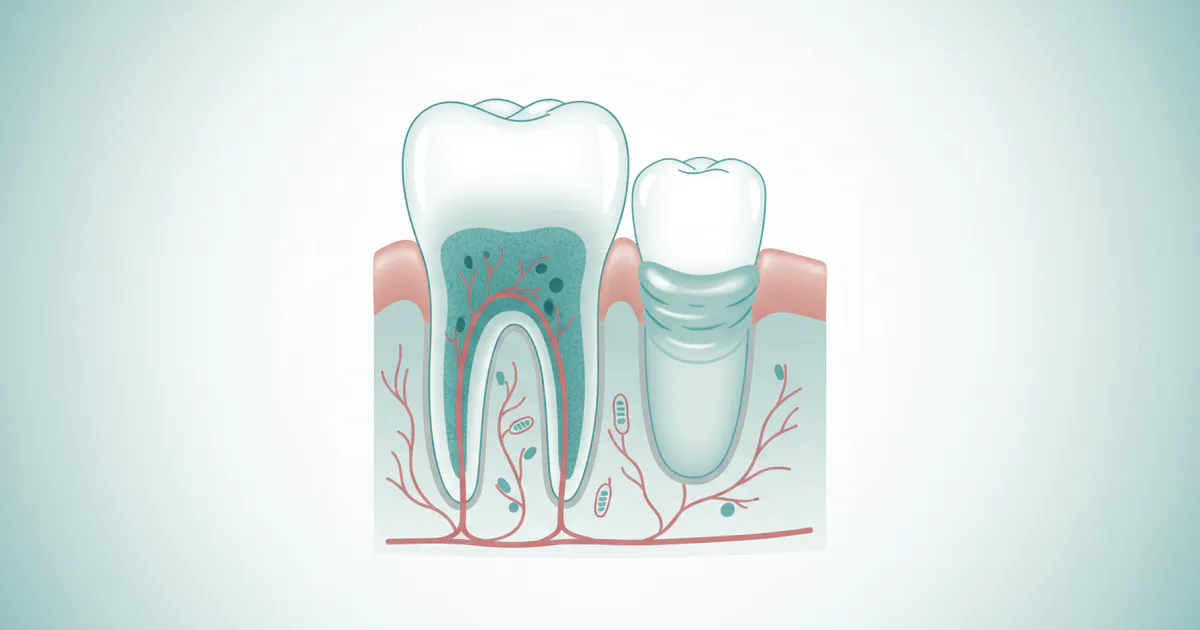
A gum infection, medically known as periodontal disease, is an inflammatory condition affecting the tissues surrounding and supporting your teeth. It begins when bacteria in plaque, a sticky film that constantly forms on your teeth, produce toxins that irritate the gum tissue. If not removed through daily brushing and flossing, plaque hardens into tartar (calculus), which can only be removed by a dental professional.

The body's immune response to these bacteria and their toxins leads to inflammation, causing the gums to become red, swollen, and prone to bleeding. This initial stage is called gingivitis. Gingivitis is reversible; with proper treatment and improved oral hygiene, the gums can return to health.
However, if gingivitis is left untreated, the inflammation can progress, leading to a more severe condition known as periodontitis. In periodontitis, the infection spreads below the gum line, causing the gums to pull away from the teeth, forming pockets. These pockets collect more plaque and bacteria, further deepening the infection. Over time, the chronic inflammation and bacterial toxins begin to destroy the connective tissue and bone that hold your teeth in place. Unlike gingivitis, the damage caused by periodontitis, particularly the bone loss, is often irreversible. The goal of treatment at this stage is to stop the progression of the disease and prevent further damage.
Understanding this progression is key to recognizing the importance of early detection and intervention. A healthy mouth has firm, pink gums that don't bleed when brushed or flossed. Any deviation from this should be a signal to consult your dentist.
Types of Gum Infections
Gum infections manifest in various forms, primarily categorized by their severity and specific characteristics. The two main types are gingivitis and periodontitis, with periodontitis having several sub-classifications.
Gingivitis
Gingivitis is the mildest form of gum disease and is solely an inflammation of the gum tissue (gingiva). It does not involve the loss of bone or attachment of the tooth to the surrounding structures.
- Key Characteristics:
- Red, swollen gums.
- Gums that bleed easily during brushing or flossing.
- Tenderness or mild discomfort.
- Often painless, which can lead to delayed treatment.
- Reversible with professional cleaning and consistent home care.
Periodontitis
Periodontitis is a more serious, chronic infection that, if left untreated, can lead to irreversible damage to the bone and tissues supporting your teeth. It is the leading cause of tooth loss in adults.
1. Chronic Periodontitis
This is the most common form of periodontitis and typically affects adults, though it can occur at any age. It progresses slowly over time.
- Key Characteristics:
- Inflammation below the gum line.
- Formation of periodontal pockets.
- Gradual loss of attachment (receding gums) and supporting bone.
- Often characterized by periods of slow progression followed by rapid destruction.
- Symptoms can include persistent bad breath, swollen gums, pain, and eventually loose teeth.
2. Aggressive Periodontitis
This form of periodontitis is less common but characterized by rapid attachment loss and bone destruction. It can occur in otherwise clinically healthy individuals, often with a genetic predisposition.
- Key Characteristics:
- Rapid progression of bone and attachment loss.
- Can affect localized areas (e.g., front teeth and molars) or generalized throughout the mouth.
- Often occurs in younger individuals (under 30), though it can affect older patients.
- Family history is often a factor.
3. Necrotizing Periodontal Diseases
These are severe forms of periodontitis characterized by tissue necrosis (tissue death). They are typically associated with systemic conditions, such as immunosuppression (e.g., HIV/AIDS, malnutrition, severe stress, smoking).
- Necrotizing Ulcerative Gingivitis (NUG): Characterized by painful, bleeding gums, ulcerated and "punched out" gum tissue between teeth, and severe bad breath.
- Necrotizing Ulcerative Periodontitis (NUP): A more severe progression of NUG, involving loss of bone and attachment, leading to rapid destruction of periodontal tissues.
- Necrotizing Stomatitis: The most severe form, involving extensive tissue necrosis beyond the gingiva and periodontal ligaments, extending into other oral tissues.
4. Periodontitis as a Manifestation of Systemic Diseases
In some cases, periodontitis can be a secondary symptom of an underlying systemic condition that affects the body's inflammatory response or immune system. Examples include diabetes-associated periodontitis, blood disorders, and genetic conditions like Down syndrome.
Understanding these distinctions helps dental professionals tailor the most effective treatment plan for your specific condition.
Causes: Why Gum Infections Happen
The primary cause of gum infection is the accumulation of bacterial plaque on your teeth, particularly along the gum line. However, a combination of factors contributes to its development and progression.
1. Plaque and Tartar Accumulation
- Bacterial Plaque: This sticky, colorless film is constantly forming on your teeth. It consists of bacteria, food particles, and saliva. If not removed daily through brushing and flossing, these bacteria produce toxins that irritate the gum tissue, leading to inflammation and infection.
- Tartar (Calculus): If plaque is not removed, it hardens into tartar, a calcified substance that adheres firmly to the tooth surface. Tartar provides a rough, porous surface that acts as a haven for more plaque accumulation, making it even more difficult to clean. Tartar can only be removed by a professional dental cleaning.
2. Poor Oral Hygiene
Inadequate brushing and flossing allow plaque to build up and mature, creating an environment ripe for gum infection. Brushing at least twice a day and flossing daily are essential for disrupting this bacterial film.
3. Smoking and Tobacco Use
Smoking is one of the most significant risk factors for developing severe gum disease.
- It impairs the immune system's ability to fight off gum infections.
- It reduces blood flow to the gums, masking common gingivitis symptoms like bleeding, which can delay diagnosis.
- It hinders the healing process after treatment.
4. Hormonal Changes
Fluctuations in hormones can make gums more sensitive and prone to inflammation.
- Pregnancy: "Pregnancy gingivitis" is common due to increased hormone levels that can exaggerate the gum's response to plaque.
- Puberty, Menstruation, Menopause: These periods can also lead to increased gum sensitivity and inflammation.
5. Certain Medications
Some medications can affect oral health, indirectly contributing to gum infection.
- Dry Mouth (Xerostomia): Many medications (e.g., antidepressants, antihistamines, decongestants) cause dry mouth, reducing saliva's protective cleansing effect and allowing plaque to accumulate more easily.
- Anticonvulsants (e.g., phenytoin), Immunosuppressants (e.g., cyclosporine), and Calcium Channel Blockers (e.g., nifedipine): These can cause gingival overgrowth (enlarged gums), making proper cleaning difficult and creating areas for bacteria to thrive.
6. Systemic Diseases
Underlying health conditions can compromise the body's immune system or inflammatory response, increasing susceptibility to gum infections.
- Diabetes: People with diabetes are at higher risk for gum disease, and severe gum disease can also make blood sugar control more difficult. It's a two-way street.
- Heart Disease: Research suggests a link between gum disease and cardiovascular issues, although the exact nature of the relationship is still being studied.
- Autoimmune Diseases (e.g., Crohn's disease, Lupus): These can affect the body's inflammatory response.
- Immunocompromised Conditions (e.g., HIV/AIDS, cancer treatment): Weaken the immune system, making individuals more vulnerable to severe infections.
7. Genetics
Some individuals are genetically predisposed to developing gum disease, making them more susceptible even with good oral hygiene practices. If a parent or sibling has gum disease, you may be at higher risk.

8. Poor Nutrition
A diet lacking essential nutrients, particularly Vitamin C, can weaken the immune system and make it harder for gum tissue to repair itself.
9. Crooked Teeth or Ill-Fitting Restorations
Teeth that are crowded or misaligned can create hard-to-clean areas where plaque and tartar accumulate. Old, poorly fitted fillings, crowns, or bridges can also trap plaque and irritate gum tissue.
10. Stress
Chronic stress can compromise the immune system, making it more challenging for the body to fight off infections, including those in the gums.
Signs and Symptoms: What to Look For
Recognizing the signs of a gum infection early is crucial for effective treatment and preventing irreversible damage. Symptoms can vary depending on the stage and severity of the disease.
Early Signs (Gingivitis Symptoms)
These are often subtle and may be overlooked, but they indicate the initial stage of inflammation.
- Red or Dark Gums: Healthy gums are typically pink. A change to a darker red or purplish hue is a common sign of inflammation.
- Swollen Gums (Edema): Your gums may appear puffy or enlarged, particularly around the base of the teeth. This is a primary indicator of irritation.
- Bleeding Gums: One of the most common and earliest gingivitis symptoms is bleeding when you brush, floss, or even eat hard foods. Healthy gums should not bleed.
- Tender Gums: Gums may feel sore or tender to the touch.
- Bad Breath (Halitosis): Persistent bad breath, even after brushing, can be a sign of bacterial accumulation and infection.
Advanced Signs (Periodontitis Symptoms)
If gingivitis progresses to periodontitis, more severe and noticeable symptoms will develop as the infection begins to destroy supporting structures.
- Persistent Bad Breath: Worsened chronic bad breath due to deeper bacterial pockets.
- Receding Gums: Gums pull away or "recede" from the teeth, making your teeth appear longer. This exposes the tooth roots, which can lead to sensitivity.
- Pus Between Teeth and Gums: A sign of active infection. You might notice pus when you press on your gums.
- Changes in Tooth Alignment: Teeth may shift, become loose, or new spaces may appear between them as the supporting bone is lost.
- Loose or Wobbly Teeth: As the bone and ligaments supporting the teeth are destroyed, teeth can become mobile, making chewing difficult. This is a very serious sign.
- Changes in Bite: Your teeth may not fit together properly when you bite down.
- Sores or Abscesses: Painful sores or localized pus-filled swellings can develop on the gums.
- Severe Pain: While gum disease can often be painless in its early stages, advanced periodontitis can cause significant pain, especially when chewing.
Pro Tip: Don't ignore bleeding gums, even if it's just a little pink in the sink. Many people mistakenly think bleeding gums are normal when brushing hard, but it's almost always a sign of inflammation or infection that requires attention.
Treatment Options
Treating a gum infection depends on its severity, ranging from non-surgical approaches for gingivitis and mild-to-moderate periodontitis to surgical interventions for advanced cases. The primary goals are to remove the bacteria, stop the progression of the disease, and restore gum health.
Non-Surgical Treatments
These are typically the first line of defense for gingivitis and early to moderate periodontitis.
1. Professional Dental Cleaning (Prophylaxis)
- What it is: A routine cleaning where a dental hygienist or dentist removes plaque and tartar from above and slightly below the gum line using specialized instruments.
- Purpose: Primarily for preventing gum disease or treating mild gingivitis.
- Pros: Non-invasive, quick, effective for early stages.
- Cons: Not sufficient for established periodontitis with deep pockets.
- Cost: Typically $75 - $200 without insurance, often covered by most dental plans.
2. Scaling and Root Planing (SRP) - "Deep Cleaning"
- What it is: A non-surgical procedure for treating periodontitis. Scaling involves removing plaque and tartar from above and below the gum line. Root planing smooths the root surfaces of the teeth to remove bacterial toxins and make it harder for plaque to reattach.
- Purpose: To clean deep periodontal pockets and eliminate bacterial reservoirs.
- Process: Usually done under local anesthesia and may require multiple appointments (e.g., one quadrant per appointment).
- Pros: Highly effective for stopping disease progression in mild-to-moderate periodontitis, less invasive than surgery.
- Cons: Can cause temporary sensitivity, discomfort, and gum recession; not a cure for advanced periodontitis.
- Cost: Typically $200 - $600 per quadrant (e.g., upper right, lower left) without insurance, or $800 - $2,400 for a full mouth deep cleaning. Insurance coverage varies but often covers a significant portion.
3. Antibiotics (Oral or Topical)
- What it is: Used in conjunction with scaling and root planing to target specific bacteria.
- Oral Antibiotics: Systemic antibiotics (e.g., amoxicillin, doxycycline, metronidazole) may be prescribed for a short course to reduce aggressive or persistent infections.
- Topical Antibiotics: Antibiotic gels, chips, or microspheres containing medications like minocycline or doxycycline can be placed directly into deep periodontal pockets after SRP. These release medication slowly over time.
- Purpose: To kill bacteria that cause periodontitis and promote healing.
- Pros: Can enhance the effectiveness of mechanical cleaning.
- Cons: Oral antibiotics can have systemic side effects (e.g., digestive upset), potential for antibiotic resistance; topical treatments are only for specific cases.
- Cost: Oral antibiotics typically $10-$50 (generic), topical applications $75-$200 per pocket.
Surgical Treatments
When non-surgical treatments are insufficient to manage deep pockets or significant bone loss, surgical interventions may be necessary.
1. Flap Surgery (Pocket Reduction Surgery)
- What it is: The periodontist makes small incisions in the gum tissue to lift back a section of the gums (a "flap"). This allows for thorough cleaning of the root surfaces and removal of diseased tissue and tartar from deep pockets. The bone may also be reshaped if necessary. The gums are then sutured back into place, often resulting in shallower pockets.
- Purpose: To reduce pocket depth and make it easier to clean teeth and gums.
- Pros: Highly effective for reducing deep pockets, allows direct visualization and thorough cleaning.
- Cons: Invasive, post-operative discomfort, temporary sensitivity, gum recession is common.
- Cost: Typically $500 - $1,500 per quadrant without insurance.
2. Bone Grafting
- What it is: If periodontitis has caused significant bone loss, bone grafting may be performed to regenerate lost bone. Fragments of your own bone, synthetic bone, or donated bone are used to replace the destroyed bone and promote natural bone growth.
- Purpose: To restore lost bone support around teeth.
- Pros: Can save teeth that would otherwise be lost, provides a stable foundation for teeth.
- Cons: Invasive, longer recovery period, variable success rate, potential for complications.
- Cost: Typically $600 - $2,500 per site without insurance, depending on the material and extent.
3. Soft Tissue Grafts (Gum Grafts)
- What it is: Used to treat receding gums, where the gum tissue has pulled away from the tooth, exposing the root. Tissue is usually taken from the roof of your mouth (palate) or a donor source and attached to the affected area.
- Purpose: To cover exposed tooth roots, reduce sensitivity, and protect against further recession and bone loss.
- Pros: Reduces sensitivity, improves aesthetics, protects roots.
- Cons: Invasive, potential discomfort at donor site, specific aftercare requirements.
- Cost: Typically $400 - $1,200 per tooth without insurance, depending on the size and type of graft.
4. Guided Tissue Regeneration (GTR)
- What it is: A surgical procedure that uses a small piece of mesh-like material (membrane) to be placed between the bone and gum tissue. This membrane prevents gum tissue from growing into the area where bone and ligament should regenerate, allowing slower-growing bone and connective tissue cells to colonize the area and regenerate.
- Purpose: To stimulate the growth of new bone and connective tissue.
- Pros: Can regenerate lost periodontal structures, improves long-term prognosis for affected teeth.
- Cons: More complex and expensive surgery, longer healing time, variable success rates.
- Cost: Often integrated with flap surgery or bone grafting, adding $500 - $1,500 to the cost.
5. Dental Implants
- What it is: While not a direct treatment for gum infection, if a tooth is lost due to severe periodontitis, a dental implant can be a replacement option. It involves surgically placing a titanium post into the jawbone to serve as an artificial tooth root, onto which a crown is later attached.
- Purpose: To replace missing teeth in cases of irreversible tooth loss due to gum disease.
- Pros: Highly durable, natural-looking, preserves bone, improves chewing function.
- Cons: Expensive, requires sufficient bone density, surgical procedure, long healing time.
- Cost: $3,000 - $6,000 per implant (including post, abutment, and crown) without insurance.
Step-by-Step Treatment Process: What to Expect
Let's walk through what you can generally expect for a common non-surgical treatment like Scaling and Root Planing (SRP) for moderate periodontitis.
Initial Consultation and Diagnosis
- Comprehensive Exam: Your dentist or periodontist will conduct a thorough examination of your teeth and gums. This includes:
- Probing: Measuring the depth of the pockets around your teeth using a small ruler (periodontal probe). Pockets deeper than 3mm often indicate gum disease.
- X-rays: To assess bone loss around your teeth.
- Visual Inspection: Looking for swollen gums, redness, bleeding, and signs of recession.
- Medical History Review: To identify any systemic risk factors.
- Diagnosis and Treatment Plan: Based on the findings, your dentist will diagnose the stage of your gum infection (gingivitis, mild, moderate, or severe periodontitis) and recommend a personalized treatment plan. This plan will outline the specific procedures, expected outcomes, and estimated costs.

Scaling and Root Planing (Deep Cleaning)
If SRP is recommended, here's the typical process:
- Anesthesia: To ensure comfort, your dentist or hygienist will administer local anesthesia to numb the specific area(s) being treated. This might be a quadrant of your mouth (e.g., upper left).
- Scaling: Using specialized instruments, such as ultrasonic scalers (which use vibrations and water spray) and hand scalers, the hygienist will meticulously remove plaque and tartar from the tooth surfaces, both above and below the gum line, and inside the periodontal pockets. You might feel some pressure and hear scraping noises.
- Root Planing: After scaling, the root surfaces are carefully smoothed. This process removes bacterial toxins and makes it more difficult for plaque to adhere in the future, promoting gum reattachment to the cleaned root surfaces.
- Irrigation (Optional): Some practitioners may use an antimicrobial rinse during or after the procedure to further reduce bacteria.
- Antibiotic Placement (Optional): In some cases, a localized antibiotic gel or chip may be placed directly into deeper pockets to continue fighting bacteria and aid healing.
- Multiple Appointments: SRP is often performed over 2 to 4 appointments, treating one or two quadrants of the mouth at a time, allowing for proper numbing and thorough cleaning.
- Post-Treatment Instructions: You will receive detailed instructions on aftercare, including pain management, oral hygiene, and dietary recommendations.
Follow-Up and Maintenance
- Re-evaluation: About 4-6 weeks after completing SRP, you'll have a follow-up appointment. The dentist will re-measure pocket depths to assess how well the gums have healed and if pocket depths have reduced.
- Supportive Periodontal Therapy (SPT): For individuals treated for periodontitis, regular maintenance cleanings (often every 3-4 months, instead of the typical 6 months) are crucial. These appointments, sometimes called "perio maintenance," help monitor gum health, remove new plaque and tartar buildup, and prevent the infection from recurring.
This multi-step approach ensures that the infection is thoroughly addressed and that your oral health is maintained long-term.
Cost and Insurance
Understanding the financial aspect of gum infection treatment is vital. Costs can vary significantly based on the type and severity of the infection, the specific procedures required, geographical location, and whether you have dental insurance.
Average US Costs Without Insurance (Ranges)
- Routine Dental Cleaning (Prophylaxis): For gingivitis prevention or mild gingivitis.
- $75 - $200
- Scaling and Root Planing (SRP): For mild to moderate periodontitis.
- $200 - $600 per quadrant
- $800 - $2,400 for a full mouth deep cleaning
- Topical Antibiotic Placement (e.g., Arestin):
- $75 - $200 per pocket
- Flap Surgery (Pocket Reduction Surgery): For moderate to severe periodontitis.
- $500 - $1,500 per quadrant
- Bone Grafting: For bone loss from periodontitis.
- $600 - $2,500 per site
- Soft Tissue Graft (Gum Graft): For receding gums.
- $400 - $1,200 per tooth
- Guided Tissue Regeneration (GTR):
- $500 - $1,500 (often in addition to flap surgery)
- Perio Maintenance (after SRP): More extensive than a routine cleaning.
- $120 - $250 per visit (typically every 3-4 months)
Pro Tip: Costs can be higher in major metropolitan areas (e.g., New York, Los Angeles) and lower in rural areas. Always ask for a detailed estimate from your dental office before starting treatment.
Dental Insurance Coverage
Most dental insurance plans in the US categorize treatments into different tiers, affecting coverage percentages:
- Preventive Care (Type A): Routine cleanings, exams, X-rays. Typically covered at 80-100%. This often includes prophylaxis for gingivitis.
- Basic Procedures (Type B): Fillings, simple extractions, sometimes scaling and root planing. Usually covered at 50-80%. Many plans cover SRP but might have limitations (e.g., once every 2-3 years, or only for specific pocket depths).
- Major Procedures (Type C): Crowns, bridges, dentures, and often periodontal surgeries (flap surgery, bone grafts, gum grafts). Typically covered at 30-50%.
- Orthodontics (Type D): Separate category, usually with its own lifetime maximum.
Key Insurance Considerations:
- Deductible: An amount you must pay out-of-pocket before your insurance begins to cover costs (e.g., $50-$150 annually).
- Co-insurance/Co-pay: Your share of the cost after your deductible is met (e.g., if insurance covers 80%, you pay 20%).
- Annual Maximum: The maximum amount your insurance will pay in a benefit year (e.g., $1,000-$2,500). If your treatment costs exceed this, you are responsible for the remainder.
- Waiting Periods: Some plans have waiting periods (e.g., 6-12 months) before they will cover major procedures like periodontal surgery.
ADA Codes: Dental procedures are standardized by Current Dental Terminology (CDT) codes from the ADA. For example:
- D1110: Prophylaxis (Adult)
- D4341: Periodontal Scaling and Root Planing – Four or More Teeth Per Quadrant
- D4342: Periodontal Scaling and Root Planing – One to Three Teeth Per Quadrant
- D4240: Gingival Flap Procedure, Including Root Planing – Four or More Teeth Per Quadrant
When discussing costs, ask your dental office for the CDT codes they plan to use so you can verify coverage with your insurance provider.
Payment Plans and Financing Options
If you don't have insurance or face high out-of-pocket costs, many dental offices offer:
- In-house Payment Plans: Monthly installment plans directly with the office.
- Third-Party Financing: Companies like CareCredit or LendingClub offer specialized health care credit cards or loans with deferred interest or low-interest rates.
- Dental Savings Plans: Not insurance, but a membership that provides discounts on dental services from participating providers.
Recovery and Aftercare
Proper recovery and diligent aftercare are essential for successful gum infection treatment, especially after non-surgical procedures like scaling and root planing, or any surgical intervention.
After Scaling and Root Planing (SRP)
- Discomfort and Sensitivity:
- Expect some gum soreness, tenderness, and sensitivity to hot/cold for a few days to a week.
- Over-the-counter pain relievers (ibuprofen, acetaminophen) can manage discomfort.
- Sensitivity toothpaste can help reduce tooth sensitivity.
- Bleeding: Slight bleeding for the first 24 hours is normal.
- Swelling: Mild swelling might occur. Cold compresses can help.
- Diet: Stick to soft foods for a few days (e.g., soup, yogurt, mashed potatoes). Avoid crunchy, sticky, or very hot/cold foods.
- Oral Hygiene:
- Continue gentle brushing and flossing, but avoid aggressively brushing the treated areas for the first day. Your dental hygienist will provide specific instructions.
- Rinse with a warm salt water solution (1/2 teaspoon salt in 8 ounces warm water) several times a day to aid healing and reduce swelling. Your dentist might prescribe a medicated mouthwash (e.g., chlorhexidine) for a short period.
- Avoid: Smoking, alcohol, and vigorous rinsing for at least 24-48 hours.
After Periodontal Surgery (Flap Surgery, Grafts, Bone Regeneration)
Surgical recovery is more involved and requires strict adherence to post-operative instructions.
- Pain Management: Your periodontist will likely prescribe stronger pain medication. Take as directed.
- Swelling and Bruising: Expect more significant swelling and potentially some bruising. Apply ice packs intermittently for the first 24-48 hours.
- Bleeding: Some oozing or light bleeding is normal for the first day. Bite gently on a piece of gauze if needed.
- Diet: A soft diet is crucial for a longer period (often 1-2 weeks or more) to avoid disturbing the surgical site.
- Oral Hygiene:
- Do NOT brush or floss the surgical site directly until instructed by your periodontist.
- Use a prescribed antimicrobial mouthwash (e.g., chlorhexidine) to keep the area clean.
- Gently brush and floss other areas of your mouth.
- Avoid vigorous rinsing, spitting, or using a straw, as this can dislodge blood clots.
- Sutures: You may have dissolvable sutures or need to return for suture removal, typically within 7-10 days.
- Stent/Dressing: If a periodontal dressing or stent was placed, follow instructions for its care and removal.
- Activity: Avoid strenuous physical activity for several days to a week, as it can increase bleeding and swelling.
- Follow-Up: Attend all scheduled post-operative appointments for suture removal, evaluation, and further instructions.
Pro Tip: The success of any gum treatment heavily relies on your commitment to meticulous home care and attending all follow-up appointments. This is your long-term maintenance phase.
Prevention of Gum Infections
Preventing gum infection is far easier and less costly than treating it. A consistent routine and healthy habits can dramatically reduce your risk.
-
Brush Your Teeth Twice Daily:
- Use a soft-bristled toothbrush and fluoride toothpaste.
- Brush for at least two minutes, covering all surfaces of your teeth.
- Use proper technique: angle the brush at 45 degrees to the gum line, gently brushing in small circular motions. Don't scrub aggressively.
- Consider an electric toothbrush, which can be more effective at removing plaque.
-
Floss Daily:
- Flossing removes plaque and food particles from between your teeth and under the gum line where your toothbrush can't reach.
- Use about 18 inches of floss, wrapping it around your middle fingers. Guide it gently between teeth, curving it around each tooth in a "C" shape, and sliding it carefully below the gum line.
- If traditional floss is difficult, try interdental brushes, water flossers (oral irrigators), or floss picks.
-
Use an Antimicrobial Mouthwash:
- Over-the-counter therapeutic mouthwashes containing ingredients like cetylpyridinium chloride (CPC) or essential oils can help reduce plaque and gingivitis.
- Pro Tip: Consult your dentist before incorporating a new mouthwash, especially if you have sensitive gums or specific concerns.
-
Regular Dental Check-ups and Professional Cleanings:
- Visit your dentist at least every six months for a comprehensive examination and professional cleaning.
- These appointments allow your dental team to identify early signs of gum infection, remove hardened plaque (tartar) that you can't remove at home, and provide personalized advice.
- For individuals with a history of periodontitis, your dentist may recommend more frequent "perio maintenance" visits (e.g., every 3-4 months).
-
Maintain a Balanced Diet:
- Eat a nutritious diet rich in fruits, vegetables, and whole grains.
- Limit sugary snacks and drinks, which can contribute to plaque formation.
- Ensure adequate intake of vitamins, especially Vitamin C, which is crucial for gum health.
-
Avoid Tobacco Products:
- Smoking and chewing tobacco are major risk factors for gum disease. Quitting is one of the most significant steps you can take to protect your gums and overall health.
-
Manage Systemic Conditions:
- If you have conditions like diabetes, ensure it is well-controlled, as this directly impacts your susceptibility to and severity of gum disease.
- Inform your dentist about all medical conditions and medications you are taking.
-
Address Misaligned Teeth or Poor Restorations:
- Crooked teeth can create plaque traps. Orthodontic treatment may be recommended.
- Ensure old fillings, crowns, or bridges are in good condition and not contributing to plaque retention or gum irritation.
Adopting these preventive measures is your best defense against developing a debilitating gum infection and maintaining a healthy, confident smile for life. The ADA (American Dental Association) consistently emphasizes the importance of these practices for optimal oral health.
Risks and Complications
If left untreated, a gum infection, particularly periodontitis, can lead to a cascade of oral and systemic health problems, some of which are severe and life-threatening.
Oral Complications
- Tooth Loss: This is the most common and devastating complication of advanced periodontitis. As the bone and connective tissues are destroyed, teeth lose their support, become loose, and eventually fall out or require extraction.
- Receding Gums: Exposes the tooth roots, leading to increased sensitivity to hot and cold, and making the teeth more vulnerable to decay.
- Tooth Mobility and Shifting: Loss of bone support causes teeth to become loose and shift, altering your bite and affecting chewing function and aesthetics.
- Dental Abscesses: Pockets of pus can form in the gums or around the tooth root, causing severe pain, swelling, and potentially spreading infection.
- Persistent Bad Breath: Chronic halitosis due to the ongoing bacterial infection.
- Difficulty Chewing and Speaking: Loose or missing teeth can impair your ability to eat and communicate effectively.

Systemic Health Complications
The link between oral health and overall systemic health is well-established. The chronic inflammation and bacteria from gum infections can enter the bloodstream and impact distant organs.
- Cardiovascular Disease: Research suggests a strong correlation between severe periodontitis and an increased risk of heart disease, stroke, and bacterial endocarditis. The inflammation from gum disease may contribute to atherosclerosis (hardening of the arteries).
- Diabetes: There's a bidirectional relationship. Individuals with diabetes are more susceptible to gum disease, and severe gum disease can make it harder to control blood sugar levels, increasing the risk of diabetic complications.
- Respiratory Diseases: Oral bacteria from gum infections can be aspirated into the lungs, contributing to respiratory conditions like pneumonia, bronchitis, and chronic obstructive pulmonary disease (COPD).
- Pregnancy Complications: Pregnant women with periodontitis have an increased risk of preterm birth, low birth weight babies, and preeclampsia.
- Rheumatoid Arthritis: Some studies indicate a link between periodontitis and an increased risk and severity of rheumatoid arthritis, an inflammatory autoimmune disease.
- Osteoporosis: Bone loss in the jaw associated with periodontitis can be exacerbated in individuals with osteoporosis.
- Kidney Disease: Chronic periodontitis has been linked to an increased risk of chronic kidney disease.
- Dementia/Alzheimer's Disease: Emerging research suggests a potential link between chronic inflammation from gum disease and cognitive decline, including an increased risk of Alzheimer's disease.
Given these serious risks, treating gum infections is not just about saving your teeth; it's about safeguarding your overall health and well-being.
Comparison Tables
To help you understand the differences and treatment approaches more clearly, here are two comparison tables:
Table 1: Gingivitis vs. Periodontitis
| Feature | Gingivitis | Periodontitis |
|---|---|---|
| Severity | Mildest form of gum infection | Advanced, chronic gum infection |
| Tissue Damage | Only affects gum tissue | Affects gums, ligaments, and supporting bone |
| Bone Loss | None | Irreversible bone loss |
| Gum Pockets | No true pockets; slight gum swelling | True periodontal pockets formed (4mm+) |
| Symptoms | Red, swollen gums, bleeding, bad breath | All gingivitis symptoms, plus receding gums, pus, loose teeth, changes in bite, severe bone loss |
| Pain Level | Often painless or mild discomfort | Can be painful, especially in advanced stages |
| Reversibility | Fully reversible with treatment | Irreversible damage; progression can be stopped |
| Treatment Focus | Routine cleaning, improved oral hygiene | Scaling & Root Planing, surgery, ongoing maintenance |
Table 2: Non-Surgical vs. Surgical Periodontal Treatments
| Feature | Non-Surgical Treatments (e.g., SRP) | Surgical Treatments (e.g., Flap Surgery, Grafts) |
|---|---|---|
| Target Stage | Gingivitis, Mild-to-Moderate Periodontitis | Moderate-to-Severe Periodontitis, specific defects |
| Procedure | Deep cleaning below gum line, root smoothing | Incisions, lifting gum tissue, bone reshaping, grafts |
| Invasiveness | Minimally invasive | Invasive |
| Anesthesia | Local anesthetic | Local anesthetic, sometimes sedation |
| Pain/Discomfort | Mild to moderate, manageable with OTC pain relievers | Moderate to severe, often requires prescription pain medication |
| Recovery Time | Few days to a week | Several weeks to months |
| Cost (Ranges) | $200 - $600 per quadrant | $400 - $2,500+ per site/quadrant |
| Key Benefits | Stops disease progression, reduces inflammation | Reduces pocket depth, regenerates bone/tissue, saves teeth |
| Limitations | Cannot regenerate lost bone/tissue, less effective for deep pockets | More complex, higher cost, longer recovery, potential for more gum recession |
Children / Pediatric Considerations
While often associated with adults, gum infections can affect children and adolescents too. Understanding pediatric considerations is important for parents.
Gingivitis in Children
Gingivitis is quite common in children, often called "eruptive gingivitis" during periods of tooth eruption.
- Causes: Primarily poor oral hygiene, similar to adults. Inadequate brushing and flossing allow plaque to build up. Hormonal changes during puberty can also contribute to gingivitis in adolescents.
- Symptoms: Red, swollen, and bleeding gums. These gingivitis symptoms might be subtle and easy to miss, especially in the back of the mouth.
- Prevention & Treatment:
- Early Habits: Start cleaning an infant's gums even before teeth erupt. Brush primary teeth as soon as they appear.
- Supervised Brushing & Flossing: Parents should supervise and assist children with brushing until around age 7-8 and flossing until age 10-12 to ensure thorough cleaning.
- Regular Dental Visits: Pediatric dentists can detect gingivitis early and provide professional cleanings and guidance.
- Education: Teach children about the importance of oral hygiene in an age-appropriate manner.
Periodontitis in Children and Adolescents
While less common than in adults, periodontitis can occur in younger individuals, often with specific characteristics:
- Aggressive Periodontitis (previously Juvenile Periodontitis): This form can occur in otherwise healthy adolescents, characterized by rapid bone and attachment loss, often localized to specific teeth (e.g., molars and incisors). A genetic predisposition is often involved.
- Periodontitis as a Manifestation of Systemic Disease: In some cases, gum infections in children can be a sign of an underlying medical condition, such as certain genetic disorders (e.g., Down syndrome, Papillon-Lefèvre syndrome), blood disorders, or immune deficiencies.
- Diagnosis & Treatment:
- Diagnosis involves clinical examination, probing, and X-rays, similar to adults.
- Treatment can range from scaling and root planing to surgical interventions, often combined with antibiotics.
- Early diagnosis is critical to prevent extensive tooth loss and ensure that any underlying systemic issues are identified and managed.
Pro Tip for Parents: If you notice your child's gums are red, swollen, or bleed when they brush, or if they complain of bad breath that doesn't go away, schedule an appointment with their pediatric dentist right away. Don't assume it's just "growing pains" or normal.
Cost Breakdown for Gum Infection Treatment
A detailed look at costs helps in planning and budgeting for gum infection treatment. These are general US averages and can vary.
Average US Costs (Low, Mid, High) for Common Procedures (Without Insurance)
| Procedure | Low Range | Mid Range | High Range | Description |
|---|---|---|---|---|
| Routine Cleaning (Prophylaxis) | $75 | $120 | $200 | Preventive care, mild gingivitis. |
| Scaling & Root Planing (per quadrant) | $200 | $350 | $600 | "Deep cleaning" for periodontitis. Often 4 quadrants. |
| Full Mouth SRP | $800 | $1,400 | $2,400 | Total cost for all 4 quadrants. |
| Topical Antibiotic (per pocket) | $75 | $120 | $200 | Localized antibiotic placement. |
| Flap Surgery (per quadrant) | $500 | $800 | $1,500 | For moderate to severe periodontitis. |
| Bone Grafting (per site) | $600 | $1,500 | $2,500 | To regenerate lost jaw bone. |
| Soft Tissue Graft (per tooth) | $400 | $750 | $1,200 | For receding gums. |
| Guided Tissue Regeneration | $500 | $1,000 | $1,500 | Often combined with other surgeries. |
| Periodontal Maintenance (per visit) | $120 | $180 | $250 | Follow-up cleanings after periodontitis treatment. |
With vs. Without Insurance
- Without Insurance: You pay 100% of the listed costs. This can be substantial, especially for surgical procedures or full-mouth SRP.
- With Insurance: Costs are significantly reduced.
- Preventive: 80-100% covered.
- Basic (e.g., SRP): 50-80% covered after deductible. Example: For a $1,400 full mouth SRP, if insurance covers 70% after a $100 deductible, you pay $100 (deductible) + (0.30 * ($1,400-$100)) = $100 + $390 = $490.
- Major (e.g., Surgery): 30-50% covered after deductible. Example: For a $1,000 bone graft, if insurance covers 40% after a $100 deductible, you pay $100 (deductible) + (0.60 * ($1,000-$100)) = $100 + $540 = $640.
- Annual Maximum: Be aware of your annual maximum. If you need extensive treatment (e.g., SRP + multiple surgeries), you might hit your maximum quickly, and subsequent costs will be fully out-of-pocket for that year.
Payment Plans and Financing Options
- Dental Office Payment Plans: Many practices offer interest-free payment plans for larger treatment costs, spreading payments over several months.
- CareCredit/LendingClub: These medical credit cards offer promotional financing options, often with 0% interest for a set period (e.g., 6-24 months) if paid in full. Be mindful of deferred interest if the balance isn't paid off in time.
- Personal Loans: Banks and credit unions offer personal loans that can cover dental costs, but these typically carry interest.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use pre-tax dollars to pay for qualified dental expenses, effectively saving you money.
Cost-Saving Tips
- Early Intervention: Treating gingivitis is significantly cheaper than treating advanced periodontitis. Don't wait for symptoms to worsen.
- Preventive Care: Regular cleanings and good home care prevent the need for more expensive treatments.
- Shop Around: Get quotes from a few different dental offices or periodontists.
- Maximize Insurance Benefits: Understand your plan's coverage, deductibles, and annual maximums. If you have extensive treatment, consider phasing it over two benefit years to utilize two annual maximums.
- Dental Schools: University dental schools often provide treatment at a reduced cost, as procedures are performed by students under the supervision of experienced faculty.
- Dental Savings Plans: If you don't have insurance, consider a dental savings plan for discounts on services.

Frequently Asked Questions
What are the earliest signs of a gum infection?
The earliest signs of a gum infection, or gingivitis, include gums that are redder than usual, appear slightly swollen, and bleed easily when you brush or floss. You might also notice persistent bad breath. These gingivitis symptoms often develop without pain, which is why they are frequently overlooked.
Can a gum infection go away on its own?
No, a gum infection, especially periodontitis, will not go away on its own. While mild gingivitis might improve with diligent brushing and flossing, established plaque and tartar require professional cleaning to remove. If left untreated, the infection will almost always worsen, leading to irreversible damage.
Is scaling and root planing painful?
Scaling and root planing (deep cleaning) is typically performed under local anesthesia, so you should not feel pain during the procedure itself. Afterward, you might experience some soreness, tenderness, and increased tooth sensitivity for a few days to a week, which can usually be managed with over-the-counter pain relievers.
How long does it take to recover from gum surgery?
Recovery time for gum surgery varies depending on the type and extent of the procedure. For flap surgery, initial healing may take 1-2 weeks, but full tissue maturation can take several months. Bone or soft tissue grafts may require longer recovery periods, often 2-4 weeks for initial healing, with full integration taking many months.
Can gum infections affect other parts of my body?
Yes, absolutely. Gum infections are linked to various systemic health issues. The bacteria and inflammation from your gums can enter your bloodstream and contribute to conditions like heart disease, stroke, diabetes complications, respiratory diseases, and even pregnancy complications such as preterm birth.
How much does it cost to treat a gum infection?
The cost varies significantly based on the severity and type of treatment. A routine cleaning for gingivitis might cost $75-$200. Scaling and root planing for periodontitis can range from $800-$2,400 for a full mouth. Surgical treatments like flap surgery or bone grafting can cost $500-$2,500 per site or quadrant. Insurance typically covers a portion, but out-of-pocket expenses can still be substantial.
Can I treat a gum infection at home with natural remedies?
While good oral hygiene (brushing, flossing) is crucial for prevention and supporting professional treatment, natural remedies cannot cure an existing gum infection or remove hardened plaque and tartar. Things like salt water rinses can help soothe inflamed gums and kill some bacteria, but they are not a substitute for professional dental care.
How often should I get dental cleanings if I have gum disease?
If you have been diagnosed and treated for periodontitis, your dentist or periodontist will likely recommend "periodontal maintenance" cleanings more frequently than standard cleanings, typically every 3-4 months. This helps to control bacterial regrowth and prevent the disease from recurring or progressing.
What happens if I ignore my swollen gums?
Ignoring swollen gums can lead to the progression of gingivitis to periodontitis. As the infection deepens, it can cause irreversible bone loss, gum recession, persistent bad breath, and eventually loose teeth, potentially leading to tooth extraction. Untreated gum infection also poses risks to your overall health.
What are alternatives to gum surgery?
For mild to moderate periodontitis, non-surgical options like scaling and root planing are often the first choice. Antibiotics (oral or topical) may also be used in conjunction with these deep cleanings. While effective, these non-surgical methods cannot fully regenerate lost bone or tissue in advanced cases, which is where surgery becomes necessary.
When to See a Dentist
Knowing when to seek professional help for a gum infection is critical for preventing irreversible damage and protecting your overall health. Don't wait for pain to be your guide, as gum disease can often be painless until it's very advanced.
Routine Care Guidance:
- Annual or Bi-Annual Check-ups: Everyone should visit their dentist at least once a year, and ideally every six months, for a comprehensive examination and professional cleaning. These regular visits are crucial for detecting early signs of gum infection, like subtle gingivitis symptoms, before they become serious.
Red Flags That Need Attention Soon (Schedule an Appointment):
- Bleeding Gums: If your gums bleed when you brush, floss, or even eat, it's a primary indicator of gum inflammation or infection. This is NOT normal.
- Red, Swollen, or Tender Gums: If your gums appear unusually red, puffy, or feel sore to the touch.
- Persistent Bad Breath: If you have chronic bad breath that doesn't go away with brushing and flossing.
- Receding Gums: If your teeth appear longer than they used to, indicating your gum tissue is pulling away.
- Increased Sensitivity: If you experience new or increased sensitivity to hot or cold foods/drinks due to exposed tooth roots.
- Changes in Bite: If your teeth don't fit together the same way when you bite down.
Emergency Signs That Need Immediate Attention:
- Severe Pain: If you experience intense, throbbing pain in your gums or around a tooth.
- Loose or Shifting Teeth: If any of your teeth feel wobbly or appear to have shifted position. This is a sign of advanced bone loss.
- Pus or Abscess: If you notice pus coming from your gums, or a painful, swollen bump (abscess) on your gum tissue.
- Rapidly Worsening Symptoms: If your swollen gums or other symptoms rapidly become more severe within a short period.
- Systemic Symptoms: If oral symptoms are accompanied by fever, facial swelling, or difficulty swallowing, which could indicate a spreading infection.
If you observe any of these signs, especially the emergency red flags, contact your dentist or a periodontist (a gum specialist) immediately. Early diagnosis and treatment are your best defense against the damaging effects of gum infection.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
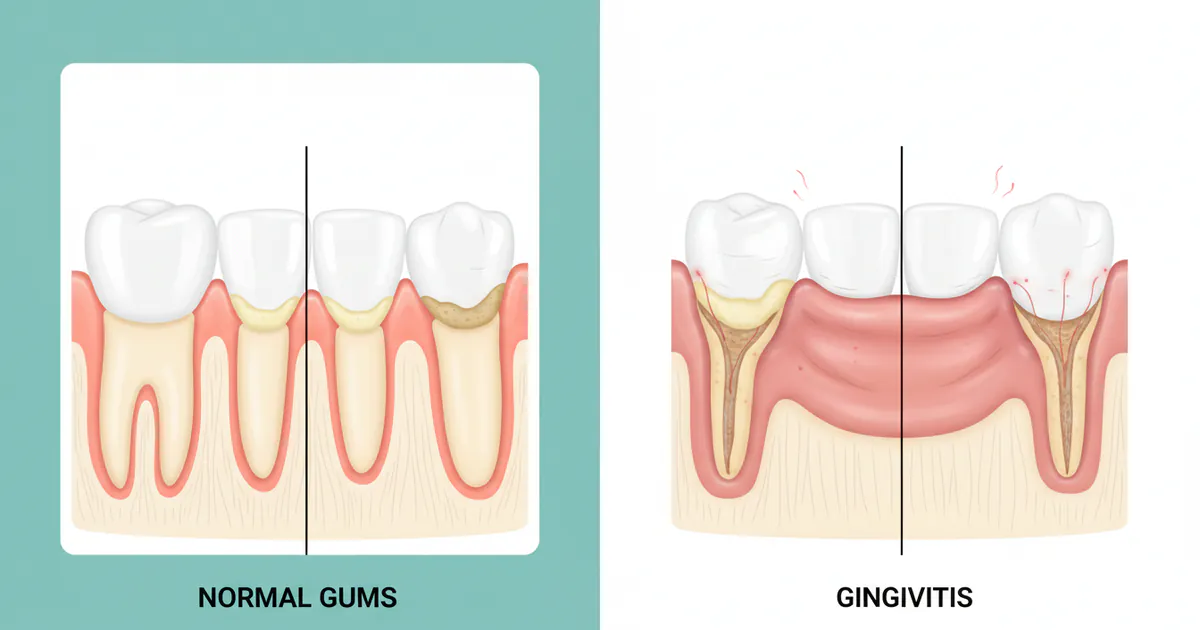
Normal Gums vs Gingivitis: Complete Comparison Guide
Did you know that nearly half of American adults over 30 show signs of gum disease, a condition that can range from mild inflammation to severe infection leading to tooth loss? Understanding the difference between healthy gums and those affected by early gum disease, known as gingivitis, is cruc
February 22, 2026
Can You Get Rid of Gingivitis
More than 50% of American adults aged 30 or older suffer from some form of gum disease, with gingivitis being the earliest and most common stage. This often silent condition, marked by inflammation of the gums, can seem daunting, leading many to wonder: can you get rid of gingivitis? The good ne
February 22, 2026
What Causes Receding Gums
Receding gums, a condition where the gum tissue surrounding the teeth pulls back or wears away, exposing more of the tooth or the tooth's root, affects a significant portion of the adult population in the United States. In fact, estimates suggest that **up to 88% of people over the age of 65 have on
February 22, 2026
Signs of Gingivitis: Complete Guide
Did you know that nearly half of American adults aged 30 and older suffer from some form of gum disease? While that statistic might sound alarming, the good news is that the earliest and most common stage, gingivitis, is entirely reversible. Recognizing the signs of gingivitis early is your
February 22, 2026