Can You Get Rid of Gingivitis
Key Takeaways
- More than 50% of American adults aged 30 or older suffer from some form of gum disease, with gingivitis being the earliest and most common stage. This often silent condition, marked by inflammation of the gums, can seem daunting, leading many to wonder: can you get rid of gingivitis? The good ne
More than 50% of American adults aged 30 or older suffer from some form of gum disease, with gingivitis being the earliest and most common stage. This often silent condition, marked by inflammation of the gums, can seem daunting, leading many to wonder: can you get rid of gingivitis? The good news is a resounding yes. Unlike its more advanced and irreversible counterpart, periodontitis, gingivitis is entirely treatable and reversible with proper care. Ignoring the early signs of gingivitis, however, can lead to serious health complications, including tooth loss and a potential link to systemic diseases. This comprehensive guide from SmilePedia.net will explore what gingivitis is, its causes, how it's treated, the costs involved, and most importantly, how you can effectively eliminate it and maintain optimal gum health. We'll delve into everything from professional dental cleanings to daily oral hygiene practices, ensuring you have all the information needed to protect your smile and overall well-being.
Key Takeaways:
- Yes, Gingivitis is Reversible: With proper treatment and diligent oral hygiene, gingivitis can be completely resolved, restoring gum health.
- Early Intervention is Crucial: Untreated gingivitis can progress to periodontitis, a more severe and irreversible form of gum disease that damages bone and can lead to tooth loss.
- Professional Cleaning is Key: A professional dental cleaning (prophylaxis) by a dentist or hygienist is typically the first and most effective step, usually costing between $75 and $200 without insurance.
- Daily Oral Hygiene Matters: Brushing twice daily, flossing once daily, and using an antiseptic mouthwash are essential for treatment and prevention.
- Timeline for Improvement: Visible improvement can often be seen within 1-2 weeks of starting treatment and consistent home care, with full resolution taking a few weeks to months.
- Cost Varies: Treatment costs range from routine cleanings ($75-$200) to more intensive scaling and root planing (SRP) for deeper pockets ($200-$500 per quadrant), with insurance significantly reducing out-of-pocket expenses.
- Prevention is Ongoing: Regular dental check-ups (every 6 months), a balanced diet, and avoiding tobacco products are vital for long-term prevention.
What is Gingivitis? An Overview of Gum Inflammation
Gingivitis is the mildest form of periodontal disease, an inflammation of the gums (gingiva) caused by the accumulation of plaque—a sticky, colorless film of bacteria—on the teeth. When plaque isn't removed effectively through regular brushing and flossing, it produces toxins that irritate the gum tissue, leading to inflammation.

The key characteristic of gingivitis is that the inflammation affects only the soft gum tissue, without damaging the underlying bone or ligaments that support the teeth. This is a critical distinction from periodontitis, its more advanced stage, where the infection spreads below the gum line and begins to erode bone and connective tissue. Because gingivitis does not involve irreversible damage to the bone, it is entirely curable and reversible with appropriate treatment and consistent oral hygiene.
According to the Centers for Disease Control and Prevention (CDC), nearly half of all adults aged 30 and older in the United States show signs of gum disease, with a significant portion experiencing gingivitis. Its high prevalence makes it a major public health concern, yet many people are unaware they have it because it often presents with mild symptoms, or no pain, in its early stages.
Understanding gingivitis is the first step toward preventing its progression and maintaining a healthy mouth. It's a localized bacterial infection that, while initially confined to the gums, serves as a significant warning sign that your oral health routine needs attention. Addressing gingivitis promptly not only restores gum health but also protects against the development of more severe and potentially systemic health issues.
Causes: Why Gingivitis Happens
The primary cause of gingivitis is the accumulation of bacterial plaque on the teeth, particularly along the gum line. However, several contributing factors can exacerbate this issue or make individuals more susceptible.
1. Plaque and Tartar Buildup
Plaque: This sticky, colorless film forms constantly on your teeth. It consists of bacteria, food particles, and saliva. If not removed by daily brushing and flossing, the bacteria in plaque produce toxins that irritate the gum tissue, leading to inflammation. Tartar (Calculus): When plaque remains on the teeth for too long, it hardens into tartar. Tartar provides a rough surface where more plaque can accumulate, and it's much harder to remove with just a toothbrush. Tartar buildup acts as a constant irritant to the gums, creating a breeding ground for bacteria and making professional cleaning essential.
2. Poor Oral Hygiene
Inadequate brushing and flossing are direct pathways to gingivitis. If plaque isn't regularly and thoroughly removed, it will inevitably lead to gum inflammation. The American Dental Association (ADA) recommends brushing twice a day for two minutes with fluoride toothpaste and flossing once a day.
3. Hormonal Changes
Fluctuations in hormones can make gums more sensitive and increase blood flow, making them more susceptible to inflammation. This is particularly common during:
- Pregnancy: "Pregnancy gingivitis" is a well-known phenomenon, affecting 60-75% of pregnant women.
- Puberty: Increased hormone levels can lead to more pronounced gingival inflammation.
- Menstruation: Some women experience temporary gum changes during their menstrual cycle.
- Menopause: Hormonal shifts can also affect gum health.
4. Certain Medications
Some medications can reduce saliva flow (xerostomia or dry mouth), which is crucial for washing away food particles and neutralizing acids. Reduced saliva allows plaque to accumulate more easily. Examples include:
- Antihistamines
- Antidepressants
- Diuretics
- Antihypertensives Other medications, like certain anticonvulsants (e.g., phenytoin) and calcium channel blockers (e.g., nifedipine), can cause gingival overgrowth, making gums harder to clean and more prone to inflammation.
5. Systemic Diseases and Conditions
Underlying health issues can compromise the body's immune response or affect gum tissue directly:
- Diabetes: Individuals with uncontrolled diabetes are at a higher risk of developing gingivitis and more severe periodontal disease due to impaired immune function and blood vessel changes.
- Compromised Immunity: Conditions like HIV/AIDS or treatments like chemotherapy can weaken the immune system, making the body less able to fight off bacterial infections in the gums.
- Crohn's Disease and Other Inflammatory Conditions: Systemic inflammation can manifest in the oral cavity.
6. Nutritional Deficiencies
A diet lacking essential nutrients can impair the body's ability to maintain healthy tissues and fight infection.
- Vitamin C Deficiency: Scurvy, caused by severe vitamin C deficiency, is known to cause severe gum inflammation and bleeding.
- Other Micronutrients: Deficiencies in vitamins A, B, and D, as well as calcium and iron, can also impact gum health.
7. Tobacco Use
Smoking and other forms of tobacco use are significant risk factors for gum disease. Tobacco reduces blood flow to the gums, impairs the immune system, and interferes with the healing process, masking the typical signs of inflammation and making it harder for the body to fight off infection.
8. Genetics
Some individuals may be genetically predisposed to developing gum disease, making them more susceptible even with good oral hygiene.
9. Age
The risk of gum disease increases with age, possibly due to a lifetime of exposure to contributing factors and cumulative wear and tear on oral tissues.
By understanding these causes, individuals can take proactive steps to mitigate their risk and address gingivitis effectively.
Signs and Symptoms: What to Look For
Recognizing the early signs of gingivitis is crucial for timely intervention and preventing its progression to more severe forms of gum disease. While some symptoms can be subtle, especially in the initial stages, knowing what to look for can help you identify a problem before it escalates.
Here are the most common signs and symptoms of gingivitis:
- Red or Puffy Gums: Healthy gums should be firm and pale pink. Gums affected by gingivitis often appear darker red, purplish, or inflamed. They may look swollen or puffy rather than taut around the teeth.
- Bleeding Gums: This is one of the most classic and noticeable signs. Gums that bleed easily during brushing, flossing, or even when eating certain foods are a strong indicator of gingivitis. Healthy gums should not bleed.
- Tender or Sore Gums: Your gums might feel tender to the touch or sore, especially when brushing or flossing. While gingivitis typically doesn't cause significant pain in its early stages, mild discomfort or sensitivity is common.
- Receding Gums: In some cases, gingivitis can lead to gums pulling away from the teeth, making the teeth appear longer. This creates pockets where more plaque and bacteria can accumulate, worsening the condition.
- Bad Breath (Halitosis): Persistent bad breath that doesn't go away after brushing or using mouthwash can be a sign of bacterial accumulation in the mouth, particularly around the gum line. The bacteria responsible for gingivitis release volatile sulfur compounds that cause an unpleasant odor.
- Shiny Gums: Inflamed gums can sometimes have a glossy or shiny appearance due to swelling and fluid retention.
- Soft Gums: Instead of being firm, gums affected by gingivitis may feel soft and spongy when touched.
It's important to note that many people with gingivitis may not experience pain, which can lead them to overlook the condition. This is why regular dental check-ups are so important – a dentist or hygienist can spot gingivitis even before you notice significant symptoms. If you observe any of these signs, particularly bleeding gums, it's a clear indication that you need to schedule a dental appointment.
``
Can You Get Rid of Gingivitis? The Definitive Answer
Yes, absolutely. You can get rid of gingivitis completely. This is the most crucial distinction between gingivitis and its more severe counterpart, periodontitis. Because gingivitis only affects the soft tissues of the gums and does not yet involve damage to the underlying bone or connective tissue, it is fully reversible. The key lies in prompt diagnosis and consistent, effective treatment.

When the bacterial plaque that causes the inflammation is thoroughly removed, and good oral hygiene practices are established and maintained, the gum tissue has an incredible capacity to heal and return to a healthy state. The redness, swelling, and bleeding will subside, and the gums will become firm and pink again.
However, the reversibility of gingivitis hinges entirely on action. Ignoring the symptoms or neglecting proper oral care will lead to its progression. If left untreated, gingivitis will almost certainly advance to periodontitis, which is an irreversible condition where the infection spreads to destroy the bone and ligaments supporting your teeth. Once bone is lost, it cannot be fully regenerated naturally. This is why early intervention for gingivitis is not just recommended, but essential for preserving your oral health and preventing a lifetime of more complex and costly dental issues, including the potential need for a best periodontist near me if the condition becomes severe.
The path to getting rid of gingivitis involves a combination of professional dental care and diligent personal oral hygiene. This two-pronged approach ensures that both existing plaque and tartar are removed, and future accumulation is minimized.
Treatment Options for Gingivitis
Successfully treating gingivitis involves a combination of professional dental procedures and a rigorous at-home oral hygiene routine. The goal is to eliminate plaque and tartar, reduce inflammation, and prevent recurrence.
1. Professional Dental Cleaning (Prophylaxis)
This is the cornerstone of gingivitis treatment. A dental hygienist or dentist uses specialized tools to remove plaque and tartar (hardened plaque) from the surfaces of your teeth, both above and slightly below the gum line.
- Description: A standard cleaning removes soft plaque and calcified tartar that cannot be removed by regular brushing and flossing.
- Pros: Highly effective for early-stage gingivitis, relatively quick, non-invasive, and helps prevent progression.
- Cons: Requires regular scheduling; not sufficient for advanced gum disease.
- Cost: Typically ranges from $75 to $200 in the US without insurance, often covered by most dental plans.
2. Scaling and Root Planing (SRP)
While standard prophylaxis is usually sufficient for mild gingivitis, if the gingivitis has caused deeper pockets to form around the teeth, or if there are signs of early bone loss (indicating mild periodontitis), your dentist might recommend scaling and root planing. This is a deeper cleaning procedure.
- Description: Scaling involves removing plaque and tartar from above and below the gum line, all the way down to the root. Root planing then smooths the tooth root surfaces, which helps prevent bacteria from reattaching and allows the gums to reattach to the teeth. It's often performed under local anesthesia.
- Pros: More thorough cleaning for deeper pockets, can reverse early stages of gum disease where bone loss is minimal, and prepares gums for reattachment.
- Cons: More invasive than a standard cleaning, can cause temporary sensitivity and discomfort, and more expensive.
- Cost: Ranges from $200 to $500 per quadrant (a quarter of the mouth) without insurance, often partially covered by dental insurance.
3. Antiseptic Mouthwashes
Prescription-strength antiseptic mouthwashes can be a valuable adjunct to brushing and flossing, especially when directed by your dentist.
- Description: Products containing chlorhexidine gluconate are highly effective at reducing bacteria and controlling gingival inflammation. Over-the-counter mouthwashes with ingredients like essential oils (e.g., Listerine) or cetylpyridinium chloride (e.g., Scope) can also help.
- Pros: Reduces bacterial load, helps manage inflammation, and freshens breath.
- Cons: Prescription strength can temporarily stain teeth or alter taste perception; overuse of alcohol-based mouthwashes can cause dry mouth.
- Cost: Over-the-counter options typically cost $5-$15, while prescription options can be $15-$30.
4. Antibiotics (Topical or Oral)
In rare cases, or if gingivitis is particularly aggressive or unresponsive to initial treatments, antibiotics might be prescribed.
- Description: Topical antibiotics (gels or chips placed in periodontal pockets) or oral antibiotics may be used to target specific bacteria causing the infection.
- Pros: Can help control severe bacterial infections.
- Cons: Risk of antibiotic resistance, side effects like stomach upset, not a primary treatment for typical gingivitis.
- Cost: Varies by antibiotic, typically $10-$50 for a course.
5. At-Home Oral Hygiene Instruction
A crucial part of treatment involves improving your daily oral hygiene routine. Your dental professional will provide personalized instructions.
- Description: This includes demonstrating proper brushing techniques (using a soft-bristled brush, electric toothbrush often recommended), effective flossing, and potentially interdental brushes or water flossers.
- Pros: Empowers you to maintain gum health, essential for preventing recurrence, and cost-effective.
- Cons: Requires consistency and commitment.
Comparison Table: Common Gingivitis Treatments
| Treatment Type | Description | Typical Cost (US, without insurance) | Key Benefits | Best For |
|---|---|---|---|---|
| Professional Cleaning (Prophylaxis) | Removal of plaque and tartar above and slightly below gum line. | $75 - $200 | Reverses mild gingivitis, prevents progression, fresh breath. | Mild to moderate gingivitis, routine maintenance. |
| Scaling & Root Planing (SRP) | Deep cleaning below the gum line, removal of tartar, and root smoothing. | $200 - $500 per quadrant | Treats deeper pockets, prevents mild periodontitis, promotes reattachment. | More advanced gingivitis or early mild periodontitis with pocketing. |
| Antiseptic Mouthwash | Rinses containing antibacterial agents (e.g., chlorhexidine). | $5 - $30 | Reduces bacteria, controls inflammation, adjunct to brushing/flossing. | As an adjunct therapy, especially if advised by a dentist. |
| Oral Hygiene Instruction | Personalized guidance on proper brushing, flossing, and interdental cleaning. | Included in dental visit | Empowers patient, essential for long-term prevention. | All stages of gingivitis, prevention of recurrence. |
Pro Tip: For persistent or recurring gingivitis, especially if you suspect it's progressing to mild periodontitis, consider consulting a periodontist. A best periodontist near me specializes in gum disease and can offer advanced diagnostic and treatment options.
Step-by-Step Process for Treatment
Successfully treating and reversing gingivitis typically follows a structured process, combining professional intervention with diligent home care.
Step 1: Initial Dental Examination and Diagnosis
- What to expect: Your journey begins with a comprehensive oral examination by a general dentist. They will visually inspect your gums for signs of redness, swelling, and bleeding. A dental hygienist will typically use a periodontal probe to measure the depth of the pockets around your teeth. Healthy gums have pocket depths of 1-3 millimeters. Depths greater than 3mm, especially with bleeding, indicate gingivitis or more advanced gum disease. X-rays may be taken to check for bone loss, which differentiates gingivitis from periodontitis.
- Outcome: A definitive diagnosis of gingivitis and a personalized treatment plan.
Step 2: Professional Dental Cleaning (Prophylaxis or Scaling and Root Planing)
- What to expect: This is the core of professional treatment.
- Prophylaxis: For mild gingivitis, a routine cleaning will be performed. The dental hygienist will use ultrasonic scalers and hand instruments to meticulously remove all plaque and tartar from the tooth surfaces, both above and slightly below the gum line.
- Scaling and Root Planing (SRP): If your gingivitis is more advanced, with deeper pockets (4mm or more) and persistent inflammation, or if there's suspicion of early bone involvement (mild periodontitis), a deep cleaning might be recommended. This usually requires local anesthesia to numb the gums and ensure comfort. The hygienist will go deeper under the gum line to remove tartar and smooth the root surfaces. This procedure is often done in multiple appointments, treating one quadrant of the mouth at a time.
- Outcome: Removal of bacterial irritants, providing a clean surface for gum healing.
``
Step 3: Oral Hygiene Instruction
- What to expect: After the cleaning, your dental professional will spend time educating you on proper oral hygiene techniques. This is critical for long-term success. They will demonstrate:
- Brushing: Using a soft-bristled brush, proper angle (45 degrees to the gum line), gentle circular motions, and brushing for two minutes, twice a day. An electric toothbrush is often recommended for its efficiency.
- Flossing: Correct technique for interdental cleaning, ensuring you clean up both sides of each tooth.
- Optional Aids: Recommendations for antiseptic mouthwash, interdental brushes, or a water flosser, depending on your individual needs.
- Outcome: You gain the knowledge and skills to effectively maintain your oral health at home.
Step 4: Follow-up and Maintenance
- What to expect: A follow-up appointment is often scheduled a few weeks after SRP to assess gum healing and ensure pockets are reducing. Regardless of the initial cleaning type, regular dental check-ups and cleanings (typically every six months, but sometimes more frequently for gingivitis patients) are essential to prevent recurrence. Your dentist will monitor your gum health and reinforce good habits.
- Outcome: Long-term prevention of gingivitis and early detection of any issues.

Pro Tip: Consistency is key. Even the most thorough professional cleaning won't prevent gingivitis from returning if daily brushing and flossing are neglected. Make oral hygiene a non-negotiable part of your routine.
Cost and Insurance for Gingivitis Treatment
Understanding the financial aspect of gingivitis treatment is crucial for patients in the US. Costs can vary significantly based on the severity of the condition, the type of treatment needed, the dental professional's location, and whether you have dental insurance.
Typical US Price Ranges for Gingivitis Treatments (Without Insurance)
- Initial Dental Exam (D0120/D0150):
- Range: $50 - $150
- Includes visual inspection, charting, and sometimes a basic screening.
- Dental X-rays (D0210/D0274):
- Full Mouth Series: $100 - $250
- Bitewings (4 films): $40 - $100
- Essential for detecting bone loss or other underlying issues.
- Professional Cleaning (Prophylaxis - D1110):
- Range: $75 - $200
- This is the standard cleaning for healthy gums or mild gingivitis.
- Scaling and Root Planing (SRP - D4341/D4342):
- Range: $200 - $500 per quadrant
- A full mouth SRP can therefore cost between $800 and $2,000. This deep cleaning is for moderate to severe gingivitis or mild periodontitis.
- Antiseptic Mouthwash (Prescription):
- Range: $15 - $30
- Over-the-counter options are generally less than $15.
- Periodontal Maintenance (D4910):
- Range: $100 - $250
- After SRP, patients often require more frequent and specialized cleanings to prevent recurrence.
Regional Variations: Costs can fluctuate based on the cost of living in a particular area. Major metropolitan areas (e.g., New York City, Los Angeles) tend to have higher prices compared to rural areas or states with lower costs of living.
Insurance Coverage Details
Most dental insurance plans in the US offer some level of coverage for gingivitis treatment, as it is considered a preventative or basic restorative service.
- Preventative Care (Exams, Cleanings, X-rays):
- Typically covered at 80-100%. Most plans cover two routine cleanings per year, and one set of bitewing X-rays annually or a full mouth series every 3-5 years. This means your out-of-pocket cost for a routine cleaning for gingivitis could be very low or even zero.
- Scaling and Root Planing (SRP):
- Often categorized under "Basic Restorative" or "Major Restorative" services, depending on the plan.
- Coverage typically ranges from 50-80% after you've met your deductible. You would be responsible for the remaining percentage (copay) and any applicable deductible.
- Deductibles: Many plans have an annual deductible (e.g., $50-$100) that you must pay out-of-pocket before your insurance starts covering costs.
- Annual Maximums: Most dental insurance plans have an annual maximum benefit (e.g., $1,000 - $2,000). Once you reach this limit, you pay 100% of subsequent costs. SRP for a full mouth could easily hit or exceed this maximum.
- Waiting Periods: Some plans have waiting periods (e.g., 3-6 months for basic procedures, 6-12 months for major procedures) before certain treatments are covered. If you need SRP immediately after enrolling, you might have to pay out-of-pocket.
Payment Plans and Financing Options
If you don't have insurance or face significant out-of-pocket costs, several options can help manage the financial burden:
- Dental Payment Plans: Many dental offices offer in-house payment plans, allowing you to pay for treatment in interest-free installments.
- Third-Party Financing (e.g., CareCredit, LendingClub): These companies offer specialized healthcare credit cards with deferred interest options or low-interest payment plans, often over periods of 6 to 60 months.
- Discount Dental Plans: Not insurance, but these plans offer a discount on services from participating dentists for an annual fee. Discounts can range from 10-60%.
- Community Dental Clinics: Often provide services at reduced rates based on income.
- Dental Schools: May offer lower-cost treatment performed by students under supervision of experienced faculty.
Cost-Saving Tips
- Preventative Care: The single best way to save money is to prevent gingivitis from developing or progressing. Regular brushing, flossing, and routine check-ups are far less expensive than treating advanced gum disease.
- Utilize Insurance Benefits: Understand your plan's coverage, deductibles, and annual maximums. Schedule treatments strategically to maximize benefits.
- Ask for a Treatment Plan Estimate: Always request a written estimate from your dentist detailing the proposed treatments and their costs before proceeding.
- Compare Dentists: Prices can vary. If you're looking for a best periodontist near me or general dentist, call around for price comparisons, especially for specific procedures.
Comparison Table: Cost of Gingivitis Treatment With vs. Without Insurance
| Procedure | Typical Cost (Without Insurance) | Typical Cost (With Insurance, after deductible) |
|---|---|---|
| Initial Exam & X-rays | $150 - $400 | $0 - $50 (Often 80-100% covered) |
| Professional Cleaning | $75 - $200 | $0 - $20 (Often 80-100% covered) |
| Scaling & Root Planing (per quadrant) | $200 - $500 | $40 - $250 (Often 50-80% covered) |
| Periodontal Maintenance | $100 - $250 | $20 - $125 (Often 50-80% covered) |
Understanding these costs and insurance details empowers you to make informed decisions about your gingivitis treatment and maintain your oral health affordably.
Recovery and Aftercare for Gingivitis Treatment
Once you've undergone professional treatment for gingivitis, the journey to full gum health is largely dependent on your commitment to recovery and diligent aftercare. The good news is that with proper maintenance, your gums can fully heal and remain healthy.
Immediate Post-Treatment Expectations
After a professional cleaning (prophylaxis) for mild gingivitis, you might experience very minor and temporary effects:
- Mild Sensitivity: Your teeth or gums might feel a bit sensitive, especially to hot or cold, for a day or two. This is normal as the gums heal.
- Minor Gum Tenderness: Your gums might be slightly sore or tender, particularly if significant tartar was removed.
If you underwent Scaling and Root Planing (SRP) for more advanced gingivitis or mild periodontitis, the recovery period might involve:
- Increased Sensitivity: More pronounced tooth and gum sensitivity, potentially lasting a few days to a couple of weeks. Your dentist might recommend a desensitizing toothpaste.
- Gum Soreness/Swelling: Gums may be sore, swollen, or even slightly bruised for a few days. Over-the-counter pain relievers like ibuprofen or acetaminophen can help manage discomfort.
- Slight Bleeding: Some minor bleeding when brushing or flossing can occur for a few days as the gums heal.
- Dietary Adjustments: It's often recommended to stick to soft foods for a day or two after SRP, especially if you received anesthesia. Avoid extremely hot, cold, spicy, or crunchy foods.
Long-Term Aftercare and Maintenance
The key to preventing gingivitis from returning is consistent and effective long-term aftercare. This is where your daily habits become paramount.
-
Meticulous Oral Hygiene:
- Brush Twice Daily: Use a soft-bristled toothbrush or an electric toothbrush. Brush for at least two minutes, covering all surfaces of your teeth and gently along the gum line.
- Floss Once Daily: Flossing removes plaque and food particles from between your teeth and under the gum line where your toothbrush can't reach. This is non-negotiable for gum health.
- Antiseptic Mouthwash: Your dentist might recommend an antimicrobial mouthwash (prescription or over-the-counter) to further reduce bacteria. Use as directed.
- Interdental Cleaners/Water Flossers: If you have larger gaps between teeth or struggle with traditional floss, interdental brushes or a water flosser can be highly effective.
-
Regular Dental Check-ups and Cleanings:
- Frequency: For most individuals, especially those who have had gingivitis, a professional cleaning and check-up every six months is crucial. Your dentist may recommend more frequent visits (e.g., every 3-4 months for periodontal maintenance) if you had SRP or are at higher risk of recurrence.
- Purpose: These visits allow your dental team to monitor your gum health, remove any new plaque and tartar buildup, and address issues before they escalate.
-
Healthy Lifestyle Choices:
- Balanced Diet: Consume a diet rich in vitamins and minerals, especially Vitamin C and calcium, which are vital for gum health. Limit sugary snacks and drinks.
- Quit Smoking: Tobacco use severely compromises gum health and healing. Quitting is one of the most impactful steps you can take.
- Manage Systemic Conditions: If you have conditions like diabetes, ensure they are well-controlled, as they directly impact gum health.
- Hydration: Drink plenty of water to help wash away food particles and bacteria.
-
Monitor Your Gums:
- Pay attention to the color, texture, and any bleeding from your gums. If you notice any returning signs of gingivitis, contact your dentist promptly. Early detection can prevent a relapse.
Pro Tip: Consider investing in an electric toothbrush and a water flosser. Many studies show they are more effective at plaque removal than manual brushing and traditional flossing, providing an extra layer of protection against gingivitis recurrence.
By diligently following these aftercare instructions, you can ensure that your efforts to get rid of gingivitis are successful and that you maintain healthy, resilient gums for years to come.
Prevention: How to Keep Gingivitis Away
Preventing gingivitis is largely within your control and revolves around consistent, effective oral hygiene and healthy lifestyle choices. Since gingivitis is caused by bacterial plaque, the goal of prevention is to minimize plaque accumulation and reduce factors that contribute to gum inflammation.
-
Brush Your Teeth Twice Daily:
- Technique: Use a soft-bristled toothbrush and fluoride toothpaste. Angle the brush at 45 degrees to the gum line, gently moving it back and forth in short strokes.
- Duration: Brush for at least two minutes each time, ensuring you cover all tooth surfaces, including the tongue to remove bacteria.
- Replacement: Replace your toothbrush every 3-4 months, or sooner if the bristles are frayed. Frayed bristles are less effective at cleaning.
- Electric Toothbrushes: Many dentists recommend electric toothbrushes as they can be more effective at removing plaque than manual brushing.
-
Floss Daily:
- Importance: Flossing is crucial because it removes plaque and food particles from between your teeth and under the gum line, areas your toothbrush cannot reach.
- Technique: Use about 18 inches of floss, wrapping it around your middle fingers. Guide the floss between your teeth, forming a "C" shape against one tooth, and gently slide it up and down the side of the tooth and below the gum line. Repeat for the adjacent tooth. Use a clean section of floss for each tooth.
- Alternatives: If you find traditional flossing difficult, consider interdental brushes, dental picks, or a water flosser.
-
Use an Antiseptic Mouthwash:
- As an Adjunct: While not a substitute for brushing and flossing, an antimicrobial mouthwash can help reduce bacteria and plaque throughout the mouth.
- Types: Look for mouthwashes containing ingredients like cetylpyridinium chloride, essential oils, or fluoride. Discuss with your dentist if a prescription-strength mouthwash like chlorhexidine is appropriate for you, especially if you have a history of gingivitis.
-
Regular Dental Check-ups and Professional Cleanings:
- Frequency: Visit your dentist at least once every six months for a professional cleaning and examination. For individuals prone to gum disease, your dentist might recommend more frequent visits.
- Purpose: These visits allow dental professionals to remove hardened plaque (tartar) that you cannot remove at home, check for early signs of gum disease, and provide personalized advice.
-
Maintain a Healthy, Balanced Diet:
- Nutrients: A diet rich in fruits, vegetables, and whole grains provides essential vitamins and minerals that support overall health, including gum health. Vitamin C, for instance, is vital for healthy gum tissue.
- Limit Sugary Foods and Drinks: Sugar promotes bacterial growth and acid production, leading to plaque formation and tooth decay, which can exacerbate gum problems.
-
Avoid Tobacco Products:
- Impact: Smoking and chewing tobacco are major risk factors for gingivitis and periodontitis. Tobacco reduces blood flow to the gums, impairs the immune response, and hinders healing.
- Recommendation: Quitting tobacco is one of the most effective steps you can take to prevent gum disease and improve your overall health.
-
Manage Systemic Health Conditions:
- Diabetes Control: If you have diabetes, managing your blood sugar levels is crucial for preventing gum disease, as uncontrolled diabetes increases susceptibility to infections.
- Other Conditions: Discuss any systemic health issues or medications with your dentist, as they may impact your gum health.
-
Address Dental Issues Promptly:
- Crooked Teeth/Poorly Fitting Restorations: Misaligned teeth, crowded teeth, or poorly fitting dental fillings and crowns can create areas where plaque accumulates easily and are difficult to clean effectively. Addressing these issues can improve oral hygiene.
By incorporating these preventative measures into your daily routine, you can significantly reduce your risk of developing gingivitis and maintain a healthy, vibrant smile.
Risks and Complications of Untreated Gingivitis
While gingivitis is reversible, ignoring its warning signs and neglecting treatment can lead to a cascade of serious oral and systemic health problems. The most significant risk is its progression to a more advanced and destructive form of gum disease.
1. Progression to Periodontitis
This is the most direct and severe consequence of untreated gingivitis.
- What happens: When gingivitis is left unaddressed, the inflammation and infection spread from the gums to the underlying structures supporting the teeth. The bacterial toxins break down the bone and connective tissue that hold teeth in place, forming deeper pockets between the teeth and gums.
- Irreversible Damage: Unlike gingivitis, periodontitis causes irreversible bone loss. Once bone is lost, it cannot regenerate naturally to its previous level. This leads to gum recession, loose teeth, and eventually, tooth loss. Early stages of this progression are often referred to as mild periodontitis.
- Treatment: Periodontitis requires more aggressive and complex treatments, often involving deep scaling and root planing, antibiotics, and potentially surgical procedures performed by a specialist (a best periodontist near me).

2. Tooth Loss
As periodontitis advances, the destruction of bone and connective tissue weakens the support structures of the teeth. Teeth may become progressively loose, shift out of alignment, and eventually fall out or require extraction. This has significant impacts on chewing, speech, and facial aesthetics.
3. Chronic Bad Breath (Halitosis)
The persistent bacterial activity and breakdown of tissue in inflamed and infected gums release foul-smelling volatile sulfur compounds, leading to chronic and often severe bad breath that regular brushing and mouthwash cannot mask.
4. Abscess Formation
Infected periodontal pockets can accumulate pus, leading to the formation of painful gum abscesses. These localized infections can cause significant pain, swelling, and can sometimes spread to other areas.
5. Increased Risk of Systemic Health Issues
Growing research indicates a strong link between periodontal disease (including untreated gingivitis progressing to periodontitis) and various systemic health conditions. The bacteria and inflammatory byproducts from infected gums can enter the bloodstream and travel throughout the body.
- Cardiovascular Disease: Periodontal disease is associated with an increased risk of heart attack, stroke, and other cardiovascular problems.
- Diabetes: There's a bidirectional relationship; diabetics are more prone to gum disease, and severe gum disease can make blood sugar control more difficult.
- Respiratory Diseases: Oral bacteria can be aspirated into the lungs, potentially leading to pneumonia or exacerbating existing respiratory conditions.
- Pregnancy Complications: Pregnant women with periodontitis may have a higher risk of preterm birth and low birth weight babies.
- Other Conditions: Links have also been suggested with rheumatoid arthritis, certain cancers, and cognitive decline.
6. Compromised Aesthetics and Self-Esteem
Inflamed, bleeding, or receding gums, along with potential tooth loss or shifting, can significantly impact the appearance of your smile, leading to self-consciousness and reduced quality of life.
7. Increased Dental Costs
Ignoring gingivitis means facing more complex, invasive, and expensive treatments down the line. Preventative care and early gingivitis treatment are far more cost-effective than managing advanced periodontitis, which might involve surgery, implants, or dentures.
The risks associated with untreated gingivitis are substantial. Taking proactive steps to address gum inflammation early is not just about saving your teeth; it's about safeguarding your overall health and well-being.
Children / Pediatric Considerations for Gingivitis
Gingivitis is not exclusive to adults; children and adolescents can also develop this common gum condition. While often milder in children, recognizing and treating it early is crucial to instill good oral hygiene habits and prevent future complications.
Causes in Children
Similar to adults, the primary cause of gingivitis in children is poor oral hygiene leading to plaque buildup. However, some specific factors might be more prevalent in younger populations:
- Inadequate Brushing/Flossing: Children may lack the dexterity or motivation for thorough cleaning.
- Orthodontic Appliances: Braces, retainers, and other orthodontic devices create more surfaces for plaque to accumulate and can make brushing and flossing more challenging. "Gingivitis associated with orthodontic treatment" is common.
- Eruption Gingivitis: As permanent teeth erupt, the surrounding gum tissue can become temporarily inflamed, making it more susceptible to plaque buildup.
- Hormonal Changes: Puberty brings hormonal fluctuations that can make gums more sensitive and prone to inflammation, particularly in teenagers.
- Mouth Breathing: Chronic mouth breathing can dry out the gums, especially in the front of the mouth, making them more vulnerable to inflammation.
- Poor Diet: Frequent consumption of sugary snacks and drinks contributes to plaque formation.
Signs and Symptoms in Children
Parents should look for these indicators:
- Red, Swollen Gums: Gums appear redder than usual, puffy, or slightly enlarged.
- Bleeding Gums: Gums bleeding during brushing, flossing, or even when eating.
- Bad Breath: Persistent bad breath that doesn't resolve after brushing.
- Tenderness: The child might complain of sensitive or sore gums.
Treatment for Children
The treatment principles for children are similar to adults, focusing on eliminating plaque and improving oral hygiene:
- Professional Cleaning: A pediatric dentist or hygienist will perform a gentle cleaning to remove plaque and tartar.
- Oral Hygiene Education: This is paramount. The dental team will educate both the child and parents on proper brushing and flossing techniques, emphasizing the importance of consistency. Parents often need to supervise younger children's brushing.
- Dietary Advice: Counseling on limiting sugary foods and drinks.
- Addressing Contributing Factors: If orthodontic appliances are present, specific cleaning instructions will be given. If mouth breathing is an issue, referral to an ENT might be considered.
Prevention Tips for Parents
- Start Early: Begin cleaning a baby's gums with a soft cloth even before teeth erupt. Once teeth appear, brush twice daily with a soft-bristled, appropriately sized toothbrush and a tiny smear of fluoride toothpaste (rice grain size for under 3, pea-size for 3-6).
- Supervise Brushing: Help younger children brush and floss until they develop the dexterity, usually around age 7-8.
- Make it Fun: Use child-friendly toothbrushes, flavored toothpaste, and make brushing a positive experience.
- Regular Dental Visits: Schedule the first dental visit by age one or when the first tooth appears. Regular check-ups every six months are vital for early detection and preventative care.
- Lead by Example: Children are more likely to adopt good habits if they see their parents practicing them.
- Healthy Snacks: Offer nutritious snacks and limit sugary treats and drinks.
Addressing gingivitis in children promptly not only resolves the current inflammation but also lays the foundation for a lifetime of healthy oral habits and prevents the progression to more serious gum disease in adulthood.
Frequently Asked Questions
Can gingivitis go away on its own?
No, gingivitis typically does not go away on its own. While its symptoms might fluctuate in severity, the underlying cause—bacterial plaque and tartar buildup—requires active removal through professional cleaning and diligent daily oral hygiene to resolve. Without intervention, it is likely to persist or worsen.

How long does it take to get rid of gingivitis?
Visible improvement in gum health, such as reduced bleeding and swelling, can often be seen within 1-2 weeks of starting professional treatment and consistent home care. Complete resolution, with gums returning to a firm, pink state, usually takes a few weeks to a couple of months, depending on the initial severity and your commitment to daily hygiene.
Is gingivitis painful?
Gingivitis typically causes very little to no pain in its early stages. You might experience mild tenderness, sensitivity, or discomfort, especially during brushing or flossing, but it's rarely acutely painful. This lack of pain is often why many people don't realize they have it until it's more advanced.
What happens if gingivitis is left untreated?
If left untreated, gingivitis will almost certainly progress to periodontitis. This is a more severe and irreversible form of gum disease where the infection spreads to destroy the bone and ligaments supporting your teeth, leading to gum recession, loose teeth, and eventually tooth loss. It also increases the risk of systemic health issues.
Do I need to see a specialist like a periodontist for gingivitis?
For mild to moderate gingivitis, a general dentist or dental hygienist can effectively treat and manage the condition with professional cleanings and oral hygiene instruction. However, if your gingivitis is severe, unresponsive to initial treatment, or has progressed to mild periodontitis, your dentist may refer you to a periodontist, who specializes in gum disease. This is when you might search for the best periodontist near me.
Can I get gingivitis even if I brush and floss regularly?
While good oral hygiene is the best defense, it is possible. Factors like hormonal changes (pregnancy), certain medications, systemic diseases (diabetes), genetic predisposition, tobacco use, or even poorly aligned teeth that create hard-to-clean areas can still contribute to gingivitis, even with diligent care. However, good hygiene significantly reduces the risk and severity.
What kind of toothpaste and mouthwash should I use for gingivitis?
For toothpaste, any fluoride toothpaste is generally recommended. For mouthwash, your dentist might suggest an antiseptic mouthwash containing ingredients like chlorhexidine gluconate (prescription), cetylpyridinium chloride (CPC), or essential oils. Always consult your dentist for specific recommendations tailored to your needs.
Is it normal for my gums to bleed after I start flossing regularly?
When you first start flossing regularly after a period of neglect, your gums might bleed because they are inflamed due to gingivitis. This is a sign that you need to continue flossing. As you consistently remove plaque, the inflammation will subside, and the bleeding should decrease and eventually stop within a week or two. If bleeding persists, consult your dentist.
Does gingivitis affect overall health?
Yes, absolutely. Untreated gingivitis can progress to periodontitis, which has been linked to a higher risk of various systemic health conditions. These include cardiovascular diseases (heart attack, stroke), diabetes complications, respiratory infections, and even adverse pregnancy outcomes. Oral health is an integral part of overall health.
How often should I get professional dental cleanings to prevent gingivitis?
The American Dental Association (ADA) generally recommends professional dental cleanings and check-ups every six months for most adults. For individuals who are more susceptible to gingivitis or have a history of gum disease, your dentist might advise more frequent visits, such as every three or four months, to maintain optimal gum health.
When to See a Dentist
Recognizing when to seek professional dental care for gingivitis is critical for preventing its progression and maintaining your overall oral health. While regular check-ups are essential for preventative care, certain signs indicate that you should schedule an appointment sooner rather than later.
Routine Care Guidance (Every 6 Months):
- Regular Dental Check-ups: Even if you don't notice any symptoms, routine dental exams and professional cleanings every six months are crucial. They allow your dentist to identify early signs of gingivitis, remove hardened plaque (tartar) that you can't remove at home, and provide preventative advice. This is your first line of defense against gingivitis and other oral health issues.
Clear Warning Signs for Prompt Attention: You should schedule a dental appointment promptly if you experience any of the following symptoms, as they are strong indicators of gingivitis or potentially more advanced gum disease:
- Bleeding Gums: If your gums bleed consistently when you brush, floss, or even eat, it's a primary sign of gum inflammation that needs attention. Healthy gums should not bleed.
- Red, Swollen, or Tender Gums: If your gums appear noticeably redder, puffier, or more swollen than usual, or if they feel tender to the touch.
- Persistent Bad Breath: If you have chronic bad breath that doesn't improve with brushing and flossing, it could be a sign of bacterial accumulation.
- Receding Gums: If your gums appear to be pulling away from your teeth, making your teeth look longer.
- Loose or Shifting Teeth: While more indicative of periodontitis, any changes in tooth stability should be evaluated immediately.
- Pain or Discomfort: Although gingivitis is typically not painful, any persistent pain in your gums or teeth warrants a dental visit.
- Pus Between Teeth and Gums: This is a sign of an active infection and requires immediate professional attention.
Red Flags vs. Emergency Guidance:
- Red Flags (Schedule a prompt, non-emergency appointment): Bleeding gums, persistent swelling, tenderness, bad breath, or slight gum recession typically fall into this category. While not an immediate emergency, these symptoms should not be ignored for more than a few days or a week.
- Emergency (Seek immediate attention): Severe, throbbing pain in your gums or teeth, facial swelling, a fever accompanied by gum pain, or difficulty swallowing could indicate a serious infection (like an abscess) and warrants an emergency dental visit.
Don't wait for pain to develop before seeking treatment. Early detection and intervention are key to successfully getting rid of gingivitis and preventing its progression to more severe, irreversible conditions like periodontitis, which might necessitate the care of a best periodontist near me. Your gums are a window to your overall health, and their well-being is crucial for your entire body.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
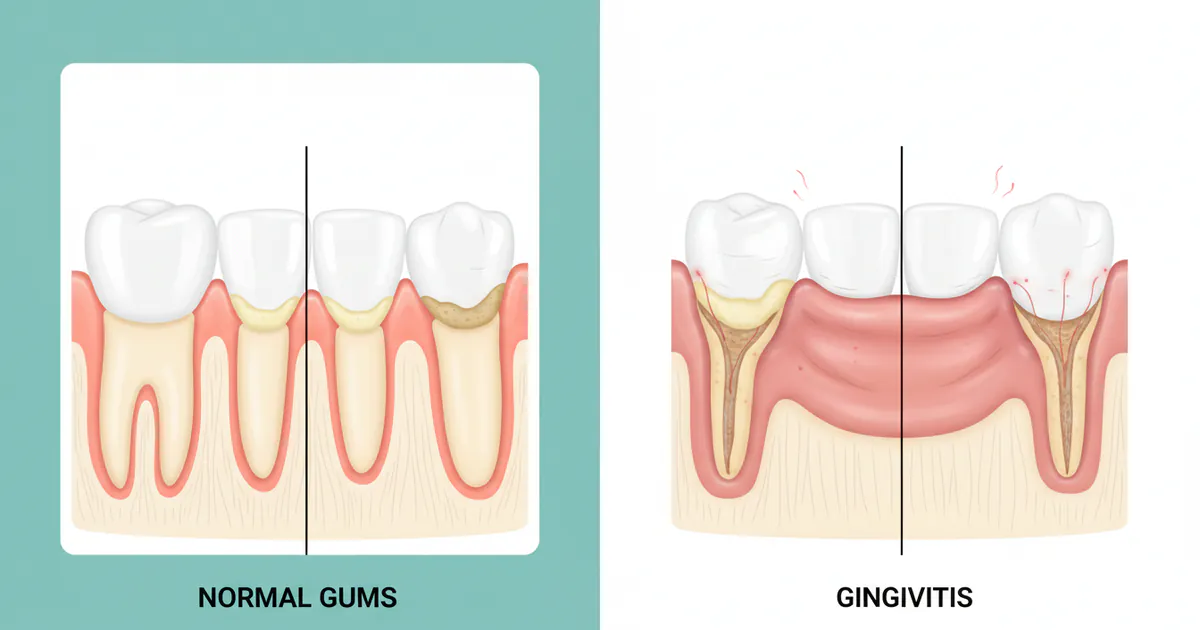
Normal Gums vs Gingivitis: Complete Comparison Guide
Did you know that nearly half of American adults over 30 show signs of gum disease, a condition that can range from mild inflammation to severe infection leading to tooth loss? Understanding the difference between healthy gums and those affected by early gum disease, known as gingivitis, is cruc
February 22, 2026
What Causes Receding Gums
Receding gums, a condition where the gum tissue surrounding the teeth pulls back or wears away, exposing more of the tooth or the tooth's root, affects a significant portion of the adult population in the United States. In fact, estimates suggest that **up to 88% of people over the age of 65 have on
February 22, 2026
Signs of Gingivitis: Complete Guide
Did you know that nearly half of American adults aged 30 and older suffer from some form of gum disease? While that statistic might sound alarming, the good news is that the earliest and most common stage, gingivitis, is entirely reversible. Recognizing the signs of gingivitis early is your
February 22, 2026
Gum Disease Medical Procedure: Complete Guide
Gum Disease Medical Procedure: Complete Guide
February 22, 2026