Complete Guide to Oral Surgery: Everything You Need to Know
Key Takeaways
- Oral surgery, a specialized field within dentistry, addresses a wide array of conditions affecting the mouth, teeth, jaws, and facial structures. Whether you're facing a straightforward tooth extraction or a more complex procedure like wisdom teeth removal, understanding what to expect can s
Oral surgery, a specialized field within dentistry, addresses a wide array of conditions affecting the mouth, teeth, jaws, and facial structures. Whether you're facing a straightforward tooth extraction or a more complex procedure like wisdom teeth removal, understanding what to expect can significantly ease anxieties and lead to better outcomes. In fact, tooth extractions, often performed by an oral surgeon, are among the most common surgical procedures in the United States, with millions occurring annually to preserve overall oral health. This comprehensive guide will demystify oral surgery, offering insights into various procedures, recovery expectations, costs, and how to choose the right oral surgeon near me to ensure your smile remains healthy and strong.
Key Takeaways:
- Oral surgery encompasses diverse procedures, from common wisdom teeth removal and tooth extraction to dental implants and corrective jaw surgery.
- Impacted wisdom teeth are a frequent reason for surgical intervention, often recommended between ages 17-25 to prevent future complications.
- The average cost for a simple tooth extraction ranges from $75-$250, while an impacted wisdom tooth removal can cost $500-$1,100 per tooth without insurance.
- Recovery typically involves 3-7 days of limited activity, with full healing of the normal socket after tooth extraction taking several weeks to months.
- Choosing a board-certified oral surgeon is crucial for complex procedures, ensuring expertise in surgical techniques and anesthesia.
- Diligent aftercare, including avoiding straws and smoking, is essential to prevent complications like dry socket, particularly after wisdom tooth procedures.
What is Oral Surgery?
Oral surgery is a highly specialized branch of dentistry that focuses on diagnosing and surgically treating diseases, injuries, and defects involving the hard and soft tissues of the mouth, jaws, and face. An oral surgeon, also known as an oral and maxillofacial surgeon (OMFS), undergoes extensive additional training—typically four to six years beyond dental school—to gain expertise in advanced surgical techniques, anesthesia administration, and comprehensive patient care.
While general dentists can perform minor surgical procedures like simple tooth extraction, complex cases, such as impacted wisdom teeth removal, intricate bone grafting, or corrective jaw surgery, are best handled by an oral surgeon. Their expanded scope of practice and specialized training ensure that patients receive the highest level of care for intricate oral and facial conditions.
Common Types of Oral Surgery Procedures
Oral surgery addresses a wide spectrum of issues. Here are some of the most frequently performed procedures:
Tooth Extraction
A tooth extraction is the removal of a tooth from its socket in the bone. While permanent teeth are meant to last a lifetime, various circumstances can necessitate their removal.
- Why it's needed:
- Severe decay: When a tooth is extensively damaged by decay beyond repair with a filling or crown.
- Infection: If an infection (abscess) has spread to the pulp of the tooth and is too severe to be treated by root canal therapy.
- Periodontal disease: Advanced gum disease can loosen teeth, making extraction necessary.
- Trauma: A tooth severely fractured or damaged due to an injury.
- Orthodontic treatment: To create space in the mouth for teeth to shift properly during braces.
- Impacted teeth: Teeth that fail to erupt properly, most commonly wisdom teeth.
- Simple vs. Surgical Extraction:
- Simple Extraction: Performed on visible teeth that are above the gum line and easily accessible. The dentist loosens the tooth with an instrument called an elevator and then removes it with forceps.
- Surgical Extraction: Required for teeth that are not easily accessible, such as impacted wisdom teeth, teeth that have broken off at the gum line, or those with complex root structures. This involves an incision into the gum tissue, and sometimes the removal of bone or sectioning of the tooth before it can be extracted.
Wisdom Teeth Removal
The removal of wisdom teeth, or third molars, is one of the most common oral surgical procedures, especially among young adults.
- What are Wisdom Teeth? These are the last set of molars to erupt, typically between the ages of 17 and 25.
- Why They Often Need Removal:
- Impaction: This is the most common reason. Impacted wisdom teeth are those that do not fully erupt through the gum line or grow in at an improper angle due to lack of space. They can be partially or fully impacted. There are several types of impaction:
- Mesial Impaction: The tooth is angled forward, towards the front of the mouth.
- Distal Impaction: The tooth is angled backward, towards the back of the mouth.
- Vertical Impaction: The tooth is upright but trapped within the jawbone.
- Horizontal Impaction: The tooth is lying completely on its side, often pressing into the roots of the second molar.
- Crowding: Even if fully erupted, wisdom teeth can push other teeth out of alignment.
- Pericoronitis: When a wisdom tooth partially erupts, a flap of gum tissue can cover part of the tooth, trapping food and bacteria, leading to infection, pain, and swelling.
- Cysts and Tumors: In rare cases, a cyst or tumor can form around an impacted wisdom tooth, potentially damaging the jawbone and adjacent teeth.
- Decay/Gum Disease: Wisdom teeth are often difficult to clean, making them prone to decay and gum disease, which can then spread to neighboring teeth.
- Impaction: This is the most common reason. Impacted wisdom teeth are those that do not fully erupt through the gum line or grow in at an improper angle due to lack of space. They can be partially or fully impacted. There are several types of impaction:
- Age Considerations: Removal is often recommended in late adolescence or early adulthood when the roots are not fully developed and the surrounding bone is softer, making the procedure easier and recovery faster.
!Illustration showing the different types of wisdom tooth impactions (mesial, distal, vertical, horizontal).
Dental Implants
Dental implants are considered the gold standard for replacing missing teeth. An oral surgeon places a small, titanium post into the jawbone, which acts as an artificial tooth root. After a healing period, a crown, bridge, or denture is attached to the implant.
- Benefits: Restore chewing function, prevent bone loss, maintain facial structure, and provide a stable foundation for prosthetic teeth.
- Process: Involves surgical placement of the implant, followed by osseointegration (bone fusing with the implant), and then restoration by a general dentist or prosthodontist.
Corrective Jaw Surgery (Orthognathic Surgery)
This procedure corrects irregularities of the jaw bones and realigns the jaws and teeth to improve overall function and facial harmony.
- When needed: To address issues like severe overbites, underbites, open bites, crossbites, temporomandibular joint (TMJ) disorders, sleep apnea, or facial asymmetry that cannot be corrected with orthodontics alone.
- Process: Often performed in conjunction with orthodontics, involving precise cuts in the jawbones to reposition them, then secured with plates and screws.
Bone Grafting and Ridge Augmentation
These procedures involve adding bone material to the jaw where bone loss has occurred.
- Purpose: Essential for patients who require dental implants but lack sufficient bone density. It can also be performed to preserve the bone after a tooth extraction (socket preservation) or to prepare the jaw for dentures.
- Materials: Bone can be taken from the patient's own body (autogenous), from a donor (allograft), from animal sources (xenograft), or synthetic materials (alloplast).
Pre-Prosthetic Surgery
These are minor surgical procedures performed to prepare the mouth for the placement of dentures.
- Examples: Removing excess bone, reshaping the jaw ridge, or removing soft tissue obstructions to ensure a comfortable and stable fit for dentures.
Biopsies and Lesion Removal
Oral surgeons diagnose and treat oral pathology, which includes cysts, tumors, and other lesions in the mouth or jaw.
- Process: A biopsy involves removing a small tissue sample for laboratory analysis to determine if it is benign or malignant. If needed, the entire lesion is surgically removed.
Causes and Conditions Leading to Oral Surgery
Several factors can necessitate oral surgical intervention:
- Severe Tooth Decay or Infection: Untreated cavities that penetrate deep into the tooth can lead to abscesses and extensive damage, often requiring tooth extraction or complex root canal surgery.
- Dental Trauma: Accidents, sports injuries, or falls can result in fractured teeth, avulsed (knocked out) teeth, or jaw fractures, all of which may require immediate surgical repair.
- Impacted Teeth: As discussed, impacted wisdom teeth are a primary reason for surgery. Other teeth, like canines, can also become impacted and require surgical exposure to guide them into place orthodontically.
- Missing Teeth: Whether from decay, trauma, or congenital conditions, missing teeth are often restored with dental implants, which require surgical placement.
- Periodontal Disease: Advanced gum disease can destroy the bone supporting teeth, leading to tooth mobility and eventual tooth extraction. Bone grafting may be needed to restore lost bone.
- Temporomandibular Joint (TMJ) Disorders: Severe and chronic TMJ pain or dysfunction that doesn't respond to conservative treatments may necessitate surgical intervention to repair or replace the joint.
- Oral Pathology: The presence of cysts, benign tumors, or malignant lesions (oral cancer) in the soft tissues or jawbone requires surgical removal and often biopsy.
- Congenital Conditions: Birth defects such as cleft lip and palate require a series of reconstructive surgeries, often performed by oral surgeons in conjunction with other specialists.
- Sleep Apnea: In some cases, obstructive sleep apnea caused by jaw abnormalities can be treated with corrective jaw surgery to widen the airway.
Signs and Symptoms Indicating a Need for Oral Surgery
Recognizing the signs that you might need to see an oral surgeon is crucial for timely intervention.
- Persistent Pain: Chronic or severe pain in your teeth, gums, or jaw that doesn't subside with over-the-counter pain relievers. This is a common indicator, especially for an impacted wisdom tooth.
- Swelling, Redness, or Pus: These are classic signs of infection (pericoronitis, abscess) around a tooth, particularly the back of the jaw where wisdom teeth are located.
- Difficulty Opening Mouth or Chewing: Limited jaw movement (trismus) or pain while chewing can indicate an underlying issue with a tooth, jaw joint, or muscle.
- Bad Breath or Unpleasant Taste: Persistent bad breath (halitosis) or a foul taste in your mouth, especially near a wisdom tooth, could signal an infection or trapped food.
- Loose Teeth: While some tooth mobility is normal, significant looseness beyond what's expected for baby teeth can indicate advanced gum disease or trauma.
- Changes in Bite: If your teeth no longer fit together properly, it could be a sign of shifting teeth, a jaw issue, or the emergence of wisdom teeth.
- Bleeding Gums: While often a sign of gum disease, persistent or excessive bleeding, especially around a partially erupted wisdom tooth, warrants evaluation.
- Visible Lesions or Lumps: Any unusual growths, sores that don't heal, or white/red patches in your mouth should be checked by a professional for oral pathology.
- Facial Trauma: Any injury to the face or jaw, including fractures, requires immediate assessment by an oral surgeon.
The Oral Surgery Process: What to Expect
Undergoing oral surgery can seem daunting, but understanding the step-by-step process can help alleviate concerns.
Initial Consultation and Diagnosis
Your journey begins with a thorough examination by an oral surgeon.
- Medical History Review: The surgeon will review your complete medical history, including any medications, allergies, and existing health conditions, to ensure your safety during and after the procedure.
- Clinical Examination: A detailed inspection of your mouth, teeth, gums, and jaw will be performed.
- Diagnostic Imaging: X-rays are essential. This often includes panoramic X-rays (showing the entire jaw and all teeth) and sometimes 3D cone-beam computed tomography (CBCT) scans for complex cases like impacted wisdom teeth or implant planning. These images allow the surgeon to assess tooth position, bone structure, nerve pathways, and potential pathology.
- Treatment Planning: Based on the examination and imaging, the oral surgeon will discuss the diagnosis, recommended treatment plan, alternative options, and potential risks and benefits. You'll have the opportunity to ask questions.
Pre-Operative Instructions
Once a treatment plan is established, you'll receive specific instructions to prepare for your surgery.
- Medications: You may be advised to stop certain medications (e.g., blood thinners) or start antibiotics.
- Fasting: For procedures requiring IV sedation or general anesthesia, you'll typically need to fast (no food or drink) for 6-8 hours prior.
- Transportation: Arrange for a responsible adult to drive you home after surgery if you're receiving sedation or general anesthesia.
- Comfort: Wear loose, comfortable clothing and avoid makeup or jewelry.
Anesthesia Options
Oral surgeons are highly trained in administering various types of anesthesia to ensure your comfort during the procedure.
- Local Anesthesia"): Numbness of the surgical area while you remain fully awake. Often used for simple tooth extraction.
- Nitrous Oxide (Laughing Gas): Mild sedative inhaled through a mask, providing a sense of relaxation. Wears off quickly.
- IV Sedation (Conscious Sedation): Administered intravenously, putting you into a deeply relaxed, "twilight sleep" state where you are unlikely to remember the procedure. You will still be able to respond to commands.
- General Anesthesia: You are completely unconscious during the procedure. Typically reserved for very complex cases, fearful patients, or specific medical conditions, and usually administered in a hospital or accredited surgical center.
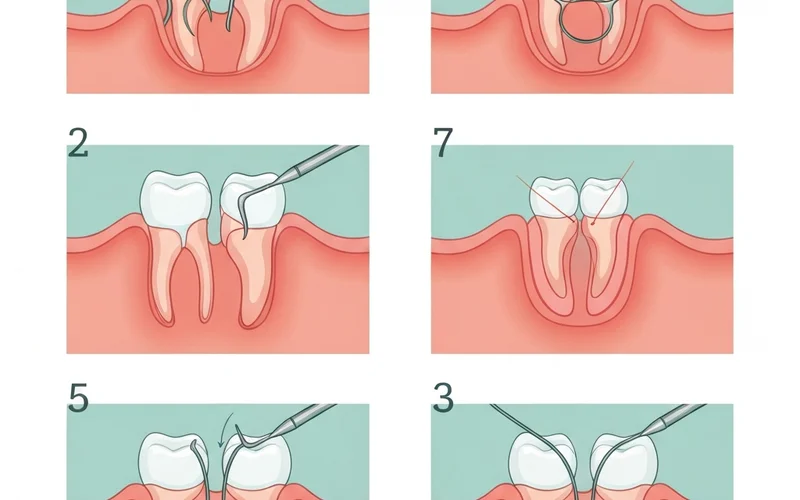
The Surgical Procedure (Step-by-Step Example: Wisdom Tooth Removal)
Let's walk through a typical wisdom teeth removal procedure for an impacted wisdom tooth:
- Anesthesia Administration: The oral surgeon or anesthesiologist will administer the chosen anesthesia (e.g., IV sedation and local anesthesia). You'll quickly become relaxed and comfortable.
- Incision (if needed): For an impacted wisdom tooth, the surgeon may make a small incision in the gum tissue to expose the tooth and surrounding bone.
- Bone Removal (if needed): If the tooth is covered by bone (as in many impacted wisdom teeth), a small amount of bone may be carefully removed using a surgical drill to access the tooth.
- Tooth Sectioning (if needed): To minimize the amount of bone removed and make extraction easier, especially for complex or impacted wisdom teeth, the surgeon may divide the tooth into smaller pieces.
- Extraction: The tooth or its sections are gently removed using specialized instruments.
- Debridement and Irrigation: The socket is cleaned of any tooth fragments or debris, and thoroughly irrigated with saline to ensure it is clean.
- Sutures: The gum tissue is typically closed with sutures (stitches), which may be dissolvable or require removal at a follow-up appointment. Gauze is placed over the extraction site to control bleeding.
!Detailed step-by-step illustration of a surgical wisdom tooth extraction, showing gum incision, bone removal, tooth sectioning, and suturing.
Immediate Post-Operative Care
After the procedure, you'll rest in a recovery area while the anesthesia wears off. The oral surgeon or nurse will provide detailed post-operative instructions and ensure you're stable before you are discharged with your escort.
Cost of Oral Surgery in the US and Insurance Coverage
Understanding the financial aspect of oral surgery is a critical part of preparation. Costs can vary significantly based on the procedure's complexity, anesthesia used, geographic location, and the oral surgeon's fees.
Factors Influencing Cost
- Type and Complexity of Procedure: A simple tooth extraction is far less expensive than a multi-stage dental implant placement or corrective jaw surgery. The difficulty of removing an impacted wisdom tooth heavily influences its cost.
- Number of Teeth/Sites: The cost increases with the number of teeth extracted or implants placed.
- Anesthesia Used: Local anesthesia is typically included, but IV sedation or general anesthesia will add to the overall cost, ranging from $300-$1,000+.
- Geographic Location: Costs tend to be higher in metropolitan areas and on the coasts compared to rural areas or the Midwest.
- Surgeon's Fees: Highly experienced or board-certified oral surgeons may have higher fees.
- Diagnostic Imaging: X-rays and 3D scans are separate costs, typically $50-$300.
- Prescription Medications: Post-operative pain medication and antibiotics are an additional expense.

Average Cost Ranges by Procedure (Without Insurance)
These are general ranges and can fluctuate. It's always best to get a detailed estimate from your oral surgeon.
- Simple Tooth Extraction: $75 - $250 per tooth
- Surgical Tooth Extraction (non-impacted): $150 - $650 per tooth
- Wisdom Teeth Removal (Erupted/Soft Tissue Impaction): $200 - $750 per tooth
- Impacted Wisdom Teeth Removal (Bony Impaction): $500 - $1,100 per tooth
- Dental Implant Placement (surgical component only): $1,500 - $3,000 per implant (does not include the crown/abutment, which adds another $1,000-$2,500)
- Bone Grafting (minor, e.g., socket preservation): $300 - $1,000
- Corrective Jaw Surgery: $20,000 - $50,000+ (can be covered by medical insurance)
Insurance Coverage
- Dental Insurance: Most dental insurance plans cover a portion of oral surgery procedures, especially medically necessary extractions like wisdom teeth removal. Coverage usually falls under "major restorative" services, meaning the plan may cover 50-80% after you meet your deductible, up to your annual maximum (often $1,000-$2,000).
- Medical Insurance: For more extensive procedures like corrective jaw surgery, treatment of facial trauma, or pathology removal, your medical insurance may provide significant coverage, especially if the condition affects your overall health or quality of life. Be sure to check with both dental and medical insurance providers.
- Pre-Authorization: It is highly recommended to get a pre-authorization or pre-determination from your insurance company before scheduling surgery to understand your exact out-of-pocket costs.
Payment Plans and Financial Aid
Many oral surgery practices offer financing options to make treatment more affordable.
- CareCredit and LendingClub: Third-party medical financing companies that offer deferred interest or low-interest payment plans.
- In-House Payment Plans: Some offices may offer their own payment arrangements.
- Dental Schools: University dental schools often provide services at a reduced cost, as procedures are performed by residents under the supervision of experienced faculty.
Table 1: Estimated Oral Surgery Costs in the US (Without Insurance)
| Procedure | Low End | High End | Notes |
|---|---|---|---|
| Simple Tooth Extraction | $75 | $250 | Per tooth, visible, non-surgical |
| Surgical Tooth Extraction | $150 | $650 | Per tooth, broken below gum line or requiring incision |
| Erupted Wisdom Tooth Removal | $200 | $750 | Per tooth, fully erupted or soft tissue impaction |
| Impacted Wisdom Tooth Removal (Bony) | $500 | $1,100 | Per tooth, requiring bone removal or sectioning |
| Minor Bone Grafting (Socket Preserve) | $300 | $1,000 | To maintain bone volume after extraction |
| Single Dental Implant (Surgical Part) | $1,500 | $3,000 | Does not include abutment and crown (add $1,000-$2,500) |
| IV Sedation (Anesthesia Fee) | $300 | $1,000+ | Per hour, depending on duration and complexity |
Recovery and Aftercare: Ensuring a Smooth Healing Process
Proper recovery and diligent aftercare are paramount for preventing complications and ensuring a successful outcome from any oral surgery, especially following a tooth extraction or wisdom teeth removal.
Immediate Post-Op (First 24-48 hours)
This period is critical for initial healing and managing discomfort.
- Bleeding Control: Bite down firmly on the gauze pads placed by your oral surgeon for 30-60 minutes, then replace if still bleeding. A small amount of oozing for the first 24 hours is normal.
- Pain Management: Take prescribed pain medication as directed, usually starting before the local anesthesia wears off. Over-the-counter options like ibuprofen or acetaminophen can supplement or substitute.
- Swelling Reduction: Apply ice packs to the outside of your face (15-20 minutes on, 15-20 minutes off) for the first 24-48 hours to minimize swelling. Swelling usually peaks on day 2 or 3.
- Rest: Avoid strenuous activity for at least 24-48 hours. Elevate your head with pillows when lying down.
- Diet: Stick to soft foods and liquids (e.g., yogurt, mashed potatoes, soup, smoothies) that don't require chewing. Avoid hot liquids.
- Hydration: Drink plenty of fluids, but DO NOT use a straw, as the sucking motion can dislodge the blood clot and lead to a dry socket.
- Oral Hygiene: DO NOT rinse, spit vigorously, or brush directly near the surgical site for the first 24 hours. This helps the blood clot form.
Days 3-7
You should start to feel better, but continue to be cautious.
- Diet Progression: Gradually introduce semi-soft foods as tolerated.
- Gentle Rinsing: Begin gently rinsing your mouth with warm salt water (1/2 teaspoon salt in 8 ounces of warm water) 2-3 times a day, especially after meals. This helps keep the surgical site clean.
- Brushing: Brush your teeth gently, avoiding the surgical area initially. You can carefully brush adjacent teeth.
- Activity: You can gradually return to light activities, but avoid heavy lifting or intense exercise for at least a week, or as advised by your oral surgeon.
- Normal Socket After Tooth Extraction: Begin to observe the healing site. A normal socket after tooth extraction will typically be covered by a dark red blood clot, which will gradually be replaced by new gum tissue. It should not be visibly empty bone.
Weeks 1-2 and Beyond
- Suture Removal: If non-dissolving sutures were used, you'll have a follow-up appointment, typically around 7-10 days, to have them removed.
- Full Healing: While initial recovery for a tooth extraction may take a week or two, the bone and gum tissue will continue to remodel for several months. For a normal socket after tooth extraction, it typically takes 6-8 weeks for the soft tissue to fully cover the site, and 3-6 months for complete bone fill.
Preventing Complications: Dry Socket (Alveolar Osteitis)
Dry socket is the most common complication after tooth extraction, particularly wisdom teeth removal.
- What it is: Occurs when the blood clot that forms in the extraction socket either dislodges or dissolves prematurely, exposing the underlying bone and nerves. This leads to intense pain, often radiating to the ear, and a foul odor or taste. It typically develops 3-5 days after surgery.
- Prevention:
- Avoid straws: The suction can dislodge the clot.
- No smoking or vaping: Nicotine constricts blood vessels, impairing healing, and the sucking motion can dislodge the clot.
- Avoid vigorous rinsing or spitting.
- Follow all post-operative instructions meticulously.
- Treatment: If you suspect dry socket, contact your oral surgeon immediately. They will clean the socket, place a medicated dressing, and prescribe pain relief.
Pro Tip: Always follow your oral surgeon's specific instructions meticulously to ensure optimal healing and prevent complications like dry socket, especially after wisdom teeth removal.
!Infographic illustrating proper post-extraction care: avoiding straws, soft foods, gentle rinsing, cold compress.
Risks and Potential Complications of Oral Surgery
While oral surgery is generally safe, as with any surgical procedure, there are potential risks and complications. Your oral surgeon will discuss these with you before your procedure.
- Infection: Although antibiotics are often prescribed, any surgical site can become infected. Signs include increased pain, swelling, redness, fever, or pus.
- Dry Socket (Alveolar Osteitis): As detailed above, this painful condition results from the premature loss of the blood clot from the extraction socket. It is more common after wisdom teeth removal.
- Nerve Damage (Paresthesia): This is a rare but serious complication, particularly with lower wisdom teeth removal. Nerves close to the surgical area (inferior alveolar nerve, lingual nerve) can be bruised or damaged, leading to temporary or, in very rare cases, permanent numbness, tingling, or altered sensation in the lip, chin, tongue, or gums.
- Excessive Bleeding: While some oozing is normal, prolonged or heavy bleeding needs immediate attention.
- Sinus Perforation: For extractions of upper back teeth, especially if the roots are close to the maxillary sinus, a small opening can occur between the mouth and the sinus. This usually heals spontaneously but may require additional treatment.
- Jaw Fracture: Extremely rare, but the jawbone can fracture during a very difficult tooth extraction or if the bone is thin or weakened.
- Damage to Adjacent Teeth or Restorations: Instruments used during surgery can potentially chip or dislodge existing fillings or crowns on neighboring teeth.
- Anesthesia Complications: Though rare with modern anesthesia, risks include allergic reactions, respiratory issues, or adverse drug interactions. Your oral surgeon will review your medical history thoroughly to minimize these risks.
- TMJ Issues: Jaw stiffness or pain in the temporomandibular joint can occur due to keeping the mouth open for an extended period during surgery.
- Trismus: Difficulty opening the mouth fully due to muscle spasms or swelling, which usually resolves within a few days or weeks.
Prevention: Minimizing the Need for Oral Surgery
While some oral surgery procedures are unavoidable (e.g., genetic predisposition for impacted wisdom teeth), many can be prevented through proactive oral care and early intervention.
- Excellent Oral Hygiene: Regular brushing (twice a day for two minutes) and daily flossing effectively remove plaque and food debris, preventing cavities and gum disease, the leading causes of tooth extraction.
- Routine Dental Check-ups and Cleanings: Visiting your general dentist every six months allows for early detection and treatment of issues before they become severe enough to require surgery. X-rays can identify problems like impacted wisdom teeth or developing cysts.
- Balanced Diet: Limiting sugary foods and drinks reduces the risk of tooth decay.
- Protective Gear: Wearing a mouthguard during sports activities can prevent dental trauma, saving teeth from fracture or avulsion.
- Prompt Treatment of Dental Problems: Don't delay treatment for cavities or gum inflammation. Addressing issues like a small cavity with a filling is much less invasive and costly than waiting until it requires a root canal or tooth extraction.
- Monitoring Wisdom Teeth: Regular dental visits allow your dentist to monitor the development of your wisdom teeth. If impaction is likely, early intervention (proactive wisdom teeth removal) can prevent more serious complications down the line.
- Quit Smoking/Tobacco Use: Smoking significantly increases the risk of gum disease, oral cancer, and impairs healing after surgery.
Children and Pediatric Oral Surgery Considerations
Oral surgery in children requires a specialized approach, focusing on growth and development, as well as managing anxiety. Pediatric oral surgeons or general dentists trained in pediatric procedures are best suited for these cases.
- Primary Tooth Extractions: Baby teeth may need to be extracted due to severe decay, infection, or trauma. They might also be removed to make space for permanent teeth or if they fail to fall out naturally, blocking the eruption of permanent teeth.
- Frenectomy: A frenectomy is a procedure to remove or modify a frenum (a small fold of tissue), most commonly the lingual frenum (tongue-tie) or labial frenum (connecting lip to gum). This can improve speech, feeding, or prevent orthodontic problems.
- Exposure of Impacted Canines: Permanent canine teeth can sometimes become impacted (trapped) in the jawbone. An oral surgeon may expose the tooth and bond an orthodontic bracket to it to help guide it into its proper position.
- Monitoring Wisdom Teeth: Dentists begin monitoring the development of wisdom teeth in adolescents, often around age 12-14, using panoramic X-rays. This allows for proactive planning if wisdom teeth removal is anticipated.
- Space Maintainers: After premature tooth extraction of a baby tooth, a space maintainer may be placed to hold the space open for the permanent tooth, preventing neighboring teeth from drifting.
- Anxiety Management: Children often experience anxiety about dental procedures. Pediatric oral surgeons are skilled in various techniques, including local anesthesia, nitrous oxide, and even IV sedation, to ensure the child's comfort and safety during surgery. Parents play a vital role in preparing their child and following pre- and post-operative instructions.
Cost Breakdown (Detailed)
Delving deeper into the financial aspects, a full cost breakdown helps in planning for oral surgery.
Average US Costs (Low, Mid, High)
These figures represent national averages and can fluctuate based on the factors mentioned previously.
- Simple Tooth Extraction: $75 (low) - $150 (mid) - $250 (high) per tooth
- Surgical Tooth Extraction: $150 (low) - $350 (mid) - $650 (high) per tooth
- Erupted/Soft Tissue Impacted Wisdom Tooth Removal: $200 (low) - $450 (mid) - $750 (high) per tooth
- Bony Impacted Wisdom Tooth Removal: $500 (low) - $800 (mid) - $1,100 (high) per tooth
- Single Dental Implant (Surgical Placement Only): $1,500 (low) - $2,200 (mid) - $3,000 (high) per implant
- Full Arch Dental Implants (All-on-4/6 concept): $15,000 - $30,000 per arch (mid), up to $50,000+ per arch (high, depending on materials and complexity). This is a comprehensive solution replacing all teeth in an arch.
- Bone Grafting (moderate): $500 - $2,000
- Anesthesia (IV Sedation): $300 (per hour, low) - $600 (per hour, mid) - $1,000+ (per hour, high)
With vs. Without Insurance
- Without Insurance: You are responsible for 100% of the cost. Prices may be slightly negotiable, especially if paying in cash upfront.
- With Insurance: Dental insurance typically covers a portion of medically necessary oral surgery.
- Deductibles: You'll pay an initial amount (e.g., $50-$150) out-of-pocket before your insurance starts to cover costs.
- Co-pays/Coinsurance: After meeting your deductible, your insurance might cover 50-80% of "major" procedures, meaning you're responsible for the remaining 20-50%. For example, if a wisdom tooth removal costs $800 and your insurance covers 80%, you'd pay $160 (plus deductible).
- Annual Maximums: Most dental plans have an annual limit (e.g., $1,000-$2,000). Once this limit is reached, you pay 100% of further costs for that year. For extensive procedures like multiple impacted wisdom teeth removal, you might exceed this maximum.
Payment Plans and Financing Options
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): These tax-advantaged accounts allow you to set aside pre-tax money for healthcare expenses, including oral surgery.
- Credit Cards: Standard credit cards can be used, but be mindful of interest rates.
- CareCredit/LendingClub: These specialized healthcare credit cards offer promotional financing options, often with 0% interest for a certain period if the balance is paid in full.
- In-House Payment Plans: Some oral surgeon offices offer flexible payment schedules directly, often requiring an initial down payment.
Cost-Saving Tips
- Get Multiple Estimates: If time permits, consult with a few different oral surgeons to compare costs and treatment plans.
- Utilize Your Insurance Maximally: Understand your plan's benefits, deductibles, and annual maximums. If you need extensive work, consider phasing treatments across two calendar years to take advantage of two annual maximums.
- Ask About Cash Discounts: Many practices offer a discount (e.g., 5-10%) for patients paying in full at the time of service with cash.
- Dental Schools: As mentioned, university dental schools can be a more affordable option for high-quality care, performed by supervised residents.
- Community Health Centers: Some non-profit clinics offer services on a sliding scale based on income.
Table 2: Regional Cost Variation for Impacted Wisdom Tooth Removal (Per Tooth)
| Region | Low Complexity (Soft Tissue) | High Complexity (Bony) |
|---|---|---|
| Midwest (e.g., OH, MO) | $350 - $650 | $600 - $900 |
| South (e.g., GA, TX) | $300 - $600 | $550 - $850 |
| Northeast (e.g., NY, MA) | $450 - $750 | $750 - $1,100 |
| West (e.g., CA, WA) | $400 - $700 | $700 - $1,050 |
| Florida | $300 - $600 | $500 - $850 |
Note: These ranges are approximate and subject to change. They do not include anesthesia fees beyond local anesthesia.
Frequently Asked Questions
How long does recovery from wisdom teeth removal take?
Initial recovery for wisdom teeth removal typically takes about 3-7 days, during which you should avoid strenuous activity and stick to soft foods. Full healing of the bone and gum tissue inside the normal socket after tooth extraction can take several weeks to a few months. Most people return to normal routines within a week.
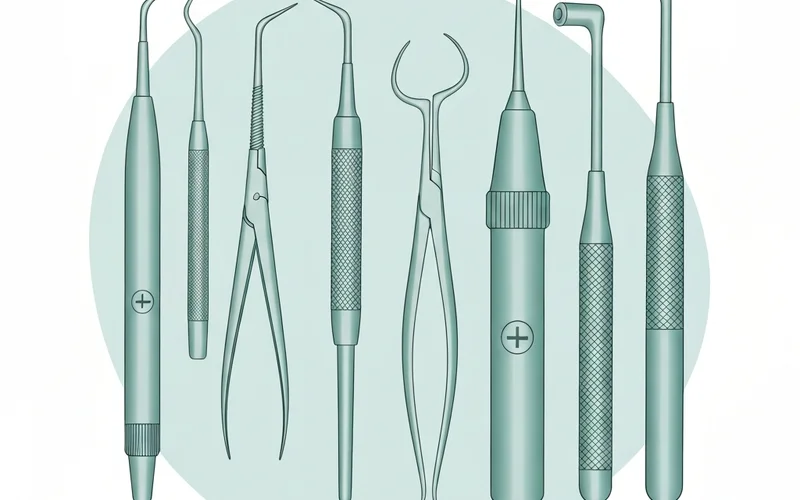
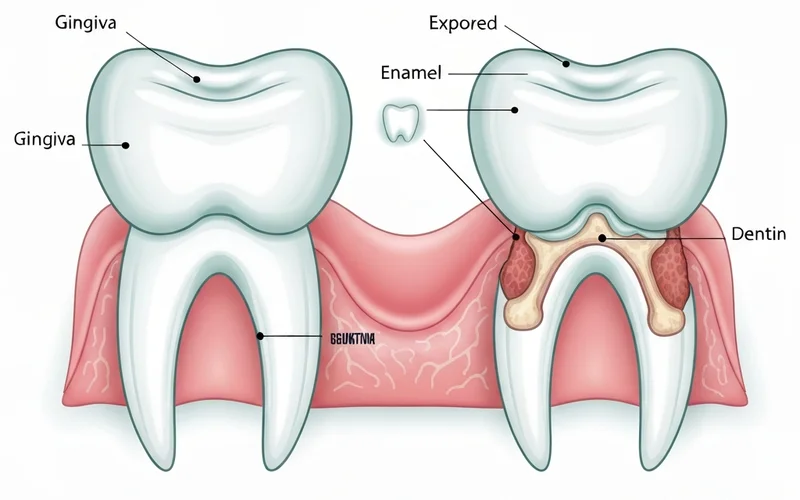
What is a normal socket after tooth extraction supposed to look like?
Immediately after a tooth extraction, the socket will contain a dark red blood clot. This clot is vital for healing. Over the next few days, it will gradually be replaced by granulation tissue, and then new gum tissue will grow over the site. A normal socket after tooth extraction should appear dark and slightly concave, not empty or exposing bone.
How much does it cost to get a wisdom tooth pulled?
The cost to get a wisdom tooth pulled varies widely, from $200-$750 for an erupted or soft-tissue impacted tooth to $500-$1,100 per tooth for a complex, bony impacted wisdom tooth removal. These prices are without insurance and do not include anesthesia costs beyond local anesthetic.
Is oral surgery painful?
With modern anesthesia techniques, you should not feel pain during oral surgery. Your oral surgeon will ensure you are adequately numbed or sedated. Post-operative pain is managed with prescribed medications, which effectively control discomfort during the initial recovery period.
Can I avoid wisdom teeth removal if my wisdom teeth aren't bothering me?
Not necessarily. Even if your wisdom teeth aren't currently causing pain, they can still lead to problems like impaction, damage to adjacent teeth, crowding, or infection. Your oral surgeon will evaluate your X-rays and recommend removal if there's a high risk of future complications.
What's the difference between a dentist and an oral surgeon?
A general dentist is trained to diagnose and treat common dental problems and perform routine procedures. An oral surgeon (oral and maxillofacial surgeon) is a dentist who has completed an additional 4-6 years of specialized surgical training, focusing on complex extractions (like impacted wisdom teeth), jaw surgery, implants, and facial trauma.
What are the risks of leaving impacted wisdom teeth untreated?
Leaving impacted wisdom teeth untreated can lead to severe issues including infection (pericoronitis), damage to adjacent molars (decay or root resorption), cyst or tumor formation, and orthodontic problems due to crowding. Regular dental check-ups are key to monitoring them.
How do I choose the best oral surgeon near me?
Look for an oral surgeon who is board-certified by the American Board of Oral and Maxillofacial Surgery. Ask for recommendations from your general dentist. Check online reviews and consider their experience with your specific procedure, anesthesia options, and the clarity of their communication regarding treatment plans and costs.
What should I eat after tooth extraction?
Immediately after a tooth extraction, stick to soft, cool foods like yogurt, applesauce, mashed potatoes, and lukewarm soup. Avoid anything hot, crunchy, sticky, or requiring heavy chewing for at least 24-48 hours. Gradually reintroduce normal foods as comfort allows.
When can I go back to work after oral surgery?
For a simple tooth extraction, you might return to work the next day. For more extensive procedures like wisdom teeth removal with sedation, most people take 2-3 days off, and sometimes up to a full week, depending on the number of teeth removed, complexity, and type of anesthesia used.
When to See a Dentist or Oral Surgeon
Knowing when to seek professional help is vital for maintaining your oral health and preventing minor issues from escalating into major ones requiring extensive oral surgery.
- Routine Care: Regular dental check-ups (every six months) are essential for preventative care. Your general dentist can monitor the development of your wisdom teeth, detect early signs of decay, and identify any issues that might eventually require an oral surgeon's expertise.
- Persistent Pain or Discomfort: If you experience ongoing toothache, jaw pain, or discomfort that doesn't resolve after a day or two, particularly around your back molars or an impacted wisdom tooth, schedule an appointment promptly.
- Swelling or Redness: Any unexplained swelling in your face, jaw, or gums, especially if accompanied by redness or warmth, could indicate an infection. This warrants immediate attention from either your dentist or an oral surgeon.
- Difficulty Chewing or Opening Mouth: If you suddenly find it hard to chew food, or if your jaw feels stiff and you can't open your mouth fully (trismus), it could be a sign of a dental infection or a problem with your jaw joint.
- Visible Oral Abnormalities: Any new lumps, bumps, sores that don't heal within two weeks, or unusual white/red patches in your mouth should be evaluated by a dentist or oral surgeon to rule out oral pathology.
- Red Flags (Emergency Situations): Seek immediate attention if you experience:
- Excessive, uncontrollable bleeding from the mouth.
- Sudden, severe swelling that impedes breathing or swallowing.
- Trauma to the face or jaw resulting in fractured bones or knocked-out teeth.
- High fever accompanied by oral pain or swelling.
- Signs of dry socket (intense, throbbing pain several days after tooth extraction, foul odor/taste, visible empty socket).
Your general dentist is often the first point of contact. If they determine your condition requires specialized surgical care, they will provide a referral to a qualified oral surgeon. Don't hesitate to reach out to a professional if you have any concerns about your oral health.
!Diagram of a healthy tooth socket vs. a dry socket, highlighting the exposed bone in dry socket.
!Visual representation of various oral surgery instruments, such as elevators, forceps, and surgical drills.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Oral Surgery: Complete Guide
More than 178 million Americans are missing at least one tooth, and millions more experience jaw pain, impacted wisdom teeth, or facial trauma annually. These common issues often lead to a specialized area of dentistry: oral surgery. Far from being a last resort, oral surgery encompasses a wide
February 22, 2026
When Do Wisdom Teeth Come in
When do wisdom teeth come in? It's a question many young adults ponder as they approach their late teens and early twenties, often accompanied by a mix of curiosity and apprehension. These late-arriving molars, officially known as third molars, represent a significant developmental milestone in your
February 22, 2026
Wisdom Tooth Removal: Complete Guide
Wisdom tooth removal is one of the most common oral surgical procedures performed in the United States, affecting millions of individuals annually. For many, the emergence of wisdom teeth, or third molars, can herald a range of uncomfortable and potentially serious dental issues, making their extrac
February 22, 2026
Wisdom Teeth Removal Cost: Complete Price Guide 2026
For many young adults, the emergence of wisdom teeth – the third molars – is an inevitable rite of passage, often accompanied by discomfort and, eventually, a trip to the oral surgeon. In fact, approximately 85% of people will require wisdom teeth removal at some point in their lives, making it
February 22, 2026