When Do Wisdom Teeth Come in
Key Takeaways
- When do wisdom teeth come in? It's a question many young adults ponder as they approach their late teens and early twenties, often accompanied by a mix of curiosity and apprehension. These late-arriving molars, officially known as third molars, represent a significant developmental milestone in your
When do wisdom teeth come in? It's a question many young adults ponder as they approach their late teens and early twenties, often accompanied by a mix of curiosity and apprehension. These late-arriving molars, officially known as third molars, represent a significant developmental milestone in your oral health journey. For some, their arrival is uneventful, but for many, it signals the potential for discomfort, complications, and the eventual need for extraction. Understanding the typical timeline, potential issues like impaction, and the critical importance of proper dental evaluation can save you from pain, infection, and more serious oral health problems down the line. This comprehensive guide will walk you through everything you need to know about when wisdom teeth come in, from their normal eruption patterns to the intricacies of extraction, recovery, and what to do if you encounter common complications like dry socket wisdom teeth. We'll also delve into the financial aspects, including the potential for a $99 tooth extraction, helping you navigate your options with confidence.
Key Takeaways:
- Typical Eruption: Wisdom teeth generally emerge between the ages of 17 and 25, though this can vary significantly.
- Impaction is Common: Up to 70% of individuals experience at least one impacted wisdom tooth, meaning it doesn't fully erupt.
- Extraction Costs: Simple extractions range from $75-$250 per tooth, while surgical extractions for impacted teeth can cost $200-$600 per tooth, often totaling $600-$3,000+ for all four.
- Dry Socket Risk: A common complication after extraction, especially for lower wisdom teeth, characterized by intense pain and delayed healing. It's preventable with proper aftercare.
- Early Evaluation is Key: Regular dental check-ups, particularly in late adolescence, allow dentists to monitor wisdom tooth development and recommend timely intervention.
- "$99 Tooth Extraction" Caveat: While some clinics advertise this, it typically applies only to simple, fully erupted extractions and rarely to impacted wisdom teeth, which require more complex surgical procedures.
What It Is: Understanding Your Wisdom Teeth
Wisdom teeth are the third and final set of molars to erupt, located at the very back of your mouth. They are technically known as "third molars" and most people develop four of them – two in the upper jaw and two in the lower jaw. Their colloquial name, "wisdom teeth," is attributed to the fact that they typically emerge much later than other teeth, at an age when individuals are supposedly wiser.
Historically, these molars played a crucial role for our ancestors, providing extra chewing power needed to process a coarser, more abrasive diet. However, over generations, the human diet has softened, and jaw sizes have progressively reduced. As a result, many modern mouths simply don't have enough room to accommodate these late arrivals, leading to a host of common problems.
When Do Wisdom Teeth Come In? The Typical Timeline
The most common period for wisdom teeth to make their appearance is between the ages of 17 and 25. However, it's not uncommon for them to emerge earlier or later, or even not at all. Some individuals may experience partial eruption, where the tooth only breaks through the gum surface, while others may have completely impacted wisdom teeth that remain fully embedded within the jawbone.
The eruption process can be gradual, often taking several months or even years for a single tooth to fully emerge. During this time, you might experience intermittent discomfort, swelling, or tenderness in the back of your mouth as the tooth pushes through the gum tissue.
Types of Wisdom Teeth Eruption and Impaction
Not all wisdom teeth erupt in the same way, and understanding the different types of eruption and impaction is crucial for determining potential problems and necessary interventions.
Fully Erupted Wisdom Teeth
These are teeth that have completely emerged through the gum line and have sufficient space to align properly with the other molars. They are often functional and easy to clean, posing minimal risk. However, even fully erupted wisdom teeth can sometimes be problematic if they are difficult to reach for proper brushing and flossing, making them susceptible to cavities and gum disease.
Partially Erupted Wisdom Teeth
A partially erupted wisdom tooth has only managed to break through the gum tissue partially, leaving a flap of gum (operculum) covering part of its crown. This scenario is particularly problematic because the flap can trap food particles and bacteria, creating an ideal breeding ground for infection, known as pericoronitis. These teeth are often symptomatic, causing pain, swelling, and bad breath.
Impacted Wisdom Teeth
An impacted wisdom tooth is one that is unable to fully erupt into the mouth due to a physical barrier, such as another tooth, bone, or soft tissue. Impacted teeth are very common, affecting a significant portion of the population. The classification of impaction is based on the tooth's angle and depth within the jawbone:
- Mesial (Angled Forward) Impaction: The tooth is angled forward towards the front of the mouth. This is the most common type of impaction.
- Vertical Impaction: The tooth is oriented correctly but is "stuck" against the tooth in front or under the bone, unable to erupt further.
- Distal (Angled Backward) Impaction: The tooth is angled backward towards the rear of the mouth. This is less common.
- Horizontal Impaction: The tooth is lying completely on its side, often pushing against the roots of the second molar. This is one of the most problematic types.
- Soft Tissue Impaction: The tooth has erupted through the bone but is still covered by gum tissue, often leading to pericoronitis.
- Bony Impaction: The tooth is still encased partially or completely within the jawbone, requiring surgical removal of bone to access it. This can be further categorized as partial or full bony impaction.
Absence of Wisdom Teeth (Agenesis)
It's also worth noting that some individuals never develop one or more wisdom teeth. This is a genetic trait and is becoming increasingly common due to evolutionary changes in human jaw structure. An X-ray will confirm the absence of these teeth.
Supernumerary Wisdom Teeth
Rarely, some individuals may develop more than the typical four wisdom teeth, known as supernumerary teeth. These extra teeth can also cause crowding and impaction issues.
Causes: Why Wisdom Teeth Become Problematic
The primary reason why wisdom teeth often cause problems boils down to a mismatch between the size of our jaws and the number and size of our teeth.
- Evolutionary Jaw Reduction: As humans evolved, our diets became softer, reducing the need for strong, large jaws. Consequently, our jaws have become smaller over thousands of years.
- Lack of Space: Many people simply don't have enough room in their dental arches to accommodate the wisdom teeth when they finally erupt. This crowding pushes other teeth out of alignment or prevents the wisdom teeth from emerging properly.
- Genetic Predisposition: Genetics play a significant role in jaw size, tooth size, and the timing of eruption. If your parents had problematic wisdom teeth, you might too.
- Angle of Eruption: Due to the limited space, wisdom teeth can emerge at various angles, leading to the impaction types described above. They might push against adjacent teeth, bone, or even grow into the jawbone itself.
- Delayed Eruption: Sometimes, wisdom teeth may attempt to erupt very slowly or get stuck along the way, increasing the risk of infection and cyst formation around the developing tooth.
Signs and Symptoms: When to Suspect a Problem
While some wisdom teeth can erupt without any noticeable symptoms, many will signal their problematic arrival with a range of discomforts. Recognizing these signs early can help you seek timely dental care.
- Pain: This is the most common symptom. It can be a dull ache, a throbbing pain, or sharp, intermittent pain localized to the back of the mouth, jaw, or even radiating to the ear or temple.
- Swelling and Tenderness: The gums around the erupting or impacted wisdom tooth may become swollen, red, and tender to the touch.
- Pericoronitis: This is an infection of the gum tissue surrounding a partially erupted wisdom tooth. Symptoms include severe pain, swelling, pus discharge, a bad taste in the mouth, and difficulty chewing or swallowing.
- Bad Breath (Halitosis): Food particles and bacteria trapped under a gum flap or around an impacted tooth can lead to persistent bad breath.
- Difficulty Opening Your Mouth (Trismus): Inflammation and infection can cause the jaw muscles to spasm, making it painful and difficult to open your mouth wide.
- Jaw Stiffness or Soreness: Constant pressure from an erupting or impacted tooth can cause generalized jaw discomfort.
- Headaches or Earaches: Pain can radiate to other areas of the head and neck.
- Crowding of Other Teeth: Although less common and often occurring over time, an impacted wisdom tooth can sometimes exert pressure that shifts other teeth, potentially undoing previous orthodontic work.
- Cyst or Tumor Formation: In rare but more serious cases, a fluid-filled sac (cyst) or even a benign tumor can develop around an impacted wisdom tooth. These can damage the jawbone, adjacent teeth, and nerves.
Pro Tip: Don't wait for severe pain to consult a dentist. Even mild, intermittent discomfort or a persistent bad taste could indicate an underlying issue that needs attention.
``
Treatment Options: Monitoring vs. Extraction
Once your dentist or oral surgeon has evaluated your wisdom teeth, typically through a comprehensive oral exam and X-rays, they will discuss the appropriate course of action.
Monitoring
In some cases, if wisdom teeth are fully erupted, healthy, asymptomatic, and can be easily cleaned, your dentist may recommend a "wait and see" approach. Regular dental check-ups will be crucial to monitor their condition and ensure they don't develop problems later. This is often an option only for those with sufficient jaw space.

Extraction
This is the most common treatment for problematic wisdom teeth. Extraction is recommended if the wisdom teeth are:
- Impacted and causing pain, infection, or damage to adjacent teeth.
- Partially erupted and prone to pericoronitis.
- Fully erupted but difficult to clean, leading to recurrent cavities or gum disease.
- Contributing to orthodontic problems (though this is less common).
- Associated with cysts or tumors.
There are two main types of extraction procedures:
- Simple Extraction: This is performed when the wisdom tooth is fully erupted and visible in the mouth, similar to removing any other tooth. The dentist can grasp the tooth with forceps and gently rock it to loosen it from the socket.
- Surgical Extraction: This is required for impacted wisdom teeth, where the tooth is either fully or partially embedded in the bone or gum tissue. This procedure is more complex and often performed by an oral and maxillofacial surgeon. It typically involves an incision in the gum, removal of bone covering the tooth, and sometimes sectioning the tooth into smaller pieces for easier removal.
Comparison Table 1: Monitoring vs. Wisdom Tooth Extraction
| Feature | Monitoring | Extraction (Surgical) |
|---|---|---|
| When Recommended | Fully erupted, asymptomatic, easily cleaned | Impacted, symptomatic, infected, damaging adjacent teeth |
| Procedure | Regular dental check-ups, X-rays | Surgical removal of tooth (and sometimes bone/tissue) |
| Anesthesia | None | Local anesthesia, sedation, or general anesthesia |
| Cost (per tooth) | Included in regular check-ups (if healthy) | $200 - $600+ (impacted) |
| Recovery Time | None | 3-7 days for initial healing, weeks for full recovery |
| Risks | Potential for future problems (cavities, infection, impaction if not fully erupted) | Dry socket, infection, nerve damage, swelling, pain |
| Long-Term Outcome | Continued presence of tooth | Permanent removal of source of potential problems |
Step-by-Step Process: What to Expect During Wisdom Tooth Extraction
If extraction is recommended, here's a general overview of what you can expect:
- Initial Consultation and Examination: Your dentist or oral surgeon will perform a thorough examination, review your medical history, and take detailed X-rays (often a panoramic X-ray, which shows all your teeth and surrounding bone). This helps them assess the position of the wisdom teeth, their proximity to nerves and sinuses, and plan the extraction.
- Anesthesia Discussion: You'll discuss your anesthesia options.
- Local Anesthesia: Numbing injections around the tooth site. You'll be awake but won't feel pain.
- Sedation: Often combined with local anesthesia. Options include oral sedatives, inhaled nitrous oxide ("laughing gas"), or intravenous (IV) sedation, which makes you drowsy and relaxed, often with little memory of the procedure.
- General Anesthesia: You will be completely unconscious. This is typically reserved for complex cases or patients with high anxiety, and is administered by an anesthesiologist.
- The Extraction Procedure:
- Once the anesthesia takes effect, the surgeon will begin.
- Incision: For impacted teeth, the surgeon will make an incision in the gum tissue to expose the tooth and bone.
- Bone Removal: If the tooth is embedded in bone (bony impaction), a small amount of bone may be carefully removed using a dental drill.
- Tooth Sectioning: To minimize the amount of bone removal and make extraction easier, the tooth may be cut into smaller pieces.
- Removal: The tooth (or pieces of the tooth) will then be carefully extracted from the socket.
- Cleaning and Suturing: The surgeon will clean the socket thoroughly, removing any bone fragments or debris. The gum flap is then repositioned, and sutures (stitches) are placed to help the gum heal and protect the blood clot in the socket. These sutures may be dissolvable or require removal at a follow-up appointment.
- Post-Procedure Instructions: Before you leave, you'll receive detailed instructions on how to care for the extraction sites, manage pain, and prevent complications.
``
Cost and Insurance: Understanding the Financial Aspect in the US
The cost of wisdom tooth extraction in the US can vary significantly based on several factors, including the complexity of the extraction, the type of anesthesia used, the geographic location, and whether a general dentist or an oral surgeon performs the procedure.
Average US Costs (Per Tooth):
- Simple Extraction (fully erupted): $75 - $250
- Surgical Extraction (soft tissue impacted): $150 - $400
- Surgical Extraction (bony impacted): $200 - $600
- Surgical Extraction (deeply bony impacted, complex): $500 - $1,100+
Additional Costs:
- Consultation & X-rays: $50 - $250 (often covered by insurance or included in the extraction fee if performed at the same office). Panoramic X-rays can range from $75 - $150.
- Anesthesia: This can significantly add to the cost.
- Nitrous Oxide (Laughing Gas): $50 - $150
- Oral Sedation: $100 - $300
- IV Sedation (conscious sedation): $300 - $800+ per hour
- General Anesthesia: $500 - $1,500+ per hour (often administered by an anesthesiologist)
- Follow-up Appointments: May be included in the extraction fee or charged separately (e.g., for suture removal or check-up).
- Medications: Prescriptions for pain relief or antibiotics.
Total Cost for All Four Wisdom Teeth: Without insurance, the total cost for removing all four wisdom teeth, including anesthesia and consultation, can range from $600 to over $3,000, and sometimes up to $5,000 for very complex cases with general anesthesia.
Insurance Coverage Details:
- Dental Insurance: Most dental insurance plans cover a portion of wisdom tooth extractions, especially if they are medically necessary (e.g., causing pain, infection, impaction). Coverage typically ranges from 50% to 80% of the procedure cost after your deductible is met. However, there are usually annual maximums (often $1,000 - $2,000) that you might exceed, leaving you responsible for the remainder.
- Medical Insurance: In some cases, if the extraction is considered a major surgical procedure (e.g., deeply impacted teeth requiring extensive bone removal, or if nerve damage is a concern), portions of the cost, particularly anesthesia and hospital facility fees, might be covered by your medical insurance, especially if performed by an oral surgeon. It's crucial to verify this with both your dental and medical insurance providers beforehand.
- "$99 Tooth Extraction": This common marketing tactic typically refers to a very simple, fully erupted tooth extraction performed by a general dentist, usually for promotional purposes. It is highly unlikely to apply to impacted wisdom teeth, which require a more complex surgical procedure. Always ask for a detailed quote that includes all potential costs (anesthesia, X-rays, follow-ups) and confirm if the offer applies to your specific situation, especially when dealing with wisdom teeth. An impacted wisdom tooth will almost always cost more than $99.
Payment Plans and Financing Options:
- In-Office Payment Plans: Some dental offices offer interest-free payment plans, allowing you to pay in installments.
- Third-Party Financing: Services like CareCredit are widely accepted in dental offices, offering special financing options, often with deferred interest if paid within a certain period.
- Dental Schools: University dental schools often provide services at a reduced cost, as procedures are performed by students under the supervision of experienced faculty.
- Community Dental Clinics: Many communities have clinics that offer services on a sliding scale based on income or at significantly reduced rates.
Pro Tip: Always get a detailed, itemized estimate in writing from your chosen provider before proceeding with any treatment. Understand what your insurance will cover and what your out-of-pocket expenses will be.
Recovery and Aftercare: Ensuring a Smooth Healing Process
Proper aftercare is paramount to a smooth recovery and to prevent complications like dry socket wisdom teeth. Following your surgeon's instructions diligently is critical.
Immediately After the Procedure:
- Bleeding Control: You'll bite down gently on gauze pads placed over the extraction sites for 30-60 minutes to control bleeding. Change pads as needed. Slight oozing for 24-48 hours is normal.
- Pain Management: Take prescribed pain medication or over-the-counter pain relievers (e.g., ibuprofen, acetaminophen) as directed, before the anesthesia wears off.
- Swelling Reduction: Apply ice packs to the outside of your face, over the extraction sites, for 20 minutes on, 20 minutes off, during the first 24-48 hours. This significantly helps reduce swelling and discomfort.
- Rest: Go home and rest. Avoid strenuous activity for at least 24-48 hours, or longer if advised.
First 24-48 Hours:
- Diet: Stick to soft foods like yogurt, applesauce, mashed potatoes, broth, and scrambled eggs. Avoid hot liquids, crunchy foods, and anything that requires vigorous chewing.
- Oral Hygiene: Do NOT rinse your mouth vigorously, spit, or use a straw during this time. This is crucial to protect the blood clot that forms in the socket, which is essential for healing and preventing dry socket wisdom teeth.
- No Smoking/Alcohol: Avoid smoking and alcohol as they can significantly impair healing and increase the risk of complications.
- Sleeping Position: Sleep with your head elevated on pillows to help reduce swelling.
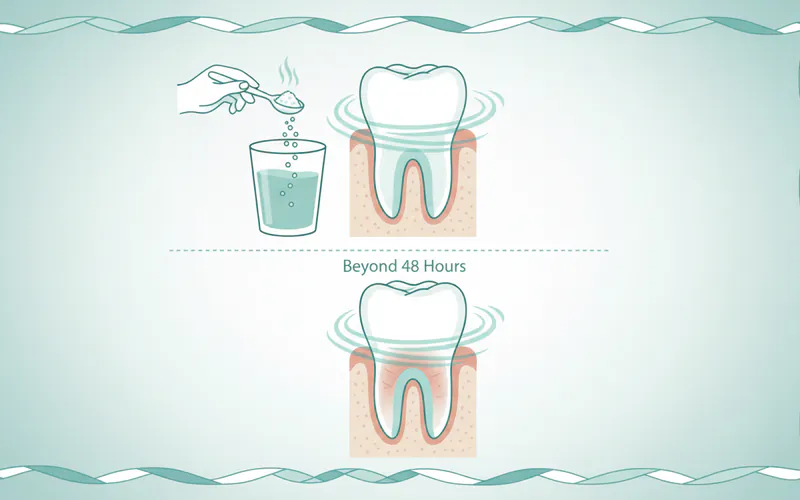
Beyond 48 Hours:
- Gentle Rinsing: You can start gently rinsing your mouth with warm salt water (1/2 teaspoon salt in 8 ounces of warm water) 3-4 times a day, especially after meals. This helps keep the area clean.
- Brushing: Brush your other teeth gently, but avoid the extraction sites initially.
- Diet Progression: Gradually introduce more solid foods as comfort allows.
- Stitches: If you have dissolvable stitches, they will typically disappear within 1-2 weeks. If you have non-dissolvable stitches, you'll have an appointment to get them removed, usually 7-10 days after the surgery.
- Continue Avoiding: Straws, smoking, and vigorous activity for at least a week, or as advised by your surgeon.
What to Watch For:
- Excessive Bleeding: If bleeding is heavy and doesn't stop with pressure from gauze, contact your surgeon.
- Severe Pain: Intense, throbbing pain that doesn't improve with medication, especially a few days after surgery, could indicate a dry socket wisdom teeth complication or infection.
- Increased Swelling: Swelling that worsens after 2-3 days, or is accompanied by fever, could indicate infection.
- Numbness: Persistent numbness in the lip, chin, or tongue beyond the initial anesthesia effect.
- Pus/Fever: Clear signs of infection.
Pro Tip: Stay hydrated by drinking plenty of water. Avoid carbonated beverages and sugary drinks which can irritate the healing sites.
Prevention: Minimizing Wisdom Teeth Complications
While you can't prevent wisdom teeth from coming in, you can take proactive steps to minimize potential problems:
- Regular Dental Check-ups: Consistent visits to your dentist allow them to monitor the development of your wisdom teeth through X-rays and clinical exams, starting in your mid-teens. Early detection of impaction or potential issues allows for timely intervention.
- Orthodontic Evaluation: An orthodontist can assess jaw space and growth patterns, sometimes providing insights into future wisdom tooth issues.
- Good Oral Hygiene: If your wisdom teeth have erupted and are causing no problems, meticulous brushing and flossing are essential to prevent cavities and gum disease in these hard-to-reach areas.
- Timely Intervention: If your dentist or oral surgeon recommends extraction, don't delay. Waiting until severe pain, infection, or damage to adjacent teeth occurs can lead to more complex procedures and prolonged recovery.
Risks and Complications: Understanding What Can Go Wrong
While wisdom tooth extraction is a very common and generally safe procedure, like any surgery, it carries potential risks and complications.
The Dreaded Dry Socket (Alveolar Osteitis)
This is one of the most common and painful complications following wisdom tooth extraction, particularly for lower molars.
- What it is: A dry socket occurs when the blood clot that normally forms in the empty tooth socket either dislodges, dissolves, or fails to form properly, exposing the underlying bone and nerve endings.
- Symptoms: Intense, throbbing pain usually starts 2-5 days after surgery, radiating to the ear, temple, or neck. It's often accompanied by a foul odor or taste in the mouth.
- Causes: Smoking, vigorous rinsing/spitting, drinking through a straw, certain medications, and poor oral hygiene can increase the risk.
- Treatment: Your dentist will clean the socket, place a medicated dressing to protect the exposed bone, and provide pain relief. The dressing may need to be changed every day or two until the pain subsides.
Other Potential Complications:
- Infection: Bacteria can enter the extraction site, especially if the area isn't kept clean. Symptoms include increased pain, swelling, fever, and pus discharge. Antibiotics may be prescribed.
- Nerve Damage (Paresthesia): In rare cases, especially with lower wisdom teeth, the removal can injure the inferior alveolar nerve (which provides sensation to the lower lip, chin, and tongue) or the lingual nerve (which provides sensation to the tongue). This can result in temporary or, very rarely, permanent numbness, tingling, or altered sensation. Most nerve injuries resolve within weeks to months.
- Excessive Bleeding: While some oozing is normal, prolonged heavy bleeding should be reported to your surgeon.
- Sinus Perforation: For upper wisdom teeth, the roots can sometimes be very close to the maxillary sinus. During extraction, a small hole may inadvertently be created, connecting the mouth to the sinus cavity. This usually heals on its own but may require additional treatment or precautions.
- Damage to Adjacent Teeth: The second molar in front of the wisdom tooth can sometimes be inadvertently damaged during the extraction process, though this is rare with skilled surgeons.
- Jaw Fracture: Extremely rare, but possible, especially in patients with weakened jawbones or during very difficult extractions.
- Swelling and Bruising: These are normal side effects that usually subside within a week.
- TMJ (Temporomandibular Joint) Issues: Keeping the mouth open for an extended period during surgery can sometimes cause temporary jaw stiffness or discomfort.
Comparison Table 2: Wisdom Tooth Complications & Management
| Complication | Key Symptoms | When it Occurs | Management | Prevention Tips |
|---|---|---|---|---|
| Dry Socket | Intense, throbbing pain; foul odor/taste; exposed bone | 2-5 days post-extraction | Medicated dressing, pain relief, irrigation | Avoid straws, smoking, vigorous rinsing/spitting |
| Infection | Increased pain, swelling, fever, pus | Days to weeks post-extraction | Antibiotics, drainage (if abscess), diligent oral hygiene | Follow aftercare; saltwater rinses; complete antibiotics |
| Nerve Damage | Numbness/tingling in lip, chin, or tongue | Immediately post-op, persists | Observation, nerve medication (rarely surgery) | Pre-op X-rays/3D imaging, skilled surgeon |
| Excessive Bleeding | Heavy, persistent bleeding despite pressure | Immediately post-op, or later | Apply firm pressure with gauze, consult surgeon | Avoid strenuous activity, follow blood thinner advice |
| Sinus Perforation | Air or liquid escaping into nose; nasal congestion | Immediately post-op | Observation, avoid nose blowing, antibiotics, sometimes sutures | Pre-op imaging, skilled surgeon |
Children / Pediatric Considerations
While this article primarily focuses on when do wisdom teeth come in for young adults, it's worth noting that wisdom teeth are not a concern for children. The development of wisdom teeth begins in the jawbone much earlier, typically around 7-10 years of age, but they remain completely submerged.
For pre-teens and early teenagers, the focus of pediatric dental care related to wisdom teeth is on early detection and planning. Dentists may take panoramic X-rays during routine check-ups to monitor the development and position of these developing third molars. This allows for:
- Early Prediction of Space Issues: Identifying if there might be insufficient room in the jaw for proper eruption.
- Orthodontic Planning: Informing orthodontic treatment, as overcrowded jaws might make future wisdom tooth extraction more likely or even necessary to preserve orthodontic results.
- Identification of Anomalies: Detecting any unusual development, such as cysts forming around the unerupted tooth.
Parents don't need to worry about wisdom teeth problems in their young children, but ensuring regular dental visits throughout adolescence is key to proactive management as their wisdom teeth begin to mature.
Cost Breakdown Revisited and Payment Strategies
Given the varying costs, a clear cost breakdown and understanding of payment options are vital.
Average US Costs (Recap):
- General Dentist - Simple Eruption: $75 - $250 per tooth
- Oral Surgeon - Soft Tissue Impaction: $150 - $400 per tooth
- Oral Surgeon - Bony Impaction: $200 - $600 per tooth
- Oral Surgeon - Complex Impaction: $500 - $1,100+ per tooth
- Sedation Anesthesia (IV): $300 - $800+ per hour (often a significant portion of the total bill)
With vs. Without Insurance:
- Without Insurance (Self-Pay): You are responsible for 100% of the costs. This is where researching dental schools, community clinics, and comparing quotes becomes critical. Negotiating cash discounts is sometimes possible.
- With Insurance: Your dental insurance will typically cover 50-80% of the "reasonable and customary" fee for extractions, often categorized as a "major procedure." However, be mindful of:
- Deductibles: You'll need to pay this amount out-of-pocket before your insurance starts covering costs.
- Annual Maximums: Most dental plans have an annual limit (e.g., $1,000 - $2,000). If the total cost exceeds this, you'll pay the difference.
- Waiting Periods: Some plans have waiting periods for major procedures, meaning you can't get coverage immediately after signing up.
Payment Plans and Financing Options:
- CareCredit & LendingClub: These third-party medical credit cards offer low or no-interest financing for a set period (e.g., 6, 12, 18 months). They are widely accepted.
- In-Office Payment Plans: Discuss directly with your oral surgeon's office. Many offer flexible payment options to help manage the cost.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, these are excellent tax-advantaged ways to pay for dental expenses, including wisdom tooth extractions.
- Dental Schools: As mentioned, these often provide high-quality care at a lower cost because students perform procedures under close supervision. This can be a significant cost-saving measure for those without extensive insurance coverage.
Cost-Saving Tips:
- Get Multiple Quotes: Don't settle for the first estimate. Call a few oral surgery practices and ask for quotes based on your specific X-rays and diagnosis.
- Understand Your Insurance Benefits: Call your dental and medical insurance providers to get a detailed breakdown of your coverage, deductibles, annual maximums, and any waiting periods.
- Ask About Cash Discounts: Some providers offer a discount for patients paying upfront in cash (or debit card) without involving insurance.
- Consider Timing: If you're close to your annual maximum on your dental insurance, you might want to schedule the procedure late in the year or early the next year to maximize benefits across two cycles.
Frequently Asked Questions
Do all wisdom teeth need to be removed?
No, not all wisdom teeth need to be removed. If they erupt fully, are properly aligned, don't cause pain, and can be easily cleaned, they may not require extraction. Regular dental check-ups are essential to monitor their status.

How painful is wisdom tooth extraction?
During the procedure, you should feel no pain due to anesthesia. Afterward, you will experience discomfort and pain, which can be managed with prescribed pain medication and over-the-counter anti-inflammatories. Pain typically subsides significantly within 3-7 days.
How long does recovery take?
Initial healing, with reduced pain and swelling, usually takes 3-7 days. However, complete healing of the soft tissue can take several weeks, and bone remodeling in the socket can take months. Follow your aftercare instructions carefully to speed recovery.
What is dry socket and how is it prevented?
Dry socket (alveolar osteitis) occurs when the blood clot in the extraction site dislodges or dissolves, exposing the underlying bone and nerves. It's characterized by intense pain starting 2-5 days post-op. Prevention includes avoiding straws, spitting vigorously, smoking, and following all post-operative instructions diligently.
Can I get all four wisdom teeth removed at once?
Yes, it is very common and often recommended to remove all four wisdom teeth in a single surgical appointment, especially if they are impacted. This allows for a single recovery period and one course of anesthesia, streamlining the process.
What are the alternatives to extraction?
For problematic wisdom teeth, there are generally no effective alternatives to extraction. Monitoring might be an option for healthy, fully erupted teeth. However, if teeth are impacted, causing pain, infection, or damage, removal is typically the recommended and safest course of action.
When is the best age to remove wisdom teeth?
The ideal age for wisdom tooth removal is typically between the late teens and early twenties (17-25 years old). At this stage, the roots are usually not fully developed, and the surrounding bone is softer, making the extraction procedure generally easier and recovery quicker.
Is a "$99 tooth extraction" legitimate for wisdom teeth?
A "$99 tooth extraction" promotion is almost exclusively for a simple extraction of a fully erupted tooth, not for impacted wisdom teeth. Impacted wisdom teeth require a surgical procedure that is significantly more complex and costly due to the need for incisions, bone removal, and more advanced anesthesia, typically ranging from $200-$1,100+ per tooth.
What foods should I avoid after extraction?
For the first few days, avoid hard, crunchy, sticky, or hot foods. Stick to soft foods like yogurt, mashed potatoes, broth, applesauce, and smoothies (without a straw). Gradually reintroduce solid foods as your comfort allows.
How do I know if I have an impacted wisdom tooth?
Symptoms of an impacted wisdom tooth can include pain, swelling, tenderness, bad breath, difficulty opening your mouth, or a persistent bad taste. However, some impacted teeth are asymptomatic. The only definitive way to know is through a dental examination and X-rays performed by a dentist or oral surgeon.
When to See a Dentist
Don't wait for severe pain or a full-blown infection to seek professional help. Proactive dental care is the best approach when it comes to wisdom teeth.
Schedule a routine appointment if:
- You are between 17 and 25 years old and haven't had your wisdom teeth evaluated.
- You experience any mild, intermittent discomfort, tenderness, or a feeling of pressure in the back of your jaw.
- You notice any swelling or redness around your back molars.
- You have a persistent bad taste or bad breath.
Seek immediate dental attention if:
- You experience severe, throbbing pain that doesn't subside with over-the-counter pain relievers.
- You have significant swelling in your jaw, cheek, or neck that is worsening.
- You develop a fever, chills, or difficulty swallowing.
- You have difficulty opening your mouth wide (trismus).
- You notice pus or a foul discharge from the back of your mouth.
- You experience persistent numbness in your lip, chin, or tongue after an extraction.
Regular check-ups, ideally starting in your mid-teens, are crucial for monitoring wisdom tooth development and intervening before problems escalate. Your dental professional is your best resource for guidance on when do wisdom teeth come in and how to manage their arrival to protect your overall oral health.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Oral Surgery: Complete Guide
More than 178 million Americans are missing at least one tooth, and millions more experience jaw pain, impacted wisdom teeth, or facial trauma annually. These common issues often lead to a specialized area of dentistry: oral surgery. Far from being a last resort, oral surgery encompasses a wide
February 22, 2026
Wisdom Tooth Removal: Complete Guide
Wisdom tooth removal is one of the most common oral surgical procedures performed in the United States, affecting millions of individuals annually. For many, the emergence of wisdom teeth, or third molars, can herald a range of uncomfortable and potentially serious dental issues, making their extrac
February 22, 2026
Wisdom Teeth Removal Cost: Complete Price Guide 2026
For many young adults, the emergence of wisdom teeth – the third molars – is an inevitable rite of passage, often accompanied by discomfort and, eventually, a trip to the oral surgeon. In fact, approximately 85% of people will require wisdom teeth removal at some point in their lives, making it
February 22, 2026
Wisdom Tooth Extraction: Complete Guide
Have you ever experienced a throbbing ache deep in your jaw, or noticed swelling at the very back of your mouth? If so, you're not alone. An estimated 5 million people undergo wisdom tooth extraction in the United States each year, making it one of the most common oral surgical procedures. This
February 22, 2026