Jaw: Complete Dental Guide

Key Takeaways
- The jaw is far more than just the framework that holds your teeth; it is a complex and vital structure integral to some of life's most basic functions, from eating and speaking to breathing and forming facial expressions. For anyone seeking to understand "what is jaw" or exploring aspects of "jaw de
The jaw is far more than just the framework that holds your teeth; it is a complex and vital structure integral to some of life's most basic functions, from eating and speaking to breathing and forming facial expressions. For anyone seeking to understand "what is jaw" or exploring aspects of "jaw dental" health, this comprehensive guide from SmilePedia.net aims to be your definitive resource.
Introduction
At its core, the jaw is the bony framework of the mouth, consisting of two primary components: the upper jaw, known as the maxilla, and the lower jaw, called the mandible. Together, these powerful bones not only provide the foundational support for your teeth but also sculpt the lower and mid-facial contours, creating your unique appearance. The jaw's intricate design allows for a remarkable range of motion, facilitating the complex actions of chewing, biting, and articulating speech.
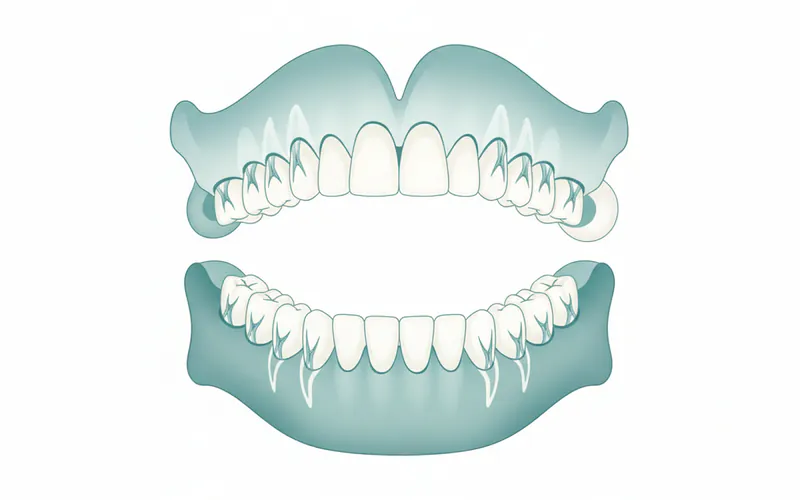
The health and proper alignment of your jaw are paramount to overall dental and systemic well-being. A well-functioning jaw ensures an optimal bite, preventing excessive wear on teeth, and supports clear speech. It also plays a crucial role in maintaining the health of the Temporomandibular Joints (TMJ), which connect the jawbone to the skull and are responsible for all jaw movements. When the jaw is misaligned or experiences dysfunction, it can lead to a cascade of problems, from chronic pain and difficulty eating to sleep disturbances and even issues with breathing.
Jaw-related issues are surprisingly common. For instance, malocclusion, or a "bad bite" where the upper and lower teeth don't align properly, affects a significant portion of the population, with estimates suggesting 60-75% of individuals experiencing some form of it. Similarly, Temporomandibular Joint (TMJ) disorders, which encompass pain and dysfunction of the jaw joints and muscles, are prevalent, impacting approximately 10 million Americans at any given time. Understanding the jaw, its potential problems, and the available solutions is a critical step in maintaining a healthy, functional smile and a comfortable life.
Key Takeaways:
- The jaw consists of two main bones: the fixed maxilla (upper jaw) and the movable mandible (lower jaw).
- It is crucial for holding teeth, chewing food, speaking, and shaping the face.
- Jaw alignment issues, known as malocclusion, are common and can impact dental health.
- The Temporomandibular Joint (TMJ) connects the jaw to the skull and is essential for jaw movement; disorders can cause significant pain and dysfunction.
- Various factors, including genetics, trauma, and habits, can affect jaw health.
- Many jaw-related problems are treatable through non-surgical or surgical interventions.
Detailed Explanation
The jaw is a marvel of biological engineering, capable of withstanding immense forces while performing delicate, precise movements. Understanding its structure and the conditions that can affect it is key to maintaining optimal dental health.
Types and Classifications of the Jaw
When we refer to the "jaw," we're generally talking about two distinct bones that work in concert:
- Maxilla (Upper Jaw): This is the fixed, non-movable upper jawbone. It's a central bone of the face, forming the roof of the mouth (hard palate), the floor of the nasal cavity, and parts of the eye sockets. The maxilla houses the upper teeth and contributes significantly to the mid-facial structure. Its stability is vital for biting and supporting the upper dental arch.
- Mandible (Lower Jaw): This is the movable lower jawbone and is the largest and strongest bone of the face. It is the only truly movable bone in the skull, articulating with the temporal bone of the skull at the Temporomandibular Joints (TMJ). The mandible houses the lower teeth and is crucial for chewing, speaking, and forming facial expressions. Its movement allows us to open and close our mouths, grind food, and articulate a wide range of sounds.
Both the maxilla and mandible contain alveolar bone, which is the specialized bone that surrounds and supports the roots of the teeth. This bone is dynamic, constantly remodeling in response to the forces exerted during chewing and orthodontic treatment.
Beyond these basic anatomical classifications, jaw issues are often classified by their developmental or functional characteristics:
- Skeletal Malocclusion: Refers to discrepancies in the size or position of the maxilla and mandible relative to each other or to the base of the skull. This can result in conditions like:
- Dentoalveolar Malocclusion: Involves the alignment of the teeth within the jawbones, such as crowding, spacing, or rotated teeth, even if the jawbones themselves are proportionally sized.
Causes and Risk Factors for Jaw Problems
A variety of factors can contribute to issues affecting the jaw and its function:
- Genetics and Heredity: Many jaw discrepancies, such as prognathism or retrognathism, have a strong genetic component. If parents have a particular jaw structure or malocclusion, their children are more likely to inherit similar traits.
- Trauma and Injury: Fractures of the maxilla or mandible, dislocations of the TMJ, or injuries to the surrounding soft tissues can occur due to falls, sports accidents, car crashes, or physical altercations. These can lead to immediate pain, swelling, and long-term functional problems if not properly treated.
- Developmental Anomalies: Conditions present at birth, such as cleft lip and palate, can significantly affect the development and structure of the maxilla, leading to significant jaw and dental issues. Other genetic syndromes can also impact jaw growth.
- Habits: Persistent habits during childhood, such as prolonged thumb-sucking, pacifier use beyond age 3, or tongue thrusting, can exert pressure on developing jawbones and teeth, leading to malocclusion (e.g., open bite).
- Bruxism (Teeth Grinding/Clenching): Chronic grinding or clenching of teeth, often subconsciously during sleep, can put immense stress on the TMJ and jaw muscles, leading to pain, wear on teeth, and TMJ dysfunction.
- Arthritis: Degenerative joint diseases like osteoarthritis or inflammatory conditions like rheumatoid arthritis can affect the TMJ, leading to pain, stiffness, and reduced jaw mobility.
- Stress: High levels of psychological stress can exacerbate bruxism and increase muscle tension in the jaw, contributing to TMJ pain.
- Dental Issues: Missing teeth, poorly fitting dental restorations (crowns, bridges, dentures), or extensive tooth decay can alter the bite and put uneven stress on the jaw, potentially leading to TMJ problems or further malocclusion.
- Tumors or Cysts: While rare, abnormal growths within the jawbones can lead to structural changes, pain, and functional impairment.
Signs and Symptoms to Watch For
Recognizing the early signs of jaw problems is crucial for timely intervention. Be alert to:
- Pain: Persistent pain in the jaw, face, ear, neck, or head (especially morning headaches). Pain may worsen when chewing or speaking.
- Clicking, Popping, or Grating Sounds: Sounds emanating from the TMJ when opening or closing the mouth. While occasional sounds can be normal, persistent, painful, or loud noises are concerning.
- Limited Jaw Movement: Difficulty opening the mouth wide, stiffness, or the sensation that the jaw is "stuck" or "locked" in an open or closed position.
- Difficulty Chewing or Biting: Pain, discomfort, or an inability to chew certain foods effectively.
- Facial Swelling or Asymmetry: Noticeable swelling around the jaw or changes in facial symmetry.
- Changes in Bite: A sudden change in how the upper and lower teeth fit together (malocclusion).
- Tooth Sensitivity or Wear: Often a result of bruxism or an improper bite, leading to excessive wear on tooth enamel.
- Ear-related Symptoms: Ringing in the ears (tinnitus), earaches, or a feeling of fullness in the ears (without infection).
Diagnosis Process — What Your Dentist Does
If you experience any of these symptoms, a visit to your dentist or an oral and maxillofacial surgeon is essential. The diagnostic process typically involves:
- Comprehensive Dental and Medical History: The dentist will ask about your symptoms, when they started, their severity, and any relevant medical conditions or habits (bruxism, trauma).
- Clinical Examination: This includes:
- Palpation: The dentist will gently feel your jaw joints and muscles for tenderness, swelling, or spasms.
- Observation: Assessing your jaw's range of motion, symmetry, and how your teeth come together when you bite.
- Auscultation: Listening for clicks, pops, or grinding noises in the TMJ with a stethoscope.
- Imaging Studies:
- Dental X-rays: Panoramic X-rays provide a broad view of the entire maxilla and mandible, including the teeth and TMJs. Periapical X-rays focus on individual teeth and surrounding bone.
- CT Scans (Computed Tomography): Offer detailed 3D images of bone structures, useful for diagnosing fractures, bone deformities, or growths.
- MRI Scans (Magnetic Resonance Imaging): Provide detailed images of soft tissues, crucial for assessing the TMJ disc, ligaments, and muscles, especially in cases of suspected TMJ internal derangement.
- Cone Beam CT (CBCT): A specialized dental CT that provides 3D images with less radiation than traditional CT, often used for detailed orthodontic or surgical planning.
- Bite Analysis: Your dentist may take impressions of your teeth to create models, allowing for a precise analysis of your malocclusion and how your teeth fit together.
Treatment Options with Pros, Cons, and Costs
Treatment for jaw problems varies widely depending on the underlying cause, severity, and individual patient needs. Options can range from conservative, non-invasive approaches to complex surgical procedures.
Non-Surgical Treatment Options:
- Oral Appliances (Splints/Nightguards): Custom-made acrylic devices worn over the teeth, primarily for bruxism or TMJ disorders.
- Pros: Non-invasive, reversible, can reduce pain and protect teeth from wear.
- Cons: Requires consistent wear, can be bulky, does not always correct the underlying problem.
- Cost (US): $300 - $1,500 (without insurance).
- Orthodontics (Braces, Clear Aligners): Used to correct malocclusion by repositioning teeth and sometimes guiding jaw growth.
- Pros: Corrects bite, improves aesthetics, can prevent future jaw problems.
- Cons: Can be lengthy (months to years), requires commitment, temporary discomfort, dietary restrictions with traditional braces.
- Cost (US): $3,000 - $8,000 (without insurance, varies by complexity and type of appliance).
- Medications:
- Pain Relievers: Over-the-counter (ibuprofen, acetaminophen) or prescription (muscle relaxants, anti-inflammatories) to manage pain and inflammation.
- Pros: Quick relief of symptoms.
- Cons: Addresses symptoms, not always the root cause; potential side effects.
- Cost (US): Varies from $10 - $100+ per prescription.
- Physical Therapy: Exercises to strengthen jaw muscles, improve range of motion, and reduce muscle tension.
- Pros: Non-invasive, improves function, empowers patients with self-management techniques.
- Cons: Requires commitment and consistency.
- Cost (US): $50 - $200 per session; often covered by medical insurance.
- Lifestyle Modifications: Stress reduction techniques, avoiding hard/chewy foods, applying moist heat or cold packs, practicing good posture.
- Pros: Low cost, often highly effective for mild cases, improves overall well-being.
- Cons: Requires self-discipline.
Surgical Treatment Options:
- Orthognathic Surgery (Jaw Surgery): Corrects severe jaw discrepancies and malocclusions by surgically repositioning the maxilla, mandible, or both.
- Pros: Definitive correction of severe skeletal problems, significant functional and aesthetic improvement, improves speech and breathing.
- Cons: Invasive, requires general anesthesia, significant recovery period (weeks to months), risks include nerve damage, infection, bleeding, and potential relapse.
- Cost (US): $20,000 - $50,000+ (without insurance, highly variable based on single vs. double jaw, complexity).
- TMJ Surgery: A range of procedures for severe TMJ disorders not responsive to conservative care.
- Arthrocentesis: Minimally invasive, involves flushing the joint with fluid.
- Arthroscopy: Uses a small camera to visualize and treat joint issues.
- Open-Joint Surgery: More invasive, used for severe degeneration, disc repair/replacement, or removal of growths.
- Pros: Can provide significant relief for chronic, debilitating TMJ pain and dysfunction.
- Cons: Invasive, risks similar to orthognathic surgery, long recovery.
- Cost (US): $5,000 - $25,000+ (without insurance, depending on the procedure).
- Fracture Repair: Surgical stabilization of jaw fractures using wires, plates, and screws.
- Pros: Restores jaw integrity, allows proper healing, preserves function.
- Cons: Invasive, risks of infection, non-union, malunion.
- Cost (US): $1,500 - $10,000+ (without insurance, highly dependent on severity and location of fracture).
Step-by-Step: What to Expect During Treatment (Example: Orthognathic Surgery)
For complex jaw issues requiring orthognathic surgery, the process is typically multi-phase:
- Pre-surgical Orthodontics (6-18 months): Most patients undergo orthodontic treatment (braces or aligners) before surgery to align the teeth within their respective jaws. This often makes the bite worse initially as teeth are moved into positions that will be correct once the jawbones are repositioned.
- Surgical Planning: Detailed imaging (CBCT scans), dental models, and computer simulations are used to precisely plan the jaw movements. The surgeon and orthodontist work closely together.
- The Surgery (2-6 hours): Performed under general anesthesia by an oral and maxillofacial surgeon, usually in a hospital setting.
- Incisions are made inside the mouth (no visible external scars).
- The surgeon carefully cuts the jawbone(s) (osteotomies) to allow for repositioning.
- The jaw is moved into its planned new position and secured with small titanium plates and screws, which are biocompatible and typically remain permanently.
- Post-surgical Recovery (1-2 weeks in hospital/home): Patients typically stay in the hospital for 1-3 days. Swelling and discomfort are significant in the first week. Pain medication will be prescribed. Your jaw may be "wired shut" or held with elastics for a period (often 2-6 weeks) to ensure proper healing, requiring a liquid diet.
- Post-surgical Orthodontics (6-12 months): After the initial healing, orthodontics continue to fine-tune the bite and achieve optimal dental alignment.
- Retention: Once active orthodontic treatment is complete, retainers are worn to maintain the new jaw and teeth positions long-term.
Recovery Timeline and Aftercare
Recovery timelines vary based on the treatment:
- Oral Appliances: Immediate symptom relief for some, but continuous wear is necessary.
- Orthodontics: Discomfort after adjustments lasts a few days. The full process can take 18-36 months. Retainers are a lifelong commitment.
- Jaw Surgery:
- Initial Healing: 2-6 weeks of significant swelling and a liquid/soft diet. Most patients return to light activities within 2-4 weeks.
- Moderate Recovery: Bone fully heals in about 6-12 weeks. Normal chewing can gradually resume.
- Full Recovery: Numbness, if present, can take 6-12 months to fully resolve, or may be permanent in rare cases. Full adaptation to the new bite and facial structure can take up to a year.
- Aftercare for Surgery: Strict adherence to dietary restrictions, meticulous oral hygiene (mouthwashes), avoiding strenuous activity, taking prescribed medications, and attending all follow-up appointments. Physical therapy for jaw exercises may be recommended.
Prevention Strategies
While not all jaw problems are preventable, several strategies can reduce your risk:
- Early Orthodontic Evaluation: Visiting an orthodontist by age 7 can help identify and intervene early for developing malocclusion or jaw growth issues.
- Wear a Mouthguard: Protect your jaws and teeth from trauma during sports activities.
- Manage Bruxism: If you grind or clench your teeth, wear a custom nightguard. Address stress through relaxation techniques, meditation, or therapy.
- Avoid Harmful Habits: Discourage thumb-sucking or pacifier use beyond appropriate ages.
- Maintain Good Posture: Poor head and neck posture can contribute to jaw muscle strain and TMJ discomfort.
- Limit Chewy/Hard Foods: If you have a history of TMJ issues, avoid excessively chewy foods (e.g., gum, jerky) or very hard foods (e.g., nuts, hard candies) that can strain the joint.
- Regular Dental Check-ups: Consistent visits allow your dentist to monitor jaw health and address issues before they become severe.
Cost Ranges in the US (with/without insurance)
The cost of jaw treatment can vary significantly, depending on the diagnosis, the complexity of the treatment, the specialist performing it, and geographic location.
- Oral Appliances (Nightguards/Splints):
- Without Insurance: $300 - $1,500
- With Dental Insurance: Often partially covered, may pay 50-80% after deductible.
- Orthodontics (Braces/Aligners):
- Without Insurance: $3,000 - $8,000
- With Dental Insurance: Varies greatly; some plans cover 10-50% of the cost, often with a lifetime maximum.
- TMJ Non-Surgical Treatment (Medication, PT, Injections):
- Without Insurance: Medications $10 - $100+, PT $50 - $200 per session.
- With Medical Insurance: Often covered as a medical condition, subject to deductibles and co-pays.
- TMJ Surgery:
- Without Insurance: $5,000 - $25,000+ (depending on procedure type)
- With Medical Insurance: Coverage is often strong if deemed medically necessary, but can require pre-authorization and referrals.
- Orthognathic Surgery (Jaw Surgery):
- Without Insurance: $20,000 - $50,000+ (this often includes hospital fees, anesthesia, and surgeon's fees, but typically excludes pre- and post-surgical orthodontics).
- With Medical Insurance: If the surgery is deemed medically necessary (e.g., to correct a severe functional problem like inability to chew or sleep apnea), it is usually covered by medical insurance, subject to deductibles and out-of-pocket maximums. Cosmetic reasons are typically not covered.
It's crucial to discuss treatment plans and costs with your dental and medical providers, and always verify insurance coverage beforehand.
Comparison Table: Non-Surgical vs. Surgical Jaw Treatment
| Feature | Non-Surgical Options (e.g., Orthodontics, Splints, PT) | Surgical Options (e.g., Orthognathic Surgery, TMJ Surgery) |
|---|---|---|
| Indication | Mild to moderate malocclusion, mild TMJ pain, bruxism, dental trauma | Severe skeletal jaw discrepancies, persistent TMJ dysfunction, fractures, facial asymmetry |
| Invasiveness | Minimal to none | High (requires general anesthesia, incisions, bone manipulation) |
| Recovery Time | Variable (days to weeks for initial discomfort; ongoing for orthodontics or chronic conditions) | Weeks to months for initial healing; up to a year for full recovery and adaptation |
| Cost (US) | $300 - $8,000 (depending on treatment) | $5,000 - $50,000+ (depending on procedure, excludes orthodontics for jaw surgery) |
| Risks | Minor discomfort, prolonged treatment, limited effectiveness for severe cases | Infection, nerve damage, bleeding, anesthesia risks, temporary or permanent numbness, relapse |
| Effectiveness | Very effective for appropriate cases; symptomatic relief for chronic conditions | Definitive structural correction for severe skeletal and functional issues |
| Insurance | Dental insurance often covers partially; medical for some TMJ symptoms/PT | Medical insurance often covers if medically necessary; dental may cover associated orthodontics |
For Parents / Pediatric Considerations
The jaw's development begins even before birth and continues throughout childhood and adolescence. Monitoring jaw growth in children is a critical aspect of pediatric dental care.
- Growth and Development: Children's jaws are still growing, making them amenable to "interception" and guidance. Early detection of jaw growth problems can often lead to simpler, less invasive treatment.
- Common Pediatric Issues:
- Malocclusion: Overbites (retrognathism), underbites (prognathism), crossbites, and open bites are frequently identified during childhood.
- Habits: Persistent thumb-sucking, pacifier use beyond age 3-4, and tongue thrusting can exert abnormal forces on the developing jaws, potentially leading to malocclusion and affecting facial development.
- Early Loss of Primary Teeth: Can lead to space loss, affecting the eruption path of permanent teeth and potentially leading to crowding or malocclusion.
- Interceptive Orthodontics (Phase 1 Orthodontics): This involves early treatment, typically between ages 6 and 10, to correct severe jaw problems as they develop. This might include:
- Palatal Expanders: To widen the upper jaw (maxilla) and correct crossbites.
- Space Maintainers: To hold space for permanent teeth if primary teeth are lost prematurely.
- Growth Modification Appliances: Devices designed to encourage or restrict jaw growth, addressing skeletal discrepancies before they become too severe.
- Trauma Prevention: Children are prone to falls and sports injuries. Wearing appropriate mouthguards during sports is vital to protect the jaws and teeth from fractures and dislocations.
- Monitoring Jaw Function: Parents should watch for signs of TMJ issues in children, such as persistent jaw clicking, difficulty opening the mouth, or jaw pain, especially if the child is also exhibiting signs of bruxism (grinding teeth). Early intervention in pediatric jaw issues can often simplify later treatment, reduce its duration and cost, and prevent more complex problems down the line.
Frequently Asked Questions
Q: How much does jaw treatment cost without insurance?
A: The cost varies enormously depending on the specific treatment. It can range from a few hundred dollars for a basic oral appliance to $8,000 for comprehensive orthodontics, and well over $50,000 for complex orthognathic surgery. Always get a detailed quote from your provider.
Q: Is jaw treatment painful?
A: The level of pain depends on the treatment. Non-surgical options like oral appliances or physical therapy typically cause minimal discomfort. Orthodontics can lead to soreness after adjustments. Surgical treatments, such as jaw surgery, involve significant post-operative pain, which is managed effectively with prescription pain medication during the initial recovery period.
Q: How long does jaw treatment take?
A: This varies greatly. Treatment for acute issues like a dislocated jaw might be a quick, single procedure. Non-surgical treatments for TMJ may provide relief within weeks or months. Comprehensive orthodontic treatment usually takes 18 to 36 months. Jaw surgery itself takes a few hours, but the entire process, including pre- and post-surgical orthodontics and full recovery, can span 2 to 3 years.
Q: Are there alternatives to surgery for jaw problems?
A: Yes, many jaw problems can be effectively managed with non-surgical approaches, including oral appliances, orthodontics, physical therapy, medications, and lifestyle changes. Surgery is generally reserved for severe structural issues, trauma, or when conservative treatments have failed. Your dentist or specialist will discuss all appropriate options for your specific condition.
Q: Does insurance cover jaw treatment?
A: Coverage depends on your specific insurance plan (dental vs. medical) and the nature of the treatment. Dental insurance often provides partial coverage for orthodontics and some oral appliances. Medical insurance typically covers jaw surgery and significant TMJ treatments if they are deemed medically necessary to correct a functional problem (e.g., inability to chew, sleep apnea) rather than purely cosmetic concerns. It's crucial to pre-authorize treatment with both your dental and medical insurance providers.
Q: Can jaw problems cause headaches?
A: Absolutely. TMJ disorders are a common cause of tension headaches, migraines, and facial pain. The muscles that control jaw movement are closely linked to muscles in the head and neck, so dysfunction in one area can easily lead to pain in the others.
Q: What is the difference between the maxilla and mandible?
A: The maxilla is the fixed, non-movable upper jawbone that forms the roof of the mouth and part of the face. The mandible is the movable lower jawbone, connected to the skull by the TMJ, and is responsible for all jaw movements like chewing and speaking.
Q: Can I prevent jaw problems?
A: While not all jaw problems are preventable, you can significantly reduce your risk. Strategies include wearing mouthguards for sports, managing bruxism (teeth grinding), discouraging harmful childhood habits (like prolonged thumb-sucking), maintaining good oral hygiene, and having regular dental check-ups to catch issues early.
When to See a Dentist
Knowing when to seek professional dental care for jaw-related issues is important for prompt and effective treatment.
Emergency Signs (Seek immediate dental or medical attention):
- Severe Jaw Pain: Sudden, intense pain that does not subside with over-the-counter pain relievers.
- Inability to Open or Close Mouth: Your jaw is locked open or closed, making it impossible to move.
- Suspected Jaw Fracture: Following trauma (fall, accident), if you have intense pain, swelling, bruising, or difficulty biting down, you may have a broken jaw.
- Significant Facial Swelling: Rapidly developing swelling around the jaw area, potentially indicating infection or trauma.
- Bleeding from the Jaw/Mouth: Especially after an injury.
- Difficulty Breathing or Swallowing: If jaw swelling or injury is impacting your airway.
Routine Care / Non-Emergency Signs (Schedule an appointment soon):
- Persistent Jaw Clicking or Popping: Even if not immediately painful, consistent sounds from your TMJ should be evaluated.
- Chronic Jaw Pain: Ongoing dull aches, stiffness, or discomfort in your jaw, face, or ears.
- Difficulty Chewing or Biting: If eating becomes uncomfortable or challenging.
- Recurrent Headaches or Neck Pain: Especially if they seem related to jaw movement or clenching.
- Changes in Your Bite: If your teeth no longer fit together as they used to.
- Worn or Sensitive Teeth: Often a sign of bruxism or malocclusion.
- Concerns about Jaw Appearance: If you are unhappy with the aesthetic alignment or proportion of your jaw.
Your jaw is a complex and indispensable part of your oral and overall health. Understanding its functions, potential issues, and available treatments empowers you to take proactive steps towards a healthier, more comfortable life. Regular dental check-ups are key to monitoring jaw health and addressing any concerns before they escalate.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Zirconia: Complete Dental Guide
In the ever-evolving landscape of modern dentistry, zirconia stands out as a groundbreaking material that has transformed how dental professionals restore smiles. At its core, zirconia is a robust, tooth-colored ceramic material, chemically known as zirconium dioxide (ZrO2). It's not a metal
February 22, 2026
X-Ray (Dental): Complete Dental Guide
Short Definition: Diagnostic imaging that uses low-dose radiation to capture images of teeth, bones, and surrounding tissues, revealing problems not visible during a clinical examination.
February 22, 2026
Xerostomia: Complete Dental Guide
Xerostomia, more commonly known as chronic dry mouth, is a condition characterized by a reduced flow of saliva, leading to a persistently dry oral cavity. Far more than just an uncomfortable sensation, xerostomia is a serious dental health concern that can significantly impact an individual's qualit
February 22, 2026
Wisdom Tooth: Complete Dental Guide
Welcome to SmilePedia.net, your definitive resource for understanding all aspects of dental health. In this comprehensive article, we delve deep into the topic of wisdom teeth, often a source of curiosity, concern, and sometimes, discomfort for many adults.
February 22, 2026