Tmj Anatomy: Complete Guide
Key Takeaways
- Understanding the intricate workings of your body is a powerful step towards maintaining optimal health. One area often overlooked until pain strikes is the temporomandibular joint (TMJ) – a complex, dual-sided joint that acts as the hinge connecting your jawbone (mandible) to your skull. An estimat
Understanding the intricate workings of your body is a powerful step towards maintaining optimal health. One area often overlooked until pain strikes is the temporomandibular joint (TMJ) – a complex, dual-sided joint that acts as the hinge connecting your jawbone (mandible) to your skull. An estimated 10 million Americans suffer from temporomandibular joint disorders (TMDs), experiencing symptoms ranging from persistent jaw pain to debilitating headaches. Without a grasp of the fundamental TMJ anatomy, it's challenging to comprehend the source of discomfort or the rationale behind various treatment approaches.
This comprehensive guide will meticulously dissect the tmj anatomy, providing you with an in-depth understanding of its bony structures, ligaments, muscles, and the crucial articular disc that facilitates smooth jaw movement. We will explore how these components work in harmony to enable essential functions like speaking, chewing, and swallowing. Furthermore, we'll delve into the common causes of TMJ dysfunction, recognizable symptoms of tmj disorders, a full spectrum of treatment options, associated costs, and practical preventive measures. By the end of this article, you will have a definitive resource for understanding this vital joint and how to safeguard your jaw health.
Key Takeaways:
- The temporomandibular joint (TMJ) is a complex hinge and sliding joint connecting the jaw to the skull, crucial for speaking, chewing, and swallowing.
- Key anatomical components include the mandibular condyle, temporal bone's articular fossa and eminence, and the articular disc.
- TMJ disorders (TMDs) affect an estimated 10 million Americans, often presenting with pain, clicking/popping sounds, and limited jaw movement.
- Initial non-invasive treatments for TMDs, such as oral splints or physical therapy, typically cost between $300 and $2,500 and can take weeks to months to show improvement.
- More advanced interventions, including surgery, can range from $5,000 to $25,000+ per joint and involve recovery times of several weeks to several months.
- Many dental insurance plans offer some coverage for TMD diagnosis and non-surgical treatments, but surgical interventions often require medical insurance pre-authorization.
- Prevention involves stress management, avoiding hard foods, maintaining good posture, and addressing habits like teeth grinding (bruxism) early on.
What It Is / Overview: The Intricate TMJ Anatomy
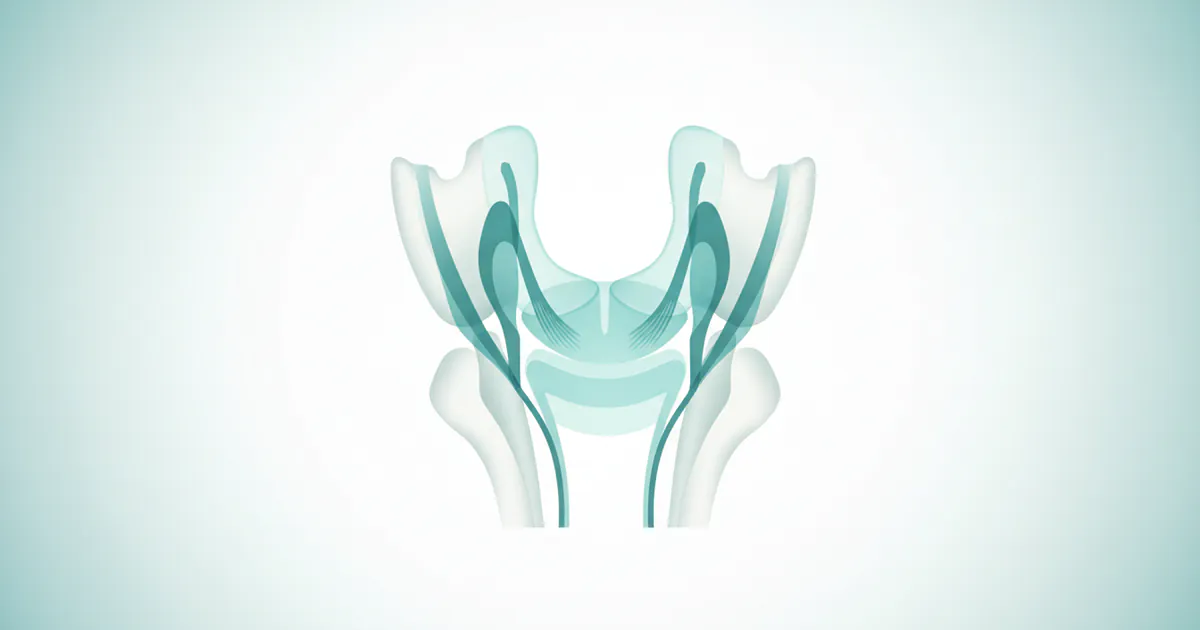
The temporomandibular joint (TMJ) is truly one of the most complex joints in the human body, allowing for a wide range of jaw movements crucial for everyday life. It's a bilateral synovial joint, meaning there are two joints—one on each side of your head—that must work in perfect synchrony. Each TMJ is a combination hinge and sliding joint, capable of both rotation and translation, making it uniquely versatile.

At its core, the temporomandibular joint is formed by the articulation of two main bones:
- Mandible (Jawbone): Specifically, the head of the condyle (a rounded projection) of the mandible.
- Temporal Bone (Skull): A depression in the temporal bone called the mandibular fossa (or glenoid fossa) and a rounded ridge just in front of it, the articular eminence.
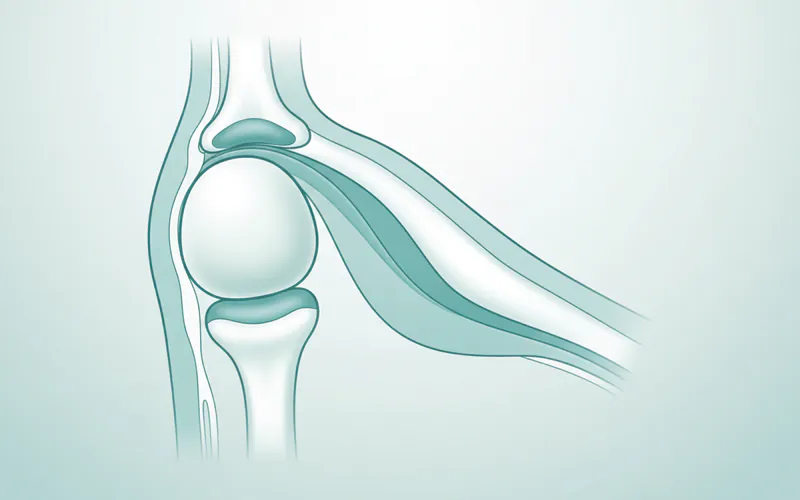
Beyond these bony structures, several other critical components contribute to the joint's function and stability:
The Articular Disc (Meniscus)
Perhaps the most crucial component for smooth TMJ function, the articular disc is a small, oval-shaped, biconcave (concave on both sides) piece of fibrous cartilage. It sits between the mandibular condyle and the temporal bone's fossa and eminence, essentially dividing the joint into two separate compartments:
- Superior Compartment: Between the disc and the temporal bone, primarily responsible for sliding (translation).
- Inferior Compartment: Between the disc and the mandibular condyle, primarily responsible for rotation (hinge movement).
The disc acts as a shock absorber, distributing forces evenly across the joint surfaces and facilitating smooth, frictionless movement. It is attached to the joint capsule and certain muscles, allowing it to move synchronously with the condyle. Any displacement or damage to this disc is a primary cause of TMJ disorders.
Joint Capsule and Ligaments
The entire TMJ is enclosed within a fibrous joint capsule that provides stability and contains the synovial fluid. This fluid lubricates the joint, nourishing the articular cartilage and facilitating smooth movement.
Several ligaments further reinforce the TMJ, limiting excessive movement and preventing dislocation:
- Temporomandibular Ligament (Lateral Ligament): The main stabilizing ligament, preventing posterior displacement of the mandible and limiting the extent of mouth opening.
- Sphenomandibular Ligament: Extends from the sphenoid bone to the inner surface of the mandible, acting as a passive support.
- Stylomandibular Ligament: Extends from the styloid process of the temporal bone to the angle of the mandible, helping limit excessive protrusion.
These ligaments are essential for maintaining the integrity and proper alignment of the joint during dynamic movements.
Muscles of Mastication
The movement of the temporomandibular joint is orchestrated by a group of powerful muscles known as the muscles of mastication. These muscles enable jaw closing, opening, protrusion (forward movement), retrusion (backward movement), and lateral (side-to-side) movements. They are often deeply involved in TMJ pain and dysfunction.
The primary muscles include:
- Masseter: The strongest muscle, responsible for jaw closing (elevation) and some protrusion. You can feel it bulge when you clench your teeth.
- Temporalis: A fan-shaped muscle on the side of the head, also responsible for jaw closing and retrusion.
- Medial Pterygoid: Works with the masseter to elevate and protrude the jaw, and aids in lateral movements.
- Lateral Pterygoid: This is the only muscle primarily responsible for opening the mouth (depression), as well as protrusion and lateral movements. It has two heads, superior and inferior, each with specific roles in disc and condyle movement.
Pro Tip: Understanding the interplay between these muscles and the joint structures is key. Often, muscle tension or spasms, particularly in the masseter and temporalis, can mimic or exacerbate TMJ pain, leading to what is known as myofascial pain dysfunction.
Types of TMJ Disorders (TMDs)
While the anatomy of the TMJ is universal, the disorders that affect it can manifest in various ways, often categorized into three main types based on the underlying issue:
- Myofascial Pain: This is the most common type of TMD and involves discomfort or pain in the muscles that control jaw function (masseter, temporalis, etc.) and in the neck and shoulder muscles. It often results from overuse, tension, or muscle imbalances. This type of pain does not necessarily indicate a problem with the joint itself but rather with the surrounding soft tissues.
- Internal Derangement of the Joint: This refers to a problem within the joint itself, specifically involving the articular disc.
- Disc Displacement with Reduction: The disc slips out of its normal position (usually anteriorly) when the mouth is closed but clicks back into place upon opening, producing a "click" or "pop" sound.
- Disc Displacement without Reduction: The disc remains displaced even when the mouth is open, blocking the condyle's movement and often leading to limited mouth opening (known as "closed lock"). This is typically more painful and restrictive.
- Perforation of the Disc: The disc can tear or develop a hole, compromising its shock-absorbing function and leading to grinding sounds (crepitus).
- Degenerative Joint Disease (Arthritis): This includes conditions like osteoarthritis or rheumatoid arthritis affecting the TMJ.
- Osteoarthritis: Caused by the breakdown of cartilage and bone in the joint, often due to wear and tear, trauma, or long-standing internal derangement. Leads to pain, stiffness, and crepitus.
- Rheumatoid Arthritis: An autoimmune disease that can affect any joint, including the TMJ, causing inflammation, pain, and potentially severe damage.
Some individuals may experience a combination of these types of TMDs, making diagnosis and treatment complex.
Causes / Why It Happens: The Roots of TMJ Dysfunction
Given the complexity of TMJ anatomy, it's not surprising that its dysfunction can stem from a multitude of factors, often acting in concert. Understanding these causes is crucial for effective prevention and treatment.
Anatomical and Structural Factors
- Disc Displacement: As discussed, the articular disc can slip out of its normal position. This can be due to trauma, chronic clenching/grinding, or lax ligaments.
- Arthritis: Degenerative changes (osteoarthritis) or inflammatory conditions (rheumatoid arthritis) can directly damage the joint surfaces and disc.
- Trauma: A direct blow to the jaw, a whiplash injury, or even prolonged wide-mouth opening (e.g., during dental procedures) can injure the joint structures, ligaments, or disc.
- Malocclusion (Bad Bite): While not a primary cause for all TMDs, a significant discrepancy in how the upper and lower teeth meet can sometimes put excessive strain on the TMJ. However, current research suggests malocclusion is less of a direct cause than once thought.
- Structural Anomalies: Congenital anomalies or developmental issues in the jaw bones or joint structures can predispose individuals to TMD.
Behavioral and Lifestyle Factors
- Bruxism (Teeth Grinding/Clenching): One of the most significant contributing factors. Chronic clenching and grinding, often stress-induced or occurring unconsciously during sleep, puts immense, sustained pressure on the TMJ and surrounding muscles. This can lead to muscle fatigue, pain, and disc displacement over time.
- Stress and Anxiety: High stress levels often manifest physically as increased muscle tension, including in the jaw and neck. This can exacerbate bruxism and myofascial pain.
- Habitual Jaw Movements: Chewing gum excessively, biting nails, frequently leaning on your chin, or habitually resting your jaw in an unnatural position can strain the joint.
- Poor Posture: Forward head posture, common with extended computer use, can shift the alignment of the jaw and neck, placing increased strain on the TMJ muscles.
Other Contributing Factors
- Dental Procedures: Prolonged mouth opening during dental work can sometimes strain the joint, leading to temporary or, in some cases, persistent issues.
- Systemic Conditions: Certain autoimmune diseases (beyond rheumatoid arthritis), fibromyalgia, and chronic fatigue syndrome can be associated with increased TMD symptoms.
- Hormonal Factors: There is some evidence suggesting a higher prevalence of TMDs in women, particularly during reproductive years, indicating a potential hormonal link.
- Genetics: A predisposition to chronic pain or inflammatory conditions might run in families.
It's important to note that for many people, the exact cause of their TMJ disorder remains elusive, often described as multifactorial.
Signs and Symptoms: Recognizing TMJ Disorders
The symptoms of tmj disorders can vary widely in intensity and presentation, making diagnosis challenging. They often mimic other conditions, so a thorough dental and medical evaluation is essential. If you experience one or more of these symptoms persistently, it's advisable to consult a dentist or a TMJ specialist.
Common Symptoms
- Pain or Tenderness:
- Jaw pain: Often felt in front of the ear, spreading to the cheek, temple, or neck.
- Earache: Pain deep inside or around the ear, often mistaken for an ear infection.
- Headache: Tension-type headaches, especially in the temples, forehead, or behind the eyes.
- Facial pain: Aching pain around the face, often worse when chewing or speaking.
- Neck and shoulder pain: Referred pain from jaw muscles or compensatory muscle tension.
- Joint Sounds:
- Clicking or popping: A distinct sound when opening or closing the mouth, often due to disc displacement with reduction. It may or may not be painful.
- Grating or grinding (crepitus): A rougher, sand-like sound, often indicating degenerative changes or perforation of the articular disc.
- Limited Jaw Movement or Locking:
- Difficulty opening the mouth wide: Restricted range of motion, making eating or yawning challenging.
- Jaw locking: The jaw gets "stuck" in an open or closed position, making it difficult to move. This often indicates disc displacement without reduction ("closed lock") or occasionally hypermobility ("open lock").
- Difficulty chewing: Pain or inability to chew hard foods effectively.
- Changes in Bite:
- Feeling that your upper and lower teeth no longer fit together correctly (malocclusion).
- A sudden change in the way your teeth meet.
- Other Symptoms:
- Dizziness or vertigo.
- Tinnitus (ringing in the ears).
- Hearing changes (muffled hearing or sensitivity to sound).
- Tooth sensitivity (often from clenching/grinding).
- Swelling on the side of the face.
- Fatigue in the jaw muscles.
Pro Tip: While clicking or popping sounds are common, they are not always indicative of a problem if they are not accompanied by pain or limited movement. Many people have asymptomatic jaw clicks. However, if new clicks develop with pain or stiffness, seek evaluation.
Treatment Options for TMJ Disorders
Treating TMDs often involves a conservative, step-by-step approach, starting with the least invasive options. The goal is to reduce pain, restore normal jaw function, and prevent further damage. The American Dental Association (ADA) generally supports reversible, non-surgical therapies as the first line of treatment.
A. Conservative (Non-Invasive) Treatments
These are often the first line of defense and are successful for many patients.
-
Self-Care and Lifestyle Modifications:
- Soft Diet: Avoiding hard, chewy, or crunchy foods to rest the jaw muscles.
- Moist Heat/Ice Packs: Applying heat to relax muscles or ice to reduce inflammation.
- Gentle Jaw Exercises: Specific stretches and exercises to improve jaw mobility and strengthen muscles, guided by a physical therapist.
- Stress Management: Techniques like meditation, yoga, or counseling to reduce overall tension and bruxism.
- Avoidance of Parafunctional Habits: Stopping gum chewing, nail biting, jaw clenching, and leaning on the chin.
- Good Posture: Maintaining proper head and neck alignment.
- Pain Relievers: Over-the-counter NSAIDs (non-steroidal anti-inflammatory drugs) like ibuprofen or naproxen for pain and inflammation.
-
Oral Appliances (Splints/Occlusal Guards):
- Description: Custom-made acrylic devices worn over the upper or lower teeth, primarily at night.
- Purpose: To reduce bruxism, stabilize the bite, relieve pressure on the TMJ, and allow jaw muscles to relax.
- Types:
- Stabilization Splints (Flat Plane Splints): Most common, designed to achieve an ideal bite relationship and muscle relaxation.
- Repositioning Splints: Designed to temporarily reposition the jaw and disc. Used less commonly and often only for short periods.
- Pros: Non-invasive, reversible, often highly effective, protects teeth from wear.
- Cons: Requires consistent wear, can be costly, may not be a permanent solution.
-
Physical Therapy:
- Description: A therapist guides you through exercises, stretches, massage, and modalities like ultrasound or TENS (transcutaneous electrical nerve stimulation).
- Purpose: To improve range of motion, strengthen jaw muscles, reduce pain, and correct posture.
- Pros: Non-invasive, teaches self-management techniques.
- Cons: Requires commitment and consistent follow-through, results can take time.
-
Medications:
- Prescription NSAIDs: Stronger anti-inflammatories.
- Muscle Relaxants: To alleviate muscle spasms and pain.
- Tricyclic Antidepressants: In low doses, can help reduce pain, improve sleep, and manage bruxism, even without treating depression.
- Botulinum Toxin (Botox): Injections into jaw muscles (masseter, temporalis) can relax them, reducing pain and clenching. Not ADA-approved specifically for TMD, but widely used off-label.
B. Minimally Invasive Procedures
If conservative treatments are insufficient, these options may be considered.
-
Arthrocentesis:
- Description: A procedure involving the insertion of two needles into the joint to lavage (wash out) the joint space with sterile fluid.
- Purpose: To remove inflammatory byproducts, release adhesions, and improve joint lubrication.
- Pros: Minimally invasive, relatively quick recovery, can provide significant pain relief.
- Cons: Not always a permanent solution, may require repeat procedures.
-
Injections:
- Corticosteroid Injections: Directly into the joint to reduce inflammation and pain.
- Hyaluronic Acid Injections (Viscosupplementation): To improve joint lubrication, similar to knee injections.
- Trigger Point Injections: Local anesthetic and/or steroid injected into specific muscle knots.
- Pros: Can provide temporary to long-lasting relief, avoids surgery.
- Cons: Risks of infection or local tissue damage, effects can be temporary.
C. Surgical Interventions
Surgery is typically reserved for severe cases where conservative and minimally invasive approaches have failed, or when there is significant structural damage that requires repair.
-
Arthroscopy:
- Description: A minimally invasive surgical procedure where a tiny incision is made, and a small camera (arthroscope) is inserted into the joint. Surgical instruments can then be used to remove inflamed tissue, wash out the joint, or reposition the disc.
- Purpose: Diagnostic and therapeutic.
- Pros: Less invasive than open surgery, quicker recovery, smaller scars.
- Cons: Not suitable for all types of structural damage, limited scope for complex repairs.
-
Open-Joint Surgery (Arthroplasty):
- Description: Involves making an incision in front of the ear to directly access the joint.
- Purpose: To repair or replace the articular disc, remove adhesions, reshape the condyle or fossa, or replace the entire joint (total joint replacement).
- Pros: Allows for comprehensive repair of severe structural damage.
- Cons: Most invasive option, longer recovery time, higher risk of complications (nerve damage, infection, scarring), typically a last resort.
-
Condylotomy:
- Description: A procedure where the mandibular condyle is surgically cut and repositioned to improve alignment and reduce pain, without opening the joint capsule.
- Purpose: To correct certain types of bite problems and reduce joint loading.
- Pros: Can be effective for specific alignment issues.
- Cons: Invasive, requires careful patient selection.
D. Step-by-Step Treatment Process Overview
What to expect during a typical TMJ treatment journey:

- Initial Consultation & Diagnosis: Your dentist will take a detailed medical history, perform a physical examination of your jaw, neck, and facial muscles, and listen for joint sounds. X-rays, MRI, or CT scans may be ordered to assess the bone and soft tissue structures of the TMJ. This phase is critical for accurate diagnosis and typically costs $150 - $500 without insurance, varying by specialist.
- Phase 1: Conservative Management (Weeks to Months):
- Begin with self-care, lifestyle modifications, and over-the-counter pain relief.
- If no improvement, an oral splint (night guard) may be prescribed, along with physical therapy.
- Medications (muscle relaxants, NSAIDs) might be used temporarily.
- Regular follow-ups (every 2-4 weeks) to monitor progress and adjust treatment.
- Phase 2: Minimally Invasive Options (If needed):
- If conservative approaches fail after 3-6 months, injections (corticosteroids, Botox, hyaluronic acid) or arthrocentesis may be considered. These are usually outpatient procedures.
- Phase 3: Surgical Intervention (Last Resort):
- If severe pain and dysfunction persist despite all other treatments, and significant anatomical damage is identified, surgical consultation for arthroscopy or open-joint surgery will be recommended. This involves pre-surgical evaluations, the surgery itself, and an intensive post-operative recovery period.
Pro Tip: Always seek a second opinion before committing to irreversible treatments like surgery. Look for specialists with extensive experience in TMD.
Cost and Insurance: Navigating TMJ Treatment Expenses in the US
The cost of TMJ treatment in the United States can vary significantly based on the severity of the condition, the type of treatment chosen, the practitioner's fees, and your geographic location. Understanding these costs and insurance coverage is vital.
Average US Price Ranges (Without Insurance)
- Initial Consultation & Diagnosis (including X-rays/Imaging):
- General Dentist: $150 - $300
- TMJ Specialist/Oral Surgeon: $300 - $700 (for initial visit; imaging like MRI can add $500 - $2,000)
- Conservative Treatments:
- Oral Splint/Night Guard: Custom-made appliances range from $300 - $1,200. High-end splints with specialized designs can be $1,500 - $2,500.
- Physical Therapy: $75 - $200 per session. A typical course might involve 6-12 sessions, totaling $450 - $2,400.
- Medications: Over-the-counter NSAIDs are inexpensive. Prescription muscle relaxants or antidepressants can range from $10 - $100 per month, depending on the drug and insurance.
- Minimally Invasive Procedures:
- Botox Injections: $400 - $1,500 per treatment, often requiring repeat injections every 3-6 months. Cost varies by units used.
- Corticosteroid Injections: $150 - $500 per injection.
- Arthrocentesis: $1,000 - $3,000 per joint.
- Surgical Interventions:
- TMJ Arthroscopy: $5,000 - $15,000 per joint, depending on complexity.
- Open-Joint Surgery (Arthroplasty): $10,000 - $25,000+ per joint.
- Total Joint Replacement: Can exceed $30,000 - $50,000+ per joint, often covered more by medical insurance due to complexity.
Cost by Region: Major metropolitan areas (e.g., New York, Los Angeles) typically have higher costs compared to rural or less populated regions. For example, a custom oral splint might be $800 in a rural area versus $1,500 in a major city.
Insurance Coverage Details
Navigating insurance for TMD can be complex because it often straddles the line between dental and medical coverage.
- Dental Insurance: Often covers diagnosis (exams, X-rays) and some non-surgical treatments like oral splints (under "occlusal guard" or "splint therapy"). Coverage varies greatly; some plans might cover 50-80% after your deductible, up to your annual maximum. They generally do not cover surgical procedures.
- Medical Insurance: More likely to cover complex diagnostic imaging (MRI, CT scans) and surgical procedures, especially if the condition is deemed "medically necessary" and not purely dental. Physical therapy and prescription medications are also typically covered by medical insurance. You will need to check your deductible, co-pays, and out-of-pocket maximums. Often requires a referral from a primary care physician or dentist.
- Pre-authorization: For more expensive treatments like surgery or certain injections, pre-authorization from your insurance company is almost always required. Without it, you could be responsible for the full cost.
- Payment Plans and Financing: Many dental and medical offices offer in-house payment plans. Third-party financing options like CareCredit are also widely used, allowing you to pay for treatments over time with interest or interest-free periods.
Cost-Saving Tips
- Verify Insurance Coverage: Contact both your dental and medical insurance providers before treatment to understand what's covered. Ask for specific CPT codes for procedures.
- Start with Conservative Care: These are often less expensive and can be highly effective, potentially avoiding costly advanced treatments.
- Shop Around (Carefully): Get quotes from a few different reputable providers, but prioritize expertise and patient reviews over price alone.
- Negotiate Cash Prices: If you don't have insurance, ask if there's a discount for paying in cash upfront.
- Consider University Dental Schools: These often offer lower costs for treatment, performed by supervised students or residents.
Recovery and Aftercare
Recovery from TMJ disorders varies greatly depending on the severity of the condition and the type of treatment received. Consistent aftercare is crucial for long-term success.
After Conservative Treatments
- Oral Splint Use: Consistent wear as prescribed (e.g., every night). Clean the splint daily.
- Continued Self-Care: Maintain soft diet, stress reduction techniques, gentle jaw exercises, and good posture.
- Regular Follow-ups: Periodic visits to your dentist or specialist to adjust the splint and monitor progress.
- Pain Management: Continue with OTC pain relievers as needed, gradually reducing reliance.
After Minimally Invasive Procedures (Arthrocentesis, Injections)
- Immediate Post-Procedure: Some soreness, swelling, or bruising at the injection site or around the jaw is common. Ice packs can help.
- Activity Restriction: Your doctor may advise avoiding strenuous activities or hard chewing for a day or two.
- Physical Therapy: Often recommended post-procedure to maximize benefits, improve range of motion, and prevent stiffness.
- Results: Pain relief can be immediate or take a few days/weeks to become noticeable. Effects can be temporary, requiring repeat procedures.
After Surgical Interventions (Arthroscopy, Open-Joint Surgery)
- Hospital Stay: Arthroscopy is often outpatient or a short overnight stay. Open-joint surgery may require a longer hospital stay (1-3 days).
- Pain and Swelling: Significant post-operative pain and swelling are expected. Pain medication will be prescribed. Ice packs are critical for the first 24-48 hours.
- Diet: A soft or liquid diet will be necessary for several days to weeks, gradually transitioning back to solid foods.
- Physical Therapy: Essential for regaining jaw mobility and strength. This is a critical component of recovery, often starting soon after surgery and continuing for several weeks or months.
- Activity Restrictions: Avoid strenuous activity, heavy lifting, and any impact to the jaw for several weeks.
- Follow-up Appointments: Regular visits to monitor healing, remove sutures, and adjust physical therapy.
- Full Recovery: Can take anywhere from several weeks to several months, depending on the extent of the surgery. Complete resolution of symptoms is not guaranteed, but significant improvement is the goal.
Pro Tip: Adherence to physical therapy exercises and all post-operative instructions is paramount for successful surgical outcomes and preventing reoccurrence. Neglecting these can lead to stiffness, limited range of motion, or even re-injury.
Prevention: Safeguarding Your Temporomandibular Joints
Preventing TMJ disorders often boils down to managing stress, protecting your jaw from undue strain, and maintaining overall oral health. Since many TMDs are multifactorial, a holistic approach is most effective.
- Manage Stress: Stress is a major contributor to bruxism and muscle tension. Incorporate stress-reduction techniques into your daily routine, such as:
- Mindfulness and meditation
- Yoga or deep breathing exercises
- Regular physical activity
- Adequate sleep
- Seeking counseling if stress feels overwhelming.
- Protect Your Jaw from Overuse and Trauma:
- Avoid Hard/Chewy Foods: Limit gum chewing, sticky candies, and very hard foods that require excessive jaw effort.
- Don't Wide Yawn: Support your chin with your hand during a wide yawn to prevent overextension.
- Maintain Good Posture: Be mindful of your posture, especially if you spend a lot of time at a computer. Keep your head aligned over your shoulders, not jutted forward.
- Avoid Resting Chin on Hand: This puts uneven pressure on the TMJ.
- Practice Jaw Awareness: Notice if you are clenching your jaw during the day, especially when concentrating or stressed, and consciously relax it. A useful reminder is "lips together, teeth apart."
- Address Bruxism: If you grind or clench your teeth, especially at night, discuss this with your dentist. A night guard can protect your teeth and jaw joints from damaging forces.
- Regular Dental Check-ups: Your dentist can identify early signs of bruxism, malocclusion, or jaw joint issues. They can also provide guidance on proper oral hygiene and bite assessment.
- Ergonomic Adjustments: Ensure your workstation is ergonomically set up to prevent neck and shoulder strain that can refer pain to the jaw.
Risks and Complications of TMJ Disorders and Treatments
While many TMJ disorders are successfully managed with conservative treatments, there are potential risks associated with both the untreated condition and more aggressive interventions.
Risks of Untreated TMJ Disorders
- Chronic Pain: Persistent and worsening pain in the jaw, face, head, and neck.
- Progressive Joint Damage: Untreated disc displacement or chronic inflammation can lead to irreversible degenerative changes in the joint (osteoarthritis), including bone erosion.
- Permanent Limited Mouth Opening: "Closed lock" can become permanent, severely impacting eating and speech.
- Nutritional Deficiencies: Inability to chew a wide variety of foods can lead to poor nutrition.
- Psychological Impact: Chronic pain can lead to depression, anxiety, social isolation, and reduced quality of life.
- Sleep Disturbances: Pain and discomfort can interfere with sleep, creating a vicious cycle.
Risks and Complications of TMJ Treatments
While generally safe, all medical and dental procedures carry some risks:
- Oral Appliances (Splints):
- Initial discomfort or speech changes.
- Can potentially shift bite if not properly designed or monitored (rare but possible with poorly managed repositioning splints).
- Allergic reaction to material (rare).
- Medications:
- Side effects (e.g., drowsiness with muscle relaxants, stomach upset with NSAIDs).
- Dependence on pain medication.
- Injections (Corticosteroid, Botox):
- Pain, swelling, bruising at the injection site.
- Infection (rare).
- Temporary facial weakness or asymmetry (with Botox if injected improperly).
- Damage to surrounding tissues or nerves.
- Temporary flare-up of pain.
- Arthrocentesis:
- Pain, swelling, bruising.
- Infection (rare).
- Damage to joint structures or nerves (very rare).
- Surgical Interventions (Arthroscopy, Open-Joint Surgery):
- General Surgical Risks: Infection, excessive bleeding, adverse reaction to anesthesia.
- Specific TMJ Surgical Risks:
- Nerve Damage: Damage to the facial nerve (can cause temporary or permanent facial weakness or paralysis) or other sensory nerves, leading to numbness.
- Scarring: Visible scarring, especially with open-joint surgery.
- Limited Mouth Opening: Can sometimes worsen after surgery due to scar tissue formation.
- Continued Pain: Surgery does not guarantee complete pain relief for everyone.
- Failure of Procedure: Need for revision surgery or further treatment.
- Hearing Loss: Very rare, due to proximity to the ear structures.
- Heterotopic Ossification: Abnormal bone formation in soft tissues, potentially limiting movement.
It's crucial to have a thorough discussion with your healthcare provider about all potential risks and benefits before making treatment decisions.
Comparison Tables
Table 1: Common TMJ Treatment Options Overview
| Treatment Type | Description | Pros | Cons | Avg. Cost Range (US) | Recovery/Timeline |
|---|---|---|---|---|---|
| Oral Splint (Night Guard) | Custom-made acrylic device worn over teeth. | Non-invasive, reversible, protects teeth. | Requires consistent wear, not a cure for all TMDs. | $300 - $1,500 | Weeks to months for symptom improvement. |
| Physical Therapy | Guided exercises, stretches, massage, posture correction. | Non-invasive, empowers self-management, drug-free. | Requires commitment, results take time. | $450 - $2,400 (6-12 sessions) | Ongoing, with initial results in weeks. |
| Medications | NSAIDs, muscle relaxants, antidepressants, Botox injections. | Can provide rapid relief, non-invasive (except Botox). | Side effects, temporary relief, not a long-term solution. | $10 - $100/mo (Rx) | Varies. Botox: 3-6 months. |
| Arthrocentesis | Joint lavage with sterile fluid via needles. | Minimally invasive, quick procedure, often effective. | Temporary relief for some, not suitable for all issues. | $1,000 - $3,000 | Few days of discomfort, full recovery in 1-2 weeks. |
| TMJ Arthroscopy | Minimally invasive surgery with small camera and instruments. | Less invasive than open surgery, quicker recovery. | Limited scope for complex repairs, not always permanent fix. | $5,000 - $15,000 | 2-4 weeks for initial recovery, months for full return. |
| Open-Joint Surgery | Direct access to joint via incision for repair/replacement. | Addresses severe structural damage directly. | Most invasive, longer recovery, higher complication risk. | $10,000 - $25,000+ | Months of recovery, extensive physical therapy. |
Table 2: Insurance Coverage for TMJ Treatments
| Treatment Type | Typical Dental Insurance Coverage | Typical Medical Insurance Coverage | Notes |
|---|---|---|---|
| Initial Exam/Diagnosis | Partial (50-80%) | Varies, often for specialist consult | Imaging (MRI/CT) usually medical. |
| Oral Splint | Partial (50-80%) | Rarely | May be covered under "occlusal guard." |
| Physical Therapy | Rarely | Good (50-80%) | Often requires a physician's referral. |
| Medications | Rarely | Good (50-90% for Rx) | Check your specific prescription plan. |
| Botox Injections | Rarely | Possible (variable) | Often considered "off-label," may require appeals or specific criteria. |
| Arthrocentesis | Varies (limited) | Good (50-80%) | Often considered a surgical procedure by medical plans. |
| TMJ Arthroscopy | Rarely | Good (50-80%) | Requires pre-authorization, high deductible may apply. |
| Open-Joint Surgery | Rarely | Good (50-80%) | Requires extensive pre-authorization, highest deductible. |

Children / Pediatric Considerations
TMJ disorders are less common in children than in adults, but they can occur and often present with unique challenges. The developing jaw and growth plates mean that careful diagnosis and treatment are crucial.
Causes in Children
- Trauma: Falls, sports injuries, or direct blows to the jaw are common causes.
- Rheumatoid Arthritis: Juvenile idiopathic arthritis can affect the TMJ, leading to pain, swelling, and potential growth disturbances in the jaw.
- Bruxism: Teeth grinding is very common in children, often related to stress, airway issues (like enlarged tonsils/adenoids), or sleep disorders. While often outgrown, severe or persistent bruxism can contribute to TMD.
- Orthodontic Treatment: While often beneficial, in rare cases, prolonged or aggressive orthodontic forces can sometimes exacerbate pre-existing TMJ issues.
- Congenital Abnormalities: Rare cases of developmental issues with the jaw or TMJ structures.
Signs and Symptoms in Children
Symptoms can be similar to adults but may be less obvious or difficult for younger children to articulate:
- Jaw pain, earache, or headaches.
- Clicking or popping sounds in the jaw.
- Difficulty chewing, especially hard foods.
- Limited mouth opening.
- Changes in bite.
- Unexplained facial swelling.
- Reluctance to open mouth wide for dental exams.
Diagnosis and Treatment
- Conservative First: Similar to adults, conservative approaches are always preferred. This includes soft diets, warm compresses, gentle exercises, and stress management.
- Orthodontic Consultation: If malocclusion is a significant factor, an orthodontist may be involved.
- Physical Therapy: Specialized pediatric physical therapy for jaw and facial muscles can be very effective.
- Oral Appliances: Custom-made oral appliances can be used, but careful monitoring is needed to ensure they don't interfere with jaw growth.
- Medications: NSAIDs for pain, with careful dosing based on age and weight.
- Surgery: Extremely rare and only considered in very severe cases of structural damage or growth disturbance that cannot be managed otherwise.
- Multidisciplinary Approach: Often, a team including a pediatric dentist, orthodontist, oral surgeon, physical therapist, and potentially a rheumatologist (if arthritis is suspected) is best.
Pro Tip for Parents: If your child complains of persistent jaw pain, earaches without infection, or you notice jaw clicking/grinding, consult a pediatric dentist or an oral and maxillofacial surgeon experienced in pediatric TMJ issues. Early intervention can prevent long-term complications.
Frequently Asked Questions
What does "temporomandibular" actually mean?
"Temporomandibular" refers to the two bones that form the joint. "Temporo-" relates to the temporal bone of the skull, which contains the socket for the joint. "-mandibular" refers to the mandible, which is your jawbone that fits into that socket. So, it literally describes the joint where your jawbone meets your temporal bone.
Can TMJ disorders be cured permanently?
For many people, TMJ disorders can be effectively managed and symptoms significantly reduced or eliminated, often with conservative treatments. However, a "cure" implies that the underlying anatomical or physiological predispositions are entirely gone, which isn't always the case, especially with chronic conditions like arthritis or disc displacement. Long-term management and adherence to preventive measures are often necessary.
How long does it take to recover from TMJ pain?
Recovery time varies widely. Mild cases of muscle pain may improve within a few days or weeks with self-care. More complex issues involving disc displacement or chronic pain can take several months of consistent treatment. Surgical recovery can extend for several months, with full functional recovery taking up to a year.
Is TMJ pain always accompanied by clicking or popping sounds?
No, TMJ pain is not always accompanied by clicking or popping sounds. While these sounds are common symptoms of tmj internal derangement, many individuals experience significant pain from muscle issues (myofascial pain) or arthritis without any audible joint sounds. Conversely, some people have jaw clicks without any pain or functional problems.
Are there home remedies for TMJ pain?
Yes, many effective home remedies can provide significant relief for TMJ pain, especially for mild to moderate cases. These include applying moist heat or ice packs, eating a soft diet, avoiding excessive jaw movements, practicing gentle jaw stretches, and using over-the-counter pain relievers like ibuprofen. Stress reduction techniques are also crucial for managing tension-related TMJ pain.
How much does an MRI for TMJ typically cost?
An MRI (Magnetic Resonance Imaging) for TMJ can cost anywhere from $500 to $2,000 or more in the US, without insurance. The price depends on the facility, your location, and whether contrast dye is used. Medical insurance typically covers a portion of the cost if deemed medically necessary by a referring physician or specialist.
Can my bite be permanently changed by TMJ issues?
Yes, chronic or severe TMJ issues, especially those involving disc displacement or degenerative changes within the joint, can lead to permanent changes in your bite (malocclusion). This is because the position of your jaw, and thus how your teeth come together, is directly influenced by the health and alignment of your temporomandibular joints.
What are some alternatives to surgery for severe TMJ?
Before considering surgery, alternatives include comprehensive physical therapy, targeted injections (Botox, corticosteroids, hyaluronic acid), arthrocentesis (joint lavage), and prolonged use of custom oral appliances. A multidisciplinary approach involving various specialists is often employed to exhaust all non-surgical options before moving to invasive procedures.
Does dental insurance cover TMJ surgery?
Typically, dental insurance does not cover TMJ surgery. Surgical interventions for the temporomandibular joint are generally considered medical procedures and are usually covered by your medical insurance, not your dental plan. However, coverage still depends on your specific medical insurance policy, deductible, and whether the procedure is deemed medically necessary and pre-authorized.
Can TMJ pain be a sign of a more serious condition?
While most TMJ pain is not life-threatening, it can sometimes be a symptom of a more serious underlying condition. For example, severe and rapidly progressing pain could indicate significant joint degeneration, infection, or even, rarely, tumors in the surrounding areas. Persistent, worsening, or atypical symptoms should always be evaluated by a healthcare professional to rule out other serious conditions.
When to See a Dentist
Recognizing when to seek professional help for your jaw discomfort is key to preventing escalation of TMJ disorders. While occasional jaw stiffness or a minor click might resolve on its own, certain signs warrant a prompt visit to your dentist or a TMJ specialist.
You should schedule an appointment if you experience any of the following:
- Persistent Pain: Jaw pain, ear pain, headaches, or facial pain that doesn't subside within a few days, even with self-care measures.
- Limited Jaw Movement: Difficulty opening your mouth wide, making it hard to eat, speak, or yawn.
- Jaw Locking: Your jaw gets stuck in an open or closed position, even momentarily. This is a significant red flag.
- Painful Clicking or Popping: While asymptomatic clicks might be harmless, any clicking or popping that is accompanied by pain, stiffness, or changes in your bite needs evaluation.
- Grating or Grinding Sensations (Crepitus): A rough, gritty sound or feeling in your jaw joint, which can indicate degenerative changes.
- Changes in Your Bite: A sudden feeling that your teeth no longer fit together properly, or new gaps appearing between your teeth.
- Facial Swelling: Unexplained swelling on one or both sides of your face near the jaw joint.
- Inability to Chew: If pain makes it difficult or impossible to chew food properly.
Red Flags for Immediate Attention (Emergency vs. Scheduled):
- Sudden, Severe Jaw Locking: If your jaw locks completely and you cannot move it at all, especially if it's painful, seek immediate dental or medical attention. This could be an acute disc displacement without reduction.
- Acute Trauma: If you've experienced a direct blow to the jaw, a car accident (whiplash), or a fall that resulted in significant jaw pain, swelling, or difficulty moving, go to an urgent care center or emergency room to rule out fractures or severe joint damage.
- Signs of Infection: Intense pain accompanied by fever, redness, warmth, and pus drainage around the jaw joint. This is rare but requires urgent medical care.
For most other symptoms, a scheduled appointment with your general dentist is the appropriate first step. They can assess your condition, provide initial recommendations, or refer you to a specialist such as an oral and maxillofacial surgeon, a prosthodontist, or a TMJ specialist who focuses on complex jaw disorders. Early intervention can significantly improve outcomes and prevent the progression of TMJ issues.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Tmj Massage Near Me: Complete Guide
Temporomandibular joint disorder, commonly known as TMJD, affects millions of Americans, causing debilitating pain, discomfort, and significantly impacting quality of life. If you're experiencing jaw pain, clicking, or difficulty chewing, you're not alone. Up to 15% of American adults experience
February 23, 2026
Tmd Treatment: Complete Guide
Experiencing persistent jaw pain, clicking sounds when you chew, or debilitating headaches that seem to originate from your face? You're not alone. Temporomandibular joint (TMJ) disorders, often referred to collectively as TMD, affect an estimated 10 million Americans, with women disproportionat
February 23, 2026
Tmj Nerve Damage Symptoms: Complete Guide
Experiencing persistent facial pain, numbness, or tingling can be distressing, especially when the source is unclear. While many people are familiar with general jaw pain associated with temporomandibular joint (TMJ) disorders, the less commonly understood aspect of tmj nerve damage symptoms can
February 23, 2026
Remi Night Guard: Complete Guide
Remi Night Guard: Complete Guide
February 23, 2026