Tmj Exercises: Complete Guide

Key Takeaways
- Experiencing persistent jaw pain, clicking, or limited mouth movement can be incredibly frustrating and significantly impact your daily life. If you're one of the over 10 million Americans affected by temporomandibular joint (TMJ) disorders, you understand this reality firsthand. While the disco
Tmj Exercises: Complete Guide
Experiencing persistent jaw pain, clicking, or limited mouth movement can be incredibly frustrating and significantly impact your daily life. If you're one of the over 10 million Americans affected by temporomandibular joint (TMJ) disorders, you understand this reality firsthand. While the discomfort can be debilitating, effective solutions exist, and a cornerstone of many successful treatment plans involves TMJ exercises. These targeted movements, when performed correctly and consistently, can offer significant relief, improve jaw function, and contribute to long-term management of TMJ pain.

This comprehensive guide from SmilePedia.net will delve deep into the world of TMJ exercises, providing you with medically accurate, actionable information. We’ll explore what TMJ disorders are, why they occur, the specific types of exercises that can help, and how to integrate them into a broader treatment strategy. From understanding the underlying causes to navigating treatment options, costs, and recovery, this article aims to be your definitive resource for managing and potentially overcoming your TMJ challenges. You'll learn step-by-step techniques, discover when professional intervention is necessary, and gain insights into preventing future flare-ups, ultimately empowering you to regain comfort and control over your jaw health.
Key Takeaways:
- TMJ Exercises are a Core Treatment: They are often the first line of defense, focusing on improving jaw mobility, strengthening muscles, and reducing pain.
- Consistency is Crucial: Regular, gentle exercise routines (often 2-3 times a day for 5-10 minutes) are vital for noticeable improvement, typically seen within 2-6 weeks.
- Professional Guidance is Recommended: While many exercises can be done at home, a dentist or physical therapist can diagnose correctly and tailor an exercise plan, crucial for preventing worsening symptoms.
- Costs Vary Widely: Initial dental/medical consultations range from $100-$300. Physical therapy sessions can cost $75-$250 per session, with insurance often covering a portion. Home exercises are low-cost.
- TMJ Disorders Are Multifactorial: Causes range from bruxism and stress to injury and arthritis, necessitating a holistic approach to treatment.
- No Single "Cure": While TMJ exercises can provide significant relief and long-term management, "curing TMJ permanently" often involves addressing underlying causes and a combination of therapies, not just exercises.
- Prevention is Key: Stress management, good posture, and avoiding habits like clenching can significantly reduce the risk of developing or worsening TMJ symptoms.
What It Is / Overview
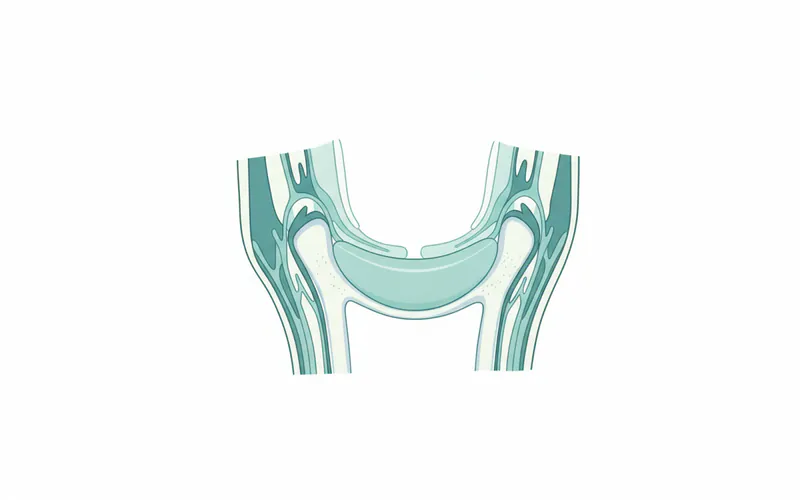
The temporomandibular joint (TMJ) is a complex and highly active joint connecting your jawbone (mandible) to your skull (temporal bone). Located on each side of your head, just in front of your ears, these two joints are crucial for a wide range of essential functions, including chewing, speaking, swallowing, and even facial expressions. Imagine the TMJ as a sliding hinge, capable of both rotational and translational movements, allowing your jaw to open and close, move side to side, and protrude forward.
Within each TMJ, a small, soft, oval-shaped disc made of cartilage acts as a cushion between the bones. This disc absorbs shock and ensures smooth, frictionless movement of the jaw. Surrounding the joint are various muscles, ligaments, and nerves that work in harmony to control jaw movement and provide stability.
When something goes wrong with these joints or the muscles and ligaments supporting them, it can lead to a group of conditions collectively known as Temporomandibular Disorders (TMD). While "TMJ" is often used colloquially to refer to the disorder, it technically refers to the joint itself. TMD refers to the actual problems or pain affecting the joint and its surrounding structures.
TMDs are remarkably common, affecting an estimated 10-15% of the adult US population at any given time, according to data from the National Institute of Dental and Craniofacial Research (NIDCR). They are more prevalent in women than men, particularly those aged 20-40. The symptoms can range from mild discomfort to severe, debilitating pain, significantly impacting an individual's quality of life. Understanding the intricate mechanics of the TMJ is the first step toward appreciating how targeted exercises can help restore balance and function.
Types / Variations of TMJ Issues
TMJ disorders are not a single condition but rather a broad category encompassing various problems that affect the jaw joint and its associated muscles. Understanding the specific type of TMJ issue is crucial for determining the most effective treatment approach, including the appropriate TMJ exercises. The American Dental Association (ADA) recognizes several classifications of TMD:
1. Myofascial Pain (Muscle-Related TMJ)
This is the most common type of TMD, characterized by pain in the muscles that control jaw function (the masticatory muscles) and the muscles of the neck and shoulders. Myofascial pain can stem from overuse, tension, or injury to these muscles.
- Causes: Often linked to stress, teeth clenching (bruxism), teeth grinding (sleep bruxism), poor posture, or habits like excessive gum chewing.
- Symptoms: Dull, aching pain in and around the jaw, temples, ear, neck, and shoulders. Tenderness in jaw muscles upon palpation, limited jaw opening due to muscle tightness, and headaches.
- Exercise Focus: Relaxation, stretching, and strengthening exercises aimed at releasing muscle tension and improving muscle coordination.
2. Internal Derangement of the Joint (Disc-Related TMJ)
This category involves a problem with the disc or cartilage within the temporomandibular joint. The disc can be displaced, usually forward, preventing the smooth movement of the jaw.
- Disc Displacement with Reduction: The disc slips out of place when the mouth is closed but pops back into place upon opening, often causing a clicking, popping, or clunking sound. The jaw can typically open fully.
- Disc Displacement without Reduction: The disc remains displaced even when the mouth is open, blocking the jaw's full range of motion. This can lead to a "locked" jaw and significant difficulty opening the mouth widely.
- Causes: Trauma, ligament laxity, degenerative changes, or chronic muscle imbalance that pulls the disc out of position.
- Symptoms: Clicking, popping, or grinding sounds (crepitus), pain within the joint, limited jaw opening, jaw locking (open or closed), and sometimes ear pain.
- Exercise Focus: Gentle range-of-motion exercises, stabilization exercises, and techniques to encourage disc repositioning and maintain joint lubrication.
3. Degenerative Joint Disease (Arthritis-Related TMJ)
Similar to other joints in the body, the TMJ can be affected by various forms of arthritis.
- Osteoarthritis: The cartilage disc wears down, and the underlying bone changes, leading to pain and reduced joint function. This is more common in older adults.
- Rheumatoid Arthritis: An autoimmune disease that can affect the TMJ, causing inflammation, pain, and eventual joint damage.
- Causes: Age-related wear and tear, injury, chronic inflammation.
- Symptoms: Pain, stiffness, grinding sounds (crepitus), limited movement, swelling in the joint area.
- Exercise Focus: Gentle, non-weight-bearing range-of-motion exercises to maintain flexibility and lubrication, avoiding high-impact or resisted movements.
4. Trauma-Induced TMJ
Direct injury to the jaw, joint, or surrounding muscles can lead to TMD.
- Causes: Whiplash, direct blow to the jaw, sports injuries, or dental procedures requiring prolonged mouth opening.
- Symptoms: Acute pain, swelling, bruising, limited movement, and potential fracture.
- Exercise Focus: After initial healing, a gradual introduction of gentle stretching and range-of-motion exercises under professional guidance to restore function.
It's important to note that many individuals with TMD may experience a combination of these issues, making diagnosis and treatment planning complex. A thorough examination by a dental professional or TMJ specialist is essential to accurately identify the specific problem and tailor an appropriate treatment strategy, including the most beneficial TMJ exercises.
Causes / Why TMJ Pain Happens
The origins of TMJ pain are often multifactorial, meaning several elements can contribute to its development. Pinpointing the exact cause can be challenging, but understanding common contributing factors is vital for effective management and prevention.
1. Bruxism (Teeth Clenching and Grinding)
One of the most common culprits, bruxism involves clenching your jaw or grinding your teeth, often unconsciously while awake (awake bruxism) or during sleep (sleep bruxism).
- Impact: This places immense, sustained pressure on the TMJ and surrounding muscles, leading to muscle fatigue, inflammation, and disc displacement. Over time, it can wear down tooth enamel and damage the joint.
- Triggers: Stress, anxiety, certain medications, malocclusion (misalignment of teeth), and sleep disorders.
2. Stress and Anxiety
Emotional stress and anxiety frequently manifest physically, with the jaw being a prime target.
- Impact: Chronic stress can lead to increased muscle tension throughout the body, including the jaw muscles. This sustained tension contributes to myofascial pain and exacerbates bruxism.
- Mechanism: The body's "fight or flight" response, when activated frequently, keeps muscles in a state of readiness, leading to overuse and fatigue.
3. Trauma or Injury
Direct impact to the jaw, head, or neck can damage the TMJ or its surrounding structures.
- Examples: A car accident (whiplash), a sports injury, a fall, or even a prolonged dental procedure requiring the mouth to be open for an extended period.
- Impact: Can cause disc displacement, ligament tears, fractures, or inflammation within the joint.
4. Arthritis and Other Inflammatory Conditions
Degenerative diseases or autoimmune conditions can affect the TMJ.
- Osteoarthritis: The breakdown of cartilage in the joint, common with aging or injury, leading to pain, stiffness, and reduced mobility.
- Rheumatoid Arthritis: An autoimmune disease that can cause inflammation and destruction of joint tissues, including the TMJ.
- Impact: Directly damages the joint structure, causing pain, crepitus (grinding sounds), and progressive limitation of movement.
5. Malocclusion (Bad Bite)
While historically considered a primary cause, the role of an imperfect bite in TMJ disorders is now understood to be less direct and more complex.
- Impact: In some cases, a significant misalignment of teeth or an improper bite can lead to uneven stress distribution across the TMJs and masticatory muscles. This can contribute to muscle fatigue and joint problems for certain individuals. However, many people with malocclusion never develop TMD.
6. Poor Posture
Chronic poor posture, particularly forward head posture, can significantly impact the jaw.
- Impact: When the head is consistently thrust forward (e.g., from prolonged computer use or looking down at phones), the neck and shoulder muscles become strained. This imbalance can pull the jaw out of its natural resting position, placing undue stress on the TMJ and surrounding muscles.
- Mechanism: The jaw is intimately connected to the cervical spine via muscles and ligaments. Poor neck posture can alter the resting length of jaw muscles, leading to tension and pain.
7. Connective Tissue Disorders
Conditions like Ehlers-Danlos syndrome, which affect collagen production, can lead to joint hypermobility and instability, including in the TMJ.
- Impact: Increased joint laxity can make the TMJ more susceptible to disc displacement and subluxation (partial dislocation).
Understanding these diverse causes helps explain why a multi-faceted approach, often including TMJ exercises, stress management, and professional dental or medical intervention, is frequently required for successful treatment.
Signs and Symptoms
Recognizing the signs and symptoms of a TMJ disorder is the first step toward seeking appropriate care. The manifestations can be varied and sometimes mimic other conditions, making accurate diagnosis by a healthcare professional essential. Look out for the following common indicators:
1. Jaw Pain or Tenderness
- Location: Often felt in the jaw joint itself, in front of the ear, but can also radiate to the face, neck, and shoulders.
- Characteristics: Can range from a dull ache to sharp, intense pain, often worse with jaw movement, chewing, or yawning.
2. Clicking, Popping, or Grating Sounds (Crepitus)
- Occurrence: These sounds can happen when you open your mouth, chew, or move your jaw.
- Significance: While occasional clicking without pain might not be problematic, persistent, painful, or loud sounds usually indicate disc displacement or degenerative changes within the joint. Crepitus often signals bone-on-bone friction.
3. Limited Jaw Movement or Locking
- Limited Opening: Difficulty opening the mouth fully, experiencing a feeling of stiffness or restriction.
- Locking: The jaw can get "stuck" in an open or closed position, making it impossible to move until it "unlocks." This can be a distressing symptom, often indicating a severely displaced disc.
4. Headaches
- Type: TMJ-related headaches are often tension-type headaches, manifesting as a dull ache around the temples, forehead, or back of the head.
- Mechanism: Muscle tension in the jaw, neck, and shoulders can trigger referred pain to the head.
5. Ear Pain or Fullness
- Characteristics: Pain in or around the ear, often mistaken for an ear infection, when in fact the ear itself is healthy.
- Accompanying Symptoms: Sometimes accompanied by a feeling of fullness in the ear, ringing in the ears (tinnitus), or even dizziness. This is due to the close proximity of the TMJ to the ear canal and shared nerve pathways.
6. Neck and Shoulder Pain
- Location: Stiffness, soreness, or aching in the muscles of the neck and shoulders.
- Connection: Poor posture, which contributes to TMJ issues, can also directly cause neck and shoulder strain. Jaw muscle tension can also refer pain to these areas.
7. Facial Pain
- Location: Aching or soreness in the face, sometimes feeling like sinus pressure.
- Characteristics: Can be unilateral (one side) or bilateral (both sides), and may be exacerbated by touching the affected areas.
8. Pain or Difficulty Chewing
- Mechanism: Chewing puts direct stress on the TMJ and masticatory muscles. If these structures are inflamed or damaged, eating can become very painful and difficult.
- Impact: May lead to avoidance of certain foods or a change in diet.
9. Changes in Bite
- Sensation: You might feel like your upper and lower teeth don't fit together properly, or that your bite has shifted.
- Cause: Swelling in the joint or disc displacement can temporarily alter the alignment of the jaw.
10. Swelling on the Side of the Face
- Appearance: Visible swelling near the TMJ, often accompanied by tenderness.
- Cause: Indicates inflammation within the joint.
If you experience any combination of these symptoms persistently, it is crucial to consult a dentist or a TMJ specialist. Early diagnosis and intervention can prevent the condition from worsening and improve your chances of effective long-term management.
The Role of TMJ Exercises
TMJ exercises are a cornerstone of conservative treatment for temporomandibular disorders, especially those involving muscle pain (myofascial TMD) or mild disc displacement. They are designed to address the underlying musculoskeletal imbalances that contribute to jaw pain and dysfunction. The primary goals of these exercises are to:
- Reduce Muscle Tension and Pain: Tight, overused jaw muscles are a major source of TMJ pain. Stretching and relaxation exercises help release this tension, improving blood flow and reducing discomfort.
- Improve Range of Motion: Over time, TMJ disorders can lead to restricted jaw movement. Exercises help restore the full, pain-free opening and closing of the mouth, as well as side-to-side and forward movements.
- Strengthen Jaw Muscles: Weak or imbalanced jaw muscles can contribute to joint instability. Strengthening exercises improve muscle endurance and coordination, supporting proper joint function.
- Promote Disc Repositioning (in some cases): For individuals with disc displacement, certain exercises can encourage the disc to move back into its correct position or improve the joint's ability to adapt to the displacement, leading to smoother movement.
- Increase Joint Lubrication: Gentle movement helps circulate synovial fluid within the joint, which lubricates the cartilage and disc, reducing friction and wear.
- Improve Posture: Many TMJ issues are linked to poor head and neck posture. Incorporating postural exercises helps align the head and neck, reducing strain on the jaw.
- Enhance Proprioception and Coordination: Exercises help retrain the neuromuscular system, improving your awareness of jaw position and movement, and promoting healthier movement patterns.
It's crucial to understand that TMJ exercises are most effective when part of a comprehensive treatment plan, often guided by a dental professional, physical therapist, or TMJ specialist. They are a self-management tool that empowers you to actively participate in your recovery and long-term well-being. The ADA supports the use of conservative, reversible therapies like exercises as a first-line approach for many TMJ disorders.
Types of TMJ Exercises
Implementing a regular routine of TMJ exercises can significantly alleviate pain and improve jaw function. It's important to perform these gently and consistently, always stopping if you experience sharp pain. Consult with a dental professional or physical therapist to ensure you are performing them correctly and that they are appropriate for your specific condition.
1. Relaxation Exercises
These exercises focus on reducing overall muscle tension, which is often a significant contributor to TMJ pain, especially myofascial pain.
a. Relaxed Jaw Exercise
- Purpose: To find your jaw's natural resting position and release tension.
- How to do it:
- Place your tongue gently on the roof of your mouth, directly behind your upper front teeth.
- Let your teeth come apart slightly, but keep your lips together.
- Allow your jaw to relax completely, so your teeth are not touching.
- Frequency: Practice throughout the day, especially when you notice yourself clenching.
b. Diaphragmatic Breathing
- Purpose: To promote relaxation of the entire body, reducing stress-induced muscle tension.
- How to do it:
- Lie on your back or sit comfortably. Place one hand on your chest and the other on your abdomen.
- Breathe in slowly through your nose, feeling your abdomen rise (your chest should remain relatively still).
- Exhale slowly through your mouth, feeling your abdomen fall.
- Frequency: 5-10 minutes, 2-3 times a day.
c. Progressive Muscle Relaxation
- Purpose: To learn to distinguish between tense and relaxed muscles.
- How to do it:
- Tense a group of muscles (e.g., in your feet) for 5-10 seconds, then relax them completely.
- Work your way up the body, including facial and jaw muscles (gently clench for a few seconds, then release).
- Frequency: Once a day for 15-20 minutes.
2. Stretching Exercises
Stretches aim to improve flexibility and lengthen tight jaw muscles.
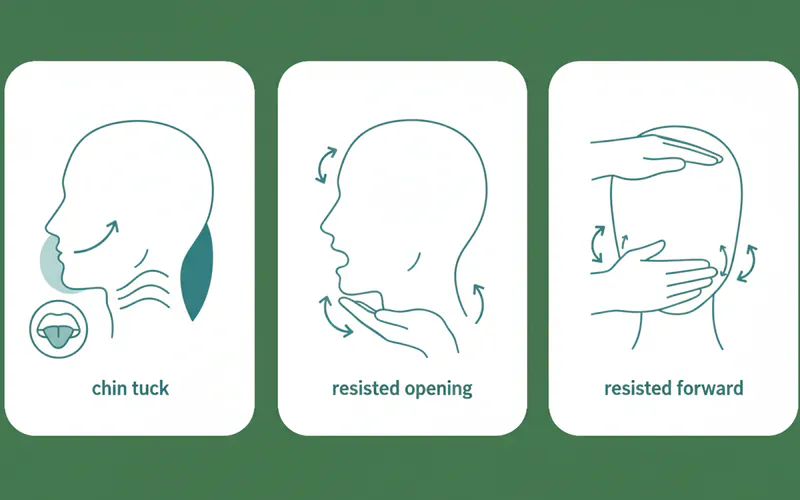
a. Chin Tucks
- Purpose: To improve neck posture and reduce forward head posture, which strains the jaw.
- How to do it:
- Sit or stand tall, looking straight ahead.
- Gently pull your chin straight back, as if making a double chin. You should feel a stretch at the back of your neck.
- Hold for 5 seconds.
- Frequency: 10 repetitions, 3 times a day.
b. Tongue Up Exercise (Stabilized Jaw Opening)
- Purpose: To gently stretch jaw muscles while keeping the disc stable.
- How to do it:
- Place the tip of your tongue on the roof of your mouth, directly behind your upper front teeth. Keep it there.
- Slowly open your mouth as wide as comfortable, keeping your tongue in contact with the roof of your mouth.
- Hold for 5 seconds, then slowly close.
- Frequency: 5-10 repetitions, 3 times a day.
c. Forward Jaw Stretch
- Purpose: To gently stretch the muscles involved in jaw protrusion.
- How to do it:
- Gently push your lower jaw slightly forward until you feel a gentle stretch.
- Hold for 5 seconds.
- Frequency: 5-10 repetitions, 3 times a day.
3. Strengthening Exercises
These exercises, often isometric (involving resistance without movement), help build endurance and coordination in the jaw muscles. They should be performed gently, without causing pain.
a. Resisted Opening
- Purpose: To strengthen the muscles that open the jaw.
- How to do it:
- Place your thumb under your chin.
- Slowly open your mouth, gently pushing up with your thumb to create resistance.
- Hold for 5-10 seconds, then slowly release.
- Frequency: 5-10 repetitions, 3 times a day.
b. Resisted Closing
- Purpose: To strengthen the muscles that close the jaw.
- How to do it:
- Place your index and middle fingers on top of your chin.
- Slowly close your mouth, gently pushing down with your fingers to create resistance.
- Hold for 5-10 seconds, then slowly release.
- Frequency: 5-10 repetitions, 3 times a day.
c. Resisted Side-to-Side Movement
- Purpose: To strengthen muscles involved in lateral jaw movement.
- How to do it:
- Place the palm of your hand against one side of your chin.
- Push your jaw gently towards your hand, while simultaneously resisting with your hand.
- Hold for 5-10 seconds.
- Repeat on the other side.
- Frequency: 5-10 repetitions per side, 3 times a day.
4. Range of Motion Exercises
These help restore and maintain the full, natural movement of the jaw.
a. Full Jaw Opening
- Purpose: To maximize the range of jaw opening.
- How to do it:
- Open your mouth as wide as comfortable, without pain.
- Hold for 5-10 seconds.
- Slowly close.
- Frequency: 5-10 repetitions, 3 times a day.
b. Side-to-Side Jaw Movement
- Purpose: To improve lateral mobility.
- How to do it:
- Gently move your lower jaw as far as comfortable to one side.
- Hold for 5 seconds.
- Return to the center.
- Repeat on the other side.
- Frequency: 5-10 repetitions per side, 3 times a day.
c. Forward Jaw Movement (Protrusion)
- Purpose: To improve forward mobility.
- How to do it:
- Gently move your lower jaw straight forward, without moving it to the sides.
- Hold for 5 seconds.
- Return to the starting position.
- Frequency: 5-10 repetitions, 3 times a day.
5. Posture Correction Exercises
As poor posture directly impacts TMJ health, integrating these can be very beneficial.
a. Scapular Retractions
- Purpose: To strengthen upper back muscles and counteract rounded shoulders, which contribute to forward head posture.
- How to do it:
- Sit or stand tall.
- Gently squeeze your shoulder blades together, as if holding a pencil between them. Keep your shoulders down, away from your ears.
- Hold for 5-10 seconds.
- Frequency: 10-15 repetitions, 2-3 times a day.
Pro Tip: Always start with gentle movements and gradually increase repetitions and duration as your comfort allows. If any exercise causes sharp or increasing pain, stop immediately and consult your healthcare provider. Consistency is far more important than intensity when it comes to TMJ exercises. Many individuals find that performing these routines in front of a mirror helps ensure correct form.
Step-by-Step Process for Implementing TMJ Exercises
Successfully integrating TMJ exercises into your routine requires a structured approach. Here's a step-by-step guide to ensure you're setting yourself up for success:
1. Consultation and Diagnosis
- Action: Schedule an appointment with a dentist specializing in TMJ disorders, an oral and maxillofacial surgeon, or a physical therapist.
- Why it matters: A professional can accurately diagnose the specific type of TMD you have (myofascial, disc derangement, arthritic, etc.), which is crucial for tailoring the most effective exercise regimen. They will also rule out other conditions.
2. Personalized Exercise Plan
- Action: Work with your healthcare provider to develop a customized exercise plan.
- Why it matters: Generic exercises might not be suitable for your specific condition and could potentially worsen symptoms. A professional will guide you on which exercises to prioritize, the correct technique, repetitions, sets, and frequency.
3. Start Gently and Gradually
- Action: Begin with the easiest, most gentle exercises prescribed. Focus on correct form over intensity.
- Why it matters: Your jaw muscles and joints may be inflamed or sensitive. Pushing too hard too soon can cause pain and setback recovery. The goal is to gradually restore function.
4. Establish a Routine and Be Consistent
- Action: Incorporate your exercises into your daily schedule. Many find it helpful to perform them 2-3 times a day for 5-10 minutes each session.
- Why it matters: Like any muscle rehabilitation, consistency is key. Sporadic effort will yield minimal results. Choose times when you can focus without interruption.
5. Monitor Your Symptoms
- Action: Pay close attention to how your jaw feels before, during, and after exercises. Keep a simple pain journal.
- Why it matters: This helps you identify which exercises are beneficial and which might be counterproductive. Share this information with your healthcare provider during follow-up appointments.
6. Integrate Relaxation and Posture
- Action: Don't just focus on the jaw-specific movements. Include relaxation techniques (like diaphragmatic breathing) and posture correction exercises.
- Why it matters: Stress and poor posture are major contributors to TMD. Addressing these holistically enhances the effectiveness of jaw exercises.
7. Avoid Triggers
- Action: While doing exercises, consciously avoid habits that aggravate your TMJ, such as chewing gum, clenching your teeth, excessive yawning, or eating hard, chewy foods.
- Why it matters: Continuously irritating the joint will undermine the benefits of the exercises.
8. Gradual Progression
- Action: As your pain decreases and range of motion improves, your physical therapist or dentist may advise you to gradually increase the intensity, duration, or resistance of certain exercises.
- Why it matters: This ensures continued progress in strengthening and stabilizing the joint.
9. Follow-Up Appointments
- Action: Attend all scheduled follow-up appointments with your healthcare provider.
- Why it matters: These appointments allow your provider to assess your progress, make adjustments to your exercise plan, and introduce other therapies if needed.
10. Long-Term Maintenance
- Action: Even after symptoms improve, continue a maintenance program of exercises to prevent recurrence.
- Why it matters: TMJ disorders can recur. Regular, gentle exercises can help maintain jaw health and prevent future flare-ups, contributing to "how to cure tmj permanently" by managing symptoms effectively long-term.
Other Treatment Options for TMJ Pain
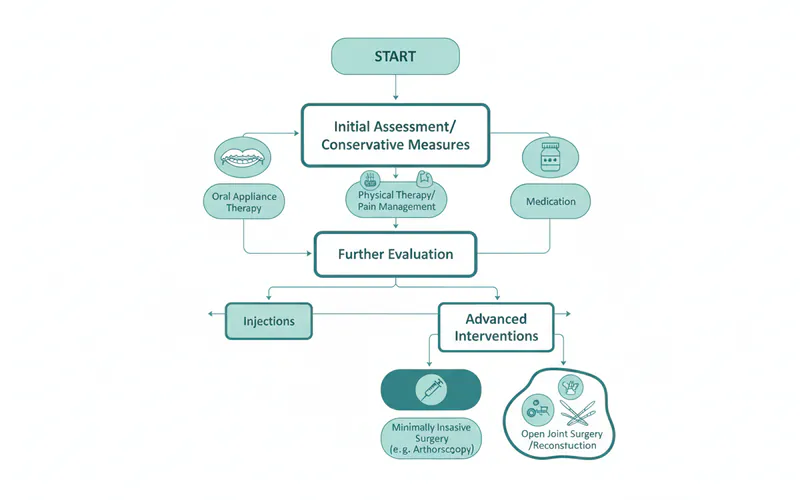
While TMJ exercises are a fundamental component of conservative treatment, they are often part of a broader, integrated approach to manage and alleviate TMJ pain. Depending on the severity and specific cause of your TMD, your healthcare provider may recommend one or more of the following treatment options:
1. Medications
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): Over-the-counter options like ibuprofen or naproxen can reduce pain and inflammation. Prescription-strength NSAIDs may be used for more severe cases.
- Pros: Readily available, generally safe for short-term use.
- Cons: Potential for side effects like stomach upset, kidney issues with prolonged use.
- Muscle Relaxants: Medications like cyclobenzaprine can help relieve muscle spasms and tension in the jaw.
- Pros: Effective for myofascial pain and clenching.
- Cons: Can cause drowsiness, dizziness, and should be used short-term.
- Tricyclic Antidepressants: Low doses of drugs like amitriptyline, particularly taken at bedtime, can help with pain control, muscle relaxation, and improve sleep for chronic pain sufferers, even without depression.
- Pros: Can address chronic pain and sleep disturbances.
- Cons: Potential side effects include dry mouth, drowsiness, constipation.
- Corticosteroids: Can be prescribed orally or as an injection directly into the joint to reduce inflammation.
- Pros: Powerful anti-inflammatory effect.
- Cons: Injections are invasive; oral steroids have systemic side effects with prolonged use.
2. Oral Appliances (Mouthguards/Splints)
- Description: Custom-made acrylic devices that fit over your upper or lower teeth. They come in various designs:
- Stabilization Splints (Occlusal Splints): Most common. Cover all teeth, create a stable bite, and reduce muscle activity, especially helpful for bruxism.
- Repositioning Splints: Less common, designed to temporarily move the jaw into a specific position to help reposition the disc. Used with caution and typically for short durations.
- Pros: Non-invasive, reversible, can protect teeth from grinding, reduce muscle tension, provide a stable bite.
- Cons: Can be expensive, requires consistent wear, some patients find them uncomfortable, potential for changes in bite if improperly fitted or used for too long.
3. Physical Therapy (Beyond Just Exercises)
- Description: A physical therapist (PT) specializing in craniofacial pain can provide advanced techniques.
- Techniques: Manual therapy (massage, mobilization), heat/cold therapy, ultrasound, electrical stimulation (TENS), posture education, and advanced TMJ exercises.
- Pros: Holistic approach, personalized care, addresses underlying biomechanical issues.
- Cons: Requires multiple sessions, can be costly without good insurance.
4. Injections
- Corticosteroid Injections: Directly into the joint to reduce inflammation and pain, often for arthritic conditions.
- Botox (Botulinum Toxin) Injections: Injected into the masticatory muscles (e.g., masseter, temporalis) to relax them and reduce clenching/grinding.
- Pros: Can provide significant pain relief and reduce muscle hyperactivity.
- Cons: Temporary effects (typically 3-6 months), requires repeat injections, potential for temporary facial weakness or asymmetry (Botox), invasive.
5. Alternative and Complementary Therapies
- Acupuncture: Involves placing thin needles at specific points to relieve pain and muscle tension.
- Biofeedback: Teaches you to control involuntary bodily functions like muscle tension, often used for stress reduction and bruxism.
- Massage Therapy: Can help release tension in jaw, neck, and shoulder muscles.
- Stress Management Techniques: Mindfulness, meditation, yoga, and counseling can significantly reduce stress-induced clenching.
6. Surgical Interventions
Surgery is typically reserved for severe cases of TMD that haven't responded to conservative treatments and when there's a clear structural problem within the joint.
- Arthrocentesis: A minimally invasive procedure involving flushing the joint with sterile fluid to remove inflammatory byproducts and free up any adhesions.
- Pros: Minimally invasive, relatively quick recovery.
- Cons: May not be effective for all disc problems.
- Arthroscopy: A minimally invasive procedure where a small camera and instruments are inserted into the joint to diagnose and treat issues like disc repositioning, adhesion removal, or tissue repair.
- Pros: Less invasive than open surgery, quicker recovery than open surgery.
- Cons: Still surgical, risks include nerve damage, infection.
- Open-Joint Surgery: Traditional surgery for complex problems like severe joint degradation, tumors, or extensive disc repair/replacement.
- Pros: Can address severe structural damage.
- Cons: Highly invasive, longer recovery, greater risks (nerve damage, scarring, infection, potential for jaw immobility).
Comparison Table 1: Non-Surgical TMJ Treatments
| Treatment Option | Primary Mechanism | Typical Efficacy (Pain Relief) | Pros | Cons |
|---|---|---|---|---|
| TMJ Exercises | Muscle relaxation, strengthening, range of motion | Moderate to High | Non-invasive, self-empowering, low cost | Requires consistency, not for all TMD types |
| Oral Appliances | Stabilizes bite, reduces muscle activity/bruxism | Moderate to High | Non-invasive, protects teeth, reversible | Can be costly, requires consistent wear, potential bite changes |
| Medications (NSAIDs) | Reduces inflammation and pain | Moderate | Readily available, quick relief | Side effects (GI, kidney), temporary relief |
| Medications (Muscle Relaxants) | Reduces muscle spasms and tension | Moderate to High | Effective for myofascial pain | Drowsiness, temporary, potential for dependency |
| Botox Injections | Paralyses overactive jaw muscles, reduces clenching | High | Significant pain reduction, non-surgical | Temporary (3-6 months), costly, potential for side effects |
| Physical Therapy | Manual therapy, posture, advanced exercises | High | Addresses root causes, personalized, holistic | Requires multiple sessions, can be costly |
| Stress Management | Reduces muscle tension, clenching/grinding | Moderate to High | Addresses underlying cause, improves overall wellbeing | Requires consistent effort, not a standalone treatment |
The ADA recommends starting with the most conservative, reversible treatments first, such as TMJ exercises, oral appliances, and stress management, before considering more invasive options.
Cost and Insurance
Understanding the financial aspects of TMJ treatment, particularly in the US, is crucial for patients seeking relief. Costs can vary significantly based on the severity of the condition, the chosen treatment path, geographical location, and whether you have insurance coverage.

Diagnostic Costs
Before any treatment begins, an accurate diagnosis is essential.
- Initial Consultation (Dentist/Oral Surgeon/TMJ Specialist): $100 - $300
- X-rays (Panoramic or Cone Beam CT): $50 - $250
- MRI (Magnetic Resonance Imaging): Used to visualize soft tissues like the disc. $300 - $1,500 (can be higher in some regions). Often requires medical insurance.
TMJ Exercise-Related Costs
The exercises themselves are generally free if performed at home. However, professional guidance incurs costs.
- Physical Therapy (PT) Sessions: A common approach for guided TMJ exercises and manual therapy.
- Per session: $75 - $250, depending on location and therapist.
- Typical course: 6-12 sessions initially, potentially more for chronic cases. Total cost: $450 - $3,000+
- Dental Appliances (Oral Splints/Mouthguards): Often used in conjunction with exercises, especially for bruxism.
- Custom-made: $300 - $800 (some advanced splints can be $1,500 - $2,500). Over-the-counter options are cheaper (around $20-$50) but less effective and not recommended by most dentists for long-term TMJ issues.
Other Treatment Costs
- Medications:
- Over-the-counter NSAIDs: $10 - $30 per month.
- Prescription muscle relaxants/antidepressants: $15 - $100+ per month, depending on generic vs. brand and insurance.
- Botox Injections: $500 - $1,500 per treatment session, typically needed every 3-6 months. Most insurance does NOT cover Botox for TMJ unless it's for severe, documented medical necessity.
- Surgical Procedures: These are the most expensive options and vary widely.
- Arthrocentesis: $1,000 - $3,000 per joint.
- Arthroscopy: $5,000 - $15,000 per joint.
- Open-Joint Surgery: $10,000 - $20,000+ per joint, often significantly more if joint replacement is needed.
Insurance Coverage Details
Navigating insurance for TMJ treatment can be complex because it often straddles medical and dental insurance.
- Medical Insurance:
- Often covers diagnostic tests (X-rays, MRI), physical therapy, consultations with medical specialists, prescription medications, and surgical procedures (as they are considered medical).
- Deductibles and Co-pays: You will likely need to meet your medical deductible (e.g., $500 - $5,000) before full coverage kicks in, and pay co-pays (e.g., $20 - $70) per visit for PT or doctor appointments.
- Pre-authorization: Many procedures, especially MRIs and surgeries, require pre-authorization from your medical insurer.
- Dental Insurance:
- May cover a portion of oral appliances (splints/mouthguards), especially if deemed medically necessary by a dentist and submitted with appropriate coding. Coverage varies widely, with some plans covering 50-80% after a deductible.
- Generally does NOT cover physical therapy, medications, or surgery for TMJ.
- Combined Coverage: In some cases, a patient might use dental insurance for an oral appliance and medical insurance for PT or medications. Coordination of benefits can be complex.
- In-network vs. Out-of-network: Costs will be significantly higher if you use out-of-network providers. Always verify your coverage with your insurance provider beforehand.
Pro Tip: Always call your insurance company directly to inquire about coverage for "Temporomandibular Joint Disorder" specifically. Ask about diagnostic codes (e.g., K07.6 for TMJ disorders, M26.6 for TMD), procedure codes, and if a referral from your primary care physician is needed. Document everything, including dates, names of representatives, and reference numbers.
Recovery and Aftercare
Recovery from TMJ disorders is a journey that often requires consistent effort and attention to detail. TMJ exercises are a vital part of this process, but a holistic approach to aftercare ensures long-term relief and prevention of recurrence.
1. Consistency with Exercises
- Action: Continue your prescribed TMJ exercise regimen diligently, even as symptoms improve.
- Why it matters: Regular exercises maintain muscle flexibility, strength, and joint mobility, preventing stiffness and re-establishing healthy movement patterns. Think of them as preventative maintenance for your jaw.
2. Pain Management Strategies
- Action: Utilize prescribed or over-the-counter pain relievers (NSAIDs) as needed, but avoid chronic reliance. Explore non-pharmacological methods like moist heat or cold packs.
- Why it matters: Managing breakthrough pain allows you to continue exercises and daily activities without severe discomfort. Moist heat (15-20 minutes) can relax muscles; cold packs can reduce acute inflammation and pain.
3. Dietary Modifications
- Action: Stick to a soft or semi-soft diet, especially during flare-ups or periods of intense pain. Avoid hard, chewy, or crunchy foods (e.g., nuts, hard candy, raw carrots, gum, bagels, tough meat). Cut food into small, manageable pieces.
- Why it matters: Reducing the workload on your jaw minimizes stress on the joint and muscles, allowing them to heal and preventing irritation.
4. Stress Reduction Techniques
- Action: Incorporate stress-reduction practices into your daily life: meditation, mindfulness, deep breathing exercises (like diaphragmatic breathing), yoga, or counseling.
- Why it matters: Stress is a major trigger for teeth clenching and grinding (bruxism), which exacerbates TMJ pain. Managing stress directly addresses a root cause.
5. Posture Awareness and Correction
- Action: Be mindful of your posture, especially when sitting at a computer, driving, or looking at your phone. Ensure your head is balanced directly over your spine, not thrust forward.
- Why it matters: Poor posture (e.g., forward head posture) strains neck and jaw muscles, pulling the jaw out of alignment. Correcting it reduces this strain.
6. Avoid Parafunctional Habits
- Action: Consciously stop habits like nail-biting, pen-chewing, leaning on your hand, or resting your chin on your fist.
- Why it matters: These habits place undue and uneven stress on the TMJ, hindering recovery.
7. Gentle Jaw Movements
- Action: When yawning, gently support your chin to prevent overstretching. Avoid excessive wide opening of your mouth.
- Why it matters: Preventing extreme movements helps protect the healing joint and disc.
8. Consistent Oral Appliance Use
- Action: If you've been prescribed an oral splint or mouthguard, wear it exactly as instructed by your dentist, typically at night.
- Why it matters: These devices protect your teeth from grinding, reduce muscle activity, and stabilize the bite, complementing the effects of exercises.
9. Regular Follow-Up Appointments
- Action: Continue scheduled visits with your dentist or TMJ specialist as recommended.
- Why it matters: These appointments allow your healthcare provider to monitor your progress, make necessary adjustments to your treatment plan, and address any new concerns.
10. Stay Hydrated and Maintain a Healthy Lifestyle
- Action: Drink plenty of water, get adequate sleep, and engage in moderate, full-body exercise (which can help reduce overall body tension).
- Why it matters: Overall health and well-being positively impact your body's ability to heal and manage pain.
Long-term recovery and effective management of TMJ pain ("how to cure tmj permanently" by effective management) depend heavily on a sustained commitment to these aftercare principles. It's about developing new, healthier habits that support jaw health for life.
Prevention
Preventing TMJ disorders, or at least minimizing their recurrence, often involves modifying behaviors and adopting healthier habits that reduce stress on the jaw joint and surrounding muscles. While not all causes are preventable (e.g., trauma, severe arthritis), many contributing factors can be managed.
1. Manage Stress and Anxiety
- Why it matters: Stress is a primary trigger for clenching and grinding, which significantly strains the TMJ.
- Actions: Practice relaxation techniques (meditation, deep breathing, yoga), ensure adequate sleep, engage in regular physical activity, and consider counseling or biofeedback if stress is chronic.
2. Avoid Parafunctional Habits
- Why it matters: These habits put abnormal and prolonged stress on the jaw.
- Actions: Break habits like teeth clenching, teeth grinding (if awake), nail-biting, pen-chewing, gum chewing, and habitually resting your chin on your hand. Be mindful of these throughout the day.
3. Maintain Good Posture
- Why it matters: Forward head posture strains the neck and shoulder muscles, which in turn pull the jaw out of its natural alignment, increasing TMJ stress.
- Actions: Practice sitting and standing tall, keeping your ears aligned over your shoulders. Take breaks from computer or phone use to stretch your neck and shoulders. Use ergonomic setups for workstations.
4. Protect Your Jaw from Overuse
- Why it matters: Excessive or forceful jaw movements can irritate the joint and muscles.
- Actions: Avoid opening your mouth too wide during yawning (gently support your chin). Cut hard, crunchy, or chewy foods into small pieces. Choose softer foods when possible.
5. Use an Oral Appliance (if recommended)
- Why it matters: For individuals with diagnosed bruxism, a custom-fitted nightguard protects teeth from wear and helps reduce muscle activity during sleep.
- Actions: If your dentist recommends a nightguard, wear it consistently as instructed.
6. Maintain Oral Health and Regular Dental Check-ups
- Why it matters: Your dentist can spot early signs of bruxism, tooth wear, or jaw problems during routine visits.
- Actions: Visit your dentist for regular check-ups and cleanings (every 6 months). Discuss any jaw pain, clicking, or difficulty opening your mouth with them.
7. Be Mindful of Sleeping Position
- Why it matters: Sleeping on your stomach can twist your neck and place awkward pressure on your jaw.
- Actions: Try to sleep on your back or side, using a supportive pillow that keeps your head and neck in neutral alignment.
8. Correct Jaw Resting Position
- Why it matters: Many people unconsciously clench their teeth or rest their jaw in a strained position.
- Actions: Practice the "relaxed jaw" exercise (tongue on the roof of the mouth, teeth slightly apart, lips gently together) throughout the day to encourage a neutral, relaxed resting position.
By integrating these preventive measures into your lifestyle, you can significantly reduce the risk of developing TMJ pain or minimize its severity if it does occur.
Risks and Complications
While TMJ exercises are generally considered a safe and conservative treatment, it's important to be aware of potential risks, especially if exercises are performed incorrectly or without proper guidance. Additionally, other TMJ treatments carry their own set of complications.
Risks Associated with TMJ Exercises
-
Increased Pain or Worsening Symptoms:
- Cause: Performing exercises too aggressively, using incorrect technique, or attempting exercises not suitable for your specific type of TMD. For example, forceful stretching of a hypermobile joint or a significantly displaced disc can cause more harm.
- Prevention: Always start gently, follow professional guidance, and stop immediately if you experience sharp or increasing pain.
-
Joint Damage:
- Cause: Repeated incorrect or excessive movements could potentially exacerbate disc displacement or contribute to cartilage wear over time.
- Prevention: Professional assessment and guidance are paramount. Exercises should be tailored to your diagnosis.
-
Muscle Fatigue or Strain:
- Cause: Overdoing strengthening exercises or not allowing adequate rest between sessions.
- Prevention: Follow prescribed repetitions and sets, and ensure rest periods.
Risks and Complications of Other TMJ Treatments
1. Oral Appliances (Mouthguards/Splints)
- Bite Changes: If a splint is improperly designed or worn for too long without supervision, it can sometimes lead to permanent changes in your bite (malocclusion).
- Increased Pain/Discomfort: A poorly fitted splint can irritate gums, teeth, or even increase TMJ pain if it exacerbates existing issues.
- Dependence: Some individuals may become dependent on their splint and experience discomfort without it.
2. Medications
- NSAIDs: Gastrointestinal upset, ulcers, kidney damage with long-term high-dose use.
- Muscle Relaxants: Drowsiness, dizziness, dry mouth, potential for dependency with prolonged use.
- Antidepressants: Dry mouth, constipation, blurred vision, drowsiness, weight gain.
- Corticosteroid Injections: Infection, temporary facial flushing, localized tissue damage or atrophy with repeated injections, temporary blood sugar elevation.
3. Botox Injections
- Temporary Facial Weakness/Asymmetry: If injected incorrectly, it can temporarily affect adjacent muscles, leading to a lopsided smile or difficulty with certain facial expressions.
- Bruising/Swelling: Common at the injection site.
- Rare but Serious: Allergic reactions, spread of toxin to distant muscles (very rare).
4. Surgical Interventions (Arthrocentesis, Arthroscopy, Open-Joint Surgery)
- Infection: Any surgery carries a risk of infection.
- Nerve Damage: Damage to facial nerves can cause temporary or permanent numbness, weakness, or paralysis of facial muscles (e.g., facial nerve, trigeminal nerve).
- Bleeding: Risk of excessive bleeding.
- Scarring: Visible scarring, especially with open-joint surgery.
- Limited Jaw Movement: Paradoxically, surgery can sometimes lead to fibrosis and reduced jaw mobility.
- Anesthesia Risks: Risks associated with general anesthesia (e.g., respiratory issues, adverse drug reactions).
- Failure of Treatment: Even with surgery, there's no guarantee of a complete "cure," and symptoms may persist or recur.
- Revision Surgery: The need for additional surgical procedures.
It is paramount to have a thorough discussion with your healthcare provider about all potential risks and benefits before embarking on any TMJ treatment, especially invasive procedures. Choosing conservative, reversible treatments first, as advocated by the ADA, minimizes these risks.
Comparison Table 2: TMJ Treatment Cost & Timeline Overview
| Treatment Option | Average Cost Range (US, without insurance) | Typical Timeline for Initial Relief | Long-Term Commitment |
|---|---|---|---|
| TMJ Exercises (Self-guided) | $0 - $50 (for basic supplies) | 2-6 weeks | Lifelong maintenance |
| TMJ Exercises (with PT) | $450 - $3,000+ (6-12 sessions) | 4-8 weeks | Lifelong maintenance |
| Custom Oral Appliance (Splint) | $300 - $800 | 1-3 months | Nightly use (long-term) |
| NSAIDs (Prescription) | $15 - $100/month | Days to 2 weeks | Short-term use (weeks) |
| Muscle Relaxants | $20 - $100/month | Days to 1 week | Short-term use (weeks) |
| Botox Injections | $500 - $1,500/treatment | 1-2 weeks | Every 3-6 months |
| Arthrocentesis | $1,000 - $3,000 | Days to 2 weeks | Varies, sometimes one-time |
| Arthroscopy | $5,000 - $15,000 | 2-4 weeks (initial recovery) | Varies, may require PT |
| Open-Joint Surgery | $10,000 - $20,000+ | 6-12 weeks (initial recovery) | Varies, extensive PT |
Children / Pediatric Considerations
TMJ disorders are not exclusive to adults; they can also affect children and adolescents. While less common than in adults, the prevalence is increasing, and early diagnosis and intervention are crucial to prevent long-term complications.
Prevalence and Causes in Children
- Increasing Incidence: Studies suggest that TMD symptoms can be found in 6-12% of children and adolescents, with girls more commonly affected than boys, similar to adults.
- Common Causes:
- Bruxism (Clenching/Grinding): Often a significant factor in children, sometimes linked to stress, malocclusion, or sleep disorders. Parents may hear grinding sounds at night.
- Trauma: Falls, sports injuries, or direct blows to the jaw or head are common in active children.
- Oral Habits: Prolonged thumb-sucking, pacifier use, or nail-biting can contribute to jaw misalignment and muscle strain.
- Malocclusion: While not a direct cause, severe bite problems can sometimes place undue stress on the developing TMJ.
- Orthodontic Treatment: In some rare instances, aggressive or prolonged orthodontic treatment can temporarily contribute to TMJ discomfort, though modern orthodontics aims to minimize this.
- Connective Tissue Disorders: Conditions like Ehlers-Danlos syndrome can cause joint laxity, making the TMJ more prone to issues.
Signs and Symptoms in Children
Symptoms in children can be similar to adults but may sometimes be less obvious or harder for a child to articulate.
- Jaw Pain: The child might complain of pain around the ears, face, or jaw, especially when chewing.
- Clicking/Popping: Audible sounds from the jaw joint during eating or talking.
- Difficulty Opening Mouth: The child might struggle to open their mouth wide for a bite or during dental visits.
- Headaches: Frequent headaches, especially in the temporal region.
- Earaches: Unexplained ear pain, often misdiagnosed as an ear infection.
- Changes in Eating Habits: Avoiding hard foods or showing reluctance to chew.
Gentle Exercise Approach for Children
For children, the emphasis is always on gentle, non-strenuous movements and play-based activities to encourage jaw mobility and relaxation.
- Parental Involvement: Parents play a crucial role in observing symptoms, encouraging compliance, and ensuring exercises are performed correctly.
- Relaxation Exercises: Simple relaxation techniques, deep breathing, and encouraging a "soft jaw" position can be taught.
- Gentle Stretching: "Tongue up" exercises or gentle jaw opening stretches, framed as a game, can be effective.
- Posture Correction: Encouraging good posture, especially during screen time or reading, is vital.
- Avoiding Overuse: Teaching children to avoid habits like excessive gum chewing or clenching.
Other Pediatric Treatments
- Oral Appliances: Custom-fitted nightguards are often used for children with bruxism to protect teeth and stabilize the jaw.
- Medications: Over-the-counter NSAIDs can be used for pain relief under parental guidance.
- Physical Therapy: Pediatric physical therapists specializing in craniofacial pain can provide age-appropriate manual therapy and exercise instruction.
- Orthodontic Assessment: An orthodontist can evaluate the bite and jaw development.
- Psychological Support: If stress or anxiety are significant factors, counseling or biofeedback can be beneficial.
The ADA emphasizes conservative, reversible treatments for children, prioritizing approaches that support natural growth and development without invasive procedures unless absolutely necessary. Early detection by a pediatrician or pediatric dentist is key.
Cost Breakdown
A comprehensive understanding of TMJ treatment costs in the US involves looking at various scenarios, as expenses can swing wildly depending on the severity of your condition, the chosen treatment modalities, and your insurance status.
Average US Costs (Low, Mid, High Scenarios)
-
Low-Cost Scenario (Conservative, Self-Managed):
- Initial Dental/Medical Consultation: $100 - $250
- Over-the-counter NSAIDs: $10 - $30/month
- Self-guided TMJ Exercises: $0
- Total (initial few months): $110 - $280 (excluding ongoing medication)
- Best for: Mild, acute muscle-related pain, stress-induced clenching.
-
Mid-Cost Scenario (Comprehensive Non-Surgical):
- Initial Consultation + X-rays: $150 - $400
- Physical Therapy (6-8 sessions): $450 - $1,600
- Custom Oral Appliance (Nightguard): $300 - $800
- Prescription Medications (e.g., muscle relaxants): $50 - $200 (for a few months)
- Total: $950 - $3,000+
- Best for: Chronic myofascial pain, mild disc displacement, moderate bruxism.
-
High-Cost Scenario (Advanced/Surgical):
- Comprehensive Diagnostics (MRI, extensive exams): $500 - $2,000
- Botox Injections (multiple sessions/year): $1,000 - $3,000+ per year
- Surgical Intervention (e.g., Arthroscopy): $5,000 - $15,000 (per joint)
- Post-surgical Physical Therapy: $500 - $2,000+
- Total: $7,000 - $22,000+ (can be significantly higher for open-joint surgery or joint replacement, which can exceed $50,000)
- Best for: Severe, intractable pain, significant disc derangement not responsive to conservative care, advanced degenerative joint disease.
With vs. Without Insurance
- Without Insurance (Out-of-Pocket): You are responsible for 100% of the costs. This highlights the importance of cost-saving tips and payment plans.
- With Insurance:
- Medical Insurance: Typically covers diagnostic imaging (MRI, X-rays), physical therapy, specialist consultations, and surgical procedures (often 80-90% after deductible). You'll still owe deductibles ($500-$5,000+) and co-pays ($20-$70 per visit). Botox is usually NOT covered.
- Dental Insurance: May cover a portion of oral appliances (e.g., 50-80% of $300-$800 splint, after a deductible of $50-$200), but often has an annual maximum benefit (e.g., $1,000-$2,500), which can quickly be exhausted. Rarely covers other TMJ treatments.
Example with Insurance:
- Mid-Cost Scenario with a $1,000 medical deductible and $50 co-pay for PT:
- Initial Consult + X-rays: $400 (assume part counted towards deductible)
- PT (8 sessions): $1,600 -> Patient pays $1,000 deductible first, then $50 co-pay for remaining sessions (total $1,000 + $50 * 7 = $1,350 assuming first session clears deductible).
- Custom Splint: $800 (assume dental insurance covers 50% after a $100 deductible -> $100 + ($800-$100)*0.5 = $450)
- Estimated Total Patient Cost: $400 + $1,350 + $450 = $2,200 (compared to $3,000 without insurance). This is a simplified example, actual costs vary.
Payment Plans and Financing Options
- Dental Office Payment Plans: Many dental offices offer in-house payment plans or work with third-party financing companies (e.g., CareCredit). These allow you to pay off a larger bill over several months, often with low or no interest for a promotional period.
- Healthcare Credit Cards: Specifically designed for medical expenses, these cards offer deferred interest periods, but high interest rates if the balance isn't paid on time.
- Personal Loans: Banks or credit unions offer personal loans that can cover medical expenses, usually with fixed interest rates.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have these accounts, you can use pre-tax dollars to pay for qualified medical expenses, including many TMJ treatments, effectively saving you money.
Cost-Saving Tips
- Start Conservative: Always begin with the least invasive and most affordable treatments, like TMJ exercises and self-care, as recommended by the ADA.
- Get Multiple Opinions: For complex cases, consult more than one specialist to compare treatment plans and costs.
- Verify Insurance: Before any treatment, contact your insurance provider to understand exact coverage, deductibles, co-pays, and whether pre-authorization is required.
- Ask for Itemized Bills: Ensure you understand all charges and check for any discrepancies.
- In-Network Providers: Stick to providers within your insurance network to maximize coverage.
- Negotiate Cash Prices: If you're uninsured, ask providers if they offer a discount for cash payments.
- Utilize HSAs/FSAs: Plan for medical expenses using these tax-advantaged accounts.
Frequently Asked Questions
How long do TMJ exercises take to work?
The timeline for relief from TMJ exercises varies, but many individuals experience noticeable improvement in 2 to 6 weeks of consistent, correct practice. For chronic or more severe conditions, it may take several months to achieve significant, sustained relief and improved jaw function. It's important to remember that consistency and proper technique are key to seeing results.
Can TMJ be cured permanently?
The concept of a "permanent cure" for TMJ disorders is complex. While symptoms can often be effectively managed and significantly reduced, many TMJ issues are chronic and require ongoing management. Addressing underlying causes like stress or bruxism and adhering to a maintenance routine of TMJ exercises and preventive measures can lead to long-term relief and prevent recurrence, essentially "curing" the disruptive symptoms. However, structural changes like disc displacement or arthritis may persist even if pain-free.
What exercises should I avoid with TMJ?
You should avoid any exercises that cause sharp or increasing pain, clicking, or locking in your jaw. Generally, exercises that involve forceful stretching, excessive resistance, or wide, unsupported jaw opening should be approached with caution or avoided, especially initially. It's crucial to get a professional diagnosis and guidance to ensure the exercises you perform are appropriate for your specific TMJ condition.
Are there side effects to TMJ exercises?
When performed correctly and gently, TMJ exercises have minimal side effects. However, if done too aggressively or incorrectly, they can potentially lead to increased muscle soreness, temporary pain, or irritation of the joint. This underscores the importance of proper instruction from a dentist or physical therapist and stopping any exercise that causes discomfort.
Can stress worsen TMJ?
Absolutely. Stress is one of the most significant contributing factors to TMJ flare-ups. Emotional or psychological stress often leads to unconscious teeth clenching and grinding (bruxism), which places excessive strain on the jaw muscles and joints, exacerbating pain and dysfunction. Managing stress through relaxation techniques is a critical component of TMJ treatment and prevention.
Is heat or ice better for TMJ pain?
Both heat and ice can be beneficial, depending on the type of pain. Moist heat (e.g., a warm, damp towel) is generally better for relaxing tense jaw muscles and increasing blood flow, offering relief for myofascial pain. Apply for 15-20 minutes. Ice packs (wrapped in a cloth) are usually more effective for acute pain, swelling, or inflammation within the joint itself. Apply for 10-15 minutes. You can experiment to see which provides more relief for your specific symptoms.
When should I consider surgery for TMJ?
TMJ surgery is typically considered a last resort, reserved for severe cases that have not responded to a comprehensive course of conservative treatments (including exercises, splints, medications, and physical therapy). It's usually indicated when there's a clear structural problem within the joint, such as severe disc derangement, advanced arthritis, or significant anatomical abnormalities causing persistent pain and dysfunction. The ADA recommends exhausting all reversible, non-invasive options first.
Can my diet affect my TMJ?
Yes, your diet can significantly affect your TMJ. Eating hard, chewy, or crunchy foods (like tough meats, raw vegetables, hard bread, nuts, or chewing gum) puts extra strain on your jaw joint and muscles, potentially aggravating pain and inflammation. Opting for softer foods, cutting food into small pieces, and avoiding repetitive chewing can help reduce stress on your TMJ.
What is the average cost of TMJ treatment without insurance?
Without insurance, the cost of TMJ treatment can range widely, from a few hundred dollars for self-managed exercises and over-the-counter medications to thousands for physical therapy and custom oral appliances, and potentially tens of thousands for surgical interventions. For example, a custom nightguard might cost $300-$800, and a course of physical therapy might be $450-$3,000+ without any insurance coverage.
Are mouthguards effective for TMJ?
Custom-fitted stabilization splints (often called mouthguards or nightguards) are often very effective for TMJ disorders, particularly those related to bruxism (teeth clenching/grinding) and muscle pain. They work by providing a stable bite, protecting teeth from wear, and reducing muscle overactivity. However, they should be professionally made and monitored, as ill-fitting or prolonged use of some types of splints can potentially worsen symptoms or change your bite.
When to See a Dentist
While TMJ exercises and self-care can be incredibly helpful, it's crucial to know when professional intervention is necessary. Ignoring persistent or worsening symptoms can lead to more complex problems and prolonged discomfort. You should make an appointment with a dentist, an oral and maxillofacial surgeon, or a TMJ specialist if you experience any of the following:
Clear Warning Signs for Professional Evaluation:
- Persistent Jaw Pain: If your jaw pain is constant, severe, or doesn't improve with self-care (like rest, soft diet, and gentle exercises) after a few days to a week, it's time to see a professional.
- Limited Jaw Movement: If you find it difficult to open your mouth widely, experience stiffness, or cannot move your jaw from side to side normally, this indicates a potential mechanical problem within the joint.
- Jaw Locking: If your jaw gets stuck in an open or closed position, even temporarily, this is a significant red flag often indicating disc displacement without reduction, and requires immediate attention.
- Loud or Painful Clicking/Popping: While some people have painless jaw clicks, if the sounds are loud, accompanied by pain, or have recently started/worsened, it's a sign of joint dysfunction. Grinding sounds (crepitus) also warrant evaluation.
- Severe Headaches or Earaches: If you experience frequent or intense headaches (especially around your temples) or earaches that are not explained by other conditions, your TMJ could be the source.
- Sudden Changes in Your Bite: If you suddenly feel like your upper and lower teeth don't fit together correctly, or your bite feels "off," this can indicate swelling or structural changes in the TMJ.
- Facial Swelling: Any noticeable swelling around the jaw joint area, especially if accompanied by redness or warmth, could indicate inflammation or infection.
- Pain Radiating to Neck and Shoulders: While common, if this pain is severe and consistently linked to jaw movement, it points to a significant TMJ or related muscle issue.
- Inability to Eat Normally: If chewing or eating has become consistently difficult or painful, impacting your nutrition, seek help.
Emergency vs. Scheduled Appointment Guidance:
- Emergency Care: Immediate locking of the jaw (unable to close or open), severe trauma to the jaw, or intense, debilitating pain that makes basic functions impossible warrant an emergency visit to your dentist or an urgent care facility.
- Scheduled Appointment: For most other persistent symptoms listed above, a scheduled appointment with a general dentist is the first step. They can diagnose many common TMJ issues and refer you to a specialist (like an oral and maxillofacial surgeon, prosthodontist, or physical therapist) if your condition requires more specialized care.
Early diagnosis and intervention are key to effective management of TMJ disorders, preventing them from becoming chronic and more difficult to treat. Don't hesitate to seek professional advice if your symptoms are concerning or impacting your quality of life.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Tmj Massage Near Me: Complete Guide
Temporomandibular joint disorder, commonly known as TMJD, affects millions of Americans, causing debilitating pain, discomfort, and significantly impacting quality of life. If you're experiencing jaw pain, clicking, or difficulty chewing, you're not alone. Up to 15% of American adults experience
February 23, 2026
Tmd Treatment: Complete Guide
Experiencing persistent jaw pain, clicking sounds when you chew, or debilitating headaches that seem to originate from your face? You're not alone. Temporomandibular joint (TMJ) disorders, often referred to collectively as TMD, affect an estimated 10 million Americans, with women disproportionat
February 23, 2026
Tmj Nerve Damage Symptoms: Complete Guide
Experiencing persistent facial pain, numbness, or tingling can be distressing, especially when the source is unclear. While many people are familiar with general jaw pain associated with temporomandibular joint (TMJ) disorders, the less commonly understood aspect of tmj nerve damage symptoms can
February 23, 2026
Remi Night Guard: Complete Guide
Remi Night Guard: Complete Guide
February 23, 2026