Tmj Massage Near Me: Complete Guide
Key Takeaways
- Temporomandibular joint disorder, commonly known as TMJD, affects millions of Americans, causing debilitating pain, discomfort, and significantly impacting quality of life. If you're experiencing jaw pain, clicking, or difficulty chewing, you're not alone. Up to 15% of American adults experience
Temporomandibular joint disorder, commonly known as TMJD, affects millions of Americans, causing debilitating pain, discomfort, and significantly impacting quality of life. If you're experiencing jaw pain, clicking, or difficulty chewing, you're not alone. Up to 15% of American adults experience chronic facial pain stemming from the temporomandibular joint, with many actively searching for effective relief options like "tmj massage near me." This comprehensive guide from SmilePedia.net will explore TMJ massage as a vital component of a broader treatment strategy, delving into its benefits, techniques, costs, and how to find the best professional care. We'll cover everything from what to expect during a session to how it integrates with other tmj physical therapy approaches and overall tmj treatment near me, ensuring you have the knowledge to make informed decisions about your oral and overall health.
Key Takeaways:
- TMJ Massage Basics: Focuses on relaxing muscles surrounding the jaw joint (temporomandibular joint) to alleviate pain, improve mobility, and reduce tension.
- Professional Care is Key: While self-massage helps, seeking a licensed physical therapist or massage therapist specializing in TMJ is crucial for proper diagnosis and effective treatment.
- Cost & Coverage: A single TMJ massage session typically ranges from $80 to $200, depending on location and provider. Many health insurance plans cover
tmj physical therapywhen prescribed by a dentist or physician.- Session Frequency: Initial treatment often involves 1-2 sessions per week for 4-6 weeks, with maintenance as needed.
- Benefits Beyond Pain Relief: Can reduce headaches, earaches, jaw clicking, and improve sleep quality and mouth opening.
- Integrated Approach: Best results often come from combining massage with other therapies like oral appliances, exercises, and stress management as part of a comprehensive
tmj treatment near meplan.- Actionable Tip: Always consult your dentist or physician before starting any new TMJ treatment to ensure it's appropriate for your specific condition.
What is TMJ Massage and How Can It Help?
The temporomandibular joints (TMJ) are the two joints connecting your lower jaw to your skull, located just in front of your ears. These complex joints allow for the wide range of motions necessary for chewing, speaking, and yawning. When these joints or the surrounding muscles become inflamed, irritated, or dysfunctional, it leads to a temporomandibular joint disorder (TMJD or TMD).
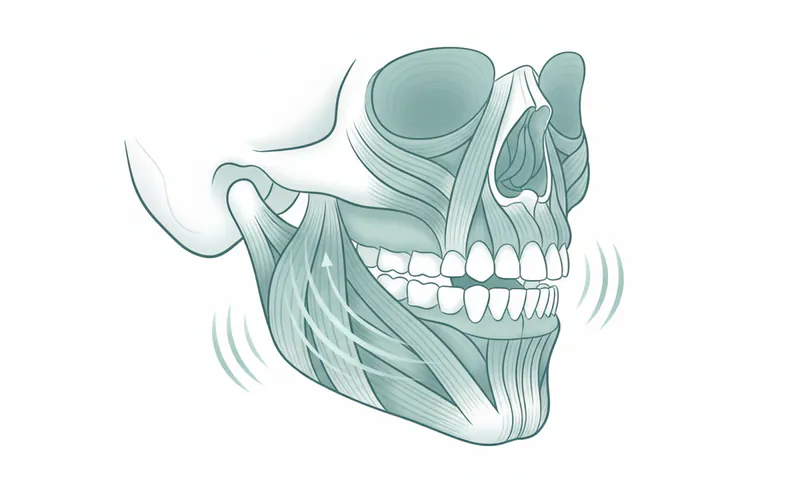
TMJ massage is a specialized therapeutic technique designed to relieve pain and dysfunction associated with TMJD. It targets the muscles of the jaw, face, head, and neck that contribute to TMJ pain and restricted movement. These muscles, such as the masseter, temporalis, and pterygoids, can become chronically tight, spastic, or inflamed due to various factors, leading to a cascade of symptoms.
The primary goal of TMJ massage is to:
- Reduce muscle tension: By applying specific pressure and strokes, the therapist helps to release knots (trigger points) and tightness in the jaw and surrounding musculature.
- Improve blood circulation: Increased blood flow brings vital nutrients to the tissues and helps flush out metabolic waste products, promoting healing.
- Decrease pain: Relaxing tense muscles directly reduces the pain signals sent to the brain.
- Restore range of motion: By releasing tight muscles, the joint can move more freely and comfortably.
- Reduce inflammation: Massage can help mitigate inflammatory responses in the soft tissues.
For many individuals suffering from TMJD, finding "tmj massage near me" is a crucial step towards finding relief, as it offers a non-invasive, drug-free approach to managing symptoms.
Types and Approaches to TMJ Massage
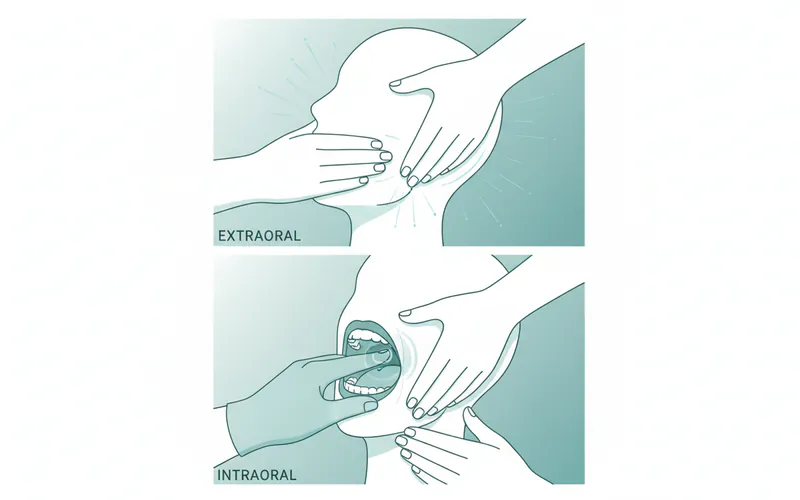
TMJ massage can be broadly categorized into two main types based on where the massage is performed: extraoral (external) and intraoral (internal). Both types are often used together for a comprehensive approach.
Extraoral TMJ Massage
This technique involves massaging the muscles on the outside of the face, head, and neck. It’s typically the first approach taken and can be performed by various licensed professionals, including physical therapists, massage therapists, and sometimes chiropractors specializing in TMJ.
Muscles targeted:
- Masseter: The main chewing muscle, located on the side of your jaw, often tight in individuals who clench or grind.
- Temporalis: A fan-shaped muscle on the side of your head, also involved in chewing and often a source of tension headaches.
- Sternocleidomastoid (SCM): Muscles on the sides of the neck that connect to the skull, often contributing to jaw and head pain due to forward head posture.
- Trapezius and Scalenes: Neck and shoulder muscles that can refer pain to the jaw and head.
- Suboccipitals: Small muscles at the base of the skull, frequently associated with headaches and neck stiffness.
Techniques used:
- Myofascial Release: Gentle, sustained pressure applied to connective tissues (fascia) to release restrictions.
- Trigger Point Therapy: Applying pressure to specific hypersensitive spots (trigger points) in muscles to alleviate pain and referrred discomfort.
- Swedish Massage: General relaxation techniques to reduce overall muscle tension.
- Deep Tissue Massage: More intense pressure to target deeper layers of muscle and connective tissue.
Intraoral TMJ Massage
This more specialized technique involves the therapist inserting a gloved finger inside the mouth to directly access the internal jaw muscles. This is often performed by a physical therapist or a massage therapist with specialized training.
Muscles targeted:
- Medial Pterygoid: Located deep inside the jaw, it helps close the jaw and move it side-to-side.
- Lateral Pterygoid: Crucial for opening the jaw and moving it forward, often implicated in jaw clicking and locking.
Benefits of Intraoral Massage:
- Direct Access: Allows for direct manipulation of muscles that are otherwise inaccessible.
- Deep Release: Can achieve a more profound release of deep-seated tension.
- Improved Jaw Mechanics: Directly addresses muscles affecting jaw movement and alignment.
Self-Massage Techniques
While professional treatment is highly recommended, self-massage can offer temporary relief and complement professional sessions.
Basic Self-Massage Steps:
- Warm-up: Apply a warm compress to your jaw for 5-10 minutes.
- Masseter Muscles: Place your index and middle fingers on your jawline, below your ear. Gently massage in small circles, moving along the jaw towards the chin. Apply moderate pressure.
- Temporalis Muscles: Place your fingertips on your temples. Massage in circular motions, moving up towards your hairline and down towards your cheekbones.
- Intraoral (Careful!): With clean hands, use a gloved finger or very clean thumb to gently press and massage the muscles inside your mouth, along your upper and lower molars. Sweep your finger upwards and outwards to reach the pterygoid muscles. Be very gentle and stop if you feel sharp pain.
Pro Tip: Always consult your physical therapist or dentist before attempting intraoral self-massage to ensure you are targeting the correct areas safely and effectively. They can guide you on proper technique.
Causes and Contributing Factors of TMJD
Understanding the root causes of TMJD is essential for effective treatment. TMJD is often multifactorial, meaning several factors can contribute to its development.
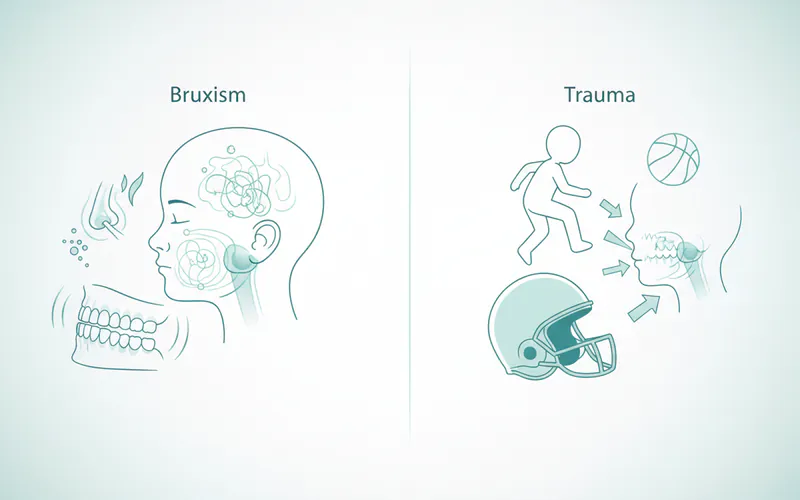
- Bruxism (Teeth Grinding/Clenching): One of the most common culprits. Chronic clenching or grinding, often stress-related or occurring during sleep, puts immense strain on the jaw muscles and joints. The American Dental Association (ADA) recognizes bruxism as a significant contributor to TMJD.
- Stress and Anxiety: High stress levels often lead to muscle tension throughout the body, including the jaw. Emotional stress can trigger or exacerbate bruxism and jaw clenching.
- Trauma to the Jaw, Head, or Neck: A direct blow to the jaw, whiplash injury, or even a dental procedure that requires the mouth to be open for extended periods can cause TMJD.
- Malocclusion (Misaligned Bite): If teeth don't fit together properly when the jaw closes, it can create uneven stress on the TMJ and surrounding muscles. However, dental professionals often debate the extent of its contribution to TMJD compared to other factors.
- Arthritis: Degenerative joint diseases like osteoarthritis or inflammatory conditions like rheumatoid arthritis can affect the TMJ, leading to pain and limited function.
- Disk Displacement: The small articular disc within the TMJ can become displaced, causing clicking, popping, and sometimes locking of the jaw.
- Poor Posture: Forward head posture, common with extended computer use, can strain the neck and jaw muscles, pulling the jaw out of alignment.
- Connective Tissue Diseases: Conditions that affect connective tissues throughout the body, such as Ehlers-Danlos syndrome, can impact joint stability, including the TMJ.
- Habitual Behaviors: Chewing gum excessively, biting nails, or frequently resting your chin on your hand can contribute to jaw strain over time.
Signs and Symptoms of TMJD
The symptoms of TMJD can vary widely in intensity and type. If you experience any of the following, it's worth exploring tmj treatment near me options, including specialized massage:
- Jaw Pain or Tenderness: Often felt in front of the ear, spreading to the cheek, neck, or temples. It can range from dull aching to sharp, acute pain.
- Clicking, Popping, or Grating Sounds: These sounds may occur when opening or closing your mouth. While not always indicative of a problem if pain-free, painful clicking is a red flag.
- Limited Jaw Movement or Locking: Difficulty opening your mouth wide, or feeling like your jaw gets "stuck" in an open or closed position.
- Headaches: Often tension-type headaches, migraines, or pain behind the eyes, frequently stemming from jaw muscle tension.
- Earaches or Ringing in the Ears (Tinnitus): Pain that feels like an earache but isn't an infection, or a persistent ringing sound.
- Facial Pain: General aching or tenderness in the face.
- Pain while Chewing or Biting: Difficulty or pain when eating hard or chewy foods.
- Changes in Bite: A sensation that your upper and lower teeth don't fit together properly.
- Neck and Shoulder Pain: Referred pain from jaw muscles can extend into the neck and shoulders.
- Dizziness: In some cases, TMJD can contribute to feelings of vertigo or imbalance.
Comprehensive TMJ Treatment Options
While tmj massage near me is an excellent tool, it's usually part of a broader, multimodal approach to tmj treatment near me. The goal is to address both symptoms and underlying causes.
1. TMJ Massage and Physical Therapy
- Pros: Non-invasive, often provides immediate pain relief, improves range of motion, reduces muscle tension, can be integrated with home exercises.
- Cons: May require multiple sessions, temporary relief if underlying causes aren't addressed, not a standalone cure for severe structural issues.
- Explanation: A
tmj physical therapyprogram often combines specialized manual therapy (including massage) with therapeutic exercises, postural training, and modalities like heat/cold therapy, ultrasound, or TENS (Transcutaneous Electrical Nerve Stimulation) to strengthen muscles and improve jaw function.
2. Oral Appliances (Splints or Nightguards)
- Pros: Protects teeth from grinding/clenching, repositions the jaw, reduces muscle strain, often very effective for bruxism-related TMJD.
- Cons: Can be costly (custom-made), requires consistent wear, may not be effective for all types of TMJD, some patients find them uncomfortable initially.
- Explanation: Custom-fitted acrylic appliances worn over the teeth, primarily at night. They prevent teeth from grinding, absorb clenching forces, and can help stabilize or reposition the jaw joint.
3. Medications
- Pros: Can quickly alleviate acute pain and inflammation, readily available.
- Cons: Treat symptoms, not causes; potential side effects; not for long-term use.
- Types:
- NSAIDs (Nonsteroidal Anti-Inflammatory Drugs): Over-the-counter (ibuprofen, naproxen) or prescription strength to reduce pain and inflammation.
- Muscle Relaxants: Prescription medications (e.g., cyclobenzaprine) to relieve severe muscle spasms.
- Antidepressants: Low-dose tricyclic antidepressants can help manage pain and improve sleep, even in non-depressed individuals.
- Botox Injections: Injections into the jaw muscles (masseter, temporalis) can relax them, reducing clenching and grinding, providing relief for several months.
4. Lifestyle Modifications and Stress Management
- Pros: Empowering, no side effects, improves overall well-being, addresses a common underlying cause.
- Cons: Requires consistent effort and commitment.
- Explanation: Techniques include mindfulness, meditation, yoga, regular exercise, limiting caffeine, improving sleep hygiene, and avoiding hard or chewy foods.
5. Corrective Dental Treatments
- Pros: Can address structural issues contributing to TMJD.
- Cons: Invasive, potentially expensive, not always necessary or effective for TMJD.
- Explanation: In rare cases, orthodontic treatment (braces), dental crowns, or other restorative procedures may be considered if a significant bite problem is clearly contributing to TMJD, as determined by a qualified dental professional.
6. Minimally Invasive Procedures
- Pros: Less invasive than open surgery, quicker recovery.
- Cons: May not be suitable for all cases, potential for repeat procedures.
- Types:
- Arthrocentesis: A procedure involving the insertion of needles into the joint to lavage (wash out) the joint space, removing inflammatory byproducts and improving disc mobility.
- Steroid Injections: Corticosteroids injected into the joint can reduce inflammation and pain.
7. Surgery (Arthroplasty or Open-Joint Surgery)
- Pros: Can provide long-term relief for severe, intractable cases where other treatments have failed.
- Cons: Invasive, significant risks (nerve damage, infection, scarring), long recovery period, typically a last resort.
- Explanation: Reserved for cases with severe structural damage, tumors, or intractable pain.
Pro Tip: The ADA emphasizes a conservative, reversible approach to TMJD treatment whenever possible, starting with methods like massage, physical therapy, and oral appliances before considering more invasive options.
What to Expect: The Step-by-Step TMJ Massage Process
When you seek professional TMJ massage or tmj physical therapy for your jaw pain, here's a general idea of what to expect:
Step 1: Initial Consultation and Assessment (30-60 minutes)
- Medical History: The therapist will ask about your symptoms, medical history, dental history (e.g., bruxism, past trauma), and any previous treatments.
- Physical Examination:
- Observation: They'll observe your posture, facial symmetry, and how you hold your jaw.
- Palpation: Gently feel the jaw, neck, and facial muscles for tenderness, trigger points, and tightness. They will assess the TMJ joint itself.
- Range of Motion: They'll measure how wide you can open your mouth (vertical opening), and how far you can move your jaw side-to-side and forward.
- Joint Sounds: Listen for clicking, popping, or grating sounds during jaw movement.
- Diagnosis & Treatment Plan: Based on their assessment, the therapist will explain their findings and propose a personalized treatment plan, including the type and frequency of massage, exercises, and other therapies. This is often done in coordination with your dentist or physician.
Step 2: The Massage Session (30-60 minutes)
- Positioning: You'll typically lie on your back on a massage table, or sometimes sit in a chair, to ensure your head and neck are supported and relaxed.
- Extraoral Techniques: The therapist will begin by gently massaging the muscles of your neck, shoulders, and scalp to release general tension that can refer to the jaw. They will then focus on the masseter and temporalis muscles with various strokes, kneading, and trigger point pressure.
- Intraoral Techniques (if indicated): If necessary and agreed upon, the therapist will put on gloves and ask you to open your mouth slightly. They will then gently access the pterygoid muscles inside your mouth, applying pressure and massaging to release deep tension. This part of the massage can feel unusual or slightly intense, but should not be sharply painful. Communicate any discomfort immediately.
- Breathing and Relaxation: Throughout the session, the therapist may guide you to focus on slow, deep breathing to enhance muscle relaxation.
Step 3: Post-Massage Guidance and Home Program
- Immediate Feedback: After the massage, the therapist will ask about your immediate relief and any changes in symptoms.
- Home Exercises: You'll likely be given specific stretches and exercises to perform at home to maintain the benefits of the massage and strengthen jaw muscles. These might include gentle jaw stretches, posture exercises, and relaxation techniques.
- Post-Care Advice: Recommendations may include applying moist heat or cold packs, avoiding hard/chewy foods temporarily, and stress management strategies.
- Follow-Up: The therapist will schedule follow-up appointments based on your individual needs and progress.
Pro Tip: Consistency is key. Adhering to your home exercise program and follow-up sessions will significantly improve your long-term outcome.
Cost and Insurance Coverage for TMJ Massage and Physical Therapy
Understanding the financial aspect of tmj treatment near me is crucial for many patients. Costs for TMJ massage and physical therapy can vary significantly.
Average US Costs (Out-of-Pocket)
- Initial Consultation/Assessment (Physical Therapist): $150 - $350 (Often longer and more comprehensive than follow-up sessions).
- TMJ Massage Session (Specialized Massage Therapist): $80 - $200 per 30-60 minute session.
- TMJ Physical Therapy Session: $100 - $300 per 45-60 minute session (often includes massage, exercises, and modalities).
- Dry Needling (if used by PT): May be an additional $20 - $50 per session or included in the PT session cost.
Factors Influencing Cost:
- Provider Type: Physical therapists and chiropractors often have higher rates than massage therapists due to their broader scope of practice and clinical expertise.
- Location: Urban areas and regions with a higher cost of living (e.g., NYC, California) tend to have higher prices than rural areas.
- Session Length: Longer sessions naturally cost more.
- Clinic Reputation/Specialization: Highly specialized clinics or therapists with advanced certifications may charge more.
- Package Deals: Some clinics offer discounted rates if you purchase a package of multiple sessions.
Insurance Coverage
Navigating insurance for TMJD can be complex.
- Medical Insurance: Most health insurance plans do cover
tmj physical therapywhen it is deemed medically necessary and prescribed by a physician or dentist. However, coverage can vary widely.- Diagnosis Codes: Ensure your referring doctor uses appropriate diagnostic codes (e.g., K07.6 for temporomandibular joint disorders) and the therapist uses relevant CPT (Current Procedural Terminology) codes for the treatments provided (e.g., 97140 for manual therapy, 97110 for therapeutic exercise).
- Referral: Many plans require a referral from a primary care physician (PCP) or dentist.
- Network: Check if the provider is "in-network" with your insurance plan. Out-of-network providers will result in higher out-of-pocket costs.
- Deductibles, Co-pays, Co-insurance: You will still be responsible for these based on your plan.
- Massage Therapy: Standalone massage therapy (without a PT component) is less frequently covered by medical insurance, unless explicitly part of a physical therapy plan or wellness benefit.
- Dental Insurance: Dental insurance generally does not cover TMJ physical therapy or massage, as it typically focuses on dental procedures (fillings, crowns, extractions). However, it may cover oral appliances (nightguards) if deemed medically necessary for TMJD by your dentist.
- HSA/FSA: Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs) can typically be used to pay for TMJ treatment costs, including massage and physical therapy, as they are considered medical expenses.
Pro Tip: Before starting treatment, always contact your insurance provider directly to understand your specific benefits, coverage limits, and any referral requirements for tmj physical therapy or specialized massage. Get pre-authorization if necessary.
Recovery and Aftercare for TMJ Massage
The benefits of TMJ massage extend beyond the session itself. Proper recovery and aftercare are crucial for long-lasting relief and preventing recurrence.
Immediate Aftercare:
- Hydration: Drink plenty of water. Massage helps release toxins, and hydration aids in flushing them out.
- Gentle Movement: Slowly move your jaw through its full, pain-free range of motion. Avoid sudden or forceful movements.
- Heat or Cold: Apply a warm compress or ice pack to the jaw area as recommended by your therapist to soothe muscles and reduce any post-massage soreness.
- Rest: Allow your jaw muscles to rest. Avoid hard, chewy foods for the rest of the day.
Ongoing Home Care:
- Follow Your Home Exercise Program: This is paramount. Your therapist will provide specific stretches and strengthening exercises tailored to your needs. Consistency with these exercises helps maintain jaw mobility and muscle balance.
- Posture Correction: Practice good posture, especially if you spend a lot of time at a computer. Ensure your head is aligned over your shoulders, not jutting forward.
- Stress Management: Implement stress-reduction techniques like meditation, deep breathing, yoga, or spending time in nature. Stress is a major trigger for jaw clenching.
- Dietary Modifications: Stick to soft foods, especially during flare-ups. Avoid chewing gum, hard candies, nuts, and tough meats. Cut food into small pieces.
- Awareness of Habits: Be mindful of habits like nail-biting, lip-biting, or clenching your jaw when stressed or focused.
- Oral Appliance Use: If prescribed a nightguard or splint, wear it consistently as instructed by your dentist.
- Regular Dental Check-ups: Inform your dentist about your TMJ symptoms and treatment plan. Regular check-ups can help monitor your jaw health.
Pro Tip: Keep a symptom journal. Note down your pain levels, triggers, and the effectiveness of your home care routine. This information is invaluable for your therapist to adjust your treatment plan.
Prevention of TMJD
Preventing TMJD involves addressing common risk factors and adopting healthy habits.
- Manage Stress: Since stress is a leading cause of bruxism and jaw clenching, finding effective stress management techniques (e.g., mindfulness, exercise, therapy) is crucial.
- Practice Good Posture: Maintain proper alignment of your head, neck, and shoulders. Avoid forward head posture, especially when using computers or phones.
- Avoid Excessive Jaw Movement:
- Limit wide yawning.
- Avoid excessive gum chewing.
- Do not bite nails, pens, or other hard objects.
- Cut food into smaller, manageable pieces to avoid straining your jaw.
- Identify and Break Bad Habits: Become aware of habits like clenching your jaw during the day. Place gentle reminders (e.g., sticky notes) to keep your jaw relaxed, with your teeth slightly apart and tongue resting on the roof of your mouth.
- Ergonomic Workstation Setup: Ensure your computer screen is at eye level, your chair provides good back support, and your arms are comfortably supported to reduce neck and shoulder strain.
- Regular Dental Check-ups: Your dentist can identify early signs of bruxism or malocclusion and recommend preventative measures or early intervention. If you suspect grinding, discuss a nightguard.
- Balanced Diet: A diet rich in anti-inflammatory foods can support joint health.
Risks and Complications of TMJ Massage
While TMJ massage is generally safe and beneficial, it's important to be aware of potential risks, especially if performed incorrectly or without proper assessment.
Risks Associated with TMJ Massage:
- Temporary Soreness or Bruising: It's common to feel some tenderness or muscle soreness after a deep tissue massage, similar to post-workout muscle ache. Rarely, minor bruising can occur.
- Increased Pain (if improperly performed): If the massage is too forceful, targets the wrong areas, or if there's an underlying acute injury, it could exacerbate pain or inflammation. This highlights the importance of seeking a qualified professional.
- Jaw Joint Discomfort: In rare cases, if the joint itself is unstable or severely inflamed, improper manipulation could cause temporary discomfort.
- Allergic Reaction: To massage oils or lotions used (less common but possible).
- Infection: With intraoral massage, there's a minimal risk of introducing bacteria if the therapist's hygiene isn't impeccable (gloves are mandatory).
Risks of Untreated TMJD:
More significant complications arise from ignoring TMJD symptoms:
- Chronic Pain: Persistent and worsening pain in the jaw, face, head, and neck.
- Permanent Joint Damage: Untreated inflammation or disc displacement can lead to degenerative changes within the TMJ.
- Difficulty Eating and Speaking: Severe pain or locking can make basic functions like chewing and talking extremely difficult.
- Nutritional Deficiencies: Chronic pain or difficulty eating can lead to reduced food intake and subsequent nutritional problems.
- Sleep Disturbances: Pain and discomfort can severely impact sleep quality, leading to fatigue and reduced overall well-being.
- Psychological Impact: Chronic pain is strongly linked to increased rates of depression, anxiety, and reduced quality of life.
- Referred Pain: Persistent TMJD can cause referred pain to other areas, including chronic headaches, neck pain, and ear symptoms.
Pro Tip: Always choose a licensed and experienced therapist (physical therapist, massage therapist, or chiropractor) who specializes in TMJ disorders. Don't hesitate to ask about their qualifications and experience.
Comparison Tables
Here are two tables to help you compare aspects of TMJ treatment.
Table 1: Comparison of Common TMJ Treatment Options
| Treatment Option | Primary Goal | Invasiveness | Typical Duration | Average US Cost Range (Out-of-Pocket) | Pros | Cons |
|---|---|---|---|---|---|---|
| TMJ Massage / Physical Therapy | Muscle relaxation, mobility | Non-invasive | 4-8 weeks (multiple sessions) | $80-$300 per session | Non-pharmacological, improves function, immediate relief | Requires consistent sessions & home exercises, temporary relief alone |
| Oral Appliance (Nightguard) | Jaw repositioning, protection | Non-invasive | Long-term use | $300-$800 (OTC), $500-$2,500 (Custom) | Prevents clenching/grinding, protects teeth, stabilizes joint | Requires consistent wear, can be costly (custom), not for all TMJD |
| Medications (NSAIDs, Muscle Relaxants) | Pain/inflammation reduction | Non-invasive | Short-term | $10-$100+ (Rx) | Quick symptom relief | Treats symptoms, not cause; potential side effects |
| Botox Injections | Muscle relaxation | Minimally invasive | Every 3-6 months | $400-$1,000+ per treatment | Effective for severe clenching/grinding, long-lasting | Temporary, relatively expensive, potential for mild side effects |
| Surgery (Arthrocentesis, etc.) | Joint repair/lavage | Invasive | One-time or rare repeats | $1,000 - $10,000+ | Can resolve severe structural issues | Last resort, higher risks, longer recovery |
Table 2: Estimated Cost Ranges for TMJ Massage / Physical Therapy by US Region
| US Region | Average Cost per 60-min Session (Massage Therapist) | Average Cost per 45-min Session (Physical Therapist) |
|---|---|---|
| Northeast (NYC, Boston) | $120 - $250 | $180 - $350 |
| West Coast (LA, SF) | $110 - $220 | $160 - $320 |
| Midwest (Chicago, Dallas) | $90 - $180 | $130 - $280 |
| Southeast (Atlanta, Miami) | $80 - $160 | $120 - $250 |
| Mountain West (Denver, Phoenix) | $90 - $170 | $130 - $260 |
Note: These are average out-of-pocket costs and can vary based on specific provider, clinic, and insurance coverage.
Children and Pediatric Considerations for TMJD
TMJD is not exclusive to adults; children and adolescents can also experience temporomandibular joint issues. The prevalence in children is lower than in adults but is still a significant concern for parents.
Causes in Children:
- Bruxism: Night grinding is common in children, often related to stress, allergies, or airway issues.
- Trauma: Falls, sports injuries, or blows to the jaw are frequent in childhood.
- Orthodontic Issues: While not a direct cause, some bite irregularities or extensive orthodontic treatment can sometimes contribute or exacerbate TMJD symptoms.
- Clenching: Stress from school, peer pressure, or family issues can lead to jaw clenching.
- Systemic Conditions: Juvenile idiopathic arthritis or other inflammatory conditions can affect the TMJ.
Signs and Symptoms in Children:
Symptoms can be similar to adults but may be harder for children to articulate. Parents should look for:
- Complaints of jaw or ear pain (often mistaken for ear infections).
- Headaches.
- Difficulty chewing certain foods.
- Clicking or popping sounds in the jaw.
- Limited mouth opening.
- Unusual jaw movements.
- Changes in eating habits.
- Tooth wear (from grinding).
Diagnosis and Treatment:
Diagnosis often involves a pediatrician or a pediatric dentist. The approach to tmj treatment near me for children is typically very conservative, prioritizing non-invasive methods.
- Conservative Management: Focus on pain relief, reducing inflammation, and correcting habits.
- TMJ Physical Therapy / Massage: Gentle jaw exercises, stretches, and specialized massage can be highly effective in children to reduce muscle tension and improve jaw function. This is often preferred over medication.
- Oral Appliances: Custom-made nightguards may be used to protect teeth from grinding and help reposition the jaw.
- Lifestyle Changes: Stress reduction techniques, avoiding hard/chewy foods, and ensuring good sleep hygiene.
- Observation: In many cases, especially trauma-related TMJD, symptoms may resolve with time and conservative care as the child grows and heals.
Pro Tip for Parents: If your child complains of jaw pain, headaches, or you notice jaw clicking or tooth grinding, consult your pediatric dentist or a TMJ specialist early. Early intervention can prevent chronic issues.
Cost Breakdown: TMJ Treatment Near Me
A dedicated breakdown of costs to help you budget for comprehensive tmj treatment near me.
Average US Costs (Out-of-Pocket, ranges can vary widely):
| Service / Item | Low Range | Mid Range | High Range | Notes |
|---|---|---|---|---|
| Initial TMJ Consultation (Dentist/PT) | $100 | $250 | $400 | Can be higher for specialists. |
| TMJ Massage Session (30-60 min) | $80 | $150 | $250 | Dependent on therapist, location, and specialization. |
| TMJ Physical Therapy Session (45-60 min) | $100 | $200 | $300 | Includes various modalities and exercises. |
| Custom Oral Appliance (Nightguard) | $500 | $1,500 | $2,500 | Varies by dentist, materials, and complexity. OTC guards are cheaper ($30-$100) but less effective. |
| Botox Injections (for bruxism/pain) | $400 | $700 | $1,200 (per session) | Typically lasts 3-6 months. Cost depends on units used. |
| Medications (monthly supply) | $10 (OTC) | $50 (Generic Rx) | $200+ (Brand Rx) | Varies by prescription, pharmacy, and insurance. |
With vs. Without Insurance:
- Without Insurance (Self-Pay): You will pay the full cash price for all services. Clinics may offer self-pay discounts or package deals.
- With Medical Insurance: For medically necessary
tmj physical therapyprescribed by a doctor, your insurance will typically cover a portion after you meet your deductible. You'll then pay co-pays (e.g., $30-$60 per visit) or co-insurance (e.g., 20% of the cost). Total out-of-pocket costs will depend on your plan's deductible, out-of-pocket maximum, and whether the provider is in-network.
Payment Plans and Financing Options:
- Clinic Payment Plans: Many dental and physical therapy clinics offer in-house payment plans, allowing you to pay for treatment over several months.
- Third-Party Financing: Companies like CareCredit or LendingClub offer specialized healthcare credit cards with deferred interest options for medical and dental expenses.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): These tax-advantaged accounts are excellent ways to save for and pay for TMJ treatment, including massage, physical therapy, and oral appliances.
Cost-Saving Tips:
- Shop Around: Get quotes from multiple providers in your area.
- Check Insurance: Always verify your benefits and coverage before starting treatment.
- Ask for Discounts: Inquire about self-pay discounts, package deals, or hardship programs.
- Start Conservative: Begin with less invasive, often less expensive treatments like massage and
tmj physical therapybefore considering more costly interventions.
Frequently Asked Questions
Is TMJ massage painful?
TMJ massage can cause some discomfort, especially if your muscles are very tense or have trigger points. However, it should not be sharply painful. A qualified therapist will work within your pain tolerance. Communication with your therapist is key; always let them know if the pressure is too much.
How long does it take for TMJ massage to work?
Many people experience some immediate relief after their first session. For more lasting results, a course of treatment, typically 4-8 weeks with 1-2 sessions per week, is often recommended. Consistency with home exercises also significantly impacts the duration of relief.
Can I do TMJ self-massage at home?
Yes, gentle self-massage can provide temporary relief and complement professional treatment. Focus on the masseter and temporalis muscles. However, for intraoral techniques or for addressing underlying issues, professional guidance is essential to avoid potential injury and ensure effectiveness.
Is TMJ massage covered by insurance?
Specialized TMJ massage performed as part of tmj physical therapy and prescribed by a physician or dentist is often covered by medical insurance, subject to your plan's deductible, co-pays, and network restrictions. Standalone massage therapy may not be covered unless explicitly stated in your plan. Always verify with your insurance provider.
How do I find a qualified TMJ massage therapist near me?
Look for physical therapists (PTs) or licensed massage therapists (LMTs) who specialize in craniofacial pain, orofacial pain, or TMJ disorders. You can search online directories for "tmj physical therapy near me" or "tmj massage specialist," or ask your dentist or physician for a referral.
What are the alternatives to TMJ massage?
Alternatives or complementary treatments include tmj physical therapy exercises, oral appliances (nightguards), medications (NSAIDs, muscle relaxants), stress management techniques, Botox injections, and in severe cases, minimally invasive procedures or surgery. A comprehensive tmj treatment near me plan often combines several of these.
How often should I get TMJ massage?
Initially, your therapist might recommend 1-2 sessions per week for a few weeks to address acute symptoms. As your condition improves, sessions may become less frequent, moving to maintenance sessions once a month or as needed.
Can TMJ massage fix jaw clicking?
TMJ massage can help reduce muscle tension that contributes to jaw clicking or popping, especially if the sounds are related to muscle imbalance or tightness. However, if the clicking is due to a displaced disc within the joint, massage alone may not "fix" it but can help alleviate associated pain and improve joint mechanics.
What qualifications should a TMJ massage therapist have?
For optimal care, look for a licensed physical therapist (DPT or PT) or a licensed massage therapist (LMT) who has received specialized training or certification in TMJ dysfunction, myofascial release, or craniofacial therapy. Their expertise ensures they understand the complex anatomy and physiology of the jaw.
How long does a typical TMJ massage session last?
A typical professional TMJ massage session usually lasts between 30 to 60 minutes. Initial assessment appointments may be longer.
When to See a Dentist
While TMJ massage and physical therapy can provide significant relief, it's crucial to know when to seek professional dental or medical attention for your TMJ symptoms.
You should see a dentist or doctor if you experience any of the following:
- Persistent Jaw Pain: If your jaw pain is constant, worsening, or interfering with daily activities (eating, speaking, sleeping) and doesn't improve with conservative home care or over-the-counter pain relievers.
- Difficulty Opening or Closing Your Mouth: If your jaw frequently locks open or closed, making it impossible to move, seek immediate dental or medical attention.
- Significant Changes in Your Bite: If you notice that your teeth suddenly don't fit together properly, or your bite feels "off."
- Unexplained Facial Swelling: Swelling around the jaw joint can indicate inflammation or infection.
- Loud, Painful Clicking or Grating Sounds: While some clicking can be benign, if it's accompanied by pain or discomfort, it warrants a professional evaluation.
- Severe Headaches, Earaches, or Neck Pain: Especially if these symptoms are new, severe, or seem directly related to your jaw movements.
- Limited Jaw Movement: If you can't open your mouth wide enough to eat comfortably or perform oral hygiene.
Emergency vs. Scheduled Appointment:
- Emergency: A locked jaw (where you cannot open or close your mouth at all), severe acute pain, or sudden facial swelling around the jaw joint should prompt an urgent call to your dentist, oral surgeon, or an emergency room.
- Scheduled Appointment: For persistent but manageable pain, chronic clicking, general stiffness, or concerns about bruxism, schedule a regular appointment with your general dentist. They can diagnose the issue, provide initial recommendations, or refer you to a TMJ specialist (oral surgeon, oral and maxillofacial pain specialist, or
tmj physical therapyspecialist).
Your dental health professional is your primary resource for diagnosing TMJD and coordinating a comprehensive tmj treatment near me plan. Do not delay seeking professional advice if your symptoms are concerning or significantly impacting your quality of life.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Tmd Treatment: Complete Guide
Experiencing persistent jaw pain, clicking sounds when you chew, or debilitating headaches that seem to originate from your face? You're not alone. Temporomandibular joint (TMJ) disorders, often referred to collectively as TMD, affect an estimated 10 million Americans, with women disproportionat
February 23, 2026
Tmj Nerve Damage Symptoms: Complete Guide
Experiencing persistent facial pain, numbness, or tingling can be distressing, especially when the source is unclear. While many people are familiar with general jaw pain associated with temporomandibular joint (TMJ) disorders, the less commonly understood aspect of tmj nerve damage symptoms can
February 23, 2026
Remi Night Guard: Complete Guide
Remi Night Guard: Complete Guide
February 23, 2026
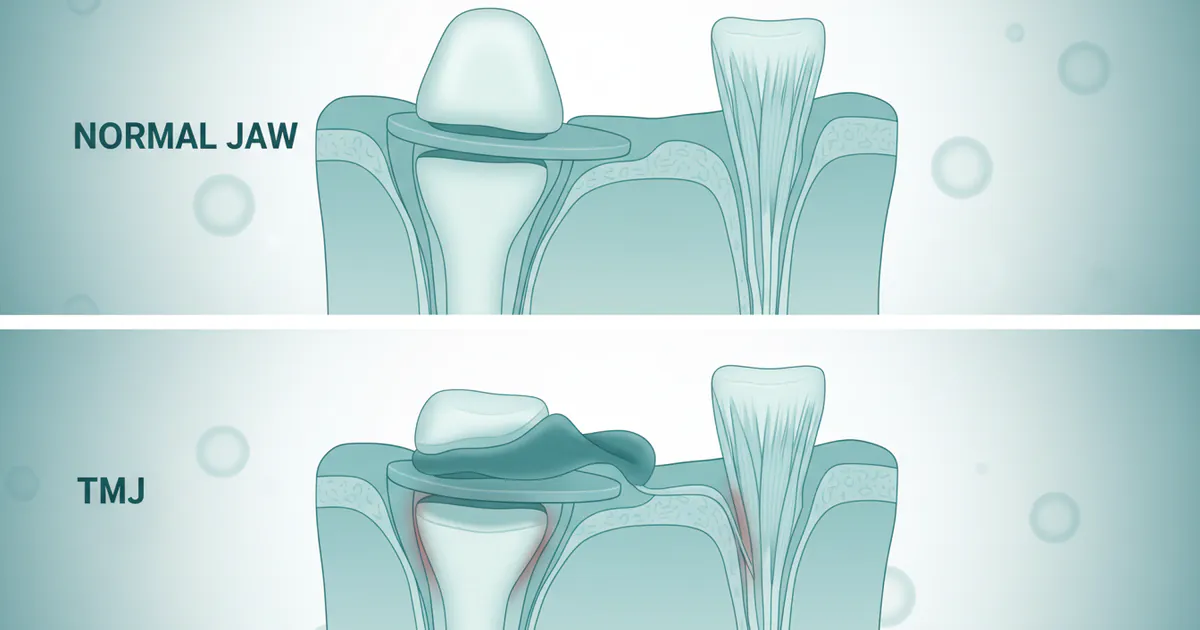
Tmj vs Normal Jaw: Complete Comparison Guide
Experiencing persistent jaw pain, clicking sounds, or difficulty chewing can be frustrating and disruptive to daily life. While many people occasionally feel a stiff jaw, when these symptoms become chronic, they often signal an underlying issue with the temporomandibular joint (TMJ). Understanding t
February 23, 2026