Tmj Meaning: Complete Guide
Key Takeaways
- Temporomandibular joint disorder, often simply referred to as "TMJ," affects millions of Americans, causing a spectrum of uncomfortable and sometimes debilitating symptoms. Imagine struggling to chew your favorite foods, experiencing persistent headaches that medication can’t touch, or hearing a gra
Temporomandibular joint disorder, often simply referred to as "TMJ," affects millions of Americans, causing a spectrum of uncomfortable and sometimes debilitating symptoms. Imagine struggling to chew your favorite foods, experiencing persistent headaches that medication can’t touch, or hearing a grating sound every time you open your mouth. These are daily realities for many. In fact, an estimated 10-15% of adults in the U.S. experience some form of TMJ disorder at any given time, according to the National Institute of Dental and Craniofacial Research (NIDCR). Understanding the tmj meaning isn't just about knowing an acronym; it's about recognizing the complex interplay of your jaw joint, muscles, and nerves, and how disruptions can significantly impact your quality of life. This comprehensive guide from SmilePedia.net will demystify TMJ disorders, exploring everything from their root causes and varied symptoms to the most effective, cutting-edge treatments available, including tmj botox and tmj massage techniques. We'll equip you with the knowledge to identify, manage, and even prevent these common but often misunderstood conditions.
Key Takeaways:
- TMJ (Temporomandibular Joint) refers to the joint itself; TMD (Temporomandibular Disorder) refers to the conditions affecting it.
- Common symptoms include jaw pain, headaches, clicking sounds, and limited jaw movement.
- Conservative treatments like oral appliances (splints), physical therapy (including tmj massage), and lifestyle changes are often the first line of defense and highly effective.
- Botox injections for TMJ (TMD) can provide significant relief for muscle-related pain, with costs ranging from $500 to $1,500 per session and effects lasting 3-6 months.
- The diagnostic process typically involves a dental exam, X-rays, and sometimes MRI or CT scans, costing $50 to $500 depending on complexity and imaging required.
- Most TMD treatments, especially conservative ones, are covered to some extent by dental or medical insurance, but surgical interventions may require extensive pre-authorization.
- Preventative measures focus on stress management, maintaining good posture, and avoiding habits like teeth grinding or excessive gum chewing.
What It Is / Overview: Demystifying the TMJ Meaning
When people say "TMJ," they are often referring to a set of conditions known as Temporomandibular Disorders (TMDs), which affect the jaw joints and the muscles that control jaw movement. However, the acronym TMJ actually stands for the Temporomandibular Joint itself—the two joints connecting your lower jaw (mandible) to your skull (temporal bone) on each side of your head. Think of them as hinges that allow you to open and close your mouth, move your jaw side to side, and forward and back.

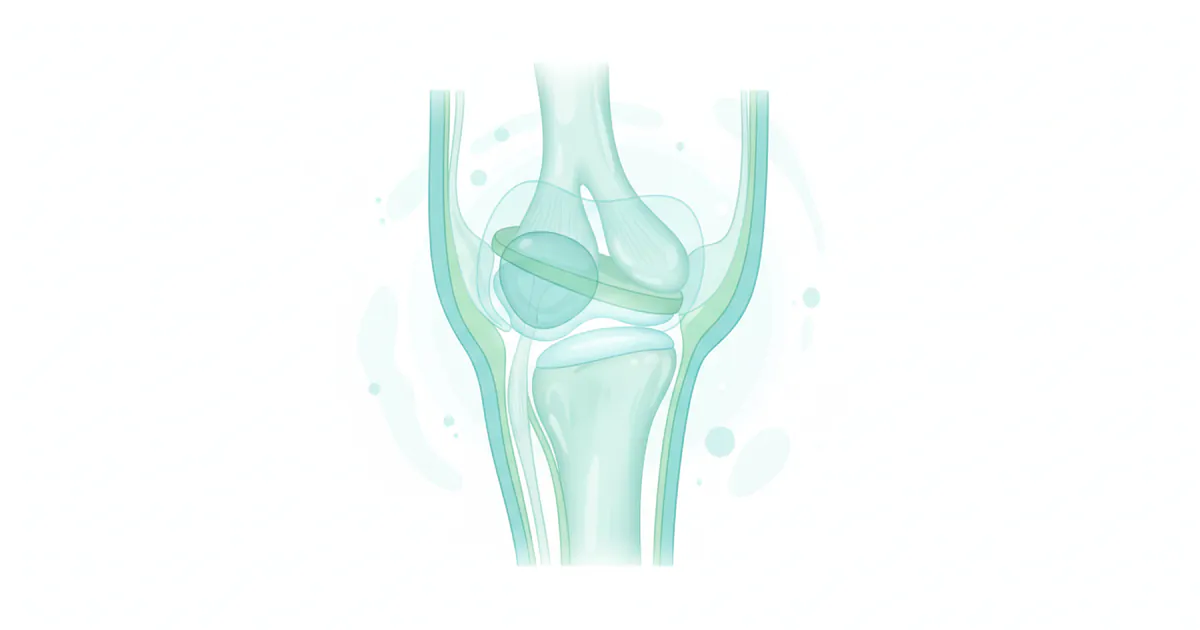
These are among the most complex joints in the body. Each TMJ is composed of:
- The condyle (the rounded end of the lower jawbone).
- The temporal bone (a part of the skull just in front of your ear).
- An articular disc (a small, oval, cushion-like cartilage) located between the condyle and the temporal bone. This disc acts as a shock absorber, ensuring smooth, friction-free movement of the jaw.
- A network of muscles (such as the masseter, temporalis, and pterygoids) that control jaw movement.
- Ligaments that stabilize the joint.
The primary function of your TMJs is to enable essential oral functions: chewing, speaking, yawning, and swallowing. When any part of this intricate system – the joint, disc, muscles, or ligaments – is injured, inflamed, or not working correctly, it can lead to a TMD.
TMDs are relatively common, affecting millions of people. While women are more frequently diagnosed, particularly between the ages of 20 and 40, TMDs can affect anyone regardless of age or gender. The conditions can range from mild discomfort to severe, chronic pain that significantly impacts daily life. Understanding the tmj meaning is the first step toward understanding the challenges and solutions related to these disorders.

Types / Variations of Temporomandibular Disorders (TMDs)
TMDs are not a single condition but a group of complex disorders. Dentists and oral specialists generally categorize them into three main types, although patients often experience a combination:
1. Myofascial Pain
This is the most common type of TMD. It involves discomfort or pain in the muscles that control jaw function (the masseter, temporalis, and pterygoid muscles) and the muscles of the neck and shoulders. This pain is often described as a dull, aching sensation that can spread to the face, head, and neck. It's frequently associated with muscle tension, clenching, grinding (bruxism), or stress.
2. Internal Derangement of the Joint
This refers to a problem with the articular disc (the soft cushion between the ball and socket of the joint).
- Disc Displacement with Reduction: The disc slips out of its normal position when the jaw is closed but returns to its correct position when the mouth is opened. This often causes a "click" or "pop" when opening or closing the mouth.
- Disc Displacement without Reduction: The disc remains displaced even when the jaw is opened. This can lead to limited jaw movement (lockjaw) and often causes a grating sensation rather than a click.
- Perforation of the Disc: In severe cases, the disc can wear down or tear.
3. Degenerative Joint Disease (Arthritis)
This category includes inflammatory and degenerative conditions of the joint itself, similar to arthritis in other joints of the body.
- Osteoarthritis: The cartilage in the joint breaks down, leading to pain, stiffness, and crepitus (a grinding sound or sensation). It's often related to aging and wear and tear.
- Rheumatoid Arthritis: An autoimmune disease that can affect the TMJ, causing inflammation, pain, and damage to the joint structures.
- Other Arthritides: Psoriatic arthritis, ankylosing spondylitis, and gout can also affect the TMJ.
Understanding these distinctions is crucial for accurate diagnosis and tailoring the most effective treatment plan for your specific tmj meaning of discomfort.
Causes / Why It Happens
The exact cause of TMDs is often multifactorial and can be challenging to pinpoint precisely. It's rarely due to a single event but rather a combination of factors. Here are the most common contributors:
Trauma to the Jaw or Joint
A direct impact or injury to the jaw, TMJ, or the surrounding muscles can lead to TMD. This includes:
- Direct facial trauma: Sports injuries, falls, or car accidents (e.g., whiplash) can damage the joint structures or muscles.
- Macro-trauma: A sudden opening of the mouth too wide, such as during a dental procedure, prolonged yawning, or singing, can sometimes strain the joint.
Bruxism (Teeth Grinding and Clenching)
Habitual grinding of teeth (bruxism) or clenching the jaw, especially during sleep (sleep bruxism) or unconsciously during waking hours (awake bruxism), puts immense stress on the TMJ and surrounding muscles. This constant pressure and friction can lead to:
- Muscle fatigue and pain.
- Wear and tear of the articular disc.
- Damage to the tooth enamel.
- Headaches and facial pain. Pro Tip: If you wake up with a sore jaw or headache, you might be clenching or grinding in your sleep. Your dentist can often spot signs of bruxism during a routine exam.
Stress and Anxiety
Emotional stress and anxiety are significant contributors to myofascial TMD pain. When stressed, many individuals unconsciously clench their jaw muscles, leading to muscle tension, fatigue, and pain in the face, head, and neck. This also exacerbates bruxism.
Malocclusion (Bite Issues)
While once considered a primary cause, the role of malocclusion (an improper bite) in TMD is now understood to be more complex and often secondary. Significant bite discrepancies or changes in the way teeth fit together can, in some cases, contribute to uneven stress on the TMJ, leading to symptoms. However, many people with malocclusion never develop TMD, and many with TMD have perfectly aligned bites.
Arthritis and Connective Tissue Disorders
As mentioned in the "Types" section, various forms of arthritis (osteoarthritis, rheumatoid arthritis) can directly affect the TMJ, leading to inflammation, pain, and degeneration of the joint components. Connective tissue disorders like lupus or Ehlers-Danlos syndrome can also predispose individuals to joint laxity and TMDs.
Poor Posture
Chronic poor posture, particularly forward head posture often associated with prolonged computer use or smartphone usage, can strain the neck and shoulder muscles. These muscles are intricately connected to the jaw muscles, and imbalances can lead to tension and pain referred to the TMJ area.
Other Factors
- Hormonal factors: The higher prevalence of TMD in women suggests a potential hormonal link, though research is ongoing.
- Genetics: Some individuals may have a genetic predisposition to chronic pain conditions or joint issues.
- Nutritional deficiencies: Rarely, certain deficiencies can impact joint health.
A thorough diagnosis by a dental professional is essential to identify the specific contributing factors to your TMD, allowing for a targeted and effective treatment strategy.
Signs and Symptoms
The symptoms of TMD can vary widely in intensity and presentation, often mimicking other conditions. This makes accurate diagnosis crucial. If you experience one or more of these symptoms persistently, it's time to consult a dentist or oral health specialist.
Pain and Tenderness
- Jaw pain: Aching or sharp pain in or around the ear, jaw, and face. It might be constant or intermittent.
- Pain while chewing, speaking, or yawning: Activities that engage the jaw can exacerbate discomfort.
- Referred pain: Pain that spreads to the temples, neck, shoulders, or even behind the eyes. Often mistaken for tension headaches or migraines.
- Ear pain: Often confused with an ear infection, this pain can be localized in front of or inside the ear, but it is not typically associated with hearing loss or discharge.
Sounds in the Jaw Joint
- Clicking or popping: A distinct sound when opening or closing the mouth. This usually indicates disc displacement with reduction. It's common and not necessarily problematic unless accompanied by pain or limited movement.
- Grating or crunching (crepitus): A more continuous, rough sound or sensation, often indicative of wear and tear, disc degeneration, or arthritic changes within the joint (disc displacement without reduction).
Restricted Jaw Movement
- Limited mouth opening: Difficulty opening your mouth wide, making it hard to eat or yawn comfortably.
- Jaw locking: The jaw can get "stuck" in an open or closed position, making it difficult to move. This is often sudden and can be quite alarming.
- Stiffness: A feeling of stiffness in the jaw muscles, especially upon waking.
Headaches and Other Symptoms
- Headaches: Frequent tension headaches, migraine-like headaches, or cluster headaches often originate from or are exacerbated by TMD. The pain is typically felt in the temples, forehead, or behind the eyes.
- Ear symptoms: In addition to pain, you might experience ringing in the ears (tinnitus), a feeling of fullness in the ear, or even slight changes in hearing, though these are less common.
- Dizziness: Some individuals report episodes of dizziness.
- Changes in bite: A feeling that your teeth don't fit together properly, or a sudden change in your bite alignment.
- Facial swelling: Rarely, swelling on the side of the face around the affected joint.
If you are experiencing any combination of these symptoms, particularly chronic jaw pain or difficulty with jaw movement, seeking professional evaluation is crucial. Early diagnosis and intervention can prevent the condition from worsening and lead to more effective management.
Treatment Options
The approach to TMD treatment is highly individualized, starting with the least invasive, conservative methods before considering more advanced or surgical interventions. The goal is to reduce pain, restore normal jaw function, and improve your quality of life.
1. Conservative and Non-Invasive Treatments
These are typically the first line of defense and are effective for a large percentage of TMD sufferers.
a. Self-Care and Lifestyle Modifications
Many people find significant relief through simple changes at home:
- Soft food diet: Temporarily avoiding hard, chewy, or sticky foods to rest the jaw.
- Hot/cold packs: Applying moist heat or ice packs to the jaw and temple area for 10-20 minutes several times a day can relieve muscle pain.
- Gentle jaw exercises: Specific stretches and exercises, recommended by your dentist or physical therapist, can improve jaw mobility and reduce muscle tension.
- Stress management: Techniques like meditation, yoga, deep breathing exercises, and counseling can help reduce jaw clenching and muscle tension.
- Avoid habits: Refrain from clenching, grinding, chewing gum, biting nails, or resting your chin on your hand.
- Good posture: Maintain upright posture, especially when sitting for long periods, to reduce strain on neck and jaw muscles.
b. Medications
- Over-the-counter pain relievers: Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen can reduce pain and inflammation.
- Prescription pain relievers: For more severe pain, a dentist may prescribe stronger NSAIDs or, in rare cases, short-term opioids.
- Muscle relaxants: These can help alleviate muscle spasms and tension, especially when taken before bedtime.
- Tricyclic antidepressants: Low doses of these medications, like amitriptyline, can help manage pain and improve sleep, even in individuals without depression.
- Corticosteroids: Occasionally, a short course of oral corticosteroids may be prescribed to reduce severe inflammation.
c. Oral Appliances (Splints or Nightguards)
These custom-made devices are worn over the teeth, usually at night, to reduce the effects of clenching and grinding.
- Stabilization splints (nightguards): These hard acrylic appliances fit over the upper or lower teeth and help relax jaw muscles, protect teeth from wear, and stabilize the bite. They do not permanently change your bite.
- Repositioning splints: Less common, these are designed to temporarily reposition the jaw and disc. Their long-term effectiveness is debated, and they are typically used only for specific cases under close supervision. Pro Tip: An over-the-counter nightguard might offer temporary relief, but a custom-fitted appliance from your dentist is far more effective and comfortable, ensuring proper bite alignment and protecting your jaw.
d. Physical Therapy
A specialized physical therapist can teach you exercises and techniques to improve jaw function. This can include:
- Stretching and strengthening exercises: To improve jaw mobility and muscle coordination.
- Posture training: Correcting head and neck posture to reduce strain on the TMJ.
- Manual therapy: Techniques such as trigger point release, mobilization, and tmj massage to alleviate muscle tension and improve joint movement. A skilled therapist can pinpoint tight areas in the masseter, temporalis, and neck muscles, applying specific pressure and stretching to release knots and improve circulation. TMJ massage is a powerful tool for pain relief and restoring function, often involving both external and intra-oral techniques.
e. Complementary Therapies
- Acupuncture: Some patients find relief from pain and muscle tension through acupuncture.
- Biofeedback: Learning to control physiological responses like muscle tension can help manage pain.
2. Minimally Invasive Procedures
When conservative treatments aren't enough, dentists might consider these options.
a. Trigger Point Injections
Anesthetic or corticosteroid is injected directly into painful muscle trigger points to relieve localized pain and muscle spasms.
b. Botox Injections for TMJ (TMD Botox)
TMJ Botox injections have emerged as a highly effective treatment for chronic TMD, particularly for myofascial pain and headaches related to jaw clenching and grinding.
- How it works: Botulinum toxin (Botox) is injected into the overactive jaw muscles (primarily the masseter and temporalis). It temporarily blocks nerve signals to these muscles, causing them to relax and weaken. This reduces the force of clenching and grinding, thereby alleviating pain and headaches.
- The process: The procedure is quick, usually taking 10-20 minutes, and involves several small injections into the targeted muscles. Discomfort is minimal.
- Duration of effect: The effects typically become noticeable within a few days to a week and last for 3 to 6 months. Repeat injections are necessary to maintain results.
- Pros: Highly effective for muscle-related pain, non-surgical, minimal downtime, can reduce tooth wear.
- Cons: Temporary, requires repeat treatments, potential for temporary facial asymmetry or weakness (rare), not covered by all insurance plans.
- Cost: TMJ Botox costs in the U.S. generally range from $500 to $1,500 per session, depending on the number of units required and the provider's fees.
c. Arthrocentesis
This involves inserting small needles into the joint and flushing it with sterile fluid to remove inflammatory byproducts and adhesions. It can also help lubricate the joint. It's an outpatient procedure often performed under local anesthesia.
3. Surgical Interventions
Surgery is considered a last resort for TMD and is only recommended for severe cases where other treatments have failed, or when there are structural problems within the joint that require repair.

a. Arthroscopy
A minimally invasive surgery where a small incision is made, and a tiny camera (arthroscope) is inserted into the joint. The surgeon can then visualize the joint and perform minor repairs, remove scar tissue, or reposition the disc.
b. Open-Joint Surgery (Arthroplasty)
For more extensive repairs, such as removing bone spurs, reshaping joint structures, or repairing/replacing the disc, open-joint surgery may be necessary. This involves a larger incision to access the joint directly.
c. Total Joint Replacement
In rare, severe cases of irreparable joint damage (e.g., due to trauma, severe arthritis, or developmental abnormalities), the entire temporomandibular joint may need to be surgically replaced with an artificial implant.
Step-by-Step Process: What to Expect During Treatment
Navigating TMD treatment involves several stages, beginning with diagnosis and moving through various therapeutic interventions. Here’s a typical patient journey:
1. Initial Consultation and Diagnosis
- Dental Visit: Your journey usually starts with your general dentist, who will take a detailed medical history, asking about your symptoms, pain levels, and any previous treatments.
- Physical Examination: The dentist will physically examine your jaw, palpating the muscles, checking for tenderness, listening for clicks or pops during jaw movement, and assessing your range of motion. They will also examine your teeth for signs of wear from grinding.
- Imaging:
- X-rays: Standard dental X-rays (panoramic X-rays) can show the bone structure of the jaw and TMJ.
- CT Scan (Computed Tomography): Provides more detailed images of the bone structure.
- MRI (Magnetic Resonance Imaging): The gold standard for visualizing the soft tissues of the joint, including the articular disc and surrounding muscles, to assess for displacement or inflammation.
- Referral: If the case is complex, your dentist may refer you to a specialist such as an oral and maxillofacial surgeon, an oral medicine specialist, or a prosthodontist.
2. Developing a Treatment Plan
Based on the diagnosis, your dental professional will discuss a personalized treatment plan. This often begins with the most conservative approaches.
3. Implementation of Conservative Treatments
- Oral Appliance Fitting: If a nightguard or splint is recommended, impressions of your teeth will be taken, and the custom appliance will be fabricated. You'll have follow-up appointments to adjust the fit.
- Physical Therapy Sessions: If prescribed, you'll begin regular sessions with a physical therapist, learning exercises, posture correction, and receiving manual therapy, including tmj massage.
- Medication Management: Your dentist will prescribe or recommend appropriate medications and monitor their effectiveness.
- Lifestyle Changes: You'll receive guidance on modifying your diet, stress management techniques, and avoiding harmful habits.
4. Considering Minimally Invasive Options (If Needed)
If conservative methods don't provide sufficient relief after several weeks or months, your dentist might discuss options like:
- TMJ Botox Injections: If chosen, you’ll schedule an appointment for the injection. The procedure itself is quick, and you can typically resume normal activities immediately. Follow-up appointments will be scheduled to assess effectiveness and determine if repeat injections are needed.
- Arthrocentesis: This outpatient procedure is performed by an oral surgeon, usually under local anesthesia.
5. Surgical Evaluation (Rarely Necessary)
For a small percentage of patients with severe, persistent symptoms and structural damage, surgical consultation will be initiated. This involves detailed discussions with an oral and maxillofacial surgeon about the specific procedure, potential outcomes, and recovery.
6. Ongoing Management and Follow-Up
TMD is often a chronic condition requiring ongoing management. Regular follow-up appointments with your dentist or specialist are crucial to monitor your progress, adjust treatments, and prevent recurrence. This includes checking the fit of oral appliances, assessing muscle tension, and reviewing your overall symptom management.
Cost and Insurance
Understanding the financial aspect of TMD treatment is critical, as costs can vary significantly depending on the severity of the condition, the type of treatment, and geographic location within the U.S.
Diagnostic Costs
- Initial Consultation: $50 - $250 (can vary based on specialist vs. general dentist).
- X-rays (e.g., panoramic): $50 - $200.
- CT Scan: $300 - $800.
- MRI: $500 - $2,500 (more expensive due to detailed soft tissue imaging).
- Electromyography (EMG) or other specialized tests: $100 - $500.
Treatment Costs
| Treatment Type | Average US Cost Range (Without Insurance) | Notes |
|---|---|---|
| Conservative Treatments | ||
| Over-the-counter NSAIDs | $5 - $20 per bottle | Ongoing expense. |
| Prescription Muscle Relaxants/Analgesics | $20 - $200 per prescription | Varies by medication and duration. |
| Custom Oral Appliance (Nightguard/Splint) | $300 - $800 | One-time cost, but may need replacement every 3-7 years. Some basic OTC nightguards are $20-$50 but are less effective and can sometimes worsen conditions. |
| Physical Therapy Sessions | $75 - $250 per session | Often requires 6-12 sessions. |
| Minimally Invasive Procedures | ||
| Trigger Point Injections | $100 - $300 per session | May require multiple injections. |
| TMJ Botox Injections | $500 - $1,500 per session | Depends on the number of units used and the provider. Effects last 3-6 months, so this is an recurring cost. |
| Arthrocentesis | $1,000 - $3,000 | Usually a single outpatient procedure. |
| Surgical Interventions | ||
| TMJ Arthroscopy | $5,000 - $15,000 | Includes surgeon's fees, anesthesia, and facility costs. |
| Open-Joint Surgery (Arthroplasty) | $15,000 - $50,000+ | Highly variable depending on complexity, includes surgeon's fees, hospital stay, anesthesia. |
| Total Joint Replacement | $30,000 - $100,000+ per joint | Complex procedure, high costs for prosthetic joint, surgery, hospital stay, and extensive follow-up. Some advanced prosthetic joints can push costs even higher. |
Insurance Coverage Details
The good news is that many TMD treatments are covered, at least in part, by either dental or medical insurance. However, coverage can be complex and depends heavily on your specific plan.
- Medical Insurance: Generally, medical insurance is more likely to cover TMD treatments, especially if the condition is diagnosed as a medical problem (e.g., musculoskeletal disorder, chronic pain). This includes diagnostic imaging (MRI, CT scans), physical therapy, prescription medications, tmj botox injections, and surgical procedures. You'll likely need a referral from your physician or dentist to a specialist for coverage.
- Dental Insurance: Dental insurance typically covers treatments related to the teeth, such as oral appliances (splints/nightguards) for bruxism, as these are considered preventative or restorative for dental health. However, coverage for tmj botox or extensive medical procedures related to the joint itself is less common through dental plans.
- Deductibles and Co-pays: Be prepared for deductibles (the amount you pay before insurance starts covering) and co-pays (a fixed amount you pay for each service) as per your insurance policy.
- Pre-authorization: For more expensive treatments like tmj botox or surgery, insurance companies almost always require pre-authorization. This means your provider must submit documentation to your insurer demonstrating medical necessity before the treatment is performed. Without it, your claim might be denied.
Payment Plans and Financing Options
Many dental and oral surgery offices offer:
- Payment plans: In-house plans allowing you to pay for treatment over several months.
- Third-party financing: Companies like CareCredit or LendingClub offer specialized healthcare credit cards with deferred interest options if paid within a certain timeframe.
- Discounts: Some providers offer discounts for upfront payment or for patients without insurance.
Pro Tip: Always contact your insurance provider directly before starting any major treatment to understand your specific coverage, deductibles, co-pays, and pre-authorization requirements for TMD. Get everything in writing if possible.
Recovery and Aftercare
Recovery from TMD treatment varies significantly based on the interventions used, but general principles apply to support healing and prevent recurrence.
General Aftercare for Conservative Treatments
- Consistency with Appliances: If you have an oral appliance, wear it as directed by your dentist. Consistent use is key for muscle relaxation and joint stabilization. Clean it regularly with a toothbrush and mild soap or denture cleaner.
- Adherence to Exercises: Continue with any prescribed jaw exercises and stretches. They help maintain flexibility and strength.
- Dietary Modifications: Continue to follow a soft food diet, especially during flare-ups. Avoid hard, chewy, or sticky foods. Cut food into small pieces.
- Stress Management: Integrate stress-reduction techniques into your daily routine. This is crucial for managing muscle tension and preventing clenching/grinding.
- Posture Awareness: Be mindful of your posture throughout the day, especially if you spend a lot of time at a desk or looking at screens.
- Regular Check-ups: Continue with your scheduled dental appointments to monitor your TMJ health and the effectiveness of your treatment.
Specific Aftercare for TMJ Botox Injections
- Immediate Post-Injection: You may experience mild bruising, swelling, or redness at the injection sites. This is typically temporary.
- Avoid Rubbing: Do not rub or massage the treated areas for at least 24 hours, as this can cause the Botox to spread to unintended muscles.
- Activity: You can usually resume normal activities immediately, but avoid strenuous exercise for 24 hours.
- Results: Noticeable relief often begins within 3-7 days, with full effects seen at 2 weeks. Plan for repeat injections every 3-6 months to maintain benefits.
Aftercare for Surgical Procedures (Arthrocentesis, Arthroscopy, Open Surgery)
Surgical recovery will be more involved and require specific instructions from your oral surgeon.
- Pain Management: You will likely be prescribed pain medication. Take it as directed.
- Diet: A soft or liquid diet will be necessary for a period, gradually transitioning back to solid foods.
- Ice Packs: Apply ice to the surgical site to reduce swelling.
- Limited Jaw Movement: You will need to limit jaw movement for a specific period to allow for healing.
- Physical Therapy: Often, post-surgical physical therapy is crucial to restore range of motion and strengthen jaw muscles.
- Follow-up Appointments: Attend all scheduled follow-up appointments to ensure proper healing and monitor for complications.
Prevention
While not all TMDs are preventable, many cases, especially those related to muscle tension and teeth grinding, can be mitigated through proactive measures.
-
Practice Good Oral Habits:
- Avoid clenching and grinding: Become aware of when you clench or grind your teeth during the day. If you catch yourself, try to relax your jaw.
- Don't chew gum excessively: Constant chewing can overwork your jaw muscles.
- Avoid hard foods: Limit extremely crunchy or chewy foods that put strain on your jaw.
- Don't open your mouth too wide: Try to control extreme yawns or stretches.
-
Manage Stress:
- Incorporate relaxation techniques: Yoga, meditation, deep breathing exercises, and mindfulness can help reduce overall body tension, including in the jaw.
- Seek professional help: If stress and anxiety are overwhelming, consider counseling or therapy.
-
Maintain Good Posture:
- Ergonomics: Set up your workspace to promote good posture, keeping your computer screen at eye level and your shoulders relaxed.
- Awareness: Avoid prolonged forward head posture (e.g., looking down at phones for extended periods) which strains neck and jaw muscles.
-
Regular Dental Check-ups:
- Your dentist can identify early signs of bruxism, malocclusion, or jaw problems. Early intervention is key.
- If you're prescribed a nightguard, ensure it fits properly and is used consistently.
-
Protect Your Jaw from Trauma:
- Wear a mouthguard during contact sports.
- Be cautious during activities that could lead to head or jaw injury.
By adopting these preventative strategies, you can significantly reduce your risk of developing TMD or minimize the severity of symptoms if they occur.
Risks and Complications
While TMD treatments are generally safe and effective, like any medical intervention, they carry potential risks and complications. It's important to discuss these with your healthcare provider.
Risks of Conservative Treatments
- Medication Side Effects: NSAIDs can cause stomach upset, and long-term use can lead to ulcers or kidney problems. Muscle relaxants can cause drowsiness. Antidepressants have various side effects, including dry mouth or dizziness.
- Oral Appliance Discomfort: Initial discomfort or slight changes in speech may occur with nightguards, though these usually subside. Rarely, a poorly fitted appliance can exacerbate symptoms.
- Physical Therapy Soreness: Muscle soreness after tmj massage or exercises is common and temporary.
Risks of Minimally Invasive Procedures
- TMJ Botox Injections:
- Temporary Weakness: Temporary weakness of adjacent muscles can lead to subtle changes in facial expression, drooping eyelid (ptosis), or difficulty chewing (rare).
- Asymmetry: Slight facial asymmetry can occur if the Botox spreads unevenly.
- Bruising/Swelling: Temporary bruising or swelling at the injection sites.
- Headache: Mild, temporary headache.
- Allergic Reaction: Extremely rare, but possible.
- Arthrocentesis:
- Infection: Risk of infection, though low.
- Nerve Damage: Temporary or permanent nerve damage (rare).
- Bleeding: Minor bleeding.
- Pain: Post-procedure pain and swelling.
Risks of Surgical Interventions
Surgical risks are more significant and vary based on the invasiveness of the procedure.
- Infection: Any surgery carries a risk of infection.
- Nerve Damage: Damage to facial nerves can lead to temporary or permanent facial weakness, numbness, or altered sensation.
- Bleeding: Post-operative bleeding.
- Scarring: Visible scarring from incisions.
- Anesthesia Risks: Adverse reactions to general anesthesia.
- Persistent Pain: Surgery doesn't guarantee complete pain relief, and some patients may still experience discomfort.
- Limited Jaw Movement: Adhesions or scar tissue can sometimes lead to continued restricted jaw movement.
- Failed Procedure: The surgery may not achieve the desired outcome, or complications might require further intervention.

Complications of Untreated TMD
Ignoring TMD symptoms can lead to more severe problems:
- Chronic Pain: Persistent and worsening pain in the jaw, face, head, and neck.
- Severe Joint Damage: Progressive degeneration of the TMJ, leading to arthritis and potentially requiring surgery.
- Permanent Bite Changes: Irreversible alterations in how your teeth fit together.
- Nutritional Deficiencies: Difficulty eating can impact nutrition.
- Psychological Impact: Chronic pain can lead to depression, anxiety, and reduced quality of life.
Therefore, seeking timely diagnosis and appropriate treatment is crucial for managing TMD and preventing long-term complications.
Comparison Table: Oral Appliances vs. TMJ Botox
Choosing between different treatment modalities can be challenging. Here's a comparison of two popular and effective non-surgical options: custom oral appliances (nightguards/splints) and TMJ Botox injections.
| Feature | Custom Oral Appliance (Nightguard/Splint) | TMJ Botox Injections |
|---|---|---|
| Primary Goal | Protect teeth from grinding/clenching, stabilize joint, relax muscles. | Relax hyperactive jaw muscles, reduce clenching/grinding force, alleviate pain. |
| Mechanism | Physical barrier and bite repositioning to reduce force on joint. | Neuromuscular blocker that temporarily weakens specific jaw muscles. |
| Ideal For | Bruxism, mild to moderate myofascial pain, disc displacement with reduction. | Chronic myofascial pain, tension headaches, severe clenching/grinding where muscle relaxation is key. |
| Cost (avg. US) | $300 - $800 (one-time, excluding replacement) | $500 - $1,500 per session (recurring every 3-6 months) |
| Duration of Effect | Continuous while worn, durable for several years. | 3-6 months, requires repeat injections. |
| Pros | Non-invasive, durable, protects teeth, often covered by dental insurance. | Highly effective for muscle pain, quick procedure, minimal downtime, can significantly reduce pain and associated headaches. |
| Cons | Can be uncomfortable initially, requires consistent wear, doesn't address muscle hyperactivity directly. | Temporary, requires repeat injections, higher recurring cost, potential for temporary side effects (weakness, asymmetry), less likely covered by dental insurance (more medical coverage). |
| Insurance | Often covered by dental insurance. | Often covered by medical insurance (if deemed medically necessary), less likely by dental. |
Children / Pediatric Considerations
TMD is not exclusive to adults; children and adolescents can also experience temporomandibular disorders, though often with different prevalence rates and symptom presentations. It's estimated that 6-20% of children and adolescents may experience some form of TMD.
Causes in Children
- Trauma: Falls, sports injuries, or direct blows to the jaw or head are common causes in children.
- Parafunctional Habits: While less frequent in very young children, older children and adolescents can develop habits like teeth grinding (bruxism), clenching, nail-biting, or excessive gum chewing.
- Orthodontic Treatment: While often beneficial for bite correction, in some cases, orthodontic forces or prolonged mouth opening during procedures can temporarily stress the TMJ. However, orthodontic treatment is rarely a direct cause of chronic TMD.
- Developmental Factors: Congenital anomalies or developmental issues with the jaw or joint structures can contribute.
- Stress: Academic pressure, social anxiety, or family issues can manifest as jaw clenching or muscle tension in children, similar to adults.
- Systemic Conditions: Juvenile rheumatoid arthritis or other systemic inflammatory conditions can affect the TMJ.
Signs and Symptoms in Children
Children may not always articulate their pain clearly. Parents should look for:
- Difficulty chewing: Child complains of pain when eating, or avoids certain foods.
- Clicking or popping sounds: Heard or felt by the child or parent when the child opens or closes their mouth.
- Headaches: Frequent headaches, especially in the temporal region.
- Ear pain: Unexplained earaches without signs of infection.
- Limited mouth opening: Child struggles to open their mouth wide.
- Facial pain: Child points to pain in the jaw or face.
- Tooth wear: Signs of teeth grinding may be evident on dental examination.
Treatment for Children
Treatment for TMD in children is generally very conservative and focuses on guiding proper development and alleviating symptoms.
- Education and Awareness: Teaching children about their habits (e.g., stopping thumb sucking, nail biting, clenching) and the importance of gentle jaw movements.
- Soft Diet: Temporary dietary modifications.
- Physical Therapy: Gentle exercises and tmj massage techniques adapted for children.
- Oral Appliances: Custom-made nightguards or splints may be used, especially for bruxism, but often with careful consideration for growth and development.
- Stress Management: Helping children develop coping mechanisms for stress.
- Medications: Over-the-counter pain relievers for short-term symptom relief. Prescription medications are used sparingly.
- Orthodontic Consultation: If malocclusion is a significant contributing factor, an orthodontist may be consulted, though orthodontic treatment alone is rarely a primary TMD solution.
- Psychological Support: Counseling for children experiencing significant stress or anxiety.
Surgical intervention for pediatric TMD is extremely rare and only considered in cases of severe structural damage or developmental abnormalities that profoundly impact function and quality of life. The American Dental Association (ADA) emphasizes a conservative, reversible approach for TMD in both adults and children, focusing on non-invasive therapies first.
Frequently Asked Questions
What does "TMJ" actually mean, and how is it different from "TMD"?
TMJ stands for the Temporomandibular Joint, which is the anatomical hinge connecting your lower jaw to your skull. TMD stands for Temporomandibular Disorder, which is the medical condition referring to problems and pain in these joints and the surrounding muscles. So, you have two TMJs, but you might suffer from TMD.
How painful is TMD, and does it go away on its own?
TMD pain varies greatly from mild discomfort to severe, debilitating pain. It can be constant or intermittent. While some mild cases, especially those triggered by temporary stress, might resolve on their own with self-care, most persistent TMD symptoms require professional intervention. Untreated TMD can worsen over time.
How long does TMJ treatment take to work?
The timeline for relief varies. Conservative treatments like medications, soft diets, and lifestyle changes can provide some relief within days to weeks. Oral appliances may take several weeks to months to show full benefits. TMJ Botox injections typically start working within 3-7 days, with full effect at 2 weeks, lasting 3-6 months. Surgical recovery is longer, ranging from weeks to several months.
Is TMJ Botox a permanent solution for jaw pain?
No, TMJ Botox is not a permanent solution. Its effects are temporary, typically lasting 3 to 6 months. To maintain the benefits of muscle relaxation and pain reduction, repeat injections are necessary. It effectively manages symptoms but does not cure the underlying condition.
How much does TMJ Botox cost, and is it covered by insurance?
In the U.S., TMJ Botox typically costs between $500 and $1,500 per session. The price depends on the number of units used and the provider's fees. Medical insurance may cover it if deemed medically necessary for chronic pain or severe bruxism, but dental insurance usually does not. Pre-authorization is often required.
What are the main alternatives to TMJ Botox for muscle pain?
Alternatives to TMJ Botox for muscle-related TMD pain include custom oral appliances (nightguards/splints), physical therapy (including specific tmj massage techniques and exercises), prescription muscle relaxants, trigger point injections (using anesthetics or corticosteroids), and stress management techniques.
Can TMJ massage really help with jaw pain?
Yes, TMJ massage, especially when performed by a skilled physical therapist or massage therapist trained in jaw musculature, can be very effective. It helps to release tension in the jaw, neck, and facial muscles, reduce muscle spasms, improve circulation, and increase range of motion, providing significant pain relief for myofascial TMD.
Do I need surgery for my TMJ?
Surgery for TMD is considered a last resort. It's typically recommended only for a small percentage of patients (less than 10%) who have severe structural problems within the joint and have not found relief from extensive conservative or minimally invasive treatments. Always seek multiple opinions before considering surgery.
Can stress cause TMJ problems?
Yes, stress and anxiety are major contributors to TMD, particularly myofascial pain. When under stress, many people unconsciously clench their jaw muscles, grind their teeth (bruxism), or tense their neck and shoulder muscles, which directly impacts the TMJ and causes pain and dysfunction.
What's the best type of doctor to see for TMJ problems?
You should start with your general dentist. If your condition is complex or persistent, they may refer you to a specialist such as an oral and maxillofacial surgeon, a prosthodontist, an oral medicine specialist, or a physical therapist specializing in head and neck conditions.
When to See a Dentist
Recognizing the signs and knowing when to seek professional help for your TMJ symptoms can prevent conditions from worsening and lead to more effective treatment outcomes.
Clear Warning Signs That Need Attention:
- Persistent Jaw Pain: If you experience daily or near-daily pain in your jaw, face, ear, or neck that lasts for more than a few days and doesn't improve with basic self-care (like soft foods or over-the-counter pain relievers).
- Limited Jaw Movement: You notice you can't open your mouth as wide as before, or your jaw feels stiff or gets stuck (locked) when trying to open or close it. This is a significant red flag.
- Loud Clicking, Popping, or Grating with Pain: While some jaw sounds can be normal, if they are loud, persistent, and especially if accompanied by pain or difficulty chewing, it warrants an evaluation.
- Frequent Headaches or Earaches: If you experience chronic headaches (especially tension-type or migraine-like) or earaches that are not related to colds, flu, or ear infections, and you also have jaw symptoms, TMD could be the cause.
- Changes in Your Bite: If you suddenly feel that your teeth don't fit together properly, or your bite feels "off," this can indicate a TMJ issue.
Red Flags vs. Routine Care Guidance:
- Routine Care: Mild, infrequent jaw clicking without pain, occasional jaw stiffness that resolves quickly, or minor discomfort after a very chewy meal are generally not immediate emergencies but should be mentioned during your next routine dental check-up. Your dentist can monitor these.
- Red Flags: Any of the "warning signs" listed above, especially if they are severe, worsening, or significantly interfering with your ability to eat, speak, or sleep, are red flags that necessitate a prompt dental visit.
Emergency vs. Scheduled Appointment Guidance:
- Emergency Appointment: If your jaw is completely locked (unable to open or close) and you are in severe pain, or if you suspect a jaw dislocation or fracture after trauma, seek immediate emergency dental or medical care.
- Scheduled Appointment: For most other persistent or worsening TMD symptoms, a scheduled appointment with your general dentist is the appropriate first step. They can diagnose the issue and guide you toward the right specialist or treatment plan.
Delaying treatment for TMD can lead to more chronic pain, increased joint damage, and more complex and costly interventions down the line. Don't hesitate to reach out to your dental professional if you suspect you might have a temporomandibular disorder.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Tmj Massage Near Me: Complete Guide
Temporomandibular joint disorder, commonly known as TMJD, affects millions of Americans, causing debilitating pain, discomfort, and significantly impacting quality of life. If you're experiencing jaw pain, clicking, or difficulty chewing, you're not alone. Up to 15% of American adults experience
February 23, 2026
Tmd Treatment: Complete Guide
Experiencing persistent jaw pain, clicking sounds when you chew, or debilitating headaches that seem to originate from your face? You're not alone. Temporomandibular joint (TMJ) disorders, often referred to collectively as TMD, affect an estimated 10 million Americans, with women disproportionat
February 23, 2026
Tmj Nerve Damage Symptoms: Complete Guide
Experiencing persistent facial pain, numbness, or tingling can be distressing, especially when the source is unclear. While many people are familiar with general jaw pain associated with temporomandibular joint (TMJ) disorders, the less commonly understood aspect of tmj nerve damage symptoms can
February 23, 2026
Remi Night Guard: Complete Guide
Remi Night Guard: Complete Guide
February 23, 2026