Tmd Treatment: Complete Guide
Key Takeaways
- Experiencing persistent jaw pain, clicking sounds when you chew, or debilitating headaches that seem to originate from your face? You're not alone. Temporomandibular joint (TMJ) disorders, often referred to collectively as TMD, affect an estimated 10 million Americans, with women disproportionat
Tmd Treatment: Complete Guide
Experiencing persistent jaw pain, clicking sounds when you chew, or debilitating headaches that seem to originate from your face? You're not alone. Temporomandibular joint (TMJ) disorders, often referred to collectively as TMD, affect an estimated 10 million Americans, with women disproportionately impacted. These conditions can range from mild discomfort to severe, chronic pain that significantly interferes with daily life, impacting everything from eating and speaking to sleeping and overall well-being. Understanding the complexities of TMD and the comprehensive range of available tmd treatment options is the crucial first step toward finding relief and reclaiming your quality of life. This complete guide from SmilePedia.net will demystify TMD, exploring its causes, symptoms, and the full spectrum of treatments, from conservative home remedies and the effectiveness of a night guard for TMJ to advanced medical and surgical interventions. We'll provide you with detailed insights into what to expect, associated costs, recovery, and how to prevent future flare-ups, empowering you with the knowledge to make informed decisions about your dental health.
Key Takeaways:
- TMD is common: Affects over 10 million Americans, often manifesting as jaw pain, headaches, and clicking sounds.
- Diagnosis is key: A thorough dental and medical evaluation is essential to determine the specific type and tmj causes of your disorder.
- Conservative first: Initial tmd treatment often involves self-care, physical therapy, stress management, and medications, with many finding relief through these methods.
- Night guards are effective: Custom-fitted oral appliances, like a night guard for TMJ, are a common and effective non-invasive treatment for bruxism-related TMD, typically costing $300-$800.
- Costs vary widely: Treatment expenses can range from $50-$200 for basic self-care and over-the-counter medications to $2,000-$5,000+ for complex dental work or $10,000-$50,000+ for surgical interventions.
- Insurance coverage: Dental and medical insurance coverage for TMD treatments is highly variable; always verify with your provider.
- Prevention is possible: Managing stress, avoiding hard foods, and maintaining good posture can help prevent TMD symptoms.
What It Is / Overview
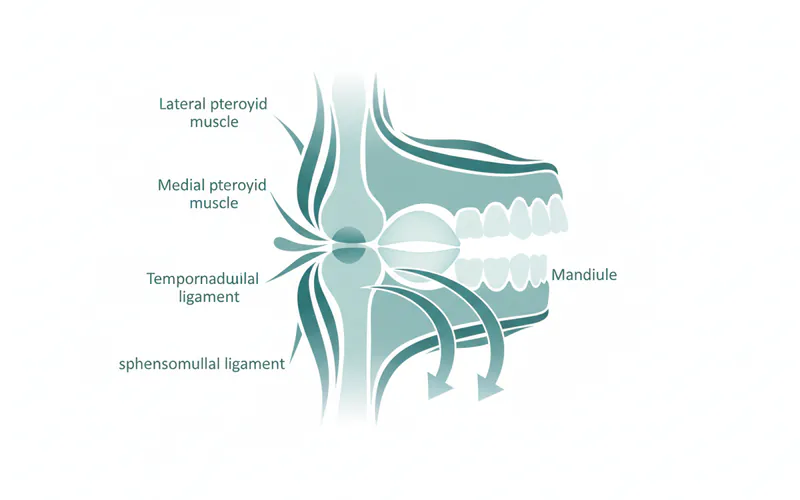
Temporomandibular joint (TMJ) disorders, commonly referred to as TMD, are a group of conditions that affect the jaw joint and the muscles that control jaw movement. The temporomandibular joints are the two joints connecting your lower jaw (mandible) to your skull, located just in front of your ears on both sides of your head. These complex joints, along with the surrounding muscles, ligaments, and discs, enable crucial functions like chewing, speaking, yawning, and facial expressions.
When one or both of these joints or their surrounding structures become inflamed, injured, or dysfunctional, it can lead to TMD. This can manifest as pain, tenderness, clicking sounds, limited jaw movement, and a host of other symptoms. The term "TMJ" is often colloquially used to refer to the disorder itself, but technically, TMJ is the joint, and TMD is the disorder affecting it. According to the National Institute of Dental and Craniofacial Research (NIDCR), TMD is not a single disease but rather a collection of conditions with overlapping symptoms.
The temporomandibular joint is unique in its structure. It's a sliding hinge joint, meaning it allows both hinge-like motions (opening and closing your mouth) and gliding motions (moving your jaw forward, backward, and side-to-side). Between the bones of the joint (the condyle of the mandible and the temporal bone of the skull) lies a small, oval-shaped articular disc, which acts as a shock absorber and allows for smooth, painless movement. When this disc is displaced, or the joint's cartilage or surrounding muscles are affected, tmd treatment becomes necessary.
Types / Variations of TMD
TMD is a broad term encompassing various conditions. Dentists and oral health specialists often categorize them into three main types based on the primary source of the problem:
Myofascial Pain
This is the most common form of TMD. Myofascial pain refers to discomfort or pain in the muscles that control jaw function—the masticatory muscles, located in the face, head, and neck. This type of pain often results from muscle overuse, tension, or fatigue, frequently associated with habits like teeth grinding (bruxism) or clenching, stress, or even prolonged jaw activity. The pain can feel like a dull ache or spasm and may radiate to other areas of the head and neck.
Internal Derangement of the Joint
This category involves a structural problem within the temporomandibular joint itself. It typically refers to a displaced or dislocated articular disc (the soft cushion between the ball and socket of the joint).
- Disc Displacement with Reduction: The disc moves out of its normal position when the jaw is at rest but snaps back into place when the mouth opens wide or closes. This often causes a clicking, popping, or clunking sound.
- Disc Displacement Without Reduction: The disc remains displaced even when the mouth opens, often blocking the movement of the condyle. This can result in limited jaw opening (often described as a "locked jaw"), pain, and difficulty chewing.
- Dislocation: In severe cases, the condyle (the ball of the joint) can completely dislocate from its socket.
Degenerative or Inflammatory Joint Disease
This category includes various inflammatory and degenerative conditions that can affect the TMJ, similar to how they might affect other joints in the body.
- Osteoarthritis: Degeneration of the cartilage and bone within the joint, often leading to pain, stiffness, and crepitus (a grating sound or sensation). This is more common in older adults.
- Rheumatoid Arthritis: An autoimmune disease that can affect multiple joints, including the TMJ, causing inflammation, pain, and potentially joint destruction.
- Ankylosis: A rare condition where the joint becomes stiff due to fusion of the bones, severely limiting jaw movement.
Understanding which type of TMD you have is critical, as it directly influences the most effective tmd treatment approach.
Causes / Why It Happens: Unraveling the Roots of TMD
Identifying the specific tmj causes can be challenging, as TMD often results from a combination of factors rather than a single event. However, common contributors include:
Jaw Injury
Trauma to the jaw, TMJ, or the muscles of the head and neck can lead to TMD. This could be anything from a direct blow to the face, a whiplash injury, or even prolonged wide-mouth opening during dental procedures. Fractures, dislocations, or sprains can disrupt the delicate balance of the joint, leading to chronic pain and dysfunction.
Bruxism (Teeth Grinding and Clenching)
One of the most significant and prevalent tmj causes is bruxism, which involves habitually grinding or clenching teeth, often subconsciously, especially during sleep. This places immense pressure and strain on the temporomandibular joints and the surrounding muscles. Over time, this constant force can lead to muscle fatigue, inflammation, disc displacement, and even wear and tear on the joint cartilage. A night guard for TMJ is often prescribed to mitigate the effects of bruxism.
Stress and Psychological Factors
Emotional stress, anxiety, and tension are well-known to contribute to bruxism and muscle tension in the jaw. Many individuals hold their stress in their jaw muscles, leading to clenching, tightening, and eventual pain. Chronic stress can also heighten pain perception, making existing TMD symptoms feel worse. Psychological distress is increasingly recognized as a significant exacerbating factor for TMD.
Malocclusion (Bad Bite)
While historically considered a primary cause, the role of an "improper bite" (malocclusion) as a direct cause of TMD is now debated. However, a significant discrepancy in how the upper and lower teeth meet, or missing teeth, can sometimes contribute to an uneven distribution of force on the TMJ, potentially leading to muscle fatigue and joint strain in susceptible individuals. Orthodontic treatment may sometimes be part of a comprehensive tmd treatment plan.
Arthritis
Degenerative diseases like osteoarthritis can affect the TMJ just like any other joint in the body. The breakdown of cartilage within the joint can lead to bone-on-bone friction, pain, inflammation, and limited movement. Inflammatory arthritis, such as rheumatoid arthritis, psoriatic arthritis, or gout, can also cause inflammation and damage to the TMJ.
Other Contributing Factors:
- Connective Tissue Diseases: Conditions like Ehlers-Danlos syndrome can lead to hypermobility of joints, including the TMJ, making them more prone to displacement.
- Poor Posture: Forward head posture can put strain on the neck and jaw muscles, contributing to TMD symptoms.
- Diet: A diet heavy in hard, chewy foods can exacerbate symptoms in individuals with pre-existing TMD.
- Genetics: Some research suggests a genetic predisposition to developing chronic pain conditions, including TMD.
- Hormonal Factors: The higher prevalence of TMD in women, particularly those of childbearing age, suggests a potential hormonal link, though more research is needed.
Signs and Symptoms: What to Look For
TMD symptoms can vary widely in severity and presentation, often mimicking other conditions. Recognizing these signs early is crucial for effective tmd treatment.
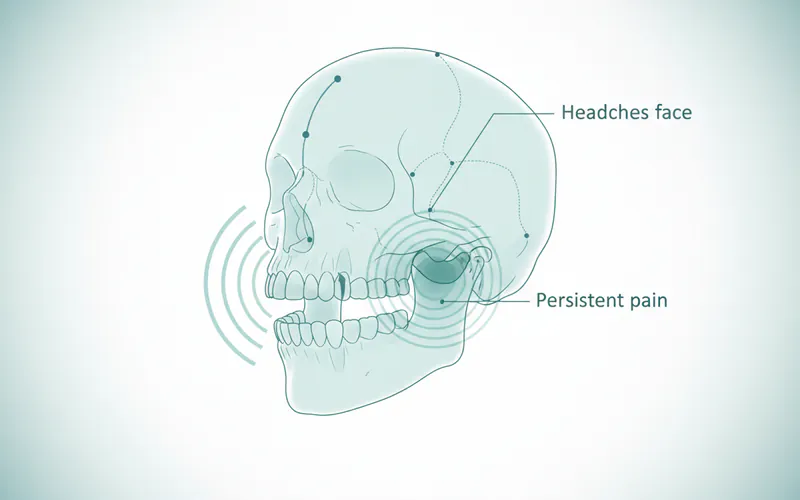
Pain and Tenderness
- Jaw Pain: Aching or tenderness in and around the ear, jaw, and face. This is often the most common symptom.
- Facial Pain: Pain that spreads to the temples, cheeks, or neck.
- Earaches: A dull, persistent ache in or around the ear, often mistaken for an ear infection.
- Headaches: Frequent headaches, often resembling tension headaches or migraines, can originate from jaw muscle tension.
- Pain while Chewing: Discomfort or sharp pain when biting, chewing, or yawning.
Jaw Sounds and Movement Issues
- Clicking, Popping, or Grating Sounds: Sounds when opening or closing your mouth. While not always indicative of a problem if painless, persistent or painful clicking warrants investigation.
- Limited Jaw Movement: Difficulty opening the mouth wide, or the jaw feeling "stuck" or "locked" in an open or closed position.
- Jaw Stiffness: A feeling of stiffness or tightness in the jaw, especially upon waking.
- Deviation: The jaw moving to one side when opening or closing.
Other Associated Symptoms
- Tooth Sensitivity: Due to excessive grinding or clenching.
- Ringing in the Ears (Tinnitus): Though less common, some TMD patients report tinnitus.
- Dizziness: In rare cases, TMD can be associated with feelings of dizziness or vertigo.
- Neck and Shoulder Pain: Muscle tension can radiate to these areas.
- Changes in Bite: Feeling that your upper and lower teeth don't fit together properly.
- Swelling: Occasionally, swelling on the side of the face.
If you experience any combination of these symptoms, especially if they are persistent or worsen, it's essential to consult a dental professional experienced in TMD.
Tmd Treatment Options: A Comprehensive Approach
Tmd treatment aims to alleviate pain, restore normal jaw function, and prevent recurrence. The approach is typically conservative initially, progressing to more invasive options only if necessary. A multidisciplinary approach involving dentists, oral surgeons, physical therapists, and pain specialists is often most effective.
A. Conservative Treatments (First Line of Defense)
These non-invasive methods are often recommended first, as many patients find significant relief without needing more aggressive interventions.
-
Self-Care and Lifestyle Modifications:
- Soft Food Diet: Avoid hard, chewy, sticky foods that strain the jaw. Opt for softer options like yogurt, mashed potatoes, and soups.
- Ice and Heat Packs: Apply ice to reduce inflammation immediately after a flare-up, then moist heat to relax tense muscles.
- Gentle Jaw Exercises: Your dentist or physical therapist may recommend specific exercises to stretch and strengthen jaw muscles and improve range of motion.
- Stress Management: Techniques like meditation, yoga, deep breathing exercises, and counseling can reduce overall stress and associated jaw clenching.
- Avoid Extreme Jaw Movements: Limit wide yawning, chewing gum, or biting nails.
- Good Posture: Maintain proper head and neck alignment to reduce strain on jaw muscles.
- Pro Tip: For acute pain, try over-the-counter pain relievers like ibuprofen (Advil) or naproxen (Aleve) as directed.
-
Medications:
- Over-the-Counter Pain Relievers: NSAIDs (nonsteroidal anti-inflammatory drugs) like ibuprofen or naproxen can reduce pain and inflammation.
- Muscle Relaxants: Prescription medications like cyclobenzaprine or diazepam can help alleviate muscle spasms and tension, especially for nighttime use.
- Tricyclic Antidepressants: Low doses of medications like amitriptyline, often prescribed for nerve pain and sleep disorders, can also help manage TMD pain and improve sleep quality.
- Anti-anxiety Medications: In cases where anxiety significantly contributes to clenching, short-term use might be considered.
-
Physical Therapy:
- A physical therapist can teach you specific stretches, strengthening exercises, and relaxation techniques for the jaw and neck.
- Modalities like ultrasound, moist heat, ice, and transcutaneous electrical nerve stimulation (TENS) may also be used to relieve pain and improve muscle function.
- Postural training is also a key component.
-
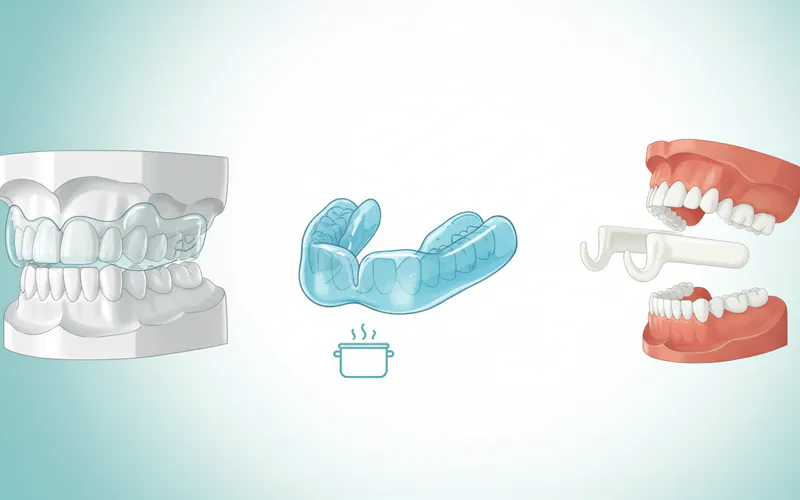
Oral Appliances (Splints or Mouthguards):
- Night Guard for TMJ: A custom-made oral appliance, often called an occlusal splint or stabilization splint, is a very common and effective tmd treatment, particularly for myofascial pain and bruxism. It fits over your upper or lower teeth and is usually worn at night.
- How it works: It creates a barrier between the teeth, preventing direct contact, reducing clenching forces, and protecting teeth from wear. It also helps to reposition the jaw joint into a more relaxed and anatomically correct position, reducing stress on the TMJ and surrounding muscles.
- Types: Soft night guards (less common for TMD, more for tooth protection), hard acrylic night guards (most common and effective for TMD), and anterior repositioning splints (used short-term to move the jaw forward).
- Pros: Non-invasive, reversible, highly effective for many patients, protects teeth.
- Cons: Requires consistent use, can be initially uncomfortable, needs to be professionally fitted and adjusted, can range from $300-$800 (custom-made). Over-the-counter boil-and-bite guards are cheaper but rarely effective for TMD and can even worsen symptoms.
- ADA Guidelines: The American Dental Association (ADA) supports the use of professionally fitted oral appliances as a conservative tmd treatment.
- Night Guard for TMJ: A custom-made oral appliance, often called an occlusal splint or stabilization splint, is a very common and effective tmd treatment, particularly for myofascial pain and bruxism. It fits over your upper or lower teeth and is usually worn at night.
B. Dental Treatments (Addressing Underlying Dental Issues)
-
Bite Adjustments (Occlusal Equilibration):
- Minor reshaping of specific teeth to improve the way the upper and lower teeth fit together. This is controversial as a primary tmd treatment unless there's a clear, identifiable bite discrepancy contributing to TMD. It's often reserved for severe malocclusion.
- Pros: Can improve bite function.
- Cons: Irreversible, may not resolve TMD symptoms if malocclusion isn't the primary cause.
- Cost: $200-$1,500+ depending on complexity.
-
Orthodontics:
- In cases where significant malocclusion is a contributing factor, braces or clear aligners might be considered to realign teeth and improve jaw alignment. This is usually a long-term tmd treatment option.
- Pros: Addresses fundamental bite issues.
- Cons: Long treatment duration (1-3 years), significant cost, not always effective for TMD itself.
- Cost: $3,000-$8,000+.
-
Restorative Dentistry:
- Replacing missing teeth with implants or bridges can help stabilize the bite and prevent undue stress on the TMJ.
- Cost: Highly variable, from $1,500-$5,000+ per tooth for implants.
C. Minimally Invasive Procedures (If Conservative Methods Fail)
-
Botox Injections:
- Botulinum toxin (Botox) can be injected into the jaw muscles (masseter and temporalis) to relax them, reduce muscle spasms, and alleviate pain. This is typically an off-label use for TMD but has shown promise for myofascial pain.
- Pros: Effective for muscle-related pain, relatively quick procedure.
- Cons: Temporary (effects last 3-6 months), requires repeat injections, cost can be significant.
- Cost: $500-$1,500 per session, often not covered by insurance.
-
Corticosteroid Injections:
- Anti-inflammatory steroids can be injected directly into the TMJ to reduce inflammation and pain, particularly for arthritis or capsulitis.
- Pros: Can provide rapid pain relief.
- Cons: Temporary, repeated injections carry risks (joint damage, infection).
- Cost: $100-$300 per injection.
-
Arthrocentesis:
- A procedure where a small needle is inserted into the joint to lavage (wash out) the joint space with sterile fluid. This helps remove inflammatory byproducts and can sometimes free up a stuck disc.
- Pros: Minimally invasive, relatively quick.
- Cons: May require sedation, not effective for all types of TMD.
- Cost: $1,500-$3,000.
D. Surgical Treatments (Last Resort)
Surgery is considered only when conservative and minimally invasive treatments have failed, and there is clear evidence of structural damage within the joint.
-
Arthroscopy:
- A minimally invasive surgical procedure where a tiny incision is made, and a small instrument (arthroscope) with a camera is inserted into the joint. The surgeon can then visualize the joint, remove inflamed tissue, correct disc position, or lavage the joint.
- Pros: Less invasive than open surgery, quicker recovery.
- Cons: Limited visibility, may not be suitable for complex cases.
- Cost: $5,000-$10,000.
-
Open-Joint Surgery (Arthroplasty):
- Performed when there's significant damage, bone abnormalities, or severe disc displacement. The surgeon makes an incision in front of the ear to directly access the joint. Procedures can include disc repair/removal, removal of scar tissue, or reshaping of the jaw bone.
- Pros: Allows for direct repair of complex issues.
- Cons: More invasive, longer recovery, higher risks (nerve damage, infection, scarring).
- Cost: $10,000-$20,000+.
-
Total Joint Replacement:
- In rare, severe cases where the joint is completely damaged (e.g., severe arthritis, trauma), the TMJ may be replaced with an artificial implant.
- Pros: Can restore function and eliminate pain in extreme cases.
- Cons: Major surgery, significant risks, long recovery, potential for revision surgeries.
- Cost: $30,000-$50,000+.
Step-by-Step Process: What to Expect During TMD Treatment
Navigating tmd treatment can feel overwhelming, but understanding the typical process can help ease concerns.
-
Initial Consultation and Diagnosis:
- Detailed History: Your dentist or oral surgeon will ask about your symptoms, medical history, stress levels, and lifestyle habits (e.g., bruxism).
- Physical Examination: This includes palpating your jaw muscles, listening for clicking/popping sounds, checking your jaw's range of motion, and evaluating your bite.
- Imaging: X-rays are standard. More advanced imaging like a CT scan (to view bone structure) or MRI (to visualize the soft tissues, especially the disc) may be ordered to assess the joint's condition.
- Diagnosis: Based on the examination and imaging, a specific diagnosis (e.g., myofascial pain, disc displacement) will be made.
-
Treatment Planning (Conservative Phase First):
- Your dental professional will discuss initial conservative tmd treatment options, emphasizing self-care, physical therapy, and potentially medication.
- If bruxism is suspected, a custom-fitted night guard for TMJ will likely be recommended. Impressions of your teeth will be taken to fabricate the appliance.
-
Implementation of Conservative Treatments:
- You'll begin implementing self-care strategies, medications, and any recommended physical therapy exercises.
- If a night guard is prescribed, you'll receive it and instructions on how to wear and care for it. Several follow-up appointments may be needed for adjustments to ensure proper fit and comfort.
-
Monitoring and Evaluation:
- Regular follow-up visits will be scheduled to assess your progress, manage pain, and adjust treatments as needed.
- The goal is to reduce symptoms significantly within a few weeks to months.
-
Escalation to More Invasive Options (If Necessary):
- If conservative methods don't provide sufficient relief after a reasonable period (e.g., 3-6 months), your doctor may discuss minimally invasive procedures (Botox, injections, arthrocentesis).
- For severe, persistent structural issues, referral to an oral and maxillofacial surgeon for consideration of arthroscopy or open-joint surgery will be made.
-
Recovery and Aftercare:
- Following any procedure, detailed recovery instructions will be provided.
- Long-term management often includes continued self-care, stress reduction, and periodic use of a night guard for TMJ to prevent recurrence.
Cost and Insurance: Understanding the Financial Aspect of TMD Treatment
The cost of tmd treatment in the US can vary dramatically based on the type of intervention, geographic location, and the expertise of the provider.
Average US Cost Ranges:
| Treatment Type | Average Cost Range (USD) | Notes |
|---|---|---|
| Self-Care / OTC Meds | $50 - $200 | Per incident/month for basic pain relievers, heat/ice packs. |
| Prescription Medications | $20 - $200 | Per prescription (muscle relaxants, NSAIDs, antidepressants). |
| Physical Therapy | $50 - $200 per session | Often 6-12 sessions needed. |
| Custom Night Guard for TMJ | $300 - $800 | Custom-fitted by dentist; crucial for bruxism. Over-the-counter $20-50 (not recommended). |
| Bite Adjustment (minor) | $200 - $1,500 | For minor occlusal changes. |
| Botox Injections | $500 - $1,500 per session | Effects last 3-6 months; multiple sessions likely. |
| Corticosteroid Injections (TMJ) | $100 - $300 per injection | Often performed by oral surgeon; temporary relief. |
| Arthrocentesis | $1,500 - $3,000 | Minimally invasive, often outpatient. |
| TMJ Arthroscopy | $5,000 - $10,000 | Outpatient or short hospital stay. |
| Open-Joint Surgery (Arthroplasty) | $10,000 - $20,000+ | Requires hospital stay, significant recovery. |
| Total Joint Replacement (TMJ) | $30,000 - $50,000+ | Rare, complex, extensive recovery. |
| Orthodontics (Braces/Aligners) | $3,000 - $8,000+ | If malocclusion is a significant contributing factor. |
Insurance Coverage Details:
This is one of the most confusing aspects of tmd treatment.
- Dental Insurance: Often covers services performed by a dentist, such as examinations, X-rays, and the fabrication of a night guard for TMJ. However, coverage for "medical" aspects of TMD (like physical therapy or Botox) is typically limited or denied. Some plans may cover a portion of oral appliances.
- Medical Insurance: May cover medical-related aspects, such as physician consultations, prescription medications, diagnostic imaging (CT/MRI), physical therapy, and surgical procedures performed by an oral surgeon or physician. However, many medical insurance plans classify TMD as a "dental" issue and explicitly exclude coverage, or require extensive justification.
- Pre-Authorization: Always contact both your dental and medical insurance providers before starting any significant tmd treatment to understand your benefits, exclusions, deductibles, and co-pays. Many procedures require pre-authorization.
- ADA Guidance: The ADA encourages a collaborative approach between dental and medical professionals for TMD management and advocates for appropriate insurance coverage.
Payment Plans and Financing Options:
- In-Office Payment Plans: Many dental and oral surgery offices offer interest-free payment plans.
- Healthcare Financing: Companies like CareCredit or LendingClub offer specialized healthcare credit cards with deferred interest options.
- Health Savings Accounts (HSAs) / Flexible Spending Accounts (FSAs): These tax-advantaged accounts can be used to pay for qualified medical and dental expenses, including many TMD treatments.
Recovery and Aftercare: Sustaining Your Progress
The recovery period and aftercare instructions vary significantly depending on the tmd treatment received.

For Conservative Treatments (Night Guard, Physical Therapy):
- Consistent Use: If prescribed a night guard for TMJ, wear it consistently as directed. Neglecting it can lead to symptom recurrence.
- Home Exercises: Continue with prescribed jaw exercises to maintain flexibility and strength.
- Stress Management: Integrate stress-reduction techniques into your daily routine. This is crucial for preventing muscle tension and clenching.
- Dietary Awareness: Be mindful of your diet, avoiding excessively chewy or hard foods, especially during flare-ups.
- Regular Dental Check-ups: Continue with your routine dental visits so your dentist can monitor your TMD condition and adjust your appliance if needed.
For Minimally Invasive Procedures (Botox, Arthrocentesis):
- Immediate Post-Procedure: Expect some tenderness, swelling, or bruising at the injection site or around the joint. Ice packs can help.
- Activity Restrictions: Your doctor may advise avoiding strenuous activity or certain foods for a short period.
- Follow-Up: Keep all follow-up appointments to assess the effectiveness of the treatment and address any concerns.
- Maintenance: These procedures often provide temporary relief, so you'll likely need to continue with conservative therapies and potentially repeat injections.
For Surgical Procedures (Arthroscopy, Open-Joint Surgery):
- Pain Management: You'll be prescribed pain medication, and swelling and discomfort are expected.
- Dietary Restrictions: A soft or liquid diet will be necessary for several weeks to months to allow the joint to heal.
- Physical Therapy: Post-operative physical therapy is often critical to regain full jaw movement and prevent stiffness. This can be extensive and prolonged.
- Activity Limitations: Avoid heavy lifting and strenuous activities for a period.
- Long-Term Follow-up: Regular check-ups with your oral surgeon and dentist will be required to monitor healing and function. Complete recovery can take several months.
Pro Tip: Regardless of your specific tmd treatment, patience and adherence to your doctor's instructions are paramount for successful long-term outcomes. Many TMD patients benefit from ongoing vigilance and a proactive approach to managing their jaw health.
Prevention: How to Avoid TMD
While some tmj causes are unavoidable (like injury), many cases of TMD can be prevented or their severity reduced through proactive measures and lifestyle adjustments.
- Manage Stress: Since stress is a major contributor to jaw clenching and grinding, actively manage it through techniques like meditation, yoga, regular exercise, or counseling.
- Avoid Clenching and Grinding: Become aware of daytime clenching. If you catch yourself, gently separate your teeth by placing your tongue between them. If you grind at night, a custom night guard for TMJ is a preventative tool.
- Practice Good Posture: Maintain proper head, neck, and shoulder alignment, especially if you spend long hours at a computer. This reduces strain on the jaw muscles.
- Limit Chewy/Hard Foods: Reduce consumption of gum, chewy candies, nuts, and tough meats, especially if you have a history of jaw pain.
- Avoid Extreme Jaw Movements: Try to avoid wide yawning, singing loudly, or prolonged jaw opening.
- Don't Rest Your Chin on Your Hand: This puts undue pressure on the TMJ.
- Regular Dental Check-ups: Your dentist can spot early signs of wear from bruxism or jaw misalignment before they become chronic TMD.
Risks and Complications: What Can Go Wrong
While tmd treatment is generally safe and effective, like any medical intervention, there are potential risks and complications.
For Untreated TMD:
- Chronic Pain: Persistent, debilitating pain in the jaw, face, head, and neck.
- Permanent Joint Damage: Erosion of cartilage, bone changes, or irreversible disc displacement.
- Difficulty Eating and Speaking: Leading to nutritional deficiencies or social isolation.
- Sleep Disturbances: Pain and discomfort can severely impact sleep quality.
- Psychological Impact: Chronic pain can lead to depression, anxiety, and reduced quality of life.
For Conservative Treatments (e.g., Night Guard for TMJ):
- Initial Discomfort: It may take time to adjust to wearing an oral appliance.
- Changes in Bite (rare): If not properly fitted or adjusted, some appliances could potentially cause slight, temporary changes in bite, though this is rare with professionally made splints.
- No Improvement: The tmd treatment may not be effective for all individuals, requiring escalation.
For Minimally Invasive and Surgical Treatments:
- Infection: Risk at the injection site or within the joint.
- Nerve Damage: Particularly with surgery, there's a risk of damage to facial nerves, leading to numbness or weakness.
- Bleeding: Risk during or after any invasive procedure.
- Anesthesia Risks: Standard risks associated with local or general anesthesia.
- Scarring: Especially with open-joint surgery.
- Limited Efficacy: The treatment may not fully resolve symptoms or may require repeat procedures.
- Joint Stiffness: Post-surgical stiffness can occur, necessitating intensive physical therapy.
- Revision Surgery: In some cases, the initial surgery may not be successful, requiring further intervention.
Comparison Table: Common TMD Treatments
| Treatment Type | Primary Goal | Typical Duration/Frequency | Average Cost Range (USD) | Pros | Cons |
|---|---|---|---|---|---|
| Self-Care/Lifestyle | Pain relief, muscle relaxation | Ongoing | $50 - $200 (monthly) | Non-invasive, empowering, accessible | Requires discipline, may not be sufficient alone |
| Custom Night Guard for TMJ | Reduce clenching/grinding, stabilize joint | Worn nightly (long-term) | $300 - $800 | Non-invasive, protects teeth, effective for bruxism | Requires professional fitting, compliance needed |
| Physical Therapy | Improve jaw function, reduce pain | 6-12 sessions (over weeks/months) | $300 - $2,400 (total) | Non-invasive, teaches self-management | Requires commitment, not always covered by insurance |
| Botox Injections | Reduce muscle spasm/pain | Every 3-6 months | $500 - $1,500 (per session) | Effective for myofascial pain, quick | Temporary, expensive, not always covered, off-label use |
| Arthrocentesis | Wash joint, free disc | Single procedure | $1,500 - $3,000 | Minimally invasive, relatively quick | Requires sedation, may need repetition, not for all TMD |
| TMJ Arthroscopy | Diagnose/repair internal damage | Single procedure | $5,000 - $10,000 | Minimally invasive surgery, direct visualization | Surgical risks, limited for complex issues |
| Open-Joint Surgery | Major joint repair/reconstruction | Single procedure | $10,000 - $20,000+ | Addresses severe structural damage | Highly invasive, significant risks, long recovery |
Children / Pediatric Considerations for TMD
While less common than in adults, children and adolescents can also develop TMD. The symptoms might be slightly different or harder to diagnose in younger patients.
- Common Causes in Children: Trauma (falls, sports injuries), bruxism (often related to stress or airway issues), orthodontic treatment (sometimes a contributing factor if not managed carefully), and inflammatory conditions.
- Symptoms: Children may complain of headaches, earaches, difficulty chewing, clicking or popping in the jaw, or limited mouth opening. Parents might notice their child clenching or grinding teeth.
- Diagnosis: Diagnosis in children requires careful evaluation by a pediatric dentist or oral surgeon, considering their growth and development. Imaging might be used cautiously to minimize radiation exposure.
- Treatment: Tmd treatment for children is almost always conservative initially. This includes stress management, soft food diets, physical therapy, and sometimes a custom night guard for TMJ specifically designed for a growing mouth. Orthodontic intervention might be considered if malocclusion is clearly a significant factor, but typically not as the first line of TMD treatment. Surgical interventions are extremely rare in children and reserved for severe, unresponsive cases.
Pro Tip for Parents: If your child complains of persistent jaw pain, headaches, or you notice unusual jaw sounds or limited movement, consult a pediatric dentist promptly. Early intervention can prevent chronic issues.
Cost Breakdown: A Deeper Dive
Beyond the average ranges, understanding what drives tmd treatment costs can help you budget.
Average US Costs (Low, Mid, High):
- Low-Cost (Self-managed/OTC): $50 - $200 per month (OTC meds, heat/ice, basic jaw exercises).
- Mid-Cost (Conservative Professional Care):
- Night guard for TMJ: $300 - $800 (one-time).
- Physical Therapy: $50 - $200 per session (total $300 - $2,400 for 6-12 sessions).
- Botox (initial course): $500 - $1,500 per session (often 2-3 sessions per year: $1,000 - $4,500 annually).
- High-Cost (Invasive Procedures/Surgery):
- Arthrocentesis: $1,500 - $3,000.
- TMJ Arthroscopy: $5,000 - $10,000.
- Open-Joint Surgery: $10,000 - $20,000+.
- Total Joint Replacement: $30,000 - $50,000+.
- Comprehensive Orthodontics: $3,000 - $8,000+.
With vs. Without Insurance:
- Without Insurance: You will be responsible for 100% of all costs. This makes conservative treatments and payment plans essential. Negotiating cash discounts with providers is sometimes possible.
- With Insurance: Coverage is highly variable.
- Dental Insurance: May cover diagnostic X-rays, exams, and often a portion (e.g., 50-80%) of a custom night guard for TMJ. Check your policy for "oral appliance" or "splint therapy" coverage.
- Medical Insurance: If your TMD is deemed a "medical condition" by your insurer, they might cover doctor visits, physical therapy, diagnostic imaging (MRI/CT), prescription medications, Botox, and surgery. However, exclusions for TMD are common. You'll still be responsible for deductibles, co-pays, and co-insurance.
Cost-Saving Tips:
- Verify Insurance: Always call both your medical and dental insurance companies before treatment to understand what's covered. Get it in writing if possible.
- Seek Referrals: Ask your primary care physician or dentist for referrals to specialists who accept your insurance.
- Generic Medications: Opt for generic versions of prescription medications when available.
- Preventative Care: Investing in early diagnosis and conservative tmd treatment (like a night guard) can prevent more expensive, invasive procedures later.
- Payment Plans: Inquire about interest-free payment plans offered by dental offices or specialized healthcare financing options.
Frequently Asked Questions
1. What is the difference between TMJ and TMD?
TMJ refers to the temporomandibular joint itself – the hinge connecting your jaw to your skull. TMD (Temporomandibular Disorder) is the term for a group of conditions that cause pain and dysfunction in the TMJ and the muscles controlling jaw movement. So, you have two TMJs, but you suffer from TMD.
2. Can TMD be cured completely?
For many people, TMD symptoms can be effectively managed and significantly reduced, leading to a high quality of life. For some, especially those with myofascial pain or stress-related bruxism, a "cure" may involve long-term self-management and consistent use of a night guard for TMJ. For those with severe structural damage, surgery can resolve the immediate issue but may require ongoing care.
3. How long does TMD treatment typically take to show results?
Conservative tmd treatment often starts showing results within a few weeks to a couple of months. For instance, a custom night guard for TMJ can reduce clenching symptoms relatively quickly. More complex cases or surgical recoveries can take several months to a year or more for full healing and functional improvement.
4. Is a night guard for TMJ the same as a sports mouthguard?
No, they are different. A sports mouthguard protects teeth from impact during physical activity. A night guard for TMJ (also called an occlusal splint) is designed to reposition the jaw, reduce muscle strain, and prevent teeth grinding, which are common tmj causes. Night guards are custom-fitted and made to be worn for extended periods, usually overnight.
5. Does insurance cover TMD treatment?
Insurance coverage for tmd treatment is highly variable and often complex. Dental insurance may cover basic exams, X-rays, and parts of oral appliances. Medical insurance might cover diagnostic imaging, physical therapy, and surgery if the condition is classified as medical, but many policies have specific exclusions for TMD. Always verify with both your dental and medical insurance providers.
6. What if conservative treatments don't work?
If conservative treatments like self-care, physical therapy, and a night guard for TMJ don't provide sufficient relief after several months, your dental professional may recommend exploring minimally invasive options such as Botox injections, corticosteroid injections, or arthrocentesis. Surgery is typically considered a last resort for severe, unresponsive cases with clear structural damage.
7. Can stress really cause TMJ problems?
Yes, stress is a significant contributing factor to tmj causes. Many people subconsciously clench or grind their teeth (bruxism) when under stress, leading to excessive strain on the jaw muscles and joints, ultimately contributing to or exacerbating TMD symptoms like pain, headaches, and muscle fatigue.
8. Are there any home remedies for TMD pain relief?
Yes, several home remedies can offer temporary relief. These include applying moist heat or ice packs to the jaw, eating a soft food diet, avoiding excessive jaw movements, practicing gentle jaw stretches, and using over-the-counter pain relievers like ibuprofen. Stress reduction techniques are also crucial.
9. What specialists treat TMD?
A range of specialists may be involved in tmd treatment. These include general dentists (often the first point of contact), oral and maxillofacial surgeons, prosthodontists (specializing in bite and artificial teeth), orthodontists, physical therapists, neurologists, and pain management specialists.
10. Can TMD go away on its own?
Mild cases of TMD, particularly those related to temporary stress or minor muscle strain, may resolve on their own with self-care measures. However, persistent or worsening symptoms, especially involving pain, locking, or significant functional impairment, warrant professional evaluation as they are unlikely to disappear without intervention and could potentially worsen.
When to See a Dentist
It's important to know when your jaw pain warrants a professional consultation.
Schedule an appointment if you experience:
- Persistent Jaw Pain: Any pain or tenderness in your jaw, face, or around your ear that doesn't improve with basic self-care after a few days.
- Clicking or Popping with Pain: Jaw sounds that are consistently accompanied by pain or discomfort when opening or closing your mouth.
- Limited Jaw Movement: Difficulty opening your mouth wide, or if your jaw gets "stuck" or "locked."
- Changes in Bite: A sudden feeling that your upper and lower teeth don't fit together properly.
- Frequent Headaches or Earaches: Especially if they seem to be originating from or related to your jaw.
- Signs of Bruxism: If you or your partner notice you grinding or clenching your teeth, or if your teeth appear worn down.
Seek immediate attention (emergency or urgent care) if you experience:
- Acute Jaw Lock: Your jaw becomes completely locked open or closed and you cannot manipulate it back into place.
- Severe, Sudden Pain: Excruciating pain in your jaw or face that is debilitating.
- Trauma to the Jaw: Following an accident or injury where you suspect a fracture or dislocation.
Early diagnosis and intervention are key to effective tmd treatment and preventing the condition from becoming chronic or requiring more invasive procedures. Don't let jaw pain become a permanent part of your life – consult a dental professional to explore your options.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Tmj Massage Near Me: Complete Guide
Temporomandibular joint disorder, commonly known as TMJD, affects millions of Americans, causing debilitating pain, discomfort, and significantly impacting quality of life. If you're experiencing jaw pain, clicking, or difficulty chewing, you're not alone. Up to 15% of American adults experience
February 23, 2026
Tmj Nerve Damage Symptoms: Complete Guide
Experiencing persistent facial pain, numbness, or tingling can be distressing, especially when the source is unclear. While many people are familiar with general jaw pain associated with temporomandibular joint (TMJ) disorders, the less commonly understood aspect of tmj nerve damage symptoms can
February 23, 2026
Remi Night Guard: Complete Guide
Remi Night Guard: Complete Guide
February 23, 2026
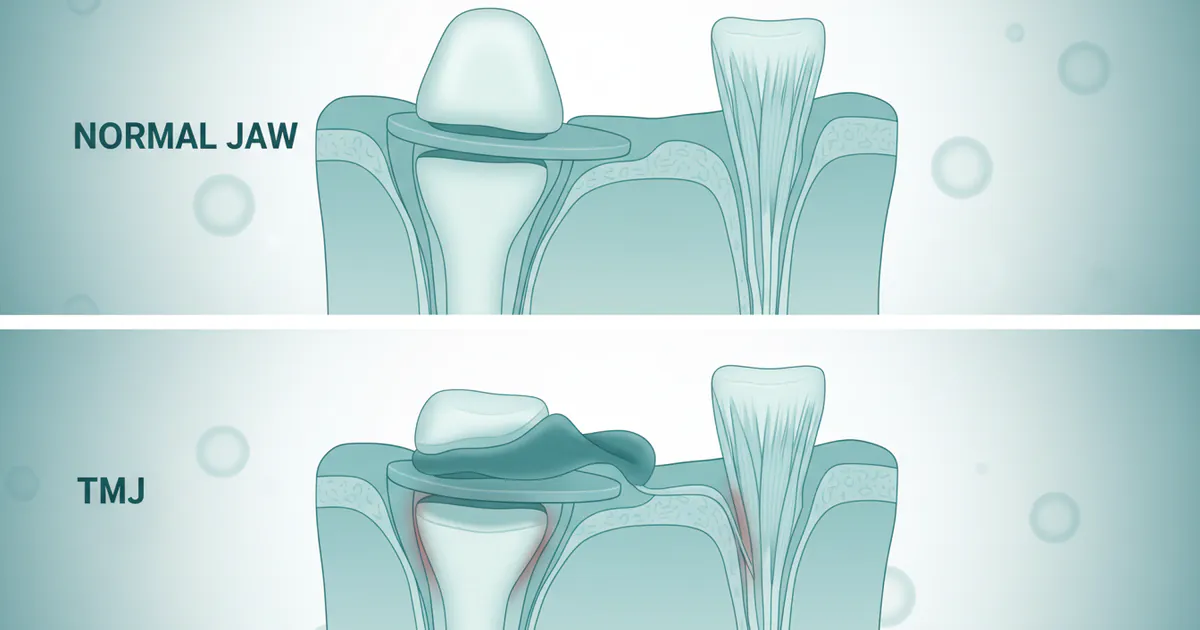
Tmj vs Normal Jaw: Complete Comparison Guide
Experiencing persistent jaw pain, clicking sounds, or difficulty chewing can be frustrating and disruptive to daily life. While many people occasionally feel a stiff jaw, when these symptoms become chronic, they often signal an underlying issue with the temporomandibular joint (TMJ). Understanding t
February 23, 2026