Tmd Symptoms: Complete Guide
Key Takeaways
- Temporomandibular Disorders (TMD) affect millions of Americans, causing persistent pain and significantly impacting daily life. If you've ever experienced persistent jaw pain, clicking sounds when you open your mouth, or chronic headaches, you might be familiar with some common tmd symptoms. The
Temporomandibular Disorders (TMD) affect millions of Americans, causing persistent pain and significantly impacting daily life. If you've ever experienced persistent jaw pain, clicking sounds when you open your mouth, or chronic headaches, you might be familiar with some common tmd symptoms. These uncomfortable and often debilitating issues stem from problems with your temporomandibular joint, commonly known as the tmj joint, and the surrounding muscles and ligaments. Understanding whats tmj truly means for your health, beyond just a simple joint, is crucial for effective management. This comprehensive guide from SmilePedia.net aims to provide you with all the information you need to recognize the signs, understand the causes, explore treatment options, and ultimately regain control over your oral health and quality of life. We'll delve into everything from the subtle indicators to the most severe manifestations, offering insights into diagnosis, cost, and long-term care.
Key Takeaways:
- Prevalence: TMD affects an estimated 10-15% of the adult US population, with women being more commonly diagnosed than men.
- Common Symptoms: Jaw pain, clicking/popping sounds, limited jaw movement, headaches, and ear pain are among the most frequently reported tmd symptoms.
- Diagnosis: A definitive diagnosis often involves a physical exam, patient history, and sometimes imaging like X-rays or MRI, costing between $150 and $800 for initial consultation and basic imaging.
- Treatment Approaches: Most cases respond well to conservative treatments such as physical therapy, oral splints (mouthguards), and medication. These can range from $300 (medication) to $1,500 (splint).
- Surgical Intervention: Surgery is typically a last resort for severe cases, with costs ranging from $5,000 to $50,000+ depending on the procedure.
- Recovery Timeline: Conservative treatments may show improvement within weeks to a few months, while surgical recovery can take several months to over a year.
- Prevention: Stress management, avoiding excessive gum chewing, and maintaining good posture can help prevent or alleviate tmd symptoms.

What It Is / Overview
Temporomandibular Disorders (TMD) refer to a group of conditions that affect the temporomandibular joint (TMJ), the jaw muscles, and the nerves in the face. This complex system allows you to chew, speak, and make facial expressions. To understand tmd symptoms, it's essential to first grasp whats TMJ – it's not the disorder itself, but rather the hinge that connects your jaw to the temporal bones of your skull, located just in front of your ears. You have two TMJs, one on each side of your head.
Each tmj joint is a marvel of biomechanical engineering, comprising several key components:
- Condyle: The rounded end of the lower jawbone (mandible).
- Temporal Bone: The part of the skull it articulates with.
- Articular Disc: A small, oval-shaped piece of cartilage (meniscus) located between the condyle and the temporal bone, acting as a shock absorber and allowing for smooth jaw movement.
- Muscles: A network of muscles (masseter, temporalis, pterygoids) that control jaw movement.
- Ligaments: Connective tissues that stabilize the joint.
When any of these components become dysfunctional, irritated, or inflamed, it can lead to TMD. The problems can arise from a misalignment of the disc, inflammation of the joint capsule, muscle spasm, or damage to the cartilage. While often referred to colloquially as "TMJ," it's more accurate to use TMD to describe the collection of disorders, reserving TMJ for the joint itself.
Types / Variations
TMD is not a single condition but rather a broad category encompassing several distinct problems. The American Academy of Orofacial Pain (AAOP) generally classifies TMD into three main categories, though overlap is common:
1. Myofascial Pain
This is the most common type of TMD and involves discomfort or pain in the muscles that control jaw function, as well as the muscles of the neck and shoulders. Myofascial pain is often characterized by tenderness, aching, and stiffness. It can be caused by muscle overuse, clenching (bruxism), grinding, or sustained stress. The pain may spread from the jaw to other areas of the head and neck.
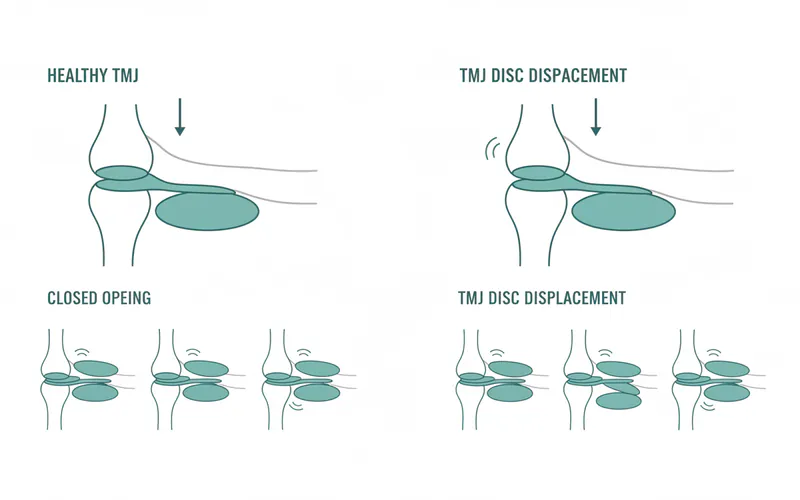
2. Internal Derangement of the TMJ
This category refers to structural problems within the tmj joint itself. These issues often involve the articular disc, which can be displaced, dislocated, or damaged.
- Disc Displacement with Reduction: The disc moves out of its normal position when the jaw is at rest but returns to its correct position when the mouth opens (often accompanied by a click or pop).
- Disc Displacement without Reduction: The disc is permanently displaced and does not return to its normal position, even when the mouth opens fully. This can lead to limited jaw opening and a "locked" jaw sensation.
- Perforation of the Disc: The disc is torn or damaged, reducing its shock-absorbing capacity.
3. Degenerative Joint Disease (Arthritis)
Similar to arthritis in other joints, the cartilage of the tmj joint can break down due to wear and tear, injury, or inflammatory conditions like osteoarthritis or rheumatoid arthritis. This can lead to pain, stiffness, grinding sensations (crepitus), and progressive damage to the joint structures.
Other less common types of TMD can include:
- Traumatic TMD: Resulting from direct injury to the jaw, such as a blow to the face or whiplash.
- Infectious Arthritis: Infection within the joint.
- Neoplastic Conditions: Tumors, though rare, can affect the TMJ.
Causes / Why It Happens
The exact causes of TMD are often multifactorial and can vary significantly from person to person. It's rarely a single identifiable event but rather a combination of physical, physiological, and psychological factors. Understanding these root causes is crucial for effective treatment and prevention of tmd symptoms.
1. Jaw Trauma or Injury
A direct blow to the jaw, head, or neck (e.g., from an accident, sports injury, or whiplash) can damage the tmj joint or surrounding muscles. Even micro-traumas from repetitive strain can contribute over time.
2. Chronic Clenching and Grinding (Bruxism)
Many people unconsciously clench their jaw or grind their teeth, especially during sleep or times of stress. This habit, known as bruxism, puts excessive force on the tmj joint and jaw muscles, leading to fatigue, inflammation, and pain. It's a major contributor to myofascial pain type TMD.
3. Stress and Anxiety
Emotional stress and anxiety are significant exacerbating factors for TMD. Stress often leads to muscle tension throughout the body, including the jaw, and can trigger or worsen clenching and grinding habits. The body's "fight or flight" response can keep jaw muscles perpetually taut.
4. Arthritis
Various forms of arthritis can affect the tmj joint:
- Osteoarthritis: The most common form, resulting from wear and tear on the joint's cartilage.
- Rheumatoid Arthritis: An autoimmune disease that can attack the joint lining, causing inflammation and damage.
- Psoriatic Arthritis: Another inflammatory type that can affect the TMJ.
5. Malocclusion (Bad Bite)
While once considered a primary cause, severe malocclusion (misalignment of the upper and lower teeth) is now generally thought to be a contributing factor in only a minority of TMD cases. However, certain bite problems, especially those causing chronic strain or uneven force distribution on the tmj joint, can play a role in developing tmd symptoms.
6. Connective Tissue Diseases
Conditions like Ehlers-Danlos syndrome or lupus can affect the integrity of connective tissues, including those supporting the tmj joint, making it more susceptible to dysfunction.
7. Genetics
Some research suggests a genetic predisposition to chronic pain conditions, including TMD. Certain individuals may be genetically more vulnerable to developing these disorders.
8. Hormonal Factors
Women are more prone to TMD than men, especially during reproductive years. Hormonal fluctuations, particularly estrogen, are thought to play a role in pain perception and joint tissue integrity, though research is ongoing.
9. Poor Posture
Chronic poor posture, particularly a forward head posture, can place strain on the neck and jaw muscles, contributing to imbalances that affect the tmj joint.
Signs and Symptoms: What to Look For
Recognizing tmd symptoms is the first step toward seeking appropriate care. These symptoms can be diverse, ranging from mild discomfort to severe, debilitating pain, and can affect various parts of the head and neck, not just the jaw. It's important to note that you don't need to experience all of these to have TMD.
1. Pain and Tenderness
- Jaw Pain: Aching, throbbing, or sharp pain in the jaw muscles, especially when chewing, talking, or yawning. Pain can be localized to one side or spread across the entire jaw.
- Facial Pain: Dull, aching pain in the face, often around the cheeks, temples, or forehead. This can sometimes be mistaken for sinusitis.
- Ear Pain: A common symptom, often mistaken for an ear infection. The pain can be deep inside the ear or around its opening. It may or may not be accompanied by actual ear problems.
- Headaches: Frequent tension-type headaches or migraines, often originating from the temples or radiating across the forehead.
- Neck and Shoulder Pain: Pain and stiffness that can extend from the jaw down into the neck and shoulders, reflecting referred pain or muscle tension.
2. Jaw Sounds and Movement Issues
- Clicking or Popping Sounds: Often heard when opening or closing the mouth, or when chewing. This typically indicates disc displacement with reduction, where the disc briefly slips out and then back into place.
- Grating or Grinding Sounds (Crepitus): A harsher, sand-like sound, usually suggesting degenerative changes or roughness within the joint, often due to cartilage breakdown.
- Limited Jaw Movement: Difficulty opening the mouth wide, making it hard to eat or yawn.
- Locked Jaw: The jaw can get "stuck" in an open or closed position, which can be painful and frightening. This indicates disc displacement without reduction or muscle spasm.
- Jaw Stiffness: A feeling of tightness in the jaw muscles, particularly in the morning or after periods of inactivity.
3. Other Related Symptoms
- Tinnitus: Ringing, buzzing, or hissing sounds in the ears, often fluctuating in intensity. This is thought to be related to the proximity of the TMJ to the ear canal and shared nerve pathways.
- Vertigo or Dizziness: A sensation of spinning or unsteadiness, though less common, can occur in some individuals with TMD.
- Tooth Sensitivity: General tooth sensitivity or pain that isn't explained by dental decay or gum disease. This can be due to excessive clenching and grinding leading to enamel wear or stress fractures.
- Changes in Bite: A feeling that your upper and lower teeth don't fit together properly, or a sudden change in your bite alignment.
- Swelling: Occasional swelling on the side of the face, usually around the tmj joint.
Pro Tip: Keeping a symptom journal can be very helpful for your dentist or doctor. Note down when symptoms occur, what makes them better or worse, and their intensity. This can aid in diagnosis and tracking treatment effectiveness.
Treatment Options
The approach to treating tmd symptoms is typically conservative and multifaceted, focusing on pain relief, restoring normal jaw function, and addressing underlying causes. Surgery is generally considered a last resort.
1. Conservative Treatments (First-Line)
- Self-Care and Lifestyle Modifications:
- Soft Diet: Eating soft foods to reduce strain on the jaw.
- Ice and Heat: Applying ice packs (10-15 minutes) for acute pain and inflammation, or moist heat (20 minutes) for muscle relaxation.
- Gentle Jaw Exercises: Specific stretches and strengthening exercises prescribed by a physical therapist to improve jaw mobility and reduce muscle tension.
- Stress Management: Techniques like meditation, yoga, deep breathing, and counseling can significantly reduce jaw clenching and muscle tension.
- Avoid Habits: Refraining from gum chewing, nail biting, excessive yawning, and supporting the jaw with your hand.
- Good Posture: Maintaining proper head and neck alignment to reduce strain on jaw muscles.
- Medications:
- Over-the-Counter (OTC) Pain Relievers: NSAIDs like ibuprofen or naproxen can reduce pain and inflammation.
- Muscle Relaxants: Prescription medications like cyclobenzaprine can relieve muscle spasms and tension, often taken at bedtime.
- Antidepressants: Low doses of tricyclic antidepressants (e.g., amitriptyline) can help with pain management, especially for chronic pain and sleep disturbances, independent of their antidepressant effects.
- Corticosteroids: Occasionally prescribed for acute inflammation, either orally or via injection into the joint.
- Oral Appliances (Splints/Mouthguards):
- Stabilization Splints (Occlusal Splints): Custom-made acrylic devices that fit over the upper or lower teeth. They are designed to create a more harmonious bite, reduce clenching and grinding, and allow jaw muscles to relax. Worn primarily at night, sometimes during the day.
- Repositioning Splints: Less commonly used, these appliances are designed to temporarily reposition the lower jaw forward to encourage the disc to return to a more stable position. Their long-term effectiveness is debated, and they are usually used for short periods.
- Physical Therapy:
- Manual Therapy: Hands-on techniques to release muscle tension and improve joint mobility.
- Therapeutic Exercises: Specific exercises to strengthen jaw muscles, improve range of motion, and correct posture.
- Modalities: Ultrasound, electrical stimulation (TENS), or laser therapy may be used for pain relief and healing.
- Acupuncture: Some patients find relief from pain and muscle tension through acupuncture, a traditional Chinese medicine technique involving fine needles inserted into specific points.
- Botox Injections: Botulinum toxin (Botox) can be injected into the jaw muscles (e.g., masseter, temporalis) to relax them, reduce clenching, and alleviate pain. Effects typically last 3-6 months.
2. Interventional Treatments (Second-Line, for severe cases)
- Arthrocentesis: A minimally invasive procedure where needles are inserted into the joint to flush out inflammatory byproducts and inject lubricants or corticosteroids. Often done under local anesthesia.
- Injections:
- Corticosteroid Injections: Directly into the joint to reduce severe inflammation.
- Hyaluronic Acid Injections: To improve joint lubrication.
- Prolotherapy/PRP: Injections of irritants or platelet-rich plasma to stimulate tissue repair, though evidence for TMJ is limited.
- Surgery: Reserved for severe cases that haven't responded to conservative treatments, especially when there's significant structural damage or persistent locking.
- Arthroplasty (Open-Joint Surgery): More invasive, involves an incision in front of the ear to directly visualize and repair or replace joint structures (e.g., disc repair, removal of bone spurs, joint replacement). Recovery is longer and more complex.
- Arthroscopy: A minimally invasive surgical procedure where a tiny camera and instruments are inserted through small incisions to diagnose and treat joint issues, such as removing inflamed tissue, flushing the joint, or repositioning the disc.
Step-by-Step Process: What to Expect During Treatment
Navigating the journey from initial tmd symptoms to effective management can seem daunting, but understanding the typical steps involved can empower you.
1. Initial Consultation and Diagnosis (Weeks 1-2)
- Patient History: Your dentist or oral surgeon will ask detailed questions about your symptoms, medical history, lifestyle, and habits (e.g., stress levels, clenching/grinding).
- Physical Examination: This includes palpating your jaw muscles, listening for clicks or pops when you move your jaw, assessing your range of motion, and checking for tenderness in and around the tmj joint. They may also evaluate your bite.
- Imaging (if needed):
- Panoramic X-ray: Provides a broad view of your jaw and teeth.
- CT Scan: Offers detailed bone structure images.
- MRI (Magnetic Resonance Imaging): Best for visualizing the soft tissues, especially the articular disc, and is crucial for diagnosing internal derangements.
- Cone Beam CT (CBCT): A specialized dental CT scan providing 3D images with lower radiation.
- Diagnosis: Based on this information, your provider will diagnose the type and severity of your TMD.
2. Conservative Treatment Initiation (Weeks 2-6)
- Education and Self-Care Plan: You'll receive instructions on dietary modifications, applying heat/cold, gentle exercises, and stress reduction techniques.
- Medication: Prescription for NSAIDs, muscle relaxants, or low-dose antidepressants may be given.
- Oral Appliance (Splint) Fabrication: If an oral splint is recommended, impressions of your teeth will be taken. It usually takes 1-2 weeks for the custom splint to be made.
- Referrals: You might be referred to a physical therapist specializing in craniomandibular disorders, a pain management specialist, or a psychologist for stress management.
3. Monitoring and Adjustment (Months 1-6)
- Follow-up Appointments: Regular visits (e.g., every 2-4 weeks initially) to assess your progress, adjust your splint if necessary, and modify your exercise routine.
- Physical Therapy Sessions: Typically 1-2 sessions per week for several weeks, focusing on manual therapy, exercises, and posture correction.
- Symptom Tracking: Continue your symptom journal to help your provider understand what's working and what's not.
- Gradual Improvement: Many patients experience significant reduction in tmd symptoms within 1-3 months of consistent conservative treatment.
4. Advanced or Interventional Treatment Consideration (After 6+ Months of failed conservative care)
- Re-evaluation: If conservative treatments are not effective after several months, your provider will re-evaluate your condition.
- Injections: If muscle pain persists or the joint is severely inflamed, Botox or corticosteroid injections might be considered. This typically involves a quick in-office procedure.
- Arthrocentesis: A procedure done in a clinic or outpatient surgical center, usually under local anesthesia, taking less than an hour. Recovery is relatively quick, with mild soreness.
- Surgical Consultation: For severe, intractable pain, significant structural damage, or persistent locking, a consultation with an oral and maxillofacial surgeon will be recommended to discuss surgical options.
5. Surgical Procedure and Recovery (Highly Variable)
- Pre-operative: Imaging, lab tests, and medical clearance.
- Procedure: Arthroscopy is an outpatient procedure, while open-joint surgery may require a hospital stay of 1-2 days.
- Post-operative: Pain management, wound care, and restricted diet are typical.
- Rehabilitation: Intensive physical therapy is crucial for regaining jaw function after surgery, often lasting several months to a year. Full recovery can be prolonged.
Pro Tip: Be an active participant in your treatment. Ask questions, report all symptoms honestly, and follow your care plan diligently. Consistency is key to managing TMD.
Cost and Insurance
Understanding the financial aspect of treating tmd symptoms is vital, as costs can vary widely depending on the diagnostic tools, treatment modalities, and your insurance coverage.
Diagnostic Costs:
- Initial Consultation: $150 - $400 (specialist fees may be higher).
- X-rays (Panoramic): $50 - $150.
- CT Scan / CBCT: $300 - $800.
- MRI: $700 - $2,000 (often required for detailed soft tissue assessment of the tmj joint).
Conservative Treatment Costs:
- Medications (monthly):
- NSAIDs: $10 - $30 (OTC).
- Muscle Relaxants/Antidepressants: $20 - $100 (generic vs. brand).
- Oral Appliance (Splint/Mouthguard): $300 - $1,500 (custom-made, depending on complexity and material).
- Physical Therapy: $75 - $200 per session (often 1-2 sessions/week for several weeks/months).
- Botox Injections: $300 - $1,000 per session (typically 2-3 sessions per year for maintenance). This is often considered cosmetic by insurance, though some medical plans might cover it for severe TMJ pain.
- Acupuncture: $50 - $150 per session.
Interventional/Surgical Treatment Costs:
- Arthrocentesis: $1,000 - $3,000 per joint.
- Corticosteroid Injections: $100 - $400 per injection (often covered by medical insurance).
- TMJ Arthroscopy: $5,000 - $15,000 (outpatient facility fees, surgeon fees, anesthesia).
- Open-Joint TMJ Surgery (Arthroplasty): $15,000 - $50,000+ (can be higher for total joint replacement, includes hospital stay, surgeon, and anesthesia).
Insurance Coverage:
The most confusing aspect of TMD treatment is often insurance coverage.
- Medical vs. Dental Insurance: TMD is frequently viewed as a medical condition, not purely dental. Many dental insurance plans offer limited or no coverage for TMD treatments, especially oral appliances. However, some dental plans might cover a portion of diagnostic X-rays or examinations.
- Medical Insurance: Most medical insurance plans (HMO, PPO, EPO) will cover a portion of diagnostic services (consultations, MRI, CT scans) and medical treatments like physical therapy, medication, and surgical procedures if deemed medically necessary. Coverage varies widely based on your specific plan's deductible, co-pays, and out-of-pocket maximums. You will likely need a referral from your primary care physician or a pre-authorization from your insurance company for specialist visits or costly procedures.
- Medicare/Medicaid: Coverage for TMD treatment under Medicare or Medicaid can be complex and depends on the state and specific plan. Generally, medically necessary procedures and consultations are covered, but specific appliances or long-term physical therapy might have limitations.
- "In-Network" vs. "Out-of-Network": Always check if your chosen providers (dentist, oral surgeon, physical therapist) are in-network with your medical insurance to maximize benefits and reduce out-of-pocket costs.
Pro Tip: Before starting any significant treatment, especially for more expensive options like splints or surgery, contact your medical insurance provider directly. Ask about coverage for "Temporomandibular Joint Disorder" (TMD) under specific procedure codes (CPT codes) that your dentist or doctor can provide. Get pre-authorization in writing whenever possible.
Recovery and Aftercare
Recovery from tmd symptoms is a continuous process that involves not just treating the immediate problem but also adopting long-term strategies for comfort and prevention. The duration and intensity of aftercare depend on the treatment received.
After Conservative Treatment (Splints, PT, Medication, Injections):
- Consistent Appliance Wear: If prescribed an oral splint, wear it exactly as directed, typically nightly. Regular cleaning of the splint is crucial to prevent bacterial buildup.
- Adherence to Exercises: Continue with the prescribed jaw exercises and stretches even after pain subsides to maintain flexibility and strength.
- Medication Management: Follow your doctor's instructions for medications. Do not abruptly stop unless advised.
- Dietary Awareness: Continue to favor softer foods during symptom flare-ups. Avoid excessively chewy or hard foods.
- Stress Reduction: Implement ongoing stress management techniques into your daily routine. This is critical for preventing relapse, especially if bruxism is a factor.
- Regular Follow-ups: Maintain periodic check-ups with your dentist or specialist to monitor your condition and adjust your treatment plan as needed. The ADA emphasizes a conservative, reversible approach as the first line of management.
After Surgical Procedures (Arthrocentesis, Arthroscopy, Open-Joint):
- Immediate Post-Op (Days 1-7):
- Pain Management: You'll be prescribed pain medication. Take it as directed.
- Ice Packs: Apply ice to the surgical site to reduce swelling and bruising.
- Soft Diet: Stick to liquids and soft, non-chewy foods to minimize jaw movement.
- Rest: Avoid strenuous activities.
- Oral Hygiene: Gentle brushing and rinsing as advised by your surgeon.
- Intermediate Recovery (Weeks 2-8):
- Physical Therapy: This is paramount. A structured rehabilitation program will begin early to regain jaw mobility and strength. Exercises will gradually increase in intensity.
- Gradual Diet Progression: Slowly reintroduce firmer foods as tolerated, still avoiding anything that requires excessive chewing.
- Follow-up Appointments: Essential for monitoring healing, removing sutures (if any), and adjusting physical therapy.
- Long-Term Aftercare (Months 3+):
- Continued PT/Home Exercises: Many patients need to continue a home exercise program for several months or even a year to optimize results.
- Lifestyle Modifications: Reaffirm good habits like stress management, avoiding clenching, and maintaining good posture.
- Splint Therapy: Some patients may still require an oral splint at night to protect the joint or maintain the surgical outcome.
- Regular Dental Care: Ongoing dental check-ups are important for overall oral health and early detection of any recurrent issues.

Risks and Complications While most TMD treatments are safe and effective, like any medical intervention, there are potential risks and complications:
Risks of Conservative Treatments:
- Medications: Side effects like drowsiness, stomach upset, or allergic reactions. Long-term use of NSAIDs can lead to kidney problems or stomach ulcers.
- Oral Appliances: Initial discomfort, temporary changes in bite (rarely permanent), or allergic reaction to material.
- Physical Therapy: Temporary soreness or increased pain if exercises are too aggressive.
- Botox: Temporary bruising, swelling, or muscle weakness at the injection site. Rarely, temporary asymmetry of the face or difficulty with certain expressions.
Risks of Interventional/Surgical Treatments:
- Infections: Any invasive procedure carries a risk of infection.
- Nerve Damage: Temporary or permanent damage to facial nerves, leading to numbness, weakness, or altered sensation in the face or tongue (especially with open-joint surgery).
- Bleeding: Excessive bleeding during or after the procedure.
- Scarring: Visible scarring, particularly with open-joint surgery.
- Anesthesia Risks: Reactions to anesthesia.
- Limited Jaw Opening: Post-surgical stiffness or fibrosis can sometimes lead to persistent difficulty opening the jaw.
- Failed Outcome: Despite best efforts, some treatments may not fully alleviate tmd symptoms, or the problem may recur.
- TMJ Ankylosis: A rare but serious complication where the joint fuses, resulting in complete inability to open the mouth.
Prevention
While not all cases of TMD can be prevented, especially those due to injury or degenerative conditions, many tmd symptoms can be avoided or minimized by adopting proactive lifestyle habits and being mindful of jaw health.
1. Manage Stress Effectively
- Mindfulness and Relaxation: Practice meditation, deep breathing exercises, or yoga to reduce overall body tension, including in the jaw.
- Regular Exercise: Physical activity is a proven stress reducer.
- Adequate Sleep: Ensure you get 7-9 hours of quality sleep nightly to help your body and muscles recover.
2. Avoid Excessive Jaw Movements and Habits
- Limit Chewing Gum: Frequent and vigorous gum chewing can overuse jaw muscles.
- Avoid Hard, Chewy Foods: Minimize consumption of tough meats, nuts, and crunchy snacks that put strain on the tmj joint.
- Break Oral Habits: Consciously stop nail-biting, pen-chewing, or holding the phone between your ear and shoulder.
- Don't Rest Your Chin on Your Hand: This puts uneven pressure on the jaw.
- Control Yawning: When yawning, try to support your chin with your hand to prevent over-stretching the jaw.
3. Improve Posture
- Maintain Good Ergonomics: Ensure your workstation, computer screen, and chair promote good posture, especially if you sit for long periods. Keep your head aligned over your shoulders, not jutting forward.
- Neck and Shoulder Awareness: Be mindful of tension in your neck and shoulders, as this can transfer to the jaw muscles. Regular stretching can help.
4. Address Teeth Grinding/Clenching (Bruxism)
- Awareness: If you suspect you clench or grind, become aware of it during the day and try to gently relax your jaw.
- Nightguards/Splints: If daytime or nighttime bruxism is an issue, a custom-fitted oral appliance can protect your teeth and jaw joints from excessive force.
5. Regular Dental Check-ups
- Early Detection: Routine visits to your dentist can help identify early signs of bruxism, malocclusion, or jaw joint issues before they escalate into severe tmd symptoms.
- Bite Assessment: Your dentist can monitor your bite and any changes that might contribute to TMD.
Comparison Tables
Table 1: Conservative vs. Surgical TMD Treatments
| Feature | Conservative Treatments (e.g., Splint, PT, Meds) | Surgical Treatments (e.g., Arthroscopy, Arthroplasty) |
|---|---|---|
| Invasiveness | Non-invasive to minimally invasive (injections) | Minimally invasive (arthroscopy) to highly invasive (open-joint) |
| Cost Range | $300 - $3,000+ (depending on duration, services) | $5,000 - $50,000+ (depending on procedure, facility) |
| Recovery | Weeks to a few months for significant relief; ongoing self-care | Weeks to several months for initial healing; 6-12+ months for full recovery and rehab |
| Effectiveness | Highly effective for 80-90% of TMD cases | Reserved for severe, intractable cases; outcomes vary |
| Risks | Minimal; side effects from meds, temporary discomfort | Higher risks: infection, nerve damage, scarring, anesthesia risks |
| Insurance | Often covered by medical insurance (PT, meds), partial for splints | Generally covered by medical insurance (if medically necessary) |
Table 2: Common Oral Appliances for TMD
| Appliance Type | Primary Function | Typical Cost Range (US) | Pros | Cons |
|---|---|---|---|---|
| Stabilization Splint (Nightguard) | Reduces clenching/grinding, protects teeth, repositions jaw slightly for muscle relaxation. | $300 - $800 | Non-invasive, widely effective, protects teeth. | Requires consistent wear, can be lost/broken. |
| Repositioning Splint (Anterior Repositioning Appliance) | Temporarily holds jaw in a forward position to allow disc to "recapture." | $800 - $1,500 | Can provide immediate relief for disc displacement. | May cause bite changes if used long-term, debated long-term effectiveness. |
| Soft/Flexible Splint | Acts as a cushion for teeth, minimal jaw repositioning. | $200 - $500 | More comfortable for some, less bulky. | Less durable, may encourage clenching due to elasticity. |
Children / Pediatric Considerations
TMD is not exclusive to adults; children and adolescents can also experience tmd symptoms, though often less severe and sometimes with different presentations. It's estimated that up to 7% of children and adolescents may report some form of TMD.
Common Factors in Children:
- Bruxism: Nighttime teeth grinding is very common in children and can contribute to jaw pain and muscle fatigue.
- Trauma: Sports injuries, falls, or dental procedures (like prolonged mouth opening during treatment) can directly impact the tmj joint.
- Orthodontic Treatment: While not a direct cause, some argue that certain orthodontic mechanics or prolonged periods of appliance wear might stress the TMJ in susceptible individuals. However, the ADA states there's no evidence that orthodontic treatment causes or cures TMD.
- Stress: Academic pressure, social issues, or family stress can manifest as jaw clenching or muscle tension.
- Hypermobility: Some children have naturally more flexible joints, including the TMJ, which can lead to instability.
Pediatric TMD Symptoms to Look For:
- Facial Pain: Often reported as earache, headache, or pain around the jaw.
- Clicking or Popping: Parents might notice sounds when their child eats or talks.
- Difficulty Chewing: Child might avoid certain foods or complain of pain while eating.
- Limited Mouth Opening: Noticeable restriction in how wide they can open their mouth.
- Changes in Bite: Child might say their "teeth don't fit together."
Diagnosis and Treatment for Children:
- Conservative Approach: Treatment for children is overwhelmingly conservative.
- Parental Guidance: Educating parents on soft food diets, warm compresses, and stress reduction is key.
- Oral Appliances: Custom-made nightguards are common to manage bruxism and protect the joint.
- Physical Therapy: Gentle exercises and stretches, sometimes guided by a pediatric physical therapist.
- Behavioral Therapy: Helping children manage stress or break habits like nail-biting.
- Avoidance of Surgery: Surgical intervention is extremely rare in children, reserved only for the most severe and intractable structural problems that don't respond to any other treatment. The focus is always on promoting natural growth and development.
Cost Breakdown
As discussed, TMD costs are highly variable, but here's a consolidated breakdown of average US costs, with and without insurance, and payment options.
Average US Costs (Without Insurance):
- Low-End Estimate (Self-Care & Basic Meds): $50 - $300 (OTC pain relievers, heat/ice packs, basic exercises).
- Mid-Range Estimate (Diagnosis, Splint, PT, Some Meds): $1,000 - $4,000 (Initial consultation, basic imaging, custom oral splint, a few months of physical therapy, prescription medications).
- High-End Estimate (Advanced Diagnosis, Injections, Surgery): $5,000 - $50,000+ (MRI, Botox or corticosteroid injections, arthrocentesis, or surgical procedures like arthroscopy or open-joint surgery, including recovery and extensive rehabilitation).
With Insurance:
- Dental Insurance: Often provides limited or no coverage for TMD. May cover a small portion of diagnostic X-rays or exams if related to dental structures.
- Medical Insurance (Typical PPO/HMO):
- Deductible: You'll likely pay 100% of costs until your annual deductible is met (e.g., $500 - $5,000).
- Co-insurance: After deductible, you typically pay a percentage (e.g., 10-30%) of the allowed cost, while insurance covers the rest.
- Co-pays: Fixed fees for doctor visits ($20 - $75) or prescriptions ($10 - $60).
- Out-of-Pocket Maximum: A cap on how much you pay in a year, offering protection for very high-cost treatments.
Example Scenario (with medical insurance): Suppose your deductible is $2,000 and co-insurance is 20%.
- Initial diagnosis ($500) + MRI ($1,000) = $1,500. You pay $1,500, still $500 from your deductible.
- Oral splint ($1,000). You pay $500 (remaining deductible) + 20% of $500 ($100) = $600.
- Physical Therapy (10 sessions at $100/session = $1,000). You pay 20% of $1,000 ($200).
- Total out-of-pocket for this mid-range treatment: $1,500 + $600 + $200 = $2,300.
Payment Plans and Financing Options:
- In-Office Payment Plans: Many dental and oral surgery offices offer interest-free payment plans for a portion of the cost.
- Medical Credit Cards: Services like CareCredit offer special financing options, often with deferred interest if paid within a certain period.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have these, they are excellent ways to pay for TMD diagnostic and treatment costs with pre-tax dollars.
- Personal Loans: Banks or credit unions can provide personal loans, though interest rates may be higher.
Cost-Saving Tips:
- Verify Insurance Coverage: Always call your medical insurance provider before treatment to understand your benefits, deductibles, co-pays, and specifically ask about TMD coverage.
- Get Pre-Authorization: For expensive procedures, request pre-authorization from your insurance company to ensure coverage.
- Ask for Itemized Bills: Review all charges and ensure they are accurate and in line with what was quoted.
- Generic Medications: Opt for generic versions of prescription drugs when available.
- Shop Around (for non-urgent care): For things like physical therapy or oral appliances, compare costs and in-network status among different providers.
- Utilize Public Health Services: If you have limited income, some community health centers or dental schools may offer reduced-cost services.
Frequently Asked Questions
What are the earliest tmd symptoms?
The earliest tmd symptoms often include mild jaw pain or tenderness, especially in the morning or after a stressful day, occasional clicking or popping sounds when opening or closing your mouth, and a slight stiffness in the jaw muscles. Some individuals might first notice tension headaches or mild earaches without a clear cause.
Can TMD go away on its own?
Mild cases of TMD, especially those related to temporary stress or muscle overuse, can sometimes resolve on their own with self-care measures like rest, a soft diet, and stress reduction. However, persistent or worsening tmd symptoms typically require professional evaluation and intervention to prevent chronic pain and further joint damage.
Is TMD a serious condition?
While not life-threatening, TMD can be a serious condition due to its chronic nature and significant impact on quality of life. Untreated, it can lead to persistent debilitating pain, limited jaw function affecting eating and speaking, and related issues like chronic headaches, sleep disturbances, and even depression or anxiety. Early diagnosis and treatment are crucial.
What is the best treatment for TMD?
There is no single "best" treatment for TMD, as it depends on the specific cause, type, and severity of your condition. The most effective approach is typically conservative and multidisciplinary, often involving self-care, oral appliances, physical therapy, and medication. Surgery is generally considered a last resort for complex, intractable cases.
Does insurance cover TMD treatment?
Insurance coverage for TMD is often complex. While dental insurance usually has limited coverage, most medical insurance plans will cover medically necessary diagnostic tests (like MRI, CT scans), physical therapy, medications, and surgical procedures. It's crucial to verify your specific plan's benefits with your medical insurance provider, as deductibles, co-pays, and pre-authorization requirements vary.
How long does it take for TMD symptoms to improve?
Improvement from tmd symptoms varies greatly. Many individuals experience significant relief from conservative treatments within a few weeks to three months of consistent adherence to their treatment plan. More severe or chronic cases, especially those requiring surgery, can take several months to over a year for full recovery and rehabilitation.
What foods should I avoid with TMD?
If you have TMD, it's advisable to avoid hard, crunchy, or excessively chewy foods that put strain on your jaw. This includes nuts, hard candies, raw carrots, apples (unless cut into small pieces), chewy meats, and gum. A soft diet consisting of foods like yogurt, mashed potatoes, soups, soft-cooked vegetables, and fish can help reduce jaw stress.
Can stress cause TMD?
Yes, stress is a significant contributing factor to TMD. Emotional stress often leads to increased muscle tension throughout the body, including the jaw, and can trigger or worsen habits like teeth clenching and grinding (bruxism). These actions put excessive force on the tmj joint and surrounding muscles, leading to pain and dysfunction.
Can I treat TMD at home?
For mild tmd symptoms, home remedies can provide relief. These include applying ice or moist heat, eating a soft diet, practicing gentle jaw stretches, avoiding excessive jaw movements, and stress reduction techniques. However, if symptoms persist or worsen, professional evaluation is essential to prevent the condition from becoming chronic.
What happens if TMD is left untreated?
If TMD is left untreated, tmd symptoms can become chronic and progressively worse. This may lead to severe, constant pain in the jaw, face, head, and neck, increased difficulty with chewing and speaking, persistent jaw locking, significant joint damage (e.g., disc degeneration, bone erosion), and a substantial decrease in quality of life due to chronic discomfort and limitations.
When to See a Dentist
Recognizing when your tmd symptoms warrant professional attention is crucial for timely and effective management. While occasional jaw stiffness or mild clicking might not always be a cause for immediate alarm, certain signs indicate it's time to schedule an appointment with your dentist or an oral health specialist.
Schedule a Routine Appointment if You Experience:
- Persistent Jaw Pain: Any jaw pain or tenderness that lasts for more than a few days and doesn't improve with self-care (soft diet, warm compresses).
- Regular Clicking, Popping, or Grating Sounds: If these sounds are consistent and accompanied by discomfort or changes in jaw movement.
- Difficulty Chewing or Yawning: If you notice a limitation in your ability to open your mouth wide or feel discomfort when using your jaw.
- Frequent Headaches or Earaches: Especially if these are not explained by other conditions and seem to be related to jaw movement or tension.
- Noticeable Jaw Stiffness: A consistent feeling of tightness in your jaw, particularly in the morning.
- Changes in Your Bite: If your teeth suddenly feel like they don't fit together properly.
Seek Prompt Attention (within a few days) if You Experience:
- Intense or Worsening Pain: If your jaw or facial pain becomes severe and significantly interferes with eating, speaking, or sleeping.
- Repeated Jaw Locking: If your jaw frequently gets stuck in an open or closed position, making it difficult or impossible to move.
- Sudden Swelling or Redness: Around the tmj joint, which could indicate inflammation or infection.
When to Consider Emergency Care (Rare, but important):
- Completely Locked Jaw: If your jaw is completely locked and you cannot open or close your mouth at all, causing severe distress and inability to eat or speak. This requires immediate professional intervention.
- Suspected Jaw Fracture: Following a traumatic injury, if you experience severe pain, swelling, bruising, and difficulty moving your jaw, seek emergency medical attention.
Remember, early diagnosis and intervention are key to successfully managing TMD and preventing its progression. Don't dismiss your tmd symptoms; consulting a dental professional can provide you with clarity and a path to relief.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Tmj Massage Near Me: Complete Guide
Temporomandibular joint disorder, commonly known as TMJD, affects millions of Americans, causing debilitating pain, discomfort, and significantly impacting quality of life. If you're experiencing jaw pain, clicking, or difficulty chewing, you're not alone. Up to 15% of American adults experience
February 23, 2026
Tmd Treatment: Complete Guide
Experiencing persistent jaw pain, clicking sounds when you chew, or debilitating headaches that seem to originate from your face? You're not alone. Temporomandibular joint (TMJ) disorders, often referred to collectively as TMD, affect an estimated 10 million Americans, with women disproportionat
February 23, 2026
Tmj Nerve Damage Symptoms: Complete Guide
Experiencing persistent facial pain, numbness, or tingling can be distressing, especially when the source is unclear. While many people are familiar with general jaw pain associated with temporomandibular joint (TMJ) disorders, the less commonly understood aspect of tmj nerve damage symptoms can
February 23, 2026
Remi Night Guard: Complete Guide
Remi Night Guard: Complete Guide
February 23, 2026