Complete Guide to TMJ & Jaw Disorders: Everything You Need to Know
Key Takeaways
- Do you frequently experience nagging jaw pain, persistent headaches, or a clicking sound when you open your mouth? You're not alone. Approximately 10 million Americans suffer from some form of temporomandibular joint dysfunction, commonly referred to as TMJ disorder. This complex con
Complete Guide to TMJ & Jaw Disorders: Everything You Need to Know
Do you frequently experience nagging jaw pain, persistent headaches, or a clicking sound when you open your mouth? You're not alone. Approximately 10 million Americans suffer from some form of temporomandibular joint dysfunction, commonly referred to as TMJ disorder. This complex condition affects the joints that connect your jawbone to your skull, impacting your ability to speak, chew, and even express emotions without discomfort. Left unaddressed, TMJ symptoms can significantly diminish your quality of life, leading to chronic pain, sleep disturbances, and a range of secondary health issues.
At SmilePedia.net, we understand the profound impact that jaw disorders can have. That's why we've compiled this comprehensive guide – your definitive resource for understanding everything about TMJ disorders. From deciphering what is TMJ to exploring the full spectrum of TMJ treatment options, this article will empower you with the knowledge needed to recognize the signs, seek appropriate care, and find lasting relief. We'll delve into causes, symptoms, diagnostic methods, various treatment pathways (including the role of a night guard), cost considerations, and essential prevention strategies. Let's unlock the secrets to a healthier, pain-free jaw.
Key Takeaways:
- Prevalence: Over 10 million Americans experience TMJ disorders, making it a common source of chronic facial pain.
- Symptoms: Common signs include jaw pain, clicking/popping sounds, limited jaw movement, headaches, and earaches.
- Diagnosis: A thorough dental examination, often supported by imaging like MRI, is crucial for accurate diagnosis.
- Treatment Diversity: Conservative approaches (e.g., pain relievers, physical therapy, oral splints/night guards) are usually the first line of defense, with surgical options reserved for severe cases.
- Cost Varies Widely: Initial consultations typically range from $50-$300. A custom night guard can cost anywhere from $300-$1,500. Physical therapy sessions are $75-$200 per visit. Surgical interventions can range from $5,000 to over $25,000.
- Insurance: Coverage depends on your specific medical and/or dental plan, often requiring pre-authorization for more complex treatments. Many plans will cover a portion of conservative treatments.
- Actionable Steps: Early intervention is key. If you suspect TMJ, consult a dentist or oral surgeon specializing in these disorders. Lifestyle changes like stress management and avoiding clenching can significantly aid recovery.
What It Is / Overview
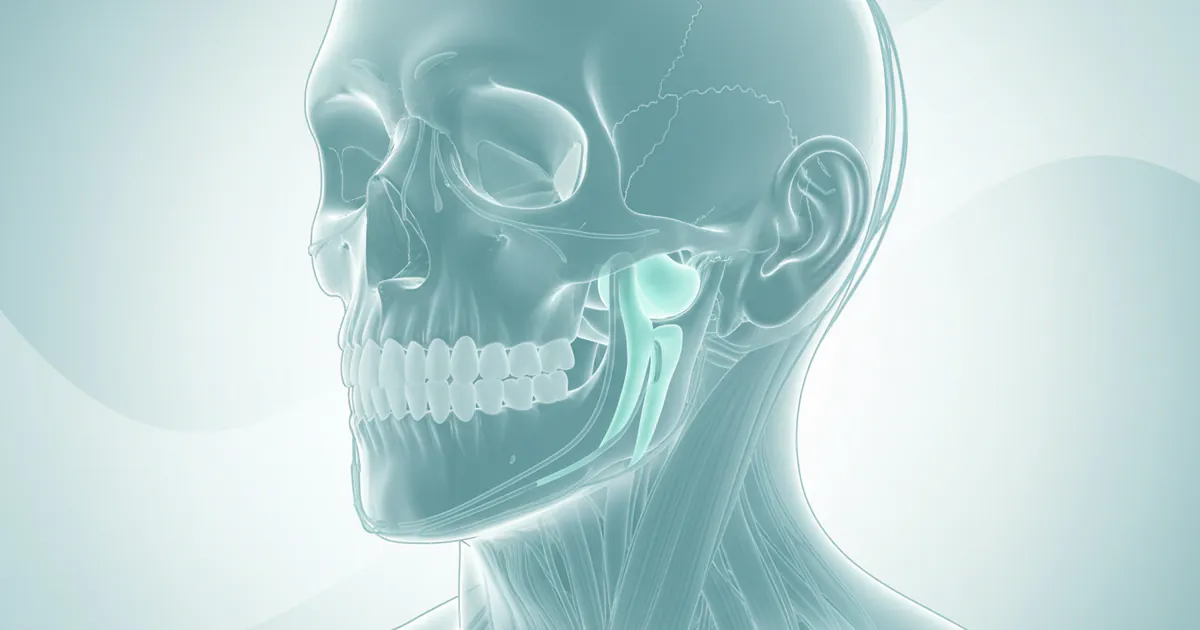
The temporomandibular joints (TMJs) are two of the most complex joints in the human body. Located on each side of your head, just in front of your ears, these joints act like a sliding hinge, connecting your lower jaw (mandible) to the temporal bones of your skull. This intricate anatomical setup allows for a wide range of movements essential for everyday functions such as chewing, speaking, yawning, and swallowing.
Each TMJ consists of several key components:
- Condyle: The rounded end of the lower jawbone.
- Temporal Bone: The part of the skull it articulates with.
- Articular Disc (Meniscus): A small, oval-shaped piece of cartilage positioned between the condyle and the temporal bone. This disc acts as a shock absorber and ensures smooth jaw movement.
- Ligaments and Muscles: A network of ligaments stabilizes the joint, while powerful muscles surrounding the jaw enable its various movements.
When we talk about TMJ disorder (TMD), we are referring to a group of conditions that cause pain and dysfunction in these joints and the surrounding muscles. It's crucial to understand that "TMJ" is the name of the joint itself, while "TMD" or "TMJ disorder" refers to the problem affecting it. The pain and discomfort associated with temporomandibular joint dysfunction can be debilitating, often manifesting as chronic facial pain that can radiate to the ears, neck, and shoulders.
According to the National Institute of Dental and Craniofacial Research (NIDCR), TMDs are a major public health problem, affecting an estimated 10 to 15 percent of the adult population in the United States. While they can affect anyone, TMDs are more common in women, particularly those between the ages of 20 and 40. Understanding the fundamental anatomy and function of your jaw joint is the first step toward recognizing and effectively addressing any issues that may arise.
!Detailed anatomical illustration of the temporomandibular joint, showing the mandible, temporal bone, articular disc, and surrounding ligaments and muscles.
Types / Variations of TMJ Disorders
TMJ disorders are not a single entity but rather a collection of conditions affecting the jaw joint and its associated structures. They are generally categorized into three main types, though some individuals may experience a combination of these:
Myofascial Pain
This is the most common type of TMD, characterized by pain in the muscles that control jaw function (masticatory muscles) and the muscles of the neck and shoulders. The pain is often described as a dull, aching sensation, sometimes accompanied by tenderness, stiffness, or the presence of "trigger points" in the affected muscles. Myofascial pain is frequently linked to habits like teeth clenching (bruxism), grinding, or excessive stress.
Internal Derangement of the Joint
This category involves structural problems within the TMJ itself, particularly issues with the articular disc.
- Disc Displacement with Reduction: The disc slips out of its normal position when the mouth is closed but returns to its correct position when the mouth opens. This often causes a clicking or popping sound when the jaw moves.
- Disc Displacement Without Reduction: The disc remains displaced even when the mouth is open, leading to limited jaw movement, stiffness, and sometimes a "locked jaw" sensation where the mouth cannot open fully. This type is generally more severe and can be quite painful.
- Luxation: This refers to the dislocation of the jaw joint, where the condyle moves too far forward and gets stuck in front of the articular eminence.
Degenerative or Inflammatory Joint Disease
This category includes conditions that affect the bony parts of the joint or cause inflammation.
- Osteoarthritis: A degenerative joint disease that causes breakdown of the cartilage and bone within the TMJ, leading to pain, stiffness, and a grating sensation (crepitus) during jaw movement. It's often related to aging or overuse.
- Rheumatoid Arthritis: An autoimmune disease that can affect multiple joints throughout the body, including the TMJ. It causes inflammation, pain, swelling, and can lead to significant joint destruction.
- Trauma-Induced Arthritis: Direct injury to the jaw can lead to inflammation and damage within the joint, resulting in pain and dysfunction.
Understanding the specific type of TMJ disorder is crucial for effective diagnosis and tailored TMJ treatment planning.
Causes / Why It Happens
The exact cause of TMJ disorder is often complex and multifactorial, meaning several factors can contribute to its development. In many cases, it's not a single event but a combination of influences that lead to the onset of TMJ symptoms.
Here are the primary causes and contributing factors:
- Bruxism (Teeth Grinding and Clenching): This is one of the most common and significant contributors. Chronic clenching or grinding of teeth, especially during sleep (sleep bruxism), puts immense pressure on the TMJs and surrounding muscles. This repetitive stress can lead to muscle fatigue, inflammation, and disc displacement.
- Trauma to the Jaw, Head, or Neck: A direct blow to the jaw, a whiplash injury, or other impact can damage the TMJ, surrounding tissues, or jaw muscles. Even micro-traumas from poor posture can contribute over time.
- Stress and Anxiety: Psychological stress is a powerful exacerbating factor. When stressed, many people unconsciously clench their jaw or tense their facial muscles, leading to increased pressure on the TMJs and muscle fatigue. Stress can also heighten pain perception.
- Arthritis:
- Osteoarthritis: The "wear and tear" arthritis, it can affect the TMJ just like other joints in the body. Breakdown of the cartilage leads to friction, pain, and impaired movement.
- Rheumatoid Arthritis: An inflammatory autoimmune disease that can affect the TMJs, causing inflammation, swelling, and potential joint destruction.
- Disc Displacement: The soft disc that cushions the TMJ can erode or move out of its proper alignment. If the disc slips forward or backward, it can interfere with normal jaw movement, leading to clicking, locking, or pain.
- Dental Malocclusion (Bad Bite): While historically thought to be a primary cause, the role of malocclusion in TMJ disorders is still debated among dental professionals. Some research suggests that significant bite discrepancies might contribute to TMJ dysfunction by altering jaw mechanics, while others argue its impact is minimal compared to other factors. However, an unbalanced bite can contribute to muscle strain.
- Connective Tissue Diseases: Conditions like Ehlers-Danlos syndrome, which affect connective tissues throughout the body, can also impact the TMJs, leading to hypermobility or instability.
- Poor Posture: Sustained poor posture, especially forward head posture (often seen with prolonged computer use), can strain the neck and shoulder muscles, which in turn can affect the jaw muscles and alignment.
- Genetic Predisposition: Some individuals may have a genetic susceptibility to developing chronic pain conditions, including TMDs.
It's important to remember that TMJ disorders are often multifactorial. Your dentist or TMJ specialist will conduct a thorough examination to identify the specific contributing factors in your case to tailor the most effective TMJ treatment.
Signs and Symptoms
Recognizing the TMJ symptoms is the first step toward seeking appropriate care. The symptoms can vary widely in intensity and presentation, often mimicking other conditions, which can make diagnosis challenging. If you experience any of these persistently, it's time to consult a dental professional.
Common TMJ symptoms include:
- Pain or Tenderness in the Jaw: This is the hallmark symptom, often described as a dull ache in the jaw joint area, around the ear, or radiating throughout the face. The pain may worsen with jaw movement.
- Pain in or Around the Ear: Many people confuse TMJ pain with an ear infection because the joint is so close to the ear canal. The pain might be deep inside the ear or just in front of it.
- Facial Pain: Chronic, aching pain that can affect the temples, cheeks, or around the eyes.
- Clicking, Popping, or Grating Sounds (Crepitus): These sounds occur when opening or closing the mouth. While occasional clicks without pain might be benign, persistent, painful, or loud sounds usually indicate disc displacement or joint degeneration.
- Limited Jaw Movement: Difficulty opening the mouth wide, or a feeling of stiffness in the jaw.
- "Locked Jaw": A sensation where the jaw gets stuck in an open or closed position, making it impossible to move until it "unlocks." This can be a very distressing symptom.
- Headaches: Frequent tension headaches or even migraines, often originating in the temples or forehead, can be closely linked to TMJ disorders.
- Neck and Shoulder Pain: The muscles connecting the jaw to the head, neck, and shoulders are intertwined. Tension in one area can easily spread to others.
- Difficulty or Discomfort While Chewing: Pain when biting, chewing, or even swallowing, particularly with hard or chewy foods. Your bite might also feel "off."
- Swelling on One Side of the Face: Inflammation in the joint or surrounding muscles can sometimes lead to visible swelling.
- Tinnitus (Ringing in the Ears): Though less common, TMJ disorders can sometimes affect the auditory system due to the close proximity of the jaw joint to the inner ear structures.
- Dizziness or Vertigo: Rarely, severe TMJ dysfunction can be associated with balance issues.
- Tooth Sensitivity or Pain: Due to excessive clenching and grinding, teeth can become sensitive, cracked, or loose.
It's important to note that experiencing a clicking jaw does not automatically mean you have a TMJ disorder, especially if there's no pain or restricted movement. However, if any of these symptoms are persistent, worsening, or significantly impacting your daily life, it is crucial to seek professional evaluation.
Diagnosis of TMJ Disorders
Diagnosing TMJ disorder often requires a comprehensive approach, as its symptoms can overlap with various other conditions. Your dental professional will typically follow a systematic process to accurately identify the cause and type of your jaw discomfort.
Initial Consultation and Medical History
The diagnostic process usually begins with a thorough discussion of your medical and dental history. Your dentist will ask about:
- The nature, location, and intensity of your pain.
- When your symptoms started and what makes them better or worse.
- Any history of jaw injury, arthritis, or chronic pain conditions.
- Your habits, such as teeth grinding or clenching, stress levels, and diet.
Clinical Examination
A physical examination is crucial. Your dentist will:
- Palpate (feel) your jaw joints and muscles: They will gently press on your jaw, neck, and facial muscles to identify areas of tenderness, spasm, or trigger points.
- Observe and listen to your jaw: They will ask you to open and close your mouth, noting the range of motion, any deviations in jaw movement, and listening for clicks, pops, or grating sounds.
- Check your bite: They will assess how your upper and lower teeth come together (occlusion) and look for signs of excessive wear on your teeth, which can indicate bruxism.
- Evaluate your posture: Especially your head and neck alignment, as poor posture can contribute to TMD.
Imaging Studies
In some cases, imaging may be necessary to visualize the joint structures and rule out other conditions.
- Dental X-rays (Panorex): Provide a general overview of the teeth and jawbones.
- Computed Tomography (CT) Scan: Offers detailed images of the bone structure of the joint, useful for detecting arthritis or fractures.
- Magnetic Resonance Imaging (MRI): Considered the gold standard for visualizing the soft tissues of the TMJ, particularly the articular disc and surrounding muscles. An MRI can show if the disc is displaced, if there is inflammation, or if there is fluid accumulation within the joint.
- Arthrography: Involves injecting a contrast dye into the joint before an X-ray or CT scan, providing detailed images of the joint surfaces and disc. This is less commonly used today due to MRI advances.
Differential Diagnosis
Due to the varied nature of TMJ symptoms, your dentist will also consider other conditions that might mimic TMD, such as:
- Sinus infections
- Toothaches or dental abscesses
- Trigeminal neuralgia (a nerve disorder causing facial pain)
- Cluster headaches or migraines
- Ear infections
- Salivary gland disorders
A thorough diagnosis is critical to ensure that the chosen TMJ treatment strategy is effective and targeted to your specific condition.
Treatment Options
The approach to TMJ treatment is typically conservative and non-invasive, focusing on pain relief and restoring normal jaw function. Surgery is generally considered a last resort after other methods have failed. The American Dental Association (ADA) emphasizes a conservative, reversible approach first.
Conservative Treatments (First Line of Defense)
1. Self-Care and Home Remedies
These simple yet effective strategies can provide significant relief, especially for mild to moderate jaw pain.
- Soft Food Diet: Avoid hard, chewy, or sticky foods that put strain on the jaw. Opt for soups, yogurt, mashed potatoes, and smoothies.
- Ice and Heat Packs: Apply ice packs for acute pain and swelling (15-20 minutes, several times a day) or moist heat for muscle relaxation and chronic stiffness.
- Gentle Jaw Exercises: Your dentist or physical therapist may recommend specific stretches and exercises to improve jaw mobility and strength.
- Stress Reduction: Techniques like meditation, yoga, deep breathing, and adequate sleep can reduce muscle tension caused by stress.
- Avoid Extreme Jaw Movements: Limit wide yawns, excessive chewing gum, or biting nails.
- Good Posture: Maintain proper head and neck alignment to reduce strain on the jaw muscles.
2. Medications
- Over-the-Counter (OTC) Pain Relievers: Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen can reduce pain and inflammation.
- Muscle Relaxants: Prescription medications like cyclobenzaprine can help alleviate muscle spasms and tension, especially when taken before bed.
- Tricyclic Antidepressants: Low doses of drugs like amitriptyline can be prescribed to help control pain, promote sleep, and reduce clenching, even if depression isn't present.
- Corticosteroids: In some cases, a corticosteroid injection directly into the joint can reduce inflammation and pain, though this is usually a short-term solution.
3. Oral Appliances (Splints or Night Guards)
A night guard or oral splint is one of the most common and effective TMJ treatment options, particularly for bruxism-related TMD.
- Mechanism: These custom-made acrylic devices fit over your upper or lower teeth. They work by:
- Creating a barrier between the upper and lower teeth, preventing grinding and clenching.
- Repositioning the jaw to a more comfortable and relaxed position, reducing strain on the TMJ.
- Distributing bite forces more evenly across the teeth.
- Types:
- Stabilization Splints: The most common type, designed to relax the jaw muscles and protect teeth from grinding. Worn primarily at night.
- Repositioning Splints: Less common, these are designed to temporarily change the bite by holding the jaw in a specific position to encourage disc repositioning. These require careful monitoring.
- Pros: Non-invasive, reversible, effective for many, protects teeth.
- Cons: Can be expensive (custom-made), requires adaptation period, some people find them uncomfortable.
!Illustration showing a transparent custom-fitted night guard worn over the upper teeth, with an arrow pointing to the TMJ joint.
4. Physical Therapy
A physical therapist specializing in craniomandibular disorders can teach you exercises and techniques to improve jaw function and reduce pain.
- Exercises: Stretching, strengthening, and coordination exercises for the jaw muscles.
- Manual Therapy: Massage, trigger point release, and joint mobilization techniques.
- Posture Correction: Guidance on proper head, neck, and shoulder posture.
- Therapeutic Ultrasound or Laser Therapy: Can be used to reduce inflammation and promote healing.
5. Injections
- Botox Injections: Botulinum toxin (Botox) can be injected into the masseter and temporalis muscles to temporarily relax them, reducing clenching and grinding and thereby alleviating pain. Effects typically last 3-6 months.
- Trigger Point Injections: Local anesthetic and sometimes corticosteroids injected directly into muscle trigger points to relieve pain and spasm.
Advanced/Interventional Treatments (When Conservative Methods Fail)
If conservative TMJ treatment options don't provide sufficient relief, more advanced interventions may be considered.
1. Arthrocentesis
- Description: A minimally invasive procedure where small needles are inserted into the joint to lavage (wash out) the joint space with sterile fluid. This can remove inflammatory byproducts, release adhesions, and improve joint lubrication.
- Pros: Minimally invasive, relatively quick recovery.
- Cons: May not address underlying structural issues.
2. Arthroscopy
- Description: A minimally invasive surgical procedure where a small incision is made, and a tiny camera (arthroscope) is inserted into the joint. The surgeon can then visualize the joint, remove inflamed tissue, address adhesions, or reposition the disc using small instruments.
- Pros: Minimally invasive, faster recovery than open surgery.
- Cons: Limited view, not suitable for all complex cases.
3. Open-Joint Surgery
- Description: Traditional surgery that involves making a larger incision to access and operate on the TMJ. This is reserved for severe cases such as:
- Repairing or removing a severely damaged disc.
- Removing bone spurs.
- Repositioning the jaw bone.
- Ankylosis (fusion of the joint).
- Pros: Can address complex structural issues directly.
- Cons: More invasive, longer recovery, higher risks of complications.
4. Total Joint Replacement
- Description: For extremely severe and debilitating cases where the TMJ is irreversibly damaged (e.g., due to severe arthritis, trauma, or failed previous surgeries), the joint may be replaced with a prosthetic implant.
- Pros: Can restore function and eliminate pain for those with end-stage disease.
- Cons: Major surgery, significant recovery, potential for long-term complications or need for revision surgery.
5. Alternative and Complementary Therapies
- Acupuncture: Some patients find relief from pain through acupuncture, which involves inserting thin needles into specific points on the body.
- Biofeedback: Teaches patients to control involuntary body functions, such as muscle tension, to reduce clenching and pain.
Pro Tip: Always discuss all available options and their potential risks and benefits thoroughly with your dental professional or oral surgeon before committing to any treatment plan. A multidisciplinary approach involving dentists, oral surgeons, physical therapists, and pain management specialists often yields the best results.
Comparison Table: Conservative vs. Invasive TMJ Treatments
| Feature | Conservative Treatments (e.g., Night Guard, PT, Meds) | Invasive Treatments (e.g., Arthroscopy, Open Surgery) |
|---|---|---|
| Goal | Pain relief, muscle relaxation, restore function, prevent damage. | Address severe structural damage, disc displacement, joint degeneration. |
| Approach | Non-surgical, reversible, focuses on self-care and minimal intervention. | Surgical intervention requiring incisions, anesthesia, and recovery. |
| Typical Cost Range | $300 - $3,000+ (depending on duration, night guard type, therapy sessions). | $5,000 - $25,000+ (highly variable by procedure complexity and location). |
| Recovery Time | Days to weeks for initial relief, ongoing management. | Weeks to several months, potentially requiring extensive physical therapy. |
| Effectiveness | Highly effective for most patients, especially for myofascial pain and bruxism. | Reserved for severe cases; can provide significant relief where conservative methods fail. |
| Risks | Minimal (e.g., temporary discomfort from splint, medication side effects). | Higher risks (e.g., infection, nerve damage, scarring, anesthesia complications). |
Step-by-Step Process for Common TMJ Treatment (Oral Appliance Therapy)
For many individuals experiencing TMJ symptoms, particularly those related to bruxism or muscle tension, the use of a custom-fabricated oral appliance (like a night guard or stabilization splint) is a highly effective and common first-line TMJ treatment. Here’s what you can expect:
Step 1: Initial Consultation and Diagnosis
- Dental Visit: Your journey begins with a visit to your dentist or a TMJ specialist. They will conduct a thorough examination as described in the "Diagnosis" section, including reviewing your medical history, palpating your jaw muscles, observing jaw movement, and potentially taking X-rays or an MRI.
- Discussion: Based on the diagnosis, your dentist will explain if an oral appliance is a suitable TMJ treatment option for you and discuss other potential contributing factors.
Step 2: Impressions and Fabrication
- Jaw Impressions: If an oral appliance is recommended, the dental team will take precise impressions (molds) of your upper and/or lower teeth. This can be done using traditional putty or digital scanning technology.
- Bite Registration: They will also take a "bite registration" to capture how your teeth come together, ensuring the appliance is custom-designed to position your jaw comfortably.
- Lab Fabrication: These impressions and bite records are sent to a dental laboratory, where skilled technicians will custom-fabricate your night guard or splint from durable acrylic material. This process typically takes 1-3 weeks.
Step 3: Appliance Fitting and Adjustment
- First Fitting: Once your custom appliance is ready, you'll return for a fitting appointment. The dentist will ensure the appliance fits snugly but comfortably over your teeth.
- Bite Adjustment: They will meticulously check your bite with the appliance in place and make any necessary adjustments to ensure it doesn't create new discomfort or pressure points. The goal is a balanced and relaxed jaw position.
- Instructions: You'll receive detailed instructions on how to insert and remove your appliance, how often to wear it (usually nightly, but sometimes during the day for severe cases), and how to clean and care for it.

Step 4: Adaptation Period
- Initial Discomfort: It's normal to experience a short adaptation period. You might feel some initial tightness, increased saliva production, or a slight change in your bite sensation. This usually subsides within a few days to a week as your mouth adjusts.
- Consistency is Key: Adhering to the prescribed wearing schedule is crucial for the success of the treatment.
Step 5: Follow-up and Ongoing Adjustments
- Follow-up Appointments: You'll typically have follow-up appointments within a few weeks to assess your progress and make any further adjustments to the appliance. Your dentist will check for improvements in TMJ symptoms like pain, clicking, and jaw mobility.
- Long-Term Care: Depending on your condition, you may need periodic check-ups to monitor your appliance's fit and wear. Over time, your bite can shift, or the appliance itself can wear down, necessitating adjustments or replacement.
- Integration with Other Therapies: Oral appliance therapy is often combined with other conservative treatments, such as physical therapy, stress management, or medication, for a holistic approach to TMJ treatment.
This step-by-step process ensures that your custom night guard or splint is tailored precisely to your needs, maximizing its effectiveness in relieving jaw pain and improving your overall jaw health.
Cost and Insurance
Understanding the financial aspects of TMJ treatment is crucial, as costs can vary significantly based on the severity of your condition, the type of treatment, your location, and your insurance coverage. It's important to get a clear estimate from your dental professional.
Average US Cost Ranges for TMJ Treatments:
| Treatment Type | Average US Cost Range (Without Insurance) | Notes |
|---|---|---|
| Initial Consultation/Diagnosis | $50 - $300 | Includes exam, possibly X-rays; specialists may charge more. |
| Over-the-Counter Medications | $10 - $30 per month | NSAIDs, pain relievers. |
| Prescription Medications | $10 - $100+ per prescription | Muscle relaxants, antidepressants, depending on drug and dosage. |
| Custom Oral Appliance (Night Guard/Splint) | $300 - $1,500 | Varies by material, complexity, and dentist's fees. Over-the-counter guards are cheaper but less effective. |
| Physical Therapy (per session) | $75 - $200 | Multiple sessions are often required; typically covered by medical insurance. |
| Botox Injections (for TMJ) | $400 - $1,000 per treatment | Cost varies by units injected and provider; typically requires repeat treatments every 3-6 months. |
| Corticosteroid Injections | $150 - $500 per injection | May be covered by medical insurance if deemed medically necessary. |
| Arthrocentesis | $1,000 - $3,000 per joint | Often outpatient, can be covered by medical insurance. |
| Arthroscopy | $5,000 - $10,000 per joint | More invasive, usually covered by medical insurance with prior authorization. |
| Open-Joint Surgery | $15,000 - $25,000+ per joint | Major surgery, highly variable, almost always covered by medical insurance for severe cases. |
| Total Joint Replacement | $30,000 - $50,000+ per joint | Most complex and expensive, typically covered by medical insurance for specific indications. |
Insurance Coverage Details:
Navigating insurance for TMJ treatment can be complex because it often blurs the lines between dental and medical coverage.
-
Medical Insurance:
- Most often covers diagnostic services (like MRI scans, CT scans) and non-dental treatments such as physical therapy, prescription medications, Botox injections, and all surgical procedures (arthrocentesis, arthroscopy, open-joint surgery).
- Coverage for oral appliances (like a night guard) can be a gray area. Some medical plans may cover it if it's explicitly prescribed for a medical condition (like TMD, not just teeth grinding) and deemed medically necessary. You'll likely need a letter of medical necessity from your dentist or oral surgeon.
- Always check with your medical insurance provider for specifics on deductibles, co-pays, and services requiring pre-authorization. Use CPT codes provided by your doctor to inquire about coverage.
-
Dental Insurance:
- Generally covers routine dental care, fillings, crowns, and sometimes a portion of orthodontic treatment.
- Limited coverage for TMJ. Most dental plans do NOT cover TMD treatment beyond basic diagnostic X-rays or possibly a small portion of an oral appliance. They typically classify TMJ as a "medical condition" rather than a "dental procedure."
- However, some premium dental plans might offer limited coverage for night guards if prescribed for bruxism or TMD.
-
Payment Plans and Financing Options:
- Many dental and oral surgery offices offer in-house payment plans, allowing you to pay for treatment over several months.
- Third-party financing companies like CareCredit® or LendingClub® provide healthcare credit cards with low or no-interest payment options for qualified patients.
- Pro Tip: Don't let cost deter you from seeking help. Discuss financing options with your provider's office. Many are willing to work with patients to make treatment affordable.
Recovery and Aftercare
Recovery from TMJ treatment varies significantly depending on the type and invasiveness of the intervention. However, aftercare is crucial for achieving long-term relief and preventing recurrence of jaw pain.
After Conservative Treatments (e.g., Oral Appliance, Physical Therapy, Medications)
-
Oral Appliance (Night Guard/Splint):
- Consistent Wear: Adhere strictly to your dentist's instructions regarding how often and how long to wear your appliance. Inconsistent use can hinder progress.
- Hygiene: Clean your night guard daily with a toothbrush and mild soap or denture cleaner. Store it in a protective case when not in use.
- Follow-up Adjustments: Attend all scheduled follow-up appointments for adjustments. Your bite can shift, or the appliance may need fine-tuning.
- Patience: It may take several weeks or even months to experience significant relief. Be patient and consistent.
-
Physical Therapy:
- Exercise Adherence: Diligently perform all prescribed jaw exercises and stretches at home. These are vital for strengthening muscles, improving flexibility, and correcting posture.
- Posture Awareness: Consciously maintain good posture throughout the day, especially if you have a desk job.
- Ergonomics: Adjust your workspace to support proper head and neck alignment.
-
Medications:
- Follow Prescriptions: Take medications exactly as prescribed by your doctor. Do not self-adjust dosages.
- Report Side Effects: Inform your doctor about any adverse side effects.
- Not a Long-Term Solution: Medications typically manage symptoms; they don't cure the underlying TMJ disorder.
After Interventional/Surgical Treatments
Recovery from procedures like arthrocentesis, arthroscopy, or open-joint surgery will be more involved.
-
Immediate Post-Op:
- Pain Management: You will be prescribed pain medication. Take it as directed.
- Ice Packs: Apply ice to the surgical area to reduce swelling and bruising.
- Soft Diet: Stick to a very soft or liquid diet for the initial days or weeks, gradually reintroducing solid foods as advised by your surgeon.
- Rest: Limit jaw movement and get plenty of rest.
-
Rehabilitation (Physical Therapy):
- Crucial Component: Post-surgical physical therapy is paramount for successful recovery. It helps restore jaw mobility, prevent stiffness, and regain strength.
- Guided Exercises: Follow a structured rehabilitation program, starting with passive movements and progressing to active exercises.
- Gradual Increase: Do not rush the recovery process. Pushing your jaw too hard, too soon, can lead to setbacks.
-
Long-Term Aftercare:
- Avoid Habits: Continue to avoid habits like teeth grinding, clenching, and excessive gum chewing.
- Stress Management: Implement stress-reduction techniques to prevent muscle tension.
- Regular Dental Check-ups: Continue regular dental visits to monitor your oral health and TMJ condition.
- Lifestyle Adjustments: Be mindful of your posture, sleep positions, and activities that might strain your jaw.
Pro Tip: Open communication with your dental professional or surgeon is key throughout your recovery. Report any new or worsening symptoms, persistent pain, or concerns immediately. Adherence to aftercare instructions significantly impacts the success and longevity of your TMJ treatment.
Prevention
While not all TMJ disorder cases are preventable, especially those stemming from severe trauma or degenerative conditions, many instances, particularly those related to muscle tension and habits, can be mitigated or avoided through proactive measures. Incorporating these practices into your daily life can significantly reduce your risk of developing jaw pain and dysfunction.
- Manage Stress Effectively: Stress is a major contributor to teeth clenching and jaw tension. Practice relaxation techniques such as meditation, deep breathing exercises, yoga, or engaging in hobbies.
- Be Mindful of Jaw Habits:
- Avoid Clenching and Grinding (Bruxism): Be aware of when you're clenching your jaw, especially during stressful situations or while concentrating. Gently remind yourself to relax your jaw, letting your lips touch but keeping your teeth apart.
- Use a Night Guard (Prophylactically): If you know you clench or grind your teeth at night, even without severe symptoms, a custom night guard can protect your teeth and joints from damaging forces.
- Avoid Excessive Chewing: Limit chewing gum, ice, or very tough foods.
- Don't Bite Nails or Pens: These habits place undue stress on your jaw joints.
- Maintain Good Posture:
- Head and Neck Alignment: Keep your head balanced directly over your spine, avoiding a forward head posture, which can strain neck and jaw muscles.
- Ergonomics: Ensure your workspace (computer screen height, chair support) promotes good posture.
- Practice Jaw Relaxation Techniques: Throughout the day, periodically check in with your jaw. Let your jaw hang loose, with your teeth slightly apart, and your tongue resting gently on the roof of your mouth.
- Eat a Jaw-Friendly Diet: For those prone to jaw issues, a softer diet can reduce strain. Cut food into small pieces.
- Avoid Extreme Jaw Movements: Try not to open your mouth excessively wide, especially during yawning. Support your chin during a wide yawn.
- Regular Dental Check-ups: Your dentist can spot early signs of bruxism, tooth wear, or jaw misalignment during routine examinations, allowing for early intervention.
- Protect Your Jaw from Trauma: Wear a mouthguard during contact sports to prevent direct impact injuries to the jaw.
By adopting these preventive strategies, you can reduce the strain on your temporomandibular joints and the surrounding muscles, thereby lowering your risk of developing TMJ disorder and avoiding the discomfort of chronic jaw pain.
Risks and Complications
While most TMJ disorder cases respond well to conservative TMJ treatment, there are potential risks and complications associated with both the condition itself and its various treatments. Being aware of these can help you make informed decisions and seek timely intervention.

Risks Associated with Untreated TMJ Disorders:
- Chronic Pain: If left untreated, acute jaw pain can become chronic, impacting daily activities, sleep, and overall quality of life.
- Permanent Jaw Dysfunction: Long-term disc displacement, joint degeneration (arthritis), or muscle imbalance can lead to irreversible changes in the joint structure, causing persistent locking, limited jaw opening, or severe asymmetry.
- Tooth Damage: Chronic bruxism (grinding and clenching) can lead to excessive tooth wear, fractures, sensitivity, and even loss of teeth.
- Malnutrition/Weight Loss: Severe jaw pain and difficulty chewing can lead to changes in diet, potentially causing nutritional deficiencies or unintended weight loss.
- Psychological Impact: Living with chronic pain can contribute to anxiety, depression, frustration, and reduced social interaction.
- Spread of Pain: Untreated TMJ issues can exacerbate or contribute to chronic headaches, neck pain, and earaches.
Risks and Complications of TMJ Treatments:
Conservative Treatments:
- Oral Appliances (Night Guards/Splints):
- Initial Discomfort: Temporary soreness, increased salivation, or gagging reflex.
- Bite Changes: Improperly designed or adjusted splints, or long-term use of certain repositioning splints, can potentially lead to undesirable changes in your bite (though rare with stabilization splints under professional guidance).
- Allergic Reactions: Rare, but possible to materials used in the appliance.
- Medications: Side effects vary by medication (e.g., drowsiness, stomach upset for NSAIDs, dry mouth for muscle relaxants).
- Physical Therapy: Minimal risks, mainly temporary muscle soreness.
- Botox Injections:
- Temporary Weakness: Possible temporary weakness in surrounding muscles, leading to difficulty smiling or speaking.
- Bruising/Swelling: At injection sites.
- Asymmetry: Rarely, temporary facial asymmetry.
Surgical Treatments (Arthrocentesis, Arthroscopy, Open-Joint Surgery, Total Joint Replacement):
Surgical procedures carry inherent risks common to all surgeries, plus specific risks related to the delicate anatomy of the jaw joint:
- Infection: Risk of bacterial infection at the surgical site.
- Nerve Damage: The facial nerve and other nerves are in close proximity to the TMJ. Damage can lead to temporary or permanent facial weakness, numbness, or altered sensation.
- Bleeding: Excessive bleeding during or after surgery.
- Anesthesia Risks: Allergic reactions, respiratory issues, or cardiovascular events.
- Scarring: Especially with open-joint surgery.
- Limited Jaw Opening (Fibrosis/Ankylosis): Post-surgical scarring or complications can lead to reduced jaw mobility.
- Failed Treatment/Recurrence: Surgery does not guarantee permanent relief, and symptoms can recur or new problems may develop.
- Hardware Complications (for Joint Replacement): Prosthetic joint components can fracture, loosen, or become infected, requiring revision surgery.
- Hearing Changes: Rarely, due to the proximity of the joint to the ear.
It is crucial to have a detailed discussion with your oral surgeon about the potential risks and benefits specific to the recommended TMJ treatment for your condition. A thorough understanding empowers you to make informed decisions about your care.
Comparison Table: Common TMJ Medications
| Medication Type | Purpose | Pros | Cons |
|---|---|---|---|
| NSAIDs (e.g., Ibuprofen) | Reduce pain and inflammation | Widely available OTC, generally safe. | Stomach upset, liver/kidney issues with prolonged use. |
| Muscle Relaxants (e.g., Cyclobenzaprine) | Alleviate muscle spasms and tension | Effective for acute muscle pain, aids sleep. | Drowsiness, dizziness, dry mouth. Cannot be used long-term. |
| Tricyclic Antidepressants (low dose, e.g., Amitriptyline) | Pain modulation, sleep aid, anti-clench properties | Can manage chronic pain and improve sleep. | Drowsiness, dry mouth, constipation, potential cardiac effects. |
| Botulinum Toxin (Botox) | Temporarily relax jaw muscles | Highly effective for muscle-related pain and bruxism. | Expensive, temporary (3-6 months), rare facial asymmetry. |
| Corticosteroids (oral or injected) | Reduce severe inflammation and pain | Rapid reduction of swelling and pain. | Short-term use only, potential side effects (e.g., blood sugar). |
Children / Pediatric Considerations
TMJ disorder is not exclusive to adults; children and adolescents can also experience jaw pain and dysfunction, although it is often less recognized and diagnosed in younger populations. The causes and symptoms can differ slightly, and treatment approaches are adapted to account for a child's growth and development.
Causes of TMJ in Children:
- Trauma: Direct injury to the jaw or head from falls, sports accidents, or other impacts is a common cause in children.
- Bruxism: While often temporary in young children, persistent teeth grinding and clenching can still lead to TMJ symptoms.
- Habits: Thumb-sucking, nail-biting, or prolonged pacifier use can sometimes contribute to jaw misalignment or stress.
- Developmental Issues: Congenital anomalies, malocclusion (bad bite), or orthodontic issues (e.g., extreme overbite/underbite) can sometimes play a role.
- Juvenile Idiopathic Arthritis: Similar to adult rheumatoid arthritis, this autoimmune condition can affect the TMJs in children, potentially leading to joint damage and growth disturbances.
- Stress: Academic pressure, social issues, or anxiety can manifest as jaw clenching in children, just as in adults.
Signs and Symptoms in Children:
Children may not always articulate their jaw pain clearly, so parents should look for:
- Difficulty chewing hard foods or reluctance to eat.
- Clicking or popping sounds in the jaw, especially if painful.
- Headaches (often reported as forehead or temple pain).
- Earaches without signs of infection.
- Limited ability to open the mouth wide.
- Changes in bite or the way teeth fit together.
- Facial swelling or asymmetry.
- Morning stiffness or pain when waking up.
- Changes in behavior, such as irritability or withdrawal, possibly due to pain.
Diagnosis and Treatment for Children:
Diagnosis in children often involves a thorough clinical examination by a pediatric dentist or orthodontist, a review of medical history, and sometimes imaging (with careful consideration of radiation exposure).
Treatment for children is always conservative and reversible, prioritizing growth and development:
- Behavioral Modification: Addressing habits like bruxism or thumb-sucking.
- Soft Diet: Temporary dietary adjustments.
- Pain Relief: OTC pain relievers (like ibuprofen) under medical guidance.
- Physical Therapy: Gentle exercises and stretches tailored for children.
- Oral Appliances: Custom-made night guards or splints may be used, but with careful monitoring to avoid interfering with jaw growth. These are often made from softer materials.
- Orthodontic Treatment: In some cases, addressing severe malocclusion may alleviate TMJ stress, but this is approached cautiously and often after conservative TMD management.
- Stress Management: Teaching children relaxation techniques.
Pro Tip for Parents: If your child complains of persistent jaw pain, difficulty chewing, or exhibits unusual jaw sounds or movements, consult a pediatric dentist or an orthodontist specializing in TMJ disorders. Early intervention can prevent long-term complications and ensure healthy jaw development.
Frequently Asked Questions
Is TMJ permanent?
TMJ disorder is not necessarily permanent. While some underlying structural issues like severe arthritis can lead to lasting changes, many cases, especially those related to muscle tension or disc displacement, can be effectively managed and even resolved with conservative TMJ treatment and lifestyle changes. The goal is often to manage symptoms and improve function, which can lead to long-term relief.
How long does TMJ last?
The duration of TMJ symptoms varies greatly. Acute symptoms, often triggered by stress or minor injury, might resolve within a few days or weeks with self-care. Chronic TMJ can last for months or years, often with cycles of flare-ups and periods of relief. Consistent TMJ treatment and adherence to management strategies are key to controlling its duration.

Can TMJ go away on its own?
Mild cases of TMJ disorder, particularly those caused by temporary stress or minor muscle strain, can sometimes resolve on their own with rest, a soft diet, and stress reduction. However, persistent or worsening TMJ symptoms like significant jaw pain, locking, or severe clicking warrant professional evaluation, as these conditions are less likely to disappear without intervention.
What is the fastest way to relieve TMJ pain?
For immediate relief, apply an ice pack to the painful area (15-20 minutes), take an over-the-counter NSAID like ibuprofen, stick to a soft diet, and practice gentle jaw stretches. Stress reduction techniques and conscious relaxation of your jaw muscles can also provide quick relief. However, these are temporary solutions; consult a dentist for a long-term plan.
Does insurance cover TMJ treatment?
Insurance coverage for TMJ treatment is often a gray area. Medical insurance typically covers diagnostic tests (like MRI) and medically necessary treatments such as physical therapy, prescription medications, Botox injections, and surgical interventions. Dental insurance may offer limited coverage for oral appliances like a night guard, but often classifies TMD as a medical condition. Always verify with both your medical and dental insurance providers for specific coverage details.
What is the difference between a dental night guard and a TMJ splint?
While often used interchangeably by the public, a dental night guard primarily protects teeth from grinding and clenching by providing a barrier. A TMJ splint (or stabilization splint) is a more precisely fabricated oral appliance designed not just to protect teeth but also to reposition the jaw, relax the muscles, and distribute forces more evenly across the jaw joint, specifically for TMJ disorder management. Both are custom-made, but a TMJ splint often has a more therapeutic function.
Can TMJ affect my ears?
Yes, TMJ disorder can significantly affect your ears due to the close proximity of the jaw joint to the ear canal. Common ear-related TMJ symptoms include earaches (often mistaken for infections), a feeling of fullness in the ear, muffled hearing, and tinnitus (ringing in the ears). These symptoms usually improve as the TMJ condition is treated.
What foods should I avoid with TMJ?
If you have TMJ disorder, it's best to avoid foods that require excessive chewing or put strain on your jaw. This includes hard candies, nuts, raw vegetables (unless finely chopped), crusty bread, bagels, tough meats, chewing gum, and sticky foods like caramel. Opt for a soft diet of soups, yogurt, mashed potatoes, pasta, and cooked vegetables.
Is surgery necessary for TMJ?
For the vast majority of patients, surgery is NOT necessary for TMJ treatment. Conservative, non-invasive therapies such as oral appliances (night guards), physical therapy, medications, and lifestyle changes are highly effective for most cases. Surgical interventions are typically reserved for severe, debilitating cases that have not responded to any other forms of treatment.
How do I choose a TMJ specialist?
Look for a dentist, oral and maxillofacial surgeon, or an orofacial pain specialist with specific training and experience in diagnosing and treating TMJ disorder. You can ask your general dentist for a referral, check professional organizations like the American Academy of Orofacial Pain, and read patient reviews. Ensure they advocate for a conservative, evidence-based approach to TMJ treatment.
When to See a Dentist
While occasional jaw stiffness or a benign click may not warrant immediate concern, certain TMJ symptoms indicate that it's time to seek professional evaluation from a dentist or TMJ specialist. Early intervention can often prevent the condition from worsening and lead to more effective, conservative TMJ treatment.
You should schedule a routine appointment with your dentist if you experience any of the following:
- Persistent Jaw Pain: If your jaw pain lasts for more than a few days, does not improve with self-care, or becomes a regular occurrence.
- Chronic Headaches or Earaches: Especially if they are unresponsive to typical remedies and are accompanied by other TMJ symptoms.
- Difficulty Chewing: If you find it painful or challenging to eat certain foods.
- Clicking, Popping, or Grating with Pain: If jaw sounds are accompanied by discomfort or changes in your bite.
- Limited Jaw Movement: If you can't open your mouth as wide as usual, or if your jaw feels stiff upon waking.
- Signs of Bruxism: If you or your partner notice teeth grinding or clenching, especially if it leads to tooth sensitivity or wear.
Seek more urgent or emergency dental attention if you experience these red flags:
- Sudden, Severe Jaw Pain: Especially if it's excruciating and debilitating.
- "Locked Jaw": If your jaw gets completely stuck in an open or closed position and you cannot move it back into place on your own. This requires immediate attention to prevent further damage and alleviate intense discomfort.
- Significant Swelling: If there is noticeable swelling on one side of your face that is accompanied by severe pain, fever, or difficulty swallowing, as this could indicate an infection or other serious issue.
- Pain After Trauma: If you've experienced a direct injury to your jaw, head, or neck and are now experiencing jaw pain, limited movement, or swelling, get it checked immediately to rule out fractures or severe joint damage.
Don't ignore jaw pain or other TMJ symptoms. Consulting a dental professional specializing in temporomandibular joint dysfunction will help you get an accurate diagnosis and embark on an effective TMJ treatment plan, restoring comfort and function to your jaw.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Tmj Massage Near Me: Complete Guide
Temporomandibular joint disorder, commonly known as TMJD, affects millions of Americans, causing debilitating pain, discomfort, and significantly impacting quality of life. If you're experiencing jaw pain, clicking, or difficulty chewing, you're not alone. Up to 15% of American adults experience
February 23, 2026
Tmd Treatment: Complete Guide
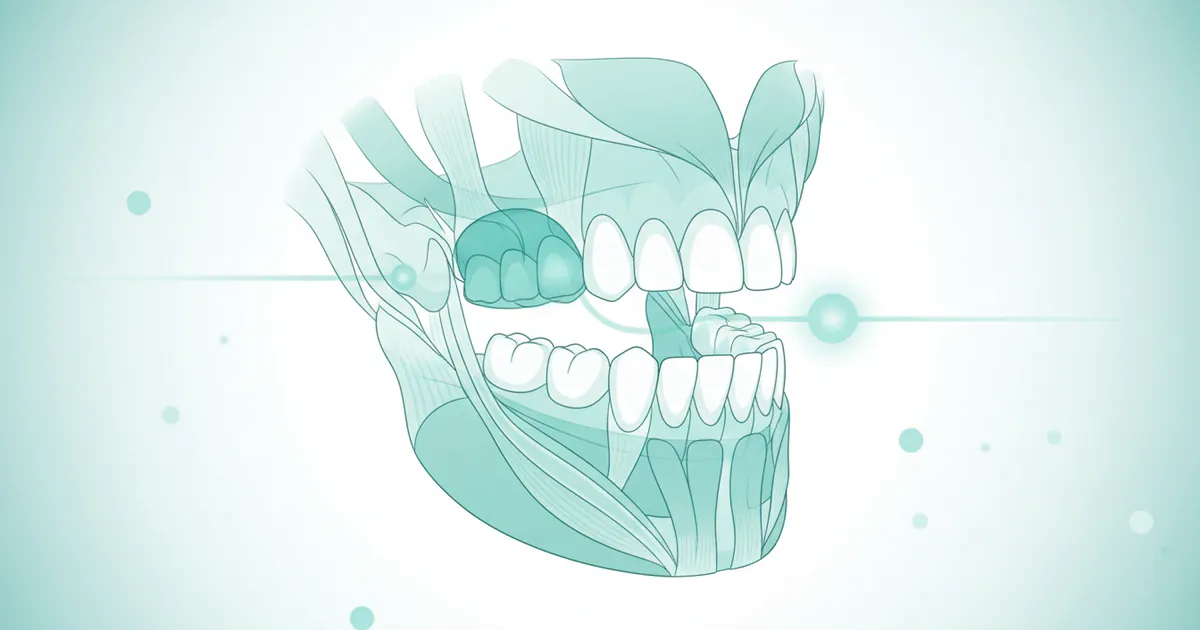
Experiencing persistent jaw pain, clicking sounds when you chew, or debilitating headaches that seem to originate from your face? You're not alone. Temporomandibular joint (TMJ) disorders, often referred to collectively as TMD, affect an estimated 10 million Americans, with women disproportionat
February 23, 2026
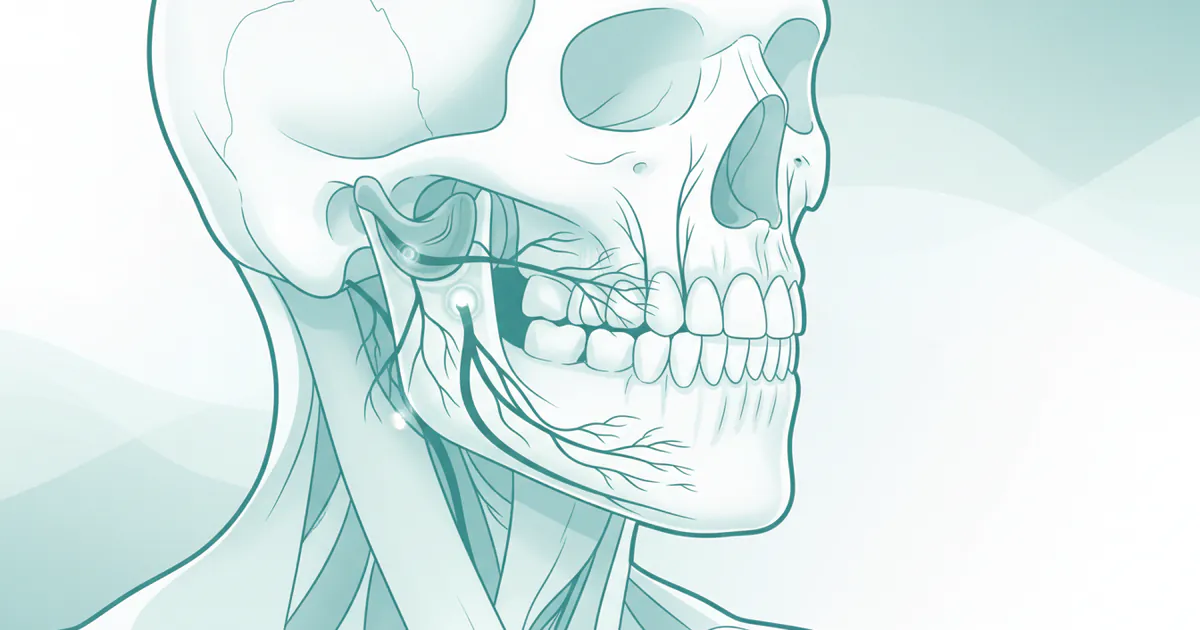
Tmj Nerve Damage Symptoms: Complete Guide
Experiencing persistent facial pain, numbness, or tingling can be distressing, especially when the source is unclear. While many people are familiar with general jaw pain associated with temporomandibular joint (TMJ) disorders, the less commonly understood aspect of tmj nerve damage symptoms can
February 23, 2026
Remi Night Guard: Complete Guide
Remi Night Guard: Complete Guide
February 23, 2026