Tmj vs Normal Jaw: Complete Comparison Guide
Key Takeaways
- Experiencing persistent jaw pain, clicking sounds, or difficulty chewing can be frustrating and disruptive to daily life. While many people occasionally feel a stiff jaw, when these symptoms become chronic, they often signal an underlying issue with the temporomandibular joint (TMJ). Understanding t
Tmj vs Normal Jaw: Complete Comparison Guide
Experiencing persistent jaw pain, clicking sounds, or difficulty chewing can be frustrating and disruptive to daily life. While many people occasionally feel a stiff jaw, when these symptoms become chronic, they often signal an underlying issue with the temporomandibular joint (TMJ). Understanding the difference between a tmj vs normal jaw is crucial for recognizing when you need professional help and embarking on the path to relief. Did you know that an estimated 10 to 15 million Americans are affected by temporomandibular joint disorders (TMDs) at any given time? This comprehensive guide will equip you with the knowledge to distinguish between a healthy, functional jaw and one experiencing the challenges of a TMJ disorder, exploring everything from causes and symptoms to the full spectrum of treatment for tmj and practical advice for managing and preventing discomfort, including persistent ear and jaw pain. We'll delve into the anatomy of a healthy jaw, dissect the various types of TMJ disorders, and provide a detailed roadmap for diagnosis, treatment, and recovery, ensuring you have the authoritative information you need from SmilePedia.net.

Key Takeaways:
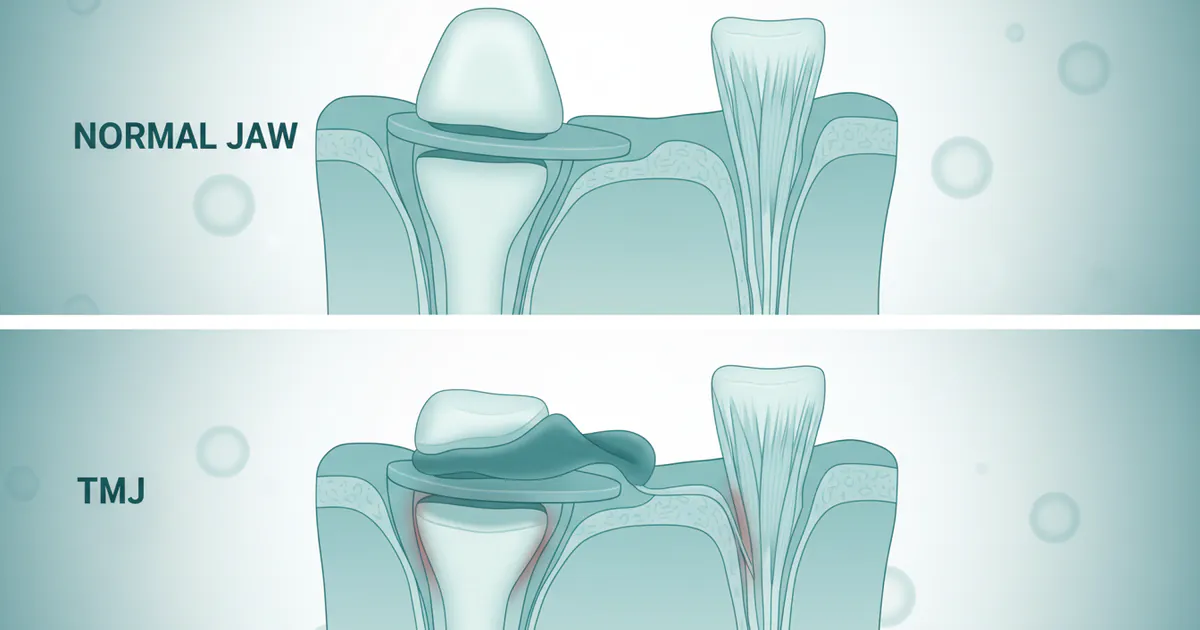
- Normal Jaw Function: A healthy jaw moves smoothly, silently, and without pain, allowing for full range of motion during chewing, speaking, and yawning.
- TMJ vs. TMD: The "TMJ" refers to the temporomandibular joint itself; "TMD" (Temporomandibular Joint Disorder) refers to a collection of conditions affecting this joint and surrounding muscles.
- Common Symptoms: TMD often presents with pain in the jaw, ear, or temple, clicking/popping sounds, limited jaw movement, and headaches. Persistent ear and jaw pain is a hallmark symptom.
- Treatment Diversity: Treatment for TMJ ranges from conservative options like self-care, physical therapy, and oral appliances (e.g., nightguards, costing $300-$800 without insurance) to advanced interventions like injections or surgery.
- Cost Variation: Treatment costs vary widely. Initial consultations typically range from $100-$300, while complex surgical procedures can exceed $15,000. Insurance coverage for TMD is often complex, sometimes falling under medical, sometimes dental.
- Recovery Timeline: Most conservative treatments show improvement within 2-6 weeks, though ongoing management might be required. Surgical recovery can take several months.
- Prevention is Key: Managing stress, avoiding teeth clenching/grinding, and practicing good posture can significantly reduce the risk of developing TMD.
Understanding the Jaw: Normal Anatomy and Function
To truly grasp what constitutes a TMJ disorder, it's essential to first understand the intricate mechanics of a healthy, "normal jaw." The temporomandibular joint (TMJ) is one of the most complex joints in the human body, enabling a remarkable range of motion essential for everyday functions.
The Anatomy of a Healthy TMJ
The TMJ is actually a pair of joints, one on each side of your head, located just in front of your ears. Each joint connects your lower jaw (mandible) to the temporal bone of your skull. This sophisticated joint comprises several key components:
- Condyle: The rounded upper end of the mandible.
- Temporal Bone: The socket portion of the joint, located at the base of the skull.
- Articular Disc (Meniscus): A small, oval-shaped piece of cartilage that acts as a shock absorber between the condyle and the temporal bone. It allows the joint to glide smoothly and protects the bone surfaces.
- Ligaments: Strong bands of fibrous tissue that stabilize the joint and limit excessive movement.
- Muscles: A complex network of muscles surrounding the joint, including the masseter, temporalis, and pterygoid muscles, which are responsible for jaw movement (opening, closing, side-to-side, forward, and backward).
Characteristics of a Healthy Jaw
A healthy jaw functions with remarkable efficiency and comfort. Here's what you should expect from a normal temporomandibular joint:
- Smooth Movement: The jaw opens and closes without catching, locking, or sudden jerks. The articular disc stays perfectly positioned between the bones, ensuring a frictionless glide.
- Silence: A healthy TMJ operates silently. You should not hear clicking, popping, grating, or grinding sounds when you move your jaw.
- Pain-Free: There should be no pain or discomfort in the jaw joint, muscles, face, head, or neck during jaw movements or at rest.
- Full Range of Motion: You should be able to open your mouth wide enough to comfortably fit three fingers stacked vertically between your upper and lower front teeth (typically 40-50mm). You should also be able to move your jaw smoothly from side to side and forward.
- Stable Bite: Your upper and lower teeth should come together evenly and comfortably, without any feeling of misalignment or strain in the jaw muscles.
In essence, a normal jaw is something you rarely think about because it simply works as it should, facilitating essential activities like eating, speaking, and expressing emotions without any noticeable effort or pain.
What is Temporomandibular Joint (TMJ) Disorder?
While "TMJ" is often used colloquially to refer to a problem, it's important to clarify that TMJ stands for the Temporomandibular Joint itself. The actual condition is called a Temporomandibular Joint Disorder, often abbreviated as TMD or TMJD. TMDs are a group of conditions that affect the jaw joints, the muscles of mastication (chewing), and/or the surrounding facial structures.
TMDs are incredibly common, affecting a significant portion of the population. Estimates suggest that over 10 million Americans experience TMD symptoms at any given time, with women being two to three times more likely to be affected than men, particularly those in their childbearing years. The exact reasons for this gender disparity are still being researched but may involve hormonal influences, anatomical differences, and varying pain perception thresholds.
Unlike a single disease, TMDs encompass a wide spectrum of issues, from minor muscle discomfort to severe joint degeneration. They are often characterized by pain, restricted jaw movement, and noises originating from the joint. The complexity of the TMJ and its surrounding structures means that symptoms can be diverse and sometimes mimic other conditions, making accurate diagnosis crucial.
Unpacking the Differences: TMJ vs Normal Jaw
Understanding the distinction between a healthy, normal jaw and one affected by a TMJ disorder lies primarily in the presence or absence of symptoms and proper function. Here’s a detailed comparison:
Comparison Table: TMJ vs Normal Jaw Characteristics
| Feature | Normal Jaw | TMJ Disorder (TMD) |
|---|---|---|
| Pain | Absent | Present, often chronic, can be dull ache or sharp pain |
| Location of Pain | None | Jaw joint, face, ear, head, neck, shoulders |
| Jaw Movement | Smooth, unrestricted, full range of motion | Limited opening, stiffness, locking (open or closed) |
| Joint Sounds | Silent or very subtle | Clicking, popping, grating, grinding (crepitus) |
| Function | Easy chewing, speaking, yawning | Difficulty chewing, biting, speaking; discomfort |
| Muscle Tenderness | Absent | Present, especially in jaw, temple, and neck muscles |
| Bite Sensation | Stable, comfortable occlusion | Feels "off" or changing, malocclusion |
| Ear Symptoms | None | Ear pain, ringing (tinnitus), feeling of fullness |
| Headaches/Migraines | Infrequent, unrelated to jaw | Frequent tension headaches, migraines |
Detailed Symptom Comparison
- Pain:
- Normal Jaw: A healthy jaw does not produce pain. Any occasional soreness is usually due to temporary strain (e.g., eating very chewy food) and resolves quickly.
- TMJ Disorder: Pain is the most common symptom of TMD. It can be localized to the jaw joint itself, radiate into the face, temples, neck, or even shoulders. The pain can range from a dull, constant ache to sharp, stabbing pain, especially with movement. This often contributes to chronic ear and jaw pain.
- Jaw Movement and Range of Motion:
- Normal Jaw: You should be able to open your mouth wide (typically 40-50mm or the width of three fingers), move your jaw from side to side, and protrude it forward without effort or sensation of obstruction.
- TMJ Disorder: Restricted jaw opening is a classic sign. You might find it difficult to yawn, bite into an apple, or even speak comfortably. The jaw might "catch," "stick," or "lock" in either an open or closed position, requiring manipulation to release it.
- Joint Sounds:
- Normal Jaw: A normal TMJ is typically silent.
- TMJ Disorder: Many people with TMD experience sounds like clicking, popping, or grating (crepitus) when opening or closing their mouth. Clicking and popping usually indicate that the articular disc has temporarily displaced and then returned to its proper position during movement. Grating or grinding sounds often suggest more advanced degeneration or arthritic changes within the joint.
- Associated Symptoms:
- Normal Jaw: No associated symptoms beyond the immediate area.
- TMJ Disorder: TMD can manifest with a surprisingly wide range of referred symptoms due to the complex nerve connections in the head and neck. These include:
- Ear Pain: Often confused with an ear infection, this ear and jaw pain can be persistent and severe, even though the ear itself is healthy.
- Tinnitus: Ringing, buzzing, or hissing sounds in the ears.
- Vertigo/Dizziness: Feelings of imbalance.
- Headaches: Frequent tension-type headaches, migraines, or pain behind the eyes.
- Neck and Shoulder Pain: Tightness and pain due to compensatory muscle strain.
- Changes in Bite: A feeling that your teeth don't fit together properly or a sudden change in how your bite feels.
Types of TMJ Disorders
TMJ disorders are not a single condition but rather a collection of problems affecting the joint and its surrounding musculature. Dentists and oral surgeons typically categorize TMDs into three main groups, though a patient may experience more than one type concurrently:
1. Myofascial Pain
This is the most common type of TMD, accounting for approximately 70-80% of all cases. Myofascial pain involves discomfort or pain in the muscles that control jaw function (masseter, temporalis, pterygoids) and muscles in the neck and shoulders. It often stems from:
- Bruxism: Chronic teeth grinding or clenching (awake or asleep).
- Stress and Tension: Leading to muscle hyperactivity and spasms.
- Trauma: Acute injury to the jaw muscles.
- Poor Posture: Especially forward head posture, which strains jaw and neck muscles.
Symptoms typically include a dull, aching pain in the jaw, face, and temples, often accompanied by headaches and restricted jaw opening due to muscle stiffness.
2. Internal Derangement of the Joint
This category refers to structural problems within the TMJ itself, specifically involving the articular disc. The disc is designed to stay between the condyle and temporal bone, acting as a cushion.
- Disc Displacement with Reduction: The disc slips out of its normal position when the mouth is closed, but "reduces" or snaps back into place when the mouth opens, causing a characteristic click or pop. This is often an early stage of disc derangement.
- Disc Displacement Without Reduction: The disc remains displaced even when the mouth is open, meaning it never returns to its proper position. This can lead to limited jaw opening (often called a "closed lock") and sometimes grating or grinding sounds (crepitus) as bone rubs against bone. Pain can be constant.
- Dislocation: In severe cases, the condyle can completely dislocate from the temporal bone socket, making it impossible to close the mouth (an "open lock"). This requires immediate medical attention to manually reduce the dislocation.
3. Degenerative Joint Disease (Arthritis)
Like other joints in the body, the TMJ can be affected by various forms of arthritis.
- Osteoarthritis: This is the most common form, typically occurring in older individuals or as a result of long-standing disc displacement. It involves the breakdown of cartilage and bone within the joint, leading to pain, stiffness, and crepitus (grating sounds).
- Rheumatoid Arthritis: An autoimmune inflammatory disease that can affect multiple joints, including the TMJ. It causes chronic inflammation, pain, and can lead to significant joint destruction and deformity.
- Psoriatic Arthritis, Ankylosing Spondylitis: Other less common forms of arthritis can also manifest in the TMJ.
Understanding the specific type of TMD is crucial for a targeted and effective treatment for TMJ.
Why TMJ Disorders Develop: Causes and Contributing Factors
The development of TMD is often multifactorial, meaning a combination of factors usually contributes to its onset. It's rarely a single cause but rather a complex interplay of physical, behavioral, and sometimes psychological elements.
Primary Causes and Risk Factors:
- Trauma to the Jaw, Head, or Neck: A direct blow to the jaw, whiplash injury from a car accident, or even prolonged mouth opening during a dental procedure can damage the TMJ or surrounding muscles.
- Bruxism (Teeth Grinding or Clenching): This involuntary habit, often occurring during sleep or stressful situations, puts immense, sustained pressure on the TMJs and jaw muscles. Chronic clenching can lead to muscle fatigue, inflammation, and even structural changes in the joint. The American Dental Association (ADA) recognizes bruxism as a significant contributing factor to TMD.
- Stress and Anxiety: Psychological stress is a powerful exacerbating factor. High stress levels can lead to muscle tension throughout the body, including the jaw, and can significantly increase instances of bruxism.
- Malocclusion (Misaligned Bite): While historically thought to be a primary cause, the role of bite problems in TMD is still debated. However, a significant discrepancy in how the upper and lower teeth meet may, in some individuals, lead to compensatory muscle activity and joint strain, contributing to TMD symptoms.
- Arthritis and Other Inflammatory Conditions: As mentioned, osteoarthritis, rheumatoid arthritis, and other systemic inflammatory conditions can directly affect the TMJ, leading to pain, stiffness, and joint degeneration.
- Connective Tissue Diseases: Conditions like Ehlers-Danlos syndrome, which affect collagen and connective tissues, can lead to joint hypermobility and instability, making the TMJ more susceptible to derangement.
- Hormonal Factors: The higher prevalence of TMD in women, particularly during reproductive years, suggests a potential hormonal link. Estrogen receptors are present in the TMJ, and fluctuations may influence pain perception and joint health.
- Genetics: Some individuals may have a genetic predisposition to developing TMD, influencing their joint structure or pain processing.
- Poor Posture: Maintaining a forward head posture, often seen with prolonged computer use, can strain the neck and jaw muscles, shifting the alignment of the jaw and placing undue stress on the TMJs.
- Diet and Habits: Consistently chewing gum, eating very hard or chewy foods, or habitually biting nails can put repetitive strain on the jaw joints and muscles over time.
It's important to remember that for many individuals, identifying a single, definitive cause can be challenging. A thorough evaluation by a dental professional is essential to uncover the contributing factors in each specific case and guide appropriate treatment for TMJ.
Recognizing the Signs: Symptoms of TMJ Disorders
The symptoms of a TMJ disorder can be diverse and sometimes mimic other conditions, making accurate self-diagnosis difficult. If you experience any of the following, especially if they are persistent or recurrent, it's time to consult a dentist or oral surgeon.
Primary Symptoms:
- Pain or Tenderness in the Jaw: This is the most common symptom. The pain can be felt in front of the ear, in the jaw joint itself, or spread along the side of the face. It often worsens with chewing, speaking, or wide jaw movements.
- Pain in or Around the Ear: This is a very common and often misleading symptom. Many people initially consult an ENT (ear, nose, and throat) doctor because they experience intense ear and jaw pain, a feeling of fullness in the ear, or even hearing changes, only to find no ear infection. The pain can radiate from the jaw joint due to nerve pathways.
- Headaches: Frequent tension-type headaches, often located in the temples or behind the eyes, are strongly associated with TMD. In some cases, TMD can even trigger or exacerbate migraines.
- Clicking, Popping, or Grating Sounds: These sounds occur in the joint when opening, closing, or moving the jaw. While occasional, painless clicks might be considered within normal variation, persistent or painful sounds often indicate disc displacement or degenerative changes.
- Difficulty or Discomfort While Chewing: Painful or limited jaw movement can make it hard to bite or chew food, leading to a preference for soft diets.
- Limited Jaw Movement or Locking: You might find it difficult to open your mouth wide (e.g., to yawn or eat a large apple). In some cases, the jaw can "lock" in an open or closed position, making it impossible to move without manual manipulation.
- Muscle Tenderness and Fatigue: The muscles around the jaw, temples, neck, and even shoulders can feel sore, stiff, or fatigued, especially in the mornings if bruxism is present.
- Facial Swelling: Inflammation in the joint or surrounding muscles can sometimes cause noticeable swelling on one or both sides of the face.
Associated and Referred Symptoms:
- Tinnitus (Ringing in the Ears): A persistent ringing, buzzing, or hissing sound, often unilateral, can be a frustrating symptom of TMD.
- Vertigo or Dizziness: Feelings of unsteadiness or spinning sensations can occur due to the close proximity of the TMJ to the inner ear structures and shared nerve pathways.
- Changes in Bite: A sudden feeling that your upper and lower teeth don't fit together correctly, or a constant sensation that your bite is shifting.
- Shoulder and Neck Pain: Chronic tension in the jaw and facial muscles can refer pain and stiffness to the neck and shoulders.
- Numbness or Tingling: Less common, but nerve compression or irritation can sometimes lead to altered sensations in the face or jaw.
Pro Tip: Keep a symptom journal. Note down when your pain or other symptoms occur, what makes them better or worse, and how frequently they appear. This information will be invaluable for your dentist in making an accurate diagnosis.
Diagnosing TMJ Disorders
An accurate diagnosis is the cornerstone of effective treatment for TMJ. Because TMD symptoms can overlap with other conditions (e.g., sinus infections, dental problems, neuralgias), a thorough diagnostic process is crucial.
Clinical Examination:
- Patient History: The dentist or oral surgeon will ask detailed questions about your symptoms, medical history, lifestyle habits (like stress, bruxism), and any relevant injuries.
- Palpation: The clinician will gently press on the jaw joints and surrounding muscles (masseter, temporalis, neck muscles) to identify areas of pain or tenderness.
- Range of Motion Assessment: You'll be asked to open and close your mouth, move your jaw side to side, and protrude it forward. The clinician will measure the maximum opening distance and observe for any deviations, clicking, popping, or locking.
- Auscultation: Listening to the jaw joints with a stethoscope (or simply by ear) to detect abnormal sounds during movement.
- Dental Evaluation: Examination of your bite, tooth wear patterns (suggesting bruxism), and any existing dental problems that could contribute to TMD.
Imaging Studies:
While a clinical exam is often sufficient for an initial diagnosis, imaging can provide more detailed information about the joint structures.
- Panoramic X-rays: Provide an overview of the jawbones and joints, helping to rule out other dental issues and spot gross skeletal abnormalities.
- Computed Tomography (CT) Scan: Offers detailed images of the bone structure of the joint, useful for identifying degenerative changes, fractures, or structural abnormalities.
- Magnetic Resonance Imaging (MRI): The gold standard for visualizing soft tissues, including the articular disc. An MRI can clearly show the position of the disc, any displacement, inflammation, or fluid accumulation within the joint, as well as muscle health. This is particularly useful for diagnosing internal derangements.
- Cone Beam CT (CBCT): A specialized type of CT scan that provides highly detailed 3D images of the teeth and jaw structures with less radiation than traditional CT.
Differential Diagnosis:
Given the broad range of TMD symptoms, the diagnostic process also involves ruling out other conditions that can cause similar pain or dysfunction, such as:
- Dental infections (abscesses)
- Sinusitis
- Trigeminal neuralgia
- Salivary gland disorders
- Ear infections
- Headaches of non-TMJ origin
Comprehensive Treatment Options for TMJ Disorders
The good news is that most TMJ disorders respond well to conservative, non-surgical approaches. The goal of treatment for TMJ is to reduce pain, restore normal jaw function, and prevent further damage. Treatment plans are highly individualized, depending on the specific type and severity of the disorder.
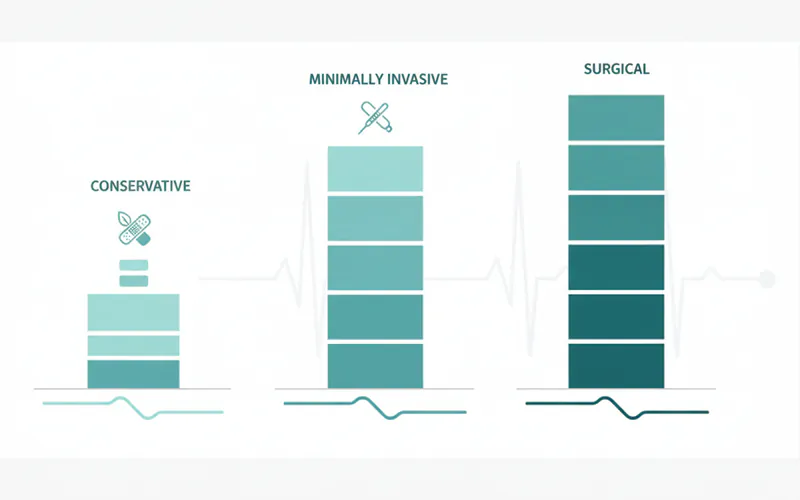
Conservative Treatments (First Line of Defense):
-
Self-Care and Home Remedies:
- Soft Diet: Avoid hard, chewy, or crunchy foods to reduce strain on the jaw.
- Moist Heat/Cold Packs: Apply heat to relax muscles and cold to reduce inflammation.
- Gentle Jaw Exercises: Your dentist or physical therapist may recommend specific stretches to improve jaw mobility and reduce stiffness.
- Avoid Extreme Jaw Movements: Limit wide yawns, excessive chewing gum, or clenching.
- Stress Management: Techniques like meditation, yoga, or deep breathing can help reduce muscle tension and bruxism.
- Over-the-Counter Medications: NSAIDs (e.g., ibuprofen, naproxen) can help manage pain and inflammation.
-
Medications (Prescription):
- Muscle Relaxants: To alleviate muscle spasms and pain.
- Anti-inflammatory Drugs: Stronger NSAIDs than OTC options.
- Tricyclic Antidepressants: Low doses can help control pain, promote sleep, and reduce bruxism, even without treating depression.
- Corticosteroids: Can be prescribed in short courses to reduce severe inflammation.
-
Oral Appliances (Splints or Nightguards):
- Occlusal Splints (Stabilization Splints): These custom-fitted acrylic guards are worn over the upper or lower teeth, often at night. They create a stable bite, protect teeth from grinding, and can help reposition the jaw or relax muscles. They do not permanently change your bite.
- Repositioning Splints: Designed to temporarily hold the jaw in a different position to encourage disc recapture or relieve joint pressure. These are used more cautiously and often for shorter durations.
- Pros: Non-invasive, reversible, often highly effective for myofascial pain and bruxism.
- Cons: Can be expensive, requires consistent wear, may need adjustments over time.
-
Physical Therapy:
- A physical therapist specializing in craniomandibular disorders can teach exercises for strengthening jaw muscles, improving posture, and increasing range of motion.
- Techniques may include massage, ultrasound, trigger point therapy, and electrical stimulation (TENS).
Advanced Treatments (Second Line, When Conservative Fails):
-
Injections:
- Botulinum Toxin (Botox) Injections: Injected into the jaw muscles (masseter, temporalis) to relax them, reduce muscle spasms, and alleviate pain caused by bruxism and myofascial TMD. Effects typically last 3-6 months.
- Corticosteroid Injections: Directly into the joint to reduce inflammation and pain, often used for arthritic conditions.
- Trigger Point Injections: Anesthetic is injected into specific "trigger points" in the muscles to relieve pain and muscle spasm.
- Pros: Minimally invasive, relatively quick relief.
- Cons: Temporary effects, potential side effects (bruising, swelling, muscle weakness).
-
Arthrocentesis:
- A minimally invasive procedure where needles are inserted into the joint to lavage (wash out) inflammatory byproducts and adhesions, and sometimes inject corticosteroids. It can improve disc mobility and reduce pain.
- Pros: Outpatient procedure, faster recovery than surgery.
- Cons: May require repeat treatments, not effective for severe structural issues.
-
Arthroscopy:
- A minimally invasive surgical procedure where a tiny camera (arthroscope) is inserted into the joint through small incisions. The surgeon can then visualize the joint, remove inflammatory tissue, reposition the disc, or perform other minor repairs.
- Pros: Less invasive than open surgery, faster recovery.
- Cons: Limited visibility and scope for complex repairs.
-
Open-Joint Surgery (Arthroplasty):
- Reserved for severe cases where conservative and minimally invasive treatments have failed, especially when there's significant structural damage, severe degeneration, or an inability to move the jaw.
- Procedures range from disc repair or removal to total joint replacement.
- Pros: Can address severe structural problems.
- Cons: Invasive, longer recovery, higher risks (infection, nerve damage, scarring), not always a guaranteed cure for pain.
-
Orthodontics and Restorative Dentistry:
- In some cases, if a significant malocclusion is identified as a contributing factor, orthodontic treatment (braces or aligners) or restorative procedures (crowns, bridges) may be recommended to correct the bite. This is typically done after initial pain and inflammation have been managed.
Pro Tip: Always start with the least invasive treatment for TMJ. Many patients find significant relief without needing advanced interventions. A multidisciplinary approach, involving your dentist, oral surgeon, physical therapist, and potentially a pain specialist, often yields the best results.
What to Expect: The Step-by-Step Treatment Process
Navigating treatment for TMJ can seem daunting, but understanding the typical progression can help set expectations and empower you throughout the process.
-
Initial Consultation and Diagnosis (Week 1-2):
- Your journey begins with a detailed examination by a dentist, oral surgeon, or TMJ specialist.
- They will review your symptoms, medical history, conduct a thorough clinical exam (palpation, range of motion, bite analysis), and potentially order imaging (X-rays, MRI).
- A precise diagnosis of the type of TMD (myofascial, internal derangement, arthritis) will be made.
-
Developing a Personalized Treatment Plan (Week 1-3):
- Based on your diagnosis, a tailored treatment plan will be created. This plan prioritizes conservative, reversible methods first.
- You'll discuss goals, potential outcomes, costs, and timelines.
- Pro Tip: Don't hesitate to ask questions about alternative treatments, success rates, and potential risks.
-
Initiating Conservative Therapies (Week 2 Onward):
- This often starts with self-care instructions (soft diet, moist heat, stress reduction) and over-the-counter pain relief.
- Prescription medications (muscle relaxants, NSAIDs) may be prescribed for immediate symptom management.
- If bruxism is a factor, an oral appliance (nightguard/splint) will be fabricated, which can take 1-2 weeks after impressions are taken.
- Referrals to a physical therapist specializing in craniomandibular disorders are common, with sessions typically beginning within a few weeks.
-
Monitoring and Adjustments (Weeks to Months):
- Regular follow-up appointments (e.g., every 2-4 weeks) will be scheduled to assess your progress.
- Your oral appliance may be adjusted to ensure proper fit and effectiveness.
- Medication dosages might be altered, or different medications introduced.
- Physical therapy exercises will progress as your condition improves.
- Many patients experience significant relief within 2-6 weeks of consistent conservative treatment.
-
Considering Advanced Treatments (If Conservative Fails - Months 3-6+):
- If conservative approaches do not provide sufficient relief after several months, your specialist might discuss more advanced options.
- This could include Botox injections, arthrocentesis, or, in rare and severe cases, surgical interventions like arthroscopy or open-joint surgery.
- Each advanced treatment has its own preparatory steps, procedure, and recovery timeline. For instance, arthrocentesis is typically an outpatient procedure with a few days of recovery, while open-joint surgery requires several weeks of initial recovery followed by months of rehabilitation.
-
Recovery and Long-Term Management (Ongoing):
- Even after symptoms improve, ongoing self-care, stress management, and possibly continued use of an oral appliance may be recommended to prevent recurrence.
- Regular dental check-ups are essential to monitor your jaw health.
This step-by-step process emphasizes a gradual, patient-centered approach, starting with the least invasive options and progressing only if necessary, ensuring your comfort and long-term well-being.
Recovery and Aftercare: Sustaining Jaw Health
Successful treatment for TMJ doesn't end when your symptoms subside. Long-term recovery and diligent aftercare are essential to maintain jaw health, prevent recurrence, and ensure lasting relief.
Post-Treatment Care Instructions:
-
Continue Self-Care Practices:
- Soft Diet: Even if your pain is gone, avoid excessively hard, chewy, or large foods. Cut food into small pieces.
- Heat/Cold Therapy: Use as needed for any residual stiffness or muscle soreness.
- Gentle Exercises: Continue with any prescribed jaw exercises or stretches to maintain flexibility and muscle strength.
- Posture Awareness: Maintain good posture, especially if you spend a lot of time at a computer. This helps align your head, neck, and jaw.
-
Consistent Oral Appliance Use:
- If you've been prescribed a nightguard or splint, wear it exactly as directed, even if you feel better. This is crucial for protecting your teeth, maintaining jaw position, and preventing clenching/grinding. Clean your appliance daily according to your dentist's instructions.
-
Stress Management Techniques:
- Stress is a major contributor to bruxism and muscle tension. Continue practicing stress-reduction techniques like meditation, yoga, mindfulness, or regular exercise. Consider professional counseling if stress is overwhelming.
-
Avoid Jaw-Straining Habits:
- Break habits like clenching your teeth, chewing gum, biting your nails, or resting your chin on your hand. Be mindful of how you hold your jaw during the day.
-
Regular Dental Follow-ups:
- Schedule regular check-ups with your dentist or TMJ specialist. They can monitor your jaw health, check your appliance, and address any new concerns promptly. Follow-up frequency might be initially every 1-3 months, then annually once stable.
-
Medication Management:
- If you were prescribed medications, follow your doctor's instructions for tapering off or continuing maintenance doses, as advised. Do not stop medications abruptly without medical guidance.
-
Physical Therapy Maintenance:
- If you underwent physical therapy, continue with the home exercise program provided by your therapist. These exercises are designed to support long-term muscle health and joint mobility.
Lifestyle Modifications for Long-Term Health:
- Ergonomics: Optimize your workspace to support good posture. Ensure your computer screen is at eye level and your chair provides adequate back support.
- Sleep Hygiene: Establish a regular sleep schedule and create a comfortable sleep environment. A supportive pillow can help maintain proper neck and head alignment, indirectly benefiting your jaw.
- Hydration: Staying well-hydrated is good for overall muscle function.
- Balanced Diet: A nutritious diet supports overall health and tissue repair.

By committing to these aftercare practices, you can significantly improve your chances of long-term relief from TMD symptoms and enjoy a healthy, functional jaw.
Preventing TMJ Disorders
While not all TMJ disorders are preventable, especially those stemming from acute trauma or certain systemic diseases, many common forms, particularly myofascial pain, can be mitigated through proactive measures.
-
Manage Stress Effectively: Stress is a primary trigger for teeth clenching and grinding. Incorporate stress-reduction techniques into your daily routine, such as:
- Mindfulness and meditation
- Deep breathing exercises
- Regular physical activity
- Sufficient sleep
- Hobbies and relaxation activities
- Professional counseling if needed.
-
Break Oral Habits: Be mindful of habits that strain your jaw:
- Avoid chewing gum excessively.
- Don't bite your nails, pen caps, or other hard objects.
- Avoid habitually resting your chin on your hand.
- Be aware of daytime clenching or grinding, and consciously relax your jaw.
-
Protect Your Teeth from Bruxism: If you're a known clencher or grinder (bruxer), especially at night, discuss an occlusal splint or nightguard with your dentist. This device can protect your teeth from wear and reduce the stress on your TMJs.
-
Maintain Good Posture: Poor posture, particularly a forward head posture, can lead to muscle imbalances and strain in the neck and jaw.
- Ensure your computer screen is at eye level.
- Use ergonomic chairs that support your back.
- Practice good standing and sitting posture throughout the day.
- Consider chiropractic care or physical therapy for posture correction if necessary.
-
Limit Extreme Jaw Movements:
- Avoid opening your mouth too wide, such as during excessive yawning or when biting into very large foods.
- Cut hard or chewy foods into smaller, manageable pieces.
-
Regular Dental Check-ups: Your dentist can spot early signs of bruxism, tooth wear, or changes in your bite that could indicate a developing TMD, allowing for early intervention.
-
Stay Hydrated and Eat a Balanced Diet: Good nutrition supports overall joint and muscle health, and adequate hydration can help maintain tissue elasticity.
By adopting these preventive strategies, you can significantly reduce your risk of developing TMJ disorders and promote long-term jaw health.
Risks and Complications of TMJ Treatments
While treatment for TMJ aims to relieve pain and restore function, like any medical intervention, there are potential risks and complications, particularly with more invasive procedures. Understanding these can help you make informed decisions with your dental professional.
Risks of Conservative Treatments (Generally Low):
- Oral Appliances (Splints/Nightguards):
- Temporary Discomfort: Initial soreness or changes in bite sensation as you adjust.
- Increased Salivation: Common at first, usually resolves.
- Speech Impediment: Temporary lisp, especially with lower splints.
- Bite Changes (rare, with long-term improper use): If an appliance is worn constantly for extended periods without proper adjustment, it can theoretically lead to subtle, undesirable bite changes. Adhering to professional guidance minimizes this risk.
- Medications: Side effects vary by medication (e.g., drowsiness with muscle relaxants, stomach upset with NSAIDs).
- Physical Therapy/Self-Care: Minimal risks, mostly temporary soreness from exercises if overdone.
Risks of Minimally Invasive Treatments:
- Injections (Botox, Corticosteroid, Trigger Point):
- Bruising and Swelling: At the injection site.
- Pain: Temporary discomfort during and after the injection.
- Infection: Rare, but possible at any injection site.
- Nerve Damage: Extremely rare, but possible if a nerve is inadvertently punctured.
- Muscle Weakness: With Botox, can temporarily affect adjacent muscles, leading to subtle changes in facial expression or chewing ability.
- Allergic Reaction: Rare.
- Arthrocentesis:
- Pain and Swelling: Post-procedure discomfort.
- Infection: Rare.
- Nerve Damage: Very rare, due to proximity of facial nerves.
- Bleeding: Minor bleeding is possible.
- Limited Success: May not fully resolve symptoms, especially in cases of severe disc displacement or degeneration.
Risks of Surgical Treatments (Higher and More Significant):
- Arthroscopy:
- Infection: Risk is higher than injections, though still low.
- Nerve Damage: Potential damage to the facial nerve (can lead to temporary or permanent facial weakness) or other nerves in the area.
- Bleeding.
- Scarring: Small scars from incisions.
- Limited Improvement: May not achieve complete pain relief or functional improvement.
- Recurrence: Symptoms may return over time.
- Open-Joint Surgery:
- Significant Pain and Swelling: More pronounced post-operative discomfort.
- Infection: Higher risk than arthroscopy.
- Nerve Damage: Increased risk of damage to the facial nerve (leading to facial weakness or paralysis), and other sensory nerves (leading to numbness).
- Scarring: More noticeable scarring.
- Bleeding and Hematoma formation.
- Adverse Reaction to Anesthesia.
- Failure to Relieve Pain: Even with successful surgery, some patients may still experience persistent pain.
- Stiffness or Restricted Jaw Movement: Due to scar tissue formation.
- Need for Revision Surgery: In some cases, initial surgery may not be successful, or complications may require additional procedures.
- Changes in Bite: Can occur, sometimes necessitating further dental work.
- Total Joint Replacement: Carries the most significant risks, similar to other major joint replacements, including implant failure and the need for future revision.
It is crucial to have a thorough discussion with your oral surgeon or dental specialist about the potential benefits, risks, and alternatives for any recommended treatment for TMJ, especially before considering surgical options.
Cost and Insurance: Navigating TMJ Treatment Expenses
Understanding the financial aspects of treatment for TMJ is crucial for patients in the US. Costs can vary significantly based on the severity of your condition, the types of treatments needed, your geographic location, and whether you have insurance coverage.
Average US Costs for TMJ Treatments (without insurance):
| Treatment Type | Average Cost Range (USD) | Notes |
|---|---|---|
| Initial Consultation/Diagnosis | $100 - $300 | Includes exam, sometimes initial X-rays. |
| Over-the-Counter Medications | $10 - $30/month | NSAIDs, pain relievers. |
| Prescription Medications | $30 - $200/month | Muscle relaxants, antidepressants; varies by drug and insurance. |
| Custom Oral Appliance (Nightguard/Splint) | $300 - $800 | Fabricated by dentist. Over-the-counter guards are cheaper but less effective. |
| Physical Therapy (per session) | $50 - $200 | Often requires multiple sessions (e.g., 6-12). |
| Botox Injections (per treatment) | $400 - $1,500 | Depends on number of units needed and practitioner fees. Typically every 3-6 months. |
| Corticosteroid/Trigger Point Injections | $150 - $500 | Per injection, sometimes multiple are needed. |
| Arthrocentesis | $1,000 - $3,000 | For one joint, may be more for both. |
| TMJ Arthroscopy | $5,000 - $15,000 | For one joint, includes surgeon, anesthesia, facility fees. |
| Open-Joint Surgery (Arthroplasty) | $10,000 - $25,000+ | For one joint, highly variable based on complexity, includes hospital stay. |
| TMJ Total Joint Replacement | $30,000 - $60,000+ | Extremely complex and rare, for one joint. |
Insurance Coverage Details:
Navigating insurance for TMD can be complex because it often straddles the line between medical and dental coverage.
- Medical Insurance: Most often, medical insurance will cover the diagnostic procedures (doctor visits, MRI scans, CT scans) and more invasive treatments like injections, physical therapy, and surgery, especially if deemed medically necessary and not primarily dental in nature. It's crucial to check your policy for "TMJ disorder" or "craniomandibular disorder" coverage, CPT codes, and pre-authorization requirements. Many medical plans consider TMJ treatments elective or experimental, particularly oral appliances, so clear communication with your insurer is essential.
- Dental Insurance: Typically covers procedures related to teeth and gums. While some dental plans may cover a portion of an oral appliance (nightguard) if it's preventative for bruxism, they are less likely to cover TMJ-specific medical treatments.
- Hybrid Coverage: Some treatments, like oral appliances, might have partial coverage under both medical and dental, requiring coordination of benefits.
Pro Tip: Always call your insurance provider directly to verify coverage for specific procedures using the CPT (Current Procedural Terminology) codes provided by your dental or medical office. Ask about deductibles, co-pays, and out-of-pocket maximums.
Payment Plans and Financing Options:
If insurance coverage is limited, or if you're facing high out-of-pocket costs, several options may be available:
- In-Office Payment Plans: Many dental and oral surgery offices offer interest-free payment plans, allowing you to pay for treatment in installments.
- Third-Party Medical Financing: Companies like CareCredit or LendingClub offer specialized healthcare credit cards with deferred interest options or low-interest payment plans.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): These tax-advantaged accounts allow you to save and pay for qualified medical expenses, including many TMJ treatments, with pre-tax dollars.
- Negotiate with Providers: In some cases, providers may offer a discount for upfront cash payments.
Cost-Saving Tips:
- Start Conservative: Most TMDs respond to less expensive, non-invasive treatments first. Avoid jumping to costly, irreversible procedures without trying conservative options.
- Shop Around (Carefully): Get quotes from different specialists, but prioritize expertise and experience over cost alone.
- Verify Insurance: Always confirm coverage beforehand.
- Preventive Care: Regular dental check-ups can help identify and address issues like bruxism early, potentially preventing more severe TMDs.
Children / Pediatric Considerations
While TMJ disorders are more commonly diagnosed in adults, they can affect children and adolescents. The presentation and management of TMD in younger patients have unique considerations.
Prevalence and Causes in Children:
- TMD symptoms in children are often underdiagnosed or misdiagnosed because children may have difficulty articulating their pain, or symptoms might be attributed to other conditions.
- Trauma: A common cause in children, often from falls, sports injuries, or even blows to the chin.
- Bruxism: Teeth grinding or clenching is very common in children, particularly during sleep, and can contribute to muscle pain and joint strain.
- Orthodontic Issues: While not a direct cause, severe malocclusions or certain orthodontic treatments (especially those involving prolonged mouth opening or specific appliances) can sometimes be a contributing factor or exacerbate existing TMJ issues. The role of orthodontics in causing or curing TMD is still debated, and the ADA advises against starting orthodontic treatment solely to prevent or treat TMD.
- Hypermobility: Children with generalized joint hypermobility (e.g., Ehlers-Danlos syndrome) may be more prone to TMJ instability.
- Developmental Anomalies: Rare congenital abnormalities of the jaw or TMJ can predispose a child to TMD.
- Juvenile Idiopathic Arthritis: This systemic inflammatory disease can affect the TMJs, leading to pain, stiffness, and potentially affecting jaw growth.
Signs and Symptoms in Children:
Symptoms in children can be similar to adults but might be less obvious:
- Difficulty Opening Mouth: Parents might notice a child struggling to eat larger foods or chew certain textures.
- Clicking or Popping Sounds: Often noticed by parents during eating.
- Facial Pain or Tenderness: The child might point to their ear or cheek area when asked about pain.
- Headaches: Frequent complaints of headaches, sometimes mistaken for migraines.
- Ear Pain: Often misdiagnosed as ear infections.
- Changes in Eating Habits: Avoiding certain foods or taking longer to eat.
- Asymmetrical Jaw Growth: In severe, chronic cases, especially with arthritis, one side of the jaw may grow differently, leading to facial asymmetry.
Treatment Approaches for Children:
Treatment for TMD in children typically follows conservative, reversible principles, with a strong emphasis on growth and development:
- Parental Education and Reassurance: Educating parents about the condition and reassuring them that most cases are manageable.
- Self-Care: Encouraging a soft diet, applying warm compresses, and teaching children to be aware of clenching habits.
- Behavior Modification: Helping children break habits like nail-biting, thumb-sucking (if still present), or pen-chewing.
- Oral Appliances: Custom-fitted nightguards may be used, but their design and long-term use must consider jaw growth.
- Physical Therapy: Gentle exercises to improve range of motion and reduce muscle tension.
- Medications: Over-the-counter pain relievers (like ibuprofen) are typically the first line for pain and inflammation. Prescription medications are used cautiously.
- Orthodontic Consultation: If malocclusion is severe, an orthodontist may be consulted, but treatment would be carefully coordinated with TMJ management.
- Monitoring Growth: For children, it's particularly important to monitor jaw growth and development, especially if there are signs of asymmetry or advanced joint degeneration.
Surgical interventions are extremely rare in children and are only considered in very severe cases of joint pathology that are unresponsive to all other treatments and are significantly impacting growth or function. The focus is always on supporting the child's natural growth and minimizing invasive procedures.
Frequently Asked Questions
What does TMJ pain feel like?
TMJ pain typically manifests as a dull, aching pain in the jaw joint area, often just in front of the ear. It can radiate into the face, temples, neck, and even cause severe earaches. The pain often intensifies with jaw movements like chewing, speaking, or yawning, and can be accompanied by muscle tenderness or stiffness.
Can TMJ go away on its own?
In some cases, mild TMJ symptoms, especially those caused by temporary stress or muscle strain, may resolve on their own with self-care like a soft diet, warm compresses, and stress reduction. However, chronic or severe symptoms, particularly those involving clicking, locking, or persistent pain, usually require professional intervention to prevent worsening and achieve lasting relief.
How long does TMJ treatment take?
The duration of TMJ treatment varies widely. Conservative treatments such as oral appliances, physical therapy, and medication often show significant improvement within 2-6 weeks. However, long-term management with an oral appliance or continued self-care might be necessary to prevent recurrence. More advanced treatments like injections have effects lasting 3-6 months, while surgical recovery can take several months.
Can TMJ cause ear pain only, without jaw pain?
Yes, it's very common for TMJ disorders to cause ear and jaw pain, and sometimes ear pain can be the predominant or even sole symptom. This referred pain is due to the close proximity of the TMJ to the ear canal and shared nerve pathways. Many patients initially consult an ENT specialist for ear pain before a TMJ disorder is identified as the true cause.
What is the best way to sleep with TMJ?
Sleeping on your back is generally recommended for TMJ sufferers as it helps maintain proper alignment of your head, neck, and jaw. If you prefer side sleeping, use a supportive pillow that keeps your head and neck aligned with your spine, avoiding placing direct pressure on your jaw joint. Try to avoid stomach sleeping, as it can twist your neck and strain your jaw.
Does insurance cover TMJ treatment?
Insurance coverage for TMJ treatment can be complex. Medical insurance typically covers diagnostic procedures (MRI, CT scans) and more invasive treatments (injections, surgery, physical therapy) if deemed medically necessary. Dental insurance might cover oral appliances (nightguards) for bruxism. It's crucial to contact your specific medical and dental insurance providers to understand your benefits, as coverage varies greatly by plan and specific procedure.
What specialist treats TMJ?
A variety of specialists can treat TMJ disorders. Your primary point of contact is usually your dentist, who can often manage mild to moderate cases. For more complex cases, you might be referred to an oral and maxillofacial surgeon, a TMJ specialist, a physical therapist specializing in craniomandibular disorders, or sometimes an orthodontist or pain management specialist.
Are there effective home remedies for TMJ pain relief?
Yes, several home remedies can provide significant relief for mild to moderate TMJ pain. These include applying moist heat or cold packs to the jaw, eating a soft diet to rest the jaw, performing gentle jaw stretches and massages, and practicing stress-reduction techniques like meditation or deep breathing. Over-the-counter pain relievers like ibuprofen can also help manage discomfort.
Can TMJ affect my bite?
Yes, TMJ disorders can definitely affect your bite. Inflammation, disc displacement, or muscle spasms within the joint can alter the way your upper and lower teeth meet, making your bite feel "off," uncomfortable, or unstable. In some severe cases, chronic TMD can even lead to changes in tooth wear patterns or jaw alignment over time.
Is TMJ treatment painful?
Most conservative TMJ treatments, such as oral appliances, physical therapy, and medications, are generally not painful. There might be some initial discomfort or adjustment period, but the goal is pain relief. More invasive treatments like injections might involve temporary pain at the injection site, and surgical procedures will naturally have post-operative pain managed with medication.
When to See a Dentist
Recognizing the signs that warrant professional attention for your jaw pain is vital. While occasional stiffness might resolve on its own, certain symptoms indicate it's time to consult a dentist or TMJ specialist.
You should schedule a non-emergency appointment if you experience:
- Persistent Jaw Pain: If your jaw pain, ear and jaw pain, or facial discomfort lasts for more than a few days and doesn't improve with self-care.
- Chronic Headaches: Especially if they are tension-type headaches centered around your temples or seem related to jaw movement.
- Regular Clicking, Popping, or Grating Sounds: If these sounds are consistent when you open or close your mouth, even if they're not always painful.
- Difficulty Chewing or Biting: If eating common foods becomes uncomfortable or challenging.
- Limited Jaw Opening: If you notice you can't open your mouth as wide as you used to, or if your jaw feels stiff in the mornings.
- Muscle Tenderness: If you frequently feel soreness or tenderness in your jaw muscles, temples, or neck.
- Changes in Your Bite: If your teeth suddenly feel like they don't fit together properly, or your bite feels "off."
You should seek immediate dental attention (potentially an emergency appointment) if you experience:
- Acute Jaw Locking: If your jaw locks completely in an open or closed position and you cannot move it back to normal without significant pain or manipulation. This can sometimes require immediate reduction.
- Severe, Debilitating Pain: If your jaw or facial pain is sudden, excruciating, and prevents you from eating, speaking, or sleeping.
- Sudden Swelling: Significant, unexplained swelling in your jaw or facial area.
- Inability to Open Your Mouth: If you suddenly find it nearly impossible to open your mouth at all.
Early diagnosis and treatment for TMJ are crucial to prevent the condition from worsening and to achieve the best possible long-term outcomes. Don't delay seeking professional advice if your jaw discomfort persists or significantly impacts your quality of life. Your healthy smile and comfortable jaw function are worth it.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Tmj Massage Near Me: Complete Guide
Temporomandibular joint disorder, commonly known as TMJD, affects millions of Americans, causing debilitating pain, discomfort, and significantly impacting quality of life. If you're experiencing jaw pain, clicking, or difficulty chewing, you're not alone. Up to 15% of American adults experience
February 23, 2026
Tmd Treatment: Complete Guide
Experiencing persistent jaw pain, clicking sounds when you chew, or debilitating headaches that seem to originate from your face? You're not alone. Temporomandibular joint (TMJ) disorders, often referred to collectively as TMD, affect an estimated 10 million Americans, with women disproportionat
February 23, 2026
Tmj Nerve Damage Symptoms: Complete Guide
Experiencing persistent facial pain, numbness, or tingling can be distressing, especially when the source is unclear. While many people are familiar with general jaw pain associated with temporomandibular joint (TMJ) disorders, the less commonly understood aspect of tmj nerve damage symptoms can
February 23, 2026
Remi Night Guard: Complete Guide
Remi Night Guard: Complete Guide
February 23, 2026