Tmj Surgery: Complete Guide
Key Takeaways
- TMJ Surgery: Complete Guide
TMJ Surgery: Complete Guide
Experiencing persistent jaw pain, clicking sounds, or difficulty chewing can be debilitating, affecting millions of Americans. Estimates suggest that over 10 million individuals in the United States suffer from temporomandibular joint (TMJ) disorders, often referred to as TMD. While many cases respond well to conservative treatments, for a significant subset of patients, structural damage or chronic dysfunction necessitates more advanced interventions, including TMJ surgery. Understanding the complexities of these procedures, from diagnosis to recovery, is crucial for anyone considering this path to relief. This comprehensive guide will demystify TMJ surgery, exploring its various types, indications, the step-by-step process, associated costs, potential risks, and what you can expect on your journey to improved jaw health.
Key Takeaways:
- TMJ surgery is considered only after conservative treatments for temporomandibular joint (TMJ) disorders have failed to provide adequate relief.
- Procedures range from minimally invasive (e.g., arthrocentesis, arthroscopy) to open-joint surgery and total joint replacement, chosen based on the severity and nature of the disorder.
- Arthrocentesis typically costs $1,000-$5,000, with recovery in days. Arthroscopy ranges from $5,000-$15,000, with recovery weeks. Open-joint surgery can be $15,000-$40,000, requiring months of recovery. Total joint replacement is the most complex, costing $30,000-$80,000+ per joint, with a recovery of 6-12 months.
- Most TMJ surgeries are covered by medical insurance rather than dental, but require prior authorization and often extensive documentation of failed conservative therapies.
- Recovery involves pain management, physical therapy, and a modified diet, crucial for successful outcomes and regaining jaw function.
- Potential risks include nerve damage, infection, persistent pain, and limited jaw motion.
- Consultation with an experienced oral and maxillofacial surgeon is essential to determine if surgery is the appropriate next step for your specific condition.
What It Is / Overview
The temporomandibular joint (TMJ) is a complex hinge joint that connects your jawbone (mandible) to your skull (temporal bone). You have two TMJs, one on each side of your jaw. These joints, along with surrounding muscles, ligaments, and a small disc that acts as a shock absorber, enable you to move your jaw up and down, side to side, and forward and back, allowing for essential functions like chewing, speaking, and yawning.

Temporomandibular joint (TMJ) disorders (TMD) refer to a group of conditions that cause pain and dysfunction in the jaw joint and the muscles that control jaw movement. When conservative treatments—such as medication, physical therapy, oral appliances, and lifestyle modifications—fail to alleviate severe, chronic pain or correct significant structural problems, TMJ surgery may become a necessary consideration.
TMJ surgery encompasses a range of procedures designed to repair, realign, or replace parts of the temporomandibular joint. The goal is to reduce pain, restore normal jaw function, and improve your overall quality of life. The decision to pursue surgery is always made after careful diagnosis and evaluation by an oral and maxillofacial surgeon or a TMJ specialist, considering the specific nature of your disorder and the impact it has on your daily activities. It's an intervention reserved for those whose conditions are severe, persistent, and unresponsive to less invasive approaches.
Types / Variations of TMJ Surgery
The type of TMJ surgery recommended depends heavily on the specific diagnosis, the severity of the condition, and the extent of damage to the joint. Procedures range from minimally invasive arthrocentesis to extensive open-joint reconstruction or total joint replacement.
Arthrocentesis
What it is: Arthrocentesis is the least invasive surgical procedure for the TMJ. It involves flushing the joint with a sterile solution (saline or Ringer's lactate) using two small needles. Procedure: Under local anesthesia, sometimes with light sedation, two small needles are inserted into the joint space. One needle infuses the fluid, while the other drains it, washing out inflammatory byproducts and potentially releasing a "stuck" disc by reducing negative pressure within the joint. Sometimes, a corticosteroid or hyaluronic acid may be injected after lavage to further reduce inflammation and improve lubrication. Indications: Primarily used for acute closed lock (inability to open the mouth fully due to disc displacement without reduction), recent onset of pain, and limited jaw opening caused by inflammation or adhesions. Benefits: Minimally invasive, quick recovery, relatively low risk, often provides rapid relief from pain and improves jaw mobility. Recovery: Typically a few days to a week. Patients can usually resume normal activities quickly. Cost: Generally ranges from $1,000 to $5,000 in the US, depending on facility and anesthesia.
Arthroscopy
What it is: TMJ arthroscopy is a minimally invasive surgical procedure that allows a surgeon to visualize and operate within the joint using a small camera (arthroscope) and specialized instruments. Procedure: Under general anesthesia, a small incision (typically less than half an inch) is made in front of the ear. The arthroscope is inserted, providing a magnified view of the joint structures on a monitor. The surgeon can then perform diagnostic examination, lavage (flushing), removal of adhesions, reshaping of bone spurs, or even repositioning of the articular disc using small instruments. Indications: Chronic pain, persistent locking, internal derangement (disc displacement with reduction that causes significant symptoms, or without reduction that causes limited opening), chronic inflammation, and sometimes for diagnostic purposes when other imaging is inconclusive. Benefits: Less invasive than open-joint surgery, smaller scars, reduced pain and swelling post-operatively, faster recovery compared to open procedures. Recovery: Typically a few weeks for initial recovery, with full recovery taking a couple of months. Physical therapy is often initiated shortly after surgery. Cost: Ranges from $5,000 to $15,000 in the US, depending on the complexity of the procedure, facility fees, and surgeon's fees.
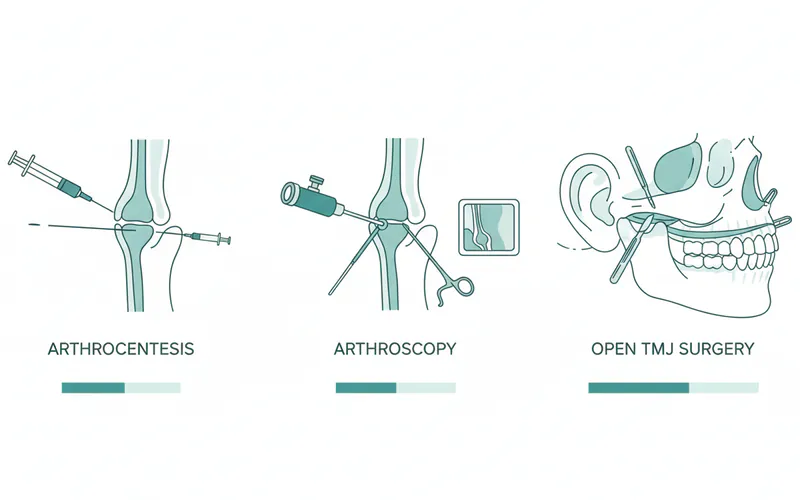
Arthroplasty (Open Joint Surgery)
What it is: Arthroplasty refers to a range of open-joint surgical procedures where the surgeon makes a larger incision to directly access and visualize the TMJ. This allows for more extensive repair or reconstruction. Procedure: Performed under general anesthesia, an incision is made, usually extending from in front of the ear down into the neck or along the hairline, to expose the joint. The specific procedure then depends on the underlying problem:
- Discectomy/Disc Repositioning: If the articular disc is severely damaged, displaced, or perforated, it may be repaired, repositioned (using sutures or anchors), or removed (discectomy). If removed, sometimes an autogenous graft (from your own body) or a synthetic implant may be placed.
- Condylectomy/Condylotomy: In cases of severe condylar hyperplasia (overgrowth of the condyle) or ankylosis (fusion of the joint), a portion of the condyle may be removed (condylectomy) or reshaped (condylotomy) to restore proper movement.
- Eminence Repositioning: For recurrent TMJ dislocation (when the jaw pops out of its socket frequently), the bony prominence (articular eminence) can be reshaped or augmented to prevent the condyle from dislocating.
- Osteotomy: Reshaping of the jaw bone to correct significant structural issues that affect TMJ function. Indications: Severe internal derangement unresponsive to less invasive methods, extensive disc damage, degenerative joint disease, ankylosis, tumors, fractures, and recurrent dislocations. Benefits: Allows for direct visualization and comprehensive repair of complex joint issues. Risks: More invasive, longer recovery, potential for facial nerve damage (leading to temporary or permanent facial weakness), more scarring, increased risk of infection and bleeding. Recovery: Can take several months for full recovery. Intensive physical therapy is crucial. Diet restrictions are significant initially. Cost: Open-joint surgeries are more expensive, typically ranging from $15,000 to $40,000 in the US, depending on the specific procedure and its complexity.
Total Joint Replacement
What it is: Total joint replacement is the most extensive TMJ surgery, involving the removal of the damaged parts of the joint (condyle and fossa) and replacing them with a custom or stock prosthetic device. Procedure: Performed under general anesthesia, an open incision is made. The surgeon removes the damaged condyle and part of the temporal bone (fossa) and replaces them with an artificial joint made of biocompatible materials (e.g., titanium, cobalt-chromium, polyethylene). These prostheses are designed to mimic the natural joint movement. Indications: Severe degenerative joint disease (e.g., osteoarthritis, rheumatoid arthritis) causing irreversible damage, ankylosis (complete fusion of the joint), failed previous TMJ surgeries, trauma leading to irreparable damage, or tumors affecting the joint. Benefits: Can provide significant pain relief and restore function in severely damaged joints, particularly when other treatments have failed. Risks: Major surgery with all associated risks, including infection, nerve damage, hardware failure, and the need for revision surgery in the future. Long-term outcomes vary. Recovery: The longest recovery period, often 6-12 months, involving extensive physical therapy and diet modification. Cost: The most expensive TMJ surgery, ranging from $30,000 to $80,000 or more per joint in the US, depending on whether it's a stock or custom prosthesis, facility, and surgeon.
Causes / Why TMJ Disorders Happen
TMJ disorders are often multifactorial, meaning they arise from a combination of causes rather than a single event. When these factors lead to severe or chronic structural damage, surgery may become necessary.
- Trauma: A direct blow to the jaw, head, or neck (e.g., from an accident or sports injury) can damage the joint structures, including the disc, ligaments, or bones. Whiplash injuries can also contribute.
- Arthritis:
- Osteoarthritis: Degenerative joint disease, often related to aging or overuse, which breaks down the cartilage and bone within the joint.
- Rheumatoid Arthritis: An autoimmune disease that can attack the TMJ, causing inflammation and destruction of joint tissues.
- Psoriatic Arthritis, Gout: Other forms of inflammatory arthritis can also affect the TMJ.
- Disc Displacement: The articular disc within the TMJ can become displaced, either with reduction (it clicks back into place) or without reduction (it stays displaced, leading to locking and limited movement). Chronic displacement without reduction often leads to degenerative changes.
- Bruxism and Clenching: While not a direct cause of TMJ structural damage, chronic teeth grinding (bruxism) or clenching puts excessive stress on the joint and surrounding muscles, accelerating wear and tear on the disc and joint surfaces, and exacerbating existing problems.
- Anatomical Abnormalities/Developmental Issues: Congenital malformations, hypoplasia (underdevelopment), or hyperplasia (overdevelopment) of the condyle or other joint structures can lead to chronic dysfunction.
- Infections: Although rare, infections in or around the TMJ can lead to inflammation and damage.
- Tumors: Benign or malignant growths within or near the TMJ can affect its structure and function.
- Connective Tissue Diseases: Conditions like Ehlers-Danlos syndrome can lead to joint hypermobility and instability.
Signs and Symptoms
Recognizing the signs and symptoms of TMJ disorders is the first step towards seeking appropriate treatment. If these symptoms are severe, persistent, and unresponsive to conservative care, they may indicate a need for surgical evaluation.
- Pain: The most common symptom. It can manifest as:
- Jaw pain or tenderness, often worse with chewing or jaw movement.
- Facial pain, extending to the cheeks, temples, or around the eyes.
- Earache or pain around the ear, often mistaken for an ear infection.
- Headaches, particularly tension-type headaches or migraines.
- Neck and shoulder pain.
- Joint Sounds:
- Clicking or popping sounds when opening or closing your mouth. These are common and not always indicative of a problem unless accompanied by pain or limitation.
- Grating or grinding sounds (crepitus), which often suggest degenerative changes within the joint.
- Limited Jaw Movement:
- Difficulty or pain when opening your mouth wide.
- "Locking" of the jaw, where it gets stuck in an open or closed position.
- Stiffness in the jaw muscles, especially in the morning.
- Changes in Bite: A feeling that your upper and lower teeth don't fit together properly.
- Swelling: Swelling on the side of your face around the TMJ.
- Associated Symptoms: Less common but sometimes reported symptoms include tinnitus (ringing in the ears), dizziness, hearing changes, and even tooth sensitivity (though this usually points to other dental issues).
Treatment Options
The journey to TMJ relief typically begins with the least invasive treatments. Surgery is reserved for cases where these conservative approaches have failed or when there is severe structural damage.
Conservative/Non-Surgical Treatments (First Line of Defense)
Before considering any surgical intervention, your dentist or TMJ specialist will exhaust a range of non-surgical options.
- Rest and Lifestyle Modifications: Avoiding hard, chewy, or sticky foods; cutting food into small pieces; avoiding extreme jaw movements (wide yawning, yelling); applying moist heat or ice packs to the jaw.
- Physical Therapy: Jaw exercises to stretch and strengthen muscles, improve range of motion, and reduce muscle spasms. Techniques like massage, ultrasound, and trigger point therapy may also be used.
- Oral Appliances (Splints/Nightguards): Custom-made devices worn over the teeth, typically at night, to reduce the effects of clenching or grinding, reposition the jaw, or provide a protective barrier.
- Medication (Temporomandibular Joint Dysfunction Medication):
- Over-the-counter Pain Relievers: NSAIDs like ibuprofen or naproxen for pain and inflammation.
- Prescription NSAIDs: Stronger anti-inflammatory drugs.
- Muscle Relaxants: To alleviate muscle spasms and tightness.
- Corticosteroids: Oral steroids or direct injections into the joint to reduce severe inflammation.
- Tricyclic Antidepressants: Low doses, often prescribed at bedtime, can help control pain, relax muscles, and improve sleep for chronic pain sufferers.
- Botulinum Toxin (Botox) Injections: Can be injected into jaw muscles to reduce muscle spasms and pain, though this is considered off-label for TMJ by the FDA.
- Stress Management: Techniques like meditation, yoga, or counseling can help reduce jaw clenching and grinding exacerbated by stress.
Pro Tip: Always pursue and rigorously follow conservative treatment plans for several months before considering surgery. Documenting the failure of these treatments is often a requirement for insurance coverage of surgical procedures.
When is Surgery Indicated?
TMJ surgery is typically considered only when:
- Conservative treatments have been thoroughly attempted for a significant period (e.g., 6-12 months) and have failed to provide lasting relief from pain or dysfunction.
- There is clear diagnostic evidence (from MRI, CT scans, or clinical examination) of significant structural damage within the joint, such as severe disc displacement, degeneration, ankylosis, or fractures, that cannot be resolved non-surgically.
- The patient experiences chronic, debilitating pain or severely limited jaw function that significantly impairs quality of life.
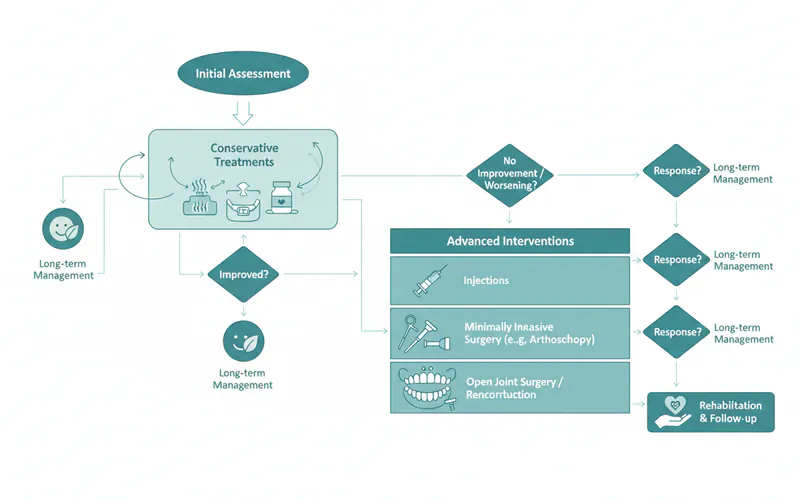
Step-by-Step Process
Undergoing TMJ surgery is a multi-stage process, from initial evaluation to long-term follow-up.
1. Initial Consultation and Diagnosis
- Comprehensive Examination: Your journey begins with a thorough dental and medical history, physical examination of your jaw, neck, and facial muscles, and assessment of your bite and jaw movement.
- Imaging Studies: To confirm the diagnosis and assess the extent of joint damage, your specialist may order:
- X-rays: To view the bony structures.
- MRI (Magnetic Resonance Imaging): The gold standard for visualizing soft tissues, especially the articular disc, ligaments, and fluid within the joint.
- CT Scan (Computed Tomography): Provides detailed images of the bone structure, useful for evaluating degenerative changes, fractures, or ankylosis.
- Discussion of Options: The surgeon will discuss all available treatment options, including non-surgical alternatives you may not have fully explored, and explain the recommended surgical procedure in detail, including its benefits, risks, and expected outcomes.
2. Pre-Surgical Evaluations
- Medical Clearance: You will undergo a complete medical evaluation, including blood tests, EKG, and potentially other diagnostic tests, to ensure you are healthy enough for surgery and general anesthesia.
- Anesthesia Consultation: You'll meet with the anesthesiologist to discuss the type of anesthesia (local with sedation or general anesthesia) and any associated risks.
- Informed Consent: You will sign consent forms after thoroughly understanding the procedure, potential risks, benefits, and alternatives. This is your opportunity to ask any remaining questions.
- Medication Review: You'll receive instructions on which medications to stop before surgery (e.g., blood thinners) and which to continue.
3. The Surgical Procedure
- Hospital or Outpatient Facility: Depending on the complexity, the surgery may be performed in a hospital setting or an accredited outpatient surgical center.
- Anesthesia Administration: You will receive the agreed-upon anesthesia.
- Procedure Execution: The surgeon will perform the specific TMJ surgery as planned (arthrocentesis, arthroscopy, open-joint procedure, or total joint replacement). The duration varies significantly by procedure, from under an hour for arthrocentesis to several hours for complex open-joint or replacement surgeries.
4. Immediate Post-Operative Recovery
- Recovery Room: After surgery, you will be monitored in a recovery room as you wake from anesthesia.
- Pain Management: Pain medication will be administered to manage post-surgical discomfort.
- Swelling and Nausea: You may experience swelling, bruising, and potentially nausea. Ice packs and anti-nausea medication will be provided as needed.
- Discharge Instructions: You'll receive detailed instructions on wound care, medication, diet, activity restrictions, and signs of complications. You'll need someone to drive you home.
5. Post-Operative Follow-up and Rehabilitation
- Follow-up Appointments: Scheduled visits with your surgeon to monitor healing, remove sutures (if applicable), and assess your progress.
- Physical Therapy: Crucial for regaining jaw mobility and strength. This often starts very soon after surgery, with specific exercises to prevent stiffness and improve function.
- Diet Progression: You will typically start with a liquid or soft diet and gradually progress to a more regular diet as healing permits.
- Long-Term Management: Adherence to rehabilitation exercises and lifestyle modifications is essential for the long-term success of the surgery.
Pro Tip: Active participation in your rehabilitation, especially physical therapy, is paramount to achieving the best possible outcome from TMJ surgery. Skipping exercises can lead to stiffness and poor functional recovery.
Cost and Insurance
The cost of TMJ surgery in the US can vary significantly based on the type of procedure, the surgeon's fees, anesthesia costs, facility fees, and geographic location. Understanding these costs and your insurance coverage is vital.

Average US Cost Ranges (Without Insurance)
| TMJ Surgery Type | Average Cost Range (USD) |
|---|---|
| Arthrocentesis | $1,000 - $5,000 |
| Arthroscopy | $5,000 - $15,000 |
| Open Joint Surgery | $15,000 - $40,000 |
| Total Joint Replacement | $30,000 - $80,000+ |
Factors Influencing Cost:
- Surgeon's Fees: Varies based on experience, reputation, and geographic location.
- Anesthesia Fees: Depends on the type of anesthesia and duration of the surgery.
- Facility Fees: Cost of using the hospital or outpatient surgical center. This can include operating room time, nursing care, and supplies.
- Pre- and Post-Operative Care: Imaging, consultations, medications, and physical therapy sessions.
- Implant Costs: For total joint replacement, the cost of the prosthetic joint significantly impacts the total.
Insurance Coverage
This is a critical area for TMJ surgery.
- Medical vs. Dental Insurance: While TMJ disorders affect the jaw, most surgical procedures for TMJ are considered medical rather than dental procedures. This means your health insurance plan is more likely to provide coverage.
- Prior Authorization: Almost all TMJ surgeries require extensive prior authorization from your medical insurance company. This process can be lengthy and requires detailed documentation from your treating physicians, including:
- Evidence of a clear diagnosis (e.g., MRI reports).
- Documentation of severe symptoms and functional impairment.
- Proof of failed conservative treatments (e.g., physical therapy notes, medication trials, oral appliance therapy). Many insurance companies require at least 6-12 months of documented conservative treatment failure before approving surgery.
- In-Network vs. Out-of-Network: Your out-of-pocket costs will be significantly lower if your surgeon and surgical facility are in your insurance plan's network.
- Deductibles, Co-pays, Co-insurance: Even with insurance, you will be responsible for your plan's deductible, co-pays, and co-insurance percentages until you reach your out-of-pocket maximum. These can still amount to several thousand dollars.
Pro Tip: Before committing to surgery, contact your medical insurance provider directly. Understand your benefits, specifically for TMJ disorders, and clarify what documentation is required for pre-authorization. Your surgeon's office often has a dedicated team to help with this process.
Recovery and Aftercare
Recovery from TMJ surgery varies significantly depending on the invasiveness of the procedure. Adhering to post-operative instructions is critical for a successful outcome.
Immediate Post-Operative Period (First few days to weeks)
- Pain Management: You will be prescribed pain medication (opioids initially, transitioning to NSAIDs) to manage discomfort. Follow dosing instructions carefully.
- Swelling and Bruising: Expect swelling and possibly bruising around the jaw and temple area. Apply ice packs intermittently (20 minutes on, 20 minutes off) for the first 48-72 hours. Elevating your head, even while sleeping, can help reduce swelling.
- Diet: You will start with a liquid or very soft diet immediately after surgery. This is crucial to allow the joint to heal without strain. Gradually, you will progress to pureed foods, then soft solids, over several weeks or even months, depending on the surgery type. Avoid chewing hard, sticky, or chewy foods for an extended period.
- Oral Hygiene: Gentle oral hygiene is vital to prevent infection. You may be given a special rinse or instructed on how to carefully brush your teeth without disturbing the surgical site.
- Activity Restrictions: Avoid strenuous activity, heavy lifting, or anything that could jar your jaw. You'll typically be advised to rest and limit jaw movement to talking softly and swallowing.
Rehabilitation and Physical Therapy (Weeks to Months)
- Jaw Exercises: This is arguably the most crucial part of recovery, especially for more invasive surgeries. A physical therapist specializing in craniomandibular disorders will guide you through gentle jaw exercises designed to:
- Increase range of motion (opening and closing your mouth).
- Improve jaw muscle strength and coordination.
- Reduce stiffness and prevent scar tissue formation.
- These exercises must be done consistently and correctly to prevent re-ankylosis (fusion) or persistent stiffness.
- Heat Therapy: Applying moist heat before exercises can help relax muscles and improve flexibility.
- Manual Therapy: Your physical therapist may use techniques to gently mobilize the joint and surrounding tissues.
- Splint Therapy: In some cases, a post-operative splint may be used to stabilize the jaw or maintain disc position during healing.
Long-Term Management and Expectations
- Follow-up Care: Regular follow-up appointments with your surgeon are essential to monitor healing, assess progress, and adjust your rehabilitation plan.
- Lifestyle Modifications: Continue to avoid habits that stress the TMJ, such as excessive gum chewing, nail biting, or leaning on your jaw.
- Stress Reduction: Manage stress to reduce clenching and grinding.
- Dietary Awareness: Be mindful of your diet, especially avoiding foods that require excessive chewing.
- Realistic Expectations: While TMJ surgery can significantly improve pain and function, it may not provide a complete cure, and some patients may experience residual symptoms. The goal is significant improvement and enhanced quality of life. Success rates vary depending on the procedure and individual patient factors. For instance, arthroscopy typically has a success rate of 70-85% for pain reduction and improved function, while total joint replacement boasts success rates for pain relief often above 90% after 5 years, though functional recovery can be more variable.
Prevention
While not all TMJ disorders can be prevented, particularly those caused by trauma or systemic diseases, you can significantly reduce your risk of developing severe TMD that might necessitate surgery.
- Address Bruxism/Clenching: If you grind or clench your teeth (especially at night), wear a custom-fitted nightguard (occlusal splint) prescribed by your dentist.
- Practice Good Posture: Poor posture, especially forward head posture, can strain jaw and neck muscles. Maintain good alignment of your head, neck, and shoulders.
- Manage Stress: Stress is a major contributor to jaw tension, clenching, and grinding. Incorporate stress-reduction techniques like meditation, yoga, deep breathing exercises, or regular exercise into your routine.
- Avoid Excessive Jaw Movements: Try not to open your mouth too wide when yawning or eating. Avoid chewing gum frequently, eating very hard or chewy foods, and nail-biting.
- Maintain Proper Bite: Regular dental check-ups can ensure your bite is stable. Addressing malocclusion (improper bite) with orthodontic treatment or restorative dentistry may help in some cases.
- Protect Your Jaw from Trauma: Wear appropriate protective gear during contact sports.
- Seek Early Intervention: If you experience early symptoms of TMJ pain or dysfunction, consult your dentist or a TMJ specialist promptly. Early diagnosis and conservative treatment can often prevent the progression to more severe conditions requiring surgery.
Risks and Complications
Like any surgical procedure, TMJ surgery carries potential risks and complications. It's crucial to discuss these thoroughly with your surgeon before making a decision.
General Surgical Risks:
- Infection: Though precautions are taken, any surgical site can become infected.
- Bleeding: Excessive bleeding during or after surgery.
- Anesthesia Complications: Adverse reactions to anesthesia, ranging from nausea to more severe respiratory or cardiac issues.
- Pain: Persistent or new pain in the surgical area.
- Scarring: Visible scarring at the incision site, especially with open-joint procedures.
Specific TMJ Surgical Risks:
- Facial Nerve Damage: The facial nerve (cranial nerve VII) runs close to the TMJ. Damage to this nerve, especially during open-joint surgery, can lead to temporary or permanent facial weakness, asymmetry, or paralysis. This is a significant concern for many patients.
- Damage to Adjacent Structures: Injury to blood vessels, ear structures (leading to hearing changes or tinnitus), or salivary glands.
- Joint Stiffness (Fibrosis/Ankylosis): Despite physical therapy, some patients may develop excessive scar tissue, leading to limited jaw opening and persistent stiffness. In rare, severe cases, the joint can fuse (ankylosis), requiring further surgery.
- Persistent Pain or Dysfunction: The surgery may not fully alleviate pain or restore normal function. In some cases, the condition may recur or worsen.
- Malocclusion (Bite Changes): Surgery can sometimes alter the way your teeth fit together, requiring subsequent orthodontic or restorative dental work.
- Hardware Failure (for Joint Replacements): Prosthetic joints can wear out, loosen, fracture, or become infected over time, necessitating revision surgery.
- Auriculotemporal Nerve Syndrome (Frey's Syndrome): A rare complication where nerve damage leads to sweating and flushing of the skin near the ear when eating or anticipating food.
Pro Tip: Choose a board-certified oral and maxillofacial surgeon with extensive experience in TMJ disorders and the specific surgical procedure you are considering. Their expertise can significantly mitigate risks.
Comparison Tables
To help visualize the differences between TMJ surgical options and the overall treatment landscape, here are two comparison tables.
Table 1: Comparison of TMJ Surgical Procedures
| Feature | Arthrocentesis | Arthroscopy | Open Joint Surgery | Total Joint Replacement |
|---|---|---|---|---|
| Invasiveness | Minimally Invasive | Minimally Invasive | Invasive (Major Surgery) | Very Invasive (Major Surgery) |
| Procedure | Joint lavage (flushing), injection | Diagnostic & therapeutic (scope, tools) | Direct access for repair/resection | Remove/replace joint with prosthesis |
| Anesthesia | Local with sedation | General | General | General |
| Indications | Acute closed lock, inflammation | Chronic pain, locking, internal derangement | Severe disc damage, ankylosis, trauma, tumors, degeneration | End-stage degeneration, ankylosis, failed surgeries |
| Recovery Time | Days to 1 week | Weeks (initial), 1-2 months (full) | 2-6 months (initial), up to 1 year (full) | 6-12 months or longer |
| Avg. Cost (US) | $1,000 - $5,000 | $5,000 - $15,000 | $15,000 - $40,000 | $30,000 - $80,000+ per joint |
| Success Rate | High for acute conditions (e.g., 70-80% relief for acute lock) | 70-85% for pain and function improvements | Varies widely by specific procedure and patient condition | 90%+ for pain relief; functional outcomes vary |
Table 2: Conservative vs. Surgical TMJ Treatments
| Feature | Conservative/Non-Surgical Treatments | Surgical Treatments |
|---|---|---|
| Approach | Non-invasive, reversible, focuses on symptom management and healing | Invasive, irreversible in many cases, focuses on structural repair/replacement |
| Goal | Reduce pain, inflammation, muscle spasms; improve function | Eliminate severe pain, restore function, correct structural defects |
| Invasiveness | None to minor (injections) | Ranges from minimally invasive to major surgery |
| Cost Range (US) | $100 - $5,000+ (depending on therapies, appliances, medications, injections) | $1,000 - $80,000+ per joint (depending on procedure) |
| Recovery | Ongoing management, often no downtime | Days to over a year, with significant rehabilitation |
| Risks | Minimal (e.g., medication side effects, appliance discomfort) | General surgical risks + specific TMJ risks (e.g., nerve damage) |
| Efficacy | Effective for majority of TMD cases, especially early stages | Reserved for severe, intractable cases; high success for selected patients |
Children / Pediatric Considerations
TMJ disorders can affect children and adolescents, though they are often less common than in adults. The approach to diagnosis and treatment in pediatric patients requires special considerations due to their ongoing growth and development.
- Prevalence: While less common, the incidence of TMD in children and adolescents is increasing, possibly due to factors like increased stress, bruxism, and sports injuries.
- Diagnosis: Diagnosing TMD in children can be challenging as they may not articulate symptoms as clearly as adults. Parents should look for signs like jaw clicking, difficulty eating, recurrent headaches, or changes in how the teeth fit together. Imaging, especially MRI, is used cautiously to limit radiation exposure.
- Conservative Approach is Paramount: For children, the emphasis is almost always on conservative management first. This includes:
- Education and counseling for both the child and parents regarding jaw habits and soft diet.
- Physical therapy with gentle exercises.
- Oral appliances (splints) carefully designed to accommodate growth.
- Medication (NSAIDs) for pain and inflammation, with careful dosing.
- Stress management techniques.
- When Surgery Might Be Considered: TMJ surgery in children is a rare and last resort, typically reserved for:
- Congenital deformities: Such as severe condylar aplasia (underdevelopment) or hyperplasia (overgrowth) that significantly impact facial development and function.
- Severe trauma: Leading to fractures or displacement that cannot be reduced non-surgically.
- Ankylosis: Fusion of the joint, which can severely restrict jaw growth and function, often requiring surgical release (gap arthroplasty) and aggressive physical therapy.
- Tumors: Rare cases of growths affecting the TMJ.
- Growth Considerations: Any surgical intervention must account for the child's remaining growth potential. Procedures that alter bone structure can impact facial development. For example, if a total joint replacement is needed, a pediatric-specific or custom-designed prosthesis that can accommodate growth or be replaced later may be necessary.
- Specialist Referral: Children with suspected or diagnosed TMJ disorders should be evaluated by a pediatric dentist, orthodontist, or an oral and maxillofacial surgeon with expertise in pediatric TMJ conditions.
Cost Breakdown
As discussed in the main content, the costs of TMJ surgery vary widely. Here's a summary of the breakdown for US patients.
Average US Costs (Low, Mid, High Estimates)
- Arthrocentesis:
- Low: $1,000 (simple, in-office, local anesthesia)
- Mid: $2,500 (outpatient clinic, light sedation)
- High: $5,000 (hospital setting, general anesthesia)
- Arthroscopy:
- Low: $5,000 (simple diagnostic, outpatient)
- Mid: $10,000 (therapeutic, outpatient)
- High: $15,000 (complex therapeutic, hospital)
- Open Joint Surgery:
- Low: $15,000 (simple disc repair/repositioning)
- Mid: $25,000 (more extensive reconstruction)
- High: $40,000+ (complex procedures, long hospital stay)
- Total Joint Replacement (per joint):
- Low: $30,000 (stock prosthesis, single joint)
- Mid: $50,000 (custom prosthesis, single joint)
- High: $80,000+ (bilateral replacement, complex case, extended hospital stay)
These figures generally include surgeon's fees, anesthesia, and facility charges. They typically do not include pre-operative diagnostics (MRI, CT scans, consultations), post-operative medications, or long-term physical therapy, which can add several thousands of dollars to the total.
With vs. Without Insurance
- Without Insurance (Self-Pay): You will be responsible for 100% of the costs. Some providers may offer a discount for upfront cash payment.
- With Insurance (Medical Insurance):
- After meeting your deductible (which could be anywhere from $500 to $10,000+), your insurance will typically cover a percentage of the remaining cost (e.g., 80%), with you paying the co-insurance (e.g., 20%).
- You will also likely have co-pays for office visits and prescriptions.
- Your financial liability will be capped at your plan's out-of-pocket maximum (often $3,000 to $9,000+ for individuals, higher for families). Once this is met, insurance covers 100% of in-network costs for the remainder of the policy year.

Payment Plans and Financing Options
- Medical Financing Companies: Companies like CareCredit or Alphaeon Credit offer specialized credit lines for healthcare expenses, often with promotional interest-free periods if the balance is paid within a set timeframe.
- In-Office Payment Plans: Some oral surgery practices may offer their own interest-free payment plans for a portion of the cost, especially for the patient's out-of-pocket share.
- Personal Loans: Banks or credit unions may offer personal loans for larger medical expenses.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): If you have an HSA or FSA, you can use pre-tax dollars to pay for qualified medical expenses, including TMJ surgery, which can lead to significant tax savings.
Cost-Saving Tips
- Compare Providers: Get quotes from several qualified surgeons and facilities. Costs can vary significantly even within the same geographic area.
- Understand Your Insurance: Know your plan's specifics for TMJ treatment, including deductibles, co-pays, co-insurance, and your out-of-pocket maximum.
- Verify Network Status: Ensure all providers (surgeon, anesthesiologist, facility) are in-network to avoid higher out-of-pocket costs.
- Ask for Itemized Bills: Review your bills carefully for accuracy and challenge any charges you don't understand.
- Negotiate Cash Prices: If you are uninsured or facing high out-of-pocket costs, ask about cash payment discounts or negotiate prices before the procedure.
Frequently Asked Questions
Is TMJ surgery painful?
While surgery is an invasive procedure, your surgeon and medical team will prioritize pain management. You'll receive anesthesia during the procedure, and powerful pain medications will be prescribed for the initial recovery phase. As you heal, discomfort will lessen, but some soreness and stiffness are normal. Adhering to your prescribed pain regimen and following recovery instructions are key to minimizing discomfort.
How long is TMJ surgery recovery?
Recovery time varies greatly depending on the type of surgery. For arthrocentesis, initial recovery is a few days. Arthroscopy typically requires a few weeks for initial healing, with full recovery spanning 1-2 months. Open-joint surgery can involve several months of recovery. Total joint replacement demands the longest recovery, often 6-12 months, with diligent physical therapy being crucial throughout.
What are the alternatives to TMJ surgery?
A wide range of conservative, non-surgical alternatives are always explored first. These include oral appliances (nightguards), physical therapy, medication (NSAIDs, muscle relaxants, sometimes antidepressants), stress management techniques, soft diets, and injections (corticosteroids, Botox). Surgery is considered only when these less invasive methods fail to provide adequate relief for severe symptoms or structural damage.
How much does TMJ surgery cost?
The cost varies significantly. Arthrocentesis can range from $1,000 to $5,000. Arthroscopy typically costs $5,000 to $15,000. Open-joint surgeries are generally $15,000 to $40,000. Total joint replacement is the most expensive, often $30,000 to $80,000+ per joint. These are estimates and depend on the surgeon, facility, and specific complexities of the case.
Will my insurance cover TMJ surgery?
Most medical insurance plans (not dental insurance) cover TMJ surgery, as it's typically considered a medical procedure. However, almost all plans require extensive prior authorization and documentation of failed conservative treatments. You will still be responsible for deductibles, co-pays, and co-insurance, up to your out-of-pocket maximum. It's vital to check with your specific insurance provider.
What is the success rate of TMJ surgery?
Success rates vary by procedure type and individual patient factors. Minimally invasive procedures like arthroscopy generally have success rates for pain reduction and improved function in the 70-85% range. Total joint replacement for severe cases often boasts high rates of pain relief (over 90%), though functional outcomes can be more variable. The ultimate success often depends on diligent post-operative physical therapy and lifestyle modifications.
Can TMJ surgery fix clicking?
TMJ surgery can sometimes fix clicking, especially if it's due to a disc displacement that can be successfully repositioned (e.g., during arthroscopy or open-joint surgery). However, clicking alone, without pain or functional limitation, is usually not an indication for surgery. For many, clicking can persist even after surgery, but often without pain or with improved function.
When should I consider TMJ surgery?
You should consider TMJ surgery only after you have exhausted all appropriate conservative treatments for an extended period (typically 6-12 months) without significant and lasting relief. It's also indicated when imaging shows severe, irreversible structural damage (like advanced degeneration, ankylosis, or significant disc displacement) that significantly impairs your jaw function and quality of life.
What kind of doctor performs TMJ surgery?
TMJ surgery is primarily performed by an oral and maxillofacial surgeon (OMS). These specialists are dental surgeons who have completed extensive hospital-based surgical residency training beyond dental school, preparing them to diagnose and treat conditions of the mouth, face, and jaw, including complex TMJ disorders. Some ENTs (Ear, Nose, and Throat specialists) or plastic surgeons with specialized training may also perform certain TMJ procedures.
Can TMJ come back after surgery?
Unfortunately, for some patients, TMJ symptoms can recur even after surgery. This can happen due to progression of the underlying disease, development of scar tissue, failure of the implant (in replacement cases), or a continuation of contributing factors like bruxism or stress. While surgery aims for long-term relief, it's not always a permanent cure, and ongoing management and lifestyle changes are often necessary to maintain the results.
When to See a Dentist
Recognizing when to seek professional help for jaw issues is paramount, as early intervention can often prevent the need for more invasive treatments like surgery.
Red Flags that Need Immediate Attention:
- Acute Jaw Locking: If your jaw suddenly locks in an open or closed position and you cannot manually manipulate it back into place.
- Severe, Sudden Pain: An abrupt onset of intense pain in the jaw joint or surrounding muscles, especially if accompanied by swelling.
- Inability to Open Your Mouth: If you suddenly find it extremely difficult or impossible to open your mouth even slightly.
- Signs of Infection Post-Treatment: If you've recently had an injection or minor procedure and experience increasing pain, swelling, redness, warmth, or pus from the area.
When to Schedule a Prompt Appointment (Routine Care Guidance):
- Persistent Jaw Pain: If you experience jaw pain, tenderness, or aching that lasts for more than a few days and doesn't improve with basic home care (rest, soft diet, over-the-counter pain relievers).
- Frequent Clicking or Popping with Pain: While occasional clicking can be normal, if it's accompanied by pain, stiffness, or limited movement, it warrants evaluation.
- Difficulty Chewing or Speaking: If chewing becomes consistently painful, difficult, or your bite feels "off."
- Chronic Headaches or Earaches: If you experience unexplained chronic headaches, earaches, or neck pain that your general practitioner hasn't been able to diagnose or treat, and you suspect it might be related to your jaw.
- Limited Jaw Movement: If you notice a gradual reduction in your ability to open your mouth wide.
- Failed Conservative Treatment: If you've been managing TMJ symptoms with conservative measures and they are no longer effective, or your symptoms are worsening.
Pro Tip: Start with your general dentist. They can assess your overall oral health, rule out other dental issues, and refer you to a TMJ specialist, oral and maxillofacial surgeon, or other appropriate healthcare provider if your symptoms suggest a complex TMJ disorder. The American Dental Association (ADA) recommends starting with the most conservative, reversible treatments.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Tmj Massage Near Me: Complete Guide
Temporomandibular joint disorder, commonly known as TMJD, affects millions of Americans, causing debilitating pain, discomfort, and significantly impacting quality of life. If you're experiencing jaw pain, clicking, or difficulty chewing, you're not alone. Up to 15% of American adults experience
February 23, 2026
Tmd Treatment: Complete Guide
Experiencing persistent jaw pain, clicking sounds when you chew, or debilitating headaches that seem to originate from your face? You're not alone. Temporomandibular joint (TMJ) disorders, often referred to collectively as TMD, affect an estimated 10 million Americans, with women disproportionat
February 23, 2026
Tmj Nerve Damage Symptoms: Complete Guide
Experiencing persistent facial pain, numbness, or tingling can be distressing, especially when the source is unclear. While many people are familiar with general jaw pain associated with temporomandibular joint (TMJ) disorders, the less commonly understood aspect of tmj nerve damage symptoms can
February 23, 2026
Remi Night Guard: Complete Guide
Remi Night Guard: Complete Guide
February 23, 2026