Wisdom Tooth Pain: Complete Guide
Key Takeaways
- Experiencing wisdom tooth pain can be an incredibly disruptive and uncomfortable ordeal. For many, the dull ache or sharp throbbing behind their molars is the first sign that these late-arriving teeth, also known as third molars, are attempting to emerge, often with insufficient space. In fact, stud
Wisdom Tooth Pain: Complete Guide
Experiencing wisdom tooth pain can be an incredibly disruptive and uncomfortable ordeal. For many, the dull ache or sharp throbbing behind their molars is the first sign that these late-arriving teeth, also known as third molars, are attempting to emerge, often with insufficient space. In fact, studies suggest that over 70% of individuals will experience at least one impacted wisdom tooth during their lifetime, frequently leading to significant discomfort and a host of potential oral health issues. This guide from SmilePedia.net aims to provide a comprehensive understanding of wisdom tooth pain, from its underlying causes and varied symptoms to the most effective treatment options, recovery protocols, and crucial preventive measures, empowering you to make informed decisions about your dental health.
Key Takeaways:
- Wisdom tooth pain typically stems from impaction (lack of space) or infection (pericoronitis).
- Common symptoms include jaw pain, swelling, difficulty opening your mouth, and bad breath; pain can even refer to the nasal cavity or ears.
- Initial tooth pain relief can involve OTC medications and salt water rinses, but persistent pain often requires professional intervention.
- Wisdom tooth extraction costs typically range from $75 - $200 per tooth for simple extractions to $250 - $600 per tooth for surgical removal of impacted teeth, without insurance.
- Recovery from extraction usually takes 3-7 days for most discomfort, with full healing spanning several weeks.
- Untreated wisdom tooth issues can lead to serious complications like infection, cysts, and damage to adjacent teeth.
- Consult your dentist promptly if you experience persistent pain, swelling, or difficulty eating.
What It Is / Overview
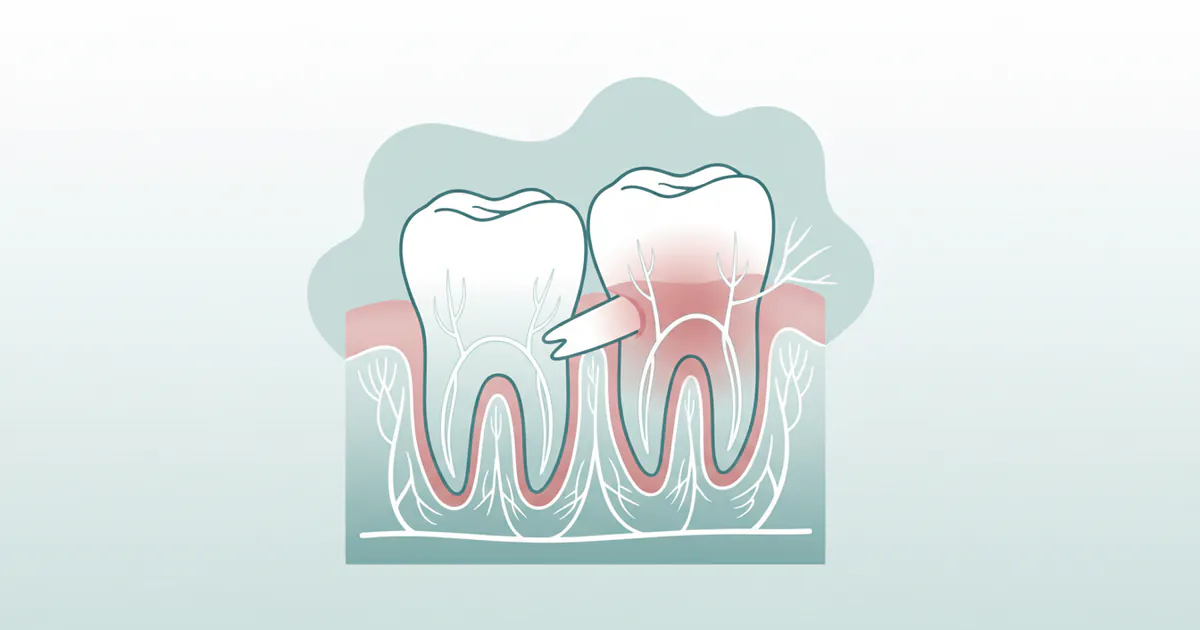
Wisdom teeth are the final set of molars to erupt in the mouth, typically appearing between the ages of 17 and 25. While some individuals may have no issues with their wisdom teeth, for many, their emergence is fraught with complications. The most common problem leading to wisdom tooth pain is impaction – a condition where the wisdom tooth doesn't have enough room to erupt properly and gets stuck beneath the gum line or against an adjacent tooth. This can lead to a variety of painful symptoms and can compromise overall oral health.
When a wisdom tooth is impacted, it can cause pressure, inflammation, and create a breeding ground for bacteria, often resulting in an infection known as pericoronitis. This infection can cause significant localized pain, swelling, and can sometimes spread, affecting the jaw, throat, and even causing referred pain that might be felt in the ear or around the nasal cavity. Understanding the nature of this pain and its origins is the first step toward effective management and treatment.
Types / Variations of Wisdom Tooth Impaction
The way a wisdom tooth is impacted can significantly influence the type and severity of pain experienced, as well as the complexity of its removal. Dentists classify impactions based on their angle, depth, and the amount of gum and bone covering them.
- Mesial Impaction (Angled Forward): This is the most common type of impaction. The wisdom tooth is angled forward, towards the front of the mouth, pressing against the molar in front of it. This can cause significant pressure and potential damage to the adjacent tooth.
- Distal Impaction (Angled Backward): Less common than mesial impaction, the wisdom tooth is angled backward, towards the rear of the mouth.
- Vertical Impaction: The wisdom tooth is positioned correctly (straight up and down) but is still unable to erupt fully due to lack of space, often getting stuck under the gum line or bone.
- Horizontal Impaction: The most problematic type, where the wisdom tooth lies completely sideways, usually pushing directly into the root of the second molar. This often causes intense pain and can severely damage the adjacent tooth.
Beyond the angle, impactions are also categorized by the tissue covering them:
- Soft Tissue Impaction: The tooth has erupted through the bone but is still covered by gum tissue, often leading to pericoronitis.
- Partial Bony Impaction: Part of the tooth has erupted, but a portion remains covered by bone and gum tissue. This also commonly leads to pericoronitis as food and bacteria can get trapped.
- Full Bony Impaction: The entire tooth is completely encased within the jawbone and gum tissue. This type typically requires a more complex surgical extraction.
``
| Type of Impaction | Description | Common Issues | Complexity of Extraction |
|---|---|---|---|
| Mesial Impaction | Angled forward, towards the front of the mouth | Pressure on adjacent tooth, decay, pericoronitis | Moderate |
| Distal Impaction | Angled backward, towards the rear of the mouth | Less common issues, potential pressure, cysts | Moderate |
| Vertical Impaction | Straight up and down, but stuck under gum/bone | Lack of eruption space, pericoronitis, cysts | Moderate |
| Horizontal Impaction | Lying completely sideways, pushing into adjacent molar | Severe pain, damage to adjacent tooth, nerve compression, cysts | High |
| Soft Tissue Impaction | Tooth has broken through bone, covered only by gum tissue | Pericoronitis (infection of gum flap), swelling, difficulty cleaning | Low to Moderate |
| Partial Bony Impaction | Part of tooth visible, part covered by bone and gum tissue | High risk of pericoronitis, decay, food trapping | Moderate |
| Full Bony Impaction | Entire tooth completely encased within jawbone and gum tissue | Potential for cysts, pressure, referred pain, difficult to diagnose without X-ray | High |
Causes / Why It Happens
The primary reason for wisdom tooth pain is a lack of sufficient space in the jaw for these teeth to erupt normally. Our modern diets and genetic predispositions often result in smaller jaws compared to our ancestors, leading to a crowded dental arch. When the wisdom teeth try to push through, they encounter resistance, leading to the various forms of impaction discussed above.
Beyond simple impaction, several factors contribute to the onset and severity of wisdom tooth pain:
- Pericoronitis: This is an inflammation or infection of the gum tissue surrounding a partially erupted wisdom tooth. When a wisdom tooth only partially emerges, it creates a flap of gum tissue (operculum) that can trap food particles, plaque, and bacteria. This trapped debris is difficult to clean and provides an ideal environment for bacterial growth, leading to infection, swelling, and intense localized tooth pain relief becomes urgent. This infection can spread to the jaw, cheek, or neck.
- Pressure on Adjacent Teeth: An impacted wisdom tooth can push against the second molar, causing pain in that tooth, damage to its roots, or even contributing to misalignment of other teeth.
- Cyst Formation: In some cases, a fluid-filled sac (dentigerous cyst) can form around the crown of an impacted wisdom tooth. These cysts can grow, putting pressure on nerves and bone, causing pain, and potentially damaging adjacent teeth or jaw structure. While rare, if left untreated, they can lead to benign tumors.
- Tooth Decay: Partially erupted wisdom teeth are often difficult to clean effectively. This makes them highly susceptible to tooth decay (cavities), which can also occur in the adjacent second molar due to the difficult-to-clean area created by the impaction.
- Gum Disease: The chronic inflammation and bacterial trapping around a partially erupted wisdom tooth can contribute to localized gum disease (periodontitis), which can weaken the bone support of surrounding teeth.
- Referred Pain: The nerves supplying the wisdom teeth are connected to other areas of the head and neck. Pain from an impacted wisdom tooth can be referred to the ear, temple, throat, or even cause sinus pressure and discomfort, mimicking issues within the nasal cavity.
Signs and Symptoms
Recognizing the signs and symptoms of wisdom tooth pain is crucial for timely intervention. While the most obvious symptom is pain, it can manifest in various ways and be accompanied by other indicators.
- Localized Pain: A dull, persistent ache or sharp, throbbing pain in the back of your mouth, specifically behind the second molars. This pain can come and go or be constant.
- Swelling: Noticeable swelling of the gum tissue around the erupting or impacted tooth. The cheek or jaw on the affected side may also appear swollen.
- Tenderness and Redness: The gum tissue in the area may be red, inflamed, and tender to the touch.
- Difficulty Opening Mouth (Trismus): Inflammation and muscle spasms in the jaw can make it painful or difficult to open your mouth wide.
- Difficulty Chewing or Swallowing: Eating and drinking can become uncomfortable due to pain and swelling.
- Bad Breath (Halitosis) and Unpleasant Taste: Bacteria trapped around a partially erupted wisdom tooth can lead to infection, producing foul odors and a bad taste in your mouth, often a hallmark of pericoronitis.
- Jaw Pain and Stiffness: Pain radiating to the jaw, making it stiff or sore. This can sometimes feel like earache.
- Headaches: Persistent headaches can be a symptom, often related to muscle tension from jaw clenching or referred pain.
- Swollen Lymph Nodes: In cases of infection, the lymph nodes under the jaw or in the neck may become swollen and tender.
- Referred Pain: As mentioned, pain can radiate to other areas. Some patients report a feeling of pressure or pain in the nasal cavity or sinuses, especially with upper wisdom teeth impactions where roots can be close to the maxillary sinus floor. Earaches without an actual ear infection are also common.
Treatment Options
When experiencing wisdom tooth pain, the treatment approach depends largely on the severity of symptoms, the extent of impaction, and the presence of infection. Initial tooth pain relief often focuses on managing symptoms, but definitive treatment usually involves extraction.
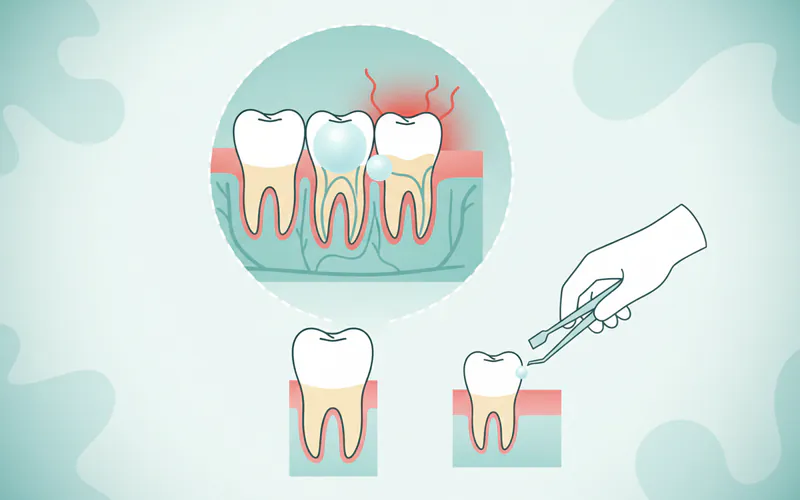
A. Initial Pain Management and Symptomatic Relief (Temporary)
These methods are for temporary relief while awaiting a dental appointment or during the early stages of eruption.
- Over-the-Counter (OTC) Pain Relievers:
- Pros: Readily available, affordable.
- Cons: Only address symptoms, don't treat the underlying cause.
- Examples: Ibuprofen (Advil, Motrin) or Acetaminophen (Tylenol) can help reduce pain and inflammation. Follow dosage instructions carefully.
- Saltwater Rinses:
- Pros: Natural antiseptic, helps reduce inflammation and kill bacteria, promotes healing.
- Cons: Not a cure, only symptomatic relief.
- Method: Dissolve half a teaspoon of salt in 8 ounces of warm water. Swish gently in your mouth for 30-60 seconds, then spit it out. Repeat several times a day, especially after meals.
- Cold Compress:
- Pros: Reduces swelling and numbs the area.
- Cons: Temporary relief.
- Method: Apply an ice pack wrapped in a cloth to the outside of your cheek for 15-20 minutes at a time, several times a day.
- Oral Anesthetics (Topical Gels):
- Pros: Provides localized, temporary numbing.
- Cons: Short-lived effect, doesn't treat infection.
- Examples: Gels containing benzocaine (e.g., Orajel) can be applied directly to the painful gum area.
- Improved Oral Hygiene:
- Pros: Crucial for preventing infection from worsening.
- Cons: Can be difficult and painful.
- Method: Gently brush and floss around the affected area to remove trapped food and bacteria. Use an antimicrobial mouthwash if recommended by your dentist.
B. Professional Intervention (Definitive Treatment)
For persistent pain, swelling, or signs of infection, professional dental care is essential.
-
Antibiotics (for Infection):
- Pros: Treats bacterial infections like pericoronitis, reduces pain and swelling significantly.
- Cons: Requires a prescription, doesn't solve the underlying impaction issue.
- When: Prescribed by a dentist or oral surgeon if there are signs of active infection (pus, fever, spreading swelling). Common antibiotics include Amoxicillin or Metronidazole.
-
Irrigation of Pericoronal Flap:
- Pros: Cleans the area under the gum flap, removing trapped debris and bacteria.
- Cons: Temporary, does not prevent recurrence if the flap remains.
- When: Performed by a dentist using a sterile saline solution or antiseptic rinse to flush out the infected area.
-
Operculectomy (Gum Flap Removal):
- Pros: Removes the problematic gum flap, reducing the chance of food trapping and pericoronitis.
- Cons: Not always successful if the tooth remains impacted or only partially erupted; pain may return.
- When: For soft tissue impactions where the tooth is otherwise well-positioned but continually gets infected. Can be done with a scalpel or laser.
-
Wisdom Tooth Extraction:
-
Pros: The definitive solution, removes the source of pain and future complications.
-
Cons: Surgical procedure, requires recovery time, potential for complications.
-
When: Recommended for most symptomatic impacted wisdom teeth, or those identified as high-risk for future problems (e.g., potential for decay, cyst formation, or damage to adjacent teeth). This is the most common and effective treatment.
-
Simple Extraction:
- Description: Performed when the wisdom tooth has fully erupted and is visible in the mouth, similar to extracting any other tooth. The dentist uses instruments to loosen and remove the tooth.
- Anesthesia: Local anesthetic.
- Recovery: Generally quicker, 2-3 days of mild discomfort.
-
Surgical Extraction:
- Description: Required for impacted wisdom teeth, especially those partially or fully covered by gum tissue or bone. The oral surgeon makes an incision in the gum, removes bone if necessary, and sometimes divides the tooth into smaller pieces for easier removal.
- Anesthesia: Local anesthetic, conscious sedation (nitrous oxide, oral sedatives, IV sedation), or general anesthesia.
- Recovery: More involved, 3-7 days of significant discomfort, swelling, and dietary restrictions.
Pro Tip: Always seek professional dental advice for persistent wisdom tooth pain. Self-treatment is only for temporary relief and does not address the underlying cause or potential for serious infection.
-
Step-by-Step Process: What to Expect During Wisdom Tooth Extraction
If extraction is recommended, understanding the process can help alleviate anxiety. The exact steps may vary based on the complexity of your case and the type of anesthesia used.
- Consultation and X-rays:
- Before any procedure, your dentist or oral surgeon will conduct a thorough examination and take X-rays (often panoramic X-rays). These images are crucial to visualize the position of the wisdom teeth, their roots, proximity to nerves (like the inferior alveolar nerve) and sinuses (related to the nasal cavity), and the surrounding bone structure.
- Discussion about your medical history, current medications, and anesthesia options will take place.
- Anesthesia Administration:
- On the day of the procedure, local anesthesia will be administered to numb the area around the tooth. If you've opted for conscious sedation (oral, nitrous oxide, or IV sedation) or general anesthesia, these will be administered prior to the local anesthetic. Sedation helps you relax or sleep through the procedure.
- Tooth Exposure (Surgical Extraction Only):
- For impacted teeth, the oral surgeon will make a small incision in the gum tissue to expose the tooth.
- If bone is covering the tooth, a small amount may be carefully removed using a dental drill to access the tooth.
- Tooth Removal:
- The surgeon may need to divide the tooth into several smaller pieces to minimize the amount of bone removal required and facilitate easier extraction.
- Dental instruments are then used to gently loosen and remove the tooth or tooth fragments.
- Site Cleaning and Suturing:
- Once the tooth is removed, the socket is thoroughly cleaned to ensure no debris or infection remains.
- The gum flap is then repositioned, and sutures (stitches) are often placed to help the wound heal properly and control bleeding. Some sutures are dissolvable, while others may need to be removed by the dentist after about a week.
- Gauze Placement:
- A piece of sterile gauze is placed over the extraction site, and you'll be instructed to bite down firmly to apply pressure. This helps to form a blood clot, which is crucial for healing and preventing complications like dry socket.
- Post-Procedure Instructions:
- You will receive detailed written and verbal instructions regarding post-operative care, including pain management, diet, hygiene, and activity restrictions. If you received sedation, someone will need to drive you home.
``
Cost and Insurance
The cost of wisdom tooth pain treatment, particularly extraction, can vary significantly based on several factors, including the type of impaction, the number of teeth extracted, the type of anesthesia used, the geographic location, and whether the procedure is performed by a general dentist or an oral surgeon.
Average US Costs (Without Insurance):
- Simple Eruption (Non-impacted):
- Range: $75 - $200 per tooth
- This is for a fully erupted tooth that can be removed with standard dental instruments.
- Soft-Tissue Impaction:
- Range: $250 - $400 per tooth
- Requires an incision to access the tooth covered by gum tissue.
- Partial Bony Impaction:
- Range: $350 - $500 per tooth
- Involves removing some bone to access the tooth.
- Full Bony Impaction:
- Range: $450 - $600 per tooth
- The most complex, requiring significant bone removal and often tooth sectioning.
Anesthesia Costs (Additional):
- Nitrous Oxide (Laughing Gas): $50 - $150 per visit
- Oral Sedation (Pills): $100 - $300 per visit
- IV Sedation (Conscious Sedation): $300 - $800 per hour (often a flat fee for the procedure)
- General Anesthesia: $500 - $1,000+ per hour (typically for complex cases or multiple extractions, administered by an anesthesiologist)
Total Cost for 4 Impacted Wisdom Teeth (e.g., 4 Full Bony Impactions with IV Sedation):
- Low End: 4 x $450 (teeth) + $300 (IV sedation) = $2,100
- High End: 4 x $600 (teeth) + $800 (IV sedation) = $3,200
- These are general estimates; actual costs can be higher in urban areas or with highly experienced specialists.
Insurance Coverage:
Most dental insurance plans provide some level of coverage for wisdom tooth extractions, as they are considered medically necessary.
- Basic Plans: May cover 50-80% of simple extractions.
- Comprehensive Plans: May cover 50-80% of surgical extractions, sometimes up to 90% if deemed critical.
- Medical Insurance: In some cases, if the extraction is particularly complex or leads to significant medical complications (e.g., nerve damage, severe infection), a portion of the cost might be covered by your medical insurance, especially if performed in a hospital setting. It's crucial to check with both your dental and medical insurance providers.
- Deductibles and Annual Maximums: Remember to account for your annual deductible (the amount you pay before insurance starts covering) and annual maximums (the total amount your insurance will pay in a year). Many dental plans have annual maximums ranging from $1,000 to $2,000. If your procedure exceeds this, you will pay the difference.
Pro Tip: Before undergoing any procedure, always request a detailed estimate from your dental office. They can help you understand what your insurance will cover and your out-of-pocket expenses.
Recovery and Aftercare
Proper aftercare is crucial for a smooth recovery and to prevent complications like dry socket, infection, and prolonged wisdom tooth pain.
- Bleeding Control:
- Bite firmly on the gauze pads placed by your surgeon for 30-60 minutes after the procedure. Change the gauze every 30-45 minutes until bleeding subsides.
- A small amount of oozing for the first 24 hours is normal. If heavy bleeding persists, bite on a moist tea bag (tannic acid helps clotting) or contact your dentist.
- Pain Management:
- Take prescribed pain medication or OTC pain relievers (e.g., Ibuprofen) as directed before the local anesthetic wears off. This is key for effective tooth pain relief.
- Continue taking medication as needed for the first 3-5 days.
- Swelling Reduction:
- Apply an ice pack to the outside of your cheek for 15-20 minutes on, 15-20 minutes off, for the first 24-48 hours. This is most effective in preventing initial swelling.
- After 48 hours, switch to moist heat (a warm compress) to help reduce remaining swelling.
- Diet:
- First 24-48 hours: Stick to soft foods that don't require chewing (e.g., yogurt, applesauce, mashed potatoes, soups, smoothies - but no straws!).
- Avoid: Hot liquids, spicy foods, crunchy or sticky foods, and alcohol for at least 72 hours.
- NO STRAWS! The sucking motion can dislodge the blood clot, leading to a painful dry socket.
- Oral Hygiene:
- First 24 hours: Do NOT rinse your mouth vigorously, spit forcefully, or brush the extraction site.
- After 24 hours: Gently rinse with warm salt water (half teaspoon salt in 8 oz warm water) 3-4 times a day, especially after meals.
- Brush your other teeth gently, avoiding the surgical site.
- Activity Restrictions:
- Rest for at least 24-48 hours after surgery. Avoid strenuous activity, heavy lifting, or bending over for 3-5 days. Increased blood pressure can cause bleeding or discomfort.
- Elevate your head with pillows while sleeping to help reduce swelling.
- Smoking and Alcohol:
- Absolutely NO SMOKING for at least 72 hours, ideally longer. Smoking significantly increases the risk of dry socket and delays healing.
- Avoid alcohol for at least 24-48 hours, or while taking pain medication.
- Sutures:
- If non-dissolvable sutures were used, your dentist will schedule an appointment to remove them, typically 7-10 days after surgery.
Pro Tip: Stay well-hydrated by drinking plenty of water, but avoid carbonated beverages and straws.
Prevention
While you can't prevent wisdom teeth from forming, you can take steps to prevent or mitigate the severity of wisdom tooth pain and associated complications.
- Early Dental Assessments:
- Regular dental check-ups, especially in the late teenage years (ages 16-20), are crucial. Your dentist can monitor the development of wisdom teeth through X-rays even before they start to erupt.
- The American Dental Association (ADA) recommends regular check-ups, which include assessment of erupting teeth. Early detection of potential impaction allows for proactive planning.
- Proactive Extraction (Elective Removal):
- If X-rays show that wisdom teeth are impacted and are likely to cause problems (e.g., angled horizontally, close to nerves/sinuses, no room for eruption), your dentist or oral surgeon may recommend prophylactic (preventive) extraction.
- Extracting wisdom teeth before they cause pain, infection, or damage to adjacent teeth can prevent future complications and often leads to an easier recovery, as the roots are less developed in younger individuals.
- Good Oral Hygiene:
- Maintain excellent brushing and flossing habits, even in the very back of your mouth, to prevent food and bacteria from accumulating around partially erupted wisdom teeth. This can help prevent pericoronitis.
- Use an antimicrobial mouthwash if recommended by your dentist.
Risks and Complications
While wisdom tooth extraction is a common and generally safe procedure, like any surgery, it carries potential risks and complications. Being aware of these can help you identify issues early and seek prompt attention.
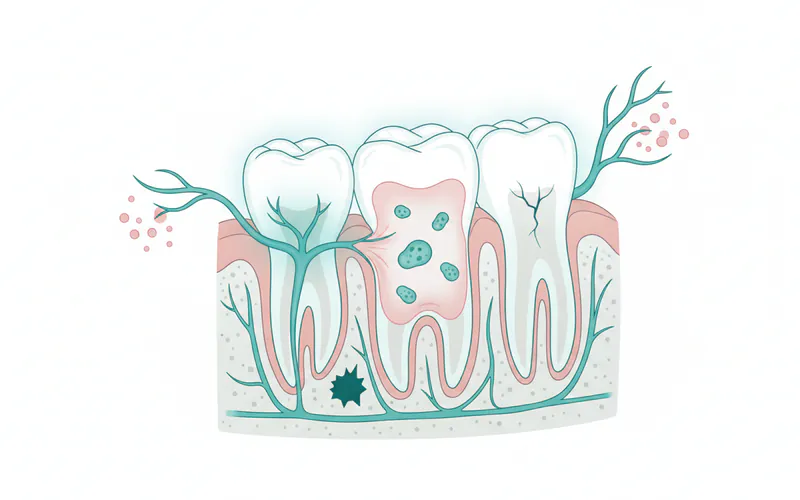
- Dry Socket (Alveolar Osteitis): This is the most common complication, occurring in 5-10% of cases, especially in lower wisdom teeth. It happens when the blood clot that forms in the extraction socket dislodges prematurely or dissolves, exposing the underlying bone and nerves.
- Symptoms: Intense, throbbing pain (often radiating to the ear or temple) starting 2-5 days after surgery, a foul odor or taste, and visible empty socket.
- Treatment: Dentist will clean the socket, pack it with medicated gauze, and provide pain relief.
- Infection: Although antibiotics may be given pre- or post-operatively, infection can still occur at the surgical site.
- Symptoms: Persistent pain, swelling, redness, pus drainage, fever, and swollen lymph nodes.
- Treatment: Drainage, antibiotics, and further cleaning.
- Nerve Damage (Paresthesia): This is a rare but serious complication, usually temporary, where the inferior alveolar nerve (supplying sensation to the lip, chin, and tongue) or lingual nerve (supplying sensation to the tongue) can be bruised or damaged during extraction, especially if the tooth roots are very close to the nerve canal.
- Symptoms: Numbness, tingling, or altered sensation in the lip, chin, tongue, or gums.
- Outlook: Most cases resolve within weeks or months, but in very rare instances, it can be permanent.
- Sinus Communication: For upper wisdom teeth, the roots can be very close to or extend into the maxillary sinus (a cavity above the upper jaw and lateral to the nasal cavity). Extraction can sometimes create an opening (oro-antral communication) between the mouth and the sinus.
- Symptoms: Air or fluid passing between the mouth and nose, difficulty blowing nose, sometimes sinus pain or infection.
- Treatment: Usually closes on its own or with sutures; sometimes requires a minor surgical repair.
- Damage to Adjacent Teeth: During extraction, there's a small risk of damaging the adjacent second molar, either to its crown (e.g., chipping) or root.
- Fractured Jaw: An extremely rare complication, usually associated with very difficult extractions of fully impacted teeth, especially in older patients or those with weakened bone.
- Excessive Bleeding: While some bleeding is normal, prolonged heavy bleeding requires immediate attention.
``
| Complication | Symptoms | Severity | Likelihood | Management |
|---|---|---|---|---|
| Dry Socket | Intense pain 2-5 days post-op, foul odor/taste, empty socket | Moderate | Common | Medicated packing, pain relief |
| Infection | Persistent pain, swelling, pus, fever, redness | Moderate | Less Common | Antibiotics, drainage, cleaning |
| Nerve Damage | Numbness/tingling in lip, chin, or tongue | Moderate-High | Rare | Monitoring, medication, specialist referral (usually resolves) |
| Sinus Communication | Air/fluid in nose from mouth, sinus symptoms | Low-Moderate | Rare (upper) | Sutures, antibiotics, avoidance of nose blowing, sometimes surgical repair |
| Damage to Adjacent Tooth | Chipped enamel, root damage to second molar | Low | Rare | Restoration of damaged tooth |
| Excessive Bleeding | Persistent heavy bleeding beyond normal oozing | Moderate | Less Common | Pressure, sutures, professional intervention |
Children / Pediatric Considerations
Wisdom teeth typically begin developing around ages 10-12, but don't usually erupt until late teens or early twenties. Therefore, wisdom tooth pain is not a common issue in young children. However, early monitoring is important:
- Orthodontic Assessment: Often, children undergoing orthodontic treatment will have panoramic X-rays taken around ages 10-14. These X-rays can reveal the presence and position of developing wisdom teeth (also known as "tooth buds").
- Early Intervention: If these X-rays show wisdom teeth developing at a severe angle or indicating a high likelihood of impaction later on, an orthodontist or general dentist might recommend monitoring their development. In very rare cases, if the wisdom tooth is threatening the root of the second molar at a very young age, an "odontomy" (surgical removal of the tooth bud before root formation) might be considered, though this is uncommon.
- Adolescent Monitoring: For teenagers (16-18 years old) who haven't started experiencing symptoms, regular dental check-ups with updated X-rays are crucial. This allows the dentist to assess whether there is enough room for eruption or if extraction might be necessary before symptoms like wisdom tooth pain and infection develop. Early extraction in adolescents (before full root development) can often lead to an easier procedure and quicker recovery.
Cost Breakdown
Understanding the financial aspect of wisdom tooth removal is crucial for planning. While covered earlier, here's a detailed breakdown.
Average US Costs (Per Tooth)
| Procedure Type | Low Range | Mid Range | High Range |
|---|---|---|---|
| Simple Eruption | $75 | $125 | $200 |
| Soft Tissue Impaction | $250 | $325 | $400 |
| Partial Bony Impaction | $350 | $425 | $500 |
| Full Bony Impaction | $450 | $525 | $600 |
- These costs are for the extraction itself, not including anesthesia or pre/post-operative appointments.
Anesthesia Costs (Per Visit/Hour)
| Anesthesia Type | Low Range | Mid Range | High Range |
|---|---|---|---|
| Nitrous Oxide | $50 | $100 | $150 |
| Oral Sedation | $100 | $200 | $300 |
| IV Sedation (per hour) | $300 | $550 | $800 |
| General Anesthesia (per hour) | $500 | $750 | $1,000+ |
With vs Without Insurance
- Without Insurance: You will be responsible for 100% of the costs as detailed above.
- With Insurance: Most dental insurance plans cover 50-80% of wisdom tooth extractions, depending on your plan and the complexity.
- Example (Full Bony Impaction, $525 per tooth, 80% coverage):
- Your portion: $525 * 0.20 = $105 per tooth.
- Insurance pays: $420 per tooth.
- Remember deductibles: If your deductible is $50, you'll pay the first $50, then insurance covers 80% of the remaining amount up to your annual maximum.
- Annual Maximums: Many plans have annual maximums of $1,000 - $2,000. If you're having all four wisdom teeth removed, you might exceed this, and you'll be responsible for the remaining balance.
- Example (Full Bony Impaction, $525 per tooth, 80% coverage):
Payment Plans and Financing Options
Many dental offices and oral surgery centers understand the financial burden and offer solutions:
- In-house Payment Plans: Some offices allow you to pay in installments over several months, often without interest.
- Third-Party Financing: Companies like CareCredit or LendingClub offer specialized healthcare credit cards with deferred interest options (if paid within a certain timeframe) or low-interest payment plans.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use these tax-advantaged accounts to pay for wisdom tooth extraction expenses.
Cost-Saving Tips
- Shop Around: Get quotes from a few different oral surgeons or dentists. Prices can vary.
- Ask for Itemized Estimates: Understand every charge, including the extraction, anesthesia, and facility fees.
- Utilize Insurance Benefits Early: If you know you need extractions, schedule them before your annual maximum resets (e.g., at the end of the year).
- Dental Schools: If there's a dental school nearby, they often offer services at a reduced cost, performed by supervised students.
- Discuss Less Expensive Anesthesia: If possible, consider local anesthesia with nitrous oxide instead of IV sedation, which can significantly reduce costs.
Frequently Asked Questions
What does wisdom tooth pain feel like?
Wisdom tooth pain can range from a dull, constant ache to sharp, throbbing sensations in the back of your jaw, often radiating towards the ear, temple, or even causing sinus pressure. It's commonly associated with swelling, tenderness, and difficulty chewing or opening your mouth wide.
How can I get temporary tooth pain relief at home?
For temporary relief, you can use over-the-counter pain relievers like Ibuprofen or Acetaminophen, rinse with warm salt water several times a day to reduce inflammation and kill bacteria, and apply a cold compress to the outside of your cheek to reduce swelling and numb the area. However, these are not long-term solutions.

When should I see a dentist for wisdom tooth pain?
You should see a dentist immediately if you experience severe, persistent pain, significant swelling, difficulty swallowing or opening your mouth, fever, or a foul taste/smell in your mouth. These symptoms could indicate an infection that requires prompt professional treatment.
Is wisdom tooth removal always necessary?
No, not always. If wisdom teeth erupt fully and correctly without causing pain, impaction, or damage to other teeth, they may not need to be removed. However, if they are impacted, causing pain, infection, or other oral health problems, extraction is generally recommended to prevent future complications.
How long does wisdom tooth pain last after extraction?
Significant pain typically subsides within 3-7 days after extraction. You'll likely experience some discomfort, swelling, and bruising for a week or two. Full healing of the socket can take several weeks to months, but the acute pain should resolve much faster with proper aftercare.
Can wisdom teeth cause problems with my nasal cavity or sinuses?
Yes, upper wisdom teeth can have roots that are very close to or extend into the maxillary sinus, which is near the nasal cavity. If these teeth become infected, the infection can spread to the sinus, causing sinus pressure, congestion, or referred pain. Extraction can also, in rare cases, create a temporary opening between the mouth and sinus.
What is a dry socket and how can I prevent it?
A dry socket (alveolar osteitis) is a painful complication where the blood clot in the extraction site dislodges, exposing bone and nerves. You can help prevent it by avoiding smoking, vigorous rinsing, forceful spitting, and drinking through straws for at least 72 hours post-extraction. Following all aftercare instructions diligently is crucial.
What are the average costs for wisdom tooth removal with and without insurance?
Without insurance, a simple wisdom tooth extraction can cost $75 - $200 per tooth, while a complex surgical extraction for a fully impacted tooth can range from $450 - $600 per tooth, plus anesthesia fees. With dental insurance, plans often cover 50-80% of the cost, but you'll need to consider deductibles and annual maximums.
Are there alternatives to wisdom tooth extraction?
For symptomatic wisdom teeth causing pain or infection, extraction is generally the definitive treatment. Temporary alternatives include antibiotics for infection, saltwater rinses, and pain relievers. In some rare cases, an operculectomy (removal of gum flap) might be done, but it doesn't solve impaction.
How long is the recovery from wisdom tooth extraction?
Initial recovery with significant swelling and discomfort typically lasts 3 to 7 days. Most individuals can return to normal non-strenuous activities within a week. Complete healing of the jawbone and soft tissues around the extraction site can take several weeks to a few months.
When to See a Dentist
It's crucial to seek professional dental attention when dealing with wisdom tooth pain, as ignoring symptoms can lead to more severe complications.
Red Flags Requiring Immediate Attention (Emergency):
- Severe, Unmanageable Pain: If over-the-counter pain relievers or home remedies aren't providing any relief, or if the pain is debilitating.
- Rapidly Worsening Swelling: If swelling in your cheek, jaw, or around the wisdom tooth area increases rapidly and significantly, especially if it affects your ability to open your mouth or swallow.
- Difficulty Breathing or Swallowing: This is a serious sign of a spreading infection that could compromise your airway. Seek emergency care immediately.
- Fever or Chills: These are indicators of a systemic infection that requires immediate medical attention and antibiotics.
- Pus Drainage: If you see or taste pus coming from the gum around your wisdom tooth, it's a clear sign of infection.
- Pain Radiating to Ear or Throat: While common with wisdom tooth issues, if this pain is severe or combined with other infection symptoms, it warrants prompt evaluation.
Guidance for Routine vs. Scheduled Appointments:
- Routine Care/Monitoring: If you are in your late teens or early twenties and have not experienced symptoms, but your dentist identified wisdom teeth on an X-ray, discuss their potential future impact during your regular check-ups. Proactive discussions can lead to preventative extraction before problems arise.
- Scheduled Appointment: If you experience mild, intermittent wisdom tooth pain, occasional swelling, or notice food getting consistently trapped in the back of your mouth, schedule an appointment with your dentist promptly. These symptoms, while not an emergency, indicate that your wisdom teeth are likely causing problems and require evaluation. Early intervention can prevent minor issues from escalating into painful infections or damage to adjacent teeth.
Do not delay in addressing wisdom tooth issues. Your oral health is intrinsically linked to your overall well-being, and a timely visit to your dentist can save you from unnecessary pain and potential complications.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
What Is an Abscess
Imagine a throbbing pain deep within your jaw, a persistent ache that keeps you awake at night and makes even the softest foods unbearable. This isn't just a bad toothache; it could be a sign of something much more serious: a dental abscess. Affecting millions of Americans annually, an abscess is an
February 22, 2026
Cracked Tooth Syndrome: Complete Guide
Cracked Tooth Syndrome: Complete Guide Category: Dental Conditions & Diseases
February 22, 2026
Dentinogenesis Imperfecta: Complete Guide
Imagine a world where your teeth, fundamental to chewing, speaking, and even smiling confidently, are inherently fragile, discolored, and prone to rapid wear from the moment they emerge. For individuals affected by dentinogenesis imperfecta (DI), this is a reality. While relatively rare, affecti
February 22, 2026
Stage 1 Early Cavity: Complete Guide
Did you know that dental cavities are one of the most common chronic diseases globally, affecting both children and adults? In the United States, over 90% of adults have had a cavity, and a significant portion of these begin as a stage 1 early cavity. Often invisible and painless in its nasc
February 22, 2026