Complete Guide to Sleep Dentistry & Apnea: Everything You Need to Know

Key Takeaways
- Do you or a loved one snore loudly? Are you constantly tired, even after a full night's sleep? You're not alone. An estimated 30% of adults experience habitual snoring, and up to 1 in 5 adults suffer from obstructive sleep apnea (OSA), a serious condition where breathing repeatedly stops and
Complete Guide to Sleep Dentistry & Apnea: Everything You Need to Know
Do you or a loved one snore loudly? Are you constantly tired, even after a full night's sleep? You're not alone. An estimated 30% of adults experience habitual snoring, and up to 1 in 5 adults suffer from obstructive sleep apnea (OSA), a serious condition where breathing repeatedly stops and starts during sleep. This isn't just about disturbing your partner; unchecked sleep apnea can have profound implications for your overall health, increasing your risk of heart disease, stroke, diabetes, and even accidents.

Welcome to the comprehensive guide to understanding sleep apnea and the innovative field of sleep dentistry. At SmilePedia.net, we believe that informed patients are empowered patients. This article will demystify sleep apnea, explore its various forms, detail the causes and symptoms, and — crucially — outline the full spectrum of modern treatment options available, from lifestyle changes and CPAP machines to custom sleep apnea mouth guards and advanced surgical interventions. We'll dive deep into topics like what is sleep apnea, the effectiveness of a mandibular advancement device, and even address questions about mouth tape for snoring. By the end, you'll have a clear roadmap to better sleep and a healthier life.
Key Takeaways:
- Prevalence: Up to 20% of adults experience obstructive sleep apnea (OSA), often characterized by loud
snoringand daytime fatigue. Many are undiagnosed.- Diagnosis: Requires a sleep study (polysomnography or home sleep test), often recommended by a primary care physician or dentist. Costs typically range from $250 - $1,500 for a home test to $2,000 - $5,000+ for an in-lab study, usually covered by medical insurance.
- Primary Treatments: CPAP (Continuous Positive Airway Pressure) is the gold standard for moderate to severe OSA. Oral appliance therapy (OAT) using a
mandibular advancement device(MAD) is an excellent alternative for mild to moderate OSA or for those who cannot tolerate CPAP.- Oral Appliance Costs: Custom-fitted
mouth guards for sleep apneafrom a dentist typically cost $2,000 - $5,000, with many medical insurance plans offering coverage. Over-the-counter options are significantly cheaper (under $200) but are generally not recommended for diagnosedsleep apneadue to lack of customization and potential for jaw issues.- Treatment Timeline: Diagnosis can take weeks. Fitting a custom oral appliance usually involves 2-3 appointments over 4-8 weeks. CPAP setup is often quicker but requires an adaptation period.
- Actionable Steps: If you
snoreloudly or experience daytime sleepiness, consult your dentist or physician to discuss a sleep apnea screening. Early diagnosis and treatment are crucial for preventing serious health complications.
What Is Sleep Apnea? An Overview
Sleep apnea is a serious sleep disorder characterized by repeated interruptions in breathing during sleep. The word "apnea" literally means "without breath." These interruptions, or apneas, can last from a few seconds to more than a minute and can occur hundreds of times a night, preventing deep, restorative sleep. Each time breathing stops, your brain briefly wakes you up to restart breathing, often with a gasp or snort, though you may not remember waking.
The primary concern with sleep apnea is the intermittent lack of oxygen to the brain and other vital organs, alongside the constant disruption of sleep cycles. Over time, this chronic stress on the body can lead to a host of significant health problems.
Types of Sleep Apnea
There are three main types of sleep apnea:
- Obstructive Sleep Apnea (OSA): This is the most common form, accounting for about 85-90% of cases. OSA occurs when the muscles in the back of your throat relax too much, causing the soft tissues to collapse and block your airway. As you try to breathe, the air struggle creates the sound of
snoring. - Central Sleep Apnea (CSA): Less common, CSA occurs when your brain fails to send the proper signals to the muscles that control breathing. This means your body simply "forgets" to breathe for short periods, and there's no obstruction in the airway. It's often associated with underlying medical conditions like heart failure, stroke, or certain medications.
- Complex (Mixed) Sleep Apnea Syndrome: This is a combination of both obstructive and central sleep apnea, initially presenting as OSA but developing features of CSA during treatment, typically with CPAP.
Causes and Why It Happens
Understanding why sleep apnea occurs is crucial for effective treatment. While the specific mechanisms differ slightly between OSA and CSA, several factors contribute to their development.
Causes of Obstructive Sleep Apnea (OSA):
- Anatomical Factors:
- Enlarged Tonsils or Adenoids: Especially common in children, these can block the airway.
- Large Tongue or Uvula: The soft tissue hanging at the back of your throat.
- Recessed Jaw (Retrognathia) or Small Airway: The physical structure of your jaw and throat can predispose you to collapse.
- Nasal Obstruction: Chronic nasal congestion from allergies, polyps, or a deviated septum can make breathing through the nose difficult, leading to mouth breathing and increased airway collapse.
- Obesity: Excess weight, particularly around the neck, can narrow the airway and increase the likelihood of soft tissue collapse. Fat deposits can thicken the walls of the throat, reducing the internal diameter.
- Lifestyle Factors:
- Alcohol and Sedatives: These substances relax the muscles in the throat, making airway collapse more likely. Even over-the-counter sleep aids can have this effect.
- Smoking: Smokers are three times more likely to have OSA than non-smokers. Smoking can increase inflammation and fluid retention in the upper airway.
- Sleeping Position: Sleeping on your back allows gravity to pull your tongue and soft palate backward, potentially obstructing the airway.
- Genetics: A family history of sleep apnea can increase your risk, suggesting a genetic predisposition to certain anatomical features.
- Age: While it can affect anyone, the risk of OSA increases with age, particularly after 40.
- Gender: Men are more likely to develop OSA than women, although the risk for women increases after menopause.
- Medical Conditions: Hypothyroidism, acromegaly, and certain neurological conditions can contribute to OSA.
Causes of Central Sleep Apnea (CSA):
CSA is not related to a physical blockage but to a malfunction in the brain's control of breathing.
- Heart Failure: The most common cause, often related to the heart's inability to pump enough blood efficiently.
- Stroke or Brain Tumors: Damage to the brainstem can disrupt breathing regulation.
- Kidney Failure: Can affect breathing patterns.
- Opioid Use: Certain medications, especially opioids, can suppress the brain's respiratory drive.
- High Altitude: Can induce CSA in some individuals.
Signs and Symptoms: What to Look For
Recognizing the signs and symptoms of sleep apnea is the first step toward diagnosis and treatment. While snoring is a common indicator, it's essential to look for a broader pattern of symptoms.

Common Symptoms of Sleep Apnea:
- Loud, Persistent Snoring: This is often the most noticeable symptom, especially to a bed partner. The
snoringcan be punctuated by periods of silence, followed by gasps or choking sounds. - Daytime Sleepiness (Hypersomnia): Despite sleeping for what seems like enough hours, individuals with sleep apnea often feel excessively tired, fatigued, or sleepy during the day. This can manifest as falling asleep at work, while driving, or during conversations.
- Witnessed Breathing Pauses: A bed partner may observe clear pauses in breathing, followed by gasping, choking, or snorting as breathing resumes.
- Morning Headaches: Waking up with a dull headache is common due to changes in oxygen and carbon dioxide levels in the blood overnight.
- Dry Mouth or Sore Throat in the Morning: Often a result of mouth breathing during the night.
- Irritability, Mood Swings, or Depression: Chronic sleep deprivation can significantly impact emotional regulation and mental health.
- Difficulty Concentrating or Memory Problems: Reduced cognitive function is a hallmark of disrupted sleep.
- High Blood Pressure: Sleep apnea is a significant risk factor for hypertension and can make existing high blood pressure harder to control.
- Night Sweats: Some individuals experience excessive sweating during sleep.
- Frequent Nighttime Urination (Nocturia): Can be related to the body's response to oxygen deprivation.
- Decreased Libido: Sleep disruption can affect hormone levels and overall well-being.
Pro Tip: If your bed partner regularly reports your loud snoring and observed breathing pauses, or if you consistently wake up feeling unrefreshed, it's highly recommended to discuss these symptoms with your dentist or primary care physician. They can initiate a screening for sleep apnea.
Diagnosis of Sleep Apnea
Diagnosing sleep apnea requires a comprehensive evaluation, typically involving a sleep study. While a dentist can play a crucial role in screening and identifying risk factors, the definitive diagnosis usually comes from a sleep physician.
The Diagnostic Process:
- Initial Consultation: Your dentist or physician will discuss your symptoms, medical history, and sleep habits. They might use questionnaires (like the Epworth Sleepiness Scale) and examine your mouth, throat, and neck for anatomical factors contributing to
sleep apnea. - Referral for a Sleep Study: If
sleep apneais suspected, you'll be referred to a sleep specialist for a sleep study, also known as polysomnography.- In-Lab Polysomnography (PSG): Considered the gold standard, this involves an overnight stay at a sleep center. Sensors are attached to your body to monitor brain activity (EEG), eye movements (EOG), muscle activity (EMG), heart rate (ECG), breathing effort, airflow, blood oxygen levels (oximetry), and body position. This provides a comprehensive picture of your sleep architecture and breathing patterns.
- Home Sleep Apnea Test (HSAT): A more convenient and less expensive option for individuals with a high probability of moderate to severe OSA and no significant comorbidities. You wear a simplified device at home that records fewer channels than an in-lab PSG, typically airflow, breathing effort, heart rate, and oxygen saturation. The data is then analyzed by a sleep physician.
Interpreting the Results:
The primary metric used to diagnose and assess the severity of sleep apnea is the Apnea-Hypopnea Index (AHI), which measures the average number of apneas (complete breathing cessation) and hypopneas (partial breathing reduction) per hour of sleep.
- Normal: AHI < 5
- Mild Sleep Apnea: AHI 5-15
- Moderate Sleep Apnea: AHI 15-30
- Severe Sleep Apnea: AHI > 30
Treatment Options for Sleep Apnea
Once sleep apnea is diagnosed, a range of treatment options is available, tailored to the type and severity of your condition, as well as your personal preferences and health profile. The goal is to restore normal breathing patterns during sleep and alleviate symptoms.
1. Lifestyle Changes
Often the first line of defense for mild sleep apnea or as an adjunct to other treatments.
- Weight Loss: Even a modest reduction in weight can significantly improve
sleep apneasymptoms, particularly for those with obesity. - Positional Therapy: Sleeping on your side can prevent the tongue and soft palate from collapsing into the airway. Special pillows or devices that encourage side sleeping can be helpful.
- Avoid Alcohol and Sedatives: Especially in the hours before bedtime, as they relax throat muscles.
- Quit Smoking: Smoking irritates and inflames the airways.
- Nasal Decongestants or Strips: Can help with nasal congestion, promoting nasal breathing.
2. Continuous Positive Airway Pressure (CPAP) Therapy
CPAP is the most common and generally most effective treatment for moderate to severe OSA.
- How it works: A CPAP machine delivers a continuous stream of filtered, pressurized air through a mask worn over your nose, mouth, or both. This gentle air pressure keeps your airway open, preventing collapses.
- Pros: Highly effective, quickly reduces AHI, improves daytime sleepiness and associated health risks.
- Cons: Some people find the mask uncomfortable or claustrophobic, noise from the machine (though modern ones are quiet), dry mouth/nose, cleaning requirements. Compliance can be an issue.
- Variations:
- Auto-CPAP (APAP): Automatically adjusts pressure based on your breathing needs.
- BiPAP (Bi-level Positive Airway Pressure): Delivers higher pressure when you inhale and lower pressure when you exhale, often preferred for those who struggle with CPAP or have central
sleep apnea.
``
3. Oral Appliance Therapy (OAT)
OAT involves wearing a custom-fitted dental device, similar to a mouthguard, during sleep. This is often an excellent alternative for individuals with mild to moderate OSA or those who cannot tolerate CPAP.
- Mandibular Advancement Devices (MADs): The most common type of
sleep apnea mouth guard. MADs work by gently repositioning your lower jaw (mandible) and tongue forward. This opens the airway at the back of the throat, preventing soft tissue collapse.- How they work: Custom-fitted by a dentist specializing in sleep medicine, MADs are adjustable, allowing for precise titration (fine-tuning) of the jaw position to achieve optimal airway opening.
- Pros: Non-invasive, quiet, portable, generally well-tolerated, and effective for many patients.
- Cons: Can cause temporary jaw discomfort, tooth sensitivity, or changes in bite, especially during the initial adjustment period. Requires regular follow-up with the dentist. Not suitable for all cases, especially severe OSA.
- Tongue Retaining Devices (TRDs): Less common, TRDs hold the tongue in a forward position using suction, rather than repositioning the jaw. They are an option for patients who cannot advance their jaw due to jaw joint issues or missing teeth.
Pro Tip: While you can buy mouth guards for sleep apnea online or over-the-counter (often called "boil-and-bite" guards), these are not recommended for treating diagnosed sleep apnea. They lack the custom fit and adjustability of a professional MAD, can be uncomfortable, ineffective, and may even cause dental or jaw joint problems over time. Always consult with a qualified dentist for a custom-fitted best mouth guard for sleep apnea.
4. Surgical Options
Surgery is typically reserved for patients who cannot tolerate or benefit from CPAP or OAT, or in cases where there is a clear anatomical obstruction that can be corrected.
- Uvulopalatopharyngoplasty (UPPP): Removes excess tissue from the back of the throat, including part of the soft palate and uvula.
- Tonsillectomy and Adenoidectomy: Often highly effective for children with OSA caused by enlarged tonsils and adenoids. Can also be considered in adults.
- Genial Advancement/Hyoid Suspension: Procedures to move the lower jaw bone or hyoid bone forward, tightening the soft tissues around the airway.
- Maxillomandibular Advancement (MMA): A more extensive surgery that moves both the upper and lower jaws forward, significantly enlarging the airway. Highly effective but involves a longer recovery.
- Nasal Surgery: To correct issues like a deviated septum or remove polyps that impede nasal breathing.
5. Newer Therapies
- Hypoglossal Nerve Stimulation (e.g., Inspire): An implantable device that stimulates the hypoglossal nerve, which controls tongue movement, to keep the airway open during sleep. It's typically for moderate to severe OSA patients who have failed CPAP.
6. Mouth Tape for Snoring
Mouth tape for snoring has gained popularity, but it's important to understand its limitations.
- How it works: Mouth tape is designed to encourage nasal breathing by keeping the lips sealed during sleep.
- Target Use: Primarily for simple
snoringcaused by mouth breathing, or for individuals looking to enhance nasal breathing benefits. - Limitations: It does not treat
sleep apnea. If your airway is collapsing internally, mouth tape will not prevent this. Using it with undiagnosedsleep apneacould be dangerous by preventing you from gasping for air. - Pros: Inexpensive, non-invasive for simple snoring.
- Cons: Not a treatment for
sleep apnea, can cause skin irritation, potential for anxiety or discomfort. - Recommendation: If you
snore, get evaluated forsleep apneabefore trying mouth tape.
Step-by-Step Process for Oral Appliance Therapy (OAT)
If you're considering a mouth guard for sleep apnea, here's what to expect:

- Initial Consultation & Screening: Your dentist will conduct a thorough oral examination, review your sleep study results, and discuss your symptoms and medical history. They'll assess your jaw, teeth, and airway to determine if you're a good candidate for an oral appliance.
- Impressions & Records: If OAT is suitable, the dentist will take precise impressions of your teeth and gums, along with bite registrations, using digital scans or physical molds. This ensures a custom fit. They may also take X-rays or photographs.
- Appliance Fabrication: The impressions and records are sent to a specialized dental lab, where a custom
mandibular advancement device(MAD) is fabricated. This process typically takes 2-4 weeks. - Fitting & Initial Adjustment: You'll return to the dentist for the initial fitting. The dentist will ensure the appliance fits comfortably and securely. They will then adjust the jaw position to a starting point, usually by advancing the lower jaw by a few millimeters. You'll receive instructions on how to insert, remove, and care for your device.
- Titration & Follow-Up: This is a crucial phase. You'll wear the appliance at home and gradually adjust the advancement of your lower jaw (usually in very small increments) over several weeks, under the guidance of your dentist. This titration process is designed to find the optimal jaw position that eliminates
sleep apneaevents without causing excessive discomfort. Regular follow-up appointments (e.g., every 2-4 weeks initially) are necessary for adjustments and to monitor for any side effects like jaw pain-jaw-disorders-everything-you-need-to-know "Complete Guide to TMJ & Jaw Disorders: Everything You Need to Know") or bite changes. - Efficacy Check (Repeat Sleep Study): Once an optimal position is found and you've adapted to the appliance, your dentist or sleep physician may recommend a follow-up sleep study (often a home sleep test) with the appliance in place. This confirms the effectiveness of the device in reducing your AHI.
- Ongoing Care: You'll need periodic dental check-ups (typically every 6-12 months) to ensure the appliance is still fitting correctly, is effective, and to monitor your oral health for any changes in bite or TMJ issues. The lifespan of a custom oral appliance is generally 3-5 years, after which it may need replacement.
``
Cost and Insurance: US Price Ranges
The cost of sleep apnea diagnosis and treatment can vary significantly based on the type of test, chosen therapy, geographic location, and insurance coverage.
Diagnostic Costs (US Averages):
- Home Sleep Apnea Test (HSAT):
- Without insurance: $250 - $700
- With medical insurance: Often fully covered or subject to copay/deductible, reducing out-of-pocket to $50 - $200.
- In-Lab Polysomnography (PSG):
- Without insurance: $2,000 - $5,000+
- With medical insurance: Often largely covered, with patient responsibility ranging from $200 - $1,500 depending on deductible, coinsurance, and facility fees.
Treatment Costs (US Averages):
| Treatment Option | Without Insurance (Self-Pay) | With Medical Insurance (Est. Patient Share) | Notes |
|---|---|---|---|
| CPAP Machine | $500 - $2,000 (basic to advanced) | $100 - $500 (after deductible/coinsurance) | Includes humidifier, but masks ($100-$300 each) and supplies (tubing, filters, cushions - $50-$150/month) are ongoing costs. Often classified as Durable Medical Equipment (DME). |
| Custom Oral Appliance (MAD) | $2,000 - $5,000 | $500 - $2,500 | Typically covered under medical insurance (not dental) as an alternative to CPAP. Includes fabrication, fitting, and initial adjustments. Follow-up adjustments may incur minor fees. |
| OTC "Boil-and-Bite" Mouthguard | $20 - $150 | Not covered | Not recommended for sleep apnea treatment. Only for temporary snoring relief, and can cause dental issues. |
| Uvulopalatopharyngoplasty (UPPP) | $5,000 - $15,000+ | $1,000 - $5,000+ | Varies widely by facility, complexity, and region. Often requires prior authorization and may have high deductibles. |
| Maxillomandibular Advancement (MMA) | $25,000 - $75,000+ | $5,000 - $15,000+ | Major surgery; patient share will depend heavily on the specifics of the insurance plan and overall healthcare costs. |
| Hypoglossal Nerve Stimulation (Inspire) | $20,000 - $40,000 (device + surgery) | $2,000 - $8,000+ | Generally covered by major medical insurers for specific criteria (moderate-severe OSA, CPAP failure, certain BMI limits). Requires significant prior authorization. |
Insurance Coverage Details:
- Medical Insurance is Key: For
sleep apneadiagnosis and most treatments (CPAP, oral appliances, surgery), your medical insurance is the primary payer, not your dental insurance.Sleep apneais considered a medical condition. - Durable Medical Equipment (DME): CPAP machines and supplies are typically covered under the DME benefit of your medical insurance. Be aware of rental agreements vs. purchase options.
- Oral Appliance Coverage: Many medical insurance plans (including Medicare and some Medicaid plans) now cover custom oral appliances, recognizing them as an effective treatment for
sleep apnea. However, the dentist providing the OAT must be an approved medical provider and usually needs specific training and credentials in dental sleep medicine. Always confirm coverage with your medical insurance provider prior to treatment. - Prior Authorization: For many
sleep apneatreatments, especially oral appliances and surgery, your insurance company will require prior authorization from your physician and/or dentist. This means they need to approve the treatment plan before it begins.
Pro Tip: Always call your medical insurance provider directly to understand your specific benefits, deductibles, copayments, and whether a sleep study and specific treatments (like a sleep apnea mouth guard) are covered. Ask for clarification on whether they cover "Durable Medical Equipment" for CPAP and "Oral Appliance Therapy" for sleep apnea.
Recovery and Aftercare
Successful sleep apnea treatment isn't just about initiating therapy; it's about consistent adherence and proper aftercare.
For CPAP Users:
- Regular Cleaning: Masks, tubing, and humidifiers must be cleaned daily or weekly according to manufacturer instructions to prevent bacterial growth and maintain hygiene.
- Mask Fit and Comfort: If you experience leaks, skin irritation, or discomfort, work with your sleep specialist or DME provider to find a better mask fit or type. There are many options available (nasal pillows, nasal masks, full face masks).
- Humidification: Using a humidifier with your CPAP can alleviate dry mouth and nasal passages.
- Compliance Monitoring: Many CPAP machines record usage data. Your sleep physician will review this periodically to ensure effective treatment.
For Oral Appliance Therapy (OAT) Users:
- Appliance Cleaning: Clean your
sleep apnea mouth guarddaily with a soft toothbrush and mild soap or a specialized dental appliance cleaner. Avoid abrasive toothpastes. - Oral Hygiene: Continue your regular brushing and flossing routine. Remove the appliance for oral care.
- Temporary Side Effects: You might experience some temporary jaw soreness, tooth sensitivity, excessive salivation, or a slight change in your bite when you first remove the appliance in the morning. These usually resolve within 30-60 minutes. Your dentist can provide exercises or adjustments to help mitigate these.
- Regular Dental Check-ups: It's crucial to have regular check-ups (typically every 6-12 months) with the dentist who provided your
mandibular advancement device. They will check for proper fit, wear, and tear, and monitor for any long-term changes to your bite or TMJ (temporomandibular joint) health. - Appliance Longevity: A custom MAD typically lasts 3-5 years, but this can vary depending on care and individual wear patterns.
Prevention of Sleep Apnea
While some risk factors for sleep apnea (like anatomy or genetics) are beyond your control, many can be managed or prevented through lifestyle choices.

- Maintain a Healthy Weight: This is one of the most impactful preventative measures. Losing even 10-15% of body weight can significantly reduce or eliminate
sleep apneain some individuals. - Adopt Healthy Sleep Habits:
- Sleep on Your Side: Avoid sleeping on your back if you are prone to
snoringor mildsleep apnea. - Consistent Sleep Schedule: Go to bed and wake up at the same time each day, even on weekends.
- Create a Conducive Sleep Environment: Dark, quiet, cool room.
- Sleep on Your Side: Avoid sleeping on your back if you are prone to
- Avoid Alcohol and Sedatives: Especially in the evening, as they relax throat muscles.
- Quit Smoking: Smoking contributes to inflammation and fluid retention in the airway.
- Manage Nasal Congestion: Address allergies or chronic sinus issues that make nasal breathing difficult. Consult an ENT for persistent issues like a deviated septum.
- Stay Physically Active: Regular exercise can improve muscle tone, including those in the airway.
Risks and Complications of Untreated Sleep Apnea
Ignoring sleep apnea isn't just about feeling tired; it poses significant risks to your long-term health and well-being.
- Cardiovascular Problems:
- High Blood Pressure (Hypertension):
Sleep apneacan cause sudden drops in blood oxygen levels, increasing blood pressure and straining the cardiovascular system. - Heart Attack and Stroke: Untreated
sleep apneasignificantly increases the risk of recurrent heart attack, stroke, and abnormal heartbeats (arrhythmias) like atrial fibrillation. - Heart Failure: Can worsen existing heart failure and increase the risk of developing it.
- High Blood Pressure (Hypertension):
- Type 2 Diabetes:
Sleep apneacontributes to insulin resistance, increasing the risk of developing Type 2 diabetes. - Increased Risk of Accidents: Chronic daytime sleepiness drastically impairs concentration, reaction time, and alertness, increasing the risk of car accidents and workplace errors.
- Metabolic Syndrome: A cluster of conditions — increased blood pressure, high blood sugar, excess body fat around the waist, and abnormal cholesterol levels — that occur together, increasing your risk of heart disease, stroke, and diabetes.
Sleep apneais a major contributor. - Liver Problems: Non-alcoholic fatty liver disease (NAFLD) is more common in individuals with
sleep apnea. - Surgical Complications: People with
sleep apneaare at higher risk of complications after surgery due to breathing problems, especially when sedated and lying on their back. - Quality of Life: Beyond physical health,
sleep apneacan severely impact mood, relationships (due tosnoringand irritability), job performance, and overall mental health.
``
Potential Complications from Treatments:
- CPAP: Skin irritation from masks, dry mouth/nose, aerophagia (swallowing air), claustrophobia, noise intolerance.
- Oral Appliance Therapy: Temporary jaw joint discomfort (TMJ pain), tooth sensitivity, changes in bite, increased salivation. Long-term, rare cases of irreversible bite changes or TMJ issues if not properly managed by an experienced dentist.
- Surgery: Infection, bleeding, pain, voice changes, difficulty swallowing, failed outcome requiring further treatment.
Comparison Tables
Here are two comparison tables to help you understand your treatment options better:
Comparison: CPAP vs. Oral Appliance Therapy (OAT) for OSA
| Feature | CPAP (Continuous Positive Airway Pressure) | Oral Appliance Therapy (OAT) - Mandibular Advancement Device (MAD) |
|---|---|---|
| Effectiveness | Highly effective for moderate to severe OSA; "gold standard." | Highly effective for mild to moderate OSA; good alternative for severe OSA patients who can't tolerate CPAP. |
| Mechanism | Delivers pressurized air to keep airway open. | Repositions jaw and tongue forward to open airway. |
| Comfort/Portability | Requires mask, machine, tubing; less portable; some find restrictive/noisy. | Custom-fitted device worn in mouth; highly portable, quiet, less obtrusive. |
| Compliance | Can be challenging due to mask fit, claustrophobia, dry mouth (average ~60-70%). | Generally higher compliance due to comfort and ease of use (average ~80%). |
| Side Effects | Dry mouth/nose, skin irritation, aerophagia, noise. | Temporary jaw discomfort, tooth sensitivity, changes in bite, excessive salivation. Rare long-term bite changes. |
| Maintenance | Regular cleaning of mask, tubing, humidifier; replacement of supplies (filters). | Daily cleaning of appliance; regular dental check-ups (6-12 months). |
| Cost (Estimated) | Machine: $500-$2000; Supplies: $50-$150/month. Covered by medical insurance (DME). | Device: $2,000-$5,000. Often covered by medical insurance. |
| Dental Impact | Minimal direct dental impact. | Potential for minor tooth movement or bite changes over time; requires dental monitoring. |
Comparison: Custom Oral Appliance vs. Over-the-Counter Mouthguards for Snoring/Sleep Apnea
| Feature | Custom Mandibular Advancement Device (MAD) (Prescribed by Dentist) | OTC "Boil-and-Bite" Mouthguard (e.g., for snoring) |
|---|---|---|
| Fit & Customization | Precision custom-fitted to your unique dental anatomy. | Generic, self-molded; not truly custom, often bulky. |
| Adjustability | Micro-adjustable jaw advancement, allowing for titration. | Little to no adjustment once molded. |
| Effectiveness for OSA | Clinically proven for mild-moderate OSA. | Not recommended for diagnosed OSA; minimal or no clinical evidence. |
| Effectiveness for Snoring | Very effective for snoring. | Can reduce simple snoring caused by mouth breathing, limited effectiveness for airway collapse. |
| Safety & Side Effects | Designed by a professional; side effects managed by dentist. | Can exacerbate TMJ issues, cause tooth movement, or worsen sleep apnea if misused. |
| Cost (Estimated) | $2,000 - $5,000 (often medical insurance covered). | $20 - $150 (not insurance covered). |
| Longevity | 3-5 years with proper care. | Weeks to months. |
| Professional Oversight | Essential for fitting, adjustment, and follow-up. | None. User-dependent. |
Children / Pediatric Considerations
Sleep apnea isn't just an adult problem; it affects children too, often with different causes and symptoms. Pediatric sleep apnea affects an estimated 1-5% of children.

Causes in Children:
- Enlarged Tonsils and Adenoids: This is by far the most common cause of OSA in children.
- Obesity: Increasing prevalence in children is a growing risk factor.
- Craniofacial Anomalies: Conditions like Down syndrome, Pierre Robin sequence, or cerebral palsy can lead to anatomical airway obstructions.
- Neuromuscular Disorders: Can affect muscle tone in the airway.
Signs and Symptoms in Children:
Symptoms can be subtle and often differ from adults.
- Loud
Snoring: Still a primary indicator. - Pauses in Breathing: Witnessed by parents.
- Restless Sleep: Tossing and turning, unusual sleeping positions (e.g., hyperextending the neck).
- Mouth Breathing: Especially during sleep.
- Bedwetting (Enuresis): More common in children with
sleep apnea. - Daytime Behavioral Issues: Unlike adults who often show sleepiness, children may present with hyperactivity, irritability, difficulty concentrating, or aggression (often misdiagnosed as ADHD).
- Poor School Performance: Due to chronic sleep deprivation.
- Slow Growth or Weight Gain (Failure to Thrive): In severe cases.
Treatment in Children:
- Tonsillectomy and Adenoidectomy: This is the first-line treatment for most children with OSA caused by enlarged tissues and is highly effective.
- Orthodontic Treatment/Palatal Expansion: For children with narrow dental arches or recessed jaws, orthodontists can use appliances to widen the palate and jaws, which can significantly open the airway.
- Weight Management: For obese children.
- CPAP: Used for children when surgery isn't an option or hasn't been fully effective, especially in those with craniofacial anomalies or severe OSA.
- Oral Appliances: Custom-made oral appliances may be considered for older children or adolescents with mild to moderate OSA who cannot undergo surgery or use CPAP.
Pro Tip for Parents: If your child snores regularly, gasps during sleep, or exhibits behavioral issues, discuss this with your pediatrician or pediatric dentist. Early diagnosis and treatment are vital for a child's development, health, and academic success. The American Academy of Pediatrics recommends screening for snoring in all children.
Cost Breakdown: Average US Costs
To further consolidate, here's a general breakdown of the average costs associated with sleep apnea care in the US. Remember, these are estimates, and actual costs can vary significantly by region, provider, and insurance plan.
| Service/Item | Average Low (Self-Pay) | Average Mid (Self-Pay) | Average High (Self-Pay) | Average Patient Share (with Medical Insurance) |
|---|---|---|---|---|
| Initial Sleep Consult | $150 | $250 | $400 | $30 - $80 (copay/coinsurance) |
| Home Sleep Test (HSAT) | $250 | $500 | $700 | $50 - $200 |
| In-Lab Sleep Study (PSG) | $2,000 | $3,500 | $5,000+ | $200 - $1,500 |
| CPAP Machine (Basic) | $500 | $1,000 | $2,000 | $100 - $500 |
| CPAP Mask (Replacement) | $100 | $200 | $300 | $20 - $80 |
| CPAP Supplies (Monthly) | $50 | $100 | $150 | $10 - $30 |
| Custom Oral Appliance (MAD) | $2,000 | $3,500 | $5,000 | $500 - $2,500 |
| Tonsillectomy/Adenoidectomy | $3,000 | $7,000 | $10,000+ | $500 - $3,000+ |
| UPPP Surgery | $5,000 | $10,000 | $15,000+ | $1,000 - $5,000+ |
Payment Plans and Financing Options:
- Dental/Medical Office Payment Plans: Many dental and medical offices offer in-house payment plans, allowing you to pay for treatments like oral appliances in installments.
- Third-Party Financing: Companies like CareCredit or Alphaeon Credit offer specialized healthcare credit cards with deferred interest options for medical and dental expenses.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): These tax-advantaged accounts are excellent for covering
sleep apneadiagnostic and treatment costs. - Non-Profit Organizations: Some organizations may offer assistance programs, especially for those with severe financial hardship, though this is less common for
sleep apneaspecifically.
Cost-Saving Tips:
- Verify Insurance Coverage: Always call your medical insurance provider to understand what's covered before any procedure or purchase. Ask about in-network providers to minimize costs.
- Get Multiple Quotes: Especially for services like custom oral appliances, compare pricing from different qualified dentists in your area.
- Ask About Bundled Pricing: Some providers may offer a single price that includes the appliance, fitting, and initial follow-up adjustments.
- Consider Home Sleep Tests: If appropriate for your case, an HSAT is significantly less expensive than an in-lab study.
- Utilize HSAs/FSAs: Maximize contributions to these accounts to pay for healthcare costs with pre-tax dollars.
Frequently Asked Questions
1. What exactly is the difference between snoring and sleep apnea?
Snoring is the sound produced when air is partially obstructed as it passes through the relaxed tissues in your throat during sleep. While disruptive, it doesn't always indicate a medical problem. Sleep apnea, however, is a serious medical condition where breathing repeatedly stops and starts for 10 seconds or more. While most people with sleep apnea snore, not everyone who snores has sleep apnea. The key difference is the complete or near-complete cessation of breathing, leading to oxygen deprivation.
2. Can a dentist treat sleep apnea?
Yes, dentists play a crucial role in screening for sleep apnea and providing certain treatments. While diagnosing sleep apnea typically requires a sleep physician and a sleep study, a qualified dentist specializing in dental sleep medicine can custom-fit and manage oral appliance therapy (OAT), such as a mandibular advancement device, for patients with mild to moderate OSA, or for those with severe OSA who cannot tolerate CPAP.
3. How long does it take to get used to a sleep apnea mouth guard?
Adjusting to a sleep apnea mouth guard typically takes a few weeks to a couple of months. You might experience temporary side effects like jaw soreness, tooth sensitivity, or increased salivation initially. These usually subside as your mouth adapts. Your dentist will work with you through a "titration" process, gradually adjusting the device until the optimal, comfortable position is found.
4. Is oral appliance therapy painful?
Oral appliance therapy is generally not painful, but you may experience some discomfort, soreness in your jaw muscles, or tooth tenderness, especially during the first few weeks of use or after an adjustment. This is usually mild and temporary. If you experience persistent or severe pain, it's crucial to contact your dentist immediately, as adjustments may be needed.
5. Are there any alternatives to CPAP for severe sleep apnea?
Yes, while CPAP is the gold standard for severe sleep apnea, alternatives exist for those who cannot tolerate it. These include custom oral appliances (mandibular advancement device), various surgical options (such as UPPP, genial advancement, or maxillomandibular advancement), and newer therapies like hypoglossal nerve stimulation (e.g., Inspire). The best alternative depends on your specific anatomy, severity, and overall health, and should be discussed with a sleep physician.
6. Can lifestyle changes really help with sleep apnea?
For mild sleep apnea or as an adjunct to other treatments, lifestyle changes can be very effective. Losing even a modest amount of weight, avoiding alcohol and sedatives before bed, and sleeping on your side can significantly reduce the frequency and severity of breathing disruptions. Quitting smoking also plays a vital role in reducing airway inflammation.
7. How often do I need to replace my sleep apnea mouth guard?
A custom sleep apnea mouth guard is durable and typically lasts between 3 to 5 years with proper care and cleaning. However, the exact lifespan can vary depending on factors like how well you maintain it, the materials used, and whether you grind your teeth at night. Your dentist will assess its condition during your regular follow-up appointments.
8. Does mouth tape for snoring treat sleep apnea?
No, mouth tape for snoring does not treat sleep apnea. It's designed to encourage nasal breathing by keeping your mouth closed, which can reduce simple snoring caused by mouth breathing. However, it does not address the underlying physical collapse of the airway that causes sleep apnea. If you have sleep apnea, mouth taping could potentially be dangerous by preventing you from opening your mouth to gasp for air during an apneic event. Always consult a professional for sleep apnea diagnosis and treatment.
9. What's the role of my primary care doctor in sleep apnea?
Your primary care doctor is often the first point of contact for sleep apnea concerns. They can assess your symptoms, discuss risk factors, order initial screenings, and provide referrals to sleep specialists for a definitive diagnosis and comprehensive treatment plan. They also manage any related health conditions like high blood pressure or diabetes.
10. Can untreated sleep apnea lead to serious health problems?
Absolutely. Untreated sleep apnea significantly increases your risk for a multitude of serious health issues, including high blood pressure, heart attack, stroke, irregular heartbeats, Type 2 diabetes, metabolic syndrome, and even certain cancers. It also impairs cognitive function, increases accident risk, and severely diminishes quality of life. Prompt diagnosis and treatment are crucial for preventing these complications.
When to See a Dentist
While a sleep physician is essential for diagnosing sleep apnea, your dentist plays a vital role in the screening process and often in treatment through oral appliance therapy. Here's when you should definitely see a dentist:
- If you snore loudly and frequently: Especially if your
snoringis disruptive to others or if your bed partner notices pauses in your breathing followed by gasps or choking sounds. - If you experience chronic daytime fatigue: Even if you think you're getting enough sleep, persistent tiredness, difficulty concentrating, or morning headaches warrant a discussion with your dentist.
- If you're considering a
sleep apnea mouth guard: A qualified dentist is essential for determining if you're a candidate for oral appliance therapy, taking precise impressions, custom-fitting the device, and managing adjustments. - If you've been diagnosed with mild to moderate
sleep apnea: Your dentist can discuss oral appliance therapy as an effective alternative or complement to CPAP. - If you cannot tolerate CPAP: Your dentist can evaluate you for an oral appliance as a viable alternative for
sleep apneamanagement. - If you have dental issues that could contribute to
sleep apnea: A dentist can assess conditions like a small jaw, crowded teeth, or bite problems that might impact your airway.
Red Flags vs. Routine Care Guidance:
- Routine Care: Discussing any
snoringor fatigue during your regular dental check-ups is always a good idea. Your dentist can screen for risk factors. - Red Flags/Scheduled Appointment: If you consistently experience loud
snoringwith witnessed breathing pauses, severe daytime sleepiness, or morning headaches, don't wait for your next routine cleaning. Schedule an appointment specifically to discusssleep apneascreening with your dentist or physician. - Emergency: While
sleep apneaitself doesn't typically present as a dental emergency, sudden and severe difficulty breathing during the day, accompanied by chest pain or confusion, requires immediate medical attention (call 911). If an oral appliance causes severe, unrelenting pain or damage, contact your dentist's office as soon as possible.
Remember, early detection and treatment of sleep apnea are paramount to safeguarding your long-term health and improving your quality of life. Your dental professional can be a key partner in this journey.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
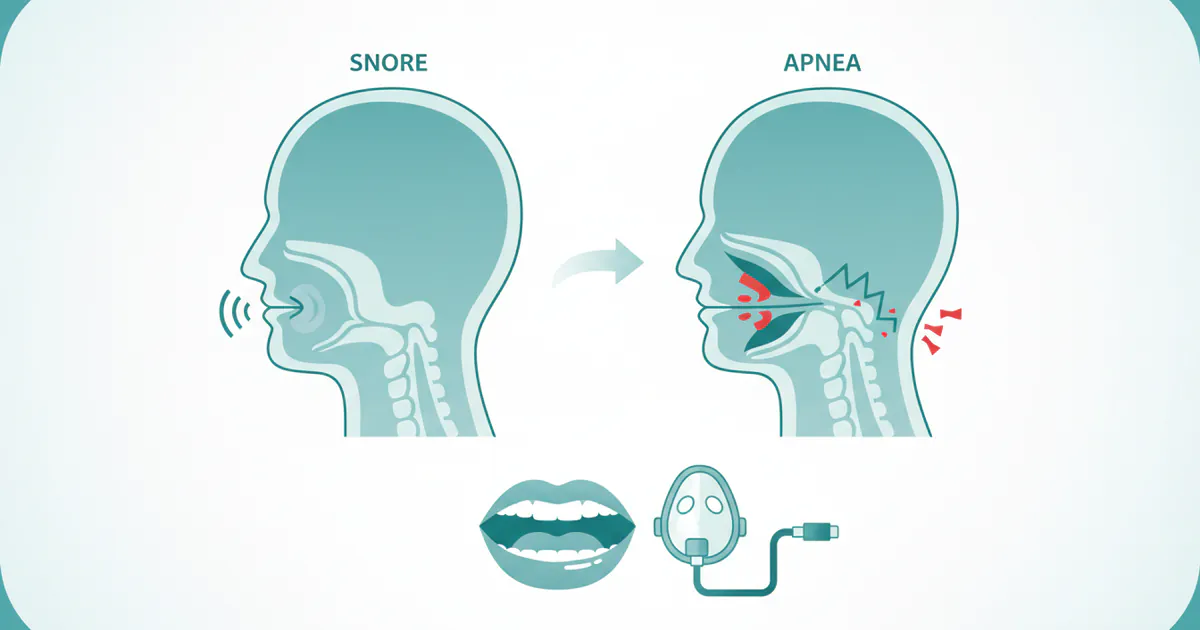
Difference Between Snoring and Sleep Apnea: Complete Guide
More than 80 million Americans regularly snore, and while often dismissed as a mere nuisance, loud and persistent snoring can be a critical indicator of a much more serious underlying health condition: sleep apnea. The difference between snoring and sleep apnea is profound, impacting not just yo
February 23, 2026

Mouth Taping for Snoring: Complete Guide
Snoring. It's the nocturnal soundtrack for millions of Americans, often a source of frustration for bed partners and a potential indicator of underlying health issues for the snorer themselves. Roughly 45% of adults snore occasionally, and 25% are habitual snorers, impacting sleep quality, relat
February 23, 2026
Is All Snoring Sleep Apnea
Many individuals, perhaps even you or a loved one, have been told they snore loudly. It's often dismissed as a harmless, albeit annoying, nocturnal habit. However, what if that nightly rumble is more than just noise? What if it's a critical indicator of an underlying health condition that significan
February 23, 2026
Cpap Dry Mouth Even With Humidifier: Complete Guide
Experiencing dry mouth while using a CPAP machine, even with a humidifier, is a common and incredibly frustrating issue for millions of Americans. It can disrupt sleep, diminish the effectiveness of your sleep apnea treatment, and significantly impact your oral health. Imagine waking up every mornin
February 23, 2026