Cpap Dry Mouth Even With Humidifier: Complete Guide
Key Takeaways
- Experiencing dry mouth while using a CPAP machine, even with a humidifier, is a common and incredibly frustrating issue for millions of Americans. It can disrupt sleep, diminish the effectiveness of your sleep apnea treatment, and significantly impact your oral health. Imagine waking up every mornin
Cpap Dry Mouth Even With Humidifier: Complete Guide
Experiencing dry mouth while using a CPAP machine, even with a humidifier, is a common and incredibly frustrating issue for millions of Americans. It can disrupt sleep, diminish the effectiveness of your sleep apnea treatment, and significantly impact your oral health. Imagine waking up every morning with your mouth feeling like sandpaper, your throat parched, and an uncomfortable taste lingering – despite diligently using your CPAP machine as prescribed and ensuring its humidifier is filled. This persistent problem, often referred to as xerostomia, affects an estimated 30-50% of CPAP users, leading to discomfort, poor adherence to therapy, and serious long-term dental complications. Understanding the root causes of CPAP dry mouth even with a humidifier and knowing the effective strategies to combat it is crucial for maintaining both your overall health and the success of your sleep apnea treatment. This comprehensive guide will explore why this happens, the range of solutions available, and how you can achieve a truly restful and comfortable night's sleep.

Key Takeaways:
- Mouth Breathing is Key: The primary reason for CPAP dry mouth, even with a humidifier, is often unintentional mouth breathing, leading to air bypassing the humidified nasal passages.
- Mask Fit Matters: Leaky CPAP masks, especially ill-fitting nasal or full-face masks, allow air to escape and dry out the mouth and throat.
- Humidifier Settings: Incorrect humidifier temperature or humidity levels, or using distilled water, can render the device ineffective.
- Dental Solutions: Custom oral appliances, like mouth guard snoring devices designed to keep the mouth closed or advance the jaw, can significantly reduce dry mouth and improve CPAP adherence (costs $500-$3,000 for custom dental appliances).
- Comprehensive Approach: Effective solutions involve a combination of CPAP adjustments (mask, settings), behavioral changes (hydration, sleep position), and dental interventions, often requiring collaboration between your sleep physician and dentist.
- Long-Term Risks: Untreated chronic dry mouth increases risks of tooth decay, gum disease, oral infections, and can lead to early tooth loss, necessitating vigilant oral hygiene and regular dental check-ups (costs for treatments like fillings can range from $150-$450 per tooth).
- Troubleshooting Timeline: Expect to troubleshoot and find effective solutions within 2-6 weeks through careful adjustments and professional consultations.
What It Is / Overview: Understanding CPAP Dry Mouth
Xerostomia, commonly known as dry mouth, is a condition characterized by a decrease in saliva production, leading to a persistent feeling of dryness in the mouth. When this occurs in individuals using Continuous Positive Airway Pressure (CPAP) therapy, it's specifically referred to as CPAP dry mouth. While CPAP machines are equipped with humidifiers designed to add moisture to the pressurized air, many users still experience significant dryness.
The primary function of CPAP therapy is to keep the airway open during sleep, preventing episodes of apnea and hypopnea that characterize sleep apnea. The machine delivers a continuous stream of pressurized air through a mask. A humidifier, integrated into or attached to the CPAP device, works by heating distilled water to create moisture, which is then delivered with the air to prevent the drying of nasal passages and throat. However, the complexity of human physiology and device interaction means this system isn't always foolproof.
Chronic dry mouth, regardless of its cause, has significant health implications. Saliva plays a vital role in maintaining oral health. It neutralizes acids produced by bacteria, washes away food particles, aids in digestion, protects against microbial growth, and helps remineralize tooth enamel. A lack of saliva leaves the mouth vulnerable to increased rates of tooth decay (cavities), gum disease (gingivitis and periodontitis), fungal infections (thrush), bad breath (halitosis), difficulty speaking and swallowing, and general discomfort. For CPAP users, this can lead to a vicious cycle: discomfort from dry mouth reduces adherence to CPAP therapy, which in turn compromises sleep apnea treatment and overall health.
Types / Variations: Exploring CPAP Masks and Humidifier Technologies
Understanding the different components of your CPAP setup is critical to identifying potential sources of dry mouth.
CPAP Mask Types
The type of CPAP mask you use directly influences the likelihood and severity of dry mouth:
- Nasal Masks: These masks cover only the nose, sealing around the nostrils or the bridge of the nose.
- Pros: Less claustrophobic, good for those who breathe through their nose.
- Cons: Highly prone to dry mouth if the user unconsciously opens their mouth during sleep, allowing pressurized, humidified air to escape through the mouth instead of going into the lungs via the nasal passages. This "mouth leak" dries out the oral cavity significantly.
- Nasal Pillow Masks: These feature small cushions that fit directly into the nostrils.
- Pros: Minimal contact, very lightweight, excellent for claustrophobia.
- Cons: Similar to nasal masks, they are very susceptible to dry mouth if mouth breathing occurs. The smaller contact area can sometimes make them less stable with significant movement.
- Full-Face Masks: These masks cover both the nose and mouth.
- Pros: Ideal for mouth breathers or those with nasal congestion/obstruction, as they deliver air to both passages. They typically reduce the direct issue of mouth breathing drying out the mouth.
- Cons: Can still cause dry mouth if the mask itself is leaky, if the mouth cavity is simply being dried out by constant airflow, or if the individual's natural salivary flow is low. Some users find them more restrictive or prone to pressure marks.
- Hybrid Masks: A combination of nasal pillows and an oral cushion.
- Pros: Offers some benefits of both, can be less bulky than a full face mask while accommodating mouth breathing.
- Cons: Can still be prone to leaks if not fitted correctly, leading to dry mouth.
Humidifier Technologies
Modern CPAP machines almost universally come with integrated heated humidifiers. These are far more effective than older "pass-over" humidifiers which simply allowed air to pass over a water reservoir without heating.
- Heated Humidifiers: These units heat distilled water to a user-selected temperature, increasing the moisture content of the air delivered by the CPAP machine.
- Pros: Most effective at adding moisture to the air, preventing dryness in the nasal passages and throat.
- Cons: Requires distilled water, can run out of water during the night if the reservoir is too small or settings are too high, can sometimes be too humid leading to "rainout" (condensation in the tubing).
- Climate Control/Heated Tubing: Many advanced CPAP machines offer "climate control" features, often involving heated tubing.
- Pros: Prevents "rainout" by maintaining a consistent temperature along the entire length of the tubing, ensuring the humidified air reaches the mask without losing moisture through condensation. This allows higher humidity settings without discomfort.
- Cons: Adds to the cost and complexity of the setup, requires specific heated tubing compatible with the CPAP machine.
Causes / Why It Happens Even With Humidifier
The frustration of CPAP dry mouth even with a humidifier stems from a multi-faceted interplay of factors. While the humidifier is designed to prevent dryness, several issues can bypass or overwhelm its effectiveness.
1. Unintentional Mouth Breathing
This is by far the most common culprit. Even with a nasal or nasal pillow mask and a fully functioning humidifier, if you instinctively open your mouth during sleep, the pressurized, humidified air from the CPAP machine enters through your nose but then escapes directly through your open mouth. This creates a "wind tunnel" effect, rapidly drying out your oral cavity. * Causes of Mouth Breathing: * Nasal Congestion: Allergies, colds, deviated septum, or chronic sinusitis can force you to breathe through your mouth. * Muscle Relaxation: During deep sleep, the muscles of the jaw and tongue relax, leading to the mouth falling open. * High CPAP Pressure: Sometimes, higher CPAP pressures can make nasal breathing feel difficult, prompting mouth opening.
2. Mask Leaks
An improperly fitting mask, regardless of its type, can significantly contribute to dry mouth. * How it happens: If air leaks out from around the edges of your mask, it's not being delivered efficiently to your airway. This leaking air can blow across your mouth, eyes, and face, leading to localized dryness. * Causes of Leaks: * Wrong Size/Shape: A mask that's too large or too small, or not suited to your facial anatomy. * Worn-out Seal: Silicone cushions degrade over time and lose their sealing ability. * Improper Strapping: Overtightening can cause creases and leaks; undertightening doesn't create a seal. * Sleep Position: Sleeping on your side or stomach can shift the mask and create leaks.
3. Inadequate Humidifier Settings or Malfunction
Even with a humidifier, its settings might not be optimized for your individual needs or the environmental conditions. * Low Humidity Setting: The machine might be set to a level that simply isn't sufficient for your body's needs, especially in dry climates or during winter months. * Water Reservoir Issues: Not filling the reservoir enough, or the reservoir running dry halfway through the night. * Humidifier Malfunction: A faulty heating element or sensor in the humidifier can prevent it from adequately moisturizing the air. * Lack of Heated Tubing: Without heated tubing, warm, humidified air can cool as it travels to the mask, leading to "rainout" (condensation) in the tubing and reducing the actual humidity delivered to your airway.
4. Medical Conditions and Medications
Several non-CPAP related factors can exacerbate or directly cause dry mouth, making it worse when combined with CPAP therapy. * Dehydration: Simply not drinking enough water throughout the day can lead to systemic dehydration and dry mouth at night. * Medications: Many common medications have dry mouth as a side effect, including antihistamines, decongestants, antidepressants, anti-anxiety drugs, blood pressure medications, and diuretics. * Systemic Diseases: Conditions like diabetes, Sjögren's syndrome, rheumatoid arthritis, and autoimmune diseases can reduce salivary gland function. * Radiation Therapy: Head and neck radiation can permanently damage salivary glands. * Nerve Damage: Injury to the head or neck can affect nerves controlling salivary glands.
5. Oral Health and Appliances
Certain oral factors can contribute to or worsen dry mouth. * Poor Oral Hygiene: A mouth already prone to bacteria and inflammation might feel drier. * Dental Appliances: While some oral appliances, like custom mouth guard snoring devices, are designed to prevent mouth breathing, poorly fitting ones or certain designs could potentially interfere with normal salivary flow for some individuals, though this is less common than CPAP-induced dry mouth. If you use a mouth guard snoring device in conjunction with CPAP, ensure it's professionally fitted and adjusted.
6. Environmental Factors
The environment in your bedroom can play a role. * Low Room Humidity: A very dry bedroom environment, especially with heating or air conditioning running, can "pull" moisture from your body and your CPAP's humidified air. * Room Temperature: If the room is too cold, the humidified air from the CPAP might cool too quickly, leading to condensation in the tube before it reaches your mask, thus reducing delivered humidity.
Signs and Symptoms: What to Look For
Recognizing the signs of CPAP dry mouth is the first step toward finding a solution. These symptoms can range from merely annoying to severely impacting your daily life and long-term health.

Oral Symptoms:
- Persistent Dry Sensation: The most obvious symptom, feeling like your mouth is constantly parched, especially upon waking.
- Thick or Stringy Saliva: Instead of being watery, saliva may become thick, foamy, or stringy.
- Difficulty Speaking or Swallowing: Lack of lubrication makes it hard to move the tongue and swallow food or even saliva.
- Sore Throat: A raw, scratchy, or burning sensation in the throat due to dryness.
- Hoarseness: Dryness in the vocal cords can lead to a raspy voice.
- Bad Breath (Halitosis): Saliva helps wash away food particles and bacteria; without enough, bacteria multiply, leading to odor.
- Changes in Taste: Food may taste different, or you might experience a metallic taste.
- Tongue Changes: The tongue may appear dry, red, fissured, or feel rough. It might stick to the roof of your mouth.
- Increased Thirst: A constant need to drink water, especially during the night or immediately after waking.
- Lip and Mouth Corner Cracking: Dryness around the mouth can lead to chapped lips and cracks at the corners (angular cheilitis).
- Dental Problems:
- Rapid Cavity Development: A dramatic increase in tooth decay, particularly on the root surfaces or along the gum line, where saliva usually pools.
- Gum Inflammation (Gingivitis) and Periodontal Disease: Lack of saliva allows bacteria to proliferate, leading to inflamed, bleeding gums.
- Oral Infections: Increased susceptibility to fungal infections like oral thrush (candidiasis), appearing as white patches in the mouth.
General Symptoms:
- Disrupted Sleep: Waking up frequently due to discomfort, leading to fragmented sleep.
- Reduced CPAP Adherence: The discomfort of dry mouth can make you less likely to use your CPAP machine consistently, compromising your sleep apnea treatment.
- Daytime Fatigue: If dry mouth disrupts your CPAP use and sleep quality, you may still experience daytime sleepiness, irritability, and difficulty concentrating, negating the benefits of CPAP.
Treatment Options: A Multi-Pronged Approach
Effectively addressing CPAP dry mouth, even with a humidifier, usually requires a combination of strategies, often involving your sleep physician and a dental professional.
1. CPAP Equipment Adjustments
- Mask Optimization:
- Check Fit and Seal: This is paramount. A leaky mask is a primary cause. Work with your CPAP provider to try different mask types, sizes, and brands. Ensure the headgear is adjusted correctly – not too tight, not too loose. Replace cushions/seals every 3-6 months, and the entire mask every 6-12 months, as they lose their integrity.
- Switch Mask Type: If you're a mouth breather using a nasal mask, consider switching to a full-face mask or a hybrid mask that covers both the nose and mouth.
- Humidifier Settings:
- Increase Humidity Level: Gradually increase the temperature/humidity setting on your CPAP machine.
- Use Heated Tubing: This is highly recommended to prevent "rainout" (condensation) and ensure the humidified air reaches your mask effectively. It allows for higher humidity settings without discomfort.
- Check Water Reservoir: Ensure it's filled nightly with distilled water and doesn't run dry during the night. Consider a larger reservoir if available for your machine.
- Chin Strap: If you use a nasal mask and mouth breathe, a chin strap can help keep your mouth closed during sleep. There are various designs; experiment to find one that is comfortable and effective.
- Mouth Taping: Some individuals find success with medical-grade tape over their lips to keep the mouth closed. This should only be attempted after consulting with a sleep specialist or dentist, and ensure you can easily open your mouth if needed.
- CPAP Pressure Adjustments: Sometimes, very high CPAP pressure can make it difficult to breathe nasally, leading to mouth opening. Discuss with your sleep physician if a pressure adjustment (especially if you have an auto-CPAP) could help, although this is less common than other causes.
2. Dental Interventions
A dentist, especially one specializing in sleep dentistry, can offer crucial solutions.
- Custom Oral Appliances (Dental Sleep Appliances):
- Mandibular Advancement Devices (MADs): These are custom-fitted devices that look like a sports mouth guard snoring device. They gently reposition the lower jaw and tongue forward, which can help keep the airway open, potentially reducing the need for very high CPAP pressures, and crucially, prevent the mouth from falling open. For individuals with mild to moderate sleep apnea or severe snoring, these devices can sometimes be an alternative to CPAP or used in conjunction with CPAP.
- Pros: Highly effective for preventing mouth breathing, can be an alternative to CPAP for some, custom-fit for comfort.
- Cons: Costly (typically $1,800-$3,000), requires professional fitting by a dentist experienced in sleep medicine, may cause temporary jaw soreness or tooth movement.
- Tongue-Retaining Devices (TRDs): These devices hold the tongue in a forward position using suction.
- Pros: Can be effective for specific types of airway obstruction.
- Cons: Can be uncomfortable, some patients find the suction irritating.
- Oral Shields/Guards: Simple devices that fit inside the mouth to cover the teeth and gums, preventing air from drying the oral tissues. These are less common as primary solutions but can offer relief.
- Pros: Inexpensive relative to MADs (stock versions can be $50-$200, custom $300-$800).
- Cons: May not address the root cause of mouth breathing.
- Mandibular Advancement Devices (MADs): These are custom-fitted devices that look like a sports mouth guard snoring device. They gently reposition the lower jaw and tongue forward, which can help keep the airway open, potentially reducing the need for very high CPAP pressures, and crucially, prevent the mouth from falling open. For individuals with mild to moderate sleep apnea or severe snoring, these devices can sometimes be an alternative to CPAP or used in conjunction with CPAP.
- Saliva Substitutes and Stimulants:
- Artificial Saliva: Available over-the-counter as sprays, gels, or rinses. They provide temporary relief by lubricating the mouth.
- Cost: $8-$25 per bottle/tube.
- Xylitol Products: Chewing gum, lozenges, or mouthwashes containing xylitol can stimulate saliva flow and help prevent cavities. The ADA supports xylitol's oral health benefits.
- Cost: $5-$15 per pack/bottle.
- Prescription Medications: For severe cases of dry mouth due to salivary gland dysfunction, your doctor might prescribe medications like pilocarpine or cevimeline, which stimulate saliva production.
- Cost: Varies by insurance, often $30-$200 per month without insurance.
- Artificial Saliva: Available over-the-counter as sprays, gels, or rinses. They provide temporary relief by lubricating the mouth.
- Fluoride Treatments: Regular professional fluoride applications and prescription fluoride toothpaste (e.g., 5000 ppm fluoride) are essential to protect teeth from rampant decay caused by dry mouth.
- Cost: Professional fluoride application $30-$70 per visit; prescription toothpaste $15-$30 per tube.
- Regular Dental Check-ups: Due to the increased risk of cavities and gum disease, vigilant dental care, including more frequent cleanings (e.g., every 3-4 months instead of 6), is crucial.
- Cost: Dental check-up and cleaning $75-$200 (without insurance).
3. Behavioral and Lifestyle Changes
- Hydration: Drink plenty of water throughout the day, but avoid excessive amounts right before bed to minimize nighttime bathroom trips.
- Avoid Irritants:
- Caffeine and Alcohol: These are diuretics and can contribute to dehydration.
- Tobacco: Smoking severely irritates oral tissues and reduces saliva flow.
- Sugary/Acidic Foods: These increase the risk of decay in a dry mouth.
- Antihistamines/Decongestants: If possible, avoid these or use them sparingly, as they often worsen dry mouth. Discuss alternatives with your doctor.
- Mouth Breathing Exercises: Some patients benefit from exercises to strengthen tongue and jaw muscles, promoting nasal breathing.
- Sleep Position: Experiment with different sleep positions. Sleeping on your back might encourage mouth breathing for some, while side sleeping can sometimes shift masks.
- Bedroom Humidifier: In addition to your CPAP humidifier, running a standalone room humidifier can increase ambient humidity, especially in dry climates.
- Cost: $30-$150 for a good quality room humidifier.
4. Medical Evaluation
- Review Medications: Discuss with your doctor if any of your current medications could be contributing to dry mouth and if alternative drugs with fewer side effects are available.
- Address Underlying Conditions: Ensure any medical conditions known to cause dry mouth (e.g., diabetes, autoimmune disorders) are well-managed.
- Allergy/Sinus Treatment: If nasal congestion is forcing you to mouth breathe, address it with your doctor or an ENT specialist. This might involve allergy medications, nasal sprays, or even surgical correction for issues like a deviated septum.
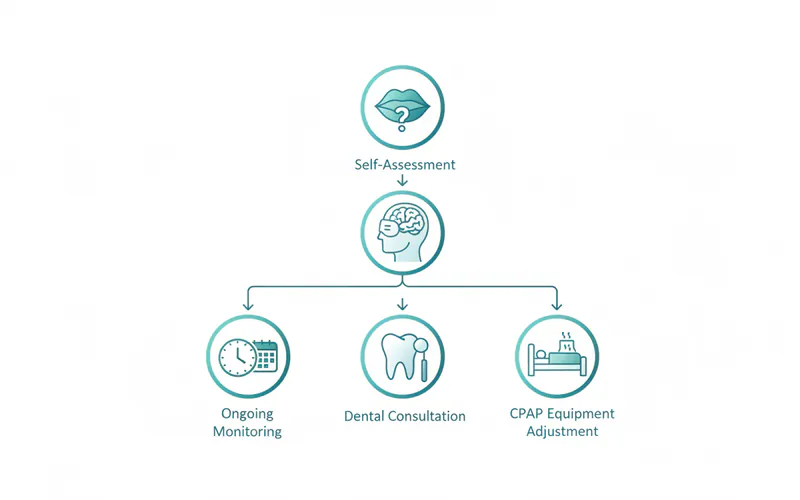
Step-by-Step Process: Finding Relief from CPAP Dry Mouth
Tackling CPAP dry mouth requires a systematic approach, often involving collaboration between you, your sleep physician, and your dentist.
-
Self-Assessment & Initial Adjustments (Weeks 1-2):
- Identify the Problem: Confirm you are experiencing dry mouth primarily with CPAP use, even with the humidifier on.
- Check CPAP Basics:
- Water Level: Is your humidifier reservoir full at bedtime? Does it run dry by morning?
- Humidifier Setting: Is it on a low setting? Try increasing it gradually.
- Heated Tubing: Are you using heated tubing? If not, consider acquiring one.
- Mask Seal: Perform a mask fit check. Put on your mask and turn on your CPAP. Feel around the edges for air leaks. Lie down in your typical sleep position and check again. Adjust straps, or try a different size if needed.
- Hydration: Increase your daily water intake.
- Avoid Irritants: Minimize caffeine, alcohol, and tobacco.
- Consider a Chin Strap: If you suspect mouth breathing with a nasal mask, try a chin strap.
-
Consult Your Sleep Physician/CPAP Provider (Weeks 2-4):
- Report Symptoms: Explain your persistent dry mouth and the adjustments you've already tried.
- Review Mask Fit: Your provider can help you try different mask types and sizes. They might use pressure mapping or other tools to ensure a proper seal.
- Optimize Humidifier & Settings: Discuss your humidifier settings, the need for heated tubing, and ensure your humidifier is functioning correctly.
- Address High Pressure: If mouth breathing is due to high CPAP pressure, your doctor might consider adjusting your pressure settings (if appropriate for your sleep apnea severity) or prescribing a different type of positive airway pressure device (e.g., BiPAP).
- Medication Review: Discuss any medications you're taking that might contribute to dry mouth.
- Underlying Medical Conditions: Rule out or manage any medical conditions exacerbating dry mouth.
-
Consult Your Dentist (Specializing in Sleep Dentistry, if possible) (Weeks 3-6):
- Oral Health Assessment: Your dentist will check for signs of decay, gum disease, and oral infections caused by dry mouth.
- Discuss Mouth Breathing: A dentist can assess your oral anatomy and habits to determine if mouth breathing is a primary issue.
- Oral Appliance Options:
- For chronic mouth breathing with a nasal CPAP, they may recommend a custom-fitted oral appliance (like a MAD) to keep your mouth closed or advance your jaw, used in conjunction with your CPAP.
- For individuals with mild to moderate sleep apnea who struggle with CPAP, a custom dental sleep appliance might be an alternative solution (though this requires discussion with your sleep physician).
- Saliva Management: They can recommend specific over-the-counter or prescription saliva substitutes, stimulants, or fluoride products.
- Preventive Care: Discuss increasing the frequency of dental cleanings and fluoride treatments to protect your teeth.
-
Ongoing Monitoring & Adjustment:
- Consistency: Continue with chosen solutions consistently.
- Monitor Symptoms: Keep a log of your dry mouth symptoms, CPAP settings, and any changes you make.
- Follow-up: Maintain regular follow-ups with both your sleep physician and your dentist to ensure the solutions are effective and your oral health is protected.
Cost and Insurance: Understanding the Financial Aspect
The cost of addressing CPAP dry mouth can vary significantly based on the chosen solutions and your insurance coverage.
CPAP-Related Costs:
- CPAP Machine with Humidifier:
- Without Insurance: $500 - $1,500 for a basic model, $1,500 - $3,000+ for advanced models with integrated heated tubing and smart features.
- With Insurance: Often covered by Medicare and private insurance as Durable Medical Equipment (DME). You'll typically pay a deductible, copayment (10-20%), or coinsurance. Many policies require a rental period before purchase.
- CPAP Masks:
- Without Insurance: $100 - $300 per mask.
- With Insurance: Covered as DME, subject to deductibles and copayments. Masks usually need replacement every 3-12 months.
- Heated Tubing:
- Without Insurance: $30 - $80.
- With Insurance: Often covered with the CPAP machine or as a supply item. Replace every 6-12 months.
- Chin Straps:
- Without Insurance: $15 - $40.
- With Insurance: Usually not covered, considered an accessory.
- Distilled Water:
- Cost: $1-$3 per gallon, used nightly. Annual cost can be $50-$150.
- Insurance: Not covered.
Dental-Related Costs:
- Dental Consultation (for sleep apnea/dry mouth):
- Without Insurance: $50 - $200.
- With Dental Insurance: May be covered as a general consultation; if specialized, coverage varies.
- Custom Oral Appliance (Mandibular Advancement Device):
- Without Insurance: $1,800 - $3,000. This includes impressions, custom fabrication, fitting, and follow-up adjustments.
- With Medical Insurance: Often covered under the medical benefit for the treatment of sleep apnea, not dental. Requires a sleep apnea diagnosis and physician's prescription. Coverage can be 50-80% after deductible, but varies widely. It's crucial to verify benefits specific to sleep apnea appliances.
- With Dental Insurance: Rarely covered for sleep apnea. Some dental plans might offer a small allowance for "occlusal guards," but usually not enough for a MAD.
- Saliva Substitutes/Xylitol Products:
- Cost: $5 - $25 per item.
- Insurance: Not covered (over-the-counter).
- Prescription Saliva Stimulants:
- Cost: $30 - $200 per month without insurance.
- With Medical Insurance: Usually covered with a prescription, subject to copay.
- Fluoride Treatments & Prescription Fluoride Toothpaste:
- Professional Fluoride: $30 - $70 per application. Often covered by dental insurance for children, sometimes for adults with high-risk factors.
- Prescription Toothpaste: $15 - $30 per tube. May be covered by medical insurance if prescribed, otherwise out-of-pocket.
- Routine Dental Cleanings & Exams:
- Without Insurance: $75 - $200 per visit.
- With Dental Insurance: Usually covered 80-100% for preventive care (often two cleanings per year). If more frequent cleanings are needed due to dry mouth, coverage may be less or require prior authorization.
- Cavity Fillings/Gum Treatments:
- Cost: Fillings $150-$450 per tooth; gum treatments $200-$1,000+ depending on severity.
- With Dental Insurance: Typically covered 50-80% after deductible.
Cost-Saving Tips:
- Verify Insurance: Always contact your medical and dental insurance providers directly to confirm coverage for CPAP equipment, oral appliances, and related treatments. Ask for specific CPT and HCPCS codes (your provider can supply these).
- In-Network Providers: Choose CPAP suppliers and dental sleep medicine providers who are in your insurance network to maximize benefits.
- Payment Plans: Many dental offices and DME suppliers offer payment plans.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): Use pre-tax dollars from these accounts for eligible medical and dental expenses.
- Shop Around: For non-covered items like chin straps or over-the-counter products, compare prices online and at various retailers.
- Preventive Care: Investing in good oral hygiene and early intervention is always cheaper than treating advanced dental problems.
Recovery and Aftercare: Sustaining Comfort and Oral Health
Once you've identified and implemented solutions for your CPAP dry mouth, maintaining long-term comfort and protecting your oral health requires consistent aftercare.

- Consistent CPAP Adherence: The primary goal is to ensure you can comfortably use your CPAP machine every night. Continued adherence means better sleep apnea management and reduced overall health risks. If dry mouth recurs, revert to the troubleshooting steps.
- Diligent Oral Hygiene:
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste (consider a prescription-strength fluoride toothpaste if recommended by your dentist).
- Floss Daily: Remove plaque and food particles from between teeth.
- Use Fluoride Rinse: An alcohol-free fluoride mouthwash can provide additional protection against cavities.
- Xylitol Products: Incorporate xylitol chewing gum or lozenges during the day to stimulate saliva.
- Stay Hydrated: Continue to drink plenty of water throughout the day. Keep a glass of water by your bedside if you wake with a dry mouth, but avoid large quantities right before sleep.
- Regular Dental Check-ups: Due to the heightened risk of dental issues from dry mouth, schedule more frequent dental visits. Your dentist might recommend cleanings every 3-4 months instead of the standard 6. This allows for early detection and treatment of cavities and gum disease.
- Monitor Mask and Equipment:
- Replace Mask Components Regularly: Cushions/seals should be replaced every 3-6 months, headgear every 6 months, and the entire mask every year. Worn-out parts are a common source of leaks.
- Clean CPAP Equipment: Follow manufacturer guidelines for daily and weekly cleaning of your mask, tubing, and humidifier chamber. This prevents bacterial growth.
- Distilled Water: Always use distilled water in your humidifier to prevent mineral buildup and ensure optimal function.
- Review Medications: Periodically discuss all medications with your physician to see if any alternatives with fewer dry mouth side effects are available, especially if new medications are added.
- Awareness of Symptoms: Pay attention to any return of dry mouth symptoms or new oral discomfort. Promptly address them with your sleep physician or dentist.
Pro Tip: Consider using a CPAP cleaner like an ozone or UV light device for automated sanitization of your mask and tubing, though manual cleaning is still recommended. This helps maintain hygiene and prolong the life of your equipment.
Prevention: Proactive Steps to Avoid Dry Mouth
Preventing CPAP dry mouth starts with proactive measures and establishing good habits from the outset of your CPAP therapy.
- Optimal Mask Fit from Day One:
- Work with Your Provider: Don't settle for an uncomfortable or leaky mask. Utilize your CPAP provider's expertise to find the perfect mask type and size that fits your facial anatomy and preferred sleep position.
- Test Thoroughly: Test the mask extensively before committing. Many providers offer trial periods.
- Proper Humidifier Usage:
- Always Use Distilled Water: This prevents mineral buildup and ensures consistent humidifier performance.
- Experiment with Settings: Start with a moderate humidity setting and adjust upward as needed, especially in dry environments or during winter.
- Utilize Heated Tubing: If your machine supports it, always use heated tubing. It's the best way to ensure humidified air reaches your mask without condensation.
- Address Mouth Breathing:
- Chin Strap: If using a nasal mask, proactively use a chin strap from the beginning to prevent the mouth from falling open.
- Consider a Full-Face Mask: If you know you're a mouth breather, or suspect you might become one with CPAP, a full-face mask is often the best initial choice.
- Nasal Hygiene: Treat any underlying nasal congestion or allergies. Use saline nasal sprays, allergy medications, or seek ENT consultation if needed to ensure clear nasal passages.
- Maintain Excellent Oral Hygiene:
- Brush and Floss Religiously: This is the first line of defense against the dental complications of dry mouth.
- Fluoride is Your Friend: Use a fluoride toothpaste and consider an alcohol-free fluoride mouthwash.
- Stay Hydrated: Make consistent daily water intake a habit.
- Limit Dry Mouth Triggers: Reduce consumption of caffeine, alcohol, and sugary drinks. Avoid tobacco products entirely.
- Regular Dental Check-ups: Inform your dentist about your CPAP use and dry mouth. They can help monitor your oral health and provide preventive fluoride treatments or recommendations for saliva-stimulating products.
Risks and Complications: What Can Go Wrong
Untreated or poorly managed CPAP dry mouth carries significant risks that extend beyond simple discomfort, potentially impacting both your overall health and the efficacy of your sleep apnea treatment.
1. Dental and Oral Health Complications:
- Rampant Tooth Decay (Cavities): Without adequate saliva, the mouth's natural defense against acid is severely compromised. This leads to a rapid increase in cavities, often aggressive ones at the gum line or on root surfaces, which are difficult and costly to treat.
- Gum Disease (Gingivitis and Periodontitis): Dry mouth creates an environment where harmful bacteria thrive, leading to inflammation, bleeding, and eventually destruction of the tissues and bone supporting the teeth.
- Oral Infections: Reduced saliva makes you more susceptible to fungal infections like oral thrush (candidiasis) and bacterial infections.
- Difficulty with Dentures: For those with dentures, dry mouth can make them uncomfortable, cause them to slip, and increase the risk of sores and infections.
- Bad Breath (Halitosis): Persistent dry mouth often leads to chronic bad breath, which can affect social interactions and self-confidence.
- Tooth Loss: In severe, untreated cases, rampant decay and gum disease can ultimately lead to premature tooth loss.
2. CPAP Adherence Issues:
- Reduced Compliance: The constant discomfort of a dry mouth is a major reason why many individuals abandon or inconsistently use their CPAP therapy.
- Ineffective Sleep Apnea Treatment: Poor CPAP adherence means your sleep apnea remains untreated or undertreated, negating the health benefits of the therapy.
3. Worsening Sleep Apnea Symptoms:
- Continued Daytime Fatigue: If CPAP is not used consistently due to dry mouth, you will continue to experience the symptoms of untreated sleep apnea, such as daytime sleepiness, irritability, difficulty concentrating, and impaired cognitive function.
- Increased Risk of Associated Health Problems: Untreated sleep apnea is linked to higher risks of high blood pressure, heart attack, stroke, diabetes, and other serious cardiovascular and metabolic conditions.
4. Discomfort and Quality of Life:
- Chronic Discomfort: The persistent feeling of a dry, sticky, or burning mouth significantly diminishes quality of life, impacting eating, speaking, and overall well-being.
- Disrupted Sleep: Waking up frequently due to dry mouth further fragments sleep, even if the sleep apnea itself is technically being treated, leading to overall poor sleep quality.
- Sore Throat and Hoarseness: Chronic dryness can lead to persistent sore throats, irritation, and hoarseness.
Pro Tip: The ADA (American Dental Association) strongly emphasizes the importance of managing dry mouth, especially for individuals at high risk (like CPAP users), due to its profound impact on oral health and systemic well-being. Regular dental check-ups and a proactive approach to oral hygiene are not merely cosmetic but crucial for preventing serious health complications.
Comparison Tables
To help visualize the various aspects and potential solutions for CPAP dry mouth, here are two comparison tables:
Table 1: CPAP Mask Types and Their Impact on Dry Mouth Risk
| Mask Type | Primary Air Delivery | Dry Mouth Risk (without intervention) | Best for... | Pros | Cons |
|---|---|---|---|---|---|
| Nasal Mask | Nose | High (if mouth breathing occurs) | Nasal breathers, claustrophobic individuals | Less obstructive, wide field of vision | Requires conscious nasal breathing, high risk of dry mouth if mouth opens |
| Nasal Pillow | Nose (directly into nostrils) | High (if mouth breathing occurs) | Minimalists, active sleepers, claustrophobic | Smallest footprint, very lightweight | Similar to nasal mask for dry mouth, can cause nostril irritation, pressure marks |
| Full-Face Mask | Nose & Mouth | Moderate (due to leaks or airflow) | Mouth breathers, those with nasal congestion | Accommodates mouth breathing, robust seal | More bulky, can feel claustrophobic, higher chance of leaks around edges if not fitted well, more pressure on face |
| Hybrid Mask | Nasal pillows & Oral cushion | Moderate | Those needing nasal pillows but prone to mouth leaks | Less bulky than full-face, allows some mouth breathing | Can be complex to fit, potential for leaks from multiple points |
Table 2: Solutions for CPAP Dry Mouth: Effectiveness, Cost, and Effort
| Solution Category | Specific Intervention | Effectiveness for Dry Mouth | Estimated Cost (US, without insurance) | Effort Level | Notes |
|---|---|---|---|---|---|
| CPAP Adjustments | Proper Mask Fit & Type | High | $0 - $300 (new mask/accessories) | Medium | Crucial first step. Requires trial and error. |
| Optimized Humidifier Settings | High | $0 (if already have humidifier) | Low | Experiment with temp/humidity levels. | |
| Heated Tubing | High | $30 - $80 | Low | Prevents "rainout," improves humidity delivery. | |
| Chin Strap | Moderate-High | $15 - $40 | Low | Effective for preventing mouth opening with nasal masks. | |
| Dental Interventions | Custom Oral Appliance (MAD) | High | $1,800 - $3,000 | High | Prevents mouth breathing, may need medical insurance coverage. |
| Saliva Substitutes (OTC) | Moderate (temporary relief) | $8 - $25 per item | Low | Sprays, gels, rinses for temporary comfort. | |
| Xylitol Products | Moderate (stimulates saliva) | $5 - $15 per pack | Low | Gums, lozenges. Also helps prevent cavities. | |
| Prescription Saliva Stimulants | High (for severe cases) | $30 - $200/month | Low | Physician prescribed, for compromised salivary glands. | |
| Prescription Fluoride Treatment | High (for protection) | $15 - $70 per application/tube | Low | Essential to prevent rampant decay from dry mouth. | |
| Behavioral Changes | Increased Hydration | Moderate | $0 | Low | Crucial for overall health and systemic dryness. |
| Avoid Irritants (Caffeine, Alcohol, Tobacco) | Moderate | $0 (lifestyle change) | Low | Reduces dehydration and oral tissue irritation. | |
| Room Humidifier | Moderate | $30 - $150 | Low | Increases ambient air moisture, especially in dry climates. | |
| Medical Evaluation | Medication Review | Moderate-High | $50 - $200 (consultation) | Medium | Identify and potentially change medications causing dry mouth. |
| Treat Nasal Congestion | High | Varies (meds, ENT visit: $100-$500+) | Medium | Allows for easier nasal breathing, reducing mouth breathing. |
Frequently Asked Questions
Q1: Why do I get dry mouth with CPAP even with a humidifier?
Even with a humidifier, the primary reason for CPAP dry mouth is often unintentional mouth breathing. If you open your mouth while using a nasal mask, the humidified air enters through your nose but escapes through your mouth, rapidly drying out your oral cavity. Mask leaks, inadequate humidifier settings, or underlying medical conditions and medications can also contribute.
Q2: Can a dental mouth guard help with CPAP dry mouth?
Yes, a custom-fitted dental appliance, often referred to as a mouth guard snoring device, can be highly effective. These devices, specifically Mandibular Advancement Devices (MADs), gently hold your jaw and tongue forward, helping to keep your mouth closed during sleep. This prevents the "wind tunnel" effect of air escaping through your mouth, thus reducing dry mouth.
Q3: What is "rainout" and how does it relate to dry mouth?
"Rainout" occurs when warm, humidified air from your CPAP humidifier cools down as it travels through the tubing to your mask, causing condensation (water droplets) to form. This not only makes a gurgling noise and can spray water on your face but also reduces the actual humidity delivered to your airway, contributing to dry mouth. Heated tubing effectively prevents rainout by maintaining a consistent temperature.
Q4: Is it always sleep apnea if I snore loudly?
No, is snoring always sleep apnea? While loud, chronic snoring is a hallmark symptom of obstructive sleep apnea (OSA), it does not always indicate sleep apnea. Many people snore without having OSA. However, if your snoring is accompanied by gasping, choking, pauses in breathing, daytime fatigue, morning headaches, or difficulty concentrating, it's crucial to be evaluated for sleep apnea by a sleep specialist.
Q5: How often should I replace my CPAP mask and humidifier parts?
To maintain effectiveness and hygiene, CPAP mask cushions/nasal pillows should typically be replaced every 3-6 months, and the headgear every 6 months. The entire mask assembly should be replaced annually. Humidifier chambers often need replacement every 6-12 months to prevent mineral buildup and maintain efficiency. Check your manufacturer's specific recommendations.
Q6: Are there any natural remedies for CPAP dry mouth?
Beyond increasing overall hydration, some natural approaches include chewing sugar-free gum (especially with xylitol) to stimulate saliva, sucking on ice chips, or using natural oils (like coconut oil) as a temporary oral moisturizer. However, these are often supplementary and do not replace addressing the root cause of the dry mouth.
Q7: Can dry mouth from CPAP lead to serious dental problems?
Absolutely. Chronic dry mouth significantly increases your risk of severe dental problems. Without saliva's protective effects, you are much more prone to rapid tooth decay (cavities), gum disease (gingivitis and periodontitis), and oral infections like thrush. Regular dental check-ups and heightened oral hygiene are critical.
Q8: What if increasing my humidifier settings makes my mask feel wet or causes condensation?
If increasing your humidifier settings leads to your mask feeling wet or causes condensation in your tubing, it's a sign of "rainout." The most effective solution is to use heated CPAP tubing, which maintains the air temperature throughout its journey to your mask, preventing the moisture from condensing before it reaches you.
Q9: My doctor said I might have a deviated septum. Could this cause CPAP dry mouth?
Yes, a deviated septum or other nasal obstructions can make nasal breathing difficult, forcing you to breathe through your mouth. If you're using a nasal CPAP mask, this will inevitably lead to significant dry mouth, even with a humidifier. Addressing the nasal obstruction (e.g., with decongestants, allergy treatment, or surgery) can be a key part of the solution.
Q10: How long does it take to find a solution for CPAP dry mouth?
Finding the optimal solution can take some time and patience, typically ranging from 2 to 6 weeks. It involves a process of trial and error with different mask types, humidifier settings, and potentially incorporating dental or medical interventions. Consistent communication with your sleep physician and dentist will expedite the process.
When to See a Dentist
While self-troubleshooting your CPAP dry mouth is a good starting point, there are clear indicators that it's time to involve a dental professional, especially one experienced in sleep dentistry.
See a Dentist Immediately (Red Flags):
- Sudden Increase in Cavities: If you notice new dark spots on your teeth, sensitivity, or your dentist informs you of multiple new cavities, especially in areas typically less prone to decay (like gum lines or root surfaces). This indicates severe salivary deficiency and warrants urgent attention.
- Persistent Oral Pain or Sores: Any chronic pain, burning sensation, or non-healing sores in your mouth, on your tongue, or at the corners of your lips. This could be a sign of infection (like thrush) or other serious oral health issues.
- Difficulty Eating or Swallowing: If dry mouth makes it consistently difficult or painful to chew, taste, or swallow food, significantly impacting your nutrition and quality of life.
- Severe Gum Inflammation or Bleeding: If your gums are noticeably red, swollen, or bleed frequently during brushing or flossing, it indicates advanced gum disease exacerbated by dry mouth.
Schedule a Dentist Appointment (Routine Care & Persistent Symptoms):
- Persistent Dry Mouth Symptoms: If you've tried adjusting your CPAP mask, humidifier settings, and lifestyle changes, but your mouth still feels uncomfortably dry every morning.
- Suspected Mouth Breathing: If you use a nasal mask and suspect you're mouth breathing at night (e.g., often wake with a very dry mouth, your chin strap isn't effective). A dentist specializing in sleep can assess your oral anatomy and discuss solutions like custom oral appliances.
- Bad Breath that Won't Go Away: If you've maintained good oral hygiene but still suffer from chronic halitosis, it could be a symptom of dry mouth or an underlying oral infection.
- Prior to Starting CPAP Therapy: If you are about to begin CPAP therapy, consult your dentist to establish a baseline for your oral health and discuss preventive strategies for potential dry mouth.
- Regular Check-ups: Inform your dentist about your CPAP use at every routine check-up. They can monitor your oral health for early signs of dry mouth complications and recommend preventive measures like fluoride treatments.
Remember, your oral health is an integral part of your overall well-being. Don't underestimate the impact of chronic dry mouth; proactive dental care can prevent severe, costly, and painful complications.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
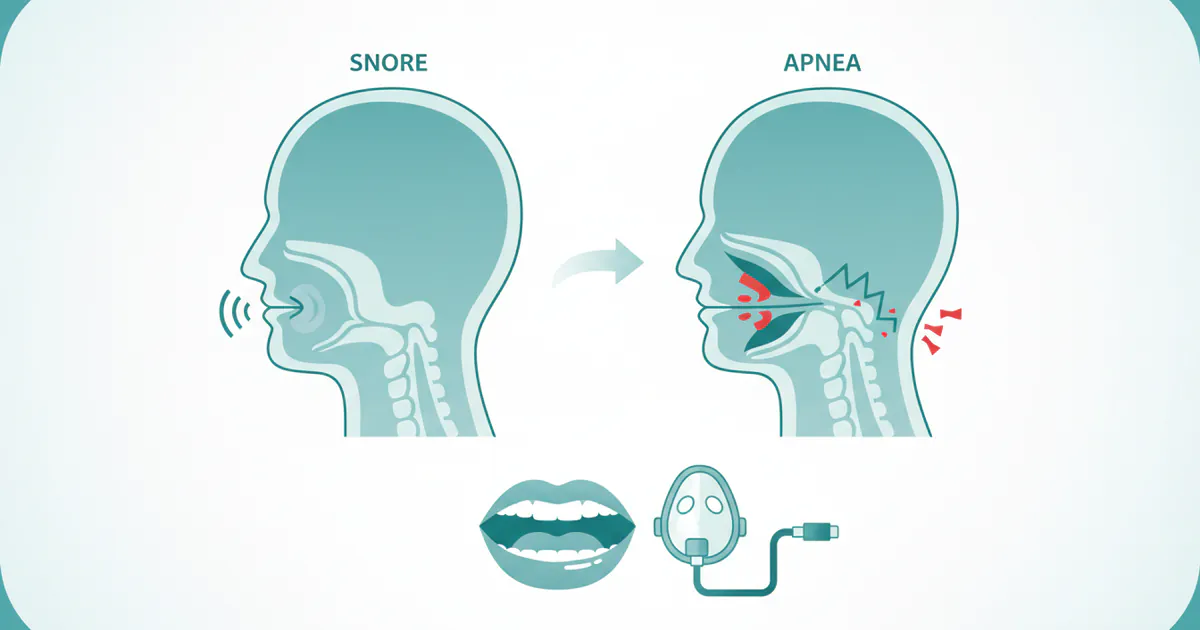
Difference Between Snoring and Sleep Apnea: Complete Guide
More than 80 million Americans regularly snore, and while often dismissed as a mere nuisance, loud and persistent snoring can be a critical indicator of a much more serious underlying health condition: sleep apnea. The difference between snoring and sleep apnea is profound, impacting not just yo
February 23, 2026

Mouth Taping for Snoring: Complete Guide
Snoring. It's the nocturnal soundtrack for millions of Americans, often a source of frustration for bed partners and a potential indicator of underlying health issues for the snorer themselves. Roughly 45% of adults snore occasionally, and 25% are habitual snorers, impacting sleep quality, relat
February 23, 2026
Is All Snoring Sleep Apnea
Many individuals, perhaps even you or a loved one, have been told they snore loudly. It's often dismissed as a harmless, albeit annoying, nocturnal habit. However, what if that nightly rumble is more than just noise? What if it's a critical indicator of an underlying health condition that significan
February 23, 2026
Sleep Apnea Mouth Tape: Complete Guide
You've likely heard the sound – the unmistakable rumble of snoring, echoing through the night. For many, snoring is more than just an annoyance; it's a potential warning sign of a serious underlying condition: sleep apnea. Affecting an estimated 30 million adults in the United States, sleep apne
February 23, 2026