Does Snoring Mean Sleep Apnea
Key Takeaways
- Snoring is often dismissed as a harmless, albeit annoying, nocturnal habit. However, for many, the rumble from the bedroom is a critical indicator of a far more serious underlying health condition: sleep apnea. In the United States, does snoring mean sleep apnea is a question that affects millio
Snoring is often dismissed as a harmless, albeit annoying, nocturnal habit. However, for many, the rumble from the bedroom is a critical indicator of a far more serious underlying health condition: sleep apnea. In the United States, does snoring mean sleep apnea is a question that affects millions, with estimates suggesting that nearly 30% of adults habitually snore, and a significant portion of these individuals unknowingly suffer from obstructive sleep apnea (OSA). This condition, characterized by repeated pauses in breathing during sleep, extends far beyond just disturbing your partner's rest. It can lead to severe health consequences, from chronic fatigue and impaired daily function to an increased risk of heart disease, stroke, and diabetes.
Understanding the distinction between benign snoring and sleep apnea is crucial for your long-term health and well-being. While not all snoring indicates sleep apnea, virtually all individuals with sleep apnea snore. This article delves deep into this intricate relationship, distinguishing between different types of sleep apnea, exploring their causes, and outlining the comprehensive diagnostic and treatment approaches available. We will examine cutting-edge solutions like mandibular advancement devices (MADs), discuss the effectiveness and potential side effects of CPAP therapy, including how to manage issues like CPAP dry mouth, and provide a clear roadmap for anyone concerned about their nighttime breathing. By the end of this comprehensive guide, you'll have the knowledge to recognize the warning signs and take proactive steps toward healthier, more restorative sleep.
Key Takeaways:
- Snoring is a primary symptom of sleep apnea, but not all snoring indicates the condition. Approximately 30% of adults habitually snore, and a significant portion have undiagnosed sleep apnea.
- Obstructive Sleep Apnea (OSA) is the most common type, caused by physical airway blockage, while Central Sleep Apnea (CSA) involves brain signals.
- Diagnosis requires a sleep study (polysomnography) or home sleep test. Costs for a home test range from $250-$500, while in-lab studies can be $1,000-$5,000 without insurance.
- Treatment options vary widely. Continuous Positive Airway Pressure (CPAP) is a highly effective first-line therapy, but alternatives like mandibular advancement devices (MADs) are excellent for mild to moderate OSA or CPAP intolerance.
- MADs are custom-made by dentists and typically cost between $1,800-$3,500, often covered by medical insurance if prescribed for sleep apnea.
- Managing side effects like CPAP dry mouth is common. Solutions include humidifiers, nasal sprays, and specific oral hygiene practices.
- Untreated sleep apnea carries serious health risks, including cardiovascular disease, diabetes, and increased accident risk. Early intervention is key.
Snoring vs. Sleep Apnea: Unraveling the Connection
Many people believe that snoring is just a noisy habit, perhaps an annoyance to a bed partner, but ultimately harmless. However, the truth is more complex. While simple snoring can occur without serious health implications, it is also the most common and recognizable symptom of a potentially life-threatening condition: sleep apnea. Understanding the critical differences and the crucial link between these two phenomena is the first step toward better sleep and improved overall health.
What Is Snoring?
Snoring is the harsh sound produced when air flows past relaxed tissues in your throat, causing them to vibrate as you breathe during sleep. These tissues can include your soft palate, uvula, tonsils, and the base of your tongue. Several factors contribute to this relaxation and narrowing of the airway, including:
- Anatomy: A low, thick soft palate, enlarged tonsils, or a large tongue can narrow your airway.
- Alcohol or Sedatives: These substances relax throat muscles, increasing the likelihood of snoring.
- Nasal Problems: Chronic nasal congestion or a deviated septum can restrict airflow, leading to mouth breathing and snoring.
- Sleep Position: Sleeping on your back often causes the tongue to fall back, partially blocking the airway.
- Weight: Excess weight around the neck can compress the airway.
Simple snoring, sometimes called primary snoring, is not associated with drops in blood oxygen levels or frequent arousals from sleep. It's an issue of noise, not necessarily a medical danger, though it can severely disrupt a partner's sleep and lead to relationship strain.
What Is Sleep Apnea?
Sleep apnea, on the other hand, is a serious sleep disorder in which your breathing repeatedly stops and starts while you sleep. These pauses, called apneas, can last from a few seconds to more than a minute and can occur dozens or even hundreds of times each night. When your breathing pauses, your brain briefly wakes you up to restart breathing, often with a gasp, snort, or choking sound, though you may not remember these awakenings. This constant disruption prevents you from getting deep, restorative sleep.
The key difference between simple snoring and sleep apnea lies in the physiological impact. While snoring is merely the sound of vibrating tissues, sleep apnea involves actual cessation of breathing and subsequent drops in blood oxygen saturation, putting immense strain on your cardiovascular system and leading to severe daytime consequences.
Types of Sleep Apnea
There are primarily three types of sleep apnea:
- Obstructive Sleep Apnea (OSA): This is by far the most common type, accounting for approximately 90% of all sleep apnea cases. OSA occurs when the muscles in your throat relax too much during sleep, causing your soft palate, uvula, tongue, and/or tonsils to collapse and block your airway. Your chest and diaphragm muscles still try to breathe, but they can't move air past the obstruction. The characteristic loud snoring associated with OSA is due to the vibrating tissues as air struggles to pass through the narrowed opening.
- Central Sleep Apnea (CSA): Less common than OSA, CSA occurs when your brain fails to send the proper signals to the muscles that control breathing. This means there's no effort to breathe for a short period, leading to a pause in respiration. CSA is often associated with underlying medical conditions such as heart failure, stroke, or certain medications (e.g., opioids). Snoring is typically not as prominent a symptom in CSA compared to OSA.
- Mixed or Complex Sleep Apnea: This refers to a combination of both OSA and CSA. It often begins as OSA but then develops central characteristics, particularly during CPAP therapy (known as treatment-emergent central sleep apnea).
Pro Tip: If your snoring is accompanied by gasping, choking, or pauses in breathing (as observed by a bed partner), or if you experience significant daytime fatigue despite getting "enough" sleep, it's highly probable you have sleep apnea, not just simple snoring.
Why Snoring and Sleep Apnea Happen: Root Causes and Contributing Factors
The mechanisms behind snoring and sleep apnea are rooted in the anatomy and function of your upper airway during sleep. Understanding these causes is crucial for effective diagnosis and treatment.
Anatomical Factors
The structure of your mouth and throat plays a significant role:
- Relaxed Throat Muscles: During sleep, muscles in the soft palate, uvula, tonsils, and tongue naturally relax. In some individuals, this relaxation is excessive, leading to collapse.
- Enlarged Tissues: Large tonsils, adenoids, or a bulky tongue can partially or fully obstruct the airway. A thick soft palate or uvula can also contribute.
- Jaw and Facial Structure: A recessed chin (retrognathia) or a smaller lower jaw can push the tongue backward, narrowing the airway.
- Nasal Obstruction: Chronic nasal congestion from allergies, colds, or anatomical issues like a deviated septum or nasal polyps force mouth breathing, which can increase the likelihood of snoring and sleep apnea. Breathing through the mouth allows the soft tissues at the back of the throat to vibrate more freely.
Lifestyle and Medical Factors
Beyond anatomy, several other factors significantly increase your risk:
- Obesity: Excess weight, particularly around the neck, compresses the airway. Fat deposits can also thicken the walls of the upper airway, making it more prone to collapse. This is one of the most significant risk factors for OSA.
- Alcohol and Sedatives: These substances depress the central nervous system, causing throat muscles to relax excessively and reducing the brain's ability to rouse you when breathing is obstructed.
- Smoking: Smoking irritates the airways, causing inflammation and fluid retention in the throat, which can narrow the breathing passage.
- Age: The risk of sleep apnea increases with age, as muscle tone generally decreases, making tissues more prone to collapse.
- Gender: Men are more likely to develop sleep apnea than women, though the risk for women increases after menopause.
- Family History: If family members have sleep apnea, you are at a higher risk, suggesting a genetic predisposition to certain anatomical features or regulatory issues.
- Medical Conditions:
- High Blood Pressure: Often co-occurs with sleep apnea.
- Diabetes: There's a strong bidirectional link between sleep apnea and insulin resistance.
- Heart Failure/Stroke: Can contribute to CSA.
- Hypothyroidism: An underactive thyroid can lead to fluid retention and weight gain, increasing apnea risk.
- Acromegaly: A condition causing excess growth hormone, leading to enlarged tissues.
- Polycystic Ovary Syndrome (PCOS): Women with PCOS have a higher risk of OSA.
Signs and Symptoms Beyond the Snore
While loud, chronic snoring is the most common red flag, sleep apnea manifests in a variety of ways that extend beyond nocturnal noise. Recognizing these additional signs and symptoms is crucial for early diagnosis.
Nocturnal Symptoms (Observed by others)
- Loud, chronic snoring: Often punctuated by silences, followed by gasps or choking sounds.
- Witnessed breathing pauses: A bed partner might notice you stop breathing for several seconds.
- Gasping or choking during sleep: You might suddenly wake up gasping for air.
- Restless sleep: Frequent tossing and turning, or frequent trips to the bathroom.
Daytime Symptoms (Experienced by the individual)
- Excessive daytime sleepiness (EDS): Falling asleep at inappropriate times, difficulty staying awake during sedentary activities like driving or watching TV. This is often the most debilitating symptom.
- Morning headaches: Caused by elevated carbon dioxide levels in the blood during apneic episodes.
- Irritability and mood changes: Chronic sleep deprivation can lead to frustration, anxiety, and depression.
- Difficulty concentrating or memory problems: Cognitive impairment due to fragmented sleep.
- Dry mouth or sore throat upon waking: Often due to mouth breathing during the night or, if on CPAP, CPAP dry mouth issues.
- Decreased libido: Sleep apnea can affect hormone levels.
- High blood pressure: A significant number of individuals with sleep apnea have hypertension, which can be difficult to control.
If you or your partner recognize several of these symptoms, it's time to consult a healthcare professional.
Diagnosing Sleep Apnea: The Path to Understanding Your Sleep
Diagnosing sleep apnea requires a thorough evaluation, typically involving a sleep study. The process usually begins with a consultation with your primary care physician or a sleep specialist, who will assess your symptoms, medical history, and risk factors. Dentists also play a vital role in screening for sleep apnea and offering certain treatment modalities.
Initial Assessment
Your doctor will likely ask about your sleep habits, daytime fatigue levels, and any observations from a bed partner. They may use questionnaires like the Epworth Sleepiness Scale to assess your level of daytime sleepiness. A physical examination may involve checking your neck circumference, tonsil size, and jaw structure.

Sleep Studies (Polysomnography)
The definitive diagnostic tool for sleep apnea is a sleep study, known as polysomnography (PSG).
- In-Lab Polysomnography: This involves spending a night at a sleep center, where technicians monitor various bodily functions during sleep. Sensors are attached to your body to record:
- Brain waves (EEG)
- Eye movements (EOG)
- Muscle activity (EMG)
- Heart rhythm (ECG)
- Airflow through your nose and mouth
- Blood oxygen levels (oximetry)
- Breathing effort (chest and abdominal bands)
- Leg movements
- Snoring intensity This comprehensive data allows sleep specialists to determine the presence, type, and severity of sleep apnea (measured by the Apnea-Hypopnea Index, or AHI). An AHI of 5-15 indicates mild, 15-30 moderate, and >30 severe sleep apnea.
- Home Sleep Apnea Test (HSAT): For many individuals suspected of having moderate to severe OSA, a simpler home sleep test can be performed. You'll receive a portable device to use in your own bed, which typically monitors airflow, breathing effort, heart rate, and blood oxygen levels. HSATs are convenient and less expensive, but they are not as comprehensive as in-lab PSG and may not detect all cases of sleep apnea, particularly mild or central sleep apnea.
Pro Tip: Your dentist can often be the first to spot signs of sleep apnea during a routine oral exam, noticing things like a highly scalloped tongue, enlarged tonsils, or specific jaw characteristics. They can then refer you to a sleep physician for a sleep study.
Treatment Options for Sleep Apnea
Once diagnosed, several effective treatment options are available, ranging from lifestyle modifications to medical devices and surgical procedures. The choice depends on the type and severity of your sleep apnea, as well as individual patient preferences and co-existing health conditions.
1. Lifestyle Changes and Behavioral Therapies
For mild sleep apnea or as an adjunct to other treatments, lifestyle adjustments can be highly beneficial:
- Weight Loss: Even a modest reduction in weight can significantly improve or resolve sleep apnea, particularly for individuals who are overweight or obese.
- Positional Therapy: Sleeping on your side can prevent the tongue and soft tissues from collapsing into the airway. Special pillows or devices that prevent back sleeping are available.
- Avoid Alcohol and Sedatives: Especially in the hours before bedtime, as these relax throat muscles.
- Quit Smoking: Smoking exacerbates airway inflammation.
- Treat Nasal Congestion: Use nasal sprays or allergy medications to keep nasal passages clear.
- Elevate the Head of Your Bed: Raising your head by a few inches can help open the airway.
2. Continuous Positive Airway Pressure (CPAP) Therapy
What It Is: CPAP is the most common and highly effective treatment for moderate to severe OSA. A CPAP machine delivers a continuous stream of filtered, pressurized air through a mask worn over your nose or nose and mouth while you sleep. This gentle air pressure acts as an "air splint" to keep your airway open, preventing apneas and hypopneas.
- Pros:
- Highly effective in resolving breathing pauses and improving oxygen saturation.
- Reduces daytime sleepiness and other symptoms.
- Significant health benefits, including reduced risk of heart disease and stroke.
- Generally safe and non-invasive.
- Cons:
- Can be uncomfortable initially; some find the mask claustrophobic.
- Noise from the machine (though modern machines are very quiet).
- Requires consistent use every night for optimal benefits.
- Potential side effects, including CPAP dry mouth.
Managing CPAP Dry Mouth
CPAP dry mouth is a common complaint among CPAP users. It occurs when the airflow from the machine dries out the mucous membranes in the mouth and throat.
- Causes:
- Mouth breathing: If you breathe through your mouth while using a nasal mask, air can escape, causing dryness.
- Mask leaks: Improperly fitting masks can allow air to escape, leading to dryness.
- Lack of humidification: Not using or incorrectly setting the humidifier on your CPAP machine.
- Medications: Certain medications can contribute to overall dryness.
- Solutions:
- Use a heated humidifier: Most modern CPAP machines come with an integrated heated humidifier, which adds moisture to the air you breathe. Adjust the heat and humidity levels to find what works best for you.
- Full-face mask: If you are a mouth breather, a full-face mask that covers both your nose and mouth can prevent air leakage and reduce dryness.
- Chin strap: If you use a nasal mask but tend to open your mouth during sleep, a chin strap can help keep your mouth closed.
- Check for mask leaks: Ensure your mask fits properly. Adjust straps or try different mask types if leaks are persistent.
- Biotene products: Use over-the-counter dry mouth sprays, gels, or rinses before bed.
- Hydration: Stay well-hydrated throughout the day.
- Nasal saline spray: Can help moisturize nasal passages.
3. Oral Appliance Therapy (OAT)
What It Is: For individuals with mild to moderate OSA, or those who cannot tolerate CPAP, oral appliance therapy is an excellent alternative. These custom-made, removable dental devices are worn during sleep and work by repositioning the lower jaw and/or tongue to keep the airway open. The most common type is the mandibular advancement device (MAD).
Mandibular Advancement Devices (MADs)
Mandibular advancement devices (MADs) are designed by dentists specializing in sleep medicine. They typically consist of two small plastic trays, similar to orthodontic retainers, that fit over your upper and lower teeth. These trays are connected by hinges or other mechanisms that gently push the lower jaw (mandible) forward. This forward movement of the jaw, in turn, moves the tongue and soft palate forward, increasing the space in the back of the throat and preventing airway collapse.
- How MADs Work: By maintaining an open airway, MADs prevent the vibrations that cause snoring and the obstructions that lead to sleep apnea events. They are adjustable, allowing the dentist to gradually advance the jaw to the optimal position for effective treatment.
- Pros:
- Non-invasive and comfortable for many users.
- Portable and easy to travel with.
- Quiet, unlike CPAP machines.
- High patient compliance rates compared to CPAP for mild to moderate OSA.
- Effective for primary snoring and mild to moderate OSA.
- Cons:
- Less effective for severe OSA compared to CPAP.
- Can cause temporary side effects: jaw soreness, tooth discomfort, excessive salivation or dry mouth (less common than CPAP dry mouth, but possible).
- Requires regular follow-up with a dentist for adjustments and monitoring.
- Cannot be used with certain dental conditions (e.g., severe gum disease, insufficient healthy teeth).
Pro Tip: While over-the-counter MADs are available, they are generally not recommended for treating sleep apnea. Custom-fitted mandibular advancement devices (MADs) from a qualified dentist are crucial for effectiveness, comfort, and preventing adverse dental changes. The American Academy of Dental Sleep Medicine (AADSM) and the American Dental Association (ADA) emphasize the importance of custom-fitted, titratable oral appliances.
4. Surgical Options
Surgery is typically considered when other treatments have failed or for specific anatomical issues.
- Uvulopalatopharyngoplasty (UPPP): Removes excess tissue from the back of the throat and palate.
- Maxillomandibular Advancement (MMA): A more invasive surgery that moves the upper and lower jaws forward, significantly enlarging the airway. Highly effective but complex.
- Genioglossus Advancement: Tightens the tendon that attaches the tongue to the lower jaw, preventing the tongue from falling back.
- Nasal Surgery: Corrects structural issues like a deviated septum to improve airflow.
- Hypoglossal Nerve Stimulation: An implantable device that stimulates the nerve controlling tongue movement, keeping the airway open during sleep.
5. Other Therapies
- Expiratory Positive Airway Pressure (EPAP) devices: Small, disposable devices placed over the nostrils that create back pressure when exhaling, keeping the airway open. For mild to moderate OSA.
- Oral exercises (orofacial myofunctional therapy): Strengthening the tongue and throat muscles can reduce snoring and mild OSA severity.
The Journey to Better Sleep: What to Expect During Treatment
Embarking on sleep apnea treatment involves a series of steps, from diagnosis to ongoing management. Understanding this process can help you feel more prepared and engaged in your care.
Step-by-Step Process for CPAP Therapy
- Diagnosis: Confirmed sleep apnea via a sleep study.
- Prescription: Your sleep physician prescribes CPAP therapy, specifying pressure settings.
- Equipment Setup: You'll work with a durable medical equipment (DME) provider to select a CPAP machine, humidifier, and mask. They will show you how to set up and use the device.
- Acclimation Period: It takes time to adjust to CPAP. Start by wearing the mask for short periods while awake, then during naps, and finally for a full night.
- Troubleshooting: Address common issues like mask leaks, discomfort, or CPAP dry mouth with your DME provider or sleep specialist. Adjustments to mask type, humidification, or pressure settings may be needed.
- Compliance Monitoring: Modern CPAP machines record usage data, which your doctor can review to ensure consistent use and effectiveness.
- Regular Follow-ups: Periodic check-ups with your sleep physician are essential to monitor your progress and address any new concerns.
Step-by-Step Process for Mandibular Advancement Device (MAD) Therapy
- Initial Consultation with a Sleep Dentist: Your dentist, specializing in dental sleep medicine, will assess your oral health, jaw structure, and sleep study results. They'll determine if you're a good candidate for a mandibular advancement device (MAD).
- Impressions and Molds: The dentist will take detailed impressions of your teeth and jaw, and potentially a bite registration, to create custom molds.
- Device Fabrication: A dental lab custom-fabricates your MAD based on the molds and your dentist's specifications. This typically takes 2-4 weeks.
- Fitting Appointment: You'll return to the dentist for the initial fitting. The dentist will ensure the device fits comfortably and adjust it to gently advance your lower jaw.
- Titration and Adjustment: Over several weeks or months, you'll gradually advance the MAD forward, typically in small increments (e.g., 0.5-1 mm at a time), under the guidance of your dentist. This titration process finds the optimal jaw position that effectively opens your airway without causing excessive discomfort.
- Follow-up Sleep Study (Optional but Recommended): Once the MAD is titrated to an effective position, a follow-up home sleep study may be recommended to objectively confirm the device's efficacy in reducing apneas.
- Ongoing Care: Regular dental check-ups (typically every 6-12 months) are necessary to monitor the device's condition, check for any changes in your bite, and ensure continued effectiveness.
Understanding the Financials: Cost and Insurance
The cost of diagnosing and treating sleep apnea can vary significantly depending on the type of test, treatment chosen, and your insurance coverage. It's essential to understand these potential expenses in the US market.
Diagnostic Costs
| Diagnostic Test | Average Cost (Without Insurance) | Insurance Coverage | Notes |
|---|---|---|---|
| Home Sleep Apnea Test | $250 - $500 | Often covered | Less expensive, convenient, but less comprehensive. |
| In-Lab Polysomnography | $1,000 - $5,000 | Often covered | More comprehensive, necessary for complex cases or initial diagnosis. |
| Consultation with Specialist | $100 - $300 | Often covered | Initial visit to a sleep physician or dental sleep specialist. |
Treatment Costs (Average US Price Ranges)
| Treatment Option | Average Cost (Without Insurance) | Insurance Coverage | Notes |
|---|---|---|---|
| CPAP Machine (with humidifier) | $500 - $1,500 | Often covered (DME benefit) | Can be rented or purchased. Masks and supplies (tubing, filters) are ongoing costs. |
| CPAP Mask & Supplies (annual) | $200 - $500 | Often covered (DME benefit) | Masks typically need replacement every 3-6 months. |
| Mandibular Advancement Device (MAD) | $1,800 - $3,500 | Often covered by medical insurance (not dental) | Custom-made by a qualified sleep dentist. Includes initial fitting, adjustments, and follow-up care. |
| Surgical Procedures (e.g., UPPP) | $3,000 - $15,000 | Often covered | Highly variable depending on complexity and facility fees. Maxillomandibular Advancement (MMA) can be significantly higher ($30,000+). |
| Hypoglossal Nerve Stimulator | $20,000 - $40,000+ | Increasingly covered by medical insurance | Includes device cost and implantation surgery. Requires specific criteria for candidacy. |
| Oral Myofunctional Therapy | $50 - $150 per session | Rarely covered; check with individual provider | Can involve multiple sessions. |
Important Considerations for Insurance Coverage:
- Medical vs. Dental Insurance: While sleep apnea is a medical condition, some dental appliances (like MADs) are fabricated by dentists. Typically, MADs are covered under your medical insurance, not dental insurance, because they are treating a medical diagnosis (sleep apnea). You will need a prescription from a sleep physician.
- Durable Medical Equipment (DME): CPAP machines and related supplies fall under DME benefits. Coverage usually requires a prescription and proof of diagnosis. Many plans have specific rules for replacement parts.
- Deductibles and Co-pays: You will likely be responsible for your plan's deductible and co-pays, even with coverage.
- Medicare and Medicaid: Medicare generally covers sleep studies and CPAP therapy if medically necessary. Medicaid coverage varies by state but often includes diagnostic tests and CPAP. MAD coverage under these programs can be more limited and may require specific prior authorizations.
- Payment Plans and Financing: Many dental and sleep clinics offer payment plans or work with third-party financing options (e.g., CareCredit) to help manage out-of-pocket costs.
Cost-Saving Tips:
- Verify Insurance Coverage: Always contact your medical insurance provider before any diagnostic test or treatment to understand your specific benefits, deductibles, co-pays, and any prior authorization requirements.
- Compare Providers: Costs for sleep studies and MADs can vary between providers. Get quotes if possible.
- Used CPAP Equipment: Be cautious with used CPAP machines, as they may not be calibrated correctly or may harbor germs. If considering, ensure it's professionally refurbished.
- Buy Supplies Online: Once you know your specific mask and supply needs, purchasing replacements from reputable online retailers can sometimes be cheaper than through your DME provider.
- Generic Medications: For any related health issues (like nasal congestion), opt for generic medications if available.
Life After Treatment: Recovery and Aftercare
Effective sleep apnea treatment is an ongoing commitment. Recovery involves adapting to your chosen therapy and maintaining a proactive approach to your health.
CPAP Aftercare
- Consistent Use: The most crucial aspect of CPAP aftercare is consistent use, every night, for the entire sleep period. Partial use offers only partial benefits.
- Mask Hygiene: Regularly clean your mask, tubing, and humidifier water chamber as per manufacturer guidelines to prevent bacterial growth and skin irritation.
- Supplies Replacement: Adhere to recommended replacement schedules for masks (every 3-6 months), filters (monthly), and tubing (every 6 months) to maintain effectiveness and hygiene.
- Follow-up with Sleep Specialist: Schedule regular appointments (e.g., annually) to review your progress, address any issues (like CPAP dry mouth), and adjust pressure settings if needed.
- Lifestyle Maintenance: Continue with any recommended lifestyle changes (weight management, avoiding alcohol/sedatives) to optimize treatment outcomes.
Oral Appliance (MAD) Aftercare
- Daily Cleaning: Clean your mandibular advancement device (MAD) daily with a toothbrush and mild soap or a denture cleaner. Avoid abrasive toothpastes.
- Proper Storage: Store your MAD in its protective case when not in use to prevent damage.
- Monitor for Side Effects: Be aware of potential side effects such as temporary jaw soreness, tooth tenderness, or changes in bite. Report persistent issues to your dentist.
- Regular Dental Check-ups: Continue with your regular dental cleanings and exams. Schedule specific follow-up appointments with your sleep dentist (every 6-12 months) to assess the appliance's fit, condition, and your oral health. The ADA recommends regular dental visits to monitor for potential bite changes.
- Replacement: MADs typically last 3-5 years, but this can vary. Your dentist will advise on replacement when necessary.
Pro Tip: If you experience any persistent discomfort, worsening of symptoms, or new issues (like extreme CPAP dry mouth that isn't resolving, or significant jaw pain with your MAD), contact your healthcare provider immediately. Adjustments are often simple and can significantly improve comfort and effectiveness.
Proactive Steps: Preventing Snoring and Sleep Apnea
While some risk factors for snoring and sleep apnea are genetic or anatomical, many can be modified through lifestyle choices.
- Maintain a Healthy Weight: Losing even a small amount of weight can reduce the fatty tissue in the throat, decreasing the likelihood of airway collapse.
- Avoid Alcohol and Sedatives Before Bed: These substances relax throat muscles, exacerbating snoring and sleep apnea.
- Quit Smoking: Smoking irritates and inflames the airways, leading to swelling and increased risk.
- Sleep on Your Side: Positional therapy can prevent the tongue and soft palate from falling back and obstructing the airway.
- Keep Nasal Passages Clear: Use saline sprays, decongestants, or allergy medications if you have chronic nasal congestion. Address conditions like a deviated septum with your doctor.
- Regular Exercise: Tones muscles throughout the body, including those in the throat, and helps with weight management.
- Elevate Your Head: Using an extra pillow or raising the head of your bed can help.
Potential Pitfalls: Risks and Complications of Untreated Sleep Apnea
Untreated sleep apnea is far more than just a noisy nuisance. The repeated drops in blood oxygen and fragmented sleep put immense stress on the body, leading to a cascade of serious health problems.
- Cardiovascular Disease:
- High Blood Pressure (Hypertension): Sleep apnea is a major cause of secondary hypertension. The sudden drops in oxygen and frequent awakenings stress the heart and blood vessels.
- Heart Attack and Stroke: Untreated sleep apnea significantly increases the risk of heart attack, stroke, and irregular heartbeats (arrhythmias like atrial fibrillation).
- Heart Failure: Can worsen or contribute to the development of heart failure.
- Type 2 Diabetes: Sleep apnea is strongly linked to insulin resistance and an increased risk of developing type 2 diabetes.
- Daytime Fatigue and Accidents: Chronic sleep deprivation leads to excessive daytime sleepiness, impaired concentration, and slower reaction times, increasing the risk of workplace accidents and drowsy driving accidents.
- Metabolic Syndrome: A cluster of conditions including high blood pressure, high blood sugar, excess body fat around the waist, and abnormal cholesterol levels, which collectively increase your risk of heart disease, stroke, and diabetes.
- Liver Problems: Non-alcoholic fatty liver disease (NAFLD) is more common in people with sleep apnea.
- Complications with Medications and Surgery: Patients with untreated sleep apnea may experience more complications with general anesthesia or certain sedatives, as they are more prone to breathing difficulties during recovery. It's crucial to inform your doctor if you have sleep apnea before any surgery.
- Mental Health Issues: The chronic stress of poor sleep can exacerbate or contribute to depression, anxiety, and irritability.
Children / Pediatric Considerations
Sleep apnea is not exclusively an adult condition; it can also affect children, often with different symptoms and causes. Pediatric sleep apnea can have significant impacts on a child's development, behavior, and academic performance.
Causes in Children
- Enlarged Tonsils and Adenoids: This is the most common cause of OSA in children.
- Obesity: Increasing rates of childhood obesity are contributing to higher rates of pediatric OSA.
- Craniofacial Abnormalities: Conditions like Down syndrome, Pierre Robin sequence, or Treacher Collins syndrome can predispose children to airway obstruction.
- Neuromuscular Disorders: Conditions affecting muscle tone can also lead to sleep apnea.
- Allergies and Chronic Nasal Congestion: Can contribute to mouth breathing and airway obstruction.
Signs and Symptoms in Children
Unlike adults who typically present with daytime sleepiness, children with sleep apnea may exhibit:
- Behavioral problems: Hyperactivity, attention deficit (often misdiagnosed as ADHD), aggression.
- Poor school performance: Difficulty concentrating, learning problems.
- Slow growth or "failure to thrive": Due to the increased metabolic demands of disrupted sleep.
- Bedwetting (enuresis): May develop or worsen.
- Loud snoring (often daily): Can be the most obvious sign.
- Pauses in breathing or gasping during sleep.
- Restless sleep: Unusual sleeping positions (e.g., neck hyperextended).
- Mouth breathing during the day and night.
- Morning headaches.
- Difficulty waking up.
Diagnosis and Treatment in Children
- Diagnosis: A pediatric sleep physician will typically recommend an in-lab sleep study for definitive diagnosis, as home sleep tests are less reliable in children.
- Treatment:
- Adenotonsillectomy: Removal of enlarged tonsils and adenoids is often the first-line treatment and can cure OSA in many children.
- Weight management: For obese children.
- CPAP: Used for children when surgery is not an option or unsuccessful, especially in more severe cases or those with underlying conditions.
- Orthodontic interventions: Rapid maxillary expansion or other dental appliances can help widen the airway in some children, a role where dentists are crucial.
Pro Tip: If you notice your child snores loudly, struggles to breathe at night, or has behavioral/academic issues despite adequate sleep, consult your pediatrician immediately. Early intervention is critical for healthy development.
Frequently Asked Questions
Is it normal to snore every night?
No, habitually snoring every night, especially if it's loud or accompanied by gasping, is not normal and is a strong indicator of a potential underlying issue like sleep apnea. While occasional light snoring might be harmless, consistent heavy snoring warrants evaluation by a healthcare professional.
What is the primary difference between snoring and sleep apnea?
The primary difference is that snoring is merely the sound of obstructed breathing, whereas sleep apnea involves actual pauses in breathing that lead to reduced oxygen levels in the blood and fragmented sleep. All sleep apnea patients snore, but not all snorers have sleep apnea.
Can a dentist diagnose sleep apnea?
While dentists cannot officially diagnose sleep apnea (that requires a sleep physician and a sleep study), they are often the first healthcare providers to screen for it. Dentists can recognize oral and facial indicators of sleep apnea and refer patients for a sleep study. They also play a crucial role in treating sleep apnea with oral appliances like mandibular advancement devices (MADs).
How much do mandibular advancement devices (MADs) cost?
Custom-fitted mandibular advancement devices (MADs) typically cost between $1,800 and $3,500 in the US without insurance. This price usually includes the initial consultation, impressions, device fabrication, multiple fitting appointments, and follow-up adjustments. Many medical insurance plans will cover a significant portion of this cost, as MADs treat a medical condition.
How do I know if my snoring is serious enough to be sleep apnea?
Look for accompanying symptoms: pauses in breathing, gasping or choking during sleep (reported by a bed partner), excessive daytime sleepiness, morning headaches, difficulty concentrating, or high blood pressure. If you experience any of these, it's serious enough to warrant a medical evaluation and potentially a sleep study.
What are the side effects of CPAP therapy?
Common side effects of CPAP therapy include mask discomfort, skin irritation from the mask, nasal congestion, and CPAP dry mouth. Many of these issues can be resolved or significantly reduced with proper mask fitting, adjusting humidity settings, or trying different mask types. Persistent side effects should be discussed with your sleep specialist.
Is surgery a cure for sleep apnea?
Surgery can be an effective treatment for specific anatomical causes of sleep apnea, and in some cases, it can significantly improve or even cure the condition. However, it's not a guaranteed cure for everyone and is typically considered after other non-invasive options, like CPAP or mandibular advancement devices (MADs), have been tried or are not suitable.
How long does it take to get used to CPAP or a MAD?
For both CPAP and mandibular advancement devices (MADs), there's usually an adjustment period. It can take anywhere from a few days to several weeks or even a few months to fully acclimate to wearing the device consistently and comfortably. Patience and consistent use are key.
Can I just buy an over-the-counter snoring mouthpiece?
While over-the-counter snoring mouthpieces exist, they are not recommended for treating sleep apnea. They are not custom-fitted, may not be effective, and can cause jaw pain or other dental issues. For sleep apnea, a custom-fabricated mandibular advancement device (MAD) prescribed and fitted by a qualified dentist is essential for safety and efficacy.
What if I can't tolerate CPAP?
If you can't tolerate CPAP, don't despair. There are excellent alternatives. Mandibular advancement devices (MADs) are a highly effective second-line treatment for mild to moderate OSA. Other options include positional therapy, lifestyle changes, and in some cases, surgical interventions or newer therapies like hypoglossal nerve stimulation. Discuss all options with your sleep physician.
When to See a Dentist
Your dental health professional plays a surprisingly vital role in the screening and treatment of sleep apnea. Knowing when to involve your dentist can be a critical step on your journey to better sleep.
You should see a dentist specializing in dental sleep medicine if:
- You snore loudly and consistently: Even if you don't suspect sleep apnea, your dentist can assess your oral anatomy and provide guidance.
- A sleep physician has diagnosed you with mild to moderate obstructive sleep apnea (OSA): Your dentist can evaluate you for mandibular advancement device (MAD) therapy as an alternative or complement to CPAP.
- You have been diagnosed with OSA but cannot tolerate CPAP therapy: If CPAP causes discomfort, claustrophobia, CPAP dry mouth, or you're simply non-compliant, a MAD fitted by a dentist might be your next best option.
- You experience symptoms like chronic dry mouth, teeth grinding (bruxism), or jaw pain (TMJ issues): These can sometimes be related to sleep-disordered breathing, and a sleep dentist can evaluate the connection.
- You notice changes in your bite or tooth alignment after using an oral appliance for sleep apnea: Regular follow-ups with your sleep dentist are crucial to monitor and manage these potential side effects.
Red flags that require immediate medical attention (from a physician, not just a dentist):
- Witnessed breathing pauses or gasping/choking during sleep.
- Excessive and debilitating daytime sleepiness that interferes with daily activities or driving.
- New or worsening high blood pressure, heart problems, or other serious health conditions that could be exacerbated by untreated sleep apnea.
While your primary care physician or a sleep specialist will handle the initial diagnosis and medical management of sleep apnea, your dentist is an indispensable part of the treatment team, particularly for the fitting and ongoing care of oral appliances. Don't underestimate the role your dental professional can play in improving your sleep and overall health.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
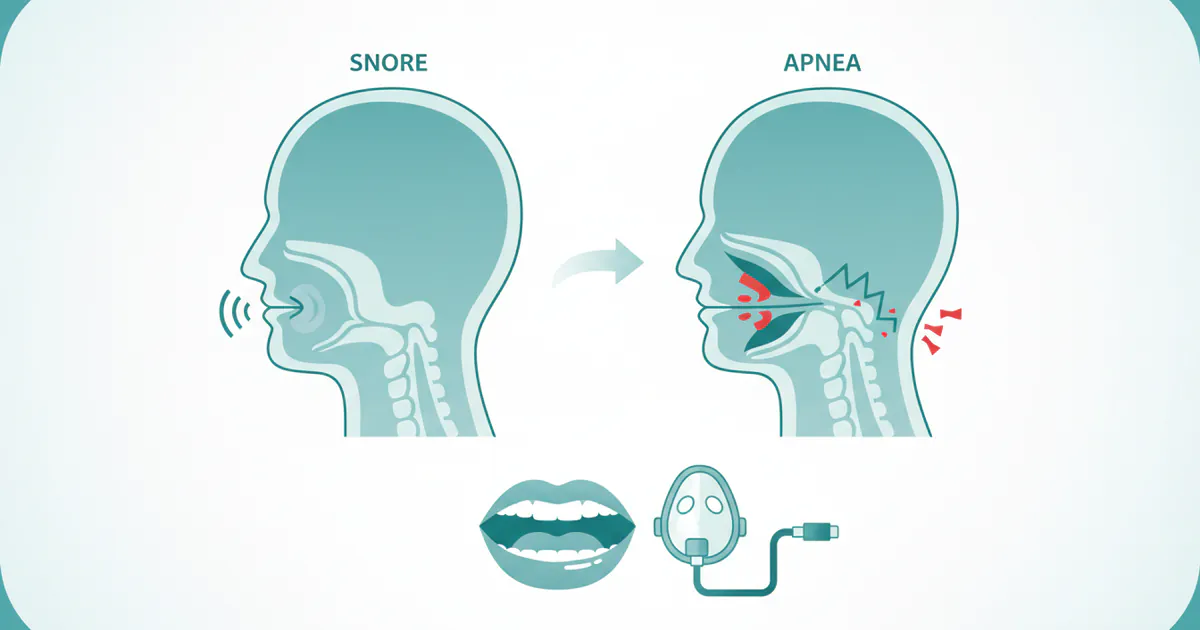
Difference Between Snoring and Sleep Apnea: Complete Guide
More than 80 million Americans regularly snore, and while often dismissed as a mere nuisance, loud and persistent snoring can be a critical indicator of a much more serious underlying health condition: sleep apnea. The difference between snoring and sleep apnea is profound, impacting not just yo
February 23, 2026

Mouth Taping for Snoring: Complete Guide
Snoring. It's the nocturnal soundtrack for millions of Americans, often a source of frustration for bed partners and a potential indicator of underlying health issues for the snorer themselves. Roughly 45% of adults snore occasionally, and 25% are habitual snorers, impacting sleep quality, relat
February 23, 2026
Is All Snoring Sleep Apnea
Many individuals, perhaps even you or a loved one, have been told they snore loudly. It's often dismissed as a harmless, albeit annoying, nocturnal habit. However, what if that nightly rumble is more than just noise? What if it's a critical indicator of an underlying health condition that significan
February 23, 2026
Cpap Dry Mouth Even With Humidifier: Complete Guide
Experiencing dry mouth while using a CPAP machine, even with a humidifier, is a common and incredibly frustrating issue for millions of Americans. It can disrupt sleep, diminish the effectiveness of your sleep apnea treatment, and significantly impact your oral health. Imagine waking up every mornin
February 23, 2026