Mandibular Advancement Devices: Complete Guide
Key Takeaways
- Snoring isn't just a nuisance for your bed partner; it can be a warning sign of a serious underlying health condition: obstructive sleep apnea (OSA). Affecting an estimated 30 million adults in the US, sleep apnea can lead to severe health consequences, from chronic fatigue and irritability to i
Mandibular Advancement Devices: Complete Guide
Snoring isn't just a nuisance for your bed partner; it can be a warning sign of a serious underlying health condition: obstructive sleep apnea (OSA). Affecting an estimated 30 million adults in the US, sleep apnea can lead to severe health consequences, from chronic fatigue and irritability to increased risks of heart disease, stroke, and diabetes. While continuous positive airway pressure (CPAP) remains the gold standard for many, a significant number of individuals find it uncomfortable or difficult to use consistently. This is where mandibular advancement devices (MADs) offer a promising and highly effective alternative, often referred to as a "sleep apnea mouth device." These custom-fit oral appliances can dramatically improve sleep quality, reduce or eliminate snoring, and mitigate the health risks associated with mild to moderate sleep apnea.

This comprehensive guide from SmilePedia.net will explore everything you need to know about mandibular advancement devices. We'll delve into what they are, how they work, the different types available, the process of obtaining one, their costs and insurance coverage, and importantly, how they compare to other treatment options. Whether you're tired of sleepless nights, concerned about loud snoring, or looking for an alternative to CPAP, understanding MADs could be your first step towards better health and restful sleep. We’ll also touch on related questions like "does mouth tape stop snoring" to provide a full picture of available solutions.
Key Takeaways:
- Mandibular Advancement Devices (MADs) are custom-fit oral appliances primarily used to treat mild to moderate obstructive sleep apnea (OSA) and primary snoring.
- They work by gently repositioning the lower jaw forward, preventing the collapse of soft tissues in the throat that obstruct the airway during sleep.
- MADs are a non-invasive, often preferred alternative for patients who cannot tolerate or achieve consistent use of CPAP therapy.
- The process involves a comprehensive dental exam, a sleep study for diagnosis, custom impressions, fitting, and follow-up adjustments with a qualified sleep dentist.
- Costs for a custom MAD in the US typically range from $1,800 to $4,500, generally covered by medical insurance (not dental) if prescribed for OSA, though deductibles and co-pays apply.
- Effectiveness is high for appropriate candidates, with studies showing significant reduction in snoring and sleep apnea events (Apnea-Hypopnea Index - AHI).
- While generally safe, potential side effects include jaw discomfort, tooth movement, and changes in bite, which are usually manageable with proper care and follow-ups.
What It Is / Overview
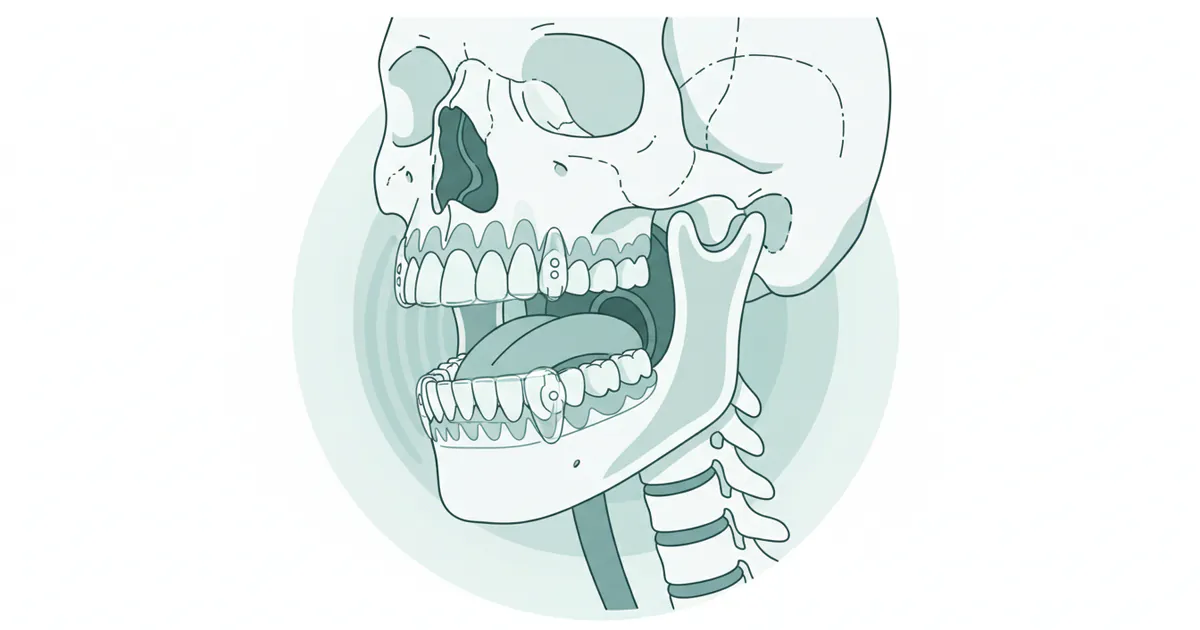
A Mandibular Advancement Device (MAD) is a custom-fabricated oral appliance designed to treat snoring and obstructive sleep apnea (OSA). Often referred to as a "sleep apnea mouth device," it works by repositioning the mandible (lower jaw) slightly forward and downward. This subtle adjustment helps to open the airway by pulling the tongue and associated soft tissues away from the back of the throat, preventing them from collapsing and blocking the airway during sleep.
When you sleep, the muscles in your throat, tongue, and jaw naturally relax. For some individuals, this relaxation allows the soft tissues to fall back into the airway, narrowing it and causing the vibrations we know as snoring. In more severe cases, this collapse can completely block the airway, leading to an apneic event – a temporary cessation of breathing. MADs counteract this by actively holding the jaw in a forward position, thereby maintaining an open and unobstructed air passage throughout the night.
These devices are typically made from durable, biocompatible acrylic materials, consisting of two separate pieces that fit over your upper and lower teeth, similar to a retainer or mouthguard. The two pieces are connected by hardware (often hinges or screw mechanisms) that allows for precise adjustment of the jaw's advancement. This adjustability is crucial, as the optimal position for each patient can vary and may need fine-tuning over time.
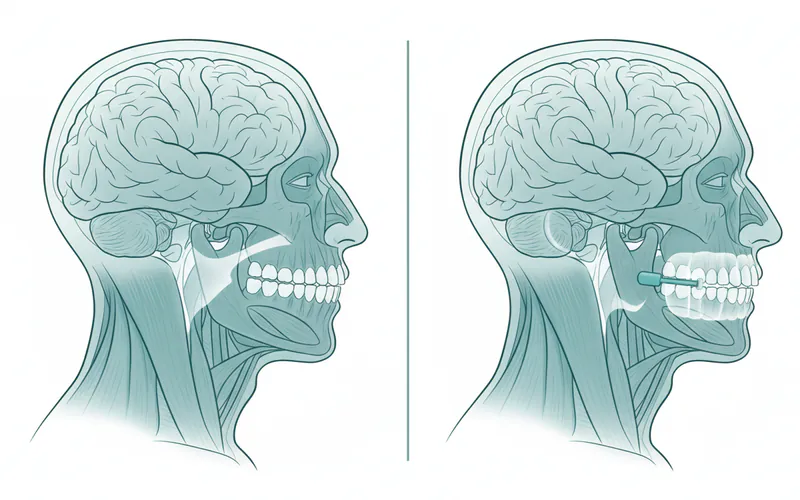
Types / Variations of Mandibular Advancement Devices
While the basic principle of jaw advancement remains the same, MADs come in several variations, broadly categorized by their customization and mechanism.
Custom-Made, Dentist-Prescribed MADs
These are the most effective and recommended type of MADs, designed and fitted by a qualified sleep dentist or orthodontist.
- Process: After a comprehensive oral examination and a diagnosis of OSA (typically confirmed by a sleep study), the dentist takes precise impressions of your teeth and jaw. These impressions are sent to a specialized dental lab where the custom device is fabricated.
- Materials and Design: Custom MADs are made from high-quality, durable acrylics. They typically consist of two trays—one for the upper arch and one for the lower—connected by a hinge or screw mechanism on the sides. This connection allows the dentist to incrementally adjust the degree of forward advancement of the lower jaw.
- Advantages:
- Precise Fit: Ensures maximum comfort, retention, and effectiveness.
- Adjustability: Allows for fine-tuning the jaw position, crucial for optimizing treatment and minimizing side effects.
- Durability: Built to last for several years with proper care.
- Medical Acceptance: These devices are FDA-cleared and typically covered by medical insurance for OSA treatment.
- Professional Oversight: Regular follow-ups with your dentist ensure the device remains effective and any potential side effects are managed.
- Disadvantages: Higher initial cost and a longer process due to custom fabrication.
Boil-and-Bite (Thermoplastic) Devices
These are over-the-counter (OTC) options that offer a more generic, self-fitted approach.
- Process: You submerge the device in hot water to soften the material, then bite into it to create an impression of your teeth. The material hardens, creating a semi-custom fit.
- Mechanism: Most boil-and-bite devices advance the jaw by a fixed amount or have limited adjustability using shims or different-sized pieces.
- Advantages: Lower cost and immediate availability.
- Disadvantages:
- Poor Fit: Rarely achieve the precise fit and comfort of a custom device, leading to discomfort, gum irritation, or even falling out during sleep.
- Limited Adjustability: Makes it difficult to find the optimal jaw position, potentially reducing effectiveness or increasing side effects.
- Lack of Professional Oversight: No dental professional guides the fitting or monitors progress, which can be risky, especially for undiagnosed OSA.
- Less Durable: Tend to wear out faster than custom devices.
- Not Recommended for OSA: While they might reduce simple snoring for some, the American Academy of Sleep Medicine (AASM) and American Dental Association (ADA) do not recommend boil-and-bite devices for treating diagnosed obstructive sleep apnea due to their unproven efficacy and potential for harm without professional supervision. They should generally be avoided for any condition more serious than occasional, mild snoring.
Pro Tip: For effective and safe treatment of sleep apnea or persistent snoring, always consult a sleep dentist for a custom-made, professionally fitted mandibular advancement device. Avoid over-the-counter boil-and-bite devices for anything beyond very occasional, mild snoring, and never for diagnosed sleep apnea.
Tongue Retaining Devices (TRDs)
While not strictly MADs, TRDs are another type of oral appliance sometimes used for snoring and sleep apnea.
- Mechanism: Instead of advancing the jaw, a TRD holds the tongue in a forward position using suction. It's often a soft, pliable device with a bulb that the tongue fits into.
- Indication: Useful for patients who cannot tolerate a MAD, have few or no teeth, or have temporomandibular joint (TMJ) issues that prevent jaw advancement.
- Advantages: Can be effective, especially for those with large tongues.
- Disadvantages: Some people find them uncomfortable or experience excess salivation or tongue soreness.
Causes / Why Snoring and Sleep Apnea Happen
Understanding the root causes of snoring and obstructive sleep apnea (OSA) helps clarify why mandibular advancement devices are an effective treatment. Both conditions stem from a collapse or narrowing of the airway during sleep.
Anatomical Factors
- Relaxed Throat Muscles: During sleep, muscles supporting the soft palate, uvula, tonsils, tongue, and throat walls relax. This relaxation can cause these tissues to sag into the airway.
- Large Tongue: An oversized tongue (macroglossia) can easily obstruct the airway when it relaxes and falls backward.
- Excess Throat Tissue: Extra tissue in the throat, such as enlarged tonsils or adenoids, or simply a thicker soft palate, can narrow the airway.
- Recessed Lower Jaw (Retrognathia): If your lower jaw naturally sits further back than your upper jaw, your airway may be inherently smaller, making you more prone to obstruction. This is a common indicator that a MAD could be particularly effective.
- Nasal Obstruction: A deviated septum, nasal polyps, or chronic congestion can force you to breathe through your mouth, which can exacerbate snoring and sleep apnea by allowing the jaw to drop further back.
Lifestyle and Other Contributing Factors
- Obesity: Excess weight, particularly around the neck, can contribute to thicker tissues in the throat and increase pressure on the airway, making collapse more likely. Fat deposits around the neck can narrow the internal diameter of the throat.
- Alcohol and Sedatives: These substances relax throat muscles excessively, increasing the likelihood and severity of snoring and apneic events.
- Smoking: Smoking irritates the throat tissues, causing inflammation and swelling, which can narrow the airway.
- Sleeping Position: Sleeping on your back often causes the tongue and soft palate to fall backward into the throat due due to gravity, worsening snoring and sleep apnea.
- Age: As we age, muscle tone throughout the body, including the throat, decreases, making us more susceptible to airway collapse.
- Genetics: A predisposition to certain facial structures or airway characteristics can be inherited.
Pro Tip: While a MAD can effectively treat the symptoms of snoring and OSA, addressing underlying lifestyle factors like weight management, avoiding alcohol before bed, and quitting smoking can significantly enhance treatment outcomes and improve overall health.
Signs and Symptoms of Snoring and Obstructive Sleep Apnea
It's crucial to differentiate between simple snoring and snoring that indicates obstructive sleep apnea, as the latter carries significant health risks. A mandibular advancement device can effectively treat both, but a proper diagnosis is key.
Common Signs and Symptoms
- Loud, Persistent Snoring: This is the most common and often the first symptom reported, frequently by a bed partner. Snoring associated with OSA is typically very loud and punctuated by silences.
- Observed Pauses in Breathing: A bed partner might notice you stop breathing for short periods (10 seconds or more) during sleep, followed by a gasp, choke, or snort as breathing resumes. This is a hallmark sign of sleep apnea.
- Daytime Sleepiness (Hypersomnia): Despite what feels like a full night's sleep, you wake up feeling unrefreshed and struggle to stay awake during the day. This can manifest as falling asleep at work, while driving, or during conversations.
- Morning Headaches: Waking up with a dull headache, which often resolves within an hour or two. This is thought to be due to decreased oxygen and increased carbon dioxide levels during sleep.
- Dry Mouth or Sore Throat: Frequent mouth breathing and gasping for air during sleep can lead to a dry mouth or sore throat upon waking.
- Irritability and Mood Changes: Chronic sleep deprivation can lead to increased irritability, mood swings, anxiety, and even depression.
- Difficulty Concentrating or Memory Problems: Lack of restorative sleep impairs cognitive function, making it hard to focus, remember things, or make decisions.
- High Blood Pressure: OSA is a significant risk factor for hypertension and is often found in patients with resistant hypertension.
- Frequent Urination at Night (Nocturia): Sleep apnea can cause changes in heart pressure that trigger the body to produce more urine, leading to frequent nighttime awakenings for bathroom trips.
- Restless Sleep: Tossing and turning, frequent awakenings, and a feeling of not getting deep, restorative sleep.
If you or your bed partner notice any combination of these symptoms, especially loud snoring accompanied by observed pauses in breathing and daytime fatigue, it's essential to seek medical evaluation. A sleep study (polysomnography) is necessary to accurately diagnose obstructive sleep apnea and determine its severity.
Treatment Options for Snoring and Obstructive Sleep Apnea
Mandibular Advancement Devices are one of several effective treatments for snoring and OSA. The best option depends on the severity of the condition, patient preferences, and other health factors.
1. Mandibular Advancement Devices (MADs)
- How it Works: As detailed, MADs reposition the lower jaw and tongue forward to keep the airway open.
- Pros:
- Non-Invasive: No surgery required.
- Portable: Easy to travel with.
- Quiet: Silent operation, unlike some CPAP machines.
- Comfortable: Custom-fit devices offer good comfort for many patients.
- Effective: Highly effective for mild to moderate OSA and primary snoring. The American Academy of Sleep Medicine (AASM) recommends oral appliances as a first-line treatment for patients with mild to moderate OSA who prefer them over CPAP, or for those with severe OSA who are intolerant of CPAP.
- Cons:
- Requires Adaptation: May cause initial jaw soreness, tooth sensitivity, or excess salivation.
- Not for Everyone: May not be suitable for individuals with severe OSA, certain dental conditions (e.g., severe gum disease, insufficient teeth), or TMJ disorders.
- Potential for Bite Changes: Long-term use can sometimes lead to minor changes in bite alignment, necessitating regular dental monitoring.
2. Continuous Positive Airway Pressure (CPAP) Therapy
- How it Works: CPAP machines deliver a continuous stream of pressurized air through a mask worn over the nose or mouth, creating an air splint that prevents the airway from collapsing.
- Pros:
- Gold Standard: Widely considered the most effective treatment for moderate to severe OSA.
- Highly Effective: Can normalize breathing patterns and significantly reduce AHI (Apnea-Hypopnea Index) scores.
- Cons:
- Mask Discomfort: Many users find the mask uncomfortable, claustrophobic, or irritating.
- Noise: The machine can produce some noise, though modern units are quieter.
- Portability Issues: Can be bulky to travel with.
- Compliance: A significant number of patients struggle with consistent CPAP use (compliance rates often cited as 50-70%).
- Dryness/Irritation: Can cause dry nose, throat, or skin irritation from the mask.
3. Lifestyle Modifications
- How it Works: Addressing contributing factors to improve overall health and reduce airway obstruction.
- Pros:
- No Side Effects: Generally beneficial for overall health.
- Cost-Effective: Often involves no direct cost.
- Cons:
- Requires Discipline: Can be challenging to implement and maintain.
- Limited Efficacy: May only be sufficient for very mild snoring or sleep apnea; rarely a standalone solution for moderate to severe cases.
- Examples: Weight loss, avoiding alcohol/sedatives before bed, changing sleep position (side sleeping), quitting smoking.
4. Surgical Interventions
- How it Works: Various procedures designed to physically remove or stiffen tissues that obstruct the airway.
- Pros:
- Potentially Curative: Some surgeries can eliminate the need for other treatments.
- Cons:
- Invasive: Involves significant recovery time and risks associated with surgery.
- Variable Success Rates: Success is not guaranteed, and effectiveness can diminish over time.
- Examples: Uvulopalatopharyngoplasty (UPPP), genial advancement, tongue reduction, maxillomandibular advancement (MMA). Often considered for severe cases, those with anatomical abnormalities, or when other treatments fail.
5. Tongue Retaining Devices (TRDs)
- How it Works: Holds the tongue forward using suction, as described above.
- Pros:
- Alternative: Good option for patients who can't tolerate MADs or have few teeth.
- Cons:
- Comfort Issues: Can cause tongue soreness or excess salivation.
- Less Common: Not as widely used as MADs.
6. Mouth Tape / Nasal Strips: Does Mouth Tape Stop Snoring?
- How it Works:
- Nasal Strips: Applied to the outside of the nose, they gently pull the nostrils open to improve nasal airflow. Primarily for nasal congestion-related snoring.
- Mouth Tape: Designed to keep the mouth closed during sleep, encouraging nasal breathing.
- Pros: Inexpensive, non-invasive.
- Cons:
- Limited Efficacy: These are not treatments for obstructive sleep apnea. They may help with very light, primary snoring caused by mouth breathing or minor nasal congestion.
- No Airway Support: They do not address the underlying anatomical collapse of the airway that causes OSA.
- Safety Concerns (Mouth Tape): If you have significant nasal obstruction, taping your mouth shut can be dangerous as it may restrict breathing further. There is no medical evidence to suggest mouth tape effectively treats or prevents OSA.
- Conclusion on "Does mouth tape stop snoring?": For mild snoring due to mouth breathing, it might help some individuals. However, for any snoring that is loud, persistent, or accompanied by symptoms of sleep apnea, mouth tape is completely inadequate and potentially unsafe. Always consult a medical professional for proper diagnosis and treatment.
Pro Tip: If you're diagnosed with OSA, always prioritize professionally prescribed and fitted treatments like MADs or CPAP over unproven home remedies.
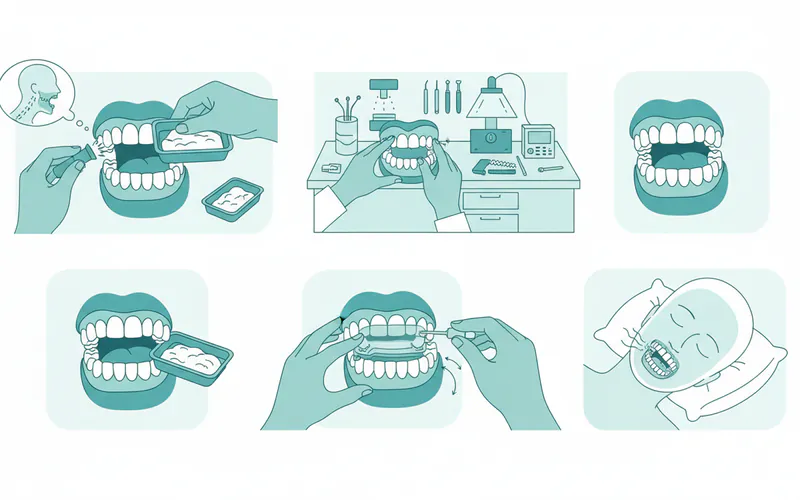
Step-by-Step Process for Getting a Mandibular Advancement Device
Obtaining a custom-fit mandibular advancement device is a structured process involving collaboration between your physician and a qualified sleep dentist.

1. Initial Consultation and Referral
- Your Primary Care Physician/Sleep Specialist: The journey usually begins with a visit to your doctor if you suspect you have sleep apnea or if a bed partner reports loud snoring and breathing pauses. They will likely recommend a sleep study.
- Sleep Study (Polysomnography): This diagnostic test, performed either in a sleep lab or at home, measures your breathing, oxygen levels, heart rate, and brain activity during sleep. It's essential to confirm a diagnosis of obstructive sleep apnea and determine its severity (mild, moderate, or severe).
- Referral to a Sleep Dentist: If you are diagnosed with mild to moderate OSA, or if you have severe OSA but cannot tolerate CPAP, your physician or sleep specialist will typically refer you to a dentist who specializes in dental sleep medicine (a "sleep dentist"). The ADA recognizes dental sleep medicine as an area of special interest for qualified dentists.
2. Comprehensive Dental Evaluation
- Oral Health Assessment: The sleep dentist will conduct a thorough examination of your teeth, gums, jaw joints (TMJ), and surrounding oral structures. They will check for signs of gum disease, loose teeth, TMJ dysfunction, and other conditions that might affect the suitability of a MAD.
- Airway Assessment: The dentist may also assess your throat and airway anatomy to understand potential areas of collapse.
- Impressions and Measurements: If you are deemed a good candidate, the dentist will take precise impressions (molds) of your upper and lower teeth, often using a digital scanner or traditional putty. They will also take specific measurements of your jaw, including the maximum comfortable forward position, to determine the optimal advancement range for your device. This often involves a "bite registration" where your jaw is positioned slightly forward.
3. Device Fabrication
- Dental Lab Work: The impressions and measurements are sent to a specialized dental laboratory. Highly trained technicians use these to custom-fabricate your MAD, ensuring it fits your unique oral anatomy perfectly. This process can take several weeks.
4. Fitting and Initial Adjustment
- Delivery Appointment: Once the device is ready, you'll return to the sleep dentist for the fitting. The dentist will ensure the MAD fits comfortably and securely over your teeth.
- Initial Advancement Setting: The dentist will set the initial advancement of your lower jaw. This is often a conservative setting to allow your jaw and muscles to adapt.
- Instructions: You will receive detailed instructions on how to insert and remove the device, clean it, and what to expect during the adaptation phase.
5. Follow-up Adjustments and Titration
- Gradual Adjustment: Over the next few weeks or months, you'll likely have several follow-up appointments. The dentist will gradually advance the lower jaw forward in small increments until the optimal therapeutic position is found. This process, known as "titration," aims to maximize airway opening while maintaining comfort.
- Objective Monitoring: To confirm the effectiveness of the device at its optimal setting, your dentist and sleep physician may recommend a follow-up sleep study or home sleep test with the MAD in place. This verifies that the device is successfully reducing your AHI and improving oxygen levels.
6. Ongoing Care and Maintenance
- Regular Dental Check-ups: You'll need periodic check-ups with your sleep dentist to monitor the device's condition, check for any changes in your bite or jaw comfort, and make any necessary adjustments.
- Device Longevity: With proper care, a custom MAD typically lasts 3-5 years, sometimes longer, before needing replacement.
Cost and Insurance for Mandibular Advancement Devices
Understanding the financial aspects of a mandibular advancement device is crucial. While the initial investment can seem substantial, the long-term health benefits and improved quality of life often outweigh the cost.
Average US Costs
The cost of a custom-made, dentist-prescribed mandibular advancement device in the United States generally ranges from $1,800 to $4,500.
- Low End ($1,800 - $2,500): May reflect simpler device designs, dentists with less specialized experience, or specific regional pricing.
- Mid-Range ($2,500 - $3,500): Most common price range, reflecting high-quality materials, custom lab fabrication, and comprehensive dental sleep medicine services.
- High End ($3,500 - $4,500+): Can include more advanced device designs, highly specialized practitioners, or regions with higher healthcare costs.
These costs typically include:
- Initial consultation and examination by the sleep dentist.
- Impressions or digital scans.
- The custom fabrication of the appliance by a dental lab.
- Initial fitting and several follow-up adjustment appointments.
- Follow-up sleep testing if required to verify efficacy.
Pro Tip: Be wary of significantly lower-priced "custom" options, as they might compromise on material quality, customization, or crucial follow-up care. Remember that boil-and-bite devices are considerably cheaper (often $50-$200) but are generally not recommended for treating sleep apnea due to lack of efficacy and potential risks.
Insurance Coverage
This is a critical distinction: Mandibular Advancement Devices are medically necessary devices for the treatment of a medical condition (obstructive sleep apnea). Therefore, they are typically covered by medical insurance, not dental insurance.
-
Medical Insurance:
- Most major medical insurance providers (e.g., Aetna, Anthem, Blue Cross Blue Shield, Cigna, UnitedHealthcare) offer coverage for MADs when prescribed by a physician for diagnosed OSA.
- Prior Authorization: Almost all medical insurance plans require prior authorization from your insurance company. Your sleep dentist's office will typically handle this submission on your behalf, providing the necessary documentation (e.g., sleep study results, physician's prescription).
- Deductibles and Co-pays: You will still be responsible for meeting your annual deductible and paying any co-insurance or co-pays as dictated by your plan.
- In-Network vs. Out-of-Network: Check if the sleep dentist is in your insurance network. Out-of-network providers may result in higher out-of-pocket costs.
- Medicare/Medicaid: Medicare generally covers oral appliances for OSA, often under Durable Medical Equipment (DME) benefits, similar to CPAP. Medicaid coverage varies significantly by state. It's essential to verify coverage directly with your specific plan.
-
Dental Insurance: Generally, dental insurance does not cover MADs because they are not primarily for dental care (like fillings or crowns) but for a medical condition. Some dental plans might offer a small benefit for oral appliances, but this is rare and usually very limited.
Payment Plans and Financing Options
If you have a high deductible, limited insurance coverage, or wish to pay out-of-pocket, several options are available:
- In-Office Payment Plans: Many dental offices offer flexible payment plans, allowing you to pay the cost over several months.
- Healthcare Financing (e.g., CareCredit): Specialized credit lines for healthcare expenses, often offering interest-free periods if paid within a certain timeframe.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): You can use pre-tax dollars from these accounts to pay for MADs, making them a tax-advantadvantaged way to cover costs.
Pro Tip: Always have your sleep dentist's office verify your specific medical insurance benefits before beginning treatment. They should provide a detailed breakdown of estimated costs, what insurance will cover, and your out-of-pocket responsibility.
Recovery and Aftercare with a Mandibular Advancement Device
Adjusting to a mandibular advancement device takes time and consistent effort. Proper aftercare and adherence to your dentist's instructions are key to maximizing effectiveness and minimizing side effects.
Initial Adaptation Period (First Few Weeks)
- Jaw Soreness and Discomfort: It's common to experience some mild soreness or stiffness in your jaw joints (TMJ) and muscles, especially during the first few mornings. This usually subsides as your jaw adapts.
- Management: Your dentist may recommend jaw exercises, warm compresses, or over-the-counter pain relievers.
- Tooth Sensitivity: Some teeth might feel slightly sensitive or tender, particularly when you first remove the device in the morning. This typically diminishes over time.
- Excess Salivation or Dry Mouth: Both are possible. Some individuals produce more saliva initially, while others experience dry mouth if their mouth opens slightly around the device.
- Changes in Bite Sensation: When you remove the MAD in the morning, your bite may feel "off" or different for a short period. This is temporary as your jaw muscles naturally return to their resting position.
- Management: Your dentist may provide a morning "repositioner" or instruct you on specific exercises (e.g., biting down on cotton rolls for 5-10 minutes) to help your bite return to normal quickly.
Ongoing Daily Care
- Cleaning Your Device:
- Daily: Clean your MAD every morning after removal using a soft toothbrush and mild soap or non-abrasive denture cleaner. Avoid toothpaste, which can be too abrasive and scratch the acrylic.
- Rinsing: Rinse thoroughly with cool water.
- Storage: Store the device in its protective case when not in use to prevent damage and keep it clean. Do not expose it to hot water or direct sunlight, as this can warp the acrylic.
- Oral Hygiene: Continue your regular oral hygiene routine, including brushing and flossing, as recommended by your general dentist. A clean mouth helps keep your appliance clean.
- Hydration: Drink plenty of water, especially if you experience dry mouth.
- Listen to Your Body: Pay attention to any persistent discomfort, pain, or changes in your bite that do not resolve.
Regular Follow-Up Appointments
- Sleep Dentist: Schedule and attend all recommended follow-up appointments with your sleep dentist. These are crucial for:
- Monitoring the device's fit and comfort.
- Making necessary adjustments to the jaw advancement.
- Assessing the health of your teeth and jaw joints.
- Ensuring the device continues to be effective.
- Typically, initial follow-ups are more frequent (e.g., every few weeks), then transition to annual check-ups.
- Sleep Physician: Your sleep physician may also want to monitor your overall sleep health and potentially recommend repeat sleep studies with the device to objectively confirm its effectiveness over time.
What to Watch For
- Persistent Jaw Pain or TMJ Symptoms: If jaw pain or clicking/popping in your jaw joints persists or worsens, contact your sleep dentist immediately.
- Significant Bite Changes: While minor temporary bite changes are normal, any significant or lasting changes should be reported.
- Loose Teeth or Gum Irritation: Though rare with custom devices, any new tooth mobility or persistent gum irritation needs professional attention.
- Damaged Device: If your MAD cracks or breaks, contact your dentist for repair or replacement instructions. Do not attempt to fix it yourself.
Pro Tip: Consistency is key. Wear your MAD every night as prescribed, even if you feel rested. Skipping nights can delay adaptation and reduce overall effectiveness.
Prevention of Snoring and Obstructive Sleep Apnea
While a mandibular advancement device treats existing snoring and OSA, certain lifestyle changes and awareness can help prevent these conditions or reduce their severity.
- Maintain a Healthy Weight: Obesity is a leading risk factor for OSA. Even a modest weight loss (e.g., 10-15% of body weight) can significantly reduce the severity of sleep apnea and snoring by reducing fat deposits around the neck and throat.
- Avoid Alcohol and Sedatives Before Bed: Alcohol, sedatives, and some muscle relaxants can overly relax throat muscles, increasing the likelihood of airway collapse. Avoid these substances for at least 3-4 hours before bedtime.
- Quit Smoking: Smoking irritates and inflames throat tissues, leading to swelling and narrowing of the airway. Quitting smoking can significantly improve respiratory health and reduce snoring.
- Change Sleep Position: Sleeping on your back allows gravity to pull the tongue and soft palate back, obstructing the airway. Try sleeping on your side. Special pillows or positional therapy devices can help maintain a side-sleeping position.
- Address Nasal Congestion: Chronic nasal congestion from allergies, colds, or anatomical issues (like a deviated septum) can force mouth breathing, exacerbating snoring. Use nasal sprays, antihistamines, or saline rinses, and consult an ENT specialist if congestion is persistent.
- Treat Underlying Medical Conditions: Conditions like hypothyroidism or chronic allergies can contribute to weight gain or nasal congestion, indirectly affecting sleep apnea. Managing these conditions can help.
- Regular Exercise: Physical activity improves overall muscle tone, including the throat muscles, and helps with weight management.
- Good Sleep Hygiene: While not directly preventing airway collapse, consistent sleep schedules and a comfortable sleep environment can improve overall sleep quality, which can be beneficial.
Pro Tip: If you have risk factors for OSA, proactive lifestyle changes can be highly beneficial. Even if you're already using a MAD, combining it with preventive measures can lead to better long-term outcomes and potentially reduce your reliance on the device or prevent progression of the condition.
Risks and Complications of Mandibular Advancement Devices
While custom-fit mandibular advancement devices are generally safe and well-tolerated, like any medical treatment, they come with potential risks and side effects. Most are mild and manageable, especially under the care of a qualified sleep dentist.
Common and Mild Side Effects (Usually Temporary)
- Jaw Soreness or Stiffness: This is the most frequently reported side effect, especially during the first few weeks of use. It typically resolves as your jaw muscles adapt to the new position. Your dentist can provide exercises or recommend pain relief.
- Tooth Tenderness or Sensitivity: You might notice some mild sensitivity in your teeth, particularly in the morning after removing the device.
- Excess Salivation or Dry Mouth: The presence of an appliance can stimulate saliva production, or conversely, if the device doesn't fully seal the mouth, it can lead to dry mouth.
- Gum Irritation: Rarely, the edges of the device might rub against the gums, causing irritation. A properly fitted custom device minimizes this risk.
- Temporary Bite Changes: Your bite might feel "off" or different for about 10-30 minutes after you remove the device in the morning. This is normal and usually resolves quickly as your jaw settles back into its natural position. Morning bite exercises (e.g., clenching on a bite plate) can speed up this process.

Less Common and Potentially More Significant Complications (Long-Term Use)
- Permanent Bite Changes (Malocclusion): This is the most significant long-term concern. Over many years of use, the forward pull on the lower jaw can lead to subtle, permanent changes in your dental occlusion (how your upper and lower teeth meet). This might include:
- Posterior Open Bite: Your back teeth no longer meet when you bite down.
- Anterior Open Bite: Your front teeth no longer meet when you bite down.
- Retrusion of Maxillary Incisors / Protrusion of Mandibular Incisors: Subtle tilting of front teeth.
- Management: Regular follow-up with your sleep dentist is crucial. They monitor for these changes and can sometimes adjust the device or prescribe specific exercises to mitigate them. In rare cases, orthodontic intervention might be considered. The ADA emphasizes proper patient selection and monitoring to minimize this risk.
- Temporomandibular Joint (TMJ) Dysfunction: While MADs are often carefully fitted to avoid exacerbating TMJ issues, some individuals might develop new or worsening TMJ pain, clicking, or limited jaw movement.
- Management: If you have pre-existing TMJ issues, discuss them thoroughly with your dentist. They might recommend alternative treatments or a specific MAD design. If new TMJ symptoms arise, the device may need adjustment or even discontinuation in severe cases.
- Tooth Movement or Loosening: With a custom-fit device, this risk is very low, as the forces are distributed evenly. However, poorly fitting or improperly adjusted devices could theoretically place undue stress on individual teeth. This is a significant risk with over-the-counter devices.
- Allergic Reactions: Very rarely, individuals might be allergic to the materials used in the appliance (e.g., certain acrylics). This is typically identified and addressed during the fitting process.
- Device Breakage: Although made of durable materials, MADs can crack or break, especially if dropped or mishandled.
Pro Tip: The best way to mitigate risks and complications is to ensure your MAD is custom-made and fitted by a qualified sleep dentist. Regular follow-up appointments are essential for monitoring your oral health, jaw joint function, and the device's effectiveness, allowing for early detection and management of any potential issues.
Comparison Tables
To help visualize the differences between key treatment options and device types, here are two comparison tables.
Table 1: Mandibular Advancement Devices vs. Other OSA Treatments
| Feature | Mandibular Advancement Device (MAD) | CPAP Therapy (Continuous Positive Airway Pressure) | Lifestyle Modifications (Weight Loss, Positional Therapy) | Surgery (e.g., UPPP, MMA) |
|---|---|---|---|---|
| Primary Indication | Mild-Moderate OSA, Primary Snoring; CPAP intolerant (any severity) | Moderate-Severe OSA (Gold Standard); also for mild OSA if preferred | Very Mild OSA, Simple Snoring; Adjunct to other treatments | Moderate-Severe OSA; When other treatments fail or anatomical abnormality |
| Mechanism | Repositions lower jaw & tongue forward to open airway | Delivers pressurized air to keep airway open | Reduces weight, avoids back sleeping, abstains from depressants | Physically alters/removes airway-obstructing tissues |
| Invasiveness | Non-invasive (oral appliance) | Non-invasive (mask and machine) | Non-invasive | Highly invasive |
| Cost Range (US) | $1,800 - $4,500 | $800 - $3,000 (machine + mask, without humidifier) | $0 - $500 (for specific pillows/devices, gym memberships) | $5,000 - $100,000+ (depending on procedure, facility fees) |
| Insurance Coverage | Medical (for OSA), requires prior auth. | Medical (DME), requires prior auth. | Generally none, except for some specific medical weight loss programs | Medical (for OSA), requires prior auth. |
| Effectiveness | High for appropriate candidates (mild-mod OSA) | Very High (Gold Standard) | Variable; often limited as standalone treatment | Variable; success rates can be unpredictable and may decrease over time |
| Comfort/Portability | High comfort (custom-fit), very portable | Can be uncomfortable (mask issues), less portable | Very comfortable, no devices needed | Post-surgery recovery discomfort, then potentially no discomfort |
| Common Side Effects | Jaw soreness, tooth sensitivity, temporary bite changes | Mask discomfort, dry mouth, skin irritation, noise | None directly, but lifestyle changes can be challenging | Pain, swelling, bleeding, infection, voice changes, swallowing difficulty |
| Long-Term Care | Regular dental check-ups, device cleaning | Regular mask/tubing replacement, machine maintenance | Ongoing commitment to lifestyle changes | Post-op monitoring, potential for revision surgery |
Table 2: Custom MADs vs. Over-the-Counter Boil-and-Bite Devices
| Feature | Custom-Made Mandibular Advancement Device (MAD) | Over-the-Counter Boil-and-Bite Device (e.g., "Snoring Mouthguard") |
|---|---|---|
| Fit & Comfort | Precisely custom-fit to your unique dental anatomy; high comfort | Generic, self-fitted, thermoplastic material; often poor fit and comfort |
| Effectiveness | Clinically proven for mild-moderate OSA & snoring; FDA-cleared | Unproven for OSA; may offer temporary, limited relief for simple snoring only |
| Adjustability | Highly adjustable by dentist; gradual titration for optimal jaw position | Limited or no adjustability; fixed jaw position |
| Professional Oversight | Required (sleep dentist consultation, fitting, follow-ups) | None; self-administered |
| Materials | High-quality, durable, biocompatible dental acrylics | Generic, often less durable thermoplastic plastics |
| Cost Range (US) | $1,800 - $4,500 | $50 - $200 |
| Insurance Coverage | Typically covered by medical insurance for OSA | Generally not covered by any insurance |
| Risks | Minimal when professionally managed; minor long-term bite changes possible | Significant risk of jaw pain, TMJ issues, tooth movement, gum irritation, exacerbation of undiagnosed OSA |
| FDA Clearance | Yes, as Class II medical devices for OSA | Some may have general "anti-snoring" claims, but not cleared for OSA treatment |
| Longevity | 3-5 years with proper care | 3-12 months (due to wear and tear, material degradation) |
Children / Pediatric Considerations
While Mandibular Advancement Devices are primarily for adults, snoring and sleep-disordered breathing are concerns in children too. Pediatric obstructive sleep apnea (POSA) affects 1-5% of children, and if left untreated, can lead to serious developmental, behavioral, and cardiovascular problems.
Causes of POSA in Children: Unlike adults, where obesity is a major factor, the most common cause of POSA in children is enlarged tonsils and adenoids. Other factors include craniofacial abnormalities (e.g., smaller jaws), obesity, and neuromuscular disorders.
Diagnosis: Diagnosis also involves a sleep study (polysomnography), ideally conducted in a pediatric sleep lab.
Treatment Approaches for POSA:
- Adenotonsillectomy: The removal of enlarged tonsils and adenoids is often the first-line treatment for POSA, especially if these are the primary cause of obstruction. It has a high success rate.
- Orthodontic/Orthopedic Interventions: For children with craniofacial growth deficiencies or smaller jaws (like a recessed lower jaw), orthodontic treatments can play a crucial role.
- Rapid Palatal Expansion (RPE): This device can widen the upper jaw, creating more space in the nasal and oral cavities, which can improve breathing.
- Functional Appliances: These devices (not strictly MADs in the adult sense, but similar in principle) can guide jaw growth in developing children and adolescents to achieve better airway dimensions. These are typically used for children whose bones are still growing.
- Mandibular Advancement Devices for Adolescents: For older adolescents who have stopped growing and have mild to moderate OSA or significant snoring, a custom-fit MAD, similar to those used in adults, may be considered if adenotonsillectomy is not indicated or unsuccessful, or if CPAP is not tolerated. However, careful assessment of dental development and growth status is paramount.
- Weight Management: For obese children, weight loss is a critical component of treatment.
- CPAP: For severe POSA that doesn't respond to other treatments, CPAP can be used in children, though compliance can be challenging.
Pro Tip for Parents: If your child snores loudly, gasps for breath, wets the bed, exhibits daytime sleepiness, or has behavioral issues (like ADHD-like symptoms), consult your pediatrician. Early diagnosis and treatment of POSA are vital for preventing long-term health and developmental problems. A pediatric sleep specialist or an orthodontist specializing in airway issues can provide specific guidance.
Frequently Asked Questions
1. How effective are Mandibular Advancement Devices for sleep apnea?
Mandibular Advancement Devices are highly effective for patients with mild to moderate obstructive sleep apnea (OSA) and primary snoring. Studies show they can reduce the Apnea-Hypopnea Index (AHI) by 50% or more in a significant percentage of suitable patients, often comparable to CPAP for mild to moderate cases. The American Academy of Sleep Medicine (AASM) recommends them as a first-line treatment option.
2. Is getting a custom MAD painful?
The process of getting a custom MAD is generally not painful. Taking impressions is non-invasive, and the fitting appointment involves adjusting the device for comfort. You may experience some temporary jaw soreness, tooth tenderness, or muscle stiffness during the initial adaptation period (first few weeks), but this usually subsides. Your dentist can recommend strategies to manage any discomfort.
3. How long does a MAD last?
A custom-made mandibular advancement device typically lasts for 3 to 5 years with proper care and maintenance. The longevity depends on the quality of the materials, how well you care for it, and any changes in your oral health or bite over time. Regular check-ups with your sleep dentist can help extend its lifespan.
4. What are the main alternatives to a MAD?
The primary alternatives include Continuous Positive Airway Pressure (CPAP) therapy, which is the gold standard for moderate to severe OSA. Other options include lifestyle modifications (weight loss, positional therapy), surgical interventions (e.g., UPPP, genial advancement), and, in rare cases, tongue-retaining devices. The choice depends on OSA severity, patient preference, and other health factors.
5. Will a MAD cure my sleep apnea?
A mandibular advancement device effectively manages the symptoms of sleep apnea by keeping your airway open during sleep. While it can dramatically reduce or eliminate apneic events and snoring, it is a treatment, not a cure. If you stop using the device, your sleep apnea symptoms will typically return. Combining MAD use with healthy lifestyle changes can lead to optimal long-term management.
6. Can I get a MAD if I have missing teeth or dentures?
Whether you can use a MAD with missing teeth or dentures depends on the extent of tooth loss and the stability of your dental structures. If you have several missing teeth, a MAD may not have enough stable anchor points. For complete dentures, a special type of oral appliance may be fabricated, but this requires careful assessment by a sleep dentist. Partial dentures might need to be removed or designed to integrate with the MAD.
7. How long does it take to get used to wearing a MAD?
Most patients adapt to wearing a custom MAD within a few days to a few weeks. Initial discomfort, such as jaw soreness or excess salivation, typically lessens over this period. Consistent nightly use is key to faster adaptation. Your sleep dentist will guide you through the gradual adjustment (titration) process to find the most comfortable and effective jaw position.
8. What are the long-term side effects of using a MAD?
The most significant long-term side effect, though relatively uncommon with proper monitoring, is a subtle and gradual change in bite (occlusion), such as a posterior open bite where back teeth no longer meet. Regular follow-up appointments with your sleep dentist are crucial to monitor for these changes and implement strategies (like morning bite exercises) to minimize or manage them.
9. Can I use a MAD if I have TMJ problems?
The suitability of a MAD for individuals with Temporomandibular Joint (TMJ) problems needs careful evaluation by a sleep dentist. Some MAD designs can exacerbate TMJ symptoms, while others are specifically designed to be gentler on the joints. Depending on the severity and type of your TMJ issues, your dentist might recommend specific treatments before or in conjunction with MAD therapy, or suggest alternative OSA treatments.
10. Do I still need a sleep study if I use a MAD?
Yes, a sleep study (polysomnography) is essential for the initial diagnosis of obstructive sleep apnea and to determine its severity before a MAD is prescribed. After the device has been fitted and adjusted to its optimal position, your sleep physician or dentist may recommend a follow-up sleep study or home sleep test with the MAD in place. This objective monitoring confirms the device's effectiveness in reducing your AHI and improving your breathing.
When to See a Dentist
Recognizing when to seek professional dental and medical attention for snoring and sleep apnea is crucial for your health.
You should see a dentist specializing in sleep medicine if:
- You've been diagnosed with mild to moderate Obstructive Sleep Apnea (OSA) by a physician or sleep specialist and are looking for an alternative to CPAP or find CPAP difficult to tolerate.
- You snore loudly and consistently, even if you haven't been formally diagnosed with OSA, and suspect it's impacting your sleep quality or your partner's.
- Your physician has recommended an oral appliance as a treatment option for your sleep-disordered breathing.
- You experience symptoms of OSA, such as observed pauses in breathing during sleep, chronic daytime fatigue, morning headaches, or high blood pressure, even if you are already using a CPAP and suspect you need an alternative.
When to see your general dentist (who may refer you to a sleep dentist):
- You are experiencing any new or worsening oral health issues while using a MAD, such as persistent jaw pain, tooth sensitivity, changes in your bite, or gum irritation.
- Your MAD becomes damaged or no longer fits comfortably.
- It's time for your annual dental check-up, and you want to discuss your sleep health.
When to seek immediate medical attention (from your physician or emergency services):
- You or your bed partner observe prolonged or severe breathing pauses during sleep.
- You experience severe chest pain or shortness of breath along with sleep disturbances.
- You have sudden, severe headaches that are out of character for you.
- You have sudden, extreme daytime sleepiness that puts you at risk (e.g., while driving).
Remember, addressing snoring and sleep apnea is not just about quiet nights; it's about protecting your long-term cardiovascular, metabolic, and cognitive health. Don't hesitate to consult with healthcare professionals if you have concerns.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Difference Between Snoring and Sleep Apnea: Complete Guide
More than 80 million Americans regularly snore, and while often dismissed as a mere nuisance, loud and persistent snoring can be a critical indicator of a much more serious underlying health condition: sleep apnea. The difference between snoring and sleep apnea is profound, impacting not just yo
February 23, 2026

Mouth Taping for Snoring: Complete Guide
Snoring. It's the nocturnal soundtrack for millions of Americans, often a source of frustration for bed partners and a potential indicator of underlying health issues for the snorer themselves. Roughly 45% of adults snore occasionally, and 25% are habitual snorers, impacting sleep quality, relat
February 23, 2026
Is All Snoring Sleep Apnea
Many individuals, perhaps even you or a loved one, have been told they snore loudly. It's often dismissed as a harmless, albeit annoying, nocturnal habit. However, what if that nightly rumble is more than just noise? What if it's a critical indicator of an underlying health condition that significan
February 23, 2026
Cpap Dry Mouth Even With Humidifier: Complete Guide
Experiencing dry mouth while using a CPAP machine, even with a humidifier, is a common and incredibly frustrating issue for millions of Americans. It can disrupt sleep, diminish the effectiveness of your sleep apnea treatment, and significantly impact your oral health. Imagine waking up every mornin
February 23, 2026