Best Mouth Guard for Snoring: Complete Guide
Key Takeaways
- Snoring isn't just a nuisance; for millions of Americans, it's a nightly disruption that impacts sleep quality, relationships, and overall health. If you're one of the approximately 90 million adults in the US who snore, you know the frustration it can cause – from sleep-deprived partners to wak
Best Mouth Guard for Snoring: Complete Guide
Snoring isn't just a nuisance; for millions of Americans, it's a nightly disruption that impacts sleep quality, relationships, and overall health. If you're one of the approximately 90 million adults in the US who snore, you know the frustration it can cause – from sleep-deprived partners to waking up feeling anything but refreshed. While snoring is often dismissed as a harmless habit, it can be a sign of underlying health issues, including obstructive sleep apnea (OSA). Fortunately, a solution as straightforward as a specialized snoring mouth piece can offer significant relief. In this comprehensive guide, we'll explore everything you need to know about finding the best mouth guard for snoring, delving into their types, efficacy, costs, and how they can transform your nights. Understanding these devices is the first step toward quieter nights and healthier days, providing a non-invasive, often highly effective way to manage snoring and improve sleep quality for you and your household.

Key Takeaways:
Key Takeaways:
- Primary Solution: Mandibular Advancement Devices (MADs) and Tongue Retaining Devices (TRDs) are the main types of snoring mouth guards. MADs are more common.
- How They Work: These devices work by repositioning the jaw forward or holding the tongue in place, preventing soft tissues from collapsing and obstructing the airway during sleep.
- Effectiveness: Custom-fitted mouth guards prescribed by a dentist are significantly more effective and comfortable than over-the-counter (OTC) options, with success rates often exceeding 80% for primary snoring and mild to moderate obstructive sleep apnea.
- Cost: OTC mouth guards range from $20 to $150. Custom-fitted dental snoring mouth pieces typically cost between $800 and $3,000, with some high-end appliances reaching $4,000, reflecting personalized design and professional oversight.
- Insurance Coverage: Custom dental appliances for snoring, especially when prescribed for diagnosed sleep apnea, are often covered by medical insurance (not dental insurance) under Durable Medical Equipment (DME) benefits. Verification of benefits is crucial.
- Timeline: The process for getting a custom mouth guard involves an initial consultation, potentially a sleep study, impressions, and fittings, usually taking 2-4 weeks from start to finish.
- Maintenance: Daily cleaning with a soft brush and non-abrasive cleaner, along with proper storage, is essential for device longevity and oral hygiene. Regular dental check-ups are also vital to monitor oral health and appliance fit.
What It Is: An Overview of Snoring Mouth Guards
A snoring mouth guard, more accurately termed an oral appliance, is a custom-made or prefabricated device worn in the mouth during sleep. Its primary purpose is to alleviate snoring by addressing the anatomical factors that contribute to it. Snoring occurs when the airflow through the mouth and nose is obstructed, causing the soft tissues in the back of the throat to vibrate. This obstruction can be due to a relaxed jaw, a tongue falling backward, or excess tissue in the throat.
These dental devices work by repositioning the lower jaw (mandible) slightly forward or by holding the tongue in a more anterior position. By doing so, they increase the space in the airway, preventing the collapse of the soft palate, uvula, and tongue base that commonly leads to the noisy vibrations of snoring. While often considered a treatment for snoring, these appliances are also a recognized treatment for mild to moderate obstructive sleep apnea (OSA), a more serious condition characterized by repeated pauses in breathing during sleep.
The effectiveness of a snoring mouth piece stems from its ability to create a clear, open passage for air, reducing or eliminating the vibrations that cause snoring. They offer a non-surgical, relatively comfortable, and often highly effective alternative for individuals who cannot tolerate or do not require more invasive treatments like Continuous Positive Airway Pressure (CPAP) therapy or surgery.
Types of Snoring Mouth Guards
Not all snoring mouth guards are created equal. They generally fall into two main categories, each with its own mechanism of action, advantages, and disadvantages. Understanding these types is crucial in determining the best mouth guard for snoring for your specific needs.
Mandibular Advancement Devices (MADs)
Mandibular Advancement Devices (MADs) are the most common and widely prescribed type of oral appliance for snoring and sleep apnea. These devices work by gently pushing the lower jaw and tongue forward, which tightens the soft tissues and muscles in the upper airway, preventing them from collapsing backward and obstructing breathing.
1. Custom-Fitted MADs (Dentist-Prescribed)
- Description: These are precision-made devices crafted by a dental professional after taking impressions or digital scans of your teeth. They are typically made from acrylic or other durable dental plastics.
- Pros:
- Superior Fit and Comfort: Custom-fitted MADs offer the most comfortable and secure fit, minimizing discomfort and maximizing compliance.
- Adjustability: Most custom MADs are adjustable, allowing your dentist to fine-tune the degree of jaw advancement for optimal effectiveness and comfort. This adjustability is key to finding the "sweet spot" for airway opening without excessive jaw strain.
- Durability: Made from high-quality materials, they are designed to last for several years with proper care.
- Effectiveness: Significantly more effective than OTC options, especially for mild to moderate OSA, often with a success rate of 80% or more for primary snoring.
- Professional Oversight: Prescribed and monitored by a dentist trained in sleep medicine, ensuring safety and efficacy.
- Cons:
- Cost: Considerably more expensive than over-the-counter options, ranging from $800 to $3,000+.
- Time Commitment: Requires multiple dental visits for impressions, fitting, and adjustments.
- Potential Side Effects: Can cause temporary jaw soreness, tooth sensitivity, or changes in bite, though these are usually managed with adjustments.
2. Boil-and-Bite MADs (Over-the-Counter)
- Description: These devices are purchased without a prescription and are designed to be molded at home. They typically involve softening the device in hot water and then biting into it to create an impression of your teeth.
- Pros:
- Affordability: Much less expensive, typically ranging from $20 to $150.
- Accessibility: Easily purchased online or at pharmacies without a prescription.
- Immediate Use: Can be used relatively quickly after purchase and molding.
- Cons:
- Limited Customization/Adjustability: While they offer a basic custom fit, they lack the precise adjustability of dentist-prescribed devices, making it harder to find the optimal jaw position. Some advanced OTC models offer limited adjustability.
- Less Comfortable: The fit is often not as secure or comfortable as custom-made devices, potentially leading to discomfort, gum irritation, or even falling out during the night.
- Variable Effectiveness: Effectiveness can be inconsistent due to the less precise fit and lack of professional guidance. They are generally less effective for serious snoring or sleep apnea.
- Durability: Often made from less durable materials, requiring more frequent replacement.
- Risk of Misuse: Without professional guidance, there's a risk of improper fitting, which can exacerbate jaw issues or provide inadequate treatment.
Tongue Retaining Devices (TRDs)
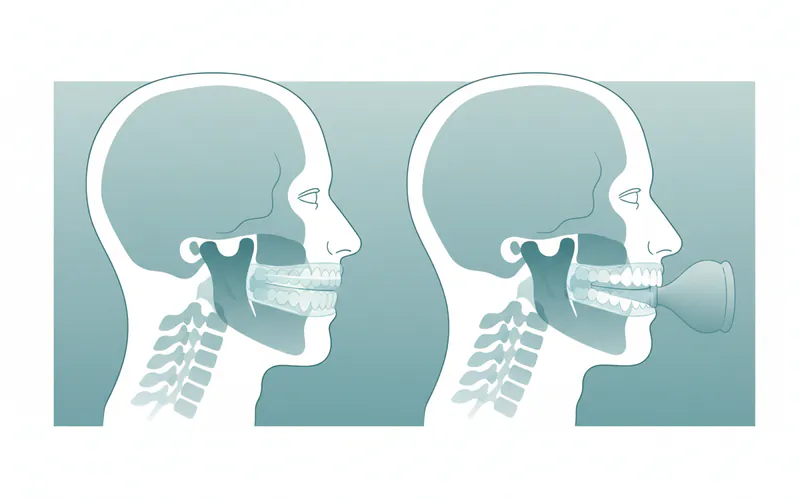
Tongue Retaining Devices (TRDs) are less common than MADs but can be an effective alternative, especially for individuals who cannot tolerate MADs or have specific dental issues (e.g., missing teeth, dentures, TMJ disorders). TRDs work by holding the tongue in a forward position using a suction bulb, preventing it from falling back into the throat and obstructing the airway.
- Description: A TRD is typically a soft, flexible mouthpiece that fits between the lips and teeth. It has a small bulb that creates suction to hold the tongue gently forward.
- Pros:
- No Jaw Movement: Does not require advancement of the lower jaw, making it suitable for those with TMJ issues, dental restorations, or no teeth.
- Simplicity: Often simpler in design and use compared to MADs.
- Effectiveness: Can be very effective for snoring and mild OSA, particularly if tongue base collapse is the primary cause.
- Cons:
- Foreign Body Sensation: Some users find the feeling of the tongue being held forward by suction uncomfortable or strange, leading to a gag reflex.
- Excess Salivation: Can initially cause increased salivation.
- Limited Availability: Fewer options are available, and custom versions are less common than custom MADs.
- Tongue Soreness: Can cause temporary tongue soreness.
Choosing Between OTC and Custom-Fitted
| Feature | Over-the-Counter (Boil-and-Bite MAD) | Custom-Fitted (Dentist-Prescribed MAD/TRD) |
|---|---|---|
| Cost | $20 - $150 | $800 - $3,000+ |
| Fit & Comfort | Basic, less precise, can be bulky | Superior, precise, customized to your mouth |
| Adjustability | Limited or none | Highly adjustable, dentist-controlled |
| Effectiveness | Variable, best for very mild snoring | High, proven for snoring & mild-moderate OSA |
| Durability | 3-6 months | 2-5 years |
| Professional Input | None | Essential, ongoing monitoring |
| Insurance | Generally not covered | Often covered by medical insurance for OSA |
| Risk of Side Effects | Higher risk of jaw pain, tooth movement | Lower risk due to precise fit & adjustment |
Pro Tip: While OTC options are tempting due to their low cost, it's highly recommended to consult a dentist specializing in sleep medicine if you're experiencing chronic snoring or suspect sleep apnea. A professional evaluation ensures proper diagnosis and selection of the best mouth guard for snoring that won't cause unintended dental or jaw issues.
Causes of Snoring: Why It Happens
Understanding why you snore is the first step toward effective treatment. Snoring occurs when the soft tissues in your upper airway vibrate as air passes through them during sleep. This vibration is typically caused by a partial obstruction of the airway.
Anatomical Factors
- Relaxed Jaw and Tongue: During sleep, the muscles in your jaw, tongue, and throat relax. If they relax too much, the tongue can fall back into the throat, or the jaw can drop, narrowing the airway.
- Soft Palate and Uvula: An elongated soft palate or uvula (the fleshy teardrop-shaped tissue hanging at the back of the throat) can vibrate intensely as air passes, creating snoring sounds.
- Large Tonsils or Adenoids: Enlarged tonsils or adenoids, particularly in children but also in adults, can obstruct the airway.
- Nasal Obstruction: Blocked nasal passages due to allergies, colds, deviated septum, or nasal polyps force you to breathe through your mouth, which can increase the likelihood of snoring.
- Narrow Throat: Some individuals naturally have a narrower throat due to their anatomy, which makes them more prone to airway collapse during sleep.
Lifestyle and Other Contributing Factors
- Obesity: Excess weight, particularly around the neck, can lead to increased soft tissue in the throat, narrowing the airway.
- Alcohol and Sedatives: Alcohol and certain medications (like tranquilizers or sleeping pills) relax throat muscles, making snoring more likely and often louder.
- Sleep Position: Sleeping on your back often causes the tongue and soft palate to fall back and obstruct the airway more easily due to gravity.
- Smoking: Smoking can irritate and inflame the lining of the throat and nasal passages, leading to swelling and reduced airflow.
- Age: As we age, throat muscles tend to lose tone, contributing to increased snoring.
- Congestion: Temporary conditions like a cold or allergies can cause nasal and throat swelling, leading to snoring.
The Connection to Sleep Apnea
It's critical to distinguish between primary snoring and snoring that is a symptom of obstructive sleep apnea (OSA). While both involve obstructed breathing, OSA is characterized by recurrent episodes of complete or partial airway collapse that lead to reduced blood oxygen levels and disrupted sleep. This is why addressing snoring and sleep apnea together is so important. A snoring mouth guard can be an effective treatment for both, but a proper diagnosis is key.
Signs and Symptoms: When Snoring Is More Than Just Noise
Recognizing the signs and symptoms associated with snoring is crucial, not just for your own health but for your sleep partner's well-being too. While a single night of snoring due to a cold might be harmless, chronic, loud snoring can indicate a more serious underlying issue.
Common Signs of Snoring
- Loud, Disruptive Snoring: The most obvious sign is the audible vibration of soft tissues in the throat during sleep, often described as rattling, snorting, or gasping sounds. This can be loud enough to disturb others in the household.
- Witnessed Breathing Pauses: If a sleep partner observes you repeatedly stopping breathing during sleep, followed by a gasp or choke, this is a significant red flag for obstructive sleep apnea.
- Daytime Fatigue and Drowsiness: Despite seemingly getting enough sleep, individuals who snore heavily or have OSA often wake up feeling unrefreshed and experience excessive daytime sleepiness.
- Morning Headaches: Persistent headaches upon waking can be a sign of oxygen deprivation during sleep.
- Dry Mouth or Sore Throat: Breathing through the mouth due to nasal obstruction or simply due to a wide-open mouth during snoring can lead to a dry mouth and a sore throat in the morning.
- Restless Sleep: Individuals may toss and turn frequently, searching for a position that allows for easier breathing.
- Frequent Nighttime Urination (Nocturia): Sleep apnea can increase the production of a hormone that causes the kidneys to produce more urine.
- Irritability and Difficulty Concentrating: Chronic sleep deprivation caused by snoring or sleep apnea can affect mood, memory, and cognitive function.
- High Blood Pressure: There is a strong correlation between chronic snoring (especially with sleep apnea) and an increased risk of hypertension.
Pro Tip: If you or your partner notice any of these symptoms, especially witnessed breathing pauses or severe daytime fatigue, it's imperative to consult a healthcare professional. A sleep study (polysomnography) may be recommended to accurately diagnose the severity of your snoring and rule out or confirm obstructive sleep apnea.
Treatment Options for Snoring
Addressing snoring involves a range of approaches, from simple lifestyle changes to more advanced medical interventions. The best mouth guard for snoring is just one piece of the puzzle, often used in conjunction with or as an alternative to other treatments.
1. Oral Appliance Therapy (Snoring Mouth Guards)
As discussed, MADs and TRDs are highly effective for primary snoring and mild to moderate OSA. They are a popular choice for their non-invasiveness and often high compliance rates compared to other medical devices.
- Pros: Non-invasive, portable, generally well-tolerated, high success rates for appropriate candidates.
- Cons: Requires professional fitting and follow-up for custom devices, potential for jaw discomfort or tooth movement, may not be effective for severe OSA.
2. Lifestyle Modifications
Many snoring cases can be improved with simple changes.
- Weight Loss: Losing even a small amount of weight can reduce fatty tissue around the throat, widening the airway.
- Avoid Alcohol and Sedatives: Especially in the hours before bed, as these relax throat muscles.
- Change Sleep Position: Sleeping on your side (lateral position) can prevent the tongue from falling back. Positional therapy devices (e.g., special pillows, backpack devices) can help.
- Quit Smoking: Smoking causes inflammation and irritation in the airways.
- Address Nasal Congestion: Use nasal strips, saline sprays, or decongestants (short-term) to clear nasal passages if snoring is due to a stuffy nose.
- Elevate Head: Sleeping with the head slightly elevated can sometimes reduce snoring.
3. Continuous Positive Airway Pressure (CPAP) Therapy
CPAP is the gold standard treatment for moderate to severe obstructive sleep apnea.
- Pros: Highly effective in keeping the airway open, significantly reduces OSA symptoms and associated health risks.
- Cons: Can be uncomfortable (mask, noise, air pressure), requires consistent use, challenges with portability and maintenance. Many patients find it difficult to tolerate long-term.
4. Surgical Options
Various surgical procedures can address anatomical issues contributing to snoring and OSA.
- Uvulopalatopharyngoplasty (UPPP): Removes excess tissue from the soft palate and uvula.
- Laser-Assisted Uvulopalatoplasty (LAUP): A less invasive procedure using a laser to shorten the uvula and trim the soft palate.
- Genioglossus Advancement: Moves the tongue muscle forward.
- Maxillomandibular Advancement (MMA): A more extensive surgery that moves both the upper and lower jaws forward.
- Pillar Procedure: Implants small polyester rods into the soft palate to stiffen it.
- Pros: Can be curative for some individuals, especially with specific anatomical obstructions.
- Cons: Invasive, involves recovery time, potential risks (pain, bleeding, infection, voice changes), not always 100% effective, especially for OSA.
5. Other Devices and Therapies
- Nasal Dilators/Strips: Widen nasal passages, useful for snoring caused by nasal congestion.
- Expiratory Positive Airway Pressure (EPAP) Devices: Small, disposable devices placed over the nostrils that create back pressure to keep the airway open.
- Positional Therapy: Devices or techniques to encourage side sleeping.

| Treatment Option | Primary Use | Effectiveness for Snoring | Pros | Cons |
|---|---|---|---|---|
| Oral Appliance (MAD/TRD) | Primary Snoring, Mild-Moderate OSA | High | Non-invasive, portable, often well-tolerated | Requires professional fitting, potential jaw discomfort, cost for custom models |
| Lifestyle Changes | Mild Snoring, General Health | Variable | No cost, holistic health benefits | Requires discipline, may not be sufficient for moderate/severe cases |
| CPAP Therapy | Moderate-Severe OSA | Very High | Gold standard for OSA, highly effective for airway patency | Can be uncomfortable, mask irritation, noise, travel inconvenience, low long-term compliance for some |
| Surgical Procedures | Specific Anatomical Obstructions | Variable | Can be curative, permanent solution for some | Invasive, recovery time, risks (pain, infection, scarring), not always effective |
| Nasal Strips/Dilators | Nasal Congestion-Related Snoring | Moderate | Inexpensive, non-invasive, immediate relief | Only addresses nasal issues, not effective for throat-based snoring |
Pro Tip: For effective treatment of snoring and sleep apnea, a thorough evaluation by a dentist or physician specializing in sleep medicine is essential. They can help you navigate these options and determine the most appropriate course of action, often starting with a snoring mouth piece.
Step-by-Step Process for Getting a Custom Snoring Mouth Guard
Obtaining a custom-fitted oral appliance for snoring or sleep apnea is a structured process involving several steps to ensure the device is effective, comfortable, and safe.
1. Initial Consultation and Evaluation
- Dental Exam: Your dentist will conduct a comprehensive oral examination to assess your dental health, jaw structure, bite, and look for any signs of temporomandibular joint (TMJ) dysfunction.
- Medical History Review: Discussion of your general health, sleep habits, snoring history, and any symptoms of sleep apnea (e.g., daytime sleepiness, witnessed breathing pauses).
- Referral for Sleep Study (if needed): If your dentist suspects obstructive sleep apnea, they will likely refer you to a sleep physician for a sleep study (polysomnography). This diagnostic test is crucial to determine if you have OSA, and if so, its severity. A formal diagnosis of OSA is often required for insurance coverage of a custom oral appliance.
- Discussion of Options: Your dentist will discuss whether a MAD or TRD is suitable for your case, explaining the pros and cons.
2. Impressions and Measurements
- Dental Impressions or Digital Scans: Accurate impressions of your upper and lower teeth are taken using traditional dental putty or a digital intraoral scanner. These impressions serve as a blueprint for fabricating your custom appliance.
- Bite Registration: Specific measurements are taken to determine the ideal advanced position of your lower jaw. This is a critical step, as it dictates how much the jaw will be moved forward to open the airway. Your dentist will often guide your jaw into a comfortable forward position.
3. Appliance Fabrication
- Lab Work: The impressions and measurements are sent to a specialized dental laboratory. Skilled technicians use these to custom-fabricate your oral appliance, ensuring it fits precisely and comfortably. This process typically takes 1-3 weeks.
4. Fitting Appointment
- Initial Fitting: Once the appliance is ready, you'll return for a fitting appointment. Your dentist will ensure the appliance fits snugly over your teeth without causing undue pressure or discomfort.
- Instruction and Demonstration: You will receive detailed instructions on how to insert and remove the appliance, how to clean it, and what to expect during the initial adjustment period.
5. Adjustment and Follow-up
- Gradual Adjustment: It's common for your dentist to recommend a gradual advancement of the jaw over several nights or weeks, especially with adjustable MADs. This allows your jaw and muscles to adapt, minimizing discomfort while optimizing effectiveness.
- Follow-up Appointments: Several follow-up appointments are scheduled over the first few weeks or months. During these visits, your dentist will check the fit, comfort, and effectiveness of the appliance. They will make any necessary adjustments to the device or the degree of jaw advancement.
- Monitoring Effectiveness: You might be asked to monitor your snoring (e.g., with a snoring app) or report changes in daytime sleepiness. In some cases, a follow-up sleep study with the appliance in place might be recommended to objectively verify its effectiveness in treating OSA.
- Ongoing Dental Care: Regular dental check-ups (typically every 6-12 months) are essential to monitor your oral health, check the appliance's condition, and ensure its continued effectiveness and comfort.

Cost and Insurance for Snoring Mouth Guards
Understanding the financial aspect of obtaining a snoring mouth guard is crucial. Costs vary significantly based on the type of device and whether it's custom-fitted. Insurance coverage can also be complex.
Cost Breakdown
Over-the-Counter (OTC) Snoring Mouth Guards (Boil-and-Bite MADs or Basic TRDs)
- Price Range: $20 - $150
- What it includes: The device itself.
- Considerations: These are the most affordable but come with limitations in fit, comfort, adjustability, and long-term durability. They generally offer a less precise and less effective solution compared to custom devices.
Custom-Fitted Snoring Mouth Guards (Dentist-Prescribed MADs or TRDs)
- Price Range: $800 - $3,000+
- What it includes:
- Initial consultation and examination.
- Diagnostic procedures (e.g., impressions, bite registration).
- The custom-fabricated device.
- Fitting appointments.
- Follow-up adjustments and monitoring.
- Some higher-end, advanced appliances for severe cases can reach $3,500 - $4,000.
- Factors influencing cost: Geographic location (costs tend to be higher in major metropolitan areas), the specific materials used, the complexity of the design, and the dentist's fees and experience.
Insurance Coverage
This is where it gets a bit tricky, but generally, custom oral appliances for snoring and sleep apnea often fall under medical insurance, not dental insurance.
-
Medical Insurance:
- Diagnosis is Key: For medical insurance to cover a custom oral appliance, you almost always need a formal diagnosis of obstructive sleep apnea (OSA), confirmed by a sleep study (polysomnography). Snoring alone (without OSA) is rarely covered by medical insurance.
- Durable Medical Equipment (DME): Oral appliances for OSA are typically classified as Durable Medical Equipment (DME). Coverage often falls under your DME benefits, similar to CPAP machines.
- Pre-authorization: Most insurance companies require pre-authorization before you begin treatment. Your dental office, if they specialize in sleep dentistry, will usually assist with this.
- Deductibles and Co-pays: You will still be responsible for your annual deductible, co-insurance, and co-pays, as dictated by your specific plan.
- In-Network vs. Out-of-Network: Check if your dentist is in-network with your medical insurance plan to minimize out-of-pocket costs.
- CPT Codes: Common CPT (Current Procedural Terminology) codes for oral appliances used to treat sleep apnea include E0486 (Oral device/appliance used to reduce upper airway collapsibility, adjustable or non-adjustable, custom fabricated, includes fitting and adjustment).
-
Dental Insurance:
- Dental insurance typically covers procedures related to general dental health, like cleanings, fillings, and crowns. It generally does not cover oral appliances for snoring or sleep apnea, as these are considered medical treatments.
- However, your dental benefits may cover the initial dental exam or X-rays related to the appliance fabrication, so it's worth checking.
Payment Plans and Financing Options
If insurance coverage is limited or unavailable, several options can help manage the cost:
- In-Office Payment Plans: Many dental practices offer in-house payment plans, allowing you to pay for the appliance in installments.
- Third-Party Financing: Services like CareCredit or LendingClub offer specialized healthcare financing with various interest rates and payment terms, including interest-free options for a limited period.
- Flexible Spending Accounts (FSAs) and Health Savings Accounts (HSAs): Funds from FSAs and HSAs can be used to pay for medical expenses, including custom oral appliances, often with pre-tax dollars, providing a significant saving.
Pro Tip: Always call your medical insurance provider directly to verify your benefits for "Durable Medical Equipment for Obstructive Sleep Apnea (OSA)" before starting treatment. Ask specific questions about coverage for oral appliances, deductibles, co-insurance, and if pre-authorization is required.
Recovery and Aftercare for Your Snoring Mouth Guard
Once you receive your custom snoring mouth guard, proper care and attention are essential for its longevity, your oral health, and the continued effectiveness of your treatment.
Initial Adjustment Period
It's normal to experience an adjustment period when you first start using a snoring mouth piece.
- Jaw Discomfort/Soreness: Your jaw muscles and joints may feel sore or stiff, especially in the mornings. This usually subsides within a few days to a couple of weeks as your body adapts to the new jaw position.
- Increased Salivation: Some people experience an increase in saliva production initially, which typically resolves as your mouth gets used to the device.
- Dry Mouth: Conversely, some might experience temporary dry mouth due to changes in airflow.
- Temporary Bite Changes: Your bite might feel "off" for a few minutes after removing the appliance in the morning. This is normal and usually self-corrects within 15-30 minutes. Chewing sugar-free gum briefly can help realign your bite.
- Gag Reflex: A temporary gag reflex can occur, particularly with TRDs, but often diminishes with consistent use.
Pro Tip: If discomfort is persistent or severe, contact your dentist. They can make minor adjustments to the appliance to improve comfort and fit. Never try to adjust the device yourself.
Daily Care and Maintenance
Proper cleaning and storage are vital for hygiene and device lifespan.
- Daily Cleaning:
- Brush Gently: After each use, gently brush your mouth guard with a soft-bristled toothbrush and mild, non-abrasive soap (like liquid hand soap or dish soap) or a specialized oral appliance cleaner. Avoid toothpaste, as it can be abrasive and scratch the surface, creating nooks for bacteria.
- Rinse Thoroughly: Rinse the appliance thoroughly under cool or lukewarm water.
- Air Dry: Allow the appliance to air dry completely before storing it, or pat it dry with a clean cloth.
- Weekly Cleaning (Optional): Some dentists recommend soaking the appliance once a week in a denture or oral appliance cleaning solution for 15-30 minutes, or as directed by the product. Always rinse thoroughly afterward.
- Storage: Always store your mouth guard in its protective case when not in use. This prevents damage, keeps it clean, and protects it from pets or accidental loss. Keep it away from high heat, which can warp the material.
- Avoid Harsh Chemicals: Do not use bleach, hot water, or harsh abrasive cleaners, as these can damage the material and compromise the fit.
Regular Dental Check-ups
- Follow-Up Schedule: Continue with the follow-up appointments recommended by your dentist, especially in the initial months, to ensure optimal fit and effectiveness.
- Annual Checks: Even after the initial adjustment period, plan for annual check-ups with your sleep dentist to inspect the appliance for wear and tear, check your oral health, and monitor the effectiveness of the treatment. Your bite will also be checked to ensure no long-term changes are occurring.
- Appliance Replacement: Oral appliances typically last 2-5 years, depending on the material, care, and individual wear patterns. Your dentist will advise you when a replacement might be necessary.
Prevention: Reducing Your Risk of Snoring
While a snoring mouth piece can be a highly effective treatment, adopting preventative measures can significantly reduce the likelihood and severity of snoring, and contribute to overall better health.
- Maintain a Healthy Weight: Losing excess weight, especially around the neck, can reduce the amount of soft tissue that contributes to airway obstruction. Even a modest weight loss can make a noticeable difference.
- Avoid Alcohol and Sedatives Before Bed: Alcohol and certain medications relax the muscles in your throat, increasing the chance of snoring. Try to avoid them at least 3-4 hours before sleep.
- Change Your Sleep Position: Sleeping on your back allows gravity to pull your tongue and soft palate backward, narrowing the airway. Sleeping on your side is often recommended. You can use a body pillow or even sew a tennis ball into the back of a pajama top to prevent rolling onto your back.
- Practice Good Sleep Hygiene:
- Maintain a consistent sleep schedule.
- Create a dark, quiet, and cool bedroom environment.
- Avoid large meals close to bedtime.
- Keep Nasal Passages Clear:
- If you suffer from allergies, manage them with antihistamines or nasal sprays.
- Use nasal strips or a saline rinse before bed if congestion is a chronic issue.
- Address structural nasal problems (e.g., deviated septum) with a doctor.
- Quit Smoking: Smoking irritates the throat and nasal passages, leading to inflammation and swelling that can exacerbate snoring.
- Elevate Your Head: Using an extra pillow or elevating the head of your bed by a few inches can help open the airway.
- Stay Hydrated: Dehydration can cause the secretions in your nose and soft palate to become stickier, potentially leading to more snoring. Drink plenty of water throughout the day.
Risks and Complications of Snoring Mouth Guards
While oral appliances are generally safe and well-tolerated, it's important to be aware of potential risks and complications, especially with long-term use.
- Jaw Discomfort or Pain (TMJ Issues): This is the most common side effect. Advancing the jaw can put stress on the temporomandibular joints (TMJ) and surrounding muscles. While often temporary, persistent pain or new TMJ symptoms should be reported to your dentist immediately.
- Tooth Sensitivity or Movement: Minor tooth sensitivity can occur, particularly when first using the device. Over very long periods (years), there's a small risk of slight changes in tooth position or bite alignment, especially with poorly fitted or improperly adjusted devices. Regular monitoring by a dentist helps mitigate this.
- Excessive Salivation or Dry Mouth: Some individuals experience an initial increase in saliva production (hypersalivation), while others might notice dry mouth symptoms. Both usually resolve with continued use.
- Gum or Tooth Soreness: Pressure points from a poorly fitted device can cause localized soreness. Custom devices are designed to minimize this.
- Gag Reflex: Particularly with TRDs or some MADs, a temporary gag reflex can be an issue until the patient adapts.
- Device Breakage or Wear: Although custom devices are durable, they can wear down over time, or in rare cases, break, especially if you clench or grind your teeth (bruxism).
- Delayed Diagnosis of Obstructive Sleep Apnea (OSA): A major risk of self-treating snoring with OTC devices without a professional diagnosis is the potential to mask undiagnosed OSA. If snoring improves but OSA persists untreated, serious health consequences (e.g., cardiovascular issues, stroke) can worsen. This underscores the importance of a proper medical evaluation.
- Ineffectiveness: The appliance may not be effective for all individuals, particularly those with severe OSA, where CPAP therapy is often the more appropriate first-line treatment.
Pro Tip: Regular follow-up with your prescribing dentist is crucial to monitor for any side effects and make adjustments as needed. Report any persistent discomfort or changes in your bite or jaw immediately.
Children / Pediatric Considerations for Snoring
Snoring in children is a common concern for parents and warrants careful attention. While occasional snoring during a cold is usually harmless, chronic snoring in children can be a sign of underlying issues, potentially impacting their health and development.
Causes of Snoring in Children
- Enlarged Tonsils and Adenoids: This is the most common cause of chronic snoring and sleep-disordered breathing in children.
- Obesity: Similar to adults, excess weight can contribute to narrowed airways.
- Allergies and Nasal Congestion: Chronic allergies can lead to swollen nasal passages and mouth breathing.
- Craniofacial Anomalies: Certain genetic conditions or structural abnormalities of the jaw or airway can predispose children to snoring.

When to Be Concerned
Not all childhood snoring indicates a problem, but certain signs suggest a need for medical evaluation:
- Chronic Snoring (3+ nights/week): If snoring is loud, consistent, and happens most nights.
- Witnessed Breathing Pauses: If you observe your child stopping breathing, gasping, or choking during sleep.
- Daytime Symptoms: Poor concentration, hyperactivity (often misdiagnosed as ADHD), irritability, difficulty waking up, morning headaches, or persistent daytime sleepiness.
- Developmental Delays: Untreated sleep apnea can impact growth and development.
- Bedwetting (Nocturnal Enuresis): May be associated with sleep apnea in children.
Treatment and Oral Appliances in Children
- First-Line Treatment: For children, the first line of treatment for sleep-disordered breathing, particularly if enlarged tonsils and adenoids are present, is often surgical removal of the tonsils and adenoids (adenotonsillectomy). This often resolves the issue.
- Orthodontic Expansion: In some cases, if the issue is a narrow upper jaw or palate, a pediatric dentist or orthodontist may recommend palatal expansion to widen the upper arch and improve nasal breathing.
- Oral Appliances (Mouth Guards): Oral appliances, like MADs or TRDs, are generally not the primary treatment for snoring or sleep apnea in children.
- Limited Use: Their use is typically reserved for older adolescents whose facial growth is largely complete, or in specific cases where other treatments are not suitable or have been unsuccessful.
- Growth Considerations: Because a child's jaw and teeth are still developing, using a device that alters jaw position can interfere with growth and orthodontic development.
- Specialized Expertise: If an oral appliance is considered, it must be prescribed and monitored by a dentist or orthodontist with specialized training in pediatric sleep medicine and appliance therapy, working closely with the child's pediatrician and ENT specialist.
Pro Tip: If your child snores regularly, especially with any of the concerning symptoms mentioned, consult your pediatrician immediately. They can refer you to a pediatric sleep specialist, ENT (Ear, Nose, and Throat) doctor, or a pediatric dentist for a thorough evaluation.
Cost Breakdown: Custom Snoring Mouth Guards in the US
A clear understanding of the financial commitment for a custom-fitted snoring mouth guard (oral appliance) is vital. As previously mentioned, these devices are significantly different from their over-the-counter counterparts in terms of cost, efficacy, and professional oversight.
Average US Costs
The cost of a custom-fitted oral appliance for snoring and/or sleep apnea can vary widely across the United States.
- Low End: In some rural areas or less expensive practices, costs might start around $800 - $1,200.
- Mid-Range: Most practices, especially in suburban areas, will typically charge between $1,500 - $2,500.
- High End: In major metropolitan areas, specialized sleep dentistry clinics, or for more complex appliance designs, the cost can reach $2,800 - $3,500, with some reaching up to $4,000.
These costs generally cover:
- Initial consultation and diagnostic exams.
- Impressions or digital scans.
- The fabrication of the custom appliance.
- Fitting appointments.
- Follow-up adjustments for a specified period (e.g., 6 months to 1 year).
With vs. Without Insurance
- Without Insurance (Self-Pay): If you don't have medical insurance that covers oral appliances for OSA, or if you are seeking a device solely for primary snoring (which is usually not covered), you will be responsible for the full amount. In these cases, it's always worth discussing potential cash discounts or payment plans with the dental office.
- With Insurance (Medical Insurance for OSA):
- Diagnosis of OSA is Crucial: As noted, coverage nearly always hinges on a formal diagnosis of Obstructive Sleep Apnea from a sleep study.
- Deductibles: You will first need to meet your medical insurance deductible. For many plans, this can range from $500 to $5,000+ per year.
- Co-insurance/Co-pays: After your deductible is met, you will typically pay a percentage of the remaining cost (co-insurance, e.g., 10-30%) or a fixed co-pay per visit/service.
- Example: If an appliance costs $2,000 and you have a $1,000 deductible with 20% co-insurance, and you haven't met your deductible yet:
- You pay the first $1,000 (deductible).
- Of the remaining $1,000, insurance pays 80% ($800), and you pay 20% ($200).
- Your total out-of-pocket cost would be $1,000 (deductible) + $200 (co-insurance) = $1,200.
- Prior Authorization: Your dental office will submit a request for prior authorization to your medical insurance. This step is essential and can take several weeks.
Payment Plans and Financing Options
To make custom oral appliances more accessible, most dental practices offer solutions:
- In-Office Payment Plans: Many clinics allow patients to pay in monthly installments, often interest-free for shorter periods.
- Third-Party Medical Financing: Companies like CareCredit or Alphaeon Credit offer specialized financing for healthcare expenses. They often have deferred interest plans for 6, 12, or 18 months, or longer-term plans with fixed interest rates.
- Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs): These tax-advantaged accounts allow you to save and pay for qualified medical expenses, including oral appliances, using pre-tax dollars. This can effectively reduce your out-of-pocket cost by your income tax rate.
Pro Tip: Don't let the upfront cost deter you. Discuss all financial options with your dentist's administrative staff. They are usually well-versed in navigating insurance complexities and can help you find an affordable solution.
Frequently Asked Questions
What is the difference between a snoring mouth guard and a night guard for teeth grinding?
While both are worn in the mouth at night, their purposes differ. A snoring mouth guard (MAD or TRD) is designed to reposition the jaw or tongue to open the airway and reduce snoring. A night guard for teeth grinding (bruxism) is designed to protect teeth from clenching and grinding, preventing dental wear and jaw pain, without necessarily affecting the airway.
How long does it take to get used to wearing a snoring mouth guard?
Most people adjust to wearing a snoring mouth guard within a few days to a couple of weeks. Initial side effects like jaw soreness, tooth sensitivity, or increased salivation are common but typically subside as your mouth and jaw adapt. Consistent use helps speed up the adjustment period.
Can a snoring mouth guard cure sleep apnea?
A snoring mouth guard can effectively treat mild to moderate obstructive sleep apnea (OSA) by keeping the airway open, but it is not a "cure" in the sense of permanently eliminating the condition. It manages the symptoms while worn. For severe OSA, CPAP therapy or surgery may be more appropriate.
Are over-the-counter snoring mouth guards effective?
Over-the-counter (OTC) boil-and-bite snoring mouth guards can offer some relief for very mild, occasional snoring. However, they are generally less effective, less comfortable, and less durable than custom-fitted devices. They also lack the precise adjustability and professional oversight crucial for optimal treatment and to prevent potential side effects.
How do I clean my snoring mouth guard?
You should clean your snoring mouth guard daily by gently brushing it with a soft-bristled toothbrush and a mild, non-abrasive soap (avoid toothpaste). Rinse it thoroughly with cool water and let it air dry before storing it in its protective case. Specialized oral appliance cleaning solutions can be used for deeper cleaning, following product instructions.
What if I have dentures or missing teeth? Can I still use a snoring mouth guard?
If you have full dentures, a Mandibular Advancement Device (MAD) might not be suitable as it needs stable teeth to anchor to. However, a Tongue Retaining Device (TRD) which holds the tongue forward using suction, can often be used effectively with dentures or missing teeth. Consult a sleep dentist to discuss your specific situation.
Will a snoring mouth guard affect my bite or cause jaw pain long-term?
Custom-fitted snoring mouth guards, especially MADs, can sometimes cause temporary changes in bite or jaw discomfort. Your dentist will monitor your bite and TMJ health during follow-up visits. While minor, reversible changes are possible, significant long-term adverse effects are rare with professional oversight and proper adjustment.
How often do I need to replace my custom snoring mouth guard?
A custom-fitted snoring mouth guard typically lasts between 2 to 5 years, depending on the material, how well it's maintained, and whether you clench or grind your teeth. Your dentist will assess its condition during your regular check-ups and advise when a replacement is needed.
Can I use a snoring mouth guard if I wear braces or other orthodontic appliances?
Generally, MADs are not recommended with traditional braces because they can interfere with orthodontic treatment and proper fit. If you are undergoing orthodontic treatment, discuss your snoring concerns with both your orthodontist and a sleep dentist. Clear aligners might allow for certain types of oral appliances, but it requires careful coordination.
Is a snoring mouth guard covered by insurance?
Custom-fitted oral appliances for snoring are often covered by medical insurance (not dental insurance) if you have a diagnosed case of obstructive sleep apnea (OSA) and if your plan includes Durable Medical Equipment (DME) benefits. It requires prior authorization and you will be responsible for deductibles and co-insurance. Purely for primary snoring, it's rarely covered.
When to See a Dentist
While occasional snoring might be harmless, certain signs indicate that it's time to consult a dental professional or a sleep specialist. Ignoring persistent or severe snoring can lead to significant health consequences and disrupt your quality of life.
You should schedule an appointment with a dentist specializing in sleep medicine if you experience any of the following:
- Loud, Chronic Snoring: If your snoring is a nightly occurrence, consistently loud, and disruptive to your sleep or that of your partner.
- Witnessed Breathing Pauses: If your sleep partner observes you repeatedly stopping breathing, gasping, or choking during sleep. This is a primary red flag for obstructive sleep apnea.
- Excessive Daytime Sleepiness: Despite getting adequate hours of sleep, if you consistently feel tired, drowsy, or fall asleep unintentionally during the day (e.g., while driving or watching TV).
- Morning Headaches: Persistent headaches upon waking that are not otherwise explained.
- Difficulty Concentrating or Irritability: If you notice a decline in your cognitive function, memory, or mood due to poor sleep.
- High Blood Pressure: Snoring, particularly when associated with sleep apnea, is a significant risk factor for hypertension. If you have been diagnosed with high blood pressure, discuss your snoring with your doctor and dentist.
- Dry Mouth or Sore Throat in the Morning: Consistent symptoms that could indicate mouth breathing and airway issues during sleep.
- If You Have Been Diagnosed with Sleep Apnea but Cannot Tolerate CPAP: A snoring mouth piece can be an excellent alternative for those who find CPAP difficult to use consistently.
Red Flags vs. Routine Care Guidance:
- Red Flags (See a Dentist/Sleep Doctor Promptly): Witnessed breathing pauses, severe daytime sleepiness, and chronic, loud snoring accompanied by any of the above symptoms. These warrant a comprehensive evaluation and potentially a sleep study to rule out or diagnose obstructive sleep apnea.
- Routine Care Guidance: If your snoring is mild, intermittent, and not accompanied by other concerning symptoms, you might start with lifestyle modifications. However, if those don't help, or if you simply want to explore options for quieter nights, a consultation with a dentist trained in sleep dentistry is a proactive and beneficial step.
Don't underestimate the impact of snoring on your health and well-being. A proper diagnosis and the right snoring mouth piece can lead to profoundly better sleep quality for you and your entire household.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
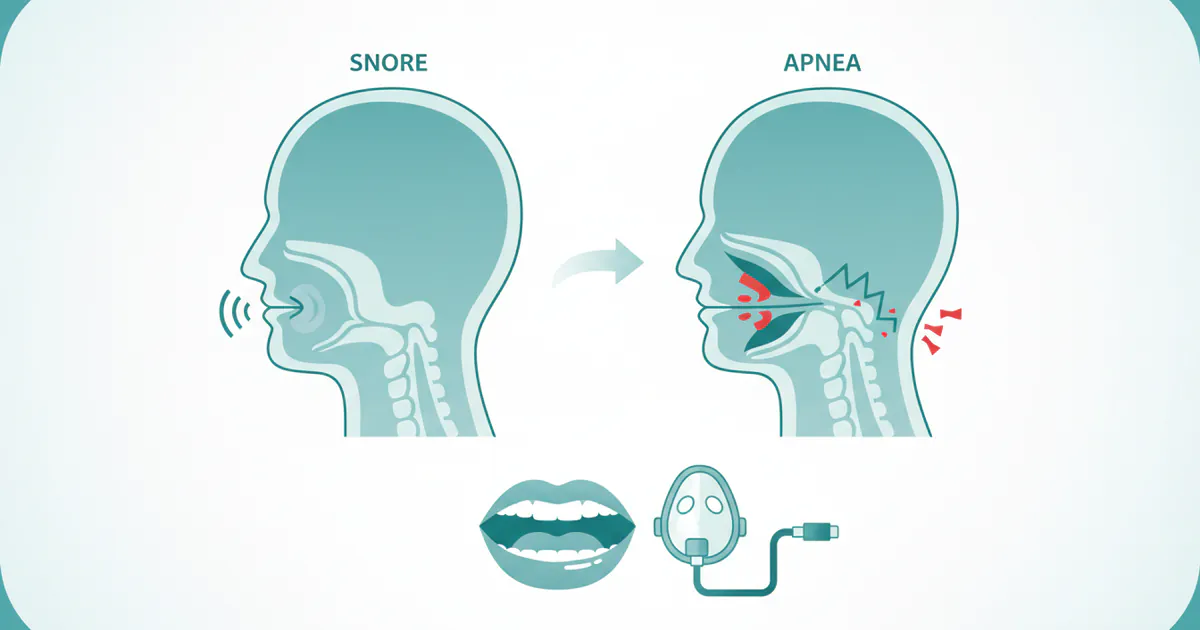
Difference Between Snoring and Sleep Apnea: Complete Guide
More than 80 million Americans regularly snore, and while often dismissed as a mere nuisance, loud and persistent snoring can be a critical indicator of a much more serious underlying health condition: sleep apnea. The difference between snoring and sleep apnea is profound, impacting not just yo
February 23, 2026

Mouth Taping for Snoring: Complete Guide
Snoring. It's the nocturnal soundtrack for millions of Americans, often a source of frustration for bed partners and a potential indicator of underlying health issues for the snorer themselves. Roughly 45% of adults snore occasionally, and 25% are habitual snorers, impacting sleep quality, relat
February 23, 2026
Is All Snoring Sleep Apnea
Many individuals, perhaps even you or a loved one, have been told they snore loudly. It's often dismissed as a harmless, albeit annoying, nocturnal habit. However, what if that nightly rumble is more than just noise? What if it's a critical indicator of an underlying health condition that significan
February 23, 2026
Cpap Dry Mouth Even With Humidifier: Complete Guide
Experiencing dry mouth while using a CPAP machine, even with a humidifier, is a common and incredibly frustrating issue for millions of Americans. It can disrupt sleep, diminish the effectiveness of your sleep apnea treatment, and significantly impact your oral health. Imagine waking up every mornin
February 23, 2026