Full Mouth Implants: Complete Guide
Key Takeaways
- Imagine regaining the ability to eat your favorite foods, speak with complete confidence, and smile freely without a second thought. For millions of Americans suffering from extensive tooth loss or failing dentition, this isn't just a dream – it's a reality made possible by full mouth implants.
Full Mouth Implants: Complete Guide
Imagine regaining the ability to eat your favorite foods, speak with complete confidence, and smile freely without a second thought. For millions of Americans suffering from extensive tooth loss or failing dentition, this isn't just a dream – it's a reality made possible by full mouth implants. Over 36 million adults in the US are missing all their teeth in one or both arches, and many more struggle with severely damaged or decayed teeth. While traditional dentures offer a solution, they often come with limitations like discomfort, movement, and the need for adhesives. Full mouth implants provide a permanent, stable, and natural-feeling alternative that can dramatically improve quality of life, oral health, and overall well-being.

This comprehensive guide from SmilePedia.net will delve into every aspect of full mouth implants, from understanding what they are and the various types available, to the detailed treatment process, associated costs, and what to expect during recovery. We'll explore why this transformative dental procedure might be the right choice for you, address common concerns, and equip you with the knowledge to make informed decisions about your dental future. Prepare to discover how modern dentistry can restore not just your smile, but your confidence and quality of life.
Key Takeaways:
- What they are: Full mouth implants are a permanent solution for replacing all teeth in an upper or lower jaw (or both) using surgically placed dental implants to support a fixed prosthetic arch.
- Cost (approximate US ranges): Expect to pay $20,000 to $50,000 per arch for full mouth implants (e.g., All-on-4), with conventional full arch implant bridges potentially reaching $60,000 to $90,000+ per arch. A single tooth implant costs between $3,000 and $6,000.
- Procedure Timeframe: The entire process, from initial consultation to final restoration, can take 3 to 12 months, depending on bone health, need for grafting, and the chosen implant system.
- Key Benefits: Enhanced chewing efficiency, improved speech, restored facial aesthetics, preserved jawbone, and a permanent solution that feels like natural teeth.
- Success Rate: Dental implants boast a high success rate, typically 95-98% over 10 years when performed by experienced professionals and maintained properly.
- Recovery: Initial recovery from surgery usually takes 1-2 weeks, with minor discomfort manageable with medication. Full integration (osseointegration) takes 3-6 months.
- Maintenance: Requires diligent oral hygiene, including brushing, flossing, and regular dental check-ups, similar to natural teeth.
What Are Full Mouth Implants? An Overview
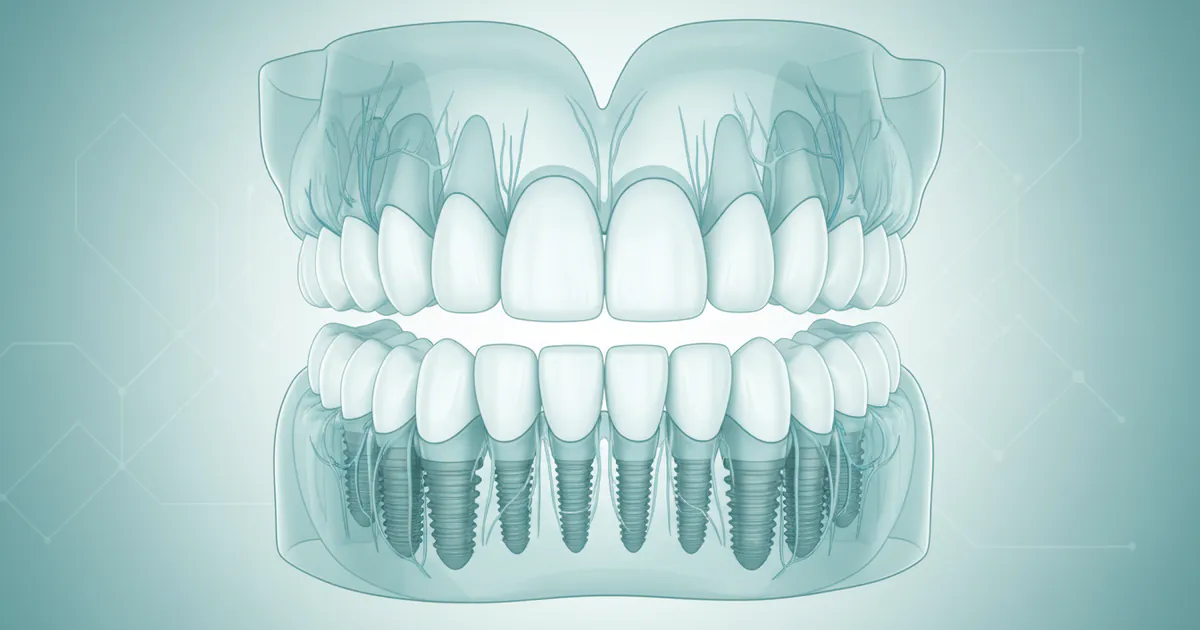
Full mouth implants represent the pinnacle of modern dental restoration, offering a robust and long-lasting solution for individuals who have lost most or all of their teeth in an upper arch, lower arch, or both. Unlike removable dentures that rest on the gums, full mouth implants consist of several dental implant posts surgically placed into the jawbone. These titanium or zirconia posts act as artificial tooth roots, providing an incredibly stable foundation for a custom-fabricated, fixed dental prosthesis – typically a full arch bridge or denture that is permanently screwed or cemented into place.
The underlying principle is osseointegration, a biological process where the implant material (usually titanium) fuses directly with the surrounding bone tissue over several months. This creates a bond that is remarkably strong and durable, allowing the implants to withstand the powerful forces of biting and chewing, just like natural tooth roots. Once osseointegration is complete, the implants can reliably support a full set of replacement teeth, offering superior stability, comfort, and function compared to traditional removable dentures.
This treatment is a significant investment in both oral health and overall quality of life. Patients often report a dramatic improvement in their ability to eat a wide variety of foods, speak clearly, and smile confidently. Beyond aesthetics and function, full mouth implants also play a crucial role in preserving jawbone health. When teeth are lost, the jawbone naturally begins to resorb or shrink due to lack of stimulation. Implants transmit chewing forces to the bone, stimulating it and helping to prevent this bone loss, thereby maintaining facial structure and preventing a "collapsed" appearance often associated with long-term denture wear.
Types and Variations of Full Mouth Implant Solutions
The world of full mouth implants offers several sophisticated approaches, each tailored to different patient needs, bone densities, and budget considerations. The primary goal remains the same: to provide a stable, functional, and aesthetically pleasing full arch of teeth.
All-on-4® and All-on-X Systems
The All-on-4® concept, pioneered by Nobel Biocare, is one of the most popular and efficient methods for full mouth restoration. It involves strategically placing four dental implants in the jawbone to support an entire arch of prosthetic teeth. Two implants are placed vertically in the anterior (front) jaw, and two are angled up to 45 degrees in the posterior (back) jaw. This angulation allows for maximum contact with existing bone, often eliminating the need for bone grafting, even in cases of moderate bone loss.
- All-on-4: Uses four implants per arch. Often allows for immediate loading, meaning a temporary set of teeth can be attached on the day of surgery.
- All-on-6 / All-on-8 (All-on-X): Similar to All-on-4 but uses six or eight implants per arch. This provides even greater stability and strength, particularly beneficial for patients with strong bites, extensive bone loss requiring more support, or when greater prosthetic design flexibility is desired. While it might involve more implants, the principle remains the same.
Pros: Often immediate load capability (new teeth in one day), less invasive than traditional full arch implants, typically avoids bone grafting, fixed and stable. Cons: Requires precise surgical planning, more limited adjustability once placed compared to individual implants, higher cost than traditional dentures.
Traditional Full Arch Implant-Supported Bridges
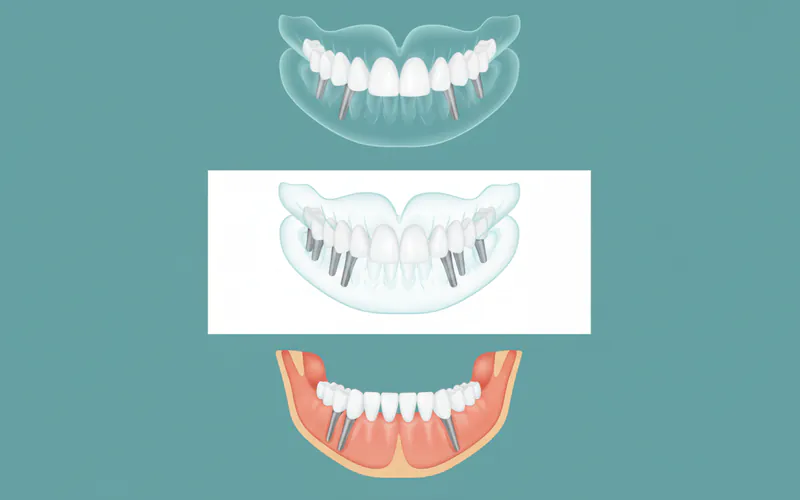
In this approach, a greater number of individual dental implants (typically 6 to 10 or more per arch) are placed throughout the jawbone. Each implant may eventually support an individual crown, or more commonly, several implants are strategically positioned to support a custom-designed, fixed bridge that replaces all teeth in the arch.
- Process: Often involves a longer healing period for osseointegration before the final bridge is attached. Temporary restorations are typically worn during this time.
- Bone Grafting: More likely to require bone grafting if significant bone loss is present, as implants need to be placed more uniformly across the arch.
Pros: Maximum stability and load distribution, potentially more adaptable to complex cases, mimics natural dentition most closely. Cons: Can be more invasive due to more implants, often requires bone grafting, longer overall treatment timeline, typically the most expensive option.
Zygomatic Implants (Specialized Cases)
For patients with severe bone loss in the upper jaw, where traditional implants or even All-on-4 are not feasible, zygomatic implants offer a specialized solution. These longer implants are anchored into the zygomatic bone (cheekbone) instead of the maxillary (upper jaw) bone.
- Purpose: Primarily for upper jaw reconstruction when there is insufficient bone for conventional implants.
- Procedure: A complex surgical procedure requiring highly skilled oral and maxillofacial surgeons.
Pros: Provides a fixed solution even in extreme bone loss scenarios, often avoids extensive bone grafting. Cons: More invasive surgery, higher risk profile, specialized expertise required, often higher cost.
Materials for Full Arch Prosthetics
Once the implants are integrated, the final prosthetic teeth need to be fabricated. Common materials include:
- Acrylic with Titanium Frame: Often used for temporary or immediate load prostheses, and can also be used for final restorations. It's lighter and more shock-absorbent than zirconia.
- Zirconia: A highly durable, biocompatible ceramic material known for its strength and aesthetic appeal. Zirconia bridges are monolithic (one piece), highly resistant to chipping and staining, and mimic the translucency of natural teeth very well.
- Porcelain Fused to Metal (PFM): Offers a good balance of strength and aesthetics, though less common for full arches than zirconia or acrylic over titanium today.
Why Consider Full Mouth Implants? (Indications and Benefits)
While not a "cause" in the traditional sense, the necessity for full mouth implants arises from significant oral health deterioration that impacts function, aesthetics, and overall well-being. Understanding these indications and the profound benefits of choosing implants can help you determine if this treatment is right for you.
Indications for Full Mouth Implants:
- Extensive Tooth Loss (Edentulism): You are missing most or all of your teeth in an upper, lower, or both jaws.
- Failing Dentition: You have numerous teeth that are severely decayed, fractured, loose due to advanced periodontal disease, or otherwise beyond repair and require extraction.
- Dissatisfaction with Traditional Dentures: You find your removable dentures uncomfortable, unstable, prone to slipping, or interfering with speech and eating.
- Bone Loss: While many implant systems are designed to minimize the need for bone grafting, implants can help prevent further bone resorption caused by missing teeth.
- Chronic Dental Problems: You experience ongoing issues with pain, infection, or difficulty chewing due to widespread dental problems.
Profound Benefits of Full Mouth Implants:
- Restored Chewing Efficiency: Full mouth implants are anchored securely in your jawbone, providing biting forces comparable to natural teeth. This means you can enjoy a full range of foods, including crunchy fruits, vegetables, and tough meats, without discomfort or fear of your teeth slipping.
- Improved Speech: Removable dentures can sometimes shift or click, affecting pronunciation. Implant-supported teeth are stable, allowing for clear and natural speech.
- Enhanced Aesthetics and Confidence: A complete, beautiful smile significantly boosts self-esteem. Full mouth implants are custom-designed to match your facial structure, providing a natural-looking and permanent smile that feels like your own.
- Preservation of Jawbone: The dental implants stimulate the jawbone, preventing the bone loss that inevitably occurs after tooth loss. This maintains the integrity of your facial structure, preventing the sunken appearance often associated with long-term denture wear.
- Durability and Longevity: With proper care, dental implants can last a lifetime, and the prosthetic teeth can last 10-25 years or more before needing replacement, making them a highly cost-effective long-term solution.
- Comfort and Convenience: Unlike removable dentures that require adhesives, special cleaning solutions, and can cause gum irritation, implant-supported teeth are permanently fixed. You clean them like natural teeth, and they become an integral part of your mouth.
- No More Messy Adhesives: Say goodbye to denture creams and sticky pastes.
- Prevention of Remaining Tooth Movement: If you still have some natural teeth, replacing missing ones with implants helps prevent the remaining teeth from shifting into the empty spaces, which can lead to further dental problems.
Treatment Options: A Comparison
When facing extensive tooth loss, several treatment options exist, each with its own set of advantages and disadvantages. Understanding these alternatives is crucial for making an informed decision.
| Feature | Full Mouth Implants (Fixed Bridge) | Implant-Supported Dentures (Removable) | Traditional Removable Dentures |
|---|---|---|---|
| Stability | Excellent (permanent, fixed) | Very Good (snaps onto implants, removable) | Fair (rests on gums, can slip) |
| Chewing Power | Excellent (close to natural teeth) | Good (significantly better than traditional) | Poor (approx. 10-20% of natural chewing force) |
| Comfort | Excellent (feels like natural teeth) | Good (more secure, less gum irritation) | Fair (can cause sore spots, gum irritation) |
| Speech | Excellent (natural) | Good (minimal interference) | Fair (can be affected by movement, bulkiness) |
| Bone Preservation | Excellent (implants stimulate jawbone) | Good (implants help stimulate bone) | Poor (accelerates bone loss) |
| Maintenance | Like natural teeth (brush, floss, check-ups) | Remove daily for cleaning, regular check-ups | Remove daily for cleaning, adhesives, relines |
| Aesthetics | Excellent (highly natural appearance) | Very Good (stable, natural appearance) | Good (can look artificial, affects facial profile) |
| Longevity (Prosthesis) | 10-25+ years | 5-10+ years (prosthesis); implants last decades | 5-8 years (often needs relining sooner) |
| Cost (Per Arch, US) | $20,000 - $90,000+ | $10,000 - $30,000 | $1,500 - $8,000 (for basic to premium) |
| Invasiveness | Surgical placement of 4-10+ implants | Surgical placement of 2-6 implants | Non-surgical |
Traditional Removable Dentures: These are the most conventional and least expensive option. They consist of a plate with artificial teeth, relying on suction and denture adhesives to stay in place. While they restore some appearance, they offer limited chewing efficiency, can cause discomfort, and accelerate jawbone loss over time. They are a good option for those seeking a quick, economical solution or who are not candidates for surgery.
Implant-Supported Dentures (Overdentures): A significant improvement over traditional dentures, these prostheses snap onto a few strategically placed implants (typically 2-6 per arch). They are removable by the patient for cleaning but offer vastly superior stability, comfort, and chewing power compared to traditional dentures. They still allow some bone stimulation from the implants.
Full Mouth Implants (Fixed Bridge): As discussed, this is the most advanced and robust solution, providing a permanently fixed set of teeth that most closely mimics natural dentition in terms of function, aesthetics, and bone preservation.
The Step-by-Step Process of Getting Full Mouth Implants
Embarking on the journey to full mouth implants is a multi-stage process that requires meticulous planning, precise surgical execution, and patient commitment to healing. While individual timelines may vary, the general steps are consistent.
Step 1: Initial Consultation and Comprehensive Evaluation
This crucial first step involves a detailed discussion with your dental implant specialist (oral surgeon, periodontist, or prosthodontist).
- Medical and Dental History: A thorough review to assess your overall health, any existing medical conditions, medications, and previous dental experiences.
- Oral Examination: A visual inspection of your mouth, gums, and remaining teeth.
- Advanced Imaging: 3D Cone Beam Computed Tomography (CBCT) scans are essential. These provide detailed cross-sectional images of your jawbone, allowing the dentist to precisely map nerve pathways, sinus cavities, and assess bone quality and quantity. Panoramic X-rays and traditional dental X-rays are also taken.
- Impressions: Molds of your mouth are taken to create detailed models of your existing bite and jaw structure.
- Treatment Planning: Based on the evaluation, a customized treatment plan is developed, outlining the number and ideal placement of implants, the type of prosthetic (e.g., All-on-4, traditional bridge), timelines, and estimated costs. Digital smile design may be used to visualize your future smile.
Step 2: Pre-Surgical Preparations
Depending on your oral health, additional procedures might be necessary before implant placement.
- Extractions: Any remaining compromised teeth that cannot be saved will be carefully extracted.
- Bone Grafting: If the CBCT scan reveals insufficient bone volume or density in certain areas, a bone graft may be necessary to create a strong foundation for the implants. This involves adding bone material (from your own body, a donor, or synthetic sources) to the jawbone. This typically requires several months of healing before implant placement can occur.
- Gum Disease Treatment: Any active periodontal disease must be treated and resolved before surgery to ensure a sterile environment.
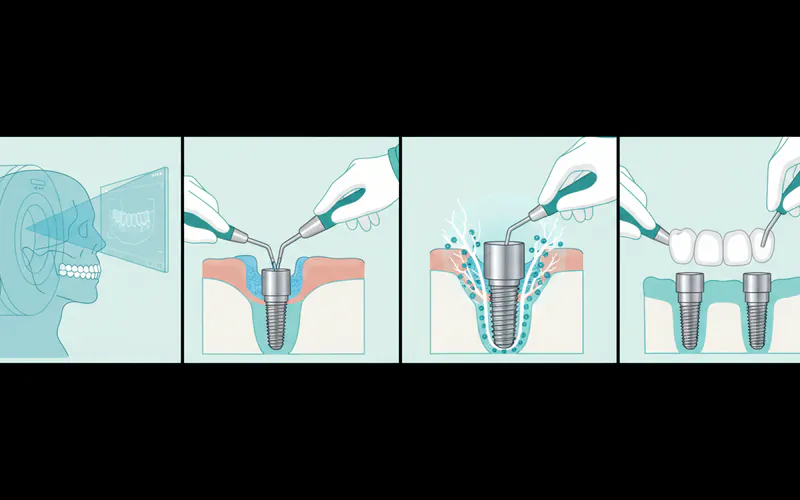
Step 3: Implant Placement Surgery
This is the surgical phase where the dental implants are precisely positioned in your jawbone.
- Anesthesia: Local anesthesia is always used, and sedation options (oral, IV sedation, or general anesthesia) are typically available to ensure your comfort.
- Incision: The surgeon makes small incisions in the gum tissue to expose the underlying jawbone.
- Osteotomy: Using specialized drills, precise pilot holes are created in the bone at the pre-planned locations and angles.
- Implant Insertion: The titanium or zirconia implant posts are then gently screwed into these prepared sites.
- Suturing: The gum tissue is carefully closed with sutures.
- Immediate Provisional (Optional): In cases like All-on-4, a temporary, non-removable arch of teeth (a provisional bridge) may be attached to the newly placed implants on the very same day. This allows you to leave the office with a functional and aesthetic smile. For traditional implants, a removable temporary denture or bridge might be provided.
Step 4: Osseointegration (Healing Period)
This is a critical biological phase where the implants fuse with your jawbone.
- Duration: This process typically takes 3 to 6 months, though it can vary based on individual healing capacity and bone quality.
- Dietary Restrictions: During this time, a soft diet is usually recommended to avoid placing excessive stress on the healing implants.
- Regular Check-ups: Your dentist will monitor your healing progress during this period.
Step 5: Abutment Placement (If Not Already Integrated)
Once osseointegration is complete, the implants are ready to support the final prosthetic.

- Exposure (if submerged): If the implants were fully covered by gum tissue during healing, a minor procedure is performed to expose the top of the implant.
- Abutment Attachment: An abutment – a small connector post – is attached to each implant. This abutment protrudes through the gum line and will serve as the attachment point for your new teeth.
Step 6: Fabrication and Placement of the Final Prosthesis
This is where your new, permanent smile is meticulously crafted and delivered.
- Impressions: New, highly accurate impressions are taken of your mouth and the abutments.
- Custom Fabrication: These impressions are sent to a specialized dental lab where your custom-designed full arch bridge (made of acrylic over a titanium frame, zirconia, or other materials) is precisely fabricated. This involves multiple try-in appointments to ensure perfect fit, bite, and aesthetics.
- Final Placement: Once the final prosthesis is ready and approved, it is securely attached to the abutments. This is typically done by screwing the bridge into place, making it a non-removable, permanent solution.
Step 7: Post-Treatment Care and Follow-up
Your journey doesn't end after the final placement. Regular maintenance and professional check-ups are essential for the long-term success of your full mouth implants.
- Oral Hygiene Education: You will receive detailed instructions on how to properly clean your new implant-supported teeth, including specific brushes, floss, or water picks.
- Regular Check-ups: Consistent dental visits (typically every 6 months) are vital for monitoring the health of your implants, gums, and remaining oral structures.
Pro Tip: Choose a dental implant team with extensive experience in full mouth implant cases. Their expertise in surgical planning, execution, and prosthetic design is paramount to a successful outcome. Don't hesitate to ask about their experience, success rates, and to see before-and-after photos of similar cases.
Cost and Insurance: Understanding the Investment
One of the most significant considerations for full mouth implants is the cost. It's an investment, not just in your teeth, but in your overall health, confidence, and quality of life. Understanding how much do teeth implants cost involves considering multiple factors and components. For those wondering about the cost of a single tooth implant, it's important to note that full mouth solutions are significantly more complex and therefore have a higher overall price tag.
Components of Full Mouth Implant Cost:
The total cost encompasses several stages and components:
-
Diagnostic Phase:
- Initial consultation: $100 - $300
- 3D CBCT Scans, X-rays, impressions: $300 - $800
- Treatment planning and digital smile design: $500 - $1,500
-
Surgical Phase (Per Arch): This includes the implant posts and the surgical procedure to place them.
- Per Implant Post: Each implant itself can range from $1,500 - $3,000.
- Surgical Fee: This varies widely based on the complexity, number of implants, and the surgeon's expertise.
- Anesthesia/Sedation: $500 - $2,000+, depending on the type and duration.
- Extractions: If needed, $75 - $400 per tooth (complex extractions cost more).
- Bone Grafting: If required, can add $200 - $3,000+ per site, depending on the extent and material.
- Sinus Lift: If required for upper jaw implants, $1,500 - $3,000+ per sinus.
-
Prosthetic Phase (Per Arch): This includes the abutments and the final full arch bridge/denture.
- Abutments: Typically $500 - $1,000 per abutment.
- Temporary Provisional (Immediate Load): If provided, $2,000 - $6,000+.
- Final Full Arch Prosthesis: This is a major cost component and varies significantly by material.
- Acrylic with Titanium Bar: $8,000 - $20,000 per arch.
- Full Zirconia: $15,000 - $30,000 per arch.
-
Follow-up and Maintenance:
- Post-operative visits: Often included in the total fee.
- Annual maintenance/hygiene: $150 - $400+ per visit.
Average US Cost Ranges for Full Mouth Implants:
It's crucial to understand these are broad estimates, and prices can vary by region, provider, and specific patient needs.
| Type of Full Mouth Implant Solution | Average Cost Range (Per Arch, US Dollars) |
|---|---|
| All-on-4® (Acrylic/Titanium) | $20,000 - $35,000 |
| All-on-4® (Full Zirconia) | $30,000 - $50,000 |
| All-on-6 / All-on-8 (Zirconia) | $40,000 - $70,000 |
| Traditional Full Arch Bridge (6-10+ implants, PFM/Zirconia) | $50,000 - $90,000+ |
A single tooth implant costs between $3,000 and $6,000, which includes the implant post, abutment, and crown. This helps illustrate the scale of cost for full mouth solutions.
Regional Variations: Costs can be significantly higher in major metropolitan areas (e.g., New York, Los Angeles) compared to rural areas or smaller cities. It's always recommended to get multiple quotes.
Insurance Coverage: What to Expect
Dental insurance typically offers limited coverage for dental implants, especially for full mouth solutions.
- Coverage for Implants: Many dental insurance plans do not cover the implant itself, considering it a "cosmetic" or "major" procedure. If covered, it might only be a small percentage (e.g., 10-20%) after deductibles are met, and up to your annual maximum (often $1,000 - $2,500).
- Coverage for Ancillary Procedures: Some plans might cover portions of the diagnostic phase (X-rays, consultations), extractions, or bone grafting, especially if deemed medically necessary.
- Medical Insurance: If the cause of tooth loss (e.g., trauma, severe infection affecting overall health) or bone grafting is deemed medically necessary, your medical insurance might cover a portion of the surgical costs. This is rare for full mouth procedures but worth investigating.
- Max Out-of-Pocket: Be prepared for significant out-of-pocket expenses, even with insurance.
Pro Tip: Before committing to treatment, have your dental team submit a pre-treatment estimate to your insurance provider(s) to understand exactly what will be covered. This prevents surprises.
Payment Plans and Financing Options:
Given the significant investment, most dental practices offer or work with third-party financing solutions.
- In-Office Payment Plans: Many practices offer flexible payment schedules, allowing you to pay in installments over several months, often interest-free for a short period.
- Third-Party Financing: Companies like CareCredit, LendingClub, or Alphaeon Credit specialize in healthcare financing. They offer various plans, including interest-free options for a specific period (e.g., 6, 12, 18 months) or longer-term plans with competitive interest rates.
- Personal Loans: Banks and credit unions offer personal loans that can be used for dental treatment.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): If you have an HSA or FSA through your employer, you can use pre-tax dollars to pay for dental implant treatment, saving you money on taxes.
Pro Tip: Don't let cost deter you from exploring options. Many people successfully finance their full mouth implants through a combination of insurance benefits, savings, and flexible payment plans. Discuss your financial concerns openly with your dental provider.
Recovery and Aftercare for Full Mouth Implants
Proper recovery and diligent aftercare are paramount to the long-term success and comfort of your full mouth implants. Understanding what to expect during the healing phases and how to maintain your new smile will ensure optimal results.
Immediate Post-Operative Period (First 24-72 Hours):
The first few days after implant surgery are critical for initial healing and managing discomfort.
- Pain Management: Expect some discomfort once the anesthesia wears off. Your surgeon will prescribe pain medication (e.g., prescription painkillers or strong over-the-counter NSAIDs like ibuprofen). Take as directed.
- Swelling: Swelling is common and can peak around 48-72 hours post-surgery. Apply ice packs to the outside of your face in 20-minute intervals (20 minutes on, 20 minutes off) for the first 24-48 hours to minimize swelling.
- Bleeding: Slight oozing or bleeding is normal. Your dentist will provide gauze pads; bite down firmly on them and change as needed. Avoid spitting forcefully, which can dislodge blood clots.
- Diet: Stick to a soft, cold diet for the first few days (e.g., yogurt, smoothies, mashed potatoes, applesauce, lukewarm soup). Avoid hot liquids, hard, crunchy, or chewy foods.
- Oral Hygiene:
- Do NOT brush near the surgical sites for the first 24 hours.
- After 24 hours, you can gently rinse with a prescribed antimicrobial mouthwash (e.g., chlorhexidine) or warm salt water (1/2 teaspoon salt in 8 ounces warm water) several times a day, especially after eating. Swish gently; do not spit forcefully.
- Be extremely careful if you have a temporary prosthesis; clean it gently without dislodging it.
- Activity: Rest is crucial. Avoid strenuous physical activity for at least 48-72 hours to prevent increased bleeding and swelling. Keep your head elevated when resting.
- Smoking/Alcohol: Absolutely avoid smoking and alcohol, as they significantly impair healing and increase the risk of complications.
Intermediate Healing (Weeks 1-2):
As the initial discomfort subsides, the focus shifts to ensuring proper healing and protecting the surgical sites.
- Dietary Progression: Gradually introduce softer, chewable foods as comfort allows, but continue to avoid very hard, sticky, or spicy foods.
- Oral Hygiene: Continue gentle brushing of non-surgical areas. Carefully clean the temporary prosthesis as instructed by your dentist. Continue with antiseptic rinses.
- Suture Removal: If non-dissolvable sutures were used, they will be removed by your dentist at a follow-up appointment, usually around 7-14 days.
- Return to Activity: You can generally return to light daily activities, but continue to avoid heavy lifting or vigorous exercise.
Osseointegration Period (3-6 Months):
This is the phase where the implants fuse with your jawbone. You will typically be wearing a temporary bridge during this time.
- Diet: Maintain a softer diet, especially if you have an immediate provisional bridge. Your dentist will provide specific guidelines to prevent overloading the healing implants. Avoid biting directly into hard foods with your temporary teeth.
- Oral Hygiene: Continue meticulous oral hygiene to prevent infection.
- Regular Check-ups: Attend all scheduled follow-up appointments to monitor the osseointegration process.
Long-Term Aftercare (After Final Restoration):
Once your permanent full arch prosthesis is in place, the focus is on maintaining its longevity and the health of your supporting tissues.
- Daily Oral Hygiene:
- Brushing: Brush at least twice a day with a soft-bristled brush. Special brushes (e.g., interdental brushes, angled brushes) may be recommended to clean around and under the fixed bridge.
- Flossing/Water Pik: Regular use of dental floss (especially super floss or implant-specific floss) or an oral irrigator (Water Pik) is crucial to clean underneath the bridge and around the implants, where food debris and plaque can accumulate. ADA guidelines emphasize thorough cleaning to prevent peri-implantitis.
- Regular Dental Check-ups: Schedule professional cleanings and examinations every 6 months or as advised by your dentist. Your hygienist will have specialized tools for cleaning around implants.
- Nightguard: If you clench or grind your teeth (bruxism), your dentist may recommend wearing a custom nightguard to protect your implants and prosthesis from excessive forces.
- Avoid Damaging Habits: Refrain from biting on hard objects (ice, pens, fingernails), using your teeth as tools, and smoking. Smoking is a significant risk factor for implant failure.
Pro Tip: Think of your full mouth implants as your natural teeth. They require the same (if not more) dedication to oral hygiene and professional care to ensure their long-term success.
Risks and Complications of Full Mouth Implants
While full mouth implants boast a high success rate (typically 95-98% over 10 years), like any surgical procedure, they carry potential risks and complications. Understanding these can help you discuss concerns with your dental team and make informed decisions.
Common Risks and Minor Complications:
- Infection at the Implant Site: This is the most common complication. Symptoms include pain, swelling, pus, and fever. It's often treatable with antibiotics and local cleaning, but in severe cases, the implant may need to be removed.
- Swelling, Bruising, and Discomfort: These are normal post-operative symptoms, typically manageable with medication and cold compresses.
- Numbness: Temporary numbness of the lips, chin, or tongue can occur if nerves are irritated or bruised during surgery. Permanent nerve damage is rare but possible if a nerve is severed or severely compressed.
- Sinus Perforation (Upper Jaw Implants): If implants are placed in the upper jaw, there's a small risk of perforating the maxillary sinus cavity. This is usually easily managed during surgery, but can lead to sinus issues if not addressed.
- Implant Loosening: Though rare, an implant may not properly integrate with the bone or can loosen over time. This typically requires removal of the implant and, after a healing period, potentially a new implant placement.
More Serious (But Less Common) Complications:
- Implant Failure (Lack of Osseointegration): The implant fails to fuse with the bone. This can be due to poor bone quality, infection, smoking, certain medical conditions, or early loading of the implant.
- Peri-Implantitis: This is a chronic inflammatory condition affecting the tissues around the dental implant, similar to gum disease (periodontitis) around natural teeth. It can lead to bone loss around the implant and eventually implant failure if not treated. Poor oral hygiene, smoking, and certain systemic diseases are major risk factors.
- Damage to Adjacent Structures: Rarely, implants can damage adjacent teeth, blood vessels, or bone during placement.
- Prosthetic Complications: The final bridge or denture might chip, fracture, or loosen. This usually requires repair or replacement of the prosthesis.
- Allergic Reaction: While rare with titanium or zirconia, some individuals can have an allergic reaction to implant materials.
Factors That Increase Risk:
- Smoking: Significantly reduces blood flow, impairs healing, and increases the risk of implant failure and peri-implantitis.
- Poor Oral Hygiene: Leads to plaque and bacterial buildup, increasing infection risk.
- Uncontrolled Chronic Diseases: Conditions like diabetes, autoimmune disorders, and osteoporosis can affect healing and bone integration.
- Radiation Therapy: Previous radiation therapy to the head and neck area can compromise bone healing.
- Certain Medications: Some medications (e.g., bisphosphonates) can affect bone metabolism and implant success.
- Insufficient Bone Quality/Quantity: Increases the complexity and risk, often requiring bone grafting.
- Operator Inexperience: Choosing an inexperienced surgeon increases the risk of complications.

Mitigating Risks:
- Thorough Planning: Advanced 3D imaging (CBCT) and digital planning are essential to avoid vital structures and ensure optimal implant placement.
- Sterile Surgical Environment: Strict adherence to sterile protocols minimizes infection risk.
- Patient Education: Understanding proper oral hygiene and aftercare instructions is crucial.
- Smoking Cessation: Patients are strongly advised to quit smoking before and after surgery.
- Medical Clearance: Ensuring any underlying medical conditions are well-managed before surgery.
- Experienced Surgeon: Choosing a board-certified oral surgeon, periodontist, or prosthodontist with extensive experience in full mouth implant cases is the best way to minimize risks.
Pro Tip: Discuss any medical conditions, medications you are taking, or concerns you have with your dental team during your initial consultation. Transparency is key to a safe and successful outcome.
Prevention (Maintaining Oral Health to Avoid Full Mouth Implants)
While full mouth implants are a remarkable solution for extensive tooth loss, the ideal scenario is to prevent such loss in the first place. Comprehensive oral hygiene and regular dental care are the cornerstones of preventing the need for such extensive interventions.
Key Pillars of Prevention:
-
Diligent Oral Hygiene:
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes, covering all surfaces of your teeth and gently brushing your tongue.
- Floss Daily: Flossing removes plaque and food particles from between teeth and under the gum line, areas your toothbrush can't reach. This is critical for preventing gum disease and cavities.
- Use Mouthwash (Optional): An antimicrobial or fluoride mouthwash can provide an added layer of protection but should not replace brushing and flossing.
- Clean Your Tongue: A tongue scraper or toothbrush can remove bacteria and freshen breath.
-
Regular Dental Check-ups and Professional Cleanings:
- Every Six Months: The American Dental Association (ADA) recommends professional dental examinations and cleanings at least twice a year. These visits allow your dentist to:
- Detect and treat cavities early before they become large and require extensive work or extraction.
- Identify and manage gum disease (gingivitis or periodontitis) before it leads to bone loss and tooth mobility.
- Check for signs of oral cancer or other issues.
- Remove hardened plaque (calculus) that brushing and flossing can't.
- Every Six Months: The American Dental Association (ADA) recommends professional dental examinations and cleanings at least twice a year. These visits allow your dentist to:
-
Healthy Diet:
- Limit Sugary and Acidic Foods/Drinks: Sugars feed bacteria that produce acids, leading to tooth decay. Acidic foods and drinks (like sodas, citrus fruits) can erode tooth enamel.
- Choose Nutrient-Rich Foods: A diet rich in fruits, vegetables, lean proteins, and dairy products (for calcium) supports strong teeth and healthy gums.
-
Avoid Damaging Habits:
- Smoking/Tobacco Use: Tobacco products are a leading cause of gum disease, tooth loss, and oral cancer. Quitting is one of the best things you can do for your oral health.
- Teeth Grinding/Clenching (Bruxism): Can wear down teeth, cause fractures, and lead to temporomandibular joint (TMJ) issues. If you grind your teeth, your dentist may recommend a nightguard.
- Using Teeth as Tools: Don't use your teeth to open packages, cut threads, or bite on non-food items (pens, ice).
- Excessive Alcohol Consumption: Can contribute to dry mouth, erosion, and increase the risk of oral cancer.
-
Address Dental Issues Promptly:
- Don't Ignore Pain: Any persistent toothache, sensitivity, bleeding gums, or loose teeth should be evaluated by a dentist immediately. Delaying treatment often leads to more severe and costly problems.
- Treat Gum Disease Early: Gingivitis is reversible; advanced periodontitis is manageable but can lead to irreversible bone loss and tooth loss.
By adhering to these preventive measures, you significantly reduce your risk of extensive tooth loss and the need for comprehensive treatments like full mouth implants, preserving your natural smile for as long as possible.
Frequently Asked Questions
Q1: Is the full mouth implant procedure painful?
A1: The actual implant placement surgery is performed under local anesthesia, and often with sedation (oral, IV, or general anesthesia), so you will not feel pain during the procedure. Post-operative discomfort, swelling, and bruising are normal but are typically managed effectively with prescribed pain medication and over-the-counter pain relievers. Most patients report manageable discomfort rather than severe pain.
Q2: How long do full mouth implants last?
A2: The dental implants themselves (the titanium or zirconia posts) are designed to be a permanent solution and can last a lifetime with proper care and successful osseointegration. The prosthetic teeth (the full arch bridge) typically last 10 to 25 years or more before they might need repair or replacement due to wear and tear. Regular maintenance and hygiene are crucial for longevity.
Q3: What is the success rate of full mouth implants?
A3: Dental implants have an impressive long-term success rate, generally reported to be between 95% and 98% over 10 years when placed by experienced professionals and maintained properly. Factors such as overall health, smoking status, bone quality, and diligent oral hygiene significantly influence success rates.
Q4: Can I get new teeth in one day with full mouth implants?
A4: Yes, in many cases, especially with systems like All-on-4®, it is possible to receive a temporary set of prosthetic teeth on the same day as your implant surgery. This is known as "immediate load" or "teeth in a day." These temporary teeth function while your implants heal, after which they are replaced with a permanent, custom-fabricated prosthesis. Not all patients are candidates for immediate loading.
Q5: Will full mouth implants look and feel like natural teeth?
A5: Yes, one of the primary benefits of full mouth implants is their ability to closely mimic the look and feel of natural teeth. They are custom-designed to match your facial structure and blend aesthetically. Because they are anchored in your jawbone, they provide exceptional stability, chewing power, and comfort, virtually indistinguishable from your original teeth.
Q6: What are the alternatives to full mouth implants?
A6: The main alternatives for full arch tooth replacement are traditional removable dentures and implant-supported removable dentures (overdentures). Traditional dentures are the least expensive but offer limited stability and chewing power. Implant-supported removable dentures provide better stability than traditional dentures but are still removable for cleaning, unlike fixed full mouth implants.
Q7: How do I clean and care for full mouth implants?
A7: Caring for full mouth implants is similar to caring for natural teeth, but with specific considerations. You should brush at least twice daily with a soft-bristled brush. Crucially, you'll need to use special tools like dental floss threaders, super floss, or an oral irrigator (Water Pik) to clean thoroughly under and around the fixed prosthetic bridge, where food particles and plaque can accumulate. Regular professional cleanings and check-ups every 6 months are also essential.
Q8: Am I a good candidate for full mouth implants?
A8: Generally, good candidates are adults in good overall health with sufficient jawbone to support the implants (or are candidates for bone grafting). Non-smokers or those willing to quit have higher success rates. A comprehensive evaluation by an implant dentist, including 3D imaging, is necessary to determine your specific candidacy. Conditions like uncontrolled diabetes or certain autoimmune diseases may affect candidacy.
Q9: What's the difference between All-on-4 and traditional full arch implants?
A9: The primary difference lies in the number and placement of implants. All-on-4 uses four strategically angled implants to support a full arch, often allowing for immediate provisional teeth and avoiding bone grafts. Traditional full arch implants typically use 6-10 or more implants placed more uniformly across the jawbone, often requiring longer healing periods and sometimes bone grafting, but potentially offering even greater long-term stability in complex cases.
Q10: How much does a single tooth implant cost compared to full mouth implants?
A10: The cost of a single tooth implant typically ranges from $3,000 to $6,000, which includes the implant post, abutment, and the final crown. Full mouth implants, which involve multiple implants and a full arch prosthesis, are a much more extensive procedure. As discussed, the cost of full mouth implants can range from $20,000 to $90,000+ per arch, depending on the type of system, materials, and complexity.
When to See a Dentist
Recognizing when to seek professional dental care is crucial for maintaining oral health and ensuring the longevity of any dental work, including full mouth implants.
For Initial Consultation:
- You're Missing Multiple or All Teeth: If you've lost several teeth in an arch, or are facing complete tooth loss, it's time to explore replacement options like full mouth implants.
- Failing or Severely Damaged Teeth: If you have numerous teeth that are chronically painful, infected, loose, or deemed beyond repair by your current dentist, consider a consultation to discuss full mouth implant solutions before further deterioration.
- Dissatisfaction with Dentures: If you struggle with uncomfortable, ill-fitting, or unstable removable dentures that impact your ability to eat, speak, or smile confidently, an implant consultation can provide information on a more permanent solution.
- Chronic Oral Health Issues: Persistent pain, infection, or difficulty chewing that significantly impacts your quality of life warrants a detailed evaluation.
Post-Implant Surgery (Red Flags Needing Immediate Attention):
While some discomfort and swelling are normal after implant surgery, certain symptoms warrant immediate contact with your dental implant specialist:
- Severe or Worsening Pain: If pain is intense and not managed by prescribed medication, or if it suddenly worsens days after surgery.
- Excessive Bleeding: If bleeding is heavy and does not stop after biting firmly on gauze for 30-60 minutes, or if it persists for an extended period.
- Persistent Swelling After 72 Hours: If swelling continues to increase after the third day post-surgery, or is accompanied by severe pain or fever.
- Signs of Infection: Pus, foul taste or smell, fever, or red streaks extending from the surgical site.
- Numbness That Doesn't Resolve: If persistent numbness in your lip, chin, or tongue does not begin to subside after the local anesthesia should have worn off.
- Dislodged or Loose Temporary Prosthesis: If your temporary bridge becomes loose, breaks, or falls out, contact your dentist immediately, especially if it was an immediate load provisional.
- Implant Movement: Any feeling of movement or instability in the implant site itself.
These are critical warning signs that should not be ignored. Prompt professional attention can prevent more serious complications and ensure the success of your full mouth implants. For any concerns or unusual symptoms, always err on the side of caution and reach out to your dental professional.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Implantologist: Complete Guide
Losing a tooth can be a significant setback, impacting not only your smile but also your ability to speak, chew, and maintain overall oral health. In fact, over 3 million Americans currently have dental implants, and that number is projected to grow significantly as more people seek a durable, n
March 8, 2026
Dentures Over Implants: Complete Guide
Missing multiple teeth or even an entire arch can profoundly impact your life, affecting everything from your ability to chew and speak to your self-confidence. For millions of Americans, traditional removable dentures have long been a solution, but they often come with compromises: slipping, discom
March 8, 2026
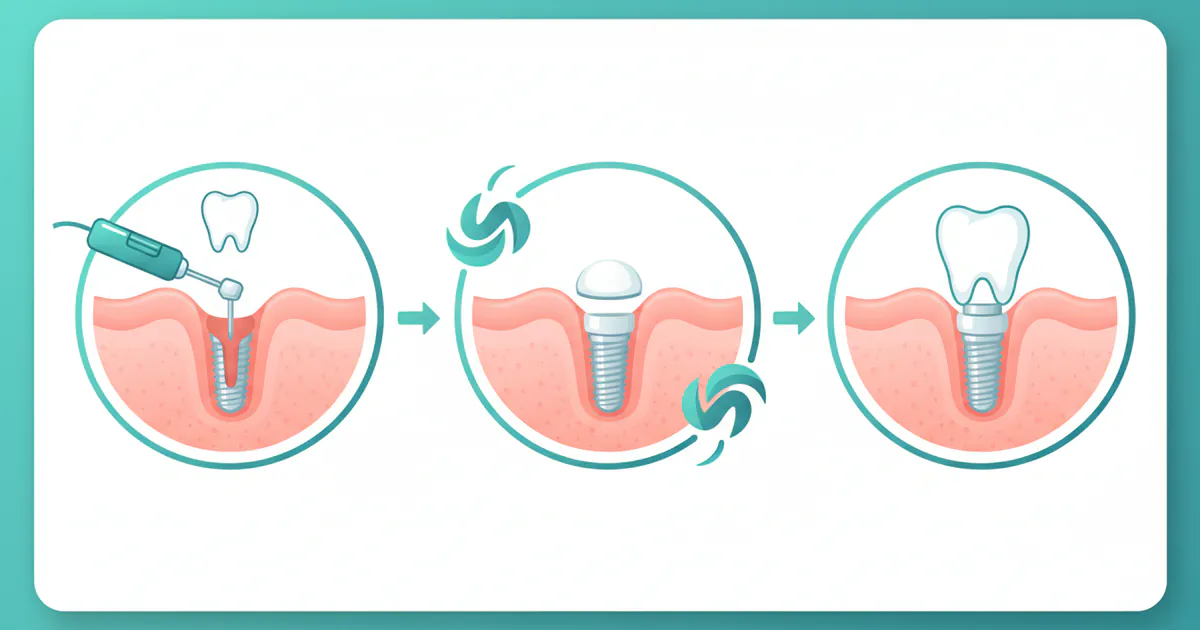
Implants Process: Complete Guide
Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the
March 8, 2026

Implants Dentaires: Complete Guide
Missing teeth can dramatically impact not just your smile, but your overall health, confidence, and quality of life. In the United States, an estimated 178 million adults are missing at least one tooth, while approximately 40 million are missing all their teeth. These statistics underscore a
March 8, 2026