Tooth Implant Side Effects: Complete Guide
Key Takeaways
- Dental implants have revolutionized tooth replacement, offering a durable and natural-looking solution for millions. In the United States, an estimated 3 million people currently have dental implants, with this number growing by about 500,000 annually. For those considering this advanced restora
Tooth Implant Side Effects: Complete Guide
Dental implants have revolutionized tooth replacement, offering a durable and natural-looking solution for millions. In the United States, an estimated 3 million people currently have dental implants, with this number growing by about 500,000 annually. For those considering this advanced restorative option, understanding the potential tooth implant side effects is a crucial step in making an informed decision. While dental implants boast an impressive success rate of over 95%, no surgical procedure is entirely without risk. This comprehensive guide from SmilePedia.net aims to provide a detailed, medically accurate overview of common and rare side effects, complications, their causes, and how they are managed, ensuring you are fully prepared for your implant journey. We will delve into specific considerations for procedures like full arch implants and the implications of same day tooth extraction and implant placement, equipping you with the knowledge to discuss your treatment confidently with your dental professional.

Key Takeaways:
- Dental implants have a success rate exceeding 95%, making them a highly reliable tooth replacement option.
- Most tooth implant side effects are minor, temporary, and manageable, such as pain, swelling, and bruising, peaking within 2-3 days post-surgery.
- Serious complications like infection, nerve damage, or implant failure are rare but require immediate dental attention.
- The average cost for a single dental implant in the US ranges from $3,000 to $6,000, including the abutment and crown. Full arch implants can cost $15,000 to $30,000 per arch.
- Effective prevention of side effects involves choosing an experienced surgeon, thorough pre-operative planning, meticulous oral hygiene, and adhering to post-operative instructions.
- Recovery for a single implant typically involves 1-2 weeks for initial healing, with full osseointegration taking 3-6 months.
- Insurance coverage for dental implants is often limited, but financing options and HSAs/FSAs can help manage costs.
What Are Dental Implants? An Overview
A dental implant is a sophisticated medical device designed to replace missing tooth roots and support a prosthetic tooth, bridge, or denture. It typically consists of three main components:
- The Implant Post (Fixture): A small, screw-shaped post, usually made of biocompatible titanium, that is surgically placed into the jawbone. This post acts as the artificial tooth root.
- The Abutment: A connector piece that attaches to the implant post and extends above the gum line. It serves as the base for the final restoration.
- The Prosthetic Restoration: This can be a dental crown (for a single tooth), a multi-tooth bridge, or a full denture, custom-made to match your natural teeth and bite.
The magic behind dental implants lies in a biological process called osseointegration, where the titanium implant post fuses directly with the surrounding jawbone. This fusion provides remarkable stability and strength, allowing the implant to function much like a natural tooth root. This strong foundation not only supports chewing function but also helps preserve jawbone density, preventing the bone loss that often occurs after tooth extraction. The American Dental Association (ADA) recognizes dental implants as a safe and effective treatment for tooth loss.
![A detailed diagram illustrating the components of a dental implant: a screw-shaped post embedded in the jawbone, an abutment(/glossary/abutment) connecting to it, and a crown placed on top of the abutment.]
Types of Dental Implants and Their Relevance to Side Effects
While the basic concept remains similar, dental implants come in various forms and are used in different treatment approaches, each with specific considerations regarding potential tooth implant side effects.
Endosteal Implants
These are the most common type of dental implant. "Endosteal" means "in the bone." They are typically titanium screws, cylinders, or blades surgically placed directly into the jawbone. They are suitable for most patients with healthy jawbone.
- Relevance to Side Effects: Being the standard, most documented side effects and complications relate to endosteal implants. Their predictable surgical protocol generally leads to fewer unexpected issues compared to more complex types, provided adequate bone volume is present.
Subperiosteal Implants
Less common today, subperiosteal implants are placed on top of the jawbone but still under the gum tissue. They consist of a metal framework that is custom-made to fit over the bone and has posts that protrude through the gums to hold the prosthetic teeth. They are typically used for patients who cannot wear conventional dentures and have minimal bone height.
- Relevance to Side Effects: Due to their placement, risks can include gum irritation, infection around the frame, and less long-term stability than endosteal implants, making them a less favorable option in modern dentistry.
Zygomatic Implants
These are specialized, long implants anchored into the cheekbone (zygoma) rather than the jawbone. They are reserved for patients with severe bone loss in the upper jaw who are not candidates for traditional implants or extensive bone grafting.
- Relevance to Side Effects: Zygomatic implants are considerably more complex surgeries performed by highly specialized oral surgeons. Side effects can be more significant and include sinusitis, numbness, and swelling around the cheek and eye area, given their proximity to critical anatomical structures. The recovery period can also be more intensive.
Mini Implants (MDIs)
Mini dental implants are smaller in diameter than traditional implants (typically less than 3mm). They are often used for stabilizing lower dentures, providing temporary support, or in areas with limited bone width without the need for extensive bone grafting.
- Relevance to Side Effects: While less invasive, they may have a higher risk of fracture or instability in some cases due to their smaller size. Side effects are generally milder but can include loosening or breakage if not properly indicated or cared for.
Full Arch Implants (e.g., All-on-4, All-on-6)
These procedures replace an entire arch of missing teeth (upper or lower) using a reduced number of implants (typically four to six) that strategically support a full fixed bridge. The full arch implants approach often allows for immediate loading, meaning a temporary bridge can be placed on the same day as implant surgery.
- Relevance to Side Effects: While highly effective, full arch implants involve more extensive surgery. Potential tooth implant side effects can include increased swelling and bruising due to multiple implant placements, higher risk of nerve involvement if careful planning isn't followed, and potential complications related to immediate loading if proper patient selection isn't observed. The success relies heavily on the quality of the remaining bone and the surgeon's expertise.
Same Day Tooth Extraction and Implant Placement (Immediate Implants)
This technique involves placing a dental implant immediately after a tooth extraction during the same surgical appointment. In some cases, a temporary crown can also be placed right away (immediate loading). This approach saves time and reduces the number of surgical procedures.
- Relevance to Side Effects: While convenient, same day tooth extraction and implant placement carries specific risks. The immediate post-extraction socket may not always be ideal for implant stability, potentially increasing the risk of early implant failure due to lack of primary stability or infection if the site is not thoroughly debrided. Careful patient selection, sufficient bone quality at the extraction site, and excellent surgical technique are paramount to minimize tooth implant side effects in this scenario.
Understanding Tooth Implant Side Effects and Complications
While dental implant surgery is highly successful, it's essential to differentiate between expected post-surgical discomfort (minor side effects) and less common, more serious complications. Most issues are minor and easily managed.
Minor and Expected Post-Surgical Side Effects
These are normal responses to any oral surgery and typically resolve within a few days to a week.
- Pain and Discomfort: This is the most common side effect. It's usually mild to moderate and manageable with over-the-counter pain relievers like ibuprofen or acetaminophen, or prescription medication provided by your dentist. Pain typically peaks within the first 24-48 hours and gradually subsides.
- Swelling: Expect some swelling in the gums and face near the surgical site. It often peaks around 48-72 hours after surgery and can last for several days.
- Bruising: Discoloration of the skin and gums around the surgical area is common, especially after more extensive procedures. It usually resolves within a week to ten days.
- Minor Bleeding/Oozing: It's normal to experience slight bleeding or oozing from the surgical site for the first 24-48 hours. Your dentist will provide gauze pads and instructions to manage this.
- Numbness: Temporary numbness of the lips, tongue, or chin can occur due to local anesthesia. This usually wears off within a few hours. In rare cases, if a nerve is inadvertently irritated during surgery, temporary or persistent numbness can occur (see "Nerve Damage" below).
- Jaw Stiffness: Limited jaw opening or soreness of the jaw muscles can occur due to the surgical procedure and keeping your mouth open for an extended period. This typically improves within a few days.
Pro Tip: Apply an ice pack to the outside of your face, over the surgical area, for 15-20 minutes on and 15-20 minutes off during the first 24-48 hours to minimize swelling and bruising. Elevating your head while sleeping can also help.
Potential Complications (More Serious Tooth Implant Side Effects)
These complications are less common, affecting a small percentage of patients, but they are important to recognize and address promptly.
- Infection: Although prophylactic antibiotics are often prescribed, infection can occur at the implant site.
- Causes: Poor oral hygiene, compromised immune system, pre-existing infection, contamination during surgery.
- Signs & Symptoms: Persistent or worsening pain, fever, pus discharge, severe swelling, redness, bad taste or odor.
- Treatment: Antibiotics, drainage of the infection, surgical cleaning (debridement) of the implant site, or in severe cases, removal of the implant.
- Nerve Damage: This is a rare but serious complication, especially with implants placed in the lower jaw where the inferior alveolar nerve runs.
- Causes: Implant placed too close to or directly into a nerve, trauma during drilling.
- Signs & Symptoms: Persistent numbness, tingling, or even pain in the lips, chin, tongue, or gum tissue. It can be temporary or, rarely, permanent.
- Treatment: May involve medication, observation, or in some cases, removal of the implant to alleviate pressure on the nerve. Early intervention is key.
- Sinus Issues: For implants placed in the upper jaw, especially in the posterior region, there's a risk of penetrating the maxillary sinus.
- Causes: Insufficient bone height between the implant site and the sinus cavity.
- Signs & Symptoms: Sinus congestion, pain, persistent drainage, nosebleeds, or the implant protruding into the sinus cavity.
- Treatment: Minor perforations may heal on their own or with antibiotics. Larger perforations may require a sinus lift procedure or, in severe cases, implant removal and surgical repair of the sinus membrane.
- Implant Failure (Lack of Osseointegration): This occurs when the implant does not successfully fuse with the jawbone. This is a primary reason for early tooth implant side effects leading to failure.
- Causes: Poor bone quality, uncontrolled systemic diseases (e.g., uncontrolled diabetes), heavy smoking, premature loading of the implant, infection, trauma to the implant during healing, insufficient primary stability during placement.
- Signs & Symptoms: Implant mobility (feeling loose), persistent pain or discomfort around the implant, inflammation, or visible bone loss around the implant on X-rays.
- Treatment: The failed implant must be removed. After a healing period, and possibly a bone graft, another implant can often be placed.
- Peri-implantitis: This is an inflammatory condition affecting the tissues surrounding a dental implant, leading to bone loss. It's similar to periodontal disease around natural teeth.
- Causes: Poor oral hygiene, accumulation of plaque and bacteria, residual cement from the crown, smoking, uncontrolled diabetes, certain genetic factors.
- Signs & Symptoms: Red, swollen, or bleeding gums around the implant, pus discharge, deep probing depths, visible recession of gum tissue, and bone loss around the implant seen on X-rays, eventually leading to implant mobility.
- Treatment: Initial treatment involves deep cleaning (debridement) and local or systemic antibiotics. More advanced cases may require surgical intervention to remove infected tissue, reshape bone, or regenerate lost bone around the implant. If untreated, it can lead to implant loss.
- Damage to Adjacent Structures:
- Causes: Incorrect angulation during drilling, inadequate surgical planning.
- Signs & Symptoms: Damage to adjacent teeth (roots or crowns), blood vessels, or surrounding bone during implant placement.
- Treatment: May involve restorative dental work on damaged teeth or management of bleeding.
- Allergic Reaction: While titanium is highly biocompatible, very rare allergic reactions to titanium or other implant materials have been reported.
- Signs & Symptoms: Swelling, rash, itching, or failure of osseointegration without other clear causes.
- Treatment: Implant removal may be necessary.
- Fracture of Implant Components: The implant post, abutment, or crown can fracture.
- Causes: Excessive biting forces (e.g., bruxism, clenching), improper bite alignment, fatigue over time.
- Signs & Symptoms: Pain, mobility of the crown or abutment, visible crack, difficulty chewing.
- Treatment: Replacement of the fractured component. If the implant post itself fractures, removal and replacement are usually required.
Why Do Tooth Implant Side Effects Occur? (Causes and Contributing Factors)
Understanding the underlying reasons for tooth implant side effects can help patients and clinicians take proactive steps to minimize risks.
1. Surgical Factors
- Inexperienced Surgeon: Inadequate training or lack of experience can lead to errors in implant placement, such as incorrect angulation, placing implants too close to nerves or sinuses, or poor sterilization protocols.
- Inadequate Pre-surgical Planning: Failing to use advanced imaging (like 3D CT scans) to accurately assess bone volume, density, and the proximity of vital anatomical structures (nerves, sinuses) significantly increases risks.
- Poor Surgical Technique: Aggressive drilling, overheating the bone during drilling, or insufficient primary stability of the implant can hinder osseointegration.
2. Patient Factors
- Smoking: Tobacco use is a major risk factor, significantly impairing blood flow, healing, and increasing the risk of infection and peri-implantitis. Smokers have a considerably higher rate of implant failure.
- Uncontrolled Systemic Diseases:
- Diabetes: Poorly controlled diabetes impairs healing, reduces bone regeneration, and increases susceptibility to infection.
- Osteoporosis: While not an absolute contraindication, severe osteoporosis (especially when treated with certain medications like bisphosphonates) can affect bone healing and integration, increasing the risk of osteonecrosis of the jaw.
- Autoimmune Diseases: Conditions that suppress the immune system or require certain medications can affect healing.
- Bruxism (Teeth Grinding/Clenching): Excessive forces on implants can lead to component fracture, bone loss around the implant, or failure of osseointegration.
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque and bacteria to accumulate, leading to gum inflammation and potentially peri-implantitis.
- Radiation Therapy: Previous radiation to the head and neck area can compromise bone health and healing capacity, increasing implant failure rates.
3. Anatomical Factors
- Insufficient Bone Volume or Density: Lack of adequate jawbone makes stable implant placement difficult and increases the need for bone grafting, which introduces additional surgical risks.
- Proximity to Vital Structures: Nerves (e.g., inferior alveolar nerve in the mandible) and sinus cavities (in the maxilla) are close to potential implant sites. Inadequate planning can lead to their injury.
4. Material Factors
- Allergic Reaction to Titanium: Extremely rare, but some individuals might have a hypersensitivity to titanium or other components of the implant.
- Low-Quality Implant Materials: Using inferior implant systems can affect their long-term stability and success. Reputable dentists use implants from established, research-backed manufacturers.
5. Post-operative Care
- Non-compliance with Instructions: Failing to follow post-operative instructions regarding diet, oral hygiene, medication, and activity levels can severely jeopardize healing and lead to complications.
- Early or Excessive Loading: Placing too much force on an implant before complete osseointegration can lead to micro-movement and failure of fusion.
Signs and Symptoms: When to Be Concerned
While some discomfort is normal after dental implant surgery, certain signs and symptoms warrant immediate attention from your dentist or oral surgeon.
Contact your dental professional if you experience any of the following:
- Severe or Worsening Pain: Pain that is not controlled by prescribed medication, or pain that significantly increases after the first 2-3 days post-surgery.
- Fever or Chills: These can be signs of a systemic infection.
- Pus or Discharge: Any yellow, green, or foul-smelling discharge from the surgical site is a clear sign of infection.
- Increasing Swelling or Bruising: Swelling and bruising that worsen after 72 hours or spread significantly, rather than gradually diminishing.
- New or Persistent Numbness: If the numbness from anesthesia does not wear off within several hours, or if you develop new numbness, tingling, or unusual sensations in the lips, chin, or tongue days after surgery.
- Implant Mobility: If the implant feels loose, wobbly, or moves when touched. This is a critical sign of implant failure.
- Uncontrolled Bleeding: Bleeding that soaks gauze pads quickly and does not slow down with direct pressure after several hours.
- Significant Difficulty Swallowing or Breathing: While rare, these could indicate a severe allergic reaction or significant swelling impacting airways.
- Visible Exposure of the Implant Thread: If you can see the metal threads of the implant post through the gum tissue after the initial healing period.
- Persistent Sinus Symptoms: For upper jaw implants, persistent congestion, pain, or drainage that doesn't improve.
These "red flag" symptoms are distinct from the expected mild post-operative discomfort. Don't hesitate to reach out to your dental team if you have any concerns.
The Dental Implant Process: Minimizing Risks
A well-executed dental implant process is crucial for minimizing the risk of tooth implant side effects and ensuring long-term success.
1. Initial Consultation and Assessment
This is the foundational step. Your dentist or oral surgeon will conduct a thorough examination of your oral health, including:
- Comprehensive Medical and Dental History: To identify any systemic conditions, medications, or habits (e.g., smoking) that could impact implant success.
- Oral Examination: Assessment of your remaining teeth, gums, and bite.
- Imaging: X-rays and often a 3D Cone Beam Computed Tomography (CBCT) scan. The CBCT provides detailed images of your jawbone, nerve pathways, and sinus cavities, allowing for precise implant placement planning and avoiding vital structures.
- Treatment Plan Development: Based on the assessment, a personalized treatment plan is created, outlining the type of implants, number needed, potential need for bone grafting, and overall timeline.
2. Bone Grafting (If Needed)
If your jawbone lacks sufficient height or density to support an implant, a bone grafting procedure may be necessary before or at the time of implant placement.
- Purpose: To build up the bone volume.
- Types: Autograft (your own bone), allograft (donor human bone), xenograft (animal bone), or synthetic materials.
- Process: Bone material is placed at the deficient site, often covered with a membrane to protect it.
- Recovery: This procedure adds a healing period of several months (typically 4-9 months) before the implant can be placed, to allow the graft to integrate.
3. Tooth Extraction (If Necessary)
If a damaged tooth needs to be removed prior to implant placement, this is done with care to preserve as much bone as possible.
- Same Day Tooth Extraction and Implant: In suitable cases, the implant can be placed immediately into the fresh extraction socket. This requires excellent bone quality and stability at the site. This single-stage approach minimizes patient appointments and healing time but requires careful patient selection to avoid complications.
4. Implant Placement Surgery
This is the surgical phase where the implant post is placed into your jawbone.
- Anesthesia: Local anesthesia is typically used, often combined with sedation (oral, IV, or nitrous oxide) to ensure your comfort.
- Procedure: A small incision is made in the gum tissue to expose the bone. A precise hole is drilled into the jawbone, and the titanium implant post is carefully threaded into place. The gum tissue is then either closed over the implant (submerged technique) or a healing abutment is placed to keep the gum tissue open (one-stage technique).
- Duration: A single implant placement usually takes 30-60 minutes, while multiple implants or full arch implants will take longer.
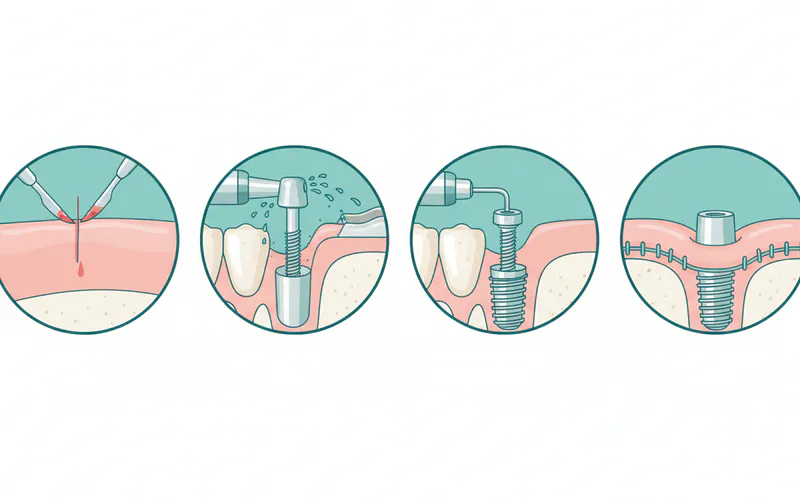
5. Osseointegration Period
This is the critical healing phase where the implant fuses with the surrounding jawbone.
- Timeline: This process typically takes 3 to 6 months, depending on bone quality, patient health, and the specific implant system used. During this time, the implant is usually left undisturbed.
- Importance: Successful osseointegration is fundamental to the long-term stability and success of the implant.
6. Abutment Placement (If Not Already Placed)
If the implant was initially covered by gum tissue, a minor surgical procedure is performed to expose the implant and attach a healing abutment. This allows the gum tissue to heal around it, forming a cuff that will protect the final restoration. This usually takes a few weeks.
7. Crown/Prosthesis Placement
Once osseointegration is complete and the gums have healed around the abutment, impressions are taken to create your custom-made crown, bridge, or denture.
- Customization: The prosthetic is designed to match the color, shape, and size of your natural teeth and to ensure proper bite alignment.
- Attachment: The final restoration is then securely attached to the abutment.
Recovery and Aftercare: Preventing Complications
Proper post-operative care is paramount in preventing tooth implant side effects and ensuring the long-term success of your implant. Your dental professional will provide specific instructions, but here are general guidelines:
Immediate Post-Operative (First 24-48 Hours)
- Bleeding Control: Bite firmly on gauze pads placed over the surgical site for 30-45 minutes. Change pads as needed. Slight oozing is normal; heavy bleeding is not.
- Pain Management: Take prescribed pain medication as directed, or use over-the-counter options. Start taking it before the local anesthetic completely wears off.
- Swelling Reduction: Apply an ice pack to the outside of your face (15-20 minutes on, 15-20 minutes off) for the first 24-48 hours. Keep your head elevated, even when sleeping.
- Diet: Stick to soft, cool foods and liquids. Avoid hot foods, crunchy or chewy items, and using a straw (which can dislodge the blood clot). Examples: yogurt, applesauce, mashed potatoes, smoothies (no straw), soft scrambled eggs.
- Oral Hygiene: Do NOT rinse vigorously or spit forcefully for the first 24 hours. After 24 hours, gently rinse with a warm salt-water solution (1/2 teaspoon salt in 8 ounces of warm water) 3-4 times a day, especially after meals. Brush other teeth normally but avoid the surgical site.
- Activity: Rest, avoid strenuous activity, heavy lifting, or bending over for at least 24-48 hours.

First Week to Two Weeks
- Diet: Gradually reintroduce semi-soft foods, chewing on the opposite side of your mouth if possible. Avoid very hard, crunchy, or spicy foods until fully healed.
- Oral Hygiene: Continue gentle salt-water rinses. You may be instructed to gently brush the surgical site with a very soft toothbrush after a few days, or use a prescribed antimicrobial rinse (e.g., chlorhexidine).
- Avoid Smoking & Alcohol: These significantly impair healing and increase the risk of infection and implant failure. Avoid completely for as long as possible, ideally permanently.
- Medications: Complete any prescribed antibiotics to prevent infection. Continue pain medication as needed.
- Follow-up Appointments: Attend all scheduled follow-up appointments so your dentist can monitor healing, remove sutures (if non-dissolvable), and address any concerns.
Long-Term Aftercare (After Osseointegration and Restoration)
- Meticulous Oral Hygiene: Treat your implant like a natural tooth. Brush twice daily with a soft-bristle brush, floss daily (using specific implant-friendly floss or interdental brushes), and consider a water flosser. Peri-implantitis is largely preventable with excellent oral hygiene.
- Regular Dental Check-ups: Visit your dentist for professional cleanings and examinations at least twice a year. Your dentist will monitor the health of your implant and surrounding tissues.
- Protect Against Grinding: If you clench or grind your teeth (bruxism), your dentist may recommend a nightguard to protect your implant and natural teeth from excessive forces, which can lead to implant component fracture or bone loss.
- Healthy Lifestyle: Maintain a balanced diet and manage any systemic health conditions (like diabetes) to support overall oral health.
Pro Tip: If you notice any unusual redness, swelling, or pain around your implant, even years after placement, contact your dentist immediately. Early detection of peri-implantitis can prevent implant loss.
Treatment Options for Tooth Implant Complications
When tooth implant side effects progress into complications, timely and appropriate treatment is essential to save the implant or manage the issue effectively.
For Infection
- Antibiotics: Often the first line of defense, targeting the bacteria causing the infection.
- Debridement/Surgical Cleaning: Removal of infected tissue, plaque, and calculus around the implant.
- Chlorhexidine Rinses: Antimicrobial rinses to reduce bacterial load.
- Implant Removal: In severe or persistent cases, especially if the infection is spreading or osseointegration never occurred, the implant may need to be removed, followed by a healing period and potentially a bone graft before re-implantation.
For Peri-implantitis
Treatment strategies depend on the stage of peri-implantitis.
- Non-Surgical: For early stages, this involves professional cleaning (debridement) of the implant surface, often using specialized tools, followed by local or systemic antibiotics.
- Surgical: For advanced peri-implantitis with significant bone loss:
- Flap Surgery: Lifting the gum tissue to thoroughly clean the implant surface and remove infected bone.
- Osseous Resection/Reshaping: Removing diseased bone and reshaping the remaining bone to create a healthier environment.
- Bone Regeneration: Using bone grafts and membranes to attempt to regenerate lost bone around the implant.
- Implant Surface Decontamination: Various methods (laser, chemical agents) to clean the implant surface.
- Implant Removal: If bone loss is extensive and the implant is mobile, removal is often the only option.
For Nerve Damage
- Observation: For mild, temporary numbness, observation and time may be sufficient as nerves can sometimes heal.
- Medication: Anti-inflammatory drugs or nerve-specific medications may be prescribed.
- Implant Removal: If the implant is directly impinging on a nerve and causing severe or persistent symptoms, immediate removal of the implant is often recommended to prevent permanent damage. Referral to an oral and maxillofacial surgeon specializing in nerve repair may be necessary.
For Sinus Perforation
- Conservative Management: Small perforations may heal spontaneously with antibiotics and nasal decongestants.
- Surgical Repair: Larger perforations or persistent sinus communication may require surgical repair of the sinus membrane, possibly with a bone graft, and removal of the implant.
- Sinus Lift Procedure: If an implant has perforated the sinus but is stable, a subsequent sinus lift may be performed to create more bone.
For Implant Failure (Lack of Osseointegration)
- Implant Removal: The failed implant must be removed.
- Site Management: The site is cleaned, and a healing period follows.
- Bone Grafting: Often, bone grafting is required to rebuild the bone volume lost during the initial failure and removal.
- Re-implantation: After adequate healing (typically 3-6 months post-graft), another implant can usually be placed. The success rate for re-implantation is high if the underlying cause of the initial failure is addressed.
For Component Fracture (Abutment or Crown)
- Replacement: Fractured abutments or crowns are typically replaced. This is usually straightforward unless the fracture extends into the implant body.
- Implant Fracture: If the implant post itself fractures, it usually requires removal of the fractured implant and often replacement with a new implant after a healing period.
Cost of Dental Implants and Managing Side Effect Costs
Understanding the financial investment in dental implants is crucial, especially when considering potential tooth implant side effects and their associated treatment costs. Prices vary significantly based on geographic location, complexity of the case, materials used, and the experience of the dental professional.
Average US Costs for Dental Implant Procedures
| Procedure Type | Average Low Range (USD) | Average Mid Range (USD) | Average High Range (USD) |
|---|---|---|---|
| Single Dental Implant | $3,000 | $4,500 | $6,000 |
| (Includes implant post, abutment, crown) | |||
| Full Arch Implants (All-on-4/6) per arch | $15,000 | $22,500 | $30,000 |
| Bone Graft (per site) | $200 | $1,000 | $3,000 |
| Tooth Extraction (simple) | $75 | $150 | $300 |
| Tooth Extraction (surgical) | $150 | $300 | $600 |
| 3D CT Scan | $100 | $250 | $500 |
- Geographic Variation: Costs can be significantly higher in major metropolitan areas (e.g., New York City, Los Angeles) compared to rural areas.
- Same Day Tooth Extraction and Implant: While saving time and appointments, this may slightly increase the initial cost of the implant procedure due to the added complexity and immediate provisional restoration. However, it combines two procedures into one fee, often resulting in overall savings compared to separate appointments for extraction, healing, and then implant placement.
Cost of Treating Complications
The cost to treat tooth implant side effects can range from minor adjustments to significant surgical interventions.
- Minor Complications (e.g., infection): May involve antibiotics ($20-$200) or debridement ($100-$500).
- Peri-implantitis Treatment: Non-surgical treatment can range from $300-$1,500 per implant, while surgical options (bone grafting, flap surgery) can range from $1,000-$4,000 per implant site.
- Implant Removal: $300-$800, plus costs for any subsequent bone grafting ($200-$3,000) and re-implantation ($3,000-$6,000).
- Nerve Damage/Sinus Repair: Can vary widely depending on complexity, from several hundred to several thousand dollars, potentially involving specialists.
Insurance Coverage
- Limited Coverage: Many dental insurance plans offer limited or no coverage for dental implants themselves, classifying them as a "major" or "cosmetic" procedure.
- Partial Coverage: Some plans may cover portions of the treatment, such as the initial consultation, X-rays, tooth extraction, bone grafting, or the crown itself. It is crucial to check with your insurance provider to understand your specific benefits.
- Medical Insurance: In rare cases, if the implant procedure is deemed medically necessary due to trauma or a medical condition, some medical insurance plans might offer partial coverage, but this is uncommon.
Payment Plans and Financing Options
- In-Office Payment Plans: Many dental offices offer flexible payment schedules.
- Third-Party Financing: Companies like CareCredit or LendingClub provide healthcare-specific credit options with various interest rates and repayment terms.
- Health Savings Accounts (HSAs) & Flexible Spending Accounts (FSAs): These tax-advantaged accounts allow you to save and pay for qualified medical and dental expenses with pre-tax dollars, significantly reducing your out-of-pocket costs.
- Dental Schools: University dental schools often provide services at a reduced cost, performed by students under the supervision of experienced faculty.
Prevention: Minimizing Your Risk of Tooth Implant Side Effects
Preventing complications is always better than treating them. Taking proactive steps can significantly reduce your risk of experiencing tooth implant side effects.
- Choose an Experienced Professional: Select an oral surgeon, periodontist, or general dentist with extensive training and experience in implant dentistry. Look for board certification and a strong track record of successful implant cases. Ask about their continuing education in implantology.
- Thorough Pre-Surgical Planning: Ensure your dental professional utilizes advanced diagnostic tools like 3D CBCT scans for precise surgical planning. This helps identify optimal implant placement locations and avoid vital anatomical structures.
- Disclose Full Medical History: Be completely transparent with your dentist about all medical conditions, medications (prescription, over-the-counter, supplements), allergies, and habits (smoking, alcohol use). This allows them to assess risks and tailor your treatment plan accordingly.
- Quit Smoking: If you smoke, quitting is the single most impactful step you can take to improve implant success rates and reduce the risk of infection and peri-implantitis.
- Control Systemic Diseases: If you have conditions like diabetes, ensure they are well-managed and under control before and after implant surgery.
- Follow Pre-Operative Instructions: Adhere strictly to any instructions given before surgery, such as taking prescribed antibiotics or avoiding certain medications.
- Diligent Post-Operative Care: Scrupulously follow all recovery and aftercare instructions provided by your dental professional regarding diet, oral hygiene, activity levels, and medication use. This is crucial for successful healing and osseointegration.
- Maintain Excellent Oral Hygiene: Once your implant is restored, commit to meticulous daily oral hygiene, including brushing twice a day, flossing, and using any recommended interdental cleaning tools.
- Regular Dental Check-ups: Attend all scheduled follow-up appointments and maintain regular professional dental cleanings (every 6 months, or as advised) to monitor implant health and prevent peri-implantitis.
- Manage Bruxism: If you grind or clench your teeth, wear a custom-fitted nightguard to protect your implant and surrounding structures from excessive force.
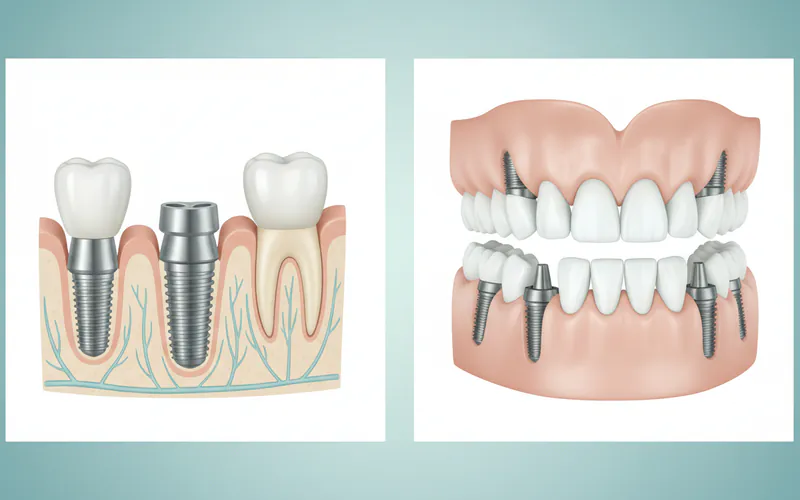
Comparison of Implant Options and Their Associated Risks
Understanding the nuances of different implant approaches can help you weigh the benefits against the potential risks, especially when considering more extensive procedures like full arch implants or the accelerated same day tooth extraction and implant process.
| Feature / Procedure Type | Standard Single Implant | Full Arch Implants (e.g., All-on-4/6) | Same Day Extraction & Implant Placement (Immediate Implant) |
|---|---|---|---|
| Purpose | Replaces a single missing tooth. | Replaces an entire arch of missing teeth with a fixed bridge on multiple implants. | Places an implant immediately after tooth extraction, often with a temporary crown. |
| Complexity | Moderate. Less invasive, usually one implant. | High. Involves multiple implants (4-6), often with angled placement, and a full bridge. | Moderate-High. Requires precise assessment of extraction site bone quality and stability. |
| Typical Timeline (Healing & Restoration) | 3-7 months (3-6 months osseointegration + 1 month for abutment/crown). | 4-8 months (if immediate load, temporary bridge same day, permanent in 4-6 months). | 3-7 months (immediate placement, 3-6 months osseointegration, then permanent crown). |
| Average Cost (USD) | $3,000 - $6,000 (per implant). | $15,000 - $30,000 (per arch, includes temporary/permanent prosthesis). | Often similar to single implant cost but may include extraction fee ($75-$600). |
| Common Side Effects | Pain, swelling, bruising, minor bleeding. | More extensive pain, swelling, bruising due to multiple implant sites. | Similar to standard implant, potentially slightly increased initial swelling/bleeding. |
| Potential Complications | Infection, nerve damage (lower jaw), sinus perforation (upper jaw), implant failure, peri-implantitis. | Higher risk of widespread infection if hygiene is poor. More significant nerve/sinus risk if planning is inadequate. Increased risk of non-integration if not good candidate. | Increased risk of early implant failure if primary stability is not achieved in extraction socket. Higher infection risk if site not perfectly clean. |
| Success Rate | >95% | >90-95% (highly dependent on patient selection and surgeon expertise). | >90% (slightly lower than conventional, but rising with technology). |
| Ideal Candidate | Good general health, adequate bone volume, good oral hygiene. | Good general health, moderate to severe tooth loss in an arch, sufficient bone volume (or candidates for grafting). | Good general health, healthy gums, sufficient bone around extraction site for immediate stability. |
Frequently Asked Questions
Is dental implant surgery painful?
Dental implant surgery is performed under local anesthesia, so you won't feel pain during the procedure. Many patients also opt for sedation dentistry for a more relaxed experience. Afterward, it's normal to experience mild to moderate pain and discomfort, which is usually manageable with prescribed or over-the-counter pain medication. This discomfort typically subsides within a few days.
How long do dental implant side effects last?
Minor side effects like pain, swelling, and bruising usually peak within 2-3 days post-surgery and gradually resolve over 7-10 days. Temporary numbness from anesthesia wears off within hours. If you experience persistent or worsening pain, swelling, or new numbness beyond this timeframe, it's crucial to contact your dentist, as it could indicate a more serious complication.
Can dental implants cause headaches or sinus problems?
While rare, dental implants can indirectly contribute to headaches if they lead to bite issues or jaw pain. For upper jaw implants, improper placement too close to or into the maxillary sinus can cause sinus problems like chronic congestion, pain, or infection (sinusitis). Thorough pre-surgical planning with 3D imaging helps prevent such complications.
What is the success rate of dental implants, despite potential side effects?
Dental implants boast an impressive success rate of over 95% when performed by experienced professionals and maintained with good oral hygiene. Even with the possibility of minor side effects and rare complications, their long-term reliability and benefits as a tooth replacement option far outweigh the risks for most patients.
Are full arch implants more prone to side effects?
Full arch implants involve more extensive surgery with multiple implants, which can lead to more significant initial swelling and bruising compared to a single implant. While the overall success rate remains high, the complexity means there's a slightly increased risk of complications like infection or nerve involvement if surgical planning isn't meticulous. However, for suitable candidates, the benefits are substantial.
What are the alternatives to dental implants?
Alternatives to dental implants include traditional dental bridges (which require altering adjacent healthy teeth), partial dentures (removable), and full dentures (removable). While these options can replace missing teeth, they do not offer the same stability, bone preservation benefits, or long-term durability as dental implants.
How do I know if my implant is failing?
Signs of a failing implant include persistent or worsening pain, swelling, or tenderness around the implant site, gum recession, a bad taste in your mouth, or most critically, any mobility or looseness of the implant itself. If you notice any of these symptoms, contact your dental professional immediately.
Can I get a dental implant the same day as an extraction?
Yes, same day tooth extraction and implant placement is a viable option for many patients. This technique, also known as immediate implant placement, can save time and reduce the number of surgical visits. However, it requires careful patient selection, excellent bone quality at the extraction site, and the absence of infection to ensure successful integration and minimize tooth implant side effects.
How much does it cost to fix a dental implant complication?
The cost to fix a complication varies widely depending on its nature and severity. Minor issues like treating an infection might cost a few hundred dollars for antibiotics and cleaning. More serious complications, such as treating peri-implantitis or removing and replacing a failed implant, can range from $1,000 to several thousand dollars, including potential bone grafting and specialist fees.
Can I be allergic to my dental implant?
Allergic reactions to dental implants made of titanium are extremely rare, as titanium is highly biocompatible. In very infrequent cases, a patient might exhibit sensitivity to titanium or other trace metals in the implant alloy, leading to inflammation or failure of osseointegration. If suspected, testing can be done, and alternative materials like zirconia implants might be considered.
When to See a Dentist
While minor post-operative symptoms are expected after dental implant surgery, it's crucial to know when to seek professional dental attention. Do not delay in contacting your dentist or oral surgeon if you experience any of the following:
-
Emergency Situations (Seek immediate attention):
- Uncontrolled Bleeding: Bleeding that doesn't subside after applying firm pressure with gauze for several hours, or heavy, continuous bleeding.
- Significant Swelling that Impairs Breathing or Swallowing: This is very rare but indicates a severe reaction or spreading infection.
- New or Worsening Numbness: If your initial numbness doesn't wear off, or if you develop new numbness, tingling, or pain in your lips, chin, or tongue days after surgery, especially if it's severe or spreading.
- Sudden, Severe Pain: Pain that is not relieved by prescribed medication and is significantly worse than expected.
-
Urgent Concerns (Contact your dentist promptly):
- Fever or Chills: A temperature above 100°F (37.8°C) or feeling unwell can indicate an infection.
- Pus or Foul Discharge: Any yellow, green, or bad-smelling discharge from the surgical site.
- Increasing Swelling: If swelling continues to increase after the third day, or if it spreads rapidly, rather than gradually diminishing.
- Implant Mobility: If your implant feels loose, wobbly, or moves when you touch it.
- Persistent Symptoms: Any pain, swelling, or discomfort that does not improve after a week, or seems to be worsening.
- Allergic Reaction Symptoms: Rash, hives, or severe itching.
- Unexpected Bite Changes: If your temporary or permanent crown feels high, uncomfortable, or changes your bite significantly.
For routine follow-up questions, mild discomfort, or general concerns, a scheduled appointment or phone consultation is appropriate. However, for any of the red-flag symptoms above, it's always best to err on the side of caution and contact your dental professional right away. Your dental team is your best resource for guidance and care throughout your implant journey.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
Implantologist: Complete Guide
Losing a tooth can be a significant setback, impacting not only your smile but also your ability to speak, chew, and maintain overall oral health. In fact, over 3 million Americans currently have dental implants, and that number is projected to grow significantly as more people seek a durable, n
March 8, 2026
Dentures Over Implants: Complete Guide
Missing multiple teeth or even an entire arch can profoundly impact your life, affecting everything from your ability to chew and speak to your self-confidence. For millions of Americans, traditional removable dentures have long been a solution, but they often come with compromises: slipping, discom
March 8, 2026
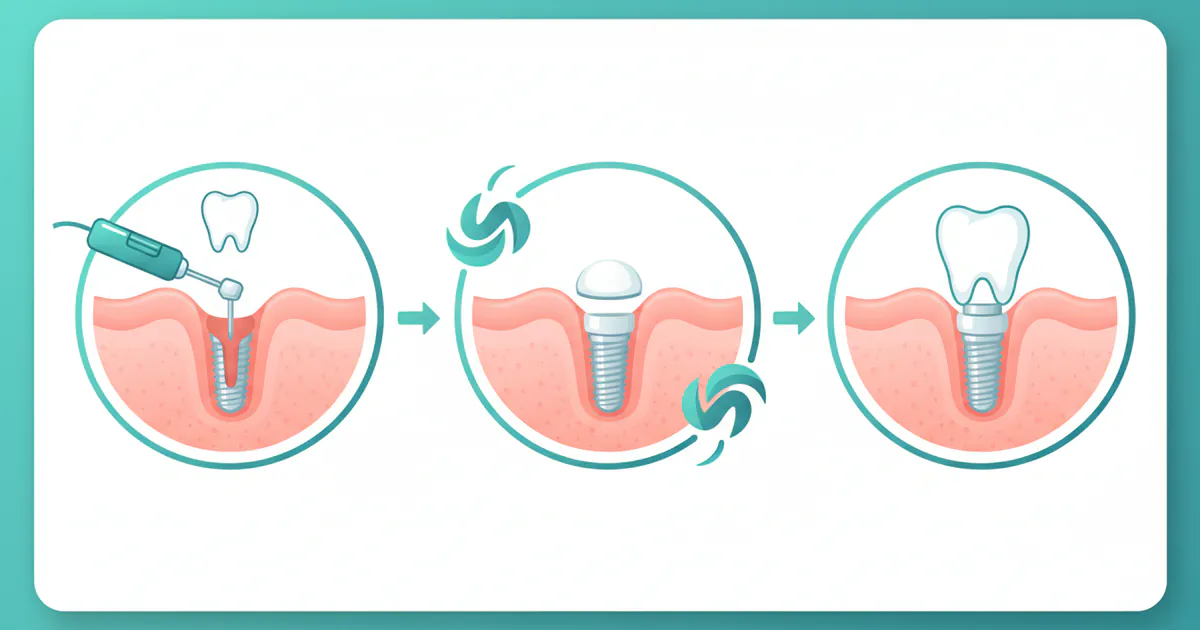
Implants Process: Complete Guide
Missing teeth can impact more than just your smile; they can affect your ability to eat, speak, and even your overall confidence. In fact, over 178 million Americans are missing at least one tooth, and about 40 million are missing all of their teeth. When faced with tooth loss, understanding the
March 8, 2026

Implants Dentaires: Complete Guide
Missing teeth can dramatically impact not just your smile, but your overall health, confidence, and quality of life. In the United States, an estimated 178 million adults are missing at least one tooth, while approximately 40 million are missing all their teeth. These statistics underscore a
March 8, 2026