Gingiva
5,290 words · 18 min read
Quick Definition
The gum tissue that surrounds and supports the teeth, covering the alveolar bone. Healthy gingiva is pink, firm, and stippled (textured like orange peel).
Gingiva: Your Gums – The Foundation of a Healthy Smile
Your smile is more than just teeth; it's a complex system, and at its heart lies the gingiva – more commonly known as your gums. This vital tissue forms a protective seal around your teeth, anchoring them firmly in your jawbone and shielding the sensitive roots from bacteria and trauma. Healthy gingiva is the bedrock of a healthy mouth, preventing issues ranging from discomfort to tooth loss. When people search "what is gingiva" or "gingiva dental," they are seeking to understand this often-overlooked but incredibly important component of their oral health.
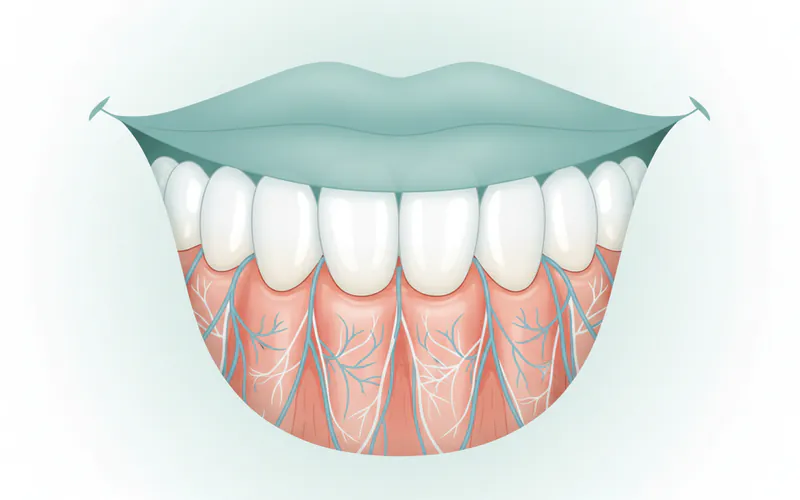
Ignoring the health of your gingiva can lead to serious consequences, including gingivitis (the early, reversible stage of gum inflammation) and periodontal disease (a more advanced, irreversible condition that affects the supporting structures of your teeth). These conditions, collectively referred to as gum disease, are incredibly common. According to the Centers for Disease Control and Prevention (CDC), nearly half of adults aged 30 years or older in the United States— 47.2%, or 64.7 million people—have some form of periodontal disease. This staggering statistic underscores the importance of understanding the gingiva, its role, and how to keep it healthy. This comprehensive guide from SmilePedia.net will be your definitive resource for everything you need to know about your gingiva.
Key Takeaways:
- Gingiva is your gum tissue, crucial for supporting teeth.
- Healthy gingiva is pink, firm, and stippled.
- It protects teeth roots and jawbone from bacteria.
- Poor oral hygiene can lead to gingivitis and periodontal disease.
- Nearly half of US adults over 30 have some form of gum disease.
- Regular dental care and proper home hygiene are essential for gingival health.
Detailed Explanation
Understanding the gingiva goes beyond its basic definition. Its structure, function, and susceptibility to various conditions are key to maintaining a healthy smile.
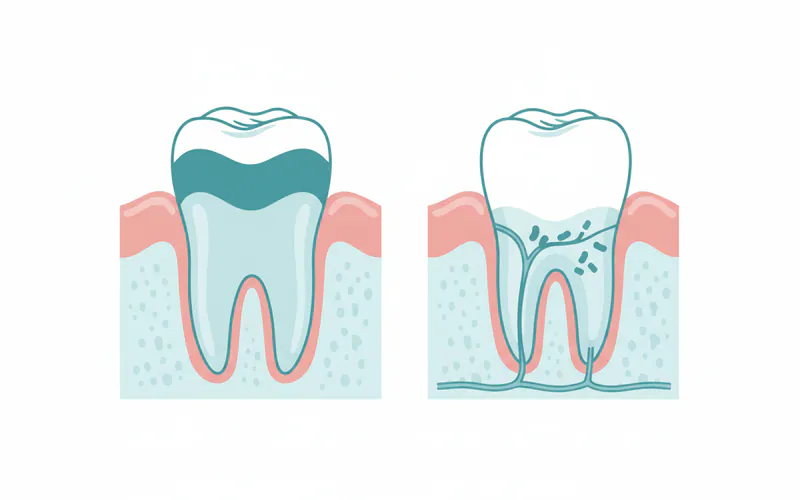
Types and Classifications of Gingiva
The gingiva isn't a single uniform tissue; it's comprised of different zones, each with unique characteristics and functions. These classifications are based on their location relative to the tooth and the jawbone.
-
Marginal Gingiva (Free Gingiva):
- This is the unattached, collar-like band of gum tissue that surrounds each tooth, extending from the free gingival margin to the attached gingiva.
- It typically has a smooth surface and is about 0.5 to 2 mm wide.
- The space between the marginal gingiva and the tooth surface is called the gingival sulcus (or gingival crevice). In a healthy mouth, this sulcus is shallow, typically 1-3 mm deep, and contains a small amount of gingival crevicular fluid. Deeper sulci indicate inflammation or disease.
- It is not bound to the underlying bone, allowing for flexibility during chewing and brushing.
-
Attached Gingiva:
- Located immediately below the marginal gingiva, this tissue is firmly bound to the underlying alveolar bone (the bone that holds your tooth roots) and the cementum (the outer layer of your tooth root).
- It is typically firm, resilient, and often has a stippled or "orange peel" texture due to the connective tissue fibers binding it down. This stippling is a key indicator of healthy gingiva.
- The width of the attached gingiva varies throughout the mouth, usually widest in the incisor regions and narrowest around the premolars. Its primary function is to provide a stable, immobile base for the free gingiva and to withstand the forces of chewing.
- A sufficient band of attached gingiva is crucial for preventing gum recession and protecting the tooth root.
-
Interdental Gingiva (Gingival Papilla):
- This is the gum tissue that fills the space between adjacent teeth, extending upwards from the attached gingiva.
- In the anterior (front) teeth, it's often pyramidal or knife-edged. In the posterior (back) teeth, it typically has a slightly flatter, "col" shape due to the broader contact points between molars.
- Its main role is to prevent food impaction between teeth and to protect the underlying bone from bacterial invasion. Healthy papillae are pointy and fill the entire space.
- Inflammation often causes the papillae to become swollen, rounded, and bleed easily.
-
Alveolar Mucosa:
- While not technically part of the gingiva, the alveolar mucosa is the thin, red, movable tissue that lies beyond the attached gingiva, covering the rest of the alveolar bone.
- It is distinct from the gingiva by its darker red color (due to a richer blood supply), smoother texture, and lack of stippling.
- The line where the attached gingiva meets the alveolar mucosa is called the mucogingival junction.
Healthy gingiva generally presents as light pink (though color can vary with ethnicity), has a firm and resilient consistency, and often exhibits a stippled appearance. The margins are thin and knife-edged, and the gingival sulcus is shallow with no bleeding upon gentle probing. Any deviation from these characteristics can be a sign of inflammation or disease.
Causes and Risk Factors for Gingival Problems
The primary cause of gingival inflammation and disease is the accumulation of bacterial plaque – a sticky, colorless film of bacteria that constantly forms on your teeth. However, several factors can increase your susceptibility and the severity of these conditions.
Primary Cause:
- Bacterial Plaque Biofilm: When plaque isn't effectively removed through brushing and flossing, the bacteria in it produce toxins that irritate the gingival tissue, leading to inflammation. If left undisturbed, plaque hardens into calculus (tartar), which can only be removed by a dental professional. Calculus provides a rough surface for more plaque to adhere, perpetuating the cycle of inflammation.
Modifiable Risk Factors:
- Poor Oral Hygiene: Inconsistent or ineffective brushing and flossing allow plaque to accumulate, directly leading to gingivitis. This is the most significant and easily controlled risk factor.
- Smoking and Tobacco Use: Tobacco is one of the most significant risk factors for developing severe gum disease. Smokers are two to six times more likely to develop periodontal disease than non-smokers. Smoking impairs the immune system, reduces blood flow to the gums, and hinders healing, masking the typical signs of gum disease like bleeding.
- Diabetes: Individuals with uncontrolled diabetes are at a significantly higher risk for gum disease because high blood sugar levels impair the body's ability to fight infection and heal. Gum disease, in turn, can make it harder to control blood sugar.
- Hormonal Changes: Fluctuations during puberty, pregnancy, menstruation, and menopause can make the gingiva more sensitive and susceptible to inflammation. "Pregnancy gingivitis" affects 60-75% of pregnant women due to increased hormone levels.
- Certain Medications: Some drugs, such as anticonvulsants (e.g., phenytoin), immunosuppressants (e.g., cyclosporine), and calcium channel blockers (e.g., nifedipine), can cause gingival enlargement (overgrowth of gum tissue), making plaque removal difficult and increasing the risk of inflammation.
- Nutritional Deficiencies: A diet lacking essential nutrients, particularly Vitamin C, can weaken the immune system and impair gum tissue health. While rare in developed countries, severe Vitamin C deficiency can lead to scurvy, a condition characterized by severely bleeding gums.
- Stress: Chronic stress can weaken the immune system, making the body less capable of fighting off bacterial infections, including those in the gums.
- Ill-fitting Dental Restorations: Crowns, fillings, or bridges that have rough edges or don't fit properly can trap plaque and irritate the gingiva.
- Crowded or Misaligned Teeth: Teeth that are difficult to clean due to their position can lead to plaque accumulation and localized gingival inflammation.
- Mouth Breathing: Can dry out the gingival tissues, making them more prone to inflammation, particularly in the anterior region.
Non-modifiable Risk Factors:
- Genetics: Some individuals are genetically predisposed to developing gum disease, making them more vulnerable even with good oral hygiene.
- Age: The risk of developing more severe forms of gum disease increases with age.
Signs and Symptoms to Watch For
Recognizing the early warning signs of gingival problems is crucial for timely intervention and preventing the progression to more severe conditions.
- Bleeding Gums: This is often the first and most common sign of gingivitis. Healthy gums should not bleed, even with vigorous brushing or flossing. Bleeding can occur when brushing, flossing, or even spontaneously.
- Red, Swollen, or Tender Gums: Healthy gingiva is typically pink and firm. Inflamed gums appear darker red or purplish, are visibly swollen, and may feel soft or spongy to the touch. They might also be tender or painful when touched or during chewing.
- Receding Gums: The gum tissue pulls away from the teeth, making the teeth appear longer. This exposes the root surfaces, which can lead to sensitivity to hot, cold, or sweet stimuli, and increased vulnerability to root decay.
- Persistent Bad Breath (Halitosis): While bad breath can have various causes, persistent halitosis, especially when accompanied by other gum symptoms, is often a sign of bacterial accumulation and infection in the gums.
- Pus Between Teeth and Gums: A clear sign of active infection, pus indicates that bacteria are actively proliferating and the body is trying to fight them off.
- Loose or Shifting Teeth: This is a sign of more advanced periodontal disease, where the supporting bone around the teeth has been significantly damaged. Teeth may feel unstable, shift out of alignment, or become sensitive.
- Changes in Your Bite: As teeth shift or become loose, your bite might feel "off" or uncomfortable.
- New Spaces Developing Between Your Teeth: Shifting teeth can create gaps where none existed before.
Diagnosis Process — What Your Dentist Does
Diagnosing gingival conditions requires a thorough examination by a dental professional. Your dentist will combine visual assessment with specific diagnostic tools.
- Medical and Dental History Review: Your dentist will ask about your overall health, medications, smoking habits, and any symptoms you've noticed. This helps identify risk factors and potential systemic links to gum disease.
- Visual Examination:
- Color, Contour, Consistency: The dentist will visually assess the color of your gingiva (looking for redness or purple discoloration), its contour (swollen, blunted papillae instead of knife-edged), and its consistency (soft, spongy instead of firm).
- Stippling: The presence or absence of the healthy "orange peel" stippling is noted.
- Bleeding: Spontaneous bleeding or bleeding upon gentle manipulation.
- Recession: Measurement of any gum recession.
- Periodontal Probing: This is a critical diagnostic step. A small, sterile ruler-like instrument called a periodontal probe is gently inserted into the gingival sulcus (the space between the tooth and gum).
- Pocket Depth Measurement: The depth of the sulcus is measured at multiple points around each tooth. Healthy sulci are typically 1-3 millimeters (mm) deep. Depths greater than 3 mm usually indicate a periodontal pocket, meaning the gum has detached from the tooth due to inflammation and bone loss.
- Bleeding on Probing (BOP): The dentist notes if the gums bleed after probing. Bleeding on probing is a strong indicator of inflammation and active disease.
- Furcation Involvement: In multi-rooted teeth, the probe is used to check for bone loss in the area where the roots diverge.
- Mobility: Your dentist will check if any teeth are loose.
- Dental X-rays (Radiographs): X-rays are essential for assessing the bone supporting your teeth.
- Bone Loss Assessment: They reveal the presence and extent of alveolar bone loss, which is characteristic of periodontal disease. Gingivitis typically does not involve bone loss, making X-rays particularly useful for differentiating between gingivitis and periodontitis.
- Calculus Detection: X-rays can also show the presence of large calculus deposits below the gum line.
- Plaque and Calculus Assessment: The dentist will evaluate the amount of plaque and calculus present on your teeth.
Based on these findings, your dentist will diagnose the condition, classify its severity (e.g., mild, moderate, or severe gingivitis; early, moderate, or advanced periodontitis), and develop a tailored treatment plan.
Treatment Options with Pros, Cons, and Costs
Treatment for gingival problems varies significantly depending on whether it's early-stage gingivitis or more advanced periodontal disease. The goal is always to remove the source of inflammation (bacterial plaque and calculus) and halt disease progression.
Treatment for Gingivitis (Reversible Stage):
-
Professional Dental Cleaning (Prophylaxis):
- What it is: A routine cleaning where the dental hygienist removes plaque and calculus from above and slightly below the gum line using scaling instruments (manual or ultrasonic) and then polishes the teeth.
- Pros: Highly effective in reversing gingivitis, non-invasive, relatively quick.
- Cons: Requires consistent home care afterward and regular follow-up appointments. Not sufficient for periodontitis.
- Typical Cost (US): $75 - $200 (without insurance). Often fully or partially covered by dental insurance.
-
Improved Home Oral Hygiene:
- What it is: Diligent brushing twice a day with a soft-bristled brush, flossing daily, and potentially using an antiseptic mouthwash as recommended by your dentist.
- Pros: Essential for preventing and managing gingivitis; cost-effective.
- Cons: Requires patient commitment and proper technique.
- Typical Cost (US): Cost of toothbrush, floss, toothpaste, mouthwash – minimal ongoing expense.
Treatment for Periodontal Disease (Irreversible Stage):
These treatments aim to control the infection, prevent further bone loss, and, in some cases, regenerate lost tissue.
-
Scaling and Root Planing (SRP) / "Deep Cleaning":
- What it is: A non-surgical procedure performed under local anesthesia. Scaling involves thoroughly removing plaque and calculus from above and below the gum line, down to the bottom of the periodontal pockets. Root planing then smooths the root surfaces to remove bacterial toxins and prevent future plaque adhesion. Often done in quadrants (one quarter of the mouth at a time).
- Pros: Can effectively halt the progression of early to moderate periodontitis; less invasive than surgery.
- Cons: May cause temporary discomfort, sensitivity, and mild gum soreness. Requires multiple appointments. Not always sufficient for advanced cases.
- Typical Cost (US): $200 - $600 per quadrant (without insurance). Often covered partially by insurance, considered a "basic" or "major" service depending on the plan.
-
Antibiotics (Topical or Oral):
- What it is: Can be used in conjunction with SRP. Topical antibiotics (e.g., antibiotic gels or chips placed directly into pockets) or oral antibiotics (e.g., doxycycline) are prescribed to control bacterial infection.
- Pros: Directly targets bacteria; can reduce pocket depth and inflammation.
- Cons: Potential for side effects (e.g., gastrointestinal upset, yeast infections), risk of antibiotic resistance with overuse. Not a standalone treatment.
- Typical Cost (US): Topical gels $30 - $100 per site; Oral antibiotics $20 - $100+ (without insurance).
-
Surgical Interventions (Performed by a Periodontist):
- What it is: Recommended for moderate to severe periodontitis when non-surgical treatments are insufficient.
- Flap Surgery / Pocket Reduction Surgery: The gums are lifted back to allow direct access to clean roots and reshape the bone. The gums are then sutured back. This reduces pocket depth, making them easier to clean.
- Bone Grafting: If bone has been destroyed, a bone graft (using synthetic bone, donated bone, or your own bone) can be placed to stimulate new bone growth.
- Soft Tissue Grafts (Gum Grafts): Used to treat gum recession, cover exposed roots, and reinforce thin gum tissue. A small piece of tissue is taken from the roof of your mouth or a donor source and attached to the recession site.
- Guided Tissue Regeneration (GTR): A small piece of mesh-like material is inserted between the bone and gum tissue to encourage the regeneration of bone and connective tissue.
- Pros: Can halt severe disease, regenerate lost tissue, save teeth that might otherwise be lost, reduce sensitivity from exposed roots.
- Cons: More invasive, longer recovery time, potential for pain and swelling, higher cost.
- Typical Cost (US) (without insurance):
- Flap Surgery: $1,000 - $3,000+ per quadrant
- Bone Graft: $500 - $3,000+ per site
- Soft Tissue Graft: $600 - $1,200+ per tooth
- Guided Tissue Regeneration: $500 - $2,000+ per site
- These procedures are typically considered "major" and may have lower insurance coverage (e.g., 50%).
- What it is: Recommended for moderate to severe periodontitis when non-surgical treatments are insufficient.
-
Laser Therapy:
- What it is: Uses lasers to remove inflamed gum tissue and bacterial deposits. Specific protocols like LANAP (Laser Assisted New Attachment Procedure) exist.
- Pros: Often less invasive, faster healing, reduced bleeding and discomfort compared to traditional surgery.
- Cons: Not all dentists offer it; long-term efficacy compared to traditional surgery is still a topic of research and debate among specialists. Can be expensive.
- Typical Cost (US): $500 - $2,000+ per quadrant/site.
Table: Comparison of Common Gingival Treatments
| Treatment | Target Condition | Invasiveness | Typical Cost (US, w/o insurance) | Recovery Time | Key Benefit |
|---|---|---|---|---|---|
| Professional Cleaning | Gingivitis | Minimal | $75 - $200 | Immediate | Reverses gingivitis, prevents progression |
| Scaling & Root Planing | Mild-Moderate Periodontitis | Moderate (non-surgical) | $200 - $600/quadrant | Few days (sensitivity) | Halts periodontitis, reduces pocket depths |
| Flap Surgery | Moderate-Severe Periodontitis | High (surgical) | $1,000 - $3,000+/quadrant | 1-2 weeks | Reduces deep pockets, allows access for cleaning |
| Soft Tissue Graft | Gum Recession | High (surgical) | $600 - $1,200+/tooth | 1-2 weeks | Covers exposed roots, reduces sensitivity |
| Bone Grafting | Bone Loss | High (surgical) | $500 - $3,000+/site | Weeks-months | Regenerates lost bone, stabilizes teeth |
Step-by-Step: What to Expect During Treatment
Knowing what to expect can help ease anxiety about dental procedures.
-
Professional Cleaning (Prophylaxis):
- Examination: The hygienist will first examine your gums and teeth for any issues.
- Scaling: Using ultrasonic scalers and/or hand instruments, they will gently remove plaque and calculus from tooth surfaces above and just below the gum line.
- Polishing: A rotating brush with gritty paste polishes the teeth, removing surface stains and making them smooth.
- Flossing: The hygienist will floss between your teeth to ensure all areas are clean.
- Rinse: You'll rinse with water or an antiseptic mouthwash.
- Fluoride (Optional): A fluoride treatment may be applied to strengthen enamel.
- Duration: Typically 30-60 minutes.
-
Scaling and Root Planing (SRP):
- Numbing: Local anesthetic will be administered to numb the specific area being treated, ensuring comfort.
- Scaling: The hygienist or periodontist will meticulously remove plaque and calculus from deep inside the periodontal pockets, all the way down to the root surface.
- Root Planing: They will then use specialized instruments to smooth the root surfaces, removing bacterial toxins and making it harder for bacteria to reattach.
- Rinsing: You'll periodically rinse your mouth.
- Post-op Instructions: Detailed instructions will be given for post-procedure care, including managing sensitivity and pain.
- Duration: Each quadrant typically takes 45-90 minutes. A full mouth SRP may require 2-4 appointments.
-
Gum Surgery (e.g., Flap Surgery or Grafting):
- Anesthesia: Local anesthetic is used to numb the area completely. Sedation options (oral, IV) may also be offered for comfort.
- Incision/Lifting: For flap surgery, the periodontist makes small incisions to gently lift the gum tissue away from the teeth and bone. For grafting, the donor tissue is harvested (if applicable) and prepared.
- Cleaning/Reshaping/Placement: For flap surgery, the roots are thoroughly cleaned, and bone may be reshaped. For grafts, the tissue is carefully placed and secured.
- Suturing: The gum tissue is repositioned and secured with tiny sutures (stitches). Periodontal dressings might be applied for protection.
- Post-op Instructions: Extensive instructions are provided for pain management, diet, oral hygiene, and follow-up care.
- Duration: Varies greatly from 30 minutes to several hours depending on the complexity and number of sites.
Recovery Timeline and Aftercare
Recovery varies depending on the treatment intensity.
-
Professional Cleaning: No real recovery time. You can resume normal activities immediately. You might experience a temporary feeling of "cleanliness" or slight sensitivity.
-
Scaling and Root Planing:
- Immediate: Numbness will wear off in a few hours.
- First few days: Expect some mild discomfort, tenderness, and sensitivity to hot/cold. Gums may appear slightly swollen or receded. Over-the-counter pain relievers can help.
- Diet: Stick to soft foods for a few days to avoid irritating the gums.
- Oral Hygiene: Continue brushing gently and avoid flossing the treated areas for a day or two as instructed. You may be advised to use a prescription antimicrobial mouth rinse.
- Full Recovery: Gums typically heal within 1-2 weeks, becoming firmer and less inflamed.
- Follow-up: A follow-up visit is crucial to check healing and measure pocket depths. Long-term periodontal maintenance cleanings (typically every 3-4 months) are essential.
-
Gum Surgery:
- Immediate: Numbness, bleeding from the surgical site (can be controlled with gauze), swelling, and discomfort are common.
- First week: Pain medication (prescription or OTC) will be needed. Swelling usually peaks within 2-3 days and gradually subsides. A soft-food diet is critical. Avoid strenuous activity.
- Oral Hygiene: You'll be given specific instructions on how to clean the area gently (e.g., with a soft toothbrush or prescription rinse) while avoiding brushing directly on the sutures.
- Suture Removal: Sutures are typically removed in 1-2 weeks.
- Full Healing: Soft tissue healing takes 2-4 weeks. Bone regeneration, if applicable, can take several months.
- Follow-up: Multiple follow-up appointments are scheduled to monitor healing and ensure proper recovery. Adherence to a strict periodontal maintenance schedule is vital.
Prevention Strategies
Preventing gingival problems is largely within your control and relies on consistent, effective oral hygiene and healthy lifestyle choices.
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes each time, covering all surfaces of your teeth and gently along the gum line.
- Floss Daily: Flossing removes plaque and food particles from between your teeth and under the gum line, where your toothbrush can't reach. This is arguably the most critical step for preventing gingivitis.
- Regular Dental Check-ups and Cleanings: Visit your dentist or dental hygienist every six months for professional cleanings and examinations. They can remove calculus that you can't remove at home and detect early signs of problems. For those with a history of gum disease, more frequent visits (e.g., every 3-4 months) may be necessary for periodontal maintenance.
- Use an Antiseptic Mouthwash: Your dentist may recommend a therapeutic mouthwash (containing ingredients like chlorhexidine or essential oils) to help reduce plaque and gingivitis, especially if you're prone to gum issues. This is an adjunct, not a replacement for brushing and flossing.
- Eat a Healthy, Balanced Diet: Limit sugary foods and drinks that feed harmful bacteria. A diet rich in vitamins (especially Vitamin C) and minerals supports overall oral and systemic health.
- Quit Smoking and Avoid Tobacco Products: This is one of the most impactful steps you can take for your gum health and overall well-being.
- Manage Systemic Health Conditions: If you have conditions like diabetes, ensure they are well-controlled, as they significantly impact your gum health.
- Address Misaligned Teeth or Ill-fitting Restorations: If you have crowded teeth or dental work that traps food, discuss options with your dentist.
Cost Ranges in the US (with/without Insurance)
The cost of gingival treatment in the US can vary significantly based on the severity of the condition, the type of procedure, the dental professional's fees, geographic location, and whether you have dental insurance.
-
Routine Professional Cleaning (Prophylaxis):
- Without Insurance: $75 - $200
- With Insurance: Often covered at 80-100%, so your out-of-pocket might be $0 - $40. Most plans cover two cleanings per year.
-
Scaling and Root Planing (SRP):
- Without Insurance: $200 - $600 per quadrant (a full mouth deep cleaning could be $800 - $2,400+).
- With Insurance: Often covered at 50-80% as a "basic" or "major" service. Your out-of-pocket could range from $100 - $300 per quadrant. Many plans have a waiting period for this coverage.
-
Periodontal Maintenance Cleaning (After SRP):
- Without Insurance: $100 - $300
- With Insurance: Coverage varies, often similar to a regular cleaning or slightly higher. May require a separate co-pay.
-
Gum Grafting (Soft Tissue Graft):
- Without Insurance: $600 - $1,200+ per tooth.
- With Insurance: Typically considered a "major" procedure, often covered at 50%. Your out-of-pocket could be $300 - $600+ per tooth. Many plans have an annual maximum benefit, which this procedure can quickly exceed.
-
Bone Grafting:
- Without Insurance: $500 - $3,000+ per site, depending on material and complexity.
- With Insurance: Similar to gum grafting, usually 50% coverage, making your out-of-pocket $250 - $1,500+ per site.
-
Flap Surgery / Pocket Reduction Surgery:
- Without Insurance: $1,000 - $3,000+ per quadrant.
- With Insurance: Often 50% coverage. Your out-of-pocket could be $500 - $1,500+ per quadrant.
Important Considerations:
- Specialist Fees: Procedures performed by a periodontist (gum specialist) may have higher fees than a general dentist.
- Geographic Location: Costs can vary by city and state.
- Annual Maximums: Most dental insurance plans have an annual maximum benefit (e.g., $1,000 - $2,000 per year). Extensive periodontal treatment can quickly exceed this.
- Waiting Periods: Many insurance plans have waiting periods (e.g., 6-12 months) for major procedures like deep cleanings or surgery.
- Payment Plans: Many dental offices offer payment plans or work with third-party financing (e.g., CareCredit) to help manage costs.
For Parents / Pediatric Considerations
Gingival health is important from a young age. While severe periodontal disease is rare in children, gingivitis is quite common.
- Gingivitis in Children and Teens: Just like adults, children can develop gingivitis due to plaque accumulation. Puberty can intensify the inflammatory response due to hormonal changes, leading to puberty gingivitis. Orthodontic appliances (braces) can also make it harder to clean teeth effectively, increasing the risk of gingivitis.
- Importance of Early Habits: Instilling good oral hygiene habits from infancy (wiping gums, then brushing with fluoride toothpaste as soon as teeth erupt) is crucial for lifelong gingival health.
- Teething Gingivitis: While not true gingivitis, the eruption of teeth can cause temporary inflammation and tenderness of the gum tissue in infants.
- Monitoring by Pediatric Dentists: Regular check-ups with a pediatric dentist are essential to monitor gingival health, provide preventive care, and address any issues early. They can also educate parents and children on proper brushing and flossing techniques.
- Aggressive Periodontitis: In rare cases, some children and adolescents can develop aggressive forms of periodontitis, often linked to genetic factors or specific bacterial infections. Early diagnosis and treatment are critical for these conditions.
Frequently Asked Questions
Is gingivitis painful?
In its early stages, gingivitis is usually not painful. This lack of pain is often why people may not realize they have it. The primary symptom is often bleeding gums during brushing or flossing. As it progresses, it can cause tenderness, swelling, and discomfort, especially during eating or touching the gums. If gingivitis advances to periodontitis, pain can become more noticeable due to deeper infection, abscess formation, or loose teeth.

How long does it take to cure gingivitis?
With proper professional treatment (a thorough dental cleaning) and diligent home oral hygiene, gingivitis is reversible. Gums can return to a healthy state within a few days to weeks. Consistent brushing and flossing daily, along with regular dental check-ups, are key to maintaining that healthy state and preventing recurrence.
Can gingiva grow back after recession?
Unfortunately, once gingiva has receded and supporting bone is lost, it cannot grow back naturally. The lost gum tissue is gone for good. However, gum graft surgery (soft tissue grafting) can be performed by a periodontist to cover exposed root surfaces, reduce sensitivity, improve aesthetics, and protect the tooth from further recession and decay.
Is gum disease contagious?
While the bacteria that cause gum disease can be transferred through saliva (e.g., sharing utensils, kissing), gum disease itself is not considered contagious in the same way a cold or flu is. Developing gum disease depends on an individual's immune response, genetics, oral hygiene habits, and other risk factors. Simply receiving the bacteria from someone else doesn't guarantee you'll develop the disease, though it can increase your risk.
What are the alternatives to gum surgery?
For early to moderate periodontal disease, alternatives to surgery include scaling and root planing (deep cleaning), which thoroughly cleans the root surfaces. Adjunctive therapies like local or systemic antibiotics can also be used. Laser therapy (e.g., LANAP) is a less invasive surgical alternative for some patients. However, for severe, advanced periodontitis with significant bone loss or deep pockets, surgery may be the most effective, or only, option to save teeth and preserve oral health.
Will insurance cover gum disease treatment?
Most dental insurance plans do offer some coverage for gum disease treatment, but the extent of coverage varies significantly.
- Routine Cleanings (Prophylaxis): Usually covered at 80-100%.
- Scaling and Root Planing (SRP): Often covered as a "basic" or "major" service at 50-80%.
- Surgical Procedures (Grafts, Flap Surgery): Typically considered "major" procedures and are often covered at 50%. It's important to check your specific plan's benefits, annual maximums, and any waiting periods, as extensive treatment can quickly exceed coverage limits.
What's the difference between gingivitis and periodontitis?
Gingivitis is the early, mildest form of gum disease, characterized by inflamed, red, swollen gums that may bleed. It's caused solely by plaque accumulation and is reversible with good oral hygiene and professional cleaning. Crucially, it does not involve bone loss. Periodontitis is an advanced, more severe form of gum disease. It develops if gingivitis is left untreated. In periodontitis, the inflammation spreads to the supporting structures of the teeth, leading to the destruction of the periodontal ligament and irreversible bone loss. This results in the formation of periodontal pockets, gum recession, loose teeth, and eventually, tooth loss. Periodontitis is manageable but not curable in the sense of reversing lost bone.
Can smoking affect my gingiva?
Absolutely, smoking is a major risk factor for gum disease. Smokers are significantly more likely to develop both gingivitis and periodontitis, and their disease tends to be more severe and harder to treat. Smoking impairs the immune system, reduces blood flow to the gums, and can mask the classic symptom of bleeding, making it harder to detect issues early. It also hinders healing after treatment. Quitting smoking is one of the most impactful steps you can take for your gingival health.
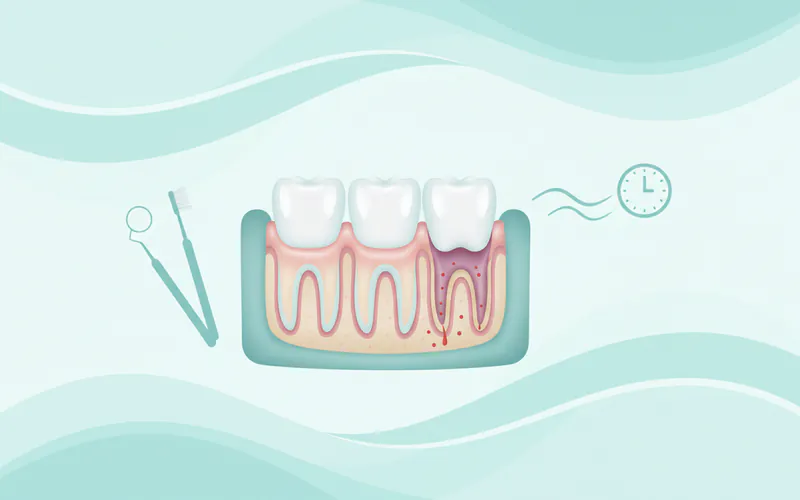
When to See a Dentist
Your gingiva is a crucial indicator of your oral and overall health. Don't wait for pain to prompt a dental visit.
-
Routine Care: Schedule regular dental check-ups and cleanings every six months. These visits are vital for preventing gingival problems and catching early signs before they become severe. For individuals with a history of gum disease, more frequent periodontal maintenance visits (e.g., every 3-4 months) are often recommended.
-
Early Signs of Trouble: See your dentist if you notice any of the following:
- Bleeding gums during brushing or flossing, even if it's minor.
- Gums that are red, swollen, or tender.
- Persistent bad breath.
- Any changes in the color or texture of your gingiva.
-
Urgent Care: Contact your dentist immediately if you experience:
- Persistent pain in your gums or teeth.
- Visible pus between your teeth and gums.
- Significantly receding gums or increased tooth sensitivity.
- Teeth that feel loose or shifting.
- Any sudden or severe swelling in your gums or face.
Addressing gingival concerns promptly is the best way to prevent the progression of gum disease, preserve your natural teeth, and maintain a healthy, confident smile for life.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.