Gingivitis
4,935 words · 16 min read
Quick Definition
The mildest form of gum disease, characterized by inflammation of the gums caused by plaque buildup. Gingivitis is reversible with proper oral hygiene and professional cleaning.
Gingivitis: Your Definitive Guide to Understanding and Treating Early Gum Disease
Welcome to SmilePedia.net, your trusted resource for comprehensive dental health information. This in-depth article is designed to be the definitive guide for anyone asking "what is gingivitis" or searching for "gingivitis dental." Here, we'll demystify this common condition, explain its causes, symptoms, and most importantly, how to prevent and reverse it.
Introduction
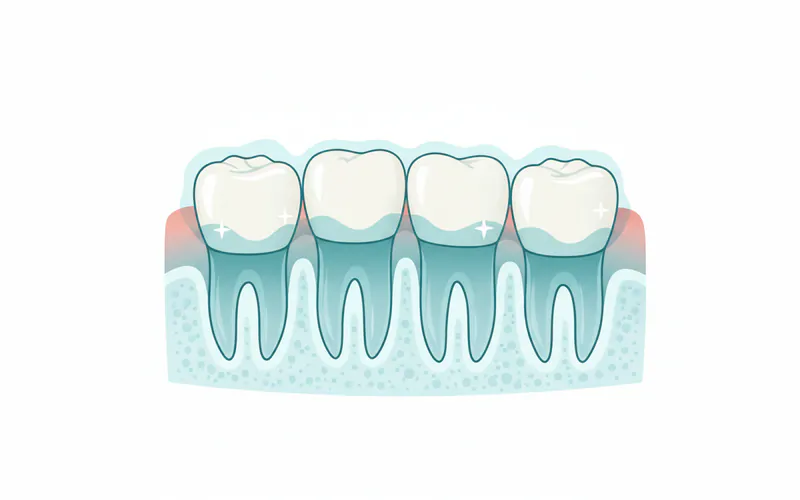
Gingivitis represents the mildest and most common form of gum disease, a term that encompasses a range of inflammatory conditions affecting the tissues supporting your teeth. Specifically, gingivitis is characterized by inflammation of the gums (gingiva), primarily caused by the accumulation of plaque – a sticky film of bacteria – along the gumline.
While gingivitis might seem minor, it's a critical indicator of your oral health. It's the body's early warning system, signaling that your gums are under attack from bacterial overgrowth. The good news is that gingivitis is fully reversible with proper oral hygiene and professional dental care. Ignoring it, however, allows the condition to progress to more severe forms of periodontal disease, which can lead to irreversible bone loss and even tooth loss.
This condition is incredibly prevalent. According to the Centers for Disease Control and Prevention (CDC), nearly half of all American adults aged 30 or older (47.2%) show signs of periodontal disease, with gingivitis being the initial stage for many. This translates to over 64 million adults in the United States. It can affect people of all ages, from children to seniors, emphasizing the universal importance of understanding and addressing gingivitis promptly.
Key Takeaways:
- Gingivitis is the mildest and most common form of gum disease.
- It's caused primarily by plaque buildup along the gumline.
- Symptoms include red, swollen, and bleeding gums.
- Gingivitis is reversible with professional cleaning and improved oral hygiene.
- If left untreated, it can progress to more serious periodontal disease, leading to irreversible damage.
- Regular dental check-ups and cleanings are crucial for prevention and early detection.
Detailed Explanation
Types and Classifications of Gingivitis
While the overarching cause of gingivitis is plaque, different factors can influence its presentation or severity. Understanding these classifications helps dental professionals tailor treatment.
-
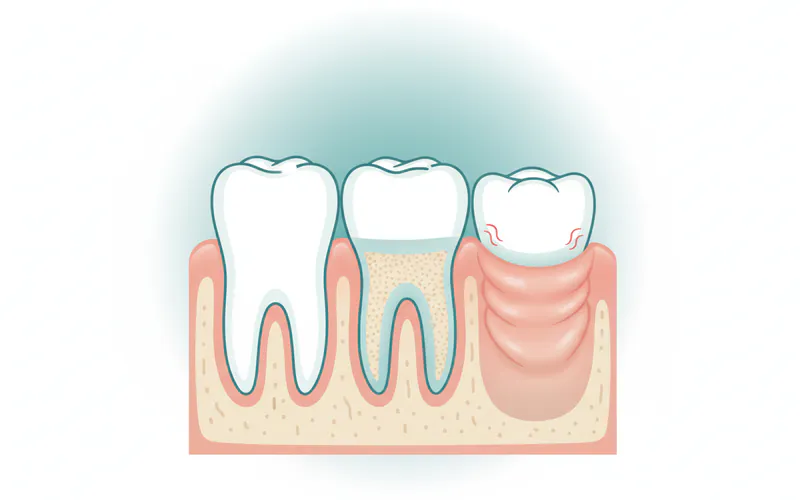
Plaque-Induced Gingivitis:
- This is by far the most common form and what most people refer to when they say "gingivitis." It's directly caused by the accumulation of dental plaque, a biofilm of bacteria that constantly forms on your teeth. When this plaque isn't adequately removed through daily brushing and flossing, the bacteria release toxins that irritate the gum tissue, leading to inflammation.
- Modifying factors can exacerbate plaque-induced gingivitis, even with similar amounts of plaque. These include:
- Systemic factors: Hormonal changes (e.g., during puberty, pregnancy, menstruation, or menopause), diabetes, certain blood disorders, and compromised immune systems can make gums more susceptible to inflammation.
- Medications: Some drugs can cause gingival enlargement (overgrowth of gum tissue), making plaque removal more difficult and increasing inflammation. Examples include anticonvulsants (like phenytoin), calcium channel blockers (like nifedipine), and immunosuppressants (like cyclosporine).
- Malnutrition: Severe vitamin deficiencies, particularly Vitamin C, can impact gum health (e.g., scurvy-related gingivitis).
- Local factors: Ill-fitting dental restorations (fillings, crowns) with rough or overhanging margins can trap plaque, making it harder to clean and contributing to localized gingivitis. Dry mouth (xerostomia) reduces saliva's natural cleansing action, increasing plaque accumulation.
-
Non-Plaque-Induced Gingivitis:
- This less common category refers to gingivitis that is not primarily caused by plaque but by other specific factors. While plaque may still be present and contribute, it's not the sole or primary instigator. These forms often require a different diagnostic approach and targeted treatment.
- Specific Bacterial, Viral, or Fungal Infections: Conditions like streptococcal gingivitis, primary herpetic gingivostomatitis (caused by the herpes simplex virus), or candidiasis (a fungal infection) can cause gum inflammation.
- Genetic/Developmental Disorders: Some rare genetic conditions can manifest with gingival signs.
- Specific Conditions of Systemic Origin: Inflammatory and immune conditions like lichen planus, pemphigoid, or lupus can affect gum tissue. Allergic reactions to dental materials (e.g., metal, acrylic, toothpaste ingredients) can also cause localized gingivitis.
- Traumatic Lesions: Physical injury to the gums, such as from aggressive brushing or chemical exposure, can cause inflammation.
For the vast majority of individuals, the focus will be on understanding and addressing plaque-induced gingivitis, as it is highly preventable and treatable through good oral hygiene and routine dental care.
Causes and Risk Factors
The primary culprit behind gingivitis is dental plaque, a colorless, sticky film of bacteria that constantly forms on the surface of your teeth. If plaque is not removed daily through brushing and flossing, it can harden into calculus (also known as tartar). Calculus is rough and porous, providing an ideal surface for more plaque to adhere and making it much harder to remove with a toothbrush alone.
Here’s a breakdown of the key causes and risk factors:
- Poor Oral Hygiene: This is the leading cause. Inadequate or infrequent brushing and flossing allow plaque to accumulate along the gumline, leading to bacterial growth and inflammation.
- Plaque and Calculus Buildup: As mentioned, plaque that isn't removed hardens into calculus, which irritates the gums and serves as a breeding ground for more bacteria.
- Smoking and Tobacco Use: Tobacco use, in any form, is a significant risk factor for gum disease. It impairs blood flow to the gums, reduces the effectiveness of the immune system, and interferes with the healing process. Smokers are twice as likely to have gum disease as non-smokers.
- Hormonal Changes: Fluctuations in hormones can make gums more sensitive and prone to inflammation. This is commonly observed during:
- Puberty: Increased hormone levels.
- Pregnancy: "Pregnancy gingivitis" affects 60-75% of pregnant women due to hormonal surges (estrogen and progesterone), which increase blood flow to the gums and make them more reactive to plaque.
- Menstruation: Mild gingival changes can occur.
- Menopause: Hormonal shifts can contribute to gum sensitivity.
- Certain Medications: Some drugs can cause side effects that contribute to gingivitis. These include:
- Anticonvulsants (e.g., phenytoin)
- Calcium channel blockers (e.g., nifedipine, amlodipine)
- Immunosuppressants (e.g., cyclosporine)
- These medications can cause gingival overgrowth, making it difficult to clean around the teeth and leading to increased plaque retention and inflammation.
- Systemic Diseases: Underlying health conditions can weaken the immune system or affect the body's inflammatory response, making individuals more susceptible to gum disease.
- Diabetes: People with uncontrolled diabetes are at a higher risk of developing infections, including gum disease. Poorly managed blood sugar levels can impair the body's ability to fight off bacteria.
- Compromised Immune System: Conditions like HIV/AIDS or treatments like chemotherapy can suppress the immune system, increasing vulnerability to infections and inflammation in the gums.
- Dry Mouth (Xerostomia): Saliva helps wash away food particles and neutralize acids produced by bacteria. A lack of saliva, often caused by medications, certain medical conditions, or radiation therapy, allows plaque to accumulate more easily.
- Poor Nutrition: A diet lacking essential nutrients, especially Vitamin C, can compromise gum health and the body's ability to fight infection.
- Genetics: Some people are genetically predisposed to developing gum disease, making them more vulnerable even with good oral hygiene.
- Stress: Chronic stress can weaken the immune system, potentially making you more susceptible to gum inflammation.
- Ill-fitting Dental Restorations: Crowns, bridges, or fillings that don't fit properly can create areas where plaque and food particles easily get trapped and are difficult to clean.
Signs and Symptoms to Watch For
Recognizing the early signs of gingivitis is crucial for timely intervention and preventing its progression. Don't wait for pain, as gingivitis is often painless in its early stages. Be vigilant for these indicators:
- Red, Swollen, or Puffy Gums: Healthy gums are typically firm and pale pink. Gums affected by gingivitis often appear vibrant red, purplish-red, or dusky red, and they may look swollen or puffy due to inflammation.
- Bleeding Gums: This is one of the most common and earliest signs. Your gums might bleed easily during brushing, flossing, or even when eating certain foods. While a little blood might seem insignificant, healthy gums should not bleed.
- Tender or Sensitive Gums: Your gums might feel sore or tender to the touch.
- Receding Gums: While more characteristic of advanced periodontal disease, early gum recession can sometimes be observed with chronic gingivitis. This means the gum tissue pulls back, exposing more of the tooth root.
- Bad Breath (Halitosis): Persistent bad breath, even after brushing, can be a symptom. The bacteria accumulating in plaque and the inflammatory processes in the gums produce foul-smelling compounds.
- Pus Between Teeth and Gums: Although less common in the very early stages of gingivitis and more indicative of periodontitis, you might occasionally notice pus emerging from the gumline, signaling an active infection.
- Shiny Gums: Inflamed gums can sometimes appear shiny or glossy due to swelling.
If you observe any of these symptoms, especially bleeding gums, it's essential to schedule an appointment with your dentist promptly.
Diagnosis Process — What Your Dentist Does
Diagnosing gingivitis is typically straightforward and part of a routine dental check-up. Your dentist or dental hygienist will employ several methods to assess your gum health:
-
Oral Examination (Visual Inspection):
- The dentist will visually inspect your gums for signs of inflammation: redness, swelling, and changes in contour or texture. They will also look for visible plaque and calculus buildup on your teeth.
- They'll check for any signs of gum recession or other abnormalities.
-
Periodontal Probing:
- This is a key diagnostic tool. A small, blunt instrument called a periodontal probe is gently inserted into the sulcus (the shallow space between the tooth and the gum). In healthy gums, this pocket depth is typically 1-3 millimeters (mm).
- For gingivitis, pocket depths generally remain within this healthy range, but the gums will often bleed upon probing, indicating inflammation. In contrast, periodontitis is characterized by deeper pockets (often 4mm or more) and bone loss.
-
Assessment of Bleeding:
- The dentist will note whether your gums bleed during probing or gentle manipulation. Bleeding on probing is a strong indicator of gingival inflammation.
-
Review of Medical and Dental History:
- Your dentist will ask about your overall health, any medications you're taking (which could contribute to gingivitis), and your oral hygiene habits. They will also inquire about risk factors such as smoking or a family history of gum disease.
-
Dental X-rays (Radiographs):
- While gingivitis primarily affects soft tissues and doesn't cause bone loss, X-rays are usually taken as part of a comprehensive exam. They are essential for ruling out periodontitis, which does involve bone loss around the teeth. If X-rays show no bone loss, and only soft tissue inflammation is present, the diagnosis is confirmed as gingivitis.
Based on this thorough evaluation, your dentist can accurately diagnose gingivitis, distinguish it from more advanced periodontal disease, and recommend the appropriate treatment plan.
Treatment Options with Pros, Cons, and Costs
The good news is that gingivitis is completely reversible, and treatment is generally straightforward. The primary goal of treatment is to eliminate the source of inflammation: plaque and calculus.
1. Professional Dental Cleaning (Prophylaxis): * Description: This is the cornerstone of gingivitis treatment. A dental hygienist or dentist uses specialized instruments to remove plaque and calculus (tartar) from above and just below the gumline. This process involves: * Scaling: Using ultrasonic devices and hand scalers to meticulously scrape off hardened deposits. * Polishing: Using a rotating rubber cup and abrasive paste to smooth the tooth surfaces, making it harder for plaque to adhere. * Pros: Highly effective, non-invasive, relatively quick. Immediately removes irritants, allowing gums to heal. Essential for areas home brushing and flossing can't reach. * Cons: Requires patient compliance with ongoing home care for sustained results. Not a "one-and-done" solution. * Cost Range (US, without insurance): $75 - $200. This cost varies significantly based on location, dental practice, and the amount of cleaning required. * Cost Range (US, with insurance): Often fully covered or requires a low co-pay (e.g., $0-$50) as most dental insurance plans cover two preventive cleanings per year.
2. Improved Home Oral Hygiene: * Description: This is equally critical. Your dental professional will provide instructions on proper brushing techniques (twice daily for two minutes with a soft-bristled brush), daily flossing, and potentially the use of an interdental cleaner. * Pros: Empowers the patient, cost-effective, prevents recurrence. * Cons: Requires discipline and consistency. Incorrect technique can be ineffective or even harmful. * Cost: Minimal (cost of toothbrush, floss, toothpaste – typically $10-$30 per month).
3. Antiseptic Mouthwash (Adjunctive Therapy): * Description: Your dentist might recommend a therapeutic mouthwash containing ingredients like chlorhexidine or cetylpyridinium chloride to help reduce bacterial load and gum inflammation. This is usually prescribed for a limited time. * Pros: Can aid in reducing bacteria, especially in hard-to-reach areas. * Cons: Not a substitute for brushing and flossing. Long-term use of some (e.g., chlorhexidine) can cause tooth staining or alter taste perception. * Cost: $5-$20 per bottle (over-the-counter or prescription).
4. Addressing Underlying Risk Factors: * Description: Managing systemic conditions like diabetes, adjusting medications (in consultation with your physician), or quitting smoking are vital for long-term gum health. * Pros: Holistic approach, improves overall health. * Cons: May require significant lifestyle changes or coordination with other healthcare providers. * Cost: Varies widely depending on the underlying condition and required medical care.
Comparison Table: Common Treatments for Gingivitis
| Treatment Option | Description | Pros | Cons | Estimated Cost (US, without insurance) | Insurance Coverage |
|---|---|---|---|---|---|
| Professional Cleaning (Prophylaxis) | Removal of plaque and calculus above and just below the gumline by a dental professional. | Highly effective, quick relief, allows gums to heal. | Requires ongoing home care for sustained results. | $75 - $200 | Often fully covered (2x/year) or low co-pay. |
| Improved Home Oral Hygiene | Daily brushing (2x/day), flossing (1x/day), proper technique. | Essential for prevention & long-term maintenance, cost-effective. | Requires discipline, can be ineffective if technique is poor. | $10 - $30/month | Not directly, but preventative care reduces future costs. |
| Antiseptic Mouthwash | Therapeutic rinse to reduce bacteria and inflammation, often prescribed for short-term use. | Aids in bacterial reduction, especially in difficult areas. | Not a substitute for mechanical cleaning, potential side effects (staining, taste alteration) with some. | $5 - $20 | Generally not covered for OTC; prescription might be. |
Note: For gingivitis, "deep cleaning" (scaling and root planing) is generally not indicated unless there are signs of early periodontitis (deeper pockets and bone loss).
Step-by-Step: What to Expect During Treatment
Treating gingivitis is a collaborative effort between you and your dental team. Here's a typical step-by-step breakdown:
- Initial Examination and Diagnosis: As described above, your dentist will conduct a thorough oral exam, probe your gums, and review your medical history to confirm the diagnosis of gingivitis and rule out more severe periodontal disease.
- Professional Dental Cleaning:
- You'll be seated comfortably in the dental chair.
- The dental hygienist will use specialized tools, often starting with an ultrasonic scaler. This device uses high-frequency vibrations and a water spray to break up and wash away plaque and calculus. You'll hear a whirring sound and feel vibrations, but it's generally not painful.
- Next, hand scalers (curettes and sickles) are used to meticulously remove any remaining deposits and smooth the tooth surfaces, especially in areas where the ultrasonic scaler might be less effective.
- Finally, your teeth will be polished using a small rotating brush or rubber cup with an abrasive paste, leaving them smooth and shiny.
- Oral Hygiene Instructions: After the cleaning, your hygienist will spend time demonstrating proper brushing and flossing techniques. They may recommend specific toothbrushes (e.g., electric toothbrushes), types of floss, or interdental cleaners based on your individual needs. This guidance is critical for preventing recurrence.
- Discussion of Risk Factors: Your dentist or hygienist will discuss any identified risk factors (e.g., smoking, medication side effects, systemic conditions) and advise on strategies to manage them.
- Scheduling Your Next Appointment: You'll typically be advised to return for your regular preventive cleaning in six months. In some cases, if the gingivitis was more pronounced, an earlier follow-up might be recommended to ensure the gums are healing properly.
Recovery Timeline and Aftercare
The good news is that with prompt treatment and diligent home care, gums affected by gingivitis can heal remarkably quickly.
- Immediate Post-Cleaning: You might experience some mild sensitivity or soreness in your gums immediately after the professional cleaning, especially if there was significant calculus buildup. This usually subsides within a few hours to a day.
- Healing Timeline: With effective daily brushing and flossing, you should notice significant improvement in your gum health within a few days to two weeks. The redness and swelling will diminish, and your gums will become firmer and return to a healthy pink color. Most importantly, the bleeding during brushing and flossing should stop.
- Long-term Aftercare:
- Consistent Oral Hygiene: This is paramount. Brush your teeth thoroughly twice a day for two minutes with fluoride toothpaste, and floss daily. Consider using an antimicrobial mouthwash if recommended by your dentist.
- Regular Dental Check-ups: Adhere to your dentist's recommended schedule for preventive cleanings, typically every six months. These appointments are vital for removing any new plaque and calculus buildup before it can cause inflammation.
- Healthy Lifestyle: Maintain a balanced diet, limit sugary snacks, and avoid tobacco products.
- Monitor Your Gums: Pay attention to any recurring symptoms like bleeding or swelling. If you notice them, don't wait for your next appointment – contact your dentist.
Successful recovery from gingivitis is largely in your hands. By committing to excellent home care and regular professional maintenance, you can keep your gums healthy and prevent the return of inflammation.
Prevention Strategies
Preventing gingivitis is simpler and less costly than treating it. The cornerstone of prevention lies in meticulous oral hygiene and regular dental visits.
- Brush Your Teeth Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes each time, covering all surfaces of your teeth and gently along the gumline. Electric toothbrushes can be particularly effective at removing plaque.
- Floss Daily: Flossing is crucial for removing plaque and food particles from between your teeth and under the gumline, areas your toothbrush can't reach. Use a clean section of floss for each tooth.
- Regular Dental Check-ups and Professional Cleanings: Visit your dentist for a check-up and professional cleaning at least every six months, or more frequently if recommended by your dentist due to specific risk factors. These appointments allow for the removal of stubborn calculus and early detection of any issues.
- Use an Antimicrobial Mouthwash: While not a substitute for brushing and flossing, an over-the-counter antimicrobial mouthwash can help reduce plaque and bacteria, complementing your routine. Your dentist might prescribe a therapeutic mouthwash for specific situations.
- Maintain a Healthy Diet: Limit sugary and starchy foods, which contribute to plaque formation. Eat a balanced diet rich in fruits, vegetables, and whole grains to support overall health, including gum health.
- Avoid Tobacco Products: Smoking and chewing tobacco are major risk factors for gingivitis and more severe periodontal disease. Quitting tobacco is one of the most impactful steps you can take for your oral and overall health.
- Manage Systemic Health Conditions: If you have conditions like diabetes, ensure they are well-managed, as uncontrolled systemic diseases can impact gum health.
- Address Dry Mouth: If you suffer from dry mouth, discuss strategies with your dentist, such as using saliva substitutes or specific mouthwashes, to mitigate its effects.
Cost Ranges in the US (with/without insurance)
Understanding the financial aspect of dental care is important. Costs can vary significantly based on your geographic location, the specific dental practice, and the complexity of your case.
-
Routine Dental Cleaning (Prophylaxis): This is the standard treatment for gingivitis.
- Without Insurance: You can expect to pay anywhere from $75 to $200. This often includes the examination, scaling, and polishing.
- With Insurance: Most dental insurance plans classify routine cleanings as preventive care, which means they are often 100% covered or require a very low co-pay, typically ranging from $0 to $50. Most plans cover two routine cleanings per year.
-
Dental Exam/Check-up (without cleaning):
- Without Insurance: $50 to $150.
- With Insurance: Often fully covered or a small co-pay.
-
Full Mouth X-rays:
- Without Insurance: $100 to $250.
- With Insurance: Often fully covered once every few years, or partially covered.
-
Antiseptic Mouthwash:
- Over-the-counter: $5 to $20 per bottle.
- Prescription: May be slightly more, but often not covered by dental insurance.
Important Considerations:
- These are estimates and can vary. Always confirm fees with your dental office before treatment.
- If your gingivitis has progressed to early periodontitis and requires a scaling and root planing (deep cleaning) procedure, the costs will be significantly higher, typically ranging from $200 to $500 per quadrant without insurance. Dental insurance usually covers a percentage (e.g., 50-80%) of deep cleaning costs after your deductible is met.
- Investing in preventive care, such as regular cleanings, is almost always more cost-effective than waiting until more extensive (and expensive) treatment is needed for advanced periodontal disease.
For Parents / Pediatric Considerations
Gingivitis is not just an adult concern; it can affect children and adolescents as well. While often milder, it's crucial for parents to be aware of the signs and promote good oral hygiene from a young age.
- Common in Children: Plaque-induced gingivitis is common in children and adolescents, especially during periods of orthodontic treatment or hormonal changes. Studies indicate that a significant percentage of children and teens exhibit some signs of gingivitis.
- Causes in Kids: Similar to adults, the primary cause is inadequate plaque removal. Poor brushing habits, infrequent flossing, and sugary diets contribute significantly.
- Puberty Gingivitis: Adolescence brings significant hormonal changes, particularly during puberty. Increased levels of sex hormones can exaggerate the inflammatory response of the gums to plaque, leading to what's known as "puberty gingivitis." Gums can become notably red, swollen, and bleed easily, even with moderate plaque levels.
- Orthodontic Gingivitis: Children and teens with braces are highly susceptible to gingivitis. The brackets and wires create additional areas where food and plaque can get trapped, making effective cleaning challenging. Special brushing techniques and tools (like interdental brushes) are often necessary.
- Signs to Watch For: Look for gums that are red instead of pink, swollen, or bleed when your child brushes or eats hard foods. Bad breath can also be a sign.
- Parental Role: Parents play a crucial role in establishing good oral hygiene habits.
- Supervise Brushing: Supervise younger children while they brush to ensure they're doing it effectively.
- Teach Flossing: Teach children how to floss correctly once their teeth are touching.
- Healthy Snacks: Encourage a diet low in sugar.
- Regular Dental Visits: Schedule regular dental check-ups and cleanings for your children starting from their first tooth (around age one). Your pediatric dentist can identify gingivitis early and provide tailored advice.
- Reversibility: Just like in adults, gingivitis in children is reversible with improved oral hygiene and professional cleaning. Addressing it early prevents progression to more serious gum problems in adulthood.
Frequently Asked Questions
How much does gingivitis treatment cost?
The primary treatment for gingivitis is a professional dental cleaning (prophylaxis). Without insurance, this typically costs between $75 and $200. With most dental insurance plans, routine cleanings are often fully covered or require a low co-pay (e.g., $0-$50), as they are considered preventive care. If more advanced treatment like deep cleaning (scaling and root planing) is needed due to progression towards periodontitis, costs can be $200-$500 per quadrant without insurance, with insurance typically covering a percentage after your deductible.
Is gingivitis treatment painful?
A routine professional cleaning to treat gingivitis is generally not painful. You might experience some pressure or vibrations from the ultrasonic scaler and a scraping sensation from hand instruments. If you have significant calculus buildup or very inflamed, sensitive gums, you might feel some discomfort. Your hygienist can often use a topical numbing gel or even local anesthetic if needed to ensure your comfort. Any post-cleaning sensitivity is usually mild and resolves within a day or two.
How long does it take to cure gingivitis?
Gingivitis can be resolved quite quickly with the right approach. After a professional dental cleaning and if you commit to diligent daily brushing and flossing, you should see significant improvement in your gum health within a few days to two weeks. The redness, swelling, and bleeding should diminish, and your gums will return to a healthier, firmer, pink appearance. Consistency in home care is key for long-term "cure."
Can gingivitis go away on its own?
No, gingivitis cannot go away on its own. While your body might attempt to fight off the inflammation, the primary cause – plaque and hardened calculus – will remain if not physically removed. Calculus, in particular, cannot be removed by brushing or flossing alone. Without professional intervention and improved home care, gingivitis will persist and may eventually progress to the more severe and irreversible condition of periodontal disease.
What are the alternatives to professional dental cleaning?
There are no true alternatives to professional dental cleaning for effectively treating gingivitis. While diligent home care (brushing and flossing) is essential for prevention and maintenance, it cannot remove hardened calculus that has built up below the gumline. Professional cleaning is necessary to physically remove these deposits. Some adjuncts like antiseptic mouthwashes can help reduce bacterial load, but they are not a substitute for the mechanical removal of plaque and calculus performed by a dental professional.
Does dental insurance cover gingivitis treatment?
Generally, yes, dental insurance typically covers gingivitis treatment. Routine professional dental cleanings, which are the primary treatment for gingivitis, are considered preventive care and are often 100% covered or covered at a high percentage (e.g., 80-100%) by most dental insurance plans, usually up to two times per year. Diagnostic procedures like exams and X-rays are also usually covered. If the gingivitis has progressed to the point where deeper cleaning (scaling and root planing) is needed, insurance plans typically cover a percentage (e.g., 50-80%) after your deductible is met. It's always best to check with your specific insurance provider for exact coverage details.
What happens if gingivitis is left untreated?
If gingivitis is left untreated, it can have serious consequences. The persistent inflammation caused by plaque and calculus will eventually lead to the breakdown of the tissues and bone that support your teeth. This progression is known as periodontal disease (or periodontitis). In periodontitis, the inflammation spreads deeper, causing the gums to pull away from the teeth, forming "pockets" that become infected. As the disease advances, the bone supporting the teeth is destroyed, leading to loose teeth, changes in your bite, and ultimately, tooth loss. Untreated gum disease has also been linked to systemic health issues, including heart disease, stroke, and diabetes complications.
Is gingivitis contagious?
No, gingivitis is not contagious. It is an inflammatory condition caused by an individual's immune response to the accumulation of bacteria (plaque) in their own mouth. While the bacteria that cause plaque are common in everyone's mouth, you cannot "catch" gingivitis from someone else through kissing, sharing food, or other close contact. It's a localized problem that develops due to personal oral hygiene habits and various risk factors.
When to See a Dentist
Given that gingivitis is often painless in its early stages, knowing when to seek professional care is critical for prevention and early intervention.
See a dentist for routine care if:
- You haven't had a dental check-up and cleaning in the past six months. Regular preventive care is your best defense against gingivitis.
Schedule an appointment promptly if you notice any of these signs of gingivitis:
- Your gums appear red, swollen, or puffy.
- Your gums bleed easily when you brush, floss, or eat. Even a little blood is not normal for healthy gums.
- You have persistent bad breath that doesn't improve with brushing.
- Your gums feel tender or sore.
- You notice any changes in the way your teeth fit together when you bite.
- You can see or feel hardened deposits (calculus) on your teeth, especially near the gumline.
Seek immediate dental attention (emergency) if:
- You experience severe, throbbing pain in your gums or teeth.
- You notice pus oozing from your gums.
- You have a sudden, significant swelling in your gums or face.
- You have uncontrolled bleeding from your gums that doesn't stop after applying pressure.
Early detection and treatment of gingivitis are paramount to maintaining your oral health and preventing the progression to more serious and irreversible periodontal disease. Don't wait for pain – be proactive with your gum health!
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.