Periodontal Disease
4,640 words · 15 min read
Quick Definition
A chronic inflammatory condition caused by bacterial infection that destroys the gums, periodontal ligament, and bone supporting the teeth. Also known as periodontitis.
Periodontal Disease: Your Definitive Guide to Understanding and Managing Gum Disease
Periodontal disease, commonly known as gum disease or periodontitis, is a chronic inflammatory condition that impacts millions of Americans. It's far more than just a minor inconvenience; it's a serious bacterial infection that can progressively destroy the soft tissues and bone supporting your teeth. If left untreated, periodontal disease can lead to tooth loss and has even been linked to a variety of systemic health issues.
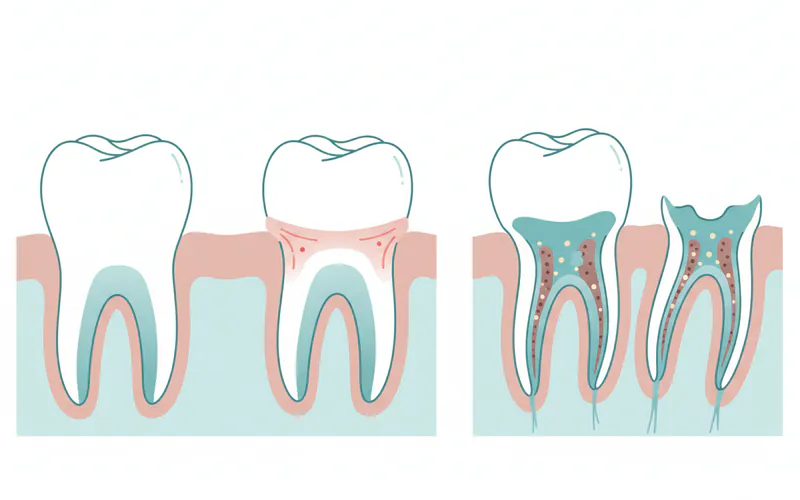
This comprehensive guide from SmilePedia.net aims to be your go-to resource for understanding what is periodontal disease, its causes, symptoms, treatments, and crucially, how to prevent it. Whether you're searching for "periodontal disease dental" information or simply want to safeguard your oral health, you'll find everything you need here.
Approximately 47.2% of American adults aged 30 and older have some form of periodontal disease, a figure that rises to 70.1% for those 65 and older, according to the Centers for Disease Control and Prevention (CDC). This widespread prevalence underscores the importance of awareness and early intervention in maintaining not just a healthy smile, but overall well-being.
Key Takeaways:
- Periodontal disease (periodontitis) is a chronic bacterial infection affecting the gums and supporting bone.
- It is the advanced stage of gum disease, progressing from gingivitis if left untreated.
- Untreated periodontitis is a primary cause of adult tooth loss.
- Symptoms include bleeding gums, bad breath, receding gums, and loose teeth.
- Prevention through good oral hygiene and regular dental visits is crucial.
- While not curable, it is manageable with professional dental treatment and diligent home care.
Types and Classifications of Periodontal Disease
Periodontal disease isn't a single condition but rather a spectrum of diseases, varying in severity and progression. Understanding the different types helps in diagnosis and tailoring effective treatment.
- Chronic Periodontitis: This is the most common form of periodontal disease, typically affecting adults, but it can occur at any age. It's characterized by slow to moderate progression of inflammation within the supporting tissues of the teeth, leading to destruction of the periodontal ligament (the fibers that hold the tooth in the socket) and the surrounding alveolar bone. This results in gum recession and the formation of deep periodontal pockets around the teeth.
- Aggressive Periodontitis: A less common but more severe form, aggressive periodontitis progresses rapidly and can cause significant tooth-supporting tissue destruction in a short amount of time. It often affects younger individuals, even those with otherwise healthy medical profiles. It can be localized (affecting specific teeth) or generalized (affecting most teeth). Genetic factors are often implicated in aggressive forms.
- Necrotizing Periodontal Diseases: These are severe forms characterized by the death of gum tissue, periodontal ligament, and alveolar bone. They are most commonly seen in individuals with weakened immune systems, such as those with HIV/AIDS, malnutrition, or severe stress. Conditions like Necrotizing Ulcerative Gingivitis (NUG) and Necrotizing Ulcerative Periodontitis (NUP) fall into this category, causing painful, bleeding gums and ulcerations.
- Periodontitis as a Manifestation of Systemic Diseases: In some cases, periodontal disease is a symptom or complication of other systemic health conditions. Diseases like diabetes, heart disease, respiratory diseases, and certain blood disorders can make individuals more susceptible to periodontal disease or worsen its progression. Genetic disorders such as Down syndrome or Papillon-Lefèvre syndrome can also predispose individuals to severe periodontitis.
Causes and Risk Factors for Periodontal Disease
The primary cause of periodontal disease is the accumulation of bacterial plaque—a sticky, colorless film that constantly forms on your teeth. However, several other factors can increase your risk and severity.
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque to accumulate and harden into calculus (tartar). Calculus is rough and porous, providing an ideal surface for bacteria to thrive and making it impossible to remove with regular brushing.
- Smoking and Tobacco Use: This is one of the most significant risk factors for developing severe periodontal disease. Smoking impairs the immune system's ability to fight off bacterial infections and can mask the classic signs of gum disease (like bleeding), making diagnosis more challenging. Smokers are twice as likely to have periodontal disease as non-smokers.
- Diabetes: Individuals with diabetes, especially those with poorly controlled blood sugar levels, are at a higher risk for developing severe periodontal disease. Diabetes reduces the body's resistance to infection, making gums more susceptible to bacterial attack.
- Genetics: Some people are genetically more susceptible to periodontal disease, even with excellent oral hygiene. If your parents or siblings have periodontitis, you might be at a higher risk.
- Hormonal Changes: Fluctuations in hormones, such as those occurring during pregnancy, puberty, menstruation, or menopause, can make gums more sensitive and increase susceptibility to inflammation.
- Certain Medications: Some drugs, including oral contraceptives, antidepressants, and certain heart medications, can reduce saliva flow (dry mouth), making the mouth more vulnerable to plaque accumulation and infection.
- Stress: Chronic stress can weaken the body's immune system, making it harder to fight off infections, including periodontal disease.
- Poor Nutrition: A diet lacking essential nutrients, especially Vitamin C, can compromise the body's immune system and make it more difficult for gum tissue to repair itself.
- Grinding or Clenching Teeth (Bruxism): These habits can put excessive force on the supporting tissues of the teeth, potentially accelerating the breakdown of the periodontal ligament and bone.
Signs and Symptoms to Watch For
Periodontal disease often progresses silently, with little or no pain in its early stages. This is why regular dental check-ups are so vital. However, as the disease advances, several warning signs may become apparent.
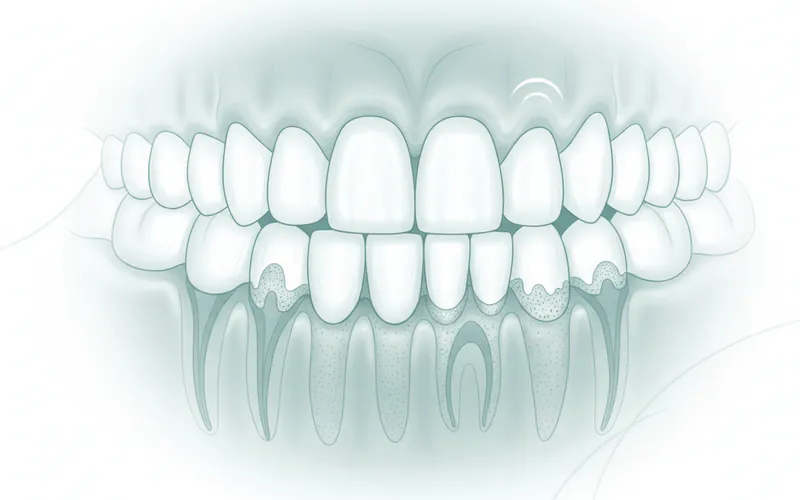
- Bleeding Gums: Gums that bleed easily when you brush, floss, or even eat hard foods are a primary indicator of gum inflammation, specifically gingivitis, the earliest stage of gum disease.
- Red, Swollen, or Tender Gums: Healthy gums are firm and pink. Gums affected by periodontitis may appear puffy, purplish-red, and feel tender to the touch.
- Persistent Bad Breath (Halitosis): The bacteria responsible for periodontal disease release foul-smelling gases, leading to chronic bad breath that doesn't go away with brushing or mouthwash.
- Receding Gums: Your gums may pull away from your teeth, making your teeth appear longer than usual. This exposes the tooth roots, which can lead to sensitivity.
- Deep Pockets Between Teeth and Gums: As the gums pull away from the teeth, they create spaces called periodontal pockets. These pockets become breeding grounds for bacteria, making them difficult to clean at home.
- Pus Between Teeth and Gums: A sign of active infection, pus may be noticeable when you press on your gums.
- Loose or Shifting Teeth: As the bone supporting your teeth deteriorates, teeth may become loose, shift their position, or even start to separate, creating new gaps.
- Changes in Your Bite: You might notice that your teeth don't fit together properly when you bite, or your partial dentures no longer fit.
- Painful Chewing: As the infection progresses and teeth loosen, chewing can become uncomfortable or painful.
If you experience any of these symptoms, it's crucial to consult a dentist or periodontist promptly. Early diagnosis and treatment can significantly improve your prognosis and help save your teeth.
Diagnosis Process — What Your Dentist Does
Diagnosing periodontal disease involves a thorough examination by your dentist or a periodontist (a dentist specializing in gum disease). The process typically includes:
- Medical and Dental History Review: Your dentist will ask about your overall health, medications you take, and any risk factors like smoking or diabetes. They'll also inquire about your oral hygiene habits and any symptoms you've noticed.
- Visual Examination: The dentist will visually inspect your gums for signs of inflammation, bleeding, swelling, redness, and gum recession. They'll also check for loose teeth and changes in your bite.
- Periodontal Probing: This is a critical diagnostic step. A small, ruler-like instrument called a periodontal probe is gently inserted into the sulcus (the space between the tooth and gum) around each tooth. Healthy gum pockets are typically 1-3 millimeters deep. Depths greater than 4 millimeters usually indicate periodontal disease, with deeper pockets correlating to more advanced disease and bone loss. The dentist will measure and record these depths.
- Dental X-rays: X-rays are essential for assessing the health of the bone supporting your teeth. They can reveal areas of bone loss, the extent of the damage, and help identify calculus buildup below the gum line.
- Plaque and Calculus Assessment: The dentist will evaluate the amount of plaque and calculus present on your teeth, both above and below the gum line.
Based on these findings, your dentist will classify the severity of your periodontal disease and recommend appropriate treatment.
Treatment Options with Pros, Cons, and Costs
Treatment for periodontal disease aims to stop the progression of the infection, reduce inflammation, and, where possible, regenerate lost tissue. Treatment options vary depending on the severity of the disease and can range from non-surgical therapies to advanced surgical procedures.
Non-Surgical Treatments
For mild to moderate periodontal disease, non-surgical approaches are often the first line of defense.
-
Scaling and Root Planing (SRP):
- Description: This is a deep cleaning procedure that goes beyond a routine dental cleaning. Scaling involves carefully removing plaque and calculus from both above and below the gum line. Root planing then smooths the tooth root surfaces, removing bacterial toxins and making it harder for plaque to reattach.
- Pros: Highly effective for early to moderate periodontitis; less invasive than surgery; typically done with local anesthetic; generally more affordable.
- Cons: Not effective for advanced cases with significant bone loss; may require multiple appointments; some post-procedure sensitivity.
- Cost (US): Typically ranges from $200 to $500 per quadrant (a quarter of your mouth), so a full mouth SRP could cost $800 to $2,000. Insurance often covers a significant portion.
-
Antibiotics (Topical or Oral):
- Description: Used in conjunction with SRP, antibiotics can help control bacterial infection. They may be prescribed as an oral rinse (e.g., chlorhexidine) or as an antibiotic gel/chip placed directly into deep periodontal pockets after scaling. Oral antibiotics may be used for widespread or aggressive infections.
- Pros: Helps eliminate lingering bacteria; effective in reducing inflammation and infection.
- Cons: Potential side effects (e.g., upset stomach with oral antibiotics, staining with rinses); risk of antibiotic resistance with overuse.
- Cost (US): Topical antibiotics can add $50-$200 per application, oral antibiotics vary by prescription, typically $20-$100.
-
Laser Therapy:
- Description: Lasers can be used as an adjunctive treatment to SRP. They can help remove diseased tissue and sterilize periodontal pockets, promoting healing.
- Pros: Minimally invasive; reduced bleeding and swelling; faster healing in some cases.
- Cons: Not a standalone treatment; effectiveness as a primary treatment is still debated; generally more expensive.
- Cost (US): Can add $200-$1,000 or more to an SRP procedure, depending on the number of teeth and clinic.
Surgical Treatments
When periodontal disease is advanced and non-surgical treatments aren't sufficient, surgical interventions may be necessary to reduce pocket depths, regenerate lost tissue, or address gum recession.
-
Flap Surgery (Pocket Reduction Surgery):
- Description: The most common periodontal surgical procedure. The periodontist lifts back the gum tissue (creating a "flap") to gain direct access to the tooth roots and bone. This allows for thorough cleaning of plaque and calculus, as well as smoothing of irregular bone surfaces. The gums are then sutured back into place, often fitting more snugly around the teeth, reducing pocket depth.
- Pros: Highly effective for reducing deep pockets; allows for thorough cleaning and reshaping of damaged bone; improves long-term prognosis.
- Cons: More invasive; longer recovery time; some temporary pain and swelling; potential for increased post-operative sensitivity and temporary gum recession.
- Cost (US): Typically $500 to $3,000 per quadrant, or $2,000 to $12,000+ for a full mouth, depending on complexity and location.
-
Bone Grafting:
- Description: Used to regenerate bone that has been destroyed by periodontitis. Fragments of your own bone, synthetic bone, or donated bone are placed in the areas of bone loss. The graft provides a scaffold for your body to grow new bone.
- Pros: Can regenerate lost bone structure; helps stabilize teeth; improves overall prognosis.
- Cons: Invasive; longer healing time; risk of graft rejection (though rare); higher cost.
- Cost (US): $300 to $1,500 per site, in addition to flap surgery costs.
-
Soft Tissue Grafts:
- Description: Addresses gum recession by taking tissue from another area of your mouth (often the roof of your mouth) or using donor tissue, and grafting it to the exposed root surface.
- Pros: Covers exposed root surfaces; reduces sensitivity; improves aesthetics; helps prevent further recession and bone loss.
- Cons: Can be uncomfortable at the donor site; involves two surgical sites if using your own tissue; moderate healing time.
- Cost (US): $600 to $2,500 per site.
-
Guided Tissue Regeneration (GTR):
- Description: This surgical technique uses a small piece of mesh-like barrier membrane placed between the bone and gum tissue. The membrane prevents gum tissue from growing into the healing bone area, allowing slower-growing bone and ligament cells to regenerate first.
- Pros: Promotes regeneration of bone and periodontal ligament; can help save teeth that would otherwise be lost.
- Cons: Invasive; requires a second surgery to remove the membrane if non-resorbable; longer healing time.
- Cost (US): Similar to bone grafting, typically $500 to $2,000 per site, in addition to flap surgery.
Comparison of Non-Surgical vs. Surgical Treatment
| Feature | Non-Surgical (e.g., Scaling & Root Planing) | Surgical (e.g., Flap Surgery, Grafts) |
|---|---|---|
| Severity | Mild to moderate periodontitis | Moderate to severe periodontitis with significant bone loss/deep pockets |
| Invasiveness | Minimally invasive | More invasive |
| Anesthesia | Local anesthetic | Local anesthetic (sometimes with sedation) |
| Procedure | Deep cleaning, smoothing root surfaces, removal of calculus and bacteria | Lifting gum tissue, thorough cleaning, reshaping bone, tissue grafting, bone regeneration |
| Recovery | Days of mild sensitivity/soreness | Weeks of discomfort, swelling, soft diet recommended |
| Effectiveness | Highly effective for early stages, helps manage progression, reduces inflammation | Necessary for advanced cases, can reduce deep pockets, regenerate tissue, save teeth |
| Cost Range | $800 - $2,000 (full mouth SRP) | $2,000 - $12,000+ (full mouth, complex procedures) |
| Insurance | Often good coverage (50-80% of basic procedures) | Typically lower coverage (20-50% of major procedures), often with deductibles |
Step-by-Step: What to Expect During Treatment
Understanding the process can help alleviate anxiety. Here’s a general overview of what to expect:
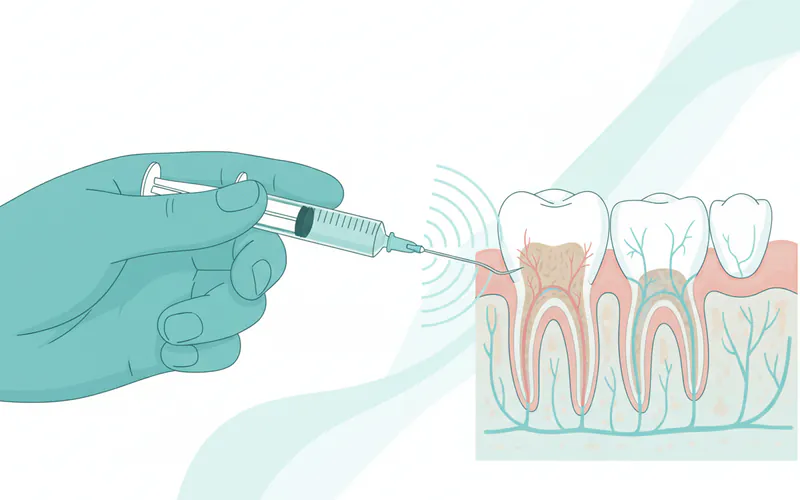
During Scaling and Root Planing (SRP):
- Numbing: The dental hygienist or dentist will administer a local anesthetic to numb the specific area(s) being treated. This ensures you remain comfortable throughout the procedure.
- Scaling: Using specialized instruments (ultrasonic scalers and hand scalers), they will meticulously remove plaque and calculus from the crown of your tooth, and most importantly, from the root surfaces below the gum line and inside the periodontal pockets.
- Root Planing: After scaling, the root surfaces are gently planed (smoothed) to remove any remaining rough spots, bacterial toxins, and make it difficult for bacteria to reattach. This promotes reattachment of the gum tissue to the cleaner, smoother root.
- Irrigation (Optional): Some practitioners may flush the pockets with an antimicrobial solution.
- Multiple Appointments: Depending on the extent of the disease, SRP may be performed over one to four appointments, typically treating one or two quadrants of the mouth at a time.
During Periodontal Surgery (e.g., Flap Surgery):
- Numbing and Sedation: Local anesthetic will be administered to numb the surgical area. For anxious patients or extensive procedures, oral or IV sedation may also be offered.
- Incision and Flap: The periodontist will make small incisions in the gum tissue and gently lift back a section (creating a "flap") to expose the root surfaces and underlying bone.
- Cleaning and Reshaping: Plaque, calculus, and diseased tissue are thoroughly removed. If necessary, the bone may be reshaped (osseous surgery) to reduce bony defects and make it easier for the gums to reattach.
- Grafting (if applicable): If bone or soft tissue grafting is planned, the graft material will be placed at this stage.
- Suturing: The gum flap is carefully repositioned and sutured back into place, often snugly around the teeth.
- Periodontal Dressing (Optional): A protective surgical dressing may be placed over the treated area to aid healing and protect the sutures.
Recovery Timeline and Aftercare
Recovery varies depending on the type and extent of treatment.
Scaling and Root Planing Recovery:
- Immediate: Mild discomfort, sensitivity to hot/cold, and some gum soreness for a few hours to a few days.
- Days 1-3: Manage discomfort with over-the-counter pain relievers (ibuprofen, acetaminophen). Avoid extremely hot or cold foods. You might notice some gum tenderness or mild bleeding when brushing.
- Aftercare: Continue diligent oral hygiene, but brush gently around treated areas. Use a prescribed antimicrobial mouth rinse if given. Avoid sticky or hard foods for a few days. Smoking cessation is highly recommended.
- Follow-up: Your dentist will schedule a follow-up appointment, usually within 4-6 weeks, to check healing and assess pocket depths.
Periodontal Surgery Recovery:
- Immediate: Swelling, bruising, and discomfort are common for several days. You will be prescribed pain medication.
- Days 1-7: Stick to a soft diet. Avoid strenuous activity. Do not rinse vigorously or brush directly on the surgical site. A prescribed antimicrobial rinse may be used. Some bleeding is normal.
- Week 1-2: Sutures are typically removed at a follow-up appointment. Sensitivity to temperature may increase temporarily as gums heal. Continue to avoid hard, crunchy, or spicy foods.
- Weeks 2-6: Healing continues. You can gradually resume normal brushing and flossing in the treated area, as advised by your periodontist.
- Long-Term Aftercare: Periodontal maintenance appointments (specialized cleanings) every 3-4 months are crucial to prevent recurrence. Lifelong commitment to meticulous oral hygiene is essential.
Prevention Strategies
The good news is that periodontal disease is largely preventable with proper care.
- Practice Excellent Oral Hygiene:
- Brush your teeth twice a day for at least two minutes each time, using a soft-bristled toothbrush and fluoride toothpaste. Angle the brush at 45 degrees to the gum line.
- Floss daily to remove plaque and food particles from between teeth and under the gum line where your toothbrush can't reach.
- Consider using an antiseptic mouthwash to reduce bacteria, but don't let it replace brushing and flossing.
- Regular Dental Check-ups and Professional Cleanings: Visit your dentist at least twice a year for check-ups and professional cleanings. These appointments allow for early detection of gingivitis or periodontal disease and removal of stubborn calculus that you can't remove at home. If you have a history of periodontitis, your dentist may recommend more frequent "periodontal maintenance" cleanings (every 3-4 months).
- Quit Smoking and Avoid Tobacco Products: This is arguably the single most impactful step you can take to prevent and manage periodontal disease.
- Manage Systemic Health Conditions: If you have diabetes, heart disease, or other systemic conditions, work closely with your medical doctor to keep them well-controlled.
- Eat a Balanced Diet: A diet rich in vitamins and minerals (especially Vitamin C) supports your immune system and overall oral health. Limit sugary foods and drinks that promote bacterial growth.
- Reduce Stress: Stress can compromise your immune system, making you more vulnerable to infections.
- Be Aware of Medications: Discuss any medications you are taking with your dentist, especially if they cause dry mouth.
Cost Ranges in the US (with/without Insurance)
The cost of periodontal disease treatment in the US can vary significantly based on the severity of the disease, the type of treatment, the number of teeth involved, the geographic location, and the specific dental practice.
- Initial Exam & X-rays: $100 - $300 (often covered by insurance)
- Scaling and Root Planing (SRP):
- Per quadrant: $200 - $500
- Full mouth (4 quadrants): $800 - $2,000
- With insurance: Expect to pay 20-50% out-of-pocket, depending on your plan's coverage for "basic" or "major" restorative services.
- Localized Antibiotic Application: $50 - $200 per tooth (in addition to SRP)
- Periodontal Maintenance Cleanings (after initial treatment):
- Per visit: $100 - $300 (recommended every 3-4 months)
- With insurance: Often covered at 80-100%, similar to routine cleanings, but may count towards a different category depending on the code used.
- Flap Surgery (Pocket Reduction):
- Per quadrant: $500 - $3,000
- Full mouth: $2,000 - $12,000+
- With insurance: Coverage typically 20-50% for "major" services, often subject to deductibles and annual maximums.
- Bone Grafting: $300 - $1,500 per site (in addition to flap surgery)
- With insurance: Similar to flap surgery, limited coverage.
- Soft Tissue Grafting: $600 - $2,500 per site
- With insurance: Similar to flap surgery, limited coverage.
- Guided Tissue Regeneration (GTR): $500 - $2,000 per site (in addition to flap surgery)
- With insurance: Similar to flap surgery, limited coverage.
It's important to note that these are estimates. Always obtain a detailed treatment plan and cost breakdown from your dentist, and check with your dental insurance provider for specific coverage details. Many periodontists offer payment plans to make treatment more accessible.
For Parents / Pediatric Considerations
While periodontal disease is far less common in children than in adults, it can occur and should not be overlooked. Gingivitis, the mildest form of gum disease, is relatively common in children and adolescents, often due to inadequate brushing and flossing. It manifests as red, swollen, or bleeding gums. This is reversible with improved oral hygiene.
More advanced forms of periodontal disease are rare but can occur in children, especially aggressive periodontitis, which may begin around puberty. Factors contributing to childhood periodontitis can include:
- Genetic predispositions: Some children inherit a susceptibility.
- Systemic conditions: Certain medical conditions (e.g., Down syndrome, diabetes, certain blood disorders) can increase risk.
- Poor oral hygiene: As with adults, plaque buildup is the primary driver.
What Parents Should Watch For:
- Persistent bad breath that doesn't improve with brushing.
- Red, swollen, or bleeding gums (especially during brushing).
- Receding gums or teeth that appear "long."
- Loose primary (baby) or permanent teeth without trauma.
- Pus around the gums and teeth.
Parents should ensure children establish excellent oral hygiene habits from a young age, including brushing twice daily and flossing once a day. Regular dental check-ups are crucial for early detection and intervention. If you notice any signs of gum disease in your child, consult a pediatric dentist or a periodontist promptly.
Frequently Asked Questions
Q1: Is periodontal disease curable, or is it a lifelong condition?
A1: Periodontal disease is generally considered a chronic condition that is manageable, not entirely curable in the sense of complete eradication and regeneration of all lost tissue. Once bone loss occurs, it's often irreversible without surgical intervention. However, with effective treatment and dedicated ongoing care (including excellent home hygiene and regular periodontal maintenance appointments), the disease can be brought into remission and its progression halted. It requires a lifelong commitment to control.
Q2: How much does periodontal disease treatment cost, and is it covered by insurance?
A2: Costs vary widely based on severity and treatment type. Non-surgical treatments like Scaling and Root Planing can range from $800 - $2,000 for a full mouth. Surgical options can be much higher, from $2,000 to over $12,000 for extensive procedures. Most dental insurance plans offer some coverage. Preventive care (routine cleanings) is often covered at 80-100%. Basic procedures like SRP might be covered at 50-80%, while major procedures like surgery often have lower coverage (20-50%), subject to deductibles and annual maximums. Always get a pre-treatment estimate from your dentist and check with your insurance provider.
Q3: Is periodontal disease treatment painful?
A3: During treatment, local anesthetic is always used to ensure your comfort, so you should not feel pain. For Scaling and Root Planing, you might experience some pressure or mild discomfort. After treatment, particularly after surgical procedures, some discomfort, sensitivity, and swelling are common. This can be managed effectively with prescribed pain medication and over-the-counter pain relievers. Your dental team will provide detailed post-operative instructions to minimize discomfort.
Q4: How long does periodontal disease treatment take?
A4: Non-surgical treatment like Scaling and Root Planing typically involves 1-4 appointments, each lasting 1-2 hours. The recovery period for SRP is usually a few days of mild sensitivity. Surgical treatments can take several hours per procedure, with recovery times ranging from several weeks to a few months for full healing. However, the entire management of periodontal disease is ongoing. After active treatment, lifelong periodontal maintenance appointments every 3-4 months are crucial.
Q5: Are there any natural or alternative treatments for periodontal disease?
A5: While some natural remedies (like tea tree oil rinses or certain herbs) are marketed for gum health, there are no proven natural or alternative treatments that can effectively treat established periodontal disease and reverse bone loss. These may offer some temporary symptom relief or complement professional care, but they cannot replace the essential mechanical removal of plaque and calculus by a dental professional. Relying solely on alternatives can lead to irreversible damage and tooth loss. Always consult your dentist.
Q6: Can periodontal disease spread to other people? Is it contagious?
A6: Periodontal disease itself is not considered contagious in the way a cold or flu is. You cannot "catch" it from another person through casual contact like sharing utensils or kissing. While the bacteria involved in periodontal disease can be transferred between individuals (e.g., through saliva), it's the host's immune response and risk factors that determine if the disease develops. Most people already have these bacteria in their mouths.
Q7: What happens if I don't treat my periodontal disease?
A7: Untreated periodontal disease will progressively worsen. The bacterial infection will continue to destroy the periodontal ligament and alveolar bone that support your teeth, leading to:
- Increased gum recession and exposed roots.
- Deepening periodontal pockets.
- Chronic bad breath and inflammation.
- Increased tooth mobility and eventual tooth loss.
- Potentially, an increased risk of systemic health issues like heart disease, stroke, and diabetes complications.
When to See a Dentist
Given that periodontal disease often progresses without significant pain, regular dental check-ups are your first line of defense.
- Routine Care: Schedule comprehensive dental examinations and professional cleanings at least twice a year. If you have risk factors or a history of gum disease, your dentist may recommend more frequent visits (e.g., every 3-4 months for periodontal maintenance). These routine visits are crucial for early detection and intervention, often catching gingivitis before it progresses to periodontitis.
- When to Seek Immediate Attention:
- Any persistent signs of gum inflammation, such as bleeding gums when brushing or flossing.
- Gums that are red, swollen, tender, or appear to be pulling away from your teeth (receding gums).
- Persistent bad breath that doesn't improve with oral hygiene.
- Changes in your bite or the way your teeth fit together.
- Loose or shifting teeth.
- Pus between your teeth and gums.
- New or increasing sensitivity to hot or cold.
- Severe pain or swelling in your gums or around a tooth.
Don't wait for pain to seek help. Early diagnosis and treatment are critical for saving your teeth and protecting your overall health. Your dental team is your best partner in managing and preventing periodontal disease.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.