What Is Periodontal Disease
Key Takeaways
- Imagine waking up to swollen, bleeding gums, bad breath that won't go away, and teeth that feel loose. This isn't just an unpleasant dream; it's the harsh reality for millions of Americans suffering from periodontal disease. Also commonly known as gum disease, this silent epidemic affects nearly
What Is Periodontal Disease
Imagine waking up to swollen, bleeding gums, bad breath that won't go away, and teeth that feel loose. This isn't just an unpleasant dream; it's the harsh reality for millions of Americans suffering from periodontal disease. Also commonly known as gum disease, this silent epidemic affects nearly half of all adults aged 30 and older in the United States, according to the Centers for Disease Control and Prevention (CDC). It's a progressive inflammatory condition that, if left untreated, can lead to irreversible damage, tooth loss, and even impact your overall systemic health. Understanding what is periodontal disease is the crucial first step toward protecting your oral health and preventing severe complications.

This comprehensive guide from SmilePedia.net will delve deep into the intricacies of periodontal disease, providing you with a definitive resource to recognize, understand, and combat this common yet serious condition. We'll explore its different forms, identify the underlying causes, detail the tell-tale signs and symptoms, outline the latest treatment options, discuss associated costs and insurance considerations, and, most importantly, equip you with the knowledge to prevent its onset. You'll also learn about the vital role of a periodontist, a dental specialist dedicated to the prevention, diagnosis, and treatment of periodontal disease. By the end, you'll have a clear understanding of how to safeguard your smile and your health.
Key Takeaways:
- Periodontal disease is a chronic inflammatory condition affecting the gums and bone supporting your teeth, progressing from reversible gingivitis to irreversible periodontitis.
- Early signs include red, swollen, or bleeding gums, while advanced symptoms involve receding gums, persistent bad breath, and loose teeth.
- Treatment costs can range from $200-$1,500 for non-surgical scaling and root planing per quadrant, to $1,000-$5,000+ per quadrant for surgical procedures like flap surgery or bone grafts. Total treatment for widespread advanced disease can exceed $10,000-$20,000.
- A periodontist is a dental specialist who diagnoses and treats gum disease, performing both non-surgical and surgical interventions.
- Untreated periodontal disease significantly increases risks for systemic health issues like heart disease, stroke, and diabetes complications, and can indirectly contribute to severe health decline. While it doesn't directly "kill you" in the way an acute infection might, its long-term systemic impact can be life-threatening.
- Prevention hinges on consistent oral hygiene (brushing twice daily, flossing once daily), regular dental check-ups (every 6 months), and a healthy lifestyle.
- Recovery from non-surgical treatment is usually quick (a few days of sensitivity), while surgical recovery can take weeks to months, requiring diligent aftercare.
What It Is / Overview
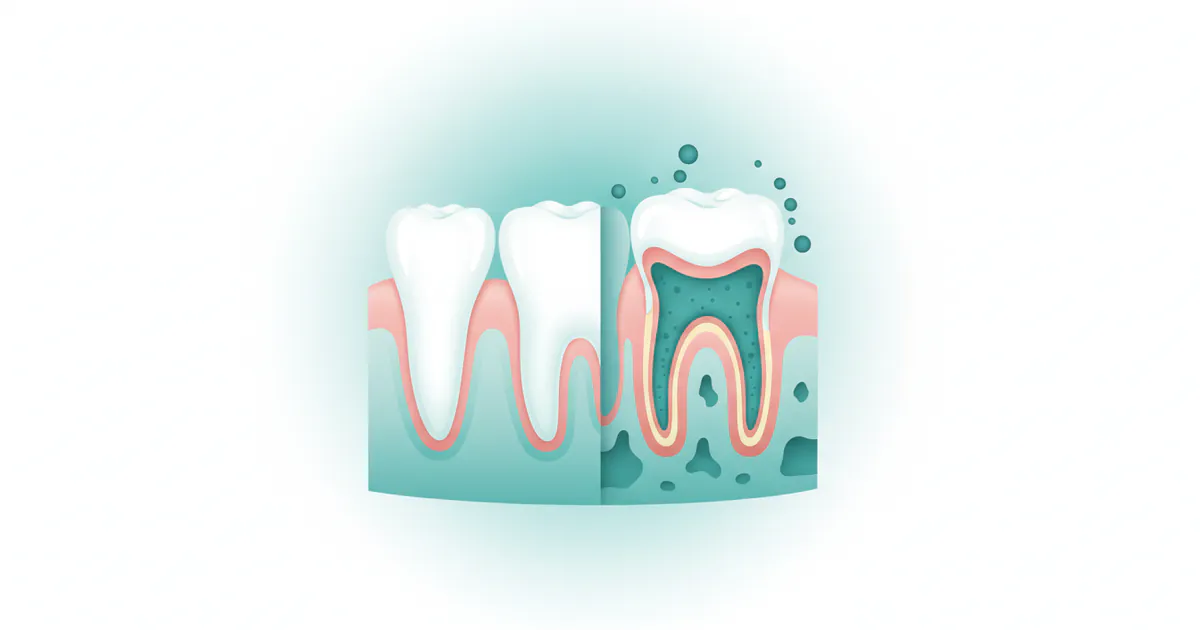
Periodontal disease, at its core, is a serious gum infection that damages the soft tissue and, without treatment, can destroy the bone that supports your teeth. It’s a progressive disease, meaning it typically starts mild and worsens over time if left unaddressed.
The journey often begins with gingivitis, the mildest form of periodontal disease. This is an inflammation of the gums, usually caused by plaque buildup along the gumline. Plaque is a sticky film of bacteria that constantly forms on your teeth. If plaque isn't removed daily by brushing and flossing, it hardens into tartar (calculus), which can only be removed by a professional dental cleaning. Tartar provides a rough surface where more plaque can accumulate, irritating the gums and leading to inflammation. At this stage, gingivitis is reversible with good oral hygiene and professional cleaning. You might notice your gums are red, swollen, and bleed easily when you brush or floss, but typically, there's no bone loss yet.
If gingivitis is ignored, the inflammation can spread below the gumline, infecting the supporting structures of the teeth. This is when it progresses to periodontitis, which literally means "inflammation around the tooth." In periodontitis, the chronic inflammation causes your body's immune system to attack the invading bacteria and, unfortunately, some of its own tissues. This leads to the formation of "pockets" – spaces that develop between the teeth and gums, filling with bacteria, plaque, and tartar. These pockets deepen over time, creating an environment where bacteria thrive and are protected from brushing. The bacteria and the inflammatory response then begin to break down the bone and connective tissue that hold your teeth in place.
As periodontitis advances, these supporting structures are progressively destroyed, leading to symptoms like persistent bad breath, receding gums, increased sensitivity, and eventually, loose teeth. In its most severe form, advanced periodontitis can result in tooth loss, impacting your ability to chew, speak, and even affecting your facial structure. The American Dental Association (ADA) emphasizes that timely diagnosis and intervention are critical to halting the progression of this disease and preserving your natural teeth.
Types / Variations of Periodontal Disease
Periodontal disease isn't a single condition but rather a spectrum of diseases, each with its own characteristics and progression. While gingivitis is the initial, reversible stage, periodontitis itself has several forms:
Chronic Periodontitis
This is the most common form of periodontal disease, typically affecting adults but can occur at any age. It's characterized by inflammation within the supporting tissues of the teeth, progressive attachment loss (gums pulling away from teeth), and bone loss. It usually progresses slowly, but periods of rapid progression can occur. Chronic periodontitis is directly linked to the accumulation of plaque and tartar. It's managed through non-surgical and surgical interventions to control the infection and prevent further damage.
Aggressive Periodontitis
A less common but more severe form, aggressive periodontitis typically affects otherwise clinically healthy individuals. It's characterized by rapid attachment loss and bone destruction, often with a familial aggregation (runs in families). Unlike chronic periodontitis, the amount of plaque and tartar present may not be proportionate to the severity of the tissue destruction. This form often requires more intensive and immediate treatment, sometimes involving systemic antibiotics. It can be localized (affecting only certain teeth) or generalized (affecting most teeth).
Necrotizing Periodontal Diseases
These are severe infections characterized by the death of gum tissue, ligaments, and bone. They include necrotizing ulcerative gingivitis (NUG), necrotizing ulcerative periodontitis (NUP), and necrotizing stomatitis. These conditions are extremely painful and characterized by ulcerated, necrotic (dead) gum tissue, severe bleeding, and often a foul odor. They are most commonly seen in individuals with compromised immune systems, such as those with HIV/AIDS, malnutrition, or severe stress. Immediate and aggressive treatment is crucial to prevent rapid tissue destruction and potential systemic complications.
Periodontitis as a Manifestation of Systemic Diseases
In some cases, periodontal disease is a symptom or complication of a systemic condition that affects the body's inflammatory response or immune system. Examples include:
- Diabetes: Individuals with uncontrolled diabetes are at a significantly higher risk for developing severe periodontitis due to impaired immune function and altered inflammatory responses.
- Cardiovascular Disease: The link between gum disease and heart conditions is increasingly recognized.
- Certain blood disorders: Conditions like leukemia can manifest with severe gum inflammation and bleeding.
- Genetic disorders: Diseases such as Down syndrome or Papillon-Lefèvre syndrome can predispose individuals to early-onset, severe periodontitis.
Periodontal Abscesses
These are localized collections of pus within the gum tissue, often associated with a periodontal pocket. They can be very painful, causing swelling, redness, and sensitivity. Treatment involves drainage of the abscess and often deep cleaning or surgical intervention.
Causes / Why It Happens
The primary cause of periodontal disease is bacterial plaque, a sticky, colorless film that constantly forms on your teeth. However, several factors contribute to its development and progression.
Bacterial Plaque and Tartar
- Plaque formation: Bacteria naturally reside in your mouth. When combined with food particles and saliva, they form plaque. If plaque isn't removed daily through effective brushing and flossing, it releases toxins that irritate the gum tissue, leading to inflammation (gingivitis).
- Tartar accumulation: Within 24-72 hours, soft plaque can harden into tartar (calculus) if not removed. Tartar is porous and rough, providing an ideal surface for more plaque to adhere and multiply, further irritating the gums and making it difficult to clean effectively. Only a dental professional can remove tartar.
Contributing Risk Factors
Beyond plaque, numerous factors can increase your susceptibility to periodontal disease or worsen its progression:
- Smoking and Tobacco Use: This is one of the most significant risk factors. Smoking impairs the immune system, making it harder for your gums to fight off infection, and restricts blood flow, hindering healing. Smokers are up to 7 times more likely to develop periodontitis than non-smokers, and the disease tends to be more severe and resistant to treatment.
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque and tartar to accumulate, directly leading to gum inflammation. The ADA recommends brushing for two minutes, twice a day, and flossing once daily.
- Genetics: Some individuals are genetically predisposed to periodontal disease. If your parents or grandparents had gum disease, you might be at a higher risk. This doesn't mean it's inevitable, but it underscores the importance of stringent preventive care.
- Systemic Diseases:
- Diabetes: People with diabetes are more prone to infections, including gum infections. Uncontrolled blood sugar levels impair the immune system and can worsen periodontitis. Conversely, severe periodontitis can make blood sugar control more difficult.
- Cardiovascular Disease: Research indicates a strong link, though the exact mechanism is still being studied. Inflammation from periodontitis may contribute to systemic inflammation, potentially affecting blood vessels.
- Autoimmune diseases: Conditions like rheumatoid arthritis or lupus can affect the body's inflammatory response, potentially impacting gum health.
- HIV/AIDS: Individuals with compromised immune systems are highly susceptible to severe and rapidly progressing forms of periodontal disease, including necrotizing types.
- Hormonal Changes: Fluctuations in hormones, such as those during pregnancy, puberty, menstruation, or menopause, can make gums more sensitive and prone to inflammation. Pregnant women, for example, are susceptible to "pregnancy gingivitis."
- Certain Medications: Some drugs can cause dry mouth (xerostomia), reducing saliva's protective effects and increasing plaque buildup. Others, like anticonvulsants (e.g., phenytoin) or calcium channel blockers (e.g., nifedipine), can cause gum overgrowth (gingival hyperplasia), making cleaning difficult and trapping plaque.
- Stress: Stress can weaken the immune system, making it harder for the body to fight off infections, including periodontal bacteria.
- Poor Nutrition: A diet lacking essential nutrients, particularly Vitamin C, can compromise the immune system and make gum tissue less resilient to infection.
- Clenching or Grinding Teeth (Bruxism): These habits can put excessive force on the supporting structures of the teeth, potentially accelerating the breakdown of bone and gum tissue already weakened by inflammation.
- Crooked Teeth or Poorly Fitting Dental Work: Teeth that are crowded, crooked, or poorly aligned can create areas that are difficult to clean, leading to plaque accumulation. Old, ill-fitting crowns or fillings can also trap plaque and irritate gums.
Pro Tip: Be honest with your dentist about your medical history and medications. This information is vital for them to assess your risk for periodontal disease and tailor your preventive and treatment plan.
Signs and Symptoms
Recognizing the signs and symptoms of periodontal disease early is critical for effective treatment and preventing irreversible damage. They can range from subtle to severe, depending on the stage of the disease.

Early Signs (Gingivitis)
- Red, swollen, or tender gums: Healthy gums are typically pink and firm.
- Bleeding gums: Gums that bleed easily when brushing, flossing, or even eating hard foods are a significant warning sign. This is often one of the first indicators.
- Persistent bad breath (halitosis): Caused by the accumulation of bacteria in the mouth.
- Gums that look shiny: Due to swelling and inflammation.
Advanced Signs (Periodontitis)
If gingivitis progresses to periodontitis, you might experience the following in addition to the early signs:
- Receding gums: Gums pull away from the teeth, making teeth look longer than usual. This exposes the tooth roots, which can lead to increased sensitivity.
- Formation of deep pockets: Spaces between your teeth and gums where bacteria thrive and are difficult to clean. Your dentist measures these pockets during examinations.
- Pus between your teeth and gums: A sign of active infection.
- Changes in the way your teeth fit together when you bite: As bone and ligament support weaken, teeth can shift.
- Loose or shifting teeth: This is a late sign, indicating significant bone loss. In severe cases, teeth may become so loose they fall out or need to be extracted.
- Changes in the fit of partial dentures: If supporting structures change, dentures may no longer fit properly.
- Persistent bad taste in your mouth: Another indicator of bacterial presence and infection.
Pro Tip: Don't ignore bleeding gums, even if it's just a small amount. Many people mistakenly think it's normal, but it's a primary indicator that something is wrong. Schedule a dental check-up immediately if you notice this symptom.
Treatment Options
The good news is that periodontal disease is treatable, especially when caught early. Treatment aims to control the infection, prevent further damage, and restore the health of your gums and supporting bone. The approach depends on the type and severity of the disease. A periodontist, a dental specialist focusing on the diagnosis, treatment, and prevention of gum disease, is often consulted for moderate to severe cases.
Non-Surgical Treatments
These are typically the first line of treatment for gingivitis and mild to moderate periodontitis.
1. Scaling and Root Planing (SRP)
- What it is: Often referred to as a "deep cleaning," SRP is a non-surgical procedure performed by a dentist or dental hygienist. Scaling involves meticulously removing plaque and tartar from above and below the gumline. Root planing then smooths the root surfaces, removing bacterial toxins and making it harder for new plaque to attach. This helps the gums reattach to the cleaned root surfaces.
- Pros: Highly effective for early to moderate periodontitis, less invasive than surgery, generally less expensive, performed under local anesthesia.
- Cons: May cause temporary sensitivity, discomfort, or mild bleeding. Not effective for very deep pockets or advanced bone loss. Usually requires multiple appointments (often one quadrant per visit).
- Cost: $200 - $600 per quadrant (there are typically 4 quadrants in the mouth). Total cost can range from $800 - $2,400 for a full mouth deep cleaning without insurance.
2. Antibiotics
- What it is: Can be used in conjunction with SRP to help control bacterial infection.
- Topical antibiotics: Applied directly into the periodontal pockets in the form of gels, chips, or antibiotic-filled fibers. These release medication slowly over time.
- Oral antibiotics: Prescribed in pill form to fight infection throughout the body. Used for more severe or aggressive cases.
- Pros: Can effectively reduce bacterial load and inflammation, aid healing.
- Cons: Topical antibiotics have limited reach. Oral antibiotics can have side effects (e.g., digestive upset), may contribute to antibiotic resistance, and are not a standalone treatment but an adjunct.
- Cost: Topical antibiotics (e.g., Arestin) can add $50 - $150 per site. Oral antibiotics are typically $10 - $50 for a prescription.
3. Antiseptic Mouthrinses
- What it is: Prescribed mouthwashes containing ingredients like chlorhexidine can help control plaque and gingivitis, particularly after procedures.
- Pros: Easy to use, can help manage bacterial load.
- Cons: Can stain teeth with prolonged use, temporary taste alteration. Not a substitute for mechanical cleaning.
- Cost: $15 - $30 for a prescription bottle.
Surgical Treatments
When non-surgical treatments are insufficient to manage deep pockets or significant bone loss, surgical interventions become necessary. These procedures are typically performed by a periodontist.
1. Flap Surgery (Pocket Reduction Surgery)
- What it is: The periodontist lifts back sections of gum tissue to gain direct access to the deeper plaque and tartar. The diseased tissue is removed, and the root surfaces are thoroughly cleaned. In some cases, irregular bone surfaces are smoothed to make it harder for bacteria to accumulate and easier for the gums to reattach. The gum tissue is then repositioned and sutured back into place.
- Pros: Reduces pocket depth, making it easier to clean, controls infection, can help prevent further bone loss.
- Cons: More invasive, requires a longer recovery time, potential for gum recession (making teeth look longer), temporary sensitivity.
- Cost: $1,000 - $3,000 per quadrant, depending on complexity and location.
2. Bone Grafting
- What it is: If periodontal disease has destroyed bone, a bone graft can be used to regenerate lost bone. Graft material can come from your own body (autograft), a synthetic material (alloplastic), or donated human or animal bone (allograft/xenograft). The graft material serves as a scaffold for your body's natural bone growth.
- Pros: Can help stabilize loose teeth, prevent tooth loss, and prepare for future dental implants.
- Cons: Significant recovery time, potential for graft failure, higher cost.
- Cost: $800 - $4,000 per site, depending on material and extent.
3. Soft Tissue Grafts (Gum Grafts)
- What it is: Used to treat gum recession, where the gum tissue has pulled away from the tooth, exposing the root. A small piece of gum tissue is taken from another area of your mouth (often the roof) or a donor source and attached to the receding area.
- Pros: Covers exposed roots, reduces sensitivity, protects roots from decay, improves aesthetics, prevents further recession.
- Cons: Can be uncomfortable at the donor site, requires careful healing.
- Cost: $600 - $2,000 per tooth/site.
4. Guided Tissue Regeneration (GTR)
- What it is: This surgical procedure helps regenerate lost bone and gum tissue. After cleaning the root surfaces, a small piece of mesh-like material (often bioresorbable) is placed between the bone and gum tissue. This barrier prevents gum tissue from growing into the area where bone should be, allowing slower-growing bone cells time to regenerate.
- Pros: Can encourage the growth of new bone and connective tissue.
- Cons: More complex procedure, longer healing time, not always predictable.
- Cost: $1,000 - $4,000 per site, often combined with bone grafting.
5. Dental Implants
- What it is: While not a treatment for periodontal disease itself, if teeth are lost due to advanced periodontitis, dental implants are often the preferred option for tooth replacement once the gum disease is controlled. Implants are titanium posts surgically placed into the jawbone, acting as artificial tooth roots.
- Pros: Long-lasting, feel like natural teeth, preserve bone structure, highly successful.
- Cons: Significant cost, surgical procedure, requires healthy bone and gums for placement.
- Cost: $3,000 - $6,000 per implant (not including crown or abutment).
6. Laser Therapy
- What it is: Lasers can be used as an adjunct to traditional treatments like SRP. They are used to remove diseased tissue, sterilize pockets, and reduce bacteria. Examples include the LANAP (Laser Assisted New Attachment Procedure) protocol.
- Pros: May be less invasive in some cases, potentially faster healing, less bleeding.
- Cons: Efficacy for true regeneration compared to traditional surgery is debated among some specialists, can be more expensive, not universally available.
- Cost: Often adds $500 - $1,500 to the cost of SRP or other surgical procedures.
Comparison of Periodontal Treatments (General Overview)
| Treatment Type | Primary Goal | Invasiveness | Typical Cost Range (per quadrant/site) | Recovery Time | Efficacy for Advanced Disease |
|---|---|---|---|---|---|
| Scaling & Root Planing (SRP) | Remove plaque/tartar below gumline, smooth roots | Low | $200 - $600 | Few days | Moderate |
| Antibiotics (Adjunctive) | Reduce bacterial infection | Very Low | $10 - $150 | None | Moderate (adjunct) |
| Flap Surgery | Reduce pocket depth, clean roots directly | Medium | $1,000 - $3,000 | 1-2 weeks | High |
| Bone Grafting | Regenerate lost jawbone | High | $800 - $4,000 | Several months | High |
| Soft Tissue Graft | Cover exposed roots, increase gum tissue | Medium | $600 - $2,000 | 1-2 weeks | High |
| Guided Tissue Regeneration | Promote new bone/tissue growth | High | $1,000 - $4,000 | Several months | High |
| Laser Therapy (Adjunctive) | Remove diseased tissue, sterilize | Low-Medium | Adds $500 - $1,500 to other treatments | Few days | Moderate (adjunct) |
Step-by-Step Process: What to Expect During Treatment
Let's walk through what you can generally expect during a common periodontal treatment like Scaling and Root Planing (SRP), which is often the first step, and a more advanced surgical procedure.
Scaling and Root Planing (Deep Cleaning) Process
- Initial Examination and Diagnosis: Your general dentist or periodontist will perform a thorough examination, including measuring pocket depths around your teeth (known as periodontal probing), taking X-rays to assess bone loss, and reviewing your medical history. They will determine if SRP is the appropriate treatment.
- Anesthesia: Before starting, your dentist or hygienist will numb the areas of your mouth to be treated using a local anesthetic. This ensures you remain comfortable throughout the procedure. For extensive SRP, your mouth may be divided into quadrants, treating one or two at a time over separate appointments.
- Scaling: Using specialized dental instruments (ultrasonic scalers and hand scalers), the hygienist or dentist will meticulously remove plaque and tartar from the crown of your teeth and below the gumline, inside the periodontal pockets.
- Root Planing: After scaling, the root surfaces of your teeth are smoothed. This removes any remaining bacterial toxins and rough spots, making it more difficult for plaque to adhere in the future and allowing the gum tissue to reattach more firmly to the tooth.
- Irrigation (Optional): Some practitioners may flush the pockets with an antiseptic solution (like chlorhexidine) after scaling and root planing to further reduce bacteria.
- Antibiotic Placement (Optional): If indicated, localized antibiotic medication (e.g., Arestin®) in the form of a gel or small chip might be placed directly into the deeper pockets to continue fighting bacteria and promote healing.
- Post-Procedure Instructions: You'll receive specific instructions on how to care for your mouth, manage sensitivity, and what to expect during recovery.
- Follow-up Appointment: A follow-up visit, typically 4-6 weeks after the last SRP appointment, is crucial to assess healing, re-measure pocket depths, and establish a maintenance schedule.
Flap Surgery (Pocket Reduction) Process
- Initial Consultation and Planning: A periodontist will thoroughly evaluate your condition, discuss the surgical options, explain the benefits and risks, and ensure you are a suitable candidate.
- Local Anesthesia: The area to be treated will be completely numbed using local anesthetic. Sedation options (oral, nitrous oxide, or IV sedation) may also be available for patient comfort.
- Incision and Flap Creation: The periodontist makes small incisions in the gum tissue to gently lift it back, creating a "flap." This provides direct access to the tooth roots and underlying bone.
- Cleaning and Root Planing: With direct visualization, the periodontist meticulously removes all plaque, tartar, and diseased tissue from the root surfaces. Any rough bone surfaces are also smoothed to reduce areas where bacteria can accumulate.
- Bone Reshaping (Osseous Surgery - Optional): If necessary, minor reshaping of the bone around the teeth may be performed to eliminate defects or reduce shallow bone craters, making the gum tissue lay flatter.
- Bone or Tissue Grafting (Optional): If there is significant bone loss or gum recession, bone or soft tissue grafting procedures may be performed at this stage to encourage regeneration.
- Repositioning and Suturing: The gum flap is repositioned to fit snugly around the teeth and secured with sutures (stitches). A periodontal dressing (a soft, putty-like material) may be placed over the surgical site to protect it during the initial healing phase.
- Post-Operative Instructions: You'll receive detailed instructions for post-surgical care, including pain management, dietary restrictions, oral hygiene modifications, and medication prescriptions (antibiotics, pain relievers).
- Follow-up Appointments: Several follow-up appointments are scheduled: typically 1-2 weeks for suture removal and initial check-up, and subsequent visits to monitor healing and ensure proper long-term maintenance.
Cost and Insurance
Understanding the financial aspect of periodontal disease treatment is crucial for patients in the US. Costs can vary significantly based on the severity of your condition, the specific treatments required, the geographic location of your dental office, and the experience of the dental professional (general dentist vs. periodontist).
Average US Price Ranges (Without Insurance)
| Treatment Type | Average Low Cost | Average Mid Cost | Average High Cost | Notes |
|---|---|---|---|---|
| Scaling & Root Planing (per quadrant) | $200 | $400 | $600 | Usually 4 quadrants for full mouth; total $800 - $2,400 |
| Localized Antibiotic Placement (per site) | $50 | $100 | $150 | For deep pockets; typically used with SRP |
| Flap Surgery (Pocket Reduction, per quadrant) | $1,000 | $2,000 | $3,000 | May involve multiple quadrants; total $4,000 - $12,000+ |
| Bone Graft (per site) | $800 | $2,500 | $4,000 | Can be combined with other surgeries |
| Soft Tissue Graft (per tooth/site) | $600 | $1,300 | $2,000 | Often for gum recession on specific teeth |
| Guided Tissue Regeneration (per site) | $1,000 | $2,500 | $4,000 | Often includes bone graft material |
| Periodontal Maintenance (per visit) | $100 | $150 | $250 | After initial treatment; usually every 3-4 months |
| Extraction of Periodontally Involved Tooth | $75 (simple) | $250 (surgical) | $600 (complex) | May be necessary if teeth are too damaged to save |
| Full Mouth Rehabilitation (Severe Cases) | $15,000 | $30,000 | $75,000+ | Involves multiple surgeries, extractions, implants, etc., over time |
These are general ranges. Costs in major metropolitan areas (e.g., New York, Los Angeles) tend to be higher than in rural areas. A specialist (periodontist) may also charge more than a general dentist.
Insurance Coverage Details
Dental insurance coverage for periodontal disease treatment varies widely:

- Preventive Care (Routine Cleanings & Exams): Most plans cover 100% of two routine cleanings and exams per year, which are crucial for prevention.
- Basic Procedures (Scaling & Root Planing): Many dental insurance plans classify SRP as a "basic" procedure and may cover 50% to 80% of the cost after your deductible is met. However, they often limit coverage to one SRP treatment per few years or per quadrant.
- Major Procedures (Surgical Treatments): Surgical procedures like flap surgery, bone grafts, and gum grafts are typically considered "major" procedures. Coverage for these is often lower, usually 20% to 50%, and subject to your annual maximum benefit (which can range from $1,000 to $2,500 per year).
- Waiting Periods: Many plans have waiting periods (e.g., 6-12 months) before they will cover major procedures. This means you might pay 100% out-of-pocket if you need immediate surgery after starting a new plan.
- Pre-authorization: For extensive or expensive treatments, your dentist or periodontist will likely submit a pre-authorization to your insurance company. This estimates what your plan will cover, preventing unexpected costs.
- HMO vs. PPO:
- PPO (Preferred Provider Organization): Offers more flexibility in choosing providers. You can see any dentist, but you'll pay less if you choose one in-network. They usually have deductibles and co-pays.
- HMO (Health Maintenance Organization) / DHMO: Requires you to choose a primary dentist within their network and get referrals for specialists. Generally lower monthly premiums and fixed co-pays, but less choice.
- Medicaid/Medicare: Medicaid typically covers basic dental care for children and sometimes limited emergency care for adults. Medicare generally does NOT cover routine dental care or most periodontal treatments, though some Medicare Advantage plans (Part C) may include dental benefits.
Payment Plans and Financing Options
- In-Office Payment Plans: Many dental offices offer interest-free payment plans for a portion of the treatment cost.
- Third-Party Financing: Companies like CareCredit or LendingClub offer specialized healthcare credit cards with deferred interest options if paid within a certain timeframe, or low-interest installment plans.
- Dental Schools: University dental schools often provide treatment at a reduced cost, as procedures are performed by students under the close supervision of experienced faculty.
- Flexible Spending Accounts (FSAs) and Health Savings Accounts (HSAs): If you have an FSA or HSA through your employer, you can use these tax-advantaged accounts to pay for qualified dental expenses.
Pro Tip: Always get a detailed treatment plan with associated costs from your dentist or periodontist, and then contact your insurance provider directly to confirm your coverage and out-of-pocket expenses before beginning extensive treatment.
Recovery and Aftercare
Proper recovery and diligent aftercare are essential for successful outcomes and preventing recurrence of periodontal disease, regardless of whether you undergo non-surgical or surgical treatment.
After Non-Surgical Treatment (Scaling and Root Planing)
- Discomfort and Sensitivity: It's normal to experience some gum soreness, tenderness, and increased tooth sensitivity to hot and cold temperatures for a few days to a week. Over-the-counter pain relievers (e.g., ibuprofen, acetaminophen) can help manage discomfort. Sensitivity toothpaste can also be beneficial.
- Bleeding: You might notice slight bleeding when brushing or flossing for a day or two. This should subside.
- Eating: Avoid very hot, cold, spicy, or crunchy foods for the first 24-48 hours. Stick to soft foods.
- Oral Hygiene: Continue brushing gently with a soft-bristled toothbrush and flossing, being careful around sensitive areas. Your hygienist might recommend an antiseptic mouthrinse for a short period.
- Follow-up: A crucial follow-up appointment (typically 4-6 weeks) is needed to assess healing, re-measure pockets, and plan your ongoing periodontal maintenance schedule.
After Surgical Treatment (e.g., Flap Surgery, Grafts)
Recovery from periodontal surgery is more involved and requires strict adherence to post-operative instructions.
- Pain Management: Your periodontist will likely prescribe stronger pain medication for the first few days, along with antibiotics to prevent infection. Over-the-counter pain relievers can be used as discomfort lessens.
- Swelling: Some swelling is common. Applying an ice pack to the outside of your face for 15-20 minutes on, 20-30 minutes off, during the first 24-48 hours can help reduce it.
- Bleeding: Minor oozing or bleeding is normal for the first day. Bite gently on a piece of gauze if bleeding persists, or apply pressure to the area. Avoid spitting or rinsing vigorously, as this can dislodge blood clots.
- Diet: Stick to a soft diet for several days to weeks, depending on the surgery. Avoid chewing on the surgical side. Avoid hot, spicy, acidic, or crunchy foods.
- Oral Hygiene: You'll be given specific instructions. This often involves very gentle brushing of non-surgical areas and using a prescribed antiseptic mouthrinse (like chlorhexidine) to keep the surgical site clean without disturbing it. Avoid flossing the surgical area until instructed.
- Activity: Avoid strenuous exercise for the first few days post-surgery, as it can increase bleeding and swelling.
- Sutures and Periodontal Dressing: Sutures (stitches) are usually removed in 1-2 weeks. A periodontal dressing, if applied, provides protection and comfort and is typically removed at the first follow-up.
- Smoking: Absolutely avoid smoking during the healing period, as it severely impairs healing and increases the risk of complications.
- Follow-up Appointments: Multiple follow-up visits are essential to monitor healing, remove sutures, and adjust your long-term maintenance plan. Complete healing can take several weeks to months.
Long-Term Periodontal Maintenance
Regardless of the treatment, ongoing periodontal maintenance is critical to prevent recurrence. This involves:
- Frequent Professional Cleanings: Typically every 3-4 months (compared to 6 months for healthy individuals), these cleanings focus on removing new plaque and tartar buildup from pockets and monitoring your gum health.
- Excellent Home Care: Consistent and meticulous brushing twice a day with a soft-bristled brush, daily flossing, and potentially interdental brushes or water flossers are non-negotiable.
- Regular Dental Check-ups: Your general dentist and periodontist will work together to monitor your condition and make adjustments to your care plan as needed.
Prevention
Preventing periodontal disease is far easier, less painful, and less costly than treating it. The cornerstones of prevention are excellent oral hygiene and regular professional dental care.
1. Maintain Excellent Oral Hygiene
- Brush Twice Daily: Brush your teeth for two minutes, twice a day, using a soft-bristled toothbrush. Consider an electric toothbrush, which can be more effective at removing plaque. Use fluoride toothpaste. The ADA seal of acceptance indicates a product has met strict safety and efficacy standards.
- Floss Daily: Floss at least once a day to remove food particles and plaque from between your teeth and under the gumline, areas your toothbrush can't reach. If traditional floss is difficult, consider a water flosser or interdental brushes.
- Use Mouthwash (Optional but helpful): An antiseptic mouthwash can help reduce bacteria that cause plaque and gingivitis. Consult your dentist for recommendations.
- Clean Your Tongue: Use a tongue scraper or your toothbrush to clean your tongue daily. This helps remove bacteria and food debris, reducing bad breath.
2. Regular Dental Check-ups and Professional Cleanings
- Visit Your Dentist Every 6 Months: Regular check-ups allow your dentist or hygienist to remove plaque and tartar buildup, which you can't remove at home. They can also identify early signs of gum disease before it progresses.
- Periodontal Evaluations: During your check-up, the dentist or hygienist will perform a periodontal probing, measuring the depth of the pockets around your teeth. This helps track gum health and detect issues early.
3. Adopt a Healthy Lifestyle
- Quit Smoking: This is arguably the single most impactful step you can take to prevent and manage periodontal disease. Smoking dramatically increases your risk and hinders treatment success. Resources are available to help you quit.
- Manage Systemic Diseases: If you have conditions like diabetes, control your blood sugar levels diligently. Work with your physician to manage any health issues that can impact your oral health.
- Eat a Balanced Diet: A diet rich in fruits, vegetables, and whole grains provides essential nutrients for your immune system and overall health. Limit sugary foods and drinks, which feed plaque-causing bacteria.
- Reduce Stress: Chronic stress can weaken your immune system, making you more vulnerable to infections, including gum disease. Practice stress-reduction techniques.
- Avoid Clenching and Grinding (Bruxism): If you grind or clench your teeth, discuss this with your dentist. They might recommend a nightguard to protect your teeth and supporting structures.
Pro Tip: Don't wait for pain to visit the dentist. Periodontal disease often progresses silently in its early stages. Regular preventive care is your best defense.
Risks and Complications
Left untreated, periodontal disease can have far-reaching and severe consequences, not only for your oral health but for your entire body.
Oral Health Complications
- Tooth Loss: This is the most direct and devastating complication. As bone and connective tissue are destroyed, teeth loosen and eventually fall out or require extraction.
- Difficulty Chewing and Speaking: Missing teeth and shifting teeth can impair your ability to eat a variety of foods and speak clearly.
- Changes in Facial Structure: Loss of teeth and jawbone can lead to changes in your facial appearance, including a "sunken" look.
- Dental Abscesses: Infections within the gum pockets can lead to painful abscesses.
- Increased Sensitivity: Receding gums expose sensitive tooth roots, leading to discomfort.
- Aesthetic Concerns: Gum recession, shifting teeth, and persistent bad breath can significantly impact self-confidence.

Systemic Health Complications: Can Gum Disease Kill You?
While periodontal disease doesn't directly "kill you" in the way an acute, rapidly fatal infection might, its chronic inflammatory nature and the entry of bacteria into the bloodstream contribute to and exacerbate several serious systemic health conditions, indirectly impacting your lifespan and quality of life. The answer to "can gum disease kill you" is therefore complex: it's not a direct cause of death, but it's a significant risk factor and contributor to diseases that are lethal.
- Cardiovascular Disease (Heart Attack and Stroke): This is one of the most well-established links. The inflammation associated with periodontitis may contribute to inflammation in blood vessels, potentially leading to atherosclerosis (hardening of the arteries). Bacteria from infected gums can also enter the bloodstream, travel to the heart, and contribute to the formation of clots or infect damaged heart valves (infective endocarditis). Studies suggest a significantly higher risk of heart attack and stroke in people with severe periodontitis.
- Diabetes: There's a bidirectional relationship. People with diabetes are more susceptible to periodontitis, and severe periodontitis can make blood sugar control more difficult. Uncontrolled gum infection can increase insulin resistance, making diabetes harder to manage and increasing the risk of diabetic complications.
- Respiratory Diseases: Oral bacteria from infected gums can be aspirated (breathed in) into the lungs, potentially leading to respiratory infections such as pneumonia (especially hospital-acquired pneumonia), bronchitis, and chronic obstructive pulmonary disease (COPD) exacerbations, particularly in older adults and those with compromised immune systems.
- Adverse Pregnancy Outcomes: Pregnant women with periodontitis have a higher risk of preterm birth and low birth weight babies. The inflammation and bacteria from the gums are thought to potentially trigger premature labor.
- Rheumatoid Arthritis: There's evidence of a link between periodontal disease and rheumatoid arthritis, an autoimmune disease. The same inflammatory pathways and bacterial presence may play a role in both conditions.
- Certain Cancers: Some research suggests a possible association between periodontitis and an increased risk of certain cancers, including oral cancer, esophageal cancer, and pancreatic cancer, though more research is needed to establish definitive causal links.
- Dementia and Alzheimer's Disease: Emerging research is exploring a potential connection between chronic inflammation from periodontal disease and an increased risk of cognitive decline and neurodegenerative diseases like Alzheimer's. Bacteria or inflammatory mediators from the mouth may potentially cross the blood-brain barrier.
- Kidney Disease: Chronic periodontitis has been linked to an increased risk of chronic kidney disease and may worsen kidney function in those already affected.
The systemic implications underscore why the ADA and other health organizations stress the importance of treating periodontal disease not just for oral health, but as a critical component of overall health management. Ignoring gum disease is akin to ignoring a chronic infection elsewhere in the body – it can have detrimental effects throughout your system.
Children / Pediatric Considerations
While chronic periodontitis is primarily an adult disease, periodontal conditions can affect children and adolescents, though less commonly. Pediatric periodontitis can manifest in various forms and requires early diagnosis and specialized care.
Types of Periodontal Disease in Children
- Gingivitis: This is the most common periodontal condition in children, often caused by inadequate brushing and flossing. Like adults, it presents as red, swollen, bleeding gums and is reversible with improved oral hygiene and professional cleaning.
- Chronic Periodontitis: While rare, some adolescents can develop chronic periodontitis, similar to the adult form, often associated with significant plaque and tartar accumulation and sometimes exacerbated by genetic predisposition or systemic factors.
- Aggressive Periodontitis (formerly Early-Onset Periodontitis): This is a more severe form, often familial, characterized by rapid bone and attachment loss. It can be localized (affecting incisors and first molars) or generalized (affecting most teeth). It often occurs in children and adolescents who are otherwise healthy and have minimal plaque, suggesting a strong genetic component or specific aggressive bacteria.
- Periodontitis as a Manifestation of Systemic Diseases: In some children, severe periodontal disease can be a sign of an underlying systemic condition, such as:
- Immune disorders: (e.g., severe congenital neutropenia, leukocyte adhesion deficiency).
- Genetic disorders: (e.g., Down syndrome, Papillon-Lefèvre syndrome).
- Diabetes mellitus.
What Parents Should Look For
Parents should be vigilant for:
- Red, swollen, or tender gums.
- Gums that bleed easily during brushing or flossing.
- Persistent bad breath.
- Pus around the teeth and gums.
- Receding gums, making teeth look longer.
- Loose baby or permanent teeth (not associated with normal exfoliation).
- Food packing between teeth.
- Sensitivity to hot or cold.
Guidance for Parents
- Emphasize Excellent Oral Hygiene: Teach children proper brushing techniques as soon as their first tooth erupts. Supervise brushing until they are 7-8 years old. Introduce flossing once teeth begin to touch.
- Regular Dental Check-ups: Ensure children visit the dentist for routine check-ups and cleanings twice a year. Pediatric dentists are trained to recognize early signs of gum disease in children.
- Balanced Diet: Limit sugary snacks and drinks that contribute to plaque formation. Encourage a diet rich in fruits, vegetables, and whole grains.
- Early Intervention: If a child is diagnosed with aggressive periodontitis, immediate treatment by a periodontist and/or pediatric dentist is crucial. This may involve scaling and root planing, antibiotics, and close monitoring. Referral to a physician may also be necessary to rule out underlying systemic conditions.
- Family History: Inform your dentist if there's a family history of gum disease, as this can indicate a higher risk for your child.
Pediatric periodontal disease, especially aggressive forms, requires prompt and specialized attention to prevent significant tooth loss and long-term oral health complications.
Cost Breakdown
To reiterate and provide a more comprehensive view of the financial commitment, here's a detailed cost breakdown for various stages and treatments of periodontal disease in the US. Remember, these are averages, and your specific costs will depend on your location, the severity of your disease, the practitioner's fees, and your insurance coverage.
Average US Costs (Without Insurance)
| Item/Procedure | Low Range | Mid Range | High Range | Notes |
|---|---|---|---|---|
| Initial Exam & X-rays | $50 - $150 | $150 - $300 | $300 - $500 | Includes comprehensive exam, full mouth X-rays or panoramic X-ray, periodontal probing. |
| Routine Cleaning (Prophylaxis) - Prevention | $75 - $125 | $125 - $200 | $200 - $250 | Covered 100% by most insurance plans. This is for healthy gums, not active disease. |
| Scaling & Root Planing (SRP) per quadrant | $200 - $350 | $350 - $500 | $500 - $600 | For a full mouth (4 quadrants): $800 - $2,400. Often requires multiple appointments. |
| Periodontal Maintenance (after SRP) per visit | $100 - $150 | $150 - $200 | $200 - $250 | Recommended every 3-4 months indefinitely after deep cleaning to prevent recurrence. |
| Localized Antibiotic (e.g., Arestin) per site | $50 - $80 | $80 - $120 | $120 - $150 | Often used as an adjunct to SRP in specific deep pockets. |
| Flap Surgery (Pocket Reduction) per quadrant | $1,000 - $2,000 | $2,000 - $3,000 | $3,000 - $4,000 | For a full mouth (4 quadrants): $4,000 - $16,000+. Can be significantly more if bone/tissue grafting is combined. |
| Bone Grafting per site | $800 - $2,000 | $2,000 - $3,000 | $3,000 - $4,000+ | Varies widely based on graft material (synthetic, cadaver, patient's own bone) and extent of defect. Often combined with other surgeries. |
| Soft Tissue Graft (Gum Graft) per tooth/site | $600 - $1,200 | $1,200 - $1,800 | $1,800 - $2,500+ | Depends on the technique (connective tissue graft, free gingival graft, pedicle graft) and donor site. |
| Guided Tissue/Bone Regeneration (GTR/GBR) per site | $1,000 - $2,500 | $2,500 - $3,500 | $3,500 - $4,500+ | Often includes the cost of bone graft material and barrier membrane. |
| Laser Periodontal Therapy (LANAP/LAPIP) per quadrant (adjunct) | $500 - $1,000 | $1,000 - $1,500 | $1,500 - $2,000 | Usually an additional cost on top of SRP or other surgical procedures. Full mouth: $2,000 - $8,000+. |
| Tooth Extraction (periodontally involved) | $75 - $200 (simple) | $200 - $400 (surgical) | $400 - $600+ (complex/wisdom) | If the tooth cannot be saved due to severe bone loss. |
| Dental Implant (single tooth, not including crown) | $3,000 - $4,500 | $4,500 - $6,000 | $6,000 - $8,000+ | If a tooth is lost and needs replacement. This is for the implant post placement only, crown and abutment are additional. Full cost with crown: $4,000 - $8,000+. |
With vs. Without Insurance
- Without Insurance: You will pay the full cash price as listed above. Many offices offer a discount for upfront cash payment.
- With Insurance: Your out-of-pocket costs will depend heavily on your specific plan's coverage, deductible, co-insurance, and annual maximums.
- Deductible: An amount you must pay before your insurance starts to cover costs (e.g., $50-$100 annually).
- Co-insurance: The percentage of the cost you are responsible for after meeting your deductible (e.g., 20% for basic, 50% for major procedures).
- Annual Maximum: The total amount your insurance will pay in a year (e.g., $1,000-$2,500). Once you hit this, you pay 100% out-of-pocket.
- Waiting Periods: Crucial for major procedures; you might have no coverage for these during the first 6-12 months of your plan.
Example Scenario:
-
Treatment: Full mouth Scaling and Root Planing (4 quadrants) at $400/quad = $1,600 total.
-
Insurance Coverage: 80% for basic procedures after a $50 deductible.
-
Your Cost: $50 (deductible) + (20% of $1,600) = $50 + $320 = $370.
-
Insurance Pays: $1,600 - $370 = $1,230. This is well within a typical annual maximum.
-
Treatment: Flap Surgery for 2 quadrants at $2,500/quad = $5,000 total.
-
Insurance Coverage: 50% for major procedures after a $50 deductible, with an annual maximum of $1,500.
-
Your Cost: $50 (deductible) + $1,500 (insurance max) = $1,550 covered by insurance, but you'll pay the remainder. So, you pay $5,000 - $1,500 = $3,500.
-
Insurance Pays: $1,500 (capped at annual maximum).
As seen, for major procedures, even with insurance, a significant portion often remains your responsibility.
Payment Plans and Financing Options
- In-house financing: Many dental practices offer interest-free payment plans, allowing you to spread out payments over a few months.
- CareCredit/LendingClub: These healthcare credit cards offer promotional interest-free periods (e.g., 6, 12, 18, 24 months) if the balance is paid in full by the end of the term. Be cautious, as high-interest rates can apply retroactively if not paid off.
- Dental Schools: As mentioned, dental schools can offer significantly reduced rates for complex cases, as students perform the work under close supervision.
- Community Dental Clinics: Some non-profit or government-subsidized clinics offer services on a sliding scale based on income.
Cost-Saving Tips
- Preventive Care: The best cost-saving tip is to prevent the disease from advancing. Regular cleanings and excellent home care are much cheaper than surgeries.
- Comparison Shop: Get quotes from a few different dentists or periodontists. Fees can vary.
- Maximize Insurance Benefits: Understand your plan, hit your deductible early, and spread out major treatments over two calendar years if your annual maximum is low.
- Use FSAs/HSAs: Contribute to these accounts if available through your employer, as they allow you to pay for healthcare costs with pre-tax dollars.
- Discuss Options: Always have an open conversation with your dental team about financial concerns and available payment options.
Frequently Asked Questions
H3: What is a periodontist and when do I need to see one?
A periodontist is a dentist who specializes in the prevention, diagnosis, and treatment of periodontal disease, and in the placement of dental implants. They have completed at least three additional years of specialized training beyond dental school. You should see a periodontist if your general dentist diagnoses you with moderate to severe periodontitis, if you have aggressive or necrotizing forms of gum disease, or if you require advanced surgical treatments like bone or gum grafts.

H3: Is periodontal disease contagious?
Periodontal disease itself is not considered contagious in the way a cold or flu is. However, the specific bacteria that contribute to gum disease can be transmitted through saliva sharing (e.g., sharing utensils, kissing). While bacteria can be shared, developing the disease depends on an individual's immune response, oral hygiene, and risk factors like genetics or smoking.
H3: How long does it take to treat periodontal disease?
The duration of treatment varies greatly. Gingivitis can often be resolved within a few weeks with professional cleaning and improved home care. Non-surgical treatments like scaling and root planing typically involve 1-4 appointments over 1-2 weeks, with follow-up assessments over 1-3 months. Surgical treatments can take several hours per procedure, with recovery lasting weeks to months, and the entire treatment plan for advanced cases often spans several months to over a year, followed by lifelong maintenance.
H3: Is periodontal disease painful?
In its early stages (gingivitis), periodontal disease is often painless, which is why many people don't realize they have it. As it progresses to periodontitis, you might experience sensitivity, tenderness, or pain when chewing, especially as teeth loosen or abscesses form. Surgical treatments involve local anesthesia, so you shouldn't feel pain during the procedure, but post-operative discomfort is common and managed with medication.
H3: Can periodontal disease be cured?
Gingivitis, the early stage, is reversible and can be "cured" with proper treatment and oral hygiene. Periodontitis, however, is a chronic disease that cannot be fully cured because the bone and attachment loss are often irreversible. The goal of treatment for periodontitis is to halt its progression, control the infection, reduce pocket depths, prevent further damage, and maintain oral health through ongoing periodontal maintenance.
H3: What happens if I don't treat my gum disease?
If left untreated, gum disease will progressively worsen. You will experience increasing bone loss, deeper periodontal pockets, gum recession, persistent bad breath, and eventually, teeth will become loose and fall out or need to be extracted. Untreated periodontal disease also significantly increases your risk for serious systemic health problems like heart disease, stroke, diabetes complications, and respiratory infections.
H3: Are there any natural remedies for gum disease?
While some natural remedies (like oil pulling or certain herbal rinses) are marketed for gum health, there is no scientific evidence that they can effectively treat or cure periodontal disease. These should never replace professional dental care. At best, some might offer mild antiseptic properties as an adjunct to professional treatment, but only your dentist can remove plaque and tartar and treat established infections. Relying solely on natural remedies for active gum disease can lead to severe and irreversible damage.
H3: What's the difference between a regular cleaning and a deep cleaning (SRP)?
A regular cleaning (prophylaxis) is for healthy gums, removing plaque and tartar above the gumline and slightly below, maintaining health. A deep cleaning (Scaling and Root Planing, SRP) is a therapeutic procedure for active periodontal disease. It involves meticulously removing plaque and tartar from deep below the gumline within periodontal pockets and smoothing the root surfaces to encourage gum reattachment. SRP targets infection and inflammation that has progressed beyond simple gingivitis.
H3: How often will I need follow-up cleanings after treatment?
After successful treatment for periodontitis (whether non-surgical or surgical), you will typically need periodontal maintenance appointments every 3-4 months. These are more frequent than standard 6-month cleanings because you are at higher risk for recurrence. These visits are crucial for monitoring your gum health, re-evaluating pocket depths, and meticulously cleaning below the gumline to prevent the disease from reactivating.
H3: Can periodontitis come back after treatment?
Yes, periodontitis can definitely come back after treatment if diligent aftercare and maintenance are not followed. It's a chronic condition, and ongoing management is key. Poor oral hygiene, skipping periodontal maintenance appointments, resuming smoking, or poorly controlled systemic conditions (like diabetes) can all lead to a relapse or progression of the disease. Lifelong commitment to your oral health routine is essential.
When to See a Dentist
Recognizing when to seek professional help is paramount in managing periodontal disease. Early intervention can prevent significant damage and more invasive treatments.
Clear Warning Signs That Need Immediate Attention
- Persistent Bleeding Gums: If your gums bleed consistently when you brush, floss, or even spontaneously, it's a primary indicator of gingivitis or periodontitis. Do not ignore it.
- Severe Gum Pain or Swelling: Sudden, throbbing pain, significant swelling, or pus oozing from your gums indicates an active infection or abscess that requires immediate attention.
- Loose or Shifting Teeth: This is a serious sign of advanced bone loss and means your teeth's supporting structures are severely compromised. Prompt evaluation is critical to try and save them.
- Persistent Bad Breath or Bad Taste: While occasional bad breath is common, if it's constant and doesn't improve with brushing, it could be a sign of bacterial infection from gum disease.
- Noticeable Gum Recession: If your teeth appear longer or you see roots exposed, your gums are receding, a sign of periodontitis. This can also lead to increased sensitivity.
- Changes in Your Bite or Denture Fit: If you notice your teeth no longer fit together comfortably when you bite, or if your partial dentures start to feel loose, it could indicate changes in your underlying bone structure due to gum disease.
Red Flags vs. Routine Care Guidance
- Red Flag (Emergency/Urgent): Severe, uncontrolled pain; rapid swelling; fever accompanied by oral symptoms; a tooth suddenly becoming very loose. These warrant contacting your dentist immediately or seeking emergency dental care.
- Warning Sign (Scheduled Appointment): Any of the persistent issues listed above (bleeding, bad breath, recession, mild discomfort). These should prompt you to schedule an appointment with your general dentist as soon as possible, ideally within a week.
- Routine Care Guidance: Even if you experience no symptoms, regular dental check-ups every six months are essential for preventing periodontal disease and catching any issues early. If you have a history of gum disease, your dentist or periodontist will likely recommend more frequent (e.g., 3-4 month) periodontal maintenance appointments.
Your oral health is an integral part of your overall well-being. Don't hesitate to contact your dental professional if you have any concerns about your gums or teeth. Early detection and treatment are your best defense against the destructive progression of periodontal disease.
Frequently Asked Questions
Medically Reviewed Content
This article was written by our dental health editorial team and reviewed for medical accuracy. Our content follows strict editorial guidelines for reliability and trustworthiness.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.
Related Articles
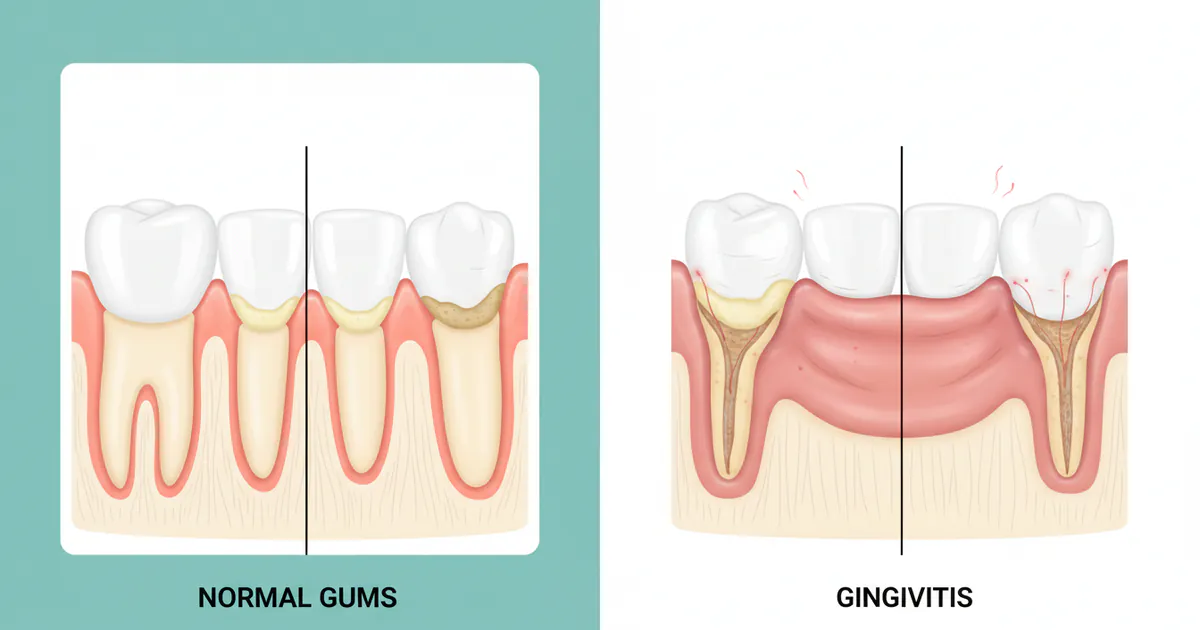
Normal Gums vs Gingivitis: Complete Comparison Guide
Did you know that nearly half of American adults over 30 show signs of gum disease, a condition that can range from mild inflammation to severe infection leading to tooth loss? Understanding the difference between healthy gums and those affected by early gum disease, known as gingivitis, is cruc
February 22, 2026
Can You Get Rid of Gingivitis
More than 50% of American adults aged 30 or older suffer from some form of gum disease, with gingivitis being the earliest and most common stage. This often silent condition, marked by inflammation of the gums, can seem daunting, leading many to wonder: can you get rid of gingivitis? The good ne
February 22, 2026
What Causes Receding Gums
Receding gums, a condition where the gum tissue surrounding the teeth pulls back or wears away, exposing more of the tooth or the tooth's root, affects a significant portion of the adult population in the United States. In fact, estimates suggest that **up to 88% of people over the age of 65 have on
February 22, 2026
Signs of Gingivitis: Complete Guide
Did you know that nearly half of American adults aged 30 and older suffer from some form of gum disease? While that statistic might sound alarming, the good news is that the earliest and most common stage, gingivitis, is entirely reversible. Recognizing the signs of gingivitis early is your
February 22, 2026