Root Planing
3,662 words · 12 min read
Quick Definition
A deep cleaning procedure that smooths the root surfaces of teeth below the gumline, removing bacterial deposits and creating a clean surface for gum tissue to reattach.
Root Planing: A Comprehensive Guide to Deep Cleaning for Gum Health
Short Definition: Root planing is a specialized deep cleaning procedure designed to meticulously smooth the root surfaces of teeth below the gumline, effectively removing bacterial deposits (plaque and calculus) and toxins. This process creates a clean, healthy surface that encourages gum tissue to reattach, reducing periodontal pockets and fighting periodontal disease.
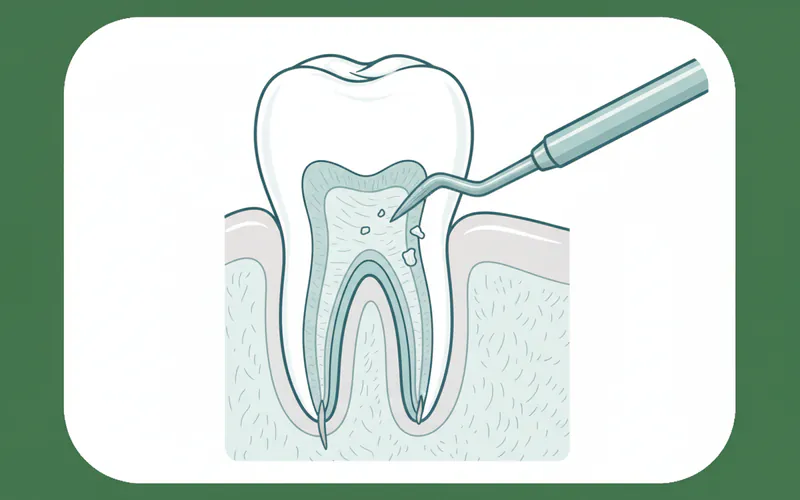
Introduction
Welcome to SmilePedia.net, your definitive resource for understanding crucial dental health procedures. Today, we delve into "root planing," a cornerstone treatment in the battle against periodontal disease. Often recommended when routine dental cleanings are insufficient, root planing goes beyond the surface to address the root causes of gum inflammation and infection.
Root planing, frequently performed in conjunction with scaling (the removal of plaque and calculus from above and below the gumline), is critical for halting the progression of gum disease, preventing tooth loss, and supporting overall systemic health. Untreated gum disease, which affects nearly half of US adults aged 30 and over (according to the CDC), has been linked to serious health conditions like heart disease, diabetes complications, and stroke. Understanding root planing is a vital step toward reclaiming and maintaining optimal oral health.
Key Takeaways:
- Root planing is a deep cleaning procedure targeting bacterial deposits and toxins on tooth root surfaces below the gumline.
- It is crucial for treating moderate to severe gingivitis and periodontitis, helping to prevent further bone loss and tooth mobility.
- The goal is to smooth root surfaces, allowing gum tissue to reattach and reduce periodontal pocket depth.
- Often performed with scaling, it typically requires local anesthesia and may be completed over multiple appointments.
- Success depends heavily on excellent home oral hygiene and regular follow-up care.
- Untreated periodontal disease, for which root planing is a primary treatment, can lead to tooth loss and impact systemic health.
Detailed Explanation
Root planing is not just a cleaning; it's a therapeutic intervention aimed at restoring gum health by directly addressing the bacterial infection and inflammation that define periodontal disease.
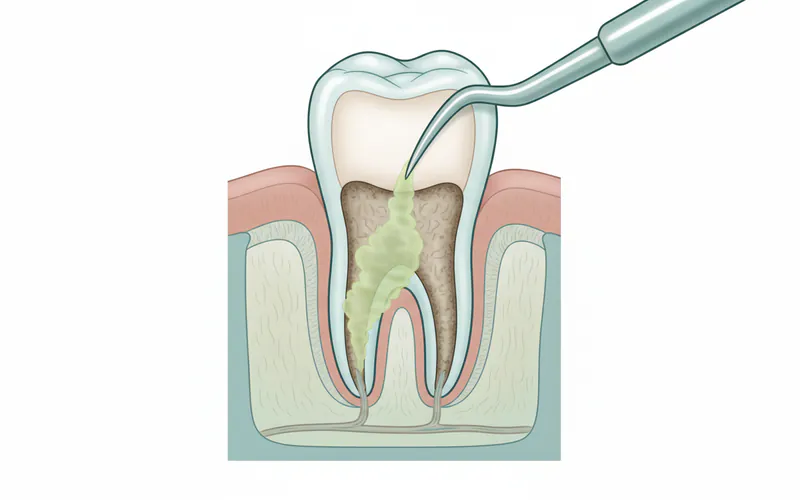
Types and Classifications of Root Planing
While "root planing" itself is a specific technique, the procedure can vary in its approach and adjunctive therapies:
- Manual Scaling and Root Planing: This traditional method utilizes specialized hand instruments called curettes to meticulously scrape away plaque, calculus, and bacterial toxins from the tooth roots. The curved tips of the curettes allow the dental professional to access and smooth the root surfaces effectively. This method offers excellent tactile sensitivity, allowing the practitioner to feel irregularities on the root surface.
- Ultrasonic Scaling and Root Planing: Ultrasonic scalers use high-frequency vibrations to dislodge plaque and calculus, combined with a water spray to flush away debris and cool the tip. While highly effective for initial debridement, manual curettes may still be used afterward to ensure thorough root smoothing and tactile refinement.
- Scaling and Root Planing (SRP) with Adjunctive Therapies: In many cases, root planing is combined with additional treatments to enhance its efficacy, especially for persistent infections:
- Localized Antibiotics: Antimicrobial agents (e.g., Arestin, PerioChip) can be placed directly into deep periodontal pockets after root planing. These slowly release medication over several days or weeks, targeting residual bacteria.
- Systemic Antibiotics: For more widespread or aggressive infections, a short course of oral antibiotics may be prescribed to supplement the local treatment.
- Laser Therapy: While not replacing root planing, certain dental lasers (e.g., Nd:YAG for LANAP protocol) can be used alongside or after root planing to reduce bacteria, remove diseased tissue, and promote tissue regeneration. It is often considered an adjunct or a specific approach to debridement in itself.
Causes and Risk Factors for Periodontal Disease (leading to Root Planing)
The primary cause of periodontal disease, which necessitates root planing, is the accumulation of bacterial plaque (a sticky film of bacteria called biofilm) on teeth, particularly along and below the gumline. If plaque is not consistently removed through daily brushing and flossing, it hardens into calculus (tartar), which provides a rough surface for more plaque to adhere, further irritating the gums.
Several factors can increase an individual's risk of developing or worsening periodontal disease:
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque to accumulate and mature.
- Smoking/Tobacco Use: This is one of the most significant risk factors. Smoking impairs the immune system, reduces blood flow to the gums, and hinders the healing process, making individuals up to 7 times more likely to develop periodontal disease.
- Diabetes: Individuals with uncontrolled diabetes are at a higher risk for infections, including gum disease. The elevated blood sugar levels can make existing gum disease harder to control and heal.
- Genetics: Some people are genetically predisposed to more severe forms of gum disease.
- Hormonal Changes: Fluctuations during pregnancy, puberty, menopause, or monthly menstruation can make gums more sensitive and susceptible to gingivitis.
- Certain Medications: Some drugs, such as oral contraceptives, antidepressants, and heart medications, can affect oral health, sometimes causing dry mouth or gum overgrowth.
- Compromised Immune System: Conditions like HIV/AIDS or treatments like chemotherapy can weaken the body's ability to fight off bacterial infections.
- Stress: Stress can weaken the immune system, making it harder for the body to fight off infection, including gum disease.
- Poor Nutrition: A diet lacking essential nutrients can compromise the immune system and make it harder for gum tissues to fight infection.
- Crowded or Misaligned Teeth: These can create areas that are difficult to clean, leading to plaque accumulation.
Signs and Symptoms to Watch For
Recognizing the early signs of gum disease is crucial for timely intervention. If you experience any of the following, consult your dentist:
- Red, Swollen, or Tender Gums: Healthy gums are firm and pink. Inflammation makes them appear puffy, red, and often sensitive to touch.
- Bleeding Gums: Gums that bleed easily during brushing, flossing, or even eating hard foods are a significant sign of gingivitis or early periodontitis.
- Persistent Bad Breath (Halitosis): Caused by bacteria accumulating in the mouth and releasing foul-smelling gases.
- Receding Gums: Gums pulling away from the teeth, making teeth appear longer. This exposes the root surfaces, which are more susceptible to decay and sensitivity.
- Pus Between Teeth and Gums: A clear sign of active infection.
- Loose or Shifting Teeth: As gum disease progresses, the supporting bone and ligaments deteriorate, leading to tooth mobility.
- Changes in Bite: Your teeth may not fit together as they once did, or your partial dentures may feel different.
Diagnosis Process — What Your Dentist Does
A thorough diagnosis is essential before recommending root planing. Your dental professional will typically perform the following:
- Medical History Review: To identify any systemic conditions or medications that could influence gum health.
- Visual Examination: The dentist will look for signs of inflammation, bleeding, calculus buildup, and gum recession.
- Periodontal Probing: Using a small, ruler-like instrument called a periodontal probe, the dentist measures the depth of the gingival sulcus (the space between the tooth and gum) around each tooth.
- Healthy pockets are typically 1-3 millimeters deep.
- Pockets of 4 millimeters or more often indicate gum disease and require deeper cleaning like root planing. Depths of 5-6 mm suggest moderate periodontitis, while 7 mm or more signify severe disease and potential bone loss.
- Dental X-rays: These images reveal the extent of bone loss around the teeth, which is a hallmark of periodontitis, and can show hidden calculus deposits.
Treatment Options with Pros, Cons, and Costs
Root planing is typically recommended for moderate periodontitis where periodontal pockets range from 4mm to 6mm or more, and there's evidence of bone loss.
A. Scaling and Root Planing (SRP)
- Pros:
- Non-surgical, less invasive than surgery.
- Effective at removing bacterial plaque and calculus below the gumline.
- Helps reduce periodontal pocket depths and inflammation.
- Can prevent further bone loss and tooth loss.
- Often the first line of treatment for moderate gum disease.
- Cons:
- May require multiple appointments (often by quadrant).
- Can cause temporary sensitivity and soreness.
- Not effective for very advanced or aggressive forms of periodontitis where surgical intervention is necessary.
- Requires consistent home care and follow-up.
- Costs: See "Cost Ranges" section below.
B. Adjunctive Therapies with SRP
- Localized Antibiotic Placement (e.g., Arestin, PerioChip):
- Pros: Targets specific, persistent infected pockets; simple, non-invasive application; extended bacterial kill.
- Cons: Additional cost; not a standalone treatment; potential for temporary mild irritation.
- Costs: $30 - $100 per site.
- Laser-Assisted New Attachment Procedure (LANAP): While a distinct procedure, LANAP is a type of periodontal treatment often compared to or used in conjunction with traditional SRP.
- Pros: Minimally invasive, preserves more gum tissue, less pain and faster recovery compared to traditional flap surgery, promotes bone regeneration.
- Cons: Higher cost, requires specialized training and equipment, not universally available.
- Costs: Often $4,000 - $8,000 for full mouth, usually more expensive than traditional SRP.
C. Surgical Interventions (When SRP is Insufficient)
If periodontal pockets are too deep (e.g., 7mm or more) or bone loss is extensive, surgical options may be considered after an initial course of SRP. These are not alternatives to root planing, but rather next steps when SRP alone is not enough.
- Flap Surgery (Pocket Reduction Surgery): The gums are folded back to allow for direct visibility and thorough cleaning of root surfaces and removal of diseased tissue. Bone reshaping may also occur.
- Bone Grafting: Used to regenerate lost bone.
- Guided Tissue Regeneration: Involves placing a membrane to guide the growth of new bone and gum tissue.
Step-by-Step: What to Expect During Treatment
Root planing is typically performed by a dentist or a dental hygienist under the supervision of a dentist. The procedure usually involves several steps:
- Numbing: Before starting, the dental professional will administer a local anesthetic to numb the area of your mouth being treated. This ensures you are comfortable and feel no pain during the procedure. Often, the mouth is divided into quadrants (upper left, upper right, lower left, lower right), and treatment is performed on one or two quadrants per appointment.
- Scaling: Using either ultrasonic instruments or hand curettes, the dental professional will first remove plaque and calculus from both above and below the gumline. This initial step is critical for removing the bulk of the bacterial deposits.
- Root Planing: Once the visible and readily accessible deposits are removed, the focus shifts to the root surfaces. The dental professional will carefully use hand curettes to smooth the rough areas on the tooth roots. This smoothing eliminates the microscopic crevices where bacteria can harbor and prevents them from easily reattaching. It also removes bacterial toxins embedded in the root surface.
- Irrigation/Rinsing: Throughout and after the procedure, the area may be rinsed with an antimicrobial solution to further reduce bacteria.
- Post-Procedure Instructions: You will receive detailed instructions on aftercare, including pain management, diet, and oral hygiene.
Recovery Timeline and Aftercare
Recovery from root planing is generally straightforward, but it requires diligent attention to aftercare.
- Immediately After: You may experience numbness for several hours due to the local anesthetic.
- First Few Days:
- Soreness and Tenderness: Your gums will likely be sore, tender, and possibly slightly swollen. This is normal and typically subsides within 1-3 days.
- Sensitivity: Teeth may be sensitive to hot, cold, or sweet foods and drinks, particularly in areas where roots were exposed. This can last for a few days to a couple of weeks.
- Bleeding: Minor bleeding may occur for a day or two.
- Pain Management: Over-the-counter pain relievers like ibuprofen (Advil, Motrin) or acetaminophen (Tylenol) are usually sufficient to manage discomfort.
- Diet: Stick to soft, easy-to-chew foods for the first few days. Avoid extremely hot, cold, spicy, or crunchy foods that could irritate your gums.
- Oral Hygiene:
- Continue gentle brushing and flossing, but avoid the treated areas vigorously for the first 24-48 hours.
- Rinse with warm salt water (1/2 teaspoon salt in 8 ounces of warm water) several times a day to aid healing and reduce inflammation. An antiseptic mouthwash may also be recommended.
- Follow-up Appointments: A follow-up visit, typically 4-6 weeks after the procedure, is crucial. The dentist or hygienist will re-evaluate your gum health, measure pocket depths, and check for signs of healing. This is also when "periodontal maintenance" cleanings are often initiated.
- Long-Term Maintenance: Successful root planing depends on consistent excellent home care and regular professional periodontal maintenance cleanings (typically every 3-4 months) to prevent the recurrence of disease.
Prevention Strategies
The best approach to root planing is to avoid needing it in the first place! Prevention is key:
- Brush Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste for at least two minutes each time.
- Floss Daily: Clean between your teeth once a day to remove plaque and food particles that your toothbrush can't reach.
- Regular Dental Check-ups and Cleanings: Visit your dentist for routine exams and professional cleanings typically every six months. If you have risk factors for gum disease, your dentist might recommend more frequent visits.
- Healthy Diet: Limit sugary foods and drinks, which contribute to plaque formation. Eat a balanced diet rich in vitamins and minerals.
- Quit Smoking: If you smoke or use tobacco, quitting is one of the most impactful steps you can take for your oral and overall health.
- Manage Systemic Diseases: Work with your doctor to control conditions like diabetes, which can significantly impact gum health.
Cost Ranges in the US (with/without Insurance)
The cost of root planing in the US can vary significantly based on several factors, including the number of teeth or quadrants treated, the severity of the disease, geographic location, and the dental provider.
- Cost Per Quadrant: Root planing is typically billed per quadrant of the mouth (upper left, upper right, lower left, lower right).
- Without Insurance: Expect to pay roughly $200 - $400 per quadrant. This means a full-mouth root planing (all four quadrants) could range from $800 to $1,600 or more.
- With Insurance: Most dental insurance plans offer coverage for root planing, as it's a therapeutic procedure for gum disease. They may cover 50% to 80% of the cost after your deductible is met. You would be responsible for the remaining co-pay. It's crucial to check your specific plan's benefits.
- Additional Costs:
- Local Anesthetic: Often included, but sometimes billed separately ($20 - $50).
- X-rays and Exam: Typically billed separately during the diagnostic phase ($100 - $250).
- Localized Antibiotic Placement: $30 - $100 per site.
- Follow-up Periodontal Maintenance: These ongoing cleanings are essential and typically cost $100 - $200 per visit, often covered at 50-80% by insurance.
Comparison Table: Treatments for Gum Health
| Feature | Routine Prophylaxis (Cleaning) | Scaling and Root Planing (SRP) | Periodontal Flap Surgery (e.g., Pocket Reduction) |
|---|---|---|---|
| Indication | Healthy gums or mild gingivitis | Moderate periodontitis | Severe periodontitis, deep pockets, bone loss |
| Goal | Prevent disease, remove supra-gingival plaque/calculus | Remove sub-gingival plaque/calculus, smooth roots, reduce pocket depth | Directly access roots, remove diseased tissue, reshape bone, reduce pockets |
| Depth of Cleaning | Above gumline and shallow pockets (<4mm) | Below gumline in deeper pockets (4-6mm+) | Direct access to root and bone; deep pockets (>6mm) |
| Invasiveness | Minimal | Moderate | High (surgical) |
| Anesthesia | Usually none or topical numbing | Local anesthetic (required) | Local anesthetic (required) |
| Appointments | 1 session (every 6 months) | 1-4 sessions (by quadrant) | 1-2 sessions per quadrant (surgical) |
| Recovery | Immediate | Mild soreness/sensitivity for a few days | Significant discomfort, swelling, longer recovery (weeks) |
| Cost (No Ins) | $80 - $150 | $200 - $400 per quadrant (full mouth $800-$1600+) | $500 - $1,500+ per quadrant (full mouth $2,000-$6,000+) |
| Insurance Cov | High (often 80-100%) | Moderate (often 50-80%) | Moderate (often 50-80%) |
| Next Step | Continued routine care | Periodontal maintenance cleanings (every 3-4 months) | Periodontal maintenance cleanings (every 3-4 months) |
For Parents / Pediatric Considerations
While root planing is commonly associated with adult periodontal disease, it's generally rare in children. Children typically do not develop the chronic, destructive forms of periodontitis that require root planing. However, certain rare conditions, such as early-onset aggressive periodontitis, can affect adolescents.
What parents should know:
- Focus on Prevention: Emphasize excellent oral hygiene from an early age. Teach children to brush twice daily and floss once a day.
- Regular Pediatric Dental Visits: Routine check-ups help detect any unusual gum inflammation (gingivitis) early.
- Watch for Signs: Be vigilant for signs like bleeding gums, persistent bad breath, or swollen gums, even in children. While often just gingivitis, it warrants a dental evaluation.
- Specific Conditions: If a child is diagnosed with a severe form of periodontitis, a pediatric dentist or periodontist will determine the appropriate course of action, which might, in rare cases, include a modified form of scaling and root planing. However, non-surgical approaches are always preferred for younger patients.
Frequently Asked Questions
How much does root planing cost?
Without insurance, root planing typically costs between $200 and $400 per quadrant. A full mouth procedure could range from $800 to $1,600 or more. With dental insurance, you can expect to pay a co-pay, as most plans cover 50% to 80% of the cost after your deductible is met. Additional costs may include exams, X-rays, and localized antibiotics.

Is root planing painful?
Thanks to local anesthetic, the root planing procedure itself should not be painful. You may feel pressure or vibrations, but no sharp pain. After the numbing wears off, it's common to experience some soreness, tenderness, and mild sensitivity for a few days. Over-the-counter pain relievers usually manage this discomfort effectively.
How long does root planing take?
The duration depends on the number of quadrants being treated and the severity of the calculus buildup. A single quadrant can take anywhere from 45 to 90 minutes. Because of the time involved and to ensure patient comfort, root planing is often performed over two to four separate appointments, treating one or two quadrants at a time.
Are there alternatives to root planing?
For mild gingivitis, excellent home oral hygiene and routine dental cleanings are sufficient. However, for established periodontitis with periodontal pockets 4mm or deeper, root planing is generally considered the gold standard non-surgical treatment. Alternatives for severe cases where root planing isn't enough include surgical interventions like flap surgery, bone grafting, or laser therapy (e.g., LANAP), which are more invasive but address advanced bone loss. Skipping treatment is not an alternative, as it will lead to worsening disease and tooth loss.
Does insurance cover root planing?
Yes, most dental insurance plans cover root planing. It is typically classified as a "major restorative" or "periodontal" procedure. Coverage usually ranges from 50% to 80% of the cost, though you will need to meet your deductible first. It's always best to contact your insurance provider directly to understand your specific benefits and any limitations.
How often do I need root planing?
Root planing is usually performed as an initial, one-time deep cleaning to treat existing moderate periodontal disease. Once the initial root planing is completed, the focus shifts to periodontal maintenance appointments. These specialized cleanings are typically recommended every 3 to 4 months (instead of the standard 6-month cleaning) to prevent the recurrence of gum disease and monitor your gum health.
Can root planing save loose teeth?
Root planing can absolutely help save teeth that are beginning to loosen due to periodontal disease. By removing the bacteria and toxins that are causing bone and tissue destruction, root planing helps to reduce inflammation, encourages gum tissue reattachment, and can stabilize teeth. While it may not completely tighten severely loose teeth, it can halt the progression of the disease that causes loosening and prevent further tooth mobility and eventual tooth loss.
What happens if I don't get root planing?
If diagnosed with periodontitis and you opt not to get root planing, the disease will likely progress. The bacterial infection will continue to destroy the supporting bone and ligaments around your teeth, leading to:
- Worsening gum inflammation, bleeding, and pain.
- Deepening periodontal pockets that are impossible to clean at home.
- Increased gum recession.
- More significant bone loss.
- Increasingly loose teeth.
- Eventual tooth loss.
- Potential impact on your overall systemic health, increasing the risk of conditions like heart disease, stroke, and uncontrolled diabetes.
When to See a Dentist
It is essential to schedule regular dental check-ups and cleanings, typically every six months, even if you don't notice any immediate problems. Many early signs of gum disease are subtle and best detected by a dental professional.
See a dentist sooner if you experience any of the following:
- Gums that bleed easily when brushing or flossing.
- Red, swollen, or tender gums.
- Persistent bad breath.
- Gums that are pulling away from your teeth (receding).
- Loose or shifting teeth.
- Pus between your teeth and gums.
- Any changes in the way your teeth fit together when you bite.
These symptoms indicate that you might have gingivitis or periodontitis and could benefit from evaluation for a deep cleaning procedure like root planing to protect your oral health and prevent more serious complications.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.