Curettage
4,749 words · 16 min read
Quick Definition
A periodontal procedure that involves scraping or cleaning the soft tissue lining of a diseased gum pocket to remove infected tissue and promote healing.
Curettage: A Comprehensive Guide to Gum Pocket Cleaning
Curettage, often a crucial step in managing periodontal disease, is a dental procedure focused on meticulously cleaning and removing infected tissue from deep gum pockets. While the term "curettage" itself may sound complex, it essentially refers to the careful scraping or debridement of the inflamed, soft tissue lining within a diseased gum pocket. This process is instrumental in halting the progression of gum disease, reducing inflammation, and promoting the healing and reattachment of the gums to the tooth roots. For anyone grappling with advanced gum issues or seeking to understand the intricacies of their periodontal treatment, grasping the concept of curettage is key to proactive oral health.
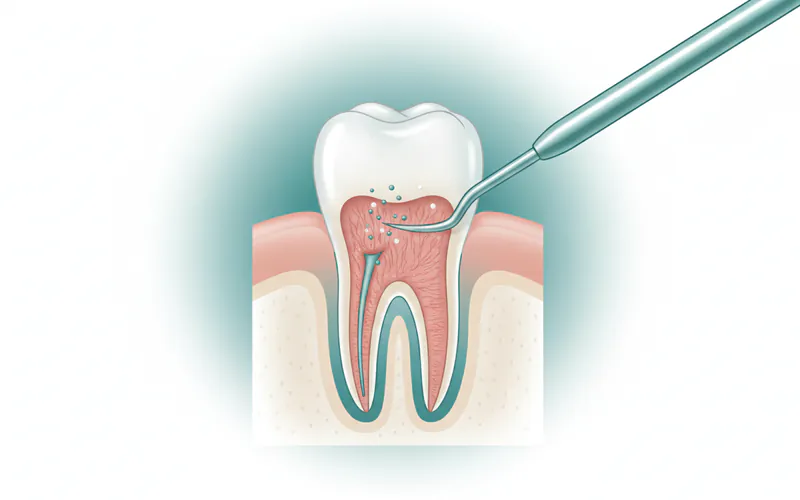
Periodontal disease, also known as gum disease, affects nearly half of all adults aged 30 and older in the United States, according to the Centers for Disease Control and Prevention (CDC). This widespread condition, if left untreated, can lead to severe issues like bone loss, tooth mobility, and ultimately, tooth loss. Curettage often plays a vital role within a broader treatment strategy, working to eliminate the bacterial strongholds and infected tissue that perpetuate the disease, thereby preserving oral health and the longevity of your teeth.
Key Takeaways:
- Curettage is a dental procedure involving the scraping of diseased soft tissue from deep gum pockets.
- It is primarily performed to treat periodontal disease and reduce inflammation.
- Often, curettage is an integral part of scaling and root planing (SRP) or more advanced surgical periodontal treatments.
- The goal is to remove infected tissue, promote healing, and facilitate gum reattachment to the tooth surface.
- Local anesthesia makes the procedure comfortable, with mild post-procedure soreness common.
- Prevention through excellent oral hygiene and regular dental check-ups is the best defense against conditions requiring curettage.
Detailed Explanation
Types and Classifications
The term "curettage" can refer to a specific action—the scraping away of diseased tissue—which is often performed as a component of larger periodontal procedures rather than a standalone treatment. Understanding its role within these classifications is important:
-
Gingival Curettage (Historical Context): Historically, gingival curettage specifically referred to the removal of the diseased soft tissue lining of the gum pocket (the epithelial lining and underlying connective tissue) without addressing the tooth root surface extensively. The rationale was to remove the inflamed tissue to allow for new, healthier tissue to form and potentially reattach. However, modern periodontology generally considers this a less effective standalone procedure because it often does not adequately address the bacterial biofilm and calculus (hardened plaque) on the root surface, which are the primary culprits of periodontal disease. Today, if performed, it's almost always done in conjunction with scaling and root planing (SRP).
-
Subgingival Curettage (Part of Scaling and Root Planing): This is the more common context in which the concept of curettage is applied today. During scaling and root planing, which is a deep cleaning procedure, the dentist or periodontist not only removes plaque and calculus from above and below the gum line (scaling) and smooths the root surfaces (root planing) but also meticulously cleans the inner lining of the gum pocket. The gentle scraping away of the diseased, inflamed tissue from the pocket wall during this process is essentially subgingival curettage. It's not usually billed as a separate procedure but is an integral part of thorough debridement.
-
Open Flap Curettage (Part of Periodontal Surgery): In more advanced cases of periodontal disease, surgical intervention may be necessary. Procedures like open flap debridement (or flap surgery) involve temporarily lifting a section of the gum tissue (a "flap") to gain direct access to the deeper root surfaces and underlying bone. Once the flap is lifted, the dentist can thoroughly clean the root surfaces, remove all plaque and calculus, and perform thorough debridement of any diseased soft tissue from the inner surface of the flap and the surrounding area. This debridement of soft tissue is a form of curettage, executed with direct visibility.
It's crucial to understand that curettage is rarely a primary treatment itself in contemporary practice. Instead, it describes a specific action of removing diseased soft tissue that is performed alongside or as part of other comprehensive treatments designed to eliminate the root causes of periodontal infection and promote healing.
Causes and Risk Factors
The primary cause of conditions requiring curettage is periodontal disease, which starts with the accumulation of bacterial plaque. If plaque isn't removed through regular brushing and flossing, it hardens into calculus (tartar). Bacteria in plaque and calculus release toxins that irritate the gingiva (gums), leading to inflammation (gingivitis).
If gingivitis is left untreated, it progresses to periodontitis. The inflammation causes the gums to pull away from the teeth, forming "pockets." These pockets deepen over time, providing more space for bacteria to thrive and further damage the supporting bone and tissue. Curettage targets these infected pockets.
Key risk factors that contribute to the development and progression of periodontal disease include:
- Poor Oral Hygiene: Inconsistent or ineffective brushing and flossing allow plaque and calculus to accumulate.
- Smoking/Tobacco Use: One of the most significant risk factors, smoking impairs the immune system's ability to fight gum infection and reduces blood flow to the gums, hindering healing.
- Genetics: Some individuals are genetically more susceptible to gum disease.
- Diabetes: People with diabetes are at a higher risk for developing infections, including gum disease, and healing is often compromised.
- Hormonal Changes: Fluctuations during pregnancy, puberty, menopause, or with the use of oral contraceptives can make gums more sensitive and prone to inflammation.
- Certain Medications: Some drugs, such as antidepressants, heart medications, and oral contraceptives, can cause dry mouth (xerostomia), which reduces saliva's protective effects, or lead to gum overgrowth (gingival hyperplasia).
- Stress: Stress can weaken the immune system, making it harder for the body to fight off infections.
- Poor Nutrition: A diet lacking essential nutrients can compromise the body's immune system and tissue health.
- Obesity: Research suggests a link between obesity and an increased risk of periodontal disease.
Signs and Symptoms to Watch For
Recognizing the signs of gum disease early is crucial for effective treatment, potentially preventing the need for more invasive procedures. If you notice any of these symptoms, it's time to see your dentist:
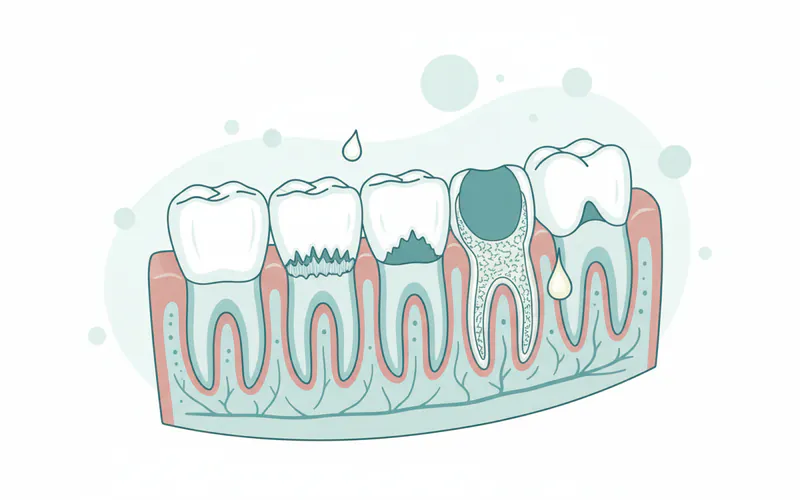
- Bleeding Gums: Gums that bleed easily when brushing, flossing, or even eating. This is often one of the earliest and most common signs.
- Red, Swollen, or Tender Gums: Healthy gums are firm and pink. Inflamed gums appear redder, puffy, and may be painful to the touch.
- Persistent Bad Breath (Halitosis): Caused by bacteria accumulating in the mouth and gum pockets.
- Receding Gums: Gums pulling away from the teeth, making teeth appear longer than usual. This exposes the root surfaces, which can be sensitive.
- Deep Pockets Between Teeth and Gums: As the disease progresses, the detachment of gums from teeth creates pockets that harbor bacteria. Your dentist measures these with a periodontal probe.
- Loose or Shifting Teeth: A sign of advanced bone loss, where the supporting structures around the teeth are weakened.
- Pus Between Teeth and Gums: Indicates an active infection.
- Changes in Bite: A change in how your teeth fit together when you bite down, or a change in the fit of partial dentures.
Diagnosis Process — What Your Dentist Does
Diagnosing periodontal disease and determining the appropriate course of treatment, including whether procedures involving curettage are necessary, involves a comprehensive evaluation by your dentist or a periodontist (a gum specialist).
- Comprehensive Oral Exam: The dentist will visually inspect your gums, teeth, and mouth for any signs of inflammation, bleeding, or other abnormalities.
- Periodontal Probing: This is a critical step. A small, ruler-like instrument called a periodontal probe is gently inserted into the space between your tooth and gum (gingival sulcus) to measure the depth of the gum pockets. Healthy pockets are typically 1-3 millimeters deep. Pockets deeper than 3-4 mm indicate gum disease, with deeper pockets suggesting more advanced disease. The dentist will measure pockets around all teeth and record the depths. Bleeding upon probing is also a significant indicator of inflammation.
- Dental X-rays: X-rays help visualize the bone levels supporting your teeth. They reveal any bone loss that has occurred due to periodontal disease, which is not visible during a clinical exam. This helps determine the severity and extent of bone damage.
- Review of Medical History: Your dentist will ask about your overall health, medications you're taking, and any lifestyle habits (like smoking) that could impact your gum health. This information is vital for understanding your risk factors and potential treatment responses.
Based on these findings, your dentist can accurately diagnose the stage of periodontal disease (gingivitis, mild, moderate, or severe periodontitis) and recommend the most suitable treatment plan.
Treatment Options with Pros, Cons, and Costs
As established, direct "curettage" is most often an integrated component of other treatments. The primary non-surgical treatment involving this action is Scaling and Root Planing (SRP), with surgical options being for more advanced disease.
1. Scaling and Root Planing (SRP)
- Description: This is a non-surgical, deep cleaning procedure performed under local anesthesia. It involves two main parts:
- Scaling: Removing plaque and calculus from above and below the gum line.
- Root Planing: Smoothing the root surfaces to remove bacterial toxins and rough spots, making it harder for plaque to reattach and promoting gum reattachment.
- Curettage Aspect: During SRP, the dentist also carefully debrides (scrapes) the diseased inner lining of the gum pocket, removing inflamed tissue to encourage healing.
- Pros:
- Non-surgical: Less invasive than surgery, minimal downtime.
- Effective: Can successfully halt the progression of early to moderate periodontitis.
- Cost-effective: Generally less expensive than surgical options.
- Comfortable: Performed under local anesthesia, so the procedure itself is not painful.
- Cons:
- Not suitable for advanced disease: May not be sufficient if pockets are excessively deep or bone loss is severe.
- Temporary sensitivity: Teeth and gums may be sensitive for a few days to weeks post-procedure.
- Gum recession: Some minimal gum recession can occur as gums heal and tighten.
- Cost (US Market): Typically ranges from $250 to $500 per quadrant (a quarter of your mouth, e.g., upper right). For a full mouth, this can range from $1,000 to $2,000 or more, depending on the severity of the disease and the dental practice's fees. Insurance often covers a significant portion (50-80%) after a deductible.
2. Surgical Periodontal Procedures (e.g., Open Flap Debridement)
- Description: For advanced periodontitis, when SRP alone isn't enough, surgical options are considered. During procedures like open flap debridement, the gum tissue is temporarily lifted (a flap) to provide direct access to the deeper root surfaces, bone, and infected tissue. This allows for thorough cleaning and debridement of plaque, calculus, and diseased tissue (including the curettage of the soft tissue lining) under direct vision. Bone reshaping or grafting may also be performed.
- Pros:
- Access for severe disease: Allows for thorough cleaning and treatment in very deep pockets or areas with significant bone loss.
- Long-term effectiveness: Can achieve better long-term results for advanced cases by thoroughly removing infection and allowing for proper healing.
- Bone regeneration (if grafting included): Can help rebuild lost bone structure.
- Cons:
- More invasive: Involves surgical incisions and sutures.
- Longer recovery: More significant post-operative discomfort and healing time.
- Potential for greater gum recession: More visible gum recession is common, which can increase tooth sensitivity and change aesthetics.
- Higher cost: Significantly more expensive than SRP.
- Cost (US Market): Can range from $1,000 to $4,000 per quadrant or more, depending on the complexity, extent of bone work, and location. Full mouth surgical treatment could easily exceed $10,000. Insurance coverage varies but usually covers a percentage, often less than for SRP.
Comparison Table: Scaling & Root Planing vs. Periodontal Surgery
| Feature | Scaling & Root Planing (SRP) | Periodontal Surgery (e.g., Open Flap) |
|---|---|---|
| Invasiveness | Non-surgical | Surgical (involves incisions) |
| Curettage Role | Integral part of debridement within deep cleaning | Integral part of debridement under direct vision |
| Anesthesia | Local anesthesia | Local anesthesia, sometimes sedation |
| Target Disease | Mild to moderate periodontitis | Moderate to severe periodontitis, deep pockets, significant bone loss |
| Recovery | Mild soreness, sensitivity 1-2 weeks | More significant discomfort, swelling, 2-4 weeks or longer |
| Cost (per quadrant) | $250 - $500 | $1,000 - $4,000+ |
| Insurance | Often 50-80% coverage | Varies, often 30-60% coverage |
| Outcomes | Reduces inflammation, decreases pocket depths, gum reattachment | Reduces inflammation, greatly reduces pocket depths, tissue repair |
Step-by-Step: What to Expect During Treatment
Let's focus on what to expect during a Scaling and Root Planing (SRP) procedure, as this is where the action of curettage is most commonly integrated.
- Anesthesia: Before starting, your dentist or hygienist will administer a local anesthetic to numb the specific area (or quadrant) being treated. This ensures you are comfortable and feel no pain during the procedure.
-
- Scaling: Using specialized dental instruments (ultrasonic scalers and/or hand instruments), the clinician will meticulously remove all plaque and hardened calculus from above and below the gum line. This involves reaching deep into the gum pockets to thoroughly clean the tooth surfaces.
- Root Planing: Once the calculus is removed, the root surfaces of your teeth will be carefully smoothed. This process removes bacterial toxins and any rough spots on the root that could harbor bacteria, making it difficult for plaque to adhere and promoting the reattachment of the gum tissue to the cleaner, smoother root surface.
- Curettage (Soft Tissue Debridement): As part of the thorough cleaning of the gum pocket, the clinician will gently scrape away any diseased, inflamed, and ulcerated soft tissue lining the inside of the pocket. This action, often referred to as curettage, helps remove the infected tissue and stimulates the growth of new, healthy gum tissue.
- Irrigation: The pockets may be rinsed with an antimicrobial solution to further reduce bacteria.
- Post-Procedure Instructions: Once the cleaning is complete, you will receive detailed instructions on how to care for your mouth during the recovery period, including dietary advice, oral hygiene practices, and pain management.
The procedure is usually performed quadrant by quadrant or on half of the mouth at a time, allowing for proper anesthesia and thoroughness. Multiple appointments may be needed for a full mouth treatment.
Recovery Timeline and Aftercare
Recovery from a procedure involving curettage (most commonly SRP) is generally straightforward, but it's important to follow your dentist's aftercare instructions closely for optimal healing.
- Immediately After (First Few Hours):
- The numbness from local anesthesia will gradually wear off.
- You may experience mild soreness, tenderness, and slight bleeding from the treated gums.
- Avoid eating until the numbness completely wears off to prevent accidental biting of your cheek or tongue.
- First Few Days (2-3 days):
- Discomfort: Mild to moderate discomfort is common. Over-the-counter pain relievers (like ibuprofen or acetaminophen) can effectively manage this.
- Sensitivity: Teeth may be sensitive to hot, cold, or sweet stimuli, especially if roots were exposed. This usually subsides over time.
- Swelling: Some minor gum swelling or bruising is possible but usually resolves quickly.
- Diet: Stick to soft foods that are easy to chew. Avoid very hot, cold, spicy, or crunchy foods that could irritate the healing gums.
- Oral Hygiene: Continue to brush your teeth gently, avoiding vigorous scrubbing of the treated areas. Your dentist may recommend a soft-bristled toothbrush and an antiseptic mouth rinse (like chlorhexidine) for a short period to help keep bacteria at bay. Avoid flossing the treated areas for the first 24-48 hours, then resume gently as tolerated.
- First Few Weeks (1-4 weeks):
- Healing: Gums will begin to heal, tighten, and reduce inflammation. Pocket depths will ideally decrease as the gums reattach to the tooth surfaces.
- Sensitivity: Tooth sensitivity should gradually diminish. Your dentist might recommend a desensitizing toothpaste.
- Follow-up: A follow-up appointment is typically scheduled a few weeks after the procedure to check the healing progress, measure pocket depths, and assess your oral hygiene.
- Long-Term Aftercare:
- Excellent Oral Hygiene: This is paramount. Brush twice daily with a soft-bristled brush, floss daily, and use any recommended interdental cleaners.
- Regular Dental Check-ups and Cleanings: Your dentist or periodontist will likely recommend more frequent maintenance cleanings (periodontal maintenance) every 3-4 months to prevent recurrence of the disease.
- Avoid Tobacco: If you smoke or use tobacco products, quitting is the single most important step you can take to maintain your periodontal health.
Prevention Strategies
Preventing periodontal disease is the most effective way to avoid the need for procedures like curettage. Good oral hygiene and healthy lifestyle choices are your best defense:
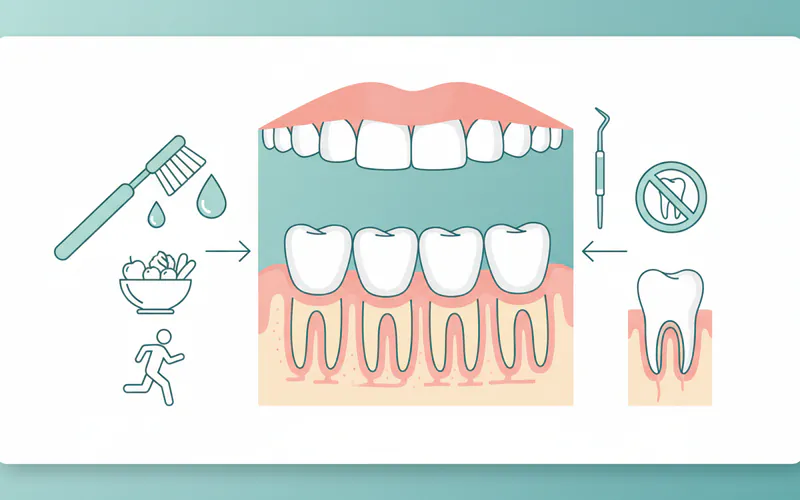
- Brush Your Teeth Twice Daily: Use a soft-bristled toothbrush and fluoride toothpaste. Brush for at least two minutes, covering all tooth surfaces and the gum line. Consider an electric toothbrush for enhanced cleaning.
- Floss Daily: Flossing removes plaque and food particles from between your teeth and under the gum line where your toothbrush can't reach. This is critical for preventing plaque buildup in these vulnerable areas.
- Use an Antimicrobial Mouthwash: While not a substitute for brushing and flossing, an antimicrobial mouthwash can help reduce bacteria in the mouth.
- Regular Dental Check-ups and Professional Cleanings: Visit your dentist for routine check-ups and professional cleanings at least twice a year, or more frequently if you have risk factors for gum disease. These appointments allow for early detection and removal of plaque and calculus.
- Quit Smoking/Tobacco Use: Tobacco is a major risk factor for periodontal disease and significantly hinders healing.
- Manage Systemic Diseases: If you have conditions like diabetes, managing them effectively will improve your overall health, including your oral health.
- Eat a Balanced Diet: A diet rich in vitamins and nutrients supports a healthy immune system and strong gum tissue. Limit sugary foods and drinks that promote bacterial growth.
- Avoid Teeth Grinding/Clenching: Chronic grinding or clenching can put excessive force on supporting tissues and accelerate bone loss.
Cost Ranges in the US (with/without insurance)
The cost of dental procedures involving curettage varies based on the extent of the disease, the type of procedure (e.g., SRP vs. surgery), the specific dental office, and geographic location.
- Scaling and Root Planing (SRP): This is typically billed per quadrant of the mouth (upper right, upper left, lower right, lower left).
- Without Insurance: Expect to pay between $250 to $500 per quadrant. A full mouth SRP could therefore range from $1,000 to $2,000 or more.
- With Insurance: Most dental insurance plans classify SRP as a major restorative procedure, covering 50% to 80% of the cost after your deductible has been met. For example, if a quadrant costs $350 and your insurance covers 80%, you might pay $70. However, annual maximums apply.
- Periodontal Surgery (Open Flap Debridement, etc.): These procedures are more complex and thus more expensive.
- Without Insurance: Costs can range significantly, from $1,000 to $4,000 or more per quadrant, depending on whether bone grafts or other complex procedures are involved. A full mouth surgical treatment could easily exceed $10,000 and reach $20,000+.
- With Insurance: Insurance coverage for surgical procedures varies widely. Some plans may cover 30% to 60% of the cost, but often with higher deductibles and strict annual maximums. You will likely have a substantial out-of-pocket expense.
Important Notes on Cost:
- Consultation: Always get a detailed treatment plan and cost estimate from your dentist before proceeding.
- Payment Plans: Many dental offices offer payment plans or work with third-party financing options (e.g., CareCredit) to help manage costs.
- HSA/FSA: If you have a Health Savings Account (HSA) or Flexible Spending Account (FSA), these funds can be used for dental procedures.
- Periodontal Maintenance: After initial treatment, you will likely need more frequent "periodontal maintenance" cleanings (e.g., every 3-4 months), which have their own costs, typically $100-$200 per visit without insurance, and usually covered by insurance at a higher percentage.
For Parents / Pediatric Considerations
While periodontal disease requiring procedures like curettage is far less common in children than in adults, it's not entirely absent. Children and adolescents can develop various forms of gum disease:
- Gingivitis: This is very common in children, often due to inadequate brushing and flossing. It presents with red, swollen, bleeding gums. Good oral hygiene typically reverses gingivitis.
- Aggressive Periodontitis: In rare cases, some adolescents can develop localized or generalized aggressive periodontitis, which can lead to significant bone loss and deep pockets. This often has a genetic component.
- Periodontitis associated with systemic conditions: Children with certain systemic diseases (e.g., diabetes, Down syndrome) or immune deficiencies are at higher risk.
Curettage in Pediatric Dentistry:
- Rare as a standalone procedure: Traditional gingival curettage is rarely performed on children. The focus is almost always on thorough scaling and root planing to remove plaque and calculus.
- Emphasis on prevention: For children, the strongest emphasis is on prevention through excellent daily oral hygiene, regular dental check-ups, and early intervention for gingivitis.
- Deep Cleaning (Scaling and Root Planing): If an adolescent develops localized aggressive periodontitis with deep pockets, a procedure akin to scaling and root planing might be performed. During such a procedure, the debridement of any diseased soft tissue lining the pocket would be an integral part of the thorough cleaning, similar to adults. However, the term "curettage" itself is less frequently used in direct reference to pediatric treatment plans.
- Monitoring: Dentists closely monitor gum health in children and adolescents during routine check-ups, using periodontal probing when appropriate for older children or those with risk factors.
Parents should ensure their children establish good oral hygiene habits early on and schedule regular dental visits. Any signs of red, swollen, or bleeding gums, or persistent bad breath in a child, warrant a visit to the dentist.
Frequently Asked Questions
Is curettage painful?
The procedure itself, typically performed as part of scaling and root planing, is not painful because local anesthesia is administered to numb the treated area. You might feel pressure or a scraping sensation, but no sharp pain. After the anesthesia wears off, it's common to experience mild to moderate soreness, tenderness, and some sensitivity for a few days to a week. This discomfort can usually be managed effectively with over-the-counter pain relievers.
How long does a curettage procedure take?
The duration depends on the extent of the area being treated. Since it's often part of scaling and root planing, the procedure is typically performed on one or two quadrants of the mouth per appointment. Each quadrant can take anywhere from 30 minutes to an hour, sometimes longer for very severe cases. A full mouth treatment usually requires two to four appointments, each lasting approximately 1-2 hours.
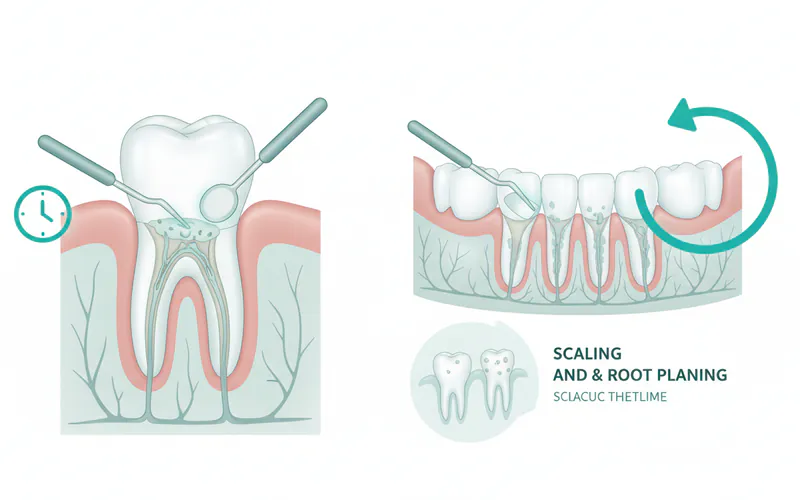
What are the alternatives to curettage?
The "alternatives" primarily depend on the stage of your periodontal disease and what aspect of curettage you're considering.
- For early gum disease (gingivitis): Regular professional cleanings, diligent brushing, and flossing are usually sufficient.
- For moderate periodontitis (where SRP is indicated): If the soft tissue debridement aspect (curettage) is considered, the primary alternative might be laser therapy which can also remove diseased tissue and sterilize pockets, sometimes with faster healing. In some cases, localized antibiotics (gels or chips placed in pockets) may be used as an adjunct. However, the foundational treatment for deep pockets remains the mechanical removal of plaque and calculus via scaling and root planing.
- For advanced periodontitis: If SRP with its integrated curettage isn't enough, surgical options like open flap debridement, guided tissue regeneration, or bone grafting become the next step. These procedures also involve thorough debridement, often more extensive than non-surgical curettage.
Does dental insurance cover curettage?
Dental insurance typically covers procedures where curettage is an integral part. Most commonly, this refers to scaling and root planing (SRP), which is usually categorized as a "major restorative" procedure. Insurance plans often cover 50% to 80% of the cost of SRP after a deductible. For surgical procedures that include extensive debridement/curettage, coverage may be lower, typically 30% to 60%, and subject to annual maximums. Always check with your specific insurance provider for detailed coverage information.
What's the difference between scaling and root planing and curettage?
Scaling and root planing (SRP) is a comprehensive deep cleaning procedure.
- Scaling focuses on removing plaque and calculus from the tooth surface, both above and below the gum line.
- Root planing involves smoothing the tooth root surfaces to remove bacterial toxins and prevent plaque reattachment.
- Curettage refers specifically to the action of scraping away the diseased, inflamed soft tissue lining the inside of the gum pocket. In modern practice, this debridement is considered an integral part of a thorough SRP or other periodontal surgical procedures, aiming to promote healing and reattachment of healthy gum tissue. So, while distinct in definition, curettage is often integrated within SRP, not usually a separate, standalone procedure.
How often is curettage needed?
Curettage, as a specific action within a procedure like SRP, is not a routine maintenance treatment. It's performed when active periodontal disease with deep pockets and infected tissue is present. Once the initial treatment is complete, the goal is to prevent recurrence through excellent daily oral hygiene and periodontal maintenance appointments. These maintenance appointments, typically scheduled every 3-4 months, involve cleaning the teeth and shallow pockets but generally do not require repeated, aggressive curettage unless the disease recurs or new pockets form.
Can curettage reverse gum disease?
Curettage, as part of a comprehensive periodontal treatment, can effectively arrest the progression of gum disease, reduce inflammation, decrease pocket depths, and promote healing and some degree of reattachment of the gums to the tooth roots. It eliminates the infection and creates an environment for healing. However, it cannot "reverse" significant bone loss or extensive tissue damage that has already occurred. The goal is to stabilize the condition, preserve remaining bone and teeth, and prevent further deterioration.
Are there any side effects?
Common side effects include:
- Sensitivity: Increased tooth sensitivity to hot, cold, or sweets, especially if root surfaces are exposed. This usually improves over weeks.
- Soreness and tenderness: Gums may be sore and tender for several days.
- Mild bleeding: Some light bleeding can occur for a day or two.
- Swelling: Minor gum swelling or bruising is possible.
- Gum recession: As the inflamed gums heal and tighten, some degree of gum recession (gums pulling back slightly) can become more noticeable, which is a natural part of the healing process.
Serious side effects like infection are rare, especially when following aftercare instructions.
When to See a Dentist
It is always better to address dental concerns sooner rather than later.
See a dentist for routine care if:
- It has been more than six months since your last dental check-up and cleaning.
- You notice any of the general signs of gingivitis, such as gums that are slightly redder than usual, or minor bleeding when you brush or floss. Early intervention can prevent the progression to more serious periodontal disease.
Seek prompt dental attention if you notice any of these signs, which may indicate a need for procedures involving curettage:
- Persistent bleeding gums: Gums that bleed easily and consistently, not just occasionally.
- Red, swollen, or tender gums: Gums that are constantly inflamed and painful.
- Persistent bad breath that doesn't go away with brushing or mouthwash.
- Visible gum recession: Your teeth appear longer than before, or you notice a gap forming between your teeth and gums.
- Loose or shifting teeth: This is a sign of advanced periodontal disease and requires immediate attention to prevent tooth loss.
- Pus between your teeth and gums.
- Any noticeable changes in your bite or the fit of partial dentures.
- Pain or discomfort in your gums or teeth that doesn't subside.
Your dentist can accurately diagnose the problem and recommend the most appropriate treatment, guiding you toward optimal oral health and preventing further complications.
Medical Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified dental professional for diagnosis and treatment. Do not delay seeking professional advice because of something you read on this website.